Boosting Your Bottom Line
|
|
|
- Megan Golden
- 5 years ago
- Views:
Transcription
1 Boosting Your Bottom Line Making More Money for Clinics Lisa Clark, MBA NYS Office of Mental Health 7/26/16
2 Partners in CTAC and MCTAC include:
3 Agenda Introduction Review of Revenue Maximization Basics Strategies Fiscal Impact Show Me the $$ Quick Tips Identify Specific Areas of Need for Fall 2016 CTAC Series Questions
4 Fiscal Viability of Article 31 Clinic Providers 100% % SURPLUS/(LOSS) OF TOTAL EXPENSES (n= 175) 80% 60% 44% 40% 30% 20% 26% 0% -20% -40% -60% -80% Data Source: 2013 CFR; Adjusted for Outliers
5 WHAT S YOUR ISSUE?
6 Challenges to Fiscal Viability Discontinuation of Comprehensive Outpatient Services (COPS) Funding Clinic rate supplements that offset the uninsured and underinsured 30 Providers with COPS rates >$130 Conversion to Ambulatory Patient Groups (APGs) 4 year transition to 100% APG rates Old System: 3 rate codes, 6 clinic services New System: 8 rate codes, 40 CPT codes Modifiers Insufficient Commercial Rates Payer Mix (% Medicaid vs Other)
7 Challenges to Fiscal Viability Productivity No Show Rates High Expenses: Rents, Staff Salaries, Fringe Benefits Claim Denials Inconsistencies amongst plans Day-to-Day Operations Transition of other BH Services to Medicaid Managed Care Not a Clinic thing or is it?
8 Revenue Maximization Review
9 Revenue Maximization Collecting the most money for the services that you re already providing OR Picking up the bags of money left on the floor!
10 What you Need to Know
11 Where s the $$? Pre-Admission Visits Initial Assessments Modifiers Physician Add-Ons Crisis Intervention Complex Care Management
12 Pre-Admission Visits OMH allows (but does not require) 3 pre-admission procedures prior to admission Pre-Admission = Screening Status Individual has not officially been admitted to the clinic 30 day clock for Treatment Plan has not started Benefits Provides reimbursement while evaluating the need for further treatment Provides revenue for services to individuals who may not want further treatment Common Pre-Admission Procedures Crisis Intervention (Brief) Initial Assessments
13 Initial Assessments Face-to-face interaction of at least 45 min, in order to: Evaluate for admission Determine MH diagnosis Develop a Treatment Plan Can be provided during Pre-Admission/screening and/or after admission NOTE: An Assessment is a procedure and Pre-Admission is a status The terms are NOT interchangeable
14 Initial Assessments OMH allows up to 3 Initial Assessments during an episode of service 2 Types of Assessments: Initial Assessment Diagnostic & Treatment Plan (45 min+) Initial Assessment Diagnostic & Treatment Plan with Medical Services (45 min+) Managed Care Plans don t have to pay for 3 They commonly pay and Know how many each plan covers
15 90792 Initial Assessment with Medical Services Can only be performed by a Psychiatrist, Physician, or Psychiatric Nurse Practitioner Using the code alone won t pay the correct rate! You MUST add a Physician Modifier to the to be paid correctly Psychiatrist = AF Physician = AG Nurse Practitioner = SA Using the modifier code adds 45% to the rate 2015: 52% of providers did NOT add the modifier $$ TIP: Have MD & NPP use rather than & program billing software to add modifier
16 How much more can you make? Adding the AF/SA modifier to 90791/90792 pays:
17 Maximize Revenue thru Initial Assessments Initial Assessment Diagnostic & Treatment Plan $ $ Amt w/physician mod Initial Assessment Diagnostic & Treatment Plan with Medical Services (Must Add Modifier AF or SA to get 45% rate increase) $ $ Amt w/physician mod Psychiatric Assessment mins New Est $ $ Amt w/add ON Psychiatric Assessment mins - ADD ON $ Psychotherapy - Indiv 45 mins $ $ Amt w/physician mod Example: 1st Visit MSW for Intake & Psychosocial (90791) 2 nd Visit MSW completes Psychosocial &/or Tx Plan (90791) 3 rd Visit Psychiatrist (45min+) for Initial Assessment w/medical (90792) + Modifier
18 Physician Add-Ons Psychotropic Medication Treatment New Est $ Psychiatric Assessment - 30 mins New Est $ Psychiatric Assessment - 30 mins - ADD ON $ Psychiatric Assessment mins New Est $ Psychiatric Assessment mins - ADD ON $ $ $ Amt w/add ON Amt w/add ON Psychiatric Assessment 30 minutes ADD-ON Psychiatric Assessment 45 minutes ADD-ON Psychotherapy - therapeutic communication and interaction for the purpose of alleviating symptoms or dysfunction associated with an individual s diagnosed mental illness or emotional disturbance, reversing or changing maladaptive patterns of behavior, encouraging personal growth and development, and supporting the individual s capacity to achieve age-appropriate developmental milestones.
19 Medicaid Physician Add-Ons Medicaid vs Medicare 90833: Total time spent >= 30 mins, incl E&M 90836: Total time spent >= 45 mins, incl E&M E&M codes = , Medicare rules are different! Time for E&M service is in addition to the time spent for psychotherapy Example: If you bill and and the total time of visit = 30 minutes this = an overpayment
20 TIP for New Patients : E&M codes for the Psychiatric Assessment of a new patient If your psychiatrist or NPP is: Spending a minimum of 45 minutes on this initial appt (they often do), Providing a basic review of health information, Determining the appropriateness for treatment, MH diagnosis, treatment planning, and medication therapy Code these visits as and have your billing system automatically add the AF/SA modifier Look at your reports and see how often are being used
21 How Much $ are you Leaving?
22 Crisis Intervention Crisis Intervention Brief (H2011) Pays $56 - $79 15 minute units, up to a max of 6 units Face-to-face or by phone Individuals don t have to have previously received services at the clinic Can be provided off-site (pays 50% more) Crisis Intervention Complex (S9484) Minimum of 1 hr of FTF contact by 2 or more staff Individual must have been in service at the clinic within 2 yrs Crisis Intervention Per Diem (S9485) 3 or more hrs of FTF time by 2 or more staff Individual must have been in service at the clinic within 2 yrs
23 Complex Care Management An ancillary service to psychotherapy, psychotropic medication treatment or crisis intervention services Must take place within 14 days of eligible service Billable in 5 minute units, 4 units max Provided in person or by phone, with or without the client Provided in order to prevent a change in community status or as a response to a complex condition NOT routine care or referrals Must be medically necessary The need for follow-up must be documented Pays $14 - $19/unit Underutilized
24 Offsite Services for Children School-based satellite clinics Must be written in Treatment Plan Home Visits after school School vacations - Home Visits - Provide services at alternate locations: e.g. Library, Boys & Girls Club, etc. Benefits Family engagement Continuity of care Increases revenue by 50% Example: Psychotherapy Family & Client 1 hr (90847) $ in clinic = $ at home = $97.82 more $$ TIP: Use whenever psychotherapy is 60 mins and family is present for > 29 mins and child for 30 mins
25 Show me the Quick Tips: 1. Check MD claims for Can they be billed as with AF/SA modifier? 2. How many Initial Assessments are you doing per individual? Should have at least and Are there and s for MD time? 4. How many Crisis-Brief visits (H2011) were done? 5. How often is Complex Care Mgmt (90882) being used? 6. If your clinic or satellites are open before 8 AM, after 6PM, or on the weekends, are you billing for After Hours (99051)? 7. If you have bi-lingual staff, are they submitting for Language other than English (U4) when translation is provided?
26 What else can you do?
27 Impact of Payer Mix Know your payer mix and understand how this impacts your bottom line!
28 Impact of Productivity *Normalized Weighted Productivity when 55% of total staff hours are billable * Normalized Weighted Productivity = conversion of CPT units of service to a standardized 45 minute unit
29 Impact of Productivity Normalized Weighted Productivity when 45% of total staff hours are billable Approximately 13% decrease in Revenue
30 Denial Rates 78% Medicaid/MMC & 2% Denial Rate Input Parameters - Revenue Revenue Per billable Rev per CPT Payer Mix Medicaid $ % Medicaid Managed $ % Medicare $ % 3rd Party $ % Uncompensated $ % No Payment (denials, voids, etc.) 2% Avg Revenue per CPT $ % Collection Rate 98% 72% Medicaid/MMC & 8% Denial Rate Input Parameters - Revenue Revenue Per billable Rev per CPT Payer Mix Medicaid $ % Medicaid Managed $ % Medicare $ % 3rd Party $ % Uncompensated $ % No Payment (denials, voids, etc.) 8% Avg Revenue per CPT $ % Collection Rate 92% What s your denial rate? Set goals for denials and track them!
31 Do you get denials from MC Plans that don t seem right?
32 OMH Can Help! Please send copies of your remittance issues along with any additional information to:
33 Dashboard Reports Staff Productivity Report % billable Billable hr. billable hours goal hrs. CPT Unit show rate John Jones % % Jun % % Jul % % Aug % % Sep % % Oct % % Nov % % Dec % % Jan % % Year to Date % % Clinic Performance to Budget Oak St MH Clinic YTD 6/30/2016 Budget Actual Variance Gross 856, ,125 (6,088) Total Rev 856, ,361 (13,852) Operating Surplus/(Deficit) 0 (7,764) (7,764) Units of Service 6,586 6,415 (171) Gross Cost per Unit Net Revenue per Unit Net Surplus/(Loss) per unit 0 (1.21) (1.21) Medicaid Participation 80.00% 82.31% 2.31% Revenue cycle performance to Benchmarks RCM Performance Benchmark Actual Variance Avg days AR Outstanding: Denial rate all sources: 5.00% 4.20% Denial rate Medicaid: 2.50% 2.10% % claims submitted on time: % 93.00% -0.07
34 Revenue Maximization Results 2016 Survey of Clinic Providers who received in-person Revenue Maximization Training
35 Fiscal Viability of Article 31 Clinic Providers 100% % SURPLUS/(LOSS) OF TOTAL EXPENSES (n= 175) 80% 60% 44% 40% 30% 20% 26% 0% -20% -40% -60% -80% Data Source: 2013 CFR; Adjusted for Outliers
36 Revised Fiscal Viability with 15% Revenue Increase SURPLUS / (LOSS) OF TOTAL EXPENSES (n= 175) 120% 100% 80% 60% 40% 17% 18% 65% 20% 0% -20% % -60% -80% Data Source: 2013 CFR; Adjusted for Outliers
37 Questions?
38 THANK YOU FOR ATTENDING TODAY S WEBINAR! Check out our new website: CTAC ctac.info@nyu.edu
The New Medicare PPS For FQHCS. Norma Mendilian, CPA Director of Healthcare Consulting and Reimbursement
 The New Medicare PPS For FQHCS Norma Mendilian, CPA Director of Healthcare Consulting and Reimbursement 508.450.6572 nmendilian@aafcpa.com Health Centers Medicare Program While the Medicare program constitutes
The New Medicare PPS For FQHCS Norma Mendilian, CPA Director of Healthcare Consulting and Reimbursement 508.450.6572 nmendilian@aafcpa.com Health Centers Medicare Program While the Medicare program constitutes
JMOC Update: Behavioral Health Redesign. December 15 th, 2016
 JMOC Update: Behavioral Health Redesign December 15 th, 2016 2 Implementation Schedule BH Redesign 7/1/2017: Medicaid requires rendering (NPI) practitioner*, ORP, and/or supervisor on claims Go Live for
JMOC Update: Behavioral Health Redesign December 15 th, 2016 2 Implementation Schedule BH Redesign 7/1/2017: Medicaid requires rendering (NPI) practitioner*, ORP, and/or supervisor on claims Go Live for
Adult BH HCBS Town Hall ROS Designated Providers. June 13, 2017
 Adult BH HCBS Town Hall ROS Designated Providers June 13, 2017 June 28, 2017 2 Why Behavioral Health Transformation is Needed June 28, 2017 3 Why Behavioral Health Transformation is Needed In NYS, members
Adult BH HCBS Town Hall ROS Designated Providers June 13, 2017 June 28, 2017 2 Why Behavioral Health Transformation is Needed June 28, 2017 3 Why Behavioral Health Transformation is Needed In NYS, members
Behavioral Health Billing and Coding Guide for Montana FQHCs & Primary Care Providers. Virna Little, PsyD, LCSW-R, SAP, CCM Laura Leone, MSSW, LMSW
 Behavioral Health Billing and Coding Guide for Montana FQHCs & Primary Care Providers Virna Little, PsyD, LCSW-R, SAP, CCM Laura Leone, MSSW, LMSW Objectives Answer questions specific to FQHC and Primary
Behavioral Health Billing and Coding Guide for Montana FQHCs & Primary Care Providers Virna Little, PsyD, LCSW-R, SAP, CCM Laura Leone, MSSW, LMSW Objectives Answer questions specific to FQHC and Primary
FQHC Behavioral Health Billing Codes
 FQHC s Eligible Documentation Assessment 90792 Psychiatric Prescribers only (MD, NP, PA, APRN) Psychiatric diagnostic evaluation with medical services. Medical though process clearly reflected in assessment
FQHC s Eligible Documentation Assessment 90792 Psychiatric Prescribers only (MD, NP, PA, APRN) Psychiatric diagnostic evaluation with medical services. Medical though process clearly reflected in assessment
Facility-Based Behavioral Health Program Professional Fees Reimbursement Policy Annual Approval Date. Approved By
 Policy Number 2016RP505A Facility-Based Behavioral Health Program Professional Fees Reimbursement Policy Annual Approval Date 09/30/2016 Approved By Optum Behavioral Reimbursement Committee IMPORTANT NOTE
Policy Number 2016RP505A Facility-Based Behavioral Health Program Professional Fees Reimbursement Policy Annual Approval Date 09/30/2016 Approved By Optum Behavioral Reimbursement Committee IMPORTANT NOTE
Updated Only for Logo and Branding Provider Notice
 Updated Only for Logo and Branding Provider Notice To: From: PerformCare Network Providers Sheryl M. Swanson, MBA, Project Manager Date: December 21, 2012 Subject: AD12 112 2013 CPT Code Update IMPLEMENTATION
Updated Only for Logo and Branding Provider Notice To: From: PerformCare Network Providers Sheryl M. Swanson, MBA, Project Manager Date: December 21, 2012 Subject: AD12 112 2013 CPT Code Update IMPLEMENTATION
Primary Care Setting Behavioral Health Billing Codes
 Primary Care Setting s Medicaid Medicare Third Eligible Documentation Assessment 90792 Psychiatric Prescribers only (MD, NP, PA, APRN) Psychiatric diagnostic evaluation with medical services. Medical though
Primary Care Setting s Medicaid Medicare Third Eligible Documentation Assessment 90792 Psychiatric Prescribers only (MD, NP, PA, APRN) Psychiatric diagnostic evaluation with medical services. Medical though
CCBHCs Part 1: Managing Service Mix and Clinical Workflows Under a PPS. Tim Swinfard. Virna Little, PsyD, LCSW-R, SAP. Rebecca Farley, MPH
 CCBHCs Part 1: Managing Service Mix and Clinical Workflows Under a PPS Tim Swinfard President, Compass Health CEO, Pathways Community Health Virna Little, PsyD, LCSW-R, SAP Senior Vice President, Psychosocial
CCBHCs Part 1: Managing Service Mix and Clinical Workflows Under a PPS Tim Swinfard President, Compass Health CEO, Pathways Community Health Virna Little, PsyD, LCSW-R, SAP Senior Vice President, Psychosocial
Transforming Healthcare Delivery, the Challenges for Behavioral Health
 Transforming Healthcare Delivery, the Challenges for Behavioral Health Presented by: M.T.M. Services, LLC P. O. Box 1027, Holly Springs, NC 27540 Phone: 919-434-3709 Fax: 919-773-8141 E-mail: mtmserve@aol.com
Transforming Healthcare Delivery, the Challenges for Behavioral Health Presented by: M.T.M. Services, LLC P. O. Box 1027, Holly Springs, NC 27540 Phone: 919-434-3709 Fax: 919-773-8141 E-mail: mtmserve@aol.com
Activity Based Cost Accounting and Payment Bundling
 Activity Based Cost Accounting and Payment Bundling 1 Agenda Introduction of Speakers Fast Facts about Jewish Senior Life/Jewish Home of Rochester Determining the need and uses for an Activity Based Cost
Activity Based Cost Accounting and Payment Bundling 1 Agenda Introduction of Speakers Fast Facts about Jewish Senior Life/Jewish Home of Rochester Determining the need and uses for an Activity Based Cost
CAMDEN CLARK MEDICAL CENTER:
 INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
INSIGHT DRIVEN HEALTH CAMDEN CLARK MEDICAL CENTER: CARE MANAGEMENT TRANSFORMATION GENERATES SAVINGS AND ENHANCES CARE OVERVIEW Accenture helped Camden Clark Medical Center, (CCMC), a West Virginia-based
February Jean C. Russell, MS, RHIT Richard Cooley, BA, CCS
 February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
Behavioral Health Providers: Frequently Asked Questions (FAQs)
 Behavioral Health Providers: Frequently Asked Questions (FAQs) Q. What has changed as far as behavioral health services? A1. Effective April 1, 2012, the professional and outpatient facility charges for
Behavioral Health Providers: Frequently Asked Questions (FAQs) Q. What has changed as far as behavioral health services? A1. Effective April 1, 2012, the professional and outpatient facility charges for
John R. Kasich, Governor Tracy J. Plouck, Director
 John R. Kasich, Governor Tracy J. Plouck, Director All Ohio March 24, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy
John R. Kasich, Governor Tracy J. Plouck, Director All Ohio March 24, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy
Deleted Codes. Agenda 1/31/ E/M Codes Deleted Codes New Codes Changed Codes
 February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
February Jean C. Russell, MS, RHIT Richard Cooley, BA, CCS
 February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 2013 E/M Codes Deleted Codes New Codes Changed Codes Agenda Documentation
Analysis of Incurred Claims Trend and Provider Payments
 Analysis of Incurred Claims Trend and Provider Payments Board of Trustees Meeting May 24, 2013 Presentation Overview Trends in Incurred Claims Paid through March 31, 2013 Per Member Per Month (PMPM) By
Analysis of Incurred Claims Trend and Provider Payments Board of Trustees Meeting May 24, 2013 Presentation Overview Trends in Incurred Claims Paid through March 31, 2013 Per Member Per Month (PMPM) By
Rebalancing the Cost Structure: Progressive Health Systems, Inc. Bob Haley, CEO Steve Hall, CFO
 Rebalancing the Cost Structure: Progressive Health Systems, Inc. Bob Haley, CEO Steve Hall, CFO THE MARKET & PHS S POSITION 2 Progressive Health Systems, Inc. (dba Pekin Hospital) Pekin, IL 3 4 5 Nearby
Rebalancing the Cost Structure: Progressive Health Systems, Inc. Bob Haley, CEO Steve Hall, CFO THE MARKET & PHS S POSITION 2 Progressive Health Systems, Inc. (dba Pekin Hospital) Pekin, IL 3 4 5 Nearby
Presented by: Jodie Edmonds VP Medicaid Revenue Consultant Passport Health Communications
 Presented by: Jodie Edmonds VP Medicaid Revenue Consultant Passport Health Communications Complete and correct coding of claims will become more important, and will have an effect on claim payment. The
Presented by: Jodie Edmonds VP Medicaid Revenue Consultant Passport Health Communications Complete and correct coding of claims will become more important, and will have an effect on claim payment. The
FQHC Behavioral Health Clinical Network Retreat
 FQHC Behavioral Health Clinical Network Retreat 1 Behavioral Health Services Agenda Provider Enrollment Review Policies and Procedure Review Behavioral Health Boot Camp Questions 2 1 Disclaimer The materials
FQHC Behavioral Health Clinical Network Retreat 1 Behavioral Health Services Agenda Provider Enrollment Review Policies and Procedure Review Behavioral Health Boot Camp Questions 2 1 Disclaimer The materials
Emerging Outpatient CDI Drivers and Technologies
 7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
Webinar Control Panel
 Clear Communications Through Dashboard Reports 1 2012 Community Action Program Legal Services, Inc. Webinar Control Panel Raise your hand to ask a question Only enabled if you have entered your Audio Pin!
Clear Communications Through Dashboard Reports 1 2012 Community Action Program Legal Services, Inc. Webinar Control Panel Raise your hand to ask a question Only enabled if you have entered your Audio Pin!
COMPLEX TRAUMA Frequently Asked Questions From the In-Person Workflow Trainings February 2017
 COMPLEX TRAUMA Frequently Asked Questions From the In-Person Workflow Trainings February 2017 Billing: Q: How do you bill for conducting the assessments? Who can bill for conducting the assessments? The
COMPLEX TRAUMA Frequently Asked Questions From the In-Person Workflow Trainings February 2017 Billing: Q: How do you bill for conducting the assessments? Who can bill for conducting the assessments? The
The Triple Aim. Productivity: Digging Deep Enough 11/4/2013. quality and satisfaction); Improving the health of populations; and
 NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
NAHC Annual Conference October, 2013 Cindy Campbell, BSN, RN Associate Director Operational Consulting Fazzi Jeanie Stoker, BSN, RN, MPA, BC Director AnMed Health Home Care Context AnMed Health Home Health
Overview of the Hospice Proposed Rule
 HOSPICE Overview of Hospice Payment Reform Robert J. Simione Managing Principal Simione Healthcare Consultants On April 29, 2013 CMS issued the proposed rule that would update FY 2014 Medicare payment
HOSPICE Overview of Hospice Payment Reform Robert J. Simione Managing Principal Simione Healthcare Consultants On April 29, 2013 CMS issued the proposed rule that would update FY 2014 Medicare payment
MEDICAID PRIOR AUTHORIZATION TRANSITION
 MEDICAID PRIOR AUTHORIZATION TRANSITION Prepared for: Mississippi Medicaid Providers of - Psychological, Neuropsychological and Developmental Testing November, 2013 December 1, 2013 The Road Ahead 2 Today
MEDICAID PRIOR AUTHORIZATION TRANSITION Prepared for: Mississippi Medicaid Providers of - Psychological, Neuropsychological and Developmental Testing November, 2013 December 1, 2013 The Road Ahead 2 Today
Implementing Medicaid Behavioral Health Reform in New York
 Redesign Medicaid in New York State Implementing Medicaid Behavioral Health Reform in New York HIV Health and Human Services Planning Council of New York March 19, 2014 Agenda Goals Timeline BH Benefit
Redesign Medicaid in New York State Implementing Medicaid Behavioral Health Reform in New York HIV Health and Human Services Planning Council of New York March 19, 2014 Agenda Goals Timeline BH Benefit
JMOC Update: Behavioral Health Redesign. March 16 th, 2017
 JMOC Update: Behavioral Health Redesign March 16 th, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy to rebuild
JMOC Update: Behavioral Health Redesign March 16 th, 2017 Ohio Medicaid Behavioral Health Redesign Initiative The Redesign Initiative is an integral component of Ohio s comprehensive strategy to rebuild
Cardinal Innovations Child Continuum of Care Philosophy. March 2014
 Cardinal Innovations Child Continuum of Care Philosophy March 2014 Disclaimer Information provided in this presentation pertains only to the counties in the Cardinal Innovations Healthcare Solutions Region.
Cardinal Innovations Child Continuum of Care Philosophy March 2014 Disclaimer Information provided in this presentation pertains only to the counties in the Cardinal Innovations Healthcare Solutions Region.
Mississippi Medicaid Outpatient Hospital Mental Health Services Provider Manual
 Mississippi Medicaid Outpatient Hospital Mental Health Services Effective Date: January 1, 2009 Revised: January 2017 Table of Contents: Hospital Outpatient Mental Health I. Getting Started Helpful Tips
Mississippi Medicaid Outpatient Hospital Mental Health Services Effective Date: January 1, 2009 Revised: January 2017 Table of Contents: Hospital Outpatient Mental Health I. Getting Started Helpful Tips
PerformCare Provider Network (MH Inpatient Psychiatric Providers) Scott Daubert, VP Operations
 Memorandum To: From: Date: July 1, 2013 Subject: PerformCare Provider Network (MH Inpatient Psychiatric Providers) Scott Daubert, VP Operations PC-11 Use of CRNP s for Inpatient Hospital Care Claims Payment
Memorandum To: From: Date: July 1, 2013 Subject: PerformCare Provider Network (MH Inpatient Psychiatric Providers) Scott Daubert, VP Operations PC-11 Use of CRNP s for Inpatient Hospital Care Claims Payment
NEW YORK STATE CHILDREN S HEALTH AND BEHAVIORAL HEALTH (BH) SERVICES CHILDREN S MEDICAID SYSTEM TRANSFORMATION BILLING AND CODING MANUAL
 NEW YORK STATE CHILDREN S HEALTH AND BEHAVIORAL HEALTH (BH) SERVICES CHILDREN S MEDICAID SYSTEM TRANSFORMATION BILLING AND CODING MANUAL 1 Table of Contents General... 5 Purpose of this Manual... 5 New
NEW YORK STATE CHILDREN S HEALTH AND BEHAVIORAL HEALTH (BH) SERVICES CHILDREN S MEDICAID SYSTEM TRANSFORMATION BILLING AND CODING MANUAL 1 Table of Contents General... 5 Purpose of this Manual... 5 New
PSYCHIATRY SERVICES: MD FOCUSED
 PSYCHIATRY SERVICES: MD FOCUSED CY2013 Risk Based Scheduled Review Agenda 2 Overview of New Risk Based Scheduled Reviews Initial review findings PhD summary MD summary Examples Template/Psychotherapy Time
PSYCHIATRY SERVICES: MD FOCUSED CY2013 Risk Based Scheduled Review Agenda 2 Overview of New Risk Based Scheduled Reviews Initial review findings PhD summary MD summary Examples Template/Psychotherapy Time
RPC and OMH Collaborative Care Webinar. February 1, pm
 RPC and OMH Collaborative Care Webinar February 1, 2018 1 2pm AGENDA Welcome & Introductions OMH Care Collaborative Overview Q&A Cathy Hoehn, LMHC RPC Initiative Director CH@clmhd.org 518 396 0788 www.clmhd.org/rpc
RPC and OMH Collaborative Care Webinar February 1, 2018 1 2pm AGENDA Welcome & Introductions OMH Care Collaborative Overview Q&A Cathy Hoehn, LMHC RPC Initiative Director CH@clmhd.org 518 396 0788 www.clmhd.org/rpc
Mobile Medical Review Team Observation Services & the 2 Midnight Rule. The Audio and/or Video Recording of this Educational Session is Prohibited
 Mobile Medical Review Team Observation Services & the 2 Midnight Rule The Audio and/or Video Recording of this Educational Session is Prohibited National Government Services, Inc. Medicare Part A & Part
Mobile Medical Review Team Observation Services & the 2 Midnight Rule The Audio and/or Video Recording of this Educational Session is Prohibited National Government Services, Inc. Medicare Part A & Part
MAGELLAN UNIVERSAL SERVICES LIST - Includes Preferred HIPAA Compliant Codes. UB-04 Revenue Codes
 Service Name & Detailed Magellan Description (see column heading explanations at end of this document) MAGELLAN UNIVERSAL SERVICES LIST - Includes Preferred HIPAA Compliant Codes Codes Used to Determine
Service Name & Detailed Magellan Description (see column heading explanations at end of this document) MAGELLAN UNIVERSAL SERVICES LIST - Includes Preferred HIPAA Compliant Codes Codes Used to Determine
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services (DMAHS)
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services (DMAHS) Outpatient Facility Behavioral Health Integration Billing Frequently Asked Questions (FAQs) 1.
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services (DMAHS) Outpatient Facility Behavioral Health Integration Billing Frequently Asked Questions (FAQs) 1.
Mental Health Services
 Mental Health Services Fee-for-Service Indiana Health Coverage Programs DXC Technology October 2017 1 Agenda Reference Materials Provider Healthcare Portal Outpatient Mental Health Inpatient Mental Health
Mental Health Services Fee-for-Service Indiana Health Coverage Programs DXC Technology October 2017 1 Agenda Reference Materials Provider Healthcare Portal Outpatient Mental Health Inpatient Mental Health
Principles of Revenue Cycle Management and Utilization Management. For Children s Providers
 Principles of Revenue Cycle Management and Utilization Management For Children s Providers Introduction & Housekeeping Housekeeping: Slides will be posted at MCTAC.org after the last of these events Questions
Principles of Revenue Cycle Management and Utilization Management For Children s Providers Introduction & Housekeeping Housekeeping: Slides will be posted at MCTAC.org after the last of these events Questions
Financing and Sustainability Strategies for Behavioral Health Integration Anna Ratzliff, MD, PhD Associate Director for Education AIMS Center
 Financing and Sustainability Strategies for Behavioral Health Integration Anna Ratzliff, MD, PhD Associate Director for Education AIMS Center Advancing Integrated Mental Health Solutions The Healthier
Financing and Sustainability Strategies for Behavioral Health Integration Anna Ratzliff, MD, PhD Associate Director for Education AIMS Center Advancing Integrated Mental Health Solutions The Healthier
Time-Based Coding. Agenda. AMA Time Rule Physical Medicine Services Anesthesia Evaluation and Management Services Mental Health Services 2016 Changes
 Time-Based Coding Presented by: Mike Strong, SFM The Work Comp Experts Agenda AMA Time Rule Physical Medicine Services Anesthesia Evaluation and Management Services Mental Health Services 2016 Changes
Time-Based Coding Presented by: Mike Strong, SFM The Work Comp Experts Agenda AMA Time Rule Physical Medicine Services Anesthesia Evaluation and Management Services Mental Health Services 2016 Changes
Cognitive Emotional Social Behavioral functioning
 TIP SHEET Health and Behavior Assessment and Intervention (HBAI) Services Coverage of Chronic Disease Self-Management Education Medicare and Medicare Advantage Purpose: The HBAI services are used to identify
TIP SHEET Health and Behavior Assessment and Intervention (HBAI) Services Coverage of Chronic Disease Self-Management Education Medicare and Medicare Advantage Purpose: The HBAI services are used to identify
Required Data for Claim Forms (CMS-1500 & UB-04) Claim Submission Instructions (MLTC) Care Healthcare and VNSNY CHOICE Transition
 2018 Provider Manual VNSNY CHOICE Appendix V Claims CMS-1500 Form (Sample) UB-04 Form (Sample) Required Data for Claim Forms (CMS-1500 & UB-04) Claim Submission Instructions (MLTC) ICD-10 FAQ Care Healthcare
2018 Provider Manual VNSNY CHOICE Appendix V Claims CMS-1500 Form (Sample) UB-04 Form (Sample) Required Data for Claim Forms (CMS-1500 & UB-04) Claim Submission Instructions (MLTC) ICD-10 FAQ Care Healthcare
Stakeholder input is gathered in several ways. Patients are given the opportunity to provide feedback, the SWOT analysis is based on information from
 Strategic Plan 27 Executive Summary The following is a summary of the information shared in this Operations Review and Plan. This plan highlights operational achievements and challenges, clinical outcomes
Strategic Plan 27 Executive Summary The following is a summary of the information shared in this Operations Review and Plan. This plan highlights operational achievements and challenges, clinical outcomes
Hospitals and the Economy. Anne McLeod Vice President, Finance Policy California Hospital Association
 Anne McLeod Vice President, Finance Policy California Hospital Association American hospitals are financially challenged and the trends in revenues and expenses will put and even greater burden on the
Anne McLeod Vice President, Finance Policy California Hospital Association American hospitals are financially challenged and the trends in revenues and expenses will put and even greater burden on the
Provider Frequently Asked Questions
 Provider Frequently Asked Questions Strengthening Clinical Processes Training CASE MANAGEMENT: Q1: Does Optum allow Case Managers to bill for services provided when the Member is not present? A1: Optum
Provider Frequently Asked Questions Strengthening Clinical Processes Training CASE MANAGEMENT: Q1: Does Optum allow Case Managers to bill for services provided when the Member is not present? A1: Optum
HOMECARE AND HOSPICE REIMBURSEMENT
 Hospice Modeling Hospice Changes to Prepare for Medicare Reimbursement and Care Delivery Reform Robert J. Simione Managing Principal Simione Healthcare Consultants, LLC HOMECARE AND HOSPICE REIMBURSEMENT
Hospice Modeling Hospice Changes to Prepare for Medicare Reimbursement and Care Delivery Reform Robert J. Simione Managing Principal Simione Healthcare Consultants, LLC HOMECARE AND HOSPICE REIMBURSEMENT
Volume 26 No. 05 July Providers of Behavioral Health Services For Action Health Maintenance Organizations For Information Only
 Newsletter Published by the N.J. Dept. of Human, Div. of Medical Assistance & Health & the Division of and Volume 26 No. 05 July 2016 TO: SUBJECT: Providers of Behavioral Health For Action Health Maintenance
Newsletter Published by the N.J. Dept. of Human, Div. of Medical Assistance & Health & the Division of and Volume 26 No. 05 July 2016 TO: SUBJECT: Providers of Behavioral Health For Action Health Maintenance
Not Covered HCPCS Codes Reimbursement Policy. Approved By
 Policy Number 2017RP506A Annual Approval Date Not Covered HCPCS Codes Reimbursement Policy 6/27/2017 Approved By Optum Behavioral Reimbursement Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY
Policy Number 2017RP506A Annual Approval Date Not Covered HCPCS Codes Reimbursement Policy 6/27/2017 Approved By Optum Behavioral Reimbursement Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY
Patient Financial Services Policy
 Patient Financial Services Policy Policy: Purpose: Billing & Collection Policy MaineHealth hospitals and physician practices are the frontline caregivers providing medically necessary care for all people
Patient Financial Services Policy Policy: Purpose: Billing & Collection Policy MaineHealth hospitals and physician practices are the frontline caregivers providing medically necessary care for all people
Annual Wellness Visit (AWV) Delivery Business Case
 Annual Wellness Visit (AWV) Delivery Business Case The implications of the adopting and/or actively promoting AWV services for the practice s bottom line are dependent on a number of factors, including:
Annual Wellness Visit (AWV) Delivery Business Case The implications of the adopting and/or actively promoting AWV services for the practice s bottom line are dependent on a number of factors, including:
Specialty Behavioral Health and Integrated Services
 Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
Clinical Utilization Management Guideline
 Clinical Utilization Management Guideline Subject: Therapeutic Behavioral On-Site Services for Recipients Under the Age of 21 Years Status: New Current Effective Date: January 2018 Description Last Review
Clinical Utilization Management Guideline Subject: Therapeutic Behavioral On-Site Services for Recipients Under the Age of 21 Years Status: New Current Effective Date: January 2018 Description Last Review
Medicaid Rehabilitation Option Provider Manual
 EDS Provider Relations Unit INDIANA HEALTH COVERAGE PROGRAMS Medicaid Rehabilitation Option Provider Manual L I B R A R Y R E F E R E N C E N U M B E R : P R P R 1 0 0 0 6 R E V I S I O N D A T E : D E
EDS Provider Relations Unit INDIANA HEALTH COVERAGE PROGRAMS Medicaid Rehabilitation Option Provider Manual L I B R A R Y R E F E R E N C E N U M B E R : P R P R 1 0 0 0 6 R E V I S I O N D A T E : D E
BHAC, ERMHS and FC MFT/LCSW Fee Table Basic Language
 BHAC, ERMHS and FC MFT/LCSW Fee Table Language Fee 90791 Diagnostic Evaluation (No Medical) MFT/LCSW 86.52 107.52 90832 Psychotherapy (16-37) min MFT/LCSW 32.45 53.45 90834 Psychotherapy (38-52) min MFT/LCSW
BHAC, ERMHS and FC MFT/LCSW Fee Table Language Fee 90791 Diagnostic Evaluation (No Medical) MFT/LCSW 86.52 107.52 90832 Psychotherapy (16-37) min MFT/LCSW 32.45 53.45 90834 Psychotherapy (38-52) min MFT/LCSW
Paying for HIV Prevention: Reimbursement & Sustainable Payer Sources
 Paying for HIV Prevention: Reimbursement & Sustainable Payer Sources About the Primary Care Development Corporation (PCDC) Founded in 1993, PCDC s mission is to catalyze excellence in primary care through
Paying for HIV Prevention: Reimbursement & Sustainable Payer Sources About the Primary Care Development Corporation (PCDC) Founded in 1993, PCDC s mission is to catalyze excellence in primary care through
Strategic KPI Report Performance to December 2017
 Strategic KPI Report Performance to December 2017 Trust Board 25 th January 2018 Strategic KPI summary SROs: All Directors Objective KPI SRO Target Apr May Jun Jul Aug Sep Oct Nov Success Is Deliver A
Strategic KPI Report Performance to December 2017 Trust Board 25 th January 2018 Strategic KPI summary SROs: All Directors Objective KPI SRO Target Apr May Jun Jul Aug Sep Oct Nov Success Is Deliver A
Are NPs and PAs Right for Your Practice?
 Society of Hospital Medicine Roundtable Are NPs and PAs Right for Your Practice? January 14, 2010 Michael L. Powe, Vice President Health Systems & Reimbursement Policy American Academy of Physician Assistants
Society of Hospital Medicine Roundtable Are NPs and PAs Right for Your Practice? January 14, 2010 Michael L. Powe, Vice President Health Systems & Reimbursement Policy American Academy of Physician Assistants
AVATAR Billing Providers Bulletin Medicare-MediCal Issue
 DPH Fiscal - CBHS Billing Page 1 of 5 What is Medicare? Medicare is a health insurance program for: people age 65 or older, people under age 65 with certain disabilities, and people of all ages with End-Stage
DPH Fiscal - CBHS Billing Page 1 of 5 What is Medicare? Medicare is a health insurance program for: people age 65 or older, people under age 65 with certain disabilities, and people of all ages with End-Stage
Medicaid Managed Care Utilization Management and Integrated Billing Overview
 Medicaid Managed Care Utilization Management and Integrated Billing Overview March, 23 2016 The Managed Care Technical Assistance Center of New York 1 st webinar in series about UM and Billing. In- person
Medicaid Managed Care Utilization Management and Integrated Billing Overview March, 23 2016 The Managed Care Technical Assistance Center of New York 1 st webinar in series about UM and Billing. In- person
JMOC Update: Behavioral Health Redesign. June 22, 2017
 JMOC Update: Behavioral Health Redesign June 22, 2017 2 Progress Since Last JMOC Update ODM and OhioMHAS communicated the actions below at the March JMOC update: Next Steps: March 2017 Rules process, Trainings
JMOC Update: Behavioral Health Redesign June 22, 2017 2 Progress Since Last JMOC Update ODM and OhioMHAS communicated the actions below at the March JMOC update: Next Steps: March 2017 Rules process, Trainings
Compliant Documentation for Coding and Billing. Caren Swartz CPC,CPMA,CPC-H,CPC-I
 Compliant Documentation for Coding and Billing Caren Swartz CPC,CPMA,CPC-H,CPC-I caren@practiceintegrity.com Disclaimer Information contained in this text is based on CPT, ICD-9-CM and HCPCS rules and
Compliant Documentation for Coding and Billing Caren Swartz CPC,CPMA,CPC-H,CPC-I caren@practiceintegrity.com Disclaimer Information contained in this text is based on CPT, ICD-9-CM and HCPCS rules and
Inpatient and Residential Psychiatric Treatment Services. October 2017
 Inpatient and Residential Psychiatric Treatment Services October 2017 Overview Provider Participation Requirements Member Eligibility Service Authorization Evaluation, Certificate of Need and Plan of Care
Inpatient and Residential Psychiatric Treatment Services October 2017 Overview Provider Participation Requirements Member Eligibility Service Authorization Evaluation, Certificate of Need and Plan of Care
Inpatient Psychiatric Facility (IPF) Coverage & Documentation. Presented by Palmetto GBA JM A/B MAC Provider Outreach and Education September 7, 2016
 Inpatient Psychiatric Facility (IPF) Coverage & Documentation Presented by Palmetto GBA JM A/B MAC Provider Outreach and Education September 7, 2016 1 Disclaimer This information is current as of August
Inpatient Psychiatric Facility (IPF) Coverage & Documentation Presented by Palmetto GBA JM A/B MAC Provider Outreach and Education September 7, 2016 1 Disclaimer This information is current as of August
UNIVERSITY OF ILLINOIS HOSPITAL & HEALTH SCIENCES SYSTEM HOSPITAL DASHBOARD
 UNIVERSITY OF ILLINOIS HOSPITAL & HEALTH SCIENCES SYSTEM HOSPITAL DASHBOARD January 19, 2017 UI Health Metrics FY17 Q1 Actual FY17 Q1 Target FY Q1 Actual Ist Quarter % change FY17 vs FY Discharges 4,836
UNIVERSITY OF ILLINOIS HOSPITAL & HEALTH SCIENCES SYSTEM HOSPITAL DASHBOARD January 19, 2017 UI Health Metrics FY17 Q1 Actual FY17 Q1 Target FY Q1 Actual Ist Quarter % change FY17 vs FY Discharges 4,836
School Based Health Services Medicaid Policy Manual MODULE 4 PSYCHOLOGICAL SERVICES
 School Based Health Services Medicaid Policy Manual MODULE 4 PSYCHOLOGICAL SERVICES BACKGROUND Administrative Requirements SCHOOL BASED HEALTH SERVICES ARE REGULATED BY THE CENTERS OF MEDICAID AND MEDICARE
School Based Health Services Medicaid Policy Manual MODULE 4 PSYCHOLOGICAL SERVICES BACKGROUND Administrative Requirements SCHOOL BASED HEALTH SERVICES ARE REGULATED BY THE CENTERS OF MEDICAID AND MEDICARE
Ages Ages 3 through 64.
 Medicaid: Follow-Up After Discharge from Community Hospitals, State Psychiatric Hospitals, and Facility Based Crisis Services for Mental Health Treatment The percentage of discharges for individuals ages
Medicaid: Follow-Up After Discharge from Community Hospitals, State Psychiatric Hospitals, and Facility Based Crisis Services for Mental Health Treatment The percentage of discharges for individuals ages
BSUH INTEGRATED PERFORMANCE REPORT. 1) Responsive Domain 2) Safe Domain 3) Effective Domain 4) Caring Domain 5) Well Led Domain
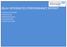 BSUH INTEGRATED PERFORMANCE REPORT 1) Responsive Domain 2) Safe Domain 3) Effective Domain 4) Caring Domain 5) Well ed Domain RESPONSIVE DOMAIN RESPONSIVE DOMAIN Metric Defined by Standard Apr-16 May-16
BSUH INTEGRATED PERFORMANCE REPORT 1) Responsive Domain 2) Safe Domain 3) Effective Domain 4) Caring Domain 5) Well ed Domain RESPONSIVE DOMAIN RESPONSIVE DOMAIN Metric Defined by Standard Apr-16 May-16
Acute Crisis Units. Shelly Rhodes, Provider Relations Manager
 Acute Crisis Units Shelly Rhodes, Provider Relations Manager Shelly.Rhodes@beaconhealthoptions.com Training Agenda Agenda: Transition and Certification Coverage of Services Service Code Definition Documentation
Acute Crisis Units Shelly Rhodes, Provider Relations Manager Shelly.Rhodes@beaconhealthoptions.com Training Agenda Agenda: Transition and Certification Coverage of Services Service Code Definition Documentation
Interactive Voice Registration (IVR) System Manual WASHINGTON STREET, SUITE 310 BOSTON, MA (800)
 Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 (800) 495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 (800) 495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
1. SMHS Section of CCR Title 9 (Division 1, Chapter 11): this is the regulation created by the California Department of Health Care Services (DHCS).
 Clinical Documentation Tool This tool compares the definitions of outpatient Specialty Mental Health s (SMHS) that appear in two different sources: 1. SMHS Section of CCR Title 9 (Division 1, Chapter 11):
Clinical Documentation Tool This tool compares the definitions of outpatient Specialty Mental Health s (SMHS) that appear in two different sources: 1. SMHS Section of CCR Title 9 (Division 1, Chapter 11):
CMS has finalized its proposal to eliminate Medicare payment for consultations and use the money from
 Consultation Services and Transfer of Care CMS has finalized its proposal to eliminate Medicare payment for consultations and use the money from these services to increase payments for visits, including
Consultation Services and Transfer of Care CMS has finalized its proposal to eliminate Medicare payment for consultations and use the money from these services to increase payments for visits, including
EHR Report Implementation Training September 26, 2016
 EHR Report Implementation Training September 26, 2016 The McSilver Institute for Poverty Policy and Research at New York University Silver School of Social Work is committed to creating new knowledge about
EHR Report Implementation Training September 26, 2016 The McSilver Institute for Poverty Policy and Research at New York University Silver School of Social Work is committed to creating new knowledge about
302: Achieving Cost Management in Home Health
 Introductory announcements: This provider-directed continuing nursing education activity was approved by the Maryland Nurses Association (MNA) to award contact hours. The MNA is accredited as an approver
Introductory announcements: This provider-directed continuing nursing education activity was approved by the Maryland Nurses Association (MNA) to award contact hours. The MNA is accredited as an approver
paymentbasics The IPPS payment rates are intended to cover the costs that reasonably efficient providers would incur in furnishing highquality
 Hospital ACUTE inpatient services system basics Revised: October 2015 This document does not reflect proposed legislation or regulatory actions. 425 I Street, NW Suite 701 Washington, DC 20001 ph: 202-220-3700
Hospital ACUTE inpatient services system basics Revised: October 2015 This document does not reflect proposed legislation or regulatory actions. 425 I Street, NW Suite 701 Washington, DC 20001 ph: 202-220-3700
Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM
 Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM Plan Year: July 2010 June 2011 Background The Harvard Pilgrim Independence Plan was developed in 2006 for the Commonwealth of Massachusetts
Frequently Asked Questions (FAQ) The Harvard Pilgrim Independence Plan SM Plan Year: July 2010 June 2011 Background The Harvard Pilgrim Independence Plan was developed in 2006 for the Commonwealth of Massachusetts
Departments to Improve. February Chad Faiella RN, Terri Martin RN. 1 Process Excellence
 Coordination of Multiple Departments to Improve ED Throughput February 2011 Chad Faiella RN, Terri Martin RN 1 Agenda OhioHealth information Grant Medical Center facts Bed assignment process Key takeaways
Coordination of Multiple Departments to Improve ED Throughput February 2011 Chad Faiella RN, Terri Martin RN 1 Agenda OhioHealth information Grant Medical Center facts Bed assignment process Key takeaways
PEDIATRIC PRIMARY CARE and BEHAVIORAL HEALTH INTEGRATION
 PEDIATRIC PRIMARY CARE and BEHAVIORAL HEALTH INTEGRATION AN OASIS IN THE FUTURE James N Bowen DO Chief Medical Officer The Guidance Center Flagstaff, AZ. WHAT WE WILL DISCUSS Why? What? How? When? WHY
PEDIATRIC PRIMARY CARE and BEHAVIORAL HEALTH INTEGRATION AN OASIS IN THE FUTURE James N Bowen DO Chief Medical Officer The Guidance Center Flagstaff, AZ. WHAT WE WILL DISCUSS Why? What? How? When? WHY
Ohio Medicaid Overview
 Ohio Medicaid Overview May 2014 John McCarthy Ohio Medicaid Director Medicaid Overview Medicaid is Ohio s largest health payer 83,000 active providers, hospitals, nursing homes and other providers care
Ohio Medicaid Overview May 2014 John McCarthy Ohio Medicaid Director Medicaid Overview Medicaid is Ohio s largest health payer 83,000 active providers, hospitals, nursing homes and other providers care
Coding and Reimbursement Tip Sheet for Transition from Pediatric to Adult Health Care
 P R A C T I C E R E S O U R C E A P R I L 2015 NO.2 Coding and Reimbursement Tip Sheet for Transition from Pediatric to Adult Health Care By Margaret McManus, MHS The National Alliance to Advance Adolescent
P R A C T I C E R E S O U R C E A P R I L 2015 NO.2 Coding and Reimbursement Tip Sheet for Transition from Pediatric to Adult Health Care By Margaret McManus, MHS The National Alliance to Advance Adolescent
A McKesson Perspective: ICD-10-CM/PCS
 A McKesson Perspective: ICD-10-CM/PCS Its Far-Reaching Effect on the Healthcare Industry Executive Overview While many healthcare organizations are focused on qualifying for American Recovery & Reinvestment
A McKesson Perspective: ICD-10-CM/PCS Its Far-Reaching Effect on the Healthcare Industry Executive Overview While many healthcare organizations are focused on qualifying for American Recovery & Reinvestment
HCBS: Getting Started with Implementation
 HCBS: Getting Started with Implementation Presentation to ACL members by Cindy Freidmutter, CLF Consulting August 4 & 5, 2016 HCBS Presentation Agenda HCBS Framework How HCBS Works HCBS Start-up Challenges
HCBS: Getting Started with Implementation Presentation to ACL members by Cindy Freidmutter, CLF Consulting August 4 & 5, 2016 HCBS Presentation Agenda HCBS Framework How HCBS Works HCBS Start-up Challenges
Peach State Health Plan Covered Services & Authorization Guidelines Programs for Behavioral Health
 Peach State Health Plan Covered s & Guidelines Programs for Health n-participating providers (those that are not contracted and credentialed with Peach State Health Plan) require prior authorization for
Peach State Health Plan Covered s & Guidelines Programs for Health n-participating providers (those that are not contracted and credentialed with Peach State Health Plan) require prior authorization for
Mental Health Updates. Presented by EDS Provider Field Consultants
 Mental Health Updates Presented by EDS Provider Field Consultants October 2007 Agenda Session Objectives Outpatient Mental Health Medicaid Rehabilitation Option (MRO) Somatic Treatment Assertive Community
Mental Health Updates Presented by EDS Provider Field Consultants October 2007 Agenda Session Objectives Outpatient Mental Health Medicaid Rehabilitation Option (MRO) Somatic Treatment Assertive Community
All ten digits are required when filing a claim.
 34 34 Psychologists Licensed psychologists are enrolled only for services provided to QMB recipients or to recipients under the age of 21 referred as a result of an EPSDT screening. The policy provisions
34 34 Psychologists Licensed psychologists are enrolled only for services provided to QMB recipients or to recipients under the age of 21 referred as a result of an EPSDT screening. The policy provisions
Florida Medicaid. Statewide Inpatient Psychiatric Program Coverage Policy
 Florida Medicaid Statewide Inpatient Psychiatric Program Coverage Policy Agency for Health Care Administration December 2015 Table of Contents 1.0 Introduction... 1 1.1 Description... 1 1.2 Legal Authority...
Florida Medicaid Statewide Inpatient Psychiatric Program Coverage Policy Agency for Health Care Administration December 2015 Table of Contents 1.0 Introduction... 1 1.1 Description... 1 1.2 Legal Authority...
Telemedicine and Health Reform. Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center
 Telemedicine and Health Reform Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center 1 telehealthresourcecenters.org Links to all TRCs National Webinar Series Reimbursement,
Telemedicine and Health Reform Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center 1 telehealthresourcecenters.org Links to all TRCs National Webinar Series Reimbursement,
MEDICAL ASSISTANCE BULLETIN
 MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER September 8, 1995 September 8, 1995 1153-95-01 SUBJECT Accessing Outpatient Wraparound
MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER September 8, 1995 September 8, 1995 1153-95-01 SUBJECT Accessing Outpatient Wraparound
Florida Medicaid. Community Behavioral Health Services Coverage and Limitations Handbook. Agency for Health Care Administration
 Florida Medicaid Community Behavioral Health Services Coverage and Limitations Handbook Agency for Health Care Administration UPDATE LOG COMMUNITY BEHAVIORAL HEALTH SERVICES COVERAGE AND LIMITATIONS HANDBOOK
Florida Medicaid Community Behavioral Health Services Coverage and Limitations Handbook Agency for Health Care Administration UPDATE LOG COMMUNITY BEHAVIORAL HEALTH SERVICES COVERAGE AND LIMITATIONS HANDBOOK
DC Medicaid EAPG Training
 DC Medicaid EAPG Training Provider Training 2013 Xerox Corporation. All rights reserved. Xerox and Xerox Design are trademarks of Xerox Corporation in the United States and/or other countries. Agenda Project
DC Medicaid EAPG Training Provider Training 2013 Xerox Corporation. All rights reserved. Xerox and Xerox Design are trademarks of Xerox Corporation in the United States and/or other countries. Agenda Project
601-Audit Plan for Medicare s Shared Visit Rule
 601-Audit Plan for Medicare s Shared Visit Rule Elin Baklid-Kunz, MBA, CPC, CCS Health Care Compliance Association 6500 Barrie Road, Suite 250, Minneapolis, MN 55435 888-580-8373 www.hcca-info.org Presentation
601-Audit Plan for Medicare s Shared Visit Rule Elin Baklid-Kunz, MBA, CPC, CCS Health Care Compliance Association 6500 Barrie Road, Suite 250, Minneapolis, MN 55435 888-580-8373 www.hcca-info.org Presentation
Behavioral Health Outpatient Authorization Request Self Service. User Guide
 Behavioral Health Self Behavioral Health Outpatient Authorization Request Self Service User Guide Introduction Tufts Health Plan Network Health has created this user guide to illustrate how to navigate
Behavioral Health Self Behavioral Health Outpatient Authorization Request Self Service User Guide Introduction Tufts Health Plan Network Health has created this user guide to illustrate how to navigate
Coding, Corroboration, and Compliance How to assure the 3 C s are met
 Coding, Corroboration, and Compliance How to assure the 3 C s are met Sue Roehl, RHIT, CCS sroehl@eidebailly.com 701-476-8770 OIG 1996 - $23.2 Billion errors Figure 1 Insufficient/No documentation 46.76%
Coding, Corroboration, and Compliance How to assure the 3 C s are met Sue Roehl, RHIT, CCS sroehl@eidebailly.com 701-476-8770 OIG 1996 - $23.2 Billion errors Figure 1 Insufficient/No documentation 46.76%
Estimated Decrease in Expenditure by Service Category
 Public Notice for June 2009 Release PUBLIC NOTICE COLORADO MEDICAID Department of Health Care Policy and Financing Fee-for-Service Provider Payments Effective July 1, 2009, in an effort to reduce expenditures
Public Notice for June 2009 Release PUBLIC NOTICE COLORADO MEDICAID Department of Health Care Policy and Financing Fee-for-Service Provider Payments Effective July 1, 2009, in an effort to reduce expenditures
Children & Adults. Children & Adolescents 8A-2. Children & Adults. Children & Adults
 Medicaid MH/SA/IDD Acute Utilization Review Guidelines Authorization Guidelines: LOCUS/CALOCUS Level Ambulatory Deto Code H0014 Criterion V 902 SAR Facility Based Crisis S9484 SAR, w/ Order SAR required
Medicaid MH/SA/IDD Acute Utilization Review Guidelines Authorization Guidelines: LOCUS/CALOCUS Level Ambulatory Deto Code H0014 Criterion V 902 SAR Facility Based Crisis S9484 SAR, w/ Order SAR required
Medication Reconciliation
 Medication Reconciliation The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart Technologies Today
Medication Reconciliation The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart Technologies Today
Behavioral Health Providers: The Key Element of Value Based Payment Success
 Behavioral Health Providers: The Key Element of Value Based Payment Success December 6, 2017 Presented by: Andrew Cleek, Psy.D. Meaghan Baier, LMSW Goals of the Presentation Understand the intersect between
Behavioral Health Providers: The Key Element of Value Based Payment Success December 6, 2017 Presented by: Andrew Cleek, Psy.D. Meaghan Baier, LMSW Goals of the Presentation Understand the intersect between
Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid
 Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid Information posted on October 8, 2010 Effective for dates of service on or after December 1, 2010, the benefit criteria
Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid Information posted on October 8, 2010 Effective for dates of service on or after December 1, 2010, the benefit criteria
Behavioral health provider overview
 Behavioral health provider overview KSPEC-1890-18 February 2018 Agenda Provider manual and provider website Behavioral Health (BH) program goals Access and availability standards Care coordination and
Behavioral health provider overview KSPEC-1890-18 February 2018 Agenda Provider manual and provider website Behavioral Health (BH) program goals Access and availability standards Care coordination and
