THE SPECIALTY CARE REFERRAL DILEMMA: The Desperate Need for Clinical Navigation to Improve Value-Based Healthcare
|
|
|
- Gervase Giles Small
- 5 years ago
- Views:
Transcription
1 THE SPECIALTY CARE REFERRAL DILEMMA: The Desperate Need for Clinical Navigation to Improve Value-Based Healthcare
2 The Specialty Care Referral Dilemma AUTHORED BY ARMADAHEALTH'S MEDICAL ADVISORY BOARD Benjamin Safirstein, MD, FACP, FACC Clinical Associate Professor of Medicine, Icahn School of Medicine at Mount Sinai, New York, USA Mary Thomas, MD Pediatrician, Pedimedica, Rochelle Park, USA Scott Swanson, MD Co-Director, Minimally Invasive Surgery, Brigham and Women s Hospital, Boston, USA Iain Kalfas, MD Head, Section of Spinal Surgery, Dept. of Neurosurgery, Cleveland Clinic, Cleveland, USA Louis Aledort, MD Professor of Medicine, Hematology and Medical Oncology, Icahn School of Medicine at Mount Sinai, New York, USA Asher Kimchi, MD Co-Medical Director, Preventive and Consultative Heart Center of Excellence, Cedars-Sinai, Los Angeles, USA Sinai, New York, USA Andrew Tucker, MD Medical Director, MedStar Union Memorial Hospital Sports Medicine, MedStar Union Memorial Hospital, Lutherville, USASinai, New York, USA David Helfet, MD Chief of Combined Orthopaedic Trauma, Hospital for Special Surgery, New York, USA Acknowledgements The authors of this white paper wish to acknowledge the collaboration of Editor, Henry Mortimer, and Research Analyst, Annika Schaefer.
3 TABLE OF CONTENTS EXECUTIVE SUMMARY 2 INTRODUCTION 2 REFERRALS TO SPECIALISTS ARE INCREASING 2 SPECIALTY CARE HAS BECOME COMPLEX 3 INACCURATE DIAGNOSES ARE HARMFUL 4 THE LANDSCAPE HAS CHANGED 4 A SOLUTION IS NEEDED 5 FACTORS FOR SUCCESS 6 IN CONCLUSION 7 SOURCES 8
4 EXECUTIVE SUMMARY As employers know firsthand, the cost of providing healthcare benefits to employees continues to rise. As this white paper illustrates, a large portion of those costs are a direct result of a broken referral process between primary and specialty care. This white paper suggests that, by using the Patient Centered Medical Home as a model, specialty care navigation programs can help employers offer employees better access to the specialty care they need. This, in turn, will help employees achieve better health outcomes and allow employers to better control costs and support employee productivity. INTRODUCTION Healthcare costs continue to rise at an alarming rate and consumers are experiencing great difficulty navigating healthcare systems on their own. Moreover, the practice of medicine is becoming increasingly complex and specialized. The primarycare landscape has also changed dramatically, and the referral process from primary care providers has not sufficiently evolved or adapted to these shifting dynamics. A relatively small number of patients consume a vastly disproportionate amount of healthcare spend on specialty care. In fact, only 5% of healthcare consumers account for almost 50% of total healthcare expenses. 1 Though only 10% of the population requires referral to specialty care services each year, they account for more than 65% of the total volume of annual claims cost. 2 The 15 most expensive health conditions account for 44% of total healthcare expenses. 1 5% 50% 5% OF HEALTHCARE CONSUMERS ACCOUNT FOR ALMOST 50% OF HEALTHCARE EXPENSES All of this data makes it clear that, although specialty referral may be needed by a small percentage of the population in a given year, it is important that it be managed judiciously as it accounts for a very large portion of the total healthcare dollars spent. REFERRALS TO SPECIALISTS ARE INCREASING According to a 2011 report, one-third of all US patients are referred to a specialist each year, yet specialist visits constitute more than half of all outpatient visits. 3 This implies that patients are visiting specialists even more than they are visiting their primary care physicians (PCP). One reason for this increase is that more patients are receiving diagnoses and referrals from providers other than their own primary MDs. Physicians in the emergency room and at various urgent care facilities are often the referring physicians. Many patients (73%) are opting to use urgent care and redimed services for their medical needs rather than their PCP due to difficulty making timely appointments, getting phone advice or receiving after-hour care without having to visit the emergency room. 4 Doctors in urgent care settings seldom have longstanding relationships with patients. Therefore they do not often have access to their full medical record and have limited or no ability to follow up on a referral once it is made. Referrals become too frequent and are very often inappropriate. A study by Barnett found that from 1999 to 2009, ambulatory visits accounted for more than 100 million referrals. 5 In a report published by the Commonwealth Fund Commission, they stated that nearly three out of four patients seek out what should be primary care by going to an ER. 4 When continuity of care is lost, effective referral and effective care are jeopardized. 2
5 Patients themselves may be contributing to the rise in specialty care referrals by using the internet as a self-diagnosis tool and/or bypassing their PCP for a specialty referral. According to one study on managed-care organizations that permit direct patient access to specialists, a large proportion of new referrals for dermatology, OB/GYN, ophthalmology, and psychiatry were patient self-referrals without a diagnosis. 6 Patientinitiated referrals are at even greater risk of being inappropriate as some insurance plans allow patients to see a specialist without a diagnosis or referral from a PCP. The growing number of self-referrals has been associated with dissatisfaction and poor continuity of care. 7 This data suggests what is intuitive; that a lack of a stable primary care relationship often leads to inappropriate specialist use and related costs. THE CURRENT REFERRAL PROCESS IS FRUSTRATING Oftentimes, patients that are referred to specialists are unable to access the specialty care that their PCPs recommend. This may be because the patient has difficulty finding a specialist in their community, insurance coverage is not accepted, there is a lack of timely appointment availability and/or the patient just becomes frustrated and gives up. The difficulty of getting an appointment for specialist care has been cited as a growing problem, especially in underserved populations. 8 Such a breakdown in the continuum of care for patients can have wide-ranging consequences. Despite the growth and frequency of specialty care referrals, the absence of collaboration between primary care doctors and specialists has been a long-standing problem. As with any complex and multistep task, the specialty referral process is prone to breakdowns and inefficiencies. Consider, for example, that patients with chronic illnesses such as diabetes must receive care from multiple providers, in multiple settings, and require complex coordination of their care. THE DIFFICULTY OF GETTING AN APPOINTMENT FOR SPECIALIST CARE HAS BEEN CITED AS A GROWING PROBLEM... The burden of this time-consuming and complicated care coordination falls on the shoulders of the already over-burdened PCP. 9 The primary care doctor must decide who the best specialist is for his patients, make sure the patient completes that referral, solicit information back from specialists about their opinions and then implement those changes as part of a medical plan. Complicating matters, nearly half of referring physicians do not know whether their patients actually see the specialists to which they are referred. 10 SPECIALTY CARE HAS BECOME COMPLEX Another problematic factor is that specialty care has become increasingly more complex and compartmentalized. In the United States, there are now more than 840,000 boardcertified specialists in approximately 200 areas of specialization treating 30,000 different diagnoses. Complicating it further is the levels of sub-specialization. 11 This broad array of options makes it virtually impossible for anyone without the proper guidance to find not only the right type of specialist, but also one that is the most experienced in treating that patient s particular disease or condition. 3
6 200 SUBSPECIALTIES 30,000 DISEASES 840,000 SPECIALISTS Delay to referral is another known flaw in the referral process. Late referrals have been associated with worse health outcomes. In a study of long-standing renal disease, patients who did not see a nephrologist at least 90 days before initiation of dialysis had a 37% higher likelihood of death in the first year of treatment. 12 Nearly one-fifth of patients with stage III or IV colorectal cancer were not referred to medical oncologists for adjuvant chemotherapy. 13 Such delays in treatment have resulted in poor outcomes. Patients in need of specialty care often spend months and sometimes years searching for the right specialist, accumulating unnecessary tests and procedures along the way; or worse, they never make it to see a specialist at all. INACCURATE DIAGNOSES ARE HARMFUL Possibly the most concerning aspect of the referral process is the frequency of inaccurate diagnosis. According to Improving Diagnosis in Health Care, a report from the Institute of Medicine, inaccurate diagnoses continue to harm an unacceptable number of patients. 14 In fact, it is likely that most people will experience at least one diagnostic error in their lifetime, sometimes with devastating consequences. 14 Researchers at Johns Hopkins University examined more than 350,000 malpractice claims over 25 years and found that diagnostic errors defined as missed, wrong or delayed diagnoses accounted for nearly 29% of claims. 15 This study also found that diagnostic errors made up the biggest share of claims payments from 1986 to 2010 and resulted in death in more than 40% of claims. 15 A recent article in the BMJ shows that inpatient medical errors are extremely common and may now be the third-leading cause of death in the United States claiming 251,000 lives every year, more than respiratory disease, suicide, fire arms and motor vehicle accidents. 16 Medical errors are clearly too frequent, but the majority of these errors do not result from individual recklessness or the actions of a particular group. In a landmark paper, To Err is Human, researchers concluded that errors are caused by faulty systems, processes and conditions that lead people to make mistakes or fail to prevent them. 17 While this is a cumulative problem in which no one group is to blame, it reveals that a better system is needed. THE LANDSCAPE HAS CHANGED The healthcare landscape has shifted and the primary care model remains in a relative state of crisis. According to a study examining family and internal medicine physician referral decisions, the reorganization of healthcare over the past few decades has increased the number of referrals made outside of office visits with the PCP. More and more referrals come from telephone conversations with a provider or from recommendations given by non-physician office staff. 18 Gone are the days when a physician could take as much time as needed to examine his or her patients to make a diagnosis and a referral for specialty care based on the patient s needs. According to a study published in Medical Economics, primary care physicians are overwhelmed and as a result, they are forced to 4
7 spend less time with patients than they want or need to. 19 Patients are acutely aware that access to and the amount of time spent with their physicians has decreased. These statistics tell us that the role of a primary care doctor is changing. PCPs no longer play the part of healthcare quarterback, synthesizing a patient s medical record and acting as a gatekeeper to connect patients with specialists once a diagnosis is made and a more complicated level of care is needed. Patients are in growing need of support for specialist referrals because their primary doctor, if one exists, has limited time and resources dedicated to this important aspect of care. A SOLUTION IS NEEDED The impending mandates of value-based care, which will require PCP s to improve the specialty referral process, recognizes the importance of the quality of the referral and its impact on cost. Streamlined collaboration helps providers provide better care. A 2002 study published in the New England Journal of Medicine demonstrated that concurrent care by both a PCP and a cardiologist in the post-mi period was associated with a further reduction in mortality than care by a PCP alone. 20 Further supporting this concept, studies have shown that patients treated by an endocrinologist and a primary care physician were more likely to receive optimal care than those seeking endocrinologists alone % WASTE IN TOTAL US HEALTHCARE EXPENDETURES We know that excellent specialist care is necessary to streamline diagnosis and correctly manage illness. In the landmark article "The Quality of Health Care Delivered to Adults in the United States," researchers reported that only 52-58% percent of patients receive recommended follow-up care. 22 The result of this lack of follow-up is extremely costly. Failure of care coordination and failures of care execution contribute to a 20% waste in total US healthcare expenditures. 17 One growing solution is the Patient Centered Medical Home (PCMH) model. This is an approach to organizing and delivering primary care that emphasizes teamwork and coordination of effort by providers. The PCMH model is designed to cut overall costs and spending by reducing inpatient visits, emergency department use and hospital readmissions. It is based on the idea that better communication leads to better and more cost-effective care. The Guided Care PCMH model, developed by an interdisciplinary team at the Johns Hopkins Bloomberg School of Public Health, features nurse coordinators and multidisciplinary physician teams working in community-based practices. 23 Studies published by RTI International, a health services research journal, suggest that accredited PCMHs deliver lower costs and improve healthcare. 24 A large part of the lower costs and more effective care experienced in the PCMH setting stems from the investment in resources for specialty referral. Emphasis is placed on the quality of the specialist and how he or she matches the patient s specific needs. Another factor in reducing healthcare cost relates to referral tracking, which has been shown to be an important task for the referring provider to assure that the patient is actually seen by the specialist. 5
8 EMPHASIS IS PLACED ON THE QUALITY OF THE SPECIALIST AND HOW HE OR SHE MATCHES THE PATIENT S SPECIFIC NEEDS. PCMH models are beginning to provide insight on the value of navigating patients to the most appropriate specialty care resources, but they reach a limited number of patients and are only scratching the surface of what could be done. We suggest that supplemental clinical navigation programs can fill that need and can be made available broadly to the population. We propose that ensuring patients are objectively matched to a specialist experienced in diagnosing and treating their specific condition will deliver significant improvement in patient satisfaction, cost and outcomes. Providing the missing link from PCP to specialist could be transformational to the healthcare system and of profound value to all constituents in the chain including sponsors of healthcare benefits. FACTORS FOR SUCCESS To be successful, a specialty clinical navigation program must have: A governing body of leading physicians with deep and broad knowledge, international prominence and the highest most objective clinical standards. An objective research and credentialing process with screening and quality standards to identify the best specialists, pinpoint their strengths down to the narrowest area of expertise and most advanced treatment modalities. An independent medical board to oversee the qualifications of accredited boardcertified specialists or the equivalent. An organized and personal approach to a patient medical intake, including understanding the clinical profile, coverage limitations and personal preferences. The ability to provide access to specialists on a timely basis. Verification of what is required by the specialist prior to seeing the patient. Verification of insurance coverages accepted. A follow-up mechanism to facilitate communication with primary care physicians about referral outcomes. The benefits of specialty clinical navigation programs extend to primary care and specialty physicians alike in a number of ways. The ideal partner, they improve the referral pathways in both directions by allowing primary and specialty care providers to stay in communication. Like the PCMH model, they offer an approach to improved coordination and continuity of care by ensuring the efficient delivery of excellent and timely patient care. They provide a specialist with an appropriate referral that matches their ideal patient which will come prepared with any prerequisite testing. For healthcare systems, they reinforce the highest and best use of their specialists. Finally, they reduce or eliminate resource requirements associated with facilitating referrals and the costly impact of errors. 6
9 IN CONCLUSION Due to a broken physician referral system, the economics and complexity associated with providing specialty care has become overwhelmingly burdensome for many Americans. The broken link between primary and secondary care is a shared problem that must be addressed by changes in process. By using a supplemental clinical navigation program, we have the power to transform this paradigm and increase patient satisfaction, improve outcomes and control costs. This solution will bridge the gap between primary care physicians and specialists to deliver more streamlined, affordable and effective care. Equally important is ensuring that the specialist is the right match for the needs of the patient in terms of location, insurance coverage and availability, as well as the specialist s specific skills and clinical relevance. A successful patient-physician match must take into account the patient s diagnosis as well as the physician s training, experience, volume and access to the latest diagnostic and therapeutic options pertinent to the patient s situation. It is time to recognize the value of accessing the right specialists at the right time. When patients receive the wrong care, it can increase cost, delay care and potentially jeopardize lives. Implementing a supplemental specialty clinical navigation program offers a way to solve the specialty care referral dilemma and improve value-based care. 7
10 SOURCES Stanton MW, Rutherford MK. The high concentration of U.S. health care expenditures. Rockville (MD): Agency for Healthcare Research and Quality; Research in Action Issue 19. AHRQ Pub. No Halvorson GC. Health care reform now!: A prescription for change. San Francisco: Jossey-Bass; Mehrotra A, Forrest CB, Lin CY. Dropping the baton. Milbank Q Mar;89(1): How SKH, Shih A, Lau J, Schoen C. Public views on U.S. health system organization: A call for new directions. August Commonwealth Fund pub Vol. 11. Barnett ML, Song Z, Landon BE. Trends in physician referrals in the United States, Arch Intern Med. 2012;172(2): Balogh EP, Miller BT, Ball JR, editors; Committee on Diagnostic Error in Health Care; Board on Health Care Services; Institute of Medicine; The National Academies of Sciences, Engineering, and Medicine. Improving diagnosis in health care. Washington (DC): National Academies Press (US); 2015 Dec. 15 Saber Tehrani AS, Lee H, Mathews SC, Shore A, Makary MA, Pronovost PJ, Newman-Toker DE. 25-year summary of US malpractice claims for diagnostic errors : An analysis from the National Practitioner Data Bank. BMJ Qual Saf Aug;22(8): Makary MA, Daniel M. Medical error-the third leading cause of death in the US. BMJ May 3;353:i Berwick DM. Eliminating waste in US healthcare. JAMA. 2012; 307(14): Forrest CB, Reid RJ. Passing the baton: HMOs influence on referrals to specialty care. Health Aff (Millwood) Nov-Dec;16(6): Forrest CB, Nutting PA, Starfield B, von Schrader S. Family physicians referral decisions: Results from the ASPN referral study. J Fam Pract Mar;51(3): Forrest CB, Weiner JP, Fowles J, Vogeli C, Frick KD, Lemke KW, Starfield B. Self-referral in point-of-service health plans. JAMA May 2;285(17): Forrest CB, Shadmi E, Nutting PA, Starfield B. Specialty referral completion among primary care patients: Results from the ASPN Referral Study. Ann Fam Med Jul- Aug;5(4): Pham HH, O'Malley AS, Bach PB, Saiontz-Martinez C, Schrag D. Primary care physicians' links to other physicians through medicare patients: The scope of care coordination. Ann Intern Med Feb 17;150(4): Bourguet C, Gilchrist V, McCord G. The consultation and referral process. A report from NEON. Northeastern Ohio Network Research Group. J Fam Pract Jan;46(1): The American Board of Medical Specialties fact sheet. Available from factsheet_10_14.pdf. 12 Avorn J, Bohn RL, Levy E, Levin R, Owen WF Jr, Winkelmayer WC, Glynn RJ. Nephrologist care and mortality in patients with chronic renal insufficiency. Arch Intern Med Sep 23;162(17): Oliveria SA, Yood MU, Campbell UB, Yood SM, Stang P. Treatment and referral patterns for colorectal cancer. Med Care Sep;42(9): The 86th annual physician report: Why administrative burdens keep physicians away from patients. Med Econ. Available from com. 20 Ayanian JZ, Landrum MB, Guadagnoli E, Gaccione P. Specialty of ambulatory care physicians and mortality among elderly patients after myocardial infarction. N Engl J Med Nov 21;347(21): Lafata JE, Martin S, Morlock R, Divine G, Xi H. Provider type and the receipt of general and diabetes-related preventive health services among patients with diabetes. Med Care May;39(5): McGlynn EA, Asch SM, Adams J, Keesey J, Hicks J, DeCristofaro A, Kerr EA. The quality of health care delivered to adults in the United States. N Engl J Med Jun 26;348(26): Grumbach K, Bodenheimer T, Grundy P. The outcomes of implementing patient-centered medical home interventions: A review of the evidence on quality, access and costs from recent prospective evaluation studies. Washington, DC: Patient-Centered Primary Care Collective; Au-gust Van Hasselt M, McCall N, Keyes V, Wensky SG, Smith KW. Total cost of care lower among Medicare fee-for-service beneficiaries receiving care from patient-centered medical homes. Health Serv Res Feb;50(1):
11 This white paper is sponsored by TopDoc Connect, a trusted leader in specialty care referrals. TopDoc Connect 230 Schilling Circle, Suite 140 Hunt Valley, MD TopDoc Connect is facilitated by ArmadaHealth, LLC, an independent company that does not have any legal or financial relationship with the physicians it recommends. ArmadaHealth, LLC, is not a provider of healthcare or medical treatment or advice.
Patient-Centered Specialty Practice (PCSP) Recognition Program. April 25, 2013
 Patient-Centered Specialty Practice (PCSP) Recognition Program April 25, 2013 Key Points Recognizes specialists who meet high standards for care coordination Builds on success of NCQA s PCMH program Area
Patient-Centered Specialty Practice (PCSP) Recognition Program April 25, 2013 Key Points Recognizes specialists who meet high standards for care coordination Builds on success of NCQA s PCMH program Area
Patient-Centered Medical Home (PCMH) & Patient-Centered Specialty Practice (PCSP)
 Patient-Centered Medical Home (PCMH) & Patient-Centered Specialty Practice (PCSP) Foundation for a Better Health Care System Presenter Jeanette Ikan, M.D., MHAI Objectives: Definition and benefits of PCMH,
Patient-Centered Medical Home (PCMH) & Patient-Centered Specialty Practice (PCSP) Foundation for a Better Health Care System Presenter Jeanette Ikan, M.D., MHAI Objectives: Definition and benefits of PCMH,
The Medical Neighborhood: Ensuring Continuity of Care with Hospital and Specialist Neighborhoods
 The Medical Neighborhood: Ensuring Continuity of Care with Hospital and Specialist Neighborhoods R. Scott Hammond MD, FAAFP Chair, CAFP PCMH Task Force Medical Director, SOC-PCMH Initiative, Colorado Associate
The Medical Neighborhood: Ensuring Continuity of Care with Hospital and Specialist Neighborhoods R. Scott Hammond MD, FAAFP Chair, CAFP PCMH Task Force Medical Director, SOC-PCMH Initiative, Colorado Associate
MAKING PROGRESS, SEEING RESULTS
 MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
Patient-Centered Specialty Practice: Building the Medical Neighborhood
 Patient-Centered Specialty Practice: Building the Medical Neighborhood Margaret E. O Kane President, National Committee for Quality Assurance June 6, 2014 1 Overview Central challenge: Creating systems
Patient-Centered Specialty Practice: Building the Medical Neighborhood Margaret E. O Kane President, National Committee for Quality Assurance June 6, 2014 1 Overview Central challenge: Creating systems
Building the Bridge- Enhancing PCP:Specialist Coordination
 Building the Bridge- Enhancing PCP:Specialist Coordination Randall Curnow, Jr, MD, MBA, FACP, FACHE, FACPE Vice President of Medical Affairs Mercy Health Physicians- Cincinnati rtcurnow@health-partners.org
Building the Bridge- Enhancing PCP:Specialist Coordination Randall Curnow, Jr, MD, MBA, FACP, FACHE, FACPE Vice President of Medical Affairs Mercy Health Physicians- Cincinnati rtcurnow@health-partners.org
CAMDEN CLARK MEDICAL CENTER:
 INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
A Miracle of Modern Medicine. What medical discovery touches everyone in the United States?
 Primary Care: A Miracle of Modern Medicine What medical discovery touches everyone in the United States? What medical breakthrough is proven to reduce the galloping growth of health care spending? What
Primary Care: A Miracle of Modern Medicine What medical discovery touches everyone in the United States? What medical breakthrough is proven to reduce the galloping growth of health care spending? What
Robert J. Welsh, MD Vice Chief of Surgical Services for Patient Safety, Quality, and Outcomes Chief of Thoracic Surgery William Beaumont Hospital
 Robert J. Welsh, MD Vice Chief of Surgical Services for Patient Safety, Quality, and Outcomes Chief of Thoracic Surgery William Beaumont Hospital Royal Oak, Michigan, USA 1 ARE OUR OPERATING ROOMS SAFE?
Robert J. Welsh, MD Vice Chief of Surgical Services for Patient Safety, Quality, and Outcomes Chief of Thoracic Surgery William Beaumont Hospital Royal Oak, Michigan, USA 1 ARE OUR OPERATING ROOMS SAFE?
Medication Management: Is It in Your Toolbox?
 Medication Management: Is It in Your Toolbox? Brian K. Esterly, MBA, SVP, Corporate Development, excellerx, Inc. O: 215.282.1676, besterly@excellerx.com What has been your Medication Management experience?
Medication Management: Is It in Your Toolbox? Brian K. Esterly, MBA, SVP, Corporate Development, excellerx, Inc. O: 215.282.1676, besterly@excellerx.com What has been your Medication Management experience?
Healthcare Clinic at Walgreens Access to Care Innovations Panel March 5, 2014
 Healthcare Clinic at Walgreens Access to Care Innovations Panel March 5, 2014 Dr. Alan London Vice President, Strategic Clinical Partnerships 2014 Walgreen Co. All rights reserved. Walgreens is Well-Positioned
Healthcare Clinic at Walgreens Access to Care Innovations Panel March 5, 2014 Dr. Alan London Vice President, Strategic Clinical Partnerships 2014 Walgreen Co. All rights reserved. Walgreens is Well-Positioned
Evolving Roles of Pharmacists: Integrating Medication Management Services
 Evolving Roles of Pharmacists: Integrating Management Services Marie Smith, PharmD, FNAP Palmer Professor and Assistant Dean, Practice and Policy Partnerships UCONN School of Pharmacy (marie.smith@uconn.edu)
Evolving Roles of Pharmacists: Integrating Management Services Marie Smith, PharmD, FNAP Palmer Professor and Assistant Dean, Practice and Policy Partnerships UCONN School of Pharmacy (marie.smith@uconn.edu)
VALUE-BASED CARE REPORT
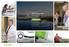 VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Objectives
 Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Morgan Pendleton, PharmD, BCOP Hematology/Oncology Clinical Pharmacist Wake Forest Baptist Health Objectives Evaluate the need
Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Morgan Pendleton, PharmD, BCOP Hematology/Oncology Clinical Pharmacist Wake Forest Baptist Health Objectives Evaluate the need
L19: Improving Transitions from the Hospital to Post Acute Care Settings
 This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
This presenter has nothing to disclose L19: Improving Transitions from the Hospital to Post Acute Care Settings Gail A. Nielsen December 8, 2013 25th Annual National Forum on Quality Improvement in Health
The Case for Home Care Medicine: Access, Quality, Cost
 The Case for Home Care Medicine: Access, Quality, Cost 1. Background Long term care: community models vs. institutional care Compared with most industrialized nations the US relies more on institutional
The Case for Home Care Medicine: Access, Quality, Cost 1. Background Long term care: community models vs. institutional care Compared with most industrialized nations the US relies more on institutional
Healthcare Today: A Leadership Primer How did we get here?
 L19 This presenter has nothing to disclose Healthcare Today: A Leadership Primer How did we get here? Evan M. Benjamin, MD, FACP Professor of Medicine Tufts University School of Medicine; Senior VP, Quality
L19 This presenter has nothing to disclose Healthcare Today: A Leadership Primer How did we get here? Evan M. Benjamin, MD, FACP Professor of Medicine Tufts University School of Medicine; Senior VP, Quality
Adopting Accountable Care An Implementation Guide for Physician Practices
 Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Click to edit Master title. style. Click to edit Master title. style. style 8/3/ Are You on Track?
 Are You on Track? Diagnostic Test Results, Consults and Referrals Click to edit Master subtitle EXPLORE Conference August 9, 2018 8/3/2018 1 EXPLORE August 9, 2018 Today s speaker is Brenda Wehrle, BS,
Are You on Track? Diagnostic Test Results, Consults and Referrals Click to edit Master subtitle EXPLORE Conference August 9, 2018 8/3/2018 1 EXPLORE August 9, 2018 Today s speaker is Brenda Wehrle, BS,
Ensuring Quality Health Care in Health Reform
 Ensuring Quality Health Care in Health Reform What Is Quality Health Care? Put simply, it s the right care, at the right time, for the right reason. It s the care we all deserve but, sadly, it s not the
Ensuring Quality Health Care in Health Reform What Is Quality Health Care? Put simply, it s the right care, at the right time, for the right reason. It s the care we all deserve but, sadly, it s not the
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management
 PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
LEADERSHIP CHALLENGES IN PATIENT SAFETY
 LEADERSHIP CHALLENGES IN PATIENT SAFETY Kenneth W. Kizer, MD, MPH. California Hospital Patient Safety Organization Annual Meeting Sacramento, CA April 8, 2013 Presentation Charge Discuss some of the challenges
LEADERSHIP CHALLENGES IN PATIENT SAFETY Kenneth W. Kizer, MD, MPH. California Hospital Patient Safety Organization Annual Meeting Sacramento, CA April 8, 2013 Presentation Charge Discuss some of the challenges
2ab and 3cd. BTS Topic Selection:
 2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
Fact Sheet. American Board of Medical Specialties (ABMS) and the ABMS Maintenance of Certification (ABMS MOC ) Program
 Fact Sheet American Board of Medical Specialties (ABMS) and the ABMS Maintenance of Certification (ABMS MOC ) Program The American Board of Medical Specialties (ABMS), established in 1933, is a highly
Fact Sheet American Board of Medical Specialties (ABMS) and the ABMS Maintenance of Certification (ABMS MOC ) Program The American Board of Medical Specialties (ABMS), established in 1933, is a highly
Inaugural Barbara Starfield Memorial Lecture
 Inaugural Barbara Starfield Memorial Lecture Wonca World Conference Prague, June 29, 2013 Copyright 2013 Johns Hopkins University,. Improving Coordination between Primary and Secondary Health Care through
Inaugural Barbara Starfield Memorial Lecture Wonca World Conference Prague, June 29, 2013 Copyright 2013 Johns Hopkins University,. Improving Coordination between Primary and Secondary Health Care through
Quality of Care for Underserved Populations
 2006 Annual Report Quality of Care for Underserved Populations The goal of The Commonwealth Fund s Program on Quality of Care for Underserved Populations is to improve the quality of health care delivered
2006 Annual Report Quality of Care for Underserved Populations The goal of The Commonwealth Fund s Program on Quality of Care for Underserved Populations is to improve the quality of health care delivered
Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care
 Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care IHI Workshop 12/6/16 Gordon Schiff, MD, Associate Dir Brigham & Women s Ctr for Patient Safety Research
Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care IHI Workshop 12/6/16 Gordon Schiff, MD, Associate Dir Brigham & Women s Ctr for Patient Safety Research
Integrating prevention into health care
 Integrating prevention into health care Due to public health successes, populations are ageing and increasingly, people are living with one or more chronic conditions for decades. This places new, long-term
Integrating prevention into health care Due to public health successes, populations are ageing and increasingly, people are living with one or more chronic conditions for decades. This places new, long-term
Strengthening Primary Care for Patients:
 Strengthening Primary Care for Patients: Geisinger Health Plan Danville, Pa. Background Geisinger Health Plan (GHP) is a nonprofit health maintenance organization serving the health care needs of more
Strengthening Primary Care for Patients: Geisinger Health Plan Danville, Pa. Background Geisinger Health Plan (GHP) is a nonprofit health maintenance organization serving the health care needs of more
Transforming Healthcare Delivery, the Challenges for Behavioral Health
 Transforming Healthcare Delivery, the Challenges for Behavioral Health Presented by: M.T.M. Services, LLC P. O. Box 1027, Holly Springs, NC 27540 Phone: 919-434-3709 Fax: 919-773-8141 E-mail: mtmserve@aol.com
Transforming Healthcare Delivery, the Challenges for Behavioral Health Presented by: M.T.M. Services, LLC P. O. Box 1027, Holly Springs, NC 27540 Phone: 919-434-3709 Fax: 919-773-8141 E-mail: mtmserve@aol.com
Reducing Elective Waits: Delivering 18 week pathways for patients. Programme Director NHS Elect Caroline Dove.
 Reducing Elective Waits: Delivering 18 week pathways for patients Programme Director NHS Elect Caroline Dove What I will cover 1. Why 18 Weeks is different 2. Where are we now 3. New models of delivery
Reducing Elective Waits: Delivering 18 week pathways for patients Programme Director NHS Elect Caroline Dove What I will cover 1. Why 18 Weeks is different 2. Where are we now 3. New models of delivery
reducing lost revenue from inpatient medical-necessity denials
 REPRINT February 2015 Olakunle Olaniyan healthcare financial management association hfma.org reducing lost revenue from inpatient medical-necessity denials A data-driven approach can help hospitals limit
REPRINT February 2015 Olakunle Olaniyan healthcare financial management association hfma.org reducing lost revenue from inpatient medical-necessity denials A data-driven approach can help hospitals limit
Click to edit Master title style
 Preventing, Detecting and Managing Chronic Disease for Medicare Kenneth E. Thorpe, Ph.D. Robert W. Woodruff Professor and Chair of the Department of Health Policy & Management, Rollins School of Public
Preventing, Detecting and Managing Chronic Disease for Medicare Kenneth E. Thorpe, Ph.D. Robert W. Woodruff Professor and Chair of the Department of Health Policy & Management, Rollins School of Public
A Pharmacist Network for Integrated Medication Management in the Medical Home
 A Pharmacist Network for Integrated Medication Management in the Medical Home Marie Smith, PharmD UConn School of Pharmacy Professor/Dept. Head Pharmacy Practice Asst. Dean, Practice and Public Policy
A Pharmacist Network for Integrated Medication Management in the Medical Home Marie Smith, PharmD UConn School of Pharmacy Professor/Dept. Head Pharmacy Practice Asst. Dean, Practice and Public Policy
PACE Performance on Post-Discharge Primary Care Evaluations from Jan-Jun 2012 PACE. By: Rocio Solano Padilla PCLP-NMF/GE Scholar Jul 23, 2012
 PACE Performance on Post-Discharge Primary Care Evaluations from Jan-Jun 2012 PACE By: Rocio Solano Padilla PCLP-NMF/GE Scholar Jul 23, 2012 2 INTRODUCTION Who am I? Physician Assistant student Towson/CCBC
PACE Performance on Post-Discharge Primary Care Evaluations from Jan-Jun 2012 PACE By: Rocio Solano Padilla PCLP-NMF/GE Scholar Jul 23, 2012 2 INTRODUCTION Who am I? Physician Assistant student Towson/CCBC
Optima Health Provider Manual
 Optima Health Provider Manual Supplemental Information For Ohio Facilities and Ancillaries This supplement of the Optima Health Ohio Provider Manual provides information of specific interest to Participating
Optima Health Provider Manual Supplemental Information For Ohio Facilities and Ancillaries This supplement of the Optima Health Ohio Provider Manual provides information of specific interest to Participating
The Minnesota Statewide Quality Reporting and Measurement System (SQRMS)
 The Minnesota Statewide Quality Reporting and Measurement System (SQRMS) Denise McCabe Quality Reform Implementation Supervisor Health Economics Program June 22, 2015 Overview Context Objectives and goals
The Minnesota Statewide Quality Reporting and Measurement System (SQRMS) Denise McCabe Quality Reform Implementation Supervisor Health Economics Program June 22, 2015 Overview Context Objectives and goals
Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University
 Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University Tuesday, March 2 nd, 2010 Health Care Delivery Reform In its
Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University Tuesday, March 2 nd, 2010 Health Care Delivery Reform In its
Culture Change. Bryan J. Weiner, Ph.D.
 Culture Change Bryan J. Weiner, Ph.D. bjweiner@uw.edu WHAT IS ORGANIZATIONAL CULTURE? The way things are done around here. WHAT KIND OF CULTURE SUPPORTS PERFORMANCE IMPROVEMENT? Learning Organization:
Culture Change Bryan J. Weiner, Ph.D. bjweiner@uw.edu WHAT IS ORGANIZATIONAL CULTURE? The way things are done around here. WHAT KIND OF CULTURE SUPPORTS PERFORMANCE IMPROVEMENT? Learning Organization:
A17/B17: Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care
 A17/B17: Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care Gordy Schiff, MD, Associate Director of Brigham and Women s Center for Patient Safety Research
A17/B17: Addressing Diagnostic Error: Creating Reliable Systems for Diagnosis and Tracking in Primary Care Gordy Schiff, MD, Associate Director of Brigham and Women s Center for Patient Safety Research
A Layered Learning Medication Reconciliation Program
 A Layered Learning Medication Reconciliation Program Brittany Bates, PharmD, BCPS Clinical Pharmacist, Lima Memorial Health System Clinical Assistant Professor, Ohio Northern University Jana Randolph,
A Layered Learning Medication Reconciliation Program Brittany Bates, PharmD, BCPS Clinical Pharmacist, Lima Memorial Health System Clinical Assistant Professor, Ohio Northern University Jana Randolph,
PC & Specialty Care in Era of Multimorbidity 1/21/11
 1 2 This slide dramatically exposes the differences between the United States and other countries and among various other western industrialized countries with regard to life expectancy (on the right side
1 2 This slide dramatically exposes the differences between the United States and other countries and among various other western industrialized countries with regard to life expectancy (on the right side
Bond University Medical Program. Oncology Rotation Clinician Guide
 Bond University Medical Program Oncology Rotation Clinician Guide YEAR 5 2018 Introduction Students in the final year of the Bond University Medical Program have 6 rotations to train in a broad array of
Bond University Medical Program Oncology Rotation Clinician Guide YEAR 5 2018 Introduction Students in the final year of the Bond University Medical Program have 6 rotations to train in a broad array of
Transitions of Care: From Hospital to Home
 Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
NHS performance statistics
 NHS performance statistics Published: 14 th December 217 Geography: England Official Statistics This monthly release aims to provide users with an overview of NHS performance statistics in key areas. Official
NHS performance statistics Published: 14 th December 217 Geography: England Official Statistics This monthly release aims to provide users with an overview of NHS performance statistics in key areas. Official
The CAHPS Ambulatory Care Improvement Guide
 The CAHPS Ambulatory Care Improvement Guide Practical Strategies for Improving Patient Experience To download the Guide s other sections, including descriptions of improvement strategies, go to https://cahps.ahrq.gov/quality-improvement/improvementguide/improvement-guide.html.
The CAHPS Ambulatory Care Improvement Guide Practical Strategies for Improving Patient Experience To download the Guide s other sections, including descriptions of improvement strategies, go to https://cahps.ahrq.gov/quality-improvement/improvementguide/improvement-guide.html.
Foundation for New Jersey Healthcare Transformation The Patient Centered Medical Home the Future
 Paul Grundy MD, MPH IBM Director, Healthcare Transformation Foundation for New Jersey Healthcare Transformation The Patient Centered Medical Home the Future @Paul_PCPCC 2015 IBM Corporation 1 https://www.youtube.com/watch?v=uy088yyq6ua
Paul Grundy MD, MPH IBM Director, Healthcare Transformation Foundation for New Jersey Healthcare Transformation The Patient Centered Medical Home the Future @Paul_PCPCC 2015 IBM Corporation 1 https://www.youtube.com/watch?v=uy088yyq6ua
Primary Care Specialist Physician Compact
 I. Purpose To provide optimal health care for our patients. To provide a framework for better communication and safe transition of care between primary care and specialty care providers. II. Principles
I. Purpose To provide optimal health care for our patients. To provide a framework for better communication and safe transition of care between primary care and specialty care providers. II. Principles
Risk Adjusted Diagnosis Coding:
 Risk Adjusted Diagnosis Coding: Reporting ChronicDisease for Population Health Management Jeri Leong, R.N., CPC, CPC-H, CPMA, CPC-I Executive Director 1 Learning Objectives Explain the concept Medicare
Risk Adjusted Diagnosis Coding: Reporting ChronicDisease for Population Health Management Jeri Leong, R.N., CPC, CPC-H, CPMA, CPC-I Executive Director 1 Learning Objectives Explain the concept Medicare
The Multidisciplinary aspects of JCI accreditation
 The Multidisciplinary aspects of JCI accreditation Saleem Kiblawi MD, FCCP, Physician consultant, Joint Commission International Oakbrook, Illinois USA Lebanese American University April 15, 2016 Beirut,
The Multidisciplinary aspects of JCI accreditation Saleem Kiblawi MD, FCCP, Physician consultant, Joint Commission International Oakbrook, Illinois USA Lebanese American University April 15, 2016 Beirut,
Ambulatory Care Practice Trends and Opportunities in Pharmacy
 Ambulatory Care Practice Trends and Opportunities in Pharmacy David Chen, R.Ph., M.B.A. Senior Director Section of Pharmacy Practice Managers ASHP Objectives Describe trends in health system pharmacy reported
Ambulatory Care Practice Trends and Opportunities in Pharmacy David Chen, R.Ph., M.B.A. Senior Director Section of Pharmacy Practice Managers ASHP Objectives Describe trends in health system pharmacy reported
Expression of Interest for Wound Care Project
 Expression of Interest for Wound Care Project November 11, 2016 Telewound Care EOI Page 1 of 12 Contents 1 Introduction... 3 2 Telewound Care Project Background... 4 2.1 Background... 4 2.2 Purpose...
Expression of Interest for Wound Care Project November 11, 2016 Telewound Care EOI Page 1 of 12 Contents 1 Introduction... 3 2 Telewound Care Project Background... 4 2.1 Background... 4 2.2 Purpose...
NCQA s Patient-Centered Medical Home Recognition and Beyond. Tricia Marine Barrett, VP Product Development
 NCQA s Patient-Centered Medical Home Recognition and Beyond Tricia Marine Barrett, VP Product Development National Committee for Quality Assurance (NCQA) Private, independent non-profit health care quality
NCQA s Patient-Centered Medical Home Recognition and Beyond Tricia Marine Barrett, VP Product Development National Committee for Quality Assurance (NCQA) Private, independent non-profit health care quality
How an Orthopedic Hospitalist Program Can Provide Value to Your Hospital
 White Paper How an Orthopedic Hospitalist Program Can Provide Value to Your Hospital By now you are likely familiar with the term "hospitalist" a physician that is dedicated to a hospitalbased practice.
White Paper How an Orthopedic Hospitalist Program Can Provide Value to Your Hospital By now you are likely familiar with the term "hospitalist" a physician that is dedicated to a hospitalbased practice.
University of Cincinnati Patient Centered Medical Home Leadership Decisions
 University of Cincinnati Patient Centered Medical Home Leadership Decisions Eric J. Warm M.D., F.A.C.P. Program Director, Internal Medicine Associate Professor of Medicine University of Cincinnati College
University of Cincinnati Patient Centered Medical Home Leadership Decisions Eric J. Warm M.D., F.A.C.P. Program Director, Internal Medicine Associate Professor of Medicine University of Cincinnati College
NHS performance statistics
 NHS performance statistics Published: 8 th February 218 Geography: England Official Statistics This monthly release aims to provide users with an overview of NHS performance statistics in key areas. Official
NHS performance statistics Published: 8 th February 218 Geography: England Official Statistics This monthly release aims to provide users with an overview of NHS performance statistics in key areas. Official
Chiropractic Orthopedics and Neuromusculoskeletal Medicine
 Chiropractic Orthopedics and Neuromusculoskeletal Medicine James J. Lehman, DC, MBA, FACO Director Health Sciences Postgraduate Education University of Bridgeport Learning Objectives Comprehend and practice
Chiropractic Orthopedics and Neuromusculoskeletal Medicine James J. Lehman, DC, MBA, FACO Director Health Sciences Postgraduate Education University of Bridgeport Learning Objectives Comprehend and practice
BUILDING THE PATIENT-CENTERED HOSPITAL HOME
 WHITE PAPER BUILDING THE PATIENT-CENTERED HOSPITAL HOME A New Model for Improving Hospital Care Authors Sonya Pease, MD Chief Medical Officer TeamHealth Anesthesia Kurt Ehlert, MD National Director, Orthopaedics
WHITE PAPER BUILDING THE PATIENT-CENTERED HOSPITAL HOME A New Model for Improving Hospital Care Authors Sonya Pease, MD Chief Medical Officer TeamHealth Anesthesia Kurt Ehlert, MD National Director, Orthopaedics
Driving Out Clinical Variation to Drive Up Your Bottom Line
 In Cooperation With: Executive White Paper Series, October 2017 Driving Out Clinical Variation to Drive Up Your Bottom Line Hospitals have always worked to be efficient. Now more than ever, it is increasingly
In Cooperation With: Executive White Paper Series, October 2017 Driving Out Clinical Variation to Drive Up Your Bottom Line Hospitals have always worked to be efficient. Now more than ever, it is increasingly
Improved Post-Discharge Phone Call Process A Case Study: St. Mary Medical Center
 Improved Post-Discharge Phone Call Process A Case Study: St. Mary Medical Center St. Mary Medical Center Improves Post-Discharge Phone Call Process Author: Roya Mirilavassani, Regional Manager Background
Improved Post-Discharge Phone Call Process A Case Study: St. Mary Medical Center St. Mary Medical Center Improves Post-Discharge Phone Call Process Author: Roya Mirilavassani, Regional Manager Background
Improving Sign-Outs in Hospital Medicine
 Improving Sign-Outs in Hospital Medicine Arpana R. Vidyarthi, MD Assistant Professor of Medicine Division of Hospital Medicine Director of Quality, Division of Hospital Medicine Director, Patient Safety
Improving Sign-Outs in Hospital Medicine Arpana R. Vidyarthi, MD Assistant Professor of Medicine Division of Hospital Medicine Director of Quality, Division of Hospital Medicine Director, Patient Safety
Innovative Business Activities in Health Care with Commercial Partners
 Innovative Business Activities in Health Care with Commercial Partners Steve Witman, CPA, MBA Vice President of Business Development / Financial and Capital Planning LifeBridge Health March 4, 2014 Business
Innovative Business Activities in Health Care with Commercial Partners Steve Witman, CPA, MBA Vice President of Business Development / Financial and Capital Planning LifeBridge Health March 4, 2014 Business
Patient Navigation Programs Leveraging Care Pathways. Tina Evans, RN, BS Director of Nursing,Onco-Nav
 Patient Navigation Programs Leveraging Care Pathways Tina Evans, RN, BS Director of Nursing,Onco-Nav Welcome Thank you for joining us today for our webinar. Patient navigation has become an important component
Patient Navigation Programs Leveraging Care Pathways Tina Evans, RN, BS Director of Nursing,Onco-Nav Welcome Thank you for joining us today for our webinar. Patient navigation has become an important component
Winning at Care Coordination Using Data-Driven Partnerships
 Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation. April 4, :45 5:00 pm
 Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
Three C s of Change in the Value-Based Economy: Competency, Culture and Compensation April 4, 2014 3:45 5:00 pm 1 Introduction Kevin McCune, MD Chief Medical Officer Advocate Medical Group Peg Stone Vice
ANNUAL REPORT Witness the transformation of healthcare
 ANNUAL REPORT 2013 Witness the transformation of healthcare A message to our community See Change, Harris Health System s FY2013 Report to Our Community, shares recent accomplishments and successful efforts
ANNUAL REPORT 2013 Witness the transformation of healthcare A message to our community See Change, Harris Health System s FY2013 Report to Our Community, shares recent accomplishments and successful efforts
National Survey on Consumers Experiences With Patient Safety and Quality Information
 Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
Introduction. Singapore. Singapore and its Quality and Patient Safety Position 11/9/2012. National Healthcare Group, SIN
 Introduction Singapore and its Quality and Patient Safety Position Singapore 1 Singapore 2004: Top 5 Key Risk Factors High Body Mass (11.1%; 45,000) Physical Inactivity (3.8%; 15,000) Cigarette Smoking
Introduction Singapore and its Quality and Patient Safety Position Singapore 1 Singapore 2004: Top 5 Key Risk Factors High Body Mass (11.1%; 45,000) Physical Inactivity (3.8%; 15,000) Cigarette Smoking
Coordinated Care: Key to Successful Outcomes
 Coordinated Care: Key to Successful Outcomes Best practices in care coordination improve health, lower costs and increase patient satisfaction 402 Lippincott Drive Marlton, NJ 08053 856.782.3300 www.continuumhealth.net
Coordinated Care: Key to Successful Outcomes Best practices in care coordination improve health, lower costs and increase patient satisfaction 402 Lippincott Drive Marlton, NJ 08053 856.782.3300 www.continuumhealth.net
Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases?
 Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases? Providing care for long-term cancer survivors? Managing depression?
Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases? Providing care for long-term cancer survivors? Managing depression?
INFORMATION ABOUT YOUR OXFORD COVERAGE REIMBURSEMENT PART I OXFORD HEALTH PLANS OXFORD HEALTH PLANS (NJ), INC.
 OXFORD HEALTH PLANS (NJ), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (NJ), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
Wired to Save Lives: A Virtual Hospital Experience
 Wired to Save Lives: A Virtual Hospital Experience Donald J. Kosiak, MD, MBA, FACEP, CPE Vice President for Medical Development Thursday, March 3 rd -- 11:30am Conflict of Interest Donald Kosiak, MD Has
Wired to Save Lives: A Virtual Hospital Experience Donald J. Kosiak, MD, MBA, FACEP, CPE Vice President for Medical Development Thursday, March 3 rd -- 11:30am Conflict of Interest Donald Kosiak, MD Has
2013 Physician Inpatient/ Outpatient Revenue Survey
 Physician Inpatient/ Outpatient Revenue Survey A survey showing net annual inpatient and outpatient revenue generated by physicians in various specialties on behalf of their affiliated hospitals Merritt
Physician Inpatient/ Outpatient Revenue Survey A survey showing net annual inpatient and outpatient revenue generated by physicians in various specialties on behalf of their affiliated hospitals Merritt
Managing Healthcare Payment Opportunity Fundamentals CENTER FOR INDUSTRY TRANSFORMATION
 Managing Healthcare Payment Opportunity Fundamentals dhgllp.com/healthcare 4510 Cox Road, Suite 200 Glen Allen, VA 23060 Melinda Hancock PARTNER Melinda.Hancock@dhgllp.com 804.474.1249 Michael Strilesky
Managing Healthcare Payment Opportunity Fundamentals dhgllp.com/healthcare 4510 Cox Road, Suite 200 Glen Allen, VA 23060 Melinda Hancock PARTNER Melinda.Hancock@dhgllp.com 804.474.1249 Michael Strilesky
Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD
 Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD Outline Quality Overview Overview and discussion of CMS programs Increasing transparency Move from P4R to P4P Expanding beyond
Health Care Systems - A National Perspective Erica Preston-Roedder, MSPH PhD Outline Quality Overview Overview and discussion of CMS programs Increasing transparency Move from P4R to P4P Expanding beyond
Laguna Honda Lean Transformation. Laguna Honda Strategic Performance Management November 2017
 Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Re: Rewarding Provider Performance: Aligning Incentives in Medicare
 September 25, 2006 Institute of Medicine 500 Fifth Street NW Washington DC 20001 Re: Rewarding Provider Performance: Aligning Incentives in Medicare The American College of Physicians (ACP), representing
September 25, 2006 Institute of Medicine 500 Fifth Street NW Washington DC 20001 Re: Rewarding Provider Performance: Aligning Incentives in Medicare The American College of Physicians (ACP), representing
Hospital Readmissions Survival Guide
 WHITE PAPER Hospital Readmissions Survival Guide The Long-Term Care Provider s Ultimate Survival Guide to Incorporating INTERACT into Health Information Technology (HIT) March 2017 In this survival guide,
WHITE PAPER Hospital Readmissions Survival Guide The Long-Term Care Provider s Ultimate Survival Guide to Incorporating INTERACT into Health Information Technology (HIT) March 2017 In this survival guide,
Multi disciplinary Team Communication and Effective Handoffs
 Multi disciplinary Team Communication and Effective Handoffs Lauren Destino, MD Clinical Associate Professor Associate Medical Director of the Pediatric Hospital Medicine Division Stanford University,
Multi disciplinary Team Communication and Effective Handoffs Lauren Destino, MD Clinical Associate Professor Associate Medical Director of the Pediatric Hospital Medicine Division Stanford University,
Ambulatory Patient Safety
 We Harm Patients Too: Ambulatory Patient Safety James Park, MD Associate Medical Director Primary & Urgent Care Jeri Craine, RN, MN Health Promotions Program Manager UW Medicine Valley Medical Center Clinic
We Harm Patients Too: Ambulatory Patient Safety James Park, MD Associate Medical Director Primary & Urgent Care Jeri Craine, RN, MN Health Promotions Program Manager UW Medicine Valley Medical Center Clinic
Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks
 Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks Agenda Define ACO, CIN, and Coordinated Care Review ACO/CIN
Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks Agenda Define ACO, CIN, and Coordinated Care Review ACO/CIN
Issue Brief. Maine s Health Care Workforce. January Maine s Unique Challenge. Current State of Maine s Health Care Workforce
 January 2009 Issue Brief Maine s Health Care Workforce Affordable, quality health care is critical to Maine s continued economic development and quality of life. Yet substantial shortages exist at almost
January 2009 Issue Brief Maine s Health Care Workforce Affordable, quality health care is critical to Maine s continued economic development and quality of life. Yet substantial shortages exist at almost
Administrators. Medical Directors. 61% The negative impact on our hospital-based program s. 44% We will need to consider the most appropriate or most
 2016 This annual survey, which began in 2009, provides key insight into nationwide developments in the business of cancer care. To better capture information from its multidisciplinary membership, this
2016 This annual survey, which began in 2009, provides key insight into nationwide developments in the business of cancer care. To better capture information from its multidisciplinary membership, this
Ayrshire and Arran NHS Board
 Paper 12 Ayrshire and Arran NHS Board Monday 9 October 2017 Planned Care Performance Report Author: Fraser Doris, Performance Information Analyst Sponsoring Director: Liz Moore, Director for Acute Services
Paper 12 Ayrshire and Arran NHS Board Monday 9 October 2017 Planned Care Performance Report Author: Fraser Doris, Performance Information Analyst Sponsoring Director: Liz Moore, Director for Acute Services
Quality Improvement in Health and Social Care
 Some Fundamentals on Quality Improvement in Health and Social Care Towards a Shared Understanding EPSO, Reykjavik, 2017-09-26 Johan Thor, MD, MPH, PhD Associate Professor E-mail: johan.thor@ju.se The death
Some Fundamentals on Quality Improvement in Health and Social Care Towards a Shared Understanding EPSO, Reykjavik, 2017-09-26 Johan Thor, MD, MPH, PhD Associate Professor E-mail: johan.thor@ju.se The death
Learning Lab Objectives. Introduce evidence showing team-based primary care leads to better patient health outcomes.
 Washington, DC L11: Team-Based Care: Effective Innovations in Practice Dr. Ed Wagner, MD, MPH Director Emeritus & Senior Investigator MacColl Center for Health Care Innovation, Group Health Research Institute
Washington, DC L11: Team-Based Care: Effective Innovations in Practice Dr. Ed Wagner, MD, MPH Director Emeritus & Senior Investigator MacColl Center for Health Care Innovation, Group Health Research Institute
Catherine Porto, MPA, RHIA, CHP Executive Director HIM. Madelyn Horn Noble 3M HIM Data Analyst
 1 Catherine Porto, MPA, RHIA, CHP Executive Director HIM Madelyn Horn Noble 3M HIM Data Analyst University of New Mexico Hospitals» The state s only academic medical center» The primary teaching hospital
1 Catherine Porto, MPA, RHIA, CHP Executive Director HIM Madelyn Horn Noble 3M HIM Data Analyst University of New Mexico Hospitals» The state s only academic medical center» The primary teaching hospital
PSYCHIATRY SERVICES UPDATE
 PSYCHIATRY SERVICES UPDATE Mark Leary MD, Interim Chief Kathy Ballou RN, Director of Nursing Anton Nigusse Bland MD, PES Medical Director Emily Lee MD, Inpatient Psychiatry Medical Director TRUE NORTH
PSYCHIATRY SERVICES UPDATE Mark Leary MD, Interim Chief Kathy Ballou RN, Director of Nursing Anton Nigusse Bland MD, PES Medical Director Emily Lee MD, Inpatient Psychiatry Medical Director TRUE NORTH
The Collaborative to Advance Social Health Integration (CASHI)
 The Collaborative to Advance Social Health Integration (CASHI) "Let me tell you the story of one patient we worked with in Boston. He was screened for unmet health-related social needs as part of a newly
The Collaborative to Advance Social Health Integration (CASHI) "Let me tell you the story of one patient we worked with in Boston. He was screened for unmet health-related social needs as part of a newly
CER Module ACCESS TO CARE January 14, AM 12:30 PM
 CER Module ACCESS TO CARE January 14, 2014. 830 AM 12:30 PM Topics 1. Definition, Model & equity of Access Ron Andersen (8:30 10:30) 2. Effectiveness, Efficiency & future of Access Martin Shapiro (10:30
CER Module ACCESS TO CARE January 14, 2014. 830 AM 12:30 PM Topics 1. Definition, Model & equity of Access Ron Andersen (8:30 10:30) 2. Effectiveness, Efficiency & future of Access Martin Shapiro (10:30
Hitting the mark... sometimes. Improve the accuracy of CPT code distribution. MGMA Connexion, Vol. 5, Issue 1, January 2005
 MGMA Connexion, Vol. 5, Issue 1, January 2005 Hitting the mark... sometimes Improve the accuracy of CPT code distribution By Margie C. Andreae, MD, associate director for clinical services, Division of
MGMA Connexion, Vol. 5, Issue 1, January 2005 Hitting the mark... sometimes Improve the accuracy of CPT code distribution By Margie C. Andreae, MD, associate director for clinical services, Division of
Original Research PRACTICE-BASED RESEARCH. University Wexner Medical Center
 Evaluation of provider documentation of medication management in a Patient-Centered Medical Home (PCMH) Trang T. Nguyen, PharmD 1 ; Bella H Mehta, PharmD, FAPhA 2 ; Jennifer L. Rodis, PharmD, BCPS 2 ;
Evaluation of provider documentation of medication management in a Patient-Centered Medical Home (PCMH) Trang T. Nguyen, PharmD 1 ; Bella H Mehta, PharmD, FAPhA 2 ; Jennifer L. Rodis, PharmD, BCPS 2 ;
THE FACTS ABOUT PRIMARY CARE
 OCTOBER This month, Health is Primary is promoting the broad message of primary care and working to activate all of our champions to spread the word during National Primary Care Week. Help us spread the
OCTOBER This month, Health is Primary is promoting the broad message of primary care and working to activate all of our champions to spread the word during National Primary Care Week. Help us spread the
EMERGENCY DEPARTMENT DIVERSIONS, WAIT TIMES: UNDERSTANDING THE CAUSES
 EMERGENCY DEPARTMENT DIVERSIONS, WAIT TIMES: UNDERSTANDING THE CAUSES Introduction In 2016, the Maryland Hospital Association began to examine a recent upward trend in the number of emergency department
EMERGENCY DEPARTMENT DIVERSIONS, WAIT TIMES: UNDERSTANDING THE CAUSES Introduction In 2016, the Maryland Hospital Association began to examine a recent upward trend in the number of emergency department
Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM
 Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM Plan Year: July 2010 June 2011 Background The Harvard Pilgrim Independence Plan was developed in 2006 for the Commonwealth of Massachusetts
Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM Plan Year: July 2010 June 2011 Background The Harvard Pilgrim Independence Plan was developed in 2006 for the Commonwealth of Massachusetts
Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System
 Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System Karen Davis President, The Commonwealth Fund IOM Workshop Series: The Policy Agenda September
Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System Karen Davis President, The Commonwealth Fund IOM Workshop Series: The Policy Agenda September
STRATEGIES AND SOLUTIONS FOR REDUCING INAPPROPRIATE READMISSIONS
 WHITE PAPER STRATEGIES AND SOLUTIONS FOR REDUCING INAPPROPRIATE READMISSIONS This paper offers a two-pronged approach to lower readmission rates and avoid Federal penalties. Jasen W. Gundersen, M.D., M.B.A.,
WHITE PAPER STRATEGIES AND SOLUTIONS FOR REDUCING INAPPROPRIATE READMISSIONS This paper offers a two-pronged approach to lower readmission rates and avoid Federal penalties. Jasen W. Gundersen, M.D., M.B.A.,
Building & Strengthening Patient Centered Medical Homes in the Safety Net
 Blue Shield of California Foundation County Coverage Expansion Planning Workshop #2 Building & Strengthening Patient Centered Medical Homes in the Safety Net July 8, 2011 Presented by: Kathryn Phillips,
Blue Shield of California Foundation County Coverage Expansion Planning Workshop #2 Building & Strengthening Patient Centered Medical Homes in the Safety Net July 8, 2011 Presented by: Kathryn Phillips,
Heart Failure Order Sets. Standardizing Care for the Heart Failure Patient 2012
 Heart Failure Order Sets Standardizing Care for the Heart Failure Patient 2012 Objectives: Standardize care for all heart failure patients in Legacy Base Practice on American Heart Association Guidelines
Heart Failure Order Sets Standardizing Care for the Heart Failure Patient 2012 Objectives: Standardize care for all heart failure patients in Legacy Base Practice on American Heart Association Guidelines
6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step
 6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step Abstract In the current model of health care delivery, the primary care physician works alone
6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step Abstract In the current model of health care delivery, the primary care physician works alone
