Deprescribing in a family health team: a study of chronic proton pump inhibitor use
|
|
|
- Eleanore Nash
- 6 years ago
- Views:
Transcription
1 Deprescribing in a family health team: a study of chronic proton pump inhibitor use Kate Walsh BSc.H, BScPhm; 1 Debbie Kwan BScPhm, MSc; 2 Patricia Marr BScPhm, PharmD; 2 Christine Papoushek PharmD; 2 W. Kirk Lyon MD 3 1 Pharmacist, Toronto Central Community Care Access Centre 2 Pharmacist, Toronto Western Family Health Team 3 Family Physician, Toronto Western Family Health Team ABSTRACT Background: Proton pump inhibitors (PPIs) are often used inappropriately, without an indication, or for longer durations than recommended. Few tools exist to guide reassessment of their continued use and deprescribing if required. We aimed to reduce inappropriate drug use by developing and implementing a PPI deprescribing tool and process in a family medicine unit. Assessment of Problem: Primary care providers of adults taking a PPI for 8 weeks with an upcoming periodic health examination were reminded to reassess therapy via electronic medical record (EMR) messaging. A PPI Deprescribing Tool was uploaded into the EMR as a second reminder and to guide reassessment and deprescribing where indicated. Ten weeks after the examination a chart review assessed changes to PPI use. A follow up survey of providers assessed the utility and barriers to implementing the Deprescribing Tool. Results: Forty-three of 46 patients on PPIs (93%) had their PPI reassessed, resulting in 11 patients (26%) having their PPI deprescribed. Strategies for Improvement: Routine reassessment of long-term medications is often overlooked because of extensive demands on primary care providers time. Deprescribing likely improved because potentially eligible patients were identified to the provider and a tool was provided at the time of the encounter to guide the deprescribing process. Lessons: Reassessment and deprescribing of PPIs can be supported by implementing a standardised process and use of guidance tools for clinicians. Providers found the timely and selective reminder message to deprescribe the most useful component of the intervention. Keywords: proton pump inhibitor; deprescribing; reassessment; primary care; medication therapy management; gastroesophageal reflux disease J PRIM HEALTH CARE 2016;8(2): /HC15946 Correspondence to: Kate Walsh 250 Dundas St West, Toronto, ON M5T 2Z6, Canada katewalsh478@gmail.com Background In 2012, proton pump inhibitors (PPIs) accounted for nine of the top 100 prescribed drugs in Canada. 1 This medication class was initially thought to have an excellent safety profile. More recent evidence suggests that longterm PPI use may be linked to increased risk of incident and recurrent Clostridium difficile infection, community and hospital acquired pneumonia, bone fractures, and nutrient malabsorption. 2 6 The risk appears to be smaller with H 2 receptor antagonists or lower PPI doses, suggesting that the degree of acid suppression plays a role in the risk of adverse effects. 2 4 Gastroesophageal reflux disease (GERD) is a common indication for PPI use. Canadian Consensus Guidelines recommend that PPIs be discontinued after 4 8 weeks of initial treatment. 7 If symptoms recur, reintroduction of PPIs at the lowest dose and frequency to control symptoms is recommended Journal Compilation Royal New Zealand College of General Practitioners 2016 This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License
2 Despite definitive recommendations for appropriate PPI use, evidence consistently shows they are not being used appropriately. A retrospective chart review performed in Australia found that only 37.1% of inpatients prescribed a PPI were taking it for an appropriate indication. 8 Only 58.5% of these patients had tried an H 2 -receptor antagonist for mild/moderate oesophagitis, which is a recommended practice. 8 As well, research recently conducted in our family medicine unit determined that many of our elderly patients who frequently visit the emergency department were taking a PPI inappropriately, according to the STOPP criteria (Screening Tool of Older Persons Potentially Inappropriate Prescriptions). 9,10 Deprescribing is the complex process of tapering or stopping medications to manage polypharmacy and improve patient outcomes. 11 Interventions to reduce unnecessary PPI use have proven successful in previous studies but these interventions are often resource heavy and may be difficult to implement in some practices A review of interventions to support appropriate PPI prescribing suggested that combining educational, multifaceted interventions that involve both health care providers and patients may be useful. 15 Electronic medical records (EMR) make it relatively easy to identify patients taking potentially inappropriate medications. However, primary care providers (PCPs) often lack the time and knowledge to intervene. The aim of this project was to develop, implement and evaluate a tool and process to guide reassessment and deprescribing of PPIs where appropriate. Additional objectives included improving documentation of indications for PPI use in the EMR and assessing the utility and barriers to implementing the deprescribing process. Assessment of Problem This prospective, descriptive quality improvement project was approved by University Health Network s research ethics board. It was conducted at the Toronto Western Family Health Team; a large, interdisciplinary, academic primary care clinic serving ~ patients in downtown west Toronto. Family medicine residents, nurse practitioners, and staff physicians see patients by appointment. Residents review their cases with a supervising staff physician before implementing a care plan with patients. Two documents were created for the project. A PPI Deprescribing Tool was developed from a review of current guidelines (Figure 1). 8,16 22 The information was consolidated into a single document and the content was reviewed by a local gastroenterologist. Standard daily doses of PPIs for GERD and endoscopic negative reflux disease were defined as: omeprazole 20 mg, lansoprazole 20 mg, pantoprazole 40 mg, rabeprazole 20 mg and esomeprazole 20 mg. 17,23 A usability pilot was conducted with several PCPs to ensure the tool would be easy to use. A handout was created to help patients understand the harms associated with long-term PPI use. It also guided patients through the taper process, including management of potential rebound symptoms. The handout was reviewed by a plain language editor in the Patient Education Department at the hospital. A trial of weekly screening of the PCP s schedules took ~30 min which demonstrated the feasibility of implementing this intervention in a resource limited environment. Eligible patients were aged 18 years or older who had an upcoming periodic health examination and were taking a PPI (for any indication) for 8 weeks. A standard EMR reminder message was sent to the PCP of these patients advising that the upcoming appointment would be an ideal opportunity to reassess therapy (Figure 2). The PPI Deprescribing Tool was uploaded into patients EMRs to serve as a second reminder at the time of the appointment and to assist with the reassessment and deprescribing process. The Tool encouraged detailed documentation of the indication for chronic PPI therapy when deemed appropriate. The patient handout was saved in the EMR for printing and distribution at the visit if required. The intervention used PCPs to perform the reassessment because their existing relationship and knowledge of their patients helped to facilitate the efficiency and success of performing this task. The periodic health examination was deliberately chosen as the opportune time to perform the intervention. These appointments are longer than usual clinic visits and the concerns regarding PPI VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE 165
3 Figure 1. PPI Deprescribing tool (Continued) 166 VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE
4 Figure 1. (continued) VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE 167
5 Figure 2. Standard EMR reminder message associated harms align with the visit s objective of preventing health-related problems. 24 Baseline data collected included patient age, PPI agent, dose, duration and indication. A chart review occurred 10 weeks after the periodic health examination to determine if the PPI had been reassessed and if changes to therapy or documentation of the indication had occurred. Reassessment of the PPI was defined as any documentation in the EMR chart notes demonstrating that the indication and intended duration of therapy were reviewed. At the conclusion of the project, an electronic survey was distributed to participating PCPs to determine the utility of the tools and process, as well as any perceived barriers to implementing the intervention. Results of Assessment/ Measurement Nurse practitioners, family medicine residents, and staff physicians had 639 periodic health examinations booked over the 10-week study period: 46 patients met the inclusion criteria. The average patient age was 59 years (range 28 89). Baseline data collection The most common PPIs prescribed were omeprazole (n = 13 (28%)), pantoprazole (n = 9 (20%)), and rabeprazole (n = 9 (20%)). Of the 46 participants, 34 (74%) were on a standard dose PPI, six were on a high dose, two were on a half dose and four were on a different regimen, including prn use. Forty two (91%) had been on the drug for more than a year. Only 34 of the 46 patients (74%) had a documented indication which included: GERD (n = 24), dyspepsia (n = 4), history of gastrointestinal ulcer (n = 4), and other indications such as esophageal carcinoma (n = 2). Follow up data collection Re-assessment and changes to PPI use Of the 46 patients, 43 (93%) had their PPI reassessed (Figure 3), resulting in one of the following outcomes: 1. No change to PPI use: Of the 43 patients, 16 (37%) had no change to their PPI use. 2. The patient was no longer taking the PPI: Of the 43 patients, 16 (37%) were identified as no longer taking the PPI despite it being documented in their medication list. Thirteen of these patients were off all therapy and three were taking an alternate therapy. 3. The PPI was deprescribed: Of the 43 patients, 11 (26%) had their PPI deprescribed, resulting in six patients taking no therapy and 4 patients taking an alternate therapy. One patient attempted a PPI taper but resumed the original dose due to worsening gastrointestinal symptoms. Documentation Documentation of indications for PPI use improved during the project. The number of patients taking a PPI without an indication for it documented in their problem list decreased from 12 at baseline to 4 at the end of the project. 168 VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE
6 During reassessment, an indication for chronic therapy was identified in seven patients but only three of them had this indication documented in their problem list. Prescriber Feedback Survey The survey response rate was 67%. Among the different intervention components, respondents stated the EMR reminder message was the most useful, followed by the PPI Deprescribing Tool. The patient handout was ranked least useful. This was perhaps because only one patient received the handout, according to the EMR chart notes. Common themes on how the intervention components facilitated practice were identified by two co-authors independently. The themes were: (1) the tools served as a reminder to review the indication and duration for use, (2) the Deprescribing Tool helped guide the reassessment and taper process, and (3) the tools guided discussion with patients and implementation of recommendations. The first two themes are validated by the fact that 93% of patients had their PPI reassessed. Patients unwillingness to stop their PPI and lack of time were the most frequently cited barriers to deprescribing. Survey respondents identified several ideas for future deprescribing initiatives including nonsteroidal anti-inflammatories, opioids, acetylsalicylic acid for primary prevention, statins for primary prevention and antidepressants. Strategies for Quality Improvement and Change Most study patients were taking a PPI at the standard dose for GERD for more than one year. This suggests that reassessment and an attempt to reduce to the lowest effective dose was not occurring on a consistent basis. Routine reassessment of chronic medications is often overlooked during appointments because of extensive demands on PCPs time. It was proposed that deprescribing rates could improve if eligible patients were pre-identified, and a tool was provided at the time of the encounter to guide the deprescribing process. Another deprescribing trial that specifically targeted patients on chronic PPI therapy for Figure 3. Results flow diagram symptom controlled GERD eliminated medication use in 15% of patients. 25 In our study, six of the 11 patients (55%) who had their PPI deprescribed were able to discontinue all acid-suppressive therapy. These results suggest that many patients who take a PPI chronically for GERD can successfully eliminate medication use. At the end of the follow up period, four patients remained on a PPI without a documented indication. Incomplete documentation can lead to important downstream events including unintentional continuation of therapy. For example, one study patient had their PPI reassessed and it was found that they did not have any indication to be on the drug. The PPI was stopped but the medication list was not updated. Later, when the patient was hospitalised, the PPI was resumed because the inaccurate medication list was used. This resulted in continuation of a PPI without an indication. Incomplete documentation was also seen in patients who did not change their PPI use. When reassessment identified an indication for longterm therapy it was rarely updated in patients VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE 169
7 problem lists. Problem lists are cumulative lists of the patients medical conditions that are readily located in the EMR. If they are not updated, this may lead to unnecessary work for other clinicians who would need to sort through chart notes to determine the PPI indication (as opposed to just looking in the problem list). An unexpected finding from this study revealed that 37% of patients had a PPI in their EMR medication list but reassessment showed they were no longer using it. Perhaps this in part due to the inclusion of relatively healthy patients who see their primary care provider only on an annual basis (and therefore their medication lists are not updated frequently). Even so, this is concerning from a broader research perspective in that EMRs are increasingly being used for data extraction and this study indicates that these records may be far from accurate. Project results were presented to all staff during grand rounds as well as to a larger audience of pharmacists at a national conference. Individuals outside our institution repeatedly asked for access to the Deprescribing Tool. This validates that such a tool was not previously available and that clinicians felt it would be a useful addition to their practice. As well, the investigators of a national deprescribing guideline project approached the study team about using the Deprescribing Tool as part of the guideline resources. LESSONS AND MESSAGES As a result of our intervention, 93% of patients had their PPI reassessed and 26% had their PPI deprescribed. The positive uptake and usefulness of the intervention was also demonstrated through a ripple effect whereby PCPs frequently informed the study team that they were using the tool and process for non-study patients. Deprescribing has the potential to reduce pill burden, reduce medication costs and decrease the risks of medication related adverse effects. In addition, patients likely benefited from an increased knowledge about their medical condition, the harms associated with long-term PPI use, and non-pharmacological methods to manage gastrointestinal symptoms. Other organisations could consider using technology to identify eligible patients as well as to support tools that assist prescribers through a clinical decision pathway. To correctly assess the impact of such an intervention, it is critical that EMR records be kept up to date with respect to current medications and medical conditions (problem list). As a result of the inaccurate EMR used in this study, unnecessary work was completed to identify and reassess therapy in patients who were not taking a PPI. A reduction in future workload may serve as a motivational factor for all clinicians to keep records up to date. The notable uptake for the project (as evidenced through the reassessment rate) was the result of an inter-professional project team that engaged the various disciplines impacted by the project ( physician, pharmacist, gastroenterologist). The project also had the support of the clinic s administration (Chief of Staff). Having an evidence-based Deprescribing Tool that was reviewed by a gastroenterologist likely increased the PCPs confidence in applying the recommendations to their patient encounters. In the months following the project s cessation, it was observed that PPI reassessment was not being routinely conducted despite having the Deprescribing Tool and patient handout accessible in the EMR. This is likely because prescribers were no longer being reminded to reassess therapy in specific patients before an encounter. PCPs also identified the importance of this reminder in the prescriber feedback survey. In response to this, a follow up project will determine if discussing the expected duration of treatment when PPIs are first prescribed would be a more sustainable way to ensure patients do not remain on medications they do not need. This proactive intervention may also be more efficient as some patients will not continue unnecessary therapy, therefore eliminating the need for a dedicated reassessment appointment. References 1. Top Rx Drugs of Pharm Pract (Granada). 2013;37 39: Kwok CS, Arthur AK, Anibueze CI. et al. Risk of Clostridium difficile infection with acid supressing drugs and antibiotics: meta-analysis. Am J Gastroenterol. 2012;107(7): doi: /ajg VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE
8 3. Eom CS, Jeon CY, Lim JW. et al. Use of acid suppressive drugs and risk of pneumonia: a systematic review and meta-analysis. CMAJ. 2011:183(3): doi: / cmaj Yu EW, Bauer SR, Bain PA, Bauer DC. Proton pump inhibitors and risk of fractures: a meta-analysis of 11 international studies. Am J Med. 2011:124(6): doi: /j.amjmed Hess MW, Hoenderop JG, Bindels RJ, Drenth JP. Systematic review: hypomagnesaemia induced by proton pump inhibition. Aliment Pharmacol Ther. 2012:36(5): doi: /j x 6. Sharma VR, Brannon MA, Carloss EA. Effect of omeprazole on oral iron replacement in patients with iron deficiency anemia. South Med J. 2004:97(9): doi: /01. SMJ Armstrong D, Marshall JK, Chiba N. et al. Canadian Consensus Conference on the management of gastroesophageal reflux disease in adults - Update Can J Gastroenterol. 2005:19(1): doi: /2005/ Naunton M, Peterson GM, Bleasel MD. Overuse of proton pump inhibitors. J Clin Pharm Ther. 2000:25(5): doi: /j x 9. Wong J, Marr P, Kwan D. et al. Identification of inappropriate medication use in elderly patients with frequent emergency department visits. Can Pharm J. 2014:147(4): doi: / Gallagher P, O Mahony D. STOPP (Screening Tool of Older Persons potentially inappropriate Prescriptions): application to acutely ill elderly patients and comparison with Beers criteria. Age Ageing. 2008:37(6): doi: /ageing/afn Thompson W, Farrell B. Deprescribing: what is it and what does the evidence tell us? Can J Hosp Pharm 2013; 66(3): [cited 2013 Dec 15] Available from: &tool=pmcentrez&rendertype=abstract 12. Bundeff AW, Zaiken K. Impact of clinical pharmacists recommendations on a proton pump inhibitor taper protocol in ambulatory care practice. J Manag Care Pharm. 2013:19(4): doi: /jmcp Lucas LM, Gerrity MS, Anderson T. A practice-based approach for converting from proton pump inhibitors to less costly therapy. Eff Clin Pract. 2001:4(6): Murie J, Allen J, Simmonds R, de Wet C. Glad you brought it up: a patient-centred programme to reduce proton-pump inhibitor prescribing in general practice. Qual Prim Care. 2012:20(2): Canadian Agency for Drugs and Technologies in Health. Interventions for appropriate prescribing of proton pump inhibitors: a literature review. COMPUS. 2007:1(4). 16. Bhatt DL, Scheiman J, Abraham NS. et al. ACCF/ACG/AHA 2008 Expert Consensus Document on Reducing the Gastrointestinal Risk of Antiplatelet Therapy and NSAID Use: A report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents. J Am Coll Cardiol. 2008:52(18): doi: /j. jacc Canadian Agency for Drugs and Technologies in Health. Optimal Therapy Report: Proton Pump Inhibitor Project Overview Summaries. 2007:1(1). 18. Kahrilas PJ, Shaheen NJ, Vaezi MF. American Gastroenterological Association Institute Technical Review on the management of gastroesophageal reflux disease. Gastroenterology. 2008:135(4): doi: /j. gastro Laine L, Jensen DM. Management of patients with ulcer bleeding. Am J Gastroenterol. 2012:107(3): doi: /ajg Lanza FL, Chan FKL, Quigley EMM. Practice Parameters Commitee of the American College of Gastroenterology. Guidelines for prevention of NSAID-related ulcer complications. Am J Gastroenterol. 2009:104(3): doi: / ajg Talley NJ, Vakil N. Practice Parameters Commitee of the American College of Gastroenterology. Guidelines for the management of dyspepsia. Am J Gastroenterol. 2005:100(10): doi: /j x 22. Veldhuyzen van Zanten SJO, Bradette M, Chiba N. et al. Evidence-based recommendations for short- and longterm management of uninvestigated dyspepsia in primary care: An update of the Canadian Dyspepsia Working Group (CanDys) clinical management tool. Can J Gastroenterol. 2005:19(5): doi: /2005/ AstraZeneca Canada Inc. Nexium Product Monograph August 29; Medical Council of Canada. Periodic Health Examination (PHE) Available at: Online/objectives.pl?lang=english&role=expert&id= Inadomi JM, Jamal R, Murata GH. et al. Step-down management of gastroesophageal reflux disease. Gastroenterology. 2001:121(5): doi: / gast Competing Interests No authors had any competing interests to declare. VOLUME 8 NUMBER 2 june 2016 J OURNAL OF PRIMARY HEALTH CARE 171
Long-Term Care Medication Management: A Demonstration Project. Training Support Deck July 2016
 Long-Term Care Medication Management: A Demonstration Project Training Support Deck July 2016 Overview Background Purpose and Guiding Principles of Demonstration Project Targeted Drug Classes Sample Scenario
Long-Term Care Medication Management: A Demonstration Project Training Support Deck July 2016 Overview Background Purpose and Guiding Principles of Demonstration Project Targeted Drug Classes Sample Scenario
Greetings from Michelle & Katie QUALITY IMPROVEMENT DIVISION OF HOSPITAL MEDICINE
 IN THIS ISSUE: Make Sure You Are Solving the Right Problem P. 1 Are Electronic Health Records Contributing to Fraud? P. 1 Stress Ulcer Prophylaxis P. 2 Antibiotic Stewardship P. 3 APeX tips for a safe
IN THIS ISSUE: Make Sure You Are Solving the Right Problem P. 1 Are Electronic Health Records Contributing to Fraud? P. 1 Stress Ulcer Prophylaxis P. 2 Antibiotic Stewardship P. 3 APeX tips for a safe
Bulletin Independent prescribing information for NHS Wales
 Bulletin Independent prescribing information for NHS Wales Medicines-related admissions February 2015 Although medicines play an important role in the management of chronic and acute illnesses, they can
Bulletin Independent prescribing information for NHS Wales Medicines-related admissions February 2015 Although medicines play an important role in the management of chronic and acute illnesses, they can
Deprescribing: Importing Innovations from Outside the US A27 and B27
 Deprescribing: Importing Innovations from Outside the US A27 and B27 Introductions Karen Smethers, BS, PharmD, BCOP, National Clinical Pharmacy Integration Leader, The Resource Group, Ascension L. Hayley
Deprescribing: Importing Innovations from Outside the US A27 and B27 Introductions Karen Smethers, BS, PharmD, BCOP, National Clinical Pharmacy Integration Leader, The Resource Group, Ascension L. Hayley
Literature review: pharmaceutical services for prisoners
 Author: Rosemary Allgeier, Principal Pharmacist in Public Health. Date: 08 October 2012 Version: 1a Publication and distribution: NHS Wales (intranet and internet) Public Health Wales (intranet and internet)
Author: Rosemary Allgeier, Principal Pharmacist in Public Health. Date: 08 October 2012 Version: 1a Publication and distribution: NHS Wales (intranet and internet) Public Health Wales (intranet and internet)
WHEN LESS IS BEST. What drugs are we talking about? What is deprescribing?
 WHEN LESS IS BEST Seniors (those age 65 and older) in Canada take more than their share of prescription drugs. As reported by the Canadian Institute for Health Information (CIHI), a great many seniors
WHEN LESS IS BEST Seniors (those age 65 and older) in Canada take more than their share of prescription drugs. As reported by the Canadian Institute for Health Information (CIHI), a great many seniors
POLICY. Use of Antipsychotic Medications in Nursing Facility Residents. Preamble. Background
 Preamble POLICY Use of Antipsychotic Medications in Nursing Facility Residents The Office of Inspector General of the U. S. Department of Health and Human Services issued a report in May 2011 finding that
Preamble POLICY Use of Antipsychotic Medications in Nursing Facility Residents The Office of Inspector General of the U. S. Department of Health and Human Services issued a report in May 2011 finding that
COMPUS Procedure Evidence-Based Best Practice Recommendations
 COMPUS Procedure Evidence-Based Best Practice Recommendations Introduction The Canadian Optimal Medication Prescribing and Utilization Service (COMPUS) identifies, evaluates, promotes, and facilitates
COMPUS Procedure Evidence-Based Best Practice Recommendations Introduction The Canadian Optimal Medication Prescribing and Utilization Service (COMPUS) identifies, evaluates, promotes, and facilitates
Making a case for medication reconciliation in primary care
 Safer Healthcare Now! MedRec National Teleconference Making a case for medication reconciliation in primary care Speakers: Karen Hall Barber, BSc (Hons), MD, CCFP Sherri Elms, BSc (Pharm), RPh ACPR Danyal
Safer Healthcare Now! MedRec National Teleconference Making a case for medication reconciliation in primary care Speakers: Karen Hall Barber, BSc (Hons), MD, CCFP Sherri Elms, BSc (Pharm), RPh ACPR Danyal
W e were aware that optimising medication management
 207 QUALITY IMPROVEMENT REPORT Improving medication management for patients: the effect of a pharmacist on post-admission ward rounds M Fertleman, N Barnett, T Patel... See end of article for authors affiliations...
207 QUALITY IMPROVEMENT REPORT Improving medication management for patients: the effect of a pharmacist on post-admission ward rounds M Fertleman, N Barnett, T Patel... See end of article for authors affiliations...
Who Cares About Medication Reconciliation? American Pharmacists Association American Society of Health-system Pharmacists The Joint Commission Agency
 The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
A. Goals and Objectives:
 III. Main A. Goals and Objectives: Primary goal(s): Improve screening for postmenopausal vaginal atrophy and enhance treatment of symptoms by engaging patients through the electronic medical record and
III. Main A. Goals and Objectives: Primary goal(s): Improve screening for postmenopausal vaginal atrophy and enhance treatment of symptoms by engaging patients through the electronic medical record and
The CMS State Operations Manual Overview and Changes
 The CMS State Operations Manual Overview and Changes Omnicare, Inc. Page 1 Overview of the CMS State Operations Manual Executive Summary Historical Perspective The Requirements Pharmacy Services Labeling
The CMS State Operations Manual Overview and Changes Omnicare, Inc. Page 1 Overview of the CMS State Operations Manual Executive Summary Historical Perspective The Requirements Pharmacy Services Labeling
Checklists for Preventing and Controlling
 Checklists for Preventing and Controlling Clostridium difficile Infection (CDI) This document has been developed to specifically assist senior management and all ward staff to take appropriate actions,
Checklists for Preventing and Controlling Clostridium difficile Infection (CDI) This document has been developed to specifically assist senior management and all ward staff to take appropriate actions,
Optimising care for patients with Inflammatory Bowel Disease:
 Optimising care for patients with Inflammatory Bowel Disease: - Rural patients burden of disease and perceived treatment barriers - Outcomes of transition care and - Evaluation of simple clinical tools
Optimising care for patients with Inflammatory Bowel Disease: - Rural patients burden of disease and perceived treatment barriers - Outcomes of transition care and - Evaluation of simple clinical tools
Original Research PRACTICE-BASED RESEARCH. University Wexner Medical Center
 Evaluation of provider documentation of medication management in a Patient-Centered Medical Home (PCMH) Trang T. Nguyen, PharmD 1 ; Bella H Mehta, PharmD, FAPhA 2 ; Jennifer L. Rodis, PharmD, BCPS 2 ;
Evaluation of provider documentation of medication management in a Patient-Centered Medical Home (PCMH) Trang T. Nguyen, PharmD 1 ; Bella H Mehta, PharmD, FAPhA 2 ; Jennifer L. Rodis, PharmD, BCPS 2 ;
Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
 Journal of Pharmacy and Pharmacology 2 (2014) 731-738 doi: 10.17265/2328-2150/2014.12.006 D DAVID PUBLISHING Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
Journal of Pharmacy and Pharmacology 2 (2014) 731-738 doi: 10.17265/2328-2150/2014.12.006 D DAVID PUBLISHING Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
Medication Therapy Management
 Medication Therapy Management Presented by Sylvia Saade, PharmD Ghada Khoury, Pharm D, BCACP Objectives Describe the components of medication therapy management (MTM) programs Discuss the needs of MTM
Medication Therapy Management Presented by Sylvia Saade, PharmD Ghada Khoury, Pharm D, BCACP Objectives Describe the components of medication therapy management (MTM) programs Discuss the needs of MTM
Transitions of Care: From Hospital to Home
 Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
National Jewish Health Best Practices for Medication Reconciliation in a Respiratory Academic Medical Center
 National Jewish Health Best Practices for Medication Reconciliation in a Respiratory Academic Medical Center Introduction/Background/History: Please include any relevant information that may be helpful
National Jewish Health Best Practices for Medication Reconciliation in a Respiratory Academic Medical Center Introduction/Background/History: Please include any relevant information that may be helpful
Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME
 Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME The Process What is medicine reconciliation? Medicine reconciliation is an evidence-based process, which has been
Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME The Process What is medicine reconciliation? Medicine reconciliation is an evidence-based process, which has been
I CSHP 2015 CAROLYN BORNSTEIN
 I CSHP 2015 CAROLYN BORNSTEIN CSHP 2015 is a quality initiative of the Canadian Society of Hospital Pharmacists that describes a preferred vision for pharmacy practice in the hospital setting by the year
I CSHP 2015 CAROLYN BORNSTEIN CSHP 2015 is a quality initiative of the Canadian Society of Hospital Pharmacists that describes a preferred vision for pharmacy practice in the hospital setting by the year
Expression of Interest for Wound Care Project
 Expression of Interest for Wound Care Project November 11, 2016 Telewound Care EOI Page 1 of 12 Contents 1 Introduction... 3 2 Telewound Care Project Background... 4 2.1 Background... 4 2.2 Purpose...
Expression of Interest for Wound Care Project November 11, 2016 Telewound Care EOI Page 1 of 12 Contents 1 Introduction... 3 2 Telewound Care Project Background... 4 2.1 Background... 4 2.2 Purpose...
Marketing. Pharmaceutical Industry: Marketing Positions 445
 Marketing Pharmaceutical Industry: Marketing Positions 445 Restricted Drug Distribution (1714) To oppose restricted drug distribution systems that (1) limit patient access to medications; (2) undermine
Marketing Pharmaceutical Industry: Marketing Positions 445 Restricted Drug Distribution (1714) To oppose restricted drug distribution systems that (1) limit patient access to medications; (2) undermine
Medication Reconciliation as a Patient Safety Practice During Transitions of Care
 Medication Reconciliation as a Patient Safety Practice During Transitions of Care Janice L. Kwan, MD, MPH, FRCPC Division of General Internal Medicine Mount Sinai Hospital, University of Toronto Recorded
Medication Reconciliation as a Patient Safety Practice During Transitions of Care Janice L. Kwan, MD, MPH, FRCPC Division of General Internal Medicine Mount Sinai Hospital, University of Toronto Recorded
Drilling Down to Defeat Clostridium difficile. Kathy Mathews, RN Infection Preventionist Sonoma Valley Hospital February 24, 2017
 Drilling Down to Defeat Clostridium difficile Kathy Mathews, RN Infection Preventionist Sonoma Valley Hospital February 24, 2017 Participation In This Webinar To connect to the audio portion of the webinar,
Drilling Down to Defeat Clostridium difficile Kathy Mathews, RN Infection Preventionist Sonoma Valley Hospital February 24, 2017 Participation In This Webinar To connect to the audio portion of the webinar,
Understanding Antimicrobial Stewardship: Is Your Organization Ready? A S H LEIGH MOUSER, PHARM D, BCPS
 Understanding Antimicrobial Stewardship: Is Your Organization Ready? A S H LEIGH MOUSER, PHARM D, BCPS Objectives Discuss the need for antimicrobial stewardship programs Explain the components of an effective
Understanding Antimicrobial Stewardship: Is Your Organization Ready? A S H LEIGH MOUSER, PHARM D, BCPS Objectives Discuss the need for antimicrobial stewardship programs Explain the components of an effective
Disclosures. Learning Objectives 4/26/2017. Impact of a Pilot Ambulatory Care Pharmacist in a Family Practice Clinic
 Impact of a Pilot Ambulatory Care Pharmacist in a Family Practice Clinic Taylor Sandvick, PharmD, PGY1 Pharmacy Resident St. Peter s Hospital, Helena, MT April 29, 2017 Disclosures 2 Financial: Nothing
Impact of a Pilot Ambulatory Care Pharmacist in a Family Practice Clinic Taylor Sandvick, PharmD, PGY1 Pharmacy Resident St. Peter s Hospital, Helena, MT April 29, 2017 Disclosures 2 Financial: Nothing
Patient Safety: 10 Years Later Why is Improvement So Hard? Patient Safety: Strong Beginnings
 Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
 HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
MEDICINE USE EVALUATION
 MEDICINE USE EVALUATION A GUIDE TO IMPLEMENTATION JOHN IRELAND VERSION 1 2013 Posi%ve Impact www.posi%veimpact4health.com Email: ji@icon.co.za Ph: 0823734585 Fax (086) 6483903, Melkbosstrand, South Africa
MEDICINE USE EVALUATION A GUIDE TO IMPLEMENTATION JOHN IRELAND VERSION 1 2013 Posi%ve Impact www.posi%veimpact4health.com Email: ji@icon.co.za Ph: 0823734585 Fax (086) 6483903, Melkbosstrand, South Africa
CMS Mega Rule: Implications for Pharmacists and Pharmacies
 CMS Mega Rule: Implications for Pharmacists and Pharmacies Curt Wood, RPh, BCGP, FASCP Disclosure and Conflict of Interest Curt Wood declares no conflicts of interest, real or apparent, and no financial
CMS Mega Rule: Implications for Pharmacists and Pharmacies Curt Wood, RPh, BCGP, FASCP Disclosure and Conflict of Interest Curt Wood declares no conflicts of interest, real or apparent, and no financial
Meet with preceptor monthly for 1 year. Preceptor to be approved by CPSO
 This individualized education plan sample is based on the CanMEDS Physician Competency Framework, an educational framework identifying and describing seven roles that lead to optimal health and health
This individualized education plan sample is based on the CanMEDS Physician Competency Framework, an educational framework identifying and describing seven roles that lead to optimal health and health
The Role of the Agency for Healthcare Research and Quality (AHRQ) in the US Drug Safety System
 The Role of the Agency for Healthcare Research and Quality (AHRQ) in the US Drug Safety System Scott R. Smith, MSPH, PhD Center for Outcomes & Evidence Agency for Healthcare Research & Quality July 20,
The Role of the Agency for Healthcare Research and Quality (AHRQ) in the US Drug Safety System Scott R. Smith, MSPH, PhD Center for Outcomes & Evidence Agency for Healthcare Research & Quality July 20,
Influence of Patient Flow on Quality Care
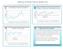 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Update on ACG Guidelines Stephen B. Hanauer, MD President American College of Gastroenterology
 Update on ACG Guidelines Stephen B. Hanauer, MD President American College of Gastroenterology Clifford Joseph Barborka Professor of Medicine Northwestern University Feinberg School of Medicine Guideline
Update on ACG Guidelines Stephen B. Hanauer, MD President American College of Gastroenterology Clifford Joseph Barborka Professor of Medicine Northwestern University Feinberg School of Medicine Guideline
Antibiotic Stewardship Program (ASP)
 Introduction: Antibiotics are among the most frequently prescribed medications in nursing centers, with up to 70% of nursing home patients receiving one or more courses of systemic antibiotics in a year.
Introduction: Antibiotics are among the most frequently prescribed medications in nursing centers, with up to 70% of nursing home patients receiving one or more courses of systemic antibiotics in a year.
PPI Deprescribing: Ascension
 PPI Deprescribing: Ascension Tonya Thomas, PharmD Clinical Pharmacist Saint Thomas West Hospital Nashville, TN, USA #derx2018 Session resources will be available at deprescribing.org/resources Learning
PPI Deprescribing: Ascension Tonya Thomas, PharmD Clinical Pharmacist Saint Thomas West Hospital Nashville, TN, USA #derx2018 Session resources will be available at deprescribing.org/resources Learning
Who s s on What? Latest Experience with the Framework Challenges and Successes. November 29, Margaret Colquhoun Project Leader ISMP Canada
 Who s s on What? Latest Experience with the Framework Challenges and Successes November 29, 2005 Margaret Colquhoun Project Leader ISMP Canada 1 Outline ISMP Canada Partnership with SHN The Canadian Getting
Who s s on What? Latest Experience with the Framework Challenges and Successes November 29, 2005 Margaret Colquhoun Project Leader ISMP Canada 1 Outline ISMP Canada Partnership with SHN The Canadian Getting
Medication Management: Is It in Your Toolbox?
 Medication Management: Is It in Your Toolbox? Brian K. Esterly, MBA, SVP, Corporate Development, excellerx, Inc. O: 215.282.1676, besterly@excellerx.com What has been your Medication Management experience?
Medication Management: Is It in Your Toolbox? Brian K. Esterly, MBA, SVP, Corporate Development, excellerx, Inc. O: 215.282.1676, besterly@excellerx.com What has been your Medication Management experience?
Telephone consultations to manage requests for same-day appointments: a randomised controlled trial in two practices
 Telephone consultations to manage requests for same-day appointments: a randomised controlled trial in two practices Brian McKinstry, Jeremy Walker, Clare Campbell, David Heaney and Sally Wyke SUMMARY
Telephone consultations to manage requests for same-day appointments: a randomised controlled trial in two practices Brian McKinstry, Jeremy Walker, Clare Campbell, David Heaney and Sally Wyke SUMMARY
Tackling the challenge of non-adherence
 Tackling the challenge of non-adherence 2 How is adherence defined? WHO definition: the extent to which a person s behaviour taking medication, following a diet and/or executing lifestyle changes corresponds
Tackling the challenge of non-adherence 2 How is adherence defined? WHO definition: the extent to which a person s behaviour taking medication, following a diet and/or executing lifestyle changes corresponds
H2H Mind Your Meds "Challenge. Webinar #3- Lessons Learned Wednesday, April 18, :00 pm 3:00 pm ET. Welcome
 H2H Mind Your Meds "Challenge Webinar #3- Lessons Learned Wednesday, April 18, 2012 2:00 pm 3:00 pm ET 1 Welcome Take Home Messages Understand how to implement the Mind Your Meds strategies and tools in
H2H Mind Your Meds "Challenge Webinar #3- Lessons Learned Wednesday, April 18, 2012 2:00 pm 3:00 pm ET 1 Welcome Take Home Messages Understand how to implement the Mind Your Meds strategies and tools in
Monitoring Medication Storage & Administration
 Monitoring Medication Storage & Administration Objectives Review F-Tags pertaining to medication management Discuss proper medication storage and administration Understand medication cart and medication
Monitoring Medication Storage & Administration Objectives Review F-Tags pertaining to medication management Discuss proper medication storage and administration Understand medication cart and medication
Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists. Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM)
 Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM) 1 Learning Objectives Upon successful completion of this
Fundamentals of Self-Limiting Conditions Prescribing for Manitoba Pharmacists Ronald F. Guse Registrar College of Pharmacists of Manitoba (CPhM) 1 Learning Objectives Upon successful completion of this
A Pharmacist Network for Integrated Medication Management in the Medical Home
 A Pharmacist Network for Integrated Medication Management in the Medical Home Marie Smith, PharmD UConn School of Pharmacy Professor/Dept. Head Pharmacy Practice Asst. Dean, Practice and Public Policy
A Pharmacist Network for Integrated Medication Management in the Medical Home Marie Smith, PharmD UConn School of Pharmacy Professor/Dept. Head Pharmacy Practice Asst. Dean, Practice and Public Policy
Implementation of STOPP/START criteria in different settings
 Implementation of criteria in different settings Professor Cristín Ryan School of Pharmacy and Pharmaceutical Sciences, Trinity College Dublin. October 2017 PhD Thesis (2006-2009), University College Cork
Implementation of criteria in different settings Professor Cristín Ryan School of Pharmacy and Pharmaceutical Sciences, Trinity College Dublin. October 2017 PhD Thesis (2006-2009), University College Cork
Translating Evidence to Safer Care
 Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Medication Management, Regulations and Resident Centered Care: What Could Possibly Go Wrong?
 PACAH Spring Conference April 29,2016 Medication Management, Regulations and Resident Centered Care: What Could Possibly Go Wrong? Jennifer L. Hardesty, PharmD, FASCP Chief Clinical Officer Corporate Compliance
PACAH Spring Conference April 29,2016 Medication Management, Regulations and Resident Centered Care: What Could Possibly Go Wrong? Jennifer L. Hardesty, PharmD, FASCP Chief Clinical Officer Corporate Compliance
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center
 Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Reducing Hospital Readmissions
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Reducing Hospital Readmissions
Organized, Evidence-based Care
 Organized, Evidence-based Care Planning Care for Individual Patients and Whole Populations MODERATOR: Nicole Van Borkulo, MEd, Practice Improvement Specialist, SNMHI, Qualis Health SPEAKERS: Ed Wagner,
Organized, Evidence-based Care Planning Care for Individual Patients and Whole Populations MODERATOR: Nicole Van Borkulo, MEd, Practice Improvement Specialist, SNMHI, Qualis Health SPEAKERS: Ed Wagner,
National clinical audit of inpatient care for adults with ulcerative colitis
 National clinical audit of inpatient care for adults with ulcerative colitis UK inflammatory bowel disease (IBD) audit Executive summary report June 2014 Prepared by the Clinical Effectiveness and Evaluation
National clinical audit of inpatient care for adults with ulcerative colitis UK inflammatory bowel disease (IBD) audit Executive summary report June 2014 Prepared by the Clinical Effectiveness and Evaluation
QI and DUE in Pharmacy Practice
 Pharmacy 483: QI and DUE in Pharmacy Practice Steve Riddle, BS Pharm, BCPS QI and Medication Utilization Lead HMC Pharmacy February 24, 2004 Acute Myocardial Infarction HA, 52yo male admitted via ER with
Pharmacy 483: QI and DUE in Pharmacy Practice Steve Riddle, BS Pharm, BCPS QI and Medication Utilization Lead HMC Pharmacy February 24, 2004 Acute Myocardial Infarction HA, 52yo male admitted via ER with
DEPARTMENT OF HEALTH AND HUMAN SERVICES CENTERS FOR MEDICARE & MEDICAID SERVICES
 Use for a resident who has potentially unnecessary medications, is prescribed psychotropic medications or has the potential for an adverse outcome to determine whether facility practices are in place to
Use for a resident who has potentially unnecessary medications, is prescribed psychotropic medications or has the potential for an adverse outcome to determine whether facility practices are in place to
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY: BOARD OF DIRECTORS 22 FEBRUARY 2012
 SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY: BOARD OF DIRECTORS C 22 FEBRUARY 2012 Subject: Supporting : Author: Status (see footnote): Update on the Clostridium difficile (C.diff)
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY: BOARD OF DIRECTORS C 22 FEBRUARY 2012 Subject: Supporting : Author: Status (see footnote): Update on the Clostridium difficile (C.diff)
TRANSITIONS of CARE. Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine
 TRANSITIONS of CARE Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine 5-15-15 Objectives At the conclusion of the presentation, the participant will be able to: 1. Improve
TRANSITIONS of CARE Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine 5-15-15 Objectives At the conclusion of the presentation, the participant will be able to: 1. Improve
CMS RULES FOR PARTICIPATION/LTC REGULATIONS: WHAT YOU NEED TO KNOW
 CMS RULES FOR PARTICIPATION/LTC REGULATIONS: WHAT YOU NEED TO KNOW SATURDAY/3:15-4:15PM ACPE UAN: 0107-9999-17-242-L04-P 0.1 CEU/1.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists:
CMS RULES FOR PARTICIPATION/LTC REGULATIONS: WHAT YOU NEED TO KNOW SATURDAY/3:15-4:15PM ACPE UAN: 0107-9999-17-242-L04-P 0.1 CEU/1.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists:
Commissioning for Quality & Innovation (CQUIN)
 Commissioning for Quality & Innovation () The following suite of s are goals relating to improvements in the quality of patient care which the Trust has agreed with commissioners (with the exception of
Commissioning for Quality & Innovation () The following suite of s are goals relating to improvements in the quality of patient care which the Trust has agreed with commissioners (with the exception of
CASE-BY-CASE REVIEW PROGRAM (CBCRP) CASE-BY-CASE REVIEW POLICY FOR CANCER DRUGS
 CASE-BY-CASE REVIEW PROGRAM (CBCRP) CASE-BY-CASE REVIEW POLICY FOR CANCER DRUGS Version: 3.0 Effective Date: October 2013 Replaces Policy: Case-by-Case Review Policy for Cancer Drugs, November 8, 2011
CASE-BY-CASE REVIEW PROGRAM (CBCRP) CASE-BY-CASE REVIEW POLICY FOR CANCER DRUGS Version: 3.0 Effective Date: October 2013 Replaces Policy: Case-by-Case Review Policy for Cancer Drugs, November 8, 2011
Journal of Pharmacy Practice and Community Medicine.2017, 3(4s):S95-S100
 Journal of Pharmacy Practice and Community Medicine.2017, 3(4s):S95-S100 http://dx.doi.org/10.5530/jppcm.2017.4s.55 RESEARCH ARTICLE OPEN ACCESS Pharmacy Technician Workload and Workforce Requirements
Journal of Pharmacy Practice and Community Medicine.2017, 3(4s):S95-S100 http://dx.doi.org/10.5530/jppcm.2017.4s.55 RESEARCH ARTICLE OPEN ACCESS Pharmacy Technician Workload and Workforce Requirements
Pfizer Independent Grants for Learning & Change Request for Proposals (RFP) Antimicrobial Stewardship in the Asia-Pacific Region
 Pfizer Independent Grants for Learning & Change Request for Proposals (RFP) Antimicrobial Stewardship in the Asia-Pacific Region I. Background The Joint Commission, in collaboration with Pfizer Independent
Pfizer Independent Grants for Learning & Change Request for Proposals (RFP) Antimicrobial Stewardship in the Asia-Pacific Region I. Background The Joint Commission, in collaboration with Pfizer Independent
Florida MEDS-AD Waiver
 Florida MEDS-AD Waiver 4 th Quarter Report October 1, 2015 December 31, 2015 Demonstration Year 10 1115 Research and Demonstration Waiver #11-W-00205/4 This page intentionally left blank Table of Contents
Florida MEDS-AD Waiver 4 th Quarter Report October 1, 2015 December 31, 2015 Demonstration Year 10 1115 Research and Demonstration Waiver #11-W-00205/4 This page intentionally left blank Table of Contents
RESEARCH ARTICLES Medication Error Identification Rates by Pharmacy, Medical, and Nursing Students
 RESEARCH ARTICLES Medication Error Identification Rates by Pharmacy, Medical, and Nursing Students Terri L. Warholak, PhD, Caryn Queiruga, PharmD,* Rebecca Roush, PharmD,* and Hanna Phan, PharmD The University
RESEARCH ARTICLES Medication Error Identification Rates by Pharmacy, Medical, and Nursing Students Terri L. Warholak, PhD, Caryn Queiruga, PharmD,* Rebecca Roush, PharmD,* and Hanna Phan, PharmD The University
The Pennsylvania PACE Program and the Academic Detailing Experience
 Models for Establishing Academic Detailing Programs to Increase Evidence-Based Prescribing The Pennsylvania PACE Program and the Academic Detailing Experience THE NATIONAL COMPARATIVE EFFECTIVENESS SUMMIT
Models for Establishing Academic Detailing Programs to Increase Evidence-Based Prescribing The Pennsylvania PACE Program and the Academic Detailing Experience THE NATIONAL COMPARATIVE EFFECTIVENESS SUMMIT
CLOSTRIDIUM DIFFICILE ACTION PLAN
 CLOSTRIDIUM DIFFICILE ACTION PLAN Action plan to address the rise in cases of Clostridium difficile (C.diff) at Sheffield Teaching Hospitals NHS Foundation Trust ACTION KEY MILESTONES PERSON RESPONSIBLE
CLOSTRIDIUM DIFFICILE ACTION PLAN Action plan to address the rise in cases of Clostridium difficile (C.diff) at Sheffield Teaching Hospitals NHS Foundation Trust ACTION KEY MILESTONES PERSON RESPONSIBLE
Keenan Pharmacy Care Management (KPCM)
 Keenan Pharmacy Care Management (KPCM) This program is an exclusive to KPS clients as an additional layer of pharmacy benefit management by engaging physicians and members directly to ensure that the best
Keenan Pharmacy Care Management (KPCM) This program is an exclusive to KPS clients as an additional layer of pharmacy benefit management by engaging physicians and members directly to ensure that the best
Integrating the LLM / JCPP-PPCP Seena Haines, PharmD, BCACP, FASHP, FAPhA, BC-ADM, CDE Jenny A. Van Amburgh, PharmD, RPh, FAPhA, BCACP, CDE
 Integrating the LLM / JCPP-PPCP Seena Haines, PharmD, BCACP, FASHP, FAPhA, BC-ADM, CDE Jenny A. Van Amburgh, PharmD, RPh, FAPhA, BCACP, CDE Integrating the LLM / JCPP-PPCP Seena Haines, PharmD, BCACP,
Integrating the LLM / JCPP-PPCP Seena Haines, PharmD, BCACP, FASHP, FAPhA, BC-ADM, CDE Jenny A. Van Amburgh, PharmD, RPh, FAPhA, BCACP, CDE Integrating the LLM / JCPP-PPCP Seena Haines, PharmD, BCACP,
POLICY AND PROCEDURE DEPARTMENT: Pharmacy Operations
 PAGE: 1 of 6 SCOPE: Centene Corporate Pharmacy Department, Centene Corporate Pharmacy and Therapeutics Committee, Health Plan Pharmacy Departments, Health Plan Pharmacy and Therapeutics Committees, and
PAGE: 1 of 6 SCOPE: Centene Corporate Pharmacy Department, Centene Corporate Pharmacy and Therapeutics Committee, Health Plan Pharmacy Departments, Health Plan Pharmacy and Therapeutics Committees, and
Boarding Impact on patients, hospitals and healthcare systems
 Boarding Impact on patients, hospitals and healthcare systems Dan Beckett Consultant Acute Physician NHSFV National Clinical Lead Whole System Patient Flow Project Scottish Government May 2014 Important
Boarding Impact on patients, hospitals and healthcare systems Dan Beckett Consultant Acute Physician NHSFV National Clinical Lead Whole System Patient Flow Project Scottish Government May 2014 Important
THE BEST OF TIMES: PHARMACY IN AN ERA OF
 OBJECTIVES THE BEST OF TIMES: PHARMACY IN AN ERA OF ACCOUNTABLE CARE Toni Fera, BS, PharmD October 17, 2014 1. Describe the role of pharmacists in accountable care organizations (ACO). 2. List four key
OBJECTIVES THE BEST OF TIMES: PHARMACY IN AN ERA OF ACCOUNTABLE CARE Toni Fera, BS, PharmD October 17, 2014 1. Describe the role of pharmacists in accountable care organizations (ACO). 2. List four key
Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination
 Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Medication Reconciliation for Older Adults Transitioning from. Long-Term Care to Home. Allison (Leverett) Kackman
 Medication Reconciliation for Older Adults Transitioning from Long-Term Care to Home By Allison (Leverett) Kackman Washington State University Spokane. Riverpoint campus Ubrary P.O. Box 1495 Spokane, WA
Medication Reconciliation for Older Adults Transitioning from Long-Term Care to Home By Allison (Leverett) Kackman Washington State University Spokane. Riverpoint campus Ubrary P.O. Box 1495 Spokane, WA
The Core Elements of Antibiotic Stewardship for Nursing Homes
 The Core Elements of Antibiotic Stewardship for Nursing Homes National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion 1 CS273578-A The Core Elements of Antibiotic
The Core Elements of Antibiotic Stewardship for Nursing Homes National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion 1 CS273578-A The Core Elements of Antibiotic
Medical Intensive Care Unit Rotation EUHM
 PGY 2 Residency Training Program Medical Intensive Care Unit Rotation EUHM Preceptor: Derek M. Polly, PharmD Office: EUHM, 2 nd Floor, Room 2182 Hours: ~ 7:30 4:00 Desk: 404 686 5674 Pager: 404 686 5500
PGY 2 Residency Training Program Medical Intensive Care Unit Rotation EUHM Preceptor: Derek M. Polly, PharmD Office: EUHM, 2 nd Floor, Room 2182 Hours: ~ 7:30 4:00 Desk: 404 686 5674 Pager: 404 686 5500
This paper provides detail of actions to reduce the incidence of Clostridium difficile at Airedale NHS Foundation Trust (ANHST).
 Airedale NHS Foundation Trust Board of Directors: 27 February 2013 Title: Update on Actions to Reduce the Incidence of Clostridium difficile at Airedale NHS Foundation Trust Author: Allison Charlesworth,
Airedale NHS Foundation Trust Board of Directors: 27 February 2013 Title: Update on Actions to Reduce the Incidence of Clostridium difficile at Airedale NHS Foundation Trust Author: Allison Charlesworth,
Background and Methodology
 Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
What is prescribing? Proposal. Non-Medical Prescribing. 4 Domains of Prescribing. Mapping the 4 Domains of Prescribing.
 Non-Medical Charles Mitchell What is prescribing? Director CSEP, University of Queensland Senior Medical Advisor, MSQ, QH Proposal should be considered in a similar way to procedures Where a combination
Non-Medical Charles Mitchell What is prescribing? Director CSEP, University of Queensland Senior Medical Advisor, MSQ, QH Proposal should be considered in a similar way to procedures Where a combination
4. Hospital and community pharmacies
 4. Hospital and community pharmacies As FIP is the international professional organisation of pharmacists, this paper emphasises the role of the pharmacist in ensuring and increasing patient safety. The
4. Hospital and community pharmacies As FIP is the international professional organisation of pharmacists, this paper emphasises the role of the pharmacist in ensuring and increasing patient safety. The
A Layered Learning Medication Reconciliation Program
 A Layered Learning Medication Reconciliation Program Brittany Bates, PharmD, BCPS Clinical Pharmacist, Lima Memorial Health System Clinical Assistant Professor, Ohio Northern University Jana Randolph,
A Layered Learning Medication Reconciliation Program Brittany Bates, PharmD, BCPS Clinical Pharmacist, Lima Memorial Health System Clinical Assistant Professor, Ohio Northern University Jana Randolph,
Enhanced Recovery Implementing Meaningful Change
 Enhanced Recovery Implementing Meaningful Change Jeff Simmons MD Associate Professor UAB Department of Anesthesiology and Perioperative Medicine I have no relevant financial relationships to disclose.
Enhanced Recovery Implementing Meaningful Change Jeff Simmons MD Associate Professor UAB Department of Anesthesiology and Perioperative Medicine I have no relevant financial relationships to disclose.
Expanding Antimicrobial Stewardship to Urgent Care Centers Through a Pharmacist-Led Culture Follow-up Program
 Infect Dis Ther (2017) 6:453 459 DOI 10.1007/s40121-017-0168-8 BRIEF REPORT Expanding Antimicrobial Stewardship to Urgent Care Centers Through a Pharmacist-Led Culture Follow-up Program Lisa E. Dumkow.
Infect Dis Ther (2017) 6:453 459 DOI 10.1007/s40121-017-0168-8 BRIEF REPORT Expanding Antimicrobial Stewardship to Urgent Care Centers Through a Pharmacist-Led Culture Follow-up Program Lisa E. Dumkow.
Medicines Governance Service to Care Homes (Care Home Service)
 Medicines Governance Service to Care Homes (Care Home Service) Locally Enhanced Service Authors: Ruth Buchan, Senior Pharmacist Medicines Management 4th Floor F Mill Dean Clough Halifax HX3 5AX Tel-01422
Medicines Governance Service to Care Homes (Care Home Service) Locally Enhanced Service Authors: Ruth Buchan, Senior Pharmacist Medicines Management 4th Floor F Mill Dean Clough Halifax HX3 5AX Tel-01422
Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit
 ORIGINAL RESEARCH Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit Barry D. Weiss, MD, Angela G. Brega, PhD, William G. LeBlanc, PhD, Natabhona
ORIGINAL RESEARCH Improving the Effectiveness of Medication Review: Guidance from the Health Literacy Universal Precautions Toolkit Barry D. Weiss, MD, Angela G. Brega, PhD, William G. LeBlanc, PhD, Natabhona
Transition of Care Practices. Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI
 Transition of Care Practices Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI Objectives Pharmacist 1. Describe transition of care opportunities 2. Explain ways to use pharmacist extenders
Transition of Care Practices Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI Objectives Pharmacist 1. Describe transition of care opportunities 2. Explain ways to use pharmacist extenders
Improving compliance with oral methotrexate guidelines. Action for the NHS
 Patient safety alert 13 Alert Immediate action Action Update Information request Ref: NPSA/2006/13 Improving compliance with oral methotrexate guidelines Oral methotrexate is a safe and effective medication
Patient safety alert 13 Alert Immediate action Action Update Information request Ref: NPSA/2006/13 Improving compliance with oral methotrexate guidelines Oral methotrexate is a safe and effective medication
Health Professionals, Decision Makers and Optimal Prescribing: Toward an Effective Strategy for All
 CADTH Symposium Halifax, 2010 Health Professionals, Decision Makers and Optimal Prescribing: Toward an Effective Strategy for All Dr. Sam Shortt Director of Knowledge Transfer & Practice Policy Canadian
CADTH Symposium Halifax, 2010 Health Professionals, Decision Makers and Optimal Prescribing: Toward an Effective Strategy for All Dr. Sam Shortt Director of Knowledge Transfer & Practice Policy Canadian
Pharmacists in Transitions of Care: We Can All Make a Difference
 Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
NSW Child Health Network Allied Health Education & Clinical Support Program Clinical Handover Report
 NSW Child Health Network Allied Health Education & Clinical Support Program Clinical Handover Report Carmel Blayden (M Health Science), Allied Health Educator Western Child Health Network, Ward 11, Bloomfield
NSW Child Health Network Allied Health Education & Clinical Support Program Clinical Handover Report Carmel Blayden (M Health Science), Allied Health Educator Western Child Health Network, Ward 11, Bloomfield
Position Statement. Enhanced Authorit y for the Pharmacist. Prescribe. Collaborative Practice Environments. September 2008
 Saskatchewan College of Pharmacists Position Statement On Enhanced Authorit y for the Pharmacist To Prescribe Drugs In Collaborative Practice Environments September 2008 Executive Summary: The Saskatchewan
Saskatchewan College of Pharmacists Position Statement On Enhanced Authorit y for the Pharmacist To Prescribe Drugs In Collaborative Practice Environments September 2008 Executive Summary: The Saskatchewan
Alberta Health Services. Strategic Direction
 Alberta Health Services Strategic Direction 2009 2012 PLEASE GO TO WWW.AHS-STRATEGY.COM TO PROVIDE FEEDBACK ON THIS DOCUMENT Defining Our Focus / Measuring Our Progress CONSULTATION DOCUMENT Introduction
Alberta Health Services Strategic Direction 2009 2012 PLEASE GO TO WWW.AHS-STRATEGY.COM TO PROVIDE FEEDBACK ON THIS DOCUMENT Defining Our Focus / Measuring Our Progress CONSULTATION DOCUMENT Introduction
Learner Manual. Document Best Possible Medication History (BPMH)
 Learner Manual Document Best Possible Medication History (BPMH) Table of Contents Medication safety... 1 Medication errors impact everyone... 1 Who should obtain the BPMH?... 1 When is the BPMH obtained?...
Learner Manual Document Best Possible Medication History (BPMH) Table of Contents Medication safety... 1 Medication errors impact everyone... 1 Who should obtain the BPMH?... 1 When is the BPMH obtained?...
emja: Measuring patient-reported outcomes: moving from clinical trials into clinical p...
 Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Maine Chronic Pain Collaborative 2 (ME CPC2) Chronic Pain Management Change Package for Primary Care Practices
 Maine Chronic Pain Collaborative 2 (ME CPC2) Chronic Pain Management Change Package for Primary Care Practices These 10 change components are intended to support enhanced safety and improved patient care
Maine Chronic Pain Collaborative 2 (ME CPC2) Chronic Pain Management Change Package for Primary Care Practices These 10 change components are intended to support enhanced safety and improved patient care
Provincial Surveillance
 Provincial Surveillance Provincial Surveillance 2011/12 Launched first provincial surveillance protocols Establishment of provincial data entry & start of formal surveillance reports Partnership with AB
Provincial Surveillance Provincial Surveillance 2011/12 Launched first provincial surveillance protocols Establishment of provincial data entry & start of formal surveillance reports Partnership with AB
Quality in Your Endoscopy Unit. David A. Greenwald, MD Mount Sinai Hospital Nancy S. Schlossberg, BSN, RN, CGRN NYSGE Course 2015 December 17, 2015
 Quality in Your Endoscopy Unit David A. Greenwald, MD Mount Sinai Hospital Nancy S. Schlossberg, BSN, RN, CGRN NYSGE Course 2015 December 17, 2015 Two Case Scenarios Patient with concerns about safety
Quality in Your Endoscopy Unit David A. Greenwald, MD Mount Sinai Hospital Nancy S. Schlossberg, BSN, RN, CGRN NYSGE Course 2015 December 17, 2015 Two Case Scenarios Patient with concerns about safety
War on Warfarin: Integrating DOACs into your Anticoagulation Service
 War on Warfarin: Integrating DOACs into your Anticoagulation Service David DeiCicchi, Pharm.D, CACP Brigham and Women s Hospital September 30 th, 2016 Disclosures I have no financial conflict of interest
War on Warfarin: Integrating DOACs into your Anticoagulation Service David DeiCicchi, Pharm.D, CACP Brigham and Women s Hospital September 30 th, 2016 Disclosures I have no financial conflict of interest
The Development of the Oncology Symptom Management Clinic
 The Development of the Oncology Symptom Management Clinic Submitted by: Catherine Brady-Copertino BSN, MS, OCN Executive Director Anne Arundel Medical Center s Geaton and JoAnn DeCesaris Cancer Institute
The Development of the Oncology Symptom Management Clinic Submitted by: Catherine Brady-Copertino BSN, MS, OCN Executive Director Anne Arundel Medical Center s Geaton and JoAnn DeCesaris Cancer Institute
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) Communication Care Bundle Guide
 Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) Communication Care Bundle Guide The Scottish Patient Safety Programme (SPSP) is a unique national initiative that aims to improve the safety and reliability
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) Communication Care Bundle Guide The Scottish Patient Safety Programme (SPSP) is a unique national initiative that aims to improve the safety and reliability
2005 American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.) Standards and Guidelines Survey
 Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 10-2006 2005 American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.)
Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 10-2006 2005 American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.)
Drug Utilization Review + Innovation + Design Thinking = Advancing Health Care Quality
 Drug Utilization Review + Innovation + Design Thinking = Advancing Health Care Quality Christopher A. Keeys, BS., PharmD., BCPS, R.Ph. President/CEO, Clinical Pharmacy Associates, Inc. and MedNovations,
Drug Utilization Review + Innovation + Design Thinking = Advancing Health Care Quality Christopher A. Keeys, BS., PharmD., BCPS, R.Ph. President/CEO, Clinical Pharmacy Associates, Inc. and MedNovations,
