Time-Critical Transfer of the Sick or Injured Child (<16 years)
|
|
|
- Avice Glenn
- 6 years ago
- Views:
Transcription
1 LRI Emergency Department Standard Operating Procedure for: Time-Critical Transfer of the Sick or Injured Child (<16 years) Staff relevant to: Medical and Nursing Staff ED senior team approval date: June 2016 Version: 8.2 Revision due: June 2017 Trust Ref: C141/2016 Written by: G Lewis, S Jones, P Barry, C Westrope, B Cagney, K Peiris, C Wighton Time-Critical Transfers v8 Review Date: June
2 0 Minutes By 5 Minutes By 15 Minutes Need for TIME-CRITICAL TRANSFER Identified Departure should occur within a MAXIMUM of 60 minutes ED Doctor in Charge* to contact CICU Consultant and Consultant Paediatric Anaesthetist via Conference Call Discuss, Identify and Release most appropriate & available Personnel to accompany patient as an EMERGENCY If no-one else more appropriate available to accompany the patient: 08:30-17:00 ANAESTHETIC REGISTRAR and CICU NURSE 17:00-08:30 CICU CONSULTANT (or Paeds Trainee) and CICU NURSE KEY PRINCIPLES Life-saving intervention required Not available at LRI Will not benefit from further stabilisation Cannot wait for specialist retrieval TEAM LOOKING AFTER THE PATIENT NOW prepare for Time-Critical transfer whilst transferring team come in: By 30 Minutes Leader 1 THE PROCESS ED Nurse in Charge alert EMAS, request Priority 1 ambulance to ED Resus via Switchboard (7711) CICU release CICU Nurse Paperwork (Checklist 3) Leader 2 THE PATIENT PREPARE (as required) Patient (Checklist 1) Parts (Checklist 2) Parameters (Checklist 4) DO NOT DELAY TRANSFER FOR UNNECESSARY PROCEDURES 60 Minutes MAX Notify receiving centre of departure Medical and Nursing personnel TRANSFER PATIENT Departure should occur within a MAXIMUM of 60 minutes ED, Anaesthetics, CICU and wider Children s Hospital Services Liaise to support any depleted areas. If CICU Consultant is transferring the patient, Paediatric Anaesthetic Consultant to be available to cover CICU. (PICU consultant available to give telephone advice) ESCALATE via Duty Manager System *Outside of the Emergency Department Setting: Attending Medical and Nursing team replace ED Doctor and Nurse in Charge Roles Time-Critical Transfers v8 Review Date: June
3 Key Points: There are rare occasions where paediatric patients require emergency interhospital transfer, to allow life-saving intervention which is not readily available onsite, which cannot wait for stabilisation or retrieval. These will by definition be the sickest children in the hospital at the time. The relevant services within the Children s Hospital will collaborate to support the emergency transfer of these children, and then liaise to support any resulting depletion in services. Introduction, definition and identification There are rare occasions where Children (<16 years) presenting to LRI require emergency inter-hospital transfer based on the following 4 key principles: 1) To allow the provision of life-saving intervention, which: i. is not readily available on-site at LRI ii. will not benefit from further stabilisation iii. cannot safely wait for specialist retrieval The commonest clinical scenario likely to require Time-Critical Transfer from LRI is of a child with an expanding intracranial haemorrhage following a head injury, requiring immediate neurosurgical intervention at the nearest paediatric neurosurgical facility. Other clinical scenarios may be identified based on the application of the above principle. Identification of the need for time-critical transfer may occur via a number of routes including the patient s clinical condition, investigation findings, or on recommendation from a specialist centre. Time-critical transfer of the sick or injured child cannot safely occur without senior involvement from ED, Anaesthetics and CICU. Time-Critical Transfers v8 Review Date: June
4 These children will often by definition be the sickest in the hospital at the time, likely having already required activation of either UHL s paediatric trauma team or paediatric arrest team. As a result, in addition to the ED team, anaesthetic and paediatric intensive care teams are likely to be aware and attending the patient in the ED Resuscitation Room prior to confirming the need for time-critical transfer. It is also likely that the child is already receiving significant airway, breathing and circulatory intervention/support. The over-arching agreement is that once identified, the relevant services within the children s hospital (Anaesthetics, ED, CICU) will collaborate to transfer the patient as SWIFTLY and as SAFELY as possible. Communication with Receiving Centre There will often be prior communication with a receiving centre to notify them of the situation and ensure bed availability. On some occasions it may be the receiving centre that identifies the need for time-critical transfer. This process must not delay a time-critical transfer. Paediatric Major Trauma In this context, as a Trauma Unit within the East Midlands Major Trauma Network, UHL may receive injured children who cannot safely reach the Major Trauma Centre at QMC Nottingham without critical intervention. For example, those requiring urgent airway, breathing or circulatory intervention. In these cases the accompanying paramedic crew will remain with the patient ready for onward transfer. Please complete the Major Trauma Network Transfer Documentation and ensure a copy accompanies the child. Once critical interventions have been performed, if onward transfer to the Major Trauma Centre is still required, it is not necessary to contact the MTC before departure, as a stop, sort, go agreement is in place. However, the decision as to whether any onward transfer is time-critical must be based on the principles above. Once the child has left the department, the receiving centre must then be notified. Departure should occur within a MAXIMUM of 60 minutes of identifying need for time-critical transfer Time-Critical Transfers v8 Review Date: June
5 The Process of Time-Critical Transfer It has been agreed that, on identification and confirmation of the need for time-critical transfer (Based on the 4 key principles outlined above): 1. The ED Doctor in Charge will contact the Duty CICU Consultant and Emergency Paediatric Anaesthetic Consultant urgently. 2. They will identify and release the most appropriate and available doctor to accompany the child on transfer*. 3. ED, Anaesthetic and any additional personnel present will prepare the patient for Time-Critical transfer urgently (see checklists 1-4 below). 4. CICU consultant will liaise with CICU Nurse in Charge to release a nurse (or suitable alternative) from CICU to accompany the patient on transfer. 5. The ED Nurse in Charge will arrange for Emergency Transport to attend Resus, most often a Priority 1 (Next available) EMAS Ambulance. 6. The patient is secured and transferred safely but swiftly, accompanied by appropriate medical and nursing personnel. 7. The receiving centre is notified of the patient s departure and estimated time of arrival. *If no-one else more appropriate is available to accompany the patient, the following applies: 08:30-17:00 ANAESTHETIC REGISTRAR and CICU NURSE 17:00-08:30 CICU CONSULTANT (or Paeds Trainee) and CICU NURSE There must be NO DELAY in releasing resources to transfer the patient Departure should occur within a MAXIMUM of 60 minutes of identifying need for time-critical transfer Once the patient has departed, the ED, Children s Hospital and paediatric anaesthetic services will liaise to support any depleted areas, with escalation as required via the UHL duty management structure. Time-Critical Transfer in the Non-ED Setting It is recognised that rarely a Time-Critical Transfer situation may be identified outside of the Emergency Department setting, for example on a ward or admissions unit. In such a scenario, it is suggested the senior medical and nursing team attending the patient in that area replace the ED Doctor and Nurse in Charge roles in the guideline. Time-Critical Transfers v8 Review Date: June
6 Staff Responsibilities It is acknowledged in advance that in order to act in the best interests of patients staff may have to provide care or interventions that are outside of their normal areas of expertise and in which they may have little or no formal training. Such responsibilities should only be undertaken if no better options are available, and all reasonable efforts should be made to seek advice / assistance from other staff members who may have more experience or formal training in the relevant areas. However, if no better alternative exists the essential requirement is that staff who are prepared to take such responsibilities use all of their existing skills and expertise to provide the best care that they can for the patients involved. Providing that these standards are met and can be confirmed / supported by appropriate documentation it is important that staff members are reassured that they will be fully supported by the Trust in any subsequent developments whether these relate to personal distress, loss of confidence, professional criticisms or even retrospective litigation. Additional Resources o The following Checklists 1-4 are designed to help make transfer as safe and swift as possible. o The PED Resus Drugs Calculator is available via INsite on the ED pages. o CICU Transfer Packs are located with the Paediatric Transfer Bags in Resus and contain: o CICU transfer documentation to complete en-route o CICU Infusion guides o East Midlands Major Trauma Network Transfer Documentation is also available in Resus Performance Measures This SOP is designed to drive safe transfer in time-critical situations. Through: o Rolling audit and review of time-critical paediatric transfers o Monthly analysis of paediatric transfers at the PED Critical Care Forum o Datix reporting of incidents (including adverse events on base as a consequence of reduced staffing). o Investigation and discussion at the monthly Paediatric ITU/Anaesthetic/ED meeting Any issues identified may result in a review of the SOP and further changes being made. References 1. UHL Paediatric ITU/Anaesthetic/ED meeting agreement 2. Embrace Referral Information - Sheffield Children s NHS Foundation Trust: 3. National Ambulance Services Clinical Conveyance Group - Inter-Hospital Transfer Protocol: October South Thames Retrieval Service Guideline: Time Critical Neurosurgical Transfer, S Hanna 2013 Time-Critical Transfers v8 Review Date: June
7 Appendix 1: Checklists. Checklist 1 - Patient Consider and confirm the following before transfer: DO NOT delay for unnecessary procedures ETT secured and position confirmed C-spine immobilisation for any trauma patient Attached to transport ventilator with continuous ETCO 2 monitoring Recent blood gas shows adequate gas exchange and normal blood glucose Gastric Tube placed on free drainage 2 points of IV access well-secured (Do NOT delay for difficult central or arterial access, consider IO) Adequate analgesia, sedation and muscle relaxation Pupillary responses monitored and recorded regularly Seizures controlled and metabolic causes excluded Maintain normothermia (temperature 36 o C-37 o C) unless otherwise advised Urinary Catheterisation Child Secured on Trolley Time-Critical Transfers v8 Review Date: June
8 Checklist 2 Parts (Equipment) The attending ambulance will provide a compatible transfer trolley If available, the dedicated CICU transport system is a desirable alternative DO NOT unnecessarily delay transfer. Otherwise, the equipment required to safely transfer a child in an emergency is readily available in the Emergency Department: Transport ventilator and circuit Oxylog 3000 (Starting settings: PEEP 5 / rate / Ti 1.0 / PIP to move chest) Gas supply (FULL and Spare) Ambu bag and mask on trolley Patient transport monitoring: ECG SaO 2 ETCO 2 BP Temperature Infusion pumps Transport Bag with Emergency Airway, Breathing and Circulation equipment Emergency Fluids and drugs Print off Children s ED Resus Drug Dose Calculator CICU Transfer pack East Midlands Major Trauma Network Transfer Form (Where applicable) Time-Critical Transfers v8 Review Date: June
9 Checklist 3 Paperwork (Documentation/Communication) Maintain clear lines of communication at all times within the team and to the designated receiving centre Update any parents/carers present on: the child s condition plans for transfer map / directions to destination and contact details Ensure transfer team have parents/carers contact details Photocopies of all (to accompany the patient): recent relevant notes investigation results drug charts Highlight/document any social concerns Ensure transfer of radiology investigations electronically (or hard copy/cd) Update receiving centre on departure Print off Children s ED Resus Drug Dose Calculator sheet Commence CICU transfer documentation pack and continue en route Time-Critical Transfers v8 Review Date: June
10 Checklist 4: Parameters If any concerns or deterioration update CICU consultant O 2 Saturations > 98% General Strategy: NO HYPOXIA or HYPOTENSION Maintain Systolic BP Approximate targets for age o <1yr >80 o 1-5yr >90 o 5-14yr >100 o >14yr >110 Maintain ETCO 2 4-5kPa Keep temperature o C Identify and treat seizures Maintain normal blood Glucose Maintenance fluid 1-2mls/kg 0.9% Saline +/- Dextrose Intracranial Pressure Spikes: Bradycardia, Hypertension, Pupil dilatation Ensure ETCO2 4-5 Give 2-3 mls/kg hypertonic saline (2.7%) Or Give 0.5g/kg 20% Mannitol Sedate Keep Moving Ensure child secure Transfer to Ambulance and Onward Journey Switch to vehicle O2 supply ASAP Request as smooth journey as possible Seatbelts worn when vehicle moving Note Observations every 15 minutes including pupil response Record on CICU Transfer documentation Time-Critical Transfers v8 Review Date: June
ISOLATED HEAD INJURY. MODULE: Intensive Care Medicine / Trauma ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND:
 ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
Version No Authored/Reviewed by Review Date 1.0 Carol Newman / Caroline Fox January Carol Newman October 2011
 Guideline for transferring Children (0-16yrs) Guideline Register no 09005 Status: Public Developed in response to: Good practice Contributes to CQC Outcome Outcome 4 Consulted With Individual/Body Date
Guideline for transferring Children (0-16yrs) Guideline Register no 09005 Status: Public Developed in response to: Good practice Contributes to CQC Outcome Outcome 4 Consulted With Individual/Body Date
Standard Operating Procedure. for the Retrieval Nurse
 Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
the victorian paediatric emergency transport service pets
 the victorian paediatric emergency transport service pets The Victorian Paediatric Emergency Transport Service The Victorian Paediatric Emergency Transport Service (PETS) is based at the Paediatric Intensive
the victorian paediatric emergency transport service pets The Victorian Paediatric Emergency Transport Service The Victorian Paediatric Emergency Transport Service (PETS) is based at the Paediatric Intensive
Modified Early Warning Score Policy.
 Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
GAMUT QI Collaborative Consensus Quality Metrics (v. 05/16/2016)
 1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
The ROHNHSFT Experience: Implementing BWCH PEWS
 The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
Recognising a Deteriorating Patient. Study guide
 Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Anaesthetic Trainees- The Trauma Call at SMH
 Anaesthetic Trainees- The Trauma Call at SMH Anaesthetic staff at a trauma call Bleep Grade Times 1201 Consultant 08:00 18:00 SpR on-call for theatres 18:00 08:00 6348 Extra SpR 08:00 17:00 Obstetric SpR
Anaesthetic Trainees- The Trauma Call at SMH Anaesthetic staff at a trauma call Bleep Grade Times 1201 Consultant 08:00 18:00 SpR on-call for theatres 18:00 08:00 6348 Extra SpR 08:00 17:00 Obstetric SpR
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT
 CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines. Version 1.0
 South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines Version 1.0 Ratified: 28 th August 2018 Date for Review: 28 th August 2019 Suzanne.sweeney@uclpartners.com South London
South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines Version 1.0 Ratified: 28 th August 2018 Date for Review: 28 th August 2019 Suzanne.sweeney@uclpartners.com South London
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
DETERIORATING PATIENT & RESUSCITATION POLICY
 DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Base Hospital Advanced Life Support Program for Durham Region
 Title: Purpose and Goals of the Base Hospital Program Number: 2.1 Category: 2.0 Base Hospital Roles and Responsibilities Written By: M. Epp Approved By: Dr. R. Vandersluis Issue Date: October 2002 Review
Title: Purpose and Goals of the Base Hospital Program Number: 2.1 Category: 2.0 Base Hospital Roles and Responsibilities Written By: M. Epp Approved By: Dr. R. Vandersluis Issue Date: October 2002 Review
Recommended Minimum Facilities for Safe Anaesthetic Practice in Organ Imaging Units
 Page 1 of 7 Recommended Minimum Facilities for Safe Anaesthetic Practice in Organ Imaging Units Version Effective Date 1 Oct 1992 (reviewed Feb 02) 2 Nov 2011 3 Dec 2016 Document No. HKCA T3 v3 Prepared
Page 1 of 7 Recommended Minimum Facilities for Safe Anaesthetic Practice in Organ Imaging Units Version Effective Date 1 Oct 1992 (reviewed Feb 02) 2 Nov 2011 3 Dec 2016 Document No. HKCA T3 v3 Prepared
SAFE STAFFING GUIDELINE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline title SAFE STAFFING GUIDELINE SCOPE 1. Safe staffing for nursing in accident and emergency departments Background 2. The National Institute for
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline title SAFE STAFFING GUIDELINE SCOPE 1. Safe staffing for nursing in accident and emergency departments Background 2. The National Institute for
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY V2. Transfer Policy for Neonates, Infants and Children Page 1 of 36
 TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
Scottish Ambulance Service. Job Description
 1. JOB IDENTIFICATION Scottish Ambulance Service Job Description Job Title: Neonatal Transport Nurse Department(s): Specialist Transport & Retrieval (SCOTSTAR) Job Holder Reference: No of Job Holders:
1. JOB IDENTIFICATION Scottish Ambulance Service Job Description Job Title: Neonatal Transport Nurse Department(s): Specialist Transport & Retrieval (SCOTSTAR) Job Holder Reference: No of Job Holders:
Standard Operating Procedure Hospital Pre-alert & Patient Handover
 Standard Operating Procedure Hospital Pre-alert & Patient Handover No of Pages: 6 Unique reference No: Implementation date: 17 th May 2010 Version: Final Version 2.0 Next review date: May 2013 Title of
Standard Operating Procedure Hospital Pre-alert & Patient Handover No of Pages: 6 Unique reference No: Implementation date: 17 th May 2010 Version: Final Version 2.0 Next review date: May 2013 Title of
Guideline for Neonatal Resuscitation GL443
 Guideline for Neonatal Resuscitation GL443 Approval and Authorisation Approved by Job Title, Chair of Committee Date Paediatric Governance Policy and Procedure Subcommittee Chair of Paediatric Clinical
Guideline for Neonatal Resuscitation GL443 Approval and Authorisation Approved by Job Title, Chair of Committee Date Paediatric Governance Policy and Procedure Subcommittee Chair of Paediatric Clinical
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS
 HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
PRACTICE GUIDELINE EM014 IMPLEMENTATION OF THE SOUTH AFRICAN TRIAGE SCALE
 PRACTICE GUIDELINE EM014 IMPLEMENTATION OF THE SOUTH AFRICAN TRIAGE SCALE This Practice Guideline sets out a method for implementing triage in the Emergency Centre. Excluding the cover page, this Practice
PRACTICE GUIDELINE EM014 IMPLEMENTATION OF THE SOUTH AFRICAN TRIAGE SCALE This Practice Guideline sets out a method for implementing triage in the Emergency Centre. Excluding the cover page, this Practice
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care
 Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
Acutely ill patients in hospital
 Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals
 Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
A AIRWAY Open the Airway B BREATHING Deliver two (2) Breaths. Code Blue Policy. Indications for Calling A Code Blue
 Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
Enhanced Recovery Programme
 Enhanced Recovery Programme Page 14 Contact details South Tyneside NHS Foundation Trust Harton Lane South Shields Tyne and Wear NE34 0PL For advice please contact ward 1 on 4041001 Or ward 3 on 0191 4041003.
Enhanced Recovery Programme Page 14 Contact details South Tyneside NHS Foundation Trust Harton Lane South Shields Tyne and Wear NE34 0PL For advice please contact ward 1 on 4041001 Or ward 3 on 0191 4041003.
Adult Critical Care Transfer Guidelines
 Adult Critical Care Transfer Guidelines Revised 2017 Transfer Forum Members: Dr Simon Whiteley, Chair of the West Yorkshire Critical Care ODN Transfer Forum Dr Jonathon Ball, Bradford Teaching Hospital
Adult Critical Care Transfer Guidelines Revised 2017 Transfer Forum Members: Dr Simon Whiteley, Chair of the West Yorkshire Critical Care ODN Transfer Forum Dr Jonathon Ball, Bradford Teaching Hospital
APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER
 APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER We are carrying out a survey to establish the quality of anaesthesia care provided to Obstetric patients in East Africa. We therefore
APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER We are carrying out a survey to establish the quality of anaesthesia care provided to Obstetric patients in East Africa. We therefore
Standard Operating Procedure INTER-HOSPITAL TRANSFERS
 Standard Operating Procedure INTER-HOSPITAL TRANSFERS DATE APPROVED: September 2010 APPROVED BY: Air Operations Manager IMPLEMENTATION DATE: November 2014 REVIEW DATE: November 2015 LEAD DIRECTOR: IMPACT
Standard Operating Procedure INTER-HOSPITAL TRANSFERS DATE APPROVED: September 2010 APPROVED BY: Air Operations Manager IMPLEMENTATION DATE: November 2014 REVIEW DATE: November 2015 LEAD DIRECTOR: IMPACT
Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee
 The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients
 UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
Importance of Effective Training and Support During the Preceptorship period
 Importance of Effective Training and Support During the Preceptorship period Alison Dinning Inter professional Education lead Nursing Development Student nurse retention in East Midlands 4.2 million wasted
Importance of Effective Training and Support During the Preceptorship period Alison Dinning Inter professional Education lead Nursing Development Student nurse retention in East Midlands 4.2 million wasted
Australian and New Zealand College of Anaesthetists (ANZCA)
 PS08 2016 Australian and New Zealand College of Anaesthetists (ANZCA) Statement on the Assistant for the Anaesthetist 1. PURPOSE The purpose of this document is to recognise the importance of and to promote
PS08 2016 Australian and New Zealand College of Anaesthetists (ANZCA) Statement on the Assistant for the Anaesthetist 1. PURPOSE The purpose of this document is to recognise the importance of and to promote
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: Early Warning Score Policy Version: 6 (May 2010) Amended version Reference Number: Supersedes Originator or modifier Approval Supersedes: EWS Policy v5 2009 August 2009
DOCUMENT CONTROL PAGE Title Title: Early Warning Score Policy Version: 6 (May 2010) Amended version Reference Number: Supersedes Originator or modifier Approval Supersedes: EWS Policy v5 2009 August 2009
Wales and West Acute Transport for Children (WATCh)
 Patient information service Bristol Royal Hospital for Children Noah s Ark Children s Hospital for Wales Wales and West Acute Transport for Children (WATCh) Respecting everyone Embracing change Recognising
Patient information service Bristol Royal Hospital for Children Noah s Ark Children s Hospital for Wales Wales and West Acute Transport for Children (WATCh) Respecting everyone Embracing change Recognising
Brief Summary. Educational Rationale. Learning Objectives: Nurse. Learning Objectives: Doctor
 Simulation Scenario Title Bacterial meningitis Version 10 Target Audience FY doctors & student nurses Run time 10-15 mins Authors Niamh Feely, Andrew Smith, Udesh Naidoo, Paul Wilder, Mark Loughrey Last
Simulation Scenario Title Bacterial meningitis Version 10 Target Audience FY doctors & student nurses Run time 10-15 mins Authors Niamh Feely, Andrew Smith, Udesh Naidoo, Paul Wilder, Mark Loughrey Last
PICU tracheostomy protocol
 PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL
 PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS Revised April 2013 Liverpool Heart and Chest Hospital Aintree University Hospital Countess
PRIMARY PERCUTANEOUS CORONARY INTERVENTION (PPCI) PROTOCOL EXTRACT FOR USE BY NORTH WEST AMBULANCE SERVICE PARAMEDICS Revised April 2013 Liverpool Heart and Chest Hospital Aintree University Hospital Countess
Clinical Guideline Trauma Care: Accessing Trauma Services
 Clinical Guideline Trauma Care: Accessing Trauma Services Guideline ID CG24 Version 1.2 Title Approved by Trauma Care: Accessing Trauma Services Clinical Effectiveness Group Date Issued 17/03/2017 Review
Clinical Guideline Trauma Care: Accessing Trauma Services Guideline ID CG24 Version 1.2 Title Approved by Trauma Care: Accessing Trauma Services Clinical Effectiveness Group Date Issued 17/03/2017 Review
DATA COLLECTION SHEET (NURSES)
 ANNEXURE A DATA COLLECTION SHEET (NURSES) 1.0 NURSES DEMOGRAPHIC DATA 1.1 Research Code 1.2 Professional Qualification 1.3 Shift Day Night 1.3 Years of Nursing Experience Years Months 1.4 Period Working
ANNEXURE A DATA COLLECTION SHEET (NURSES) 1.0 NURSES DEMOGRAPHIC DATA 1.1 Research Code 1.2 Professional Qualification 1.3 Shift Day Night 1.3 Years of Nursing Experience Years Months 1.4 Period Working
Transfer of Patients between Hospitals
 Contents Contents... 1 Policy... 2 Purpose... 2 Scope/Audience... 2 Exemptions to this policy... 2 Definitions... 2 EWS... 2 Designated person... 2 Associated documents... 3 1 Outline of Responsibilities...
Contents Contents... 1 Policy... 2 Purpose... 2 Scope/Audience... 2 Exemptions to this policy... 2 Definitions... 2 EWS... 2 Designated person... 2 Associated documents... 3 1 Outline of Responsibilities...
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Admission Record IVF/Gynae
 Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
Resuscitation Procedure
 Reference Number: UHB 227 Version Number: 2 Date of Next Review: 07 Jun 2020 Previous Trust/LHB Reference Number: Resuscitation Procedure Introduction and Aim The provision of an efficient, expedient and
Reference Number: UHB 227 Version Number: 2 Date of Next Review: 07 Jun 2020 Previous Trust/LHB Reference Number: Resuscitation Procedure Introduction and Aim The provision of an efficient, expedient and
PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE
 PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE Introduction There are currently over 500 Critical Care Transfers carried out in
PERSONNEL DOCUMENTATION QUALITY ASSURANCE & AUDIT, INSURANCE NORTH WALES CRITICAL CARE NETWORK TRANSFER TRAINING COURSE Introduction There are currently over 500 Critical Care Transfers carried out in
GUIDANCE. Clinical Guideline MATERNAL CRITICAL CARE. Central Delivery Suite, St Michael s Hospital. Medical, nursing and midwifery staff
 Clinical Guideline MATERNAL CRITICAL CARE SETTING FOR STAFF PATIENTS Central Delivery Suite, St Michael s Hospital Medical, nursing and midwifery staff Patients requiring Maternal Critical Care GUIDANCE
Clinical Guideline MATERNAL CRITICAL CARE SETTING FOR STAFF PATIENTS Central Delivery Suite, St Michael s Hospital Medical, nursing and midwifery staff Patients requiring Maternal Critical Care GUIDANCE
Example Care Pathways
 Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
FALLS RISK REDUCTION & MANAGEMENT OF INPATIENT FALLS - STANDARDS
 STANDARDS TO BE MET 1. Safe Mobilisation and Falls Prevention Assessment 1.1 The multidisciplinary team will: a) Conduct the Safe Mobilisation and Fall Prevention Assessment; b) Initiate appropriate interventions
STANDARDS TO BE MET 1. Safe Mobilisation and Falls Prevention Assessment 1.1 The multidisciplinary team will: a) Conduct the Safe Mobilisation and Fall Prevention Assessment; b) Initiate appropriate interventions
Mental Health Short Stay
 Mental Health Directorate Central Adelaide Local Health Network Mental Health Short Stay Model of Care January 2016 Extracted from Improving Unplanned Emergency Access pathways (IUEAP) Model of Care: Mental
Mental Health Directorate Central Adelaide Local Health Network Mental Health Short Stay Model of Care January 2016 Extracted from Improving Unplanned Emergency Access pathways (IUEAP) Model of Care: Mental
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue. The Development and Implementation of a Rapid Response Program at a Regional Facility
 Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Z: Perioperative Nursing Specialty
 Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Management of surge and escalation in critical care services: standard operating procedure for adult respiratory extra corporeal membrane oxygenation
 Management of surge and escalation in critical care services: standard operating procedure for adult respiratory extra corporeal membrane oxygenation 1 NHS England INFORMATION READER BOX Directorate Medical
Management of surge and escalation in critical care services: standard operating procedure for adult respiratory extra corporeal membrane oxygenation 1 NHS England INFORMATION READER BOX Directorate Medical
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Transferring critically ill patients in North West London. Transfer data analysis
 Transferring critically ill patients in North West London Transfer data analysis 2010 11 Picture: A typical intensive care (Level 3) patient with a selection of equipment and monitors that would need to
Transferring critically ill patients in North West London Transfer data analysis 2010 11 Picture: A typical intensive care (Level 3) patient with a selection of equipment and monitors that would need to
Retrieval Advanced Critical Care Practitioner Job Description
 Retrieval Advanced Critical Care Practitioner Job Description ScotSTAR February 2013 1 Job Title Location Line Manager Retrieval Advanced Critical Care Practitioner (ACCP) ScotSTAR base Glasgow Lead ACCP
Retrieval Advanced Critical Care Practitioner Job Description ScotSTAR February 2013 1 Job Title Location Line Manager Retrieval Advanced Critical Care Practitioner (ACCP) ScotSTAR base Glasgow Lead ACCP
Clinical Care Pathway for BRAIN TUMOURS in Childhood.
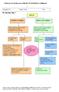 - 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
- 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
Guidelines for the transport of the critically ill adult (3rd Edition 2011)
 The Intensive Care Society Guidelines for the transport of the critically ill adult (3rd Edition 2011) Prepared on behalf of the council of the Intensive Care Society by: Simon Whiteley Ian Macartney Julian
The Intensive Care Society Guidelines for the transport of the critically ill adult (3rd Edition 2011) Prepared on behalf of the council of the Intensive Care Society by: Simon Whiteley Ian Macartney Julian
Norwegian Standard for the Safe Practice of Anaesthesia
 Norwegian Standard for the Safe Practice of Anaesthesia 1. Introduction The Norwegian standard for the safe practice of anaesthesia was first published in 1991. It was then revised in 1994, and subsequently
Norwegian Standard for the Safe Practice of Anaesthesia 1. Introduction The Norwegian standard for the safe practice of anaesthesia was first published in 1991. It was then revised in 1994, and subsequently
Implementation of the 10 minute meeting: a user s guide
 Implementation of the 10 minute meeting: a user s guide How a short daily meeting can save lives by helping emergency teams work together more effectively. What s the issue? A critical care outreach team
Implementation of the 10 minute meeting: a user s guide How a short daily meeting can save lives by helping emergency teams work together more effectively. What s the issue? A critical care outreach team
Paediatrics. PEWS & Deteriorating Patients Linda Clerihew
 Paediatrics PEWS & Deteriorating Patients Linda Clerihew SPSP 2007 SPSPP 2010 McQIC 2013 Aim 30% reduction in avoidable harm measured by the Paediatric Serious Harm Key Indicators by December 2015 Measuring
Paediatrics PEWS & Deteriorating Patients Linda Clerihew SPSP 2007 SPSPP 2010 McQIC 2013 Aim 30% reduction in avoidable harm measured by the Paediatric Serious Harm Key Indicators by December 2015 Measuring
VERIFICATION OF LIFE EXTINCT POLICY DECEMBER Verification of Life Extinct Policy December 2009 Page 1 of 18
 VERIFICATION OF LIFE EXTINCT POLICY DECEMBER 2009 Page 1 of 18 POLICY TITLE: Verification of Life Extinct Policy POLICY REFERENCE NUMBER: Med01/009 IMPLEMENTATION DATE: December 2009 REVIEW DATE: December
VERIFICATION OF LIFE EXTINCT POLICY DECEMBER 2009 Page 1 of 18 POLICY TITLE: Verification of Life Extinct Policy POLICY REFERENCE NUMBER: Med01/009 IMPLEMENTATION DATE: December 2009 REVIEW DATE: December
Minimum equipment and drug lists for cardiopulmonary resuscitation. Mental health Inpatient care
 Minimum equipment and drug lists for cardiopulmonary resuscitation Mental health Inpatient care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Published by
Minimum equipment and drug lists for cardiopulmonary resuscitation Mental health Inpatient care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Published by
SOUTH CENTRAL AMBULANCE SERVICE NHS TRUST CLINICAL SERVICES POLICY & PROCEDURE EMERGENCY CARE ASSISTANTS. March 2011
 SOUTH CENTRAL AMBULANCE SERVICE NHS TRUST CLINICAL SERVICES POLICY & PROCEDURE EMERGENCY CARE ASSISTANTS March 2011 DOCUMENT INFORMATION Author: Fizz Thompson Director of Clinical Services Consultation
SOUTH CENTRAL AMBULANCE SERVICE NHS TRUST CLINICAL SERVICES POLICY & PROCEDURE EMERGENCY CARE ASSISTANTS March 2011 DOCUMENT INFORMATION Author: Fizz Thompson Director of Clinical Services Consultation
anaesthetic services Chapter 15 Services for neuroanaesthesia and neurocritical care 2014 GUIDELINES FOR THE PROVISION OF ACSA REFERENCES
 Chapter 15 GUIDELINES FOR THE PROVISION OF anaesthetic services ACSA REFERENCES 15.1.1 15.1.2 15.1.3 15.1.4 15.1.5 15.1.8 15.1.9 15.1.11 15.2.1 15.2.9 15.2.13 15.2.17 15.2.18 15.2.19 15.3.2 15.4.2 15.5.1
Chapter 15 GUIDELINES FOR THE PROVISION OF anaesthetic services ACSA REFERENCES 15.1.1 15.1.2 15.1.3 15.1.4 15.1.5 15.1.8 15.1.9 15.1.11 15.2.1 15.2.9 15.2.13 15.2.17 15.2.18 15.2.19 15.3.2 15.4.2 15.5.1
Resuscitation Policy Policy PROV 03
 Resuscitation Policy Policy PROV 03 March 2009 1 Document Management Title of document PROV 03 Resuscitation Policy Type of document Description Target audience Author Department Directorate Approved by
Resuscitation Policy Policy PROV 03 March 2009 1 Document Management Title of document PROV 03 Resuscitation Policy Type of document Description Target audience Author Department Directorate Approved by
1. Receives report from EMS and/or outlying facility. 5. Adheres to safety and universal precaution guidelines.
 Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Medical Simulation Orientation
 Medical Simulation Orientation Familiarization with IMSE s METI ECS Simulation Manikin Getting to know the Simulator Aims and Goals of Orientation To allow participants to familiarize themselves with the
Medical Simulation Orientation Familiarization with IMSE s METI ECS Simulation Manikin Getting to know the Simulator Aims and Goals of Orientation To allow participants to familiarize themselves with the
Student Nurses. Surgical Assessment and Planning Unit-SAPU. Student Name: SAPU
 Student Nurses Surgical Assessment and Planning Unit-SAPU Student Name: SAPU Kathy Trezise [CCDHB]Jane Bilik CCDHBPage 1 2/3/2016 SAPU (Surgical Assessment and Planning Unit) is an assessment unit that
Student Nurses Surgical Assessment and Planning Unit-SAPU Student Name: SAPU Kathy Trezise [CCDHB]Jane Bilik CCDHBPage 1 2/3/2016 SAPU (Surgical Assessment and Planning Unit) is an assessment unit that
AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS
 AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS Issue:- Version2 Issue Date:- March2014 Review Date:- March 2017 Issued To:- All staff AICU Consultant Jonathan Chantler, Senior Sister
AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS Issue:- Version2 Issue Date:- March2014 Review Date:- March 2017 Issued To:- All staff AICU Consultant Jonathan Chantler, Senior Sister
Ambulatory Emergency Care The Logical Way to Go
 Ambulatory Emergency Care The Logical Way to Go Ambulatory Emergency Care The Logical Way to Go The Queens Medical Centre (QMC) is part of the Nottingham University Hospitals NHS Trust, one of the largest
Ambulatory Emergency Care The Logical Way to Go Ambulatory Emergency Care The Logical Way to Go The Queens Medical Centre (QMC) is part of the Nottingham University Hospitals NHS Trust, one of the largest
Pediatric Emergencies and Resuscitation. Color Coding Kids to optimize patient safety
 Pediatric Emergencies and Resuscitation Color Coding Kids to optimize patient safety Susan Hohenhaus, RN Project Manager Duke University Medical Center Department of Pediatric Emergency Medicine EMSC Enhancing
Pediatric Emergencies and Resuscitation Color Coding Kids to optimize patient safety Susan Hohenhaus, RN Project Manager Duke University Medical Center Department of Pediatric Emergency Medicine EMSC Enhancing
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 13th March 2014 Compliance
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 13th March 2014 Compliance
Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery
 CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
SBAR Communication Tool. Anne Marie Oglesby RGN., MSc. Health Care (Risk Management & Quality) Clinical Risk Advisor, Clinical Indemnity Scheme
 SBAR Communication Tool Anne Marie Oglesby RGN., MSc. Health Care (Risk Management & Quality) Clinical Risk Advisor, Clinical Indemnity Scheme Background Communication Tools What is SBAR SBAR in action
SBAR Communication Tool Anne Marie Oglesby RGN., MSc. Health Care (Risk Management & Quality) Clinical Risk Advisor, Clinical Indemnity Scheme Background Communication Tools What is SBAR SBAR in action
Indications for Calling A Code Blue or Pediatric Medical Emergency
 Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
Adult Retrieval Victoria -An update. DR EMMELINE FINN Clinical lead (Acting)
 Adult Retrieval Victoria -An update DR EMMELINE FINN Clinical lead (Acting) My Background Emergency Physician by trade Pre-hospital and Retrieval Medicine Specialist Disaster Management MIMMS and EMERGO
Adult Retrieval Victoria -An update DR EMMELINE FINN Clinical lead (Acting) My Background Emergency Physician by trade Pre-hospital and Retrieval Medicine Specialist Disaster Management MIMMS and EMERGO
Guide to the Anglia Ruskin Paramedic Science Practice Assessment Document
 Guide to the Anglia Ruskin Paramedic Science Practice Assessment Document Valid for Academic Year 2016/7 www.anglia.ac.uk Page 1 Purpose of this document This document is to give you, and your mentor a
Guide to the Anglia Ruskin Paramedic Science Practice Assessment Document Valid for Academic Year 2016/7 www.anglia.ac.uk Page 1 Purpose of this document This document is to give you, and your mentor a
Prone Ventilation of the Critically Ill Patient
 Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Summary of Significant Changes. Policy. Purpose. Responsibilities. Definitions
 This Management Process Description replaces MPD880/5 Copy Number Summary of Significant Changes Effective 22/09/17 Reformatting of document numbering and bullet points. Update with the new 5 hour rule
This Management Process Description replaces MPD880/5 Copy Number Summary of Significant Changes Effective 22/09/17 Reformatting of document numbering and bullet points. Update with the new 5 hour rule
ECMO a parent and family guide
 ECMO a parent and family guide This leaflet aims to provide you with some basic information about ECMO, and will hopefully answer some questions that you may have in helping to decide on ECMO for your
ECMO a parent and family guide This leaflet aims to provide you with some basic information about ECMO, and will hopefully answer some questions that you may have in helping to decide on ECMO for your
News. Ventilation procedures for intensive care air transports. Critical care
 NO. 11 News Critical care Ventilation procedures for intensive care air transports Critical Care News is published by Maquet Critical Care. Maquet Critical Care AB 171 95 Solna, Sweden Phone: +46 (0)10
NO. 11 News Critical care Ventilation procedures for intensive care air transports Critical Care News is published by Maquet Critical Care. Maquet Critical Care AB 171 95 Solna, Sweden Phone: +46 (0)10
5 Moments for Hand Hygiene
 5 Moments for Hand Hygiene Moment 1 Before Touching a Patient Patient Refers to any part of the patient, their clothes, or any medical device that is connected to the patient If the patient were to get
5 Moments for Hand Hygiene Moment 1 Before Touching a Patient Patient Refers to any part of the patient, their clothes, or any medical device that is connected to the patient If the patient were to get
EMRTS Cymru Overview
 EMRTS Cymru Overview (Published 07/04/16) 1 Who are we? The Emergency Medical Retrieval and Transfer Service (EMRTS Cymru) is an exciting new service that provides consultantdelivered pre-hospital critical
EMRTS Cymru Overview (Published 07/04/16) 1 Who are we? The Emergency Medical Retrieval and Transfer Service (EMRTS Cymru) is an exciting new service that provides consultantdelivered pre-hospital critical
Patient Sticker Paracentesis Ambulatory Emergency Care Pathway
 Patient Sticker Paracentesis Ambulatory Emergency Care Pathway 1 Patient Sticker Consultant: Dr M Oldfield Consultant: Dr D Harris Lead Nurse: Catie Paterson Ambulatory Emergency Care (AEC) Unit Open:
Patient Sticker Paracentesis Ambulatory Emergency Care Pathway 1 Patient Sticker Consultant: Dr M Oldfield Consultant: Dr D Harris Lead Nurse: Catie Paterson Ambulatory Emergency Care (AEC) Unit Open:
Women s and Children s Division. LNWH Paediatric Implementation Plan.
 Women s and Children s Division LNWH Paediatric Implementation Plan. 1. Purpose On the 18 th May 2016 the Ealing CCG Board formally agreed to implement changes to paediatric services on the Ealing Hospital
Women s and Children s Division LNWH Paediatric Implementation Plan. 1. Purpose On the 18 th May 2016 the Ealing CCG Board formally agreed to implement changes to paediatric services on the Ealing Hospital
This notice is served under Section 29 of the Health and Social Care Act 2008.
 By Email and Recorded Delivery Mr Mark Newbold Heart of England NHS Foundation Trust Bordesley Green East Birmingham West Midlands B9 5SS CQC Representations Citygate Gallowgate Newcastle upon Tyne NE1
By Email and Recorded Delivery Mr Mark Newbold Heart of England NHS Foundation Trust Bordesley Green East Birmingham West Midlands B9 5SS CQC Representations Citygate Gallowgate Newcastle upon Tyne NE1
Adult Observation Chart Policy (Incorporating National Early Warning Score NEWS)
 Adult Observation Chart Policy (Incorporating National Early Warning Score NEWS) Document Author Written By: Sister Critical Care Outreach Service Authorised Authorised By: Chief Executive Date: 1 st April
Adult Observation Chart Policy (Incorporating National Early Warning Score NEWS) Document Author Written By: Sister Critical Care Outreach Service Authorised Authorised By: Chief Executive Date: 1 st April
Level 4 Trauma Hospital Criteria
 Level 4 Trauma Hospital Criteria Hospital Commitment The board of directors, administration, and medical, nursing and ancillary staff shall make a commitment to providing trauma care commensurate to the
Level 4 Trauma Hospital Criteria Hospital Commitment The board of directors, administration, and medical, nursing and ancillary staff shall make a commitment to providing trauma care commensurate to the
NORTH WEST REGIONAL POLICY AND GUIDANCE FOR CONVEYING MENTAL HEALTH PATIENTS
 NORTH WEST REGIONAL POLICY AND GUIDANCE FOR CONVEYING MENTAL HEALTH PATIENTS Page 1 of 20 Approved by North West Regional Mental Health Forum Approval date 13 th February 2013 Version number 1.0 Review
NORTH WEST REGIONAL POLICY AND GUIDANCE FOR CONVEYING MENTAL HEALTH PATIENTS Page 1 of 20 Approved by North West Regional Mental Health Forum Approval date 13 th February 2013 Version number 1.0 Review
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012
 Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition
 Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Circumstances of Injury: Cause of burn %Burn Smoke Inhalation: Yes No How accident happened:
 Shriners Hospitals for Children Date: Galveston Burn Hospital Time: 815 Market Street Resource: Galveston, Texas 77550 Contact: Referral Calls: 409-770-6773 Fax #: 409-770-6539 Patient Name: Sex: Home
Shriners Hospitals for Children Date: Galveston Burn Hospital Time: 815 Market Street Resource: Galveston, Texas 77550 Contact: Referral Calls: 409-770-6773 Fax #: 409-770-6539 Patient Name: Sex: Home
Roles and responsibilities of adult/paediatric cardiac arrest bleep holders: QMC/City Campus
 Roles and responsibilities of adult/paediatric cardiac arrest bleep holders: QMC/City Campus Who should attend a 2222 cardiac arrest call? There are 2 types of responders to adult/paediatric cardiac arrest
Roles and responsibilities of adult/paediatric cardiac arrest bleep holders: QMC/City Campus Who should attend a 2222 cardiac arrest call? There are 2 types of responders to adult/paediatric cardiac arrest
Patient Sticker Blood Transfusion Ambulatory Emergency Care Pathway
 Patient Sticker Blood Transfusion Ambulatory Emergency Care Pathway 1 Patient Sticker Consultant: Dr M Oldfield Consultant: Dr D Harris Lead Nurse: Catie Paterson Ambulatory Emergency Care (AEC) Unit Open:
Patient Sticker Blood Transfusion Ambulatory Emergency Care Pathway 1 Patient Sticker Consultant: Dr M Oldfield Consultant: Dr D Harris Lead Nurse: Catie Paterson Ambulatory Emergency Care (AEC) Unit Open:
Welcome to the Cardiac Intensive Care Unit (CICU) at GOSH
 Welcome to the Cardiac Intensive Care Unit (CICU) at GOSH Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 The Cardiac Intensive Care Unit (CICU) at Great Ormond
Welcome to the Cardiac Intensive Care Unit (CICU) at GOSH Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 The Cardiac Intensive Care Unit (CICU) at Great Ormond
