Education Adopting and adapting clinical guidelines for local use
|
|
|
- Cordelia Griffin
- 5 years ago
- Views:
Transcription
1 Education 2007;9: /toag The Obstetrician & Gynaecologist Education Adopting and adapting clinical guidelines for local use Author Gillian C Penney Key content: Clinical guidelines help to standardise and improve patient care. Development of a valid clinical guideline requires resources and skills. Local adaptation of a national guideline provides a cost-effective approach to guideline introduction. A formal consensus process allows local stakeholders to adapt a national guideline. The adapted guideline combines the rigour of national development with the acceptability engendered by local consensus. Learning objectives: To gain an overview of the fundamental principles of clinical guideline development. To learn how to adapt national guidelines for use by local NHS organisations or by groups of clinicians in non-uk settings. Ethical issues: Guideline introduction diverts scarce resources from direct clinical care. Evidence indicates that guidelines result in only modest to moderate improvements in patient outcomes. Clinicians wishing to introduce clinical guidelines should adopt an approach that minimises resource use. Keywords clinical guidelines / decision making / evidence base Please cite this article as: Penney GC. Adopting and adapting clinical guidelines for local use. The Obstetrician & Gynaecologist 2007;9: Author details Gillian C Penney MD FRCOG FFFP Director Scottish Programme for Clinical Effectiveness in Reproductive Health, Room 64, Aberdeen Maternity Hospital, Cornhill Road, Aberdeen AB25 2ZD, UK g.c.penney@abdn.ac.uk 48
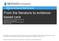
2 The Obstetrician & Gynaecologist 2007;9:48 52 Education Introduction Clinical research continually generates new findings that can contribute to effective and efficient patient care. However, research findings cannot change patient outcomes unless health services and health care professionals adopt them into practice. Recent years have witnessed much progress in the synthesis of evidence. Secondary research in the form of systematic review and metaanalysis endeavours to collate evidence relating to discrete clinical questions. 1 Clinical guidelines summarise available evidence on broader clinical topics, or patient journeys of care, in the form of practice recommendations. Guidelines have the potential to improve patient care by promoting interventions of proven benefit and discouraging ineffective interventions. The National Guideline Clearinghouse (an initiative of the United States Agency for Healthcare Research and Quality) has collated clinical guidelines that meet defined quality criteria from around the world. 2 Similarly, the Guidelines Finder within the National Electronic Library for Health provides a searchable database of quality-assessed guidelines developed by UK organisations. 3 Developing valid clinical guidelines A widely accepted definition of clinical practice guidelines is systematically developed statements to assist practitioner and patient decisions about appropriate health care for specific clinical circumstances. 4 Internationally, numerous agencies have published methodologies for guideline development. These have been collated by the Guidelines International Network. 5 Published methods for development of valid guidelines differ in their detail but all are founded on three essential principles. Firstly, guidelines must be evidencebased, with recommendations based on a systematic review, including critical appraisal, of published literature. Secondly, individual recommendations must be evidence-linked, using a recognised grading scheme that explicitly summarises the type and quality of evidence on which they are based. Thirdly, guideline development must be multidisciplinary, undertaken by a group in which all stakeholders (including patients or service users), for the clinical topic, are represented. The United Kingdom national guideline organisations: the National Institute for Health and Clinical Excellence (NICE) and the Scottish Intercollegiate Guidelines Network (SIGN), have both published comprehensive guides to the development of valid guidelines. NICE has published both an overview of the guideline development process 6 and a detailed web-based technical manual. 7 Similarly, SIGN has published a guideline developers handbook 8 which has a regularly updated web version. 9 The process of guideline development, incorporating the three essential principles (as recommended by SIGN), is summarised in Figure 1. Introducing a clinical guideline In the United Kingdom, clinical guidelines can be developed by NICE and SIGN, by national professional organisations (such as the RCOG), or by teams within local healthcare organisations. Introduction of a clinical guideline into a healthcare setting is a process involving several stages, all of which have resource implications. Moreover, the available body of evidence on the effectiveness of clinical guidelines indicates that improvements in care are only modest to moderate. 10 Therefore,when deciding to introduce a new guideline (whether by de novo guideline development or by adoption of an existing guideline), clinicians and policy makers must give attention to the implications of each stage.advice on all stages of guideline introduction is available from a number of sources, 2,4,7 and is summarised in Box 1. Adopting an existing guideline versus de novo guideline development The literature from the early years of the NHS Clinical Guidelines initiative emphasised the tensions between local and national guideline development. 11,12 Development of a local guideline by a local stakeholder group provides sense of ownership a factor thought to be associated with increased likelihood that the guideline will actually be adopted. Conversely, development by a national expert group provides greater confidence that the content will be valid but less likelihood that the guideline will actually be used in practice. A recent Figure 1 Diagrammatic representation of the development of valid clinical guidelines as recommended by the Scottish Intercollegiate Guidelines Network 49
3 Education 2007;9:48 52 The Obstetrician & Gynaecologist Box 1 Framework to aid decisions by policy makers and clinicians about introducing clinical guidelines Stage of guideline introduction Selection of clinical topic Availability of existing guidelines Guideline adaptation or development Dissemination and implementation Consider resource implications of change Evaluate impact AGREE Appraisal of Guidelines, Research and Evaluation in Europe Activities Consider: local burden of disease availability of effective and efficient healthcare interventions evidence of variation in practice evidence of current suboptimal performance receptivity and preparedness to change as indicated by a network of local stakeholders. Consider the availability, or otherwise, of existing high-quality, cost-conscious guidelines. If such a guideline is available (for example, within the databases of the National Guideline Clearinghouse or the Guidelines International Network), then it may be adapted for local use. Otherwise, the resources required to develop a robust guideline de novo are substantial. Consider using a formal consensus method with a local stakeholder group to endorse or adapt an existing robust guideline. If no existing guideline available and resources permit, develop de novo using a published methodology and self-assessment using the AGREE instrument. Seek resources for implementation: explore sources of funding through partnerships and stakeholders. Identify the most likely barriers to implementation across all levels of healthcare organisation (individual, team, organisational and environmental). Prioritise those which are most important and amenable to change. Identify available intervention options based on available resources and expertise. Seek the best fit between barriers and likely interventions in the light of known evidence of effectiveness and models of behaviour change. Distribute recommendations in paper/electronic format as a minimum. Policy makers and clinicians should be alert to the potential impact on different budgets of changes in practice resulting from adoption of guideline recommendations. Guideline introducers should design a means of evaluating the impact of guideline introduction, for example, by means of related clinical audit. meta-analysis 13 provides further support for externally developed guidelines, showing greater effect sizes for external, rather than local, guidelines after adjusting for other factors. Rigorous guideline development carries significant resource implications and clinicians in local NHS organisations (and those in non-uk settings) often choose to adopt an existing guideline from an authoritative source (for example, an RCOG Clinical Green-top Guideline or one meeting the quality criteria of the National Guideline Clearinghouse) rather than developing their own in-house guideline de novo. The adoption of an existing guideline has advantages: it removes the need for the time and skills-dependent steps of literature search and critical appraisal. However, nationally developed guidelines may not be directly transferable to local NHS organisations (or to non- UK settings): recommendations may refer to services and interventions that are unavailable, or inappropriate, in the target setting. At the Scottish Programme for Clinical Effectiveness in Reproductive Health we have developed an approach for adapting a clinical guideline for setting-specific use. 14 This approach uses a formal consensus development method (the Rand version of the nominal group technique) and is theoretically based. 15 Adaptation using a formal consensus process with a local stakeholder group has advantages over simply adopting a guideline developed nationally. Clinicians, policy makers and service users from the intended setting can bring their local perspectives to the final wording of recommendations, ensuring that these accord with local culture and with available services and interventions. In this approach to guideline adaptation, the benefits of literature search and critical appraisal conducted within the resources of the parent guideline development organisation (for example, the RCOG) are combined with the benefits of input from a multidisciplinary group representing the intended local users. Once a local stakeholder group has agreed that a given topic is appropriate and has identified a rigorously developed guideline that is considered suitable for local adaptation, then the following approach may be used. Consensus method for adapting a national guideline for local use Recruitment of local stakeholder group The local guideline adaptation group should comprise representatives of disciplines similar to those included in the original guideline development group. For a guideline addressing an obstetric topic, the group might include senior and trainee obstetricians, midwives, neonatologists, neonatal nurses, anaesthetists and representatives of a service-user group. An overview of formal consensus methods indicates that a group size of 50
4 The Obstetrician & Gynaecologist 2007;9:48 52 Education between six and 12 participants is optimal. 15 In practice, an appropriate group for guideline adaptation is likely to require nine or 11 participants to ensure that all relevant stakeholders are represented. Consensus questionnaire The Rand consensus method includes private decision making by individual participants using posted questionnaires. As an example, an extract from a consensus questionnaire developed for adaptation of the RCOG Clinical Green-top Guideline No. 21 on the management of tubal pregnancy is shown in Figure 2. Participants are sent the questionnaire in advance of a group meeting and asked to score their level of agreement with each guideline recommendation in terms of suitability for use in their own local setting. Scoring on a ninepoint Likert scale has proved to be practicable. 14 Aggregating the scores The aim of the private decision making step is to achieve consensus agreement with a proportion of guideline recommendations to reduce the number requiring face-to-face discussion at a group meeting. Authorities differ as to what level of agreement constitutes consensus. 15 Purists would argue that consensus has not been achieved unless all participants are in agreement. However, pragmatic consensus rules are acknowledged as acceptable, as long as these rules are pre-agreed at the outset. With a group of 11 participants, consensus may be deemed to have been achieved if nine of the 11 score a recommendation within a three-point band on the nine-point Likert scale. For example, for the recommendation Laparoscopic salpingotomy should be considered as the primary treatment when managing tubal pregnancy in the presence of contralateral tubal disease and the Figure 2 Extract from consensus questionnaire for adaptation of an RCOG Clinical Green-top Guideline for setting-specific use 16 51
5 Education 2007;9:48 52 The Obstetrician & Gynaecologist desire for future fertility, if 10 participants gave it an agreement score of 7, 8 or 9 and the remaining participant gave it a score of 5, then this would be deemed consensus agreement with the recommendation. Conversely, for the recommendation Expectant management is an option for clinically stable women with minimal symptoms and a pregnancy of unknown location, if eight participants gave it an agreement score of 7, 8 or 9 and the remaining participants gave scores of 2 or 3, there is no consensus and the recommendation requires face-to-face discussion. During a guideline adaptation exercise, postal questionnaires are returned to a central point and scores aggregated as described above. We have applied this approach with groups of clinicians in the UK, Iraq and Sri Lanka. Generally, the private decision making exercise results in consensus agreement with most of the recommendations in the original guideline; these can then be adopted for the local setting without modification. A minority of recommendations will remain for which the adaptation group have reached no consensus or a consensus of disagreement (at least nine participants giving a score of 1, 2 or 3): these require face-to-face discussion and local modification. The formal Rand consensus method elicits private decisions using posted questionnaires as described above. However, we have also used this approach successfully in a workshop format with private decision making taking place at the beginning of the meeting, scores being aggregated on site and face-to-face discussion taking place thereafter. Modification of contentious recommendations Following the consensus questionnaire exercise a limited number of recommendations will require group discussion and modification. For each of these the evidence base for the recommendation (as presented in the original guideline) should be reviewed and options for modified wording explored. Often, necessary modifications will be easily resolved (for example, replacement of the term NHS by a term that describes the local healthcare system, or substitution of a drug that is unavailable locally). In modifying recommendations, caution is required to ensure that key points of evidence are not ignored because they are deemed inappropriate locally. Repeat private decision making If time and resources permit, a second consensus questionnaire should be compiled containing all recommendations in the adapted guideline (those which achieved consensus agreement in the first survey and those for which the wording was modified at the face-to-face meeting). Participants should then score their level of agreement with each using the nine-point Likert scale to demonstrate that consensus has been achieved for all recommendations in the final adapted guideline. In practice, the modifications required may be few in number and minor in nature. In this case, agreement on the adapted guideline may be achieved by informal consensus at the end of the face-to-face meeting. The use of an explicit and transparent consensus process permits adaptation of a clinical guideline developed nationally for one healthcare system for use at the level of a local NHS organisation or a different healthcare system. Such adaptation results in a valid guideline that adheres to the three fundamental principles: it is evidence-based; recommendations are evidence-linked (drawing on structured literature review and critical appraisal undertaken by the parent guideline developers); and it incorporates multidisciplinary input from a local stakeholder group. References 1 The Cochrane Collaboration. [ 2 National Guideline Clearinghouse. [ 3 National Electronic Library for Health. [ guidelinesfinder/]. 4 Field MJ, Lohr K, editors. Clinical Practice Guidelines: Directions fora New Program. Washington, DC: National Academy Publishing; Guidelines International Network. [ 6 National Institute for Health and Clinical Excellence. The Guideline Development Process. An Overview forstakeholders, the Public and the NHS. 2nd ed. London: NICE; [ page.aspx?o=guidelinesprocess]. 7 National Institute for Health and Clinical Excellence. The Guidelines Manual London: NICE; [ page.aspx?o=308639]. 8 Scottish Intercollegiate Guidelines Network. Sign 50: a Guideline Developers Handbook. Edinburgh: SIGN; Scottish Intercollegiate Guidelines Network. [ 10 Grimshaw JM, Thomas RE, MacLennan G, Fraser C, Ramsay CR, Vale L, et al. Effectiveness and efficiency of guideline dissemination and implementation strategies. Health Technol Assess 2004;8:iii iv, Mann T. Clinical Guidelines: Using Clinical Guidelines to Improve Patient Care within the NHS. NHS Executive; p Grimshaw J, Eccles M, Russell I. Developing clinically valid practice guidelines. J Eval Clin Pract 1995;1: Dijkstra R, Wensing M, Thomas R, Akkermans R, Braspenning J, Grimshaw J, et al. The relationship between organisational characteristics and the effects of clinical guidelines on medical performance in hospitals, a meta-analysis. BMC Health Serv Res 2006;6:53. doi: / Glasier A, Brechin S, Raine R, Penney G. A consensus process to adapt the World Health Organization selected practice recommendations for UK use. Contraception 2003;68: doi: /j.contraception Murphy MK, Black NA, Lamping DL, McKee CM, Sanderson CFB, Askham J, et al. Consensus development methods, and their use in clinical guideline development. Health Technol Assess 1998:2:i iv, Royal College of Obstetricians and Gynaecologists. The Management of Tubal Pregnancy. Clinical Green-Top Guideline No. 21. London: RCOG Press;
Draft National Quality Assurance Criteria for Clinical Guidelines
 Draft National Quality Assurance Criteria for Clinical Guidelines Consultation document July 2011 1 About the The is the independent Authority established to drive continuous improvement in Ireland s health
Draft National Quality Assurance Criteria for Clinical Guidelines Consultation document July 2011 1 About the The is the independent Authority established to drive continuous improvement in Ireland s health
NICE Charter Who we are and what we do
 NICE Charter 2017 Who we are and what we do 1. The National Institute for Health and Care Excellence (NICE) is the independent organisation responsible for providing evidence-based guidance on health and
NICE Charter 2017 Who we are and what we do 1. The National Institute for Health and Care Excellence (NICE) is the independent organisation responsible for providing evidence-based guidance on health and
British Society for Surgery of the Hand. (BSSH) Evidence for Surgical
 British Society for Surgery of the Hand (BSSH) Evidence for Surgical Treatment (B.E.S.T.) Process Manual 1 st Edition (12 th version, November 2016) Review Date: November 2019 BSSH Evidence for Surgical
British Society for Surgery of the Hand (BSSH) Evidence for Surgical Treatment (B.E.S.T.) Process Manual 1 st Edition (12 th version, November 2016) Review Date: November 2019 BSSH Evidence for Surgical
NHS. The guideline development process: an overview for stakeholders, the public and the NHS. National Institute for Health and Clinical Excellence
 NHS National Institute for Health and Clinical Excellence Issue date: April 2007 The guideline development process: an overview for stakeholders, the public and the NHS Third edition The guideline development
NHS National Institute for Health and Clinical Excellence Issue date: April 2007 The guideline development process: an overview for stakeholders, the public and the NHS Third edition The guideline development
Effectively implementing multidisciplinary. population segments. A rapid review of existing evidence
 Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Clinical Practice Guideline Development Manual
 Clinical Practice Guideline Development Manual Publication Date: September 2016 Review Date: September 2021 Table of Contents 1. Background... 3 2. NICE accreditation... 3 3. Patient Involvement... 3 4.
Clinical Practice Guideline Development Manual Publication Date: September 2016 Review Date: September 2021 Table of Contents 1. Background... 3 2. NICE accreditation... 3 3. Patient Involvement... 3 4.
Process and methods Published: 30 November 2012 nice.org.uk/process/pmg6
 The guidelines manual Process and methods Published: 30 November 2012 nice.org.uk/process/pmg6 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
The guidelines manual Process and methods Published: 30 November 2012 nice.org.uk/process/pmg6 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Clinical audit: a guide
 Clinical audit: a guide All nurses are expected to take part in clinical audits. Stephen Ashmore and Tracy Ruthven explain how it should be done HEALTHCARE PROFESSIONALS across the NHS are being encouraged
Clinical audit: a guide All nurses are expected to take part in clinical audits. Stephen Ashmore and Tracy Ruthven explain how it should be done HEALTHCARE PROFESSIONALS across the NHS are being encouraged
Evidence Based Guidelines for
 Evidence Based Guidelines for Midwifery-Led Care in Labour Date Issued: November 2012 Review date: November 2016 The Royal College of Midwives (RCM) has a fundamental role in promoting the midwifery profession
Evidence Based Guidelines for Midwifery-Led Care in Labour Date Issued: November 2012 Review date: November 2016 The Royal College of Midwives (RCM) has a fundamental role in promoting the midwifery profession
A systematic review to examine the evidence regarding discussions by midwives, with women, around their options for where to give birth
 A systematic review to examine the evidence regarding discussions by midwives, with women, around their options for where to give birth Cathy Shneerson, Lead Researcher Beck Taylor, Co-researcher Sara
A systematic review to examine the evidence regarding discussions by midwives, with women, around their options for where to give birth Cathy Shneerson, Lead Researcher Beck Taylor, Co-researcher Sara
Final Accreditation Report
 Guidance producer: The Royal College of Physicians of London Guidance product: National Clinical Guideline for Stroke Date: 19 September 2016 Version: 1.2 Final Accreditation Report Report Page 1 of 21
Guidance producer: The Royal College of Physicians of London Guidance product: National Clinical Guideline for Stroke Date: 19 September 2016 Version: 1.2 Final Accreditation Report Report Page 1 of 21
NES Patient Safety Programme. Human Factors in Healthcare. NES Educational Developments and Resources
 NES Patient Safety Programme Human Factors in Healthcare NES Educational Developments and Resources Introduction The three Quality Ambitions articulated in the Healthcare Quality Strategy include a focus
NES Patient Safety Programme Human Factors in Healthcare NES Educational Developments and Resources Introduction The three Quality Ambitions articulated in the Healthcare Quality Strategy include a focus
The Renal Association
 Guidance producer: The Renal Association Guidance product: Clinical Practice Guidelines Date: 11 January 2017 Version: 1.4 Final Accreditation Report Contents Introduction... 3 Accreditation recommendation...
Guidance producer: The Renal Association Guidance product: Clinical Practice Guidelines Date: 11 January 2017 Version: 1.4 Final Accreditation Report Contents Introduction... 3 Accreditation recommendation...
Final Accreditation Report
 Guidance producer: Healthcare Infection Society Guidance product: Clinical Guidelines Date: 23 March 2015 Version: 1.6 Final Accreditation Report Page 1 of 19 Contents Introduction... 3 Accreditation recommendation...
Guidance producer: Healthcare Infection Society Guidance product: Clinical Guidelines Date: 23 March 2015 Version: 1.6 Final Accreditation Report Page 1 of 19 Contents Introduction... 3 Accreditation recommendation...
From the literature to evidencebased
 Medicine, Nursing and Health Sciences From the literature to evidencebased care Sue Brennan, PhD Sue.brennan@monash.edu Australasian Cochrane Centre, School of Public Health & Preventive Medicine Monash
Medicine, Nursing and Health Sciences From the literature to evidencebased care Sue Brennan, PhD Sue.brennan@monash.edu Australasian Cochrane Centre, School of Public Health & Preventive Medicine Monash
Supporting information for appraisal and revalidation: guidance for pharmaceutical medicine
 Supporting information for appraisal and revalidation: guidance for pharmaceutical medicine Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction The purpose
Supporting information for appraisal and revalidation: guidance for pharmaceutical medicine Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction The purpose
Document Details Clinical Audit Policy
 Title Document Details Clinical Audit Policy Trust Ref No 1538-31104 Main points this document covers This policy details the responsibilities and processes associated with the Clinical Audit process within
Title Document Details Clinical Audit Policy Trust Ref No 1538-31104 Main points this document covers This policy details the responsibilities and processes associated with the Clinical Audit process within
National Institute for Health and Clinical Excellence. The guidelines manual
 National Institute for Health and Clinical Excellence The guidelines manual January 2009 The guidelines manual About this document This document describes the methods used in the development of NICE guidelines.
National Institute for Health and Clinical Excellence The guidelines manual January 2009 The guidelines manual About this document This document describes the methods used in the development of NICE guidelines.
Quality Management in Pharmacy Pre-registration Training: Current Practice
 Pharmacy Education, 2013; 13 (1): 82-86 Quality Management in Pharmacy Pre-registration Training: Current Practice ELIZABETH MILLS 1*, ALISON BLENKINSOPP 2, PATRICIA BLACK 3 1 Postgraduate Academic Course
Pharmacy Education, 2013; 13 (1): 82-86 Quality Management in Pharmacy Pre-registration Training: Current Practice ELIZABETH MILLS 1*, ALISON BLENKINSOPP 2, PATRICIA BLACK 3 1 Postgraduate Academic Course
Nurse Consultant Impact: Wales Workshop report
 Nurse Consultant Impact: Wales Workshop report Background Nurse Consultant (NC) posts were established in the United Kingdom in 2000 as part of the modernisation agenda for the NHS. The roles were intended
Nurse Consultant Impact: Wales Workshop report Background Nurse Consultant (NC) posts were established in the United Kingdom in 2000 as part of the modernisation agenda for the NHS. The roles were intended
How NICE clinical guidelines are developed
 Issue date: January 2009 How NICE clinical guidelines are developed: an overview for stakeholders, the public and the NHS Fourth edition : an overview for stakeholders, the public and the NHS Fourth edition
Issue date: January 2009 How NICE clinical guidelines are developed: an overview for stakeholders, the public and the NHS Fourth edition : an overview for stakeholders, the public and the NHS Fourth edition
Public Health Skills and Career Framework Multidisciplinary/multi-agency/multi-professional. April 2008 (updated March 2009)
 Public Health Skills and Multidisciplinary/multi-agency/multi-professional April 2008 (updated March 2009) Welcome to the Public Health Skills and I am delighted to launch the UK-wide Public Health Skills
Public Health Skills and Multidisciplinary/multi-agency/multi-professional April 2008 (updated March 2009) Welcome to the Public Health Skills and I am delighted to launch the UK-wide Public Health Skills
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Interim Process and Methods of the Highly Specialised Technologies Programme
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Principles Interim Process and Methods of the Highly Specialised Technologies Programme 1. Our guidance production processes are based on key principles,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Principles Interim Process and Methods of the Highly Specialised Technologies Programme 1. Our guidance production processes are based on key principles,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Health and Social Care Directorate Quality standards Process guide
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health and Social Care Directorate Quality standards Process guide December 2014 Quality standards process guide Page 1 of 44 About this guide This guide
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health and Social Care Directorate Quality standards Process guide December 2014 Quality standards process guide Page 1 of 44 About this guide This guide
NHS QIS & NICE Advice. defi nitions & status
 NHS QIS & NICE Advice defi nitions & status NHS Quality Improvement Scotland 2006 First published August 2006 You can copy or reproduce the information in this document for use within NHSScotland and for
NHS QIS & NICE Advice defi nitions & status NHS Quality Improvement Scotland 2006 First published August 2006 You can copy or reproduce the information in this document for use within NHSScotland and for
How to use NICE guidance to commission high-quality services
 How to use NICE guidance to commission high-quality services Acknowledgement We are grateful to the many organisations and individuals who have contributed to the development of this guide. A list of these
How to use NICE guidance to commission high-quality services Acknowledgement We are grateful to the many organisations and individuals who have contributed to the development of this guide. A list of these
Engaging clinicians in improving data quality in the NHS
 Engaging clinicians in improving data quality in the NHS Key findings and recommendations from research conducted by the Royal College of Physicians ilab September 2006 Summary This document summarises
Engaging clinicians in improving data quality in the NHS Key findings and recommendations from research conducted by the Royal College of Physicians ilab September 2006 Summary This document summarises
Supporting information for appraisal and revalidation: guidance for Supporting information for appraisal and revalidation: guidance for ophthalmology
 FOREWORD As part of revalidation, doctors will need to collect and bring to their appraisal six types of supporting information to show how they are keeping up to date and fit to practise. The GMC has
FOREWORD As part of revalidation, doctors will need to collect and bring to their appraisal six types of supporting information to show how they are keeping up to date and fit to practise. The GMC has
GUIDANCE ON SUPPORTING INFORMATION FOR REVALIDATION FOR SURGERY
 ON SUPPORTING INFORMATION FOR REVALIDATION FOR SURGERY Based on the Academy of Medical Royal Colleges and Faculties Core Guidance for all doctors GENERAL INTRODUCTION JUNE 2012 The purpose of revalidation
ON SUPPORTING INFORMATION FOR REVALIDATION FOR SURGERY Based on the Academy of Medical Royal Colleges and Faculties Core Guidance for all doctors GENERAL INTRODUCTION JUNE 2012 The purpose of revalidation
Process and methods Published: 23 January 2017 nice.org.uk/process/pmg31
 Evidence summaries: process guide Process and methods Published: 23 January 2017 nice.org.uk/process/pmg31 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Evidence summaries: process guide Process and methods Published: 23 January 2017 nice.org.uk/process/pmg31 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Assessing Non-Technical Skills. A Guide to the NOTSS Tool Adapted for the Labour Ward
 Assessing Non-Technical Skills A Guide to the NOTSS Tool Adapted for the Labour Ward Acknowledgements The original NOTSS system was developed and evaluated in a multi-disciplinary project comprising surgeons,
Assessing Non-Technical Skills A Guide to the NOTSS Tool Adapted for the Labour Ward Acknowledgements The original NOTSS system was developed and evaluated in a multi-disciplinary project comprising surgeons,
IMPROVING QUALITY. Clinical Governance Strategy & Framework
 IMPROVING QUALITY Clinical Governance Strategy & Framework NHS GREATER GLASGOW & CLYDE Approval: Quality & Performance Committee Responsible Director: Medical Director Custodian: Head of Clinical Governance
IMPROVING QUALITY Clinical Governance Strategy & Framework NHS GREATER GLASGOW & CLYDE Approval: Quality & Performance Committee Responsible Director: Medical Director Custodian: Head of Clinical Governance
Supporting information for appraisal and revalidation: guidance for psychiatry
 Supporting information for appraisal and revalidation: guidance for psychiatry Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction The purpose of revalidation
Supporting information for appraisal and revalidation: guidance for psychiatry Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction The purpose of revalidation
Nursing skill mix and staffing levels for safe patient care
 EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
Maximising the impact of nursing research. RCN research conference 5-7 April 2017, Oxford, UK
 Maximising the impact of nursing research RCN research conference 5-7 April 2017, Oxford, UK Paper 1 Maximising the Impact of nursing research through collaboration Professor Daniel Kelly, RCN Professor
Maximising the impact of nursing research RCN research conference 5-7 April 2017, Oxford, UK Paper 1 Maximising the Impact of nursing research through collaboration Professor Daniel Kelly, RCN Professor
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Medicines concordance and adherence: involving adults and carers in decisions about prescribed medicines 1.1 Short title Medicines
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Medicines concordance and adherence: involving adults and carers in decisions about prescribed medicines 1.1 Short title Medicines
JBI Database of Systematic Reviews & Implementation Reports 2013;11(8) 84-96
 Competencies and skills to enable effective care of severely obese patients undergoing bariatric surgery across a multi-disciplinary health care perspective: a systematic review protocol Audrey Stephen
Competencies and skills to enable effective care of severely obese patients undergoing bariatric surgery across a multi-disciplinary health care perspective: a systematic review protocol Audrey Stephen
Final Accreditation Report
 Guidance producer: Royal College of Surgeons of England: Surgical Specialty Associations Guidance product: Clinical Commissioning Guides Date: 28 February 2013 Version: 1.3 Final Accreditation Report Royal
Guidance producer: Royal College of Surgeons of England: Surgical Specialty Associations Guidance product: Clinical Commissioning Guides Date: 28 February 2013 Version: 1.3 Final Accreditation Report Royal
Supporting information for appraisal and revalidation: guidance for Occupational Medicine, June 2014
 Supporting information for appraisal and revalidation: guidance for Occupational Medicine, June 2014 Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction
Supporting information for appraisal and revalidation: guidance for Occupational Medicine, June 2014 Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction
LIBERATING THE NHS: COMMISSIONING FOR PATIENTS. The Royal College of Obstetricians and Gynaecologists:
 Direct telephone: +44 (0) 20 7772 6369 Direct facsimile: +44 (0) 20 7772 6232 Email: cdhillon@rcog.org.uk 8 October 2010 LIBERATING THE NHS: COMMISSIONING FOR PATIENTS Key Points The Royal College of Obstetricians
Direct telephone: +44 (0) 20 7772 6369 Direct facsimile: +44 (0) 20 7772 6232 Email: cdhillon@rcog.org.uk 8 October 2010 LIBERATING THE NHS: COMMISSIONING FOR PATIENTS Key Points The Royal College of Obstetricians
HEALTH AND CARE (STAFFING) (SCOTLAND) BILL
 HEALTH AND CARE (STAFFING) (SCOTLAND) BILL POLICY MEMORANDUM INTRODUCTION 1. As required under Rule 9.3.3 of the Parliament s Standing Orders, this Policy Memorandum is published to accompany the Health
HEALTH AND CARE (STAFFING) (SCOTLAND) BILL POLICY MEMORANDUM INTRODUCTION 1. As required under Rule 9.3.3 of the Parliament s Standing Orders, this Policy Memorandum is published to accompany the Health
Supporting information for appraisal and revalidation: guidance for Occupational Medicine, April 2013
 Supporting information for appraisal and revalidation: guidance for Occupational Medicine, April 2013 Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction
Supporting information for appraisal and revalidation: guidance for Occupational Medicine, April 2013 Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors. General Introduction
ADVANCED NURSE PRACTITIONER STRATEGY
 ADVANCED NURSE PRACTITIONER STRATEGY 2016-2020 Lead Manager: Chair, GG&C Advanced Practice Group Responsible Director: Board Nurse Director Approved by: NMAHP Group Date approved Date for review: September
ADVANCED NURSE PRACTITIONER STRATEGY 2016-2020 Lead Manager: Chair, GG&C Advanced Practice Group Responsible Director: Board Nurse Director Approved by: NMAHP Group Date approved Date for review: September
SPONSORSHIP AND JOINT WORKING WITH THE PHARMACEUTICAL INDUSTRY
 SPONSORSHIP AND JOINT WORKING WITH THE PHARMACEUTICAL INDUSTRY 1 SUMMARY This document sets out Haringey Clinical Commissioning Group policy and advice to employees on sponsorship and joint working with
SPONSORSHIP AND JOINT WORKING WITH THE PHARMACEUTICAL INDUSTRY 1 SUMMARY This document sets out Haringey Clinical Commissioning Group policy and advice to employees on sponsorship and joint working with
Wandsworth CCG. Continuing Healthcare Commissioning Policy
 Wandsworth CCG Continuing Healthcare Commissioning Policy Document Control Title Originator/author: Approval Body Wandsworth CCG Continuing Healthcare Commissioning Policy Alison Kirby / Munya Nhamo Wandsworth
Wandsworth CCG Continuing Healthcare Commissioning Policy Document Control Title Originator/author: Approval Body Wandsworth CCG Continuing Healthcare Commissioning Policy Alison Kirby / Munya Nhamo Wandsworth
National Enhanced Service (NES) for Intra-uterine contraceptive device fittings and contraceptive implants
 National Enhanced Service (NES) for Intra-uterine contraceptive device fittings and contraceptive implants Service Level Agreement PRACTICE Contents: 1. Finance Details 2. Signature Sheet 3. Service Aims
National Enhanced Service (NES) for Intra-uterine contraceptive device fittings and contraceptive implants Service Level Agreement PRACTICE Contents: 1. Finance Details 2. Signature Sheet 3. Service Aims
Building an infrastructure to improve cardiac rehabilitation: from guidelines to audit and feedback Verheul, M.M.
 UvA-DARE (Digital Academic Repository) Building an infrastructure to improve cardiac rehabilitation: from guidelines to audit and feedback Verheul, M.M. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Building an infrastructure to improve cardiac rehabilitation: from guidelines to audit and feedback Verheul, M.M. Link to publication Citation for published version
Final Accreditation Report
 Guidance producer: Resuscitation Council (UK) Guidance product: 2010 resuscitation guidelines Date: 2 August 2012 Version: 1.4 Final Accreditation Report Page 1 of 19 Contents Introduction... 3 Accreditation
Guidance producer: Resuscitation Council (UK) Guidance product: 2010 resuscitation guidelines Date: 2 August 2012 Version: 1.4 Final Accreditation Report Page 1 of 19 Contents Introduction... 3 Accreditation
Prevention and control of healthcare-associated infections
 Prevention and control of healthcare-associated infections Quality improvement guide Issued: November 2011 NICE public health guidance 36 guidance.nice.org.uk/ph36 NHS Evidence has accredited the process
Prevention and control of healthcare-associated infections Quality improvement guide Issued: November 2011 NICE public health guidance 36 guidance.nice.org.uk/ph36 NHS Evidence has accredited the process
Clinical guideline for the prevention and treatment of osteoporosis
 Guidance producer: National Osteoporosis Guideline Group Guidance product: Clinical guideline for the prevention and treatment of osteoporosis Date: 9 March 2017 Version: 1.3 Final Accreditation Report
Guidance producer: National Osteoporosis Guideline Group Guidance product: Clinical guideline for the prevention and treatment of osteoporosis Date: 9 March 2017 Version: 1.3 Final Accreditation Report
Views and counter views Experiences of a 24-hour resident consultant service
 10.1576/toag.10.2.107.27399 www.rcog.org.uk/togonline Experiences of a 24-hour resident consultant service Author Simon Edmonds / Keith Allenby Key content: The Royal College of Obstetricians and Gynaecologists
10.1576/toag.10.2.107.27399 www.rcog.org.uk/togonline Experiences of a 24-hour resident consultant service Author Simon Edmonds / Keith Allenby Key content: The Royal College of Obstetricians and Gynaecologists
TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines
 TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines DATE: 05 June 2015 CONTEXT AND POLICY ISSUES Breaking drug tablets is a common practice referred to as pill
TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines DATE: 05 June 2015 CONTEXT AND POLICY ISSUES Breaking drug tablets is a common practice referred to as pill
Janet E Squires 1,2*, Katrina Sullivan 2, Martin P Eccles 3, Julia Worswick 4 and Jeremy M Grimshaw 2,5
 Squires et al. Implementation Science 2014, 9:152 Implementation Science SYSTEMATIC REVIEW Open Access Are multifaceted s more effective than single-component s in changing health-care professionals behaviours?
Squires et al. Implementation Science 2014, 9:152 Implementation Science SYSTEMATIC REVIEW Open Access Are multifaceted s more effective than single-component s in changing health-care professionals behaviours?
NHS SERVICE DELIVERY AND ORGANISATION R&D PROGRAMME
 NHS SERVICE DELIVERY AND ORGANISATION R&D PROGRAMME PROGRAMME OF RESEARCH ON ACCESS TO HEALTH CARE A Empirical studies to evaluate innovations to improve access repeat call B Empirical study of priority
NHS SERVICE DELIVERY AND ORGANISATION R&D PROGRAMME PROGRAMME OF RESEARCH ON ACCESS TO HEALTH CARE A Empirical studies to evaluate innovations to improve access repeat call B Empirical study of priority
Short Report How to do a Scoping Exercise: Continuity of Care Kathryn Ehrich, Senior Researcher/Consultant, Tavistock Institute of Human Relations.
 Short Report How to do a Scoping Exercise: Continuity of Care Kathryn Ehrich, Senior Researcher/Consultant, Tavistock Institute of Human Relations. short report George K Freeman, Professor of General Practice,
Short Report How to do a Scoping Exercise: Continuity of Care Kathryn Ehrich, Senior Researcher/Consultant, Tavistock Institute of Human Relations. short report George K Freeman, Professor of General Practice,
Delivering the QIPP programme: making existing services improve patient outcomes
 Delivering the QIPP programme: making existing services improve patient outcomes Produced by Glyn Davies MP, Chair All-Party Parliamentary Group on AF in association with the Atrial Fibrillation Association
Delivering the QIPP programme: making existing services improve patient outcomes Produced by Glyn Davies MP, Chair All-Party Parliamentary Group on AF in association with the Atrial Fibrillation Association
Guidance on supporting information for revalidation
 Guidance on supporting information for revalidation Including specialty-specific information for medical examiners (of the cause of death) General introduction The purpose of revalidation is to assure
Guidance on supporting information for revalidation Including specialty-specific information for medical examiners (of the cause of death) General introduction The purpose of revalidation is to assure
CHSD. Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary. Centre for Health Service Development
 CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
Booklet to support competence in the administration of Intranasal Flu Vaccine
 Administration of the Intranasal Flu Vaccine by Healthcare Support Workers (Level 3 and 4 on the NHS Career Framework) to children in a school setting* Booklet to support competence in the administration
Administration of the Intranasal Flu Vaccine by Healthcare Support Workers (Level 3 and 4 on the NHS Career Framework) to children in a school setting* Booklet to support competence in the administration
JOB DESCRIPTION 1. JOB IDENTIFICATION. Job Title: Trainee Health Psychologist
 JOB DESCRIPTION 1. JOB IDENTIFICATION Job Title: Trainee Health Psychologist Responsible to: Professional and Clinical Accountability to lead NHS Psychologist Stage 2 accountability to BPS accredited Health
JOB DESCRIPTION 1. JOB IDENTIFICATION Job Title: Trainee Health Psychologist Responsible to: Professional and Clinical Accountability to lead NHS Psychologist Stage 2 accountability to BPS accredited Health
Quality of Care Approach Quality assurance to drive improvement
 Quality of Care Approach Quality assurance to drive improvement December 2017 We are committed to equality and diversity. We have assessed this framework for likely impact on the nine equality protected
Quality of Care Approach Quality assurance to drive improvement December 2017 We are committed to equality and diversity. We have assessed this framework for likely impact on the nine equality protected
Assessing competence during professional experience placements for undergraduate nursing students: a systematic review
 University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
Methods: Commissioning through Evaluation
 Methods: Commissioning through Evaluation NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Commissioning Strategy
Methods: Commissioning through Evaluation NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Commissioning Strategy
A systematic review of the literature: executive summary
 A systematic review of the literature: executive summary October 2008 The effectiveness of interventions for reducing ambulatory sensitive hospitalisations: a systematic review Arindam Basu David Brinson
A systematic review of the literature: executive summary October 2008 The effectiveness of interventions for reducing ambulatory sensitive hospitalisations: a systematic review Arindam Basu David Brinson
Internal Audit. Health and Safety Governance. November Report Assessment
 November 2015 Report Assessment G G G A G This report has been prepared solely for internal use as part of NHS Lothian s internal audit service. No part of this report should be made available, quoted
November 2015 Report Assessment G G G A G This report has been prepared solely for internal use as part of NHS Lothian s internal audit service. No part of this report should be made available, quoted
Facing the Future: Standards for Paediatric Services. April 2011
 Facing the Future: Standards for Paediatric Services April 2011 Facing the Future: Standards for Paediatric Services April 2011 (First Published December 2010 and amended by RCPCH Council March 2011) 2011
Facing the Future: Standards for Paediatric Services April 2011 Facing the Future: Standards for Paediatric Services April 2011 (First Published December 2010 and amended by RCPCH Council March 2011) 2011
Staffing of Obstetric Theatres
 Staffing of Obstetric Theatres A Consensus Statement May 2009 Staffing of Obstetric Theatres A Consensus Statement In recent years, there has been an increase in the proportion of births by caesarean section
Staffing of Obstetric Theatres A Consensus Statement May 2009 Staffing of Obstetric Theatres A Consensus Statement In recent years, there has been an increase in the proportion of births by caesarean section
Newborn Screening Programmes in the United Kingdom
 Newborn Screening Programmes in the United Kingdom This paper has been developed to increase awareness with Ministers, Members of Parliament and the Department of Health of the issues surrounding the serious
Newborn Screening Programmes in the United Kingdom This paper has been developed to increase awareness with Ministers, Members of Parliament and the Department of Health of the issues surrounding the serious
Organisational factors that influence waiting times in emergency departments
 ACCESS TO HEALTH CARE NOVEMBER 2007 ResearchSummary Organisational factors that influence waiting times in emergency departments Waiting times in emergency departments are important to patients and also
ACCESS TO HEALTH CARE NOVEMBER 2007 ResearchSummary Organisational factors that influence waiting times in emergency departments Waiting times in emergency departments are important to patients and also
Section 2: Advanced level nursing practice competencies
 Advanced Level Nursing Practice Section 2: Advanced level nursing practice competencies RCN Standards for advanced level nursing practice, advanced nurse practitioners, RCN accreditation and RCN credentialing
Advanced Level Nursing Practice Section 2: Advanced level nursing practice competencies RCN Standards for advanced level nursing practice, advanced nurse practitioners, RCN accreditation and RCN credentialing
City, University of London Institutional Repository
 City Research Online City, University of London Institutional Repository Citation: Rayment, J., McCourt, C., Rance, S. & Sandall, J. (2015). What makes alongside midwifery-led units work? Lessons from
City Research Online City, University of London Institutional Repository Citation: Rayment, J., McCourt, C., Rance, S. & Sandall, J. (2015). What makes alongside midwifery-led units work? Lessons from
INTRODUCTION TO THE UK PUBLIC HEALTH REGISTER ROUTE TO REGISTRATION FOR PUBLIC HEALTH PRACTITIONERS
 INTRODUCTION TO THE UK PUBLIC HEALTH REGISTER ROUTE TO REGISTRATION FOR PUBLIC HEALTH PRACTITIONERS This introduction consists of: 1. Introduction to the UK Public Health Register 2. Process and Structures
INTRODUCTION TO THE UK PUBLIC HEALTH REGISTER ROUTE TO REGISTRATION FOR PUBLIC HEALTH PRACTITIONERS This introduction consists of: 1. Introduction to the UK Public Health Register 2. Process and Structures
The Rx for Change database: a first-in-class tool for optimal prescribing and medicines use
 Implementation Science METHODOLOGY Open Access The Rx for Change database: a first-in-class tool for optimal prescribing and medicines use Michelle C Weir 1, Rebecca Ryan 2, Alain Mayhew 1, Julia Worswick
Implementation Science METHODOLOGY Open Access The Rx for Change database: a first-in-class tool for optimal prescribing and medicines use Michelle C Weir 1, Rebecca Ryan 2, Alain Mayhew 1, Julia Worswick
Post-doctoral fellowships
 Guidance for applicants Post-doctoral fellowships Applicants should read this guidance in full before preparing an application and refer to the relevant sections at the time of completing the online application
Guidance for applicants Post-doctoral fellowships Applicants should read this guidance in full before preparing an application and refer to the relevant sections at the time of completing the online application
emja: Measuring patient-reported outcomes: moving from clinical trials into clinical p...
 Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
London Councils: Diabetes Integrated Care Research
 London Councils: Diabetes Integrated Care Research SUMMARY REPORT Date: 13 th September 2011 In partnership with Contents 1 Introduction... 4 2 Opportunities within the context of health & social care
London Councils: Diabetes Integrated Care Research SUMMARY REPORT Date: 13 th September 2011 In partnership with Contents 1 Introduction... 4 2 Opportunities within the context of health & social care
High Level Pharmaceutical Forum
 High Level Pharmaceutical Forum 2005-2008 Final Conclusions and Recommendations of the High Level Pharmaceutical Forum On 2 nd October 2008, the High Level Pharmaceutical Forum agreed on the following
High Level Pharmaceutical Forum 2005-2008 Final Conclusions and Recommendations of the High Level Pharmaceutical Forum On 2 nd October 2008, the High Level Pharmaceutical Forum agreed on the following
Nursing & Midwifery Innovation and Information Event 28/11/2014
 Perineal Repair by Midwives in Ireland: A National Survey of Skills, Knowledge and Experience Triona Cowman Director of the Centre for Midwifery Education Margaret Dunlea Assistant Professor in Midwifery
Perineal Repair by Midwives in Ireland: A National Survey of Skills, Knowledge and Experience Triona Cowman Director of the Centre for Midwifery Education Margaret Dunlea Assistant Professor in Midwifery
British Association of Dermatologists
 Guidance producer: British Association of Dermatologists Guidance product: Service Guidance and Standards Date: 13 March 2017 Version: 1.2 Final Accreditation Report Page 1 of 26 Contents Introduction...
Guidance producer: British Association of Dermatologists Guidance product: Service Guidance and Standards Date: 13 March 2017 Version: 1.2 Final Accreditation Report Page 1 of 26 Contents Introduction...
Methods: National Clinical Policies
 Methods: National Clinical Policies Choose an item. NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Commissioning
Methods: National Clinical Policies Choose an item. NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops. Commissioning
During the one session on value based assessment (VBA), the audience heard from 3 speakers:
 The chair of NICE, David Haslam, initiated the conference by focussing on the importance of NICE and other health technology assessment (HTA) bodies in terms of the need for technology appraisal in a world
The chair of NICE, David Haslam, initiated the conference by focussing on the importance of NICE and other health technology assessment (HTA) bodies in terms of the need for technology appraisal in a world
Improving patient safety through education and training - Report by the Commission on Education and Training for Patient Safety
 Education and Training Committee, 9 June 2016 Improving patient safety through education and training - Report by the Commission on Education and Training for Patient Safety Executive summary and recommendations
Education and Training Committee, 9 June 2016 Improving patient safety through education and training - Report by the Commission on Education and Training for Patient Safety Executive summary and recommendations
Learning from adverse events. Learning and improvement summary
 Learning from adverse events Learning and improvement summary November 2014 Healthcare Improvement Scotland 2014 Published November 2014 You can copy or reproduce the information in this document for use
Learning from adverse events Learning and improvement summary November 2014 Healthcare Improvement Scotland 2014 Published November 2014 You can copy or reproduce the information in this document for use
JOB DESCRIPTION. Clinical Nurse Specialist (Chronic Pain Management) Chronic Pain Service Department of Anaesthetics, Borders General Hospital
 1 Job Identification Job Title: Job Reference: Department & Base: Hours of Work: JOB DESCRIPTION Clinical Nurse Specialist (Chronic Pain Management) NM1703 Chronic Pain Service Department of Anaesthetics,
1 Job Identification Job Title: Job Reference: Department & Base: Hours of Work: JOB DESCRIPTION Clinical Nurse Specialist (Chronic Pain Management) NM1703 Chronic Pain Service Department of Anaesthetics,
THAMES VALLEY PRIORITIES COMMITTEE ETHICAL FRAMEWORK
 NHS Aylesbury Vale Clinical Commissioning Group NHS Bracknell and Ascot Clinical Commissioning Group NHS Chiltern Clinical Commissioning Group NHS Newbury and District Clinical Commissioning Group NHS
NHS Aylesbury Vale Clinical Commissioning Group NHS Bracknell and Ascot Clinical Commissioning Group NHS Chiltern Clinical Commissioning Group NHS Newbury and District Clinical Commissioning Group NHS
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Implementation Policy for NICE Guidelines
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Implementation Policy for NICE Guidelines Version No.: 5.3 Effective From: 08 May 2017 Expiry Date: 02 March 2019 Date Ratified: 23 February 2017
The Newcastle upon Tyne Hospitals NHS Foundation Trust Implementation Policy for NICE Guidelines Version No.: 5.3 Effective From: 08 May 2017 Expiry Date: 02 March 2019 Date Ratified: 23 February 2017
Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients?
 Research Article Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients? R Mallick *, Z Magama, C Neophytou, R Oliver, F Odejinmi Barts Health NHS Trust, Whipps Cross
Research Article Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients? R Mallick *, Z Magama, C Neophytou, R Oliver, F Odejinmi Barts Health NHS Trust, Whipps Cross
Uses a standard template but may have errors of omission
 Evaluation Form Printed on Apr 19, 2014 MILESTONE- BASED FELLOW EVALUATION Evaluator: Evaluation of: Date: This is a new milestone-based evaluation. To achieve a level, the fellow must satisfy ALL the
Evaluation Form Printed on Apr 19, 2014 MILESTONE- BASED FELLOW EVALUATION Evaluator: Evaluation of: Date: This is a new milestone-based evaluation. To achieve a level, the fellow must satisfy ALL the
Clinical Development Process 2017
 InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
GUIDANCE ON PROPOSING NATIONAL COMMISSIONING OF SERVICES
 National Specialist Services Committee NSSC GUIDANCE ON PROPOSING NATIONAL COMMISSIONING OF SERVICES The National Specialised Services Committee (NSSC) is responsible for recommendations to the NHS Board
National Specialist Services Committee NSSC GUIDANCE ON PROPOSING NATIONAL COMMISSIONING OF SERVICES The National Specialised Services Committee (NSSC) is responsible for recommendations to the NHS Board
NHS Governance Clinical Governance General Medical Council
 NHS Governance Clinical Governance General Medical Council Thank you for the opportunity to respond to this call for evidence. The GMC has a particular role in clinical governance, as outlined below, and
NHS Governance Clinical Governance General Medical Council Thank you for the opportunity to respond to this call for evidence. The GMC has a particular role in clinical governance, as outlined below, and
Reducing Attendances and Waits in Emergency Departments A systematic review of present innovations
 Reducing Attendances and Waits in Emergency Departments A systematic review of present innovations Report to the National Co-ordinating Centre for NHS Service Delivery and Organisation R & D (NCCSDO) January
Reducing Attendances and Waits in Emergency Departments A systematic review of present innovations Report to the National Co-ordinating Centre for NHS Service Delivery and Organisation R & D (NCCSDO) January
Supporting revalidation: methods and evidence
 PROFESSIONAL ISSUES Supporting revalidation: methods and evidence Kirstyn Shaw and Mary Armitage Kirstyn Shaw BSc PhD, Clinical Standards Project Manager, Clinical Effectiveness and Evaluation Unit, Royal
PROFESSIONAL ISSUES Supporting revalidation: methods and evidence Kirstyn Shaw and Mary Armitage Kirstyn Shaw BSc PhD, Clinical Standards Project Manager, Clinical Effectiveness and Evaluation Unit, Royal
Indicator 5c Mortality Survey
 Indicator 5c Mortality Survey Undertaken by NCEPOD on behalf of NHS England Dr Neil Smith - Clinical Researcher and Deputy CEO Dr Hannah Shotton - Clinical Researcher Dr Marisa Mason - Chief Executive
Indicator 5c Mortality Survey Undertaken by NCEPOD on behalf of NHS England Dr Neil Smith - Clinical Researcher and Deputy CEO Dr Hannah Shotton - Clinical Researcher Dr Marisa Mason - Chief Executive
Wales Psychological Therapies Plan for the delivery of Matrics Cymru The National Plan 2018
 Wales Psychological Therapies Plan for the delivery of Matrics Cymru The National Plan 2018 Written by the National Psychological Therapies Management Committee, supported by 1000 Lives Improvement, Public
Wales Psychological Therapies Plan for the delivery of Matrics Cymru The National Plan 2018 Written by the National Psychological Therapies Management Committee, supported by 1000 Lives Improvement, Public
Appendix 1 MORTALITY GOVERNANCE POLICY
 Appendix 1 MORTALITY GOVERNANCE POLICY 1 Policy Title: Executive Summary: Mortality Governance Policy For many people death under the care of the NHS is an inevitable outcome and they experience excellent
Appendix 1 MORTALITY GOVERNANCE POLICY 1 Policy Title: Executive Summary: Mortality Governance Policy For many people death under the care of the NHS is an inevitable outcome and they experience excellent
HS&DR Programme Application Plain English Summaries
 HS&DR Programme Application Plain English Summaries To assist applicants to the HS&DR programme, the following three recently funded project Plain English Summaries are provided. These were highlighted
HS&DR Programme Application Plain English Summaries To assist applicants to the HS&DR programme, the following three recently funded project Plain English Summaries are provided. These were highlighted
Learning from Deaths Policy LISTEN LEARN ACT TO IMPROVE
 Learning from Deaths Policy LISTEN LEARN ACT TO IMPROVE EQUALITY IMPACT The Trust strives to ensure equality and opportunity for all, both as a major employer and as a provider of health care. This policy
Learning from Deaths Policy LISTEN LEARN ACT TO IMPROVE EQUALITY IMPACT The Trust strives to ensure equality and opportunity for all, both as a major employer and as a provider of health care. This policy
Nicola Middleton. Background
 The role of the DSN in providing quality diabetes care within constrained finance Nicola Middleton Article points 1. Findings from a review of multi-country practice suggest that high-quality diabetes
The role of the DSN in providing quality diabetes care within constrained finance Nicola Middleton Article points 1. Findings from a review of multi-country practice suggest that high-quality diabetes
ERN Assessment Manual for Applicants
 Share. Care. Cure. ERN Assessment Manual for Applicants 3.- Operational Criteria for the Assessment of Networks An initiative of the Version 1.1 April 2016 History of changes Version Date Change Page 1.0
Share. Care. Cure. ERN Assessment Manual for Applicants 3.- Operational Criteria for the Assessment of Networks An initiative of the Version 1.1 April 2016 History of changes Version Date Change Page 1.0
