SOUTH EAST WALES CANCER NETWORK UPPER GASTROINTESTINAL CANCER CLINICAL CARE GUIDELINES
|
|
|
- Tracey Barton
- 6 years ago
- Views:
Transcription
1 SOUTH EAST WALES CANCER NETWORK UPPER GASTROINTESTINAL CANCER CLINICAL CARE GUIDELINES CREATED: JULY 2010 REVIEW DATE: JULY 2011
2 Signed on behalf of the Cwm Taf Health Board Signed: Designation: Date: Signed on behalf of Aneurin Bevan Health Board Signed: Designation: Date: Signed on behalf of Cardiff and Vale University Health Board Signed: Designation: Date: Signed on behalf of Velindre NHS Trust Signed: Designation: Date: 2
3 Contents 1. Background 1.1 Clinical model 1 2. Multi Disciplinary Teams (MDTs) 2.1 Local MDT 2.2 Network MDT 2.3 Local MDT Patient Pathways 2.4 Referral Guidelines to Network MDT Centralised Surgical Model 3.1 Pre-operative Assessment Admission and Pre-operative Care Critical Care Re-admission Arrangements Enhanced (Level 1) Surgical Ward Arrangements Operative Protocols Middle Third of Oesophagus Lower Third of Oesophagus Total Gastrectomy Laparoscopic Mobilisation Expected Post-operative Care Post operative Care Long Term Management Quality Assurance 4.1 Quality Assurance Indicators Clinical Indicators to support Clinical Lines of Enquiry Network Multidisciplinary Team Meetings Patient and Public Involvement 5.1 Oesophageal Patients Group, South Wales 5.2 Patient Information Leaflets Appendices Appendix 1 NICE Upper GI Referral Guidelines Appendix 2 Oncology Treatment Guidelines Appendix 3 Enhanced Recovery Care Pathways i. Oesophagectomy ii. Sub Total / Partial Gastrectomy and GIST Appendix 4 Upper GI Clinical Trials Appendix 5 Network Multidisciplinary Team Operational Protocol 3
4 1. Background The South East Wales oesophago-gastric cancer service is being established in response to NICE Improving Outcomes Guidance for Upper GI Cancers 1 which states that the treatment for patients with oesophago-gastric cancers should be the responsibility of Specialist Oesophago-gastric Cancer Teams based in Cancer Units or Cancer Centres which normally service populations of more than a million. The South East Wales Cancer Network serves a population approaching 1.4 million over a relatively small, compact geographic area stretching from Abergavenny and Merthyr Tydfil in the North of the region across to Cowbridge and Chepstow in the West and East and Cardiff in the South. NHS care is provided by Aneurin Bevan, Cwm Taf and Cardiff and the Vale University Health Boards. In 2005 Welsh Assembly Government National Standards for Upper Gastro- Intestinal Cancer Services were published and a review of the current service was commissioned by the South East Wales Cancer Network in 2007/2008. The Review recommendations, which were accepted by the Network Board, proposed the centralisation of specialist surgical services at the University Hospital of Wales, Cardiff and Vale University Health Board (formerly Cardiff and Vale NHS Trust). Cardiff and Vale University Health Board already has a well established Upper GI clinical team, however becoming a Surgical Centre has required redesigned patient-pathways new operational procedures, more in-depth data collection, a robust Service Level Agreement and co-operation across a number of organisations. It is also seen as an opportunity to develop a better and more coordinated managed Network to improve the care of all patients with Upper GI Cancer. Establishing the new service has been complex, and the process has taken many months. It is acknowledged that there are risks associated with establishing a service of this type and it is important, therefore, that effective ways of defining and measuring quality are established, and that systems are in place to redress poor quality should it arise. This document aims to provide a framework for assuring the quality of the new service, both during its establishment and into the future and as a result encompasses the clinical and operational guidelines that underpin the Network wide service. Agreement on a clinical model to underpin the centalised service has been a key priority and the following key assumptions underpin the clinical model: Effective team working across all Health Boards and Trusts. Effective pre planning, staging and assessment to facilitate an improved and predictable patient pathway Well managed local and central MDT arrangements 1
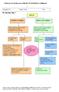
5 Effective planning and management of regular theatre lists that support continuity of patient care and provide flexibility for operating Consultants Effective mechanisms in place to facilitate improved planning of critical care and ward beds Enhanced ward care that meets Designed for Life: Quality Requirements, to support patients post operative course and allow early discharge from critical care where clinically indicated. An Enhanced Recovery After Surgery Programme established at Cardiff and Vale Health Board. Development of a Cardiff and Vale Rapid Response Services to ensure delivery of an outreach service from critical care. The agreed Clinical model is outlined below: 2
6 SEW Surgical Centre Upper GI Cancer Clinical Care Guidelines
7 2. MULTI DISCIPLINARY TEAMS (MDTS) 2.1 Local MDT There will be three local MDTs one based in each of the Health Board Trusts: Aneurin Bevan, Cwm Taf and Cardiff and Vale. Management of the diagnostic and palliative needs of the patient will be led from here, with referral to the central Upper GI MDT for those patients where curative intent is identified. Below are details of the Local MDTs: Aneurin Bevan Health Board Lead Clinician: Dr M Czajkowski The Aneurin Bevan Upper GI Multidisciplinary team meeting is held weekly on a Thursday at in the Anaesthetic Seminar Room, Royal Gwent Hospital. The deadline for submitting patients to be discussed at the Local Upper GI MDM is Tuesday 12.00md. Cardiff and Vale University Health Board Lead Clinician: Mr W Lewis The Cardiff and Vale Upper GI Multidisciplinary team meeting is held weekly on a Tuesday at 12.00md in the MDT Meeting Room, University Hospital of Wales. The deadline for submitting patients to be discussed at the Local Upper GI MDM is Friday 2.00pm. Cwm Taf Health Board Lead Clinician: Mr X Escofet The Cwm Taf Upper GI Multidisciplinary team meeting is held weekly on a Monday at 12.00md in Rooms 3 & 4 Post Graduate Centre, Royal Glamorgan Hospital. The deadline for submitting patients to be discussed at the Local Upper GI MDM is Friday 3.00pm. Patients can be referred to the local MDT in the following ways: GP referrals to any of the core MDT Consultants; From diagnostics; From consultant to consultant; From histopathology; To Clinical Nurse Specialist from community team; From Clinical Nurse Specialist to consultant; Any of the core members of the team can bring existing patients to the meeting if there is a need to discuss their plan of care. 4
8 Patients will be referred from primary care to the Local MDT in line with NICE Referral Guidelines for Upper Gastrointestinal Cancers (Appendix 1) Identifying Patients for Discussion It is intended that local MDTs will review all new UGI cancer patients and refer to the Network MDT for potential surgery or specialised/complex palliative intervention. Patients should only be referred to Network MDT following a decision to refer at local MDT. Patients should then be referred via the agreed referral form ( /canisc) to the Network MDT Coordinator and should be booked into the MDM module within CANISC as per guidelines. The Network MDT Coordinator will then list patients for discussion. Patients with high-grade dysplasia in Barrett's oesophagus and/or such patients being considered for definitive treatment will also be discussed at Network MDT, following discussion at local MDT. GP Notification, documentation of key worker and contact details For all new patients once they have a confirmed diagnosis and been informed of this, the GP will be notified within one working day. This is the responsibility of the local Upper GI team. This information must include the name of the patient's key worker and contact details. A copy of this should be filed in the patient's notes and will be audited. The Upper GI CNS should be present if possible when patients are informed of their diagnosis. The patient is given the key workers details at this time along with appropriate patient information leaflets, including contact details and the way in which they can access members of the MDT to discuss problems or concerns if required. The MDT will provide information to referring general practitioners on the appropriateness of urgent suspected cancer GP referrals. Minimum Data Set Requirements All new patients must be entered onto the CANISC database via the MDT Coordinator/Cancer Services at the local Hospital via the MDM module However, the Network MDT Coordinator will be responsible for entering information regarding potentially curative treatment such as surgery or chemo/radiotherapy onto CANISC for all patients. Documentation of Outcomes Treatment decision will be documented in the following ways: The primary clinician at the local unit is responsible for documenting the outcomes of the Local MDT Patient Management record. This must also include the key worker name. All patients should be seen by their local Upper GI Cancer Nurse Specialist prior to referral to the Surgical Centre in order for treatment co-ordination and future patient support to be facilitated between the Surgical Centre and the local hospital in accordance with IOG and related cancer policies 5
9 2.2 Network MDT The role and purpose of the Network MDT is detailed in the Operational Policy at Appendix 5. New patients with Upper GI malignancy will be discussed at their local (Unit) MDT meeting. If the patients are suitable for referral as per agreed referral protocol to the Surgical Centre for consideration of surgery then their case will be discussed at the weekly held Network MDT. It is expected that all new patients discussed at the Network MDT will have been seen by a Surgical Unit MDT member to present their case and inform the Network MDT of the patients ability to undertake any proposed treatment. A letter documenting the Network MDT decision will be produced and faxed/ ed to the GP and referring Unit s primary clinician within 24 hours. The minutes of all the MDT decisions will be written and validated by the Network MDT in real time and will be available on CANISC immediately. 6
10 ANEURIN BEVAN HEALTH BOARD (South Royal Gwent Hospital) OESOPHAGEAL CANCER PATHWAY 7
11 ANEURIN BEVAN HEALTH BOARD (South Royal Gwent Hospital) GASTRIC CANCER PATHWAY 8
12 ANEURIN BEVAN HEALTH BOARD (North Nevill Hall Hospital) OESOPHAGEAL CANCER PATHWAY 9
13 ANEURIN BEVAN HEALTH BOARD (North Nevill Hall Hospital) GASTRIC CANCER PATHWAY 10
14 CWM TAF HEALTH BOARD OESOPHAGEAL CANCER PATHWAY 11
15 CWM TAF HEALTH BOARD GASTRIC CANCER PATHWAY 12
16 2.4 Referral guidelines to Network MDT Prior to MDT: First seen Trust should (FST): Enter patient journey onto CANISC to date following histological diagnosis. Fax/ completed referral form (see appendix 10) to Network MDT Coordinator within 24 hours of local MDT decision to refer and ensure patient is booked into the MDM module complete appropriate form on CANISC. Arrange for radiological imaging to be made available to the Network MDT PACS. Circulate the patient list to local members immediately following receipt from Network MDT Coordinator. Arrange EUS where EUS has been deemed necessary prior to Network MDT discussion (or where EUS has been requested at a previous Network MDT discussion). Treating Trust (i.e. Surgical Centre) should: List patients for Network MDT discussion following receipt of referral. Where EUS result is required prior discussion, Network MDT Coordinator will liaise with EUS department regarding availability of results and tracking of EUS films to the surgical centre prior to listing patient for MDT discussion. Circulate patient list to local MDT Coordinators and Network MDT team Set up any available PACs images for review during MDT In instances where a patient representative is not available locally, arrange for a Network MDT member to have sight of notes prior to MDT discussion Following MDT: Network MDT should: Minute all Network MDT decisions. These should be validated during the meeting and will be immediately available to Network MDT members and local MDT Coordinators. Ensure surgical patients are added patient management system to ensure they are tracked and reviewed appropriately and to enable surgical team to arrange suitable surgery dates (e.g. following neo-adjuvant chemotherapy). The Network MDT Coordinator will document decisions on Cancer Management plan page within Canisc Ensure patients are relisted for discussion as appropriate (i.e. following investigations such as EUS, PET CT, CPEX and post chemo CT s. First seen Trust should: Ensure decision of the Network MDT is documented within the casenotes. Organise recommendations of the Network MDT once in receipt of Surgical Centre Network MDT minutes (to include referral for EUS, PET CT, exercise testing, pre op assessment tests and post chemo CT s etc). Remain responsible for those patients who are not proceeding to surgery at the Surgical Centre. 13
17 The first seen Trust will undertake the initial pre operative investigations ensuring the results of which are filed within the patient case notes, on CANISC and available for review at pre operative assessment. Assist Network MDT Coordinator with appropriate information where possible in updating roll call. Prior to pre operative assessment, a unified assessment should be completed within the First Seen Trust, the results of which must be communicated to the Nurse Practitioner and CNS at the Surgical Centre. Ensure patients are seen by their local Upper GI Cancer Nurse Specialist prior to referral to the Surgical Centre in order for treatment coordination and future patient support to be facilitated between the Surgical Centre and the local hospital in accordance with IOG and related cancer policies. Post surgery: Treating Trust (i.e. Surgical Centre) should: Enter all surgical data onto CANISC database. Ensure patient notes are tracked back to FST promptly following surgical episode. Ensure that discharge summary, operative notes and post operative histology are faxed back to FST following surgery (Nurse Practitioner at the surgical centre to fax to key worker at the local unit). How the information should be communicated Referral form: via fax Network MDT patient list, minutes and roll call: via Minimum dataset: via CANISC database X-ray images: all digital images should be transferred to PACS used by Network MDT. Patient notes: to be transferred via internal mail system MDT outcome sheets: via /canisc 14
18 3. SURGICAL TREATMENT 3.1 Pre-operative Assessment Once a patient has been identified for curative intent, referral will be made by the lead surgeon for anaesthetic pre assessment. This will be undertaken locally by the Anaesthetist who will be involved in the operation. Following this assessment a referral will be generated to the Critical Care team stating whether the patient will require a level 2 or 3 bed post operatively. Consideration at this stage will be given to pre operative Nutritional support and this will again be undertaken locally at outpatient clinic by the Lead Dietician for the Service. One to two weeks prior to operation, patients will attend a designated Pre- Operative Clinic (POC) at the central hospital for clerking with a Nurse Practitioner. This will include nurse assessment, clinical examination and booking of tests, as well as allowing for baseline blood screens and ECGs to be undertaken. It will ensure the appropriate documentation is in place prior to admission. At the same clinic, all oesophagectomy patients will undergo a pre-operative physiotherapy assessment, and all high risk gastrectomy patients will be reviewed if indicated following Anaesthetic pre-assessment. Attending the PAC will also provide an opportunity for patients and carers to visit and familiarise themselves with the hospital prior to admission. 3.2 Admission and Pre operative Care All elective sections will be booked via the surgical secretaries, two weeks in advance using a standard referral letter which includes requirements for predicted level of immediate post operative care required. On admission all patient will commence the Integrated Care Pathway 1, 2 or 3 (appendix ). Patients will be admitted hours on the day before surgery to a bed that will be protected for return following their surgery. Patients will be assessed by the FP1 or FP2 team with support of the Nurse Practitioner who will coordinate all test results for surgical review. Final informed consent will be obtained by the lead operating consultant. Bowel preparations will commence. All patients will be seen by the Lead Dietician on admission for reassessment. Patients will receive carbohydrate loading orally if able to take oral fluids, if not via a nasoenteral feeding tube if practical. Pre-operative starvation will be no more than 4 hours prior to surgery. Unless in exceptional circumstances. Predicted date of discharge will be documented, if enteral nutrition is envisaged at home, planning will be commenced. Joint operating between visiting consultants and UHW consultants will be encouraged for more complex cases or if laparoscopic resections are developed. 15
19 The junior surgical team at UHW will be available to provide assistance for all operating lists, optimising training opportunities and the continuity of post operative care for patients. This team comprises a year 6 SpR in upper GI surgery, a year 3/4 surgical SpR and a Clinical Fellow in Upper GI Surgery. The Surgical Nurse Practitioner will support the surgical team in caring for Upper GI patients on the ward, as well as leading and coordinating the Pre-assessment clinic activity. One oesophagectomy or a maximum of two gastrectomies can be scheduled on any full day operating list. Patients are expected to have a feeding jejunostomy placed at the time of surgery (subtotal gastrectomy at the consultant s discretion). Biopsies will be undertaken and sent to histopathology for analysis and reporting. This can frequently include complex and specialist investigations including immunohistochemistry and molecular analysis such as cytogenetic investigation of HER2 status. 3.3 Critical Care Pre-admission Arrangements Patients requiring critical care admission will require consultant to consultant referral well in advance of the day of surgery, or hospital admission. The challenges presented by such patients in the peri-operative period are such that anaesthetic pre-assessment would be required, and this might be a suitable point at which referral to consultant intensivists would take place using a critical care booking form. For booked patients, on the day prior to surgery and before hospital admission, the critical care team will confirm the availability of suitable Critical Care capacity; this communication would take the form of consultant to consultant. The purpose of this is to avoid admission to hospital of patients who have no prospect of surgery due to unusually high critical care activity. Such events would be recorded as critical incidents and work during implementation is required to address how these patients surgery can then be expedited. Once admitted to hospital booked patients surgery will proceed as planned. A process is being developed by the Critical Care Directorate for this purpose. Theatre scheduling that ensures the earliest possible completion of surgery, should be aided by this. Appropriate theatre recovery care with prompt transfer to critical care of patients requiring Level 2 care, should create capacity in recovery. Those patients who require enhanced (Level 1) surgical ward dependency post-operatively may require rather longer stays in theatre recovery to ensure appropriate stabilisation under anaesthetic supervision prior to ward transfer. 16
20 3.4 Enhanced (Level 1) Surgical Ward Provision The Critical Care component of the pathway is enabled by significant changes in provision of ward care for this patient group that is described below. The additional nurses at ward level will provide one extra nurse per shift 7 days a week, to allow a 24/7 capability of such nursing care. This will ensure an increased level of care for these patients typically for 48 hours post operatively plus increased observational care after this time as required during their post operative stay until discharge. These posts are essential in prevention and early detection of post operative complications that studies have shown have a potential to develop at day 5-6. The Surgical ward nursing team will be supported by the nurse led Critical Care Outreach team who will provide ongoing training and support to ward based nurses in the care of these patients together with clinical advice to the surgical ward team about individual patient care problems. The nurse led Critical Care Outreach team will be provided 7 days a week, as a daytime and evening service. Enhanced ward care is referring to Level 1 Ward Care as described in the Design for Life Quality Standards and will be delivered within any bed area within the designated ward, rather than a specified location within the ward. This model is preferred by medical and nursing staff because it allows maximum flexibility within the ward area by reducing the need to move patients as their dependency changes. This is an important flexibility because it subsequently reduces the risk of critical care discharge being delayed because a ward Enhanced Care unit is full. 3.5 Operative Protocols Middle Third of Oesophagus If this is for resection it will normally require a three-stage oesophagectomy. The patients will require one lung anaesthesia and an epidural catheter. A right thoracotomy will be the first intervention to mobilise the oesophagus and to assess operability. Gastric mobilisation will be done either at open laparotomy or by a laparoscopic technique if appropriate and if technically feasible. This may be done with concomitant neck dissection with two teams, if two are available. The anastomosis will be done in the neck. There will be a two-field lymph node dissection. The mediastinum will be cleared to achieve radial clearance wherever possible. If the patient has been entered into the OEO5 trial, the clearance will be as per protocol. The anastomotic technique will be at the discretion of the surgeon. The exact level of the tumour may allow for a 2-stage resection. 17
21 3.5.2 Lower Third of Oesophagus and Cardia This will normally require an Ivor Lewis (Lewis Tanner) resection with abdominal gastric mobilisation and a Right thoracotomy with intrathoracic anastomosis. The gastric mobilisation may be done laparoscopically if appropriate and if technically feasible. The patients will require one lung anaesthesia and an epidural catheter. There will be a two-field lymph node dissection. If there is attachment of the tumour to the diaphragm, a rim of diaphragm will be taken with the specimen. The mediastinal radial clearance will be to achieve clear margins, or if the patient has been entered into the OEO5 trial, will be as per protocol. The anastomotic technique will be at the discretion of the surgeon Total Gastrectomy This resection is done transabdominally. It will require an epidural catheter and two-lung anaesthesia. The surgical resection will include the greater omentum and lymph node stations appropriate to the site of the tumour. The resection will not include the spleen or the tail of the pancreas unless there is direct extension rendering preservation of these organs oncologically unsafe.reconstruction will be with a Roux loop. It is optional to construct a pouch at the distal end of the loop (to enhance post-operative nutritional recovery). The Roux loop will normally have a 50cms gap between the oesophageal anastomosis and the reattachment of the proximal jejunum Laparoscopic Mobilisation This is an established technique outside the UK, and is gaining acceptance within the UK. Any laparoscopic procedures will be subject to rigorous scrutiny and audit. It is suggested that there should be data entry into a national database for audit purposes. This is an ideal opportunity for a comparative trial of techniques subject to ethical committee approval. It is further suggested that all laparoscopic procedures should involve two surgeons in order to provide maximum benefit to the patient. 3.6 Expected Post-operative Pathways All patients require appropriate individualised care. However for the purposes of developing the clinical model three expected pathways are envisaged. Gastrectomy patients who are pain free and not requiring cardio-vascular monitoring will return to enhanced (Level 1) surgical ward beds, after an appropriate period in recovery. In addition to this care, these patients will receive a mid evening joint surgical and critical care outreach review, in order to agree an individualised overnight management plan in conjunction with the consultant surgeon. All oesophagectomy patients who remain intubated post-operatively will be transferred directly from the operating theatre to Critical Care, for overnight Level 3 care (or shorter period when indicated). Following extubation these patients will 18
22 then receive an appropriate period of Level 2 care before returning to their protected ward bed to receive enhanced (Level 1) surgical ward care. All oesophagectomy patients extubated at the end of the operative procedure, will remain in theatre recovery to ensure appropriate stabilisation under anaesthetic supervision prior to transfer to Critical Care. Similarly complex gastrectomy patients identified as requiring a period of post operative critical care will follow the same pathway. Such patients will the receive overnight Level 2 care before returning to their protected ward bed to receive enhanced (Level 1) surgical ward care. 3.7 Post operative Care The operating consultant will be available for the first 72 hours post operative period in case of an emergency requiring urgent intervention. The operating consultant and consultant anaesthetist will be expected to visit the patient on the morning of the first post-operative day and subsequently at their discretion. Mr Lewis will oversee the post operative care of Cwm Taf patients and Mr Clark will oversee the post operative care of Aneurin Bevan patients. It is expected that if further surgery is required, that the UHW anaesthetic team will be responsible for the anaesthesia, but the operating surgeon will perform the operation. Agreed shared care protocols will be in place to cover the day-to-day assessment during the post-operative period, but it is expected that the UHW surgeons will take nominal responsibility for troubleshooting. This will take the form of identifying and assessing the urgency of any problems if they should arise. The junior surgical team will undertake a morning round on all patients on Mondays to Fridays. They will provide routine post operative care and organise all post operative tests. The team will undertake the removal of abdominal and chest drains as necessary. A gastrograffin swallow will be scheduled for 7 days post op for oesophagectomy and total gastrectomy patients. Pain control will be overseen by the pain team and patients will receive a minimum of once daily visits, supported by additional input when clinically indicated which could be up to one hour, dependent on patient need. The Lead Dietitian will review the patient daily for the first 7-10 days. The Die titian will liaise with the junior doctors to ensure adequate fluid management and biochemical monitoring and correction is taking place. Feed rate and volume will be increased as tolerated by the patient. This will be on an individual basis to a patient centred approach. The Dietician will monitor the jejunostomy stoma site and discuss with colleagues any concerns to prevent the need to stop enteral feeding. Oral fluids and food will be introduced after discussion with the Consultant Surgeon, as per Enhanced Recovery Pathway 1, 2 or 3 (see appendix 3). Post-op Physiotherapy Management for Oesophagectomies will include a baseline post-op assessment and commencement of chest care 1 following surgery. Day 1-5 patients will be seen at least twice a day for assessment, chest care 1 and 19
23 mobilisation as appropriate. The focus will be on early mobilisation with patients sitting out of bed/mobilising from Day 1 as CVS and pain allows. Shoulder exercises for Ivor Lewis patients to commence Day 1. Aim to mobilise ½ length of ward and back by Day 3. Days 6 Discharge - To be seen daily to progress. Mobility and extolerance stair assessment to be completed and advice provided pre-discharge. Post-op physiotherapy Management for Gastrectomy patients will include review following surgery for high risk patients only to receive input (as per oesophagectomy). Day 1-3 Patients will receive Baseline post-op assessment performed Day 1 and will be seen at least twice a day for assessment, chest care 1 and mobilisation as appropriate. Focus will be on early mobilisation with patients sitting out of bed/ mobilising from Day 1 as CVS and pain allow. Aim to mobilise ½ length of ward and back by Day 3. Days 4 Discharge, patients will be seen daily to progress mobility and ex-tolerance. Stair assessment to be completed and advice provided pre-discharge All patients will receive a visit on the ward from the Specialist nurse who will offer and provide information on the Oesophageal Patients Association and local Support Groups as appropriate. She will assess the patient to determine how much involvement is needed over the next few weeks. Arrangements will be made to contact the patient at home following discharge, by their clinical nurse specialist, (and before their next clinic appointment). Patients and their relatives will have a discussion with the medical team regarding the final histology report prior to their discharge/follow up appointment. It is expected that the patients will stay in UHW until discharge. If there are complications that cause a delay in discharge to home, patients may be discharged back to their local hospital, following full multidisciplinary assessment and in line with discharge policy. Discharge notification and the prescribing of take home medications will be undertaken by the junior surgical team. It will be the operating consultant s responsibility to undertake or delegate appropriately the formal discharge letter which will be typed by the UHW unit secretaries. Follow up should take place at the referring hospital location. 3.8 Long-Term Management Post treatment follow up: A follow-up appointment will be given for 2 weeks. The patients will be advised to contact the ward or Specialist Nurse should any unexpected problems occur early on, following discharge. The Specialist Nurse will be available for continued support. Involvement from other services is assessed at each contact, with referrals being expedited as appropriate Follow up guidelines: All patients undergoing surgery for oesophageal and gastric cancer will be followed up according to the following protocol. 20
24 2 4 weeks following discharge in the local outpatient clinic. 3 months after operation local outpatient clinic 6 months after operation local outpatient clinic 12 months after operation local outpatient clinic Annual follow up thereafter until 5 years locally Follow up appointments to be performed by Upper G I cancer team (consultants, registrars or specialist nurses) The surgical centre will ensure that local hospitals have full information about operation, pathology and other relevant details. It may be appropriate for joint follow-up with oncology if post-operative treatment is required. Patients concerned about their symptoms should contact their local specialist nurse, GP or their referring clinician s secretary for assessment / advice No routine imaging, but if symptomatic, investigations may be arranged/advise sought from specialist (Network) MDTM or direct liaison with operating surgeon. Oncology Long term Follow Up: For patient diagnosed with Squamous Cell Carcinoma, and deemed fit for surgery, but chose not to have surgery, may have definitive radiotherapy and will require ODG and CT. Recurrence All patients who relapse but are suitable for salvage curative treatment should be referred to the Network MDM for management. 21
25 4. QUALITY ASSURANCE AND AUDIT 4.1 Quality Assurance Indicators Numbers patients having curative radiotherapy, surgery and chemo radiation; Morbidity and mortality for patients who receive curative radiotherapy, surgery and chemo radiation; Patient satisfaction every 3 years; Number of patients going into clinical trials, randomized and non randomized and track these numbers back to health boards; Nodes at surgery; Correlation of pre-op stage to post op stage in surgical patients every 3 years Waiting times for USC and non USC patients tracked back to health boards, and proportions of each 4.2 Clinical Indicators to support Clinical Lines of Enquiry Median number of 15 lymph nodes examined for all resected stomach cancers (minimum: 85%, target: 95%) Median number of 10 lymph nodes examined for all resected oesophageal cancers (minimum: 85%, target: 95%) Resection rate stomach Resection rate oesophagus % of patients offered entry into clinical trials (target: >17% into trials) % of patients having final pre treatment stage as agreed by the multi disciplinary team for all oesophago-gastric cancers (minimum: 85%, target 95%) % of patients discussed by a multi disciplinary meeting (minimum: 85%, target: 95%) year survival for curatively treated oesophago-gastric patients, stratified by stage and grade 4.3 Network Multidisciplinary Team Meetings The MDM will hold 3 meeting per year; 2 audit meeting and 1 research meeting. 22
26 5. PATIENT AND PUBLIC INVOLVEMENT Oesophageal Patients Group, South Wales This support group has been running for approximately 7 years at a local level now regionally. The group is for patients and their carers who have undergone oesophago-gastric surgery, or are about to undergo the surgery. The patient group comprises of patients who have had surgery, pre op chemotherapy with surgery and those who have had pre op chemo/radiotherapy and surgery. The aim of the group is to provide support and advice from people who have experience in dealing with these patients, as well as the patients and carer s experience that can be drawn upon. We have a number of patients who are available to speak to patients prior to their surgery if they need any additional support. The group meets 4 times a year for a coffee morning, there are regular speakers ie, dietetics, social services as wells as a reflexologist who provides therapies on the day. We also try to arrange a bus trip and a Christmas night out. The cost of these activities are mainly met by the group, as we are a charity we rely on donations or fund raising events to keep the money readily available. The group is audited to ensure the patients are receiving the support and service they feel they need and they also give feedback on the regional information leaflets. The group has an elected committee Chairman, Secretary, Treasurer and a Specialist Nurse. These people can be contact easily via telephone; their numbers are on the website The website is updated regularly with the details of forthcoming events; however it remains the responsibility of the Specialist Nurse in each area to direct patients to the group. The group is an affiliated member of the Oesophageal Patients Association (UK). 23
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician 3CCN WORCESTERSHIRE ACUTE HOSPITALS Worcestershire Acute Hospitals NHS Trust Local Upper GI MDT (11-2F-1) - 2011/12
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician 3CCN WORCESTERSHIRE ACUTE HOSPITALS Worcestershire Acute Hospitals NHS Trust Local Upper GI MDT (11-2F-1) - 2011/12
Specialised Services Service Specification: Hepatobiliary Cancer Surgery
 Specialised Services Service Specification: Hepatobiliary Cancer Surgery Document Author: Specialised Services Planner, Cancer and Blood Executive Lead: Medical Director, WHSSC Approved by: Management
Specialised Services Service Specification: Hepatobiliary Cancer Surgery Document Author: Specialised Services Planner, Cancer and Blood Executive Lead: Medical Director, WHSSC Approved by: Management
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician MCCN WIRRAL UNIVERSITY TEACHING Wirral Breast MDT (11-2B-1) - 2011/12 Miss M Callaghan Compliance Self Assessment BREAST
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician MCCN WIRRAL UNIVERSITY TEACHING Wirral Breast MDT (11-2B-1) - 2011/12 Miss M Callaghan Compliance Self Assessment BREAST
National Cancer Action Team. National Cancer Peer Review Programme EVIDENCE GUIDE FOR: Colorectal MDT. Version 1
 National Cancer Action Team National Cancer Peer Review Programme FOR: Version 1 Introduction This evidence guide has been formulated to assist Networks and their constituent teams in preparing for peer
National Cancer Action Team National Cancer Peer Review Programme FOR: Version 1 Introduction This evidence guide has been formulated to assist Networks and their constituent teams in preparing for peer
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team MVCN LUTON AND DUNSTABLE Luton & Dunstable Colorectal MDT (11-2D-1) - 2011/12 Peer Review Visit Date 11th November 2011
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team MVCN LUTON AND DUNSTABLE Luton & Dunstable Colorectal MDT (11-2D-1) - 2011/12 Peer Review Visit Date 11th November 2011
Pre Assessment Policy. Trust Policy Forum March 2004
 Policy No: OP19 Version 1.0 Name of Policy: Pre Assessment Policy Effective From: March 2004 Approved by: Trust Policy Forum March 2004 Next Review Date: March 2005 Reviewed by: This policy supercedes
Policy No: OP19 Version 1.0 Name of Policy: Pre Assessment Policy Effective From: March 2004 Approved by: Trust Policy Forum March 2004 Next Review Date: March 2005 Reviewed by: This policy supercedes
1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure
 ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
ADMISSION & DISCHARGE POLICY FOR ADULT CRITICAL CARE SERVICES CONTENTS Page 1 Introduction 2 2 Definitions of levels of care 3 3 Common principles 4 4 Admission criteria 5 5 Referral procedure 5-7 5.1
Northern Ireland Peer Review of Cancer MDTs. EVIDENCE GUIDE FOR LUNG MDTs
 Northern Ireland Peer Review of Cancer MDTs EVIDENCE GUIDE FOR LUNG MDTs CONTENTS PAGE A. Introduction... 3 B. Key questions for an MDT... 6 C. The Review of Clinical Aspects of the Service... 8 D. The
Northern Ireland Peer Review of Cancer MDTs EVIDENCE GUIDE FOR LUNG MDTs CONTENTS PAGE A. Introduction... 3 B. Key questions for an MDT... 6 C. The Review of Clinical Aspects of the Service... 8 D. The
Service Mapping Report
 Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Alfred Health, Cabrini Health,
Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Alfred Health, Cabrini Health,
West Middlesex Junior Doctors Handbook in Colorectal Surgery
 West Middlesex Junior Doctors Handbook in Colorectal Surgery Page 1 of 10 INTRODUCTION Welcome to surgery and to the colorectal team! This guide is meant to be just that, a guide and has been principally
West Middlesex Junior Doctors Handbook in Colorectal Surgery Page 1 of 10 INTRODUCTION Welcome to surgery and to the colorectal team! This guide is meant to be just that, a guide and has been principally
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT GMCCN SALFORD ROYAL Salford Specialist Gynae MDT (11-2E-2) - 2011/12 Date Self Assessment Completed 30th June 2011 Date of IV Review
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT GMCCN SALFORD ROYAL Salford Specialist Gynae MDT (11-2E-2) - 2011/12 Date Self Assessment Completed 30th June 2011 Date of IV Review
DRAFT Optimal Care Pathway
 DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
THE ROY CASTLE LUNG CANCER FOUNDATION
 Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Transforming Cancer Services In South East Wales
 Transforming Cancer Services In South East Wales Clinical Service Model January 2016 Cancer survival rates are increasing. But the number of people getting cancer is increasing too. At Velindre NHS Trust
Transforming Cancer Services In South East Wales Clinical Service Model January 2016 Cancer survival rates are increasing. But the number of people getting cancer is increasing too. At Velindre NHS Trust
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Named Key Worker for Cancer Patients Policy
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Named Key Worker for Cancer Patients Policy Version No.: 4 Effective 07 December 2017 From: Expiry Date: 07 December 2020 Date Ratified: 17 October
The Newcastle upon Tyne Hospitals NHS Foundation Trust Named Key Worker for Cancer Patients Policy Version No.: 4 Effective 07 December 2017 From: Expiry Date: 07 December 2020 Date Ratified: 17 October
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
Service Mapping Report
 Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Aneurin Bevan University Health Board Stroke Services Redesign Programme
 Aneurin Bevan University Health Board Services Redesign Programme 1 Introduction This report aims to update the Health Board on progress with the Services Redesign Programme of work which commenced in
Aneurin Bevan University Health Board Services Redesign Programme 1 Introduction This report aims to update the Health Board on progress with the Services Redesign Programme of work which commenced in
The sarcoma multi-disciplinary team
 http://www.londonsarcoma.org/ Information for patients and carers The sarcoma multi-disciplinary team University College London Hospitals NHS Foundation Trust 2 Contents An introduction to The London Sarcoma
http://www.londonsarcoma.org/ Information for patients and carers The sarcoma multi-disciplinary team University College London Hospitals NHS Foundation Trust 2 Contents An introduction to The London Sarcoma
SURGICAL ONCOLOGY MCVH
 SURGICAL ONCOLOGY MCVH PGY-4 and PGY-5 Medical Knowledge: Demonstrates knowledge about established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral) sciences;
SURGICAL ONCOLOGY MCVH PGY-4 and PGY-5 Medical Knowledge: Demonstrates knowledge about established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral) sciences;
National Cancer Peer Review Programme Evidence Guide for: Gynaecology Specialist MDT
 Intelligence National Cancer Action Team Part of the National Cancer Programme National Cancer Peer Review Programme Evidence Guide for: Gynaecology Specialist MDT Foreword This evidence guide has been
Intelligence National Cancer Action Team Part of the National Cancer Programme National Cancer Peer Review Programme Evidence Guide for: Gynaecology Specialist MDT Foreword This evidence guide has been
Surgical Treatment for Cancer of the Oesophagus
 Oxford Oesophagogastric Centre Surgical Treatment for Cancer of the Oesophagus Information for patients This leaflet gives you information about your planned operation, possible risks and complications,
Oxford Oesophagogastric Centre Surgical Treatment for Cancer of the Oesophagus Information for patients This leaflet gives you information about your planned operation, possible risks and complications,
Seven Day Services Clinical Standards September 2017
 Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
Seven Day Services Clinical Standards September 2017 11 September 2017 Gateway reference: 06408 Patient Experience 1. Patients, and where appropriate families and carers, must be actively involved in shared
Stanford Surgical Oncology II: R1 Tuesday, February 02, 2016
 Stanford University General Surgery Residency Program Surgical Oncology II Surgery goals and objectives for residents: R-1 Rotation Director: Ralph Greco, MD Description The Surgical Oncology II rotation
Stanford University General Surgery Residency Program Surgical Oncology II Surgery goals and objectives for residents: R-1 Rotation Director: Ralph Greco, MD Description The Surgical Oncology II rotation
My treatment plan booklet
 Oesophago-gastric service My treatment plan booklet Information for patients, relatives and carers Details about me Name: Address: Date of birth: Telephone number: NHS Number: Emergency contact details
Oesophago-gastric service My treatment plan booklet Information for patients, relatives and carers Details about me Name: Address: Date of birth: Telephone number: NHS Number: Emergency contact details
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT)
 TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP)
 Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Summary Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Summary Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced
Glangwili Hospital General Surgery (including Colorectal) ~ Recruitment ~
 Glangwili Hospital General Surgery (including Colorectal) ~ Recruitment ~ October 2017 What we do General Surgery (including Colorectal) Glangwili Hospital, Carmarthen There are currently seven surgical
Glangwili Hospital General Surgery (including Colorectal) ~ Recruitment ~ October 2017 What we do General Surgery (including Colorectal) Glangwili Hospital, Carmarthen There are currently seven surgical
Salisbury NHS Foundation Trust Individual Placement (Job) Descriptions for Foundation Year 1
 Salisbury NHS Foundation Trust Individual Placement (Job) Descriptions for Foundation Year 1 Placement The department The type of work to expect and learning opportunities F1 Cardiology The Department
Salisbury NHS Foundation Trust Individual Placement (Job) Descriptions for Foundation Year 1 Placement The department The type of work to expect and learning opportunities F1 Cardiology The Department
RIGHT HEMICOLECTOMY. Patient information Leaflet
 RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification. 12 months
 E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
E09/S(HSS)/b 2013/14 NHS STANDARD CONTRACT FOR VEIN OF GALEN MALFORMATION SERVICE (ALL AGES) PARTICULARS, SCHEDULE 2 THE SERVICES, A Service Specification Service Specification No. Service Commissioner
SERVICE SPECIFICATION 2 Vascular Access
 SERVICE SPECIFICATION 2 Vascular Access Table of Contents Page 1 Key Messages 1 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies with other specialties
SERVICE SPECIFICATION 2 Vascular Access Table of Contents Page 1 Key Messages 1 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies with other specialties
ANTERIOR RESECTION WHAT ARE THE BENEFITS OF HAVING AN ANTERIOR RESECTION?
 WHAT IS AN ANTERIOR RESECTION? ANTERIOR RESECTION This is an operation that is designed to remove part of your lower large bowel and then join the bowel ends back together again. This is called an anastamosis.
WHAT IS AN ANTERIOR RESECTION? ANTERIOR RESECTION This is an operation that is designed to remove part of your lower large bowel and then join the bowel ends back together again. This is called an anastamosis.
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT GMCCN SALFORD ROYAL Salford Pituitary MDT Neuroscience MDT (11-2K-4) - 2011/12 Date Self Assessment Completed 15th December 2011 Date
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT GMCCN SALFORD ROYAL Salford Pituitary MDT Neuroscience MDT (11-2K-4) - 2011/12 Date Self Assessment Completed 15th December 2011 Date
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey
 Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
Clinical Care Pathway for BRAIN TUMOURS in Childhood.
 - 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
- 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
University College Hospital. The lung cancer multidisciplinary team. Information for patients and carers
 University College Hospital The lung cancer multidisciplinary team Information for patients and carers 2 If you would like this document in another language or format, or require the services of an interpreter,
University College Hospital The lung cancer multidisciplinary team Information for patients and carers 2 If you would like this document in another language or format, or require the services of an interpreter,
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation Team YHSCN HULL AND EAST YORKSHIRE HOSPITALS Hull And East Yorkshire Hospitals Haematology MDT (13-2H-1) - 2015 Peer Review Visit
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation Team YHSCN HULL AND EAST YORKSHIRE HOSPITALS Hull And East Yorkshire Hospitals Haematology MDT (13-2H-1) - 2015 Peer Review Visit
Register No: Status: Public on ratification
 Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
St. James s Hospital, Dublin.
 Position Senior House Officer in Anaesthesia Organisational Area Department of Anaesthesia, St. James s Hospital. Closing Date Sunday the 9 th July 2018 SACC Directorate. The Surgery, Anaesthesia and Critical
Position Senior House Officer in Anaesthesia Organisational Area Department of Anaesthesia, St. James s Hospital. Closing Date Sunday the 9 th July 2018 SACC Directorate. The Surgery, Anaesthesia and Critical
North Gwent Crisis Resolution & Home Treatment Team Operational Policy
 North Gwent Crisis Resolution & Home Treatment Team Operational Policy Mission Statement The purpose of the Crisis Resolution & Home Treatment Team (CRHTT) is to provide emergency assessment and intervention
North Gwent Crisis Resolution & Home Treatment Team Operational Policy Mission Statement The purpose of the Crisis Resolution & Home Treatment Team (CRHTT) is to provide emergency assessment and intervention
Author: Kelvin Grabham, Associate Director of Performance & Information
 Trust Policy Title: Access Policy Author: Kelvin Grabham, Associate Director of Performance & Information Document Lead: Kelvin Grabham, Associate Director of Performance & Information Accepted by: RTT
Trust Policy Title: Access Policy Author: Kelvin Grabham, Associate Director of Performance & Information Document Lead: Kelvin Grabham, Associate Director of Performance & Information Accepted by: RTT
Patient Name: David Thomas Diagnosis: Cancer, Tracheostomy
 Patient Name: David Thomas Diagnosis: Cancer, Tracheostomy Overview of Scenario Simulated Patient Overview Target Audience (Part A): 2 nd year Speech Pathology students, 2 nd year Social Work students
Patient Name: David Thomas Diagnosis: Cancer, Tracheostomy Overview of Scenario Simulated Patient Overview Target Audience (Part A): 2 nd year Speech Pathology students, 2 nd year Social Work students
An introduction to the multi-disciplinary team for bowel and anal cancer
 An introduction to the multi-disciplinary team for bowel and anal cancer Providing support for patients and their families at the Royal Sussex County Hospital An introduction to the Multidisciplinary team
An introduction to the multi-disciplinary team for bowel and anal cancer Providing support for patients and their families at the Royal Sussex County Hospital An introduction to the Multidisciplinary team
Liverpool Heart and Chest Hospital NHS Foundation Trust
 Liverpool Heart and Chest Hospital NHS Foundation Trust Liverpool Heart and Chest Hospital-Vascutek Aorto-Vascular Fellowship Job Description INTRODUCTION The Thoracic Aortic Aneurysm Service at Liverpool
Liverpool Heart and Chest Hospital NHS Foundation Trust Liverpool Heart and Chest Hospital-Vascutek Aorto-Vascular Fellowship Job Description INTRODUCTION The Thoracic Aortic Aneurysm Service at Liverpool
WHY OFFER SAME DAY DISCHARGE FOR NON-RECONSTRUCTIVE BREAST CANCER SURGERY?
 WHY OFFER SAME DAY DISCHARGE FOR NON-RECONSTRUCTIVE BREAST CANCER SURGERY? Jo Marsden, Consultant Breast Surgeon, Kings College Hospital NHS Foundation Trust, London LENGTH OF STAY FOR NON-RECONSTRUCTIVE
WHY OFFER SAME DAY DISCHARGE FOR NON-RECONSTRUCTIVE BREAST CANCER SURGERY? Jo Marsden, Consultant Breast Surgeon, Kings College Hospital NHS Foundation Trust, London LENGTH OF STAY FOR NON-RECONSTRUCTIVE
St. James s Hospital, Dublin.
 Position Fellowship in Anaesthesia for Advanced Airway Management Assignment Department of Anaesthesia, St. James s Hospital. Commencement Date Monday, 09 th July, 2018. Purpose of the Post The St. James
Position Fellowship in Anaesthesia for Advanced Airway Management Assignment Department of Anaesthesia, St. James s Hospital. Commencement Date Monday, 09 th July, 2018. Purpose of the Post The St. James
CT Scanner Replacement Nevill Hall Hospital Abergavenny. Business Justification
 CT Scanner Replacement Nevill Hall Hospital Abergavenny Business Justification Version No: 3 Issue Date: 9 July 2012 VERSION HISTORY Version Date Brief Summary of Change Owner s Name Issued Draft 21/06/12
CT Scanner Replacement Nevill Hall Hospital Abergavenny Business Justification Version No: 3 Issue Date: 9 July 2012 VERSION HISTORY Version Date Brief Summary of Change Owner s Name Issued Draft 21/06/12
University College Hospital. The Specialist Centre for Head and Neck Cancer. Information for patients and carers
 University College Hospital The Specialist Centre for Head and Neck Cancer Information for patients and carers 1 Contents Page (s) 1. Introduction 2 2. Head and Neck Cancer Service at University 2 College
University College Hospital The Specialist Centre for Head and Neck Cancer Information for patients and carers 1 Contents Page (s) 1. Introduction 2 2. Head and Neck Cancer Service at University 2 College
Job Description. Job title: Uro-Oncology Clinical Nurse Specialist Band: 7
 Job Description Job title: Uro-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 37.5 (min 22.5 hrs) Reports to: Lead Nurse for Cancer We are a pioneering research active organisation
Job Description Job title: Uro-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 37.5 (min 22.5 hrs) Reports to: Lead Nurse for Cancer We are a pioneering research active organisation
Partial glossectomy. Your operation explained. Information for patients Head and Neck Centre
 Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Summarise the Impact of the Health Board Report Equality and diversity
 AGENDA ITEM 4.1 Health Board Report INTEGRATED PERFORMANCE DASHBOARD Executive Lead: Director of Planning and Performance Author: Assistant Director of Performance and Information Contact Details for further
AGENDA ITEM 4.1 Health Board Report INTEGRATED PERFORMANCE DASHBOARD Executive Lead: Director of Planning and Performance Author: Assistant Director of Performance and Information Contact Details for further
Job Description. Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7. Department: Cancer Services Hours: 30
 Job Description Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 30 Reports to: Lead Nurse for Cancer We are a pioneering research active organisation and
Job Description Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 30 Reports to: Lead Nurse for Cancer We are a pioneering research active organisation and
INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY
 St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
Survey of ERAS Nurses
 Survey of ERAS Nurses Angie Balfour & Imogen Fecher-Jones #ERASUK Objectives To investigate the variation in working hours, duties and remuneration for ERAS nursing roles in the UK. To canvas opinion on
Survey of ERAS Nurses Angie Balfour & Imogen Fecher-Jones #ERASUK Objectives To investigate the variation in working hours, duties and remuneration for ERAS nursing roles in the UK. To canvas opinion on
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation
 Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Bariatric and Metabolic Fellowship Core Curriculum for the RCS National Surgical Fellowship Scheme 1
 1 Bariatric and Metabolic Fellowship Core Curriculum for the RCS National Surgical Fellowship Scheme 1 This programme aims to enhance the delivery of metabolic surgery through world-class fellowships in
1 Bariatric and Metabolic Fellowship Core Curriculum for the RCS National Surgical Fellowship Scheme 1 This programme aims to enhance the delivery of metabolic surgery through world-class fellowships in
Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients
 Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
ANEURIN BEVAN HEALTH BOARD DELIVERING END OF LIFE CARE
 ANEURIN BEVAN HEALTH BOARD DELIVERING END OF LIFE CARE 2013-2016 1. INTRODUCTION The 5 Year NHS Plan, Together for Health, sets out the programme for health & healthcare in Wales and Together for Health
ANEURIN BEVAN HEALTH BOARD DELIVERING END OF LIFE CARE 2013-2016 1. INTRODUCTION The 5 Year NHS Plan, Together for Health, sets out the programme for health & healthcare in Wales and Together for Health
Organisational Audit Questions - Links to recommendations, standards and evidence
 Question Quoted recommendation/ standard / evidence Source Notes Section 1 - Hospital characteristics 1. a) How many adult in-patient or overnight beds (including 23- hours stay) are currently available
Question Quoted recommendation/ standard / evidence Source Notes Section 1 - Hospital characteristics 1. a) How many adult in-patient or overnight beds (including 23- hours stay) are currently available
Post Title Consultant in Palliative Medicine Inpatient Unit and Great Western Hospital
 Job Description Post Title Consultant in Palliative Medicine Inpatient Unit and Great Western Hospital Salary: Tenure: Reporting to: 76, 761-103, 490 pa pro-rata, according to level of experience Substantive.
Job Description Post Title Consultant in Palliative Medicine Inpatient Unit and Great Western Hospital Salary: Tenure: Reporting to: 76, 761-103, 490 pa pro-rata, according to level of experience Substantive.
University College Hospital. The Myeloma Cancer Multi-Disciplinary Team. University College Hospital Macmillan Cancer Centre
 University College Hospital The Myeloma Cancer Multi-Disciplinary Team University College Hospital Macmillan Cancer Centre 1 Contents Page 1. Introduction 2 2. Medical teams 3 3. Key Worker 3 4. Clinical
University College Hospital The Myeloma Cancer Multi-Disciplinary Team University College Hospital Macmillan Cancer Centre 1 Contents Page 1. Introduction 2 2. Medical teams 3 3. Key Worker 3 4. Clinical
HEALTHCARE INSPECTORATE WALES SAFEGUARDING AND PROTECTING CHILDREN IN WALES:
 HEALTHCARE INSPECTORATE WALES SAFEGUARDING AND PROTECTING CHILDREN IN WALES: A Review of the arrangements in place across the Welsh National Health Service ACTION PLAN - UPDATED August 2010 RECOMMENDATION
HEALTHCARE INSPECTORATE WALES SAFEGUARDING AND PROTECTING CHILDREN IN WALES: A Review of the arrangements in place across the Welsh National Health Service ACTION PLAN - UPDATED August 2010 RECOMMENDATION
Report to the Board of Directors 2015/16
 Attachment 9 Report to the Board of Directors 2015/16 Date of meeting 18 Subject Report of Prepared by Seven Day Services Medical Director Ashling Rivá, Project Manager Previously considered by Transformation
Attachment 9 Report to the Board of Directors 2015/16 Date of meeting 18 Subject Report of Prepared by Seven Day Services Medical Director Ashling Rivá, Project Manager Previously considered by Transformation
Board of Directors Meeting
 Board of Directors Meeting Date: 30 July 2008 Agenda item: 10.2, Part 1 Title: Prepared by: Presented by: Action required: Elaine Hobson, Director of Operations Elaine Hobson, Director of Operations The
Board of Directors Meeting Date: 30 July 2008 Agenda item: 10.2, Part 1 Title: Prepared by: Presented by: Action required: Elaine Hobson, Director of Operations Elaine Hobson, Director of Operations The
Cardio Oesophagectomy
 Cardio Oesophagectomy Information for patients Excellent Care with Compassion What is a Cardio - Oesophagectomy? It is the removal of the oesophagus (gullet) where the cancer is situated. Part of the stomach
Cardio Oesophagectomy Information for patients Excellent Care with Compassion What is a Cardio - Oesophagectomy? It is the removal of the oesophagus (gullet) where the cancer is situated. Part of the stomach
Your local NHS and you
 South Wales Programme Local Engagement Document Your local NHS and you Local NHS services in Cardiff and the Vale of Glamorgan are run by Cardiff and Vale University Health Board (UHB). The UHB is one
South Wales Programme Local Engagement Document Your local NHS and you Local NHS services in Cardiff and the Vale of Glamorgan are run by Cardiff and Vale University Health Board (UHB). The UHB is one
Elective: General Surgical - Green Service (Oncology)
 OVERVIEW The Surgical Oncology or Green Surgery service is one of the general surgery services, based at the Health Sciences Centre, but with clinics and surgery at St. Boniface General Hospital and the
OVERVIEW The Surgical Oncology or Green Surgery service is one of the general surgery services, based at the Health Sciences Centre, but with clinics and surgery at St. Boniface General Hospital and the
Meeting people s needs A Wales Cancer Alliance Policy Paper Summer 2017
 Meeting people s needs A Wales Cancer Alliance Policy Paper Summer 2017 Meeting people s needs: overview More work needs to be done to meet the needs of patients, both as they undergo treatment for cancer
Meeting people s needs A Wales Cancer Alliance Policy Paper Summer 2017 Meeting people s needs: overview More work needs to be done to meet the needs of patients, both as they undergo treatment for cancer
106,717 people accessed mental health. 192,192 access A&E. 1,011,942 patient contacts with community staff. 2,245,439 patient contacts
 Employs 15,285 2,245,439 patient contacts 192,192 Assisted 91,360 Dispensed 13,598,605 prescription items** 38,107 1,011,942 patient contacts with Across 11 clusters, 540,850 people are registered with
Employs 15,285 2,245,439 patient contacts 192,192 Assisted 91,360 Dispensed 13,598,605 prescription items** 38,107 1,011,942 patient contacts with Across 11 clusters, 540,850 people are registered with
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY
 THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
Business Case Authorisation Cover Sheet
 Business Case Authorisation Cover Sheet Section A Business Case Details Business Case Title: Directorate: Division: Sponsor Name Consultant in Anaesthesia and Pain Medicine Medicine and Rehabilitation
Business Case Authorisation Cover Sheet Section A Business Case Details Business Case Title: Directorate: Division: Sponsor Name Consultant in Anaesthesia and Pain Medicine Medicine and Rehabilitation
Mediastinal Venogram and Stent Insertion
 Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Minor Oral Surgery Service Reconfiguration
 Minor Oral Surgery Service Reconfiguration 1 Introduction The purpose of this report is to inform the Board on the status of the Minor Oral Surgery Service Reconfiguration programme and request approval
Minor Oral Surgery Service Reconfiguration 1 Introduction The purpose of this report is to inform the Board on the status of the Minor Oral Surgery Service Reconfiguration programme and request approval
Mediastinal Venogram and Stent Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients
 Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
Introduction to the lung cancer multi disciplinary team (MDT)
 Royal Berkshire NHS Foundation Trust London Road Reading Berkshire RG1 5AN 0118 322 51111 (Switchboard) www.royalberkshire.nhs.uk This document can be made available in other languages and formats upon
Royal Berkshire NHS Foundation Trust London Road Reading Berkshire RG1 5AN 0118 322 51111 (Switchboard) www.royalberkshire.nhs.uk This document can be made available in other languages and formats upon
The Royal College of Surgeons of England
 The Royal College of Surgeons of England Provision of Trauma Care Policy Briefing This policy briefing outlines the view of the Royal College of Surgeons of England in relation to the planning and provision
The Royal College of Surgeons of England Provision of Trauma Care Policy Briefing This policy briefing outlines the view of the Royal College of Surgeons of England in relation to the planning and provision
Having a sentinel lymph node biopsy and wide excision for melanoma
 Having a sentinel lymph node biopsy and wide excision for melanoma This leaflet has been given to you to help answer questions you may have about sentinel lymph node biopsy and wide excision. It explains
Having a sentinel lymph node biopsy and wide excision for melanoma This leaflet has been given to you to help answer questions you may have about sentinel lymph node biopsy and wide excision. It explains
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT EMCN UNIVERSITY HOSPITALS OF LEICESTER Leicester General Hospital Specialist Urology MDT (11-2G-2) - 2011/12 Date Self Assessment
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT EMCN UNIVERSITY HOSPITALS OF LEICESTER Leicester General Hospital Specialist Urology MDT (11-2G-2) - 2011/12 Date Self Assessment
Coroner's Corner - Inquest into the death of Gwendoline Mead
 Coroner's Corner - Inquest into the death of Gwendoline Mead Date of Findings: 22 June 2017 Coroner: Ainslie Kirkegaard Inquest Place: Brisbane Date of Death: 1 March 2015 Factual Summary: Gwendoline Mead
Coroner's Corner - Inquest into the death of Gwendoline Mead Date of Findings: 22 June 2017 Coroner: Ainslie Kirkegaard Inquest Place: Brisbane Date of Death: 1 March 2015 Factual Summary: Gwendoline Mead
Referral Guidance DIRECT REFERRAL SERVICE FOR THE ELDERLY DEAF
 Referral Guidance A & E GPs are strongly requested to contact the specialty teams DIRECTLY WHEN APPROPRIATE to avoid unnecessary delays for their patients in A & E. Relevant non-urgent conditions can be
Referral Guidance A & E GPs are strongly requested to contact the specialty teams DIRECTLY WHEN APPROPRIATE to avoid unnecessary delays for their patients in A & E. Relevant non-urgent conditions can be
Wales Critical Care & Trauma Network (North)
 Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Upper GI Cancer MCN Work Plan 2017/18
 Upper GI Cancer MCN Work Plan /18 Objective Deliverables / Outcomes Lead 1. Participation in the West of Scotland rolling programme of regional and national education events; utilising the opportunity
Upper GI Cancer MCN Work Plan /18 Objective Deliverables / Outcomes Lead 1. Participation in the West of Scotland rolling programme of regional and national education events; utilising the opportunity
STUDENT OVERVIEW AT A GLANCE
 STUDENT OVERVIEW AT A GLANCE Great North Children s Hospital and New Victoria Wing are home to the department of paediatric and teenage oncology. This consists of a children s inpatient unit (Ward 4),
STUDENT OVERVIEW AT A GLANCE Great North Children s Hospital and New Victoria Wing are home to the department of paediatric and teenage oncology. This consists of a children s inpatient unit (Ward 4),
Colorectal Multi Disciplinary Team
 Colorectal Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with Colorectal Cancer. There are many people involved in providing cancer health
Colorectal Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with Colorectal Cancer. There are many people involved in providing cancer health
PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Senior Manager, Performance and Compliance.
 Reference No: PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Trust 364 Documents to read alongside this Policy. Ministerial Letter EH/ML/004/09 WAG Rules for Managing
Reference No: PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Trust 364 Documents to read alongside this Policy. Ministerial Letter EH/ML/004/09 WAG Rules for Managing
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust NLCN BARNET AND CHASE FARM HOSPITALS Team Barnet And Chase Farm Hospitals Lcl SKIN MDT (08-2J-1) 2009/10 Peer Review Visit Date 4th February
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust NLCN BARNET AND CHASE FARM HOSPITALS Team Barnet And Chase Farm Hospitals Lcl SKIN MDT (08-2J-1) 2009/10 Peer Review Visit Date 4th February
Aneurin Bevan University Health Board Clinical Record Keeping Policy
 N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
Urology Clinical Forum. 11 th March 2015
 Urology Clinical Forum 11 th March 2015 Welcome and Introductions Justin Vale, Chair of the LCA Urology Pathway Group Progress of the Urology Pathway Group Justin Vale, Chair of the LCA Urology Pathway
Urology Clinical Forum 11 th March 2015 Welcome and Introductions Justin Vale, Chair of the LCA Urology Pathway Group Progress of the Urology Pathway Group Justin Vale, Chair of the LCA Urology Pathway
MORTALITY OF POWYS CITIZENS. Medical Director. This paper supports:
 MORTALITY OF POWYS CITIZENS QUALITY & SAFETY COMMITTEE 05 MAY 2016 AGENDA ITEM 2.2 Report of Medical Director Paper prepared by Safety & Quality Improvement Manager Purpose of Paper Action/Decision required
MORTALITY OF POWYS CITIZENS QUALITY & SAFETY COMMITTEE 05 MAY 2016 AGENDA ITEM 2.2 Report of Medical Director Paper prepared by Safety & Quality Improvement Manager Purpose of Paper Action/Decision required
Sentinel node biopsy. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Sentinel Node Biopsy What is a sentinel node biopsy? The lymphatic drainage from your
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Sentinel Node Biopsy What is a sentinel node biopsy? The lymphatic drainage from your
REFERRAL TO TREATMENT ACCESS POLICY
 Directorate of Strategy & Planning REFERRAL TO TREATMENT ACCESS POLICY Reference: DCP175 Version: 7.0 This version issued: 17/12/15 Result of last review: Major changes Date approved by owner (if applicable):
Directorate of Strategy & Planning REFERRAL TO TREATMENT ACCESS POLICY Reference: DCP175 Version: 7.0 This version issued: 17/12/15 Result of last review: Major changes Date approved by owner (if applicable):
Information for patients with gynaecological cancer. Departments of gynaecology, oncology and gynaecological oncology
 Information for patients with gynaecological cancer Departments of gynaecology, oncology and gynaecological oncology This booklet gives further information about cancers of the female reproductive system
Information for patients with gynaecological cancer Departments of gynaecology, oncology and gynaecological oncology This booklet gives further information about cancers of the female reproductive system
The investigation of a complaint by Mrs X against Aneurin Bevan Health Board. A report by the Public Services Ombudsman for Wales Case:
 The investigation of a complaint by Mrs X against Aneurin Bevan Health Board A report by the Public Services Ombudsman for Wales Case: 201302660 Contents Page Introduction 3 Summary 4 The complaint 6 Investigation
The investigation of a complaint by Mrs X against Aneurin Bevan Health Board A report by the Public Services Ombudsman for Wales Case: 201302660 Contents Page Introduction 3 Summary 4 The complaint 6 Investigation
#NeuroDis
 Each and Every Need A review of the quality of care provided to patients aged 0-25 years old with chronic neurodisability, using the cerebral palsies as examples of chronic neurodisabling conditions Recommendations
Each and Every Need A review of the quality of care provided to patients aged 0-25 years old with chronic neurodisability, using the cerebral palsies as examples of chronic neurodisabling conditions Recommendations
If you do find something out of the ordinary, bring it to the attention of the senior medical staff.
 Clerking Patients The clerk-in procedure is meant to be an independent overall assessment of a patient s condition at the time of admission. While it is good training for a trainee doctor, it is also an
Clerking Patients The clerk-in procedure is meant to be an independent overall assessment of a patient s condition at the time of admission. While it is good training for a trainee doctor, it is also an
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01
 Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Surgical Oncology II: R5 Tuesday, February 02, 2016
 Stanford University General Surgery Residency Program Surgical Oncology II Goals and Objectives for Residents: R-5 Rotation Director: Ralph Greco, MD Description The Surgical Oncology II rotation at Stanford
Stanford University General Surgery Residency Program Surgical Oncology II Goals and Objectives for Residents: R-5 Rotation Director: Ralph Greco, MD Description The Surgical Oncology II rotation at Stanford
VELINDRE NHS TRUST. Trust Procedure PROCEDURE FOR THE IMPLEMENTATION OF NATIONAL INSTITUTE OF HEALTH & CLINICAL EXCELLENCE (NICE) GUIDANCE
 Clinical Excellence (NICE) Guidance VELINDRE NHS TRUST Trust Procedure Black 21 PROCEDURE FOR THE IMPLEMENTATION OF NATIONAL INSTITUTE OF HEALTH & CLINICAL EXCELLENCE (NICE) GUIDANCE Lead: Lisa Heydon-Mann
Clinical Excellence (NICE) Guidance VELINDRE NHS TRUST Trust Procedure Black 21 PROCEDURE FOR THE IMPLEMENTATION OF NATIONAL INSTITUTE OF HEALTH & CLINICAL EXCELLENCE (NICE) GUIDANCE Lead: Lisa Heydon-Mann
