Safe Administration of High-Risk IV Medications
|
|
|
- Jeremy Price
- 6 years ago
- Views:
Transcription
1 Safe Administration of High-Risk IV Medications Intra- and Inter-Hospital Standardization: Drug Concentrations and Dosage Units Tool Kit Revised 2009
2 San Diego Patient Safety Council: High-Risk IV Medications Task Force Members Facilitator: Nancy Pratt, RN, MSN, Vice President Clinical Effectiveness, Sharp HealthCare Alvarado Hospital Medical Center Richard Chong Pat Craychee Lauré McWay, RN Daniel Page, BS, MS, PharmD Diana Schultz, RPh, MHSA Peggy Tilley, RN, BSN Lori Turgeon, RN Palomar Pomerado Health Susan Dempsey, RN, MN, CNS John Eastham, PharmD Catherine Konyn, RN, CNS Scripps Health Christine Low, PharmD Mark Parmenter, PharmD Pamela Richter, PharmD Contents Sharp HealthCare John Johnson, PharmD Albert Rizos, PharmD Tri-City Medical Center John Gama, PharmD Jan Weber, RN, MSN UCSD Medical Center Ellen Nyheim, RN Kim Tallian, PharmD VA San Diego Healthcare Jennifer Howard, PharmD Kimberly Quicci-Roberts, PharmD INTRODUCTION... 1 CREATING A SHARED NEED: THE CASE FOR STANDARDIZATION... 2 MOBILIZING COMMITMENT... 3 DEVELOPING A STANDARDIZED LIST... 5 STANDARDIZED LIST OF ADULT IV INFUSIONS HIGH-RISK MEDICATIONS... 6 STANDARDIZED LIST OF ADULT IV INFUSIONS OTHER MEDICATIONS... 7 PLANNING FOR IMPLEMENTATION: TIPS FROM THE FIELD... 8 MONITORING CHANGE, CELEBRATING SUCCESS REFERENCES APPENDIX: TOOLS TO DRIVE SUCCESS INVITATION: EXAMPLE PROJECT CHARTER: EXAMPLE ROLES AND RESPONSIBILITIES: EXAMPLE STAKEHOLDER SUPPORT/RESISTANCE ANALYSIS TOOL: EXAMPLE IMPLEMENTATION CHECKLIST: EXAMPLE TEMPORARY PHARMACY IV WRAPPER: EXAMPLE PRESS RELEASE: EXAMPLE This document is in the public domain and may be used and reprinted without permission provided appropriate reference is made to the San Diego Patient Safety Council and the authors of the included tools and documents. The information and tools in this document are also available in electronic format at: and Care Fusion does not accept any responsibility for the information contained in this document. Safe Administration of High-Risk IV Medications
3 Introduction Introduction As part of continuing efforts to improve patient and medication safety, in January 2005 members of the San Diego Patient Safety Council evaluated areas for local patient safety improvements. Standardization of intravenous (IV) infusion medication concentrations and dosage units with and across hospitals in San Diego County was identified as a significant opportunity to reduce morbidity and mortality due to preventable, high-risk IV-related adverse drug events. This toolkit provides the results of the work by the San Diego Patient Safety Council IV Safety Task Force, along with tools and information to assist other acute care organizations in implementing this standard approach. Goal Standardize high-risk IV drug concentrations and dosage units within and across hospitals area wide to reduce the likelihood of adverse drug events. Standardization of Intravenous (IV) Medication Administration Clinical practice will always involve some degree of variability, given the inherent variability in patients underlying pathophysiology and unique needs. Nevertheless, it is important to identify and reduce both unnecessary variability that increases opportunities for error and costs, and undesirable variability that reflects deviations from clinical guidelines and best practices. The challenge is to identify such variability, implement changes to reduce it, monitor the impact of those changes, and work to continuously improve patient safety and evidence-based care. The 2006 Institute of Medicine (IOM) report, Preventing Medication Errors, urges hospitals to take action to reduce the potential for errors. The experience of the San Diego Patient Safety Council shows that area wide standardization of high-risk IV drug concentrations and dosage units significantly reduces variability in IV therapy, helping to promote safer and more consistent practices in administering high-risk IV medications to patients. Potential Benefits Improved patient safety due to reduced complexity, variability, and opportunities for high-risk IV medication errors. Improved compliance with best practices. Extended institutional compliance with the Joint Commission and local IV medication safety goals area wide, across all hospitals and related medical services (e.g., home health, long-term care, and paramedic services). Increased clinician satisfaction due to a less complex, safer environment that is also attractive to prospective employees. Increased opportunities to drive vendor standardization and other improvements to reduce IV medication-related costs. Improved dose error reduction software data set for current or future smart pump and/or bar code administration systems. 1
4 Creating a Shared Need: The Case for Standardization Creating a Shared Need: The Case for Standardization IV Medications Are Associated With the Highest Risk Of Harm In seeking to improve patient safety, the primary focus should be on preventing errors with the greatest potential for harm. 1 Many of the highest risk medications (e.g., heparin, insulin, and narcotics) are delivered by IV infusion. 2-4 In fact, 61 percent of the most serious and life-threatening potential adverse drug events are IV drug related. 5 IV administration often results in the most serious outcomes of medication errors. 6 The Administration Process Is Vulnerable to Error Relative to the other points along the medication-use continuum, the administration process has the fewest safeguards and least support mechanisms, and it often relies on a single healthcare professional for accuracy This is because there is less opportunity to intercept these errors; administration is at the end of the process with no naturally occurring redundancies. Studies in the Intensive Care Unit found high-alert IV medication administration error rates of 34 percent 7,11 and 49 percent. 7,12 41 percent of drugadministration mortalities were associated with dosing errors. 7,13 Dosing errors were by far the most common type of medication error at 28 percent. 14 While 70 percent of ordering errors were intercepted; only 6 percent of the wrong dose errors occurring in the nurse administration stage were intercepted. 14 The second most common cause of nurse administration errors, at 13 percent, was infusion pump and delivery problems Extensive Variability Increases Opportunities for Errors High variability across the administration process is a significant contributor to errors, for instance: A key medication process problem related to administration and monitoring is incorrect dosing due to confusion among medications. 7 Nursing staff turnover rates are as high as 21.3 percent per year for some hospitals. 7 Many nurses now work in multiple settings, and both patients and nurses transfer among area hospitals. Standardization Is Supported by Patient Safety Initiatives and Research Lack of standardization has been at least a partial cause of many cases of overly high doses, including a number of fatal overdoses. 7,15,16 The need to reduce variability is a focus of Institute of Medicine (IOM, 1999) and Institute for Safe Medication Practices reports, 17 and Institute for Hospital Improvement initiatives. 18 Substantial unnecessary variation in IV medication practices is associated with increased risk of harm and therefore standardization has the potential to substantially improve IV medication safety. 19 The Joint Commission National Patient Safety Goals require a hospital to: Goal 3. Improve the safety of using medications. Goal 3b. Standardize and limit the number of drug concentrations available in the organization. 20 Management Support Is Essential Hospital-wide standardization of doses requires top-level decisions. Frontline operators, who make the errors in drug use, have limited ability to correct these systems problems on their own. 19
5 Creating a Shared Need: The Case for Standardization Need to Go Beyond Drug Concentrations In many institutions, concentration standardization is well on the way to full implementation. Moreover, in a 100-hospital sample, Bates et al found drug concentrations to be the least variable of the infusion parameters. 19 Extensive variability exists in drug dosing units, and selection of the wrong dosage unit can result in very large errors. For example, some hospitals use more than one dosage unit for heparin (e.g., units/hr and units/kg/hr) in the same patient care area. This creates opportunities for significant errors, (e.g., a 68-kg patient could receive a 68-fold overdose). Often the standard is not the same across all areas in a hospital, across hospitals in a system, or across all or even most hospitals in a given region where patients and staff may transfer. Policies, procedures, and standard work processes can provide a substantial margin of safety in minimizing variability in high-risk situations. Importantly, technology is not required to implement standardization of IV drug concentrations and dosage units. For institutions that do have or plan to implement smart pumps with dose error reduction software, standardization of drug concentrations and dosage units is an important first step in creating the necessary drug libraries. Standardization of drug dosing ranges is a logical next step in improving medication safety. The San Diego Patient Safety Council recommends the following methodology for successful IV standardization safety: Mobilizing Commitment Developing a Standardized List Planning for Implementation Monitoring Change, Celebrating Success Mobilizing Commitment Forming the Task Force The first step in developing an area wide IV safety campaign is to bring together the individual institutions in a geographic region to form a task force. The task force should be comprised of key individuals representing various roles and departments from each institution, such as: Critical Care Nurses* (from all institutions) Clinical Pharmacists* (from all institutions) Perinatal Nurses (from all institutions) Process Improvement Department Clinical Nurse Specialists/Educators Information Technology Department Pharmacy Buyers/Wholesaler Supplier Information Chief Nursing Officer/Nursing Leadership Pharmacy Leadership Intensivists Neonatologists OB-GYN Physicians Anesthesia Pharmacy and Therapeutics Committee Policy and Procedure Committee Those responsible for standard order sets Others, as needed (* = Task Force members) Developing an Elevator Speech An Elevator Speech can be used to quickly convey key elements of the IV safety campaign, for example: What: Why: We are creating area wide standards for high-risk IV infusion concentrations and dosage units in (name of designated area). This is important because there s great risk of harm associated with variation in practice. 3
6 Creating a Shared Need: The Case for Standardization Success: Success in our region will be achieved when a patient/nurse can transfer to any area or facility and the IV concentrations and dosing units will be the same. This will help reduce errors and confusion among clinicians. Need: We need your institution s support and participation in developing these community standards and rolling out the changes within your organization. Creating a Project Charter and Plan Once the task force is formed, a project charter for the IV safety campaign should be developed. This is key to establishing the scope of the campaign, keeping the team moving in the same direction, and preventing the goals and objectives from migrating during the course of the campaign. The goals and objectives should be time-specific and measurable. 21 Sample Primary Goal: Within one year, for selected common IV infusions, implement one community standard for each drug for 1) concentration and 2) dosing unit. Sample Objective: By (date) identify and engage the process-change participants representing each site and its clinicians. As part of any campaign, the following is recommended: Develop and endorse roles and schedules. Consider individual calendars to determine if adequate time is available for campaignrelated activities. Schedule all bi-weekly or monthly meetings early. Additionally, roles need to be identified specifically for executive sponsor, process owner, and change agents for each participating organization. Managing Resistance Some resistance should be expected considering the impact to daily work processes. Therefore, proactive change management efforts should be implemented, for example: Identify key stakeholders and anticipate the amount of resistance they will have, what the fundamental concerns are, and how to minimize the barriers and maximize the benefits. Be sure to validate assumptions with each stakeholder. Obtain a coalition of committed supporters. Develop a strategy to secure the support of front lines and management personnel, for example: We want our name to be on the list of the safest hospitals in the area. Communicating Effectively Early and continuous communication is essential during the IV safety campaign, such as: Select the audience(s) within the hospitals, including the various disciplines leaders especially nursing as well as those involved with pre-hospital medication administration, such as home health, longterm care, and emergency medical services. Convince them of the problem and staff benefits to result from implementing change. Use information to garner support, for example: Own knowledge of the most important medication errors MEDMARX and other medication error databases The medical literature Guidelines from Society of Critical Care Medicine, others 4
7 Creating a Shared Need: The Case for Standardization Desired Outcomes Expected outcomes for mobilizing commitment: Specific, identified sponsors (e.g., Chief Nursing Officers, Pharmacy Directors, and Pharmacy and Therapeutics Committees) are willing to give visible, active, and public commitment and support to the project. Stakeholders and task force members have the ability to direct resources to the project and are willing to provide leadership by example and to devote their personal focus, time, and passion to this effort. 22 Stakeholders and task force members agree on the story they wish to tell and have a quick, effective way to communicate that story. The task force has a clear goal, objectives, scope, and set of operating norms, and all meetings have been scheduled. The desired result (i.e., area-wide/regional standardization of IV medication concentrations and dosage units) is clear, widely understood, and shared. Tools Tools needed for mobilizing the task force and stakeholders are: Invitation Project Charter Roles and Responsibilities Stakeholder Support/Resistance Analysis Tool Examples of these tools are available in the Appendix: Tools to Drive Success on page 12. Developing a Standardized List The recommended approach to developing the standardized IV list is: Perform an area-wide inventory of medication concentrations and dosage units. Prioritize the high-risk medications: insulin, heparin, IIb/IIIa inhibitors, neuromuscular blockers, opioids, electrolytes (e.g., magnesium). Determine where variations exist in current practice. Identify by care area the drugs that need to be changed and consolidate the data to eliminate unnecessary variability. Through multiple iterations, develop an agreed-upon list of standardized concentrations and dosage units for common IV medications. In parallel with reviewing infusion standards, begin planning for education, training, and implementation. Work with stakeholders at each institution to obtain agreement on a consolidated list. Physicians may want to review and participate in standard-concentration changes, especially the anesthesia standards. Physicians should review any changes to dosage units, while specialty subcommittees can advise pharmacy and therapeutics committees. Desired Outcome The stated desired outcome is an agreed-upon list of standardized IV medication concentrations and dosage units. Tools A survey tool can help identify participating hospitals current practices regarding the administration of IV medications. The following tables provide a standardized list of adult IV infusions developed by the council. 5
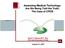
8 Creating a Shared Need: The Case for Standardization Standardized List of Adult IV Infusions High-Risk Medications DRUG Abciximab (Reopro) Eptifibatide (Integrilin) fentanyl (Sublimaze) Heparin (Warning: lookalikes: 2 units/ml vs. 50 units/ml 500 ml bags vs. Hespan) HYDROmorphone (Dilaudid) PCA or IV HIGH-RISK MEDICATIONS Antithrombotics, Electrolytes, Insulin, Opioids, Neuromuscular Blockers MIXTURE(S) Standardized rate and duration, with variable concentration being weight-based and patient specific Standard pre-mixed products (i.e., 75 mg/100ml) Varies 25,000 Units/500 ml 10 mg/50ml, 20 mg/100ml STANDARD FINAL CONCENTRATION (Single Strength) 12 hr bag, with variable concentration per patient specific, weight-based standard infusion of mcg/kg/min (max 10 mcg/min) STANDARD INFUSION RATE UNITS Flat rate 21 ml/hr; dosing units are mcg/kg/min 75 mcg/ml Mcg/kg/min IV: 10 mcg/ml (0.01 mg/ml) Non-OB epidural: 5 mcg/ml Epidural OB: 2 mcg/ml (0.02 mg/ml) (+/- bupivicaine 0.125%) IV: Mcg/hr OB: Mcg/hr 50 units/ml Units/hr 0.2 mg/ml Mg/hr Insulin 100 units/100ml 1 Unit/mL Unit/hr Magnesium Sulfate Morphine PCA or IV 20 gm/500 ml (4%) LVP OB only Otherwise, IVPB as 1 or 2 gm/50 ml, or 4gm/100ml Volume variations on a theme, depending upon device and patient needs: 50 mg/50ml, 100 mg/100 ml, 250 mg/250 ml, 300 mg/300 ml 4% LVP solution for OB use only Otherwise, IVPB as 0.02 gm/ml (2%) or 0.04 gm/ml (4%) Gm/hr 1 mg/ml Mg/hr Vecuronium 100 mg/100ml 1 mg/ml Mcg/kg/min 6
9 Creating a Shared Need: The Case for Standardization Standardized List of Adult IV Infusions Other Medications DRUG Amiodarone OTHER MEDICATIONS MIXTURE(S) Load: 150 mg/100ml Drip: 900 mg/500 ml STANDARD FINAL CONCENTRATION (Single Strength) IVPB Load: 1.5 mg/ml LVP Drip: 1.8 mg/ml STANDARD INFUSION RATE UNITS Mg/min Bumetanide Undiluted 25 mg/100 ml Undiluted 0.25 mg/ml Mg/hr DOBUTamine 500 mg/250 ml 2 mg/ml Mcg/kg/min DOPamine 400 mg/250 ml 1.6 mg/ml Mcg/kg/min EPI/CAL 2 mg epi + 1 Gm CaCl2/250 ml 8 mcg/ml Mcg/min EPINEPHrine 2 mg/250 ml 8 mcg/ml Mcg/min Esmolol (Brevibloc) 2500 mg/250ml 10 mg/ml Mcg/kg/min Furosemide 250 mg/250ml 1 mg/ml Mg/hr Isopreterenol 1 mg/250 ml 4 mcg/ml Mcg/min Labetalol 100 mg/100 ml 1 mg/ml Mg/min Lidocaine 2 gm/250 ml pre-made 8 mg/ml Mg/min LORazepam Midazolam 1 mg/ml D5W; std volume not determined 1 mg/ml D5W; std volume not determined 1 mg/ml Mg/hr 1 mg/ml Mg/hr Milrinone 20 mg/100ml pre-made 200 mcg/ml Mcg/kg/min Neosynephrine 50 mg/250 ml 200 mcg/ml Mcg/min Nesiritide 1.5mg/250ml 6 mcg/ml Mcg/kg/min nicardipine 25 mg/250 ml 0.1 mg/ml Mg/hr Nitroglycerin Glass Only 50 mg/250 ml pre-made 200 mcg/ml (0.2 mg/ml) Mcg/min Nitroprusside 50 mg/ 250 ml 200 mcg/ ml (0.2 mg/ml) Mcg/kg/min Norepinephrine (levophed) 4 mg/250 ml D5W 16 mcg/ml Mcg/min PENTobarbital 2.5 gm/500 ml 5 mg/ml Mg/hr Pitressin (vasopressin) 100 units/100ml 1 unit/ml Unit/min Procainamide 2 gm/ 250 ml 8 mg/ ml Mg/ min Propofol Undiluted Undiluted 10 mg/ ml Mcg/kg/ min Theophyllin 800 mg/500ml (pre-mixed) (1,000 mg/500 ml aminophylline) 1.6 mg/ml theo (2mg/ml aminophylline) Mg/kg/hr 7
10 Creating a Shared Need: The Case for Standardization Planning for Implementation: Tips From the Field Objective Error-free, synchronized system change implemented on a mutually determined change date/time. Standardization of high-risk IV medication concentrations and dosage units is a high-risk process change. If less than completely successful, it could result in dosage errors and serious, preventable harm to patients. Sufficient time and effort must be allocated to successfully implement the change, and activities must be well coordinated, so that staff will agree to make the changes and make the project succeed. 22 Identifying Process Owners For each site, an interdisciplinary, implementation management team is identified and ideally includes: Nurse Executive executive sponsor Pharmacist Critical Care Nurse Leader Perinatal Nurse Leader Pharmacy technician(s) to support system monitoring and IV product change-out Nurses from each affected unit Information Technology (IT) analyst(s) expert in the relevant IT systems that contain IV drug infusion dosing and concentration information such as standard orders The existing organizational departments and interdisciplinary bodies owning all the various pieces of this complex implementation must be identified. Additionally, it is necessary to include as yet non-existent, interdisciplinary bodies needed to coordinate this complex process. 8 Synchronizing System Change Within and Across Sites Effective change implementation within and across sites require coordination of these stakeholders and activities: Medication Usage: Identify the stages of the medication-use process, tools, and users potentially most impacted by these changes. Change Approval Processes: Identify the relevant change approval processes, including anticipated turnaround times for each process change (e.g., nursing and pharmacy leadership, critical care, IT, etc.). Baseline: Obtain an IV medication errors measurement baseline three to six months prior to the system change. This should be compared with a measurement with the same timeframe after go-live of the new standards. A 30-day transition between baseline and re-measure is reasonable. Timeline: Ensure all owners/approvers are on the same page at the date/time of implementation of the new standards. Policy and Procedures Committees: Identify policies that need to be changed. Update IV Medication Guidelines and any other descriptors of new standards for IV medications. Formulary/compendium: Necessary updates may require involvement of IT leadership or dedicated committees to synchronize pharmacy, nursing, computerized prescriber order entry (CPOE), and other IT systems. Medication Order Processing System: IT leadership or dedicated IT committees may need to approve updates. Order Sets: Identify preprinted and CPOE order sets that need to be changed to prevent conflicts in description of drug product and dosage units. Pharmacy and Therapeutics Committee: Established pre-approved change criteria (i.e., using standard concentration as
11 Creating a Shared Need: The Case for Standardization defined in Standard Infusion Definitions, instead of in the order sets). Thereafter, this will prevent conflicts and asynchrony between medication standards and order sets, and avoid the time-consuming, tedious, and highly error-prone task of updating and maintaining order sets. Paper: Find and replace all old order sets often a low-yield process requiring multiple cycles. Furthermore, in lieu of fully electronic documentation, print-on-demand electronic standard order forms facilitate achieving this standardization goal. However, there is added risk of each care area becoming its own print shop, creating stores of order forms. Nursing Documentation: Identify documentation forms (paper/computerized) that need to be changed (e.g., Nursing Medication Administration Record and Input and Output documentation to be updated with new dosage units). Drug Product Availability: Obtain assurance from pharmacy and vendors that any necessary new products will be available on the day of implementation of the new concentrations and reliably available thereafter through appropriate par levels. Drug Packaging: Ensure that the new concentration product is OBVIOUSLY NEW and DIFFERENT. A Pharmacy temporary wrapper should be used to alert nurses hanging the new drips. Smart pumps (if applicable): Update datasets with a unique filename communicated in the change implementation campaign and on product alert wrappers. Apply the pharmacy temporary wrapper or other product alert identifier for a long enough period after the change (i.e., two to three months, as negotiated with the nursing staff) to catch smart pumps still without the new dataset (e.g., closet pumps, rentals, etc). Ensure that software and experts are available to monitor updating of smart pump datasets with new standardized concentration and dosage units, as well as subsequent pump activation of new dataset. If manual upload of the new dataset is required, identify locations of all smart pumps. If the upload is to be done wirelessly, test the integrity of the dataset updating functionality, wireless system integrity, and scope of coverage. Communicating Start Date Clearly It is important to reinforce the momentum of the project and announce clearly, and with total management support, its imminent implementation, 21 such as: Effective (date) (or next Monday ), all employees will use the new system. Desired Outcomes Desired outcomes for implementation of the standardized list are: A clear understanding in the organization of the new system and sufficient commitment to implement it successfully. 21 Integration of the new initiative with ongoing work activities. 21 A clear sense of the official start date for the new system. 21 Tools Tools needed to implement are: Implementation Timeline Implementation Checklist Temporary Pharmacy IV Wrapper Some examples of these tools are available in the Appendix: Tools to Drive Success on page 12. 9
12 Creating a Shared Need: The Case for Standardization Monitoring Change, Celebrating Success It is important to ensure that once the change is started, it endures and flourishes, and that necessary learning and skills are transferred throughout the organization. 21 Reporting Results A baseline of IV medication errors measurements should be performed three to six months prior to the system change. Later, these should be compared with a same period of time after go-live of the new standards. A 30-day transition between baseline and re-measure is reasonable. Figures 1 and 2 show results obtained across all participating council hospitals in San Diego, California. Celebrating Success Celebrate success of area wide standardization in terms of satisfaction, service, and safety. Formal report to stakeholders, such as site quality councils, nursing leadership, etc. Public relations campaign, such as press release, newsletter article, posters, slides, web site. Desired Outcomes Expected outcomes for monitoring change and celebrating success are: Reduction in IV infusion medication errors. # Concentrations # Dosage Units Consistent, visible, and tangible reinforcement of the change initiative in the organization. 22 Sense of accomplishment shared within and across institutions. Figure 1: Elimination of Non-Standard Concentrations > > > 58 ALL MEDS (34) HIGH-RISK MEDS (9) OTHER MEDS (25) # Concentrations Before # Concentrations After Figure 2: Elimination of Non-Standard Dosage Units > > 18 9 > ALL MEDS (34) HIGH-RISK MEDS (9) OTHER MEDS (25) # Units Before # Units After 10
13 Creating a Shared Need: The Case for Standardization References 1. Williams C, Maddox RR. (2005). Implementation of an IV medication safety system. Am J Health-Syst Pharm. 62, NCC MERP taxonomy of medication errors. (1998). National Coordinating Council for Medication Error Reporting and Prevention (NCC MERP). 3. USP MEDMARX. (2001). Analysis of Participating Hospital Data. 4. Winterstein AG, Hatton RC, Gonzalez-Rothi R, et al. (2002). Identifying clinically significant preventable adverse drug events through a hospital s database of adverse drug reaction reports. Am J Health-Syst Pharm. 59, Communication with D.W. Bates, M.D., M.Sc. of Brigham & Women s Hospital in Boston, October Hicks, RW, Cousins, DD, Williams, RL. (2003). Summary of Information Submitted to MEDMARX in the Year The Quest for Quality. Rockville, MD: USP Center for the Advancement of Patient Safety. 7. Institute of Medicine. (2006). Preventing Medication Errors: Quality Chasm Series. Washington, DC: National Academies Press. PDF available at: 8. Cohen, MR. (2000). Medication Errors: Causes, Prevention, and Risk Management. Sudbury, MA: Jones and Bartlett Publishers. 9. Institute of Medicine. (2003). Priority Areas for National Action: Transforming Health Care Quality. Washington, DC: National Academy Press. 10. Institute of Medicine. (2004). Keeping Patients Safe: Transforming the Work Environment of Nurses. Washington, DC: National Academy Press. 11. Wirtz V, Taxis K, Barber ND. (2003). An observational study of intravenous medication errors in the United Kingdom and in Germany. Pharm World & Sci. 5(3), Taxis K, Barber N. (2003). Ethnographic study of incidence and severity of intravenous drug errors. Brit Med J 326(7391), Phillips J, Beam S, Brinker A, et al. (2001). Retrospective analysis of mortalities associated with medication errors. Amer J Health Syst Pharm. 58, Leape LL, Bates DW, Cullen DJ, et al. (1995). Systems analysis of adverse drug events. JAMA. 274, Institute for Safe Medication Practices. ISMP Medication Safety Alert! Cited in Bates, DW. (2005). Jt Comm J Pt Safety Qual. 31(4), Schneider PJ. (1999). A review of the safety of intravenous drug delivery systems. Hosp Pharm. 34, Cited in Bates, DW. (2005). Jt Comm J Pt Safety Qual. 31(4), ISMP Medication Safety Alert. Safety issues with patient controlled analgesia Part I How errors occur. July 10, IHI.org. 100,000 Live Campaign. Programs/Campaign/ (last accessed November 16, 2005) 19. Bates DW, Vanderveen T, Seger DL, Yamaga CC, Rothschild J. (2005). Variability in intravenous medication practices: implications for medication safety. Jt Comm J Pt Safety Qual. 31(4), JCAHO 2005 Hospitals National Patient Safety Goals. npsg/05_npsg_hap.htm 21. Palmer B. (2004). Making Change Work: Practical Tools for Overcoming Human Resistance to Change. Milwaukee, WI: ASQ Quality Press doc 11
14 Appendix: Tools To Drive Success Appendix: Tools To Drive Success The following tools are available in this appendix: Invitation: Example - This letter can be customized to invite people to join your collaborative effort. The invitation presents the goal and the process that will be followed to achieve the goal. An Agreement to participate allows people to fax back their recommendations for task force members, so that: Together we can make (area name) among the safest places in the US to receive critical healthcare. Project Charter: Example - This tool helps a task force to specify critical project elements, such as project start and length, project owner, sponsor, team members, problem statement, what success will look like, and key measurements. Roles and Responsibilities: Example - This tool specifies the common and distinct responsibilities of various task force members, such as Executive Sponsor, Process Owners, Change Agents, and Team Members. Stakeholder Support/Resistance Analysis Tool: Example - This brief process description and analysis template can be used to help identify resistance and gain support of key individuals for the project. Implementation Checklist: Example This tool is another way to check that all necessary steps have been taken for implementation of the standardized list. Pharmacy Temporary IV Wrapper - This should be used to ensure that a new concentration product is OBVIOUSLY NEW and DIFFERENT to alert nurses hanging the new standardized drips. Press Release: Example - This can be customized to communicate the work of the task force to your wider community. 12
15 Appendix: Tools To Drive Success Invitation: Example [Letterhead] (date) Re: Safe Intravenous Administration of High-Risk Medications A Collaborative Effort of the San Diego Center for Patient Safety Dear : We welcome you to join the [first] collaborative effort of the (organizing organization s name), Safe Administration of High-Risk IV Medications. This collaboration [is supported by a grant from (name) ] and is being offered to you at no charge other than your active participation. The goal of this collaboration is to help avoid medication errors and associated harm by implementing an IV infusion bundle of best practices. We hope that all hospitals and health systems in (area) will join to ensure that these best practices are routinely followed. The collaborative process will be as follows: 1. Select one or two members from your hospital to participate on the collaborative task force. These can be nurse managers, physicians, pharmacists, or administrators who have responsibility for clinical policies involving intravenous infusion of medications. 2. These representatives will attend a (name) Regional Conference on Preventing Harm Associated with High-Risk IV Medications on (date) at (location) to explore the current best practices in the safe intravenous administration of high-risk medications. 3. The task force will then meet bi-monthly for one year to develop, along with experts, the IV infusion bundle of best practices, implementation strategies for their routine use, and measurement of results. (person s name, credentials, institution) will chair the task force. (name, credentials) will serve as the task force facilitator. The (organization or person) will provide data analysis for the collaboration. Please indicate the participation of your hospital or health system in this lifesaving collaboration by signing the enclosure and listing the individuals who will represent your hospital/health system on the task force. Your participation is entirely voluntary with the intent to improve clinical practice. Thank you for your willingness to join this most important collaboration. Together we can make (area name) among the safest places in the US to receive critical healthcare. Sincerely, (name and title of organizer(s) 13
16 Appendix: Tools To Drive Success Project Charter: Example Project Start: Project Length: <Date> <Duration> Project Owner: Project Sponsor: <Name of Project Owner> <Name of Project Sponsor> Team Members: <List each team member> Problem: Increased variability in IV infusions leads to increased risk and harm What will success look like? 1. All participating organizations will have implemented the standard names, concentrations, dosage units, and safety limits 2. There will be a reduction in harm Project Scope: Develop an administration tool kit to describe the process to standardize infusion of high-risk IV medications. Must Do s: 1. Create Toolkit 2. Identify and eliminate high-risk practices Must Have: Consensus on standard names, concentrations, and dosage units Key Measurements Met: 1. Reduced harm from IV infusions 2. Implementation of standard names, concentrations, and dosage units by all participating hospitals 3. Culture survey completed 4. Reduced variability in names, concentrations, and dosage units 14
17 Appendix: Tools To Drive Success Roles and Responsibilities: Example Executive Sponsor Responsibilities Demonstrate commitment and support for project. Take responsibility and action if the project falls behind schedule or fails to bring desired results. Require the use of solid facts and data to support actions at all levels of decisionmaking. Make final decisions and make required judgment calls when conflicts arise. Assure linkage of project efforts to organizational strategies and priorities. Be prepared for and actively participate at all meetings where project sponsor is necessary (Initial Kick-off, Tollgate Reviews, and Final Report Out). Communicate project updates and expected outcomes, as appropriate, throughout the organization. Ensure speedy reviews at key decision points to accelerate decision-making, keep team members motivated, and maintain project velocity. Clearly communicate project expectations to directors, managers, and physicians. Hold the process owner and change agent accountable for: o Maintaining project scope o Providing periodic and final reports o Using effective change management strategies within the organization Provide the necessary resources (time, people, and materials) to the team. Process Owner Responsibilities Demonstrate commitment and support for project. Take responsibility and action if the project falls behind schedule or fails to bring desired results. Require the use of solid facts and data to support actions at all levels of decisionmaking. Be prepared for and facilitate (or cofacilitate with Change Agent) all meetings. Make action plan assignments to team members that are clear, specific and realistic as to the who, what, and when, and a plan for obstacles that prevent the achievement of the assignment. Communicate project updates and expected outcomes, as appropriate, throughout the organization. Ensure speedy reviews at key decision points to accelerate decision-making, keep team members motivated, and maintain project velocity. Clearly communicate project expectations to managers and team members. Maintain project scope. Provide periodic and final report. Use effective change management strategies within the organization. Use resources (time, people, and materials) efficiently. Change Agent Responsibilities Demonstrate commitment and support for project Take responsibility and action if the project falls behind schedule or fails to bring desired results. Provide solid facts and data to support actions at all levels of decision-making. Make recommendations to team for decision-making. Facilitate (or co-facilitate with process owner or champion) all meetings. Make action plan assignments to team members that are clear, specific, and realistic as to the who, what, and when, and a plan for obstacles that prevent the achievement of the assignment. 15
18 Appendix: Tools To Drive Success Recommend communication strategies to the process owner/champion. Ensure speedy reviews at key decision points to accelerate decision-making, keep team members motivated, and maintain project velocity. Maintain project scope. Provide periodic and final reports. Use effective change management strategies within the organization. Use resources (time, people, and materials) efficiently. Team Member Responsibilities Demonstrate commitment and support for project. Gain clear understanding of project assignments. Take responsibility for completing project assignments on time and communicating to process owner obstacles that prevent completion of assignments. Use solid facts and data to make decisions. Listen to, consolidate, and funnel feedback from stakeholders. Be prepared for and actively participate in decision making at all meetings. Communicate project updates and expected outcomes, as appropriate, to represented constituents. Use effective change management strategies within the organization. 16
19 Appendix: Tools To Drive Success Stakeholder Support/Resistance Analysis Tool: Example Name Strongly Agree Moderately Agree Neutral Moderately Disagree Strongly Disagree Issue Concern Win Influence Strategy Key Considerations Who are the stakeholders? Who controls the resources? Who can block the change directly or indirectly? Who must approve aspects of the change? Who owns the process? How does the stakeholder view the merits of the change initiative? How critical is each person s support to the success of the project? What is the level of attention needed for each person? (based on acceptance and criticality) What are potential issues and concerns? Technical: Costs required, lack of skills available, lack of critical resources, doubt as to outcome, etc. Political: Issues of power, authority, and relationships Cultural: Norms, mind-sets, habits, etc. What are the real, underlying issues? Can we address them? What history needs to be considered? If the stakeholder is entrenched, can we create a resolution that will let them save face? What is the stakeholder s style? How is the stakeholder best approached (1:1, informally, demo, other)? Who can best influence the stakeholder? 17
20 Appendix: Tools To Drive Success Implementation Checklist: Example When implementing the standard adult IV Infusions, be sure to perform all the following changes: Formulary/Compendium Policies and Procedures Standard work processes in IV pharmacy CPOE and standard order sets Dosing ranges and other dose-error-reduction-software (DERS) system changes IT systems, including point-of-care clinical charting, pharmacy dispensing systems, label printing system, medication ordering system, emergency department system, anesthesia system Notebooks or other hard-copy references on each nursing unit that contain standard IV infusion guidelines Orientation and preceptor documents Competency documents for annual certifications Case studies used in simulations, Advanced Cardiac Life Support, Pediatric Advanced Life Support training, and in-service education Other: 18
21 Appendix: Tools To Drive Success Temporary Pharmacy IV Wrapper: Example READ THIS FIRST!!!!! EFFECTIVE / / This is the NEW STANDARD CONCENTRATION AND DILUENT FOR HEPARIN INFUSIONS. OLD 25,000 units in 250 ml D5W (100 units/ml) NEW! (changes are underlined) 25,000 units in 500 ml ½ NS (50 units/ml) Benefits: All sites are now utilizing the same standard concentrations and diluents for their most common intravenous infusions. This will reduce the potential for user error with _(???) order entry of these infusions. To correctly use this new product, FIRST Ensure the smart pump system is updated with the new library containing this item: A. The PCU module screen should indicate (insert name of the new dataset here) B. If not, then power the unit OFF, then back ON, and wait for the green communication light (bottom left) to stop blinking, select NEW PATIENT, then perform step 1 above again. 2. Enter the Library and select this standard item. 3. Program the infusion in the defined dosage units, i.e., units/hr, NOT volume, i.e., ml/hr. 19
22 Appendix: Tools To Drive Success Press Release: Example FOR IMMEDIATE RELEASE SAN DIEGO MEDICATION SAFETY TASK FORCE CREATES UNIQUE COLLABORATION FOR SAFER USE OF INTRAVENOUS MEDICATIONS Establishing Common Practices Across Multiple Hospitals is Key to Reducing Harm; Initiative Serves as Model for Hospitals Across United States SAN DIEGO, Nov. XX, 2006 Local hospitals throughout San Diego County, along with San Diego Patient Safety Consortium and the CareFusion Center for Safety and Clinical Excellence, today announced the results of a first-of-its-kind regional task force to improve patient safety by eliminating variation in intravenous (IV) medication practices among county hospitals. The task force has created county-wide standards for safe administration of IV medicines by using a common drug identifier and standardizing the concentration and dosage units for each drug. The task force aims to make San Diego the first metropolitan area in the United States to develop and implement this new approach to significantly reduce the variation in IV therapy, resulting in safer and more consistent practices in administering high-risk IV medications to patients. The San Diego campaign for Safe Administration of High-Risk IV Medications has brought together virtually every hospital in our region to agree on IV standards that will reduce unnecessary variation among hospitals that can lead to harmful medication errors, said Nancy Pratt, Senior Vice President of Clinical Effectiveness for Sharp HealthCare and key participant in the Task Force. We hope our efforts in San Diego can serve as a model for other regions and begin to create a common standard for IV practices in hospitals across the country. The 2006 Institute of Medicine (IOM) report, Preventing Medication Errors, found that medication errors cause harm to more than 1.5 million people annually and cost hospitals more than $3.5 billion each year. The task force chose to concentrate on IV practices because 61 percent of the most serious and lifethreatening potential adverse drug events are related to IV medications 1, and the IV route of administration often results in the most serious outcomes of medication errors. 2 The report urged hospitals to take action to reduce the potential for errors, which reinforced the efforts being made by the medication safety task force in San Diego that began more than a year ago. The IOM report further points out that the most common cause of IV medication errors is the incorrect programming of infusion devices. A key problem related to drug administration is incorrect dosing due to confusion among medications and the complexity of the medication use process. The San Diego initiative focused on standardizing high-risk IV drug concentrations and dosage units within and across San Diego hospitals to reduce complexity and improve compliance with best practices. These standards improve medication safety for patients and clinicians by ensuring the safest medication process is in place regardless of the caregiver or healthcare facility. When infusion practices differ from one patient care area or hospital to another, the use of agency nurses, new graduates, traveling nurses, and nurses who change hospitals or care areas can further increase the likelihood of errors. For example, if one hospital or patient care area uses an infusion rate 1 Communication with D.W. Bates, M.D., M.Sc. of Brigham & Women's Hospital in Boston, October Hicks, RW, DD Cousins, RL Williams. (2003). Summary of Information Submitted to MEDMARX in the Year The Quest for Quality. Rockville, MD: USP Center for the Advancement of Patient Safety. 20
23 Appendix: Tools To Drive Success of milligrams per minute and another uses milligrams per hour, choosing the wrong dosage unit could result in a 60-fold overdose. San Diego County is the first region in the nation to standardize practices for safe administration of IV medications. When the task force began their work, the 15 hospitals in the San Diego task force used a combined total of more than 85 different concentrations and 57 different dosage units for 34 IV medications. Today those totals have been reduced to 34 standard, single-strength concentrations and 34 standard dosage units, effectively eliminating 100 percent of unnecessary variability in administering continuous IV infusions. Having met their goal of standardizing IV concentrations and dosage units, the task force is now working to standardize dosage ranges and drug libraries involved in the use of computerized smart pumps. While clinical practice will always involve some degree of variability, it is important to identify and reduce both unnecessary variability that increases opportunities for errors and costs, and undesirable variability that reflects deviations from clinical guidelines and best practices, said Tim Vanderveen, Vice President of CareFusion's Center for Safety and Clinical Excellence. The challenge is to identify the variability, implement changes to reduce it, monitor the impact of those changes, and use clinical data to continually improve patient safety and care. The IV Safety Task Force also created a tool kit that contains the final list of standard concentrations and dosage units, and is intended to help other regions implement similar measures to standardize IV medication practices. The tool kit also includes practical advice on forming a regional task force, identifying variations in practice across different hospitals, developing standards, and overcoming barriers that may arise during the process. In addition to patient safety benefits, the implementation of consistent IV practices is expected to help hospitals comply with measures set by the Joint Commission of Accreditation of Healthcare Organizations (JCAHO), which has identified standardization of IV concentrations as one of its National Patient Safety Goals. The tool kit will be available in mid- November at Local hospitals involved in this initiative include Alvarado Hospital Medical Center, Palomar Pomerado Health, Scripps Health, Sharp HealthCare, Tri-City Medical Center, University of California San Diego Medical Center, and VA San Diego Medical Center. # # # 21
24 Appendix: Tools To Drive Success 22
One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration
 One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration Presented by: Marla Husch Northwestern Memorial Hospital Northwestern Memorial Hospital Chicago, Illinois
One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration Presented by: Marla Husch Northwestern Memorial Hospital Northwestern Memorial Hospital Chicago, Illinois
Case Study from Parallon
 Case Study from Parallon Improving Compliance with the Smart Pump drug library across a large hospital system Part 2 Monday, July 10, 2017 AAMI Foundation Vision: To drive the safe adoption and safe use
Case Study from Parallon Improving Compliance with the Smart Pump drug library across a large hospital system Part 2 Monday, July 10, 2017 AAMI Foundation Vision: To drive the safe adoption and safe use
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach
 Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Alaris Products. Protecting patients at the point of care
 Alaris Products Protecting patients at the point of care Overview The medication process is the largest source of medical errors 1 with medication errors costing an estimated $3.5 billion yearly in hospitals.
Alaris Products Protecting patients at the point of care Overview The medication process is the largest source of medical errors 1 with medication errors costing an estimated $3.5 billion yearly in hospitals.
To prevent harm to patients from adverse medication events involving high-alert medications.
 TITLE MANAGEMENT OF HIGH-ALERT MEDICATIONS DOCUMENT # PS-46-01 PARENT DOCUMENT LEVEL LEVEL 1 PARENT DOCUMENT TITLE Management of High-alert Medications Policy APPROVAL LEVEL Alberta Health Services Executive
TITLE MANAGEMENT OF HIGH-ALERT MEDICATIONS DOCUMENT # PS-46-01 PARENT DOCUMENT LEVEL LEVEL 1 PARENT DOCUMENT TITLE Management of High-alert Medications Policy APPROVAL LEVEL Alberta Health Services Executive
Safe Medication Practices
 Safe Medication Practices Patient Safety: Preventing Adverse Events OHA Conference Renaissance Toronto Hotel at SkyDome Toronto June 14, 2004 David U President & CEO, ISMP Canada Agenda ISMP Canada Patient
Safe Medication Practices Patient Safety: Preventing Adverse Events OHA Conference Renaissance Toronto Hotel at SkyDome Toronto June 14, 2004 David U President & CEO, ISMP Canada Agenda ISMP Canada Patient
High-Risk IV Medications Dosing Limits Guidelines of Care
 San Diego Patient Safety Council High-Risk IV Medications Dosing Limits Guidelines of Care Tool Kit 2012 About This Document The purpose of this tool kit is to provide evidenced-based recommendations and
San Diego Patient Safety Council High-Risk IV Medications Dosing Limits Guidelines of Care Tool Kit 2012 About This Document The purpose of this tool kit is to provide evidenced-based recommendations and
Improving Safety Practices Anticoagulation Therapy
 Improving Safety Practices Anticoagulation Therapy Katie Cinnamon, PharmD, BCPS Clinical Pharmacist Genesis Medical Center - Davenport Objectives Review background information on medication errors and
Improving Safety Practices Anticoagulation Therapy Katie Cinnamon, PharmD, BCPS Clinical Pharmacist Genesis Medical Center - Davenport Objectives Review background information on medication errors and
Current Status: Active PolicyStat ID:
 Current Status: Active PolicyStat ID: 2002682 Origination: 05/2005 Last Approved: 02/2014 Last Revised: 02/2014 Next Review: 01/2017 Owner: Policy Area: References: Chase Walters: Director, Education Patient
Current Status: Active PolicyStat ID: 2002682 Origination: 05/2005 Last Approved: 02/2014 Last Revised: 02/2014 Next Review: 01/2017 Owner: Policy Area: References: Chase Walters: Director, Education Patient
The Colorado ALTO Project
 Using Alternatives to Opioids (ALTOs) in Hospital Emergency Departments PRE-LAUNCH CHECKLIST Based on the 2017 Opioid Prescribing & Treatment Guidelines Colorado ALTO Project Champion Sets the direction
Using Alternatives to Opioids (ALTOs) in Hospital Emergency Departments PRE-LAUNCH CHECKLIST Based on the 2017 Opioid Prescribing & Treatment Guidelines Colorado ALTO Project Champion Sets the direction
Anatomy of a Fatal Medication Error
 Anatomy of a Fatal Medication Error Pamela A. Brown, RN, CCRN, PhD Nurse Manager Pediatric Intensive Care Unit Doernbecher Children s Hospital Objectives Discuss the components of a root cause analysis
Anatomy of a Fatal Medication Error Pamela A. Brown, RN, CCRN, PhD Nurse Manager Pediatric Intensive Care Unit Doernbecher Children s Hospital Objectives Discuss the components of a root cause analysis
Background and Methodology
 Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
Medication Math Homework Part 1. Part A. Convert the following patient weights from pounds to kilograms lbs lbs. 6.
 Medication Math Homework Part 1 Part A. Convert the following patient weights from pounds to kilograms 1. 22 lbs 4. 150 lbs 7. 250 lbs 2. 80 lbs 5. 180 lbs 8. 300 lbs 3. 100 6. 200 lbs 9. 35 lbs Part B.
Medication Math Homework Part 1 Part A. Convert the following patient weights from pounds to kilograms 1. 22 lbs 4. 150 lbs 7. 250 lbs 2. 80 lbs 5. 180 lbs 8. 300 lbs 3. 100 6. 200 lbs 9. 35 lbs Part B.
Medication Safety & Electrolyte Administration. Objectives. High Alert Medications. *Med Safety Electrolyte Administration
 Medication Safety & Electrolyte Administration Jennifer Doughty, PharmD PGY2 Pharmacy Resident Emergency Medicine Stormont Vail Health, Topeka, KS Objectives Define and identify high alert medications
Medication Safety & Electrolyte Administration Jennifer Doughty, PharmD PGY2 Pharmacy Resident Emergency Medicine Stormont Vail Health, Topeka, KS Objectives Define and identify high alert medications
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE)
 COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
Medication Safety Technology The Good, the Bad and the Unintended Consequences
 Medication Safety Technology The Good, the Bad and the Unintended Consequences Michelle Mandrack RN, MSN Director of Consulting Services Matthew Fricker, RPh, MS Program Director 1 Objectives Consider
Medication Safety Technology The Good, the Bad and the Unintended Consequences Michelle Mandrack RN, MSN Director of Consulting Services Matthew Fricker, RPh, MS Program Director 1 Objectives Consider
Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use
 Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use Our vision is to create a culture where patients and those who care for them are
Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use Our vision is to create a culture where patients and those who care for them are
OHTAC Recommendation. Implementation and Use of Smart Medication Delivery Systems
 OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
Disclosure. Institute of Medicine (IOM) 1,2. Objectives 5/15/2014. Technician Education Day May 24, 2014 Ft. Lauderdale, FL
 Technician Education Day May 24, 2014 Ft. Lauderdale, FL The Pharmacy Technician s Role in Keeping Our Patients Safe Antonia Zapantis, MS, PharmD, BCPS Associate Professor, Nova Southeastern University
Technician Education Day May 24, 2014 Ft. Lauderdale, FL The Pharmacy Technician s Role in Keeping Our Patients Safe Antonia Zapantis, MS, PharmD, BCPS Associate Professor, Nova Southeastern University
Medication Safety Dashboard
 How Safe Are Your Patients? Creating a Meaningful & Actionable Medication Safety Dashboard By: Helga Brake, PharmD, CPHQ Patient Safety Leader Northwestern Memorial Hospital No Conflicts of Interest to
How Safe Are Your Patients? Creating a Meaningful & Actionable Medication Safety Dashboard By: Helga Brake, PharmD, CPHQ Patient Safety Leader Northwestern Memorial Hospital No Conflicts of Interest to
Medication Safety Action Bundle Adverse Drug Events (ADE) All High-Risk Medication Safety
 Medication Safety Action Bundle Adverse Drug Events (ADE) All High-Risk Medication Safety Background The Institute of medicine (IOM) estimates that 1.5 million preventable Adverse Drug Events (ADE) occur
Medication Safety Action Bundle Adverse Drug Events (ADE) All High-Risk Medication Safety Background The Institute of medicine (IOM) estimates that 1.5 million preventable Adverse Drug Events (ADE) occur
Considerations for Sterile Compounding of Parenteral Products for Pediatric Use: Part 2 PharMEDium Lunch and Learn Series LUNCH AND LEARN
 LUNCH AND LEARN Considerations for Sterile Compounding of Parenteral Products for Pediatric Use: Part 2 November 10, 2017 Featured Speaker: Kirsten H. Ohler, PharmD, BCPS, BCPPS Neonatal / Pediatric Clinical
LUNCH AND LEARN Considerations for Sterile Compounding of Parenteral Products for Pediatric Use: Part 2 November 10, 2017 Featured Speaker: Kirsten H. Ohler, PharmD, BCPS, BCPPS Neonatal / Pediatric Clinical
Preventing Adverse Drug Events and Harm
 Preventing Adverse Drug Events and Harm Frank Federico, RPh, IHI Executive Director Steve Meisel, PharmD, IHI Faculty March 27th,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH, Institute
Preventing Adverse Drug Events and Harm Frank Federico, RPh, IHI Executive Director Steve Meisel, PharmD, IHI Faculty March 27th,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH, Institute
High-Alert Medications (HAM)
 Approved by: Vice President & Chief Medical Officer, and Vice President & Chief Operating Officer High-Alert Medications (HAM) Corporate Policy & Procedures Manual Number: VII-A-30 Date Approved November
Approved by: Vice President & Chief Medical Officer, and Vice President & Chief Operating Officer High-Alert Medications (HAM) Corporate Policy & Procedures Manual Number: VII-A-30 Date Approved November
Objectives. Key Elements. ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management 5/20/2014
 ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
IMPACT OF TECHNOLOGY ON MEDICATION SAFETY
 Continuous Quality Improvement IMPACT OF Steven R. Abel, PharmD, FASHP TECHNOLOGY ON Nital Patel, PharmD. MBA MEDICATION SAFETY Sheri Helms, PharmD Candidate Brian Heckman, PharmD Candidate Ismaila D Badjie
Continuous Quality Improvement IMPACT OF Steven R. Abel, PharmD, FASHP TECHNOLOGY ON Nital Patel, PharmD. MBA MEDICATION SAFETY Sheri Helms, PharmD Candidate Brian Heckman, PharmD Candidate Ismaila D Badjie
POLICY. Clinician is any health care professional accepting responsibility for care of patients and their medications.
 POLICY Number: 7311-60-020 Title: HIGH ALERT MEDICATIONS IDENTIFICATION, DOUBLE CHECK AND LABELING Authorization [ ] President and CEO [X ] Vice President, Finance and Corporate Services Source: Chair,
POLICY Number: 7311-60-020 Title: HIGH ALERT MEDICATIONS IDENTIFICATION, DOUBLE CHECK AND LABELING Authorization [ ] President and CEO [X ] Vice President, Finance and Corporate Services Source: Chair,
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center
 Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Improving Staff Education
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Improving Staff Education
I ntravenous (IV) medication errors have led to considerable
 80 ORIGINAL ARTICLE Insights from the sharp end of intravenous medication errors: implications for infusion pump technology M Husch, C Sullivan, D Rooney, C Barnard, M Fotis, J Clarke, G skin... See end
80 ORIGINAL ARTICLE Insights from the sharp end of intravenous medication errors: implications for infusion pump technology M Husch, C Sullivan, D Rooney, C Barnard, M Fotis, J Clarke, G skin... See end
Measuring medication safety with smart IV systems
 Measuring medication safety with smart IV systems Introduction Inter-professional conference on intravenous medication safety: Measuring medication safety with smart IV systems The fourth invitational
Measuring medication safety with smart IV systems Introduction Inter-professional conference on intravenous medication safety: Measuring medication safety with smart IV systems The fourth invitational
Profiles in CSP Insourcing: Tufts Medical Center
 Profiles in CSP Insourcing: Tufts Medical Center Melissa A. Ortega, Pharm.D., M.S. Director, Pediatrics and Inpatient Pharmacy Operations Tufts Medical Center Hospital Profile Tufts Medical Center (TMC)
Profiles in CSP Insourcing: Tufts Medical Center Melissa A. Ortega, Pharm.D., M.S. Director, Pediatrics and Inpatient Pharmacy Operations Tufts Medical Center Hospital Profile Tufts Medical Center (TMC)
University of Mississippi Medical Center University of Mississippi Health Care. Pharmacy and Therapeutics Committee Medication Use Evaluation
 University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
Nursing Dosage Calculations Conversions Practice
 Conversions Practice Free PDF ebook Download: Conversions Practice Download or Read Online ebook nursing dosage calculations conversions practice in PDF Format From The Best User Guide Database NURSING
Conversions Practice Free PDF ebook Download: Conversions Practice Download or Read Online ebook nursing dosage calculations conversions practice in PDF Format From The Best User Guide Database NURSING
SHRI GURU RAM RAI INSTITUTE OF TECHNOLOGY AND SCIENCE MEDICATION ERRORS
 MEDICATION ERRORS Patients depend on health systems and health professionals to help them stay healthy. As a result, frequently patients receive drug therapy with the belief that these medications will
MEDICATION ERRORS Patients depend on health systems and health professionals to help them stay healthy. As a result, frequently patients receive drug therapy with the belief that these medications will
Session 2 Improving Narcotics and Opiate Management
 Session 2 Improving Narcotics and Opiate Management Frank Federico, RPh, IHI Executive Director Steve Meisel, Pharm.D., IHI Faculty January 31,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH,
Session 2 Improving Narcotics and Opiate Management Frank Federico, RPh, IHI Executive Director Steve Meisel, Pharm.D., IHI Faculty January 31,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH,
End-to-end infusion safety. Safely manage infusions from order to administration
 End-to-end infusion safety Safely manage infusions from order to administration New demands and concerns 56% 7% of medication errors are IV-related. 1 of high-risk IVs are compounded in error. 2 $3.5B
End-to-end infusion safety Safely manage infusions from order to administration New demands and concerns 56% 7% of medication errors are IV-related. 1 of high-risk IVs are compounded in error. 2 $3.5B
Required Organizational Practices Resources for 2016
 Required Organizational Practices Resources for 2016 ROPs Tests for Compliance Things to Consider Available Resources CLIENT IDENTIFICATION Working in partnership with clients and families, at least two
Required Organizational Practices Resources for 2016 ROPs Tests for Compliance Things to Consider Available Resources CLIENT IDENTIFICATION Working in partnership with clients and families, at least two
student interests. The 1. Develop of error schema. develop
 Sample Medication Safety APPE Student Rotation Rotation Description The medication safety rotation willl help students become familiar with the key principles utilized in hospitals and health systems to
Sample Medication Safety APPE Student Rotation Rotation Description The medication safety rotation willl help students become familiar with the key principles utilized in hospitals and health systems to
The Institute of Medicine concluded that medical
 Hosp Pharm 2015;50(2):113 117 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-113 Original Article Optimizing Smart Pump Technology by Increasing Critical Safety Alerts
Hosp Pharm 2015;50(2):113 117 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-113 Original Article Optimizing Smart Pump Technology by Increasing Critical Safety Alerts
Safer use of anticoagulants: the NPSA patient safety alert Steve Chaplin MSc, MRPharmS
 Safer use of anticoagulants: the NPSA patient safety alert Steve Chaplin MSc, MRPharmS Steve Chaplin describes the NPSA s anticoagulant patient safety alert and the measures it recommends for making the
Safer use of anticoagulants: the NPSA patient safety alert Steve Chaplin MSc, MRPharmS Steve Chaplin describes the NPSA s anticoagulant patient safety alert and the measures it recommends for making the
(10+ years since IOM)
 Medication Errors We're Looking Down the Tunnel and Seeing Light (10+ years since IOM) Michael R. Cohen, RPh, MS, ScD Institute for Safe Medication Practices mcohen@ismp.org 1 Disclosure Information Michael
Medication Errors We're Looking Down the Tunnel and Seeing Light (10+ years since IOM) Michael R. Cohen, RPh, MS, ScD Institute for Safe Medication Practices mcohen@ismp.org 1 Disclosure Information Michael
Managing Pharmaceuticals to Reduce Medication Errors August 26, 2003
 Managing Pharmaceuticals to Reduce Medication Errors August 26, 2003 Susan M. Proulx, Pharm.D. President, Med-E.R.R.S. Subsidiary of ISMP (www.med-errs.com) Mission of ISMP Translate errors into education
Managing Pharmaceuticals to Reduce Medication Errors August 26, 2003 Susan M. Proulx, Pharm.D. President, Med-E.R.R.S. Subsidiary of ISMP (www.med-errs.com) Mission of ISMP Translate errors into education
Importance of Clinical Leadership in Pharmacy
 Importance of Clinical Leadership in Pharmacy Rita Shane, Pharm.D., FASHP, FCSHP Chief Pharmacy Officer Cedars-Sinai Medical Center, Los Angeles Assistant Dean, Clinical Pharmacy UCSF School of Pharmacy
Importance of Clinical Leadership in Pharmacy Rita Shane, Pharm.D., FASHP, FCSHP Chief Pharmacy Officer Cedars-Sinai Medical Center, Los Angeles Assistant Dean, Clinical Pharmacy UCSF School of Pharmacy
Re-Engineering Medication Processes to Capitalize on Technology. Jane Englebright, PhD, RN Vice President, Quality HCA
 Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
Objectives. Demographics: Type and Services 1/22/2014. ICAHN Aggregate Results. ISMP Medication Safety Self Assessment for Hospitals
 ICAHN Aggregate Results ISMP Medication Safety Self Assessment for Hospitals Matthew Fricker, RPH, MS, FASHP Rebecca Lamis, PharmD, FISMP January 23, 2014 1 Objectives Report the demographic characteristics
ICAHN Aggregate Results ISMP Medication Safety Self Assessment for Hospitals Matthew Fricker, RPH, MS, FASHP Rebecca Lamis, PharmD, FISMP January 23, 2014 1 Objectives Report the demographic characteristics
PROCESS FOR HANDLING ELASTOMERIC PAIN RELIEF BALLS (ON-Q PAINBUSTER AND OTHERS)
 PROCESS FOR HANDLING ELASTOMERIC PAIN RELIEF BALLS (ON-Q PAINBUSTER AND OTHERS) REQUIRES SAFETY IMPROVEMENTS From the July 16, 2009 issue Problem: In our May 21, 2009, newsletter we noted an association
PROCESS FOR HANDLING ELASTOMERIC PAIN RELIEF BALLS (ON-Q PAINBUSTER AND OTHERS) REQUIRES SAFETY IMPROVEMENTS From the July 16, 2009 issue Problem: In our May 21, 2009, newsletter we noted an association
Overview. Improving Safety with Health Information Technology. Prioritizing Safety. Question 22/10/2013
 Improving Safety with Health Information Technology ISQua 2013, Edinburgh David Bates, MD, MSc Chief Quality Officer, Chief, Division of General Internal Medicine, Brigham and Women s Hospital Medical
Improving Safety with Health Information Technology ISQua 2013, Edinburgh David Bates, MD, MSc Chief Quality Officer, Chief, Division of General Internal Medicine, Brigham and Women s Hospital Medical
Medication Safety in the Operating Room: Using the Operating Room Medication Safety Checklist
 Medication Safety in the Operating Room: Using the Operating Room Medication Safety Checklist CPSI Safe Surgery Saves Lives Workshop Montréal, QC 29Mar2011 Julie Greenall, RPh, BScPhm, MHSc, FISMPC Institute
Medication Safety in the Operating Room: Using the Operating Room Medication Safety Checklist CPSI Safe Surgery Saves Lives Workshop Montréal, QC 29Mar2011 Julie Greenall, RPh, BScPhm, MHSc, FISMPC Institute
JCAHO Med Management
 Hospital Pharmacy Volume 41, Number 9, pp 888 892 2006 Wolters Kluwer Health, Inc. JCAHO Med Management Meeting the Standards for Emergency Medications and Labeling Patricia C. Kienle, MPA, FASHP* This
Hospital Pharmacy Volume 41, Number 9, pp 888 892 2006 Wolters Kluwer Health, Inc. JCAHO Med Management Meeting the Standards for Emergency Medications and Labeling Patricia C. Kienle, MPA, FASHP* This
Achieving safety in medication management through barcoding technology
 Achieving safety in medication management through barcoding technology Kara Marx, RN, FACHE, FHIMSS Vice President of Information Services Sharp Healthcare. SESSION OBJECTIVES Describe the primary activities
Achieving safety in medication management through barcoding technology Kara Marx, RN, FACHE, FHIMSS Vice President of Information Services Sharp Healthcare. SESSION OBJECTIVES Describe the primary activities
Plum 360 TM Infusion System with Full IV-EHR Interoperability
 Plum 360 TM Infusion System with Full IV-EHR Interoperability Your Direct Connection To Clinical Excellence > Air management that doesn t require disconnecting from the patient > A secondary line that
Plum 360 TM Infusion System with Full IV-EHR Interoperability Your Direct Connection To Clinical Excellence > Air management that doesn t require disconnecting from the patient > A secondary line that
Policy Statement Medication Order Legibility Medication orders will be written in a manner that provides a clearly legible prescription.
 POLICY POLICY PURPOSE: The purpose of this policy is to provide a foundation for safe communication of medication and nutritional orders in-scope, thereby reducing the potential for preventable medication
POLICY POLICY PURPOSE: The purpose of this policy is to provide a foundation for safe communication of medication and nutritional orders in-scope, thereby reducing the potential for preventable medication
Alaris System. Medication safety system focused at the point of care
 Alaris System Medication safety system focused at the point of care A safety platform you can build on TM Different care areas have different needs. That s why the Alaris System* gives you a platform you
Alaris System Medication safety system focused at the point of care A safety platform you can build on TM Different care areas have different needs. That s why the Alaris System* gives you a platform you
N ATIONAL Q UALITY F ORUM. Safe Practices for Better Healthcare 2006 Update A CONSENSUS REPORT
 N ATIONAL Q UALITY F ORUM Safe Practices for Better Healthcare 2006 Update A CONSENSUS REPORT NATIONAL QUALITY FORUM Foreword Every person who seeks care in a healthcare facility should expect to receive
N ATIONAL Q UALITY F ORUM Safe Practices for Better Healthcare 2006 Update A CONSENSUS REPORT NATIONAL QUALITY FORUM Foreword Every person who seeks care in a healthcare facility should expect to receive
Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016
 Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016 DISCLOSURE STATEMENT I have nothing to disclose regarding
Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016 DISCLOSURE STATEMENT I have nothing to disclose regarding
High Alert Medications: Reducing Patient Harm
 High Alert Medications: Reducing Patient Harm Building a Bridge to Better Health Coalition Brian D. Esters, PharmD, CPPS Assistant Professor of Pharmacy Practice Tennessee Pharmacist Coalition Vision Reduce
High Alert Medications: Reducing Patient Harm Building a Bridge to Better Health Coalition Brian D. Esters, PharmD, CPPS Assistant Professor of Pharmacy Practice Tennessee Pharmacist Coalition Vision Reduce
Hospital Self Assessment Worksheet
 DESCRIPTION AND INSTRUCTIONS This worksheet consists of 106 questions assessing adoption of the Hospital Self- Assessment recommendations at the hospital level. These recommendations were based on the
DESCRIPTION AND INSTRUCTIONS This worksheet consists of 106 questions assessing adoption of the Hospital Self- Assessment recommendations at the hospital level. These recommendations were based on the
Assessing Medical Technology- Are We Being Told the Truth. The Case of CPOE. David C Classen M.D., M.S. FCG and University of Utah
 Assessing Medical Technology- Are We Being Told the Truth. The Case of CPOE David C Classen M.D., M.S. FCG and University of Utah August 21, 2007 FCG 2006 Slide 1 November 2006 CPOE Adoption Growing Despite
Assessing Medical Technology- Are We Being Told the Truth. The Case of CPOE David C Classen M.D., M.S. FCG and University of Utah August 21, 2007 FCG 2006 Slide 1 November 2006 CPOE Adoption Growing Despite
5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014
 5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014 EVALUATION OF INTRAVENOUS MEDICATION ERRORS WITH INFUSION PUMPS Eija Kivekäs, MSc, RN,
5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014 EVALUATION OF INTRAVENOUS MEDICATION ERRORS WITH INFUSION PUMPS Eija Kivekäs, MSc, RN,
Reconstitution Nursing Dosage Calculation Practice Problems
 Reconstitution Practice Problems Free PDF ebook Download: Reconstitution Download or Read Online ebook reconstitution nursing dosage calculation practice problems in PDF Format From The Best User Guide
Reconstitution Practice Problems Free PDF ebook Download: Reconstitution Download or Read Online ebook reconstitution nursing dosage calculation practice problems in PDF Format From The Best User Guide
3/9/2010. Objectives. Pharmacist Role in Medication Safety and Regulatory Compliance
 Pharmacist Role in Medication Safety and Regulatory Compliance Janet Greiwe Vice President, Systems Management Cleveland County Health System Objectives By the end of this presentation, you should be able
Pharmacist Role in Medication Safety and Regulatory Compliance Janet Greiwe Vice President, Systems Management Cleveland County Health System Objectives By the end of this presentation, you should be able
Medication Safety Way Beyond the 5 Rights
 Safety Way Beyond the 5 Rights JoAnne Phillips, MSN, RN, CCRN, CCNS, CPPS The University of Pennsylvania Health System Philadelphia, PA Current State. Of Chaos Prescriptions 12 per /person / year 4 BILLION
Safety Way Beyond the 5 Rights JoAnne Phillips, MSN, RN, CCRN, CCNS, CPPS The University of Pennsylvania Health System Philadelphia, PA Current State. Of Chaos Prescriptions 12 per /person / year 4 BILLION
STATE OF WEST VIRGINIA DEPARTMENT OF HEALTH AND HUMAN RESOURCES MEMORANDUM
 STATE OF WEST VIRGINIA DEPARTMENT OF HEALTH AND HUMAN RESOURCES Martha Yeager Walker Secretary Joe Manchin III February Governor MEMORANDUM TO: EMS Agency Officials EMS Agency Squad Training Officers Regional
STATE OF WEST VIRGINIA DEPARTMENT OF HEALTH AND HUMAN RESOURCES Martha Yeager Walker Secretary Joe Manchin III February Governor MEMORANDUM TO: EMS Agency Officials EMS Agency Squad Training Officers Regional
Organizational Overview
 0 Organizational Overview First All Digital Hospital in U.S. Fully integrated EMR across 2 Hospitals & 60 Clinics National Valve Center Five Star Hotel for; Patients, Physicians, Nurses & and all team
0 Organizational Overview First All Digital Hospital in U.S. Fully integrated EMR across 2 Hospitals & 60 Clinics National Valve Center Five Star Hotel for; Patients, Physicians, Nurses & and all team
Health Management Information Systems: Computerized Provider Order Entry
 Health Management Information Systems: Computerized Provider Order Entry Lecture 2 Audio Transcript Slide 1 Welcome to Health Management Information Systems: Computerized Provider Order Entry. The component,
Health Management Information Systems: Computerized Provider Order Entry Lecture 2 Audio Transcript Slide 1 Welcome to Health Management Information Systems: Computerized Provider Order Entry. The component,
Levophed Drip Calculation Practice
 Levophed Drip Practice Free PDF ebook Download: Levophed Drip Practice Download or Read Online ebook levophed drip calculation practice in PDF Format From The Best User Guide Database Calculating a Drip
Levophed Drip Practice Free PDF ebook Download: Levophed Drip Practice Download or Read Online ebook levophed drip calculation practice in PDF Format From The Best User Guide Database Calculating a Drip
Infusion device standardisation and the use of dose error reduction software: a UK survey
 Infusion device standardisation and the use of dose error reduction software: a UK survey Ioanna Iacovides¹, Ann Blandford¹, Anna Cox¹, Bryony Dean Franklin², Paul Lee³ and Chris J. Vincent¹. ¹UCL Interaction
Infusion device standardisation and the use of dose error reduction software: a UK survey Ioanna Iacovides¹, Ann Blandford¹, Anna Cox¹, Bryony Dean Franklin², Paul Lee³ and Chris J. Vincent¹. ¹UCL Interaction
D DRUG DISTRIBUTION SYSTEMS
 D DRUG DISTRIBUTION SYSTEMS JANET HARDING ORAL MEDICATION SYSTEMS Drug distribution systems in the hospital setting should ideally prevent medication errors from occurring. When errors do occur, the system
D DRUG DISTRIBUTION SYSTEMS JANET HARDING ORAL MEDICATION SYSTEMS Drug distribution systems in the hospital setting should ideally prevent medication errors from occurring. When errors do occur, the system
Dosage Calculations For Medical Assistant Practice Tests
 For Practice Tests Free PDF ebook Download: For Practice Tests Download or Read Online ebook dosage calculations for medical assistant practice tests in PDF Format From The Best User Guide Database Page
For Practice Tests Free PDF ebook Download: For Practice Tests Download or Read Online ebook dosage calculations for medical assistant practice tests in PDF Format From The Best User Guide Database Page
Streamlining the medication order process
 Streamlining the medication order process Pyxis Connect We went from a 2.5 hour order turnaround time to 16 minutes with the help of Pyxis products. Michael Borgmann Pharmacy Technology Specialist Avera
Streamlining the medication order process Pyxis Connect We went from a 2.5 hour order turnaround time to 16 minutes with the help of Pyxis products. Michael Borgmann Pharmacy Technology Specialist Avera
Smart Pumps and Drug Libraries The Way Forward
 Smart Pumps and Drug Libraries The Way Forward Kathryn Phillips North West Regional MI Centre The first stop for professional medicines advice Outline The drivers behind the development/use of Smart Pumps
Smart Pumps and Drug Libraries The Way Forward Kathryn Phillips North West Regional MI Centre The first stop for professional medicines advice Outline The drivers behind the development/use of Smart Pumps
Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals
 Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals John M. Kessler, B.S. Pharm., Pharm. D. Steve C. Dedrick, MS Pharm. NCCMedS Project Directors
Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals John M. Kessler, B.S. Pharm., Pharm. D. Steve C. Dedrick, MS Pharm. NCCMedS Project Directors
Clinical Skills Validation: Alaris Pump System
 Clinical Skills Validation: Alaris Pump System These documents are intended for use by CW Nurse Clinical Leadership Team. The method used to implement the validation of the Alaris Pump System is unit specific.
Clinical Skills Validation: Alaris Pump System These documents are intended for use by CW Nurse Clinical Leadership Team. The method used to implement the validation of the Alaris Pump System is unit specific.
PURPOSE To establish a standardized process for the activity of an independent double check for medication administration.
 PURPOSE To establish a standardized process for the activity of an independent double check for medication administration. POLICY STATEMENTS Health Care Providers will complete the independent double check
PURPOSE To establish a standardized process for the activity of an independent double check for medication administration. POLICY STATEMENTS Health Care Providers will complete the independent double check
NATIONAL PATIENT SAFETY AGENCY DRAFT PATIENT SAFETY ALERT. Safer Use of Injectable Medicines In Near-Patient Areas
 NATIONAL PATIENT SAFETY AGENCY DRAFT PATIENT SAFETY ALERT Safer Use of Injectable Medicines In Near-Patient Areas Wide Stake Holder Consultation January March 2006 The NPSA is undertaking a wide stake
NATIONAL PATIENT SAFETY AGENCY DRAFT PATIENT SAFETY ALERT Safer Use of Injectable Medicines In Near-Patient Areas Wide Stake Holder Consultation January March 2006 The NPSA is undertaking a wide stake
The Role and Value of ED Pharmacy Services
 The Role and Value of ED Pharmacy Services John Patka, PharmD, BCPS Grady Health System SCSHP 2010 Annual Meeting Objectives Describe clinical challenges in the emergency department (ED) Describe literature
The Role and Value of ED Pharmacy Services John Patka, PharmD, BCPS Grady Health System SCSHP 2010 Annual Meeting Objectives Describe clinical challenges in the emergency department (ED) Describe literature
How BPOC Reduces Bedside Medication Errors White Paper
 How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
I-Pass in the NICU: Operationalizing and Sustaining Improved Handoffs
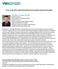 I-Pass in the NICU: Operationalizing and Sustaining Improved Handoffs Research Director Boston Children's Hospital Inpatient Pediatrics Service Director, Sleep and Patient Safety Program Brigham and Women's
I-Pass in the NICU: Operationalizing and Sustaining Improved Handoffs Research Director Boston Children's Hospital Inpatient Pediatrics Service Director, Sleep and Patient Safety Program Brigham and Women's
Adverse Drug Events: A Focus on Anticoagulation Steve Meisel, Pharm.D., CPPS Director of Patient Safety Fairview Health Services, Minneapolis, MN
 Adverse Drug Events: A Focus on Anticoagulation Steve Meisel, Pharm.D., CPPS Director of Patient Safety Fairview Health Services, Minneapolis, MN Fairview Health Services 6 hospitals, ranging from rural
Adverse Drug Events: A Focus on Anticoagulation Steve Meisel, Pharm.D., CPPS Director of Patient Safety Fairview Health Services, Minneapolis, MN Fairview Health Services 6 hospitals, ranging from rural
Is there a Need for Immersive Workshop In Safe Medication Administration for New Anesthesia Providers?
 Is there a Need for Immersive Workshop In Safe Medication Administration for New Anesthesia Providers? Hideru Inoue, RN, MSN John O Donnell, DrPH, MSN, CRNA Judith Mermigas, MSN, CRNA Laura Palmer, DNP,
Is there a Need for Immersive Workshop In Safe Medication Administration for New Anesthesia Providers? Hideru Inoue, RN, MSN John O Donnell, DrPH, MSN, CRNA Judith Mermigas, MSN, CRNA Laura Palmer, DNP,
Overview. Diane Cousins, R.Ph U.S. Pharmacopeia. 1 Pharmacy Labeling with Color
 As more medications are approved and become available to Americans, the opportunity for potentially dangerous or even deadly errors due to drug mix-ups from look alike or sound alike names becomes increasingly
As more medications are approved and become available to Americans, the opportunity for potentially dangerous or even deadly errors due to drug mix-ups from look alike or sound alike names becomes increasingly
Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses
 Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses March 2018 College of Licensed Practical Nurses of Nova Scotia http://clpnns.ca Starlite Gallery, 302-7071 Bayers Road,
Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses March 2018 College of Licensed Practical Nurses of Nova Scotia http://clpnns.ca Starlite Gallery, 302-7071 Bayers Road,
Ghalib Abbasi, RPh, MS, PharmD Pharmacy Technology Consultant Florida, USA
 Ghalib Abbasi, RPh, MS, PharmD Pharmacy Technology Consultant Florida, USA Disclosure Information Let s Fly! IV Medication Errors in the Hospital Pharmacy Ghalib Abbasi I have no financial relationship
Ghalib Abbasi, RPh, MS, PharmD Pharmacy Technology Consultant Florida, USA Disclosure Information Let s Fly! IV Medication Errors in the Hospital Pharmacy Ghalib Abbasi I have no financial relationship
Session Objectives. Medication Errors in Adults and Children. Dennis Quaid American Society of Health- System Pharmacists (ASHP) Meeting December 2009
 Medication Errors in Adults and Children Carly C. Feldott, PharmD Medication Safety Program Director, VUMC Amy L. Potts, PharmD, BCPS Assistant Director, Monroe Carell, Jr. Children s Hospital at Vanderbilt
Medication Errors in Adults and Children Carly C. Feldott, PharmD Medication Safety Program Director, VUMC Amy L. Potts, PharmD, BCPS Assistant Director, Monroe Carell, Jr. Children s Hospital at Vanderbilt
Disclosure. SwedishAmerican Hospital A Division of UW Health. Learning Objectives. Medication History. Medication History 2/2/2017
 Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
Note EDUCATION. Keywords: Pharmacists Patient Care Process, faculty development, video
 Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Chapter 13. Documenting Clinical Activities
 Chapter 13. Documenting Clinical Activities INTRODUCTION Documenting clinical activities is required for one or more of the following: clinical care of individual patients -sharing information with other
Chapter 13. Documenting Clinical Activities INTRODUCTION Documenting clinical activities is required for one or more of the following: clinical care of individual patients -sharing information with other
A shortage of everything except ERRORS
 Disclosure Succinylcholine Propofol Vitamin K Lorazepam Diltiazem Drug Shortages Current Status & State Survey Results Bill Stevenson Director of Pharmacy Oconee Medical Center I do not have a vested interest
Disclosure Succinylcholine Propofol Vitamin K Lorazepam Diltiazem Drug Shortages Current Status & State Survey Results Bill Stevenson Director of Pharmacy Oconee Medical Center I do not have a vested interest
Experiential Education
 Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
How CHRISTUS Spohn Health System uses automation to improve standardization and re-deploy pharmacists to clinical functions
 A culture of medication safety: How CHRISTUS Spohn Health System uses automation to improve standardization and re-deploy pharmacists to clinical functions Authored and produced by CareFusion, August 2013
A culture of medication safety: How CHRISTUS Spohn Health System uses automation to improve standardization and re-deploy pharmacists to clinical functions Authored and produced by CareFusion, August 2013
Canadian Paediatric High Alert Medication Delivery
 Canadian Paediatric High Alert Medication Delivery Paediatric Opioid Safety - Phase 3: Education, Knowledge Translation and Implementation Final Report January 16, 2013 Respectfully Submitted by Elaine
Canadian Paediatric High Alert Medication Delivery Paediatric Opioid Safety - Phase 3: Education, Knowledge Translation and Implementation Final Report January 16, 2013 Respectfully Submitted by Elaine
Letter of Intent and Application Instructions 2018 Award for Excellence Program
 Letter of Intent and Application Instructions 2018 Award for Excellence Program This award program is a collaboration between the ASHP Foundation and the Cardinal Health Foundation. Copyright 2017 ASHP
Letter of Intent and Application Instructions 2018 Award for Excellence Program This award program is a collaboration between the ASHP Foundation and the Cardinal Health Foundation. Copyright 2017 ASHP
Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists. Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM)
 Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM) 1 Learning Objectives Upon successful completion of this
Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM) 1 Learning Objectives Upon successful completion of this
Smart Pump Interoperability: A Multi-System Safety Journey. February 23, 2018
 Smart Pump Interoperability: A Multi-System Safety Journey February 23, 2018 Jennifer Biltoft, PharmD, BCPS System Director, Clinical Pharmacy Services, SCL Health Deborah Bonnes, RN, MS Nursing Informatics
Smart Pump Interoperability: A Multi-System Safety Journey February 23, 2018 Jennifer Biltoft, PharmD, BCPS System Director, Clinical Pharmacy Services, SCL Health Deborah Bonnes, RN, MS Nursing Informatics
FIRST PATIENT SAFETY ALERT FROM NATIONAL PATIENT SAFETY AGENCY (NPSA) Preventing accidental overdose of intravenous potassium
 abcdefghijklm Health Department St Andrew s House Regent Road Edinburgh EH1 3DG MESSAGE TO: 1. Medical Directors of NHS Trusts 2. Directors of Public Health 3. Specialists in Pharmaceutical Public Health
abcdefghijklm Health Department St Andrew s House Regent Road Edinburgh EH1 3DG MESSAGE TO: 1. Medical Directors of NHS Trusts 2. Directors of Public Health 3. Specialists in Pharmaceutical Public Health
Impact of an Innovative ADC System on Medication Administration
 Impact of an Innovative ADC System on Medication Administration March 1, 2016 Nilesh Desai, BS, RPh, MBA Administrator Pharmacy and Clinical Operations Hackensack University Medical Center Conflict of
Impact of an Innovative ADC System on Medication Administration March 1, 2016 Nilesh Desai, BS, RPh, MBA Administrator Pharmacy and Clinical Operations Hackensack University Medical Center Conflict of
Implementation Guide Version 4.0 Tools
 Implementation Guide Version 4.0 Tools Program Overview Purpose of the Guide This Guide is intended primarily for INTERACT champions and trained educators who are responsible for implementing and sustaining
Implementation Guide Version 4.0 Tools Program Overview Purpose of the Guide This Guide is intended primarily for INTERACT champions and trained educators who are responsible for implementing and sustaining
EVALUATION OF THE FINANCIAL IMPACT OF MEDICATION BACKORDERS IN A TERTIARY CARE HOSPITAL. Kalyn Marie Acker
 EVALUATION OF THE FINANCIAL IMPACT OF MEDICATION BACKORDERS IN A TERTIARY CARE HOSPITAL by Kalyn Marie Acker PharmD, University of Texas at Austin, 2015 BS in Biochemistry, Texas Tech University, 2011
EVALUATION OF THE FINANCIAL IMPACT OF MEDICATION BACKORDERS IN A TERTIARY CARE HOSPITAL by Kalyn Marie Acker PharmD, University of Texas at Austin, 2015 BS in Biochemistry, Texas Tech University, 2011
Supplementary Online Content
 Supplementary Online Content Itrat A, Taqui A, Cerejo R, et al; Cleveland Pre-Hospital Acute Stroke Treatment (PHAST) Group. Telemedicine in prehospital stroke evaluation and thrombolysis: taking stroke
Supplementary Online Content Itrat A, Taqui A, Cerejo R, et al; Cleveland Pre-Hospital Acute Stroke Treatment (PHAST) Group. Telemedicine in prehospital stroke evaluation and thrombolysis: taking stroke
Objective Competency Competency Measure To Do List
 2016 University of Washington School of Pharmacy Institutional IPPE Checklist Institutional IPPE Team Contact Info: Kelsey Brantner e-mail: ippe@uw.edu phone: 206-543-9427; Jennifer Danielson, PharmD e-mail:
2016 University of Washington School of Pharmacy Institutional IPPE Checklist Institutional IPPE Team Contact Info: Kelsey Brantner e-mail: ippe@uw.edu phone: 206-543-9427; Jennifer Danielson, PharmD e-mail:
