Quality Improvement Program Evaluation
|
|
|
- Lorraine Hardy
- 6 years ago
- Views:
Transcription
1 Quality Improvement Program Evaluation 2013
2 Care Wisconsin 2013 Quality Improvement Program Evaluation INTRODUCTION Care Wisconsin s Quality Management Program uses the Home and Community-Based Quality Framework of Discovery, Remediation, and Continuous Improvement; and incorporates the Institute of Medicine s six aims for healthcare--safety, effectiveness, member-centeredness, timeliness, efficiency, and equitability. This document provides an evaluation of the 2013 Quality Management Program; identifying both strengths and opportunities. There are four sections in this report: Executive Summary - The accomplishments, a brief analysis, and challenges or next steps are identified for each area of focus in the 2013 Quality Improvement Work Plan. Quality Improvement Work Plan - Analysis of previous and on-going initiatives and how they shape the plan ahead. These are the seven areas of focus or domains that Care Wisconsin categorizes quality into: Member access Member-centered planning Member safeguards Member rights and responsibilities Provider access and capabilities Member outcomes System performance Annual Quality Review - The results of the 2013 Annual Quality Review completed by MetaStar to ensure our compliance with the Department of Health Services standards. Medicare Part C and D Star Measures - A review of Partnership 2013 Star Rating Care Wisconsin Quality Improvement Program Evaluation Page 1
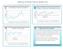
3 EXECUTIVE SUMMARY Member Access Both the Family Care and Partnership programs experienced census growth in Both programs exceeded budgeted census goals Care Wisconsin Total Census # Members End of Month Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov Dec Good Actual Budget Goal Stetch Goal Four initiatives took place in 2013 to support the strategic goal of assuring high performance in order to be the managed care organization of choice. These were (1) remain below 3 percent of the census permanently residing in a nursing home, (2) increase the use of self-directed supports, (3) reduce incidents during care transitions, and (4) reducing critical falls. The organizational strategic goal through 2018 is to achieve and maintain outstanding customer/member service and quality outcomes by (1) achieving and maintaining a 5 STAR rating for Medicare plan, (2) achieve high member/customer satisfaction, (3) achieve high quality member services through the development of programs that empower and support members, and (4) achieve care management excellence. Member-Centered Planning and Service Delivery Internal File Reviews The Internal File Review (IFR) Committee consists of senior management, front line providers and program management in both programs. A monthly score card is published to show findings from the previous month. Results are reviewed and focus is put on the indicators with low scores. Individual chart 2013 Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 2
4 reviews are shared with Program Managers who then discuss results with teams. In addition, scores are compared with AQR scores. MetaStar tended to score Care Wisconsin higher across all of the indicators except for Notices of Action sent when indicated and IDT follow up to ensure services are effective. Reasons for this are likely to be that Care Wisconsin reviews a much higher sample of charts than MetaStar. The 2014 DHS Corrective Action Plan will monitor notices of action sent when indicated and IDT follow up to ensure services are effective. Targeted training and intervention will be implemented to increase compliance. Member Centered Plan Timeliness The Member Centered Plan (MCP) is completed every six months with the member, and whomever they wish to include, and is focused on 12 quality of life domains. The team must review, revise, and obtain member signatures on MCPs every six months. Care Wisconsin monitors MCP timeliness on a monthly basis. Both Family Care and Partnership scored over 90 percent consistently in 2013 according to internal reports. However, results from the Annual Quality Review show that the timeliness of the most recent plan is much lower. This may be due to a much smaller sample size being reviewed for the quality review as opposed to Care Wisconsin s report, which pulls results for all members Challenges or Next Step Continue to monitor MCP signature dates to ensure contractual compliance with care plan timeliness. Member Safeguards The primary responsibility of the care team is to assure member safety. This is a routine part of their work in assessing, planning, and monitoring supports to meet member needs and outcomes. When risks are identified plans are developed to reduce them as much as possible, or in some cases, to develop risk agreements with members who exhibit particularly risky behavior and are unwilling to change. Incident Reporting. A robust incident reporting system is used to monitor critical incidents and adverse events. Critical incidents are reported in detail to the Department of Health Services each quarter. In-depth root cause analyses are completed for significant events. Almost eighty percent of the 686 incidents reported in 2013 were critical incidents. This is an increase in the rate per 50 members from the average in 2012, a continuing trend believed to be a result of better 2013 Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 3
5 reporting based on education provided in In both programs for 2013 there was a slight decline in the second quarter, a rise in the third, and a decline again in the fourth. Critical falls (with a fracture or head injury) were reported 232 times. Of the 78 incidents reported which occurred within 30 days of a care transition, the most common critical incident type was a fall. A care transition performance improvement project, started in 2012, is still ongoing and addressing this. In 2013 Care Wisconsin began monitoring fall assessment completion rates for critical falls. Modify the Program Manager s section on critical falls (used to help increase awareness of critical falls and falls assessment completion rate) Begin discussions on changing the process of collecting data to incorporate the transition to the new intranet and SharePoint. Use of Restrictive Measures The use of restraints or restrictive measures is only allowed when all other measures to keep members safe from themselves or to protect others have failed. The Restrictive Measures Committee approves the use of restrictive measures for members in the developmentally disabled target group before submitting the plan to the Department of Health Services for approval. In 2012 the committee began tracking data on renewal applications to determine how many were approved on the first submission to the State. In 2013 the committee began reviewing all upcoming renewals that were previously approved by the State. The restrictive measures database tracks and monitors the various categories of restraints and restrictive measures. Care Wisconsin has 20 members with medical restraints and 21 with restrictive measures. One restrictive measure was discontinued in 2013 due to non-use Challenges or Next Step The Restrictive Measures Committee Team Lead will continue to track restrictive measures and will evaluate more standardized oversight over medical restraints and restrictive measures in the physically disabled and frail elderly target groups. Member Rights and Responsibilities Grievances and Appeals The Member Rights Specialist works as a resource for members and teams in order to protect member rights and to preserve and develop relationships. Mediation skills are used to resolve member concerns whenever possible. When mediation fails grievances and appeals are encouraged. Appeals fell by about half from those reported the previous year, which made 2013 appeal numbers more consistent with those in The number of Notice of Actions (NOA) decreased by 36 percent from 2013 Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 4
6 those issued in Overall, about 6 percent of NOAs were appealed, which is fairly consistent with the 8 percent appealed in Partnership experienced an increase in the percentage of NOAs appealed, from 7 percent in 2012 to 18 percent in However, this 11 percent increase is caused by a significant drop in NOAs issued in 2013 (211) versus 2012 (977). The Partnership program restructured and reviewed care plans in 2012, which contributed to the higher number of NOAs issued that year. In Family Care the percentage of NOAs appealed decreased from 9 percent in 2012 to 4 percent in In contrast to Partnership, the number of NOAs issued in Family Care increased from 800 in 2012 to 923 in In 2013 the Quality Improvement Department continued to streamline processes, put data validation checks into place, and create process maps. Process maps were created for internal Medicaid appeals, expedited Medicaid appeals, appeals though the Division of Hearings and Appeals, level of care appeals, cost share appeals, room and board appeals, medication appeals, Medicare Part C and D appeals, and MetaStar investigations. Most of these appeal processes differ, so these maps will help Member Rights Specialists clearly explain the appeals process to members and teams. Continue efforts to increase the use of mediation in appeals Consistently and efficiently work through appeals and meet data reporting requirements Update Medicare Part C and D gap analysis and policies Member Advisory Committee Care Wisconsin met the goal, established in 2012, of having a Member Advisory Committee in each of the represented counties holding quarterly meetings. In one of those committees two counties (Sauk and Columbia) are both represented, bringing feedback from members in all ten original represented counties back to Care Wisconsin leadership. In 2013 the Member Advisory Committee meeting format became more focused and started discussing the same topics in the same quarter across all county committees. This enabled Care Wisconsin to obtain feedback from all of the counties at the same time on key agency issues to aid in decision-making and program and process improvements. Key topics for discussion based on organization strategic goals and initiatives were developed and will be discussed in 2014, including: strategic goals, member satisfaction, SDS (self directed services/supports), integrated employment, performance improvement projects, and member care plans. Following each quarter, the Member Rights Specialist will compile a report using the information from all the committee meetings summarizing the discussion on the key topics and providing recommendations from members to executive leadership staff Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 5
7 Executive leadership staff will review the report and make recommendations and decisions about ongoing projects and processes related to that topic. Member Advisory Committee members will receive written feedback each quarter indicating how their input was used in order to close the loop and continually show them the importance of their feedback. Provider Access and Capabilities Provider Quality Committee The Provider Quality Committee (PQC) charter is to assure that members receive high-quality care from providers and that care teams are supported in resolving quality of care issues that arise. This is accomplished by monitoring and discussing concerns initiated by care teams, the State, or the federal government regarding providers that currently serve members, or may potentially serve members, in order to assure that care is safe and appropriate. The Provider Quality Committee reviewed 33 providers (mostly residential) and there were eight site visits completed in All holds on admissions were at the same time as the state except for one where the committee kept the hold for an additional two weeks to ensure the Corrective Action Plan was implemented. The committee requested four Corrective Action Plans from residential providers and reviewed 22 Statement of Deficiencies during the year. A new policy and procedure was drafted for placing members in a residential facility with a No New Admit Order or in a Skilled Nursing Facility with a Discretionary Denial of Payments. A process for having the Provider Services Department follow up directly with providers to obtain State Rescind orders was developed. Continue to streamline PQC s review process Plan for expansion in Family Care and the addition of Medicaid SSI Member Outcomes Member Satisfaction The survey methodology was changed in 2013 to enable more timely and actionable data from a larger number of members. All members were given the opportunity to complete a satisfaction survey using the standard mail-in survey instrument for all managed care organizations. The surveys were mailed to members in the month following their MCP review so that members had a recent experience with the care team to rate their satisfaction on. Returned surveys were scanned into survey software and the results were analyzed on a monthly and annual basis Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 6
8 Member satisfaction data for 2013 shows improvement in satisfaction scores with both programs meeting or exceeding established goals. Changing the process for surveying member satisfaction increased both the number of surveys sent and those returned. In 2013 three times the number of surveys were returned than in With an increase in member satisfaction data and a continued focus on improving member satisfaction, Care Wisconsin was able to use the information gathered to develop new baselines and determine how best to move forward. A challenge for 2013 was to develop a strategic workgroup to focus on satisfaction results and implement a plan to make a positive impact on the results. The Member Satisfaction Strategic Team was formed, consisting of staff across the organization interested in improving member satisfaction. Customer service standards were created, reviewed by the Member Advisory Committee, and implemented. The Department of Health Services updated the annual 2014 member satisfaction survey resulting in changes that present a challenge in comparing satisfaction data year to year. Five key questions have been identified that can continue to be compared to past survey data to indicate how member satisfaction changes in Each program has a goal to achieve overall improved member satisfaction in the top box scores for these five key questions in 2014, which will be reviewed and re-evaluated midyear. HEDIS Partnership is a specific type of Medicare Advantage HMO called a Special Needs Plan (SNP) with two contracts one for Dane County and one for expansion counties. One of the requirements as a SNP is to report Health Effectiveness Data and Information Set (HEDIS) data to the Centers for Medicare and Medicaid. Care Wisconsin performed exceptionally well on HEDIS measures associated with Care of Older Adults and consistently above the Medicare mean for most other measures. One measure was not successfully reported: Call Center Timeliness-- due to insufficient data. This measure is being successfully reported in RY Challenges and Next Steps Design performance improvement projects that impact HEDIS measures with a focus on Star measures. Performance Improvement Projects Care Wisconsin is required to conduct two Performance Improvement Projects for the DHS contract (one with a long term care focus and one with an acute care focus) and two projects for CMS for the Partnership program (one with a hospital readmissions focus and one with a cardiovascular focus). Care Wisconsin s approach to these multiply projects is to align the topics with the contract requirements and organizational strategic goals. As a result, there are a total of three large-scale improvement projects that fulfill the requirements for both contracts and align with organizational goals. In 2013 Partnership 2013 Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 7
9 conducted a hospital readmissions project, a blood pressure project, and a care transitions project. Family Care conducted a care transitions project. Reducing hospital readmissions within 30 days Reducing critical incidents that occur within 30 days of a care transition= both programs are below their 2012 percentages which were Family Care=17% and Partnership=19%. Projects will be conducted using required protocols as per DHS and CMS contracts. Immunizations The Quality Improvement Department tracks influenza immunizations and pneumococcal pneumonia immunizations. The results are reported and validated as per contract with the Department of Health Services. Results in this report are from 2012 because measures are not calculated and submitted until March of the following year. Care Wisconsin immunization rates are in line with other Family Care and Partnership programs in Wisconsin and above the state average. Continue to monitor and evaluate the immunization reporting process. System Performance Utilization Management The purpose of the Utilization Management Program (a component of the Quality Management Program) is to monitor, evaluate, and manage resource allocation to: Avoid under- and over-utilization of services; Promote the provision of medically appropriate care; Monitor cost effectiveness and quality of services to ensure that services are appropriate, medically necessary and provided in a timely and resource efficient manner. This work is accomplished through a Utilization Management Committee that meets monthly to review key areas of both long term care and acute and primary healthcare utilization. Key focus areas for long term care were home care, home health care (skilled nursing), residential services, adult day services and vocational services. The acute and primary healthcare focus areas included hospitalizations, drug costs and generic drug usage. Reports are published monthly for Family Care and Partnership and posted on Care Wisconsin s intranet under Organizational Metrics. Most of the available data at this point 2013 Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 8
10 continue to be claims data, but work is continuing on the development of real time data that would be actionable more quickly was a year of stabilization in utilization of services. Sustainability initiatives had been addressed in 2012, and Care Wisconsin made significant changes in structure and careful review of services to assure members were receiving appropriate services in the right amount and in the most cost effective manner. Utilization patterns in 2013 for long term care services were favorable to budget in both programs. Hospitalization rates continue to be challenging, often due to the complexity of the population served; new strategies are continually being tested to reduce readmissions, a piece of the overall hospitalization rate issue. Most recently, support RNs are being deployed to work closely with local hospitals to begin transition planning at admission and to streamline communication for the hospital. Generic drug use and medication costs per member per month are favorable to targets. Annual Quality Review Annually, the Department of Health Services contracts with an external quality review organization, MetaStar, to perform an audit of the managed care organizations. The review is composed of three sections: (1) quality compliance review of structures and processes, (2) a care management review, and (3) a performance improvement projects review was a targeted review year which means that MetaStar only reviewed compliance standards that were not fully met in the 2012 review. Care Wisconsin changed three of five standards from partially met to met for an overall compliance rate of 96 percent. Since last year, Care Wisconsin made progress in all two of the three review areas: Quality Compliance Review, Care Management Review, and Performance Improvement Projects. Fully met three of the five Quality Compliance Review (QCR) standards that were partially met in last year s review. Overall rate of compliance was 96.2 percent for FY and 90.6 percent for FY Partnership improved its results for 7 Care Management Review (CMR) standards, and scored 90 percent or higher for 10 of the 14 standards. Family Care improved its results for four CMR standards and scored 90 percent or higher for eight standards. Continues to demonstrate sound methodology when implementing Performance Improvement Projects. Increase compliance scores for all partially met standards of the annual quality review to achieve a met status Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 9
11 Medicare Part C and D Star Measure Ratings Star ratings are used to establish quality bonuses and by consumers to compare health plans. They are a combination of results from HEDIS, Health Outcomes Survey (HOS), and Consumer Assessment of Healthcare Providers and Systems (CAHPS) and administrative data. Health plans that have overall ratings of four or more receive quality bonus payments to reward and incentivize quality. Care Wisconsin received a CMS star rating of 3-1/2 stars. Star Steering Committee will evaluate the Star rating process and develop sound methodology for increasing overall Star rating to minimum of four Stars in Care Wisconsin Quality Improvement Evaluation - Executive Summary Page 10
Quality Management Report 2017 Q2
 Quality Management Report 2017 Q2 Quality Management Program CMS STAR Ratings Member Satisfaction (CAHPS & HOS) HEDIS Risk Adjustment DHS Member Incident Reporting Member Satisfaction Surveys Pay for Performance
Quality Management Report 2017 Q2 Quality Management Program CMS STAR Ratings Member Satisfaction (CAHPS & HOS) HEDIS Risk Adjustment DHS Member Incident Reporting Member Satisfaction Surveys Pay for Performance
SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015
 SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training for our Special Needs Plan at Care Wisconsin.
SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training for our Special Needs Plan at Care Wisconsin.
Quality Management Report 2017 Q4
 Quality Management Report 2017 Q4 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels. These activities include: CMS DHS DHS & CMS HEDIS Member Satisfaction (CAHPS
Quality Management Report 2017 Q4 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels. These activities include: CMS DHS DHS & CMS HEDIS Member Satisfaction (CAHPS
Quality Management Report 2018 Q1
 Quality Management Report 2018 Q1 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels These activities include: Centers for Medicare & Medicaid Services (CMS) Department
Quality Management Report 2018 Q1 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels These activities include: Centers for Medicare & Medicaid Services (CMS) Department
2019 Quality Improvement Program Description Overview
 2019 Quality Improvement Program Description Overview Introduction Eon/Clear Spring s Quality Improvement (QI) program guides the company s activities to improve care and treatment for the member s we
2019 Quality Improvement Program Description Overview Introduction Eon/Clear Spring s Quality Improvement (QI) program guides the company s activities to improve care and treatment for the member s we
Medicare Advantage Star Ratings
 Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going?
 Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going? David Rogers Assistant Deputy Secretary for Medicaid Operations Agency for Health Care Administration 2016
Lessons Learned from MLTSS Implementation in Florida Where Have We Been and Where Are We Going? David Rogers Assistant Deputy Secretary for Medicaid Operations Agency for Health Care Administration 2016
MACOMB COUNTY COMMUNITY MENTAL HEALTH QUALITY ASSESSMENT AND PERFORMANCE IMPROVEMENT PROGRAM ANNUAL EVALUATION, FISCAL YEAR 2009 ANNUAL PLAN, FISCAL
 MACOMB COUNTY COMMUNITY MENTAL HEALTH QUALITY ASSESSMENT AND PERFORMANCE IMPROVEMENT PROGRAM ANNUAL EVALUATION, FISCAL YEAR ANNUAL PLAN, FISCAL YEAR 2010 AUGUST, 2010 MACOMB COUNTY COMMUNITY MENTAL HEALTH
MACOMB COUNTY COMMUNITY MENTAL HEALTH QUALITY ASSESSMENT AND PERFORMANCE IMPROVEMENT PROGRAM ANNUAL EVALUATION, FISCAL YEAR ANNUAL PLAN, FISCAL YEAR 2010 AUGUST, 2010 MACOMB COUNTY COMMUNITY MENTAL HEALTH
COPPER COUNTRY MENTAL HEALTH SERVICES ANNUAL QUALITY IMPROVEMENT REPORT FY Introduction
 COPPER COUNTRY MENTAL HEALTH SERVICES ANNUAL QUALITY IMPROVEMENT REPORT FY 2017 Introduction Copper Country Mental Health Services (CCMHS) focuses on improving the quality of our services and identifying
COPPER COUNTRY MENTAL HEALTH SERVICES ANNUAL QUALITY IMPROVEMENT REPORT FY 2017 Introduction Copper Country Mental Health Services (CCMHS) focuses on improving the quality of our services and identifying
INSTITUTIONAL/INSTITUTIONAL EQUIVALENT (I/IESNP) DUAL SPECIAL NEEDS PLAN (DSNP) CHRONIC SPECIAL NEEDS PLAN (LSNP)
 SNP MODEL OF CARE ANNUAL EVALUATIONS FOR 2013 INSTITUTIONAL/INSTITUTIONAL EQUIVALENT (I/IESNP) DUAL SPECIAL NEEDS PLAN (DSNP) CHRONIC SPECIAL NEEDS PLAN (LSNP) 1 7 0 1 P O N C E D E L E O N B L V D, S
SNP MODEL OF CARE ANNUAL EVALUATIONS FOR 2013 INSTITUTIONAL/INSTITUTIONAL EQUIVALENT (I/IESNP) DUAL SPECIAL NEEDS PLAN (DSNP) CHRONIC SPECIAL NEEDS PLAN (LSNP) 1 7 0 1 P O N C E D E L E O N B L V D, S
PERFORMANCE IMPROVEMENT REPORT
 PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
COMMITTEE REPORTS TO THE BOARD
 Item # 9 F i COMMITTEE REPORTS TO THE BOARD To From South East LHIN Board Members Quality Committee Reviewed by Quality Committee Committee Members of the Committee were given the opportunity to review
Item # 9 F i COMMITTEE REPORTS TO THE BOARD To From South East LHIN Board Members Quality Committee Reviewed by Quality Committee Committee Members of the Committee were given the opportunity to review
Compliance Division Staff Report
 Compliance Division Staff Report Polygraph Advisory Board Meeting Tuesday, September 26, 2017 Public Outreach Compliance Division routinely attends annual industry meetings held by TALEPI (Texas Association
Compliance Division Staff Report Polygraph Advisory Board Meeting Tuesday, September 26, 2017 Public Outreach Compliance Division routinely attends annual industry meetings held by TALEPI (Texas Association
4/9/2016. The changing health care market THE CHANGING HEALTH CARE MARKET. CPAs & ADVISORS
 CPAs & ADVISORS experience support // ADVANCED PAYMENT MODELS: CJR Eric. M. Rogers MEd. RT(R) Managing Consultant The changing health care market THE CHANGING HEALTH CARE MARKET HHS goal of 30% of traditional
CPAs & ADVISORS experience support // ADVANCED PAYMENT MODELS: CJR Eric. M. Rogers MEd. RT(R) Managing Consultant The changing health care market THE CHANGING HEALTH CARE MARKET HHS goal of 30% of traditional
ACOs in 2012: ACO Activity Doubles in 12 Months
 Healthcare Benchmarks and Metrics July 2012 ACOs in 2012: ACO Activity Doubles in 12 Months www.hin.com The Healthcare Intelligence Network 800 State Highway 71, Suite 2 Sea Girt, NJ 08750 888-446-3530
Healthcare Benchmarks and Metrics July 2012 ACOs in 2012: ACO Activity Doubles in 12 Months www.hin.com The Healthcare Intelligence Network 800 State Highway 71, Suite 2 Sea Girt, NJ 08750 888-446-3530
3. What does Any Willing Provider (AWP) refer to in the context of MLTSS?
 Overview of Any Willing Qualified Provider (AWQP) Initiative 1. What is Any Willing Qualified Provider? The Any Willing Qualified Provider (AWQP) is a Department of Human Services (DHS) Nursing Facility
Overview of Any Willing Qualified Provider (AWQP) Initiative 1. What is Any Willing Qualified Provider? The Any Willing Qualified Provider (AWQP) is a Department of Human Services (DHS) Nursing Facility
Hospitalization Patterns for All Causes, CV Disease and Infections under the Old and New Bundled Payment System
 Hospitalization Patterns for All Causes, CV Disease and Infections under the Old and New Bundled Payment System Robert N Foley, MB, FRCPI, FRCPS United States Renal Data System Data Coordinating Center
Hospitalization Patterns for All Causes, CV Disease and Infections under the Old and New Bundled Payment System Robert N Foley, MB, FRCPI, FRCPS United States Renal Data System Data Coordinating Center
A. Encounter Data Submission Requirements
 A. Encounter Data Submission Requirements APPLIES TO: A. This policy applies to all IEHP Medi-Cal Providers. POLICY: A. As of October 1, 2015, IEHP has transitioned to ICD-10 diagnosis and procedure coding
A. Encounter Data Submission Requirements APPLIES TO: A. This policy applies to all IEHP Medi-Cal Providers. POLICY: A. As of October 1, 2015, IEHP has transitioned to ICD-10 diagnosis and procedure coding
Avoiding the Cap Trap What Every Hospice Needs to Know. Matthew Gordon, CPA Principal Consultant / Founder Cap Doctor Associates, Inc.
 Avoiding the Cap Trap What Every Hospice Needs to Know Matthew Gordon, CPA Principal Consultant / Founder Cap Doctor Associates, Inc. Overview 11% of hospices exceeded the cap in 2012 with an average overage
Avoiding the Cap Trap What Every Hospice Needs to Know Matthew Gordon, CPA Principal Consultant / Founder Cap Doctor Associates, Inc. Overview 11% of hospices exceeded the cap in 2012 with an average overage
Analysis of Incurred Claims Trend and Provider Payments
 Analysis of Incurred Claims Trend and Provider Payments Board of Trustees Meeting May 24, 2013 Presentation Overview Trends in Incurred Claims Paid through March 31, 2013 Per Member Per Month (PMPM) By
Analysis of Incurred Claims Trend and Provider Payments Board of Trustees Meeting May 24, 2013 Presentation Overview Trends in Incurred Claims Paid through March 31, 2013 Per Member Per Month (PMPM) By
Updates from CMS: Value-Based Purchasing, ACOs, and Other Initiatives The Seventh National Pay for Performance Summit March 20, 2012
 Updates from CMS: Value-Based Purchasing, ACOs, and Other Initiatives The Seventh National Pay for Performance Summit March 20, 2012 Presenters David Sayen, CMS Regional Administrator Betsy L. Thompson,
Updates from CMS: Value-Based Purchasing, ACOs, and Other Initiatives The Seventh National Pay for Performance Summit March 20, 2012 Presenters David Sayen, CMS Regional Administrator Betsy L. Thompson,
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation. April 4, :45 5:00 pm
 Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
Discharge and Follow-Up Planning. Presented by the Clinical and Quality Team
 Discharge and Follow-Up Planning Presented by the Clinical and Quality Team After today s training you will be able to: Identify and summarize important information about discharge planning Have adequate
Discharge and Follow-Up Planning Presented by the Clinical and Quality Team After today s training you will be able to: Identify and summarize important information about discharge planning Have adequate
Overview of Home Health Star Ratings
 Overview of Home Health Star Ratings September 23, 2015 Presented by: Liz Silva Deyta Analytics, a division of HEALTHCAREfirst Agenda Home Health Star Ratings Quality of Patient Care Star Rating Patient
Overview of Home Health Star Ratings September 23, 2015 Presented by: Liz Silva Deyta Analytics, a division of HEALTHCAREfirst Agenda Home Health Star Ratings Quality of Patient Care Star Rating Patient
Managing Healthcare Payment Opportunity Fundamentals CENTER FOR INDUSTRY TRANSFORMATION
 Managing Healthcare Payment Opportunity Fundamentals dhgllp.com/healthcare 4510 Cox Road, Suite 200 Glen Allen, VA 23060 Melinda Hancock PARTNER Melinda.Hancock@dhgllp.com 804.474.1249 Michael Strilesky
Managing Healthcare Payment Opportunity Fundamentals dhgllp.com/healthcare 4510 Cox Road, Suite 200 Glen Allen, VA 23060 Melinda Hancock PARTNER Melinda.Hancock@dhgllp.com 804.474.1249 Michael Strilesky
PEONIES Member Interviews. State Fiscal Year 2012 FINAL REPORT
 PEONIES Member Interviews State Fiscal Year 2012 FINAL REPORT Report prepared for the Wisconsin Department of Health Services Office of Family Care Expansion by Sara Karon, PhD, PEONIES Project Director
PEONIES Member Interviews State Fiscal Year 2012 FINAL REPORT Report prepared for the Wisconsin Department of Health Services Office of Family Care Expansion by Sara Karon, PhD, PEONIES Project Director
A Million Little Pieces: Developing a Controlled Substance Diversion Program. Tanya Y. Barnhart, PharmD, BCPS
 A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
Creating Data-driven Strategies to Improve Hospital Outcomes
 Annual National Institute October 16, 2014 Creating Data-driven Strategies to Improve Hospital Outcomes A Case Manager s Guide Information Data Knowledge 1 2014 Conifer Health Solutions, LLC. All Rights
Annual National Institute October 16, 2014 Creating Data-driven Strategies to Improve Hospital Outcomes A Case Manager s Guide Information Data Knowledge 1 2014 Conifer Health Solutions, LLC. All Rights
Winning at Care Coordination Using Data-Driven Partnerships
 Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November 2017
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD
 Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD Outline Quality Overview Overview and discussion of CMS programs Increasing transparency Move from P4R to P4P Expanding beyond
Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD Outline Quality Overview Overview and discussion of CMS programs Increasing transparency Move from P4R to P4P Expanding beyond
LESSONS LEARNED IN LENGTH OF STAY (LOS)
 FEBRUARY 2014 LESSONS LEARNED IN LENGTH OF STAY (LOS) USING ANALYTICS & KEY BEST PRACTICES TO DRIVE IMPROVEMENT Overview Healthcare systems will greatly enhance their financial status with a renewed focus
FEBRUARY 2014 LESSONS LEARNED IN LENGTH OF STAY (LOS) USING ANALYTICS & KEY BEST PRACTICES TO DRIVE IMPROVEMENT Overview Healthcare systems will greatly enhance their financial status with a renewed focus
Advancing Accountability for Improving HCAHPS at Ingalls
 iround for Patient Experience Advancing Accountability for Improving HCAHPS at Ingalls A Case Study Webconference 2 Managing your audio Use Telephone If you select the use telephone option please dial
iround for Patient Experience Advancing Accountability for Improving HCAHPS at Ingalls A Case Study Webconference 2 Managing your audio Use Telephone If you select the use telephone option please dial
JMOC Update: Behavioral Health Redesign. March 16 th, 2017
 JMOC Update: Behavioral Health Redesign March 16 th, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy to rebuild
JMOC Update: Behavioral Health Redesign March 16 th, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy to rebuild
NURSING FACILITY ASSESSMENTS
 Department of Health and Human Services OFFICE OF INSPECTOR GENERAL NURSING FACILITY ASSESSMENTS AND CARE PLANS FOR RESIDENTS RECEIVING ATYPICAL ANTIPSYCHOTIC DRUGS Daniel R. Levinson Inspector General
Department of Health and Human Services OFFICE OF INSPECTOR GENERAL NURSING FACILITY ASSESSMENTS AND CARE PLANS FOR RESIDENTS RECEIVING ATYPICAL ANTIPSYCHOTIC DRUGS Daniel R. Levinson Inspector General
L19: Improving Transitions from the Hospital to Post Acute Care Settings
 This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
NHS Ayrshire & Arran Adverse Event Management: Review of Documentation Supplementary Information Requested by NHS Ayrshire & Arran
 NHS Ayrshire & Arran Adverse Event Management: Review of Documentation Supplementary Information Requested by NHS Ayrshire & Arran April 2013 Background In February 2012, the Scottish Information Commissioner
NHS Ayrshire & Arran Adverse Event Management: Review of Documentation Supplementary Information Requested by NHS Ayrshire & Arran April 2013 Background In February 2012, the Scottish Information Commissioner
The Triple Aim. Productivity: Digging Deep Enough 11/4/2013. quality and satisfaction); Improving the health of populations; and
 NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
Handling Organisational Complaints
 Council meeting 12 January 2012 Public business Handling Organisational Complaints Purpose To report to the Council on the handling of organisational complaints for the period 27 September 2010 to 30 September
Council meeting 12 January 2012 Public business Handling Organisational Complaints Purpose To report to the Council on the handling of organisational complaints for the period 27 September 2010 to 30 September
State FY2013 Hospital Pay-for-Performance (P4P) Guide
 State FY2013 Hospital Pay-for-Performance (P4P) Guide Table of Contents 1. Overview...2 2. Measures...2 3. SFY 2013 Timeline...2 4. Methodology...2 5. Data submission and validation...2 6. Communication,
State FY2013 Hospital Pay-for-Performance (P4P) Guide Table of Contents 1. Overview...2 2. Measures...2 3. SFY 2013 Timeline...2 4. Methodology...2 5. Data submission and validation...2 6. Communication,
Infection Control Quality Assurance & Performance Improvement (QAPI) Case Study Scenario 1: Following Quality Assurance (QA)
 Infection Control Quality Assurance & Performance Improvement (QAPI) Case Study Scenario 1: Following Quality Assurance (QA) The Facility Starview Convalescent Center is a 60-bed long-term care facility.
Infection Control Quality Assurance & Performance Improvement (QAPI) Case Study Scenario 1: Following Quality Assurance (QA) The Facility Starview Convalescent Center is a 60-bed long-term care facility.
Driving Quality Improvement in Managed Care. Toby Douglas, Director California Department of Health Care Services
 1 Driving Quality Improvement in Managed Care Toby Douglas, Director 2 Presentation Overview 1. Background on California s Medicaid Program (Medi-Cal) 2. California s Quality Improvement Focuses 3. Challenges
1 Driving Quality Improvement in Managed Care Toby Douglas, Director 2 Presentation Overview 1. Background on California s Medicaid Program (Medi-Cal) 2. California s Quality Improvement Focuses 3. Challenges
National Council on Disability
 An independent federal agency making recommendations to the President and Congress to enhance the quality of life for all Americans with disabilities and their families. Analysis and Recommendations for
An independent federal agency making recommendations to the President and Congress to enhance the quality of life for all Americans with disabilities and their families. Analysis and Recommendations for
Influence of Patient Flow on Quality Care
 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
National Trends Winter 2016
 National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
Medicare Value Based Purchasing Overview
 Medicare Value Based Purchasing Overview South Carolina Hospital Association DataGen Susan McDonough Bill Shyne October 29, 2015 Today s Objectives Overview of Medicare Value Based Purchasing Program Review
Medicare Value Based Purchasing Overview South Carolina Hospital Association DataGen Susan McDonough Bill Shyne October 29, 2015 Today s Objectives Overview of Medicare Value Based Purchasing Program Review
Tina Nelson, MBA, BSN Lisa Stepp, BSN, RN Rebecca Fyffe, BSN, RN Jessica Coughenour, LPN
 Establishing a Conservative Approach to the Prevention of Pressure Ulcers with the Utilization of Data Analytics to Monitor Effectiveness of Quality Efforts and Best Practice Models Tina Nelson, MBA, BSN
Establishing a Conservative Approach to the Prevention of Pressure Ulcers with the Utilization of Data Analytics to Monitor Effectiveness of Quality Efforts and Best Practice Models Tina Nelson, MBA, BSN
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM QI PROGRAM PURPOSE The Physicians Plus Quality Improvement Program is member-centric. It is designed to deliver safe and effective medical and behavioral healthcare, at the
QUALITY IMPROVEMENT PROGRAM QI PROGRAM PURPOSE The Physicians Plus Quality Improvement Program is member-centric. It is designed to deliver safe and effective medical and behavioral healthcare, at the
Collaboration Between Radiology and Utilization Management to Reduce Inappropriate MRI Orders and Patient Wait Times. Problem/Goal
 Collaboration Between Radiology and Utilization Management to Reduce Inappropriate MRI Orders and Patient Wait Times A. Chang, C. Hyun, N. Mehta, S. Kim, M. Grube, M. Blair, A. Yi VA Loma Linda Healthcare
Collaboration Between Radiology and Utilization Management to Reduce Inappropriate MRI Orders and Patient Wait Times A. Chang, C. Hyun, N. Mehta, S. Kim, M. Grube, M. Blair, A. Yi VA Loma Linda Healthcare
Executive Summary MEDICARE FEE-FOR-SERVICE (FFS) HOSPITAL READMISSIONS: QUARTER 4 (Q4) 2012 Q STATE OF CALIFORNIA
 MEDICARE FEE-FOR-SERVICE (FFS) HOSPITAL READMISSIONS: QUARTER 4 (Q4) 2012 Q3 2013 Executive Summary STATE OF CALIFORNIA The Centers for Medicare & Medicaid Services (CMS) has tasked Health Services Advisory
MEDICARE FEE-FOR-SERVICE (FFS) HOSPITAL READMISSIONS: QUARTER 4 (Q4) 2012 Q3 2013 Executive Summary STATE OF CALIFORNIA The Centers for Medicare & Medicaid Services (CMS) has tasked Health Services Advisory
Inland Empire Health Plan Quality Management Program Description Date: April, 2017
 Inland Empire Health Plan Quality Management Program Description Date: April, 2017 Page 1 of 35 Table of Contents Introduction.....3 Mission and Vision........3 Section 1: QM Program Overview........4
Inland Empire Health Plan Quality Management Program Description Date: April, 2017 Page 1 of 35 Table of Contents Introduction.....3 Mission and Vision........3 Section 1: QM Program Overview........4
JANUARY 2018 (21 work days) FEBRUARY 2018 (19 work days)
 AND CORRESPONDING DATES FOR JANUARY AND FEBRUARY 2018 JANUARY 2018 ( work days) Deadline* 12-27 12-28 12-29 1-2 1-3 1-4 1-5 1-8 1-9 1-10 Benefit Hold ** 12-28 12-29 1-2 1-3 1-4 1-5 1-8 1-9 1-10 1-11 Mailing
AND CORRESPONDING DATES FOR JANUARY AND FEBRUARY 2018 JANUARY 2018 ( work days) Deadline* 12-27 12-28 12-29 1-2 1-3 1-4 1-5 1-8 1-9 1-10 Benefit Hold ** 12-28 12-29 1-2 1-3 1-4 1-5 1-8 1-9 1-10 1-11 Mailing
From EHR Implementation to Attestation: Auditing and Monitoring Meaningful Use
 From EHR Implementation to Attestation: Auditing and Monitoring Meaningful Use Donna M. Abbondandolo, MBA, CHC, CPHQ, RHIA, CCS, CPC AVP of Compliance Laura Massa, RHIA, CCS, CTR Compliance Data Specialist
From EHR Implementation to Attestation: Auditing and Monitoring Meaningful Use Donna M. Abbondandolo, MBA, CHC, CPHQ, RHIA, CCS, CPC AVP of Compliance Laura Massa, RHIA, CCS, CTR Compliance Data Specialist
Influence of Patient Flow on Quality Care
 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
QIO Care Transitions Activity: the Good News so far
 QIO Care Transitions Activity: the Good News so far Kim Irby, MPH; kirby@cfmc.org Senior Project Director Colorado Foundation for Medical Care www.cfmc.org/integratingcare This material was prepared by
QIO Care Transitions Activity: the Good News so far Kim Irby, MPH; kirby@cfmc.org Senior Project Director Colorado Foundation for Medical Care www.cfmc.org/integratingcare This material was prepared by
State advocacy roadmap: Medicaid access monitoring review plans
 State advocacy roadmap: Medicaid access monitoring review plans Background Federal Medicaid law requires states to ensure Medicaid beneficiaries are able to access the healthcare providers they need through
State advocacy roadmap: Medicaid access monitoring review plans Background Federal Medicaid law requires states to ensure Medicaid beneficiaries are able to access the healthcare providers they need through
ACOs, CCOs: Challenges & Opportunities. Speakers. Case Study of Oregon 3/7/2014. Chris Apgar. Dick Sabath. Dawn Bonder
 s, CCOs: Challenges & Opportunities 2014 Compliance Institute Wednesday, April 2 San Diego, CA Speakers Chris Apgar CEO and President, Apgar and Associates, LLC Dick Sabath Compliance Officer, Trillium
s, CCOs: Challenges & Opportunities 2014 Compliance Institute Wednesday, April 2 San Diego, CA Speakers Chris Apgar CEO and President, Apgar and Associates, LLC Dick Sabath Compliance Officer, Trillium
Key Performance Indicators
 Regional Nephrology System (RNS) Chronic Disease Prevention and Management Key Performance Indicators 8/9 Fiscal Year End Report Version: 1. Date published: April 7th, 9 Created by: Ethel Doyle: RNS Interim
Regional Nephrology System (RNS) Chronic Disease Prevention and Management Key Performance Indicators 8/9 Fiscal Year End Report Version: 1. Date published: April 7th, 9 Created by: Ethel Doyle: RNS Interim
Medicare / Accountable Care Organization CHS Finance Division CPE Day November 2, 2015
 Medicare / Accountable Care Organization CHS Finance Division CPE Day November 2, 2015 Steve Neorr Chief Administrative Officer, Triad HealthCare Network Jeff Jones Chief Financial Officer, Cone Health
Medicare / Accountable Care Organization CHS Finance Division CPE Day November 2, 2015 Steve Neorr Chief Administrative Officer, Triad HealthCare Network Jeff Jones Chief Financial Officer, Cone Health
2014 QAPI Plan for [Facility Name]
![2014 QAPI Plan for [Facility Name] 2014 QAPI Plan for [Facility Name]](/thumbs/74/70066237.jpg) presented by: Quality Leadership for Long-Term Care 2014 QAPI Plan for [Facility Name] Vision A vision statement is sometimes called a picture of your organization in the future; it is your inspiration
presented by: Quality Leadership for Long-Term Care 2014 QAPI Plan for [Facility Name] Vision A vision statement is sometimes called a picture of your organization in the future; it is your inspiration
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
CHC-A Continuity Dashboard. All Sites Continuity - Asthma. 2nd Qtr-03. 2nd Qtr-04. 2nd Qtr-06. 4th Qtr-03. 4th Qtr-06. 3rd Qtr-04.
 PPC1: ACCESS AND COMMUNICATION Element B: Access and Communication Results Item 1: Visits with assigned PCP Continuity data is reviewed each month at our Office Redesign Committee (ORDC). The data is collected
PPC1: ACCESS AND COMMUNICATION Element B: Access and Communication Results Item 1: Visits with assigned PCP Continuity data is reviewed each month at our Office Redesign Committee (ORDC). The data is collected
2ab and 3cd. BTS Topic Selection:
 2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
Identifying Errors: A Case for Medication Reconciliation Technicians
 Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
HCAHPS. Presented by: Bill Sexton. Proudly recognized as one of the Nation s Top 100 Critical Access Hospitals - ivantage Health Analytics
 HCAHPS Presented by: Bill Sexton HCAHPS results will impact your organization's reimbursement in the era of health care reform HCAPHS results are a quality metric, not just a patient satisfaction metric
HCAHPS Presented by: Bill Sexton HCAHPS results will impact your organization's reimbursement in the era of health care reform HCAPHS results are a quality metric, not just a patient satisfaction metric
2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary
 2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary Jai Medical Systems Managed Care Organization, Inc. (JMS) and its providers have closed out their fifteenth full year in the Maryland Medicaid HealthChoice
2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary Jai Medical Systems Managed Care Organization, Inc. (JMS) and its providers have closed out their fifteenth full year in the Maryland Medicaid HealthChoice
HMO Value & Quality Roadmap for Wisconsin Medicaid. Rachel Currans-Henry Director Medicaid Bureau of Benefits Management August 8, 2017
 HMO Value & Quality Roadmap for Wisconsin Medicaid Rachel Currans-Henry Director Medicaid Bureau of Benefits Management August 8, 2017 1 Agenda A. Background B. Quality Roadmap C. 2018 SSI Managed Care
HMO Value & Quality Roadmap for Wisconsin Medicaid Rachel Currans-Henry Director Medicaid Bureau of Benefits Management August 8, 2017 1 Agenda A. Background B. Quality Roadmap C. 2018 SSI Managed Care
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs
 Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs Fourth Quarter Fiscal Year 2016-17 (April, May, June) Submitted August 1, 2017 Barbara Palmer Director
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs Fourth Quarter Fiscal Year 2016-17 (April, May, June) Submitted August 1, 2017 Barbara Palmer Director
Quality Improvement Work Plan
 NEVADA County Behavioral Health Quality Improvement Work Plan Fiscal Year 2016-2017 Table of Contents I. Quality Improvement Program Overview...1 A. Quality Improvement Program Characteristics...1 B. Annual
NEVADA County Behavioral Health Quality Improvement Work Plan Fiscal Year 2016-2017 Table of Contents I. Quality Improvement Program Overview...1 A. Quality Improvement Program Characteristics...1 B. Annual
Westchester Medical Center PPS Project Advisory Committee. April 15, 2015 Via Webinar: 10:00 am 11:30 am
 Westchester Medical Center PPS Project Advisory Committee April 15, 2015 Via Webinar: 10:00 am 11:30 am Agenda Discussion Topic Welcome & Status Update Finalizing the Implementation Plan DSRIP Year 1:
Westchester Medical Center PPS Project Advisory Committee April 15, 2015 Via Webinar: 10:00 am 11:30 am Agenda Discussion Topic Welcome & Status Update Finalizing the Implementation Plan DSRIP Year 1:
Performance Measurement Work Group Meeting 10/18/2017
 Performance Measurement Work Group Meeting 10/18/2017 Welcome to New Members QBR RY 2020 DRAFT QBR Policy Components QBR Program RY 2020 Snapshot QBR Consists of 3 Domains: Person and Community Engagement
Performance Measurement Work Group Meeting 10/18/2017 Welcome to New Members QBR RY 2020 DRAFT QBR Policy Components QBR Program RY 2020 Snapshot QBR Consists of 3 Domains: Person and Community Engagement
Emergency Department Throughput
 Emergency Department Throughput Patient Safety Quality Improvement Patient Experience Affordability Hoag Memorial Hospital Presbyterian One Hoag Drive Newport Beach, CA 92663 www.hoag.org Program Managers:
Emergency Department Throughput Patient Safety Quality Improvement Patient Experience Affordability Hoag Memorial Hospital Presbyterian One Hoag Drive Newport Beach, CA 92663 www.hoag.org Program Managers:
Emergency Department Waiting Times
 Publication Report Emergency Department Waiting Times (formerly Accident & Emergency Waiting Times) Quarter ending 30 June 2011 Publication date 30 August 2011 A National Statistics Publication for Scotland
Publication Report Emergency Department Waiting Times (formerly Accident & Emergency Waiting Times) Quarter ending 30 June 2011 Publication date 30 August 2011 A National Statistics Publication for Scotland
HSAG the QIN-QIO NHQCC II and CDI Initiative Kick-off
 (HSAG) the Quality Innovation Network-Quality Improvement Organization Ohio National Nursing Home Quality Care Collaborative II (NHQCC II) Introduction James H. Barnhart III, BSH, LNHA Quality Improvement
(HSAG) the Quality Innovation Network-Quality Improvement Organization Ohio National Nursing Home Quality Care Collaborative II (NHQCC II) Introduction James H. Barnhart III, BSH, LNHA Quality Improvement
2006 Annual Technical Report
 An independent external quality review of the Minnesota publicly funded managed care programs in accordance with the Balanced Budget Act of 1997 Presented by MPRO October 2007 2006 Annual Technical Report
An independent external quality review of the Minnesota publicly funded managed care programs in accordance with the Balanced Budget Act of 1997 Presented by MPRO October 2007 2006 Annual Technical Report
Hospital Rate Setting
 Hospital Rate Setting Calendar Year 2014 Wisconsin Department of Health Services Division of Health Care Access and Accountability Bureau of Fiscal Management September 6, 2013 1 Agenda 1. Introduction
Hospital Rate Setting Calendar Year 2014 Wisconsin Department of Health Services Division of Health Care Access and Accountability Bureau of Fiscal Management September 6, 2013 1 Agenda 1. Introduction
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August 2016
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
9/10/2013. The Session s Focus. Status of the NYS FIDA Initiative
 Leading Age NY Financial Manager s Conference, September 10-12, 2013 The Otesaga Resort Hotel, Cooperstown NY Paul Tenan VCC, Inc. FIDA: An Overview and Update The Session s Focus Overview of CMS national
Leading Age NY Financial Manager s Conference, September 10-12, 2013 The Otesaga Resort Hotel, Cooperstown NY Paul Tenan VCC, Inc. FIDA: An Overview and Update The Session s Focus Overview of CMS national
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario
 Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 4/1/2014 This document is intended to provide health care organizations in Ontario with guidance as to how they can develop
Quality Improvement Plan (QIP) Narrative for Health Care Organizations in Ontario 4/1/2014 This document is intended to provide health care organizations in Ontario with guidance as to how they can develop
Section A: Systemic Review. Review Methodology
 Purpose The Centers for Medicare and Medicaid (CMS) published its final rule related to Home and Community Based (HCBS) for Medicaid funded long-term services and supports provided in residential and non-residential
Purpose The Centers for Medicare and Medicaid (CMS) published its final rule related to Home and Community Based (HCBS) for Medicaid funded long-term services and supports provided in residential and non-residential
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs
 Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs First Quarter Fiscal Year 2012/13 (July, August, September) Submitted November 2012 Barbara Palmer Director
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs First Quarter Fiscal Year 2012/13 (July, August, September) Submitted November 2012 Barbara Palmer Director
Improving Quality of Care in Anesthesiology Session # 182, March 7, 2018
 Improving Quality of Care in Anesthesiology Session # 182, March 7, 2018 Nilesh Chandra Partner, PA Consulting Group Paul Pomerantz CEO, American Society of Anesthesiologists 1 Conflict of Interest Nilesh
Improving Quality of Care in Anesthesiology Session # 182, March 7, 2018 Nilesh Chandra Partner, PA Consulting Group Paul Pomerantz CEO, American Society of Anesthesiologists 1 Conflict of Interest Nilesh
The Patient Protection and Affordable Care Act of 2010
 INVITED COMMENTARY Laying a Foundation for Success in the Medicare Hospital Value-Based Purchasing Program Steve Lawler, Brian Floyd The Centers for Medicare & Medicaid Services (CMS) is seeking to transform
INVITED COMMENTARY Laying a Foundation for Success in the Medicare Hospital Value-Based Purchasing Program Steve Lawler, Brian Floyd The Centers for Medicare & Medicaid Services (CMS) is seeking to transform
Monthly and Quarterly Activity Returns Statistics Consultation
 Monthly and Quarterly Activity Returns Statistics Consultation Monthly and Quarterly Activity Returns Statistics Consultation Version number: 1 First published: 08/02/2018 Prepared by: Classification:
Monthly and Quarterly Activity Returns Statistics Consultation Monthly and Quarterly Activity Returns Statistics Consultation Version number: 1 First published: 08/02/2018 Prepared by: Classification:
Quality Improvement Work Plan
 NEVADA County Behavioral Health Quality Improvement Work Plan Mental Health and Substance Use Disorder Services Fiscal Year 2017-2018 Table of Contents I. Quality Improvement Program Overview...1 A. QI
NEVADA County Behavioral Health Quality Improvement Work Plan Mental Health and Substance Use Disorder Services Fiscal Year 2017-2018 Table of Contents I. Quality Improvement Program Overview...1 A. QI
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver JULY 18, 2016
 Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
Post-Acute Care Networks: How to Succeed and Why Many Fail to Deliver HEALTH FORUM AND AHA LEADERSHIP SUMMIT JULY 18, 2016 SAN DIEGO, CALIFORNIA Please note that the views expressed are those of the conference
National Council on Disability
 An independent federal agency making recommendations to the President and Congress to enhance the quality of life for all Americans with disabilities and their families. February 7, 2012 Acting Administrator
An independent federal agency making recommendations to the President and Congress to enhance the quality of life for all Americans with disabilities and their families. February 7, 2012 Acting Administrator
HOSPITAL QUALITY MEASURES. Overview of QM s
 HOSPITAL QUALITY MEASURES Overview of QM s QUALITY MEASURES FOR HOSPITALS The overall rating defined by Hospital Compare summarizes up to 57 quality measures reflecting common conditions that hospitals
HOSPITAL QUALITY MEASURES Overview of QM s QUALITY MEASURES FOR HOSPITALS The overall rating defined by Hospital Compare summarizes up to 57 quality measures reflecting common conditions that hospitals
OHPB DRAFT Coordinated Care Organization (CCO) Proposal OMA Summary and Analysis
 OHPB DRAFT Coordinated Care Organization (CCO) Proposal OMA Summary and Analysis December 15, 2011 Bryan Boehringer Courtni Dresser OMA Government Relations Overview CCOs established and implemented to
OHPB DRAFT Coordinated Care Organization (CCO) Proposal OMA Summary and Analysis December 15, 2011 Bryan Boehringer Courtni Dresser OMA Government Relations Overview CCOs established and implemented to
Board Briefing. Board Briefing of Nursing and Midwifery Staffing Levels. Date of Briefing January 2018 (December 2017 data)
 Board Briefing Board Briefing of Nursing and Midwifery Staffing Levels Date of Briefing January 2018 (December 2017 data) This paper is for: Sponsor: Chief Nurse- Dame Eileen Sills (DBE) Decision Author:
Board Briefing Board Briefing of Nursing and Midwifery Staffing Levels Date of Briefing January 2018 (December 2017 data) This paper is for: Sponsor: Chief Nurse- Dame Eileen Sills (DBE) Decision Author:
Creating A Niche: Medical-Surgical Nurses Role in Succesful Program Development (Oral)
 Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Creating A Niche: Medical-Surgical Nurses Role in Succesful Program Development (Oral) Eileen Sacco MSN, RN, CNRN, ONC
Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Creating A Niche: Medical-Surgical Nurses Role in Succesful Program Development (Oral) Eileen Sacco MSN, RN, CNRN, ONC
Quality Measure Indicators +Throughput Metrics + Automated Dashboard = Innovation to Improve Quality Goals
 Quality Measure Indicators +Throughput Metrics + Automated Dashboard = Innovation to Improve Quality Goals DMC Harper- Hutzel Hospital The DMC is an 8 facility academic medical center Harper-Hutzel is
Quality Measure Indicators +Throughput Metrics + Automated Dashboard = Innovation to Improve Quality Goals DMC Harper- Hutzel Hospital The DMC is an 8 facility academic medical center Harper-Hutzel is
Washington State LTSS System, History and Vision
 Washington State LTSS System, History and Vision Bea Rector, Director, Home and Services Aging and Long Term Support Administration Washington State Department of Social and Health Services For Northwest
Washington State LTSS System, History and Vision Bea Rector, Director, Home and Services Aging and Long Term Support Administration Washington State Department of Social and Health Services For Northwest
Enlisted Professional Military Education FY 18 Academic Calendar. Table of Contents COLLEGE OF DISTANCE EDUCATION AND TRAINING (CDET):
 Enlisted Professional Military Education FY 18 Academic Calendar Table of Contents STAFF NON-COMMISSIONED OFFICER ACADEMIES: SNCO Academy Quantico SNCO Academy Camp Pendleton SNCO Academy Camp Lejeune
Enlisted Professional Military Education FY 18 Academic Calendar Table of Contents STAFF NON-COMMISSIONED OFFICER ACADEMIES: SNCO Academy Quantico SNCO Academy Camp Pendleton SNCO Academy Camp Lejeune
Stanislaus County Behavioral Health and Recovery Services Annual Quality Management Work Plan FY
 Stanislaus County Behavioral Health and Recovery Services Annual Quality Management Work Plan FY 2015-2016 INTRODUCTION The scope of this work plan is the overarching Quality Management aspects of the
Stanislaus County Behavioral Health and Recovery Services Annual Quality Management Work Plan FY 2015-2016 INTRODUCTION The scope of this work plan is the overarching Quality Management aspects of the
Mental Health Services - Delayed Discharges: Update
 NHS Greater Glasgow & Clyde NHS Board Meeting Chief Officer, Glasgow City HSCP and Nurse Director October 20 Paper No: /56 Mental Health Services - Delayed Discharges: Update Recommendation:- The NHS Board
NHS Greater Glasgow & Clyde NHS Board Meeting Chief Officer, Glasgow City HSCP and Nurse Director October 20 Paper No: /56 Mental Health Services - Delayed Discharges: Update Recommendation:- The NHS Board
The New Clinical Research Landscape Incentives, Opportunities and Support Offered by the NIHR
 The New Clinical Research Landscape Incentives, Opportunities and Support Offered by the NIHR 1 September 2011 Dr Jonathan Gower Assistant Director CCRN The National Institute of Health Research - A real
The New Clinical Research Landscape Incentives, Opportunities and Support Offered by the NIHR 1 September 2011 Dr Jonathan Gower Assistant Director CCRN The National Institute of Health Research - A real
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs
 Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs Second Quarter Fiscal Year 2015-16 (October, November, December) Submitted February, 2016 Barbara Palmer
Quarterly Report on Agency Services to Floridians with Developmental Disabilities and Their Costs Second Quarter Fiscal Year 2015-16 (October, November, December) Submitted February, 2016 Barbara Palmer
DIME-GAFSP First Quarterly Progress Report
 DIME-GAFSP First Quarterly Progress Report Feburary 24, 2012 The World Bank s Development Impact Evaluation Initiative (DIME) has been contracted to lead in-depth impact evaluations on a subset of GAFSP
DIME-GAFSP First Quarterly Progress Report Feburary 24, 2012 The World Bank s Development Impact Evaluation Initiative (DIME) has been contracted to lead in-depth impact evaluations on a subset of GAFSP
Core Metrics for Better Care, Lower Costs, and Better Health
 Core Metrics for Better Care, Lower Costs, and Better Health IOM Roundtable on Value & Science-Driven Health Care September 27, 2012 Washington, D.C. Sam Nussbaum, M.D. Executive Vice President, Clinical
Core Metrics for Better Care, Lower Costs, and Better Health IOM Roundtable on Value & Science-Driven Health Care September 27, 2012 Washington, D.C. Sam Nussbaum, M.D. Executive Vice President, Clinical
