HIGH-IMPACT LEADERSHIP: DEVELOPING CORE LEADERS M12 Monday, December 5, 2016
|
|
|
- Eileen Stephens
- 6 years ago
- Views:
Transcription
1 HIGH-IMPACT LEADERSHIP: DEVELOPING CORE LEADERS M12 Monday, December 5, 2016 Objectives: 1. Gain an in-depth understanding of four Core Leadership Competencies 2. Apply practical insights to developing their core leaders and teams 3. Can describe new behaviors critical to the practice of leadership in the middle 8:30-9:00 Introductions and Overview 9:00-10:15 Managing the Work 10:15-10:30 Break 10:30-12:00 Improving the Work 12:00-12:45 Lunch 12:45-2:00 Build Team Capability 2:00-2:45 Shape Team Culture Part 1 2:45-3:00 Break 3:00-3:45 Shaping Team Culture Part 2 3:45-4:00 Q&A and Building Your Plan
2 Case Study: Managing the Work at Orlando Health rev Background: In the recent months, Orlando Regional Medical Center (ORMC) began implementation and organizational spread of unit/departmental based strategy and process improvement boards called Gemba boards ( Gemba : A Japanese word meaning the actual place, used for the place where the work is done, such as an exam room, the laboratory, an operating room, or the cafeteria ( Imai, 2012, p. 62)). Each unit/department reflects the same strategic imperatives that the administration s board displays. Consequently, the administration board is a reflection of strategic imperatives that have been established by the Board of Directors and senior leadership. The difference lies in the depth of the process improvements that are reflected on each board. Any team member or leader can complete an idea ticket and submit to the boards. This case reflects one such idea, where the frontline sees the opportunity for a process improvement that could have a major impact on more than one strategic imperative. A Case for Innovation at the Middle : Chris is a Physical Therapist and the supervisor for acute care therapy. Chris heard many discussions and brainstorming sessions by his own manager and the Chief Operating Officer related to spending money to make money and how we can decrease length of stay. As part of Chris s development for further leadership roles, his manager never hesitated to encourage her team to try new things that would improve care and save money. Chris had observed multiple patient discharge delays that were due to durable medical equipment (DME) arrival times. Patients often waited hours for discharge because the outside DME Company could not deliver the required walkers, wheelchairs, or commodes until the next day. It was shown to have extended patient stays for several hours and many times overnight. Chris gathered data for two weeks, looking at the resources tied into obtaining the needed DME and the cost of the bed being utilized by a patient who was ready for discharge but was only waiting on a piece of equipment. The nurse manager for the Ortho unit worked with Chris to develop an idea ticket. It was clear that their project would require buy-in from the administration team. Chris and the nurse manager brought their ticket to the weekly administration strategy board huddle and presented their idea when it was their turn. Administration was supportive and excited at the team time. They were watching the first big process change idea come from the front line team. Chris enlisted discharge planners, nurses, and care coordinators to work with him as a team to solve the problem. Chris learned through his own research that we would not be able to obtain our own DME supplies for patients and just give it away (it costs less to give away a $32 walker than to hold a bed) due to certain laws. Chris then ventured out by calling the Center for Medicare Services (CMS) on his own. Through his discussions with CMS, he learned of a way that our organization could partner with a current vendor of orthopedic supplies and maintains certain DME at the hospital. The order for that DME would then be coordinated between the hospital and the orthopedic supply company on discharge. The outside company would then make the appropriate contacts for approval of providing certain DME and the permission to bill insurance.
3 Case Study: Managing the Work at Orlando Health rev Chris created metrics that are being used to verify the success of this new process. He measures the financial impact of the decrease in length of stay on the Ortho unit and patient experience scores specific to discharge on Ortho. While Chris and the team work toward slight modifications in the process and recording the lessons learned, the ultimate end goal will be a sustainable process that can better serve other patient populations within ORMC and other Orlando Health hospitals. Activity: - List the 5 components of Manage the Work as described by Pugh and Munch (2016). - Now, identify examples of these components in practice within this case.
4 Case Study: Orlando Health Imaging Council-Improve the Work Background: A problem was identified relative to the timeliness of approved report availability for imaging studies. This had long been a challenge in our organization and was impeding our ability to excel in areas of length of stay, throughput, patient experience and physician satisfaction. All of these impact components needed consideration as we structured a process improvement activity that would provide sustainable results. Several disciplines including imaging, transcription, nursing, IT, risk management, and physicians were identified as key stakeholders and each had a different perspective as to what the real obstacles were and why they existed. In essence, we lacked an appreciation or understanding of what each discipline was experiencing as a result of the problem and therefore, the culture was lacking with respect to collaboration, support, patience and team mindedness. We needed a means of accountability through standardization and clarity of responsibility. Ultimately, we were failing to meet the needs of our patients and our physicians. Initiative: It is relevant but not surprising that considerable change was occurring in tandem with the problem that had been identified. However, the imaging managers and supervisors recognized the need to prioritize this particular problem. To be candid, they were frustrated with the feedback that was being given regularly from other areas in terms of not having timely critical information about their patients. At the root of the problem was the need for a technology that would allow our physician to interpret studies using voice recognition and self-editing, however even with the technology we had significant hurdles with respect to old processes and policies that did not align with what we identified as our future state. We needed buy-in from all stakeholders to ensure a successful transition from the current to future state which included our physicians, technologists, administration and others. The managers recognized that the amount of change involved would require everyone on the team to understand the end goal and to understand their role in helping to achieve it. Throughout the process leadership recognized the need to evaluate processes that were impacted as a result of this change and to develop subsequent plans of action to support the overarching goal of reducing time to a final approved interpretation. The action plans were critical tools in ensuring progress. We established regular meetings with the key change agents and reviewed our progress on a regular basis. Superusers were identified by the managers and were provided the time and training necessary to be able to effectively support the in that role. The managers met with the superusers regularly and provided guidance and support. Checklists and reports were crafted that provided a means for the team to understand the progress being made ( see data provided). Physician ownership of the process was paramount but so was compliance by the imaging team of the standardized work that had been redesigned as a result of the new workflow. The reports were used to understand where and when fallouts were occurring and a weekly call was established to discuss the orders that had been entered and completed and were missing approved reports. Physician leaders were informed of compliance with the new process and were responsible for addressing individual physicians who may have been identified as non-compliant. Report out to senior leadership through the Allied Health Executive Council ensured a consistent focus on the priority and to help remove barriers that were identified by the Imaging Council as they progressed through the initiative. The team worked together to change a process that involved several disciplines, had endured significant workarounds and was outdated. The results were remarkable in that they were consistent and sustainable. Consequently, the managers identified the opportunity to further drill down to a specific area (see example slide#2). While improvement had been made overall, there was opportunity for further collaboration and focus in the emergency department where efficiency is essential. The managers continue to apply the skills they learned and refined as a result of this process and are confident in their approach for the next opportunity.
5 Data: AVERAGE MINUTES Preliminary Radiology results available in PACS within 1 hour of order: Orlando Health Process Improvement FY Feb 14' Ma r 14' Apr 14' Ma y 14' Jun 14' Jul Aug Sep Oct 14' 14' 14' 14' Ma Nov Dec Jan Feb Apr r 14" 14' 15' 15' 15' 15' Ma y 15' Jun 15' Jul Aug Sep Oct 15' 15' 15' -15 Series Data: Finalized Radiology Reports are available in PACS within 1 Hour of Order for ED Lower is Better! 60 Plain Film (DX) Examinations CY MEDIAN MINUTES Jan 16 Feb 16 Mar 16 Apr 16 May 16 Jun 16 Jul 16 Aug 16 Sept 16 APMC DPH ORMC SS
6 Activity: After reviewing the case and the above documents, the following is designed to challenge you in identifying key components of the core leader skill sets and competencies: 1. Identify examples in this case for the following: Sharing vision and building will Modeling the way Promoting transparency Encouraging mindfulness 2. Give an example of how the imaging council could use what they learned from this case to further shape team culture
7 Background: Orlando Health, established five audacious goals on its quality journey in At the beginning of the quality journey, transparency with the board, leadership and team members became a guiding principle. One system goal was to reduce overall harm by 80% within five years. Medication errors was the largest category of harm events in the organization and at each individual hospital. An interdisciplinary team was charged with studying the issues associated with medication errors in the hospitals, reviewing the literature and data and make recommendation to the Chief Quality and Transformation Officer and Vice President of Patient Care. The organization has had for many years, a well-established shared leadership model in the nursing and allied health. Engaging the team in patient safety and improvement activities became a focus. The nursing leadership council, nurse practice councils, pharmacy council were highly engaged in helping the interdisciplinary team understanding the issues with support from the quality, risk and data analytics team. Chief nursing officers from throughout the system have had, for example, a weekly call discussing all harm events as do the allied health leaders. Medication reconciliation, access to timely medications, independent double verification and distractions were some of the identified drivers associated with the medication errors. A variety of process changes occurred to make medication administration safer. The system team recommended implementation of a barcoding system for medications as an essential step to develop a safer accountable system for medication administration. The success of the implementation was critical to reduce harm events. A Case for Team Engagement Dr. P. Phillips Hospital (DPH), one of the eight hospitals in the system was the third hospital to implement the barcoding system. The goal was to achieve 90% medications barcoded. With each hospital implementation there were lessons learned and improvements made. The chief nursing officer (CNO) of DPH knew the importance of a successful implementation and created a hospital steering committee that included the nurse managers, the hospital practice chair and co-chair, the pharmacy manager, learning specialist and nursing administrators several months before the hospital was to go live. She charged the team with oversight of the process, review of the policy, resources needed, communication and engagement of the team. The steering committee was a forum for discussion, debate and decision-making. The team visited the hospital that was implementing the barcoding system observing the process and engaging with their peers. The CNO s goal was to gain an understanding the issues and challenges for the team and address safety and sustainability in her hospital. The team met weekly. Five weeks before the implementation at the hospital, the CNO asked the managers and unit practice chairs to identify equipment needed including additional computers and types of scanners based on the individual unit needs. Some units preferred wireless scanners while other requested wired scanners. Meeting with the steering team, unit practice council and allied health council, the CNO proposed a revision in the medication
8 administration policy. The proposed changes were developed to ensure that patient safety was the focus. The policy revision addressed consequences if a team member deliberately chose to not administer medications using the established barcoding system. There were two offenses that would result in immediate termination including: using and carrying printed arms bands versus using he patient s armband and creating a work-around instead of following the established process of scanning medications. All staff administering medication were required to review and sign the new policy. The unit practice council chair with the nurse manager were responsible for the implementation and conducted shift huddles. The CNO and administrators in their weekly rounding spent time with the listening to the staff on successes, issues and concerns. There was weekly messaging from the CNO, reports from pharmacy and it was a regular agenda item on the unit practice council agenda. Some staff struggled during the bar-coding system implementation. Members of the practice council, learning specialist and nurse manager coached and supported them as issues arose. After several months the percentages of medication scanned met the goal and remained stable at 90-92%. The CNO challenged the steering committee to identify ways to increase the medication scanned to 95%. The pharmacy audit identified individuals who missed more than nine medications scanned in a month. In some cases, it was issues with scanning labels on prepacked medications and IV solutions and inconsistency in policy on heparin flush scanning. Initially there was a two-page list of individuals who missed more than nine medications each. Over the course of three months, the hospital reached 95% medications scanned and remains there today. Activity: List the 4 components of Building Team Capability as described by Pugh and Munch (2016). Now, identify examples of these components in practice within this case.
9 Orlando Health: Shaping Team Culture In 2012, the critical care team at Orlando Regional Medical Center was given a survey to discover opportunities to unify the team. This included nurses, physicians, residents, respiratory therapists, pharmacists, and other key clinicians. The outcomes were telling. They painted a picture of distrust, disloyalty, leadership deficits, a lack of psychological safety, and feelings of inadequacy and lack of appreciation. Over the next 24 months, administration would team with physician leaders and departmental leaders to create initiatives centered around the patient, but that would require team cohesiveness. Team building sessions were held with team members from each area and a shared vision was created. Promises were made in terms of proper communications and how debriefings would take place after major incidents. It was not without incident or minor bumps in the road, but the outcomes have been the creation and implementation of the following patient care initiatives; These initiatives would include; Evidence-based ventilator weaning guidelines Daily collaborative rounding and checklists Weekly critical care task force meetings Early mobility protocol From 8 ICU admissions order set to 1 The team has demonstrated a positive response by the most recent team member surveys. For example, respiratory care scored the lowest at ORMC in 2013 for teamwork across departments. They felt unappreciated for their expertise and a lack of trust for the physicians. In the most recent survey, they are one of the highest scoring departments in that area. Physician leaders have been given many leadership training opportunities and as the care team leader, they are expected to set the best example for the other team members. The physicians who once had adversarial relationships with the therapists, now hold successful medical director positions. Physicians spend more time teaching and guiding the team on their decisions, rather than directing orders without explanation and input. The goals are to have a psychologically safe environment where honesty and integrity are paramount, for the sake of the patient. Activity: Give an example from this case where each competency from Shaping Team Culture is demonstrated.
10 Managing Time & Attention Exercise How do you spend your day? The following exercise is designed to collect data about how you currently spend your day. The information will help you to identify what activities add value to your patients, staff, and role and what activities do not. Instructions: For one week, track all of the activities you do during your workday. Include the start and stop time, a description of the activity, if the activity was planned or unplanned, and if the activity was value added, Incidental, or waste. The following examples and operational definitions will add you in the exercise. Current State How do you spend your time? Please use the time tracking form to capture your activity data. Here is an example of how to complete the form. Start Time End Time Activity Planned or Unplanned Value- Added/Incidenta l/waste 8:30 8:42 Read and write P Incidental 8:42 9:00 Develop A3 for improvement project P Value-added 9:00 9:15 Help staff to find medical equipment needed for care U Waste Source: A Factory of One, Fig. 1.3 Example Activities: Activities may include any of the following. The list is not all-inclusive, so add activities as appropriate. Meetings Phone Calls s Instant Messaging Moving between locations Patient Care Dialogue with staff Reviewing reports/memos Generating Fixing problems Administrative Tasks Quality Improvement reports/memos (scheduling, Payroll) Coaching Customer Communication Responding to requests Other? Planned vs. Unplanned: Planned activities are reasonably clear and are activities you planned to do as part of your daily work at a scheduled time or during the course of your workday. Unplanned are activities that presented themselves to you during your workday, but you did not predict or plan for them in advance. Work s Value: Use the following operational definitions to determine if the work activity is valueadded, incidental, or wasteful. Value-Added: Incidental: Waste: Something the customer is willing to pay for Transform the product or service in some way Done correctly the first time No-value added, but necessary No-value added, but NOT necessary Resource:
11 Managing Time & Attention Exercise Type of Waste: Using one of the categories below, select the type of waste each activity is and indicate it in the table above. Defects (Rework) Over-Production (Redundant work) Waiting Not Clear (Confusion) Transporting Stuff Inventory (Too Much) Motion (Movement of People) Excess Processing Day of the week Start Time End Time Activity Planned or Unplanned Value- Added/Incide ntal/waste If Waste, what type? Source: A Factory of One, Fig. 1.3 Resource:
12 Managing Time & Attention Exercise Summarizing Your Data Add up all the hours and determine percentages of your total time for each category. Use this as a Pareto to target opportunities improvement. Activity Category Total time (hh:mm) % of Total Time Top Three (3) Wastes From the list above, what are your top three (3) wastes? Waste Activity Description of Waste Type of Waste (see definitions below) Resource:
13 Core Leader Skills and Competencies Self-Assessment Tool How well do I? Manage the Work Low High Possible Follow-up Idea 1. Manage time and resources Create standard work and process Measure: financial, quality, customer & key processes Surface and solve problems in real time Engage across departmental/team boundaries Improve the Work Low High 6. Prioritize and align to strategy and aims
14 7. Understand current state, cause and target condition Learn and use improvement tools and methods Reduce variation and waste Get results and sustain them Build Team Capability Low High 11. Develop competency through coaching Use the whole team Communicate effectively Establish respect and accountability Shape Team Culture Low High 15. Share vision and build will Promote transparency Model the way Encourage mindfulness Keep the person at the center Page 2 of 2 Version 5.0 August 2016
Laguna Honda Lean Transformation. Laguna Honda Strategic Performance Management November 2017
 Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Transformational Patient Care Redesign Project
 Transformational Patient Care Redesign Project Kaveh Houshmand Azad 1 Summary In 2008 2009, Providence Holy Cross Medical Center, a 340- bed hospital located in Mission Hills, California embarked upon
Transformational Patient Care Redesign Project Kaveh Houshmand Azad 1 Summary In 2008 2009, Providence Holy Cross Medical Center, a 340- bed hospital located in Mission Hills, California embarked upon
Identifying Errors: A Case for Medication Reconciliation Technicians
 Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Building a Lean Team. Using Lean Methodology to Develop a Collaborative Rounding Model. April 28 th, 2010
 Building a Lean Team Using Lean Methodology to Develop a Collaborative Rounding Model April 28 th, 2010 Faculty APD, Internal Medicine Residency Program Co-Sponsor, LEAN Improvement Team APD, Internal
Building a Lean Team Using Lean Methodology to Develop a Collaborative Rounding Model April 28 th, 2010 Faculty APD, Internal Medicine Residency Program Co-Sponsor, LEAN Improvement Team APD, Internal
From Implementation to Optimization: Moving Beyond Operations
 From Implementation to Optimization: Moving Beyond Operations Session 260, March 8, 2018 Scott Aikey, Sr. Director, Core Clinical Applications Children s Hospital of Philadelphia 1 Conflict of Interest
From Implementation to Optimization: Moving Beyond Operations Session 260, March 8, 2018 Scott Aikey, Sr. Director, Core Clinical Applications Children s Hospital of Philadelphia 1 Conflict of Interest
Emergency Department Throughput
 Emergency Department Throughput Patient Safety Quality Improvement Patient Experience Affordability Hoag Memorial Hospital Presbyterian One Hoag Drive Newport Beach, CA 92663 www.hoag.org Program Managers:
Emergency Department Throughput Patient Safety Quality Improvement Patient Experience Affordability Hoag Memorial Hospital Presbyterian One Hoag Drive Newport Beach, CA 92663 www.hoag.org Program Managers:
Delivering Great Care with High Reliability The Orlando Health Journey
 FE5 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 11, 2017 Frank Federico, RPh Vice President Patricia McGaffigan, RN, MS, CPPS
FE5 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 11, 2017 Frank Federico, RPh Vice President Patricia McGaffigan, RN, MS, CPPS
Advancing Accountability for Improving HCAHPS at Ingalls
 iround for Patient Experience Advancing Accountability for Improving HCAHPS at Ingalls A Case Study Webconference 2 Managing your audio Use Telephone If you select the use telephone option please dial
iround for Patient Experience Advancing Accountability for Improving HCAHPS at Ingalls A Case Study Webconference 2 Managing your audio Use Telephone If you select the use telephone option please dial
Maimonides Medical Center Makes a Quantum Leap with Advanced Computerized Patient Record Technology
 Maimonides Medical Center Makes a Quantum Leap with Advanced Computerized Patient Record Technology Healthcare Information and Management Systems Society Electronic Poster Session CPR System Planning The
Maimonides Medical Center Makes a Quantum Leap with Advanced Computerized Patient Record Technology Healthcare Information and Management Systems Society Electronic Poster Session CPR System Planning The
Safety in Mental Health Collaborative
 NHS Tayside Safety in Mental Health Collaborative Improving Safety in Mental Health Programme Aims supported by an Improvement Advisor: Dr Noeleen Devaney Support 4 UK organisations to: reduce harm improving
NHS Tayside Safety in Mental Health Collaborative Improving Safety in Mental Health Programme Aims supported by an Improvement Advisor: Dr Noeleen Devaney Support 4 UK organisations to: reduce harm improving
Hardwiring Processes to Improve Patient Outcomes
 Hardwiring Processes to Improve Patient Outcomes Barbara Adcock Mohr, Administrative Director, Rehabilitation Services Mark Prochazka, Assistant Director, Rehabilitation Services UNC Hospitals FIM, UDSMR,
Hardwiring Processes to Improve Patient Outcomes Barbara Adcock Mohr, Administrative Director, Rehabilitation Services Mark Prochazka, Assistant Director, Rehabilitation Services UNC Hospitals FIM, UDSMR,
Taming Length of Stay Challenges Through Analytics
 Taming Length of Stay Challenges Through Analytics March 3, 2016 Dr. Michelle Pezzani, Medical Director Utilization Management at El Camino Hospital & Palo Alto Medical Foundation (PAMF) Petrina Griesbach
Taming Length of Stay Challenges Through Analytics March 3, 2016 Dr. Michelle Pezzani, Medical Director Utilization Management at El Camino Hospital & Palo Alto Medical Foundation (PAMF) Petrina Griesbach
HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017
 HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017 Nebraska Medicine $1.2 billion academic health system 8,000 employees More than 1,000 affiliated physicians Primary
HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017 Nebraska Medicine $1.2 billion academic health system 8,000 employees More than 1,000 affiliated physicians Primary
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver JULY 18, 2016
 Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
Departments to Improve. February Chad Faiella RN, Terri Martin RN. 1 Process Excellence
 Coordination of Multiple Departments to Improve ED Throughput February 2011 Chad Faiella RN, Terri Martin RN 1 Agenda OhioHealth information Grant Medical Center facts Bed assignment process Key takeaways
Coordination of Multiple Departments to Improve ED Throughput February 2011 Chad Faiella RN, Terri Martin RN 1 Agenda OhioHealth information Grant Medical Center facts Bed assignment process Key takeaways
Winning at Care Coordination Using Data-Driven Partnerships
 Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
9/15/2017 THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE LEARNING OBJECTIVES
 THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE D O N N A C R I M M I N S - B O N N E L L, B S N, M H S M, C P H Q, L S S G B LEARNING OBJECTIVES 1) Define who is affected by inefficiency in throughput
THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE D O N N A C R I M M I N S - B O N N E L L, B S N, M H S M, C P H Q, L S S G B LEARNING OBJECTIVES 1) Define who is affected by inefficiency in throughput
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver JULY 18, 2016
 Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL
 Publication Year: 2008 REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL Summary: Creation of Bed Coordinator position to improve patient flow throughout the entire hospital Hospital:
Publication Year: 2008 REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL Summary: Creation of Bed Coordinator position to improve patient flow throughout the entire hospital Hospital:
Executive Director s Report: Customer Experience Update
 Executive Director s Report: Customer Experience Update Board of Directors Meeting, November 12, 215 Seconds Calls Service Center Performance 2, 18, 16, 14, 12, 1, 8, 6, 4, 2, Calls Offered Jan 215 Sept
Executive Director s Report: Customer Experience Update Board of Directors Meeting, November 12, 215 Seconds Calls Service Center Performance 2, 18, 16, 14, 12, 1, 8, 6, 4, 2, Calls Offered Jan 215 Sept
Improving Pain Center Processes utilizing a Lean Team Approach
 Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach
 Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Northern Health - Acute Services. Evidence Based Practice Venous Thromboembolism Prevention
 Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Improving Access to Pediatric MR performed under General Anesthesia Benefits of a Rapid Improvement Event (RIE)
 /3/207 Improving Access to Pediatric MR performed under General Anesthesia Benefits of a Rapid Improvement Event (RIE) N I Sarwani, MD, FRCR, FSAR M A Bruno, MS, MD, FACR S Mrozowski, MHA, NRP, CPPS Corresponding
/3/207 Improving Access to Pediatric MR performed under General Anesthesia Benefits of a Rapid Improvement Event (RIE) N I Sarwani, MD, FRCR, FSAR M A Bruno, MS, MD, FACR S Mrozowski, MHA, NRP, CPPS Corresponding
The Triple Aim. Productivity: Digging Deep Enough 11/4/2013. quality and satisfaction); Improving the health of populations; and
 NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence
 PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence Rachel Brunt, RN, BSN, MBA-HCA, CIC, CPHQ, Director Quality Jessie Hanks, BS, RHIA, Director HIM Lafayette General
PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence Rachel Brunt, RN, BSN, MBA-HCA, CIC, CPHQ, Director Quality Jessie Hanks, BS, RHIA, Director HIM Lafayette General
National Homecare KPI performance March 2017
 National Homecare KPI performance March 2017 Foreword We are pleased to publish our latest KPI report, continuing our commitment to the transparency of the service we provide to our patients and customers,
National Homecare KPI performance March 2017 Foreword We are pleased to publish our latest KPI report, continuing our commitment to the transparency of the service we provide to our patients and customers,
Relational Coordination: An Imperative Influencing our Capacity to Reach the Core
 Relational Coordination: An Imperative Influencing our Capacity to Reach the Core Linda Q. Everett, PhD, RN, NEA-BC, FAAN Executive Vice President & Chief Nurse Executive Indiana University Health 12/7/2012
Relational Coordination: An Imperative Influencing our Capacity to Reach the Core Linda Q. Everett, PhD, RN, NEA-BC, FAAN Executive Vice President & Chief Nurse Executive Indiana University Health 12/7/2012
LEAN Transformation Storyboard 2015 to present
 LEAN Transformation Storyboard 2015 to present Rapid Improvement Event Med-Surg January 2015 Access to Supply Rooms Problem: Many staff do not have access to supply areas needed to complete their work,
LEAN Transformation Storyboard 2015 to present Rapid Improvement Event Med-Surg January 2015 Access to Supply Rooms Problem: Many staff do not have access to supply areas needed to complete their work,
Influence of Patient Flow on Quality Care
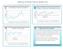 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Hard Truths Public Board 29th September, 2016
 Hard Truths Public Board 29th September, 2016 Presented for: Presented by: Author Previous Committees Governance Professor Suzanne Hinchliffe CBE, Chief Nurse/Deputy Chief Executive Heather McClelland
Hard Truths Public Board 29th September, 2016 Presented for: Presented by: Author Previous Committees Governance Professor Suzanne Hinchliffe CBE, Chief Nurse/Deputy Chief Executive Heather McClelland
Delivering Great Care with High Reliability
 FE4 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 5, 2016 Joelle Baehrend, MA Director, Institute of Healthcare Improvement 1
FE4 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 5, 2016 Joelle Baehrend, MA Director, Institute of Healthcare Improvement 1
Using Lean Principles to Decrease Outpatient Registration Wait Times. It s a Journey not a Destination
 Using Lean Principles to Decrease Wait Times It s a Journey not a Destination 533 Bed Acute Care System 461 Beds at AnMed Health Medical Center 72 Beds at AnMed Health Women s and Children's Hospital 45
Using Lean Principles to Decrease Wait Times It s a Journey not a Destination 533 Bed Acute Care System 461 Beds at AnMed Health Medical Center 72 Beds at AnMed Health Women s and Children's Hospital 45
LESSONS LEARNED IN LENGTH OF STAY (LOS)
 FEBRUARY 2014 LESSONS LEARNED IN LENGTH OF STAY (LOS) USING ANALYTICS & KEY BEST PRACTICES TO DRIVE IMPROVEMENT Overview Healthcare systems will greatly enhance their financial status with a renewed focus
FEBRUARY 2014 LESSONS LEARNED IN LENGTH OF STAY (LOS) USING ANALYTICS & KEY BEST PRACTICES TO DRIVE IMPROVEMENT Overview Healthcare systems will greatly enhance their financial status with a renewed focus
A Million Little Pieces: Developing a Controlled Substance Diversion Program. Tanya Y. Barnhart, PharmD, BCPS
 A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
Translating Evidence to Safer Care
 Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Corporate Services Employment Report: January Employment by Staff Group. Jan 2018 (Jan 2017 figure: 1,462) Overall 1,
 Corporate Services Employment Report: January Employment by Staff Group Jan (Jan 20 figure: 1,462) Jan % Overall 1,520 +58 +4.0% 8 Management (VIII+) 403 +52 4.8% Clerical & Supervisory (III to VII) 907
Corporate Services Employment Report: January Employment by Staff Group Jan (Jan 20 figure: 1,462) Jan % Overall 1,520 +58 +4.0% 8 Management (VIII+) 403 +52 4.8% Clerical & Supervisory (III to VII) 907
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario
 Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 4/1/2014 This document is intended to provide health care organizations in Ontario with guidance as to how they can develop
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 4/1/2014 This document is intended to provide health care organizations in Ontario with guidance as to how they can develop
5D QAPI from an Operational Approach. Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Pathway Health 2013
 5D QAPI from an Operational Approach Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Objectives Review the post-acute care data agenda. Explain QAPI principles Describe leadership
5D QAPI from an Operational Approach Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Objectives Review the post-acute care data agenda. Explain QAPI principles Describe leadership
Achieving Operational Excellence with an EHR a CIO s Perspective
 Achieving Operational Excellence with an EHR a CIO s Perspective Phyllis Schuck, SPHR CIO of Pinehurst Surgical HIT Session 6.02 Thursday, March 29, 2007 Pinehurst Surgical Organization Overview Founded
Achieving Operational Excellence with an EHR a CIO s Perspective Phyllis Schuck, SPHR CIO of Pinehurst Surgical HIT Session 6.02 Thursday, March 29, 2007 Pinehurst Surgical Organization Overview Founded
Patient and Family Engagement Strategy. April 10, 2013
 Patient and Family Engagement Strategy April 10, 2013 1 Webinar Agenda Overview & Introductions Kathy Wallace Why is Patient & Family Engagement the Right Thing to do? Carrie Brady Patient & Family Advisor
Patient and Family Engagement Strategy April 10, 2013 1 Webinar Agenda Overview & Introductions Kathy Wallace Why is Patient & Family Engagement the Right Thing to do? Carrie Brady Patient & Family Advisor
Change Management at Orbost Regional Health
 Change Management at Orbost Regional Health Our change management journey 1 Medication Change System Meds at Beds 2 The slightly exaggerated before process 3 Project Goals The purpose of the Meds at Beds
Change Management at Orbost Regional Health Our change management journey 1 Medication Change System Meds at Beds 2 The slightly exaggerated before process 3 Project Goals The purpose of the Meds at Beds
GRANTS.GOV Updates Federal Demonstration Partnership Meeting. Presented by Grants.gov September 7, 2017
 GRANTS.GOV Updates Federal Demonstration Partnership Meeting Presented by Grants.gov September 7, 2017 RELEASE UPDATE 09/06/2017 GRANTS.GOV Updates Federal Demonstration Partnership JAD Meeting Slide 2
GRANTS.GOV Updates Federal Demonstration Partnership Meeting Presented by Grants.gov September 7, 2017 RELEASE UPDATE 09/06/2017 GRANTS.GOV Updates Federal Demonstration Partnership JAD Meeting Slide 2
A Bigger Bang Patient Portal Strategy: How we activated 100K patients in our First Year
 A Bigger Bang Patient Portal Strategy: How we activated 100K patients in our First Year Saturday March 25 th, 2017 Lindsay Altimare, MPA Director, LVPG Operations Lehigh Valley Health Network Michael Sheinberg,
A Bigger Bang Patient Portal Strategy: How we activated 100K patients in our First Year Saturday March 25 th, 2017 Lindsay Altimare, MPA Director, LVPG Operations Lehigh Valley Health Network Michael Sheinberg,
Greetings from Michelle & Katie QUALITY IMPROVEMENT DIVISION OF HOSPITAL MEDICINE
 IN THIS ISSUE: Create Raving Fans of Your Idea P. 1 Where is our waste? P. 1 Sepsis Update P. 3 Quality Updates P. 4 APeX quality tips P.5 Division Incentive Metrics P. 6 Focus Group Findings P. 2 The
IN THIS ISSUE: Create Raving Fans of Your Idea P. 1 Where is our waste? P. 1 Sepsis Update P. 3 Quality Updates P. 4 APeX quality tips P.5 Division Incentive Metrics P. 6 Focus Group Findings P. 2 The
Criteria Led Discharge Pilot NHS Ayrshire and Arran Lorna Loudon, Linsey Stobo, Fraser Doris Implementing CLD in Scotland
 Criteria Led Discharge Pilot NHS Ayrshire and Arran Lorna Loudon, Linsey Stobo, Fraser Doris Implementing CLD in Scotland 18.3.15 Whole System Patient Flow Improvement Programme 1 Background Project Team
Criteria Led Discharge Pilot NHS Ayrshire and Arran Lorna Loudon, Linsey Stobo, Fraser Doris Implementing CLD in Scotland 18.3.15 Whole System Patient Flow Improvement Programme 1 Background Project Team
Lean Six Sigma DMAIC Project (Example)
 Lean Six Sigma DMAIC Project (Example) Green Belt Project Objective: To Reduce Clinic Cycle Time (Intake & Service Delivery) Last Updated: 1 15 14 Team: The Speeders Tom Jones (Team Leader) Steve Martin
Lean Six Sigma DMAIC Project (Example) Green Belt Project Objective: To Reduce Clinic Cycle Time (Intake & Service Delivery) Last Updated: 1 15 14 Team: The Speeders Tom Jones (Team Leader) Steve Martin
Improving HCAHPS with a Culture of Quiet St. Francis Hospital (Puget Sound)
 Improving HCAHPS with a Culture of Quiet St. Francis Hospital (Puget Sound) Problem: Surveys showed that the noise level made it difficult for patients to rest. Innovation: Implemented a culture of quiet.
Improving HCAHPS with a Culture of Quiet St. Francis Hospital (Puget Sound) Problem: Surveys showed that the noise level made it difficult for patients to rest. Innovation: Implemented a culture of quiet.
Managing Receivables Through Patient Access Ingenuity
 Managing Receivables Through Patient Access Ingenuity Managing Receivables Through Patient Access Ingenuity About the Organization Cedars-Sinai Medical Center: 886 Licensed Beds in Beverly Hills, California
Managing Receivables Through Patient Access Ingenuity Managing Receivables Through Patient Access Ingenuity About the Organization Cedars-Sinai Medical Center: 886 Licensed Beds in Beverly Hills, California
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management
 PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability
 Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability How we improved Patient Safety and Quality Outcomes at Northwest Hospital Our Journey to Shared Accountability Implementation
Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability How we improved Patient Safety and Quality Outcomes at Northwest Hospital Our Journey to Shared Accountability Implementation
Quality Improvement Program Evaluation
 Quality Improvement Program Evaluation 2013 Care Wisconsin 2013 Quality Improvement Program Evaluation INTRODUCTION Care Wisconsin s Quality Management Program uses the Home and Community-Based Quality
Quality Improvement Program Evaluation 2013 Care Wisconsin 2013 Quality Improvement Program Evaluation INTRODUCTION Care Wisconsin s Quality Management Program uses the Home and Community-Based Quality
Harm Across the Board Reporting: How your Hospital Can Get There
 Harm Across the Board Reporting: How your Hospital Can Get There Presentation to KHA Annual Quality Conference March 19, 2014 Jackie Conrad RN, BSN, MBA Improvement Advisor Cynosure Health Objectives Upon
Harm Across the Board Reporting: How your Hospital Can Get There Presentation to KHA Annual Quality Conference March 19, 2014 Jackie Conrad RN, BSN, MBA Improvement Advisor Cynosure Health Objectives Upon
Quality Improvement Medication Reconciliation Tools, Techniques and Tales
 Quality Improvement Medication Reconciliation Tools, Techniques and Tales Presented by: Marsha Nicholson, Steve Scott, City of Toronto Long-Term Care Homes and Services Division January 10, 2012 Outline
Quality Improvement Medication Reconciliation Tools, Techniques and Tales Presented by: Marsha Nicholson, Steve Scott, City of Toronto Long-Term Care Homes and Services Division January 10, 2012 Outline
Presentation Outline
 Chronic Disease Toolkits: Spreading Quality Outcomes Simply Gerald H. Angoff, MD, FACC, MBA Steve Sarette, BA Presentation Outline It Introduction ti Setting the scene Quality Improvement Project Details
Chronic Disease Toolkits: Spreading Quality Outcomes Simply Gerald H. Angoff, MD, FACC, MBA Steve Sarette, BA Presentation Outline It Introduction ti Setting the scene Quality Improvement Project Details
Enhancing Communication Skills: A Catalyst for Organizational Cultural Transformation Presented by William Maples, MD, Chief Medical Officer,
 Enhancing Communication Skills: A Catalyst for Organizational Cultural Transformation Presented by William Maples, MD, Chief Medical Officer, Professional Research Consultants and Executive Director, The
Enhancing Communication Skills: A Catalyst for Organizational Cultural Transformation Presented by William Maples, MD, Chief Medical Officer, Professional Research Consultants and Executive Director, The
7-8 September 2016 Sheraton Hotel & Towers Ho Chi Minh City, Vietnam
 7-8 September 2016 Sheraton Hotel & Towers Ho Chi Minh City, Vietnam www.hospitalmanagementasia.com 2 Empower Hospital Quality Culture through Accreditation About Vinmec Mission To deliver world class
7-8 September 2016 Sheraton Hotel & Towers Ho Chi Minh City, Vietnam www.hospitalmanagementasia.com 2 Empower Hospital Quality Culture through Accreditation About Vinmec Mission To deliver world class
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH
 IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
The Case for Optimal Staffing: A Call to Action
 The Case for Optimal Staffing: A Call to Action 2015 ANCC National Magnet Conference October 7, 2015 2:30 3:30pm Session C721 Mary Jo Assi, DNP, RN, NEA BC, FNP BC Director of Nursing Practice and Work
The Case for Optimal Staffing: A Call to Action 2015 ANCC National Magnet Conference October 7, 2015 2:30 3:30pm Session C721 Mary Jo Assi, DNP, RN, NEA BC, FNP BC Director of Nursing Practice and Work
Julie Kelley, MSW, MPH Program Chief, Mental Heath/Psychiatry Contra Costa Regional Medical Center Martinez, CA
 Julie Kelley, MSW, MPH Program Chief, Mental Heath/Psychiatry Contra Costa Regional Medical Center Martinez, CA Patients and Families as Care Partners April 20, 2011 Little about us Contra Costa Regional
Julie Kelley, MSW, MPH Program Chief, Mental Heath/Psychiatry Contra Costa Regional Medical Center Martinez, CA Patients and Families as Care Partners April 20, 2011 Little about us Contra Costa Regional
Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going?
 Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going? David Rogers Assistant Deputy Secretary for Medicaid Operations Agency for Health Care Administration 2016
Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going? David Rogers Assistant Deputy Secretary for Medicaid Operations Agency for Health Care Administration 2016
Patient-Centered LOS Reduction Initiative Improves Outcomes, Lowers Costs
 Success Story Patient-Centered LOS Reduction Initiative Improves Outcomes, Lowers Costs EXECUTIVE SUMMARY U.S. hospital stays cost the health system at least $377.5 billion per year. In today s value-based
Success Story Patient-Centered LOS Reduction Initiative Improves Outcomes, Lowers Costs EXECUTIVE SUMMARY U.S. hospital stays cost the health system at least $377.5 billion per year. In today s value-based
PPI Deprescribing: Ascension
 PPI Deprescribing: Ascension Tonya Thomas, PharmD Clinical Pharmacist Saint Thomas West Hospital Nashville, TN, USA #derx2018 Session resources will be available at deprescribing.org/resources Learning
PPI Deprescribing: Ascension Tonya Thomas, PharmD Clinical Pharmacist Saint Thomas West Hospital Nashville, TN, USA #derx2018 Session resources will be available at deprescribing.org/resources Learning
StepWise Approach To Quality In Health Service Delivery-SafeCare. IHI Africa Forum February 2018
 StepWise Approach To Quality In Health Service Delivery-SafeCare IHI Africa Forum February 2018 Quality of care in resource-restricted settings Gaps and challenges Licensing not enforced due to limited
StepWise Approach To Quality In Health Service Delivery-SafeCare IHI Africa Forum February 2018 Quality of care in resource-restricted settings Gaps and challenges Licensing not enforced due to limited
Implementation Assessment: Quantitative Interview
 CUSP 4 MVP VAP Improving Care for Mechancially Ventilated Patients Implementation Assessment: Quantitative Interview ICU Unit Type: Hospital Name: Interview Date: Interviewer Name: Section 1: Staff Safety
CUSP 4 MVP VAP Improving Care for Mechancially Ventilated Patients Implementation Assessment: Quantitative Interview ICU Unit Type: Hospital Name: Interview Date: Interviewer Name: Section 1: Staff Safety
A Multi-Phased Approach to Using Clinical Data to Drive Evidence-Based EMR Redesign. Kulik, Carole Marie; Foad, Wendy; Brown, Gretchen
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
of the respiratory checklist from July1, April 30, Measures were evaluated monthly. Primary measures:
 Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
Driving High-Value Care via Clinical Pathways. Andrew Buchert, MD Gabriella Butler, MSN, RN
 Driving High-Value Care via Clinical Pathways Andrew Buchert, MD Gabriella Butler, MSN, RN 1 Andrew Buchert, MD Medical Director, Clinical Resource Management Children s Hospital of Pittsburgh of UPMC
Driving High-Value Care via Clinical Pathways Andrew Buchert, MD Gabriella Butler, MSN, RN 1 Andrew Buchert, MD Medical Director, Clinical Resource Management Children s Hospital of Pittsburgh of UPMC
FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018
 FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018 Agenda FHA MTC Call to Action for IVAC Data Review HRET HIIN Hospital Peer Sharing
FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018 Agenda FHA MTC Call to Action for IVAC Data Review HRET HIIN Hospital Peer Sharing
Ensuring quality outcomes
 Annual integrated report 20 64 Ensuring quality outcomes Over the past five years we have built an integrated quality management system that drives quality improvement across all Netcare divisions. More
Annual integrated report 20 64 Ensuring quality outcomes Over the past five years we have built an integrated quality management system that drives quality improvement across all Netcare divisions. More
Re-Engineering Medication Processes to Capitalize on Technology. Jane Englebright, PhD, RN Vice President, Quality HCA
 Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
SFGH. Management System. Components. SFGH Management System. Improvement. Time. Strategic Planning True North. Value Streams: Rapid Improvement Events
 SFGH Management System 1 SFGH Management System Components Strategic Planning True North Improvement Management System Value Streams: Rapid Improvement Events Time 2 1 Refining our Strategic Planning PATIENT
SFGH Management System 1 SFGH Management System Components Strategic Planning True North Improvement Management System Value Streams: Rapid Improvement Events Time 2 1 Refining our Strategic Planning PATIENT
The Four Pillars of Ambulatory Care Management - Transforming the Ambulatory Operational Framework
 The Four Pillars of Ambulatory Care Management - Transforming the Ambulatory Operational Framework Institution: The Emory Clinic, Inc. Author/Co-author(s): Donald I. Brunn, Chief Operating Officer, The
The Four Pillars of Ambulatory Care Management - Transforming the Ambulatory Operational Framework Institution: The Emory Clinic, Inc. Author/Co-author(s): Donald I. Brunn, Chief Operating Officer, The
Kentucky Sepsis Summit. August 2016
 1 Kentucky Sepsis Summit August 2016 St. Elizabeth Healthcare About Us: - 7 facilities & over 1200 licensed beds - Serving the NKY/Cincinnati Region in: - Orthopedic Care - Heart and Vascular Institute
1 Kentucky Sepsis Summit August 2016 St. Elizabeth Healthcare About Us: - 7 facilities & over 1200 licensed beds - Serving the NKY/Cincinnati Region in: - Orthopedic Care - Heart and Vascular Institute
The STAAR Initiative
 The STAAR Initiative A quality effort at the heart of system redesign Amy E. Boutwell, MD, MPP The Center for Innovative Healthcare Strategies amy@innovativehealthcarestrategies.org Please note: Dr Boutwell
The STAAR Initiative A quality effort at the heart of system redesign Amy E. Boutwell, MD, MPP The Center for Innovative Healthcare Strategies amy@innovativehealthcarestrategies.org Please note: Dr Boutwell
L19: Improving Transitions from the Hospital to Post Acute Care Settings
 This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
Building Coordinated, Patient Centered Care Management Teams
 Building Coordinated, Patient Centered Care Management Teams Jim Barr, MD CMO/VP Physician Network Development Optimus Healthcare Partners ACO & VP of Medical Services Aveta Health Solutions MSO Patient
Building Coordinated, Patient Centered Care Management Teams Jim Barr, MD CMO/VP Physician Network Development Optimus Healthcare Partners ACO & VP of Medical Services Aveta Health Solutions MSO Patient
Improving the Delivery of Troponin Results to the Emergency Department using Lean Methodology
 Organization: Anne Arundel Medical Center Solution Title: Improving the Delivery of Troponin Results to the Emergency Department using Lean Methodology Program/Project Description, Including Goals: What
Organization: Anne Arundel Medical Center Solution Title: Improving the Delivery of Troponin Results to the Emergency Department using Lean Methodology Program/Project Description, Including Goals: What
Electronic Surgical Scheduling Improves Patient Safety and Productivity
 Electronic Surgical Scheduling Improves Patient Safety and Productivity Katrina Spears, MA, Manager Business & Informatics Surgical Services Lina Munoz, BSN, RN, CPAN Manger Presurgical Testing, PACU,
Electronic Surgical Scheduling Improves Patient Safety and Productivity Katrina Spears, MA, Manager Business & Informatics Surgical Services Lina Munoz, BSN, RN, CPAN Manger Presurgical Testing, PACU,
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation. April 4, :45 5:00 pm
 Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
8/31/2015. Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN
 Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN Nurse Staffing Core vs. Float Staff 30 years ago 20-10 years ago 5 yrs Prior
Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN Nurse Staffing Core vs. Float Staff 30 years ago 20-10 years ago 5 yrs Prior
QIO Care Transitions Activity: the Good News so far
 QIO Care Transitions Activity: the Good News so far Kim Irby, MPH; kirby@cfmc.org Senior Project Director Colorado Foundation for Medical Care www.cfmc.org/integratingcare This material was prepared by
QIO Care Transitions Activity: the Good News so far Kim Irby, MPH; kirby@cfmc.org Senior Project Director Colorado Foundation for Medical Care www.cfmc.org/integratingcare This material was prepared by
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario
 Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 3/31/2016 Holland Bloorview Kids Rehabilitation Hospital 1 Overview Holland Bloorview continues to lead pediatric rehabilitation
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 3/31/2016 Holland Bloorview Kids Rehabilitation Hospital 1 Overview Holland Bloorview continues to lead pediatric rehabilitation
CAMDEN CLARK MEDICAL CENTER:
 INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center
 Engaging the team: Steps to Reduce Complications Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center Safety
Engaging the team: Steps to Reduce Complications Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center Safety
Improving Clinical Flow ECHO Collaborative Change Package
 Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
PACT: The VA s Medical Home
 A5/B5 This presenter has nothing to disclose PACT: The VA s Medical Home What is working to change a big system Mike Davies, MD Director VA Systems Redesign Rich Stark, MD Director VA Primary Care Operations
A5/B5 This presenter has nothing to disclose PACT: The VA s Medical Home What is working to change a big system Mike Davies, MD Director VA Systems Redesign Rich Stark, MD Director VA Primary Care Operations
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience. Presented by: Fadwa Jabboury, RN, MSN
 Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
From Big Data to Big Knowledge Optimizing Medication Management
 From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
The influx of newly insured Californians through
 January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL
 Publication Year: 2004 BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL Summary: Cape Canaveral hospital implemented a streamlined bedside registration process in order to reduce the time patients spent waiting
Publication Year: 2004 BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL Summary: Cape Canaveral hospital implemented a streamlined bedside registration process in order to reduce the time patients spent waiting
Colorado Medical-Dental Integration Project (CO MDI)
 Colorado Medical-Dental Integration Project (CO MDI) Allison Cusick, MPA, CHES National Oral Health Conference April 2016 Colorado Medical-Dental Integration CO MDI Five-Year Initiative Launched in 2014
Colorado Medical-Dental Integration Project (CO MDI) Allison Cusick, MPA, CHES National Oral Health Conference April 2016 Colorado Medical-Dental Integration CO MDI Five-Year Initiative Launched in 2014
Mark Stagen Founder/CEO Emerald Health Services
 The Value Proposition of Nurse Staffing September 2011 Mark Stagen Founder/CEO Emerald Health Services Agenda Nurse Staffing Industry Update Improving revenue trends in healthcare staffing 100% Percentage
The Value Proposition of Nurse Staffing September 2011 Mark Stagen Founder/CEO Emerald Health Services Agenda Nurse Staffing Industry Update Improving revenue trends in healthcare staffing 100% Percentage
Preventing Health Care Associated Infections. PJ Brennan, MD Chief Medical Officer University of Pennsylvania Health System August 16, 2011.
 Preventing Health Care Associated Infections PJ Brennan, MD Chief Medical Officer University of Pennsylvania Health System August 16, 2011 Lind 2 Gaps in Knowldege? Pathogenesis Epidemiology Prevention
Preventing Health Care Associated Infections PJ Brennan, MD Chief Medical Officer University of Pennsylvania Health System August 16, 2011 Lind 2 Gaps in Knowldege? Pathogenesis Epidemiology Prevention
Elmhurst Memorial Healthcare Successfully Attests to Stage 1 Meaningful Use
 Welcome! Elmhurst Memorial Healthcare Successfully Attests to Stage 1 Meaningful Use Presented by: Larry Katzovitz & Judy Triano Elmhurst Memorial Healthcare Kay Jackson (978) 805-3104 Kay.Jackson@iatric.com
Welcome! Elmhurst Memorial Healthcare Successfully Attests to Stage 1 Meaningful Use Presented by: Larry Katzovitz & Judy Triano Elmhurst Memorial Healthcare Kay Jackson (978) 805-3104 Kay.Jackson@iatric.com
Roadmap to accountable care: The chicken or the egg technology investment or clinical process improvement?
 Roadmap to accountable care: The chicken or the egg technology investment or clinical process improvement? August 29, 2012 Meet the Presenters Michael Griffis CIO Innovative Practices Tucson, AZ Beth Hartquist,
Roadmap to accountable care: The chicken or the egg technology investment or clinical process improvement? August 29, 2012 Meet the Presenters Michael Griffis CIO Innovative Practices Tucson, AZ Beth Hartquist,
2017/18 Quality Improvement Plan Improvement Targets and Initiatives
 2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
University of Washington School of Nursing - Continuing Nursing Education 1
 A Team Approach to Patient Safety: TeamSTEPPS University of Washington Medical Center Kat Comstock, Associate Director Center for Clinical Excellence/Patient Safety Officer Describe TEAMSTEPPS using the
A Team Approach to Patient Safety: TeamSTEPPS University of Washington Medical Center Kat Comstock, Associate Director Center for Clinical Excellence/Patient Safety Officer Describe TEAMSTEPPS using the
Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections
 C10 This presenter has nothing to disclose Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections David Renfro, MS, RN NE BC Kelly Farnam, BSN, RN Gloria Martinez, MS, RN, NEA
C10 This presenter has nothing to disclose Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections David Renfro, MS, RN NE BC Kelly Farnam, BSN, RN Gloria Martinez, MS, RN, NEA
PERFORMANCE IMPROVEMENT REPORT
 PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
