Strategies to Support the Integration of Behavioral Health and Primary Care: What Have We Learned Thus Far?
|
|
|
- Allison Skinner
- 5 years ago
- Views:
Transcription
1 COMMENTARY Strategies to Support the Integration of Behavioral Health and Primary Care: What Have We Learned Thus Far? W. Perry Dickinson, MD The articles in this supplement contain a wealth of practical information regarding the integration of behavioral health and primary care. This type of integration effort is complex and greatly benefits from support from outside organizations, as well as collaboration with other practices attempting similar work. This editorial extracts from these articles some of the key lessons learned regarding the integration of behavioral health and primary care for practices and for organizations that support practice transformation. (J Am Board Fam Med 2015;28:S102 S106.) Keywords: Behavioral Medicine; Delivery of Health Care, Integrated; Mental Health; Primary Health Care; Quality of Health Care The integration of behavioral health care and primary care has become an area of focus in health care redesign efforts, with evidence that integrated care is essential to accomplishing the Triple Aim. 1 4 As in the other articles in this issue, we use the following definitions modified from Peek 5 and Butler and colleagues. 6 Behavioral health care includes care for patients around mental health and substance use conditions, health behavior change, life stressors and crises, and stress-related physical symptoms. Integrated care is care rendered by a practice team of primary care and behavioral health providers, working together with patients and families and using a systematic and cost-effective approach to provide patient-centered care. Although many primary care practices, including those involved in the studies described in this issue, have worked hard to implement integrated behavioral health care despite payment and other This article was peer reviewed. Submitted 30 March 2015; revised 26 April 2015; accepted 30 April From the Department of Family Medicine, University of Colorado School of Medicine, Aurora. Funding: This research was supported by a grant from the Colorado Health Foundation (CHF-3848). Conflict of interest: none declared. Corresponding author: Perry Dickinson, MD, Department of Family Medicine, University of Colorado School of Medicine, East 17th Avenue, Mail Stop F496, Aurora, CO perry.dickinson@ucdenver.edu. barriers, this involves trailblazing challenging terrain. The studies in this issue describe hard-earned lessons learned and effective strategies to assist practices embarking on this important work. Practice transformation in general and behavioral health integration specifically are challenging innovations for practices that are bombarded with new programs requiring multiple major changes. Most primary care practices have few mechanisms for rapidly incorporating new programs, which can slow adoption of innovations and cause disruptions when innovations are finally implemented Multiple methods have emerged to assist practices in practice transformation efforts. In particular, practice facilitation has emerged as a key method for assisting practices with organizational changes. 7 8,12 15 Facilitators assist practices in implementing quality improvement and change management programs, improving incorporation of innovations into operations and increasing sustainability. Studies suggest that the use of practice facilitation and other methods such as learning collaboratives to support practices in difficult transformation and quality improvement efforts results in better outcomes However, there are few studies that have specifically dealt with transformation support for behavioral health integration. What are the key lessons learned in this set of studies that can inform efforts to support practices in behavioral S102 JABFM September October 2015 Vol. 28 Supplement
2 health integration? And what may be different for behavioral health integration efforts from other types of practice transformation? This editorial addresses those questions, with a primary focus on behavioral health integration in primary care practices. Team-Based Care and Change Management A particularly crucial area of focus for behavioral health integration is the establishment of highly functional interprofessional teams for patient care. Although this is important in most models for practice transformation, behavioral health integration centers on bringing together professionals who have traditionally operated with different approaches and philosophies for seamless, teambased care. This requires focused, intentional work that can be greatly assisted by outside facilitation. Many practices attempting behavioral health integration have just added people working in parallel in their own siloes and using their standard approaches to care. Although this can have limited success, it does not result in the advances and improvements in care that are possible through spending the time to develop new, team-based integrated approaches. Building on the different cultures and approaches brought by medical and behavioral clinicians, practices must develop a shared vision and mental model for integration to guide the transformation process. This involves changes and the development of new skills for everyone in the practice. 16 An interprofessional, team-based process for implementing behavioral health integration helps in developing trust and rapport, learning each other s strengths and roles, understanding potential gaps, and developing effective work flows and care processes. Although the use of interprofessional quality improvement teams is standard for most practice transformation support efforts, it is particularly crucial for behavioral health integration. Workforce and Training Issues Practices implementing behavioral health integration models report considerable difficulty finding behavioral health clinicians trained in brief, solution-focused interventions, adaptable to the pace of primary care, and having an understanding of the broad-based needs of a primary care population. 17 Practices also report challenges in finding primary care clinicians with a willingness and ability to work as a team, sharing the responsibility for patient care with other clinicians and incorporating their expertise into patient care. Primary care clinicians have to be able to identify and initially deal with patients behavioral needs and then know when and how to involve behavioral health clinicians. Practice staff members require new skills in identifying behavioral health issues, facilitating screening and warm handoffs between clinicians, and dealing with sensitive and emotional issues that they may not have previously faced. All this requires thoughtful attention to training and mentoring of existing and new clinicians and staff members, with everyone learning together how to optimally adopt the new teambased integrated care. Practices that have been successful in adopting integrated models over time devote major time and effort to train and onboard new behavioral health and primary care clinicians. The onboarding process includes socializing the new clinicians to the practice culture, vision for integrated care, model of care and workflow, and promoting the development of trust and rapport and an understanding of everyone s skills and roles. This involves training programs, training manuals, an initial process of having clinicians shadow each other, ongoing mentoring, and ongoing interprofessional team meetings. 17 Support organizations must collect best practices, assist in the development of shared training programs and resources, and assist in the development of mentoring across practices within a learning community. Care Processes and Structures Team-based care in behavioral health integration requires the careful consideration of how clinicians and staff will work together to meet the needs of specific patients. Cohen et al 18 describe the use of consulting, coordinating, and collaborating as approaches depending on the clinical task. Huddles or other structured or unstructured meetings can be used to plan care on an ongoing basis, with interprofessional complex care meetings to focus on patients with more difficult issues. The ability to quickly access other clinicians to discuss patient issues or do warm handoffs often shapes the level of integration in the practice Proximity of clinicians and staff members shapes integrated care through the logistic ease of making contact with each other. This requires a thoughtful doi: /jabfm.2015.S Strategies to Support the Integration of Care S103
3 shaping or adaptation of space, workflows, protocols, and data systems (electronic health records [EHRs] and shared care plans). As described in the Article by Gunn et al, 19 the design of the physical space often shaped the quality and frequency of interactions and the level of integration of care. There is a necessary and important balance of proximity to encourage and enhance interaction and provision of personal workspace to perform work tasks with privacy and/or peace and quiet when needed. 19 The use of cell phones, instant messaging, and other methods for asynchronous communication can help, but they are no substitute for physical proximity. Although extensive consultation regarding the design of space is likely beyond the capacity of most practice support organizations, it is important that these issues be raised for consideration for practices implementing integrated models of care. Quality improvement teams implementing behavioral health integration must develop workflows and care pathways that are understood by everyone in the practice and that consider all aspects of the identification of behavioral health issues, the transitions of care between primary care and behavioral health clinicians, and the coordinated referral of patients needing more intensive or long-term care. Decisions regarding the identification of patients with behavioral health issues are a critical and deceptively complicated initial process needing consideration. Systematic screening results in a reliable process that identifies patients needing services and also provides data to better understand the needs of the patient population and to refine the integration approach. 16 Systematic screening results in a greater reach of services and more accurate patient identification than nonsystematic screening that relies on clinician judgment. However, decisions regarding screening have to balance the targeted reach and the capacity of the available behavioral health services identifying the targeted population, but being able to then deliver services to the identified patients. 16,20 21 Broad-based, systematic screening can identify a large volume of behavioral health needs that can very quickly overwhelm the capacity of the available behavioral health clinicians. This requires careful planning and consideration of the different models for implementing behavioral health care in the practice. The consideration and tracking of reach to plan and fine tune interventions such as behavioral health integration is a fundamental skill for practices, and one that practice support organizations must begin to foster. 21 As is well described in the Article by Davis et al, 20 the planning of patient scheduling and patient transitions is inescapably intertwined with decisions regarding patient identification. Although integrated behavioral health care models promote brief, primary care, problem-focused interventions and warm handoffs between clinicians, most behavioral health clinicians are trained in and more comfortable with traditional behavioral health interventions, with longer appointments with patients referred by the primary care clinician. For practices using more integrated approaches, the scheduling pattern can either enable or prevent real-time behavioral health clinician availability for warm handoffs and brief, integrated interventions. A variety of models are used for scheduling counseling visits while keeping availability for warm handoffs and dealing with issues emerging during care sessions. Scheduling return patients in a way that maintains availability for arising issues requires matching the pattern to the usual flow of patients in the practice, including identifying when real-time availability is most needed. The establishment of norms with staff and patients that interruptions are acceptable and permitted even while the behavioral health clinician is in the room with a patient also helps maintain availability. 20 Scheduling behavioral health clinicians in traditional blocks for more intensive, traditional counseling has advantages in billing and predictable scheduling, with little or no down time for the clinicians. However, this model results in limited ability for warm handoffs, consultations, or brief interventions and predominantly works in a referral framework. Some practices are adopting combined models, with scheduling of behavioral health clinicians that can allow both longer visits for traditional counseling and strategic open slots for availability for warm handoffs and brief visits, or with different behavioral health clinicians employing different scheduling approaches to make room for both models of care. Developing coordinated systems for consultation with or referral to psychiatry and long-term counseling resources is a crucial part of implementing integrated care. 16 This can be challenging when the practice hires a behavioral health clinician directly instead of contracting for the clinician s ser- S104 JABFM September October 2015 Vol. 28 Supplement
4 vices through a mental health center. This will often involve enhanced connections with a mental health center, community psychiatrists, and/or other community resources. Practice transformation support organizations can play an important role in facilitating connections among practices and community resources to improve the coordination of care in these situations. Data and Health Information Technology Issues EHRs have offered the promise of improved sharing of records across clinicians and the extraction of important clinical data for quality improvement and population management. However, there is perhaps no clinical area in which EHRs have fallen as short on this promise as in integrated care. 22 Practices commonly use separate record systems for behavioral health and medical care, and even those working from the same EHR often restrict access to important behavioral health or primary care information due to HIPAA concerns. This results in clinicians having to use double documentation, scanning, and paper documents to work around these limitations. EHRs generally lack places to document behavioral health information as structured data that could be extracted from the system. All this results in difficulty for clinicians in communicating and sharing key information regarding patients, an inability to effectively track the care that patients are receiving, and a deficit of data for quality improvement regarding integration efforts. The sharing of patient information is crucial for team-based care, and data are necessary for the provision of effective care. Practice transformation organizations or other groups supporting practices in behavioral health integration efforts should include data support tailored to the practice circumstances among the services provided to practices. Conclusion This is an exciting era for primary care practice transformation, and no area of care is riper for innovation and change than behavioral health integration in primary care. This is not a one-size-fitsall phenomenon, as is clear from the reports in this issue. New and adaptive care models are needed to fit with local needs, practice context, and new payment models. This is a complex matching process with a tremendous amount of room for innovation. Practices can be successful innovating on their own, but are generally much more successful working on complex issues such as behavioral health integration in learning collaboratives and with outside assistance. Practices and practice support organizations must learn from each other to move forward with behavioral health integration. The lessons learned that are shared in this JABFM supplement provide direction and a great start for such efforts. References 1. Butler M, Kane RL, McAlpin D, et al. Integration of mental health/substance abuse and primary care No. 173 (Prepared by the Minnesota Evidence-based Practice Center under Contract No ) AHRQ Publication No. 09-E003. Rockville, MD: Agency for Healthcare Research and Quality, October Kwan B, Nease D Jr. The state of the evidence for integrated behavioral health in primary care. In: Talen MR, Burke Valeras A, eds. Integrated behavioral health in primary care. New York: Springer, 2013; Katon W, Unützer J, Fan MY, et al. Cost-effectiveness and net benefit of enhanced treatment of depression for older adults with diabetes and depression. Diabetes Care 2006;29: Unützer J, Katon WJ, Fan MY, et al. Long-term cost effects of collaborative care for late-life depression. Am J of Manag Care 2008;14: Peek CJ. Lexicon for behavioral health and primary care integration: Concepts and definitions developed by expert consensus. Rockville, MD: Agency for Healthcare Research and Quality, Available from: default/files/lexicon.pdf. Accessed April 26, Butler M, Kane RL, McAlpine D, et al. Integration of mental health/substance abuse and primary care. Evidence report/technology assessment No Rockville, MD: Agency for Healthcare Research and Quality, Available from: research/findings/evidence-based-reports/mhsapcevidence-report.pdf. Accessed April 26, Greco PJ, Eisenberg JM. Changing physicians practices. N Engl J Med 1993;329: Nagykaldi Z, Mold JW, Aspy CB. Practice facilitators: A review of the literature. Fam Med 2005;37(8): Solberg LI, Brekke ML, Fazio ML, et al. Lessons from experienced guideline implementers: Attend to many factors and use multiple strategies. Jt Comm J Qual Improv 2000;26(4): Tallia AF, Stange KC, McDaniel RR Jr, Aita VA, Miller WL, Crabtree BF. Understanding organizadoi: /jabfm.2015.S Strategies to Support the Integration of Care S105
5 tional designs of primary care practices. Jt Comm J Qual Improv 2003;48(1):45 59; discussion Wagner EH, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A. Improving chronic illness care: Translating evidence into action. Health Aff (Millwood). 2001;20(6): Baskerville NB, Liddy C, Hogg W. Systematic review and meta-analysis of practice facilitation within primary care settings. Ann Fam Med 2012;10(1): Hogg W, Baskerville N, Nykiforuk C, Mallen D. Improved preventive care in family practices with outreach facilitation: understanding success and failure. J Health Serv Res Policy 2002;7(4): Nutting PA, Crabtree BF, Stewart EE, Miller WL, Palmer RF, Stange KC, Jaen CR. Effect of facilitation on practice outcomes in the national demonstration project model of the patient-centered medical home. Ann Fam Med 2010;8(Suppl 1):S Dickinson WP, Dickinson LM, Nutting PA, et al. Practice facilitation to improve diabetes care in primary care: A report from the EPIC randomized clinical trial. Ann Fam Med 2014;12: Cohen DJ, Balasubramanian BA, Davis M, et al. Understanding care integration from the ground up: five organizing constructs that shape integrated practices. J Am Board Fam Med 2015;28:S7 S Hall J, Cohen DJ, Davis M, et al. Preparing the workforce for behavioral health and primary care integration. J Am Board Fam Med 2015;28:S41 S Cohen DJ, Davis M, Balsubramanian BA, et al. Integrating behavioral health and primary care: consulting, coordinating and collaborating among professionals. J Am Board Fam Med 2015;28:S21 S Gunn R, Davis M, Hall J, et al. Designing clinical space for the delivery of integrated behavioral health and primary care. J Am Board Fam Med 2015;28: S52 S Davis MM, Balasubramanian BA, Fernald D, et al. Clinician staffing, scheduling, and engagement strategies among primary care practices. delivering integrated care. J Am Board Fam Med 2015;28:S32 S Balasubramanian BA, Fernald D, Dickinson LM, et al. REACH of interventions integrating primary care and behavioral health. J Am Board Fam Med 2015;28:S73 S Cifuentes M, Davis M, Gunn R, Fernald D, Dickinson WP, Cohen D. Electronic health record challenges, workarounds, and solutions observed in practices integrating behavioral health and primary care. J Am Board Fam Med 2015;28:S63 S72. S106 JABFM September October 2015 Vol. 28 Supplement
To meet the challenges of a reformed health care system, primary
 Practice Facilitation to Improve Diabetes Care in Primary Care: A Report From the EPIC Randomized Clinical Trial W. Perry Dickinson, MD 1 L. Miriam Dickinson, PhD 1 Paul A. Nutting, MD, MSPH 1 Caroline
Practice Facilitation to Improve Diabetes Care in Primary Care: A Report From the EPIC Randomized Clinical Trial W. Perry Dickinson, MD 1 L. Miriam Dickinson, PhD 1 Paul A. Nutting, MD, MSPH 1 Caroline
The Integration of Behavioral Health and Primary Care: A Leadership Perspective
 The Integration of Behavioral Health and Primary Care: A Leadership Perspective Eboni Winford, Ph.D. Behavioral Health Consultant Cherokee Health Systems Our Mission To improve the quality of life for
The Integration of Behavioral Health and Primary Care: A Leadership Perspective Eboni Winford, Ph.D. Behavioral Health Consultant Cherokee Health Systems Our Mission To improve the quality of life for
Improving primary care practices in the United States is a widely. Cost Estimates for Operating a Primary Care Practice Facilitation Program
 Cost Estimates for Operating a Primary Care Practice Facilitation Program Steven D. Culler, PhD 1 Michael L. Parchman, MD 2 Raquel Lozano-Romero, MD 3 Polly H. Noel, PhD 4 Holly J. Lanham, PhD 4 Luci K.
Cost Estimates for Operating a Primary Care Practice Facilitation Program Steven D. Culler, PhD 1 Michael L. Parchman, MD 2 Raquel Lozano-Romero, MD 3 Polly H. Noel, PhD 4 Holly J. Lanham, PhD 4 Luci K.
Physical & Behavioral Health Integration (BHI): Strategies to Overcome Implementation Barriers
 Physical & Behavioral Health Integration (BHI): Strategies to Overcome Implementation Barriers March 23, 2017 A Department of Social Services PCMH Presentation Hosted by Community Health Network of CT,
Physical & Behavioral Health Integration (BHI): Strategies to Overcome Implementation Barriers March 23, 2017 A Department of Social Services PCMH Presentation Hosted by Community Health Network of CT,
Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases?
 Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases? Providing care for long-term cancer survivors? Managing depression?
Treating sinusitis? Managing obesity? Preventing heart disease? Preventing lung cancer? Managing individuals with multiple chronic diseases? Providing care for long-term cancer survivors? Managing depression?
Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers
 Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers Virna Little Journal of Health Care for the Poor and Underserved, Volume 21, Number 4, November 2010, pp. 1103-1107
Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers Virna Little Journal of Health Care for the Poor and Underserved, Volume 21, Number 4, November 2010, pp. 1103-1107
Learning Lab Objectives. Introduce evidence showing team-based primary care leads to better patient health outcomes.
 Washington, DC L11: Team-Based Care: Effective Innovations in Practice Dr. Ed Wagner, MD, MPH Director Emeritus & Senior Investigator MacColl Center for Health Care Innovation, Group Health Research Institute
Washington, DC L11: Team-Based Care: Effective Innovations in Practice Dr. Ed Wagner, MD, MPH Director Emeritus & Senior Investigator MacColl Center for Health Care Innovation, Group Health Research Institute
Central Oregon Integrated Care Collaborative: Operational Strategies for Success
 Central Oregon Integrated Care Collaborative: Operational Strategies for Success 1 May 8, 2018 2 Welcome! Mike Franz, MD, DFAACAP, FAPA Medical Director, Behavioral Health, PacificSource Thanks to the
Central Oregon Integrated Care Collaborative: Operational Strategies for Success 1 May 8, 2018 2 Welcome! Mike Franz, MD, DFAACAP, FAPA Medical Director, Behavioral Health, PacificSource Thanks to the
Culture Change. Bryan J. Weiner, Ph.D.
 Culture Change Bryan J. Weiner, Ph.D. bjweiner@uw.edu WHAT IS ORGANIZATIONAL CULTURE? The way things are done around here. WHAT KIND OF CULTURE SUPPORTS PERFORMANCE IMPROVEMENT? Learning Organization:
Culture Change Bryan J. Weiner, Ph.D. bjweiner@uw.edu WHAT IS ORGANIZATIONAL CULTURE? The way things are done around here. WHAT KIND OF CULTURE SUPPORTS PERFORMANCE IMPROVEMENT? Learning Organization:
Creating the Collaborative Care Team
 Creating the Collaborative Care Team Social Innovation Fund July 10, 2013 Social Innovation Fund Corporation for National & Community Service Federal Funder The John A. Hartford Foundation Philanthropic
Creating the Collaborative Care Team Social Innovation Fund July 10, 2013 Social Innovation Fund Corporation for National & Community Service Federal Funder The John A. Hartford Foundation Philanthropic
Strategies for Addressing Workforce Issues through Partnerships and Policy: An FQHC-University Partnership. Columbus, Ohio.
 College of Social Work Strategies for Addressing Workforce Issues through Partnerships and Policy: An FQHC-University Partnership Staci Swenson, MA, MSW, LISW S Integrated Care Manager PrimaryOne Health
College of Social Work Strategies for Addressing Workforce Issues through Partnerships and Policy: An FQHC-University Partnership Staci Swenson, MA, MSW, LISW S Integrated Care Manager PrimaryOne Health
Request for Proposal. Promoting Integrated Behavioral Health and Primary Care in New Hampshire
 One Pillsbury Street, Suite 301 Concord, New Hampshire 03301 603-228-2448 KFirth@endowmentforhealth.org Purpose: 1 P a g e Request for Proposal Promoting Integrated Behavioral Health and Primary Care in
One Pillsbury Street, Suite 301 Concord, New Hampshire 03301 603-228-2448 KFirth@endowmentforhealth.org Purpose: 1 P a g e Request for Proposal Promoting Integrated Behavioral Health and Primary Care in
Older people s mental and physical health: strengthening Primary Care
 Older people s mental and physical health: strengthening Primary Care Dr Paul Hopper 2013 Quality care, when and where you need it Contents 1. Introduction - the scale of need 2. Current approaches 3.
Older people s mental and physical health: strengthening Primary Care Dr Paul Hopper 2013 Quality care, when and where you need it Contents 1. Introduction - the scale of need 2. Current approaches 3.
Executive Summary. BHICCI Charter
 Charter Behavioral Health Integration Complex Care Initiative Charter Clinical Transformation and Integration Department, Inland Empire Health Plan 1 Executive Summary The health care system serving the
Charter Behavioral Health Integration Complex Care Initiative Charter Clinical Transformation and Integration Department, Inland Empire Health Plan 1 Executive Summary The health care system serving the
Implementing Teams in a Patient-Centered Medical Home Residency Practice: Lessons Learned
 SPECIAL COMMUNICATION Implementing Teams in a Patient-Centered Medical Home Residency Practice: Lessons Learned Tsveti Markova, MD, Maribeth Mateo, MD, and Linda M. Roth, PhD Introduction: The new model
SPECIAL COMMUNICATION Implementing Teams in a Patient-Centered Medical Home Residency Practice: Lessons Learned Tsveti Markova, MD, Maribeth Mateo, MD, and Linda M. Roth, PhD Introduction: The new model
2
 2 3 4 5 Keep moving SUCCESS REQUIRES CONTINUOUS DISRUPTION 6 7 10 11 12 13 15 Define or be defined What is integrated behavioral health and primary care? The care that results from a practice team
2 3 4 5 Keep moving SUCCESS REQUIRES CONTINUOUS DISRUPTION 6 7 10 11 12 13 15 Define or be defined What is integrated behavioral health and primary care? The care that results from a practice team
Blending Behavioral Health and Primary Care. Cherokee Health Systems Clinical Model
 Blending Behavioral Health and Primary Care Cherokee Health Systems Clinical Model Brittany Tenbarge, Ph.D. Behavioral Health Consultant Licensed Clinical Psychologist Our Mission To improve the quality
Blending Behavioral Health and Primary Care Cherokee Health Systems Clinical Model Brittany Tenbarge, Ph.D. Behavioral Health Consultant Licensed Clinical Psychologist Our Mission To improve the quality
Improving Clinical Flow ECHO Collaborative Change Package
 Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
Effects of Hospital Systems on Medical Home Transformation in Primary Care Residency Training Practices
 J Ambulatory Care Manage Vol. 00, No. 00, pp. 1 8 Copyright C 2016 Wolters Kluwer Health, Inc. All rights reserved. Effects of Hospital Systems on Medical Home Transformation in Primary Care Residency
J Ambulatory Care Manage Vol. 00, No. 00, pp. 1 8 Copyright C 2016 Wolters Kluwer Health, Inc. All rights reserved. Effects of Hospital Systems on Medical Home Transformation in Primary Care Residency
Patient Centered Medical Home Clinician Assessment
 Patient Centered Medical Home Clinician Assessment Please answer the following questions based on the procedures and approaches used by you and your immediate care team (e.g. those nurses and office staff
Patient Centered Medical Home Clinician Assessment Please answer the following questions based on the procedures and approaches used by you and your immediate care team (e.g. those nurses and office staff
Acknowledgements K Street NW, Suite 400 Washington, DC
 A Standard Framework for Levels of Integrated Healthcare April 2013 Acknowledgements A Standard Framework for Levels of Integrated Healthcare was developed for the with funds under grant number 1UR1SMO60319-01
A Standard Framework for Levels of Integrated Healthcare April 2013 Acknowledgements A Standard Framework for Levels of Integrated Healthcare was developed for the with funds under grant number 1UR1SMO60319-01
Behavioral Health Competencies in Primary Care
 Behavioral Health Competencies in Primary Care SIM Training for Practice Facilitators and Clinical HIT Advisors Shale Wong, MD, MSPH January 20, 2016 Establishing Core Competencies for Behavioral Health
Behavioral Health Competencies in Primary Care SIM Training for Practice Facilitators and Clinical HIT Advisors Shale Wong, MD, MSPH January 20, 2016 Establishing Core Competencies for Behavioral Health
Correlation of the Care by Design Primary Care Practice Redesign Model and the Principles of the Patient-Centered Medical Home
 FAMILY MEDICINE AND THE HEALTH CARE SYSTEM Correlation of the Care by Design Primary Care Practice Redesign Model and the Principles of the Patient-Centered Medical Home Marlene J. Egger, PhD, Julie Day,
FAMILY MEDICINE AND THE HEALTH CARE SYSTEM Correlation of the Care by Design Primary Care Practice Redesign Model and the Principles of the Patient-Centered Medical Home Marlene J. Egger, PhD, Julie Day,
University of California, Davis Family Practice Center: Update 2014
 University of California, Davis Family Practice Center: Update 2014 by Lisel Blash, Catherine Dower, and Susan Chapman September 2014 Center for the Health Professions at UCSF ABSTRACT In response to long
University of California, Davis Family Practice Center: Update 2014 by Lisel Blash, Catherine Dower, and Susan Chapman September 2014 Center for the Health Professions at UCSF ABSTRACT In response to long
Behavioral Health and the Comprehensive Primary Care (CPC) Initiative: findings from the 2014 CPC behavioral health survey
 Zivin et al. BMC Health Services Research (2017) 17:612 DOI 10.1186/s12913-017-2562-z RESEARCH ARTICLE Open Access Behavioral Health and the Comprehensive Primary Care (CPC) Initiative: findings from the
Zivin et al. BMC Health Services Research (2017) 17:612 DOI 10.1186/s12913-017-2562-z RESEARCH ARTICLE Open Access Behavioral Health and the Comprehensive Primary Care (CPC) Initiative: findings from the
Design Principles for Learning and Caring in Patient-Centered Primary Care Homes
 The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
CareConcepts Integrating Payor Sponsored Disease Management into Primary Care Practice
 Integrating Payor Sponsored Disease Management into Primary Care Practice Physicians Foundation for Health Systems Excellence Grant # 9600013 (2005 PFHSE Grantees) January 2006 June 2009 PO Box 762, Farmington,
Integrating Payor Sponsored Disease Management into Primary Care Practice Physicians Foundation for Health Systems Excellence Grant # 9600013 (2005 PFHSE Grantees) January 2006 June 2009 PO Box 762, Farmington,
National Council for Behavioral Health. Trauma-informed Primary Care: Fostering Resilience and Recovery Learning Community
 National Council for Behavioral Health Trauma-informed Primary Care: Fostering Resilience and Recovery Learning Community Request for Applications INTRODUCTION The National Council for Behavioral Health
National Council for Behavioral Health Trauma-informed Primary Care: Fostering Resilience and Recovery Learning Community Request for Applications INTRODUCTION The National Council for Behavioral Health
Acknowledgements Preamble to the Competencies Eight Competencies at a Glance... 4
 This document is in the public domain and may be used and reprinted without permission except those copyrighted materials that are clearly noted in the document. Further reproduction of those copyrighted
This document is in the public domain and may be used and reprinted without permission except those copyrighted materials that are clearly noted in the document. Further reproduction of those copyrighted
Organized, Evidence-based Care
 Organized, Evidence-based Care Planning Care for Individual Patients and Whole Populations MODERATOR: Nicole Van Borkulo, MEd, Practice Improvement Specialist, SNMHI, Qualis Health SPEAKERS: Ed Wagner,
Organized, Evidence-based Care Planning Care for Individual Patients and Whole Populations MODERATOR: Nicole Van Borkulo, MEd, Practice Improvement Specialist, SNMHI, Qualis Health SPEAKERS: Ed Wagner,
There is extensive evidence from randomized controlled
 Effective Implementation of Collaborative Care for Depression: What Is Needed? Robin R. Whitebird, PhD, MSW; Leif I. Solberg, MD; Nancy A. Jaeckels, BS; Pamela B. Pietruszewski, MA; Senka Hadzic, MPH;
Effective Implementation of Collaborative Care for Depression: What Is Needed? Robin R. Whitebird, PhD, MSW; Leif I. Solberg, MD; Nancy A. Jaeckels, BS; Pamela B. Pietruszewski, MA; Senka Hadzic, MPH;
Brian E. Sandoval, Psy.D. Primary Care Behavioral Health Manager Yakima Valley Farm Workers Clinic
 Clinical Integration of Behavioral Health in Washington State: The Development of Practice Standards for Primary Care Service Delivery Brian E. Sandoval, Psy.D. Primary Care Behavioral Health Manager Yakima
Clinical Integration of Behavioral Health in Washington State: The Development of Practice Standards for Primary Care Service Delivery Brian E. Sandoval, Psy.D. Primary Care Behavioral Health Manager Yakima
Healthy Hearts Northwest : A 2 x 2 Randomized Factorial Trial to Build Quality Improvement Capacity in Primary Care
 Healthy Hearts Northwest : A 2 x 2 Randomized Factorial Trial to Build Quality Improvement Capacity in Primary Care April 7, 2017 Michael Parchman, MD, MPH This project is supported by grant number R18HS023908
Healthy Hearts Northwest : A 2 x 2 Randomized Factorial Trial to Build Quality Improvement Capacity in Primary Care April 7, 2017 Michael Parchman, MD, MPH This project is supported by grant number R18HS023908
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP)
 BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
Unit 4 Evidence-Based Clinical Practice Guidelines (CPG)
 (CPG) NCQA Reference: PCMH 3 Element A Objectives Review evidence-based clinical practice guidelines Select clinical practice guidelines for JumpStart Level I Review NCQA requirements for evidence-based
(CPG) NCQA Reference: PCMH 3 Element A Objectives Review evidence-based clinical practice guidelines Select clinical practice guidelines for JumpStart Level I Review NCQA requirements for evidence-based
National Primary Care Extension Program in the United States: A Learning Network
 National Primary Care Extension Program in the United States: A Learning Network International Forum on Quality & Safety in Healthcare 2015, London England 21-24 April 2015 Robert A. Gabbay, MD, PhD, FACP
National Primary Care Extension Program in the United States: A Learning Network International Forum on Quality & Safety in Healthcare 2015, London England 21-24 April 2015 Robert A. Gabbay, MD, PhD, FACP
Value-Based Payment Model Designs for Behavioral Health Services in Primary Care
 Value-Based Payment Model Designs for Behavioral Health Services in Primary Care Using collaborative depression care management as a case study due to existing evidence, experience, and measures Robert
Value-Based Payment Model Designs for Behavioral Health Services in Primary Care Using collaborative depression care management as a case study due to existing evidence, experience, and measures Robert
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers
 Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
A National Agenda for Research in Collaborative Care. Papers From the Collaborative Care Research Network Research Development Conference
 A National Agenda for Research in Collaborative Care Papers From the Collaborative Care Research Network Research Development Conference AHRQ is the lead Federal agency charged with supporting research
A National Agenda for Research in Collaborative Care Papers From the Collaborative Care Research Network Research Development Conference AHRQ is the lead Federal agency charged with supporting research
The 10 Building Blocks of Primary Care Building Blocks of Primary Care Assessment (BBPCA)
 The 10 Building Blocks of Primary Care Building Blocks of Primary Care Assessment (BBPCA) Background and Description The Building Blocks of Primary Care Assessment is designed to assess the organizational
The 10 Building Blocks of Primary Care Building Blocks of Primary Care Assessment (BBPCA) Background and Description The Building Blocks of Primary Care Assessment is designed to assess the organizational
CHSD. Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary. Centre for Health Service Development
 CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
Admissions, Readmissions & Transitions Core Functions & Recommended Actions
 How to use this resource An important single component of COMPASS for accomplishing the goals promised to CMS is the reduction of avoidable hospital admissions and readmissions as well as emergency room
How to use this resource An important single component of COMPASS for accomplishing the goals promised to CMS is the reduction of avoidable hospital admissions and readmissions as well as emergency room
The Chronic Care Model (Katherine Gibbs and Melanie Taylor)
 The Chronic Care Model (Katherine Gibbs and Melanie Taylor) INTRODUCTION A large proportion of time spent by those working currently within the field of primary health care revolves around short consultations
The Chronic Care Model (Katherine Gibbs and Melanie Taylor) INTRODUCTION A large proportion of time spent by those working currently within the field of primary health care revolves around short consultations
Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University
 Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University Tuesday, March 2 nd, 2010 Health Care Delivery Reform In its
Brooke Salzman, MD Assistant Professor Department of Family and Community Medicine Division of Geriatric Medicine Thomas Jefferson University Tuesday, March 2 nd, 2010 Health Care Delivery Reform In its
Journal of the Association of American Medical Colleges ACCEPTED
 Journal of the Association of American Medical Colleges Uncomposed, edited manuscript published online ahead of print. This published ahead-of-print manuscript is not the final version of this article,
Journal of the Association of American Medical Colleges Uncomposed, edited manuscript published online ahead of print. This published ahead-of-print manuscript is not the final version of this article,
The Minnesota Accountable Health Model
 The Minnesota Accountable Health Model L E A R N I N G S F R O M S I M : I N T E G R AT I O N O F P R I M A R Y A N D B E H AV I O R A L H E A LT H R U R A L H E A LT H C O N F E R E N C E J U N E 2 0,
The Minnesota Accountable Health Model L E A R N I N G S F R O M S I M : I N T E G R AT I O N O F P R I M A R Y A N D B E H AV I O R A L H E A LT H R U R A L H E A LT H C O N F E R E N C E J U N E 2 0,
Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit
 ORIGINAL RESEARCH Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit Barry D. Weiss, MD, Angela G. Brega, PhD, William G. LeBlanc, PhD, Natabhona
ORIGINAL RESEARCH Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit Barry D. Weiss, MD, Angela G. Brega, PhD, William G. LeBlanc, PhD, Natabhona
Care Coordination for Behavioral Health Problems in Primary Care Settings;
 Care Coordination for Behavioral Health Problems in Primary Care Settings; How Far Can We Stretch This Approach? Chair: Mark Williams MD Speakers: Akuh Adaji MBBS PhD, Angela Mattson D.N.P, M.S., R.N.,
Care Coordination for Behavioral Health Problems in Primary Care Settings; How Far Can We Stretch This Approach? Chair: Mark Williams MD Speakers: Akuh Adaji MBBS PhD, Angela Mattson D.N.P, M.S., R.N.,
Effectively implementing multidisciplinary. population segments. A rapid review of existing evidence
 Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Does The Chronic Care Model Work?
 Does The Chronic Care Model Work? A Chartbook created by the staff of: Improving Chronic Illness Care, At Group Health s s MacColl Institute Supported by The Robert Wood Johnson Foundation Grant # 48769
Does The Chronic Care Model Work? A Chartbook created by the staff of: Improving Chronic Illness Care, At Group Health s s MacColl Institute Supported by The Robert Wood Johnson Foundation Grant # 48769
Bringing the Clinical Mindset to the Retail Pharmacist
 Bringing the Clinical Mindset to the Retail Pharmacist Sarah Griffin, Pharm.D. Harding University College of Pharmacy White County Medical Center Objectives Describe challenging situations faced by pharmacists
Bringing the Clinical Mindset to the Retail Pharmacist Sarah Griffin, Pharm.D. Harding University College of Pharmacy White County Medical Center Objectives Describe challenging situations faced by pharmacists
Using Innovation to Maximize Behavioral Health Accommodations. Regions Hospital Case Study
 Using Innovation to Maximize Behavioral Health Accommodations Regions Hospital Case Study DISCLAIMER The following slides are provided for informational purposes only and do not constitute legal advice.
Using Innovation to Maximize Behavioral Health Accommodations Regions Hospital Case Study DISCLAIMER The following slides are provided for informational purposes only and do not constitute legal advice.
Specialty Behavioral Health and Integrated Services
 Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
TRAINING THE INTEGRATED PRIMARY CARE PROFESSIONAL
 TRAINING THE INTEGRATED PRIMARY CARE PROFESSIONAL STACY OGBEIDE, PSYD, MS ASSISTANT PROFESSOR/CLINICAL DEPARTMENT OF FAMILY & COMMUNITY MEDICINE DEPARTMENT OF PSYCHIATRY UT HEALTH SAN ANTONIO OBJECTIVES
TRAINING THE INTEGRATED PRIMARY CARE PROFESSIONAL STACY OGBEIDE, PSYD, MS ASSISTANT PROFESSOR/CLINICAL DEPARTMENT OF FAMILY & COMMUNITY MEDICINE DEPARTMENT OF PSYCHIATRY UT HEALTH SAN ANTONIO OBJECTIVES
PATIENT-CENTERED MEDICAL HOME ASSESSMENT (PCMH-A)
 SAFETY NET MEDICAL HOME INITIATIVE PATIENT-CENTERED MEDICAL HOME ASSESSMENT (PCMH-A) Organization name Site name Date completed Introduction To The PCMH-A The PCMH-A is intended to help sites understand
SAFETY NET MEDICAL HOME INITIATIVE PATIENT-CENTERED MEDICAL HOME ASSESSMENT (PCMH-A) Organization name Site name Date completed Introduction To The PCMH-A The PCMH-A is intended to help sites understand
CMS Oncology Care Model s Standards for Patient Navigation
 CMS Oncology Care Model s Standards for Patient Navigation Nikolas Buescher Executive Director of Cancer Services Penn Medicine, Lancaster November 13, 2017 Ann B Barshinger Health Cancer Institute scale
CMS Oncology Care Model s Standards for Patient Navigation Nikolas Buescher Executive Director of Cancer Services Penn Medicine, Lancaster November 13, 2017 Ann B Barshinger Health Cancer Institute scale
9/13/2017. Integrated Behavioral Health (IBH) MHCF Focus Areas. A little about myself
 Integrated Behavioral Health (IBH) 2017 www.mthcf.org Scott.Malloy@mthcf.org (406)451 7060 MHCF Focus Areas Three focus areas: 1. Behavioral Health o Integrated behavioral health initiative o Strengthening
Integrated Behavioral Health (IBH) 2017 www.mthcf.org Scott.Malloy@mthcf.org (406)451 7060 MHCF Focus Areas Three focus areas: 1. Behavioral Health o Integrated behavioral health initiative o Strengthening
Health Reform in Minnesota: An Analysis of Complementary Initiatives Implementing Electronic Health Record Technology and Care Coordination
 Health Reform in Minnesota: An Analysis of Complementary Initiatives Implementing Electronic Health Record Technology and Care Coordination Karen Soderberg 1*, Sripriya Rajamani 2, Douglas Wholey 3, Martin
Health Reform in Minnesota: An Analysis of Complementary Initiatives Implementing Electronic Health Record Technology and Care Coordination Karen Soderberg 1*, Sripriya Rajamani 2, Douglas Wholey 3, Martin
COLLABORATIVE PRACTICE SUCCESSES IN PRIMARY CARE
 COLLABORATIVE PRACTICE SUCCESSES IN PRIMARY CARE KPhA Annual Meeting September 7, 2014 Tiffany R. Shin, PharmD, BCACP Lyndsey N. Hogg, PharmD, BCACP Objectives Describe basic concepts of collaborative
COLLABORATIVE PRACTICE SUCCESSES IN PRIMARY CARE KPhA Annual Meeting September 7, 2014 Tiffany R. Shin, PharmD, BCACP Lyndsey N. Hogg, PharmD, BCACP Objectives Describe basic concepts of collaborative
New Models of Care- Looking at PCMH & Telehealth
 New Models of Care- Looking at PCMH & Telehealth Paula Block, RN, BSN, Clinical Process Improvement Manager Montana Primary Care Association pblock@mtpca.org or 406.442.2750, ext. 1003 Agenda What is PCMH?
New Models of Care- Looking at PCMH & Telehealth Paula Block, RN, BSN, Clinical Process Improvement Manager Montana Primary Care Association pblock@mtpca.org or 406.442.2750, ext. 1003 Agenda What is PCMH?
Behavioral Health Integration into Adult Primary Care Model Guideline
 Behavioral Health Integration into Adult Primary Care Model Guideline Table of Contents EXECUTIVE SUMMARY:... 2 D-H GUIDELINE ENDORSEMENT STATEMENT... 4 RECOMMENDATIONS FOR D-H IMPLEMENTATION... 4 APPENDIX
Behavioral Health Integration into Adult Primary Care Model Guideline Table of Contents EXECUTIVE SUMMARY:... 2 D-H GUIDELINE ENDORSEMENT STATEMENT... 4 RECOMMENDATIONS FOR D-H IMPLEMENTATION... 4 APPENDIX
Medical Home Renovations: A Patient-centered Medical Home Case Study
 Medical Home Renovations: A Patient-centered Medical Home Case Study Robert Reid MD PhD, Group Health Research Institute Annual Snively Lecture, University of California Davis January 18, 2011 Medical
Medical Home Renovations: A Patient-centered Medical Home Case Study Robert Reid MD PhD, Group Health Research Institute Annual Snively Lecture, University of California Davis January 18, 2011 Medical
Pediatric Behavioral Health: How to Improve Primary Care Coordination and Increase Access
 Population Health Advisor Pediatric Behavioral Health: How to Improve Primary Care Coordination and Increase Access Jasmaine McClain, PhD Senior Analyst, Research McClainJ@advisory.com 6 Introducing Population
Population Health Advisor Pediatric Behavioral Health: How to Improve Primary Care Coordination and Increase Access Jasmaine McClain, PhD Senior Analyst, Research McClainJ@advisory.com 6 Introducing Population
Integrated Primary Care in Practice
 Integrated Primary Care in Practice Integrated Primary Care is at one end of a continuum of ways medical and mental health practitioners collaborate (see Doherty, et. al. below). Nationwide, when patients
Integrated Primary Care in Practice Integrated Primary Care is at one end of a continuum of ways medical and mental health practitioners collaborate (see Doherty, et. al. below). Nationwide, when patients
Working at Top of License How do you reallocate work among a team? January 28, 2015
 Working at Top of License How do you reallocate work among a team? January 28, 2015 We Want To Hear From You! Type questions into the Questions Pane at any time during this presentation Patient-Centered
Working at Top of License How do you reallocate work among a team? January 28, 2015 We Want To Hear From You! Type questions into the Questions Pane at any time during this presentation Patient-Centered
Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms
 Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms Guide for setting up IAPT-LTC services 1. Aims The
Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms Guide for setting up IAPT-LTC services 1. Aims The
A S S E S S M E N T S
 A S S E S S M E N T S Community Design Assessment This process was developed to aid healthcare organizations in taking the pulse of their community prior to the start of capital improvement projects. A
A S S E S S M E N T S Community Design Assessment This process was developed to aid healthcare organizations in taking the pulse of their community prior to the start of capital improvement projects. A
Primary Care/Behavioral Health INTEGRATION. Neal Adams, MD MPH Deputy Director California Institute for Mental Health
 Primary Care/Behavioral Health INTEGRATION Neal Adams, MD MPH Deputy Director California Institute for Mental Health Why Integrate BH & PC? BH disorder burden is great BH and physical health problems are
Primary Care/Behavioral Health INTEGRATION Neal Adams, MD MPH Deputy Director California Institute for Mental Health Why Integrate BH & PC? BH disorder burden is great BH and physical health problems are
Using Data for Proactive Patient Population Management
 Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Community Mental Health and Care integration. Zandrea Ware and Ricardo Fraga
 Community Mental Health and Care integration Zandrea Ware and Ricardo Fraga One in Five Approximately 1 in 5 adults in the U.S. 43.8 million, or 18.5% experiences mental illness in their lifetime. Community
Community Mental Health and Care integration Zandrea Ware and Ricardo Fraga One in Five Approximately 1 in 5 adults in the U.S. 43.8 million, or 18.5% experiences mental illness in their lifetime. Community
Using population health management tools to improve quality
 Using population health management tools to improve quality Jessica Diamond, MPA, CPHQ Chief Population Health Officer CHCANYS Statewide Conference and Clinical Forum Sunday, October 18, 2015 Introduction
Using population health management tools to improve quality Jessica Diamond, MPA, CPHQ Chief Population Health Officer CHCANYS Statewide Conference and Clinical Forum Sunday, October 18, 2015 Introduction
Patient Referrals to Self-Management Programs
 October 26, 2016 Patient Referrals to Self-Management Programs Janet Tennison PhD, MSW, LCSW Senior Project Manager HealthInsight Quality Innovation Network (QIN) Quality Improvement Organization (QIO)
October 26, 2016 Patient Referrals to Self-Management Programs Janet Tennison PhD, MSW, LCSW Senior Project Manager HealthInsight Quality Innovation Network (QIN) Quality Improvement Organization (QIO)
Collaborative Care in Pediatric Mental Health: A Qualitative Case Study
 Collaborative Care in Pediatric Mental Health: A Qualitative Case Study Megan McLeod, M.D. Supervised by Sourav Sengupta, M.D., M.P.H. March 3 rd, 2017 Acknowledgements Thank you Dr. Sengupta Outline 1.
Collaborative Care in Pediatric Mental Health: A Qualitative Case Study Megan McLeod, M.D. Supervised by Sourav Sengupta, M.D., M.P.H. March 3 rd, 2017 Acknowledgements Thank you Dr. Sengupta Outline 1.
YOUR HEALTH INFORMATION EXCHANGE
 YOUR HEALTH INFORMATION EXCHANGE Introduction to Health Information Exchange Healthcare organizations are experiencing substantial pressures from initiatives and reforms such as new payment models, care
YOUR HEALTH INFORMATION EXCHANGE Introduction to Health Information Exchange Healthcare organizations are experiencing substantial pressures from initiatives and reforms such as new payment models, care
Driving Patient Engagement through Mobile Care Management
 Driving Patient Engagement through Mobile Care Management Session #97, February 21, 2017 Susan Beaton, Senior Director of Provider Services and Care Management, Blue Cross Blue Shield of Nebraska Jacob
Driving Patient Engagement through Mobile Care Management Session #97, February 21, 2017 Susan Beaton, Senior Director of Provider Services and Care Management, Blue Cross Blue Shield of Nebraska Jacob
Deeper Dive on Team Roles: Part I
 Deeper Dive on Team Roles: Part I Moderator: Diane Altman Dautoff, MSW, EdD, Sr. Consultant, Qualis Health Speakers: Ed Wagner, MD, MPH, Director (Emeritus), MacColl Institute for Healthcare Innovation
Deeper Dive on Team Roles: Part I Moderator: Diane Altman Dautoff, MSW, EdD, Sr. Consultant, Qualis Health Speakers: Ed Wagner, MD, MPH, Director (Emeritus), MacColl Institute for Healthcare Innovation
CPC+ CHANGE PACKAGE January 2017
 CPC+ CHANGE PACKAGE January 2017 Table of Contents CPC+ DRIVER DIAGRAM... 3 CPC+ CHANGE PACKAGE... 4 DRIVER 1: Five Comprehensive Primary Care Functions... 4 FUNCTION 1: Access and Continuity... 4 FUNCTION
CPC+ CHANGE PACKAGE January 2017 Table of Contents CPC+ DRIVER DIAGRAM... 3 CPC+ CHANGE PACKAGE... 4 DRIVER 1: Five Comprehensive Primary Care Functions... 4 FUNCTION 1: Access and Continuity... 4 FUNCTION
ZERO SUICIDE WORK PLAN TEMPLATE
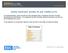 ZERO SUICIDE WORK PLAN TEMPLATE An implementation team should use this template after completing the Zero Suicide Organizational Self-Study. It is organized by Zero Suicide element and does not have to
ZERO SUICIDE WORK PLAN TEMPLATE An implementation team should use this template after completing the Zero Suicide Organizational Self-Study. It is organized by Zero Suicide element and does not have to
INTEGRATING SELF-MANAGEMENT FOR CHRONIC ILLNESSES AND PREVENTIVE BEHAVIORS INTO HEALTH CARE
 INTEGRATING SELF-MANAGEMENT FOR CHRONIC ILLNESSES AND PREVENTIVE BEHAVIORS INTO HEALTH CARE Russell E. Glasgow, Ph.D. Kaiser Permanente Colorado Denver, Colorado Overview of Presentation! The Health Care
INTEGRATING SELF-MANAGEMENT FOR CHRONIC ILLNESSES AND PREVENTIVE BEHAVIORS INTO HEALTH CARE Russell E. Glasgow, Ph.D. Kaiser Permanente Colorado Denver, Colorado Overview of Presentation! The Health Care
Three World Concept of Behavioral Health and Primary Care Integration Part 3 The Clinician Perspective
 Three World Concept of Behavioral Health and Primary Care Integration Part 3 The Clinician Perspective Colorado Behavioral Health Association October 3, 2010 Three World Model C. J. Peek suggests that
Three World Concept of Behavioral Health and Primary Care Integration Part 3 The Clinician Perspective Colorado Behavioral Health Association October 3, 2010 Three World Model C. J. Peek suggests that
Rethinking the model of primary care. Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine
 Rethinking the model of primary care Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine Why should primary care be the foundation for any healthcare
Rethinking the model of primary care Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine Why should primary care be the foundation for any healthcare
Pearson's Comprehensive Medical Assisting
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies Second Edition CHAPTER CHAPTER 9 Appointment Scheduling Lesson 1: Scheduling Systems Lesson Objectives Lesson Objectives
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies Second Edition CHAPTER CHAPTER 9 Appointment Scheduling Lesson 1: Scheduling Systems Lesson Objectives Lesson Objectives
Team-Based Care Initiative Interim Report
 F I N A L Team-Based Care Initiative Interim Report September 28, 2017 Jay Crosson Tricia Collins Higgins Lee-Lee Ellis Jasmine Little Alexander Bohn Geraldine Haile Ebo Dawson-Andoh Submitted to: The
F I N A L Team-Based Care Initiative Interim Report September 28, 2017 Jay Crosson Tricia Collins Higgins Lee-Lee Ellis Jasmine Little Alexander Bohn Geraldine Haile Ebo Dawson-Andoh Submitted to: The
Intervention to improve recruitment to randomised controlled trials
 Intervention to improve recruitment to randomised controlled trials Jenny Donovan School of Social and Community Medicine Bristol, UK Outline Problematic nature of RCT recruitment Synthesis of research
Intervention to improve recruitment to randomised controlled trials Jenny Donovan School of Social and Community Medicine Bristol, UK Outline Problematic nature of RCT recruitment Synthesis of research
The PCT Guide to Applying the 10 High Impact Changes
 The PCT Guide to Applying the 10 High Impact Changes This Guide has been produced by the NHS Modernisation Agency. For further information on the Agency or the 10 High Impact Changes please visit www.modern.nhs.uk
The PCT Guide to Applying the 10 High Impact Changes This Guide has been produced by the NHS Modernisation Agency. For further information on the Agency or the 10 High Impact Changes please visit www.modern.nhs.uk
Integrated Behavioral Health Services Austin Travis County Integral Care & CommUnityCare
 Integrated Behavioral Health Services Austin Travis County Integral Care & CommUnityCare Jim VanNorman, MD, Medical Director, ATCIC David Vander Straten, MD, FAAFP, CommUnityCare Discussion Review the
Integrated Behavioral Health Services Austin Travis County Integral Care & CommUnityCare Jim VanNorman, MD, Medical Director, ATCIC David Vander Straten, MD, FAAFP, CommUnityCare Discussion Review the
emja: Measuring patient-reported outcomes: moving from clinical trials into clinical p...
 Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Articles of Importance to Read: UnitedHealthcare Goes Live With 13th Edition of Milliman Care Guidelines. Summer 2009
 Important information for physicians and other health care professionals and facilities serving UnitedHealthcare Medicaid members Summer 2009 UnitedHealthcare Goes Live With 13th Edition of Milliman Care
Important information for physicians and other health care professionals and facilities serving UnitedHealthcare Medicaid members Summer 2009 UnitedHealthcare Goes Live With 13th Edition of Milliman Care
Who Cares About Medication Reconciliation? American Pharmacists Association American Society of Health-system Pharmacists The Joint Commission Agency
 The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH
 IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
QUALITY IMPROVEMENT. Molina Healthcare has defined the following goals for the QI Program:
 QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
Submission to the South Australian Child and Adolescent Mental Health Service Re: CAMHS Review. August 2014
 Submission to the South Australian Child and Adolescent Mental Health Service Re: CAMHS Review August 2014 Australian Association of Social Workers National Office Canberra Level 4, 33-35 Ainslie Place
Submission to the South Australian Child and Adolescent Mental Health Service Re: CAMHS Review August 2014 Australian Association of Social Workers National Office Canberra Level 4, 33-35 Ainslie Place
Adopting Accountable Care An Implementation Guide for Physician Practices
 Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Rutgers School of Nursing-Camden
 Rutgers School of Nursing-Camden Rutgers University School of Nursing-Camden Doctor of Nursing Practice (DNP) Student Capstone Handbook 2014/2015 1 1. Introduction: The DNP capstone project should demonstrate
Rutgers School of Nursing-Camden Rutgers University School of Nursing-Camden Doctor of Nursing Practice (DNP) Student Capstone Handbook 2014/2015 1 1. Introduction: The DNP capstone project should demonstrate
Joy At Work - BellinHealth and HealthPartners
 Joy At Work - BellinHealth and HealthPartners Restoring Joy in Practice through Team Based Care IHI December 2016 James Jerzak M.D. Kathy Kerscher Bellin Health Green Bay, Wisconsin 1 Agenda Crisis Emerging
Joy At Work - BellinHealth and HealthPartners Restoring Joy in Practice through Team Based Care IHI December 2016 James Jerzak M.D. Kathy Kerscher Bellin Health Green Bay, Wisconsin 1 Agenda Crisis Emerging
Using Updox to Succeed with MIPS
 Using Updox to Succeed with MIPS Who is Updox? A Communications Platform built by physicians, for physicians 56,000+ providers and more than 300,000 users--and growing 100+ EMR integrations 72 million
Using Updox to Succeed with MIPS Who is Updox? A Communications Platform built by physicians, for physicians 56,000+ providers and more than 300,000 users--and growing 100+ EMR integrations 72 million
Colorado Team-Based Care Initiative Change Package Tool Made possible with funding from the Colorado Health Foundation Contact: Alexia Eslan, JSI,
 Colorado Team-Based Care Initiative Change Package Tool Made possible with funding from the Colorado Health Foundation Contact: Alexia Eslan, JSI, aeslan@jsi.com CO Team-Based Care Initiative Change Package
Colorado Team-Based Care Initiative Change Package Tool Made possible with funding from the Colorado Health Foundation Contact: Alexia Eslan, JSI, aeslan@jsi.com CO Team-Based Care Initiative Change Package
siren Social Interventions Research & Evaluation Network Introducing the Social Interventions Research and Evaluation Network
 Introducing the Social Interventions Research and Evaluation Network Laura Gottlieb, MD, MPH Caroline Fichtenberg, PhD Nancy Adler, PhD February 27, 2017 siren Social Interventions Research & Evaluation
Introducing the Social Interventions Research and Evaluation Network Laura Gottlieb, MD, MPH Caroline Fichtenberg, PhD Nancy Adler, PhD February 27, 2017 siren Social Interventions Research & Evaluation
Exemplars in the Use of Technology for Management of Depression in Primary Care
 ORIGINAL RESEARCH Exemplars in the Use of Technology for Management of Depression in Primary Care Neftali Serrano, PsyD; Rachel Molander, MD; Kimberley Monden, PhD; Ashley Grosshans, MSW; Dean D. Krahn,
ORIGINAL RESEARCH Exemplars in the Use of Technology for Management of Depression in Primary Care Neftali Serrano, PsyD; Rachel Molander, MD; Kimberley Monden, PhD; Ashley Grosshans, MSW; Dean D. Krahn,
A Successful Patient Rounding Redesign: Staff Empowerment Blended With a Research Project
 Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing A Successful Patient Rounding Redesign: Staff Empowerment Blended With a Research Project Jody Shigo RN, CMSRN Lehigh Valley
Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing A Successful Patient Rounding Redesign: Staff Empowerment Blended With a Research Project Jody Shigo RN, CMSRN Lehigh Valley
