Version No Authored/Reviewed by Review Date 1.0 Carol Newman / Caroline Fox January Carol Newman October 2011
|
|
|
- Felicia Lyons
- 6 years ago
- Views:
Transcription
1 Guideline for transferring Children (0-16yrs) Guideline Register no Status: Public Developed in response to: Good practice Contributes to CQC Outcome Outcome 4 Consulted With Individual/Body Date Alison Cuthbertson / Miss Clinical Director for Women, Children & October 2014 Rao Sexual Health Directorate Children s Urgent & Emergency Group October 2014 Consultant Paediatricians October 2014 Mel Hodge Senior Sister Phoenix Children s Ward October 2014 Brian McConville Lead Nurse Children & Young People October 2014 Sue Wright Named Nurse Safeguarding Children October 2014 Helen Clarke Clinical Audit Lead October 2014 Victoria Machell Children s Nurse October 2014 Sarah Moon Specialist Midwife Guidelines & Audit October 2014 Professionally Approved By Dr Job Cyriac October 2014 Version Number 3.1 Issuing Directorate Children and Young People Ratified by Document Ratification Group Chairmans Action Ratified on 20th November 2014 Exec Group Sign Off December 2014 Next Review Date October 2017 Author/Contact for Information Andrea Stanley Policy to be followed by (target staff) All Healthcare professionals Distribution Method Intranet & Website Related Trust Policies (to be read in conjunction with) Hand Hygiene 11042: Adult Patient Transfer policy 11046: Observation policy CYP 04184: Blood transfusion policy Version No Authored/Reviewed by Review Date 1.0 Carol Newman / Caroline Fox January Carol Newman October to include informing GOSH of any child on a Carol Newman, Dr M Datta, October 2012 Child Protection Plan Sue Wright 3.0 Andrea Stanley October Flow chart for transfer of a child to a paediatric tertiary centre added Appendix C. Appendices C-F reordered as D-G Andrea Stanley 3 rd September 2015
2 Index 1.0 Purpose 2.0 Scope 3.0 Background 4.0 Roles and Responsibilities 5.0 Planning the Transfer 6.0 Moving and transferring critically ill children (Level 1 & Level 2) 7.0 Time critical transfers e.g. Head injuries & cranial bleeds 8.0 Moving and transferring children at Level Moving and transferring children at Level Moving and transferring children at Level Preparation for transfer 12.0 Observation during transfer 13.0 Staff training 14.0 Infection prevention 15.0 Equality and Diversity 16.0 Audit and Monitoring 17.0 Communication 18.0 References 19.0 Appendices Appendix A: Assessment tool for the safe transfer of children and young people Appendix B: Guidance on resources required for transfer Appendix C: Flow chart for transfer of a child to a paediatric tertiary centre Appendix D: Transfer checklist Appendix E: Nurse Transfer letter Appendix F: Time Critical Transfer Appendix G: Transfer and documentation requirements specific to each type of transfer Appendix H: Equality Impact Assessment 2
3 1.0 Purpose 1.1 Infants, children and young people requiring transfer either within the hospital or outside of the hospital to other providers of care have specific needs not fully addressed by the Trusts patient transfer policy. 1.2 The purpose of this policy and its supportive documents is to ensure safe and appropriate transfer of the patient with minimal risk. The aim is to clarify the clinical accountability of the nursing staff, medical team and supportive staff who are responsible for the patient s care to ensure that safe appropriate transfer of patients does occur and their care continues with minimal interruption and risk. 1.3 All patients within Mid-Essex Hospitals Trust that require transfer from one area to another either internally or externally must have the appropriate documentation completed to ensure that patient care is not compromised as a result of the transfer. 2.0 Scope 2.1 This guideline applies to all staff, professional, administrative, bank, agency and locum who may be involved in the transfer of sick infants and children either within the hospital or outside of the hospital to other providers of care. 2.2 This policy is to be used for all types of hospital transfers. 2.3 This document outlines the procedure for the transfer of all patients both within the hospital and outside of the hospital to other providers of care. 3.0 Background 3.1 Advances in technology and differing service provision means it is increasingly common for sick children to be transferred between hospital facilities for different elements of their care. It is important to ensure that guidelines are available to make sure that patients, and their records, are transferred safely. 3.2 Maintaining the well being of an acutely ill child is the principle concern. However, there are more factors to be considered: Nursing staff Medical staff Ambulance support Planned or Emergency transfer Documentation All necessary medicines and equipment Parental involvement 3.3 The referring physician assesses and initiates the need for the transfer of the child / young person, deciding on the appropriate level of transfer need required i.e. 1-5 (Refer to appendix A). The level of transfer required should match the patients identified needs and any potential needs that could occur during transportation. 3.4 The assessment of the level of transfer of the child does not depend on the destination for example inter or intra hospital but on the clinical need or dependency of the child (refer to Appendix A) 3
4 3.5 Stabilisation of the patient should include evaluation and initiation of treatment to ensure that transport will not result in death or loss of or serious impairment of bodily functions, (within reasonable medical probability). This should include the establishment and securing of appropriate intravenous (or equivalent) lines prior to transport. 4.0 Roles and Responsibilities 4.1 Chief Executive The Chief Executive is responsible for ensuring that processes are in place and are working. This responsibility is delegated to the Chief Medical Officer and Chief Nurse. 4.2 Chief Medical Officer and Chief Nurse The Chief Medical Officer and Chief Nurse are responsible for ensuring that systems are in place to support the implementation of this policy. 4.3 Heads of Nursing and Clinical Directors The Heads of Nursing and Clinical Directors are responsible for ensuring that systems are in place to support the implementation of this policy. 4.4 Medical and Nursing Staff All medical and nursing staff have a responsibility to ensure they understand this policy and act on its contents in an appropriate way. 5.0 Planning the transfer 5.1 The basic principles of good transport should be applied to all sick children moved within and between hospitals, whether or not a specialist team is involved. Effective preparation and planning are the keys to safe, successful, smooth transport of ill children. This will ensure that the right patient is taken at the right time by the right people to the right place by the right form of transport and receives the right care throughout. 5.2 Important considerations: How urgent is the transfer? Is the child in optimal condition for transfer? Does the benefit of transfer outweigh the risks involved? Who are the most appropriate people to transfer this child? What type and mode of transfer is required for this child? 5.3 It is essential to evaluate, resuscitate and stabilise a child s condition before moving him or her no child must be stabilised on the way. 5.4 Before the transfer of a child can take place the level of risk and the type of transfer that is required should be determined by senior medical and senior nursing staff. An assessment should be undertaken using the transfer guidance tool (refer to appendix A, B & C) to ascertain which level of transfer is appropriate and what 4
5 considerations should be made for that transfer including mode of transport, equipment required and transfer personnel. The decision and level of transfer to be undertaken should be documented in the patients notes. 6.0 Moving and transferring critically ill children (Level 1 and Level 2) 6.1 For all children assessed as a level 1 (Red) transfer, the on-call consultant paediatrician and attending anaesthetist will formulate a joint management plan. Discussion may need to take place with the Children s Acute Transport Service (CATS) on the appropriate mode of transport for the child and optimal PICU destinations. 6.2 Children may move between level 1 & level 2 during stabilisation as their condition fluctuates. Reassessment of the child s condition will ensure that the child is moved to the most appropriate destination in the safest manner 6.3 When a decision is made to transfer a critically ill child to a paediatric intensive care unit at another hospital CATS should be contacted at the earliest opportunity to allow a rapid response. It is important that they are kept updated of the child s progress as deterioration in the child s condition may prompt a higher urgency category and elicit earlier mobilisation of the retrieval team. 6.4 For non-intubated high dependency children a discussion should take place with the Children s Acute Transport Service (CATS) on the appropriated mode of transport for the child. CATS generally will not transfer high dependency patients but may be able to offer advice. 6.5 Any such child with actual or potential risk of significant airway, breathing or circulatory compromise must remain on the ward for further or continued assessment and stabilisation (CEWT score of a red 3 or 4 and above). 6.6 If a child meets HDU criteria and needs to be transferred to another hospital, appropriate preparations need to take place which should include decisions about personnel, equipment and mode of transport. 7.0 Time critical transfers e.g. Head Injuries and cranial bleeds (Appendix F) 7.1 All these patients should be considered to be either a level 1 or a level 2 transfer. 7.2 The consultant paediatrician and attending anaesthetist will formulate a joint management plan. The main thrust of the plan should be to provide the appropriate intensive care support and rapid transfer within the time critical period to a Paediatric Intensive Care Unit. 7.3 All patients should be transferred by staff trained in Advanced Paediatric Life Support (APLS). Assess and transfer as Level 1 (red). 7.4 The Equipment and Drugs Transfer bags and appropriate electrical equipment (e.g. infusion pumps and monitoring equipment) should be taken when accompanying the patient. 5
6 8.0 Moving and transferring children at Level Children who are assessed as level 3 have the potential for deterioration. 8.2 Children should be assessed and stabilised before transfer takes place. It is not appropriate to transfer sick unstable children. 8.3 All children assessed as a level 3 type transfer may need to be referred to the paediatric registrar on-call. Further assessment and stabilisation by senior paediatric medical staff will help to identify those at greater risk of airway, breathing or circulatory compromise who may have the potential for deterioration during transfer. 8.4 Any such child with actual or potential risk of significant airway, breathing or circulatory compromise must remain in the department/ward for assessment and stabilisation (CEWT score of a red 3 or 4 and above). 8.5 These children should be reviewed by middle grade staff or consultant, if present. Discuss these cases with anaesthetic staff if appropriate. The consultant paediatrician can be contacted directly by the staff as soon as possible to discuss further management of these critically ill children if the on call registrar is not available. 8.6 Once a decision has been taken that the child is stable for transfer it is the responsibility of the registrar to communicate all relevant information to the nursing staff on the ward. 8.7 The original notes or other documentation must be transferred with the patient. 9.0 Moving and transferring children at Level Stable children with no airway or cardiovascular compromise but requiring continuous monitoring of physiological parameters are transferred as level 4. These may include one of the following interventions: Operative intervention Received sedation / opiates Condition may change at short notice e.g. head injury Condition may reasonably evolve e.g. allergic reaction Received some from of resuscitation 9.2 A joint decision should be made between the registrar and nursing staff about the appropriate mode of transfer and escort e.g. moving to and back from theatre, imaging, stable children from A&E and OPD at tertiary hospitals. All transfers must take place in accordance with Appendix A, B & C 9.3 The registrar should make sure that the transfer is appropriate and the transfer is made in the safest possible mode. 9.4 If additional medical staff is thought to be necessary careful consideration should be given regarding the appropriateness of the transfer. 6
7 10.0 Moving and transferring children at Level Stable patient with no airway or cardiovascular compromise and not requiring continuous monitoring of physiological parameters, but requiring hospitalisation or investigation away from department 10.2 Well children who only need Specialist opinion and/or a planned elective admission can be sent in parent s car/by public transport 11.0 Preparation for Transfer (transfer requirements and documentation to accompany the patient) 11.1 Prior to all transfers, arrangements should be made for admission to the receiving hospital and / or ward The nurse caring for the child should ensure that the appropriate planning takes place For high dependency transfers to another hospital the nurse in charge with the consultant on call is responsible for ensuring that the nurse transferring the child is experienced in out of hospital transfers, and suitably experienced in the child s condition Any child that requires HDU level care requires a doctor and nurse escort. Consider the potential for the child s condition to deteriorate en route, discuss with the consultant on-call and consider discussing with CATS who may be able to give advice with out of hospital transfers After discussion with the on-call consultant consider the need for the consultant to come in to cover the registrar if they are required to transfer the child to another hospital If there are concerns or further advice is required for the planned transfer discuss with the co-ordinator and/or on-call manager If nursing staff levels are insufficient to permit the safe out of hospital transfer of the child discuss with the co-ordinator and/or on-call manager Inform the child and family of the reason for the transfer and obtain their verbal consent Arrange ambulance or porters depending on the destination. Ensure that all other necessary preparations are made prior to arranging for transport Check all equipment required for the transfer, is available and in working order. Batteries should be fully charged and that there is enough oxygen to last during the transfer All appropriate notes, x-rays, imaging, blood results and charts should be photocopied and sent with the child 7
8 11.12 If blood products need to be transferred with the patient then this should be done following the Trusts Blood Transfusion Policy If the patient has any medicines currently prescribed for them, then these should be checked against the patient prescription sheet before being transferred with the patient Appropriate monitoring should be attached to the patient if required. Monitors should be secured appropriately and not rested on the trolley, bed or patients knee. Infusion devices should be attached to a drip pole and not laid on the trolley or bed with the patient. They should be at or below heart level Clinical observations should be recorded prior to transfer and Children s Early Warning Scoring under taken in order to establish child/young persons clinical status. Transfer should be delayed if these give cause for concern Prior to leaving the clinical area the transferring nurse will check that the patient is appropriately clothed for the transfer and bedding supplied as necessary to prevent heat loss and maintain the patients dignity during the journey The child s property should be placed in a bag ready for transfer and given to the parent or carer if they are present, (or transferred directly with the child if not present) Where possible the parent/carer should be present during the transfer of the child. Parents of critically ill children, in most cases, will be able to accompany them in the ambulance with the retrieval team. When this is not possible or is not appropriate it is recommended that a hospital taxi is arranged for the transfer of the parent/carer to take them to the receiving hospital as they are usually unfit to drive due to stress. If they are transferring themselves, they should be given a route map to the hospital and advised not to attempt to keep up with the ambulance Transfer requirements: all transfer requirements should be provided as indicated (refer to appendix G) and documented on the internal / external transfer check list (Appendix D) and the original sent with patient if appropriate. A photocopy of the transfer checklist should be filed in patient s notes Documentation to accompany the patient: a Nursing Transfer Letter should be completed by the nurse caring for the child dependant on the type of transfer prior to transfer and sent with the patient (Appendix E) A letter should be completed by the doctor caring for the child and sent with the patient. A consultant to consultant referral should be requested Observation during transfer 12.1 Appropriate observations of the vital signs should be performed during the period of transfer depending on the clinical diagnosis and severity of the patients. The Children s Observation Policy will guide decision making. These should be noted and handed over to the receiving Department or external Hospital staff. 8
9 12.2 Observation notes while recorded during transfer should be photocopied at the receiving hospital and inserted into the child s MEHT notes on return Any adverse events / incidents that occur during the transfer should be documented and a datix report form completed Staff Training 13.1 All medical and nursing staff are to ensure that their knowledge, competencies and skills are up-to-date in order to complete their portfolio for appraisal All registered nurses will be trained in basic life support 13.3 All senior nurses (bands 6 and 7), registrars and consultants will be trained in Advanced Paediatric Life Support (EPLS/APLS) During induction process for junior medical staff At case presentation and junior doctor teaching sessions Infection Prevention 14.1 All staff should follow Trust guidelines on infection prevention ensuring that they effectively decontaminate their hands before and after each procedure All staff should ensure that they follow Trust guidelines on infection prevention using Aseptic Non-Touch Technique (ANTT) when carrying out procedures 15.0 Equality and Diversity 15.1 Mid Essex Hospitals is committed to the provision of a service that is fair, accessible and meets the needs of all individuals An Equality Impact Assessment is attached to the policy at appendix Monitoring compliance with policy requirements 16.1 All incidents relating to this guideline will be investigated, an action plan drawn up and recommendations made for improving care provided An annual audit of compliance with key requirements of this policy will be undertaken by the Lead Nurse for Children and Young People with the support of clinical audit. As a minimum this will assess compliance with: the transfer requirements for each patient group the documentation that should accompany the patient when being transferred the process for transfer out of hours 16.4 The findings of the audit will be reported to the Clinical Director for Women and Children and reviewed at the Women and Children and Sexual Health Governance Meeting. Where indicated, actions will be developed to address deficiencies with 9
10 named leads and timescales. Progress with any actions will be monitored at subsequent meetings Implementation and Communication 17.1 The policy will be uploaded on the Trust Intranet site and will be communicated to staff via staff focus The policy will be circulated to the Clinical Lead for paediatrics and Lead Nurse for children & young people for dissemination References Advanced Life Support Group [ALSG] (2011) Advanced paediatric Life Support: The practical Approach Fifth Edition. Wiley-Blackwell publishing: Chichester Dixon, M et al editor (2009) Nursing the Highly Dependent Child or Infant - A Manual of Care Wiley-Blackwell publishing DOH (2001) High dependency care for children report of an advisory group DOH (2003) Hospital standards document: Children s national service framework DOH (2006) The acutely or critically or injured child in the district general hospital: A team response Guidance on the provision of paediatric anaesthetic services. Royal College of anaesthesia (Revised April 2010) Health care commission (2009) Improving the services for children in hospital Joint statement from the society of British neurological surgeons and the royal college of anaesthetists regarding the provision of emergency paediatric neurosurgical services (2010) Paediatric intensive care society (2010) Standards for the care of critically ill children 4 th edition RCN (2011) Transferring children to and from theatre. Position statement and guidance for good practice Report of the intercollegiate committee for services for children in emergency departments. (2007) Services for children in emergency departments The Royal college of surgeons of England (2007) Surgery for children Children s Acute Transport Retrieval Service (online) accessed 24/10/
11 Appendix A Clinical Dependency Assessment tool for transfer of children Compromised airway / Inadequate breathing? Cardiovascularly compromised? Shock / Hypoglycaemia? Unresponsive / currently fitting? Patient has secure airway intubated? Yes Level 1 Transfer No Compromised breathing/inadequate breathing (Low Sa02/difficulty talking/acutely short of breath/oedema) Cardiovascularly compromised? (Shock / Hypoglycaemia/ hot child / rash/severe vomiting) Altered conscious level? (responds to voice or pain only / severe pain) Patient has unsecured airway Yes Level 2 Transfer No Compromised breathing but potential for deterioration? Cardiovascularly compromised but stable? (persistent vomiting / not feeding / not passing urine) Conscious level moderate pain / history of fitting / prolonged crying) Yes Level 3 Transfer No Stable patient with no airway or cardiovascular compromise but requiring continuous monitoring of physiological parameters due to: Operative intervention Received sedation / opiates Condition may change at short notice e.g. head injury Condition may reasonably evolve e.g. allergic reaction Received some from of resuscitation Yes Level 4 Transfer No Stable patient with no airway or cardiovascular compromise and not requiring continuous monitoring of physiological parameters, but requiring hospitalisation or investigation away from department Yes Level 5 Transfer 11
12 Recommended Resources for safe transfer of children Appendix B Transfer of level 1 patient with: Secure airway Vascular access Monitoring equipment ECG / SaO2 / RR / BP Resuscitation pack including oxygen Retrieval team e.g. CATS Consultant Anaesthetist If using local team Senior Nurse Inter-hospital transfer regional transport team optional (local and CATS decision regarding most appropriate) Transfer of level 2 patient with: Vascular access Monitoring equipment ECG / Sa02 / RR / BP Resuscitation pack including oxygen Consultant Anaesthetist if possible Senior Nurse Strong consideration should be given to converting to level 1 and securing airway Transfer of level 3 patient with: Vascular access Monitoring equipment ECG / SaO2 / RR / BP Resuscitation pack including oxygen Senior nurse Paramedic crew and blue light for inter-hospital transfer Transfer of Level 4 patient with: Unrestricted access to patient Continuous monitoring required for patient condition e.g. SaO2 monitoring Full oxygen cylinder Accompanied by nurse or paramedic crew Transfer of Level 5 patient with: Wheelchair or bed / stretcher Car seat transfer with parents and/or appropriate accompanying member of healthcare team 12
13 Appendix C Flow chart for transfer of a child to a paediatric tertiary centre Level 1 transfer Level 2 transfer Level 3, 4 & 5 transfer Is it Time Critical? Is the child stabilised? Yes Transfer by local team No Refer to CATS No Yes Consider converting to level 1 transfer Paediatric team to arrange transfer as per hospital policy Organise a bed Wait for the retrieval team Who will make up the Local Transfer Team 1. The transfer team should comprise those personnel (Paediatrician/Anaesthetist/Senior Nurse or ODP) with the most appropriate competencies. It should include at least a consultant or senior registrar. Consideration should be given to a two clinician transfer if the child is particularly unstable or young. Consideration should also be given to the needs of all the patients under the clinicians care and the skills and competencies of the available staff to care for them. 2. Anaesthetic consultant to liaise with the 4 tiers of on-call consultant colleagues to determine accompanying anaesthetic support (Burns ICU, General ICU, General Anaesthesia, Obstetric Anaesthesia). 3. Consultant paediatrician to liaise with paediatric team to determine if anyone has appropriate experience/competencies 4. Senior nurse on duty for phoenix and/or children s A&E dept to liaise with each other/odp s and the COMS team to determine if anyone has appropriate experience/competencies CATS can be consulted for advice and/or organise a bed to ensure safe transfer by local team. Paediatric critical care transfer equipment is available and can be obtained from Burns ICU To arrange transport contact the East of England Ambulance Service on 999 or (direct dial no) and state that you are requesting a time critical transfer. 5. If local team do not have necessary competencies to undertake transfer then CATS to be contacted ASAP and asked to transfer child. 13
14 Appendix D Surname First Name Internal/External Transferring Children Safely Checklist DOB: / / Hospital No: Clinical Dependency (see guidelines) applicable level following assessment Level 1 Level 2 Level 3 CATS or local critical care team transfer Senior doctor & nurse; anaesthetist if possible. Consider converting to level 1 Senior nurse & paramedic crew and blue lights Level 4 Level 5 Nurse &/or paramedic crew Car with parents Date & time of assessment: Date of Transfer: Dr authorising transfer: Consultant aware of transfer: Y / N Receiving ward / hospital: Receiving consultant / doctor: Telephone number of receiving ward: Contact details of receiving consultant / doctor: Pre-departure check list Discussion with nurse in Receiving hospital / Y / N charge on Phoenix dept contacted Y / N Handover Y / N Ambulance Arrival of Ambulance Parents aware control / Porter Y / N Y / N ambulance Y / N booked of transfer contacted confirmed Y / N Ventilator Y / N Oxygen Y / N Suction Y / N Monitoring Y / N Transfer bag Y / N Drugs bag Y / N Mobile phone Y / N High visibility jacket Photocopied documents sent if applicable Drug treatment card Fluid chart Map for parents IV prescription chart Nurse letter Notes Observation chart Doctor letter x-rays/imaging Name Dr accompanying Name Nurse accompanying Y / N Parent / Carer / Other accompanying Original checklist provided to patient / parent / carer Contact details of parent / carer Yes / No / NA Copy of doctor letter provided Yes / No / NA 14
15 Transfer details Departure time Arrival time Evaluation/notes/additional information/communication during transfer: Signature of accompanying Doctor: Signature of accompanying Nurse: Care handed over to: Adverse events/incidents during transfer: Document detail of equipment failure/patient deterioration/delays etc N.B. Send original checklist with patient. File photocopied checklist in patient s notes. Any adverse incident requires a datix to be completed. Please ensure all equipment / transfer bags are checked and restocked on completion of transfer. 15
16 Nurse Transfer Letter Appendix E 16
17 Appendix F Time critical transfer of the Critically Ill Child 1.0 Purpose 1.1 Used in conjunction with the transferring children guideline the transfer of critically ill children by a local team can be undertaken safely. 2.0 Background 2.1 Some children, including but not limited to those with a suspected intra-cranial haemorrhage or suspected blocked ventriculo-peritoneal shunt or penetrating trauma, the critical factor in outcome is time to definitive surgical treatment. Waiting for a retrieval team would lead to unnecessary delay in this process. Such children will need to be transferred by local staff usually a senior Anaesthetist with a senior ITU nurse or ODP. The decision to transfer a critically ill child should always be made with full advice and support from the receiving PICU and CATS (Children s Acute Transport Service) emergency referral hotline ). 2.2 These transfers must be discussed with Paediatric and Anaesthetic Consultants but by their nature time is critical and plans should be made for transfer as soon as possible. CATS should be contacted and can provide advice, find a bed and liaise with sub-specialities such as neurosurgery. Refer to CATS website for guidance. Refer to Neurosurgical Emergency and Traumatic Brain Injury guidelines for neurosurgical transfers. 3.0 The Transfer Team 3.1 This would usually consist of: A suitably experienced anaesthetic specialist trainee or specialist doctor who has completed intermediate level paediatric anaesthesia training and holds a current advanced paediatric resuscitation qualification; or a Consultant Anaesthetist. An anaesthetic assistant who is an ODP, with paediatric training and/or a senior children s nurse with HDU or ICU experience 3.2 In the case of an un-intubated child with a GCS > 9 and CEWT score < 3, requiring transfer, where there is risk of the airway or breathing deteriorating during the transfer, the accompanying doctor should be an anaesthetist. 3.3 Neonates should be managed by the paediatric team who are more familiar with the special equipment required for this age group. 3.4 Ultimately, where there is no other suitable doctor available (see above), a consultant anaesthetist will always be the best person to undertake the transfer. 17
18 4.0 Equipment 4.1 Transfer equipment is available from main theatres, A&E and burns ICU. The following equipment should be available for transfer: Equipment Bag appropriate to the age of the child, which contains the emergency equipment required for transfer. Oxylog 3000 ventilator, set for the appropriate child s weight and age (Transport ventilators for small children are available in Pheonix) Drugs: as a minimum, the following drugs should be drawn up in suitable dilutions and available for immediate use**; o Sedation morphine and midazolam infusions. o Neuromuscular blockers suxamethonium boluses available, as well as atracurium or vecuronium infusions o Inotropes advice about which is the most appropriate should be sought from the CATS team o Resuscitation drugs atropine, adrenaline o Raised ICP Mannitol or 3% Hypertonic Saline boluses, Fentanyl for bolus Mobile telephone, with all relevant numbers appended High visibility jackets Transfer Documentation for en Route Observations. **CATS electronic drug chart / prescription card printed Refer to CATS website Mode of Transport 5.1 This will usually be by road ambulance, as the distances involved are small. 5.2 Ambulance control are required to meet strict targets for dispatch of vehicles to public calls and may give a lower priority to calls from a hospital to transfer a patient than calls from the public due to a perception that the patient in hospital is less likely to die. 5.3 East of England Ambulance Service have agreed to provide a rapid response to requests for time critical transfers by our own team for example neurosurgical emergencies, intra-abdominal haemorrhage etc requiring emergency operative intervention. 5.4 In order for appropriate prioritisation of transfers by our own team early warning of the need for a vehicle to transfer a patient must be given and correct information shared with ambulance control. 5.5 Contact Ambulance Control as soon as possible and inform them of the impending need for a rapid response vehicle and the approximate time by which the rest of the 18
19 preparations will be ready: kit, drugs, monitors, staff etc. Call again when the team is almost ready to leave requesting an immediate response. 5.6 It is important that this system is not abused in less time critical situations to put pressure on ambulance control to inappropriately increase the priority for example to avoid loosing a bed in a tertiary hospital or because the staff are nearing the end of their shift etc. 6.0 Stabilisation of the child 6.1 This should occur prior to any transfer taking place. There are very few indications for a scoop and run policy, which carries a high mortality. 6.2 Airway and Breathing Where deterioration of the airway is anticipated, the child should be intubated before transfer***. The ETT should be securely fixed in place, and the child adequately sedated. The position of the ETT should be confirmed by CXR. Neuromuscular blocking drugs should be used for the journey to reduce the likelihood of inadvertent extubation. Pneumothoraces should be drained prior to transfer. Monitoring should include: SaO2, capnography, airway pressures, ABGs prior to transfer, and CXR. A nasogastric or orogastric (in the case of head injury) tube should be placed in the intubated patient. ***CATS clinical guidelines: Induction of Anaesthesia refer to CATS website 6.3 Circulation Bleeding should be controlled prior to transfer, and hypovolaemia adequately corrected. Inotropic infusions should be prepared in accordance with CATS guidelines prior to transfer where deterioration is anticipated. (please refer to MEHT guidelines as well for preparation of inotropes and other infusions) At least two cannulae should be inserted to guarantee vascular access. Invasive monitoring is not essential unless the underlying condition warrants it. A urinary catheter should be inserted 6.4 Disability Advice should be sought from the receiving unit regarding management of raised intracranial pressure.* Ensure adequate sedation and neuromuscular blockade. Establish adequate ventilation prior to transfer. Avoid ties around the neck. * CATS Clinical Guideline: Neurosurgical Emergency, Traumatic Brain Injury & Local team transfer refer to CATS website 19
20 6.5 Exposure All lines should be accessible without exposing the child to heat loss. Airway tubes, other tubing and lines should be securely fixed. The child should be well wrapped, with the head covered to avoid heat loss. 6.6 Glucose Monitor blood glucose prior to leaving and in transit if journey time is greater than 2 hours (1 hour if child has had previous blood glucose instability). 6.7 Documentation The following should accompany the patient to the receiving unit; Patient details Copy of the patient notes Transfer chart. All treatment administered by the transfer team. Relevant consent forms. Blood tests and radiographs. Check list. Telephone numbers of the receiving hospital, with the names of the receiving doctor 6.8 Pre-transfer checklist Ensure transfer checklist is completed and using the pneumonic TRANSFER to ensure a structured approach is adopted and all potential problems considered before transfer takes place. Timing: Ensure communication has taken place between the MDT in both the referring hospital and receiving hospital and the family. Resources: Ensure the most appropriate staff to facilitate the transfer are available including any additional staff Assessment: Full assessment should be undertaken prior to the child being moved. Notes: Ensure all appropriate documentation is available and up to date and an identity bracelet is clearly on the child Safety: Ensure that the personnel accompanying the child are suitably trained to undertake any care required during the transfer. Equipment should be secured and there should be enough oxygen available to complete the journey. Family: Ensure the child s family are kept informed and updated on a regular basis. They should be given full contact details of the new ward/hospital. Transport should be provided for parents/carers if unable to accompany child in ambulance and parents are unable to provide own. Equipment: Ensure the equipment to be used during the transfer is in full working order and charged Report: Handover nurse to nurse prior to transfer to facilitate preparation for the child s arrival. 20
21 6.9 Print and complete the following checklist prior to transfer 21
22 Appendix G Type of transfer Transfer requirements Documentation to accompany patient A&E to children s ward Ward informed Verbal handover Patient & parent/guardian informed & to accompany to the ward on transfer Escort if required Appropriate equipment if required Original A&E card Drug chart & O2 prescription if indicated Risk assessment if indicated CEWT score in A&E if indicated External transfer out to another acute hospital Trust External transfer in from another acute hospital Trust Transfer to other wards/departments in MEHT including radiology Children s ward to Theatre Theatre to Children s ward Ward/dept informed Verbal handover prior to leaving Patient & parent/guardian informed & to accompany on transfer Escort if required Appropriate equipment if required Appropriate mode of transport Liaise with CATS retrieval service for specific requirements on an individual basis Ward/dept informed Verbal handover prior to leaving Patient & parent/guardian informed & to accompany on transfer Escort if required Appropriate equipment if required Appropriate mode of transport Ward/department informed Verbal handover Patient & parent/guardian informed & to accompany to the ward on transfer Escort if required Appropriate equipment if required Appropriate member of the nursing team to escort to theatre and anaesthetic room Parent/guardian to accompany escort to theatre and into anaesthetic room (presence in the anaesthetic room is under the direction of the anaesthetist) Verbal handover Parent allowed to be in recovery room and escort child back to ward Registered nurse as a minimum to escort child to ward from recovery Appropriate equipment identified Transfer to ward on trolley/bed (where babies are carried then a trolley must be present) Transfer checklist Nursing and medical transfer letter Copy of notes Copy of radiological imaging and laboratory results Parent information Risk assessment Copy of medical & nursing notes Transfer letter Nursing & medical notes Drug chart & O2 prescription Risk assessment if indicated CEWT score in ward Pre op safety checklist Consent form Baseline observations Allergy status Risk assessment if indicated Op sheet Post op instructions Drug chart O2 prescription CEWT score in recovery Risk assessment if indicated Recommended level of transfer following a risk assessment using tools in Appendix A & B Level 1 CATS or local critical care team Level 2 Senior doctor & nurse; anaesthetist if possible. Consider converting to level 1 Level 3 Level 4 Level 5 Senior nurse & paramedic crew Nurse &/or paramedic crew Car with parents 22
23 Transfer and documentation requirements specific to each type of transfer Appendix H Equality Impact Assessment (EIA) Title of document: Guideline for Transferring Children 0-16 years Equality or human rights concern. (see guidance notes below) Gender Race and ethnicity Disability Religion, faith and belief Sexual orientation Age Transgender people Social class Carers. Does this item have any differential impact on the equality groups listed? Brief description of impact. None Patients and/or parents may require translation services. Access to children s wards, emergency dept and OP clinics. Patients and/or parents with cognitive or sensory impairment may have difficulty with understanding information. None None Children may have difficulty in understanding procedures. Ensure the views of all children and young people are considered. None Those patients with limited vocabulary or reading skills may have difficulty accessing and understanding patient information. Access to services and information may be affected by financial constraints. Issues relating to race, ethnicity and disability may apply. How is this impact being addressed? Trust uses The Big Word for translation services. All facilities meet building standards. Hospital Liaison Specialist LD Nurse will support these patients and their families with LD Hospital Play Specialist and parents/carers will support these children. Authors are directed to use short sentences, everyday language, and avoid the use of jargon. Information on transport and reimbursement of costs is available. As above Date of assessment: 24 th October 2014 Names of Assessor (s): Andrea Stanley and Victoria Machell 23
Time-Critical Transfer of the Sick or Injured Child (<16 years)
 LRI Emergency Department Standard Operating Procedure for: Time-Critical Transfer of the Sick or Injured Child (
LRI Emergency Department Standard Operating Procedure for: Time-Critical Transfer of the Sick or Injured Child (
Register No: Status: Public
 Care of the Critically Ill Child Clinical Guideline Register No: 16025 Status: Public Developed in response to: Best practice Contributes to CQC Fundamental Standard 9, 12 Consulted With Post/Committee/Group
Care of the Critically Ill Child Clinical Guideline Register No: 16025 Status: Public Developed in response to: Best practice Contributes to CQC Fundamental Standard 9, 12 Consulted With Post/Committee/Group
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition
 Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care
 Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Register No: Status: Public on ratification
 Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0
 CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0 Page 1 of 13 Abbreviation (P/A)HDU (P/A)ICU GCS IPPV CPAP BiPAP DKA Reg Meaning (Paediatric/Adult) High Dependency
CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0 Page 1 of 13 Abbreviation (P/A)HDU (P/A)ICU GCS IPPV CPAP BiPAP DKA Reg Meaning (Paediatric/Adult) High Dependency
Critical Care in Obstetrics Guideline
 This is an official Northern Trust policy and should not be edited in any way Critical Care in Obstetrics Guideline Reference Number: NHSCT/12/515 Target audience: This guideline is directed to all obstetricians,
This is an official Northern Trust policy and should not be edited in any way Critical Care in Obstetrics Guideline Reference Number: NHSCT/12/515 Target audience: This guideline is directed to all obstetricians,
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals
 Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
Consulted With Post/Committee/Group Date Dr Dhillon Cardiology Consultant April Professionally Approved By 2. Clinical Effectiveness
 Implantable Cardioverter Defibrillator (ICD) Deactivation End of Life Type: Clinical Guidance Register No: 17007 Status: Public on ratification Developed in response to: Best Practice Contributes to CQC
Implantable Cardioverter Defibrillator (ICD) Deactivation End of Life Type: Clinical Guidance Register No: 17007 Status: Public on ratification Developed in response to: Best Practice Contributes to CQC
GUIDELINE FOR STEP-DOWN TRANSFER OF PATIENTS FROM CRITICAL CARE AREAS
 GUIDELINE FOR STEP-DOWN TRANSFER OF PATIENTS FROM CRITICAL CARE AREAS This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the
GUIDELINE FOR STEP-DOWN TRANSFER OF PATIENTS FROM CRITICAL CARE AREAS This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS
 HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
Consulted With Individual/Body Date. Last reviewed Mags Shaughnessy Director of Operations 16 August Operations
 Root Cause Analysis for Cancer Patients exceeding National Performance Standards Policy Register No: 17005 Status: Public Developed in response to: CWT Version 9 Going Further on Cancer Waits Achieving
Root Cause Analysis for Cancer Patients exceeding National Performance Standards Policy Register No: 17005 Status: Public Developed in response to: CWT Version 9 Going Further on Cancer Waits Achieving
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
Standard Operating Procedure. for the Retrieval Nurse
 Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
Patient Transfer Policy
 Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE
 COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE (2006) The CoBaTrICE Collaboration: 1 st September 2006. European Society of Intensive Care Medicine (ESICM) Avenue Joseph Wybran 40, B-1070,Brussels.
COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE (2006) The CoBaTrICE Collaboration: 1 st September 2006. European Society of Intensive Care Medicine (ESICM) Avenue Joseph Wybran 40, B-1070,Brussels.
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT
 CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
South Tyneside NHS Foundation Trust. Clinical Policy. Chaperoning Policy. Review Date June 2011
 South Tyneside NHS Foundation Trust Clinical Policy Chaperoning Policy Date Approved by Version Issue Date June 2009 2 June Executive 2009 Director of Nursing & Clinical Services Procedure /Policy number
South Tyneside NHS Foundation Trust Clinical Policy Chaperoning Policy Date Approved by Version Issue Date June 2009 2 June Executive 2009 Director of Nursing & Clinical Services Procedure /Policy number
Standard Operating Procedure INTER-HOSPITAL TRANSFERS
 Standard Operating Procedure INTER-HOSPITAL TRANSFERS DATE APPROVED: September 2010 APPROVED BY: Air Operations Manager IMPLEMENTATION DATE: November 2014 REVIEW DATE: November 2015 LEAD DIRECTOR: IMPACT
Standard Operating Procedure INTER-HOSPITAL TRANSFERS DATE APPROVED: September 2010 APPROVED BY: Air Operations Manager IMPLEMENTATION DATE: November 2014 REVIEW DATE: November 2015 LEAD DIRECTOR: IMPACT
ISOLATED HEAD INJURY. MODULE: Intensive Care Medicine / Trauma ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND:
 ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
Clinical Care Pathway for BRAIN TUMOURS in Childhood.
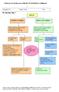 - 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
- 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
Sepsis guidance implementation advice for adults
 Sepsis guidance implementation advice for adults NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Strategy & Innovation
Sepsis guidance implementation advice for adults NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Strategy & Innovation
Inguinal hernia repair integrated care pathway (ICP)
 Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Z: Perioperative Nursing Specialty
 Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Modified Early Warning Score Policy.
 Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
The ROHNHSFT Experience: Implementing BWCH PEWS
 The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
Example Care Pathways
 Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart
 CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
JOB DESCRIPTION 1. JOB IDENTIFICATION
 JOB DESCRIPTION 1. JOB IDENTIFICATION Job Title: Anaesthetic/Recovery Nurse Practitioner/Operating Department Practitioner Responsible to: Theatre Senior Charge Nurse Department(s): Theatre and Recovery
JOB DESCRIPTION 1. JOB IDENTIFICATION Job Title: Anaesthetic/Recovery Nurse Practitioner/Operating Department Practitioner Responsible to: Theatre Senior Charge Nurse Department(s): Theatre and Recovery
PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE
 PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE Introduction There are currently over 500 Critical Care Transfers carried out in
PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE Introduction There are currently over 500 Critical Care Transfers carried out in
Hospital Discharge and Transfer Guidance. Choice, Responsiveness, Integration & Shared Care
 Hospital Discharge and Transfer Guidance Choice, Responsiveness, Integration & Shared Care Worcestershire Mental Health Partnership NHS Trust Information Reader Box Document Type: Document Purpose: Unique
Hospital Discharge and Transfer Guidance Choice, Responsiveness, Integration & Shared Care Worcestershire Mental Health Partnership NHS Trust Information Reader Box Document Type: Document Purpose: Unique
CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline 1.1. Guidelines for the use of rectus sheath catheters for the management of pain following laparotomy
CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline 1.1. Guidelines for the use of rectus sheath catheters for the management of pain following laparotomy
Seven Day Services Clinical Standards September 2017
 Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport
 Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport Transport Service Facilities 1. Access to 24/7 Cheshire and Merseyside Perinatal Cot Bureau and Data Management
Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport Transport Service Facilities 1. Access to 24/7 Cheshire and Merseyside Perinatal Cot Bureau and Data Management
anaesthetic services Chapter 15 Services for neuroanaesthesia and neurocritical care 2014 GUIDELINES FOR THE PROVISION OF ACSA REFERENCES
 Chapter 15 GUIDELINES FOR THE PROVISION OF anaesthetic services ACSA REFERENCES 15.1.1 15.1.2 15.1.3 15.1.4 15.1.5 15.1.8 15.1.9 15.1.11 15.2.1 15.2.9 15.2.13 15.2.17 15.2.18 15.2.19 15.3.2 15.4.2 15.5.1
Chapter 15 GUIDELINES FOR THE PROVISION OF anaesthetic services ACSA REFERENCES 15.1.1 15.1.2 15.1.3 15.1.4 15.1.5 15.1.8 15.1.9 15.1.11 15.2.1 15.2.9 15.2.13 15.2.17 15.2.18 15.2.19 15.3.2 15.4.2 15.5.1
Anaesthetic Trainees- The Trauma Call at SMH
 Anaesthetic Trainees- The Trauma Call at SMH Anaesthetic staff at a trauma call Bleep Grade Times 1201 Consultant 08:00 18:00 SpR on-call for theatres 18:00 08:00 6348 Extra SpR 08:00 17:00 Obstetric SpR
Anaesthetic Trainees- The Trauma Call at SMH Anaesthetic staff at a trauma call Bleep Grade Times 1201 Consultant 08:00 18:00 SpR on-call for theatres 18:00 08:00 6348 Extra SpR 08:00 17:00 Obstetric SpR
Elmarie Swanepoel 24 th September 2017
 MEDICAL EQUIPMENT TRAINING POLICY Policy Register No: 10010 Status: Public Developed in response to: Best practice Contributes to CQC Regulation: 15 Consulted With: Post/Committee/Group: Date: Medical
MEDICAL EQUIPMENT TRAINING POLICY Policy Register No: 10010 Status: Public Developed in response to: Best practice Contributes to CQC Regulation: 15 Consulted With: Post/Committee/Group: Date: Medical
Core competencies for the care of acutely ill and injured children and young people. May 2006
 Core competencies for the care of acutely ill and injured children and young people May 2006 Contents Introduction 3 How the competencies can be used 6 Core competencies : Assessment domain 7 Core competencies
Core competencies for the care of acutely ill and injured children and young people May 2006 Contents Introduction 3 How the competencies can be used 6 Core competencies : Assessment domain 7 Core competencies
DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY
 DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY (To be read in conjunction with Diagnostic Imaging Requesting and Interpreting Radiographs by Non Medical Practitioners Policy, Consent
DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY (To be read in conjunction with Diagnostic Imaging Requesting and Interpreting Radiographs by Non Medical Practitioners Policy, Consent
CHILDREN S OBSERVATIONS & SEVERITY TOOL (COAST FORMELY PEWS) & PAEDIATRIC OBSERVATION CHART POLICY
 CHILDREN S OBSERVATIONS & SEVERITY TOOL (COAST FORMELY PEWS) & PAEDIATRIC OBSERVATION CHART POLICY Document Author Written By: Paediatric Sister Authorised Authorised By: Chief Executive Date: July 2017
CHILDREN S OBSERVATIONS & SEVERITY TOOL (COAST FORMELY PEWS) & PAEDIATRIC OBSERVATION CHART POLICY Document Author Written By: Paediatric Sister Authorised Authorised By: Chief Executive Date: July 2017
Beth Israel Deaconess Medical Center Perioperative Services Manual. Guidelines for Perioperative Handoffs from OR to receiving units.
 Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Administration of urinary catheter maintenance solution by a carer
 Document level: Trustwide Code: CP71 Issue number: 1 Administration of urinary catheter maintenance solution by a carer Lead executive Director of Nursing Therapies Patient Partnership Authors details
Document level: Trustwide Code: CP71 Issue number: 1 Administration of urinary catheter maintenance solution by a carer Lead executive Director of Nursing Therapies Patient Partnership Authors details
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation
 Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Clinical Director for Women s and Children s Directorate
 MANAGEMENT OF A HOME BIRTH CLINICAL GUIDELINES Register no: 08101 Status: Public Developed in response to: Intrapartum NICE Guidelines Review of Guideline Contributes to CQC Regulation 9, 10, 12 Consulted
MANAGEMENT OF A HOME BIRTH CLINICAL GUIDELINES Register no: 08101 Status: Public Developed in response to: Intrapartum NICE Guidelines Review of Guideline Contributes to CQC Regulation 9, 10, 12 Consulted
Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster.
 Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster. Working document The Critical Care Contingency Plan in the event of an emergency
Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster. Working document The Critical Care Contingency Plan in the event of an emergency
Brief Summary. Educational Rationale. Learning Objectives: Nurse. Learning Objectives: Doctor
 Simulation Scenario Title Bacterial meningitis Version 10 Target Audience FY doctors & student nurses Run time 10-15 mins Authors Niamh Feely, Andrew Smith, Udesh Naidoo, Paul Wilder, Mark Loughrey Last
Simulation Scenario Title Bacterial meningitis Version 10 Target Audience FY doctors & student nurses Run time 10-15 mins Authors Niamh Feely, Andrew Smith, Udesh Naidoo, Paul Wilder, Mark Loughrey Last
1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure
 ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
Scottish Ambulance Service. Job Description
 1. JOB IDENTIFICATION Scottish Ambulance Service Job Description Job Title: Neonatal Transport Nurse Department(s): Specialist Transport & Retrieval (SCOTSTAR) Job Holder Reference: No of Job Holders:
1. JOB IDENTIFICATION Scottish Ambulance Service Job Description Job Title: Neonatal Transport Nurse Department(s): Specialist Transport & Retrieval (SCOTSTAR) Job Holder Reference: No of Job Holders:
Consulted With: Post/Committee/Group: Date:
 AMBULANCE HANDOVER PROTOCOL WHEN OFF LOAD TIME IS LIKELY TO EXCEED 30 MINUTES Policy Register No: 18012 Status: Public Developed in response to: NHSE Directives CQC Fundamental Standards: Safe and Responsive
AMBULANCE HANDOVER PROTOCOL WHEN OFF LOAD TIME IS LIKELY TO EXCEED 30 MINUTES Policy Register No: 18012 Status: Public Developed in response to: NHSE Directives CQC Fundamental Standards: Safe and Responsive
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY V2. Transfer Policy for Neonates, Infants and Children Page 1 of 36
 TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
NURSING SCOPE OF PRACTICE POLICY Page 1 of 10 July 2016
 Page 1 of 10 NB: Anaesthetic RN Policy has been incorporated into this policy Policy Applies to: All Mercy Hospital Nursing staff Related Standards: Health Practitioners Competency Assurance Act (HPCA)
Page 1 of 10 NB: Anaesthetic RN Policy has been incorporated into this policy Policy Applies to: All Mercy Hospital Nursing staff Related Standards: Health Practitioners Competency Assurance Act (HPCA)
Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee
 The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
Miss Rao Lead Consultant for Obstetrics and Gynaecology August 2015
 MANDATORY TRAINING POLICY FOR MATERNITY SERVICES (INCORPORATING TRAINING NEEDS ANALYSIS) CLINICAL GUIDELINES Register no: 09062 Status: Public Developed in response to: Contributes to CQC Regulation 18
MANDATORY TRAINING POLICY FOR MATERNITY SERVICES (INCORPORATING TRAINING NEEDS ANALYSIS) CLINICAL GUIDELINES Register no: 09062 Status: Public Developed in response to: Contributes to CQC Regulation 18
Nursing Practice Committee
 Nursing Practice Committee Standard Operating Procedure on Patient preparation and Admission to Operating Theatre Author: Emma Cooney CNM 3 & Rosemary Clerkin CNF Issue Date: March 2010 Review Date: March
Nursing Practice Committee Standard Operating Procedure on Patient preparation and Admission to Operating Theatre Author: Emma Cooney CNM 3 & Rosemary Clerkin CNF Issue Date: March 2010 Review Date: March
PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification. 12 months
 E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES
 CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES STANDARD OPERATING PROCEDURES Ysbyty Glan Clwyd Telephone No: 01745 534686 Fax No: 01745 534681 Date: June 2015 Authors: Neonatal Transport
CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES STANDARD OPERATING PROCEDURES Ysbyty Glan Clwyd Telephone No: 01745 534686 Fax No: 01745 534681 Date: June 2015 Authors: Neonatal Transport
Norwegian Standard for the Safe Practice of Anaesthesia
 Norwegian Standard for the Safe Practice of Anaesthesia 1. Introduction The Norwegian standard for the safe practice of anaesthesia was first published in 1991. It was then revised in 1994, and subsequently
Norwegian Standard for the Safe Practice of Anaesthesia 1. Introduction The Norwegian standard for the safe practice of anaesthesia was first published in 1991. It was then revised in 1994, and subsequently
Policy for Failure to Bring/Attend Children s Health Appointments Whittington Health 2012/2013
 Policy for Failure to Bring/Attend Children s Health Appointments Whittington Health 2012/2013 Subject: Policy Number: 1 Ratified by: Policy for Failure to Bring/Attend and Cancellation of Children s Health
Policy for Failure to Bring/Attend Children s Health Appointments Whittington Health 2012/2013 Subject: Policy Number: 1 Ratified by: Policy for Failure to Bring/Attend and Cancellation of Children s Health
Unless this copy has been taken directly from the Trust intranet site (Pandora) there is no assurance that this is the most up to date version
 Policy No: OP84 Version: 2.0 Name of Policy: Internal Patient Transfer and Escort Policy Effective From: 07/09/2015 Date Ratified 12/08/2015 Ratified SafeCare Council Review Date 01/08/2017 Sponsor Director
Policy No: OP84 Version: 2.0 Name of Policy: Internal Patient Transfer and Escort Policy Effective From: 07/09/2015 Date Ratified 12/08/2015 Ratified SafeCare Council Review Date 01/08/2017 Sponsor Director
Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital
 Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital Name: Start Date:. Mentor:. Introduction My name is Helen McCallum; I am the Clinical Skills Facilitator for St Marys Theatres. I would
Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital Name: Start Date:. Mentor:. Introduction My name is Helen McCallum; I am the Clinical Skills Facilitator for St Marys Theatres. I would
Standard Operating Procedure Hospital Pre-alert & Patient Handover
 Standard Operating Procedure Hospital Pre-alert & Patient Handover No of Pages: 6 Unique reference No: Implementation date: 17 th May 2010 Version: Final Version 2.0 Next review date: May 2013 Title of
Standard Operating Procedure Hospital Pre-alert & Patient Handover No of Pages: 6 Unique reference No: Implementation date: 17 th May 2010 Version: Final Version 2.0 Next review date: May 2013 Title of
Clinical Director for Women s and Children s Directorate
 FEEDING PRETERM AND SMALL FOR GESTATIONAL AGE INFANTS ON THE POSTNATAL WARD CLINICAL GUIDELINES Register No: 08094 Status: Public Developed in response to: Contributes to CQC Regulation 9,11 Intrapartum
FEEDING PRETERM AND SMALL FOR GESTATIONAL AGE INFANTS ON THE POSTNATAL WARD CLINICAL GUIDELINES Register No: 08094 Status: Public Developed in response to: Contributes to CQC Regulation 9,11 Intrapartum
Equivalence Guidance for GMP Domain 1
 Equivalence Guidance for GMP Domain 1 From 1 st August 2011 the new GMC approved curriculum in Intensive Care Medicine (ICM) came into effect. As a result of this new curriculum, all equivalence applications
Equivalence Guidance for GMP Domain 1 From 1 st August 2011 the new GMC approved curriculum in Intensive Care Medicine (ICM) came into effect. As a result of this new curriculum, all equivalence applications
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
Burton Hospitals NHS Foundation Trust. On: 24 October Review Date: October Corporate / Directorate. Clinical / Non Clinical
 POLICY DOCUMENT Burton Hospitals NHS Foundation Trust DISCHARGE POLICY Approved by: Trust Executive Committee On: 24 October 2017 Review Date: October 2020 Corporate / Directorate Clinical / Non Clinical
POLICY DOCUMENT Burton Hospitals NHS Foundation Trust DISCHARGE POLICY Approved by: Trust Executive Committee On: 24 October 2017 Review Date: October 2020 Corporate / Directorate Clinical / Non Clinical
PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification
 E07/S/c 2013/14 NHS STANDARD CONTRACT PAEDIATRIC LONG TERM VENTILATION PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner Lead Provider Lead Period
E07/S/c 2013/14 NHS STANDARD CONTRACT PAEDIATRIC LONG TERM VENTILATION PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner Lead Provider Lead Period
Part II. The CCT in. Intensive Care Medicine. Assessment System. The Faculty of. Intensive Care Medicine
 Part II The CCT in Intensive Care Medicine Assessment System The Faculty of Intensive Care Medicine Contents 1. Principles of Assessment... 3 1.1 Training Stage Records... 3 1.2 How many workplace-based
Part II The CCT in Intensive Care Medicine Assessment System The Faculty of Intensive Care Medicine Contents 1. Principles of Assessment... 3 1.1 Training Stage Records... 3 1.2 How many workplace-based
PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL
 PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS Revised April 2013 Liverpool Heart and Chest Hospital Aintree University Hospital Countess
PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS Revised April 2013 Liverpool Heart and Chest Hospital Aintree University Hospital Countess
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Advance Care Plan for a Child or Young Person
 Advance Care Plan for a Child or Young Person West Midlands Paediatric Palliative Care Network NHS Number: Advance Care Plan for a Child or Young Person This document is a tool for discussing and communicating
Advance Care Plan for a Child or Young Person West Midlands Paediatric Palliative Care Network NHS Number: Advance Care Plan for a Child or Young Person This document is a tool for discussing and communicating
DETERIORATING PATIENT & RESUSCITATION POLICY
 DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery
 CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
INPATIENT Annual Core Competency Performance Stations (Nursing) 2010 (Unlicensed Staff Direct & Non-Direct Care Providers * )
 County of Los Angeles INPATIENT Annual Core Competency Performance Stations (Nursing) 2010 (Unlicensed Staff Direct & Non-Direct Care Providers * ) * Staff who work in patient care areas 1 ANNUAL CORE
County of Los Angeles INPATIENT Annual Core Competency Performance Stations (Nursing) 2010 (Unlicensed Staff Direct & Non-Direct Care Providers * ) * Staff who work in patient care areas 1 ANNUAL CORE
Standard Operating Procedure
 Standard Operating Procedure Title of Standard Operation Procedure (SOP): The Prevention and Management of pressure ulcers in Special Needs Schools. Reference No: SS6 Version No: 1 Issue Date: March 2017
Standard Operating Procedure Title of Standard Operation Procedure (SOP): The Prevention and Management of pressure ulcers in Special Needs Schools. Reference No: SS6 Version No: 1 Issue Date: March 2017
CLINICAL GUIDELINES Register No: Status: Public THE SEVERELY ILL PATIENT IN MATERNITY SERVICES. RCOG guideline
 THE SEVERELY ILL PATIENT IN MATERNITY SERVICES CLINICAL GUIDELINES Register No: 09095 Status: Public Developed in response to: CQC Fundamental Standards: 11, 12 Intrapartum NICE Guidelines RCOG guideline
THE SEVERELY ILL PATIENT IN MATERNITY SERVICES CLINICAL GUIDELINES Register No: 09095 Status: Public Developed in response to: CQC Fundamental Standards: 11, 12 Intrapartum NICE Guidelines RCOG guideline
Do Not Attempt Resuscitation Policy
 Do Not Attempt Resuscitation Policy PROV 27 March 2009 1 Document Management Title of document Do Not Attempt Resuscitation Policy Type of document Policy PROV 27 Description To ensure that do not resuscitate
Do Not Attempt Resuscitation Policy PROV 27 March 2009 1 Document Management Title of document Do Not Attempt Resuscitation Policy Type of document Policy PROV 27 Description To ensure that do not resuscitate
Section 19 Mental Health Act 1983 Regulations as to the transfer of patients
 Document level: Trustwide (TW) Code: MH9 Issue number: 4 Section 19 Mental Health Act 1983 Regulations as to the transfer of patients Lead executive Authors details Type of document Target audience Document
Document level: Trustwide (TW) Code: MH9 Issue number: 4 Section 19 Mental Health Act 1983 Regulations as to the transfer of patients Lead executive Authors details Type of document Target audience Document
ECT Reference: Version 4 Effective Date: 28/02/2017. Date
 Chaperone Policy Policy Title: Executive Summary: Chaperone Policy This policy sets out guidance on the use of chaperones within the Trust and is based on recommendations from the General Medical Council,
Chaperone Policy Policy Title: Executive Summary: Chaperone Policy This policy sets out guidance on the use of chaperones within the Trust and is based on recommendations from the General Medical Council,
JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach.
 JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach. JOB TITLE: GRADE: BASE: MANAGED BY: Advanced Neonatal Nurse Practitioner Band 8a Homerton
JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach. JOB TITLE: GRADE: BASE: MANAGED BY: Advanced Neonatal Nurse Practitioner Band 8a Homerton
SCHEDULE 2 THE SERVICES
 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service E08/S/b Neonatal Intensive Care Transport Commissioner Lead Provider Lead Period Date of Review 12 Months 1. Population
SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service E08/S/b Neonatal Intensive Care Transport Commissioner Lead Provider Lead Period Date of Review 12 Months 1. Population
Summary of Significant Changes. Policy. Purpose. Responsibilities. Definitions
 This Management Process Description replaces MPD880/5 Copy Number Summary of Significant Changes Effective 22/09/17 Reformatting of document numbering and bullet points. Update with the new 5 hour rule
This Management Process Description replaces MPD880/5 Copy Number Summary of Significant Changes Effective 22/09/17 Reformatting of document numbering and bullet points. Update with the new 5 hour rule
KEY TO INITIALS OF ALL STAFF COMPLETING THIS ICP Print name Designation Initials Signature date
 Forename Surname Unit number Address (including Postcode) NHS Lothian Arrived in.unit for procedure Date: & time: GP Address Religion Ethnic Origin Tel. number Next of Kin: /address Tel. number(s):home
Forename Surname Unit number Address (including Postcode) NHS Lothian Arrived in.unit for procedure Date: & time: GP Address Religion Ethnic Origin Tel. number Next of Kin: /address Tel. number(s):home
Lincolnshire CCGs. Non-Emergency Patient Transport. Eligibility Criteria Policy
 Lincolnshire CCGs Non-Emergency Patient Transport Eligibility Criteria Policy Reference No: Version: 1.0 Ratified by: ClG058 Date ratified: May 2018 Name of originator/author: Name of responsible committee/individual:
Lincolnshire CCGs Non-Emergency Patient Transport Eligibility Criteria Policy Reference No: Version: 1.0 Ratified by: ClG058 Date ratified: May 2018 Name of originator/author: Name of responsible committee/individual:
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Injectable Medicines Policy
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Injectable Medicines Policy Version No.: 4.3 Effective From: 24 March 2017 Expiry Date: 21 January 2019 Date Ratified: 11 January 2017 Ratified By:
The Newcastle upon Tyne Hospitals NHS Foundation Trust Injectable Medicines Policy Version No.: 4.3 Effective From: 24 March 2017 Expiry Date: 21 January 2019 Date Ratified: 11 January 2017 Ratified By:
Management of Reported Medication Errors Policy
 Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
Advanced Roles and Workforce Planning. Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow
 Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
Sedation/Analgesia by Non-Anesthesiologists. THE UNIVERSITY OF TOLEDO Approving Officer:
 Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Standard of Care for MTC inpatients
 Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
EAST & NORTH HERTS, HERTS VALLEYS CCGS SAFEGUARDING CHILDREN & LOOKED AFTER CHILDREN TRAINING STRATEGY
 EAST & NORTH HERTS, HERTS VALLEYS CCGS Page 1 of 16 DOCUMENT CONTROL SHEET Document Owner: Directors of Nursing and Quality Document Author(s): Beverly Mukandi - Deputy Designated Nurse Safeguarding Children,
EAST & NORTH HERTS, HERTS VALLEYS CCGS Page 1 of 16 DOCUMENT CONTROL SHEET Document Owner: Directors of Nursing and Quality Document Author(s): Beverly Mukandi - Deputy Designated Nurse Safeguarding Children,
the victorian paediatric emergency transport service pets
 the victorian paediatric emergency transport service pets The Victorian Paediatric Emergency Transport Service The Victorian Paediatric Emergency Transport Service (PETS) is based at the Paediatric Intensive
the victorian paediatric emergency transport service pets The Victorian Paediatric Emergency Transport Service The Victorian Paediatric Emergency Transport Service (PETS) is based at the Paediatric Intensive
Children and Young Persons Do Not Attempt Resuscitation Policy
 Children and Young Persons Do Not Attempt Resuscitation Policy Version: Final Ratified by (name of Committee): Provider Services Quality and Safety Committee Date ratified: March 2011 Date issued: June
Children and Young Persons Do Not Attempt Resuscitation Policy Version: Final Ratified by (name of Committee): Provider Services Quality and Safety Committee Date ratified: March 2011 Date issued: June
Transferring critically ill patients in North West London. Transfer data analysis
 Transferring critically ill patients in North West London Transfer data analysis 2010 11 Picture: A typical intensive care (Level 3) patient with a selection of equipment and monitors that would need to
Transferring critically ill patients in North West London Transfer data analysis 2010 11 Picture: A typical intensive care (Level 3) patient with a selection of equipment and monitors that would need to
Scope of Practice for Student Nurses - Undergraduate & Entry to Professional Practice
 Scope of Practice for Student Nurses - Undergraduate & Entry to Professional Practice March 2017 2 nd edition The Royal Children's Hospital (RCH) Scope of Practice for Student Nurses. This scope of practice
Scope of Practice for Student Nurses - Undergraduate & Entry to Professional Practice March 2017 2 nd edition The Royal Children's Hospital (RCH) Scope of Practice for Student Nurses. This scope of practice
DNACPR Policy. Primrose Hospice. Approved by: Candy Cooley, Chairman Originator: Libby Mytton, Director of Care Date of approval: October 2016
 Primrose Hospice DNACPR Policy Approved by: Candy Cooley, Chairman Originator: Libby Mytton, Director of Care Date of approval: October 2016 Signature: The Primrose Hospice Clinical Governance Committee
Primrose Hospice DNACPR Policy Approved by: Candy Cooley, Chairman Originator: Libby Mytton, Director of Care Date of approval: October 2016 Signature: The Primrose Hospice Clinical Governance Committee
Wales Critical Care & Trauma Network (North)
 Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Level 3 Diploma in Healthcare and Social Care Support Skills (QCF)
 Level 3 Diploma in Healthcare and Social Care Support Skills (QCF) Qualification Specification ProQual 2015 Contents Page Introduction 3 The Qualifications and Credit Framework (QCF) 3 Qualification profile
Level 3 Diploma in Healthcare and Social Care Support Skills (QCF) Qualification Specification ProQual 2015 Contents Page Introduction 3 The Qualifications and Credit Framework (QCF) 3 Qualification profile
Admission Record IVF/Gynae
 Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
