Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres: Challenges and Success Factors
|
|
|
- Chad Marsh
- 5 years ago
- Views:
Transcription
1 Implementing Safety Solutions Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres: Challenges and Success Factors Maitreya Coffey, Patricia Cornish, Tessie Koonthanam, Edward Etchells and Anne Matlow Abstract Admission Medication Reconciliation (Med Rec) is an organizational practice designed to ensure patients pre-admission medications are ordered correctly upon hospital admission. We describe the implementation of admission Med Rec at two academic health sciences centres, each having designed distinctly different processes. Common challenges encountered included the multistep, inter-professional nature of Med Rec, staffing resource and workload concerns and frequent medical staff turnover in a teaching environment. Both teams found that participation in a national safety collaborative enabled the pilot initially; however, they later found the outcome measures suggested by the collaborative less useful and switched to internal compliance measures for establishing maintenance and spread. Common themes were identified among the critical success factors, with unique variations at each centre. Both teams acknowledged accreditation standards to be a major accelerator of implementation and spread. Using different measures of implementation success at each centre, the majority of patient admissions on the pilot units are complying with admission Med Rec. However, very high levels of compliance remain elusive. At Sunnybrook Health Sciences Centre s pilot unit, 62 77% of patients are being screened by a pharmacist and 65 75% of high-risk patients identified are undergoing Med Rec by a pharmacist. At The Hospital for Sick Children s pilot unit, 72 88% of patients have a physician s primary medication history documented on a Med Rec form and 57 73% of patients are also undergoing Med Rec by a nurse or pharmacist. Background Up to one quarter of adverse events in healthcare are related to medications (Baker et al. 2004; Leape et al. 1991). Approximately 25% of all medication-related injuries are due to medication errors and are thus considered preventable (Aspden et al. 2007). Recently, the process of admission to hospital has emerged as a key area of vulnerability as up to one half of patients have been found to have at least one error in their hospital admission medication histories (Tam et al. 2005), with a substantial 102 Healthcare Quarterly Vol.12 Special Issue 2009
2 Maitreya Coffey et al. Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres portion of these errors having the potential to cause adverse events (Cornish et al. 2005). Medication Reconciliation (Med Rec) at admission is a process whereby the final selection of medications ordered on admission takes all pre-admission medications into account. An accurate list of a patient s current home medications (best possible medication history [BPMH]) is obtained by an interview, a review of medication vials or the patient s personal medication list; contacting the patient s community pharmacy or physician; or reviewing prescription drug database information. The BPMH is compared with the hospital admission medication orders, and any discrepancies between the two are brought to the attention of the prescriber; if appropriate, changes are made to the orders (Rozich and Resar 2001). Evidence supports the assertion that pharmacists provide the gold standard when compiling the BPMH (Cornish et al. 2005; Tam et al. 2005). When the BPMH is compared with the admission medication orders, two types of discrepancies may be found. If a prescriber has made an intentional change but not documented it, this is referred to as an undocumented intentional discrepancy. While not an error, this suboptimal documentation could lead to errors at transfer or discharge. The other type, a true error, is called an unintentional discrepancy. When performing Med Rec, it is essential that the providers involved in the process communicate directly to identify and resolve discrepancies. Because Med Rec has dramatically reduced discrepancy rates in various settings (Pronovost et al. 2003; Rozich et al. 2004; Whittington and Cohen 2004), it has been endorsed by leading international patient safety organizations (Institute for Healthcare Improvement 2005; Institute for Safe Medication Practices 2005). Both the Institute for Healthcare Improvement in the United States and the Canadian Patient Safety Institute ( included Med Rec in their 100,000 Lives and Safer Healthcare Now! ( campaigns, respectively. Further attesting to its importance, Med Rec has been designated a required organizational practice by Accreditation Canada (2008) and the Joint Commission in the United States ( One admission Med Rec strategy is to have a clinical pharmacists obtain a BPMH on every admitted patient. Unfortunately, many units to do not have clinical pharmacists, while other units have clinical pharmacists who cannot possibly assess every patient given existing staffing levels and competing duties. Also, it is difficult to justify the broad deployment of clinical pharmacists to obtain BPMHs given that there is insufficient evidence to justify the routine application of Med Rec for all patients in all in-patient settings. Clinical pharmacist assessment can only be justified when the rate of clinically significant unintentional discrepancies is high. Other reasonable implementation strategies include the following: 1. Develop and implement screening criteria. Patients identified as high risk for unintentional discrepancies are seen by a clinical pharmacist for a BPMH. 2. Train additional clinical staff to obtain a BPMH. 3. Focus reconciliation efforts on comparing the primary medication history to medication orders. For example, the unit nurse could compare the admission medication history to the admission medication orders and identify discrepancies. This strategy would detect undocumented intentional discrepancies but would be less likely to detect unintentional discrepancies because no new information would be obtained from the patient. Therefore, any errors in the primary medication history would be unlikely to be corrected. Therefore, its impact on patient safety might be less. We will not discuss the third option further, but we have observed that many organizations have chosen this approach, and we believe that the potential impact on patient safety is lower. Table 1 lists the relative strengths and weaknesses of these approaches as well as the potential process measures of implementation success. We describe the implementation of admission Med Rec at two academic health sciences centres, each having designed distinctly different processes. The objectives of this study were (1) to describe admission Med Rec strategies at two academic health sciences centres, (2) to discuss common challenges and success factors and (3) to analyze different measures of implementation success. Implementation Setting and Teams Both centres are urban, university-affiliated tertiary care hospitals. Sunnybrook Health Sciences Centre has 649 adult beds, including 94 beds on the general internal medicine unit. The Hospital for Sick Children (SickKids) has 376 pediatric beds, with 60 beds on the pediatric medicine unit. Both units participated in Med Rec pilots as part of Safer Healthcare Now! Participation was voluntary and grew out of grassroots interest in medication safety. At Sunnybrook, members of the general internal medicine team had conducted audits and formal research examining admission medication discrepancies prior to the campaign. At SickKids, a number of pediatric medicine morbidity and mortality reviews involving serious medication errors had stimulated interest in the topic. Inter-professional teams were formed that included physicians, pharmacists and hospital quality and safety professionals (as well as nurses at SickKids). A generalist/hospitalist with active clinical involvement and professional interest in patient safety became the physician lead at both sites. Sunnybrook s patient safety pharmacist served as the team s pilot project manager, whereas the pilot project manager at SickKids was a Healthcare Quarterly Vol.12 Special Issue
3 Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres Maitreya Coffey et al. Table 1. Comparison of Med Rec process strategies Strategy Strengths Weaknesses Potential Measures of Implementation Pharmacist obtains BPMH and resolves discrepancies for all patients Gold standard, supported by evidence Correct medication list obtained early in admission Requires little training resources, pharmacist already skilled Pharmacist resources rarely allow for this May leave gap in Med Rec process for evenings and weekends Could compromise pharmacist s ability to perform other relevant medication safety activities Percentage of patients assessed by a pharmacists (out of total admissions) Pharmacist obtains BPMH and resolves discrepancies for selected high-risk patients Focuses application of scarce resources on highest-risk group/most likely to benefit Requires development of screening criteria, determination of who is responsible for screening and a process for doing so Percentage of patients screened (out of total admissions) Percentage with a documented pharmacist BPMH (out of those identified as high risk) Other clinical staff (e.g., nurses) obtains BPMH and resolves discrepancies Provider with most proximity to patient bedside is involved 24/7 coverage Not known how a nurse-obtained BPMH compares with gold standard of a pharmacist-obtained BPMH Extensive resources required to educate nursing staff Continued struggle with compliance (not perceived as part of nursing practice) Percentage of patients with a documented BPMH (out of total admissions) Other clinical staff (e.g., nurses) compare primary history to admission medication orders and resolve discrepancies Provider with most proximity to patient bedside is involved 24/7 coverage Potentially simple to implement BPMH not systematically obtained (no additional information from standard physician history); thus, less likely to identify unintentional discrepancies Percentage of patients undergoing comparison (out of total admissions) BPMH = best possible medication history; Med Rec = Medication Reconciliation. quality analyst with a nursing background. Initial Approach Both teams began by introducing a Med Rec form to improve the completeness and documentation of the physician s primary medication history. Though neither team expected the form to improve the accuracy of the history, it was hoped that having physicians enter the primary medication history on the form would reduce undocumented intentional discrepancies by prompting them to indicate continue, stop or change for each medication. It was assumed that this would make it easier for a second provider to compile the BPMH and correct any unintentional discrepancies. Prior to the pilot studies, pharmacists had established clinical roles in both centres and performed BPMHs or checked admission medication orders on an ad hoc basis, either at the request of a physician or through informal screening. A prior study at Sunnybrook had shown that this ad hoc system was not working well as it resulted in over half of patients having at least one unintentional discrepancy (Cornish et al. 2005). Though both teams recognized that pharmacists could provide the gold standard of Med Rec, neither site had adequate pharmacist resources to provide this service for every admission, nor did they believe a pharmacist s expertise was required for every patient. Thus, both teams devised a screening process to identify high-risk patients for the purposes of an independent BPMH creation and reconciliation by a pharmacist. Sunnybrook had found a high rate of discrepancies for patients on four or more prescription medications (Cornish et al. 2005). This cut-off, as well as the presence of a high-alert medication or an unclear history, was used to define the highrisk patient population. In the adult population at Sunnybrook, approximately three quarters of patients meet this definition of high risk, whereas in the pediatric population at SickKids, only one quarter meets this definition (one half do if over-thecounter medications and supplements are included). 104 Healthcare Quarterly Vol.12 Special Issue 2009
4 Maitreya Coffey et al. Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres Early Challenges and Ongoing Implementation Initially, physician leaders of both teams were present at the beginning of each academic rotation to orient every team to the Med Rec form. Within months, it became clear that this approach would be impossible to sustain in light of the constant turnover of both faculty and trainees. Furthermore, even when physicians agreed with Med Rec in principle, it was extremely difficult to get them to perform it in practice. Reasons included the perception that the form was extra work, difficulty finding the form and not remembering to look for the form. Both teams stocked admission packages, including the Med Rec form, with other essential paperwork in the emergency department (ED), but forms still ended up missing from the chart or being left blank. The teams could not convince physicians to write the medication list on the form instead of in the body of the admission history and physical as was their usual practice, so many physicians were duplicating the history. The involvement of clinical pharmacists was achieved with far less effort. This is likely because a less-structured version of Med Rec was already part of their practice. Since they felt they did not have the capacity to perform Med Rec for every patient and that their skills were not required for every patient, they supported screening for high-risk patients. In response to the challenge of physician turnover, both centres began to focus on permanent clinical staff. At Sunnybrook, one pharmacist fulltime equivalent was added to increase the complement to five clinical pharmacists on the medical wards, in addition to an ED pharmacist. Pharmacists were encouraged to initiate Med Rec as early in the admission process as was feasible. This could mean obtaining a BPMH in the ED prior to the physician s history and orders. Thus, the initiation of the process was no longer entirely physician dependent, allowing significant gains in Med Rec compliance without dependence on intensive re-education with each rotation. In contrast, SickKids remained committed to holding physicians accountable for use of the form. Available pharmacist resources allowed them to reconcile only a minority of patients, which led to the decision to involve nurses in the process. Over three months, the unit s entire nursing staff were trained to perform a BPMH and reconciliation, with the expectation that they would complete it for every admission and involve pharmacists only with patients on four or more medications. SickKids was simultaneously conducting a study in which virtually no clinically significant discrepancies were found in patients on less than four medications, supporting this approach. However, the absence of clinically important discrepancies in the low-risk group raised the question of whether any additional staff resources, including nursing, should be applied to this group (Coffey et al. 2008). Advantages and disadvantages of these approaches are outlined in Table 1. Evaluation Both centres established a baseline rate of discrepancies. Sunnybrook used data from their previous study, showing an average of one unintentional discrepancy per patient. SickKids pre-pilot data showed 1.5 unintentional discrepancies per Table 2. Sunnybrook Med Rec data collection summary* May 20 Jun 18, 2007 Sep 17 Oct 5, 2007 Jan 7 25, 2008 Total number of admissions to general medicine Patients screened by in-patient pharmacist 152 (62%) 118 (73%) 127 (77%) Medication history form on chart prior to pharmacist review 25 (16%) 25 (21%) 24 (19%) Patients with 1 high-risk criteria Medication history verified by pharmacist Medication history not verified by pharmacist and reason documented Medication history not verified by pharmacist and reason not documented 106 (70%) 74 (70%) 12 (11%) 20 (19%) 77 (57%) 50 (65%) 14 (18%) 13 (17%) 86 (68%) 63 (75%) 9 (11%) 14 (17%) Patients with 1 discrepancy 86 (57%) 60 (51%) 58 (46%) Mean number of discrepancies per patient (range) 1.5 ± 1.6 (0 7) 1.1 ± 1.5 (0 6) 1.0 ± 1.4 (0 7) Total number of discrepancies identified Med Rec = Medication Reconciliation. *Note these data are from the study midpoint after several months of implementation work and after pharmacy staffing increases (no performance data prior to this are available). Includes 12 patients admitted on the weekend and discharged within 72 hours (i.e., no opportunity for pharmacist to review). Includes14 patients admitted on the weekend and discharged within 72 hours (i.e., no opportunity for pharmacist to review). Healthcare Quarterly Vol.12 Special Issue
5 Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres Maitreya Coffey et al. patient. As participants in Safer Healthcare Now! both centres were encouraged to submit rates of unintentional discrepancies on a sample of 20 charts per month. The teams did not expect a change in the rate of unintentional discrepancies between the primary (physician) history and the admission medication orders over time because neither team focused on changing the primary medication history process. These discrepancies were expected to remain relatively constant as they reflect patient complexity and physician habits and skills related to compiling a primary medication history. Rather, the success of the program was to be measured by the number of patients receiving Med Rec, which would resolve unintentional discrepancies that would not otherwise have been identified. Sunnybrook performed three one-month audits of consecutive admissions capturing these measures (Table 2). After the January 2008 audit, a pharmacist and a physician reviewed all the unintentional discrepancies and estimated that 50% had the potential to cause patient harm had they not been identified and corrected by the Med Rec program (data not shown). SickKids approach to measuring Med Rec implementation success began by monitoring physician compliance with using the Med Rec form (Figure 1). Monthly audits of 30 randomly selected charts were reviewed. Compliance was highly variable (30 80%) over the first nine months, depending on the medical team s interest and the availability of the physician leader. In January 2007, the second step of a nurse-obtained BPMH and reconciliation was introduced. During the first two months, extensive resources were dedicated to a comprehensive educational campaign and frequent compliance spot checks. Fearing a loss of educational momentum, the team advised nurses to proceed with the BPMH even when physicians had not initiated the Med Rec form. This resulted in a precipitous drop in physician compliance, possibly due to physicians leaving the task for the nurses. This problem was compounded by the physician leader s leave of absence followed by a period without project management support, which illustrates the pitfall of making a process too dependent on a particular individual. In summer 2008, nurses were again advised not to proceed Figure 1. Pilot unit physician compliance at The Hospital for Sick Children BASELINE Jan 07 Feb 07 Mar 07 Apr 07 May 07 June 07 July 07 Aug 07 Sep 07 Oct 07 Nov 07 Dec 07 Jan 08 Feb 08 Mar 08 Apr 08 May 08 June 08 July 08 Aug 08 Sept 08 Oct 08 Nov 08 Dec 08 Jan 08 Feb 09 % of patients with physician step completed on Med Rec form Figure 2. Pilot unit overall compliance at The Hospital for Sick Children % of patients with physician and nursing steps completed on Med Rec form BASELINE Jan 07 Feb 07 Mar 07 Apr 07 May 07 June 07 July 07 Aug 07 Sep 07 Oct 07 Nov 07 Dec 07 Jan 08 Feb 08 Mar 08 Apr 08 May 08 June 08 July 08 Aug 08 Sept 08 Oct 08 Nov 08 Dec 08 Jan 08 Feb Healthcare Quarterly Vol.12 Special Issue 2009
6 Maitreya Coffey et al. Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres with Med Rec unless the physician initiated the form, and the physician leader and a resident champion relaunched their educational efforts. A scaling-up of project management support allowed weekly audits capturing every admission. Since the fall of 2008, audits of physician-specific compliance have been reported to the physicians, their division head and the executive sponsor. As of January 2009, despite achieving acceptable physician compliance, nursing compliance remains a challenge; so, overall compliance with both steps of Med Rec is currently around 40 60% (Figure 2). Pharmacist performance is not being audited, but spot checks show that they are consistently reconciling approximately 20% of patients, including almost all high-risk patients. Challenges, Successes and Lessons Learned Challenges to both centres implementing admission Med Rec included the following: Physicians perceive little value in documenting a medication history on a separate form and are not disposed to abandon the practice of documenting the medication list within the admission history and physical. The constant turnover of trainee and staff physicians makes it extremely difficult to educate and convince each new physician to adopt Med Rec processes. Workload concerns remain a substantial challenge. In spite of Sunnybrook s increased clinical pharmacist resources, pharmacists are available to do Med Rec only during regular business hours, resulting in the screening of approximately 75% of general medical patients and the reconciliation of about 80% of high-risk patients identified. At SickKids, extensive resources continue to be required for maintaining nursing Med Rec compliance, and Med Rec often competes poorly with other nursing tasks. Data collection and management are burdensome. Specifically, the ongoing auditing necessary to achieve current levels of performance is labour intensive and not a long-term solution. Success factors and variations at each centre are listed in Table 3. Both teams found that their participation in Safer Healthcare Now! assisted the initial launch by providing methodology for data collection, credibility and branding, as well as a forum for discussion with colleagues regionally and nationally. Once the Med Rec process was established, however, both teams turned to process measures to evaluate the proportion of patients undergoing Med Rec. The designation of Med Rec as a Required Organizational Practice by Accreditation Canada was a significant accelerator. At SickKids, for example, a full-time project manager was secured and Med Rec was declared a key corporate performance objective. Hospital-Wide Spread Both teams noted distinct uptake patterns in different clinical areas as the process was spread. At SickKids, cardiology had a high degree of concern for medication risks, an engaged physician leader and a supportive management culture, which led to immediate high levels of Med Rec compliance (Figure 3). On the other hand, more challenges were encountered in the surgical areas, where different admission processes (i.e., pre-admission clinics) and a general discomfort with medication management were unanticipated barriers. With a better understanding of workflow in surgery and a redesign from the initial pilot, compliance is slowly improving. Sunnybrook achieved excellent compliance when a pre-admission Med Rec form was completed by nurses in the preoperative clinic, and surgical residents informally reported a high degree of satisfaction when referring to these forms to create post-operative orders. Both hospitals are considering introducing a clinical pharmacist role in the preoperative clinic setting. At Sunnybrook long-term care, with stable staff and fewer new admissions, pharmacist-initiated Med Rec has been fully implemented with a high degree of reliability. Lessons learned from preliminary spread results include the following: Unit-specific processes taking into account current workflow, staffing resources and patient risk profiles are critical, even within a single institution. Shared accountability must include clarity with respect to which team members are accountable for which steps. A physician champion who is visible and directly involved with the admission process is key in each clinical area. Conclusions: The Future of Med Rec Transfer, Discharge and Beyond Though most centres have started with a focus on Med Rec at admission, it is also required at transfer and discharge. While this might seem to entail a simple extension of the admission process, there will be significant logistical hurdles to overcome in determining how the original BPMH will be combined with current in-patient medications, how prescriber intent will be documented and how repeated recopying of lists will be avoided. Furthermore, although Med Rec emerged with a focus on in-patient care, medication lists are frequently updated in the ambulatory setting. The fact that medication information is housed in so many different, often inaccessible locations cries out for the creation of federal or provincial repositories of prescription information independent of payment source or physical location. This is relevant to the larger discussion regarding the need for integrated electronic health records. Patient and family involvement is another area for future exploration. Some advocate for patient-held medication lists, which would allow patients and families to have up-to-date informa- Healthcare Quarterly Vol.12 Special Issue
7 Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres Maitreya Coffey et al. Table 3. Centre-specific Med Rec success factors Critical Success Factor Sunnybrook Health Sciences Centre Hospital for Sick Children Executive support Pilot unit physician champions Strong support from director of pharmacy regarding staffing increases Hospital patient safety leader and active clinician with academic expertise in medication safety Physician vice-president of quality and chief nursing executive key in moving physician and nursing roles forward Divisional quality leader and active clinician with improvement expertise, and resident project champion Investments in personnel resources Permanent increase in pharmacist FTE Project management support for pilot, one-year full FTE for hospital-wide spread Front-line physician communication Redundancy/mutual accountability Acceptance of a risk-based approach to providing the gold standard Morning rounds, staff meetings, resident lectures Physicians and pharmacists work together to resolve discrepancies, either can initiate Pharmacists perform all screening and are reconciling a majority of patients Morbidity and mortality reviews, staff meetings, resident lectures Physicians and nurses are mutually accountable for performing steps in a specific order Pharmacists reconcile 20 30% of patients (almost all the high-risk patients) Local data used to drive change Three audits over 8 months Monthly audits over first year, weekly over second year Individual staff feedback Clinical pharmacists participate in all audits >80% physician compliance after individual audit/feedback with group reporting commenced FTE = full-time equivalent; Med Rec = Medication Reconciliation. Figure 3. Initial compliance in clinical areas at The Hospital for Sick Children 100% 80% 60% 40% 20% 0% Cardiology Month 1 Surgery Month 2 Month 3 tion for their use and to share with health providers. Universal or Risk-Based Med Rec? The cases here illustrate two possible approaches to Med Rec. The universal approach is for every patient at every admission, as is currently required by accreditation bodies. A benefit is that it places pressure on health systems and organizations to invest in applications to facilitate the accessibility of accurate medication information throughout the continuum of care. A disadvantage is that it promotes the widespread dissemination of practices that may fulfill the appearance of compliance without truly improving medication safety. The risk-based approach involves applying enhanced resources to higher-risk populations. This is better supported by medical evidence and may represent the best investment in terms of avoiding adverse events. The challenge, however, is that the vast array of risk profiles for different populations makes it difficult to evaluate each setting against a common standard. Workload and Sustainability To ensure the sustainability and expansion of Med Rec, innovative solutions are needed to address the workload issues and inefficiencies in the process. Novel personnel arrangements should be explored, such as pharmacy students or technicians partnering with pharmacists to facilitate Med Rec. Information technology solutions for Med Rec that could be fully integrated 108 Healthcare Quarterly Vol.12 Special Issue 2009
8 Maitreya Coffey et al. Implementation of Admission Medication Reconciliation at Two Academic Health Sciences Centres with computerized physician order entry (CPOE) have the potential to create efficiencies. Although obtaining BPMHs at admission will always require an interaction with the patient or caregiver, once this information is collected, it could be entered into an electronic system that would help construct the admission medication orders through CPOE. Having the BPMH in an electronic format accessible through the CPOE system would further facilitate Med Rec at transfer and discharge, and increase information sharing across the clinical disciplines (Poon et al. 2006). Both institutions described are looking into electronic Med Rec applications; however, they acknowledge that starting with a paper and people approach has been an asset as an information technology solution can only facilitate, not replace, the complex cognitive and inter-professional aspects of high-quality Med Rec. Acknowledgments We would like to acknowledge the following people for their hard work and support during the Med Rec pilot implementation: Teresa Bishara, Sabrina Boodjan, Helene Carating, Sara Compani, Margot Follett-Rowe, Nancy Fritsch, Bev Hales, Alastair Hodinott, Margaret Keatings, Ron Laxer, Lynn Mack, Romina Marchesano, Rimona Natanson, Patrycja Nedzka, Polly Stevens, Kim Streitenberger, Chris Sulowski, Vince Teo, Jim Tjon and Lisa Zhu. In addition, we would like to thank Christina Stevancec for her assistance with manuscript preparation. References Accreditation Canada Required Organizational Practices. Ottawa, ON: Author. Retrieved September < ca/default.aspx?page=355&cat=30>. Aspden, P., J.A. Wolcott, J.L. Bootman and L.R. Cronenwett, eds Preventing Medication Errors. Washington, DC: Institute of Medicine of the National Academies Press. Baker, G.R., P.G. Norton, V. Flintoft, R. Blais, A. Brown, J. Cox, E. Etchells, W.A. Ghali, P. Hébert, S.R. Majumdar, M. O Beirne, L. Palacios-Derflingher, R.J. Reid, S. Sheps and R. Tamblyn The Canadian Adverse Events Study: The Incidence of Adverse Events among Hospital Patients in Canada. Canadian Medical Association Journal 170(11): Coffey, M., L. Mack, K. Streitenberger, T. Bishara, L. Defaveri and M. Matlow How Frequent and Clinically Significant are Medication Errors at Admission? [Abstract]. Paediatrics and Child Health 13: 46A. Cornish, P.L., S.R. Knowles, R. Marchesano, V. Tam, S. Shadowitz, D.N. Juurlink and E.E. Etchells Unintended Medication Discrepancies at the Time of Hospital Admission. Archives of Internal Medicine 165(4): Institute for Healthcare Improvement Prevention of Adverse Drug Events through Medication Reconciliation. Cambridge, MA: Author. Retrieved October 22, < AudioAndWebPrograms/WebandACTIONMedReconciliation.htm>. Institute for Safe Medication Practices Building a Case for Medication Reconciliation. Horsham, PA: Author. Retrieved September < articles/ asp>. Leape, L.L., T.A. Brennan, N. Laird, A.G. Lawthers, A.R. Localio, B.A. Barnes, L. Hebert, J.P. Newhouse, P.C. Weiler and H. Hiatt The Nature of Adverse Events in Hospitalized Patients. Results of the Harvard Medical Practice Study II. New England Journal of Medicine 324(6): Poon, E.G., B. Blumenfeld, C. Hamann, A. Turchin, E. Graydon-Baker, P.C. McCarthy, J. Poikonen, P. Mar, J.L. Schnipper, R.K. Hallisey, S. Smith, C. McCormack, M. Paterno, C.M. Coley, A. Karson, H.C. Chueh, C. Van Putten, S.G. Millar, M. Clapp, I. Bhan, G.S. Meyer, T.K. Gandhi and C.A. Broverman Design and Implementation of an Application and Associated Services to Support Interdisciplinary Medication Reconciliation Efforts at an Integrated Healthcare Delivery Network. Journal of the American Medical Informatics Association 13: Pronovost, P., B. Weast, M. Schwarz, R.M. Wyskiel, D. Prow, S.N. Milanovich, S. Berenholtz, T. Dorman and P. Lipsett P Medication Reconciliation: A Practical Tool to Reduce the Risk of Medication Errors. Journal of Critical Care 18(4): Rozich, J.D., R.J. Howard, J.M. Justeson, P.D. Macken, M.E. Lindsay and R.K. Resar Standardization as a Mechanism to Improve Safety in Health Care. Joint Commission Journal of Quality and Safety 30(1): Rozich, J.D. and R.K. Resar Medication Safety: One Organization s Approach to the Challenge. Journal of Clinical Outcomes and Management 8: Tam, V.C., S.R. Knowles, P.L. Cornish, N. Fine, R. Marchesano and E.E. Etchells Frequency, Type and Clinical Importance of Medication History Errors at Admission to Hospital: A Systematic Review. Canadian Medical Association Journal 173(5): Whittington, J. and H. Cohen OSF Healthcare s Journey in Patient Safety. Quality Management in Health Care 13(1): About the Authors Maitreya Coffey, MD, FAAP, FRCPC, is a pediatrician at The Hospital for Sick Children and an assistant professor of pediatrics in the Division of Paediatric Medicine at the University of Toronto. Patricia Cornish, BScPhm, is the pharmacist with the Patient Safety Service at Sunnybrook Health Sciences Centre, Toronto, ON. Tessie Koonthanam, RN, MN, is project manager for medication reconciliation at The Hospital for Sick Children, Toronto, ON. Edward Etchells, MD, MSc, is an internist in the Division of General Internal Medicine, director of the Patient Safety Service and researcher at the Centre for Health Services Sciences at Sunnybrook Health Sciences Centre, as well as an associate professor of medicine in the Department of Medicine at the University of Toronto. Anne Matlow, MD, FRCPC, is the medical director of patient safety at The Hospital for Sick Children and professor of pediatrics at the University of Toronto. Healthcare Quarterly Vol.12 Special Issue
Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting
 Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting Natalie McMurtry, BSc Pharm, Sr. Medication Consultant; Vanessa Moorgen,
Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting Natalie McMurtry, BSc Pharm, Sr. Medication Consultant; Vanessa Moorgen,
Who s s on What? Latest Experience with the Framework Challenges and Successes. November 29, Margaret Colquhoun Project Leader ISMP Canada
 Who s s on What? Latest Experience with the Framework Challenges and Successes November 29, 2005 Margaret Colquhoun Project Leader ISMP Canada 1 Outline ISMP Canada Partnership with SHN The Canadian Getting
Who s s on What? Latest Experience with the Framework Challenges and Successes November 29, 2005 Margaret Colquhoun Project Leader ISMP Canada 1 Outline ISMP Canada Partnership with SHN The Canadian Getting
Identifying Errors: A Case for Medication Reconciliation Technicians
 Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Who Cares About Medication Reconciliation? American Pharmacists Association American Society of Health-system Pharmacists The Joint Commission Agency
 The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
Medication Reconciliation as a Patient Safety Practice During Transitions of Care
 Medication Reconciliation as a Patient Safety Practice During Transitions of Care Janice L. Kwan, MD, MPH, FRCPC Division of General Internal Medicine Mount Sinai Hospital, University of Toronto Recorded
Medication Reconciliation as a Patient Safety Practice During Transitions of Care Janice L. Kwan, MD, MPH, FRCPC Division of General Internal Medicine Mount Sinai Hospital, University of Toronto Recorded
Medication Reconciliation: Using Pharmacy Technicians to Improve Care. Becky Johnson, CPhT Megan Ohrlund, PharmD Steve Finch, RPh
 Medication Reconciliation: Using Pharmacy Technicians to Improve Care Becky Johnson, CPhT Megan Ohrlund, PharmD Steve Finch, RPh Objectives Evaluate the medication reconciliation process and evidence for
Medication Reconciliation: Using Pharmacy Technicians to Improve Care Becky Johnson, CPhT Megan Ohrlund, PharmD Steve Finch, RPh Objectives Evaluate the medication reconciliation process and evidence for
Medication Reconciliation: Using Pharmacy Technicians to Improve Care. Objectives THE BASICS AND USING TECHNICIANS 3/22/2017
 Medication Reconciliation: Using Pharmacy Technicians to Improve Care Becky Johnson, CPhT Megan Ohrlund, PharmD Steve Finch, RPh Objectives Evaluate the medication reconciliation process and evidence for
Medication Reconciliation: Using Pharmacy Technicians to Improve Care Becky Johnson, CPhT Megan Ohrlund, PharmD Steve Finch, RPh Objectives Evaluate the medication reconciliation process and evidence for
Medication Reconciliation Using Natural Language Processing and Controlled Terminologies
 MEDINFO 2007 K. Kuhn et al. (Eds) IOS Press, 2007 2007 The authors. All rights reserved. Medication Reconciliation Using Natural Language Processing and Controlled Terminologies James J. Cimino, Tiffani
MEDINFO 2007 K. Kuhn et al. (Eds) IOS Press, 2007 2007 The authors. All rights reserved. Medication Reconciliation Using Natural Language Processing and Controlled Terminologies James J. Cimino, Tiffani
Patient Safety: 10 Years Later Why is Improvement So Hard? Patient Safety: Strong Beginnings
 Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Medication Reconciliation: Preventing Errors and Improving Patient Outcomes
 Murray State's Digital Commons Scholars Week 2016 - Spring Scholars Week Apr 18th, 12:00 PM - 2:00 PM Medication Reconciliation: Preventing Errors and Improving Patient Outcomes Amanda S. Boren Murray
Murray State's Digital Commons Scholars Week 2016 - Spring Scholars Week Apr 18th, 12:00 PM - 2:00 PM Medication Reconciliation: Preventing Errors and Improving Patient Outcomes Amanda S. Boren Murray
JHQ 177 Medication Reconciliation: A Necessity in Promoting a Safe Hospital Discharge
 JHQ 177 Medication Reconciliation: A Necessity in Promoting a Safe Hospital Discharge Donna L. Poole, Juliane N. Chainakul, Mary Pearson, LeAnn Graham Keywords: Discharge, Information technology, Medication
JHQ 177 Medication Reconciliation: A Necessity in Promoting a Safe Hospital Discharge Donna L. Poole, Juliane N. Chainakul, Mary Pearson, LeAnn Graham Keywords: Discharge, Information technology, Medication
Reducing Harm Improving Healthcare Protecting Canadians MEDICATION RECONCILIATION IN THE ICU. Change Package.
 Reducing Harm Improving Healthcare Protecting Canadians MEDICATION RECONCILIATION IN THE ICU Change Package January 2012 Background The ultimate goal of medication reconciliation is to prevent adverse
Reducing Harm Improving Healthcare Protecting Canadians MEDICATION RECONCILIATION IN THE ICU Change Package January 2012 Background The ultimate goal of medication reconciliation is to prevent adverse
SPSP Medicines. Prepared by: NHS Ayrshire and Arran
 SPSP Medicines Prepared by: NHS Ayrshire and Arran Medication Reconciliation: Story so far MR happening in primary care, acute adult, paediatrics and mental health Started in acute then mental health,
SPSP Medicines Prepared by: NHS Ayrshire and Arran Medication Reconciliation: Story so far MR happening in primary care, acute adult, paediatrics and mental health Started in acute then mental health,
Medication Reconciliation Bundle of Care. Margaret Duguid, Pharmaceutical Advisor Singapore, 21 August 2013
 Medication Reconciliation Bundle of Care Margaret Duguid, Pharmaceutical Advisor Singapore, 21 August 2013 Overview Problem of medication errors at transitions of care Who is at risk Recognition as a patient
Medication Reconciliation Bundle of Care Margaret Duguid, Pharmaceutical Advisor Singapore, 21 August 2013 Overview Problem of medication errors at transitions of care Who is at risk Recognition as a patient
St. Michael s Hospital Medication Reconciliation Learning Package
 St. Michael s Hospital Medication Reconciliation Learning Package What is Medication Reconciliation? A formal process which begins with obtaining a complete and accurate list of each patient s home medications
St. Michael s Hospital Medication Reconciliation Learning Package What is Medication Reconciliation? A formal process which begins with obtaining a complete and accurate list of each patient s home medications
H2H Mind Your Meds "Challenge. Webinar #3- Lessons Learned Wednesday, April 18, :00 pm 3:00 pm ET. Welcome
 H2H Mind Your Meds "Challenge Webinar #3- Lessons Learned Wednesday, April 18, 2012 2:00 pm 3:00 pm ET 1 Welcome Take Home Messages Understand how to implement the Mind Your Meds strategies and tools in
H2H Mind Your Meds "Challenge Webinar #3- Lessons Learned Wednesday, April 18, 2012 2:00 pm 3:00 pm ET 1 Welcome Take Home Messages Understand how to implement the Mind Your Meds strategies and tools in
Evaluation of NHS111 pilot sites. Second Interim Report
 Evaluation of NHS111 pilot sites Second Interim Report Janette Turner Claire Ginn Emma Knowles Alicia O Cathain Craig Irwin Lindsey Blank Joanne Coster October 2011 This is an independent report commissioned
Evaluation of NHS111 pilot sites Second Interim Report Janette Turner Claire Ginn Emma Knowles Alicia O Cathain Craig Irwin Lindsey Blank Joanne Coster October 2011 This is an independent report commissioned
Quality Improvement Medication Reconciliation Tools, Techniques and Tales
 Quality Improvement Medication Reconciliation Tools, Techniques and Tales Presented by: Marsha Nicholson, Steve Scott, City of Toronto Long-Term Care Homes and Services Division January 10, 2012 Outline
Quality Improvement Medication Reconciliation Tools, Techniques and Tales Presented by: Marsha Nicholson, Steve Scott, City of Toronto Long-Term Care Homes and Services Division January 10, 2012 Outline
Pharmaceutical Services Report to Joint Conference Committee September 2010
 Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management
 PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
PRISM Collaborative: Transforming the Future of Pharmacy PeRformance Improvement for Safe Medication Management Mission: To improve the health of the people of Connecticut through safe and effective medication
Measuring Harm. Objectives and Overview
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3. Measuring Harm
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Driving the value of health care through integration. Kaiser Permanente All Rights Reserved.
 Driving the value of health care through integration February 13, 2012 Kaiser Permanente 2010-2011. All Rights Reserved. 1 Today s agenda How Kaiser Permanente is transforming care How we re updating our
Driving the value of health care through integration February 13, 2012 Kaiser Permanente 2010-2011. All Rights Reserved. 1 Today s agenda How Kaiser Permanente is transforming care How we re updating our
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August 2016
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, August By: Terry Dentoni, MSN, RN, CNL, SFGH Chief Nursing Officer 1. Professional Nursing..1 2. Emergency Department
Translating Evidence to Safer Care
 Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Translating Evidence to Safer Care Patient Safety Research Introductory Course Session 7 Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg
Innovation Series Move Your DotTM. Measuring, Evaluating, and Reducing Hospital Mortality Rates (Part 1)
 Innovation Series 2003 200 160 120 Move Your DotTM 0 $0 $4,000 $8,000 $12,000 $16,000 $20,000 80 40 Measuring, Evaluating, and Reducing Hospital Mortality Rates (Part 1) 1 We have developed IHI s Innovation
Innovation Series 2003 200 160 120 Move Your DotTM 0 $0 $4,000 $8,000 $12,000 $16,000 $20,000 80 40 Measuring, Evaluating, and Reducing Hospital Mortality Rates (Part 1) 1 We have developed IHI s Innovation
Safety in Mental Health Collaborative
 NHS Tayside Safety in Mental Health Collaborative Improving Safety in Mental Health Programme Aims supported by an Improvement Advisor: Dr Noeleen Devaney Support 4 UK organisations to: reduce harm improving
NHS Tayside Safety in Mental Health Collaborative Improving Safety in Mental Health Programme Aims supported by an Improvement Advisor: Dr Noeleen Devaney Support 4 UK organisations to: reduce harm improving
Getting Started with Medication Reconciliation in Long Term Care. SHN! MedRec Teleconference September 14, EST
 Getting Started with Medication Reconciliation in Long Term Care SHN! MedRec Teleconference September 14, 2010 1200-1300 EST 1 Welcome! By the end of this teleconference, participants will: Understand
Getting Started with Medication Reconciliation in Long Term Care SHN! MedRec Teleconference September 14, 2010 1200-1300 EST 1 Welcome! By the end of this teleconference, participants will: Understand
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE)
 COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
Using Data to Inform Quality Improvement
 20 15 10 5 0 Using Data to Inform Quality Improvement Ethan Kuperman, MD FHM Aparna Kamath, MD MS Justin Glasgow, MD PhD Disclosures None of the presenters today have relevant personal or financial conflicts
20 15 10 5 0 Using Data to Inform Quality Improvement Ethan Kuperman, MD FHM Aparna Kamath, MD MS Justin Glasgow, MD PhD Disclosures None of the presenters today have relevant personal or financial conflicts
Making a case for medication reconciliation in primary care
 Safer Healthcare Now! MedRec National Teleconference Making a case for medication reconciliation in primary care Speakers: Karen Hall Barber, BSc (Hons), MD, CCFP Sherri Elms, BSc (Pharm), RPh ACPR Danyal
Safer Healthcare Now! MedRec National Teleconference Making a case for medication reconciliation in primary care Speakers: Karen Hall Barber, BSc (Hons), MD, CCFP Sherri Elms, BSc (Pharm), RPh ACPR Danyal
A Measurement Guide for Long Term Care
 Step 6.10 Change and Measure A Measurement Guide for Long Term Care Introduction Stratis Health, in partnership with the Minnesota Department of Health, is pleased to present A Measurement Guide for Long
Step 6.10 Change and Measure A Measurement Guide for Long Term Care Introduction Stratis Health, in partnership with the Minnesota Department of Health, is pleased to present A Measurement Guide for Long
Presenter Disclosure
 Improving Transitions from the Hospital to Community Settings IHI National Forum Learning Lab Sunday, December 8, 2013 Presenter Disclosure MaryAnne Elma, MPH Quality Implementation and Innovations Director
Improving Transitions from the Hospital to Community Settings IHI National Forum Learning Lab Sunday, December 8, 2013 Presenter Disclosure MaryAnne Elma, MPH Quality Implementation and Innovations Director
Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Objectives
 Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Morgan Pendleton, PharmD, BCOP Hematology/Oncology Clinical Pharmacist Wake Forest Baptist Health Objectives Evaluate the need
Administrative Update: How to Implement Discharge Pharmacy Services (DPS) Morgan Pendleton, PharmD, BCOP Hematology/Oncology Clinical Pharmacist Wake Forest Baptist Health Objectives Evaluate the need
Pharmacists in Transitions of Care: We Can All Make a Difference
 Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Medication Reconciliation with Pharmacy Technicians
 Technician Education Day March 29, 2014 Jacksonville, FL Outline with Pharmacy Technicians Roma Merrick RPhT., CPhT. Pharmacy Technician Coordinator St. Vincent s Medical Center Southside Jacksonville,
Technician Education Day March 29, 2014 Jacksonville, FL Outline with Pharmacy Technicians Roma Merrick RPhT., CPhT. Pharmacy Technician Coordinator St. Vincent s Medical Center Southside Jacksonville,
Medication Reconciliation
 Medication Reconciliation Where are we now? Angie Powell, PharmD Director of Pharmacy Baxter Regional Medical Center Disclosures I, Angie Powell, have no relevant financial relationships to disclose. Learning
Medication Reconciliation Where are we now? Angie Powell, PharmD Director of Pharmacy Baxter Regional Medical Center Disclosures I, Angie Powell, have no relevant financial relationships to disclose. Learning
National Readmissions Summit Safe and Reliable Transitions: An Integrated Approach Reducing Heart Failure Readmissions
 National Readmissions Summit Safe and Reliable Transitions: An Integrated Approach Reducing Heart Failure Readmissions Michael Kanter, MD, Medical Director Quality and Clinical Analysis Patti Harvey, RN,
National Readmissions Summit Safe and Reliable Transitions: An Integrated Approach Reducing Heart Failure Readmissions Michael Kanter, MD, Medical Director Quality and Clinical Analysis Patti Harvey, RN,
Building from the Blueprint for Patient Safety at the Hospital for Sick Children
 Designing an Agenda for Change Building from the Blueprint for Patient Safety at the Hospital for Sick Children Polly Stevens, Anne Matlow and Ronald Laxer INTRODUCTION The Hospital for Sick Children (Sick
Designing an Agenda for Change Building from the Blueprint for Patient Safety at the Hospital for Sick Children Polly Stevens, Anne Matlow and Ronald Laxer INTRODUCTION The Hospital for Sick Children (Sick
Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report
 Team 10 Med-List University of Michigan Health System Program and Operations Analysis Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report To: John Clark, PharmD, MS,
Team 10 Med-List University of Michigan Health System Program and Operations Analysis Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report To: John Clark, PharmD, MS,
University of Michigan Health System Part IV Maintenance of Certification Program [Form 12/1/14]
![University of Michigan Health System Part IV Maintenance of Certification Program [Form 12/1/14] University of Michigan Health System Part IV Maintenance of Certification Program [Form 12/1/14]](/thumbs/83/88988679.jpg) Report on a QI Project Eligible for Part IV MOC: Improving Medication Reconciliation in Primary Care Instructions Determine eligibility. Before starting to complete this report, go to the UMHS MOC website
Report on a QI Project Eligible for Part IV MOC: Improving Medication Reconciliation in Primary Care Instructions Determine eligibility. Before starting to complete this report, go to the UMHS MOC website
Targeted Solutions Tools
 TARGETED SOLUTIONS TOOL NOW AVAILABLE FOR OUR INTERNATIONAL CUSTOMERS! Joint Commission Center for Transforming Healthcare Targeted Solutions Tools Hand Hygiene Safe Surgery Hand-off Communications Preventing
TARGETED SOLUTIONS TOOL NOW AVAILABLE FOR OUR INTERNATIONAL CUSTOMERS! Joint Commission Center for Transforming Healthcare Targeted Solutions Tools Hand Hygiene Safe Surgery Hand-off Communications Preventing
Learner Manual. Document Best Possible Medication History (BPMH)
 Learner Manual Document Best Possible Medication History (BPMH) Table of Contents Medication safety... 1 Medication errors impact everyone... 1 Who should obtain the BPMH?... 1 When is the BPMH obtained?...
Learner Manual Document Best Possible Medication History (BPMH) Table of Contents Medication safety... 1 Medication errors impact everyone... 1 Who should obtain the BPMH?... 1 When is the BPMH obtained?...
Hard Truths Public Board 29th September, 2016
 Hard Truths Public Board 29th September, 2016 Presented for: Presented by: Author Previous Committees Governance Professor Suzanne Hinchliffe CBE, Chief Nurse/Deputy Chief Executive Heather McClelland
Hard Truths Public Board 29th September, 2016 Presented for: Presented by: Author Previous Committees Governance Professor Suzanne Hinchliffe CBE, Chief Nurse/Deputy Chief Executive Heather McClelland
Transitions of Care. Objectives 1/6/2016. Roman Digilio, PharmD PGY1 Resident West Kendall Baptist Hospital. The author has nothing to disclose.
 Transitions of Care Roman Digilio, PharmD PGY1 Resident West Kendall Baptist Hospital 1 The author has nothing to disclose. 2 Objectives Discuss current healthcare trends and the need for pharmacists in
Transitions of Care Roman Digilio, PharmD PGY1 Resident West Kendall Baptist Hospital 1 The author has nothing to disclose. 2 Objectives Discuss current healthcare trends and the need for pharmacists in
Patient and Family Engagement Strategy. April 10, 2013
 Patient and Family Engagement Strategy April 10, 2013 1 Webinar Agenda Overview & Introductions Kathy Wallace Why is Patient & Family Engagement the Right Thing to do? Carrie Brady Patient & Family Advisor
Patient and Family Engagement Strategy April 10, 2013 1 Webinar Agenda Overview & Introductions Kathy Wallace Why is Patient & Family Engagement the Right Thing to do? Carrie Brady Patient & Family Advisor
Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME
 Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME The Process What is medicine reconciliation? Medicine reconciliation is an evidence-based process, which has been
Medicine Reconciliation FREQUENTLY ASKED QUESTIONS NATIONAL MEDICATION SAFETY PROGRAMME The Process What is medicine reconciliation? Medicine reconciliation is an evidence-based process, which has been
Case Study of Physician Leaders in Quality and Patient Safety, and the Development of a Physician Leadership Network
 implementing safety solutions Case Study of Physician Leaders in Quality and Patient Safety, and the Development of a Physician Leadership Network Chris Hayes, Vandad Yousefi, Tamara Wallington and Amir
implementing safety solutions Case Study of Physician Leaders in Quality and Patient Safety, and the Development of a Physician Leadership Network Chris Hayes, Vandad Yousefi, Tamara Wallington and Amir
Rapid Review Evidence Summary: Manual Double Checking August 2017
 McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
Board Briefing. Board Briefing of Nursing and Midwifery Staffing Levels. Date of Briefing January 2018 (December 2017 data)
 Board Briefing Board Briefing of Nursing and Midwifery Staffing Levels Date of Briefing January 2018 (December 2017 data) This paper is for: Sponsor: Chief Nurse- Dame Eileen Sills (DBE) Decision Author:
Board Briefing Board Briefing of Nursing and Midwifery Staffing Levels Date of Briefing January 2018 (December 2017 data) This paper is for: Sponsor: Chief Nurse- Dame Eileen Sills (DBE) Decision Author:
PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November 2017
 Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Report Contents: PATIENT CARE SERVICES REPORT Submitted to the Joint Conference Committee, November By: Terry Dentoni, MSN, RN, CNL - ZSFG Chief Nursing Officer 1. Professional Nursing.....1 2. Emergency
Constant Pursuit of Medication Safety. Geraldine Koh Chief Pharmacist
 Constant Pursuit of Medication Safety Geraldine Koh Chief Pharmacist 1 Alexandra Hospital 400 beds Multi discipline except Paeds & ObGyn Restructured in Oct 2000 Transformation Creating A Safety Culture
Constant Pursuit of Medication Safety Geraldine Koh Chief Pharmacist 1 Alexandra Hospital 400 beds Multi discipline except Paeds & ObGyn Restructured in Oct 2000 Transformation Creating A Safety Culture
From Big Data to Big Knowledge Optimizing Medication Management
 From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
Auditing medication history-taking can help demonstrate improved pharmacy services
 Auditing medication history-taking can help demonstrate improved pharmacy services With an aim to share best practice on quality assessment of clinical pharmacy services, Reena Mehta and Raliat Onatade
Auditing medication history-taking can help demonstrate improved pharmacy services With an aim to share best practice on quality assessment of clinical pharmacy services, Reena Mehta and Raliat Onatade
Experiential Education
 Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
Objectives. Key Elements. ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management 5/20/2014
 ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety
 Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
Using SBAR to Communicate Falls Risk and Management in Inter-professional Rehabilitation Teams
 teamwork and communication Using SBAR to Communicate Falls Risk and Management in Inter-professional Rehabilitation Teams Angie Andreoli, Carol Fancott, Karima Velji, G. Ross Baker, Sherra Solway, Elaine
teamwork and communication Using SBAR to Communicate Falls Risk and Management in Inter-professional Rehabilitation Teams Angie Andreoli, Carol Fancott, Karima Velji, G. Ross Baker, Sherra Solway, Elaine
Patient Care: Case Study in EHR Implementation. With Help From Monkeys, Mice, and Penguins. Tom Goodwin, MHA MIT Medical Cambridge, MA March 2007
 Using Information Technology to Drive Patient Care: Case Study in EHR Implementation With Help From Monkeys, Mice, and Penguins Tom Goodwin, MHA MIT Medical Cambridge, MA March 2007 MIT Medical Staff 122
Using Information Technology to Drive Patient Care: Case Study in EHR Implementation With Help From Monkeys, Mice, and Penguins Tom Goodwin, MHA MIT Medical Cambridge, MA March 2007 MIT Medical Staff 122
Evidence-Informed ICU Rounds. Critical Care Canada Forum October 26, 2015
 Evidence-Informed ICU Rounds Critical Care Canada Forum October 26, 2015 No disclosures or conflicts of interest Many acknowledgements Objectives 1. Summarize why we round 2. Describe current rounding
Evidence-Informed ICU Rounds Critical Care Canada Forum October 26, 2015 No disclosures or conflicts of interest Many acknowledgements Objectives 1. Summarize why we round 2. Describe current rounding
Improving HPV Vaccination Rates in a Large Pediatric Practice: Implementing Effective Quality Improvement
 Improving HPV Vaccination Rates in a Large Pediatric Practice: Implementing Effective Quality Improvement Alix Casler, M.D., F.A.A.P. Chief of Pediatrics, Medical Director of Pediatrics Orlando Health
Improving HPV Vaccination Rates in a Large Pediatric Practice: Implementing Effective Quality Improvement Alix Casler, M.D., F.A.A.P. Chief of Pediatrics, Medical Director of Pediatrics Orlando Health
MEDICINES RECONCILIATION GUIDELINE Document Reference
 MEDICINES RECONCILIATION GUIDELINE Document Reference G358 Version Number 1.01 Author/Lead Job Title Jackie Stark Principle Pharmacist Clinical Services Date last reviewed, (this version) 29 November 2012
MEDICINES RECONCILIATION GUIDELINE Document Reference G358 Version Number 1.01 Author/Lead Job Title Jackie Stark Principle Pharmacist Clinical Services Date last reviewed, (this version) 29 November 2012
Quality Improvement Plans (QIP): Progress Report for the 2016/17 QIP
 Quality Improvement Plans (QIP): Progress Report for the QIP Medication Reconciliation ID Measure/Indicator from as stated on QIP 2017 1 Best possible medication history(bpmh) completion: The total number
Quality Improvement Plans (QIP): Progress Report for the QIP Medication Reconciliation ID Measure/Indicator from as stated on QIP 2017 1 Best possible medication history(bpmh) completion: The total number
PROPOSED CHANGES TO THE 2018 LEAPFROG HOSPITAL SURVEY
 PROPOSED CHANGES TO THE 2018 LEAPFROG HOSPITAL SURVEY OPEN FOR PUBLIC COMMENT Each year, The Leapfrog Group s team of researchers reviews the literature and convenes expert panels to ensure the Leapfrog
PROPOSED CHANGES TO THE 2018 LEAPFROG HOSPITAL SURVEY OPEN FOR PUBLIC COMMENT Each year, The Leapfrog Group s team of researchers reviews the literature and convenes expert panels to ensure the Leapfrog
the BE Technical Report
 Canada Health Infoway Benefits Evaluation and the BE Technical Report July 2012 Presented by What we ll cover Infoway Background Infoway s Approach to Benefits Evaluation A walk through of the BE Technical
Canada Health Infoway Benefits Evaluation and the BE Technical Report July 2012 Presented by What we ll cover Infoway Background Infoway s Approach to Benefits Evaluation A walk through of the BE Technical
Northern Health - Acute Services. Evidence Based Practice Venous Thromboembolism Prevention
 Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Northern Health - Acute Services Evidence Based Practice Venous Thromboembolism Prevention (VTE) Jeannette Kamar Christine Lamotte, Liam Carter Improving Patient Safety Preventing and Managing Venous Thromboembolism
Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA
 JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
A Million Little Pieces: Developing a Controlled Substance Diversion Program. Tanya Y. Barnhart, PharmD, BCPS
 A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
A Million Little Pieces: Developing a Controlled Substance Diversion Program Tanya Y. Barnhart, PharmD, BCPS I have no conflicts of interest to disclose Objectives Explain the importance of building a
A Multi-Phased Approach to Using Clinical Data to Drive Evidence-Based EMR Redesign. Kulik, Carole Marie; Foad, Wendy; Brown, Gretchen
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Medication Reconciliation
 Medication Reconciliation ISMP Canada Annual Report to CPSI Safer Healthcare Now! Medication Reconciliation Intervention April 2010 to March 2011 Safer Healthcare Now! Medication Reconciliation Intervention
Medication Reconciliation ISMP Canada Annual Report to CPSI Safer Healthcare Now! Medication Reconciliation Intervention April 2010 to March 2011 Safer Healthcare Now! Medication Reconciliation Intervention
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach
 Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Raising the Bar On Infusion Safety: A Patient Safety Program at Baylor Scott & White Health Improving Infusion Pump Safety: A Systematic Approach July 18, 2016 AAMI Foundation Vision: To drive the safe
Medication Reconciliation in Transitions of Care
 Medication Reconciliation in Transitions of Care Jeff West, RN MPH June 18th, 2015 Adverse Drug Events & Readmissions For every 1,000 hospital admissions, medication reconciliation could prevent 14 adverse
Medication Reconciliation in Transitions of Care Jeff West, RN MPH June 18th, 2015 Adverse Drug Events & Readmissions For every 1,000 hospital admissions, medication reconciliation could prevent 14 adverse
General practitioner workload with 2,000
 The Ulster Medical Journal, Volume 55, No. 1, pp. 33-40, April 1986. General practitioner workload with 2,000 patients K A Mills, P M Reilly Accepted 11 February 1986. SUMMARY This study was designed to
The Ulster Medical Journal, Volume 55, No. 1, pp. 33-40, April 1986. General practitioner workload with 2,000 patients K A Mills, P M Reilly Accepted 11 February 1986. SUMMARY This study was designed to
National Trends Winter 2016
 National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
National Trends Winter 216 About the National Trends data This report presents a unique and real-time view of trends within temporary nursing including bank and agency usage. The data used has been drawn
The STAAR Initiative
 The STAAR Initiative A quality effort at the heart of system redesign Amy E. Boutwell, MD, MPP The Center for Innovative Healthcare Strategies amy@innovativehealthcarestrategies.org Please note: Dr Boutwell
The STAAR Initiative A quality effort at the heart of system redesign Amy E. Boutwell, MD, MPP The Center for Innovative Healthcare Strategies amy@innovativehealthcarestrategies.org Please note: Dr Boutwell
Pharmacological Therapy Practice Guidance Note Medicine Reconciliation on Admission to Hospital for Adults in all Clinical Areas within NTW V02
 Pharmacological Therapy Practice Guidance Note Medicine Reconciliation on Admission to Hospital for Adults in all Clinical Areas within NTW V02 V02 issued Issue 1 May 11 Issue 2 Dec 11 Planned review May
Pharmacological Therapy Practice Guidance Note Medicine Reconciliation on Admission to Hospital for Adults in all Clinical Areas within NTW V02 V02 issued Issue 1 May 11 Issue 2 Dec 11 Planned review May
Analysis of Cardiovascular Patient Data during Preoperative, Operative, and Postoperative Phases
 University of Michigan College of Engineering Practicum in Hospital Systems Program and Operations Analysis Analysis of Cardiovascular Patient Data during Preoperative, Operative, and Postoperative Phases
University of Michigan College of Engineering Practicum in Hospital Systems Program and Operations Analysis Analysis of Cardiovascular Patient Data during Preoperative, Operative, and Postoperative Phases
CRITICAL ANALYSIS OF INTERNATIONAL PATIENT SAFETY GOLAS STANDARDS IN JCI ACCREDITATION AND CBAHI STANDARDS FOR HOSPITALS
 IMPACT: International Journal of Research in Business Management (IMPACT: IJRBM) ISSN (E): 2321-886X; ISSN (P): 2347-4572 Vol. 4, Issue 3, Mar 2016, 71-78 Impact Journals CRITICAL ANALYSIS OF INTERNATIONAL
IMPACT: International Journal of Research in Business Management (IMPACT: IJRBM) ISSN (E): 2321-886X; ISSN (P): 2347-4572 Vol. 4, Issue 3, Mar 2016, 71-78 Impact Journals CRITICAL ANALYSIS OF INTERNATIONAL
IMPROVING CARE TRANSITIONS: Optimizing Medication Reconciliation
 IMPROVING CARE TRANSITIONS: Optimizing Medication Reconciliation MARCH 2012 Improving Care Transitions: Optimizing Medication Reconciliation Developed by: American Pharmacists Association American Society
IMPROVING CARE TRANSITIONS: Optimizing Medication Reconciliation MARCH 2012 Improving Care Transitions: Optimizing Medication Reconciliation Developed by: American Pharmacists Association American Society
NCH Healthcare System HIMSS Michele Thoman, RN - CNO Sarah Richardson - CIO Jeff Dindak Sr. IT Director
 NCH Healthcare System HIMSS 2015 Michele Thoman, RN - CNO Sarah Richardson - CIO Jeff Dindak Sr. IT Director NCH Healthcare System Non-for-profit, multi-facility healthcare system in Naples, Florida 2
NCH Healthcare System HIMSS 2015 Michele Thoman, RN - CNO Sarah Richardson - CIO Jeff Dindak Sr. IT Director NCH Healthcare System Non-for-profit, multi-facility healthcare system in Naples, Florida 2
2017/18 Quality Improvement Plan Improvement Targets and Initiatives
 2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
2017/18 Quality Improvement Plan Improvement Targets and Initiatives AIM Measure Change Effective Effective Care for Patients with Sepsis % Eligible Nurses who have Completed the Sepsis Education Bundle
Status Report to the Board of Governors. PCORI Dissemination Workgroup. Can You Hear Us Now?
 Status Report to the Board of Governors PCORI Dissemination Workgroup Can You Hear Us Now? PCORI Board of Governors Jacksonville, Florida January 2012 1 Members of the Workgroup Carolyn Clancy, Co-Chair
Status Report to the Board of Governors PCORI Dissemination Workgroup Can You Hear Us Now? PCORI Board of Governors Jacksonville, Florida January 2012 1 Members of the Workgroup Carolyn Clancy, Co-Chair
Medication Safety Dashboard
 How Safe Are Your Patients? Creating a Meaningful & Actionable Medication Safety Dashboard By: Helga Brake, PharmD, CPHQ Patient Safety Leader Northwestern Memorial Hospital No Conflicts of Interest to
How Safe Are Your Patients? Creating a Meaningful & Actionable Medication Safety Dashboard By: Helga Brake, PharmD, CPHQ Patient Safety Leader Northwestern Memorial Hospital No Conflicts of Interest to
Why is Critical Incident Reporting and Shared Learning Important for Patient Safety?
 Why is Critical Incident Reporting and Shared Learning Important for Patient Safety? Reporting on Critical Incidents Related to Medication / IV Fluid Ontario Hospital Association Video and Webcast Toronto,
Why is Critical Incident Reporting and Shared Learning Important for Patient Safety? Reporting on Critical Incidents Related to Medication / IV Fluid Ontario Hospital Association Video and Webcast Toronto,
Two Keys to Excellent Health Care for Canadians
 Two Keys to Excellent Health Care for Canadians Dated: 22/10/01 Two Keys to Excellent Health Care for Canadians: Provide Information and Support Competition A submission to the: Commission on the Future
Two Keys to Excellent Health Care for Canadians Dated: 22/10/01 Two Keys to Excellent Health Care for Canadians: Provide Information and Support Competition A submission to the: Commission on the Future
Influence of Patient Flow on Quality Care
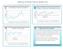 Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Influence of Patient Flow on Quality Care Patients Waiting on Trolleys for an Inpatient Bed Patients who are Medically Fit to be discharged and cared for at Home with Support or in a Nursing Home or District
Hospital pharmacists play an important role in improving
 CLINICAL PRACTICE The Invisible White Coat: Awareness of Pharmacists in a Neonatal Intensive Care Unit Rehana Bajwa, Jennifer G Kendrick, and Roxane Carr NTRODUCTION Hospital pharmacists play an important
CLINICAL PRACTICE The Invisible White Coat: Awareness of Pharmacists in a Neonatal Intensive Care Unit Rehana Bajwa, Jennifer G Kendrick, and Roxane Carr NTRODUCTION Hospital pharmacists play an important
Best Practices and Performance Measures for Systemic Treatment Computerized Prescriber Order Entry Systems (ST CPOE) in Chemotherapy Delivery
 Best Practices and Performance Measures for Systemic Treatment Computerized Prescriber Order Entry Systems (ST CPOE) in Chemotherapy Delivery Dr. Vishal Kukreti, MD, FRCPC, MSc Clinical Lead, Systemic
Best Practices and Performance Measures for Systemic Treatment Computerized Prescriber Order Entry Systems (ST CPOE) in Chemotherapy Delivery Dr. Vishal Kukreti, MD, FRCPC, MSc Clinical Lead, Systemic
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall. Total. Application Analysis 1.
 Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
EHR Enablement for Data Capture
 EHR Enablement for Data Capture Baylor Scott & White (15 min) Bonnie Hodges, RN University of Chicago Medicine(15 min) Susan M. Sullivan, RHIA, CPHQ Kaiser Permanente (15 min) Molly P. Clopp, RN Tammy
EHR Enablement for Data Capture Baylor Scott & White (15 min) Bonnie Hodges, RN University of Chicago Medicine(15 min) Susan M. Sullivan, RHIA, CPHQ Kaiser Permanente (15 min) Molly P. Clopp, RN Tammy
Structured Practical Experiential Program
 2017/18 Structured Practical Experiential Program PHARMACY STUDENT AND INTERN ROTATIONS RESOURCE COLLEGE OF PHARMACISTS OF MANITOBA COLLEGE OF PHARMACY RADY FACULTY OF HEALTH SCIENCES UNIVERSITY OF MANITOBA
2017/18 Structured Practical Experiential Program PHARMACY STUDENT AND INTERN ROTATIONS RESOURCE COLLEGE OF PHARMACISTS OF MANITOBA COLLEGE OF PHARMACY RADY FACULTY OF HEALTH SCIENCES UNIVERSITY OF MANITOBA
Development and assessment of a Patient Safety Culture Dr Alice Oborne
 Development and assessment of a Patient Safety Culture Dr Alice Oborne Consultant pharmacist safe medication use March 2014 Outline 1.Definitions 2.Concept of a safe culture 3.Assessment of patient safety
Development and assessment of a Patient Safety Culture Dr Alice Oborne Consultant pharmacist safe medication use March 2014 Outline 1.Definitions 2.Concept of a safe culture 3.Assessment of patient safety
Objectives. Prevalence of Non-Adherence. Medications and Care Transitions. The Cost of Readmissions. The Pharmacist s Role in Improving Care 4/22/2015
 MEDS TO BEDS: DELIVERING REDUCED READMISSIONS, LOWER COSTS, AND IMPROVED QUALITY Laura S. Carr PharmD, Senior Attending Pharmacist, Transitional Care Massachusetts General Hospital Ed Cohen, PharmD, FAPhA
MEDS TO BEDS: DELIVERING REDUCED READMISSIONS, LOWER COSTS, AND IMPROVED QUALITY Laura S. Carr PharmD, Senior Attending Pharmacist, Transitional Care Massachusetts General Hospital Ed Cohen, PharmD, FAPhA
MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY. April 2009 September 2012
 MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY April 2009 September 2012 Institute for Safe Medication Practices Canada Institut pour l utilisation sécuritaire des médicaments du
MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY April 2009 September 2012 Institute for Safe Medication Practices Canada Institut pour l utilisation sécuritaire des médicaments du
Pharmacy Technician led model to reduce the rate of omitted medicines
 Pharmacy Technician led model to reduce the rate of omitted medicines By Fleur Baylis Lead Pharmacist Patient Safety Brighton and Sussex University Hospitals NHS Trust Outline NPSA alert Missed doses Trust
Pharmacy Technician led model to reduce the rate of omitted medicines By Fleur Baylis Lead Pharmacist Patient Safety Brighton and Sussex University Hospitals NHS Trust Outline NPSA alert Missed doses Trust
How BPOC Reduces Bedside Medication Errors White Paper
 How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
Improving Pain Center Processes utilizing a Lean Team Approach
 Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
Improving Pain Center Processes utilizing a Lean Team Approach Organization Name: St. Joseph Medical Center Type: Acute Care Hospital Contact Person: Sue Mitchell Title: Nurse Mgr Pain Mgmt Center E-Mail:
TCLHIN Standardized Discharge Summary
 TCLHIN Standardized Discharge Summary ehealth Conference June 4, 2014 Kara Kitts Quality Improvement Manager St. Michael s Hospital Ontario Healthcare System 14 Local Health Integration Networks (LHINs)
TCLHIN Standardized Discharge Summary ehealth Conference June 4, 2014 Kara Kitts Quality Improvement Manager St. Michael s Hospital Ontario Healthcare System 14 Local Health Integration Networks (LHINs)
UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016
 UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016 Department Name: Department of Pharmacy Department Director: Steve Rough, MS,
UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016 Department Name: Department of Pharmacy Department Director: Steve Rough, MS,
Title of Case Study: Reduce medication errors with closed-loop medication administration system Leslie St. Toronto, ON M2K 1E1, Canada
 HIMSS Davies Enterprise Award Submission Title of Case Study: Reduce medication errors with closed-loop medication administration system Organization: Primary Point of Contact: Secondary Point of Contact:
HIMSS Davies Enterprise Award Submission Title of Case Study: Reduce medication errors with closed-loop medication administration system Organization: Primary Point of Contact: Secondary Point of Contact:
