Grampians Regional Palliative Care Research Centre
|
|
|
- Gerald Underwood
- 5 years ago
- Views:
Transcription
1 Grampians Regional Palliative Care Research Centre Director : Dr David Brumley Research Manager: Dr John Fisher Consultant: Professor Michael Ashby The William Buckland Foundation made a very generous grant of nearly $300,000 to facilitate rural palliative care research in Victoria. All the projects being done have very practical goals and outcomes, based on perceived needs expressed by doctors, nurses and personal care workers looking after palliative care patients in the Grampians Health Region. The principles and practical benefits derived from these research projects are being actively disseminated in publications, professional meetings and continuing staff education throughout the region and beyond.
2 Conducting and evaluating an educational intervention on the use of Graseby Syringe drivers for rural nonspecialist nurses
3 GRASEBY SYRINGE DRIVER PROJECT Who was involved? Investigators Dr David Brumley (PC physician, Gandarra, GRPCS) Ms Anne Hayes (Clinical Nurse Consultant, Wimmera Hospice Care) Professor Michael Ashby (Palliative medicine, MU) Dr John Fisher (Project Manager, GRPCS) Research Nurses Education sessions Mary Wade Lawrence Habegger Funding William Buckland Foundation multiple pc projects
4 GRASEBY SYRINGE DRIVER PROJECT Why did we do this? Some unsafe practices -> deaths. Drivers OK, human error or tampering? Several non-fatal incidents in this region Recent Coroner s cases Standardise procedures -> safe use of MS 26 Improve drug knowledge for SD use Improve cannulation site management Provide ongoing support & resource contacts
5 Graseby SD Training setup explain rate drugs Nurses confidence levels Pre Post 3-months
6 Confidence pre- x use of SD <1/mth >1/mth setup explain rate drugs Nurses confidence levels
7 Confidence post- x use of SD setup explain rate drugs Nurses confidence levels <1/mth >1/mth
8 Confidence 3-months x use of SD setup explain rate drugs Nurses confidence levels <1/mth >1/mth
9 Recommendations Use it (GSD) or lose it (confidence, that is) 1. Read the training manual monthly 2. Work through drugs information & exercises 3. Practice with a GSD 4. Annual face-to-face update on drugs For a copy of the PowerPoint training presentation using GSD, johnfi@bhs.org.au.
10 This research was presented as a paper at the Palliative Care Victoria Conference at Monash University, Gippsland Campus, in November 2004 and as part of a continuing professional development seminar for nurses in the Grampians Health Region in November Participants in these sessions were given a copy of the nurses' handbook, developed for the half-day training program, and it is also being distributed where needed by the regional palliative care nurse in the Grampians Health Region. A paper entitled, 'Evaluation of training on the use of Graseby syringe drivers for rural nonspecialist nurses' was published in the International Journal of Palliative Nursing in February This article has drawn responses from England, Wales, New Zealand and South Australia. A presentation was also made on this research at the International Hospice Conference in Seoul in March 2005.
11
12 The Acceptability and Usefulness of the Medical Treatment Act 1988 (Vic) for Palliative Care in the Grampians Health Region Victoria Sponsored by Investigators Dr David Brumley Director, Grampians Regional PC Service Prof Michael Ashby Palliative Medicine, University of Melbourne Ms Margaret Brown Consultant, University of SA Dr John Fisher Project Manager, GRPCS Mrs Jan Milliken PCNC, Ballarat Hospice Care
13 Background The Medical Treatment Act (MTA) provides individuals with the legal right to refuse medical treatment in advance of incompetence. Schedule 1 - Refusal of treatment certificate Schedule 2 Enduring Power of Attorney ( medical treatment). However few people know about this legislation. Aim To explore the usefulness and acceptability of the MTA 1988 (Vic) for palliative care in a rural region of Victoria. Participants All competent adult patients at Ballarat and Wimmera Hospices July-December 2004 were invited to participate. Method Palliative Care patients were given material explaining the MTA Schedules and opportunity to discuss them.
14 Findings 1. Timing is crucial Nearly half the palliative care patients (47%) in Ballarat and Horsham were too sick to comprehend /discuss information in the pack. 22% were not interested; 31% were able to be interviewed. 2. Understanding of the Medical Treatment Act 78% had not heard of the Medical Treatment Act. 71% knew of their right to refuse medical treatment. Only 39% knew the difference between Enduring Power of Attorney and Medical Power of Attorney after reading the material. 3. Acceptability of the MTA Rate of interest in the forms: Schedule 1 Refusal of medical treatment certificate - competent patient Schedule 2 - Enduring Power of Attorney (Medical Treatment) none 5 18% Schedule 1 only 4 14% Schedule 2 only 11 39% Both 1 & % total 28
15 How worthwhile was the process? Most patients were very positive about the process of discussing the forms. 89% said it would give more peace of mind. PCNCs reported that the introducing this information to the patients engaged them in a different way and created opportunities to discuss issues which otherwise might have been more difficult to discuss. 4. Patients need a guide to work through the MTA Many participants stated that their concentration span has been reduced by illness and/or medication. Some felt overwhelmed by the need to read the forms and book at such a critical time in their lives. Even though the MTA Information Pack was considered easy enough to read, many of the participants believe: It should be explained by people who can communicate well with older people. 5. Medical and nursing staff need training: to understand the intricacies of the Act. to explain it in simple language. to present it at an appropriate time for pc patients.
16 When this project was reported in a poster presentation at the Palliative Care Victoria Conference at Monash University, Gippsland Campus, in November 2004 and as part of a continuing professional development seminar for nurses in the Grampians Health Region in November 2004, it showed just how unaware the nurses were of the details in the Medical Treatment Act. A presentation was made at the Palliative Care Australia Conference in Sydney August A paper entitled, 'Advance directives in action in a regional palliative care service: Road testing the provisions of the Medical Treatment Act 1988(Vic)' was published in the Journal of Law and Medicine, November 2005.
17
18 Improving Access to Clinical Information in After Hours Palliative Care Sponsored by Investigators Dr David Brumley Prof Michael Ashby Dr John Fisher Ms Heather Robinson Director, Grampians Regional PC Service Palliative medicine, University of Melbourne Project Manager, GRPCS Executive Officer, Ballarat Hospice Care
19 Background Most pc patients prefer to be at home and to die at home. Need support of GP and PC nurses. Current information sharing between carers is incomplete. Difficulty providing optimum continuity of care After Hours. Hypothesis Provision of clinical information to nurses and doctors providing After Hours care to pc patients will result in improved patient, nurse and doctor satisfaction and/or reduce the rate of unwanted hospital admissions for terminal care. Participants All adult patients in Ballarat Hospice Care June - August Method Essential medical data relating to the history and current condition of any unstable patients was sent by fax each week day to doctors responsible for patients' After Hours care & on Palm Pilot for nurses on call.
20 'AFTER HOURS' INFO SHEET UR No.: Name: Address: Phone: DOB: Carer Name: Relationship: Phone: GP Name: Phone: Fax: NOK: Phone: Specialist: Brief History: Primary Diagnosis: Secondary Diagnosis: Current Clinical Condition: Stable Unstable Deteriorating Terminal Current treatment: Symptoms: Severity 1-10 Pain 1 Pain 2 Nausea / Vomiting Drowsiness Dyspnoea Mobility Anxiety Depression Appetite Constipation Restlessness/ agitation Fatigue Current medications: Allergies: Drug Name Dosage / Route Recent changes/problems Expectations of Care: Preferred Place of Care Preferred place of dying Treatment options Patient Carer Last updated:
21 Findings 1. Predicting unstable patients: a. Difficult to predict call-outs -> patients who had sheets faxed did not have call-outs, others did. e. Feedback from GPs indicated that material was useful when needed. 2. Benefits for Nurses: h. Updating Information Sheets daily aided nurses reporting, especially Expectations of Care. Very specific comments were noted. j. After initial concerns, nurses found the forms (MS Word documents) and computers easy to use and very beneficial to practice. c. Nurses' confidence markedly increased, because of immediate access to each patient's: i. full medical history vi. risks and problems ii. treatments vii. symptom control iii. current status viii. contact information iv. up-to-date meds list ix. Doctors' letters v. progress notes
22 a. Nurses saved time not having to go to the office to collect patients' notes. c. Nurses sounded informed to patients and doctors, because they were empowered by information on the Palm Pilot. e. Nurses respond to pager rapidly and give accurate information for all patients, even those they have not previously seen. Reduces worry about not knowing patients. g. Patients do not need to repeat their medical history. h. Nurses felt more confident with assessments, so patients' outcomes were improved due to increased knowledge of nurses. eg, reduced chances of error when administering drugs. i. Nurses can give more thorough information to GPs and A&E when necessary, to help provide more sound medical treatment. More professional practice. Nurses can confidently tell Drs to 'Call back if more information is needed.'
23 When this project was reported in a poster presentation at the Palliative Care Victoria Conference at Monash University, Gippsland Campus, in November 2004 and as part of a continuing professional development seminar for nurses in the Grampians Health Region in November 2004, it drew considerable attention when the nurses saw how simple, yet effective the process was. A paper was presented on it at the International Hospice Conference in Seoul in March A poster presentation was made at the Palliative Care Australia Conference in Sydney August A paper entitled, 'Improving access to clinical information in after hours community palliative care' was published in the Australian Journal of Advanced Nursing, September-November 2006.
24 Developing and using the Information Sheet about PC pts: 2. GPs and PC nurses ideas led to key data on a single A4 sheet. 2. Takes one hour to set up each new patient's file (as a Word document) on the Hospice computer. Very simple & economical. 3. Each day, PC nurses update nursing notes on Hospice computer. 4. PC nurses tried to predict which patients were unstable enough to possibly lead to callout After Hours. Information sheets for these patients were faxed to patients' home GPs. 5. The current Information Sheet, together with PCNC's initial assessment notes, any letters to GPs and/or referrer, specialist appointments, hospital discharges, etc scanned into files for all patients on a Palm Pilot for nurses 'on call' After Hours.
25 New project The After Hours project laid the foundation for an application to the Federal Department of Health & Ageing under the Local Palliative Care Grants Program Funding Round Three Care Planning. The application was granted $187,500 from July October 2008 for a project entitled Listen up! Hearing all the voices in caring for palliative patients in a regional/rural setting. This project aims to develop a process to allow sharing of patient information between all carers working with palliative patients, and to develop a process to address advanced care planning, which may involve crisis situations and advance directives.
26
27 Phase I/II Trial of Intranasal Sufentanil for Breakthrough Cancer-associated Pain (in patients at Gandarra Palliative Care Unit, Ballarat Health Services) Sponsored by Investigators Dr Kate Jackson Dr David Brumley Prof Michael Ashby Dr John Fisher Monash Medical Centre Director, Grampians Regional PC Service Palliative medicine, University of Melbourne Project Manager, GRPCS
28 Aim: That application of intranasal Sufentanil will be a simple, safe, effective and patient friendly method of opioid breakthrough dosing in palliative care patients with cancer. Method: Cancer patients who fit the inclusion criteria and have opioid responsive pain, are invited to trial the IN administration of Sufentanil (a morphine-like painkiller). Two phases dose titration phase and ongoing phase if/when an effective dose is reached. The Verbal Ratingpain Scale is used to monitor all patients pain levels, with additional questions on patient acceptability and monitoring to detect any nasal adverse effects. Information from this study will help improve patient treatments in future and results in better overall pain control for the study patients. Case study: 40+ yo woman with ca breast and bone metastases, was able to paint & garden; Pain 7->0 in 20 mins, 5->0 in <10 mins -> improved quality of life with IN Sufenta.
29 This project was reported in a presentation at the Palliative Care Victoria Conference at Monash University, Gippsland Campus, in November 2004 and as part of a continuing professional development seminar for nurses in the Grampians Health Region in November A presentation was also made at the Palliative Care Australia Conference in Sydney August Extension project: Ethics approvals have been granted for IN sufenta to be used in a follow-up study of breakthrough pain associated with radiotherapy treatment at Ballarat-Austin Radiation Oncology Centre (BAROC).
30
31 Implementing a Palliative Approach in Residential Aged Care (PARAC) Help is being provided for staff implementing a palliative approach in Residential Aged Care Facilities throughout the Grampians Health Region. Based on needs' surveys done in 2005, two PCNCs have provided four Short train-the-trainer programs for RACF staff in the GHR, approximately one month apart. Topics included: Introduction to PARAC Quality of life Medical Treatment Act Advance Directives End-of-life care Spiritual issues in PC Grief & bereavement Communication Self care Family meetings Liverpool Care Pathways Pain management The results of the program are currently being analysed. A preliminary report on this project was presented at the Palliative Care Victoria conference, La Trobe University Bendigo, July 2006.
32
33 Spiritual well-being among health service providers Fisher s Spiritual Well-Being Questionnaire (SWBQ) is being used to investigate how the personal beliefs and experiences of health services' staff relate to their perceptions of help provided to clients for SWB (in Ballarat Health Services, St John Of God Healthcare and hospices). Presentations have been made on this research at the Palliative Care Victoria conference, La Trobe University Bendigo, July 2006 and the Australian and New Zealand Society of Palliative Medicine biennial conference, Newcastle, October For further details, please johnfi@bhs.org.au.
34
35 Family Caregiver Education program The education program for family members/carers, of patients registered with regional palliative care services, has been extended from a trial run at Ballarat Hospice last year and formally evaluated. (This project was Funded by Bethlehem Griffiths Foundation, in conjunction with the Centre for Palliative Care, Melbourne)
36
37 Multidisciplinary Palliative Care Education Our services were provided to evaluate the effectiveness of two-day workshops on Palliative Care: The Essentials run in four Victorian centres (by the Centre for Palliative Care, Melbourne) in (Funded by Australian DHA through Victorian DHS) These workshops were well received by the 500 allied health workers, doctors, nurses and PCAs who participated in them. Calls for further, similar courses were made by those involved.
Hospice Isle of Man Education Prospectus 2018
 Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Safety reporting in multi-site clinical trials in Palliative Care
 Safety reporting in multi-site clinical trials in Palliative Care Belinda Fazekas Linda Devilee Zac Vandersman David Currow Flinders University receives funding for PaCCSC from the Australian Government
Safety reporting in multi-site clinical trials in Palliative Care Belinda Fazekas Linda Devilee Zac Vandersman David Currow Flinders University receives funding for PaCCSC from the Australian Government
DRAFT Optimal Care Pathway
 DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
Palliative Care Anticipatory Prescribing
 Palliative Care Anticipatory Prescribing Guidelines Gippsland Region Palliative Care Consortium Clinical Practice Group Policy No. Title Keywords Ratified GRPCC-CPG008 Anticipatory Prescribing Guidelines
Palliative Care Anticipatory Prescribing Guidelines Gippsland Region Palliative Care Consortium Clinical Practice Group Policy No. Title Keywords Ratified GRPCC-CPG008 Anticipatory Prescribing Guidelines
Community Palliative Care Service for Western Sydney. Information for clients
 Community Palliative Care Service for Western Sydney Information for clients Who we are Silver Chain Group is a not-for-profit organisation and the largest provider of community-based palliative care services
Community Palliative Care Service for Western Sydney Information for clients Who we are Silver Chain Group is a not-for-profit organisation and the largest provider of community-based palliative care services
Specialist Palliative Care Services (SPCS): Grampians Region. Quick Reference Tool
 Specialist Palliative Care Services (SPCS): Grampians Region Quick Reference Tool The right care in the right place at the right time What do Specialist Palliative Care Services (SPCS) provide? Advice,
Specialist Palliative Care Services (SPCS): Grampians Region Quick Reference Tool The right care in the right place at the right time What do Specialist Palliative Care Services (SPCS) provide? Advice,
Learning from the National Care of the Dying 2014 Audit. Dr Bill Noble Medical Director, Marie Curie Cancer Care
 Learning from the National Care of the Dying 2014 Audit Dr Bill Noble Medical Director, Marie Curie Cancer Care MARIE CURIE Major UK end of life charity Major service provider Network of 2000 Nurses caring
Learning from the National Care of the Dying 2014 Audit Dr Bill Noble Medical Director, Marie Curie Cancer Care MARIE CURIE Major UK end of life charity Major service provider Network of 2000 Nurses caring
INTEGRATED CARE PATHWAY FOR THE DYING PATIENT PATIENT S NAME.. UNIT NUMBER. DATE.. DATE OF BIRTH.. DATE OF IN PATIENT ADMISSION DIAGNOSIS: PRIMARY.
 PATIENT S NAME.. UNIT NUMBER. DATE.. DATE OF BIRTH.. DATE OF IN PATIENT ADMISSION DIAGNOSIS: PRIMARY. SECONDARY.. A Care Pathway is intended as a guide to treatment and an aid to documenting patient progress.
PATIENT S NAME.. UNIT NUMBER. DATE.. DATE OF BIRTH.. DATE OF IN PATIENT ADMISSION DIAGNOSIS: PRIMARY. SECONDARY.. A Care Pathway is intended as a guide to treatment and an aid to documenting patient progress.
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Criteria and Guidance for referral to Specialist Palliative Care Services
 Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Prescribing for Symptom Control in End of Life Care. Dr Deborah Robertson Senior Lecturer University of Chester
 Prescribing for Symptom Control in End of Life Care Dr Deborah Robertson Senior Lecturer University of Chester #hellomynameis Dr Debs Robertson Programme leader NMP Nurse and pharmacologist Champion of
Prescribing for Symptom Control in End of Life Care Dr Deborah Robertson Senior Lecturer University of Chester #hellomynameis Dr Debs Robertson Programme leader NMP Nurse and pharmacologist Champion of
One Chance to Get it Right:
 One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
National Standards Assessment Program. Quality Report
 National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
Guidance on End of Life Care-Updated July 2014
 Guidance on End of Life Care-Updated July 2014 INTRODUCTION Definition of End of Life Care: End of Life care helps all those with advanced, progressive, incurable illness to live as well as possible until
Guidance on End of Life Care-Updated July 2014 INTRODUCTION Definition of End of Life Care: End of Life care helps all those with advanced, progressive, incurable illness to live as well as possible until
What is palliative care?
 What is palliative care? Hamilton Health Sciences and surrounding communities Palliative care is a way of providing health care that focuses on improving the quality of life for you and your family when
What is palliative care? Hamilton Health Sciences and surrounding communities Palliative care is a way of providing health care that focuses on improving the quality of life for you and your family when
ORGANISATIONAL AUDIT
 [Type text] National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians,
[Type text] National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians,
PROCESS FOR INITIATING A SYRINGE DRIVER FOR COMMUNITY NURSE PATIENTS OUT OF HOURS
 STANDARD OPERATING PROCEDURE PROCESS FOR INITIATING A SYRINGE DRIVER FOR COMMUNITY NURSE PATIENTS OUT OF HOURS Issue History Issue Version one Purpose of Issue/Description of Change To facilitate patients
STANDARD OPERATING PROCEDURE PROCESS FOR INITIATING A SYRINGE DRIVER FOR COMMUNITY NURSE PATIENTS OUT OF HOURS Issue History Issue Version one Purpose of Issue/Description of Change To facilitate patients
End of life care. Patient Guide
 8 End of life care Patient Guide What happens? There is a point for many in the brain tumour journey when either the disease no longer responds to treatment, or you have had all treatment that is available
8 End of life care Patient Guide What happens? There is a point for many in the brain tumour journey when either the disease no longer responds to treatment, or you have had all treatment that is available
PRIORITIES FOR CARE OF THE DYING PERSON
 PRIORITIES FOR CARE OF THE DYING PERSON Core and other useful sessions to support education and training across health and social care Fig.1 The 5 Priorities for Care of the Dying Person INTRODUCTION One
PRIORITIES FOR CARE OF THE DYING PERSON Core and other useful sessions to support education and training across health and social care Fig.1 The 5 Priorities for Care of the Dying Person INTRODUCTION One
Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy
 Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy 2016-2017 Contents Acknowledgements Subject Page Number 1. Introduction 4 2. Vision 5 3. National policy Context 5-6 4. Local
Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy 2016-2017 Contents Acknowledgements Subject Page Number 1. Introduction 4 2. Vision 5 3. National policy Context 5-6 4. Local
1. Guidance notes. Social care (Adults, England) Knowledge set for end of life care. (revised edition, 2010) What are knowledge sets?
 Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Support services for patients with secondary breast cancer.
 Sheffield Teaching Hospitals NHS Foundation Trust Support services for patients with secondary breast cancer. Secondary breast cancer pledge: working together to improve secondary breast cancer services
Sheffield Teaching Hospitals NHS Foundation Trust Support services for patients with secondary breast cancer. Secondary breast cancer pledge: working together to improve secondary breast cancer services
Palliative and Hospice Care In the United States Jean Root, DO
 Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Serious Medical Treatment Decisions. BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE
 Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
ONE CHANCE TO GET IT RIGHT DERBYSHIRE
 ONE CHANCE TO GET IT RIGHT DERBYSHIRE A guide for professionals in Derbyshire who care for patients believed to be in the last year of life 1 ST edition July 2014 OCTGIRv1.29614 DERBYSHIRE ALLIANCE FOR
ONE CHANCE TO GET IT RIGHT DERBYSHIRE A guide for professionals in Derbyshire who care for patients believed to be in the last year of life 1 ST edition July 2014 OCTGIRv1.29614 DERBYSHIRE ALLIANCE FOR
Holistic Needs Assessment (HNA) for Adult Cancer Patients Guidelines
 Please Note: This policy is currently under review and is still fit for purpose. Holistic Needs Assessment (HNA) for Adult Cancer Patients Guidelines Handbook to accompany these guidelines is available
Please Note: This policy is currently under review and is still fit for purpose. Holistic Needs Assessment (HNA) for Adult Cancer Patients Guidelines Handbook to accompany these guidelines is available
QUALIFICATION HANDBOOK
 QUALIFICATION HANDBOOK Level 2, 3 & 5 Awards and Certificates in End of Life Care (3571-02-03-04-05) May 2013 Version 5.0 Qualification at a glance Subject area City & Guilds number 3571 End of life care
QUALIFICATION HANDBOOK Level 2, 3 & 5 Awards and Certificates in End of Life Care (3571-02-03-04-05) May 2013 Version 5.0 Qualification at a glance Subject area City & Guilds number 3571 End of life care
TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE
 ...from the Middle Ages to the 21st Century TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE Emily Bradford RN CHPN Director of Hospice Services VNA Middle Ages: 16th-18th Centuries: Religious
...from the Middle Ages to the 21st Century TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE Emily Bradford RN CHPN Director of Hospice Services VNA Middle Ages: 16th-18th Centuries: Religious
FOR ILLUSTRATIVE PURPOSES ONLY
 - Page 1 of 15 GUIDANCE Health Professional Guidance for the Care Plan for the Dying Person - Victoria RECOGNISING DYING The possibility that a person may die within the next few days or hours is recognised
- Page 1 of 15 GUIDANCE Health Professional Guidance for the Care Plan for the Dying Person - Victoria RECOGNISING DYING The possibility that a person may die within the next few days or hours is recognised
Appendix: Assessments from Coping with Cancer
 Appendix: Assessments from Coping with Cancer Primary Independent Variable of Interest (assessed at baseline with medical chart review and confirmed with clinician) 1. What treatments is the patient currently
Appendix: Assessments from Coping with Cancer Primary Independent Variable of Interest (assessed at baseline with medical chart review and confirmed with clinician) 1. What treatments is the patient currently
End of Life Care in the Acute Hospital Setting. Dr Adam Brown Consultant in Palliative Medicine
 End of Life Care in the Acute Hospital Setting Dr Adam Brown Consultant in Palliative Medicine Learning objectives Understanding a patient's priorities for end of life care How to work with the 5 priorities
End of Life Care in the Acute Hospital Setting Dr Adam Brown Consultant in Palliative Medicine Learning objectives Understanding a patient's priorities for end of life care How to work with the 5 priorities
End of life care in Secure Psychiatric Settings
 End of life care in Secure Psychiatric Dr Nuwan Galappathie MBChB MRCPsych MMedSc LLM Consultant Forensic Psychiatrist St Andrew s Healthcare, Birmingham Visiting Researcher, Institute of Psychiatry, Kings
End of life care in Secure Psychiatric Dr Nuwan Galappathie MBChB MRCPsych MMedSc LLM Consultant Forensic Psychiatrist St Andrew s Healthcare, Birmingham Visiting Researcher, Institute of Psychiatry, Kings
Primary Care Quality (PCQ) National Priorities for General Practice
 Primary Care Quality (PCQ) National Priorities for General Practice Cluster Guidance and Templates 2015/16 Authors: Primary Care Quality Team Date: November 2015 Publication/ Distribution: Version: Final
Primary Care Quality (PCQ) National Priorities for General Practice Cluster Guidance and Templates 2015/16 Authors: Primary Care Quality Team Date: November 2015 Publication/ Distribution: Version: Final
Understanding. Hospice Care
 Understanding Hospice Care What is Hospice Care? We take care of patients and families facing serious illness, so they can focus on living well. Quality of Life We are committed to the belief that there
Understanding Hospice Care What is Hospice Care? We take care of patients and families facing serious illness, so they can focus on living well. Quality of Life We are committed to the belief that there
Understanding. Hospice Care
 Understanding Hospice Care What is Hospice Care? We take care of patients and families facing serious illness, so they can focus on living well. Quality of Life We are committed to the belief that there
Understanding Hospice Care What is Hospice Care? We take care of patients and families facing serious illness, so they can focus on living well. Quality of Life We are committed to the belief that there
End of Life Care Strategy
 End of Life Care Strategy 2016-2020 Foreword Southern Health NHS Foundation Trust is committed to providing the highest quality care for patients, their families and carers. Therefore, I am pleased to
End of Life Care Strategy 2016-2020 Foreword Southern Health NHS Foundation Trust is committed to providing the highest quality care for patients, their families and carers. Therefore, I am pleased to
If patient is 24 hour dependent on NIV and decides to discontinue it, support and forward planning are essential
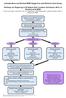 Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
PROSPECTUS - COURSES FROM AUGUST 2017 MARCH 2018 More courses added throughout the year COURSE TITLE DATE TIME VENUE TUTOR COST 2017
 PROSPECTUS - COURSES FROM AUGUST MARCH More courses added throughout the year Key: Courses held at our Shrewsbury Hospice, Bicton Heath, Shrewsbury, SY3 8HS = Course held at our Telford Hospice, Apley
PROSPECTUS - COURSES FROM AUGUST MARCH More courses added throughout the year Key: Courses held at our Shrewsbury Hospice, Bicton Heath, Shrewsbury, SY3 8HS = Course held at our Telford Hospice, Apley
Referral cover sheet and acknowledgement
 Referral cover sheet and acknowledgement Purpose: to send with a referral or to acknowledge receipt of a referral. Date: dd/mm/yyyy / / Referral To send a referral complete this section From To Organisation:
Referral cover sheet and acknowledgement Purpose: to send with a referral or to acknowledge receipt of a referral. Date: dd/mm/yyyy / / Referral To send a referral complete this section From To Organisation:
Perceptions of the role of the hospital palliative care team
 NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
Multidisciplinary care of a patient with heart failure. patient with heart failure. Dr Claire Hookey
 Multidisciplinary care of a patient with heart failure patient with heart failure Dr Claire Hookey Mr E.S 61 year old gentleman Referred to the hospice by the heart failure specialist nurse May 2010 Heart
Multidisciplinary care of a patient with heart failure patient with heart failure Dr Claire Hookey Mr E.S 61 year old gentleman Referred to the hospice by the heart failure specialist nurse May 2010 Heart
Abbreviations used in Care Pathway. CNS Clinical Nurse C Chaplain / clergy / religious adviser
 Patient's Name: D.O.B: Patient GP: Named Nurse: Name: Adapted LCP Version 12 PALLIATIVE CARE PATHWAY (End Stage) PRIMARY CARE DO NOT PUT PATIENT ON THIS PATHWAY UNLESS The Multi-professional Team have
Patient's Name: D.O.B: Patient GP: Named Nurse: Name: Adapted LCP Version 12 PALLIATIVE CARE PATHWAY (End Stage) PRIMARY CARE DO NOT PUT PATIENT ON THIS PATHWAY UNLESS The Multi-professional Team have
National Care of the Dying Audit Hospitals (NCDAH) Round 3
 National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians, and is supported
National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians, and is supported
Cancer and Advance Care Planning. Tips for Oncology Professionals
 Cancer and Advance Care Planning Tips for Oncology Professionals Each year, more than 74,000 Canadians die with cancer. When To Have the Discussion...5 Questions to Ask...6 Steps in Initiating and Having
Cancer and Advance Care Planning Tips for Oncology Professionals Each year, more than 74,000 Canadians die with cancer. When To Have the Discussion...5 Questions to Ask...6 Steps in Initiating and Having
Developing individual care plans and goals for every end of life care patient
 Developing individual care plans and goals for every end of life care patient Dr. Dee Traue Consultant in Palliative Medicine We will cover How individual care plans differ from the LCP Developing and
Developing individual care plans and goals for every end of life care patient Dr. Dee Traue Consultant in Palliative Medicine We will cover How individual care plans differ from the LCP Developing and
RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE. INSIDE Expert advice on HIV disclosure. The end of an era in Afghanistan
 Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Module 2 Excellence in practice
 Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
Fine Bore Tubing Set
 Negotiations Meetings with CME Director (lived on East coast, but came to meet me here on a few occasions) Asked for 2 pumps on loan for a few months Discussed use of locking drivers, so they can only
Negotiations Meetings with CME Director (lived on East coast, but came to meet me here on a few occasions) Asked for 2 pumps on loan for a few months Discussed use of locking drivers, so they can only
East of England. End of Life Care Education Programme. ABC Education Project Plan
 East of England End of Life Care Education Programme ABC Education Project Plan September 2010 Final Version Authors: Sarah Russell Project Lead: Bedfordshire and Hertfordshire sarah.russell@stfrancis.org.uk
East of England End of Life Care Education Programme ABC Education Project Plan September 2010 Final Version Authors: Sarah Russell Project Lead: Bedfordshire and Hertfordshire sarah.russell@stfrancis.org.uk
Respecting Patient Choices: Advance Care Planning to Improve Patient Care at Austin Health
 Respecting Patient Choices: Advance Care Planning to Improve Patient Care at Austin Health Meagan-Jane Lee, Melodie Heland, Panayiota Romios, Charin Naksook and William Silvester Medical science has the
Respecting Patient Choices: Advance Care Planning to Improve Patient Care at Austin Health Meagan-Jane Lee, Melodie Heland, Panayiota Romios, Charin Naksook and William Silvester Medical science has the
Supporting people who need Palliative and End of Life Care in the Community. Giving people a choice
 Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
End of Life Care Review Case Review Audit
 Case Review Audit : : Version: 1 NHS Wales (Intranet) / Public Health Wales (Intranet) Purpose and summary of document: This document is for use by general practices who are engaged in providing services
Case Review Audit : : Version: 1 NHS Wales (Intranet) / Public Health Wales (Intranet) Purpose and summary of document: This document is for use by general practices who are engaged in providing services
Advance Care Planning: the Clients Perspectives
 Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
Community pharmacy and palliative care
 8 This module is also online at pharmacymagazine.co.uk CPD MODULE module 261 Community pharmacy and palliative care Contributing author: Louise Baglole, healthcare/ pharmacy consultant and medical writer
8 This module is also online at pharmacymagazine.co.uk CPD MODULE module 261 Community pharmacy and palliative care Contributing author: Louise Baglole, healthcare/ pharmacy consultant and medical writer
End of Life Care. LONDON: The Stationery Office Ordered by the House of Commons to be printed on 24 November 2008
 End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada.
 CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada. For more information about advance care planning, please visit
CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada. For more information about advance care planning, please visit
SERVICE SPECIFICATION
 SERVICE SPECIFICATION Service Rotherham Hospice Lead Gail Palmer Provider Lead Paula Hill / Mike Wilkerson Period 21 st July 2010 20 th July 2013 1. Purpose This specification describes the services which
SERVICE SPECIFICATION Service Rotherham Hospice Lead Gail Palmer Provider Lead Paula Hill / Mike Wilkerson Period 21 st July 2010 20 th July 2013 1. Purpose This specification describes the services which
Palliative Care Nurse Practitioner Candidate Clinical Competencies
 Palliative Care Nurse Practitioner Candidate Clinical Competencies Enhancing care through excellence in education and research Authors: Karen Quinn, Coordinator Education and Project Officer for Victorian
Palliative Care Nurse Practitioner Candidate Clinical Competencies Enhancing care through excellence in education and research Authors: Karen Quinn, Coordinator Education and Project Officer for Victorian
Gippsland Model for After-Hours Palliative Care. Action Plan
 Gippsland Model for After-Hours Palliative Care Action Plan 2014-15 Background Six key elements are identified in the After-hours palliative care framework 1 (the Framework): 1. Best practice care planning
Gippsland Model for After-Hours Palliative Care Action Plan 2014-15 Background Six key elements are identified in the After-hours palliative care framework 1 (the Framework): 1. Best practice care planning
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee
 Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Strategic Plan Eastern Palliative Care Inc: Strategic Plan
 Strategic Plan 2017-2020 Eastern Palliative Care Inc: Strategic Plan 2017-2020 1 Table of Contents 1. Introduction from Chair and CEO 2 2. Our purpose 3 3. Our role 3 4. Our values 3 5. Our history and
Strategic Plan 2017-2020 Eastern Palliative Care Inc: Strategic Plan 2017-2020 1 Table of Contents 1. Introduction from Chair and CEO 2 2. Our purpose 3 3. Our role 3 4. Our values 3 5. Our history and
Banksia Palliative Care Service
 Banksia Palliative Care Service PCOC Initiative Departmental Action Plan Andrea McGee Manager Clinical Services & Learning Centre Linda Espie Manager Client Support Services (In absentia) Introducing Banksia
Banksia Palliative Care Service PCOC Initiative Departmental Action Plan Andrea McGee Manager Clinical Services & Learning Centre Linda Espie Manager Client Support Services (In absentia) Introducing Banksia
Informed Consent for Treatment/Intervention VHA Clinical Governance in Community Health Discussion Paper March 2009
 Informed Consent for Treatment/Intervention VHA Clinical Governance in Community Health Discussion Paper March 2009 Aim The aim of this paper is to highlight the issues related to informed consent for
Informed Consent for Treatment/Intervention VHA Clinical Governance in Community Health Discussion Paper March 2009 Aim The aim of this paper is to highlight the issues related to informed consent for
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth
 Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Understanding and Managing End of Life Symptoms: A Teaching Guide for the Primary Caregiver
 St. John Fisher College Fisher Digital Publications Nursing Masters Wegmans School of Nursing 12-2013 Understanding and Managing End of Life Symptoms: A Teaching Guide for the Primary Caregiver Christine
St. John Fisher College Fisher Digital Publications Nursing Masters Wegmans School of Nursing 12-2013 Understanding and Managing End of Life Symptoms: A Teaching Guide for the Primary Caregiver Christine
Educational Goals & Objectives
 Educational Goals & Objectives Primary care physicians are involved with patients over the course of their lives. Many of these patients will develop serious and/or life-threatening illnesses that affect
Educational Goals & Objectives Primary care physicians are involved with patients over the course of their lives. Many of these patients will develop serious and/or life-threatening illnesses that affect
Objectives: Documents/crossroads marie curie single point.doc
 PILOT PROTOCOL SINGLE POINT OF ACCESS FOR END OF LIFE CARE PROVIDED BY CROSSROADS CARE MACMILLAN PALLIATIVE CARE SERVICE & MARIE CURIE CANCER CARE EASTERN CHESHIRE CLINICAL COMMISSIONING LOCALITY Crossroads
PILOT PROTOCOL SINGLE POINT OF ACCESS FOR END OF LIFE CARE PROVIDED BY CROSSROADS CARE MACMILLAN PALLIATIVE CARE SERVICE & MARIE CURIE CANCER CARE EASTERN CHESHIRE CLINICAL COMMISSIONING LOCALITY Crossroads
transitions in care what we heard
 transitions in care what we heard Early in 2018, Health Quality Ontario asked Ontarians a simple question: what affected your transition from hospital to home? Good and bad. Big and small. We wanted to
transitions in care what we heard Early in 2018, Health Quality Ontario asked Ontarians a simple question: what affected your transition from hospital to home? Good and bad. Big and small. We wanted to
Making Your Wishes Known With the Help of the Five Wishes Document
 Making Your Wishes Known With the Help of the Five Wishes Document Lora Rhodes, MSW, LSW Oncology Social Worker Department of Medical Oncology LBBC: Annual Conference for Women living with Metastatic Breast
Making Your Wishes Known With the Help of the Five Wishes Document Lora Rhodes, MSW, LSW Oncology Social Worker Department of Medical Oncology LBBC: Annual Conference for Women living with Metastatic Breast
The Health Literacy Framework will focus on people with chronic conditions and complex care needs, including people with mental illness.
 Northern NSW Health Literacy Framework June 2016 Background The Northern NSW Local Health District (NNSW LHD) and North Coast Primary Health Network (NCPHN) have a shared commitment to creating an integrated
Northern NSW Health Literacy Framework June 2016 Background The Northern NSW Local Health District (NNSW LHD) and North Coast Primary Health Network (NCPHN) have a shared commitment to creating an integrated
FACILITATOR GUIDE. inotice Professional Development Program and Resources
 inotice Professional Development Program and Resources FACILITATOR GUIDE Heightened awareness of safe medication management for aged care community workers Contents BACKGROUND... 3 INTRODUCTION... 4 FACILITATION...
inotice Professional Development Program and Resources FACILITATOR GUIDE Heightened awareness of safe medication management for aged care community workers Contents BACKGROUND... 3 INTRODUCTION... 4 FACILITATION...
Appendix 1 -Summary of palliative care patients (modified SCR1 form from Gold standards Framework)
 Appendix 1 -Summary of palliative care patients (modified SCR1 form from Gold standards Framework) Name of patient/ Name of carer Diagnosis (+code) DNAR form Y/N GP DN Problems/ Concerns Anticipated needs
Appendix 1 -Summary of palliative care patients (modified SCR1 form from Gold standards Framework) Name of patient/ Name of carer Diagnosis (+code) DNAR form Y/N GP DN Problems/ Concerns Anticipated needs
CARE OF THE DYING IN THE NHS. The Buckinghamshire Communique 11 th March The Nuffield Trust
 CARE OF THE DYING IN THE NHS The Buckinghamshire Communique 11 th March 2003 The Nuffield Trust Everyone should be able to expect a good death and to exert control, as far as possible, over the process
CARE OF THE DYING IN THE NHS The Buckinghamshire Communique 11 th March 2003 The Nuffield Trust Everyone should be able to expect a good death and to exert control, as far as possible, over the process
I no longer feel alone with this
 I no longer feel alone with this Supportive cancer care by non-cancer community nurses in regional Victoria Or Its all about 2010 It all started here Feeling isolated Desire for local support Partnership
I no longer feel alone with this Supportive cancer care by non-cancer community nurses in regional Victoria Or Its all about 2010 It all started here Feeling isolated Desire for local support Partnership
What Is Hospice? Answers to Your Questions
 What Is Hospice? Answers to Your Questions Dear Prospective NorthShore Hospice Patients, Welcome! When you choose NorthShore Hospice, it means that you have surrounded yourself with an interdisciplinary
What Is Hospice? Answers to Your Questions Dear Prospective NorthShore Hospice Patients, Welcome! When you choose NorthShore Hospice, it means that you have surrounded yourself with an interdisciplinary
POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case
 POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case DOCUMENT NO: DN116 Lead author/initiator(s): Sarah Woodley Community Health Services Pharmacist sarah.woodley@ccs.nhs.uk
POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case DOCUMENT NO: DN116 Lead author/initiator(s): Sarah Woodley Community Health Services Pharmacist sarah.woodley@ccs.nhs.uk
Marie Curie Northern Ireland Patient Guide
 Marie Curie Northern Ireland Patient Guide Date of Issue: November 2014 Review date: November 2017 Contents 1. Introduction 1 2. Respect for patient s rights 3 3. What you can expect from our staff and
Marie Curie Northern Ireland Patient Guide Date of Issue: November 2014 Review date: November 2017 Contents 1. Introduction 1 2. Respect for patient s rights 3 3. What you can expect from our staff and
Policy for Anticipatory Prescribing and Just in Case Bags
 Policy for Anticipatory Prescribing and Just in Case Bags This policy was developed by Milton Keynes End of Life Care Medicine Group and has been adopted by all partner organisations (MK Clinical Commissioning
Policy for Anticipatory Prescribing and Just in Case Bags This policy was developed by Milton Keynes End of Life Care Medicine Group and has been adopted by all partner organisations (MK Clinical Commissioning
Suffolk End of Life Care Guidelines
 In partnership with: West Suffolk NHS Foundation Trust, The Ipswich Hospital, Suffolk Community Healthcare, St Nicholas Hospice Care, St Elizabeth Hospice, Adult Community Services, NHS Ipswich and East
In partnership with: West Suffolk NHS Foundation Trust, The Ipswich Hospital, Suffolk Community Healthcare, St Nicholas Hospice Care, St Elizabeth Hospice, Adult Community Services, NHS Ipswich and East
Patient and carer experiences: palliative care services national survey report: November 2010
 University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 1 Patient and carer experiences: palliative care services national survey report: November 1 -
University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 1 Patient and carer experiences: palliative care services national survey report: November 1 -
Nursing Role in Renal Supportive Care.
 Nursing Role in Renal Supportive Care. How far have we come and where to from here? Renal Supportive Care Symposium 2015 Elizabeth Josland Renal Supportive Care CNC St George Hospital Content Definition
Nursing Role in Renal Supportive Care. How far have we come and where to from here? Renal Supportive Care Symposium 2015 Elizabeth Josland Renal Supportive Care CNC St George Hospital Content Definition
VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES
 VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES Care Initiation: Critical Interventions VNAA Best Practice for Hospice and Palliative Care The first few days following a patient s admission to
VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES Care Initiation: Critical Interventions VNAA Best Practice for Hospice and Palliative Care The first few days following a patient s admission to
Hospice 101. Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati
 Hospice 101 Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati Hospice of Cincinnati Hospice of Cincinnati creates the best possible and most meaningful EOL experience for all who
Hospice 101 Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati Hospice of Cincinnati Hospice of Cincinnati creates the best possible and most meaningful EOL experience for all who
We need to talk about Palliative Care. The Care Inspectorate
 We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
SELF - ADMINISTRATION OF MEDICINES AND ADMINISTRATION OF MEDICINES SUPPORTED BY FAMILY/INFORMAL CARERS OF PATIENTS IN COMMUNITY NURSING
 CLINICAL PROTOCOL SELF - ADMINISTRATION OF MEDICINES AND ADMINISTRATION OF MEDICINES SUPPORTED BY FAMILY/INFORMAL CARERS OF PATIENTS IN COMMUNITY NURSING RATIONALE Medication errors can cause unnecessary
CLINICAL PROTOCOL SELF - ADMINISTRATION OF MEDICINES AND ADMINISTRATION OF MEDICINES SUPPORTED BY FAMILY/INFORMAL CARERS OF PATIENTS IN COMMUNITY NURSING RATIONALE Medication errors can cause unnecessary
An overview of Marie Curie s services
 An overview of Marie Curie s services Marie Curie Cancer Care is a charity dedicated to the care of people with any terminal illness. We provide high quality care and support through the Marie Curie Nursing
An overview of Marie Curie s services Marie Curie Cancer Care is a charity dedicated to the care of people with any terminal illness. We provide high quality care and support through the Marie Curie Nursing
Providing Hospice Care in a SNF/NF or ICF/IID facility
 Providing Hospice Care in a SNF/NF or ICF/IID facility Education program Insert name of your hospice program Insert your logo Objectives Review the philosophy of hospice care and discuss what hospice care
Providing Hospice Care in a SNF/NF or ICF/IID facility Education program Insert name of your hospice program Insert your logo Objectives Review the philosophy of hospice care and discuss what hospice care
Service Mapping Report
 Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Building the capacity for palliative care in residential homes for the elderly in Hong Kong
 Building the capacity for palliative care in residential homes for the elderly in Hong Kong Samantha Mei-che PANG RN, PhD, Professor School of Nursing, The Hong Kong Polytechnic University Why palliative
Building the capacity for palliative care in residential homes for the elderly in Hong Kong Samantha Mei-che PANG RN, PhD, Professor School of Nursing, The Hong Kong Polytechnic University Why palliative
CHEMOTHERAPY TREATMENT RECORD
 CHEMOTHERAPY TREATMENT RECORD Consultant.. Name DOB.. Hospital Number. PRIMARY DIAGNOSIS MDT discussion date.. Consent for treatment obtained Yes / No Consent Form signed Yes / No (If no do not give Chemotherapy
CHEMOTHERAPY TREATMENT RECORD Consultant.. Name DOB.. Hospital Number. PRIMARY DIAGNOSIS MDT discussion date.. Consent for treatment obtained Yes / No Consent Form signed Yes / No (If no do not give Chemotherapy
End-of-Life Nursing Education Consortium
 End-of-Life Nursing Education Consortium Celebrating 15 years DEDICATED TO EDUCATION AND PROMOTING EXCELLENT PALLIATIVE CARE END-OF-LIFE NURSING EDUCATION CONSORTIUM Millions this year will need your help
End-of-Life Nursing Education Consortium Celebrating 15 years DEDICATED TO EDUCATION AND PROMOTING EXCELLENT PALLIATIVE CARE END-OF-LIFE NURSING EDUCATION CONSORTIUM Millions this year will need your help
Scottish Palliative Care Guidelines Rapid Transfer Home in the Last Days of Life
 Rapid Transfer Home in the Last Days of Life Management Follow five steps below to: facilitate a peaceful death in the patient s preferred place facilitate seamless transfer from hospital or hospice to
Rapid Transfer Home in the Last Days of Life Management Follow five steps below to: facilitate a peaceful death in the patient s preferred place facilitate seamless transfer from hospital or hospice to
Bill Brown Scenario. Bea Console
 Bea Console Your life: You are the bereavement counseling coordinator for hospice. You provide supportive services to help meet the emotional needs of patients and families who are struggling with the
Bea Console Your life: You are the bereavement counseling coordinator for hospice. You provide supportive services to help meet the emotional needs of patients and families who are struggling with the
1. Guidance notes. Social care (Adults, England) Knowledge set for medication. What are knowledge sets? Why were knowledge sets commissioned?
 Social care (Adults, England) Knowledge set for medication 1. Guidance notes What are knowledge sets? Part of the sector skills council Skills for Care and Development Knowledge sets are sets of key learning
Social care (Adults, England) Knowledge set for medication 1. Guidance notes What are knowledge sets? Part of the sector skills council Skills for Care and Development Knowledge sets are sets of key learning
Patient views of over 75 years health assessments in general practice
 Patient views of over 75 years health assessments in general practice AUTHORS Margaret Spillman B.Sc. (Hons) Geography Research worker, School of Medicine & Dentistry, James Cook University, Rural Health
Patient views of over 75 years health assessments in general practice AUTHORS Margaret Spillman B.Sc. (Hons) Geography Research worker, School of Medicine & Dentistry, James Cook University, Rural Health
Everyone s talking about outcomes
 WHO Collaborating Centre for Palliative Care & Older People Everyone s talking about outcomes Fliss Murtagh Cicely Saunders Institute Department of Palliative Care, Policy & Rehabilitation King s College
WHO Collaborating Centre for Palliative Care & Older People Everyone s talking about outcomes Fliss Murtagh Cicely Saunders Institute Department of Palliative Care, Policy & Rehabilitation King s College
NHS CANCER SERVICES FOR CHILDREN
 NHS CANCER SERVICES FOR CHILDREN 2 NHS cancer services for children WHAT YOU CAN EXPECT When you ve heard that your child has cancer, there s a lot to take in. It can feel overwhelming, and be difficult
NHS CANCER SERVICES FOR CHILDREN 2 NHS cancer services for children WHAT YOU CAN EXPECT When you ve heard that your child has cancer, there s a lot to take in. It can feel overwhelming, and be difficult
Connected Palliative Care Partnership End of Year Report
 where everyone matters Sandwell and West Birmingham Hospitals NHS Trust Connected Palliative Care Partnership End of Year Report 2016 2017 Sandwell and West Birmingham Clinical Commissioning Group Contents
where everyone matters Sandwell and West Birmingham Hospitals NHS Trust Connected Palliative Care Partnership End of Year Report 2016 2017 Sandwell and West Birmingham Clinical Commissioning Group Contents
A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland
 A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland The aim of this session To refresh our memories about what a competency is To give a bit
A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland The aim of this session To refresh our memories about what a competency is To give a bit
Top tips for prescribing in palliative care. Dr Stephanie Lippett
 Top tips for prescribing in palliative care Dr Stephanie Lippett contents Tips Pain management Anticipatory prescribing DNACPR 3 things that primary care can do to improve things for patients/themselves
Top tips for prescribing in palliative care Dr Stephanie Lippett contents Tips Pain management Anticipatory prescribing DNACPR 3 things that primary care can do to improve things for patients/themselves
