Activation of the Rapid Response Team
|
|
|
- Kristian King
- 5 years ago
- Views:
Transcription
1 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures Manual Number: II-7 Date Approved Next Review (3 years from Effective Date) October 2017 Purpose Policy Statement To provide early intervention to patients outside of the ICU to help prevent an adverse outcome. The Rapid Response Team is a group of specially trained clinicians capable of providing critical care expertise to patients. Team members include a Critical Care nurse, respiratory therapist, nurse practitioner/clinical associate/intensivist. When called to respond, the Rapid Response Team is authorized to provide any appropriate patient care. Rapid Response Teams respond to provide care for adults (16 years or older) inpatients on units identified below (see Applicability). NOTE: For medical emergency assistance for individuals who are not inpatients, refer to Edmonton Acute Policy #II-90, Medical Emergency Response Procedure. If the individuals is pulseless, not breathing, or has aganol breathing, call a Code Blue. Do not call the Rapid Response Team. Applicability This policy and procedure applies to the following units at the Grey Nuns and Misericordia sites. Because of operational differences between the Grey Nuns Community Hospital and the Misericordia Community Hospital, program areas to which the Rapid Response Team will respond varies as outlined below. At the Grey Nuns, the Rapid Response Team responds to all units excluding the Level 2 Operating Room/PARR and ICN. At the Misericordia, the Rapid Response Team responds to the following areas: Medicine Orthopedics General Surgery Geriatrics Alternative Level of Care Medical Day ward Obstetrics Psychiatry Emergency Department - inpatients Diagnostic Imaging - inpatients Responsibility The Rapid Response Team, under the auspices of the responsible Intensive Care physician, will assess, stabilize and initiate treatment. Refer to Appendix for detailed staff responsibilities and accountabilities. Principles The principle of the Rapid Response Team is the provision of optimal patient care. Accordingly, any member of the health care team may activate the Rapid Response Team without risk of negative consequences. All applicable ICU policies apply to the Rapid Response Team.
2 II-7 Page 2 of 10 The Rapid Response Team is not intended to be a substitute for the appropriate provision of usual patient care. Procedure Indications for Rapid Response Team activation: Acute change in heart rate to less than 40 or greater than 140 per minute Acute change in systolic blood pressure to less than 90 mmhg Acute change in respiratory rate to less than 8 or greater than 36 breaths per minute Acute change in oxygen saturation to less than 90% despite oxygen at 10 lpm Upper airway compromise audible stridor Acute deterioration in patient level of consciousness Staff member is worried about the patient (eg. unexpected change in status) Related Documents Revisions March 12, Nursing staff member or respiratory therapist identifies a Rapid Response Team Trigger. Notifies unit manager/designate. 1.1 Staff member returns to patient and remains there until to communicate with and assist the Rapid Response Team. 2. Unit manager/designate calls the attending physician stat. If the attending physician does not respond within five minutes, the unit manager/designate calls 66# to activate the Rapid Response Team. 2.1 Switchboard activates Rapid Response pagers (and Respiratory pagers at the MCH), and announces Rapid Response Team to (location) on the overhead system. 3. The unit manager/designate notifies the attending physician, resident/nurse practitioner on call, and any other required healthcare provider. 4. The Rapid Response Team assesses, initiates treatment, attempts to stabilize and establishes a plan of care for the patient. 4.1 ICU care not medically appropriate; patient will remain on ward, 4.2 Patient condition stabilized and will remain on ward, or 4.3 Patient requires urgent transfer to ICU* If an immediate transfer to Critical Care is not possible, the Rapid Response Team nurse or delegate will notify the charge nurse in the Emergency Department and plan to transfer the patient to the Emergency Department. 5. Debriefing occurs with the patient s care provider team. Activation of the Rapid Response Team Process Flowchart - attached Staff Responsibilities and Accountabilities - attached
3 II-7 Page 3 of 10 The Activation of the Rapid Response Team Process is outlined in the following flowchart
4 II-7 Page 4 of 10 APPENDIX STAFF RESPONSIBILITIES AND ACCOUNTABILITIES This appendix outlines the responsibilities of unit nursing staff, respiratory therapists, nurse practitioners and physicians who request the Rapid Response Team. Unit nursing staff, respiratory therapists, nurse practitioners and physicians who request the Rapid Response Team are encouraged to participate by assisting the Rapid Response Team, which consists of a nurse, respiratory therapist, nurse practitioner/clinical associate/intensivist. UNIT NURSING STAFF ARE RESPONSIBLE FOR: 1. Recognizing the physiological triggers that warrant a Rapid Response Team intervention 2. Calling 66# to activate the Rapid Response Team 3. Contacting the patient s attending physician five minutes prior to the call for Rapid Response Team. 4. Uses the SBAR (situation, background, assessment, recommendations) form of communication when relaying information to care providers. 5. Explaining the Rapid Response Team role to patients and their families. 6. Ensuring the patient s room is equipped with suction, oxygen and resuscitation basket. 7. Having chart and medication administration record (MAR) available for the Rapid Response Team. 8. Providing Rapid Response Team with the patient s admission diagnosis. 9. Providing the Rapid Response Team with a brief overview of the patient s current condition including vital signs; intake/output; neurological vital signs, current lab work (eg. ABG s haemoglobin, platelet count WBC, potassium and magnesium values) and any recent changes to the patient s condition. 10. Reporting any medications that are infusing. 11. Assisting the Rapid Response Team in the care of the patient by: assembling required IV lines and other supplies - eg. chest tubes, cut down tray, etc. administering required blood products assisting with diagnostic procedures, eg. chest X-ray, E.C.G., etc. contacting other services as directed assisting with and/or documenting care interventions on the patient record as required providing care, monitoring and following up as directed by the Rapid Response Team 12. Activating a Code Blue or activating the emergency call bell as directed by the Rapid Response Team, in the event the patient has a cardiac arrest.
5 II-7 Page 5 of Photocopying and completing all required documents for the patient s chart. 14. Attending the debriefing session with the Rapid Response Team post call. 15. Completing and submitting the Rapid Response Team Evaluation form to the Rapid Response Team Nurse Practitioner. RESPIRATORY THERAPISTS ARE RESPONSIBLE FOR: 1. Recognizing the physiologic triggers that warrant a Rapid Response Team intervention. 2. Calling 66# to activate the Rapid Response Team. 3. Uses the SBAR (situation, background, assessment, recommendations) form of communication when relaying information to care providers. 4. Explaining the Rapid Response Team role to patients and their families. 5. Ensuring the room is equipped with suction, oxygen, and resuscitation basket. 6. At the Misericordia Community Hospital, the respiratory therapist that initiates the Rapid Response Team intervention assumes the role of the Rapid Response Team Respiratory Therapist (see the Rapid Response Team Respiratory Therapists responsibilities). PHYSICIANS/NURSE PRACTITIONERS ARE RESPONSIBLE FOR: 1. Recognizing the physiological triggers that warrant a Rapid Response Team intervention. 2. Calling 66# to activate the Rapid Response Team. 3. Providing Rapid Response Team with the patient s admission diagnosis. 4. Providing the Rapid Response Team with a synopsis of the patient s admission and a summary of the patient s current condition and the treatments already initiated. 5. Reporting any medications that are infusing. 6. Participating with the Rapid Response Team in the management of the patient. 7. Updating the family members of the patient s status. 8. Attending the debriefing session with the Rapid Response Team post call as necessary.
6 II-7 Page 6 of 10 RAPID RESPONSE TEAM MEMBERS: All Rapid Response Team members are responsible for: carrying the Rapid Response Team pager and handing it off at shift change to the oncoming Rapid Response Team designate responding to Rapid Response Team pages within 15 minutes using the SBAR form of communication when relaying information to other health care providers Rapid Response Team assignments are determined in advance of the start of shift. A. ICU Nursing Responder staff are responsible for: 1. Collaborating with the physician/nurse practitioner to take all necessary equipment to the unit and returning equipment to the appropriate area after each call. 2. Performing a head to toe assessment to determine severity of situation. 3. Following predetermined protocols for initial diagnostic and therapeutic interventions required and assisting or performing those interventions related to the care and treatment of the patient. 4. Carrying out interventions as ordered if the physician/nurse practitioner is unable to stay with the patient. The physician/nurse practitioner must reassess the patient after the interventions are completed to determine patient outcome and must be available to the ICU nurse by phone/pager for further instructions or to discuss issues that may arise. 5. Communicating with members of the Rapid Response Team, unit staff and physicians. 6. If the patient remains on the activating care unit, ICU Nursing Responder staff are responsible for: ensuring that any medications specific to RN with SCC do not require monitoring post administration. If they require monitoring, ensure this is properly and adequately in place prior to leaving the patient transferring care to the unit staff and leaving the unit once treatment has been initiated and the patient has stabilized returning to the unit to reassess the patient, if required. This is to be communicated to the unit staff assisting in education and supporting unit staff in regards to patient follow up care or treatment 7. If the patient requires transfer to ICU, ICU Nursing Responder staff are responsible for: remaining with the patient until transfer to ICU/CCU is facilitated
7 II-7 Page 7 of 10 informing the ICU/CCU charge nurse of patient s condition prior to transfer so that transfer can be arranged. If the ICU/CCU cannot accommodate the patient, the Rapid Response Team nurse, Patient Services Manager/delegate and ICU/CCU charge nurse will discuss a course of action. In the event that the patient requires transfer to the Emergency Department, the Rapid Response Team nurse will coordinate the transfer with the Emergency Department charge nurse or designate. ensuring that the following documentation is complete: The Rapid Response Team nurse will utilize the Rapid Response Team Documentation Form to document initial assessment, medications and interventions The original Rapid Response Team Documentation Form will be a permanent record on the patient s chart. A second copy of this form will need to be made by the Rapid Response Team nurse at the end of the Rapid Response Team call. This second copy will be placed in the ICU/CCU Code Blue Binder in the appropriate section (GNH) or the ICU Rapid Response Team Binder (MCH). If the patient is to be admitted to the ICU/CCU and there is a delay in transfer, documentation is to be started on the Adult Intensive Care 24 Hour Flow Sheet (GNH)/Critical Care 24 Hour Flow Record (MCH). subsequent interventions should be documented on the Patient Care (GNCH)/Nursing Notes (MCH) form. This is a permanent part of the patient s chart. initial assessment should be documented on the Adult Intensive Care 24 Hour Flow Sheet (GNCH)/Critical Care 24 hour flow record (MCH). any changes of the patient s current condition should be documented on the Assessment Sheet or Patient Care (GNCH)/Nursing Notes (MCH) all medications administered by the Rapid Response Team should be documented on the patient s Medication Administration Record (MAR). 8. Completing at the end of each Rapid Response Team call the following: debriefing with unit nursing staff to discuss the Rapid Response Team call providing the unit with an Rapid Response Team Evaluation survey to complete and forwarding to the ICU Nurse Practitioner completing a Rapid Response Team Issues Form if concerns arise while on a Rapid Response Team call or if there are comments/suggestions about the Rapid Response Team process and forwarding to the Rapid Response Nurse Practitioner. providing a copy of the Rapid Response Team documentation tool for the permanent patient record and another copy to the Rapid Response Team. maintaining the following equipment and supplies: restocking supplies after each Rapid Response Team call plugging in and ensuring cell phone is charged plugging in the monitor and ensuring blood pressure cuff and spool printer with paper are in the monitor ensuring that the back up Rapid Response Team bag/cart has the disposable lock intact. The back up bag is to be checked on the first of every month and signed off in the Rapid Response Team binder. checking the clipboard for the following documents: Data Collection Sheet/ Rapid Response Team Documentation Form Adult Intensive Care 24 hour Flow Sheet (GNCH)/Critical Care 24 Hour
8 II-7 Page 8 of 10 Flow Record (MCH) Patient Care (GNCH)/Nursing Notes (MCH)supplementary charting form Rapid Response Team RN Satisfaction Survey ensuring that Rapid Response Team chart bundles are supplied at the main desk of the ICU/CCU The night shift Rapid Response Team RN is to check Rapid Response Team equipment with checklist at start of shift to ensure all contents are present and within expiry dates. The RN is to sign off in the binder once the check has been completed and all supplies are in order. The Rapid Response Team nurse is encouraged to participate in ICU consults when operationally feasible. The attending physician, ICU nurse practitioner/clinical associate will work with the Rapid Response Team ICU nurse when on consult The consult is similar to an Rapid Response Team call and observations are recorded in the Patient Care Record but the Rapid Response Team documents are not initiated Document all medications on the MAR The Rapid Response Team nurse may function as the second Code nurse On a day shift without an RN assigned to Rapid Response Team, the charge nurse, unit supervisor or CNE will assume the Rapid Response Team nurse role In the event of simultaneous Rapid Response Team calls, the charge nurse or delegate will go on the call B. Rapid Response Team Nurse Practitioners / Clinical Associates are responsible for: 1. Responding to Rapid Response Team calls while on duty. 2. Ensuring that nursing unit staff/charge RN have contacted the attending physician. 3. Assessing the patient, ordering appropriate diagnostic tests, and initiating appropriate interventions as indicated, including procedures such as central line insertion, chest tube insertion, etc.. 4. Responding to pages from RNs, RTs at patient s bedside for further diagnostic interventions, treatments and medications as required. 5. Communicating to the intensivist the results of assessment and interventions as well as discussing the proposed management plan. 6. Reassessing the patient, as required, for response to therapy. 7. Discussing with patients/families code status or end of life issues, when appropriate. NOTE: Nurse Practitioners cannot write DNR orders. 8. Collecting data forms related to each Rapid Response Team call.
9 II-7 Page 9 of 10 C. Rapid Response Team Intensivists are responsible for 1. Responding to pages from nurse practitioners, clinical associates, nurses, respiratory therapists and other team members in relation to provision of care for patients assessed by the Rapid Response Team. 2. Leading in directing the plan of care in terms of assessment, diagnostics, required interventions and patient disposition, including philosophy of care. 3. Discussing patient outcome or transfer of care with the attending physician. D. Rapid Response Team Respiratory Therapists are responsible for: 1. Performing patient assessment, diagnostic and therapeutic measures related to respiratory care. 2. Communicating the results as appropriate to the other members of the Rapid Response Team. 3. Providing ongoing assessment and appropriate therapeutic interventions to improve the pulmonary status of the patient (i.e. secretion management, titration of O 2 ). 4. Providing blood gas sample procurement, analysis and interpretation, when clinically indicated and appropriate. 5. Providing bedside spirometry testing. 6. Providing care and management for patients with tracheostomies and nasopharyngeal tubes. 7. Providing ventilation assessment and management, including intubation/manual ventilation and non-invasive ventilation. 8. Transport of patients with unstable airways/critically ill patients within the hospital. 9. Providing clinical assessment and administration of inhaled therapeutic gases and medications. 10. Providing resuscitation and provision of life support measures. 11. Inserting arterial lines, if required. 12. Completing written documentation of all therapies and interventions and patient response.
10 II-7 Page 10 of Communicating patient status as required to other team members, providing expertise and assistance to unit specific staff for the provision of safe and appropriate care for the patient. 14. Ensure that all respiratory supplies from the Rapid Response Cart have been replaced. 15. Complete weekly Rapid Response Cart checks to ensure that; respiratory medications are not expired, battery on portable suction is charged, all supplies are stocked and checked according to supply list. 16. Ensuring that the patient is included in Respiratory Therapy change of shift report.
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue. The Development and Implementation of a Rapid Response Program at a Regional Facility
 Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Indications for Calling A Code Blue or Pediatric Medical Emergency
 Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
Document #: WR
 Rapid Response Team (RRT) Policy Northwest Network Effective Date: 2/8/2018 Version #: 2 Document #: WR.387.149 Patient Care Next Review: 2/8/2021 Page #: 1 of 7 SCOPE: All PeaceHealth St. Joseph Center
Rapid Response Team (RRT) Policy Northwest Network Effective Date: 2/8/2018 Version #: 2 Document #: WR.387.149 Patient Care Next Review: 2/8/2021 Page #: 1 of 7 SCOPE: All PeaceHealth St. Joseph Center
North York General Hospital Policy Manual
 ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
St. Vincent s Health System Page 1 of 8. Nursing Administration HOSPITAL SHARED POLICY?
 St. Vincent s Health System Page 1 of 8 TITLE: Rapid Response Team FACILITY: St. Vincent s East FUNCTION: ORIGINATING DEPT: Nursing Administration HOSPITAL SHARED POLICY? EFFECTIVE DATE: _X_ Yes No DOCUMENT
St. Vincent s Health System Page 1 of 8 TITLE: Rapid Response Team FACILITY: St. Vincent s East FUNCTION: ORIGINATING DEPT: Nursing Administration HOSPITAL SHARED POLICY? EFFECTIVE DATE: _X_ Yes No DOCUMENT
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
A AIRWAY Open the Airway B BREATHING Deliver two (2) Breaths. Code Blue Policy. Indications for Calling A Code Blue
 Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
North York General Hospital Policy Manual
 ORIGINATOR: Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: May, 2002 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012 Page
ORIGINATOR: Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: May, 2002 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012 Page
ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221. I. Title Trauma team Activation Protocol/Roles & Responsibilities of the Trauma Team
 Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221 Subject: Trauma Team Activation Protocol/Roles & Responsibilities of the Trauma Team Trauma Coordinator UTMB respects the diverse culture
Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221 Subject: Trauma Team Activation Protocol/Roles & Responsibilities of the Trauma Team Trauma Coordinator UTMB respects the diverse culture
Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients
 UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
1. Receives report from EMS and/or outlying facility. 5. Adheres to safety and universal precaution guidelines.
 Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Grey Nuns Community Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency Acute Care
 Grey Nuns Community Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency EMERGENCY RESPONSE CODE BLUE ALGORITHM First Person On-Scene If the First Person On-Scene is able to proceed
Grey Nuns Community Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency EMERGENCY RESPONSE CODE BLUE ALGORITHM First Person On-Scene If the First Person On-Scene is able to proceed
Recognising a Deteriorating Patient. Study guide
 Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT
 CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
CRITICAL CARE OUTREACH TEAM AND THE DETERIORATING PATIENT Outreach Objectives To avert or ensure more timely admission to DCCQ To ensure that patients discharged from Critical Care continue to progress
Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Ruchika D. Husa, MD, MS
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
North York General Hospital Policy Manual
 ORIGINTATOR: Chair Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29,
ORIGINTATOR: Chair Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29,
Prone Ventilation of the Critically Ill Patient
 Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Institutional Handbook of Operating Procedures Policy
 Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Acutely ill patients in hospital
 Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Title: ED Management of Trauma Patient Protocol
 Title: ED Management of Trauma Patient Protocol Document Category: Clinical Document Type: Protocol Department/Committee Owner: Emergency Department Original Date: August 2009 Approver(s) last review:
Title: ED Management of Trauma Patient Protocol Document Category: Clinical Document Type: Protocol Department/Committee Owner: Emergency Department Original Date: August 2009 Approver(s) last review:
Teaching Methods. Responsibilities
 Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Assessment and Reassessment of Patients
 Approved by: Assessment and Reassessment of Patients Senior Director, Operations, Emergency, Medicine, Critical Care & Respiratory - GNCH Senior Director, Operations, Emergency, Medicine, Critical Care
Approved by: Assessment and Reassessment of Patients Senior Director, Operations, Emergency, Medicine, Critical Care & Respiratory - GNCH Senior Director, Operations, Emergency, Medicine, Critical Care
1. CRITICAL CARE. Preamble. Adult and Pediatric Critical Care
 1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
Family/Caregiver Education Checklist Return Demonstration of Knowledge FIRST 24 HOURS
 of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN)
 ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN) NAME: EMPLOYMENT/TRANSFER DATE: BLS RENEWAL DATE: ALLIANCE ORIENTATION DATE: HOSPITAL ORIENTATION DATE: NURSING ORIENTATION
ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN) NAME: EMPLOYMENT/TRANSFER DATE: BLS RENEWAL DATE: ALLIANCE ORIENTATION DATE: HOSPITAL ORIENTATION DATE: NURSING ORIENTATION
Respiratory Nursing 2015
 QRC: 2208 Price One Day : $363 inc. GST Two Days: $490 inc. GST Date 25-26 May 2015 Venue Hotel IBIS - Therry Street 15-21 Therry Street, Melbourne, VI, 3000 CPD Hours 12 Hours 0 Mins Respiratory Nursing
QRC: 2208 Price One Day : $363 inc. GST Two Days: $490 inc. GST Date 25-26 May 2015 Venue Hotel IBIS - Therry Street 15-21 Therry Street, Melbourne, VI, 3000 CPD Hours 12 Hours 0 Mins Respiratory Nursing
Saving Lives: EWS & CODE SEPSIS. Kim McDonough RN and Margaret Currie-Coyoy MBA Last Revision: August 2013
 Saving Lives: EWS & CODE SEPSIS Kim McDonough RN and Margaret Currie-Coyoy MBA Last Revision: August 2013 Course Objectives At the conclusion of this training, you will be able to Explain the importance
Saving Lives: EWS & CODE SEPSIS Kim McDonough RN and Margaret Currie-Coyoy MBA Last Revision: August 2013 Course Objectives At the conclusion of this training, you will be able to Explain the importance
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Modified Early Warning Score Policy.
 Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY
 POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
Initiating a Rapid Response Team
 Initiating a Rapid Response Team Trials and Tribulations! Washington County Hospital Facility Location Size Hagerstown, MD 320 bed Programs/Services History Emergency Services, Critical Care, Med/Surg,
Initiating a Rapid Response Team Trials and Tribulations! Washington County Hospital Facility Location Size Hagerstown, MD 320 bed Programs/Services History Emergency Services, Critical Care, Med/Surg,
Department of Critical Care Restricted Registration Proposal for Call Coverage by Residents in TOH Intensive Care Units
 Department of Critical Care Restricted Registration Proposal for Call Coverage by Residents in TOH Intensive Care Units Background: In 2004, the CPSO adopted a model for a pilot project to institute limited
Department of Critical Care Restricted Registration Proposal for Call Coverage by Residents in TOH Intensive Care Units Background: In 2004, the CPSO adopted a model for a pilot project to institute limited
CLINICAL SKILLS ASSESSMENT (CSA)
 CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart
 CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: Early Warning Score Policy Version: 6 (May 2010) Amended version Reference Number: Supersedes Originator or modifier Approval Supersedes: EWS Policy v5 2009 August 2009
DOCUMENT CONTROL PAGE Title Title: Early Warning Score Policy Version: 6 (May 2010) Amended version Reference Number: Supersedes Originator or modifier Approval Supersedes: EWS Policy v5 2009 August 2009
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC
 Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
Simulation Design Template
 Simulation Design Template Date: May 7/8, 2008 File Name: Discipline: RN, Charge nurse, medical radiology, pharmacy tech, social work, medicine (whatever is available at the institution) Student Level:
Simulation Design Template Date: May 7/8, 2008 File Name: Discipline: RN, Charge nurse, medical radiology, pharmacy tech, social work, medicine (whatever is available at the institution) Student Level:
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS
 HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
HEALTH CARE PROFESSIONAL (HCP) ADMISSIONS Information Booklet Contents Page No Content 1 Index 2 Introduction What is a HCP Admission? 3 Booking Transport Who is authorised to book HCP Admissions? Who
Job Description. Job Title: (Respiratory Specialist)
 Job Title: (Respiratory Specialist) Reports to: Annette Moser Responsibility Level: Staff Direct Supervision: Respiratory Manager Job Location: UI Health Department: Respiratory Care Services Job Category:
Job Title: (Respiratory Specialist) Reports to: Annette Moser Responsibility Level: Staff Direct Supervision: Respiratory Manager Job Location: UI Health Department: Respiratory Care Services Job Category:
DEPARTMENT OF CRITICAL CARE MEDICINE RESIDENT ROTATION HANDOUT
 - 1 - Faculty of Medicine Critical Care Medicine DEPARTMENT OF CRITICAL CARE MEDICINE RESIDENT ROTATION HANDOUT INDEX: General Principles.. 2 Prerequisites 2 Members of the Healthcare Team.... 3 Daily
- 1 - Faculty of Medicine Critical Care Medicine DEPARTMENT OF CRITICAL CARE MEDICINE RESIDENT ROTATION HANDOUT INDEX: General Principles.. 2 Prerequisites 2 Members of the Healthcare Team.... 3 Daily
Z: Perioperative Nursing Specialty
 Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Condition O: Obstetrical Crisis
 Maternal Mortality Marie R. Baldisseri, MD, FCCM Associate Professor of Critical Care Medicine University of Pittsburgh School of Medicine Since 1975, overall mortality has decreased by 50% but has not
Maternal Mortality Marie R. Baldisseri, MD, FCCM Associate Professor of Critical Care Medicine University of Pittsburgh School of Medicine Since 1975, overall mortality has decreased by 50% but has not
HOW TO DO POST-HOC RESPONSE REVIEWS
 HOW TO DO POST-HOC RESPONSE REVIEWS Ken Hillman 6 th International Symposium on Rapid Response Systems and Medical Emergency Teams Pittsburgh, USA, 11 th -12 th May 2010 ACUTE HOSPITAL SYSTEM AUDIT OF
HOW TO DO POST-HOC RESPONSE REVIEWS Ken Hillman 6 th International Symposium on Rapid Response Systems and Medical Emergency Teams Pittsburgh, USA, 11 th -12 th May 2010 ACUTE HOSPITAL SYSTEM AUDIT OF
A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs.
 6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting
 NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting 1. Introduction To standardise the type and frequency of observations to be taken on adult
NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting 1. Introduction To standardise the type and frequency of observations to be taken on adult
Los Angeles Medical Center Policies and Procedures
 Section: OPERATIONS Title: GUIDELINES FOR RAPID RESPONSE TO CHANGES IN A PATIENT S CONDITION Approved by: POLICY & PROCEDURE COMMITTEE 10/09 MEDICAL EXECUTIVE COMMITTEE 10/09 REFERENCES: Institute for
Section: OPERATIONS Title: GUIDELINES FOR RAPID RESPONSE TO CHANGES IN A PATIENT S CONDITION Approved by: POLICY & PROCEDURE COMMITTEE 10/09 MEDICAL EXECUTIVE COMMITTEE 10/09 REFERENCES: Institute for
RAPID RESPONSE TEAM & E-ICU ROBOT. Kelly J. Green, R.N., J.D. Krieg DeVault LLP & Beth W. Munz,, R.N., M.S., J.D. Parkview Health
 RAPID RESPONSE TEAM & E-ICU ROBOT Kelly J. Green, R.N., J.D. Krieg DeVault LLP & Beth W. Munz,, R.N., M.S., J.D. Parkview Health Kelly J. Green, R.N., J.D. Krieg DeVault LLP 12800 N. Meridian Suite 300
RAPID RESPONSE TEAM & E-ICU ROBOT Kelly J. Green, R.N., J.D. Krieg DeVault LLP & Beth W. Munz,, R.N., M.S., J.D. Parkview Health Kelly J. Green, R.N., J.D. Krieg DeVault LLP 12800 N. Meridian Suite 300
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
CODE ORANGE. MASS CASUALTY INCIDENT (MCI) RESPONSE PLAN Covenant Health Edmonton Acute Care Hospitals
 Code Orange 1 CODE ORANGE MASS CASUALTY INCIDENT (MCI) RESPONSE PLAN Covenant Health Edmonton Acute Care Hospitals This document contains information specific to Grey Nuns Hospital (page 14) and information
Code Orange 1 CODE ORANGE MASS CASUALTY INCIDENT (MCI) RESPONSE PLAN Covenant Health Edmonton Acute Care Hospitals This document contains information specific to Grey Nuns Hospital (page 14) and information
Subject: Skilled Nursing Facilities (Page 1 of 6)
 Subject: Skilled Nursing Facilities (Page 1 of 6) Objective: I. To ensure that Tuality Health Alliance (THA) and delegated Providence Health Plan Medicare members are appropriately placed in skilled nursing
Subject: Skilled Nursing Facilities (Page 1 of 6) Objective: I. To ensure that Tuality Health Alliance (THA) and delegated Providence Health Plan Medicare members are appropriately placed in skilled nursing
Lippincott Williams & Wilkins Nursing Book Collection 2013
 More than 300 resources covering a wide range of sub-specialties in a convenient, cost-effective package. This vast collection features a wide range of titles in multiple nursing sub-specialties, including
More than 300 resources covering a wide range of sub-specialties in a convenient, cost-effective package. This vast collection features a wide range of titles in multiple nursing sub-specialties, including
MEDICATION ADMINISTRATION: BELOW THE DRIP CHAMBER
 KINGSTON GENERAL HOSPITAL MEDICATION ADMINISTRATION: BELOW THE DRIP CHAMBER LEARNING GUIDE FOR REGISTERED NURSES AND REGISTERED PRACTICAL NURSES Prepared by: Nursing Education Date: 2001 November Revised:
KINGSTON GENERAL HOSPITAL MEDICATION ADMINISTRATION: BELOW THE DRIP CHAMBER LEARNING GUIDE FOR REGISTERED NURSES AND REGISTERED PRACTICAL NURSES Prepared by: Nursing Education Date: 2001 November Revised:
Adult: Any person eighteen years of age or older, or emancipated minor.
 Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
DETERIORATING PATIENT & RESUSCITATION POLICY
 DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50
 Acutely ill adults in hospital: recognising and responding to deterioration Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50 NICE 2018. All rights reserved. Subject to Notice of rights
Acutely ill adults in hospital: recognising and responding to deterioration Clinical guideline Published: 25 July 2007 nice.org.uk/guidance/cg50 NICE 2018. All rights reserved. Subject to Notice of rights
Supervision of Residents/Chain of Command
 Supervision of Residents/Chain of Command Creighton University Department of Surgery Residency Training Program Chain of command for Surgery residents at CUMC PGY1: The intern on call covers the two general
Supervision of Residents/Chain of Command Creighton University Department of Surgery Residency Training Program Chain of command for Surgery residents at CUMC PGY1: The intern on call covers the two general
Policy Statement: Purpose: To establish a protocol for the initiation of Adult Extracorporeal Membrane Oxygenation outside of the Operating Room.
 Policy Name: ECMO Deployment- Adult Effective Date: 05/04/15 Policy Primary: DUH ECMO Medical Director Status: Published Final Approval: Approved by: DUH ECMO Steering Committee Date: Glossary: Term: Definition:
Policy Name: ECMO Deployment- Adult Effective Date: 05/04/15 Policy Primary: DUH ECMO Medical Director Status: Published Final Approval: Approved by: DUH ECMO Steering Committee Date: Glossary: Term: Definition:
Functional Abilities / Core Performance Standards
 Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
Fetal Scalp Blood Sampling (FSBS) (NUSURGIX NataWand FSBS & Accessory Kit with NataLux Amnioscope)
 Edmonton Acute Fetal Scalp Blood Sampling (FSBS) (NUSURGIX NataWand FSBS & Accessory Kit with NataLux Amnioscope) Women s Health Manual Respiratory Therapy Current Best Practice Guidelines Original Date
Edmonton Acute Fetal Scalp Blood Sampling (FSBS) (NUSURGIX NataWand FSBS & Accessory Kit with NataLux Amnioscope) Women s Health Manual Respiratory Therapy Current Best Practice Guidelines Original Date
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
Protocol: Name of supervising ED provider: Name of RDTC Faculty: Disposition: Date: / / Time: : (military)
 RDTC TRACKING SHEET Record patient information in top right corner When completed, place in RDTC binder at A-pod Faculty desk Name: MR# Stamp OR write patient information above ED provider (i.e. faculty/pa/resident
RDTC TRACKING SHEET Record patient information in top right corner When completed, place in RDTC binder at A-pod Faculty desk Name: MR# Stamp OR write patient information above ED provider (i.e. faculty/pa/resident
ECPR Simulation at Seattle Children s Hospital
 ECPR Simulation at Seattle Children s Hospital Justin Sleasman CCP, MS, FPP Larissa Yalon BSN, RN, CCRN ECPR- Why? AHA Get with the Guidelines Resuscitation Registry: Hospital cardiac arrest in children
ECPR Simulation at Seattle Children s Hospital Justin Sleasman CCP, MS, FPP Larissa Yalon BSN, RN, CCRN ECPR- Why? AHA Get with the Guidelines Resuscitation Registry: Hospital cardiac arrest in children
The ROHNHSFT Experience: Implementing BWCH PEWS
 The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
The ROHNHSFT Experience: Implementing BWCH PEWS Alison Warren Clinical Matron for Children and Young Peoples Services The Royal Orthopaedic Hospital NHS Foundation Trust RGN, RSCN, ENB 415 & 998 PG Cert
Developing a Hospital Based Resuscitation Program. Nicole Kupchik MN, RN, CCNS, CCRN, PCCN-CSC, CMC & Chris Laux, MSN, RN, ACNS-BC, CCRN, PCCN
 Developing a Hospital Based Resuscitation Program Nicole Kupchik MN, RN, CCNS, CCRN, PCCN-CSC, CMC & Chris Laux, MSN, RN, ACNS-BC, CCRN, PCCN Objectives: Describe components of a high quality collaborative
Developing a Hospital Based Resuscitation Program Nicole Kupchik MN, RN, CCNS, CCRN, PCCN-CSC, CMC & Chris Laux, MSN, RN, ACNS-BC, CCRN, PCCN Objectives: Describe components of a high quality collaborative
Antimicrobial Stewardship in Continuing Care. Nursing Home Acquired Pneumonia Clinical Checklist
 Antimicrobial Stewardship in Continuing Care Nursing Home Acquired Pneumonia Clinical Checklist March 2015 What is Antimicrobial Stewardship? Using the: right antimicrobial agent for a given diagnosis
Antimicrobial Stewardship in Continuing Care Nursing Home Acquired Pneumonia Clinical Checklist March 2015 What is Antimicrobial Stewardship? Using the: right antimicrobial agent for a given diagnosis
Case 1 Standard of Care. Disclosures. Defending Critical Care: Navigating Through the Malpractice Maze 5/9/2015. Defending Critical Care:
 Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Banff Mineral Springs Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency Acute Care
 Banff Mineral Springs Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency EMERGENCY RESPONSE CODE BLUE ALGORITHM First Person On-Scene First Person On-Scene Call for HELP Push code
Banff Mineral Springs Hospital EMERGENCY RESPONSE CODE BLUE Cardiac Arrest / Medical Emergency EMERGENCY RESPONSE CODE BLUE ALGORITHM First Person On-Scene First Person On-Scene Call for HELP Push code
Procedure REFERENCES. Protecting 5 Million Lives from Harm Campaign, Institute for Health Care Improvement (IHI), 2007.
 Title: Nursing Chain of Command for Deterioration of Patient Condition and/or Medical Follow-up DESCRIPTION/OVERVIEW This procedure provides patient care staff guidance for ensuring effective communication
Title: Nursing Chain of Command for Deterioration of Patient Condition and/or Medical Follow-up DESCRIPTION/OVERVIEW This procedure provides patient care staff guidance for ensuring effective communication
CLINICAL PRIVILEGES- PEDIATRIC SEDATION SERVICE APP
 Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: 8/7/2013 Applicant: Check off
Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: 8/7/2013 Applicant: Check off
SURGICAL SERVICES EE-1 9/14
 Are outpatient surgical services required to meet the same quality standards as the inpatient surgical services provided? Is the scope of the surgical services provided by the hospital defined in writing
Are outpatient surgical services required to meet the same quality standards as the inpatient surgical services provided? Is the scope of the surgical services provided by the hospital defined in writing
Wilkins: Clinical Assessment in Respiratory Care, 6 th Edition
 Wilkins: Clinical Assessment in Respiratory Care, 6 th Edition Chapter 1: Preparing for the Patient Encounter Test Bank MULTIPLE CHOICE 1. Which of the following activities is not part of the role of respiratory
Wilkins: Clinical Assessment in Respiratory Care, 6 th Edition Chapter 1: Preparing for the Patient Encounter Test Bank MULTIPLE CHOICE 1. Which of the following activities is not part of the role of respiratory
NCEPOD On the Right Trach?
 NCEPOD On the Right Trach? Hospital Number Tracheostomy insertion (1) Consent and WHO type (surgical) checklists should be adopted and used prior to tracheostomy insertion, wherever it is performed. Q8.
NCEPOD On the Right Trach? Hospital Number Tracheostomy insertion (1) Consent and WHO type (surgical) checklists should be adopted and used prior to tracheostomy insertion, wherever it is performed. Q8.
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals
 Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
Requesting Ambulance Transport (999 or Urgent) A Guide for Healthcare Professionals Contents Page No. Introduction... 3 Glossary of terms... 4 Which patients should have 999 or urgent ambulance transport
Beth Israel Deaconess Medical Center Perioperative Services Manual. Guidelines for Perioperative Handoffs from OR to receiving units.
 Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool
 Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
UPMC PRESBYTERIAN SHADYSIDE POLICY AND PROCEDURE MANUAL
 UPMC PRESBYTERIAN SHADYSIDE POLICY AND PROCEDURE MANUAL POLICY: INDEX TITLE: CP-12 Care of Patients SUBJECT: Rapid Response System DATE: February 28, 2013 I. POLICY CORRESPONDING PROCEDURES: CP-12-PRO
UPMC PRESBYTERIAN SHADYSIDE POLICY AND PROCEDURE MANUAL POLICY: INDEX TITLE: CP-12 Care of Patients SUBJECT: Rapid Response System DATE: February 28, 2013 I. POLICY CORRESPONDING PROCEDURES: CP-12-PRO
Missouri Outside the Hospital Do Not Resuscitate Order. Boone County Fire Protection District EMS Education
 Missouri Outside the Hospital Do Not Resuscitate Order 4 Times to Withhold CPR Obviously mortal wound such as decapitation Rigor mortis Livor mortis also known as dependent lividity or venous pooling Valid
Missouri Outside the Hospital Do Not Resuscitate Order 4 Times to Withhold CPR Obviously mortal wound such as decapitation Rigor mortis Livor mortis also known as dependent lividity or venous pooling Valid
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: OXYGEN ADMINISTRATION (INCLUDING Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory Care Services (Resp)
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: OXYGEN ADMINISTRATION (INCLUDING Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory Care Services (Resp)
SAHS Critical Care Residency Program
 SAHS Critical Care Residency Program Sherry Parks BSN, MS, NEA-BC VP &CNO Teri Woychick BSN, RN Director of Critical Care Cindy Malinowski RN, MN, CCRN, Nurse Educator Perfect Storm High CC turnover Lack
SAHS Critical Care Residency Program Sherry Parks BSN, MS, NEA-BC VP &CNO Teri Woychick BSN, RN Director of Critical Care Cindy Malinowski RN, MN, CCRN, Nurse Educator Perfect Storm High CC turnover Lack
Standard Operating Procedure. for the Retrieval Nurse
 Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
Standard Operating Procedure for the Retrieval Nurse 1. Introduction The Southampton PICU retrieval service performs approximately 250 retrievals per year within the Wessex region. It covers a population
Submission Form Deadline: November 9, 2015
 Submission Form Deadline: November 9, 2015 Organization: Sinai Hospital Contact Person: Pat Moloney-Harmon, MS, RN, CCNS, FAAN Title: Clinical Outcomes Specialist, Children s Services Address: 2401 W.
Submission Form Deadline: November 9, 2015 Organization: Sinai Hospital Contact Person: Pat Moloney-Harmon, MS, RN, CCNS, FAAN Title: Clinical Outcomes Specialist, Children s Services Address: 2401 W.
GAMUT QI Collaborative Consensus Quality Metrics (v. 05/16/2016)
 1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
Optimizing the clinical role of the ACP in Trauma Gena Brawley, ACNP Carolinas Healthcare Systems NPSS Asheville, NC
 Optimizing the clinical role of the ACP in Trauma Gena Brawley, ACNP Carolinas Healthcare Systems 2017 NPSS Asheville, NC Objectives Discuss the role of the Critical Care Nurse Practitioner in Trauma Identify
Optimizing the clinical role of the ACP in Trauma Gena Brawley, ACNP Carolinas Healthcare Systems 2017 NPSS Asheville, NC Objectives Discuss the role of the Critical Care Nurse Practitioner in Trauma Identify
Improving Transition Home through a Standardized Discharge Process. Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016
 Improving Transition Home through a Standardized Discharge Process Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016 Objectives Identify components of the Children s Hospital Colorado
Improving Transition Home through a Standardized Discharge Process Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016 Objectives Identify components of the Children s Hospital Colorado
TRAUMA CENTER REQUIREMENTS
 California Trauma Center Level III Criteria California Code of Regulations,, Chapter 7 - Trauma Care System with American College of Surgeons (Green Book) references; includes FAQ clarifications TRAUMA
California Trauma Center Level III Criteria California Code of Regulations,, Chapter 7 - Trauma Care System with American College of Surgeons (Green Book) references; includes FAQ clarifications TRAUMA
60 Memorial Medical Parkway Palm Coast, Florida 32164
 POLICY & PROCEDURES TITLE: Privileges of Student Nurses and Student Nursing Assistants POLICY # EDU 001 POLICY CATEGORY: Administrative / Education Origination Date: 12/2008 Last Review/Revision Date:
POLICY & PROCEDURES TITLE: Privileges of Student Nurses and Student Nursing Assistants POLICY # EDU 001 POLICY CATEGORY: Administrative / Education Origination Date: 12/2008 Last Review/Revision Date:
EM Coding Newsletter & Advisory Critical Care Update
 EM Coding Newsletter & Advisory Critical Care Update Keep Your Critical Care Up With The Times Critical Care Case Scenarios Frequently Asked Questions Keep Your Critical Care Up With The Times In the last
EM Coding Newsletter & Advisory Critical Care Update Keep Your Critical Care Up With The Times Critical Care Case Scenarios Frequently Asked Questions Keep Your Critical Care Up With The Times In the last
Clinical Transition Practicum Packet General Information Policies and Procedures Preceptor and Nursing Student Forms
 Clinical Transition Practicum Packet General Information Policies and Procedures Preceptor and Nursing Student Forms Fall 2014 1 Description The McLennan Community College Clinical Transition Practicum
Clinical Transition Practicum Packet General Information Policies and Procedures Preceptor and Nursing Student Forms Fall 2014 1 Description The McLennan Community College Clinical Transition Practicum
SUPERVISION POLICY. Roles, Responsibilities and Patient Care Activities of Subspecialty Residents (Fellows)
 Roles, Responsibilities and Patient Care Activities of Subspecialty Residents (Fellows) Definitions Pediatric Critical Care Medicine Fellowship Program Seattle Children s Hospital and Harborview Medical
Roles, Responsibilities and Patient Care Activities of Subspecialty Residents (Fellows) Definitions Pediatric Critical Care Medicine Fellowship Program Seattle Children s Hospital and Harborview Medical
Feedback from Anesthesia clinicians. 2.1 Intubate Patient Workflow
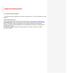 Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
PATIENT RIGHTS, PRIVACY, AND PROTECTION
 REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency
 DEPARTMENT OF ANESTHESIA Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency 1. An anesthesiology resident, during a two month rotation should gain exposure to the scope
DEPARTMENT OF ANESTHESIA Critical Care Curriculum for Two-Month Rotation as Part of an Anesthesiology Residency 1. An anesthesiology resident, during a two month rotation should gain exposure to the scope
C. Physician s orders for medication, treatment, care and diet shall be reviewed and reordered no less frequently than every two (2) months.
 SECTION 1300 - MEDICATION MANAGEMENT 1301. General A. Medications, including controlled substances, medical supplies, and those items necessary for the rendering of first aid shall be properly managed
SECTION 1300 - MEDICATION MANAGEMENT 1301. General A. Medications, including controlled substances, medical supplies, and those items necessary for the rendering of first aid shall be properly managed
Coding Guidelines for Certain Respiratory Care Services January 2018 (updates in red)
 Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
NON-HOSPITAL MEDICAL AND SURGICAL FACILITIES ACCREDITATION PROGRAM Accreditation Standards. Overnight Stay
 NON-HOSPITAL MEDICAL AND SURGICAL FACILITIES ACCREDITATION PROGRAM NON-HOSPITAL MEDICAL AND SURGICAL FACILITIES ACCREDITATION PROGRAM INTRODUCTION Overnight stay is considered a post-anesthesia level of
NON-HOSPITAL MEDICAL AND SURGICAL FACILITIES ACCREDITATION PROGRAM NON-HOSPITAL MEDICAL AND SURGICAL FACILITIES ACCREDITATION PROGRAM INTRODUCTION Overnight stay is considered a post-anesthesia level of
Department of Veterans Affairs VHA HANDBOOK HOME RESPIRATORY CARE PROGRAM
 Department of Veterans Affairs VHA HANDBOOK 1173.13 Veterans Health Administration Transmittal Sheet Washington, DC 20420 November 1, 2000 HOME RESPIRATORY CARE PROGRAM 1. REASON FOR ISSUE: This VHA Handbook
Department of Veterans Affairs VHA HANDBOOK 1173.13 Veterans Health Administration Transmittal Sheet Washington, DC 20420 November 1, 2000 HOME RESPIRATORY CARE PROGRAM 1. REASON FOR ISSUE: This VHA Handbook
