Safe Medication Administration through Direct Observation
|
|
|
- Herbert Cummings
- 6 years ago
- Views:
Transcription
1 Quality in Primary Care (2015) 23 (3): Insight Medical Publishing Group Research Article Ensuring Research Article Safe Medication Administration through Open Access Direct Observation Katelyn Young, B.A. Katie Cochran (Brehmer), B.S. Mei Mei, B.S. Karen Adkins-Bley J.D R.N. Scott Ciarkowski, PharmD Deborah Wagner, PharmD, FASHP The University of Michigan Health System: Ann Arbor, MI, USA Abstract Background and Objectives: A medication administration process was examined within a university affiliated pediatric hospital. Areas for future improvement will be identified in order to enhance medication practices and ensure the safety of patients during a medication administration. Methods: To evaluate the effectiveness of the medication administration process in regards to patient safety and quality assurance, a direct observation study of inpatient units was conducted. The outcomes of this study address labeling medication, patient identifiers, the Five Rights of medication administration, the use of nursing staff worksheets, double checks, and the presence of distractions and interruptions during the medication administration process. Results: From the 60 observations, information was collected and then analyzed both quantitatively as well as qualitatively. Background and objectives Ensuring safe medication administration is a complex and multi-factorial system involving nursing and pharmacy. Often the evaluation of it depends solely on risk reports to identify process improvement needs. Alternative methods such as trigger tools and direct observation can add to the body of knowledge without relying on a single method. One is well aware of the Five Rights of medication administration but in reality it is unknown if they indeed occur. 1 A study by Antonow found that 62.1% of medication errors were prevented at the dispensing/ delivery phase but the likelihood of prevention decreased in the later stages of the medication administration process. 2,1 (Figure 1) In the pediatric population, medication errors are usually attributed to nursing staff; in a study of 190 nursing administration errors, 57% were due to omission, wrong infusion rate, and wrong time 1. However, nursing staff are also the most likely health care professionals to catch errors before they occur. Kopp s study indicates 24 of the 110 (22%) potential adverse drug events (ADEs) were intercepted, primarily by nursing personnel (88%). 2 This becomes significantly important as medication administration errors rates The numerical outcomes are shown in the following graphs and the data are discussed at length. The data identify areas where improvements can be made to ensure safe medication administration. Conclusions: This study provides a first step towards making quality changes to ensure the safety of patients during a medication administration. In order to draw more conclusive results, collection of data would need to take place over a prolonged period of time with a sample population proportionate to the institution. Keywords: medication errors, medication administration errors, patient safety, quality assurance Abbreviations: emar: electronic Medication Administration Record; MAR: Medication Administration Record; MRN: Medical Record Number are higher in the pediatric patient population compared to adult patient populations. A Sentinel Event Alert about preventing pediatric medication errors, published by the Joint Commission, cited dosing errors as one of the root causes because of weight based dosing calculations, fractional dosing, and the need for decimal points. 3 Error rates detected by direct observation Five Rights of Medication Administration Were the Five Rights of medication administration utilized? N/O Yes 43% 47% No 10% Figure 1: Medication Labeling Graph.
2 168 Katelyn Young studies have varied reported error rates. In the Buckley study, the type of error documented as the most common (wrong dose) with 26.2% yet in other studies, using similar direct observation methods, found the error to occur infrequently with only 1.2%. 4 A medication administration error is defined as a deviation from the prescriber s medication order as written on a patient s record, manufacturers preparation, administration instructions, or institutional policies/procedures on medication administration. 5 A review of direct observational studies on medication administration errors identified a median error rate of 19.6% of total opportunities for error. The wrong time, medication omission, and wrong dosage were the three most common medication administration errors. The authors in the Keers study note bar-code medication administration (BCMA), computerized prescriber order entry, educational packets, and different drug distribution systems have shown a decrease in the rate of medication administration errors. 5 Elganzouri and colleagues found nurses averaged 15 minutes on each medication administration. The administration included the preparation, retrieval, administration and documentation. Based on the study s results, it is apparent there are opportunities for interruptions to the medication administration process. The observational study included a rural, urban and an academic hospital and represented both electronic and paper based ordering and documentation. 6 The direct observation studies done by Keers et al, in adult and pediatric medical/surgical intensive care units, found that one preventable error occurred for every five doses of medication administered. Errors occurred in each stage of the medication administration process. Wrong dose, wrong time, wrong technique and extra doses were medication administration errors observed in the studies. 5 In both direct observation studies conducted by Buckley et al and Kopp et al, proximal causes identified in the administration stage included slips and memory lapses, lack of drug knowledge, rule violations, preparation errors, faulty dose checking, infusion pump problems and faulty interaction with other services. Slips and memory lapses were identified as the most common cause of medication administration errors. 2,4 In this process improvement project, the team undertook a direct observation study of the medication administration process in our pediatric population. The University of Michigan Health System opened a new pediatric hospital, C.S. Mott Children s Hospital, prior to the study. The direct observation study was formulated in an attempt to observe medication passing in the new facility with increased Omnicell locations, different access to nursing stations, and the historical use of nursing worksheets. Nursing worksheets had previously been utilized as an organization tool for nurses. These were used, prior to the implementation of computerized physician order entry, to prioritize medication administration. The mission of the study was to bring awareness and educational initiatives to the nursing staff members. Additionally, the team intends to identify and analyze the different steps of the medication administration process for further improvement. METHODS Setting This 24-day direct observational study took place at the University of Michigan s C.S. Mott Children s Hospital a 198-bed inpatient institution between September 10 th, 2012 and October 12 th, This length of time was chosen to allow the students to observe each of the eight pediatric nursing units on at least three different occasions, with the exception of two units only being observed twice. A risk management student observer from the Office of Clinical Safety visited each of the selected inpatient units between 8am and 10am during morning medication administration; each time observing multiple patients medication administration. The demographic of patients varied among the eight units. The patients observed were both male and female patients between the ages of 11 days to 68 years old; the average patient age was four years. One of the observed units houses pediatric hematology/oncology and bone marrow transplant (BMT) patients. Adult BMT patients are also admitted to this unit, resulting in the observation of medication administration to 10 patients over the age 18. An observation form was utilized during the observation time period and consisted of questions to be answered during each medication administration, as reference during the observation time period. The questions on the form were based on issues identified in our voluntary Patient Safety Reporting System reports (i.e. contributing factors identified in medication administration errors). In addition, nursing feedback obtained at our pediatric medication safety meeting was used to supplement the questions/metrics deemed valuable to measure during the observation. The institution utilizes the electronic Medication Administration Record (emar) for information regarding medication tasks. Therefore, it is standard of practice for nursing staff that documentation will occur in the emar system. The student observer was instructed to observe the nursing staffs many uses of the emar. Medications on the inpatient floors are stored in several medication rooms located throughout the floors as well as in locked cabinets by the patients bedside. In addition, student observers were informed of the uses of the unit-specific Omnicell supply cabinets and bedside medication cabinets. The Omnicell supply cabinets contain medications such as narcotics, analgesics and protocol or algorithm-based medications. These cabinets also contain medications for emergency situations. Bedside medication cabinets are utilized for storing scheduled patient medications. Definitions According to the institution s medication administration policy, a medication administration can be defined as the provision of medications by authorized personnel in a manner that assures proper patient and medication identification, documentation of medication administration in the medical record. This policy was used as a reference for the student observers conducting the observations. 7 Medication Process & Data Collection The observation form presents sixteen questions specifically focused on the critical steps that nursing staff members adhere to during a medication administration. The medication observation form was created by the research team and was further refined
3 Ensuring Safe Medication Administration through Direct Observation 169 to accurately reflect the sequence of events during a medication administration. In addition to the original responses of Yes, No and N/A listed on the form, a column titled N/O (not observed) was created to account for the incidences where the student observers were only able to observe a fraction of the medication administration. Furthermore, for questions 2, 3, 4, 7, 8, 9, 11, 12, 15 and 16, N/A would not be an applicable answer since the reasonable choices are simply Yes, No or N/O. Nurse Managers were notified of the planned observation days and to the purposes of the observational study. In order to more accurately portray an everyday medication administration, Nurse Managers and the observed nursing staff were unaware of the specific questions included on the observation form. Once the student observers arrived at their assigned inpatient unit, the Charge Nurse or Nurse Manager would assign the student observer to a member of the nursing staff or a designated nursing station to observe. Thereafter, when the nursing staff member planned to begin a medication administration, the nursing staff would alert the student observer, and the student observer would proceed to either the medication room or the patient s room with their assigned nursing staff. During the twohour observation period, the student observer was encouraged to observe as much of the medication administration process as the situation permitted. For further analysis of the collected data, six of the sixteen questions on the observation form became a primary focus where the concern for patient safety was the highest. The six questions dealt with issues related to the following medication administration s areas: labeling medication, two patient identifiers, the Five Rights of medication administration, the use of worksheets, double-checks and presence of distractions or interruptions during the medication administration process. (Figure 2 and 3) RESULTS Data Microsoft Access was used to record and analyze the responses from the data collection sheets. The data graphs can be found in Figures 4 through 8. Distractions or Interruptions Was there a distraction or interruption during preparation or administration? There were 60 medication administration observations in total. In all 60 of the observations, the nursing staff who administered the medication either had a RN or BSN degree, or was a nurse trainee who was under the supervision of a registered nurse. On several occasions, nursing staff members were observed multiple times with different patients; however, nursing staff names were not documented during the study for privacy reasons so the exact number of nursing staff observed cannot be determined. There were a total of 57 patients whose medication administration was observed; three patients were observed twice. The total number of observations for each of the eight units was dependent on how many nursing staff members were observed. The mean number of observations was 7.5 with a range of 8; the least amount of medication administrations observed on a unit was 3 and the most observed was 11. Key Questions As mentioned in the Methods section, 6 of the 16 questions on the observation form were identified as key questions after the observational study. These questions (5, 7, 11, 13, 14 and 15) highlighted areas of concern that are vital to patient safety and quality of care. These six questions are represented graphically in Figure 4 through 8. Distractions or Interruptions Follow-Up Was the distraction or interruption avoidable? Unknown 10% Yes 20% No 70% Figure 3 : Five Rights of Medication Administration Graph. n=10 Medication Labeling The medication was labeled throughout process? Yes 17% N/O 2% 5% N/A No No 83% 5% Yes 88% Figure 2 : Patient Identifiers Graph. Figure 4 : emar Documentation Graph.
4 170 Katelyn Young Labeling Medication Question 5 addresses whether or not the medication was labeled throughout the medication administration process, from preparation to administration. At the institution, if the medication is not administered immediately, the medication label is required to have the name of the medication, dose or amount, and the expiration date (when not used within 24 hours) and expiration time (if expiration is less than 24 hours). 88% (53/60) of the medication administrations that were observed had the correct labeling while 5% (3/60) were labeled incorrectly (i.e. name and date of medication were missing). In 2% (1/60) of the observations, the student observers did not observe the medication labeling therefore, they were not able to confirm or deny whether or not the medication was labeled correctly. In another 5% (3/60) of the observations, the labeling of the medication was not necessary (N/A) because the medication was administered immediately from the medicine cabinets located in the patients room. Patient Identifiers Question 7 quantifies whether or not two patient identifiers were used prior to the administration of medication. According to institution s policies, the patient s identity needs to be confirmed, prior to critical tasks, using two different identifiers. These two identifiers can be any two of the following: patient full name, date of birth, or registration number (this is the same as the Medical Registration Number [MRN]). All three of the identifiers are included on the Positive Patient Identifier band that is required to be on the patient at all times. The nursing staff administering the medication often utilizes the identification band to obtain the two patient identifiers. 65% (39/60) of all patients were correctly identified using two identifiers while 17% (10/60) were not. In 18% (11/60) of the observations, the patient identification step of the process was not observed (N/O). The identification process was not observed during the 11 medication administrations due to a variety of reasons; most frequently due to contact precautions, requiring students to remain outside the room during the medication administration, and the patient being too young to verbalize their name and birthdate and their caregiver was not present.(figure 5) The Five Rights of Medication Administration In all six of the observations (100%), the unmet Right was Right Patient. emar Documentation Although question 12 was not identified as a key question, two follow-up questions stemmed its content: Did nursing staff immediately document the medication given on the MAR (emar) after administration? The original results for question 12 yielded 91.7% of nursing staff (51/60) immediately documented the medication on the MAR, 6.7% (4/60) did not, and on one occasion it was not observed. From the 4 observations forms with no responses, the comment section was analyzed for comments regarding the timing of the documentation if it wasn t immediate. Two possible outcomes were decided on as responses to this question: delayed or not entered during observation. It was discovered that of the 4 observations, 50% had delayed documentation and 50% were not documented during the time of the student observers observations. Of the 4 responses from question 12 that indicated the medication administration was not immediately documented in the emar, the team questioned whether the corresponding nursing staff used a personal worksheet instead of the emar to document. The 4 observation forms were collected and the corresponding response from question 13 was recorded. Furthermore, it was determined in those 4 observations forms that the medication administration was not immediately documented in the emar because the respective nursing staff was using personal worksheets.(figure 6) Nursing Staff Worksheets Question 13 refers to whether or not the nursing staff referred to a personal worksheet as a schedule for patient medications. It is preferred that nursing staff members utilize the electronic medication schedule in the emar instead of transcribing the medication schedule on a separate piece of paper. Using a handmade worksheet is a static way of keeping track of medication schedules whereas the emar provides flexibility, fluidity, and real-time updates on medication dosages, times, routes, etc. 57% (34/60) of the nursing staff utilized personal worksheets while 28% (17/60) did not. In 8% (5/60) of the instances, it was not Question 11 was framed in regards to the Five Rights of Medication Administration: verifying the Right Patient, Right Medication, Right Dose, Right Route and Right Time. 1 All Five Rights need to be completed prior to every medication administration. In 47% of all observations, all Five Rights were completed and verbalized with the student observers before administration. In 10% of the observations, one of the Five Rights was not met. The percentage of not observed responses, 43%, was almost equivalent to those where the Five Rights were completed. No 17% Patient Identifiers Were two (2) patient identifiers used prior to administration? N/O 18% Yes 65% 10% of the responses for question 11 were no therefore, six observations had at least one of the Five Rights missing. The comments for all six observation forms with a no response were queried to display which Right was unmet in each instance. Figure 5: Nursing Staff Worksheet Graph.
5 Ensuring Safe Medication Administration through Direct Observation 171 observed (N/O) whether or not a worksheet was used and in 7% of instances the use of a worksheet was not applicable (N/A). Double-Checks emar Documentation Did the nursing staff document the medication given on the emar after administration? N/O 7% 1% N Yes 92% Figure 6: Double-Checks Graph. Question 14 reviews continuous infusion guidelines. Before continuous infusions of medications are started or administered or when there is a change to the syringe or bag of continuous medication infusion, the administering nursing staff member must have another nursing staff member double-check to verify that all information on the infusion pump is correct. For question 14, 15% of all necessary infusions were doublechecked by an additional nursing staff member while 5% were not double-checked. In 70% of the observations, double-checks were not required as either an intravenous infusion was not initiated, a medication dose was not changed, or a new bag was not hung. In 10% (6/60) of the observations the double check was not observed (N/O). Distractions and Interruptions Question 15 s topic sought to determine how prominent distractions and interruptions were during the medication administration process. In 83% of the medication administrations observed, there were no distractions or interruptions. However, 17% of the observations had a distraction or an interruption during the administration. Datum from this question was analyzed further; after the observation was complete, responses were reviewed to determine if the distractions or interruptions that took place during the observations were avoidable. Examining data for this question required looking back at the 10 observations that had an interruption or distraction and classifying the response based on the corresponding comments. An avoidable distraction or interruption was considered to be a task or situation that could have waited until after the medication administration. An unavoidable distraction or interruption was considered an unforeseeable event that halts the medication administration process; for example, an unavoidable distraction could be a change in the status of the patient, or medical teams coming into the room during a medication administration to do their daily rounds. Of the 10 observations with interruptions or distractions, 20% were considered avoidable [after the fact], 70% were considered unavoidable [after the fact] and 10% could not be classified and remained unknown. DISCUSSION Labeling Medication For the purpose of this pediatric medication administration observation study, the student observers were directed to observe if nursing staff labeled the medication throughout the process. The student observers found that the majority of the nursing staff labeled the medication prior to administration. After reviewing the data, only 5% of the observations showed medications labeled incorrectly. For the student observers observing, it became apparent that the practice of nursing staff is not reflective of the institution s policy. In a number of observations the nursing staff made an attempt to label the medication, but not all the recommended information was included. For example, the patient name was not included but the drug name was. A medication container or syringe should be labeled at all times in order to prevent administering the wrong medication to the wrong person. Moreover, moving to a barcoded system of medication administration would help to validate the Five Rights of Medication Administration; that is, ensuring that patients receive the Right Drug, the Right Dose, the Right Patient, the Right Route, and at the Right Time. (Frederico, 2011) By implementing such a system, there is less room for human error and the barcoded system would serve as a doublecheck for administered medications. This would also give a more accurate portrayal of when medications are administered and would aid in the documentation process. Patient Identifiers Two patient identifiers are required to be confirmed, prior to critical tasks including medication administration, to verify a patient s identity. A preferred method of identifying patients has yet to be defined and leaves the two identifiers used up to the nursing staff s discretion. 50 of the 57 patients observed were under the age 18, some only days old. This patient population can make patient identification challenging for nursing staff. As discussed previously, in some observations the patient was too young to verbalize their name and date of birth. In other instances, the child was sleeping and a caregiver was not present to verify the identity of the patient. In these instances nursing staff needed an alternative method to verify the patient s identity, using the Positive Patient Identifier (PPI) band instead. These wrist bands are to be kept on the patient at all times and were often used to confirm patient name, birthdate, and medical record number, which was then compared to the electronic medical record. However, in some observations the PPI band was not observed directly on the patient but instead on the patient s bed or basinette. This practice could result in incorrect patient identification if the PPI band is the only form of patient identification. If the patient can advocate for themselves or a caregiver is present, having the patient state his or her name and their date of birth to the nurse verbally was the most effective and reliable form of patient identifcation.
6 172 Katelyn Young During one of the observations, a nursing staff member made a suggestion to improve the patient identification step in the medication administration process. The emar utilized at the University of Michigan provides only the patient s name and medical record number on the medication page. The nurse recommended adding the patient s date of birth to the medication page in the emar as well, which would allow the nursing staff to confirm patients name and date of birth seamlessly in the emar medication page. The Five Rights of Medication Administration In 43% of the observations done, the Five Rights were not observed. The lack of verbalization between the student observers and nursing staff, when the nursing staff was verifying the Five Rights as well as the two patient identifiers during the medication administration process, made the observations very difficult. Without verbal confirmation that the nurse checked both identifiers and all Five Rights, the student observers could not confirm nor deny whether or not either was completed. The student observers were instructed to simply observe the medication administration process and not actively participate. Therefore the nursing staff could have mentally checked the two patient identifiers and all Five Rights but the student observers could not determine this. Thus, multiple instances for both questions had to be documented as not observed (N/O). Nursing Staff Worksheets The student observers concluded that 57% (34/60) of the nursing staff observed utilized personal worksheets while 28% (17/60) did not. The remainder of observed nursing staff either did not use a worksheet or did not use a worksheet for the purpose of administering a medication. Suffice to note, the nursing worksheets appear to be used as a prioritization tool or task list; the worksheets were not being used to officially document the administration of medication, as this is done in the emar. The reason why over half of the observed nursing staff appeared to prefer to use their own worksheet as opposed to solely using the emar was not investigated during this study. This yields questions, which should be posed, during further research, to determine specific explanation of staff preferences. If worksheets are determined by nursing leadership to be a best practice in medication administration, the utilization of a standard worksheet across the institution will force standardization of practice. (Figure 7) Double-Checks In 3 (or 5%) of the 60 observed medication administrations, the nursing staff did not perform double-checks for patients who had continuous medication infusions. There could be several contributing factors that could have caused the three observed instances to occur. For example, the workflow that is practiced and advocated throughout the institution might not readily allow the first nurse enough time to notify a second nurse that a double-check is needed. Or in another case, the second nurse who agreed to perform the double-check could have been busy with his or her own patient, made a mental reminder to perform the double-check, but afterwards forgot to perform the needed double-check. The institution will be looking at technology and function to help support double-checks and decrease the impact in workflow. The lack of adherance to the doublechecks on continous medication infusions is consistent with the Institute for Safe Medication Practices (ISMP) assertion that independent double-checks are undervalued and misused. ISMP suggests that independent double-checks should reserved for very select high-risk tasks or specific high-alert medications. Use of independent checks on all high-alert medications or all continuous infusions often cause the check to be a routine task and lose its importance. (ISMP, 2013) (Figure 8) Distractions and Interruptions There are several different situations where there were unavoidable distractions and interruptions that delayed the medication administration process. In one instance, there was a change in the patient s physical status, which caused for an unavoidable delay in the medication administration. Specifically, the patient s unexpected low blood glucose was given first priority and the nursing staff immediately proceeded to stabilize the patient. The medication was never administered during the time the student observer was present on the unit. Situations such as a change in the patient s mental or health status typically should take precendence over the administration of a regularly scheduled medication. The student observers who observed the unavoidable and N/O 8% Nursing Staff Worksheets Did the nursing staff use a worksheet to refer to medications for patient and schedule? No 28% N/A 7% Yes 57% Figure 7: Distractions or Interruptions Graph. Double-Checks Was a double check performed for continuous 70% infusions? Yes 15% No 5% Figure 8 : Distractions or Interruptions Graph. N/O N/A 10%
7 Ensuring Safe Medication Administration through Direct Observation 173 avoidable interruptions and distractions were vigilient in their observation comments. Several times during the unavoidable interruptions and distractions, the nursing staff continued with the medication administration process with frequent ease. This is referring to when the patient was stable for the medication administrations. Since the nursing staff continued with the medication administration process undisturbed, the nursing staff demonstrates that these distractions and interruptions are normal occurances happening several times throughout the day. (Figure 9) CONCLUSION This observational study provides us with many possible areas of improvement which could be addressed to ensure a safe medication administration. This study identified those potential areas to focus on labeling, utilizing patient identifiers, adhering to the Five Rights of medication, using a standardized documentation method, double checking medications, and working around the presence of distractions during the medication administration process. Further research is needed to determine the root causes of these potential problem areas. The results of this study are of course limited to the willingness of nursing staff to participate, and the observations taken through this study may not accurately portray the institution s medication administration practice as a whole. Selection bias was not under the control of the study and may have occurred. Furthermore, because this was a direct observational study, the presence of the observer in the room had the potential to change the behavior of the participating nursing staff member. Regardless of the limitations of a direct observation study, this study provides a first step towards making quality changes to ensure the safety of patients during a medication administration. Moreover, this observational study highlights the need for a revision in compliance and expectations of nursing staff. However, encouraging increased compliance will not decrease errors altogether; putting hard-stop barriers in place are necessary in order to alleviate the possibility of human error or complacency. This study aims to draw awareness to the need for future policy improvements such as a barcoding system to make medication administration and documentation a safer, consistent, and streamlined process. REFERENCES 1. Frederico, F. (2011). The Five Rights of Medication Administration. Institute for Healthcare Improvement. ISMP. Independent double checks: undervalued and misused. ISMP Medication Safety Alert! 2013; 18(12): ISMP. Independent double checks: undervalued and misused. ISMP Medication Safety Alert! 2013; 18(12): Antonow, J.A. Smith, A.B. Silver, M.P. HealthInsight Salt Lake City, Utah, USA. Medication error reporting: a survey of nursing staff. Journal of Nursing Care Quality. 15(1):42-8, 2000 Oct. 4. Kopp BJ, Erstad BL, Allen ME, et al. Medication errors and adverse drug events in an intensive care unit: Direct observation approach for detection. Crit Care Med 2006; 34: "Preventing Pediatric Medication Errors." Sentinel Event Alert. The Joint Commission, 10 Apr Buckley MS, Erstad BL, Kopp BJ, et al. Direct observation approach for detecting medication errors and adverse drug events in a pediatric intensive care unit. Pediatr Crit Care Med 2007; 8: Keers RN, Williams SD, Cooke J, Ashcroft DM. Prevalence and nature of medication administration errors in health care settings: A systematic review of direct observational evidence. Ann Pharmacother 2013:47: Elganzouri ES, Standish CA, Androwich I. Medication administration time study (MATS). JONA. 2009;39(5): University of Michigan Health System. (2014) UMHHC Policy : Medication Administration Policy. Figure 9 : Observation Form.
How BPOC Reduces Bedside Medication Errors White Paper
 How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
How BPOC Reduces Bedside Medication Errors White Paper July 2008 Brad Blackwell, M.S., R.Ph. Eloise Keeler, R.N., B.S.N. Abstract Medication errors are a significant source of harm to patients in U.S hospitals,
Rapid Review Evidence Summary: Manual Double Checking August 2017
 McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
IMPACT OF TECHNOLOGY ON MEDICATION SAFETY
 Continuous Quality Improvement IMPACT OF Steven R. Abel, PharmD, FASHP TECHNOLOGY ON Nital Patel, PharmD. MBA MEDICATION SAFETY Sheri Helms, PharmD Candidate Brian Heckman, PharmD Candidate Ismaila D Badjie
Continuous Quality Improvement IMPACT OF Steven R. Abel, PharmD, FASHP TECHNOLOGY ON Nital Patel, PharmD. MBA MEDICATION SAFETY Sheri Helms, PharmD Candidate Brian Heckman, PharmD Candidate Ismaila D Badjie
Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that
 Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that hospital. 1 2 3 Note that an actual variance occurs when
Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that hospital. 1 2 3 Note that an actual variance occurs when
Running head: MEDICATION ERRORS 1. Medications Errors and Their Impact on Nurses. Kristi R. Rittenhouse. Kent State University College of Nursing
 Running head: MEDICATION ERRORS 1 Medications Errors and Their Impact on Nurses Kristi R. Rittenhouse Kent State University College of Nursing MEDICATION ERRORS 2 Abstract One in five medication dosages
Running head: MEDICATION ERRORS 1 Medications Errors and Their Impact on Nurses Kristi R. Rittenhouse Kent State University College of Nursing MEDICATION ERRORS 2 Abstract One in five medication dosages
Preventing Medical Errors
 Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
SHRI GURU RAM RAI INSTITUTE OF TECHNOLOGY AND SCIENCE MEDICATION ERRORS
 MEDICATION ERRORS Patients depend on health systems and health professionals to help them stay healthy. As a result, frequently patients receive drug therapy with the belief that these medications will
MEDICATION ERRORS Patients depend on health systems and health professionals to help them stay healthy. As a result, frequently patients receive drug therapy with the belief that these medications will
CHAPTER 7 Safe Medication Administration
 64 SECTION 3 READING MEDICATION LABELS AND SYRINGE CALIBRATIONS CHAPTER 7 Safe Medication Administration Objectives The learner will: 1. read a MAR to identify medications to be administered. 2. record
64 SECTION 3 READING MEDICATION LABELS AND SYRINGE CALIBRATIONS CHAPTER 7 Safe Medication Administration Objectives The learner will: 1. read a MAR to identify medications to be administered. 2. record
Background and Methodology
 Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
Study Sites and Investigators Emergency Department Pharmacists Improve Patient Safety: Results of a Multicenter Study Supported by the ASHP Foundation Jeffrey Rothschild, MD, MPH-Principal Investigator
CRAIG HOSPITAL POLICY/PROCEDURE
 CRAIG HOSPITAL POLICY/PROCEDURE Approved: P&T, MEC, NPC, P&P 03/09 Effective Date: 02/95 P&T, MEC, P&P 08/09; P&P 08/10; P&T, MEC 10/10, P&T, P&P 12/10 ; MEC 01/11; P&T, MEC 02/11, 04/11 ; P&T, P&P 12/11
CRAIG HOSPITAL POLICY/PROCEDURE Approved: P&T, MEC, NPC, P&P 03/09 Effective Date: 02/95 P&T, MEC, P&P 08/09; P&P 08/10; P&T, MEC 10/10, P&T, P&P 12/10 ; MEC 01/11; P&T, MEC 02/11, 04/11 ; P&T, P&P 12/11
The Impact of CPOE and CDS on the Medication Use Process and Pharmacist Workflow
 The Impact of CPOE and CDS on the Medication Use Process and Pharmacist Workflow Conflict of Interest Disclosure The speaker has no real or apparent conflicts of interest to report. Anne M. Bobb, R.Ph.,
The Impact of CPOE and CDS on the Medication Use Process and Pharmacist Workflow Conflict of Interest Disclosure The speaker has no real or apparent conflicts of interest to report. Anne M. Bobb, R.Ph.,
Objectives. Key Elements. ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management 5/20/2014
 ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
ICAHN Targeted Focus Areas: Staff Competency and Education Quality Processes and Risk Management Matthew Fricker, RPh, MS, FASHP Program Director, ISMP Rebecca Lamis, PharmD, FISMP Medication Safety Analyst,
In-Patient Medication Order Entry System - contribution of pharmacy informatics
 In-Patient Medication Order Entry System - contribution of pharmacy informatics Ms S C Chiang BPharm, MRPS, MHA, FACHSE, FHKCHSE, FCPP Senior Pharmacist Chief Pharmacist s Office In-Patient Medication
In-Patient Medication Order Entry System - contribution of pharmacy informatics Ms S C Chiang BPharm, MRPS, MHA, FACHSE, FHKCHSE, FCPP Senior Pharmacist Chief Pharmacist s Office In-Patient Medication
Drug Events. Adverse R EDUCING MEDICATION ERRORS. Survey Adapted from Information Developed by HealthInsight, 2000.
 Survey Adapted from Information Developed by HealthInsight, 2000. Adverse Drug Events R EDUCING MEDICATION ERRORS The Adverse Drug Events Survey will assist healthcare organizations evaluate the number
Survey Adapted from Information Developed by HealthInsight, 2000. Adverse Drug Events R EDUCING MEDICATION ERRORS The Adverse Drug Events Survey will assist healthcare organizations evaluate the number
Medication Safety Technology The Good, the Bad and the Unintended Consequences
 Medication Safety Technology The Good, the Bad and the Unintended Consequences Michelle Mandrack RN, MSN Director of Consulting Services Matthew Fricker, RPh, MS Program Director 1 Objectives Consider
Medication Safety Technology The Good, the Bad and the Unintended Consequences Michelle Mandrack RN, MSN Director of Consulting Services Matthew Fricker, RPh, MS Program Director 1 Objectives Consider
Objectives. Demographics: Type and Services 1/22/2014. ICAHN Aggregate Results. ISMP Medication Safety Self Assessment for Hospitals
 ICAHN Aggregate Results ISMP Medication Safety Self Assessment for Hospitals Matthew Fricker, RPH, MS, FASHP Rebecca Lamis, PharmD, FISMP January 23, 2014 1 Objectives Report the demographic characteristics
ICAHN Aggregate Results ISMP Medication Safety Self Assessment for Hospitals Matthew Fricker, RPH, MS, FASHP Rebecca Lamis, PharmD, FISMP January 23, 2014 1 Objectives Report the demographic characteristics
IV Interoperability: Smart Pump and BCMA Integration
 IV Interoperability: Smart Pump and BCMA Integration Amanda Prusch, PharmD, BCPS Medication Safety Specialist Tina Suess, RN, BSN System Administrator October 5, 2010 Lancaster General Hospital Profile
IV Interoperability: Smart Pump and BCMA Integration Amanda Prusch, PharmD, BCPS Medication Safety Specialist Tina Suess, RN, BSN System Administrator October 5, 2010 Lancaster General Hospital Profile
Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses
 Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses March 2018 College of Licensed Practical Nurses of Nova Scotia http://clpnns.ca Starlite Gallery, 302-7071 Bayers Road,
Administration of Medications A Self-Assessment Guide for Licensed Practical Nurses March 2018 College of Licensed Practical Nurses of Nova Scotia http://clpnns.ca Starlite Gallery, 302-7071 Bayers Road,
Section 2 Medication Orders
 Section 2 Medication Orders 2-1 Objectives: 1. List/recognize the components of a complete medication order. 2. Transcribe orders onto the Medication Administration Record (MAR) correctly use proper abbreviations,
Section 2 Medication Orders 2-1 Objectives: 1. List/recognize the components of a complete medication order. 2. Transcribe orders onto the Medication Administration Record (MAR) correctly use proper abbreviations,
Validating Pilot Program to Improve Discharge Medication in 12 West at C.S. Mott Children s Hospital. Final Report. Submitted To:
 Validating Pilot Program to Improve Discharge Medication in 12 West at C.S. Mott Children s Hospital Final Report Submitted To: Cathy Lewis, MSN, RN Clinical Nurse Specialist and Adjunct Clinical Instructor
Validating Pilot Program to Improve Discharge Medication in 12 West at C.S. Mott Children s Hospital Final Report Submitted To: Cathy Lewis, MSN, RN Clinical Nurse Specialist and Adjunct Clinical Instructor
COMPASS Phase II Incident Analysis Report Prepared by ISMP CANADA February 2016
 COMPASS Phase II Incident Analysis Report Prepared by ISMP CANADA February 2016 INTRODUCTION Incidents as part of COMPASS (Community Pharmacists Advancing Safety in Saskatchewan) Phase II reported by 87
COMPASS Phase II Incident Analysis Report Prepared by ISMP CANADA February 2016 INTRODUCTION Incidents as part of COMPASS (Community Pharmacists Advancing Safety in Saskatchewan) Phase II reported by 87
OHTAC Recommendation. Implementation and Use of Smart Medication Delivery Systems
 OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
Example of a Health Care Failure Mode and Effects Analysis for IV Patient Controlled Analgesia (PCA) Failure Modes (what might happen)
 Prescribing Assess patient Choose analgesic/mode of delivery Prescribe analgesic Institute for Safe Medication Practices Example of a Health Care and Effects Analysis for IV Patient Controlled Analgesia
Prescribing Assess patient Choose analgesic/mode of delivery Prescribe analgesic Institute for Safe Medication Practices Example of a Health Care and Effects Analysis for IV Patient Controlled Analgesia
Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016
 Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016 DISCLOSURE STATEMENT I have nothing to disclose regarding
Medication Errors in Chemotherapy PORSCHA L. JOHNSON, PHARM.D. CLINICAL PHARMACIST II MEDSTAR WASHINGTON HOSPITAL CENTER SATURDAY, SEPTEMBER 17, 2016 DISCLOSURE STATEMENT I have nothing to disclose regarding
University of Mississippi Medical Center University of Mississippi Health Care. Pharmacy and Therapeutics Committee Medication Use Evaluation
 University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014
 5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014 EVALUATION OF INTRAVENOUS MEDICATION ERRORS WITH INFUSION PUMPS Eija Kivekäs, MSc, RN,
5th International Conference on Well-Being in the Information Society, WIS 2014, Turku, Finland, August 18-20, 2014 EVALUATION OF INTRAVENOUS MEDICATION ERRORS WITH INFUSION PUMPS Eija Kivekäs, MSc, RN,
University of Michigan Health System. Final Report
 University of Michigan Health System Program and Operations Analysis Analysis of Medication Turnaround in the 6 th Floor University Hospital Pharmacy Satellite Final Report To: Dr. Phil Brummond, Pharm.D,
University of Michigan Health System Program and Operations Analysis Analysis of Medication Turnaround in the 6 th Floor University Hospital Pharmacy Satellite Final Report To: Dr. Phil Brummond, Pharm.D,
MEDICATION ADMINISTRATION POLICY POLICY, PROCEDURES, & GUIDELINES FOR MEDICATION ADMINISTRATION II. PROCEDURES FOR MEDICATION ADMINISTRATION
 Insytt-ma-procedures 08-09; 02-17 page 1 of 7 MEDICATION ADMINISTRATION POLICY POLICY, PROCEDURES, & GUIDELINES F MEDICATION ADMINISTRATION II. PROCEDURES F MEDICATION ADMINISTRATION Procedures used for
Insytt-ma-procedures 08-09; 02-17 page 1 of 7 MEDICATION ADMINISTRATION POLICY POLICY, PROCEDURES, & GUIDELINES F MEDICATION ADMINISTRATION II. PROCEDURES F MEDICATION ADMINISTRATION Procedures used for
MEDICINES RECONCILIATION GUIDELINE Document Reference
 MEDICINES RECONCILIATION GUIDELINE Document Reference G358 Version Number 1.01 Author/Lead Job Title Jackie Stark Principle Pharmacist Clinical Services Date last reviewed, (this version) 29 November 2012
MEDICINES RECONCILIATION GUIDELINE Document Reference G358 Version Number 1.01 Author/Lead Job Title Jackie Stark Principle Pharmacist Clinical Services Date last reviewed, (this version) 29 November 2012
2. Short term prescription medication and drugs (administered for less than two weeks):
 Medication Administration Procedure This is a companion document with Policy # 516 Student Medication To access the policy: click on Policies (under the District Information heading) The Licensed School
Medication Administration Procedure This is a companion document with Policy # 516 Student Medication To access the policy: click on Policies (under the District Information heading) The Licensed School
Pharmaceutical Services Report to Joint Conference Committee September 2010
 Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
Pharmaceutical Services Report to Joint Conference Committee September 21 Background: Pharmaceutical Services staffing has increased by 31 FTE from 26 due to program changes and to comply with regulatory
The University of Michigan Health System. Geriatrics Clinic Flow Analysis Final Report
 The University of Michigan Health System Geriatrics Clinic Flow Analysis Final Report To: CC: Renea Price, Clinic Manager, East Ann Arbor Geriatrics Center Jocelyn Wiggins, MD, Medical Director, East Ann
The University of Michigan Health System Geriatrics Clinic Flow Analysis Final Report To: CC: Renea Price, Clinic Manager, East Ann Arbor Geriatrics Center Jocelyn Wiggins, MD, Medical Director, East Ann
Management of Reported Medication Errors Policy
 Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
How to Conduct a Medication Administration Observation
 How to Conduct a Medication Administration Observation Transcript Title Slide (no narration) Welcome Hello. My name is Jill Morrow and I am the Medical Director for the Office of Developmental Programs.
How to Conduct a Medication Administration Observation Transcript Title Slide (no narration) Welcome Hello. My name is Jill Morrow and I am the Medical Director for the Office of Developmental Programs.
Just Culture Toolkit Scenarios
 Just Culture Toolkit Scenarios In order to promote a just culture where staff is comfortable in reporting errors or near misses, healthcare organizations must adopt a disciplinary system theory approach.
Just Culture Toolkit Scenarios In order to promote a just culture where staff is comfortable in reporting errors or near misses, healthcare organizations must adopt a disciplinary system theory approach.
End-to-end infusion safety. Safely manage infusions from order to administration
 End-to-end infusion safety Safely manage infusions from order to administration New demands and concerns 56% 7% of medication errors are IV-related. 1 of high-risk IVs are compounded in error. 2 $3.5B
End-to-end infusion safety Safely manage infusions from order to administration New demands and concerns 56% 7% of medication errors are IV-related. 1 of high-risk IVs are compounded in error. 2 $3.5B
To establish a consistent process for the activity of an independent double-check prior to medication administration, where appropriate.
 TITLE INDEPENDENT DOUBLE-CHECK SCOPE Provincial, Clinical DOCUMENT # PS-60-01 APPROVAL LEVEL Senior Operating Officer, Pharmacy Services SPONSOR Provincial Medication Management Committee CATEGORY Patient
TITLE INDEPENDENT DOUBLE-CHECK SCOPE Provincial, Clinical DOCUMENT # PS-60-01 APPROVAL LEVEL Senior Operating Officer, Pharmacy Services SPONSOR Provincial Medication Management Committee CATEGORY Patient
Using MEDMARX for Reporting and Benchmarking. Anne Skinner, RHIA Katherine Jones, PhD, PT
 Using MEDMARX for Reporting and Benchmarking Anne Skinner, RHIA Katherine Jones, PhD, PT Purpose of the Grant: Assist small rural hospitals to Voluntarily report and analyze medication errors Identify
Using MEDMARX for Reporting and Benchmarking Anne Skinner, RHIA Katherine Jones, PhD, PT Purpose of the Grant: Assist small rural hospitals to Voluntarily report and analyze medication errors Identify
PURPOSE To establish a standardized process for the activity of an independent double check for medication administration.
 PURPOSE To establish a standardized process for the activity of an independent double check for medication administration. POLICY STATEMENTS Health Care Providers will complete the independent double check
PURPOSE To establish a standardized process for the activity of an independent double check for medication administration. POLICY STATEMENTS Health Care Providers will complete the independent double check
Bar Code Medication Administration and MAR Resource Manual
 Bar Code Medication Administration and MAR Resource Manual Creating Orders Creating an Order in CareMobile (Ad Hoc Order Entry)...2 Creating an Order for med that is already ordered with a different dose/frequency....4
Bar Code Medication Administration and MAR Resource Manual Creating Orders Creating an Order in CareMobile (Ad Hoc Order Entry)...2 Creating an Order for med that is already ordered with a different dose/frequency....4
Penticton & District Community Resources Society. Child Care & Support Services. Medication Control and Monitoring Handbook
 Penticton & District Community Resources Society Child Care & Support Services Medication Control and Monitoring Handbook Revised Mar 2012 Table of Contents Table of Contents MEDICATION CONTROL AND MONITORING...
Penticton & District Community Resources Society Child Care & Support Services Medication Control and Monitoring Handbook Revised Mar 2012 Table of Contents Table of Contents MEDICATION CONTROL AND MONITORING...
From Big Data to Big Knowledge Optimizing Medication Management
 From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
From Big Data to Big Knowledge Optimizing Medication Management Session 157, March 7, 2018 Dave Webster, RPh MSBA, Associate Director of Pharmacy Operations, URMC Strong Maria Schutt, EdD, Director Education
Using the Just Culture Method. Stacey Thomas, BSN, RNC Risk Analyst
 Using the Just Culture Method Stacey Thomas, BSN, RNC Risk Analyst Just Culture A system of Shared Accountability Everyone in the organization is responsible for maintaining a safe and reliable system
Using the Just Culture Method Stacey Thomas, BSN, RNC Risk Analyst Just Culture A system of Shared Accountability Everyone in the organization is responsible for maintaining a safe and reliable system
One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration
 One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration Presented by: Marla Husch Northwestern Memorial Hospital Northwestern Memorial Hospital Chicago, Illinois
One or More Errors in 67% of the IV Infusions: Insights from a Study of IV Medication Administration Presented by: Marla Husch Northwestern Memorial Hospital Northwestern Memorial Hospital Chicago, Illinois
Managing medicines in care homes
 Managing medicines in care homes http://www.nice.org.uk/guidance/sc/sc1.jsp Published: 14 March 2014 Contents What is this guideline about and who is it for?... 5 Purpose of this guideline... 5 Audience
Managing medicines in care homes http://www.nice.org.uk/guidance/sc/sc1.jsp Published: 14 March 2014 Contents What is this guideline about and who is it for?... 5 Purpose of this guideline... 5 Audience
Root Cause Analysis LITE (RCA Lite)
 Root Cause Analysis LITE (RCA Lite) INTRODUCTION The root cause analysis Lite tool is designed to assist Ottawa Hospital teams to review an adverse event or near miss, identify root causes of the event
Root Cause Analysis LITE (RCA Lite) INTRODUCTION The root cause analysis Lite tool is designed to assist Ottawa Hospital teams to review an adverse event or near miss, identify root causes of the event
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center
 Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Improving Staff Education
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Improving Staff Education
Structured Practical Experiential Program
 2017/18 Structured Practical Experiential Program PHARMACY STUDENT AND INTERN ROTATIONS RESOURCE COLLEGE OF PHARMACISTS OF MANITOBA COLLEGE OF PHARMACY RADY FACULTY OF HEALTH SCIENCES UNIVERSITY OF MANITOBA
2017/18 Structured Practical Experiential Program PHARMACY STUDENT AND INTERN ROTATIONS RESOURCE COLLEGE OF PHARMACISTS OF MANITOBA COLLEGE OF PHARMACY RADY FACULTY OF HEALTH SCIENCES UNIVERSITY OF MANITOBA
Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use
 Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use Our vision is to create a culture where patients and those who care for them are
Sharp HealthCare Safety Training 2015 Module 3, Lesson 2 Always Events: Line and Tube Reconciliation and Guardrails Use Our vision is to create a culture where patients and those who care for them are
Analysis of Nursing Workload in Primary Care
 Analysis of Nursing Workload in Primary Care University of Michigan Health System Final Report Client: Candia B. Laughlin, MS, RN Director of Nursing Ambulatory Care Coordinator: Laura Mittendorf Management
Analysis of Nursing Workload in Primary Care University of Michigan Health System Final Report Client: Candia B. Laughlin, MS, RN Director of Nursing Ambulatory Care Coordinator: Laura Mittendorf Management
Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1
 Managing medicines in care homes Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Managing medicines in care homes Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Medication Administration & Preventing Errors M E A G A N R A Y, R N A M G S P E C I A L T Y H O S P I T A L
 Medication Administration & Preventing Errors M E A G A N R A Y, R N A M G S P E C I A L T Y H O S P I T A L Principles of Medication Administration Talk with the patient and explain what you are doing
Medication Administration & Preventing Errors M E A G A N R A Y, R N A M G S P E C I A L T Y H O S P I T A L Principles of Medication Administration Talk with the patient and explain what you are doing
Policy for Patient Identification. Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead:
 CONTROLLED DOCUMENT Policy for Patient Identification CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead: Approved By:
CONTROLLED DOCUMENT Policy for Patient Identification CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead: Approved By:
Quality Management Building Blocks
 Quality Management Building Blocks Quality Management A way of doing business that ensures continuous improvement of products and services to achieve better performance. (General Definition) Quality Management
Quality Management Building Blocks Quality Management A way of doing business that ensures continuous improvement of products and services to achieve better performance. (General Definition) Quality Management
MEDICATION ERRORS: KNOWLEDGE AND ATTITUDE OF NURSES IN AJMAN, UAE
 MEDICATION ERRORS: KNOWLEDGE AND ATTITUDE OF NURSES IN AJMAN, UAE JOLLY JOHNSON 1*, MERLIN THOMAS 1 1 Department of Nursing, Gulf Medical College Hospital, Ajman, UAE ABSTRACT Objectives: This study was
MEDICATION ERRORS: KNOWLEDGE AND ATTITUDE OF NURSES IN AJMAN, UAE JOLLY JOHNSON 1*, MERLIN THOMAS 1 1 Department of Nursing, Gulf Medical College Hospital, Ajman, UAE ABSTRACT Objectives: This study was
Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals
 Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals John M. Kessler, B.S. Pharm., Pharm. D. Steve C. Dedrick, MS Pharm. NCCMedS Project Directors
Assessing and improving the use of near-miss reporting to prevent adverse events and errors in rural hospitals John M. Kessler, B.S. Pharm., Pharm. D. Steve C. Dedrick, MS Pharm. NCCMedS Project Directors
CLINICAL PROTOCOL FOR THE IDENTIFICATION OF SERVICE USERS
 CLINICAL PROTOCOL FOR THE IDENTIFICATION OF SERVICE USERS RATIONALE All Professionals/healthcare workers are personally accountable for their practice and, in the exercise of their professional accountability,
CLINICAL PROTOCOL FOR THE IDENTIFICATION OF SERVICE USERS RATIONALE All Professionals/healthcare workers are personally accountable for their practice and, in the exercise of their professional accountability,
Improving Safety Practices Anticoagulation Therapy
 Improving Safety Practices Anticoagulation Therapy Katie Cinnamon, PharmD, BCPS Clinical Pharmacist Genesis Medical Center - Davenport Objectives Review background information on medication errors and
Improving Safety Practices Anticoagulation Therapy Katie Cinnamon, PharmD, BCPS Clinical Pharmacist Genesis Medical Center - Davenport Objectives Review background information on medication errors and
Nursing Home Medication Error Quality Initiative
 Nursing Home Medication Error Quality Initiative MEQI Report: Year Five October 1, 2007 to September 30, 2008 MEQI A report on the fifth year of mandatory reporting of medication errors for all state licensed
Nursing Home Medication Error Quality Initiative MEQI Report: Year Five October 1, 2007 to September 30, 2008 MEQI A report on the fifth year of mandatory reporting of medication errors for all state licensed
Supplementary Appendix
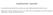 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Poon EG, Keohane CA, Yoon CS, et al. Effect of bar-code technology
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Poon EG, Keohane CA, Yoon CS, et al. Effect of bar-code technology
Chapter 13. Documenting Clinical Activities
 Chapter 13. Documenting Clinical Activities INTRODUCTION Documenting clinical activities is required for one or more of the following: clinical care of individual patients -sharing information with other
Chapter 13. Documenting Clinical Activities INTRODUCTION Documenting clinical activities is required for one or more of the following: clinical care of individual patients -sharing information with other
Definitions: In this chapter, unless the context or subject matter otherwise requires:
 CHAPTER 61-02-01 Final Copy PHARMACY PERMITS Section 61-02-01-01 Permit Required 61-02-01-02 Application for Permit 61-02-01-03 Pharmaceutical Compounding Standards 61-02-01-04 Permit Not Transferable
CHAPTER 61-02-01 Final Copy PHARMACY PERMITS Section 61-02-01-01 Permit Required 61-02-01-02 Application for Permit 61-02-01-03 Pharmaceutical Compounding Standards 61-02-01-04 Permit Not Transferable
National Patient Safety Goals from The Joint Commission
 National Patient Safety Goals from The Joint Commission Objectives After completion of this module, participants will be able to: List at least five National Patient Safety Goals that are required in a
National Patient Safety Goals from The Joint Commission Objectives After completion of this module, participants will be able to: List at least five National Patient Safety Goals that are required in a
DISPENSING BY REGISTERED NURSES (RNs) EMPLOYED WITHIN REGIONAL HEALTH AUTHORITIES (RHAs)
 2017 DISPENSING BY REGISTERED NURSES (RNs) EMPLOYED WITHIN REGIONAL HEALTH AUTHORITIES (RHAs) This Interpretive Document was approved by ARNNL Council in 2017 and replaces Dispensing by Registered Nurses
2017 DISPENSING BY REGISTERED NURSES (RNs) EMPLOYED WITHIN REGIONAL HEALTH AUTHORITIES (RHAs) This Interpretive Document was approved by ARNNL Council in 2017 and replaces Dispensing by Registered Nurses
Guideline for the notification of serious breaches of Regulation (EU) No 536/2014 or the clinical trial protocol
 1 2 31 January 2017 EMA/430909/2016 3 4 5 Guideline for the notification of serious breaches of Regulation (EU) No 536/2014 or Draft Adopted by GCP Inspectors Working Group (GCP IWG) 30 January 2017 Adopted
1 2 31 January 2017 EMA/430909/2016 3 4 5 Guideline for the notification of serious breaches of Regulation (EU) No 536/2014 or Draft Adopted by GCP Inspectors Working Group (GCP IWG) 30 January 2017 Adopted
Adopting Standardized Definitions The Future of Data Collection and Benchmarking in Alternate Site Infusion Must Start Now!
 Adopting Standardized Definitions The Future of Data Collection and Benchmarking in Alternate Site Infusion Must Start Now! Connie Sullivan, RPh Infusion Director, Heartland IV Care Lyons, CO CE Credit
Adopting Standardized Definitions The Future of Data Collection and Benchmarking in Alternate Site Infusion Must Start Now! Connie Sullivan, RPh Infusion Director, Heartland IV Care Lyons, CO CE Credit
Risk-Quality-Safety Management Reporting and the Healthcare SafetyZone Portal
 Risk-Quality-Safety Management Reporting and the Healthcare SafetyZone Portal Heather Annolino, RN, MBA, CPHRM Director, Risk-Quality-Safety Consulting Services Clarity Group, Inc. 04/22/15 1 04/22/15
Risk-Quality-Safety Management Reporting and the Healthcare SafetyZone Portal Heather Annolino, RN, MBA, CPHRM Director, Risk-Quality-Safety Consulting Services Clarity Group, Inc. 04/22/15 1 04/22/15
JCAHO Med Management
 Hospital Pharmacy Volume 41, Number 9, pp 888 892 2006 Wolters Kluwer Health, Inc. JCAHO Med Management Meeting the Standards for Emergency Medications and Labeling Patricia C. Kienle, MPA, FASHP* This
Hospital Pharmacy Volume 41, Number 9, pp 888 892 2006 Wolters Kluwer Health, Inc. JCAHO Med Management Meeting the Standards for Emergency Medications and Labeling Patricia C. Kienle, MPA, FASHP* This
Identification of Patient, Resident or Client Using Two Identifiers
 Approved by: Vice President & Chief Medical Officer; and Vice President & Chief Operating Officer Identification of Patient, Resident or Client Using Two Corporate Policy & Procedures Manual Date Approved
Approved by: Vice President & Chief Medical Officer; and Vice President & Chief Operating Officer Identification of Patient, Resident or Client Using Two Corporate Policy & Procedures Manual Date Approved
MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY. April 2009 September 2012
 MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY April 2009 September 2012 Institute for Safe Medication Practices Canada Institut pour l utilisation sécuritaire des médicaments du
MEDICATION SAFETY SELF-ASSESSMENT FOR LONG-TERM CARE ONTARIO SUMMARY April 2009 September 2012 Institute for Safe Medication Practices Canada Institut pour l utilisation sécuritaire des médicaments du
The Joint Commission Medication Management Update for 2010
 Learning Objectives The Joint Commission Medication Management Update for 2010 U.S. Army Medical Command Fort Sam Houston, TX Describe most recent changes in The Joint Commission (TJC) Accreditation Program
Learning Objectives The Joint Commission Medication Management Update for 2010 U.S. Army Medical Command Fort Sam Houston, TX Describe most recent changes in The Joint Commission (TJC) Accreditation Program
247 CMR: BOARD OF REGISTRATION IN PHARMACY
 247 CMR 9.00: CODE OF PROFESSIONAL CONDUCT; PROFESSIONAL STANDARDS FOR REGISTERED PHARMACISTS, PHARMACIES AND PHARMACY DEPART- MENTS Section 9.01: Code of Professional Conduct for Registered Pharmacists,
247 CMR 9.00: CODE OF PROFESSIONAL CONDUCT; PROFESSIONAL STANDARDS FOR REGISTERED PHARMACISTS, PHARMACIES AND PHARMACY DEPART- MENTS Section 9.01: Code of Professional Conduct for Registered Pharmacists,
Wristband Errors in Small Hospitals
 PHLEBOTOMY J a n e C. Dale, MD Stephen W. Renner, MD Wristband Errors in Small Hospitals A College of American Pathologists' Q-Probes Study of Quality ssues in Patient dentification Although methods of
PHLEBOTOMY J a n e C. Dale, MD Stephen W. Renner, MD Wristband Errors in Small Hospitals A College of American Pathologists' Q-Probes Study of Quality ssues in Patient dentification Although methods of
To provide protocol for medication and solution labeling to ensure safe medication administration. Unofficial Copy
 SUBJECT: MEDICATION / SOLUTION CONTAINER LABELING PURPOSE: To provide protocol for medication and solution labeling to ensure safe medication administration. POLICY: All medications, medication containers
SUBJECT: MEDICATION / SOLUTION CONTAINER LABELING PURPOSE: To provide protocol for medication and solution labeling to ensure safe medication administration. POLICY: All medications, medication containers
Licensed Pharmacy Technicians Scope of Practice
 Licensed s Scope of Practice Adapted from: Request for Regulation of s Approved by Council April 24, 2015 DEFINITIONS In this policy: Act means The Pharmacy and Pharmacy Disciplines Act means an unregulated
Licensed s Scope of Practice Adapted from: Request for Regulation of s Approved by Council April 24, 2015 DEFINITIONS In this policy: Act means The Pharmacy and Pharmacy Disciplines Act means an unregulated
Preventing Adverse Drug Events and Harm
 Preventing Adverse Drug Events and Harm Frank Federico, RPh, IHI Executive Director Steve Meisel, PharmD, IHI Faculty March 27th,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH, Institute
Preventing Adverse Drug Events and Harm Frank Federico, RPh, IHI Executive Director Steve Meisel, PharmD, IHI Faculty March 27th,2012 12:00-1:00pm ET Beth O Donnell, MPH Beth O Donnell, MPH, Institute
Identifying Errors: A Case for Medication Reconciliation Technicians
 Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Organization: Solution Title: Calvert Memorial Hospital Identifying Errors: A Case for Medication Reconciliation Technicians Program/Project Description and Goals: What was the problem to be solved? To
Michigan Medicine--Frankel Cardiovascular Center. Determining Direct Patient Utilization Costs in the Cardiovascular Clinic.
 Michigan Medicine--Frankel Cardiovascular Center Clinical Design and Innovation Determining Direct Patient Utilization Costs in the Cardiovascular Clinic Final Report Client: Mrs. Cathy Twu-Wong Project
Michigan Medicine--Frankel Cardiovascular Center Clinical Design and Innovation Determining Direct Patient Utilization Costs in the Cardiovascular Clinic Final Report Client: Mrs. Cathy Twu-Wong Project
How Pharmacy Informatics and Technology are Evolving to Improve Patient Care
 How Pharmacy Informatics and Technology are Evolving to Improve Patient Care HealthcareIS.com 2 Table of Contents 3 Impact of Emerging Technologies 3 CPOE 5 Automated Dispensing Machines 6 Barcode Medication
How Pharmacy Informatics and Technology are Evolving to Improve Patient Care HealthcareIS.com 2 Table of Contents 3 Impact of Emerging Technologies 3 CPOE 5 Automated Dispensing Machines 6 Barcode Medication
Practice Spotlight. Children's Hospital Central California Madera, California
 Practice Spotlight Children's Hospital Central California Madera, California http://www.childrenscentralcal.org Richard I. Sakai, Pharm.D., FASHP, FCSHP Director of Pharmacy Services IN YOUR VIEW, HOW
Practice Spotlight Children's Hospital Central California Madera, California http://www.childrenscentralcal.org Richard I. Sakai, Pharm.D., FASHP, FCSHP Director of Pharmacy Services IN YOUR VIEW, HOW
Re-Engineering Medication Processes to Capitalize on Technology. Jane Englebright, PhD, RN Vice President, Quality HCA
 Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
Re-Engineering Medication Processes to Capitalize on Technology Jane Englebright, PhD, RN Vice President, Quality HCA Who is HCA? % % % % U.K. % % % Switzerland % %% % % % % % %% % % % % % % % %% % % %
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE)
 COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
COMPUTERIZED PHYSICIAN ORDER ENTRY (CPOE) Ahmed Albarrak 301 Medical Informatics albarrak@ksu.edu.sa 1 Outline Definition and context Why CPOE? Advantages of CPOE Disadvantages of CPOE Outcome measures
Objective Competency Competency Measure To Do List
 2016 University of Washington School of Pharmacy Institutional IPPE Checklist Institutional IPPE Team Contact Info: Kelsey Brantner e-mail: ippe@uw.edu phone: 206-543-9427; Jennifer Danielson, PharmD e-mail:
2016 University of Washington School of Pharmacy Institutional IPPE Checklist Institutional IPPE Team Contact Info: Kelsey Brantner e-mail: ippe@uw.edu phone: 206-543-9427; Jennifer Danielson, PharmD e-mail:
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall. Total. Application Analysis 1.
 Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
Bar Code Medication Administration and MAR Resource Manual
 Bar Code Medication Administration and MAR Resource Manual Administering Medications Administering Meds using CareMobile (PDA)... 2 Viewing Allergies in CareMobile... 8 Determining Which Meds to Give When...
Bar Code Medication Administration and MAR Resource Manual Administering Medications Administering Meds using CareMobile (PDA)... 2 Viewing Allergies in CareMobile... 8 Determining Which Meds to Give When...
BAR CODE MEDICATION ADMINISTRATION: A STRATEGIC TECHNOLOGY INTERVENTION FOR REDUCING HOSPITAL S MEDICATION ERRORS
 Vol. VII No. 2 2016 ISSN : 2087-2879 BAR CODE MEDICATION ADMINISTRATION: A STRATEGIC TECHNOLOGY INTERVENTION FOR REDUCING HOSPITAL S MEDICATION ERRORS Faculty of Nursing, Syiah Kuala University E-mail:
Vol. VII No. 2 2016 ISSN : 2087-2879 BAR CODE MEDICATION ADMINISTRATION: A STRATEGIC TECHNOLOGY INTERVENTION FOR REDUCING HOSPITAL S MEDICATION ERRORS Faculty of Nursing, Syiah Kuala University E-mail:
ABSTRACT. dose", all steps in the setup of the secondary infusion must be conducted correctly.
 MITIGATING RISKS ASSOCIATED WITH SECONDARY INTRAVENOUS (IV) INFUSIONS: AN EMPIRICAL EVALUATION OF A TECHNOLOGY-BASED, A PRACTICE-BASED, AND A TRAINING-BASED INTERVENTION Katherine Y Chan 1,2, Sonia Pinkney
MITIGATING RISKS ASSOCIATED WITH SECONDARY INTRAVENOUS (IV) INFUSIONS: AN EMPIRICAL EVALUATION OF A TECHNOLOGY-BASED, A PRACTICE-BASED, AND A TRAINING-BASED INTERVENTION Katherine Y Chan 1,2, Sonia Pinkney
Medido, a smart medication dispensing solution, shows high rates of medication adherence and potential to reduce cost of care.
 White Paper Medido, a smart medication dispensing solution, shows high rates of medication adherence and potential to reduce cost of care. A Philips Lifeline White Paper Tine Smits, Research Scientist,
White Paper Medido, a smart medication dispensing solution, shows high rates of medication adherence and potential to reduce cost of care. A Philips Lifeline White Paper Tine Smits, Research Scientist,
Introduction. Medication Errors. Objectives. Objectives. January What is a Medication Error? Define medication errors/variances
 Medication Errors Earlene Spence, Pharm.D., Miami VA Healthcare System Neena John, Pharm.D., Miami VA Healthcare System Eva Moreira, Pharm.D., Miami VA Healthcare System Chantal Chan, Pharm.D., Miami VA
Medication Errors Earlene Spence, Pharm.D., Miami VA Healthcare System Neena John, Pharm.D., Miami VA Healthcare System Eva Moreira, Pharm.D., Miami VA Healthcare System Chantal Chan, Pharm.D., Miami VA
Improving the Patient Experience Through Pharmacy
 Rick Burnett Chief Operating Officer Kenneth Maxik Director, Patient Safety & Pharmacy Compliance Improving the Patient Experience Through Pharmacy August 19, 2015 Speakers Rick Burnett, PharmD, FACHE
Rick Burnett Chief Operating Officer Kenneth Maxik Director, Patient Safety & Pharmacy Compliance Improving the Patient Experience Through Pharmacy August 19, 2015 Speakers Rick Burnett, PharmD, FACHE
Achieving safety in medication management through barcoding technology
 Achieving safety in medication management through barcoding technology Kara Marx, RN, FACHE, FHIMSS Vice President of Information Services Sharp Healthcare. SESSION OBJECTIVES Describe the primary activities
Achieving safety in medication management through barcoding technology Kara Marx, RN, FACHE, FHIMSS Vice President of Information Services Sharp Healthcare. SESSION OBJECTIVES Describe the primary activities
Patient Safety Case Study. Clara K. Terral. Angelo State University
 Running Head: PATIENT SAFTEY CASE STUDY Patient Safety Case Study Clara K. Terral Angelo State University PATIENT SAFTEY CASE STUDY 2 The case study that stood out most to me was Case 18, which is Not
Running Head: PATIENT SAFTEY CASE STUDY Patient Safety Case Study Clara K. Terral Angelo State University PATIENT SAFTEY CASE STUDY 2 The case study that stood out most to me was Case 18, which is Not
DEPARTMENT OF HEALTH AND HUMAN SERVICES CENTERS FOR MEDICARE & MEDICAID SERVICES Medication Administration Observation
 : Make random medication observations of several staff over different shifts and units, multiple routes of administration -- oral, enteral, intravenous (IV), intramuscular (IM), subcutaneous (SQ), topical,
: Make random medication observations of several staff over different shifts and units, multiple routes of administration -- oral, enteral, intravenous (IV), intramuscular (IM), subcutaneous (SQ), topical,
Ensuring our safeguarding arrangements act to help and protect adults PRACTICE GUIDANCE FOR REPORTING MEDICATION INCIDENTS INTO SAFEGUARDING
 Ensuring our safeguarding arrangements act to help and protect adults PRACTICE GUIDANCE FOR REPORTING MEDICATION INCIDENTS INTO SAFEGUARDING Contents Page 1.0 Purpose 2 2.0 Definition of medication error
Ensuring our safeguarding arrangements act to help and protect adults PRACTICE GUIDANCE FOR REPORTING MEDICATION INCIDENTS INTO SAFEGUARDING Contents Page 1.0 Purpose 2 2.0 Definition of medication error
PHARMACY SERVICES/MEDICATION USE
 25.01. 10 Drug Reactions & Administration Errors & Incompatibilities. Drug administration errors, adverse drug reactions and incompatibilities must be immediately reported to the attending physician and
25.01. 10 Drug Reactions & Administration Errors & Incompatibilities. Drug administration errors, adverse drug reactions and incompatibilities must be immediately reported to the attending physician and
einteract User Guide July 07, 2017
 einteract User Guide July 07, 2017 This document covers the use of the einteract features in PointClickCare. Table of Contents einteract... 3 einteract Quick Reference Guide... 3 Overview of einteract...
einteract User Guide July 07, 2017 This document covers the use of the einteract features in PointClickCare. Table of Contents einteract... 3 einteract Quick Reference Guide... 3 Overview of einteract...
Patient Centric Model (PCM)
 Patient Centric Model (PCM) Operations Manual A product of your state pharmacy association For more information, contact: PCM Project Manager 804-285-4431 PCM@naspa.us Background The typical pharmacy model
Patient Centric Model (PCM) Operations Manual A product of your state pharmacy association For more information, contact: PCM Project Manager 804-285-4431 PCM@naspa.us Background The typical pharmacy model
Improving the reporting of medication-related safety incidents
 Rationale Improving the reporting of medication-related safety incidents Research shows that organisations which regularly report more patient safety incidents usually have a stronger learning culture
Rationale Improving the reporting of medication-related safety incidents Research shows that organisations which regularly report more patient safety incidents usually have a stronger learning culture
MAR/MEDICATION AUDIT NAME NAME NAME
 MAR/MEDICATION AUDIT NAME NAME NAME DATE Copies of all current prescriptions in file (correlate with MAR, Meds on hand and Healthcare Communication Forms) MAR reflects current correct medications, correct
MAR/MEDICATION AUDIT NAME NAME NAME DATE Copies of all current prescriptions in file (correlate with MAR, Meds on hand and Healthcare Communication Forms) MAR reflects current correct medications, correct
Pharmaceutical Services Instructor s Guide CFR , (a)(b)(1) F425
 Centers for Medicare & Medicaid Services (CMS) Pharmaceutical Services Instructor s Guide CFR 483.60, 483.60(a)(b)(1) F425 2006 Prepared by: American Institutes for Research 1000 Thomas Jefferson St, NW
Centers for Medicare & Medicaid Services (CMS) Pharmaceutical Services Instructor s Guide CFR 483.60, 483.60(a)(b)(1) F425 2006 Prepared by: American Institutes for Research 1000 Thomas Jefferson St, NW
