Dr Robert Scott-Jupp Consultant Paediatrician MBBS DCH MRCP FRCPCH
|
|
|
- Robyn Blankenship
- 5 years ago
- Views:
Transcription
1 Dr Robert Scott-Jupp Consultant Paediatrician MBBS DCH MRCP FRCPCH Your ref: Our ref: RSJ/ah/090212ferguson 25th February February 2013 Children s Unit Salisbury District Hospital Salisbury Wiltshire SP2 8BJ Telephone: Fax: Ext. Northern Ireland Inquiry Into Hyponatraemia Deaths Re: Raychel Ferguson Response to further witness statements received December 2012 and January I received further witness statements from medical staff involved in Raychel s acute illness, written in response to specific questions posed by the Inquiry team. I was asked whether any of these would alter the conclusions of my reports written in February In December 2012 I received statements from: Dr Mary Butler Dr Joe Devlin Dr Michael Curran (2) Dr Bernie Trainor Dr Brian McCord Dr Peter Crean Dr Donncha Hanrahan. In January 2013 I received statements from: Mrs Marie Ferguson Mr Raymond Ferguson Mr Makar Dr Gund Dr Jamison Mr Zafar Dr Allen Mr Gilliland Dr Kelly S/n Patterson S/n Noble RF - EXPERT
2 S/n McAuley nee Rice S/n Roulston S/n Gilchrist S/n Bryce Sr Millar Dr Jeremy Johnston Mr Zawislak This report replaces the draft report I wrote in December 2012 in response to the first batch of statements, and incorporates my responses to all the above statements. The statements below are limited to my responses to these witness statements, and should be considered in conjunction with my original compendium report dated 13 February ) Dr Barry Kelly Dr Kelly was the A&E SHO who initially assessed Raychel. He elicited a typical history and examination findings consistent with appendicitis. He referred her to the surgical team and she was subsequently assessed by Mr Makar. He prescribed IV Morphine (Cyclomorph) but cannot recall whether this was on the instruction of the surgeon. He did not start IV fluids. 2) Mr Ragai Makar Mr Makar was the surgical SHO who assessed and diagnosed Raychel as having acute appendicitis, and undertook the appendicectomy. Although he was not at registrar grade, it appears from his statement that he was well-qualified, fairly experienced and effectively functioning at registrar level. His consultant Mr Gilliland had confidence in his ability to assess and operate on a straightforward case of appendicitis without supervision (WS-044/2). It would have been common practice at the time for junior surgeons at this level to operate unsupervised.. He prescribed Hartmann s solution when he first saw Raychel in A&E but he recalls that this fluid was never given, because when she reached the ward at on 7/6/01, she was given 0.18% saline instead. He recalls that Hartmann s was not available on Ward 6 (WS page 6). Mr Makar prescribed the 0.18% saline himself. Although he describes why he considers Hartmann s to be preferable to 0.18% saline, he justifies giving 0.18% saline for a short period pre-operatively. He also justifies giving Raychel more than the standard maintenance quantity of IV fluid (i.e. 80 mls/hr rather than 65 mls/hr), on the basis that she may already have had a fluid deficit and in anticipation of further losses. This is reasonable: in my view 80 mls/hr was not an excessively fast infusion rate. Giving 15 mls/hr more than the standard maintenance might have been advisable to allow for extra loss of body fluid through vomiting. Mr Makar justifies the type and infusion rate of IV fluids for the pre-operative period. He does not discuss or justify continuing this fluid regime for the longer period following surgery. He did not prescribe intra- or immediate post-operative fluids for Raychel, as he considered this to be the responsibility of the anaesthetist (WS page 11). 3) Dr Vijay Gund Dr Gund was the anaesthetics SHO who undertook the general anaesthetic for Raychel s appendicectomy. He gave Hartmann s solution during the operation, and then prescribed it to be continued postoperatively. However he was told by his colleague Dr Jamison, who had been at Altnagelvin for longer, that standard ward practice was to use 0.18% saline after return to the ward, and so the prescription was changed. Although quite junior, he was considered competent to administer a general anaesthetic to a child unsupervised, which was usual practice at the time. Dr Gund s expectation was that the paediatric team would prescribe IV fluids beyond the immediate post-operative period. RF - EXPERT
3 4) Dr Claire Jamison Dr Jamison was a more experienced anaesthetics SHO who assisted her colleague Dr Gund with the GA. She recalls little and has nothing to add to Dr Gund s account. She admits that she made a retrospective addition to the anaesthetic note about the quantity of IV fluid given during the operation, and adds that her supervising consultant Dr Nesbitt advised her to do this (WS-024/2 page 5). As stated in my compendium report at 2.j, I believe that this was justified under the circumstances. 5) Dr Mary Butler Dr Butler was a junior paediatric SHO at Altnagelvin at the time. Her involvement was simply that she was asked to write a prescription continuing Raychel s IV fluid regime which had already been initiated. She prescribed continuing 0.18% Saline 4% Dextrose at 80 mls/hr. At WS-026/2 para 5e she admits that this rate was too fast. By standard calculations of maintenance fluid requirement, at 25 kg body weight Raychel should have been receiving 65 mls/hr. However as stated in my compendium report at 4.b and 4.m, Dr Butler was simply following accepted practice in continuing a fluid regime started previously, and she would have seen no reason to change this. This unquestioning continuation of what had been prescribed previously is not best practice, but nonetheless occurs frequently in many situations. Dr Butler helpfully includes, amongst other things, the Induction Booklet for paediatric SHOs from February This is mostly administrative and makes no reference at all to advice on IV fluid prescribing. This does not surprise me, as most induction guidance at the time would have looked like this. Fluids would have been considered a low priority in competition with all the many items of information that new doctors would have been expected to take on board. 6) Mr MH Zafar Mr Zafar was the surgical SHO who saw Raychel on the surgical ward round on the morning after her operation. It was the routine practice on that unit that patients on the round were not necessarily seen by the surgeon who had done the operation. He claims that he was not aware that she had vomited earlier that morning (WS-025/2 page 8). In any event he advised the nursing staff that she should be allowed small sips of oral fluids, and that the IV infusion should be continued depending on how oral fluids were tolerated. This is fairly standard advice for any first day post-op surgical case. His account suggests that the assessment of Raychel on the ward round was fairly brief. This is typical of surgical ward rounds, when there is often time pressure to see all the ward patients early in the morning before starting a full day s operating list. Surgical teams will often rely on a quick report from the nurses on the patient s condition without necessarily consulting all the charts. He had no further involvement during the day of 8/6/01, but was called urgently after Raychel had a seizure at on 9/6/01. He was unable to attend immediately because he was tied up with another seriously ill patient elsewhere. In my view, this non-attendance at that time is regrettable but not critical, as Raychel required the skills of a paediatrician, not a surgeon. In response to questions about which team had responsibility for dealing with problems as they arose in post-op children an Ward 6, there is some confusion in his replies: on p 11 he states If there were any issues about Raychel s surgical condition and general medical condition, she should have been seen by Paediatrics, and then The surgical team should be contacted if there were any surgical issues.. On p RF - EXPERT
4 18 he states Much of the day-to-day care of paediatric surgical patients, including prescribing, was undertaken by the paediatric team. This is at odds with the views expressed by several other clinicians that the primary responsibility was with the surgical team unless there was a specific medical issue. This reflects the general confusion about responsibilities which is highly pertinent to this case. 7) Dr Joe Devlin Dr Devlin was a junior house officer in surgery at Altnagelvin. Although he doesn t recall this himself, from the accounts of the nurses it appears that Raychel was not a patient under the care of his team. He was asked to help by Nurse Rice because they had been unable to contact the relevant surgical JHO, and he happened to be visiting the ward to see another patient (WS-051/2 page 15). He prescribed Ondansetron (Zofran) at about 17.30, for vomiting. He admits that he didn t consider checking her blood electrolytes then, and he didn t consider that her vomiting was significant enough to contact more senior doctors. (WS-027/2 para 4 x,y, aa). Whether this lack of action was justified depends on how severe her vomiting was considered to be, as mentioned several times in my report. In para 20 he states that he wasn t aware at the time that Raychel was suffering from prolonged vomiting 8) Dr Michael Curran Dr Curran was also a junior house officer in surgery. He became involved around when the nursing staff were concerned that Raychel was still vomiting. He prescribed Cyclizine (Valoid). He states that he is unable to recall whether he knew that Raychel had already received Zofran (WS-028/2 para 4c). It should have been clear from the drug prescription chart that Zofran had already been given. As I stated in my report (para 5.b), this is significant because the lack of any improvement after the first anti-emetic drug should have prompted a reassessment. Dr Curran s statement sheds no light on why this did not happen. At para 5 c he states that he would have believed that [the vomiting] was related to being post abdominal surgery. 9) Dr Jeremy Johnston Dr Johnston was the paediatric SHO on call on the night of 8/6/01, who was called immediately when Raychel had a seizure. He aborted the seizure with Diazepam. He correctly suspected an electrolyte abnormality and asked for blood tests. He describes some delay in getting the analysis done in the lab, but he correctly chased this up. As stated in my compendium report (para 6.h), I believe that he was justified in not changing the IV fluid regime until the result was confirmed. 10) Dr Bernie Trainor Dr Trainor was the senior (middle-grade) paediatric SHO who was called at around after Raychel had had a seizure and the low serum sodium result was known. Once the result was confirmed by a second sample, she took appropriate action in changing the IV fluids to 0.9% Saline and in reducing the infusion rate. She also, correctly, summoned Dr McCord, the duty consultant paediatrician. 11) Dr Gareth Allen Dr Allen was the anaesthetics SHO who was called to assist with the resuscitation after Raychel collapsed on 9/6/01. He has little to add regarding Raychel s management. He is the only witness to have recalled receiving any teaching on fluid balance as an undergraduate, although not specifically on hyponatraemia. RF - EXPERT
5 12) Dr Brian McCord Dr McCord was the consultant paediatrician who came in to supervise after Raychel s acute deterioration. He played little part in Raychel s immediate management, as the fluid regime had already been adjusted, she had been intubated and ventilated by the anaesthetic team, and was admitted to Intensive Care. He is unable to recall anything of relevance regarding discussions with Raychel s parents after her death. 13) Dr Peter Crean Dr Crean was the consultant anaesthetist who supervised Raychel s management after she was admitted to PICU at the RBHSC. He gives a strong opinion that Raychel s cerebral oedema and subsequent death was primarily due to hyponatraemia induced by hypotonic fluid administration. 14) Dr Donncha Hanrahan Dr Hanrahan was the Paediatric Neurologist at RBHSC who was only involved in the final stages following Raychel s transfer to PICU. He is of the same opinion as Dr Crean about the causes of her death. 15) Mr Robert Gilliland Mr Gilliland was the consultant general surgeon under whose care Raychel was admitted. Much of his statement is concerned with governance rather than clinical issues. He never saw Raychel and was not directly involved in her care. He describes the role of a consultant surgeon as he perceived it at that time. He stresses that he considered Mr Makar to be entirely competent to assess cases like Raychel, to make a diagnosis of appendicitis and to carry out surgery without the need either for supervision by, or discussion with, a more senior colleague. He considers that the symptoms and signs recorded were sufficient to indicate the need for appendicectomy. Further, he did not consider it necessary for Raychel to be seen by a consultant on the ward round the following day. In my view, by the standards of the time this was acceptable practice. He goes on to justify the later prescription of an anti-emetic by Dr Devlin at and Dr Curran at without a more detailed assessment, or calling someone more senior (WS-044/2 page 14). Here I disagree: as stated in my compendium report (4.j and 5.b), persistent vomiting so long after surgery should have been investigated more thoroughly. When Raychel deteriorated acutely on 9/6/01 he considers that the consultant surgeon on-call (which was not him) should have been called. I agree, but only because of the seriousness of the situation, rather than because of the need for any surgical intervention. Regarding whose responsibility it was to prescribe post-op IV fluids, he states specifically that it fell to the surgical pre-registration house officer (JHO). This role did not appear to be clear to all the other clinicians involved. On page 17 (para 25 d) he discusses the issue of giving extra replacement IV fluids to allow for losses through vomiting. This was and remains common practice in patients who are having significant losses from the stomach, either through vomiting or via a nasogastric tube. This does not appear to have been considered by any of the clinicians involved with Raychel. Mr Gilliland states that:..an estimation of the amount of vomiting. and replacement of that fluid with 0.9% saline or Hartmann s would have been better management. However neither an estimate of the volume of vomiting nor the use of higher solute containing fluids was common practice in the paediatric surgical unit at Altnagelvin at that time. The practice of replacing gastric losses ml for ml, with normal saline, rather than hypotonic solutions, was well-established long before 2001, at least in children. This is mentioned in standard textbooks used RF - EXPERT
6 widely at the time, e.g. Lecture Notes on General Surgery 1994 (Ref 1); Sabiston Textbook of Surgery 1997 (ref 2). However, in this case it would have required someone to make an estimate of the volume of Raychel s vomits to enable this to happen. This was not done, because none of the staff involved considered them to be large enough to justify it. 16) Mr Zawislak Mr Zawislak was the senior surgeon on-call on 7/6/01 but he denies being called and had no involvement. Nursing staff I will deal with the statements from all the Ward 6 nurses collectively, as they address much the same issues. They are Staff Nurses Patterson, Noble, Rice, Roulston, Gilchrist, Bryce and Sister Millar. All of the nurses involved were aware that the standard practice on the unit was that the routine IV fluid for children was 0.18% Saline 4% Dextrose. None of them felt that they had the knowledge or authority to challenge this. None were aware of previous problems with hyponatraemia elsewhere. None felt able to give a view on the appropriateness of the type and quantity of fluid given to Raychel. They admitted that there was incomplete recording on charts, and lack of quantification of vomit and fluid output, but in my view this is no different to what would have happened on any children s ward in the NHS at the time. S/N Noble reiterates that before Raychel s surgery she told Mr Makar that using 0.18% saline rather than Hartmann s was common practice, and the prescription was changed (WS-049/2 page 5). The nurses between them comment on the vomits that Raychel was observed to have had throughout the day on 8/6/01. Most of these appear to have been recorded on the fluid chart, but the quantity is open to question. The parents recall witnessing much larger vomits than the nurses either recall or recorded at the time. The nurses are consistent in their observations that Raychel was not sufficiently ill in herself throughout 8/6/01 to cause them concern. When the surgical JHOs were called, at and 22.00, it was just to give symptomatic relief in the form of anti-emetic drugs, not because they were concerned about more serious complications. S/N Rice noted Raychel to be up and about at around (WS-051/2 page 19 para 12). Raychel was observed by S/N Noble to be coherent and answering questions as late as (WS-049/2 page 9). This differs markedly from the parents account. They also deny that the parents expressed any particular concerns to them about Raychel s general condition other than the vomiting. Sister Millar, the senior nurse on the ward, supports all the observations and actions of her staff. She was present at the ward round, but spent much of the afternoon in her office. She describes what she would have said to the parents at the meeting after her death, but never got the opportunity. She would have said that Raychel s condition on 8/6/01 was not causing concern (WS -056/2 page 17). Parents The parents account of the quantity and frequency of Raychel s vomits is considerably in excess of that reported by the nurses, throughout the day. As their memory of exact timings is vague, it is difficult to relate what they witnessed with the nurses observations directly; however for example some time between and Mrs Ferguson reports two kidney trays full of vomit (WS page 10). None of the nurses reported this quantity of vomit. The parents recall that each time she vomited, they reported it to one of the nurses. Mrs Ferguson recalls that the vomit at around 17.00, before Dr Devlin prescribed for her, may have contained blood. This was not recorded or commented on by any of the staff. RF - EXPERT
7 RF - EXPERT
8 RF - EXPERT
BRIEF FOR CONSULTANT NEUROLOGIST RAYCHEL FERGUSON
 BRIEF FOR CONSULTANT NEUROLOGIST RAYCHEL FERGUSON Introduction 1. Raychel Ferguson is one of four children who are the subject of a public inquiry being conducted by John O Hara QC. 2. Raychel was born
BRIEF FOR CONSULTANT NEUROLOGIST RAYCHEL FERGUSON Introduction 1. Raychel Ferguson is one of four children who are the subject of a public inquiry being conducted by John O Hara QC. 2. Raychel was born
Example Care Pathways
 Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Example Care Pathways Introduction The following care pathways have been adapted from those developed to sustain provision of general surgery for children in Scotland. We have tried to avoid being too
Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery
 CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
Modified Early Warning Score Policy.
 Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Trust Policy and Procedure Modified Early Warning Score Policy. Document ref. no: PP(15)271 For use in (clinical areas): For use by (staff groups): For use for (patients): Document owner: Status: All clinical
Unless this copy has been taken directly from the Trust intranet site (Pandora) there is no assurance that this is the most up to date version
 Policy No: OP49 Version: 4.0 Name of Policy: Patient Controlled Analgesia in Adult Patients Effective From: 28/11/2017 Date Ratified 21/09/2017 Ratified Medicines Group Review Date 01/09/2019 Sponsor Director
Policy No: OP49 Version: 4.0 Name of Policy: Patient Controlled Analgesia in Adult Patients Effective From: 28/11/2017 Date Ratified 21/09/2017 Ratified Medicines Group Review Date 01/09/2019 Sponsor Director
Patient Controlled Analgesia Guidelines
 Patient Controlled Analgesia Guidelines Date: August 2005 Ref : PCD005 Vers : 2 Policy Profile Policy Reference Number PCD005 Version 2 Status Approved Trust Lead Director of Nursing/Acute Pain Team Implementation
Patient Controlled Analgesia Guidelines Date: August 2005 Ref : PCD005 Vers : 2 Policy Profile Policy Reference Number PCD005 Version 2 Status Approved Trust Lead Director of Nursing/Acute Pain Team Implementation
The Scottish Public Services Ombudsman Act 2002
 Scottish Public Services Ombudsman The Scottish Public Services Ombudsman Act 2002 Investigation Report UNDER SECTION 15(1)(a) SPSO 4 Melville Street Edinburgh EH3 7NS Tel 0800 377 7330 SPSO Information
Scottish Public Services Ombudsman The Scottish Public Services Ombudsman Act 2002 Investigation Report UNDER SECTION 15(1)(a) SPSO 4 Melville Street Edinburgh EH3 7NS Tel 0800 377 7330 SPSO Information
Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta
 Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta Abstract Introduction: Day care units are playing an increasingly important role in healthcare provision,
Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta Abstract Introduction: Day care units are playing an increasingly important role in healthcare provision,
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Independent investigation into the death of Mr John Fraser a prisoner at HMP Littlehey on 10 March 2016
 Independent investigation into the death of Mr John Fraser a prisoner at HMP Littlehey on 10 March 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr John Fraser a prisoner at HMP Littlehey on 10 March 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Health Professions Review Board
 Health Professions Review Board Suite 900, 747 Fort Street Victoria British Columbia Telephone: 250 953-4956 Toll Free: 1-888-953-4986 (within BC) Facsimile: 250 953-3195 Mailing Address: PO 9429 STN PROV
Health Professions Review Board Suite 900, 747 Fort Street Victoria British Columbia Telephone: 250 953-4956 Toll Free: 1-888-953-4986 (within BC) Facsimile: 250 953-3195 Mailing Address: PO 9429 STN PROV
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
Care of Critically Ill & Critically Injured Children in the West Midlands University Hospitals Coventry & Warwickshire NHS Trust Visit Date: 4 th December 2013 Report Date: April 2014 Images courtesy of
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
Young Peoples Transition project: Focus Group Summary
 Young Peoples Transition project: Focus Group Summary The Queen s Nursing Institute (QNI) is funded by the Burdett Trust for Nursing to deliver a programme of work to improve the experience of a young
Young Peoples Transition project: Focus Group Summary The Queen s Nursing Institute (QNI) is funded by the Burdett Trust for Nursing to deliver a programme of work to improve the experience of a young
7 NON-ELECTIVE SURGERY IN THE NHS
 Recommendations Debate whether, in the light of changes to the pattern of junior doctors working, non-essential surgery can take place during extended hours. 7 NON-ELECTIVE SURGERY IN THE NHS Ensure that
Recommendations Debate whether, in the light of changes to the pattern of junior doctors working, non-essential surgery can take place during extended hours. 7 NON-ELECTIVE SURGERY IN THE NHS Ensure that
Purpose: This document states the procedure for giving medicines via nasogastric tube, gastrostomy and jejunostomy to children in the community
 The Redway School Procedure for Administration of Medicines via External Feeding Tubes Purpose: This document states the procedure for giving medicines via nasogastric tube, gastrostomy and jejunostomy
The Redway School Procedure for Administration of Medicines via External Feeding Tubes Purpose: This document states the procedure for giving medicines via nasogastric tube, gastrostomy and jejunostomy
Time-Critical Transfer of the Sick or Injured Child (<16 years)
 LRI Emergency Department Standard Operating Procedure for: Time-Critical Transfer of the Sick or Injured Child (
LRI Emergency Department Standard Operating Procedure for: Time-Critical Transfer of the Sick or Injured Child (
North Central London Sustainability and Transformation Plan. A summary
 Sustainability and Transformation Plan A summary N C L Introduction Hospitals, local authorities, GPs, commissioners, and mental health trusts across north central London have all come together to transform
Sustainability and Transformation Plan A summary N C L Introduction Hospitals, local authorities, GPs, commissioners, and mental health trusts across north central London have all come together to transform
Inpatient Experience Survey 2016 Results for Royal Infirmary of Edinburgh
 Results for August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation in hospital
Results for August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation in hospital
Inpatient Experience Survey 2016 Results for Western General Hospital, Edinburgh
 Results for, Edinburgh August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation
Results for, Edinburgh August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation
PERSONS REFERRED TO IN THE REPORT
 Dr John Alexander Dr Trevor Anderson Consultant Anaesthetist BCH Clinical Director of Women and Children s Services Dr Philip Anslow Consultant Neuroradiologist 120 291 Dr Alison Armour Senior Registrar
Dr John Alexander Dr Trevor Anderson Consultant Anaesthetist BCH Clinical Director of Women and Children s Services Dr Philip Anslow Consultant Neuroradiologist 120 291 Dr Alison Armour Senior Registrar
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01
 Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Care of Critically Ill & Critically Injured Children in the West Midlands
 Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
Care of Critically Ill & Critically Injured Children in the West Midlands Heart of England NHS Foundation Trust Visit Date: 3 rd and 4 th October 2013 Report Date: December 2013 Images courtesy of NHS
Independent investigation into the death of Mr Stephen Woods a prisoner at HMP Liverpool on 29 April 2016
 Independent investigation into the death of Mr Stephen Woods a prisoner at HMP Liverpool on 29 April 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr Stephen Woods a prisoner at HMP Liverpool on 29 April 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
The physician associate: supporting a new role in emergency medicine
 The physician associate: supporting a new role in emergency medicine At Hairmyres Hospital in Scotland, physician associates (PAs) have become an integral part of the team in the emergency department.
The physician associate: supporting a new role in emergency medicine At Hairmyres Hospital in Scotland, physician associates (PAs) have become an integral part of the team in the emergency department.
Clinical Fellow in Paediatric Nephrology
 JOB DESCRIPTION Clinical Fellow in Paediatric Nephrology GOSH Profile Great Ormond Street Hospital for Children NHS Foundation Trust (GOSH) is a national centre of excellence in the provision of specialist
JOB DESCRIPTION Clinical Fellow in Paediatric Nephrology GOSH Profile Great Ormond Street Hospital for Children NHS Foundation Trust (GOSH) is a national centre of excellence in the provision of specialist
Contact sheet e.g SW, CPN, Nursing Home, NOK
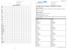 Date Time Hb Wbc Plts Hct Neuts Na K Urea Creat INR APPT CRP Tot Prot Alb Globulin Bilirubin ALT AlkPhos Gamma Amylase Phoshate Calcium Ca Corr Mag egfr BLOOD RESULTS Adult Major Burns Assessment - Integrated
Date Time Hb Wbc Plts Hct Neuts Na K Urea Creat INR APPT CRP Tot Prot Alb Globulin Bilirubin ALT AlkPhos Gamma Amylase Phoshate Calcium Ca Corr Mag egfr BLOOD RESULTS Adult Major Burns Assessment - Integrated
Financial Disclosure. Learning Objectives. Reducing GI Surgery Re-Admissions, While Increasing Patient Satisfaction
 Reducing GI Surgery Re-Admissions, While Increasing Patient Satisfaction Michelle Guibault, BSN, BS, RN Co-Author: D. Leigh Webb, MPH, CTR WellStar Health System, Marietta, GA Nothing to disclose Financial
Reducing GI Surgery Re-Admissions, While Increasing Patient Satisfaction Michelle Guibault, BSN, BS, RN Co-Author: D. Leigh Webb, MPH, CTR WellStar Health System, Marietta, GA Nothing to disclose Financial
Coroner's Corner - Inquest into the death of Gwendoline Mead
 Coroner's Corner - Inquest into the death of Gwendoline Mead Date of Findings: 22 June 2017 Coroner: Ainslie Kirkegaard Inquest Place: Brisbane Date of Death: 1 March 2015 Factual Summary: Gwendoline Mead
Coroner's Corner - Inquest into the death of Gwendoline Mead Date of Findings: 22 June 2017 Coroner: Ainslie Kirkegaard Inquest Place: Brisbane Date of Death: 1 March 2015 Factual Summary: Gwendoline Mead
West Middlesex Junior Doctors Handbook in Colorectal Surgery
 West Middlesex Junior Doctors Handbook in Colorectal Surgery Page 1 of 10 INTRODUCTION Welcome to surgery and to the colorectal team! This guide is meant to be just that, a guide and has been principally
West Middlesex Junior Doctors Handbook in Colorectal Surgery Page 1 of 10 INTRODUCTION Welcome to surgery and to the colorectal team! This guide is meant to be just that, a guide and has been principally
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER. Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow
 SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
Laparoscopic Radical Nephrectomy
 Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Inguinal hernia repair integrated care pathway (ICP)
 Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Inpatient Experience Survey 2016 Results for Dr Gray's Hospital, Elgin
 Results for, Elgin August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation in hospital
Results for, Elgin August, Official Statistics Contents Page Introduction 3 Notes of interpretation 4 Chapter 1: Rated results 6 Chapter 2: Comparison with previous surveys 28 Chapter 3: Variation in hospital
Protocol for patient controlled analgesia (PCA) with morphine in obstetrics (CG567)
 Protocol for patient controlled analgesia (PCA) with morphine in obstetrics (CG567) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee
Protocol for patient controlled analgesia (PCA) with morphine in obstetrics (CG567) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee
Inpatient Patient Experience Survey 2014 Results for NHS Grampian
 Results for August, Official Statistics Contents Page Introduction 3 Chapter 1: Rated Results 4 Chapter 2: Comparison with Previous Surveys 19 Chapter 3: Variation in NHS Board Results across 28 Chapter
Results for August, Official Statistics Contents Page Introduction 3 Chapter 1: Rated Results 4 Chapter 2: Comparison with Previous Surveys 19 Chapter 3: Variation in NHS Board Results across 28 Chapter
National Patient Experience Survey Mater Misericordiae University Hospital.
 National Patient Experience Survey 2017 Mater Misericordiae University Hospital /NPESurvey @NPESurvey Thank you! Thank you to the people who participated in the National Patient Experience Survey 2017,
National Patient Experience Survey 2017 Mater Misericordiae University Hospital /NPESurvey @NPESurvey Thank you! Thank you to the people who participated in the National Patient Experience Survey 2017,
Milton Keynes University Hospital NHS Foundation Trust
 Milton Keynes University Hospital NHS Foundation Trust Enter and View Review of Staff/ Patient Communication Ward 17 and 18 September 2017 Contents Contents... 2 1 Introduction... 3 1.1 Details of the
Milton Keynes University Hospital NHS Foundation Trust Enter and View Review of Staff/ Patient Communication Ward 17 and 18 September 2017 Contents Contents... 2 1 Introduction... 3 1.1 Details of the
Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test)
 South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
The investigation of a complaint by Ms A against Betsi Cadwaladr University Health Board
 The investigation of a complaint by Ms A against Betsi Cadwaladr University Health Board A report by the Public Services Ombudsman for Wales Case: 201504223 Contents Page Introduction 3 Summary 4 The complaint
The investigation of a complaint by Ms A against Betsi Cadwaladr University Health Board A report by the Public Services Ombudsman for Wales Case: 201504223 Contents Page Introduction 3 Summary 4 The complaint
A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum.
 Total Colectomy What is a Total Colectomy? A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum. Before an ileostomy
Total Colectomy What is a Total Colectomy? A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum. Before an ileostomy
How to conduct second line assessments. Barry Beiles-Clinical Director VASM
 How to conduct second line assessments Barry Beiles-Clinical Director VASM ASM receives notification of death Surgical case form sent to surgeon for completion by paper or Fellows Interface Completed paper
How to conduct second line assessments Barry Beiles-Clinical Director VASM ASM receives notification of death Surgical case form sent to surgeon for completion by paper or Fellows Interface Completed paper
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012
 Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
Acutely ill patients in hospital
 Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Sepsis guidance implementation advice for adults
 Sepsis guidance implementation advice for adults NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Strategy & Innovation
Sepsis guidance implementation advice for adults NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Strategy & Innovation
Referral Guidance DIRECT REFERRAL SERVICE FOR THE ELDERLY DEAF
 Referral Guidance A & E GPs are strongly requested to contact the specialty teams DIRECTLY WHEN APPROPRIATE to avoid unnecessary delays for their patients in A & E. Relevant non-urgent conditions can be
Referral Guidance A & E GPs are strongly requested to contact the specialty teams DIRECTLY WHEN APPROPRIATE to avoid unnecessary delays for their patients in A & E. Relevant non-urgent conditions can be
The Penrose Inquiry Witness Statement of Professor Philip Cachia On Topic C5
 PEN.018.0853 The Penrose Inquiry Witness Statement of Professor Philip Cachia On Topic C5 1. Current position 1.1! was appointed to my current post of Postgraduate Dean for the East of Scotland Deanery,
PEN.018.0853 The Penrose Inquiry Witness Statement of Professor Philip Cachia On Topic C5 1. Current position 1.1! was appointed to my current post of Postgraduate Dean for the East of Scotland Deanery,
Advance Health Care Planning: Making Your Wishes Known. MC rev0813
 Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
UTILIZATION MANAGEMENT Section 4. Overview The Plan s Utilization Management (UM)
 Overview The Plan s Utilization Management (UM) Program is designed to meet contractual requirements and comply with federal regulations while providing members access to high quality, cost effective medically
Overview The Plan s Utilization Management (UM) Program is designed to meet contractual requirements and comply with federal regulations while providing members access to high quality, cost effective medically
This matter was initiated by a letter from the complainant received on March 20, A response from Dr. Justin Clark was received on May 11, 2017.
 COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. Justin Clark License Number: 016409 Investigations Committee C of the College of Physicians and Surgeons
COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. Justin Clark License Number: 016409 Investigations Committee C of the College of Physicians and Surgeons
Handover of Care (Maternity) Guidelines Author s job title Lead Clinical Midwife Department Ladywell Unit. Comment / Changes / Approval
 Document Control Title Author Directorate Surgery Date Version Issued 0.1 Oct 2009 0.2 Nov 2009 1.0 Nov 2009 1.1 Feb 2010 2.0 Feb 2010 2.1 Aug 2011 2.2 Oct 2011 Handover of Care (Maternity) Guidelines
Document Control Title Author Directorate Surgery Date Version Issued 0.1 Oct 2009 0.2 Nov 2009 1.0 Nov 2009 1.1 Feb 2010 2.0 Feb 2010 2.1 Aug 2011 2.2 Oct 2011 Handover of Care (Maternity) Guidelines
Endometrial Cancer. Information for patients. Gynaecology Department. Feedback
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Survey of common practice when NGT feeding under restraint in adolescents with eating disorders
 Survey of common practice when NGT feeding under restraint in adolescents with eating disorders Sarah Fuller Specialist Eating Disorders Dietitian, Rhodes Wood Hospital Oliver Street Specialist Eating
Survey of common practice when NGT feeding under restraint in adolescents with eating disorders Sarah Fuller Specialist Eating Disorders Dietitian, Rhodes Wood Hospital Oliver Street Specialist Eating
Swindon Link Homecare
 Cleeve Hill Healthcare Limited Swindon Link Homecare Inspection report 41-51 Westlecott Road Old Town Swindon Wiltshire SN1 4EZ Date of inspection visit: 21 September 2016 Date of publication: 28 October
Cleeve Hill Healthcare Limited Swindon Link Homecare Inspection report 41-51 Westlecott Road Old Town Swindon Wiltshire SN1 4EZ Date of inspection visit: 21 September 2016 Date of publication: 28 October
Patient information. Ankle Arthroscopy. Trauma and Orthopaedic Directorate PIF 713 / V4
 Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition
 Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Abdomino-perineal Resection/Excision of the Rectum
 Abdomino-perineal Resection/Excision of the Rectum What is an Abdomino-perineal Resection/Excision of Rectum? An Abdomino-perineal Resection/Excision of Rectum is the surgical removal of part of the large
Abdomino-perineal Resection/Excision of the Rectum What is an Abdomino-perineal Resection/Excision of Rectum? An Abdomino-perineal Resection/Excision of Rectum is the surgical removal of part of the large
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey
 Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
Welcome to the Anaesthesia and Perioperative Care Prioritisation Survey We want you to nominate the most important topics for future research in anaesthesia and perioperative care. We are therefore asking
Nasogastric tube feeding
 What is nasogastric tube feeding? Nasogastric (NG) feeding is where a narrow feeding tube is placed through your nose down into your stomach. The tube can be used to give you fluids, medications and liquid
What is nasogastric tube feeding? Nasogastric (NG) feeding is where a narrow feeding tube is placed through your nose down into your stomach. The tube can be used to give you fluids, medications and liquid
It s not just Obs and Swabs!
 It s not just Obs and Swabs! Developing a pre-operative assessment service in a complex tertiary referral centre a multidisciplinary approach Emma McCone- Lead Pre op Sister Healthcare at its very best
It s not just Obs and Swabs! Developing a pre-operative assessment service in a complex tertiary referral centre a multidisciplinary approach Emma McCone- Lead Pre op Sister Healthcare at its very best
THE ROY CASTLE LUNG CANCER FOUNDATION
 Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Sample. A guide to development of a hospital blood transfusion Policy at the hospital level. Effective from April Hospital Transfusion Committee
 Sample A guide to development of a hospital blood transfusion Policy at the hospital level Name of Policy Blood Transfusion Policy Effective from April 2009 Approved by Hospital Transfusion Committee A
Sample A guide to development of a hospital blood transfusion Policy at the hospital level Name of Policy Blood Transfusion Policy Effective from April 2009 Approved by Hospital Transfusion Committee A
Maryland MOLST. Guide for Patients. Maryland MOLST Training Task Force
 Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
Patient Information. Having a Laparoscopy
 Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Elective Report. Children s Surgical Centre, Phnom Penh, Cambodia
 Elective Report Children s Surgical Centre, Phnom Penh, Cambodia I was fortunate enough to be one of two recipients of a Dr Carl Jackson Scholarship which allowed me to do my elective in Cambodia. For
Elective Report Children s Surgical Centre, Phnom Penh, Cambodia I was fortunate enough to be one of two recipients of a Dr Carl Jackson Scholarship which allowed me to do my elective in Cambodia. For
Paediatric Directorate /1791
 Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Gastroscopy. Please bring this booklet with you to your appointment. Oesophago-gastro duodenoscopy (OGD)
 Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
HIGHLAND USERS GROUP (HUG) WARD ROUNDS
 HIGHLAND USERS GROUP (HUG) WARD ROUNDS A Report on the views of Highland Users Group on what Ward Rounds are like and how they can be made more user friendly June 1997 Highland Users Group can be contacted
HIGHLAND USERS GROUP (HUG) WARD ROUNDS A Report on the views of Highland Users Group on what Ward Rounds are like and how they can be made more user friendly June 1997 Highland Users Group can be contacted
Advance Care Plan for a Child or Young Person
 Advance Care Plan for a Child or Young Person West Midlands Paediatric Palliative Care Network NHS Number: Advance Care Plan for a Child or Young Person This document is a tool for discussing and communicating
Advance Care Plan for a Child or Young Person West Midlands Paediatric Palliative Care Network NHS Number: Advance Care Plan for a Child or Young Person This document is a tool for discussing and communicating
Patient experiences of Discharge at the Royal Shrewsbury Hospital June 2016
 Patient experiences of Discharge at the Royal Shrewsbury Hospital June Chapter Introduction Healthwatch Shropshire (HWS) has received feedback on people s experience of discharge from the Royal Shrewsbury
Patient experiences of Discharge at the Royal Shrewsbury Hospital June Chapter Introduction Healthwatch Shropshire (HWS) has received feedback on people s experience of discharge from the Royal Shrewsbury
Elective Report Personal Learning Objectives and Reflections
 Manipal Teaching Hospital, Pokhara, Nepal Supervisor: Dr Asis De dr_asisde@manipalgroup.com.np Elective Report Personal Learning Objectives and Reflections Elizabeth Boyle 8/1/2013 e.z.boyle@dundee.ac.uk
Manipal Teaching Hospital, Pokhara, Nepal Supervisor: Dr Asis De dr_asisde@manipalgroup.com.np Elective Report Personal Learning Objectives and Reflections Elizabeth Boyle 8/1/2013 e.z.boyle@dundee.ac.uk
PATIENT AGREEMENT TO SYSTEMIC THERAPY: GENERIC CONSENT FORM. Patient s first names. Date of birth. Job title
 Patient identifier/label: Page 1 of 5 GENERIC CONSENT FORM Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other identifier) Male Female Special requirements
Patient identifier/label: Page 1 of 5 GENERIC CONSENT FORM Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other identifier) Male Female Special requirements
Advanced Roles and Workforce Planning. Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow
 Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
Advanced Roles and Workforce Planning Sara Dalby SFA, ANP, SCP Associate Lecturer Winston Churchill Fellow Confusion of Advanced Roles Clinical Support Worker (CSW) Nurse Practitioner (NP) Physicians Associate
Three steps to success
 Inpatient care for people with diabetes at Russells Hall Hospital (The Dudley Group NHS Foundation Trust) Three steps to success The ThinkGlucose team at Russells Hall Hospital developed a three-stage
Inpatient care for people with diabetes at Russells Hall Hospital (The Dudley Group NHS Foundation Trust) Three steps to success The ThinkGlucose team at Russells Hall Hospital developed a three-stage
Advance Directives. Important information on health care decision-making: You Have the Right to Decide
 Advance Directives Important information on health care decision-making: You Have the Right to Decide The documents provided in this package are being presented to you in accordance with the Federal Patient
Advance Directives Important information on health care decision-making: You Have the Right to Decide The documents provided in this package are being presented to you in accordance with the Federal Patient
We need to talk about Palliative Care. The Care Inspectorate
 We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet
 Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
CLAIRE ROBERTS Contents
 CLAIRE ROBERTS Contents Introduction... 124 The addition of Claire s case to the Inquiry... 125 Expert reports... 125 Schedules compiled by the Inquiry... 128 Clinical history prior to October 1996...
CLAIRE ROBERTS Contents Introduction... 124 The addition of Claire s case to the Inquiry... 125 Expert reports... 125 Schedules compiled by the Inquiry... 128 Clinical history prior to October 1996...
Ambulatory Emergency Care A Flexible Approach to Ambulatory Care at Pennine Acute Hospitals. The Pennine Acute Hospitals NHS Trust
 Ambulatory Emergency Care A Flexible Approach to Ambulatory Care at Pennine Acute Hospitals The Pennine Acute Hospitals NHS Trust A Flexible Approach to Ambulatory Care at Pennine Acute Hospitals The Pennine
Ambulatory Emergency Care A Flexible Approach to Ambulatory Care at Pennine Acute Hospitals The Pennine Acute Hospitals NHS Trust A Flexible Approach to Ambulatory Care at Pennine Acute Hospitals The Pennine
Developing an urgent care strategy for South Tees how you can have your say July/August 2015
 Developing an urgent care strategy for South Tees how you can have your say July/August 2015 Foreword Commissioning high quality, accessible urgent care services is a high priority for South Tees Clinical
Developing an urgent care strategy for South Tees how you can have your say July/August 2015 Foreword Commissioning high quality, accessible urgent care services is a high priority for South Tees Clinical
The Gynaecology Ward, The Women s Centre. Minor Surgery. Your nursing care, recovery, and getting back to normal
 The Gynaecology Ward, The Women s Centre Minor Surgery Your nursing care, recovery, and getting back to normal Contents Admission 3 Medicines 3 Visiting Hours 3 Patientline 3 Preparation for your operation
The Gynaecology Ward, The Women s Centre Minor Surgery Your nursing care, recovery, and getting back to normal Contents Admission 3 Medicines 3 Visiting Hours 3 Patientline 3 Preparation for your operation
NHS RightCare scenario: The variation between standard and optimal pathways
 NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 2: Short summary slide pack January 2018 Sarah and the sub-optimal pathway Sarah, a 70-year-old
NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 2: Short summary slide pack January 2018 Sarah and the sub-optimal pathway Sarah, a 70-year-old
Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2
 Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2 Placement The type of work to expect and learning opportunities Where the is based Clinical Supervisor(s)
Jersey General Hospital, States of Jersey Individual Placement (Job) Descriptions for Foundation Year 2 Placement The type of work to expect and learning opportunities Where the is based Clinical Supervisor(s)
Independent investigation into the death of Mr Jeffrey Rookes a prisoner at HMP Erlestoke on 14 June 2017
 Independent investigation into the death of Mr Jeffrey Rookes a prisoner at HMP Erlestoke on 14 June 2017 Crown copyright 2017 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr Jeffrey Rookes a prisoner at HMP Erlestoke on 14 June 2017 Crown copyright 2017 This publication is licensed under the terms of the Open Government Licence
Auckland District Health Board Summary 1 July 2011 to 30 June 2012 Serious and Sentinel Events
 DHB SSE Report 0 Auckland District Health Board Summary July 0 to 30 June 0 Serious and Sentinel Events There were 60 serious and sentinel events reported by ADHB in the July 0 to June 0 year. Events identified
DHB SSE Report 0 Auckland District Health Board Summary July 0 to 30 June 0 Serious and Sentinel Events There were 60 serious and sentinel events reported by ADHB in the July 0 to June 0 year. Events identified
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: Fluid Balance Policy for adult in-patient areas Version: 2 Reference Number: Supersedes Minor Amendment Author Ratification Supersedes: Version 1 Changes: See Minor Amendments
DOCUMENT CONTROL PAGE Title Title: Fluid Balance Policy for adult in-patient areas Version: 2 Reference Number: Supersedes Minor Amendment Author Ratification Supersedes: Version 1 Changes: See Minor Amendments
See the Time chapter for complete instructions on how to code using time as the controlling factor when selecting an E/M code.
 2015 EM Survival Guides Chapter 4: Initial Hospital Care (99221-99223) You should select the appropriate-level initial hospital care code (99221-99223) using the key E/M criteria of history, examination
2015 EM Survival Guides Chapter 4: Initial Hospital Care (99221-99223) You should select the appropriate-level initial hospital care code (99221-99223) using the key E/M criteria of history, examination
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY
 THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
SELF HARM RISK ASSESSMENT
 SELF HARM RISK ASSESSMENT MODULE: ASSESSING RISK OF SUICIDE & SELF- HARM TARGET: PSYCHIATRY CT1/F2/GPVTS BACKGROUND: Trainees new to Psychiatry often find themselves facing situations they have little
SELF HARM RISK ASSESSMENT MODULE: ASSESSING RISK OF SUICIDE & SELF- HARM TARGET: PSYCHIATRY CT1/F2/GPVTS BACKGROUND: Trainees new to Psychiatry often find themselves facing situations they have little
DISCHARGE AGAINST MEDICAL ADVICE (DAMA) A STUDY
 The West London Medical Journal 2010 Vol 2 No 3 pp 17-27 DISCHARGE AGAINST MEDICAL ADVICE Siba Prosad Paul 1 Rowena M. Remorin 2 ABSTRACT Objective: To establish the cause of DAMA in paediatric practice
The West London Medical Journal 2010 Vol 2 No 3 pp 17-27 DISCHARGE AGAINST MEDICAL ADVICE Siba Prosad Paul 1 Rowena M. Remorin 2 ABSTRACT Objective: To establish the cause of DAMA in paediatric practice
NHS RightCare scenario: The variation between standard and optimal pathways
 NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 1: Summary slide pack January 2018 Sarah s story This is the story of Sarah s experience
NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 1: Summary slide pack January 2018 Sarah s story This is the story of Sarah s experience
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay
 Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
Richmond Clinical Commissioning Group
 Richmond Clinical Commissioning Group South west London five year forward plan Kathryn Magson, Chief Officer, Richmond CCG 7 December 2016 South West London Five Year Forward Plan Start well, live well,
Richmond Clinical Commissioning Group South west London five year forward plan Kathryn Magson, Chief Officer, Richmond CCG 7 December 2016 South West London Five Year Forward Plan Start well, live well,
Serious Incident Report Public Board Meeting 26 November 2015
 Serious Incident Report Public Board Meeting 26 November 2015 Presented for: Presented by: Author Previous Committees Governance Yvette Oade, Chief Medical Officer Craig Brigg, Director of Quality None
Serious Incident Report Public Board Meeting 26 November 2015 Presented for: Presented by: Author Previous Committees Governance Yvette Oade, Chief Medical Officer Craig Brigg, Director of Quality None
LOUISIANA ADVANCE DIRECTIVES
 LOUISIANA ADVANCE DIRECTIVES Legal Documents that Ensure that Your Choices for Future Medical Care or the Refusal of Same are Honored and Implemented by Your Health Care Providers Peoples Health is a Medicare
LOUISIANA ADVANCE DIRECTIVES Legal Documents that Ensure that Your Choices for Future Medical Care or the Refusal of Same are Honored and Implemented by Your Health Care Providers Peoples Health is a Medicare
The investigation of a complaint by Mr D against Cwm Taf University Health Board. A report by the Public Services Ombudsman for Wales Case:
 The investigation of a complaint by Mr D against Cwm Taf University Health Board A report by the Public Services Ombudsman for Wales Case: 201604327 Contents Page Introduction 1 Summary 2 The complaint
The investigation of a complaint by Mr D against Cwm Taf University Health Board A report by the Public Services Ombudsman for Wales Case: 201604327 Contents Page Introduction 1 Summary 2 The complaint
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM FMD. Patient s first names.
 Patient identifier/label: Page 1 of 6 Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
Patient identifier/label: Page 1 of 6 Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
Why Iron? Iron is the Most prevalent micronutrient deficiency in the world (WHO 1968)
 Why Iron? Iron is the Most prevalent micronutrient deficiency in the world (WHO 1968) Iron deficiency anaemia is a Major reason for blood being transfused Iron deficiency without anaemia is 3 times as
Why Iron? Iron is the Most prevalent micronutrient deficiency in the world (WHO 1968) Iron deficiency anaemia is a Major reason for blood being transfused Iron deficiency without anaemia is 3 times as
Station Name: Mrs. Smith. Issue: Transitioning to comfort measures only (CMO)
 Station Name: Mrs. Smith Issue: Transitioning to comfort measures only (CMO) Presenting Situation: The physician will meet with Mrs. Smith s children to update them on her condition and determine the future
Station Name: Mrs. Smith Issue: Transitioning to comfort measures only (CMO) Presenting Situation: The physician will meet with Mrs. Smith s children to update them on her condition and determine the future
Patient information. Plaque Radiotherapy. St. Paul s Eye Unit PIF 529 V8
 Patient information Plaque Radiotherapy St. Paul s Eye Unit PIF 529 V8 Your Consultant / Doctor has advised you to have Plaque Radiotherapy. What is Plaque Radiotherapy? It is radiotherapy used to treat
Patient information Plaque Radiotherapy St. Paul s Eye Unit PIF 529 V8 Your Consultant / Doctor has advised you to have Plaque Radiotherapy. What is Plaque Radiotherapy? It is radiotherapy used to treat
