Cohort 20 Team 7. Improving Care Of The Pediatric Patient With A Tracheostomy
|
|
|
- Oscar Cummings
- 6 years ago
- Views:
Transcription
1 Cohort 20 Team 7 Improving Care Of The Pediatric Patient With A Tracheostomy
2 Team Members & Participants Marisa Earley, MD / Medical Resource Carlos Montano / Respiratory Resource Nelia Acuna / Nursing Resource Facilitator Edna Cruz, M.Sc., RN, CPHQ, CPPS -- Quality Resource Ad Hoc Team Members Education Staff - Rebecca Rodriquez & Rosa Leal Frontline Staff - Jene Pak, Gamze Urkun, Gina Sanchez, Jeannette Rodriguez Clinical Coordinators/ Jenny Camacho & Navil Lozano Pamela Redell Irene Sandate SPONSORS
3 Nurses, Educator, Quality Support.
4 Respiratory Support
5 Project Background Tracheostomy is one of the oldest performed surgical procedures Children born extremely premature are surviving longer and often need chronic ventilator support via tracheostomy This leads to increase use of tracheostomy in children Studies of catastrophic complications after tracheostomy Majority due to correctable deficits in: Education Nursing care Junior physician care Home care Failure to adequately secure tube Survey of community physicians: 25% are highly uncomfortable replacing tracheostomy tube, even if it were life-saving
6 Project Background Deficiencies in education of lower practitioners (i.e. non surgeons) Decrease confidence and their ability to effectively care for children with tracheostomy Nurses comfort with pediatric tracheostomy Highest with at least 5 years experience and primary ICU location Lack of standardization of education in pediatric tracheostomy care For health care providers For parents For home health aides
7 UHS Nursing Education on Tracheostomy Brief, otherwise no current education/training program or formal orientation New graduate nurses PICU=>IMC transition Seasonal Nurses Travel Nurses Unclear level of implementation Not Standardized Inconsistently Implemented Competency not assessed by preceptors assigned to new nurses No Tracheostomy Care Education Program Annual Skills Day for Tracheostomy Care insufficient training Short didactics and poster boards on topics with ~5 question quiz completed throughout the day
8 Project Aim Statement To improve clinical staff Level of Confidence and Comfort with Pediatric Tracheostomy Care on Sky 7 PICU/PIMU/PCCU by January 2018.
9 Flow Diagram MD Sporadic and disease process oriented Tracheostomy patient care Yes RN RT LVN Assess competency Mandatory in-service or training? Yes No Ready for patient care? Yes No No No Team up Remediate Reassign Reassess ready for patient care? No No tracheostomy care
10 Causes Education Plan (FLOW-Simplify) Old Existing Flow needs review & update No Mandatory Trach Education Hire of New Clinical Staff Process, Policies, Procedures (Sort, Order, Shine, Standardize, Sustain) Lack standardized competencies Old policies need review and update No bedside checklists Lack ALL emergency supplies Effect Unsafe Pediatric Care of the Patient with A Tracheostomy Clinical Staff Lack formal tracheostomy education No enforcement of education People (Education, Training, Credentials) Lack correct trach sizes Lack bedside trach care supplies Supplies not on floor/unit Equipment, Machines (Standardize, Calibrate, Software Enhancements)
11 Action Plan Aim Statement: To Improve Clinical Staff Comfort and Level of Confidence With Pediatric Tracheostomy Care on Sky 7 PICU, PIMU, and PCCU by December Action Strength Action Driver (Taken from Flow, Fishbone or Pareto) Action Who? Why? Start Date STRONG No Mandatory Tracheostomy Education Train & Educate the Team on the Integrated Old and Existing Plan With Cohort Approval. Dr. Marissa Earley Nelia Acuna Carlos Montano Standardize 4/1/2017 INTERMEDIATE Clinical Staff Lack Formal Tracheostomy Education Introduce the Plan to Staff in at Least 3 Staff Meetings. Dr. Marisa Earley Nelia Acuna Carlos Montano Standardize 3/15/2017 INTERMEDIATE No Bedside Checklists Review the Checklists & Cognitive Aides. Selected Nursing & Respiratory Teams Standardize 4/15/2017 SRONG Lack All Emergency Supplies Create Awareness and Processes Regarding Selected Nursing & Tracheostomy Tube Supplies & Location on the Respiratory Teams Floor. Standardize 5/1/2017 WEAK Old Policy Needs Revision Update Selected Nursing & Respiratory Teams Looking at Sky Video Lippincott Education for Policy & Procedure Standardize Updated & Still in review STRONG Identify the Right Scale for Survey (Likert) Initiate the Likert Survey to PICU, PIMU, PCCU, and Pedi Acute, Hemoc Dr. Marisa Earley Nelia Acuna, Rebecca Rodriguez Rosa Leal Enhance Education Pre survey 4/2017 Post 10/30/2017
12 Action Plan Standardize Education Education & Training Introduce the plan to the Nursing Staff in 3 separate staff meetings using visual aid poster board of Tracheostomy Set up training time for new staff, existing staff and seasonal staff by Educators collaborating with Respiratory Team Educate staff to access the Nursing Portal for any future dates and remediation on Tracheostomy Care Review and update the existing Tracheostomy Care Policy Reassess: Survey and observational assessment Same methods used in baseline data
13 Action Plan Continues STARDARDIZE CHECKLIST & COGNITIVE AIDES Create a checklist on what needs to be in the supply cart for an Emergency Dislodgement of Tracheostomy ( which was already developed by Respiratory Team) Organize & create an Educational Checklist for parents or care providers on care of the tracheostomy and emergency dislodgement and educate prior to discharge Teach Nurses & Respiratory to make sure the supplies in the cart are present at bedside at Hand-Off
14 Data Plan Baseline data: Survey nursing staff with questions assessing COMFORT and CONFIDENCE for various interventions on a Likert Scale Objective questions and results of Pre Survey for developing education and skills training program Possible observational assessment and rating by qualified staff (RT/MD) Intervene with educational /training program and materials **Goal would be both hands on standardized training as well as access to standardized videos and reading material Reassess: Post-survey and observational assessment Same methods used in baseline data
15 Survey Data There were 30 respondents to the Pre-Survey Identified areas for improvement Some data is surprising Overall, optimistic as everyone seems eager to learn more to improve comfort level!
16 Nursing Years of Experience TOTAL OF 30 SURVEYS LESS THAN 1 YEAR YEARS YEARS 10 GREATER THAN 10 YEARS 5
17 PEDIATRIC PICU, PCCU, & PIMU PEDIATRIC INTENSIVE CARE UNIT (PICU) 8 PEDIATRIC INTERMEDIATE UNIT (PIMU) 10 PEDIATRIC ACUTE CARE 8 PEDIATRIC HEMOTOLOGY 2 PEDIATRIC CARDIAC CARE (PCCU) 1 PEDIATRIC EMERGENCY DEPARTMENT 1
18 Q4 Did you receive tracheostomy training since starting employment at UH? Variable No 39.2% 25.0% Yes 60.8% 75.0% Q5 I have received tracheostomy training in the past. Never 7.8% 7.5% years ago or more 35.3% 25.0% year ago 37.3% 32.5% months ago 9.8% 5.0% 5 2 <6 months ago 9.8% 30.0% Q7 How long has it been since you performed a tracheostomy tube change? - Never changed tracheostomy tube 43.1% 30.0% > 1 year 29.4% 40.0% year 9.8% 15.0% months 11.8% 0.0% months 3.9% 12.5% month 2.0% 2.5% week 0.0% 0.0% Q8 My confidence level in performing routine tracheostomy care is Not at all confident 13.3% 5.0% 4 2 Not confident 13.3% 10.0% 4 4 Somewhat confident 33.3% 27.5% Confident 23.3% 37.5% 7 15 Very confident 16.7% 20.0% 5 8 Q9 My confidence level performing tracheostomy tube change is Not at all confident 26.7% 10.0% 8 4 Not confident 26.7% 22.5% 8 9 Somewhat confident 30.0% 32.5% 9 13 Confident 6.7% 25.0% 2 10 Very confident 10.0% 10.0% 3 4 Q10 My confidence level performing an emergency tracheostomy tube change is Not at all confident 30.0% 15.0% 9 6 Not confident 13.3% 22.5% 4 9 Somewhat confident 36.7% 32.5% Confident 13.3% 17.5% 4 7 Very confident 6.7% 12.5% 2 5 Q11 My experience with an emergency tracheostomy tube change was No experience 70.0% 55.0% It was pleasant, smooth 3.3% 22.5% 1 9 It was uncomfortable 16.7% 22.5% 5 9 It was terrifying 10.0% 0.0% 3 0 Q12 My training in tracheostomy care adequately prepared me for emergency tracheostomy tube change. Strongly do not agree 23.3% 12.50% 7 5 Do not agree 36.7% 20.00% 11 8 Moderately agree 10.0% 30.00% 3 12 Agree 23.3% 22.50% 7 9 Strongly agree 6.7% 15.00% 2 6 Q13 Describe your feelings regarding changing an established pediatric tracheostomy tube. This is a respiratory therapy (RT) task 10.0% 5.0% 3 2 This is a nursing task 3.3% 0.0% 1 0 This is a nursing and RT task 83.3% 95.0% This is an MD task 3.3% 0.0% 1 0
19 Q14 Describe your comfort level on changing an established pediatric tracheostomy tube. Not at all comfortable 26.7% 17.50% 8 7 Somewhat comfortable 30.0% 22.50% 9 9 Moderately comfortable 20.0% 25.00% 6 10 Comfortable 16.7% 22.50% 5 9 Extremely comfortable 6.7% 12.50% 2 5 Q15 Describe your feelings regarding accidental decannulation of pediatric tracheostomy tube, prior to the first post-operative change, e.g. a "fresh trach". This is a respiratory therapy (RT) task 6.7% 5.0% 2 2 This is a nursing task 0.0% 0.0% 0 0 This is a nursing and RT task 43.3% 45.0% This is an MD task 50.0% 50.0% Q17 Describe your feelings regarding management of accidental decannulation of an established pediatric tracheostomy tube. This is a respiratory therapy (RT) task 3.3% 0.0% 1 0 This is a nursing task 0.0% 0.0% 0 0 This is a nursing and RT task 96.7% 97.5% This is an MD task 0.0% 2.5% 0 1 Comment 1 Q18 Describe your comfort level regarding management of accidental decannulation of an established pediatric tracheostomy tube. Not at all comfortable 23.3% 20.0% 7 8 Somewhat comfortable 36.7% 25.0% Moderately comfortable 10.0% 25.0% 3 10 Comfortable 20.0% 20.0% 6 8 Extremely comfortable 10.0% 10.0% 3 4 Q19 Describe your feelings about teaching family members/caregivers how to perform tracheostomy tube changes. This is a respiratory therapy (RT) task 23.3% 25.0% 7 10 This is a nursing task 0.0% 0.0% 0 0 This is a nursing and RT task 76.7% 75.0% This is an MD task 0.0% 0.0% 0 0 Q20 Describe your comfort level related to teaching family members/caregivers how to perform tracheostomy tube change. Not at all comfortable 36.7% 35.0% Somewhat comfortable 43.3% 15.0% 13 6 Moderately comfortable 6.7% 17.5% 2 7 Comfortable 6.7% 17.5% 2 7 Extremely comfortable 6.7% 15.0% 2 6 Q21 Describe your feelings about teaching family members/caregivers how to provide tracheostomy tube care other than tube changes. This is a respiratory therapy (RT) task 10.0% 10.0% 3 4 This is a nursing task 6.7% 5.0% 2 2 This is a nursing and RT task 83.3% 85.0% This is an MD task 0.0% 0.0% 0 0 Q22 Describe your comfort level teaching family members/caregivers how to provide tracheostomy tube care other than tube change. Not at all comfortable 26.7% 20.0% 8 8 Somewhat comfortable 30.0% 22.5% 9 9 Moderately comfortable 13.3% 12.5% 4 5 Comfortable 20.0% 35.0% 6 14 Extremely comfortable 10.0% 10.0% 3 4
20 Q4 Did You Received Tracheostomy Training Since Starting Employment at UHS? Q4 Did you receive tracheostomy training since starting employment at UH? Variable No 39.2% 25.0% Yes 60.8% 75.0% % 90.0% 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% 39.2% NO Pre Survey 25% Post Survey 60.8% YES 75%
21 Q8 My confidence level in performing routine tracheostomy care is: Q8 My confidence level in performing routine tracheostomy care is Not at all confident 13.3% 5.0% 4 2 Not confident 13.3% 10.0% 4 4 Somewhat confident 33.3% 27.5% Confident 23.3% 37.5% 7 15 Very confident 16.7% 20.0% % 90.0% 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% 39.2% %% 75% 25% Not at all confident Not confident Pre Survey 33.3% 27.5% Somewhat confident Post Survey 23.3% 37.5% Confident 20.0% 16.7% Very Confident
22 Q9 My Confidence Level Performing Tracheostomy Tube Change is: Q9 My confidence level performing tracheostomy tube change is Not at all confident 26.7% 10.0% 8 4 Not confident 26.7% 22.5% 8 9 Somewhat confident 30.0% 32.5% 9 13 Confident 6.7% 25.0% 2 10 Very confident 10.0% 10.0% % Pre Survey Post Survey 90% 80% 70% 60% 50% 40% 30% 30.0% 32.5% 25.0% 20% 10% 6.7% 0% Some what Confidence Confidence
23 Q10 My Confidence Level Performing an Emergency Tracheostomy Tube Change Is: Q10 My confidence level performing an emergency tracheostomy tube change is Not at all confident 30.0% 15.0% 9 6 Not confident 13.3% 22.5% 4 9 Somewhat confident 36.7% 32.5% Confident 13.3% 17.5% 4 7 Very confident 6.7% 12.5% % Pre Survey Post Survey % 12.5% % Confident Very Confident
24 Q11 My Experience With An Emergency Tracheostomy Tube Change was Q11 My experience with an emergency tracheostomy tube change was No experience 70.0% 55.0% It was pleasant, smooth 3.3% 22.5% 1 9 It was uncomfortable 16.7% 22.5% 5 9 It was terrifying 10.0% 0.0% % 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 3.3% 22.5% It was Pleasant Smooth Pre Survey 10.0% 0.0% It was Terrifying Post Survey
25 Q12 My Training in Tracheostomy Care Adequately Prepared Me For Emergency Tracheostomy Tube Change Q12 My training in tracheostomy care adequately prepared me for emergency tracheostomy tube change. Strongly do not agree 23.3% 12.50% 7 5 Do not agree 36.7% 20.00% 11 8 Moderately agree 10.0% 30.00% 3 12 Agree 23.3% 22.50% 7 9 Strongly agree 6.7% 15.00% % 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Presurvey Postsurvey 30.0% 15.0% 10.0% 6.7% Moderately AgreeStrongly Agree
26 Q13 Describe Your Feelings Regarding Changing An Established Pediatric Tracheostomy Tube Q13 Describe your feelings regarding changing an established pediatric tracheostomy tube. This is a respiratory therapy (RT) task 10.0% 5.0% 3 2 This is a nursing task 3.3% 0.0% 1 0 This is a nursing and RT task 83.3% 95.0% This is an MD task 3.3% 0.0% 1 0 Pre Survey Post Survey 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 10.0% 5.0% This is a Respiratory (RT) Task 83.3% 95.0% This is Nursing and RT Task
27 Q14 Describe Your Comfort Level on Changing an Establish Pediatric Tracheostomy Tube Q14 Describe your comfort level on changing an established pediatric tracheostomy tube. Not at all comfortable 26.7% 17.50% 8 7 Somewhat comfortable 30.0% 22.50% 9 9 Moderately comfortable 20.0% 25.00% 6 10 Comfortable 16.7% 22.50% 5 9 Extremely comfortable 6.7% 12.50% % 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Pre Survey Post Survey 22.5% 16.7% 12.0% 6.7% Comfortable Extremely Comfortable
28 Q15 Describe Your Feelings Regarding Accidental Decannulation of Pediatric Tracheostomy Tube on First Post Operative change (Fresh Trach) Q15 Describe your feelings regarding accidental decannulation of pediatric tracheostomy tube, prior to the first post-operative change, e.g. a "fresh trach". This is a respiratory therapy (RT) task 6.7% 5.0% 2 2 This is a nursing task 0.0% 0.0% 0 0 This is a nursing and RT task 43.3% 45.0% This is an MD task 50.0% 50.0% % 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 45.0% 43.3% This is Nursing and RT Pre Survey Post Survey 50.0% 50.0% This is an MD Task
29 Q20 Describe Your Comfort Level Related to Teaching Family Members/Caregivers How to Perform a Tracheostomy Tube Change Q20 Describe your comfort level related to teaching family members/caregivers how to perform tracheostomy tube change. Not at all comfortable 36.7% 35.0% Somewhat comfortable 43.3% 15.0% 13 6 Moderately comfortable 6.7% 17.5% 2 7 Comfortable 6.7% 17.5% 2 7 Extremely comfortable 6.7% 15.0% % 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 17.5% 17.5% 15.0% 6.7% 6.7% 6.7% Moderately Comfortable Pre Survey Comfortable Post Survey Extremely Comfortable
30 Return On Investment ALOS Jan through Oct 2017 reduced from 8.0 to 4.13 Continue to measure Re-admission rate remain stable at 1 from 5 through 28 days Re-measure post survey re-admission rate. Provide for staff longevity within the acute care setting and home care environment by Reducing staff turn over/vacancies from 16.4% in 2016 to 7.6% through September 2017 Continue to measure Improve Patient Satisfaction Scores on NRC Picker Re-measure post survey Overall Hospital Rate for all Pediatric locations was 66.7 to 87.5 where the number of responses ranged from 3 to 89. The ile Rank ranged from 8 through 83. Would Recommend Hospital ranged from 64.3 to 100 where the number of responses ranged from 3 to 89. The ile Rank ranged from 2 through 100.
31 Average Length of Stay Information from University Health Systems Data Account Jan Feb Mar Apr May Jun Jul Aug Sep Oct ALOS decreased from 8.0 to 4.13
32 Reduce Staff Turn Over/Vacancies % Turn Over / Vacancies % (as of Sept) Information provided by Pamela Redell/ Director
33 NRC Picker Patient Satisfaction Hospital Rate Information provided by Annierose Abogadie, Director of Quality
34 NRC Picker Patient Satisfaction Would You Recommend Information provided by Annierose D. Abogadie, Director of Quality
35 Actions to Maintain the Gains Continue education new, establish, & seasonal Register Nurses & support staff Provide education training biannual Improve access to the Nursing Portal for remediation Hold more Just in Time education on Tracheostomy & Ventilators In-service & improve preceptors comfort level & confident to support new RN orientation Improve communication between the Nursing & Respiratory Staff Create a like mind set with the team to help care of the patient with a tracheostomy tube Increase the level of trust within the disciplines Discuss how to decrease and eliminate Nursing & Respiratory Silos/territory
36 Next Steps Re-visit the policy with NICU educators and nurses Identify the Home Health Agencies that care for Pediatric Population with tracheostomy tube Assess the Comfort/Confidence of nurses caring for Pediatric patient with a tracheostomy tube in a Home Health Provider Agency Plan Tracheostomy Fair for Promoting Education and Care for the Community Future Directions/Goals Following Moore s Expanded Outcomes Framework, we achieve Level 4/5 Participants show in an educational setting or do in practice what the educational activity intended them to be able to do Our goal would be to progress to Level 6 or 7 Level 6: Improve health status of patients due to changes in the practice behavior of participants Level 7: Improve the health status of a community of patients due to changes in practice behavior of participants This would be accomplished by extending assessment and training intervention to home health aides and parents Reference: Moore DE, et al. Achieving desired results and improved outcomes: integrating planning and assessment throughout learning activities. J Contin Educ Health Prof Winter;29(1):1-15.
37
38 References: Agarwal A, et al. Improving knowledge, technical skills, and confidence among pediatric health care providers in management of chronic tracheostomy using a simulation model. Pediatr Pulmonol Jul;51(7): Prichett CV, et al. Inpatient nursing and parental comfort in managing pediatric tracheostomy care and emergencies. JAMA Otolaryngology Head Neck Surg Feb;142(2): St. Clair JS. A New Model of Tracheostomy Care: Closing the Research Practice Gap. In: Henriksen K, Battles JB, Marks ES, et al., editors. Advances in Patient Safety: From Research to Implementation ( 3: Implementation Issues). Rockville (MD): Agency for Healthcare Research and Quality (US); 2005 Feb. Available from:
Improving Transition Home through a Standardized Discharge Process. Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016
 Improving Transition Home through a Standardized Discharge Process Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016 Objectives Identify components of the Children s Hospital Colorado
Improving Transition Home through a Standardized Discharge Process Christopher D. Baker, MD Associate Professor of Pediatrics May 10, 2016 Objectives Identify components of the Children s Hospital Colorado
Difficult Airways: All Airways are NOT Created Equal July 23, 2018
 Difficult Airways: All Airways are NOT Created Equal July 23, 2018 ACS Quality and Safety Conference Lisa Failace, MSN, RN, CCRN-K Donna Swartz, MAS, RN, CPHQ, CPPS Hackensack University Medical Center
Difficult Airways: All Airways are NOT Created Equal July 23, 2018 ACS Quality and Safety Conference Lisa Failace, MSN, RN, CCRN-K Donna Swartz, MAS, RN, CPHQ, CPPS Hackensack University Medical Center
Improve the Efficiency and Service of the Emergency Room at North Side Hospital
 Improve the Efficiency and Service of the Emergency Room at North Side Hospital John Melton, VP and CEO Washington County Operations meltonjw@msha.com Kerry Vermillion, CFO Washington County Operations
Improve the Efficiency and Service of the Emergency Room at North Side Hospital John Melton, VP and CEO Washington County Operations meltonjw@msha.com Kerry Vermillion, CFO Washington County Operations
The Effects of an Electronic Hourly Rounding Tool on Nurses Steps
 The Effects of an Electronic Hourly Rounding Tool on Nurses Steps Dr. Aimee Burch, DNP, APRN-CNS CHI Health St. Francis Katie Hottovy, Co-founder and Director of Client Services, Nobl Disclosures to Participants
The Effects of an Electronic Hourly Rounding Tool on Nurses Steps Dr. Aimee Burch, DNP, APRN-CNS CHI Health St. Francis Katie Hottovy, Co-founder and Director of Client Services, Nobl Disclosures to Participants
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience. Presented by: Fadwa Jabboury, RN, MSN
 Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
of the respiratory checklist from July1, April 30, Measures were evaluated monthly. Primary measures:
 Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
1. March RN VACANCY RATE: Overall 2320 RN vacancy rate for areas reported is 13.8%
 PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, April 2014 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. March 2014-2320 RN VACANCY RATE: Overall 2320 RN vacancy
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, April 2014 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. March 2014-2320 RN VACANCY RATE: Overall 2320 RN vacancy
Laguna Honda Lean Transformation. Laguna Honda Strategic Performance Management November 2017
 Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Laguna Honda Lean Transformation Laguna Honda Strategic Performance Management November 2017 Background MAKE IT BETTER 4. 1. Performance Improvement FIX IT Do the work and make it happen 3. Create best
Collaborate to Extubate. Clinical Safety & Effectiveness Cohort 19: Team # 7
 Collaborate to Extubate Clinical Safety & Effectiveness Cohort 19: Team # 7 The Team Division CS&E Participant: Marivel Garcia, BSRC, RRT- NPS CS&E Participant: Crisostomo Cabagay, BSN, RN, CCRN CS&E Participant:
Collaborate to Extubate Clinical Safety & Effectiveness Cohort 19: Team # 7 The Team Division CS&E Participant: Marivel Garcia, BSRC, RRT- NPS CS&E Participant: Crisostomo Cabagay, BSN, RN, CCRN CS&E Participant:
And the Evidence Shows Using Specialty Certification from The Joint Commission Improves Quality
 And the Evidence Shows Using Specialty Certification from The Joint Commission Improves Quality Leisha Buller, MSN, ACNP-BC Lindsey Canon, MSN, RNC Ashley Hodo, MSN, RN Using The Joint Commission s Certification
And the Evidence Shows Using Specialty Certification from The Joint Commission Improves Quality Leisha Buller, MSN, ACNP-BC Lindsey Canon, MSN, RNC Ashley Hodo, MSN, RN Using The Joint Commission s Certification
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November 2017
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Tina Nelson, MBA, BSN Lisa Stepp, BSN, RN Rebecca Fyffe, BSN, RN Jessica Coughenour, LPN
 Establishing a Conservative Approach to the Prevention of Pressure Ulcers with the Utilization of Data Analytics to Monitor Effectiveness of Quality Efforts and Best Practice Models Tina Nelson, MBA, BSN
Establishing a Conservative Approach to the Prevention of Pressure Ulcers with the Utilization of Data Analytics to Monitor Effectiveness of Quality Efforts and Best Practice Models Tina Nelson, MBA, BSN
Massachusetts ICU Acuity Meeting
 Massachusetts ICU Acuity Meeting Acuity Tool Certification and Reporting Requirements Acuity Tool Certification Template Suggested Guidance Acuity Tool Submission Details Submitting your acuity tool for
Massachusetts ICU Acuity Meeting Acuity Tool Certification and Reporting Requirements Acuity Tool Certification Template Suggested Guidance Acuity Tool Submission Details Submitting your acuity tool for
The presentation will begin shortly.
 The presentation will begin shortly. The content provided herein is provided for informational purposes only. The views expressed by any individual presenter are solely their own, and not necessarily the
The presentation will begin shortly. The content provided herein is provided for informational purposes only. The views expressed by any individual presenter are solely their own, and not necessarily the
Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability
 Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability How we improved Patient Safety and Quality Outcomes at Northwest Hospital Our Journey to Shared Accountability Implementation
Leveraging the Accountable Care Unit Model to create a culture of Shared Accountability How we improved Patient Safety and Quality Outcomes at Northwest Hospital Our Journey to Shared Accountability Implementation
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August 2016
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
Relational Coordination: An Imperative Influencing our Capacity to Reach the Core
 Relational Coordination: An Imperative Influencing our Capacity to Reach the Core Linda Q. Everett, PhD, RN, NEA-BC, FAAN Executive Vice President & Chief Nurse Executive Indiana University Health 12/7/2012
Relational Coordination: An Imperative Influencing our Capacity to Reach the Core Linda Q. Everett, PhD, RN, NEA-BC, FAAN Executive Vice President & Chief Nurse Executive Indiana University Health 12/7/2012
MET CALLS IN A METROPOLITAN PRIVATE HOSPITAL: A CROSS SECTIONAL STUDY
 MET CALLS IN A METROPOLITAN PRIVATE HOSPITAL: A CROSS SECTIONAL STUDY Joyce Kant, A/Prof Peter Morley, S. Murphy, R. English, L. Umstad Melbourne Private Hospital, University of Melbourne Background /
MET CALLS IN A METROPOLITAN PRIVATE HOSPITAL: A CROSS SECTIONAL STUDY Joyce Kant, A/Prof Peter Morley, S. Murphy, R. English, L. Umstad Melbourne Private Hospital, University of Melbourne Background /
4/12/2016. High Reliability and Microsystem Stress. We have no financial, professional or personal conflict of interest to disclose.
 High Reliability and Microsystem Stress Helping leaders identify and mitigate unit level stress: Next steps towards the journey of high reliability Whittney Brady RN, DNP Jackie Hausfeld, RN, MSN, NEA-BC
High Reliability and Microsystem Stress Helping leaders identify and mitigate unit level stress: Next steps towards the journey of high reliability Whittney Brady RN, DNP Jackie Hausfeld, RN, MSN, NEA-BC
Taming Length of Stay Challenges Through Analytics
 Taming Length of Stay Challenges Through Analytics March 3, 2016 Dr. Michelle Pezzani, Medical Director Utilization Management at El Camino Hospital & Palo Alto Medical Foundation (PAMF) Petrina Griesbach
Taming Length of Stay Challenges Through Analytics March 3, 2016 Dr. Michelle Pezzani, Medical Director Utilization Management at El Camino Hospital & Palo Alto Medical Foundation (PAMF) Petrina Griesbach
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2013 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer
 PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2013 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. 2320 RN Vacancy Rates for the Month of January 2013
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2013 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. 2320 RN Vacancy Rates for the Month of January 2013
1. November RN VACANCY RATE: Overall 2320 RN vacancy rate for areas reported is 12.5%
 PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, December 2013 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. November 2013-2320 RN VACANCY RATE: Overall 2320 RN
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, December 2013 Terry Dentoni, RN, MSN, CNL, Interim Chief Nursing Officer 1. November 2013-2320 RN VACANCY RATE: Overall 2320 RN
Readmission Project 2017 Janice M. Maupin, RN, MSN, CPHQ. A Catholic healthcare ministry serving Ohio and Kentucky
 Readmission Project 2017 Janice M. Maupin, RN, MSN, CPHQ A Catholic healthcare ministry serving Ohio and Kentucky 1 Mission, Values and Promise Our Mission We extend the healing ministry of Jesus by improving
Readmission Project 2017 Janice M. Maupin, RN, MSN, CPHQ A Catholic healthcare ministry serving Ohio and Kentucky 1 Mission, Values and Promise Our Mission We extend the healing ministry of Jesus by improving
Learning Objectives. Carolinas HealthCare System Who We Are
 1 Capturing Accurate Documentation Through Participation in Interdisciplinary Rounds: A Healthcare System Initiative Kay Blue, RN, BSN, CCDS, ACM, Director CDI Holley Pegram, RN, MSN, CCM, Manager CDI
1 Capturing Accurate Documentation Through Participation in Interdisciplinary Rounds: A Healthcare System Initiative Kay Blue, RN, BSN, CCDS, ACM, Director CDI Holley Pegram, RN, MSN, CCM, Manager CDI
PERFORMANCE IMPROVEMENT REPORT
 PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
PERFORMANCE IMPROVEMENT REPORT First Quarter Fiscal Year 214 October-December, 213 Daniel Coffey, CEO 1 Executive Summary The Quarterly Performance Improvement Report summarizes the measures used to monitor
Improving Outcomes for High Risk and Critically Ill Patients
 Improving Outcomes for High Risk and Critically Ill Patients KP Woodland Hills Medical Center Presented by: Sharon M. Kent RN BSN, CCRN Lynne M. Agocs-Scott RN MN, CCRN CCNS Introduction of the IHI The
Improving Outcomes for High Risk and Critically Ill Patients KP Woodland Hills Medical Center Presented by: Sharon M. Kent RN BSN, CCRN Lynne M. Agocs-Scott RN MN, CCRN CCNS Introduction of the IHI The
APP PRIVILEGES IN OTOLARYNGOLOGY
 APP PRIVILEGES IN OTOLARYNGOLOGY Education/Training Licensure (Initial and Reappointment Required Qualifications Successful completion of a PA or NP program Current Licensure as a PA or RN in the state
APP PRIVILEGES IN OTOLARYNGOLOGY Education/Training Licensure (Initial and Reappointment Required Qualifications Successful completion of a PA or NP program Current Licensure as a PA or RN in the state
Northern Health - Acute Services. Evidence Based Practice Venous Thromboembolism Prevention
 Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Maternity and Family Education
 2014 Maternity and Family Education Phone: 980-487-3983 email: crmcmaternityandfamilyeducation@carolinashealthcare.org 1 2 Maternity and Family Education Programs When it comes to having a baby, you can
2014 Maternity and Family Education Phone: 980-487-3983 email: crmcmaternityandfamilyeducation@carolinashealthcare.org 1 2 Maternity and Family Education Programs When it comes to having a baby, you can
BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL
 Publication Year: 2004 BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL Summary: Cape Canaveral hospital implemented a streamlined bedside registration process in order to reduce the time patients spent waiting
Publication Year: 2004 BEDSIDE REGISTRATION CAPE CANAVERAL HOSPITAL Summary: Cape Canaveral hospital implemented a streamlined bedside registration process in order to reduce the time patients spent waiting
Establishing a Culture of Quality and Safety and the Journey to High Reliability
 Establishing a Culture of Quality and Safety and the Journey to High Reliability Becker s Hospital Review May 9, 2013 Charles D. Stokes System Chief Operating Officer M. Michael Shabot, M.D. System Chief
Establishing a Culture of Quality and Safety and the Journey to High Reliability Becker s Hospital Review May 9, 2013 Charles D. Stokes System Chief Operating Officer M. Michael Shabot, M.D. System Chief
HOW TO DO POST-HOC RESPONSE REVIEWS
 HOW TO DO POST-HOC RESPONSE REVIEWS Ken Hillman 6 th International Symposium on Rapid Response Systems and Medical Emergency Teams Pittsburgh, USA, 11 th -12 th May 2010 ACUTE HOSPITAL SYSTEM AUDIT OF
HOW TO DO POST-HOC RESPONSE REVIEWS Ken Hillman 6 th International Symposium on Rapid Response Systems and Medical Emergency Teams Pittsburgh, USA, 11 th -12 th May 2010 ACUTE HOSPITAL SYSTEM AUDIT OF
DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING
 DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING Jenny Gilmore, BSN, RN, CMSRN Jana Jacobs, BSN, RN, CMSRN Maine Medical Center Portland, ME Objectives Describe Partnership Rounding for the staff
DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING Jenny Gilmore, BSN, RN, CMSRN Jana Jacobs, BSN, RN, CMSRN Maine Medical Center Portland, ME Objectives Describe Partnership Rounding for the staff
Medication Errors and Safety. Educating for Quality Improvement & Patient Safety
 Medication Errors and Safety Educating for Quality Improvement & Patient Safety 1 Mandie Tiball Svatek, MD has no relevant financial relationships with commercial interests to disclose. Rayanne Wilson,
Medication Errors and Safety Educating for Quality Improvement & Patient Safety 1 Mandie Tiball Svatek, MD has no relevant financial relationships with commercial interests to disclose. Rayanne Wilson,
The Digital ICU: Return On Innovation
 The Digital ICU: Return On Innovation Cheryl Hiddleson, MSN, RN, CCRN-E Director, Emory eicu Center May, 2017 The Digital ICU: Return on Innovation Cheryl Hiddleson MSN, RN, CCRN-E Director, Emory eicu
The Digital ICU: Return On Innovation Cheryl Hiddleson, MSN, RN, CCRN-E Director, Emory eicu Center May, 2017 The Digital ICU: Return on Innovation Cheryl Hiddleson MSN, RN, CCRN-E Director, Emory eicu
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue. The Development and Implementation of a Rapid Response Program at a Regional Facility
 Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Improving Pain Center Processes utilizing a Lean Team Approach
 Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
Aldijana Avdić, BSN, RN, PBMS, CPHQ Assistant Director, Patient Safety and Privacy 1
 Aldijana Avdić, BSN, RN, PBMS, CPHQ Assistant Director, Patient Safety and Privacy 1 Program Definition The timely application of evidence-based medical and surgical concepts designed to maintain hemoglobin
Aldijana Avdić, BSN, RN, PBMS, CPHQ Assistant Director, Patient Safety and Privacy 1 Program Definition The timely application of evidence-based medical and surgical concepts designed to maintain hemoglobin
Change Management at Orbost Regional Health
 Change Management at Orbost Regional Health Our change management journey 1 Medication Change System Meds at Beds 2 The slightly exaggerated before process 3 Project Goals The purpose of the Meds at Beds
Change Management at Orbost Regional Health Our change management journey 1 Medication Change System Meds at Beds 2 The slightly exaggerated before process 3 Project Goals The purpose of the Meds at Beds
Changing behaviors through education to improve patient outcomes associated with vascular access devices
 Changing behaviors through education to improve patient outcomes associated with vascular access devices Fiona Fullerton Clinical Nurse Consultant Vascular Access Surveillance Princess Alexandra Hospital,
Changing behaviors through education to improve patient outcomes associated with vascular access devices Fiona Fullerton Clinical Nurse Consultant Vascular Access Surveillance Princess Alexandra Hospital,
Driving High-Value Care via Clinical Pathways. Andrew Buchert, MD Gabriella Butler, MSN, RN
 Driving High-Value Care via Clinical Pathways Andrew Buchert, MD Gabriella Butler, MSN, RN 1 Andrew Buchert, MD Medical Director, Clinical Resource Management Children s Hospital of Pittsburgh of UPMC
Driving High-Value Care via Clinical Pathways Andrew Buchert, MD Gabriella Butler, MSN, RN 1 Andrew Buchert, MD Medical Director, Clinical Resource Management Children s Hospital of Pittsburgh of UPMC
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
Collaboration and Coordination in the MRICU: An Interprofessional Approach to Implementation of a Daily Review of Sedation Strategy, Liberation
 Collaboration and Coordination in the MRICU: An Interprofessional Approach to Implementation of a Daily Review of Sedation Strategy, Liberation Potential and Mobility Plan Amy Dean, MS, RN, CCRN Kristin
Collaboration and Coordination in the MRICU: An Interprofessional Approach to Implementation of a Daily Review of Sedation Strategy, Liberation Potential and Mobility Plan Amy Dean, MS, RN, CCRN Kristin
NCEPOD On the Right Trach?
 NCEPOD On the Right Trach? Hospital Number Tracheostomy insertion (1) Consent and WHO type (surgical) checklists should be adopted and used prior to tracheostomy insertion, wherever it is performed. Q8.
NCEPOD On the Right Trach? Hospital Number Tracheostomy insertion (1) Consent and WHO type (surgical) checklists should be adopted and used prior to tracheostomy insertion, wherever it is performed. Q8.
Improving Collaboration With Palliative Care (PC): Nurse Driven Screenings for PC Consults (C833) Oct 8, 2015 at 2pm
 2015 ANCC National Magnet Conference Week 4 of 5 Improving Collaboration With Palliative Care (PC): Nurse Driven Screenings for PC Consults (C833) Oct 8, 2015 at 2pm Melissa Browning, DNP, ARPN, CCNS Ann
2015 ANCC National Magnet Conference Week 4 of 5 Improving Collaboration With Palliative Care (PC): Nurse Driven Screenings for PC Consults (C833) Oct 8, 2015 at 2pm Melissa Browning, DNP, ARPN, CCNS Ann
REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL
 Publication Year: 2008 REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL Summary: Creation of Bed Coordinator position to improve patient flow throughout the entire hospital Hospital:
Publication Year: 2008 REASSESSING THE BED COORDINATOR S ROLE SHADY GROVE ADVENTIST HOSPITAL Summary: Creation of Bed Coordinator position to improve patient flow throughout the entire hospital Hospital:
Hip Today Home Tomorrow:
 Hip Today Home Tomorrow: A Collaborative Effort between an Orthopedic Practice and a Hospital to Create an Innovative Outpatient Total Hip Replacement Program Kimberley Murray RN MS CNS-CNOR Kelly Keenan
Hip Today Home Tomorrow: A Collaborative Effort between an Orthopedic Practice and a Hospital to Create an Innovative Outpatient Total Hip Replacement Program Kimberley Murray RN MS CNS-CNOR Kelly Keenan
2ab and 3cd. BTS Topic Selection:
 2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
2ab and 3cd. BTS Topic Selection: Meet Your Colleagues PG Pg. 3 Topic Selection Objectives By the end of this session you should be able to: List the reasons that topic selection is a critical factor in
Influence of Patient Flow on Quality Care
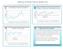 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Safer Nursing and Midwifery Staffing Recommendation The Board is asked to: NOTE the report
 To: Board of Directors Date of Meeting: 26 th July 20 Title Safer Nursing and Midwifery Staffing Responsible Executive Director Nicola Ranger, Chief Nurse Prepared by Helen O Dell, Deputy Chief Nurse Workforce
To: Board of Directors Date of Meeting: 26 th July 20 Title Safer Nursing and Midwifery Staffing Responsible Executive Director Nicola Ranger, Chief Nurse Prepared by Helen O Dell, Deputy Chief Nurse Workforce
Page 347. Avg. Case. Change Length
 Page 345 EP 8 How nurses use trended data to formulate the staffing plan and acquire necessary resources to assure consistent application of the Care Delivery Model(s). The development of operational budgets
Page 345 EP 8 How nurses use trended data to formulate the staffing plan and acquire necessary resources to assure consistent application of the Care Delivery Model(s). The development of operational budgets
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017
 HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017 Nebraska Medicine $1.2 billion academic health system 8,000 employees More than 1,000 affiliated physicians Primary
HIMSS Nicholas E. Davies Award of Excellence Case Study Nebraska Medicine October 10, 2017 Nebraska Medicine $1.2 billion academic health system 8,000 employees More than 1,000 affiliated physicians Primary
FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018
 FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018 Agenda FHA MTC Call to Action for IVAC Data Review HRET HIIN Hospital Peer Sharing
FHA Call to Action: Eliminating Infection-Related Ventilator-Associated Complications IVAC Bi-Monthly Webinar #2 May 3, 2018 Agenda FHA MTC Call to Action for IVAC Data Review HRET HIIN Hospital Peer Sharing
Case: Comparing Two Scenarios
 The Case: Case: Comparing Two Scenarios Dale Urdick and Lauren Weizhart are both Quality Improvement Managers at two large pediatric hospitals in different provinces. Although hundreds of kilomiles separate
The Case: Case: Comparing Two Scenarios Dale Urdick and Lauren Weizhart are both Quality Improvement Managers at two large pediatric hospitals in different provinces. Although hundreds of kilomiles separate
Ensuring Patient Safety and Quality Measures for RRT in AKI 2. Eileen Lischer MA, BSN, RN, CNN University of California, San Diego
 Ensuring Patient Safety and Quality Measures for RRT in AKI 2 Eileen Lischer MA, BSN, RN, CNN University of California, San Diego Today we may be doing what we can, but tomorrow we can improve Hughes,
Ensuring Patient Safety and Quality Measures for RRT in AKI 2 Eileen Lischer MA, BSN, RN, CNN University of California, San Diego Today we may be doing what we can, but tomorrow we can improve Hughes,
Compliance Division Staff Report
 Compliance Division Staff Report Polygraph Advisory Board Meeting Tuesday, September 26, 2017 Public Outreach Compliance Division routinely attends annual industry meetings held by TALEPI (Texas Association
Compliance Division Staff Report Polygraph Advisory Board Meeting Tuesday, September 26, 2017 Public Outreach Compliance Division routinely attends annual industry meetings held by TALEPI (Texas Association
Winning at Care Coordination Using Data-Driven Partnerships
 Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Idriz Limaj, LNHA, RN Chief Operating Officer Winning at Care Coordination Using Data-Driven Partnerships Session #166, February 22, 2017 1 Steven Littlehale, MS, GCNS-BC EVP & Chief Clinical Officer Speaker
Aurora will expand its geographic coverage within Wisconsin to achieve its mission to: Aurora Health Care 1991 Strategic Plan
 Objectives To describe the 20-year evolution of Aurora Medical Group within Aurora Health Care To identify the cultural characteristics necessary to improve patient access from the patient s perspective
Objectives To describe the 20-year evolution of Aurora Medical Group within Aurora Health Care To identify the cultural characteristics necessary to improve patient access from the patient s perspective
9/15/2017 THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE LEARNING OBJECTIVES
 THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE D O N N A C R I M M I N S - B O N N E L L, B S N, M H S M, C P H Q, L S S G B LEARNING OBJECTIVES 1) Define who is affected by inefficiency in throughput
THROUGHPUT. IT S NOT JUST AN EMERGENCY DEPARTMENT ISSUE D O N N A C R I M M I N S - B O N N E L L, B S N, M H S M, C P H Q, L S S G B LEARNING OBJECTIVES 1) Define who is affected by inefficiency in throughput
8/31/2015. Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN
 Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN Nurse Staffing Core vs. Float Staff 30 years ago 20-10 years ago 5 yrs Prior
Session C826 Evidence-Based Staffing Strategies Support Healthy Work-Life Balance Rachael Schweikert, RN Kevin Schwedhelm MSN RN Nurse Staffing Core vs. Float Staff 30 years ago 20-10 years ago 5 yrs Prior
Information for Hospitals wishing to join The Global Tracheostomy Collaborative (GTC)
 Information for Hospitals wishing to join The Global Tracheostomy Collaborative (GTC) What is a Quality Improvement Collaborative? (QIC) A QIC is a group of hospitals who o Agree to work together to rapidly
Information for Hospitals wishing to join The Global Tracheostomy Collaborative (GTC) What is a Quality Improvement Collaborative? (QIC) A QIC is a group of hospitals who o Agree to work together to rapidly
IMPROVING TRANSITIONS FROM ACUTE CARE TO REHAB: SPREADING CHANGE ACROSS GTA HOSPITAL SITES FOR PATIENTS POST-HIP FRACTURE
 IMPROVING TRANSITIONS FROM ACUTE CARE TO REHAB: SPREADING CHANGE ACROSS GTA HOSPITAL SITES FOR PATIENTS POST-HIP FRACTURE GTA Rehab Network Charissa Levy, Sharon Ocampo-Chan, Donna Renzetti October 2016
IMPROVING TRANSITIONS FROM ACUTE CARE TO REHAB: SPREADING CHANGE ACROSS GTA HOSPITAL SITES FOR PATIENTS POST-HIP FRACTURE GTA Rehab Network Charissa Levy, Sharon Ocampo-Chan, Donna Renzetti October 2016
Executive Director s Report: Customer Experience Update
 Executive Director s Report: Customer Experience Update Board of Directors Meeting, November 12, 215 Seconds Calls Service Center Performance 2, 18, 16, 14, 12, 1, 8, 6, 4, 2, Calls Offered Jan 215 Sept
Executive Director s Report: Customer Experience Update Board of Directors Meeting, November 12, 215 Seconds Calls Service Center Performance 2, 18, 16, 14, 12, 1, 8, 6, 4, 2, Calls Offered Jan 215 Sept
Improvements & Sustained Change through the Implementation of High Reliability Units
 Improvements & Sustained Change through the Implementation of High Reliability Units Tammy Van Dyk, MSN, RN, CPEN Quality Management & Patient Safety Manager Objective Describe how high reliability principles
Improvements & Sustained Change through the Implementation of High Reliability Units Tammy Van Dyk, MSN, RN, CPEN Quality Management & Patient Safety Manager Objective Describe how high reliability principles
Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care
 Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care April 29, 2011 Waltham, MA Presented by Lisa Payne Simon, MPH Cheryl H. Dunnington, RN, MS 1 FAST Initiative Overview 2004-2010
Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care April 29, 2011 Waltham, MA Presented by Lisa Payne Simon, MPH Cheryl H. Dunnington, RN, MS 1 FAST Initiative Overview 2004-2010
Quality Improvement Plans (QIP): Progress Report for the 2016/17 QIP
 Quality Improvement Plans (QIP): Progress Report for the QIP Medication Reconciliation ID Measure/Indicator from as stated on QIP 2017 1 Best possible medication history(bpmh) completion: The total number
Quality Improvement Plans (QIP): Progress Report for the QIP Medication Reconciliation ID Measure/Indicator from as stated on QIP 2017 1 Best possible medication history(bpmh) completion: The total number
Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections
 C10 This presenter has nothing to disclose Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections David Renfro, MS, RN NE BC Kelly Farnam, BSN, RN Gloria Martinez, MS, RN, NEA
C10 This presenter has nothing to disclose Strategies to Reduce Readmissions, Sepsis, and Health-Care Associated Infections David Renfro, MS, RN NE BC Kelly Farnam, BSN, RN Gloria Martinez, MS, RN, NEA
Tracheostomy Care Test Questions
 Care Test Questions Free PDF ebook Download: Care Test Questions Download or Read Online ebook tracheostomy care test questions in PDF Format From The Best User Guide Database Ask questions about caring
Care Test Questions Free PDF ebook Download: Care Test Questions Download or Read Online ebook tracheostomy care test questions in PDF Format From The Best User Guide Database Ask questions about caring
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
CAUTI Reduction A Clinton Memorial Presentation
 CAUTI Reduction 2016 A Clinton Memorial Presentation Clinton Memorial Statistics Rurally situated in a primarily agricultural community with a population of 42,000 The hospital is licensed for 165 beds
CAUTI Reduction 2016 A Clinton Memorial Presentation Clinton Memorial Statistics Rurally situated in a primarily agricultural community with a population of 42,000 The hospital is licensed for 165 beds
10/8/13. Passy Muir Inc. 1. Presenter THE HOME CARE TRACHEOSTOMY TEAM: NAVIGATING AND NETWORKING. Disclosure Statement
 Welcome to Passy-Muir s Event Webinar: The Home Care Tracheostomy Team: If you have not registered for this event, go to the Education Portal to complete your registration. ep.passy-muir.com This is an
Welcome to Passy-Muir s Event Webinar: The Home Care Tracheostomy Team: If you have not registered for this event, go to the Education Portal to complete your registration. ep.passy-muir.com This is an
Celebrating our Successes 2014
 Celebrating our Successes 214 Nurse Involvement in Decision Making Groups 5 CODE SEPSIS: Time from Antibiotic Order to Administration 45 4 Time in Minutes from order to administration 35 3 25 2 15 1 5
Celebrating our Successes 214 Nurse Involvement in Decision Making Groups 5 CODE SEPSIS: Time from Antibiotic Order to Administration 45 4 Time in Minutes from order to administration 35 3 25 2 15 1 5
2017/18 Quality Improvement Plan Improvement Targets and Initiatives
 2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
Corporate Services Employment Report: January Employment by Staff Group. Jan 2018 (Jan 2017 figure: 1,462) Overall 1,
 Corporate Services Employment Report: January Employment by Staff Group Jan (Jan 20 figure: 1,462) Jan % Overall 1,520 +58 +4.0% 8 Management (VIII+) 403 +52 4.8% Clerical & Supervisory (III to VII) 907
Corporate Services Employment Report: January Employment by Staff Group Jan (Jan 20 figure: 1,462) Jan % Overall 1,520 +58 +4.0% 8 Management (VIII+) 403 +52 4.8% Clerical & Supervisory (III to VII) 907
Decreasing the Unplanned Readmission Rate of Patients receiving Outpatient Antibiotic Therapy(OPAT)
 Decreasing the Unplanned Readmission Rate of Patients receiving Outpatient Antibiotic Therapy(OPAT) Dr. Jose Cadena Dr. Amruta Parekh University of Texas Health Science Center at San Antonio San Antonio,
Decreasing the Unplanned Readmission Rate of Patients receiving Outpatient Antibiotic Therapy(OPAT) Dr. Jose Cadena Dr. Amruta Parekh University of Texas Health Science Center at San Antonio San Antonio,
Using the BaldrigeCriteria to Achieve High Reliability
 Using the BaldrigeCriteria to Achieve High Reliability John Chessare MD, MPH President and CEO Carolyn Candiello Vice President for Quality and Patient Safety GBMC HealthCare System Organizational Profile:
Using the BaldrigeCriteria to Achieve High Reliability John Chessare MD, MPH President and CEO Carolyn Candiello Vice President for Quality and Patient Safety GBMC HealthCare System Organizational Profile:
Choosing a Tracheostomy for a Child with a Neuromuscular Disorder
 Choosing a Tracheostomy for a Child with a Neuromuscular Disorder This handout explains what a tracheostomy is and can help you decide if this is right for your child. What is a tracheostomy? Surgery is
Choosing a Tracheostomy for a Child with a Neuromuscular Disorder This handout explains what a tracheostomy is and can help you decide if this is right for your child. What is a tracheostomy? Surgery is
Improving Children s Health Together
 Improving Children s Health Together Improvement is our business. Committed professionals and organizations across the U.S. are working hard every day to make it easier for children and families to live
Improving Children s Health Together Improvement is our business. Committed professionals and organizations across the U.S. are working hard every day to make it easier for children and families to live
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2009 Sue Currin, RN, MS, Chief Nursing Officer
 PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2009 Sue Currin, RN, MS, Chief Nursing Officer 1. January 2009 2320 RN VACANCY RATE: Overall 2320 RN vacancy rate for
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, February 2009 Sue Currin, RN, MS, Chief Nursing Officer 1. January 2009 2320 RN VACANCY RATE: Overall 2320 RN vacancy rate for
Harm Across the Board Reporting: How your Hospital Can Get There
 Harm Across the Board Reporting: How your Hospital Can Get There Presentation to KHA Annual Quality Conference March 19, 2014 Jackie Conrad RN, BSN, MBA Improvement Advisor Cynosure Health Objectives Upon
Harm Across the Board Reporting: How your Hospital Can Get There Presentation to KHA Annual Quality Conference March 19, 2014 Jackie Conrad RN, BSN, MBA Improvement Advisor Cynosure Health Objectives Upon
Patients with Rib Fractures How We Decreased Unplanned Transfers to the ICU. Lillian Aguirre, DNP, CNS, CCRN, CCNS Orlando Regional Medical Center
 Patients with Rib Fractures How We Decreased Unplanned Transfers to the ICU Lillian Aguirre, DNP, CNS, CCRN, CCNS Orlando Regional Medical Center Disclosures I do not have any disclosures Background Struggling
Patients with Rib Fractures How We Decreased Unplanned Transfers to the ICU Lillian Aguirre, DNP, CNS, CCRN, CCNS Orlando Regional Medical Center Disclosures I do not have any disclosures Background Struggling
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, May 2010 Sharon McCole-Wicher, RN, MS, Chief Nursing Officer
 PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, May 2010 Sharon McCole-Wicher, RN, MS, Chief Nursing Officer 1. April 2010 2320 RN VACANCY RATE: Overall 2320 RN vacancy rate for
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, May 2010 Sharon McCole-Wicher, RN, MS, Chief Nursing Officer 1. April 2010 2320 RN VACANCY RATE: Overall 2320 RN vacancy rate for
Clinical Safety & Effectiveness Cohort # 18
 Clinical Safety & Effectiveness Cohort # 18 Surgery Delays DATE 1 The Team Division Dr. Howard Wang, Medical Director Jana Lee Normandin, Practice Manager Dr. Maureen Sheehan, Data Assist, Director of
Clinical Safety & Effectiveness Cohort # 18 Surgery Delays DATE 1 The Team Division Dr. Howard Wang, Medical Director Jana Lee Normandin, Practice Manager Dr. Maureen Sheehan, Data Assist, Director of
Translating Evidence to Safer Care
 Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Introduction David Roberson, MD, FACS
 Introduction David Roberson, MD, FACS Welcome Thank you for joining us GTD USA kickoff April 26, 2014 GTD USA kickoff April 26, 2014 This is a team effort Thanks to sponsors & donors Boston Children s
Introduction David Roberson, MD, FACS Welcome Thank you for joining us GTD USA kickoff April 26, 2014 GTD USA kickoff April 26, 2014 This is a team effort Thanks to sponsors & donors Boston Children s
Shaping Demand: Managing Elective OR Schedules and Predicting Downstream Demand
 This presenter has nothing to disclose. Shaping Demand: Managing Elective OR Schedules and Predicting Downstream Demand Flow Symposium Nov. 2016 Frederick C. Ryckman, MD Professor of Surgery / Transplantation
This presenter has nothing to disclose. Shaping Demand: Managing Elective OR Schedules and Predicting Downstream Demand Flow Symposium Nov. 2016 Frederick C. Ryckman, MD Professor of Surgery / Transplantation
Creating a Culture of Quality and Safety Gordon C. Hunt, MD, MBA Sr. Vice President & Chief Medical Officer, Sutter Health
 Creating a Culture of Quality and Safety Gordon C. Hunt, MD, MBA Sr. Vice President & Chief Medical Officer, Sutter Health M2 This presenter has nothing to disclose December 2012 Blue Ribbon I & II In
Creating a Culture of Quality and Safety Gordon C. Hunt, MD, MBA Sr. Vice President & Chief Medical Officer, Sutter Health M2 This presenter has nothing to disclose December 2012 Blue Ribbon I & II In
Chronic Critical Illness Decision Aid
 Chronic Critical Illness Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand options for your care. We want you to
Chronic Critical Illness Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand options for your care. We want you to
Residency Completion Record
 Residency Completion Record The following is a list of minimum requirements each resident must successfully complete in order to be considered for graduation from their residency program. If a resident
Residency Completion Record The following is a list of minimum requirements each resident must successfully complete in order to be considered for graduation from their residency program. If a resident
CHC-A Continuity Dashboard. All Sites Continuity - Asthma. 2nd Qtr-03. 2nd Qtr-04. 2nd Qtr-06. 4th Qtr-03. 4th Qtr-06. 3rd Qtr-04.
 PPC1: ACCESS AND COMMUNICATION Element B: Access and Communication Results Item 1: Visits with assigned PCP Continuity data is reviewed each month at our Office Redesign Committee (ORDC). The data is collected
PPC1: ACCESS AND COMMUNICATION Element B: Access and Communication Results Item 1: Visits with assigned PCP Continuity data is reviewed each month at our Office Redesign Committee (ORDC). The data is collected
National Trends Winter 2016
 National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
Colorado Medical-Dental Integration Project (CO MDI)
 Colorado Medical-Dental Integration Project (CO MDI) Allison Cusick, MPA, CHES National Oral Health Conference April 2016 Colorado Medical-Dental Integration CO MDI Five-Year Initiative Launched in 2014
Colorado Medical-Dental Integration Project (CO MDI) Allison Cusick, MPA, CHES National Oral Health Conference April 2016 Colorado Medical-Dental Integration CO MDI Five-Year Initiative Launched in 2014
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach
 Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence
 PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence Rachel Brunt, RN, BSN, MBA-HCA, CIC, CPHQ, Director Quality Jessie Hanks, BS, RHIA, Director HIM Lafayette General
PSI-15 Lafayette General Health 2017 Nicholas E. Davies Enterprise Award of Excellence Rachel Brunt, RN, BSN, MBA-HCA, CIC, CPHQ, Director Quality Jessie Hanks, BS, RHIA, Director HIM Lafayette General
Background & Significance
 Translating Data from the National Database for Nursing Quality Indicators for Bedside Clinicians and Administrators Michele M. Pelter, RN, PhD & Kimberly E. Stephens, RN, BSN, MPH Renown Regional Medical
Translating Data from the National Database for Nursing Quality Indicators for Bedside Clinicians and Administrators Michele M. Pelter, RN, PhD & Kimberly E. Stephens, RN, BSN, MPH Renown Regional Medical
Paediatric Critical Care and Specialised Surgery in Children Review. Paediatric critical care and ECMO: interim update
 Gateway Reference: 06662 Paediatric Critical Care and Specialised Surgery in Children Review Paediatric critical care and ECMO: interim update June 2017 Contents Executive summary 1. Introduction 2. Context
Gateway Reference: 06662 Paediatric Critical Care and Specialised Surgery in Children Review Paediatric critical care and ECMO: interim update June 2017 Contents Executive summary 1. Introduction 2. Context
Pharmaceutical Services Report to Joint Conference Committee September 2010
 Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
The Impact of a Daily Goals Tool in the ICU: More than a Checklist
 S Y S T E M The Impact of a Daily Goals Tool in the ICU: More than a Checklist May 24, 2016 Our Vision To be the Nation's leading public academic health care system. Leading. Teaching. Caring. Acknowledgements
S Y S T E M The Impact of a Daily Goals Tool in the ICU: More than a Checklist May 24, 2016 Our Vision To be the Nation's leading public academic health care system. Leading. Teaching. Caring. Acknowledgements
STAR. Safety Program and Importance of RT Education. Pediatric Home Service (PHS) Who is this man? Rebecca Long, BA, RRT-NPS, LRT.
 STAR Safety Program and Importance of RT Education Rebecca Long, BA, RRT-NPS, LRT April 30, 2012 Pediatric Home Service (PHS) An independent pediatric home health care agency in MN with 22 years experience
STAR Safety Program and Importance of RT Education Rebecca Long, BA, RRT-NPS, LRT April 30, 2012 Pediatric Home Service (PHS) An independent pediatric home health care agency in MN with 22 years experience
