anaesthetic services Chapter 15 Services for neuroanaesthesia and neurocritical care 2014 GUIDELINES FOR THE PROVISION OF ACSA REFERENCES
|
|
|
- Stewart Hubbard
- 5 years ago
- Views:
Transcription
1 Chapter 15 GUIDELINES FOR THE PROVISION OF anaesthetic services ACSA REFERENCES Services for neuroanaesthesia and neurocritical care 2014 Author Dr I E Tweedie, The Walton Centre, Liverpool Approved by the Neuroanaesthesia Society of Great Britain and Ireland (NASGBI) When considering the provision of anaesthesia, the Royal College of Anaesthetists recommends that the following areas should be addressed. The goal is to ensure a comprehensive, quality service dedicated to the care of patients and to the education and professional development of staff. The provision of adequate funding to provide the services described should be considered. These recommendations form the basis of the standard expected for departmental accreditation.
2 Summary Neuroanaesthesia should only take place in a designated neuroscience centre. There should be sufficient numbers of clinical programmed activities in consultants job plans to provide cover for all elective neurosurgical operating lists and interventional neuroradiology sessions, and also to provide adequate emergency cover. 1 Staffing levels in the operating theatre should be sufficient to allow neuroanaesthetists to work in teams during long and complex operations. 2 There should be a designated consultant lead for neurocritical care and sufficient consultant sessions to provide daytime and out-of-hours cover. 3 There should be sufficient numbers of neurosurgical critical care beds to allow timely access for patients from within an agreed geographical area. Management of critically ill patients outside the critical care unit should take place only in exceptional circumstances. 3 The care of head-injured patients is an integral part of neuroanaesthesia and neurocritical care. Units accepting head-injured patients must have specific arrangements in place, including evidence-based protocols, appropriately trained staff and sufficient resource to allow timely access for those requiring life-saving surgery. 3 6 Protocols and appropriate facilities should be in place for transfer of critically ill neuroscience patients between hospitals, and within neuroscience units. 7 8 Specific consideration should be given to the provision of anaesthetic services for paediatric imaging and neurosurgery, although life-saving emergency procedures may need to be performed in an adult unit prior to transfer The provision in neurocritical care of specialist nurses for advice on organ donation ensures it is considered in all end-of-life decisions, as well as providing bereavement counselling and support Guidelines for the Provision of Anaesthetic Services 2014
3 Introduction: the importance of neuroanaesthesia and neurocritical care services Anaesthesia for neurosurgery (neuroanaesthesia) is based in recognised neuroscience centres, which allow the grouping together of the interrelated specialties required to support neurosurgery. These centres, whether they are in specialist, teaching or district general hospitals, should provide neurosurgical, neurological, neuroradiological and other supporting specialist and general services necessary for the management of patients with neurological disease. The provision of adequate numbers of neurocritical care beds is a prerequisite for the delivery of such specialist services. 3 The centralisation of neuroscience practice is essential to ensure critical mass for delivery of efficient and high quality clinical care. The pace of development, and the scope of procedures being undertaken in neurosurgery and interventional neuroradiology, continues to increase the specialist nature of neuroanaesthesia and neurocritical care. The clinical service should provide: anaesthesia for neurosurgery intracranial, complex spinal and associated surgery anaesthesia for neuroradiology diagnostic and interventional procedures including MRI neurocritical care pre- and post-operative management of complex elective cases and the management of critically ill patients, such as those with severe head injury, intracranial haemorrhage, severe neurological disease and those who develop systemic complications secondary to their neurological condition. Levels of provision of service 1 Staffing requirements Neuroanaesthesia 1.1 The organisation of cover for neuroanaesthesia and neurocritical care requires a specific group of consultant anaesthetists (neuroanaesthetists) who may be part of, or closely affiliated with, a general department of anaesthesia and intensive care. A neuroanaesthesia service requires adequate provision of consultant programmed activities to support elective and emergency workload There should be immediate availability of a resident anaesthetist for 24 hours each day, to manage post-operative and emergency patients. In neuroscience units with a substantial caseload, this will require the provision of a resident anaesthetist dedicated to this group of patients. Out-of-hours, consultants should be available for immediate telephone advice and be able to attend the hospital within 30 minutes. 1.3 There should be sufficient programmed activities to ensure consultant cover of all neurosurgical operating lists and interventional neuroradiology sessions. Adequate arrangements for cross covering annual and study leave should be incorporated into consultants job plans. Adequate consultant cover is also required to provide general anaesthesia and sedation for diagnostic radiology sessions, including CT and MRI scans. 1.4 Consultants working in neuroanaesthesia should have sufficient regular programmed activities within this field to ensure that their specific skills and experience are maintained. A minimum of one day per week is likely to be required to fulfil this requirement. Evidence of case mix and relevant CPD to maintain skills in those areas will be required for appraisal and revalidation. The Royal College of Anaesthetists 2
4 1.5 Allocation of a single neuroanaesthetist to an operating list with long neurosurgical cases is insufficient and a team of anaesthetists should service long and complex operations. 2 Comprehensive handover arrangements must be in place to ensure continuity of care during long cases. Neurocritical care 1.6 The Royal College of Nursing suggests that the nurse:patient ratio for a patient requiring Level 3 and Level 2 care should be 1:1 and 1:2 respectively, but the actual nursing establishment to support neurocritical care services may be higher. 5 It may not be possible to leave Level 2 patients with neurological disorders alone even when they are physiologically normal, and an allowance to cover the need for closer supervision of such patients should be made when calculating the nursing establishment. 1.7 Allied health professionals are key members of the multi-professional team and a sufficient establishment is crucial to the delivery of high quality neurocritical care services and early rehabilitation input. 1.8 Consultants responsible for the care of neuroscience patients requiring critical care support should have the knowledge, skills and experience needed to treat this group of patients, irrespective of whether the services are provided in a dedicated neurocritical care unit or within the context of a general intensive care unit. There should be a designated lead consultant for neurocritical care (or director of neurocritical care) and this consultant should have programmed activities allocated to this function. 1.9 Although the management of patients requiring neurocritical care is closely shared with the neurosurgical team, a minimum of ten daytime clinical consultant programmed activities is required to cover a small neurocritical care unit (four to eight beds). In larger units it may be necessary for two consultants to be available during weekdays for all or part of the day. However, the consultant establishment for neurocritical care should be reviewed locally so that it reflects local conditions, including the skill mix of other members of the multi-professional team. It has been recommended that, in large and busy units, there may be a requirement for up to 30 consultant programmed activities per week In large units it may be appropriate to allocate consultant programmed activities to provide support to patients throughout the hospital via an outreach service There should be a resident doctor with appropriate skills and competencies immediately available for neurocritical care 24 hours each day Staffing levels must be sufficient to enable an appropriately qualified and experienced doctor and trained assistant to accompany critically ill patients during transfer between neurocritical care and operating theatres, CT and MRI scanners and angiography suites. New initiatives, such as becoming part of a Major Trauma Centre, may require additional staffing. 2 Equipment, support services and facilities Equipment 2.1 There is a high incidence of difficult intubation in neurosurgical units carrying out complex cervical spinal surgery. Specific equipment to manage the difficult airway, including the provision of sufficient numbers of fibreoptic laryngoscopes, should be available. 2.2 Equipment should be available for the safe administration of total intravenous as well as inhalational anaesthesia. 2.3 Those units conducting surgery for correction of scoliosis should have the appropriate equipment for testing spinal cord function intra-operatively. 2.4 With the increasing incidence of obesity in the population, appropriate sized mattresses and fixings for positioning those patients prone should be available. 3 Guidelines for the Provision of Anaesthetic Services 2014
5 2.5 The monitoring of patient temperature and the equipment needed to manipulate it should be available. Support services 2.6 The demand for critical care beds in neuroscience centres is high and the actual number and configuration of Level 3 and Level 2 beds should be determined locally. However, capacity should be sufficient to allow access by critically ill patients in an appropriate time scale, e.g. within four hours for those who require life-saving surgery. The Society of British Neurological Surgeons recommends the provision of ten designated Level 2 and Level 3 beds per million population for neurosurgical patients, and the Association of British Neurologists additionally estimates that between five to seven neurocritical care beds per million population are required to support the care of neurology patients A 24-hour acute pain service should be available for post-operative neurosurgical patients. 2.8 Post-operative recovery facilities, with appropriately trained staff and equipment should be available out of normal working hours to all emergency neurosurgical patients undergoing surgery and who do not require critical care Twenty-four hours a day neuroradiology support should be provided for interpretation of neuroimaging. Online review of CT scans from referring hospitals and within the neuroscience centre should be available locally, and consideration should be given to the provision of such access in the homes of consultants who provide cover to neurocritical care out of hours There should be on-site laboratory provision, or point of care testing, for arterial blood gases, serum electrolytes and activated clotting time and/or thromboelastography, to allow safe management of patients in the operating theatre during endovascular procedures and on the neurocritical care unit Rapid access to other biochemical and haematological investigations, blood transfusion and cerebrospinal fluid (CSF) microscopy should also be provided Expert neuropathological expertise should be available on request, with the ability to carry out frozen section examinations on site On-site neurophysiological support should be available seven days per week to support the management of patients in ICU requiring continuous EEG monitoring to manage their treatment Pre-admission clinics for elective neurosurgery should be available with input from the department of neuroanaesthesia For stand-alone neuroscience centres, local arrangements should be in place for specialist opinion and review of patients by other disciplines. Named consultants should be identified in core specialties to facilitate such liaison. There should be same day availability of cardiac echo investigations (including transoesophageal echo) and ultrasound scanning. To avoid the transfer of critically ill patients, this should be provided at the bedside for patients on the neurocritical care unit Each unit should have embedded a specialist nurse for organ donation to ensure that it is considered in end-of-life care, and to provide bereavement counselling and support. 11 Guidelines 2.17 Neurocritical care outcome can be improved by the delivery of management guidelines based on expert consensus. All members of the neurocritical care multi-professional team should input to the development of local protocols, which should cover all the common pathologies managed by that unit. Protocols for the management of severe head injury are particularly important and guidance for management in the acute phase should be developed in collaboration with clinicians from referring hospitals. The Royal College of Anaesthetists 4
6 2.18 Local guidelines should be agreed between clinicians in the neuroscience unit and referring hospitals for transfer and repatriation of patients, and audited as a routine Facilities Critically ill patients often require transfer to and from the operating theatre, CT and MRI scanners and angiography suites. Theatres, ICU and radiological facilities should therefore be in the closest possible proximity and preferably on the same floor. Adequate provision should be made for monitoring patients during such transfer. Local guidance should be developed for the intra-hospital transfer of critically ill neuroscience patients, based on guidance from the Intensive Care Society. 8 3 Areas of special requirement Children 3.1 Whether in a dedicated paediatric neurosurgical unit or not, every child requiring elective neurosurgery should have care delivered by an anaesthetist or anaesthetists who possess the relevant competencies as demanded by the patient s age, disease and co-morbidities. New appointees to consultant posts with a significant or whole-time interest in paediatric neuroanaesthesia should have successfully completed Advanced Level training in paediatric anaesthesia as defined in the CCT in anaesthesia (August 2010). 3.2 In a true emergency situation involving a child requiring urgent neurosurgery for a deteriorating condition admitted to an adult-only neurosurgical service, the most appropriate surgeon, anaesthetist and intensivist available would be expected to provide life-saving care including emergency resuscitation and surgery All children under the age of 16 requiring neurocritical care should be managed in a paediatric intensive care unit. 3.4 Detailed guidance for the management of children has been issued and applies equally to those requiring neurosurgical intervention (see Guidance on the provision of paediatric anaesthesia services). 4 Training and education 4.1 The specialist nature of neuroanaesthesia dictates that it is a consultant-delivered specialty. Trainees have an initial exposure to the specialty in a clinical attachment during years ST3 or ST4 of intermediate level training. Following the principle of spiral learning, a further clinical attachment occurs during higher or advanced training (ST5 ST7) with longer attachments for those wishing to follow a career in the specialty. Because of the limited time that trainees spend in the specialty, schools of anaesthesia should develop structured training programmes to cover all core topics. Successful completion is based on workplace-based assessments of the skills and knowledge required. Trainees should, therefore, also be encouraged to attend other training opportunities within the neuroscience unit, such as grand rounds, radiology and pathology case conferences and mortality and morbidity meetings. 4.2 Fellowship posts should be identified to allow additional training for those who wish to follow a career in neuroanaesthesia or neurocritical care. These should be suitable for trainees who wish to take time out of training programmes or for those who are post-cct. Such posts should provide similar or enhanced levels of teaching, training and access to study leave as regular training posts. 5 Guidelines for the Provision of Anaesthetic Services 2014
7 5 Research and audit 5.1 Departments of neuroanaesthesia and neurocritical care should be encouraged to develop research interests, even if not part of an academic department. Research collaboration with other neuroscience disciplines is good practice. Taking part in national anaesthesia and critical care projects such as the RAIN study is to be encouraged. 5.2 Audit programmes should be developed locally but should include continuous audit of transfer of brain-injured patients, neurocritical care capacity and demand, rates of unplanned admission and readmission to ICU and caseload of trainees. Collaborative audit with the other neuroscience disciplines should also be encouraged, and some M and M meetings should be joint with neurosurgeons. In general, local practice should be audited against national and expert consensus guidelines. 6 Organisation and administration 6.1 Much of neurosurgery involves acute work with a high degree of urgency. The provision of associated services must recognise this need and inappropriate delay cannot be allowed to occur due to the lack of key personnel or facilities. Laboratory services, neuroradiology and availability of operating theatre time must all be organised to cope with these demands. 6.2 Departments of neuroanaesthesia and neurocritical care, even if part of a large general department, must be provided with adequate secretarial and administrative support. Consultants with lead responsibility for neuroanaesthesia and neurocritical care should have programmed activities allocated to this function. Appropriate levels of administrative support, including data collection and analysis, should be available for neurocritical care. 6.3 Consultants in neuroanaesthesia and neurocritical care should be involved in the planning of neuroscience services at a local and regional level. 6.4 A lead consultant responsible for patient transfer should be identified both in the neuroscience unit and in referring hospitals. 7 Patient information 7.1 Each department should provide written information specific to neurosurgical procedures, including relevant risks. Information for relatives of patients requiring neurocritical care should also be available, including contact details of relevant charities and helplines. References 1 Guidance on the 2003 (new) contract and job planning for consultant anaesthetists. AAGBI, London 2005 ( default/files/jobplanning05.pdf). 2 Fatigue and the anaesthetist (expanded web version). AAGBI, London 2005 ( fatigue04.pdf). 3 Neuroscience critical care report progress in developing services (Gateway Ref: 3236). DH, London 2004 ( uk/nationalframework/documents/neuro/key%20docs/dohneurosciencecriticialcarereport.pdf). 4 Report of the working party on the management of patients with head injuries. R Coll Surg Engl, London 1999 ( ac.uk/publications/docs/report_head_injuries.html/). 5 Guidance for nurse staffing in critical care. RCN, London 2003 ( data/assets/pdf_file/0008/78560/ pdf). 6 Head injury: triage, assessment, investigations and early management of head injury in infants, children and adults (Clinical Guideline 56). Developed by the National Collaborating Centre for Acute Care (partial update of Clinical Guideline 4). NICE, London 2007 ( 7 Recommendations for transfer of patients with brain injury. AAGBI, London 2006 ( pdf). 8 Guidelines for the transport of the critically ill adult (3rd Edition). ICS, London 2011 ( The Royal College of Anaesthetists 6
8 9 Children s neurosurgical specification standards. NHS Specialised Services, May 2011 ( Children_Neurosurgical_Specification_Standards May_2011.pdf). 10 Joint statement from the Society of British Neurological Surgeons and the Royal College of Anaesthetists regarding the provision of emergency paediatric neurosurgical services. RCoA, London 2010 ( 11 Organs for transplant: a report from the Organ Donation Taskforce. DH, London 2008 ( Organs%20for%20transplants%20-%20The%20Organ%20Donor%20Task%20Force%201st%20report.pdf). 12 Immediate Post-anaesthesia Recovery Anaesth 2013;68: Claasen J et al. Recommendations on the use of EEG monitoring in critically ill patients: concensus statement from the neurointensive care section of the ESICM. Intensive Care Med 2013,39: Guidelines for the Provision of Anaesthetic Services 2014
Neurocritical Care. Does it make a difference?
 Neurocritical Care Does it make a difference? Dr Hilary Madder Neurosciences Intensive Care Unit John Radcliffe Hospital, Oxford ANZCA Neuroanaesthesia SIG July 2013 Neurocritical Care Capacity 32 neurosurgical
Neurocritical Care Does it make a difference? Dr Hilary Madder Neurosciences Intensive Care Unit John Radcliffe Hospital, Oxford ANZCA Neuroanaesthesia SIG July 2013 Neurocritical Care Capacity 32 neurosurgical
Neurocritical Care Fellowship Program Requirements
 Neurocritical Care Fellowship Program Requirements I. Introduction A. Definition The medical subspecialty of Neurocritical Care is devoted to the comprehensive, multisystem care of the critically-ill neurological
Neurocritical Care Fellowship Program Requirements I. Introduction A. Definition The medical subspecialty of Neurocritical Care is devoted to the comprehensive, multisystem care of the critically-ill neurological
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 13th March 2014 Compliance
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 13th March 2014 Compliance
E09/S/a Paediatric Neurosciences: Neurosurgery
 E09/S/a 2013/14 NHS STANDARD CONTRACT FOR PAEDIATRIC NEUROSCIENCES: NEUROSURGERY PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
E09/S/a 2013/14 NHS STANDARD CONTRACT FOR PAEDIATRIC NEUROSCIENCES: NEUROSURGERY PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England HS Foundation Trust Appendix 2 Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy
GUIDELINES FOR THE PROVISION OF. anaesthetic services. The Royal College of Anaesthetists
 GUIDELINES FOR THE PROVISION OF anaesthetic services 2013 The Royal College of Anaesthetists GUIDELINES FOR THE PROVISION OF anaesthetic services Introduction Guidelines for the Provision of Anaesthetic
GUIDELINES FOR THE PROVISION OF anaesthetic services 2013 The Royal College of Anaesthetists GUIDELINES FOR THE PROVISION OF anaesthetic services Introduction Guidelines for the Provision of Anaesthetic
TRAUMA CENTER REQUIREMENTS
 California Trauma Center Level III Criteria California Code of Regulations,, Chapter 7 - Trauma Care System with American College of Surgeons (Green Book) references; includes FAQ clarifications TRAUMA
California Trauma Center Level III Criteria California Code of Regulations,, Chapter 7 - Trauma Care System with American College of Surgeons (Green Book) references; includes FAQ clarifications TRAUMA
Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation
 Health Informatics Unit Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation April 2011 Funded by: Acknowledgements This project was funded by the Academy of
Health Informatics Unit Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation April 2011 Funded by: Acknowledgements This project was funded by the Academy of
PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification. 12 months
 E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
Equivalence Guidance for GMP Domain 1
 Equivalence Guidance for GMP Domain 1 From 1 st August 2011 the new GMC approved curriculum in Intensive Care Medicine (ICM) came into effect. As a result of this new curriculum, all equivalence applications
Equivalence Guidance for GMP Domain 1 From 1 st August 2011 the new GMC approved curriculum in Intensive Care Medicine (ICM) came into effect. As a result of this new curriculum, all equivalence applications
The Royal College of Surgeons of England
 The Royal College of Surgeons of England Provision of Trauma Care Policy Briefing This policy briefing outlines the view of the Royal College of Surgeons of England in relation to the planning and provision
The Royal College of Surgeons of England Provision of Trauma Care Policy Briefing This policy briefing outlines the view of the Royal College of Surgeons of England in relation to the planning and provision
Organisational Audit Questions - Links to recommendations, standards and evidence
 Question Quoted recommendation/ standard / evidence Source Notes Section 1 - Hospital characteristics 1. a) How many adult in-patient or overnight beds (including 23- hours stay) are currently available
Question Quoted recommendation/ standard / evidence Source Notes Section 1 - Hospital characteristics 1. a) How many adult in-patient or overnight beds (including 23- hours stay) are currently available
Wales Critical Care & Trauma Network (North)
 Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Alabama Trauma Center Designation Criteria
 2 Alabama Trauma Center Designation Criteria Office of Emergency Medical Services Master Checklist Alabama Trauma Center Designation Trauma Center Criteria: APPENDIX A Trauma Rules The following table
2 Alabama Trauma Center Designation Criteria Office of Emergency Medical Services Master Checklist Alabama Trauma Center Designation Trauma Center Criteria: APPENDIX A Trauma Rules The following table
POSITION DESCRIPTION
 POSITION DESCRIPTION Position details: Title: Department: Reports to: Location: Paediatric Anaesthetist Paediatric Anaesthesia Service Clinical Director, Paediatric Anaesthesia Starship Children s Health
POSITION DESCRIPTION Position details: Title: Department: Reports to: Location: Paediatric Anaesthetist Paediatric Anaesthesia Service Clinical Director, Paediatric Anaesthesia Starship Children s Health
Neurocritical Care Program Requirements
 Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
Seven Day Services Clinical Standards September 2017
 Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service SVTN North Bristol NHS Trust North Bristol NHS Trust Reception and Resuscitation Measures (T14-2B-1)
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service SVTN North Bristol NHS Trust North Bristol NHS Trust Reception and Resuscitation Measures (T14-2B-1)
AMERICAN COLLEGE OF SURGEONS 1999 TRAUMA FACILITIES CRITERIA (minus the Level IV criteria)
 AMERICAN COLLEGE OF SURGEONS 1999 TRAUMA FACILITIES CRITERIA (minus the Level IV criteria) Note: In the table below, (E) represents essential while (D) represents desirable criteria. INSTITUTIONAL ORGANIZATION
AMERICAN COLLEGE OF SURGEONS 1999 TRAUMA FACILITIES CRITERIA (minus the Level IV criteria) Note: In the table below, (E) represents essential while (D) represents desirable criteria. INSTITUTIONAL ORGANIZATION
POSITION STATEMENT ON THE FUTURE MODEL OF NEUROSCIENCES IN MID AND SOUTH WALES. Chief Executive
 AGENDA ITEM 5.2 23 October 2009 POSITION STATEMENT ON THE FUTURE MODEL OF NEUROSCIENCES IN MID AND SOUTH WALES Report of Chief Executive Paper prepared by Purpose of Paper Action/Decision required Link
AGENDA ITEM 5.2 23 October 2009 POSITION STATEMENT ON THE FUTURE MODEL OF NEUROSCIENCES IN MID AND SOUTH WALES Report of Chief Executive Paper prepared by Purpose of Paper Action/Decision required Link
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey
 Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
HFAP Stroke Survey. Overview of the Survey Process 8/17/2011
 HFAP Stroke Survey Surveyors Viewpoint Bernard C. McDonnell, D.O. Stroke Center Accreditation from the Surveyors Viewpoint 01.00.01 Primary stroke Center Facility Commitment. The leadership of the facility
HFAP Stroke Survey Surveyors Viewpoint Bernard C. McDonnell, D.O. Stroke Center Accreditation from the Surveyors Viewpoint 01.00.01 Primary stroke Center Facility Commitment. The leadership of the facility
St. James s Hospital, Dublin.
 Position Fellowship in Anaesthesia for Advanced Airway Management Assignment Department of Anaesthesia, St. James s Hospital. Commencement Date Monday, 09 th July, 2018. Purpose of the Post The St. James
Position Fellowship in Anaesthesia for Advanced Airway Management Assignment Department of Anaesthesia, St. James s Hospital. Commencement Date Monday, 09 th July, 2018. Purpose of the Post The St. James
Domain 5 Cardiothoracic Standards RCoA Accreditation 2017
 1 PRIORITY The Care Pathway 5.4.1.1 The process for preoperative assessment presenting for cardiac and thoracic patients (including thoracic aortic) is defined within the patient pathway. 1 A clinical
1 PRIORITY The Care Pathway 5.4.1.1 The process for preoperative assessment presenting for cardiac and thoracic patients (including thoracic aortic) is defined within the patient pathway. 1 A clinical
7 NON-ELECTIVE SURGERY IN THE NHS
 Recommendations Debate whether, in the light of changes to the pattern of junior doctors working, non-essential surgery can take place during extended hours. 7 NON-ELECTIVE SURGERY IN THE NHS Ensure that
Recommendations Debate whether, in the light of changes to the pattern of junior doctors working, non-essential surgery can take place during extended hours. 7 NON-ELECTIVE SURGERY IN THE NHS Ensure that
Neurosurgery. Themes. Referral
 06 04 Neurosurgery The following recommendations were produced by the British Society of Neurological Surgeons to highlight where resources could be released in NHS neurological services, while maintaining
06 04 Neurosurgery The following recommendations were produced by the British Society of Neurological Surgeons to highlight where resources could be released in NHS neurological services, while maintaining
MINIMUM STANDARDS FOR INTENSIVE CARE UNITS SEEKING ACCREDITATION FOR TRAINING IN INTENSIVE CARE MEDICINE
 College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Policy Date established: 1994 Date last reviewed: 2015 MINIMUM STANDARDS FOR INTENSIVE CARE UNITS SEEKING
College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Policy Date established: 1994 Date last reviewed: 2015 MINIMUM STANDARDS FOR INTENSIVE CARE UNITS SEEKING
Guidance for Advisory Appointments Committees (AAC)
 Guidance for Advisory Appointments Committees (AAC) Guidance for Regional and Deputy Regional Advisors for the Approval of Job Descriptions, Job Plans and Person Specifications 2018 Guidance for HR Departments
Guidance for Advisory Appointments Committees (AAC) Guidance for Regional and Deputy Regional Advisors for the Approval of Job Descriptions, Job Plans and Person Specifications 2018 Guidance for HR Departments
Separating emergency and elective surgical care: Recommendations for practice
 Separating emergency and elective surgical care: Recommendations for practice THE ROYAL COLLEGE OF SURGEONS OF ENGLAND September 2007 2 SEPARATING EMERGENCY AND ELECTIVE SURGICAL CARE The Royal College
Separating emergency and elective surgical care: Recommendations for practice THE ROYAL COLLEGE OF SURGEONS OF ENGLAND September 2007 2 SEPARATING EMERGENCY AND ELECTIVE SURGICAL CARE The Royal College
POLICIES AND PROCEDURES
 POLICIES AND PROCEDURES POLICY: 535.10 TITLE: EFFECTIVE: 4/13/17 REVIEW: 4/2022 SUPERCEDES: APPROVAL SIGNATURES ON FILE IN EMS OFFICE PAGE: 1 of 14 I. AUTHORITY Division 2.5, California Health and Safety
POLICIES AND PROCEDURES POLICY: 535.10 TITLE: EFFECTIVE: 4/13/17 REVIEW: 4/2022 SUPERCEDES: APPROVAL SIGNATURES ON FILE IN EMS OFFICE PAGE: 1 of 14 I. AUTHORITY Division 2.5, California Health and Safety
Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery
 CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
St. James s Hospital, Dublin.
 Position Senior House Officer in Anaesthesia Organisational Area Department of Anaesthesia, St. James s Hospital. Closing Date Sunday the 9 th July 2018 SACC Directorate. The Surgery, Anaesthesia and Critical
Position Senior House Officer in Anaesthesia Organisational Area Department of Anaesthesia, St. James s Hospital. Closing Date Sunday the 9 th July 2018 SACC Directorate. The Surgery, Anaesthesia and Critical
Consultant Anaesthetist
 www.nhsggc.org.uk Job Ref 34369D Closing Date 3rd October 2014 Interview Date 30th October 2014 SUMMARY INFORMATION Job Ref Title Specialty Special Interest Remit 34369D Consultant Anaesthetist Head And
www.nhsggc.org.uk Job Ref 34369D Closing Date 3rd October 2014 Interview Date 30th October 2014 SUMMARY INFORMATION Job Ref Title Specialty Special Interest Remit 34369D Consultant Anaesthetist Head And
Advanced Roles and Workforce Planning. Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow
 Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
SAFE STAFFING GUIDELINE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline title SAFE STAFFING GUIDELINE SCOPE 1. Safe staffing for nursing in accident and emergency departments Background 2. The National Institute for
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline title SAFE STAFFING GUIDELINE SCOPE 1. Safe staffing for nursing in accident and emergency departments Background 2. The National Institute for
Appendix 1 - Licensing and Audit Requirements for Emergency Department Services
 Appendix 1 - Licensing and Audit Requirements for Emergency Department Services Number Urgent Care Centres Emergency Department Emergency Department with Major Trauma Centre 1. Access 24/7 (This requirement
Appendix 1 - Licensing and Audit Requirements for Emergency Department Services Number Urgent Care Centres Emergency Department Emergency Department with Major Trauma Centre 1. Access 24/7 (This requirement
Trauma Center Pre-Review Questionnaire Notes Title 22
 This Pre-Review Questionnaire is designed to accompany the spread sheet appropriate for the Trauma Center being reviewed For use with review of Level III Trauma Center with American College of Surgeons'
This Pre-Review Questionnaire is designed to accompany the spread sheet appropriate for the Trauma Center being reviewed For use with review of Level III Trauma Center with American College of Surgeons'
NHS. Challenges and improvements in diagnostic services across seven days. Improving Quality
 NHS Improving Quality NHS Improving Quality working in partnership with NHS England Challenges and improvements in diagnostic services across seven days 2 Foreword Across the country, hospitals and primary
NHS Improving Quality NHS Improving Quality working in partnership with NHS England Challenges and improvements in diagnostic services across seven days 2 Foreword Across the country, hospitals and primary
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP)
 Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Summary Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Summary Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced
Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster.
 Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster. Working document The Critical Care Contingency Plan in the event of an emergency
Phases of staged response to an increased demand for Paediatric Intensive Care in the event of pandemic or other disaster. Working document The Critical Care Contingency Plan in the event of an emergency
Neurology quality indicators
 Neurology A new approach for London Neurology quality indicators For adult neurological services December 2016 Acknowledgements The London Neuroscience Clinical Network is grateful to all who have contributed
Neurology A new approach for London Neurology quality indicators For adult neurological services December 2016 Acknowledgements The London Neuroscience Clinical Network is grateful to all who have contributed
Job Planning Driving Improvement Ensuring success for consultants, the service and for improved patient care
 Job Planning Driving Improvement Ensuring success for consultants, the service and for improved patient care Dr Jeremy Cashman Associate Medical Director Delivering successful job planning The 2003 contract
Job Planning Driving Improvement Ensuring success for consultants, the service and for improved patient care Dr Jeremy Cashman Associate Medical Director Delivering successful job planning The 2003 contract
Sample Template Operational Policy
 Operational Delivery s Sample Template Operational Policy October 2014 Document MTN-OP-03-10-14 Classification: General Organisation Document Purpose Title Author Operational Delivery s Guidance Sample
Operational Delivery s Sample Template Operational Policy October 2014 Document MTN-OP-03-10-14 Classification: General Organisation Document Purpose Title Author Operational Delivery s Guidance Sample
1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure
 ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
Resuscitation Training Policy
 Resuscitation Training Policy Approved by & date HMB 12 November 2003 Date of Publication February 2003 Review date February 2005 Creator & telephone details Christopher Gabel, Senior Resuscitation Officer
Resuscitation Training Policy Approved by & date HMB 12 November 2003 Date of Publication February 2003 Review date February 2005 Creator & telephone details Christopher Gabel, Senior Resuscitation Officer
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
King s International Critical Care Fellowship Programme
 King s International Critical Care Fellowship Programme Why King s? King s College Hospital NHS Foundation Trust is one of the biggest and busiest hospital trusts in London, with a well-established national
King s International Critical Care Fellowship Programme Why King s? King s College Hospital NHS Foundation Trust is one of the biggest and busiest hospital trusts in London, with a well-established national
Barts Health Simulation and Clinical Skills Course Directory
 Barts Health Simulation and Clinical Skills Course Directory Newham University Hospital The Royal London Hospital St Bartholomews Hospital Whipps Cross University Hospital 1 Table of Contents Acute Care
Barts Health Simulation and Clinical Skills Course Directory Newham University Hospital The Royal London Hospital St Bartholomews Hospital Whipps Cross University Hospital 1 Table of Contents Acute Care
Program goals and competencies for each year of training;
 Program goals and competencies for each year of training; NS-1 Perform a neurological exam Triage of neurosurgical emergencies Neurosurgical critical care management Interpret laboratory studies Identify
Program goals and competencies for each year of training; NS-1 Perform a neurological exam Triage of neurosurgical emergencies Neurosurgical critical care management Interpret laboratory studies Identify
COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE
 COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE (2006) The CoBaTrICE Collaboration: 1 st September 2006. European Society of Intensive Care Medicine (ESICM) Avenue Joseph Wybran 40, B-1070,Brussels.
COBAFOLIO: DOCUMENTING THE EVIDENCE OF COMPETENCE (2006) The CoBaTrICE Collaboration: 1 st September 2006. European Society of Intensive Care Medicine (ESICM) Avenue Joseph Wybran 40, B-1070,Brussels.
We are looking for the following medical positions:
 We are looking for the following medical positions: United Kingdom Ipswich Location: Ipswich is a town in the east of the United Kingdom at the mouth of the Orwell River. The city has about 135,000 inhabitants.
We are looking for the following medical positions: United Kingdom Ipswich Location: Ipswich is a town in the east of the United Kingdom at the mouth of the Orwell River. The city has about 135,000 inhabitants.
Element(s) of Performance for DSPR.1
 Prepublication Issued Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Prepublication Issued Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Example Care Pathways
 Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Emergency Surgery. Standards for unscheduled surgical care. Guidance for providers, commissioners and service planners
 Emergency Surgery Standards for unscheduled surgical care Guidance for providers, commissioners and service planners February 2011 Produced by the Publications Department, The Royal College of Surgeons
Emergency Surgery Standards for unscheduled surgical care Guidance for providers, commissioners and service planners February 2011 Produced by the Publications Department, The Royal College of Surgeons
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER. Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow
 SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
Ref No 001/18. Incremental credit will be awarded in accordance with experience and qualifications.
 Post Title Consultant Oral and Maxillofacial Surgeon St. James s Hospital 15hrs / HSE Primary Care (Orthognathic) 16hrs / Our Lady s Children s Hospital Crumlin 8hrs. Ref No 001/18 Tenure Permanent This
Post Title Consultant Oral and Maxillofacial Surgeon St. James s Hospital 15hrs / HSE Primary Care (Orthognathic) 16hrs / Our Lady s Children s Hospital Crumlin 8hrs. Ref No 001/18 Tenure Permanent This
Consultation Paper. Distributed Medical Imaging in the new Royal Adelaide Hospital Central Adelaide Local Health Network
 Consultation Paper Distributed Medical Imaging in the new Royal Adelaide Hospital Central Adelaide Local Health Network Issued: April 2016 TABLE OF CONTENTS TABLE OF CONTENTS 2 1. INTRODUCTION 3 2. PURPOSE
Consultation Paper Distributed Medical Imaging in the new Royal Adelaide Hospital Central Adelaide Local Health Network Issued: April 2016 TABLE OF CONTENTS TABLE OF CONTENTS 2 1. INTRODUCTION 3 2. PURPOSE
ISOLATED HEAD INJURY. MODULE: Intensive Care Medicine / Trauma ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND:
 ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
ISOLATED HEAD INJURY MODULE: Intensive Care Medicine / Trauma TARGET: ALL ANAESTHETISTS, INTENSIVISTS & ED PHYSICIANS BACKGROUND: Head injuries are a major cause of morbidity and mortality in children
NCEPOD Recommendations that remain current
 NCEPOD Recommendations that remain current All recommendations from subsequent NCEPOD reports are considered current (Last updated 2014) 1989 The information systems, particularly clinical information
NCEPOD Recommendations that remain current All recommendations from subsequent NCEPOD reports are considered current (Last updated 2014) 1989 The information systems, particularly clinical information
Australian and New Zealand College of Anaesthetists (ANZCA)
 PS08 2016 Australian and New Zealand College of Anaesthetists (ANZCA) Statement on the Assistant for the Anaesthetist 1. PURPOSE The purpose of this document is to recognise the importance of and to promote
PS08 2016 Australian and New Zealand College of Anaesthetists (ANZCA) Statement on the Assistant for the Anaesthetist 1. PURPOSE The purpose of this document is to recognise the importance of and to promote
CCT in Anaesthetics Assessment Guidance 2017
 CCT in Anaesthetics Assessment Guidance 2017 Royal College of Anaesthetists Introduction This document describes the various assessment methods used in the anaesthetic training programme. Trainees are
CCT in Anaesthetics Assessment Guidance 2017 Royal College of Anaesthetists Introduction This document describes the various assessment methods used in the anaesthetic training programme. Trainees are
anaesthetic services Chapter 10 Paediatric anaesthesia services 2014 GUIDELINES FOR THE PROVISION OF
 Chapter 10 GUIDELINES FOR THE PROVISION OF anaesthetic services Paediatric anaesthesia Authors Dr K A Wilkinson, Norfolk and Norwich University Hospital Dr L J Brennan, Addenbrooke s Hospital, Cambridge
Chapter 10 GUIDELINES FOR THE PROVISION OF anaesthetic services Paediatric anaesthesia Authors Dr K A Wilkinson, Norfolk and Norwich University Hospital Dr L J Brennan, Addenbrooke s Hospital, Cambridge
Trauma Care Network News. West Midlands Major Trauma Clinical Lead appointed. Inside Issue 3. Issue 3
 Trauma Care Network News Issue 3 Inside Issue 3 Implementation of trauma care system Monitoring patient outcomes International Trauma Care Conference 23rd - 26th April West Midlands Major Trauma Clinical
Trauma Care Network News Issue 3 Inside Issue 3 Implementation of trauma care system Monitoring patient outcomes International Trauma Care Conference 23rd - 26th April West Midlands Major Trauma Clinical
Returning to work after a period of absence
 Introduction Doctors may be away from their normal working environment for many reasons and these periods can extend from months to years. This guidance is directed at anaesthetists returning to anaesthesia
Introduction Doctors may be away from their normal working environment for many reasons and these periods can extend from months to years. This guidance is directed at anaesthetists returning to anaesthesia
Safe staffing for nursing in A&E departments. NICE safe staffing guideline Draft for consultation, 16 January to 12 February 2015
 Safe staffing for nursing in A&E departments NICE safe staffing guideline Draft for consultation, 16 January to 12 February 2015 Safe staffing for nursing in A&E departments: NICE safe staffing guideline
Safe staffing for nursing in A&E departments NICE safe staffing guideline Draft for consultation, 16 January to 12 February 2015 Safe staffing for nursing in A&E departments: NICE safe staffing guideline
RESOURCES FOR OPTIMAL CARE OF THE INJURED PATIENT
 CALIFORNIA TRAUMA REGULATIONS (Title 22) versus ACS RESOURCES FOR OPTIMAL CARE OF THE INJURED PATIENT 2006 (Green Book) (Level I/II Trauma Centers Only) Requirement TITLE 22 ACS GREEN BOOK Trauma Medical
CALIFORNIA TRAUMA REGULATIONS (Title 22) versus ACS RESOURCES FOR OPTIMAL CARE OF THE INJURED PATIENT 2006 (Green Book) (Level I/II Trauma Centers Only) Requirement TITLE 22 ACS GREEN BOOK Trauma Medical
September 2018 April Calendar of events. Educational events to support your professional development needs
 September 2018 April 2019 Calendar of events Educational events to support your professional development needs 2 Calendar of events EVENTS CALENDAR Further information about all of our events can be found
September 2018 April 2019 Calendar of events Educational events to support your professional development needs 2 Calendar of events EVENTS CALENDAR Further information about all of our events can be found
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA
 Review PS18 (2008) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA The terms Anaesthetist, medical practitioner and practitioner
Review PS18 (2008) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA The terms Anaesthetist, medical practitioner and practitioner
TEMPORARY CONSULTANT IN INTENSIVE CARE MEDICINE (TYPE B) National Clinical Programme Integrated Care Programme Patient Flow Job Description
 TEMPORARY CONSULTANT IN INTENSIVE CARE MEDICINE (TYPE B) National Clinical Programme Integrated Care Programme Patient Flow Job Description Mater Misericordiae University Hospital 39 hours National Rehabilitation
TEMPORARY CONSULTANT IN INTENSIVE CARE MEDICINE (TYPE B) National Clinical Programme Integrated Care Programme Patient Flow Job Description Mater Misericordiae University Hospital 39 hours National Rehabilitation
Guidance for job planning
 Guidance for job planning FR/OA/03 Faculty of the Psychiatry of Old Age FACULTY REPORT Faculty Report OA/03 June 2015 2015 The Royal College of Psychiatrists The Royal College of Psychiatrists is a charity
Guidance for job planning FR/OA/03 Faculty of the Psychiatry of Old Age FACULTY REPORT Faculty Report OA/03 June 2015 2015 The Royal College of Psychiatrists The Royal College of Psychiatrists is a charity
Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency
 DEPARTMENT OF ANESTHESIA Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency 1. An anesthesiology resident, during a two month rotation should gain exposure to the scope
DEPARTMENT OF ANESTHESIA Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency 1. An anesthesiology resident, during a two month rotation should gain exposure to the scope
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation
 Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
The following policy was adopted by the San Luis Obispo County EMS Agency and will become effective March 1, 2012 at 0800 hours.
 SLO County Emergency Medical Services Agency Bulletin 2012-02 PLEASE POST New Trauma System Policies and Procedures February 9, 2012 To All SLO County EMS Providers and Training Institutions: The following
SLO County Emergency Medical Services Agency Bulletin 2012-02 PLEASE POST New Trauma System Policies and Procedures February 9, 2012 To All SLO County EMS Providers and Training Institutions: The following
Diagnostic shoulder arthroscopy
 Diagnostic shoulder arthroscopy The aim of this leaflet is to help answer some of the questions you may have about having a diagnostic shoulder arthroscopy. It explains the benefits, risks and alternatives
Diagnostic shoulder arthroscopy The aim of this leaflet is to help answer some of the questions you may have about having a diagnostic shoulder arthroscopy. It explains the benefits, risks and alternatives
Portsmouth Hospitals NHS Trust Individual Placement (Job) Descriptions for Foundation Year 1
 Portsmouth Hospitals NHS Trust Individual Placement (Job) Descriptions for Foundation Year 1 Placement The department Where the is for the in this F1 Acute Placement Acute Medicine Unit/Surgical Assessment
Portsmouth Hospitals NHS Trust Individual Placement (Job) Descriptions for Foundation Year 1 Placement The department Where the is for the in this F1 Acute Placement Acute Medicine Unit/Surgical Assessment
Part II. The CCT in. Intensive Care Medicine. Assessment System. The Faculty of. Intensive Care Medicine
 Part II The CCT in Intensive Care Medicine Assessment System The Faculty of Intensive Care Medicine Contents 1. Principles of Assessment... 3 1.1 Training Stage Records... 3 1.2 How many workplace-based
Part II The CCT in Intensive Care Medicine Assessment System The Faculty of Intensive Care Medicine Contents 1. Principles of Assessment... 3 1.1 Training Stage Records... 3 1.2 How many workplace-based
Modified Early Warning Score Policy.
 Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Moving to 7 Day Services. Kerry Gant, Head of Finance Change Team/Debbie Freake, Executive Director of Strategy
 Report to Trust Board of Directors Date of Meeting: 24 March 2015 Enclosure Number: 12 Title of Report: Author: Executive Lead: Responsible Sub- Committee (if appropriate): Executive Summary: Moving to
Report to Trust Board of Directors Date of Meeting: 24 March 2015 Enclosure Number: 12 Title of Report: Author: Executive Lead: Responsible Sub- Committee (if appropriate): Executive Summary: Moving to
#NeuroDis
 Each and Every Need A review of the quality of care provided to patients aged 0-25 years old with chronic neurodisability, using the cerebral palsies as examples of chronic neurodisabling conditions Recommendations
Each and Every Need A review of the quality of care provided to patients aged 0-25 years old with chronic neurodisability, using the cerebral palsies as examples of chronic neurodisabling conditions Recommendations
Anaesthesia Registrars
 Studley Road, Heidelberg, 3084 Anaesthesia Registrars - 2017 Name of Unit / Specialty: Head of Unit: CSU / Department: Anaesthesia A/Prof Larry McNicol Anaesthesia Contact person: Dr Shiva Malekzadeh,
Studley Road, Heidelberg, 3084 Anaesthesia Registrars - 2017 Name of Unit / Specialty: Head of Unit: CSU / Department: Anaesthesia A/Prof Larry McNicol Anaesthesia Contact person: Dr Shiva Malekzadeh,
GUIDELINE FOR THE STRUCTURED ASSESSMENT OF TRAINEE COMPETENCE PRIOR TO SUPERVISION BEYOND LEVEL ONE
 GUIDELINE FOR THE STRUCTURED ASSESSMENT OF TRAINEE COMPETENCE PRIOR TO SUPERVISION BEYOND LEVEL ONE August 2007 The following guideline was developed by a Working Party convened by the ANZCA Education
GUIDELINE FOR THE STRUCTURED ASSESSMENT OF TRAINEE COMPETENCE PRIOR TO SUPERVISION BEYOND LEVEL ONE August 2007 The following guideline was developed by a Working Party convened by the ANZCA Education
St Peter s Hospital. Guildford Road Chertsey, Surrey KT16 0PZ Anaesthetic Department Direct Line: College Tutor: Dr Robert Menzies
 St Peter s Hospital Guildford Road Chertsey, Surrey KT16 0PZ Anaesthetic Department Direct Line: 01932 722153 College Tutor: Dr Robert Menzies http://www.multimap.com/maps/?qs=&countrycode=gb&maptype=&overview=#map
St Peter s Hospital Guildford Road Chertsey, Surrey KT16 0PZ Anaesthetic Department Direct Line: 01932 722153 College Tutor: Dr Robert Menzies http://www.multimap.com/maps/?qs=&countrycode=gb&maptype=&overview=#map
Clinical Care Pathway for BRAIN TUMOURS in Childhood.
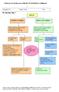 - 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
- 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
Course: Acute Trauma Care Course Number SUR 1905 (1615)
 Course: Acute Trauma Care Course Number SUR 1905 (1615) Department: Faculty Coordinator: Surgery Dr. Joseph P. Minei Hospital: Periods Offered: Length: Parkland Health & Hospital System All year 4 weeks
Course: Acute Trauma Care Course Number SUR 1905 (1615) Department: Faculty Coordinator: Surgery Dr. Joseph P. Minei Hospital: Periods Offered: Length: Parkland Health & Hospital System All year 4 weeks
Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2
 Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2 Placement The type of work to expect and learning opportunities Where the is based Clinical Supervisor(s)
Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2 Placement The type of work to expect and learning opportunities Where the is based Clinical Supervisor(s)
Working for NHS Dumfries and Galloway Specialty Doctor in Anaesthetics Ref: Salary: 38,685-72,140
 Working for NHS Dumfries and Galloway Specialty Doctor in Anaesthetics Ref: 285.18 Salary: 38,685-72,140 Follow us on Twitter: @dgmedrecruit Find us on Facebook: https://www.facebook.com/nhsdg/ Visit our
Working for NHS Dumfries and Galloway Specialty Doctor in Anaesthetics Ref: 285.18 Salary: 38,685-72,140 Follow us on Twitter: @dgmedrecruit Find us on Facebook: https://www.facebook.com/nhsdg/ Visit our
Model of Care for Paediatric Critical Care
 Table of Contents 1 FOREWORD... 5 2 EXECUTIVE SUMMARY... 7 2.1 Introduction... 7 2.2 National Clinical Programme for Critical Care... 7 2.3 Governance of Paediatric Critical Care... 8 2.4 Capacity Planning...
Table of Contents 1 FOREWORD... 5 2 EXECUTIVE SUMMARY... 7 2.1 Introduction... 7 2.2 National Clinical Programme for Critical Care... 7 2.3 Governance of Paediatric Critical Care... 8 2.4 Capacity Planning...
Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50
 Acutely ill adults in hospital: recognising and responding to deterioration Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50 NICE 2018. All rights reserved. Subject to Notice of rights
Acutely ill adults in hospital: recognising and responding to deterioration Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50 NICE 2018. All rights reserved. Subject to Notice of rights
The Anaesthesia Team
 The Anaesthesia Team Revised Edition 2005 2 Published by The Association of Anaesthetists of Great Britain and Ireland, 21 Portland Place, London W1B 1PY Telephone: 020 7631 1650, Fax: 020 7631 4352 E-mail:
The Anaesthesia Team Revised Edition 2005 2 Published by The Association of Anaesthetists of Great Britain and Ireland, 21 Portland Place, London W1B 1PY Telephone: 020 7631 1650, Fax: 020 7631 4352 E-mail:
Chapter 5 Guidelines for the Provision of Anaesthesia Services (GPAS) Guidelines for the Provision of Emergency Anaesthesia 2017
 Guidelines for the Provision of Anaesthesia Services (GPAS) Guidelines for the Provision of Emergency Anaesthesia 2017 NICE has accredited the process used by the Royal College of Anaesthetists to produce
Guidelines for the Provision of Anaesthesia Services (GPAS) Guidelines for the Provision of Emergency Anaesthesia 2017 NICE has accredited the process used by the Royal College of Anaesthetists to produce
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
UNIVERSITY HOSPITALS OF MORECAMBE BAY NHS FOUNDATION TRUST TRUST BOARD
 UNIVERSITY HOSPITALS OF MORECAMBE BAY NHS FOUNDATION TRUST TRUST BOARD Date of meeting: 25 July 2012 Title / Subject: Vascular Services at UHMBFT; the Impact of Centralising Inpatient and Emergency Vascular
UNIVERSITY HOSPITALS OF MORECAMBE BAY NHS FOUNDATION TRUST TRUST BOARD Date of meeting: 25 July 2012 Title / Subject: Vascular Services at UHMBFT; the Impact of Centralising Inpatient and Emergency Vascular
Central Adelaide Local Health Network Clinical Directorate Structures
 Central Adelaide Local Health Network Clinical Directorate Structures Consultation Paper February 2014 Version 2 Document Information and Revision History 1. Version 2. Date 3. Comment 1.0 12 February
Central Adelaide Local Health Network Clinical Directorate Structures Consultation Paper February 2014 Version 2 Document Information and Revision History 1. Version 2. Date 3. Comment 1.0 12 February
PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification
 E07/S/c 2013/14 NHS STANDARD CONTRACT PAEDIATRIC LONG TERM VENTILATION PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner Lead Provider Lead Period
E07/S/c 2013/14 NHS STANDARD CONTRACT PAEDIATRIC LONG TERM VENTILATION PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner Lead Provider Lead Period
Acutely ill patients in hospital
 Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Access to Public Information Response
 Access to Public Information Response December 24 th 2016 REQUEST UNDER THE CODE OF PRACTICE FOR ACCESS TO PUBLIC INFORMATION Request sent on December 24 th 2016: I am making a request under the Code of
Access to Public Information Response December 24 th 2016 REQUEST UNDER THE CODE OF PRACTICE FOR ACCESS TO PUBLIC INFORMATION Request sent on December 24 th 2016: I am making a request under the Code of
Delivering surgical services: options for maximising resources
 Delivering surgical services: options for maximising resources THE ROYAL COLLEGE OF SURGEONS OF ENGLAND March 2007 2 OPTIONS FOR MAXIMISING RESOURCES The Royal College of Surgeons of England Introduction
Delivering surgical services: options for maximising resources THE ROYAL COLLEGE OF SURGEONS OF ENGLAND March 2007 2 OPTIONS FOR MAXIMISING RESOURCES The Royal College of Surgeons of England Introduction
I: Neurological/ Neurosurgical
 I: Neurological/ Neurosurgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 81 Competency: I-1 Neurological Nursing I-1-1 I-1-2 I-1-3 I-1-4 Demonstrate knowledge
I: Neurological/ Neurosurgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 81 Competency: I-1 Neurological Nursing I-1-1 I-1-2 I-1-3 I-1-4 Demonstrate knowledge
