Iwant to start by showing you this
|
|
|
- Daniella Barker
- 5 years ago
- Views:
Transcription
1 From pioneer days to implementation: lessons to be learnt Mary Baines reflects on the pioneering days of palliative care, when she worked with Cicely Saunders at St Christopher s Hospice, in an article reproducing the talk she gave in Lisbon last May at the 12th Congress of the European Association for Palliative Care Iwant to start by showing you this photograph of Cicely Saunders, and I am grateful to Avril Jackson, previously of the Hospice Information Service,* for it. I like it because of her smile and because it shows her still at work in fact giving prizes to hospice staff though it was taken in 2001 when she was 83, just four years before her death. Cicely Saunders was, of course, the founder of St Christopher s Hospice in London and she is generally recognised as the founder of the palliative care movement. She trained as a nurse, then as a social worker, and it was then that she met David Tasma, a young Polish Jew, who was dying of cancer. It was through her friendship with him that God called her to devote her life to improving the care of the dying a most neglected group. She then trained in medicine and that was where I met her we were contemporaries at medical school. I wish, for your sake, that she could have given this talk on pioneering days. But this talk will be full of what she taught me and countless others. It is dedicated to her, Dame Cicely Saunders an honour given by Her Majesty the Queen the founder of our specialty and my dear friend. The beginning When Cicely Saunders opened St Christopher s in 1967 she brought together, for the first time in the world, a large number of patients with terminal illness and staff who were committed to discover and then teach the best ways of caring for them. Previously Cicely Saunders in 2001, four years before her death these patients would have been scattered in various hospital wards or at home. There were a few hospices, mostly opened around The patients in them received excellent nursing and spiritual care but there was minimal medical input, for it was generally believed that the doctor s role was to cure. These patients were, of course, incurable. I was a medical student at St Thomas s Hospital in London in the same year as Cicely Saunders. She was much older than the rest of us, having been a nurse and a social worker. When St Christopher s opened, I was working as a part-time general practitioner. Cicely asked me to join her on the staff and, very fearfully, I did. Medical friends said it was professional suicide. I found myself entering a branch of medicine with no books or conferences. Symptom control was contained in a single sheet entitled Drugs most commonly used at St Christopher s Hospice, which was given to all staff. Yet, I suggest, this sheet contains the single most COURTESY OF AVRIL JACkSON 223
2 Perspective So the practice of giving a strong opioid by mouth, regularly and in adequate doses became accepted at the hospice important advance in end-of-life care that has ever been made. It comes, of course, from Cicely herself. To understand its importance, we have to go back to medical practice in the 1950s and 1960s, when it was generally believed that strong opioids were only effective when given by injection and that tolerance and addiction would inevitably occur if they were given regularly. So, in practice, patients were given injections of morphine but only when their pain became unbearable. The revolution in symptom control Cicely Saunders had seen the value of regular oral morphine in a small London home for the dying that she often visited. After qualifying, she obtained a research scholarship to study pain control in terminal illness and she went to St Joseph s Hospice, where she was allowed to put her ideas into practice. She was permitted only four patients to start with because of the fear that regular giving caused addiction! But, to the surprise and delight of the staff, these patients became painfree and remained alert. So the practice of giving a strong opioid by mouth, regularly and in adequate doses became accepted at the hospice. When Cicely Saunders left St Joseph s, she had carefully documented records of over 1,000 patients dying of cancer quite a series. The first research project in what was to become palliative care. 1 The strong opioid used at St Christopher s at the beginning and listed in the hospice s symptom control leaflet is diamorphine or heroin, because it was widely believed to be superior to morphine, giving better pain control with fewer side-effects. Cicely Saunders herself said Diamorphine does the greatest good to the greatest number. But she also knew that this was only her impression and had never been researched. And so she invited Robert Twycross to join St Christopher s as a research fellow to conduct studies into many aspects of pain control, including a comparison between morphine and diamorphine given orally. Because of the strongly held belief that diamorphine was the better drug, the only ethical way to proceed was to do a pilot study first. Half the patients were given morphine and half diamorphine, and people like me were asked to guess which drug they were on. Not surprisingly, everyone who had good pain control with minimal side-effects we guessed to be on diamorphine. Those who were sick and drowsy we judged to be on morphine. In fact, we were right 50% of the time! The trial was then started with 700 patients entering over two years. On completion, when the data were analysed, they showed that there was no significant difference between them. 2 Cicely Saunders impression was wrong. Of course, we too have impressions but, like her, we should be keen to have them tested out even if we too are proved wrong. If you had joined our ward round in the early years, you would have found that the most common word used was why. Why is this patient having this particular pain? ; Why has his breathlessness suddenly become much worse? ; and, relating to my own special interest, Why has this patient with proven intestinal obstruction stopped vomiting?. This last question was fascinating. We admitted many patients who had had an open and close operation for intestinal obstruction and nothing could be done. We treated them simply, with a combination of analgesics, anti-emetics and antispasmodics with no nasogastric tube, and the vomiting either stopped or was reduced to once a day with no nausea. In addition, sometimes, after weeks, the bowels opened. Why was this? What was happening? It had never been described before. Fortunately, when St Christopher s was designed, Cicely Saunders included a postmortem room and we had a senior pathologist, Richard Carter, from the Royal Marsden Hospital, who came to perform limited symptom-directed post-mortems. Some of you here today attended them. I wonder if you, like me, remember that they mostly seemed to happen on a Saturday morning! The first 63 autopsies were written up in the first edition of the journal Palliative Medicine. 3 Eighteen autopsies were in connection with our study of patients with malignant intestinal obstruction and, in each case, the obstruction was confirmed, with 14 patients showing it at multiple sites. This study, with 40 patients, was published in The Lancet in [It included the 18 autopsied patients and 22 on which it was not possible or not appropriate to conduct post-mortems.] I hope that, if I joined your ward round next week, I would often hear the question why?. The hospice s symptom control leaflet has grown into the Oxford Textbook of Palliative 224
3 Medicine and countless other publications, but there is so much more to be learnt, not only on symptom control but on all the other aspects of palliative care. Total pain I said that the regular giving of drugs to control pain was the most important advance in end-of-life care, but close to it or even first is, surely, the inspired concept of total pain having physical, emotional, social and spiritual components. This came, of course, from Cicely herself and she first wrote about it in 1964, having learnt it at the bedsides of the dying patients she cared for. 5 This was revolutionary at that time, when the severity of pain was generally measured by the somatic injury that caused it. But this concept of total pain (or total suffering) gives us a wider approach and a framework to our understanding and care for patients at the end Mary Baines worked for many years alongside Cicely Saunders at St Christopher s Hospice; she was one of the founders of the first UK palliative home care service COURTESY OF LUkAS RADBRUCH of life. The physical component usually needs treatment with appropriate drugs, given regularly. Helping the emotional and social components of pain involves recognising and treating anxiety and depression when they are present, and spending time with patients and families, encouraging them to talk and ask questions, and giving kind but truthful answers. Spiritual pain may be due to guilt about the past or a fear of what happens after death. It was explored with all patients on admission by asking about the importance (or not) of faith, so that spiritual anxieties could be addressed. Time will not allow me to mention all the dimensions of total pain that were studied in the pioneer days but I will highlight just two. One important early study conducted by Professor John Hinton compared the experience of care of patients in the radiotherapy ward of a teaching hospital with those who were receiving hospice care either as an inpatient or at home, looking especially at levels of anxiety and depression. 6 Perhaps the best known of early studies are the work and writings of Colin Murray Parkes on bereavement. He had met Cicely Saunders before St Christopher s opened and she invited him to start a bereavement service from the beginning. Colin developed an assessment card to be filled in after death by the staff member who knew the family best. This gave details of the key person the one thought to be most affected by the death. Those who scored high were visited at home by a specially trained bereavement visitor. The effectiveness of this service, which was the first in palliative care, was written up in 1981 and it is considered by Colin to be his most important piece of work. 7 It showed that bereavement support reduced the risk in the high-risk group to about that of the low-risk group a major reduction in symptoms of anxiety and the consumption of alcohol and drugs. Two early evaluations of palliative care looked at anxiety, depression and bereavement. How do you, in 2011, evaluate the care you give? But for all the advances and research in this field, it is so important that we do not become people who just go round patients with questionnaires and boxes to tick. We need to remember daily the words of Cicely Saunders. I have tried to sum up the demands of this work we are planning in the 225
4 Perspective There were no other palliative care services at home to guide us and we felt it was very important to get it right words Watch with me. Our most important foundation for St Christopher s is the hope that in watching we should learn not only how to free patients from pain and distress, how to understand them and never let them down, but also how to be silent, how to listen and how just to be there. 8 Adapting home care Until 1969 St Christopher s was purely an inpatient unit as were the other older hospices. Patients were admitted and, with very few exceptions, remained there until they died. For the few who went home there was no followup. Then an incident occurred that led to the founding of the first domiciliary service. A woman in her 50s with severe pain from bone metastases due to breast cancer surprised us all by wanting to go home once the pain was controlled. We tried to make careful plans, I phoned the general practitioner, and the drugs, including a moderate dose of diamophine, were given to her. But ten days later she was readmitted in agony because the doctor had reduced and then stopped the opioid, feeling that it would otherwise turn his patient into an addict. Of course, the pain had returned. Sadly, this story does not have a happy ending. Her pain was easy to control but she had lost her nerve and did not want to go home again. She remained an inpatient until she died. However, it was this incident that prompted Cicely Saunders to say We must start hospice care at home now. She looked around the hospice to find staff who had worked in the community a field in which she had no experience. She chose Barbara McNulty, a nurse, and me, and she told us to start a domiciliary service. The way forward was far from clear. There were no other palliative care services at home to guide us and we felt it was very important to get it right. We needed our service to fit in with the Uk pattern of care in the community. So we decided to spend some months going round those already working there and asking them if they wanted a hospice home care team and, if so, what form they wanted it to take. The answers came back, the majority welcomed the hospice going out into the community, but the general practitioners wanted to remain in charge of patients at home and the district nurses wanted to continue the practical nursing that was needed. They wanted a 24-hour service with doctors and nurses in the team. 9 And so the first home care service was born in October 1969, a model for the Uk. This format has remained virtually unchanged at St Christopher s and, in 2010, no less than 1,800 new patients were visited and 48% of deaths occurred at home. This model was right for us but may well not be right for you. You need to design your service to fit in with the needs and resources in your country. Let me give you two examples that I know well, focusing on how they coped with a common problem. The Communist years in Romania left an appalling legacy, with many sick children in derelict orphanages and virtually no treatment for older people unable to return to productive work. But, in 1991, just over a year after the fall of Ceaucescu, an appeal to start hospice home care in Brasov was launched by Graham Perolls and others. A senior oncologist came to the Uk for training and, on his return, an English nurse joined him and immediately began to train Romanian nurses. There were no community nurses, so the team had to do the care themselves or teach the family. In spite of this, they offered a 24-hour service. At the start there was no oral morphine and the prescribing of morphine injections was so restricted and complicated that few received them. But the hospice team, with outside experts, worked tirelessly to change things and, in 2007, the government approved a law to allow all doctors to prescribe morphine, with no maximum dose. 10 In Uganda, hospice care at home was started in 1993 by Anne Merriman. Before agreeing to launch it, she insisted that oral morphine must be available and local doctors were amazed at the difference that this made. But hospice could only cover a fraction of those who needed help, so an approach to the government was made to permit specially trained nurses to prescribe and deliver morphine, essential in rural areas where there are no doctors. In 2003, the law allowing this was passed and, at present, over two thirds of the 108 districts in Uganda have morphineprescribing nurses working in them. 11 Two examples of how palliative care at home has tackled a specific local need. How can your service or the one you are planning serve your community better? This is a challenge to us all. 226
5 Palliative care reaching out There in no doubt that Cicely Saunders did not found St Christopher s purely to care for patients in south-east London. Her aim was to change the world s view of dying and this aim was shared by those of us who worked with her. There were many ways in which this could be achieved. Even before St Christopher s opened, Cicely Saunders was lecturing in the United States. An eight-week tour in 1963 followed by annual visits inspired many people and was one of the factors leading to the formation of the American hospice movement. She and others went on to lecture widely in the Uk and abroad and, from the start, we welcomed visitors. They came to see what we did and went home, not to copy it but to apply it to their own circumstances. These visits are always costly to staff but there are ways to minimise this, such as the monthly Friday visit at St Christopher s, when individuals are combined in a group for talks and a tour. But we also have visitors who come for a longer time. In 1973, Balfour Mount, a urological surgeon from Canada, visited. He went back and founded a unit in his hospital, the Royal Victoria Hospital in Montreal, and he gave the name Palliative Care to our specialty. Then, Gustavo de Simone from Argentina came to a hospice conference and was persuaded to stay on for a further two weeks of clinical work. He had come across our first textbook of palliative care in a remote part of Patagonia and had decided to come and see the work for himself. He went back and founded Pallium and became one of the leaders of palliative care in South America. But reaching out is not just a matter of geography. One of the things that pleases me most about the modern hospice movement in the Uk is its increasing involvement with different patient groups; for example, those in care homes and those with dementia. Perhaps the hardest groups to reach, especially at the beginning, were our own professional colleagues. Even speaking about pain control in the early days was fraught with difficulties. I well remember being asked to talk on the use of opioids at a conference on the management of cancer pain. In the question time at the end, I was attacked by both anaesthetists and neurosurgeons! Looking back, I wondered if this was because they could see that, if drugs were successful, there would be less demand for nerve blocks and percutaneous cordotomies. An outstanding exception to this was the late Vittorio Ventafridda from Milan. I remember him telling me that the use of nerve blocks for cancer pain in his clinic had fallen from 83% to 14%. But he was pleased because his concern was for the wellbeing of his patients, not the take-up of his specialty. A remarkable leader. How are you going to reach out? Perhaps by offering palliative care to a new group of patients, those with intractable cardiac failure or advanced multiple sclerosis. Perhaps by making a link with those trying to establish a palliative care service in one of the 119 countries without one or in one of the countries where the work is very difficult. Perhaps by seeking an invitation to speak to nursing or medical students at your local hospital, or writing an article in one of your professional journals. And there are hundreds more ways that I hope and pray you will explore during this conference. For the need for reaching out is as relevant today as when we started 44 years ago. It makes me want to turn the clock back all those years and join you and start all over again! * Avril Jackson was until recently International Information Manager at the Hospice Information Service run by Help the Hospices and St Christopher s Hospice. Declaration of interest The author declares that there is no conflict of interest. References 1. Du Boulay S, Rankin M. Cicely Saunders, the Founder of the Modern Hospice Movement, updated edition. London: SPCk, 2007: Twycross RG. Choice of strong analgesic in terminal cancer: diamorphine or morphine? Pain 1977; 3: Carter RL. The role of limited, symptom-directed autopsies in terminal malignant disease. Palliat Med 1987; 1: Baines M, Oliver DJ, Carter RL. Medical management of intestinal obstruction in patients with advanced malignant disease. A clinical and pathological study. Lancet 1985; 2: Saunders C. The symptomatic treatment of incurable malignant disease. Prescr J 1964; 4: Hinton J. The Adult Patient: Reactions to Hospice Care. In: Saunders C, Summers DH, Teller N (eds). Hospice: the Living Idea. London: Edward Arnold, 1981: Parkes CM. Evaluation of a bereavement service. J Prev Psychiatry 1981; 1: Saunders C. Watch with me. Nurs Times 1965; 61: Baines M. The origins and development of palliative care at home. Progress in Palliative Care 2010; 18: Mosoiu D, Ryan km, Joranson DE, Garthwaite JP. Reform of drug control policy for palliative care in Romania. Lancet 2006; 367: Merriman A. Going the extra mile with the bare essentials: home care in Uganda. Progress in Palliative Care 2010; 18: The references in this article can be obtained from the librarian at St Christopher s Hospice. To contact her, please send an to: d.brady@stchristophers.org.uk Correspondance to: Mary Baines, St Christopher s Hospice, London SE26 6DZ, UK, or: marybaines@dsl.pipex.com Mary Baines, Emeritus Consultant in Palliative Medicine, St Christopher s Hospice, London, UK One of the things that pleases me most about the modern hospice movement in the UK is its increasing involvement with different patient groups 227
10/3/2016 PALLIATIVE CARE WHAT IS THE DEFINITION OF PALLIATIVE CARE DEFINITION. What, Who, Where and When
 PALLIATIVE CARE What, Who, Where and When Mary Grant, RN, MS ANP Connections Nurse Practitioner Palliative Care Program Oregon Region WHAT IS THE DEFINITION OF PALLIATIVE CARE DEFINITION The Center for
PALLIATIVE CARE What, Who, Where and When Mary Grant, RN, MS ANP Connections Nurse Practitioner Palliative Care Program Oregon Region WHAT IS THE DEFINITION OF PALLIATIVE CARE DEFINITION The Center for
Learning from the National Care of the Dying 2014 Audit. Dr Bill Noble Medical Director, Marie Curie Cancer Care
 Learning from the National Care of the Dying 2014 Audit Dr Bill Noble Medical Director, Marie Curie Cancer Care MARIE CURIE Major UK end of life charity Major service provider Network of 2000 Nurses caring
Learning from the National Care of the Dying 2014 Audit Dr Bill Noble Medical Director, Marie Curie Cancer Care MARIE CURIE Major UK end of life charity Major service provider Network of 2000 Nurses caring
TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE
 ...from the Middle Ages to the 21st Century TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE Emily Bradford RN CHPN Director of Hospice Services VNA Middle Ages: 16th-18th Centuries: Religious
...from the Middle Ages to the 21st Century TEAMBUILDING CREATING A POSITIVE CULTURE IN HOSPICE CARE Emily Bradford RN CHPN Director of Hospice Services VNA Middle Ages: 16th-18th Centuries: Religious
The care of patients dying from cancer
 TERMINAL CARE The care of patients dying from cancer G. WOODBINE;mb,mrccp General Practitioner, Southampton SUMMARY. A census of seriously ill cancer patients at home and in hospital was undertaken in
TERMINAL CARE The care of patients dying from cancer G. WOODBINE;mb,mrccp General Practitioner, Southampton SUMMARY. A census of seriously ill cancer patients at home and in hospital was undertaken in
Rainbow Trust Children's Charity 6
 Rainbow Trust Children's Charity Rainbow Trust Children's Charity 6 Inspection report 1b Cleeve Court Cleeve Road Leatherhead Surrey KT22 7UD Date of inspection visit: 30 November 2016 Date of publication:
Rainbow Trust Children's Charity Rainbow Trust Children's Charity 6 Inspection report 1b Cleeve Court Cleeve Road Leatherhead Surrey KT22 7UD Date of inspection visit: 30 November 2016 Date of publication:
Hospice Isle of Man Education Prospectus 2018
 Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Advance Care Planning Communication Guide: Overview
 Advance Care Planning Communication Guide: Overview The INTERACT Advance Care Planning Communication Guide is designed to assist health professionals who work in Nursing Facilities to initiate and carry
Advance Care Planning Communication Guide: Overview The INTERACT Advance Care Planning Communication Guide is designed to assist health professionals who work in Nursing Facilities to initiate and carry
Care on a hospital ward
 Care on a hospital ward People with dementia may be admitted to general hospital wards either as part of a planned procedure such as a cataract operation or following an accident such as a fall. Carers
Care on a hospital ward People with dementia may be admitted to general hospital wards either as part of a planned procedure such as a cataract operation or following an accident such as a fall. Carers
NATIONAL PATIENT SURVEY, 2004
 NATIONAL PATIENT SURVEY, 2004 This survey is about your experience of the services provided by the National Health Service. What condition were you treated for when visiting the NHS Hospital Trust on the
NATIONAL PATIENT SURVEY, 2004 This survey is about your experience of the services provided by the National Health Service. What condition were you treated for when visiting the NHS Hospital Trust on the
Multidisciplinary care of a patient with heart failure. patient with heart failure. Dr Claire Hookey
 Multidisciplinary care of a patient with heart failure patient with heart failure Dr Claire Hookey Mr E.S 61 year old gentleman Referred to the hospice by the heart failure specialist nurse May 2010 Heart
Multidisciplinary care of a patient with heart failure patient with heart failure Dr Claire Hookey Mr E.S 61 year old gentleman Referred to the hospice by the heart failure specialist nurse May 2010 Heart
When and How to Introduce Palliative Care
 When and How to Introduce Palliative Care Phil Rodgers, MD FAAHPM Associate Professor, Departments of Family Medicine and Internal Medicine Associate Director for Clinical Services, Adult Palliative Medicine
When and How to Introduce Palliative Care Phil Rodgers, MD FAAHPM Associate Professor, Departments of Family Medicine and Internal Medicine Associate Director for Clinical Services, Adult Palliative Medicine
Transforming hospice care A five-year strategy for the hospice movement 2017 to 2022
 Transforming hospice care A five-year strategy for the hospice movement 2017 to 2022 Hospice care in the UK is at a pivotal moment... Radical change is needed. About Hospice UK We are the national charity
Transforming hospice care A five-year strategy for the hospice movement 2017 to 2022 Hospice care in the UK is at a pivotal moment... Radical change is needed. About Hospice UK We are the national charity
Prescribing for Symptom Control in End of Life Care. Dr Deborah Robertson Senior Lecturer University of Chester
 Prescribing for Symptom Control in End of Life Care Dr Deborah Robertson Senior Lecturer University of Chester #hellomynameis Dr Debs Robertson Programme leader NMP Nurse and pharmacologist Champion of
Prescribing for Symptom Control in End of Life Care Dr Deborah Robertson Senior Lecturer University of Chester #hellomynameis Dr Debs Robertson Programme leader NMP Nurse and pharmacologist Champion of
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM TRASTUZUMAB (HERCEPTIN) Patient s first names.
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM TRASTUZUMAB (HERCEPTIN) Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM TRASTUZUMAB (HERCEPTIN) Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number
Grampians Regional Palliative Care Research Centre
 Grampians Regional Palliative Care Research Centre Director : Dr David Brumley Research Manager: Dr John Fisher Consultant: Professor Michael Ashby The William Buckland Foundation made a very generous
Grampians Regional Palliative Care Research Centre Director : Dr David Brumley Research Manager: Dr John Fisher Consultant: Professor Michael Ashby The William Buckland Foundation made a very generous
What is palliative care?
 What is palliative care? Hamilton Health Sciences and surrounding communities Palliative care is a way of providing health care that focuses on improving the quality of life for you and your family when
What is palliative care? Hamilton Health Sciences and surrounding communities Palliative care is a way of providing health care that focuses on improving the quality of life for you and your family when
E-Learning Module B: Introduction to Hospice Palliative Care
 E-Learning Module B: Introduction to Hospice Palliative Care This Module requires the learner to have read Chapter 2 of the Fundamentals Program Guide and the other required readings associated with the
E-Learning Module B: Introduction to Hospice Palliative Care This Module requires the learner to have read Chapter 2 of the Fundamentals Program Guide and the other required readings associated with the
POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case
 POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case DOCUMENT NO: DN116 Lead author/initiator(s): Sarah Woodley Community Health Services Pharmacist sarah.woodley@ccs.nhs.uk
POLICY FOR ANTICIPATORY PRESCRIBING FOR PATIENTS WITH A TERMINAL ILLNESS Just in Case DOCUMENT NO: DN116 Lead author/initiator(s): Sarah Woodley Community Health Services Pharmacist sarah.woodley@ccs.nhs.uk
Talking to Your Family About End-of-Life Care
 Talking to Your Family About End-of-Life Care Sharing in significant life events during both happy and sad occasions often strengthens our bond with family and close friends. We plan for weddings, the
Talking to Your Family About End-of-Life Care Sharing in significant life events during both happy and sad occasions often strengthens our bond with family and close friends. We plan for weddings, the
Payment Reforms to Improve Care for Patients with Serious Illness
 Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Hospice 101. Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati
 Hospice 101 Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati Hospice of Cincinnati Hospice of Cincinnati creates the best possible and most meaningful EOL experience for all who
Hospice 101 Janet Montgomery, BSN, MBA Chief Marketing Officer, Hospice of Cincinnati Hospice of Cincinnati Hospice of Cincinnati creates the best possible and most meaningful EOL experience for all who
Advance Care Planning: the Clients Perspectives
 Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE. Patient s first names
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s
Support services for patients with secondary breast cancer.
 Sheffield Teaching Hospitals NHS Foundation Trust Support services for patients with secondary breast cancer. Secondary breast cancer pledge: working together to improve secondary breast cancer services
Sheffield Teaching Hospitals NHS Foundation Trust Support services for patients with secondary breast cancer. Secondary breast cancer pledge: working together to improve secondary breast cancer services
Hospice Residences. in Fraser Health
 Hospice Residences in Fraser Health Options for End of Life Care As a person s life draws to a close, the time comes when the focus changes from working towards a cure to loving care and comfort. Paying
Hospice Residences in Fraser Health Options for End of Life Care As a person s life draws to a close, the time comes when the focus changes from working towards a cure to loving care and comfort. Paying
Elective Report. Children s Surgical Centre, Phnom Penh, Cambodia
 Elective Report Children s Surgical Centre, Phnom Penh, Cambodia I was fortunate enough to be one of two recipients of a Dr Carl Jackson Scholarship which allowed me to do my elective in Cambodia. For
Elective Report Children s Surgical Centre, Phnom Penh, Cambodia I was fortunate enough to be one of two recipients of a Dr Carl Jackson Scholarship which allowed me to do my elective in Cambodia. For
Palliative Care Nursing: A Matter of Respect
 NURSING Palliative Care Nursing: A Matter of Respect By PATRICIA RINGOS BEACH, MSN, RN, AOCN, ACHPN It was many years ago that our palliative care team was sitting around a table in a conference room with
NURSING Palliative Care Nursing: A Matter of Respect By PATRICIA RINGOS BEACH, MSN, RN, AOCN, ACHPN It was many years ago that our palliative care team was sitting around a table in a conference room with
ORGANISATIONAL AUDIT
 [Type text] National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians,
[Type text] National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians,
Perceptions of the role of the hospital palliative care team
 NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee
 Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
E-Learning Module B: Assessment
 E-Learning Module B: Assessment This module requires the learner to have read chapter 3 of the CAPCE Program Guide and the other required readings associated with the topic. See the CAPCE Program Guide
E-Learning Module B: Assessment This module requires the learner to have read chapter 3 of the CAPCE Program Guide and the other required readings associated with the topic. See the CAPCE Program Guide
10 THINGS. Hospice is a word most people have heard, but. few know much about it unless they have had. a direct experience with hospice care with a
 10 THINGS that may surprise you about hospice care Hospice is a word most people have heard, but few know much about it unless they have had a direct experience with hospice care with a friend or family
10 THINGS that may surprise you about hospice care Hospice is a word most people have heard, but few know much about it unless they have had a direct experience with hospice care with a friend or family
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM CYTARABINE CONTINUOUS INFUSION
 Patient identifier/label: Page 1 of 6 CYTARABINE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital
Patient identifier/label: Page 1 of 6 CYTARABINE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital
Advance Directive. A step-by-step guide to help you make shared health care decisions for the future. California edition
 Advance Directive A step-by-step guide to help you make shared health care decisions for the future California edition Advance Directive Instructions for Patients TALK TO YOUR LOVED ONES This is important.
Advance Directive A step-by-step guide to help you make shared health care decisions for the future California edition Advance Directive Instructions for Patients TALK TO YOUR LOVED ONES This is important.
What Is Hospice? Answers to Your Questions
 What Is Hospice? Answers to Your Questions Dear Prospective NorthShore Hospice Patients, Welcome! When you choose NorthShore Hospice, it means that you have surrounded yourself with an interdisciplinary
What Is Hospice? Answers to Your Questions Dear Prospective NorthShore Hospice Patients, Welcome! When you choose NorthShore Hospice, it means that you have surrounded yourself with an interdisciplinary
Results of the 2012/2013 Hospice Patient Survey. General Report. Centre for Health Services Studies. Linda Jenkins and Jan Codling.
 Centre for Health Services Studies Results of the 12/13 Hospice Patient Survey General Report Linda Jenkins and Jan Codling November 13 www.kent.ac.uk/chss Results of the 12/13 Hospice Patient Survey
Centre for Health Services Studies Results of the 12/13 Hospice Patient Survey General Report Linda Jenkins and Jan Codling November 13 www.kent.ac.uk/chss Results of the 12/13 Hospice Patient Survey
I. Course goals and objectives:
 Department: Internal Medicine Course: Palliative Care Sub-Internship Faculty Coordinator: Elizabeth Paulk, M.D. Hospital: Parkland Health & Hospital System Periods offered: all Length: one month Maximum
Department: Internal Medicine Course: Palliative Care Sub-Internship Faculty Coordinator: Elizabeth Paulk, M.D. Hospital: Parkland Health & Hospital System Periods offered: all Length: one month Maximum
Hospice Residences Rev. May 28, 2014 R-4. Dame Cicely Saunders (1976) Founder of modern hospice movement. Design:
 Hospice Residences w w w. f r a s e r h e a l t h. c a in Fraser Health Dame Cicely Saunders (1976) Founder of modern hospice movement 280119 Rev. May 28, 2014 R-4 Design: www.kochink.com You matter because
Hospice Residences w w w. f r a s e r h e a l t h. c a in Fraser Health Dame Cicely Saunders (1976) Founder of modern hospice movement 280119 Rev. May 28, 2014 R-4 Design: www.kochink.com You matter because
Advance Health Care Planning: Making Your Wishes Known. MC rev0813
 Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DENOSUMAB. Patient s first names.
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DENOSUMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DENOSUMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas
Compassionate culture: Hearing and heeding patient and family voices in end of life care Chair: Cassandra Cameron, Policy Advisor Quality, NHS
 Compassionate culture: Hearing and heeding patient and family voices in end of life care Chair: Cassandra Cameron, Policy Advisor Quality, NHS Providers Speakers: Dr Katherine Sleeman, NIHR Clinician Scientist,
Compassionate culture: Hearing and heeding patient and family voices in end of life care Chair: Cassandra Cameron, Policy Advisor Quality, NHS Providers Speakers: Dr Katherine Sleeman, NIHR Clinician Scientist,
ADVANCE DIRECTIVE INFORMATION
 ADVANCE DIRECTIVE INFORMATION NOTE: This Advance Directive Information and the form Living Will and Durable Power of Attorney for Health Care on the Arkansas Bar Association s website are being provided
ADVANCE DIRECTIVE INFORMATION NOTE: This Advance Directive Information and the form Living Will and Durable Power of Attorney for Health Care on the Arkansas Bar Association s website are being provided
If patient is 24 hour dependent on NIV and decides to discontinue it, support and forward planning are essential
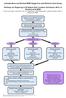 Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care
 Health Guidance McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care Publication Code: HCR-0214-083 Publication date: 26 February 2014 Page 1 of 7 Health
Health Guidance McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care Publication Code: HCR-0214-083 Publication date: 26 February 2014 Page 1 of 7 Health
Spiritual care. Velindre Cancer Centre Chaplaincy Department
 Spiritual care. Velindre Cancer Centre Chaplaincy Department SPIRITUAL CARE REV.ERIC BURKE. World Health Organisation statement 1948 Health is a state of complete physical, Mental and spiritual well-being
Spiritual care. Velindre Cancer Centre Chaplaincy Department SPIRITUAL CARE REV.ERIC BURKE. World Health Organisation statement 1948 Health is a state of complete physical, Mental and spiritual well-being
Clinical Skills Course. Workbook to accompany on line learning programme
 Clinical Skills Course Workbook to accompany on line learning programme The National GSF Centre for End of Life Care Clinical Skills Programme February 2015 www.goldstandardsframework.org.uk Prof Keri
Clinical Skills Course Workbook to accompany on line learning programme The National GSF Centre for End of Life Care Clinical Skills Programme February 2015 www.goldstandardsframework.org.uk Prof Keri
Path to Transformation Concept Paper Comments and Recommendations. Palliative Care Community Partners (PCCP)
 Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Executive Summary 10 th September Dr. Richard Wagland. Dr. Mike Bracher. Dr. Ana Ibanez Esqueda. Professor Penny Schofield
 Experiences of Care of Patients with Cancer of Unknown Primary (CUP): Analysis of the 2010, 2011-12 & 2013 Cancer Patient Experience Survey (CPES) England. Executive Summary 10 th September 2015 Dr. Richard
Experiences of Care of Patients with Cancer of Unknown Primary (CUP): Analysis of the 2010, 2011-12 & 2013 Cancer Patient Experience Survey (CPES) England. Executive Summary 10 th September 2015 Dr. Richard
Supporting people who need Palliative and End of Life Care in the Community. Giving people a choice
 Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM VISMODEGIB. Patient s first names.
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM VISMODEGIB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St.
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM VISMODEGIB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St.
Module 2 Excellence in practice
 Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
Hospice Care for the Person with Cancer
 Hospice Care for the Person with Cancer Hospice is a special type of care designed to provide comfort, support and dignity to patients with a lifelimiting or terminal illness. For hospice purposes, a life-limiting
Hospice Care for the Person with Cancer Hospice is a special type of care designed to provide comfort, support and dignity to patients with a lifelimiting or terminal illness. For hospice purposes, a life-limiting
END OF PROJECT BRIEFING
 ECONOMICS OF END OF LIFE CARE END OF PROJECT BRIEFING An overview of the project This briefing provides a summary of key findings from a four year research project which studied the economics of supportive
ECONOMICS OF END OF LIFE CARE END OF PROJECT BRIEFING An overview of the project This briefing provides a summary of key findings from a four year research project which studied the economics of supportive
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PEGYLATED LIPOSOMAL DOXORUBICIN (CAELYX)
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PEGYLATED LIPOSOMAL DOXORUBICIN (CAELYX) Patient s surname/family name Patient s first names Date of birth Hospital
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PEGYLATED LIPOSOMAL DOXORUBICIN (CAELYX) Patient s surname/family name Patient s first names Date of birth Hospital
UEMS / EACCME Event Report
 Event title: 14 th World Congress of the European Association for Palliative Care Entitled: Building Bridges Reference number: 12003 Actual number of participants: 2765 Number of certificates issued: 2631
Event title: 14 th World Congress of the European Association for Palliative Care Entitled: Building Bridges Reference number: 12003 Actual number of participants: 2765 Number of certificates issued: 2631
Serious Medical Treatment Decisions. BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE
 Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
Caring for you at Hospice and Home.
 Caring for you at Hospice and Home www.saintcatherines.org.uk CONTENTS Introduction 1 Where it all began 2 Services 3 5 In-Patient Unit Outpatients Clinic Day Hospices Physio and Occupational Therapy Lymphoedema
Caring for you at Hospice and Home www.saintcatherines.org.uk CONTENTS Introduction 1 Where it all began 2 Services 3 5 In-Patient Unit Outpatients Clinic Day Hospices Physio and Occupational Therapy Lymphoedema
End of life care in Secure Psychiatric Settings
 End of life care in Secure Psychiatric Dr Nuwan Galappathie MBChB MRCPsych MMedSc LLM Consultant Forensic Psychiatrist St Andrew s Healthcare, Birmingham Visiting Researcher, Institute of Psychiatry, Kings
End of life care in Secure Psychiatric Dr Nuwan Galappathie MBChB MRCPsych MMedSc LLM Consultant Forensic Psychiatrist St Andrew s Healthcare, Birmingham Visiting Researcher, Institute of Psychiatry, Kings
Deprivation of Liberty Safeguarding in hospice care: from law into practice
 Deprivation of Liberty Safeguarding in hospice care: from law into practice Hot Topics Study Day May 2016 Dr Corinna Midgley Saint Francis Hospice Registered Charity No: 275913 Aims of today: To review
Deprivation of Liberty Safeguarding in hospice care: from law into practice Hot Topics Study Day May 2016 Dr Corinna Midgley Saint Francis Hospice Registered Charity No: 275913 Aims of today: To review
RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE. INSIDE Expert advice on HIV disclosure. The end of an era in Afghanistan
 Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Palliative and Hospice Care In the United States Jean Root, DO
 Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
National Care of the Dying Audit Hospitals (NCDAH) Round 3
 National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians, and is supported
National Care of the Dying Audit Hospitals (NCDAH) Round 3 This audit is being led by the Marie Curie Palliative Care Institute Liverpool in collaboration with the Royal College of Physicians, and is supported
Patient identifier/label: Page 1 of 6. Patient s first names. Date of birth
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM ENZALUTAMIDE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St.
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM ENZALUTAMIDE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St.
Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016
 Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Executive Summary Serbia Hospice Appeal
 Executive Summary Serbia Hospice Appeal Making every day count for terminally ill cancer patients HONORARY PATRONS HE Mr. Leo D Aes, Belgium Ambassador to Serbia HE Mr. Denis Keefe, British Ambassador
Executive Summary Serbia Hospice Appeal Making every day count for terminally ill cancer patients HONORARY PATRONS HE Mr. Leo D Aes, Belgium Ambassador to Serbia HE Mr. Denis Keefe, British Ambassador
Putting the Patient and Family Voice Back into Measuring the Quality of Care for the Dying
 Putting the Patient and Family Voice Back into Measuring the Quality of Care for the Dying Toolkit of Instruments to Measure End of life Care (TIME) Research Team -- Department of Community Health, Brown
Putting the Patient and Family Voice Back into Measuring the Quality of Care for the Dying Toolkit of Instruments to Measure End of life Care (TIME) Research Team -- Department of Community Health, Brown
Emergency Department Patient Experience Survey Highlights
 Emergency Department Patient Experience Survey Highlights www.hqca.ca April 2008 Albertans get emergency and urgent care services in many different ways. People in cities sometimes go to emergency departments
Emergency Department Patient Experience Survey Highlights www.hqca.ca April 2008 Albertans get emergency and urgent care services in many different ways. People in cities sometimes go to emergency departments
Home Instead Birmingham
 Maranatha Healthcare Ltd Home Instead Birmingham Inspection report Radclyffe House 66-68 Hagley Road Birmingham West Midlands B16 8PF Date of inspection visit: 07 March 2017 Date of publication: 17 May
Maranatha Healthcare Ltd Home Instead Birmingham Inspection report Radclyffe House 66-68 Hagley Road Birmingham West Midlands B16 8PF Date of inspection visit: 07 March 2017 Date of publication: 17 May
The POLST Conversation POLST Script
 The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
E-Learning Module M: Assessment Review
 E-Learning Module M: Assessment Review This Module requires the learner to have read Chapter 12 of the Fundamentals Program Guide and the other required readings associated with the topic. Revised: August
E-Learning Module M: Assessment Review This Module requires the learner to have read Chapter 12 of the Fundamentals Program Guide and the other required readings associated with the topic. Revised: August
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM CHOP 21 + RITUXIMAB
 Patient identifier/label: Page 1 of 6 FORM CHOP 21 + RITUXIMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital
Patient identifier/label: Page 1 of 6 FORM CHOP 21 + RITUXIMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital
This is a repository copy of Non-medical prescribing in palliative care: a regional survey.
 This is a repository copy of Non-medical prescribing in palliative care: a regional survey. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/879/ Version: Accepted Version
This is a repository copy of Non-medical prescribing in palliative care: a regional survey. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/879/ Version: Accepted Version
End of Life Volunteer Companionship Service
 End of Life Volunteer Companionship Service Early stages of the initiative The Volunteer department was receiving frequent calls from various Wards in the Trust asking if a volunteer could sit with a dying
End of Life Volunteer Companionship Service Early stages of the initiative The Volunteer department was receiving frequent calls from various Wards in the Trust asking if a volunteer could sit with a dying
HealthStream Regulatory Script
 HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
Funding guidelines. Supporting positive change in communities
 Funding guidelines Supporting positive change in communities April 2018 March 2019 Tudor makes grants to smaller community-led groups that support people at the margins of society. Tudor s trustees are
Funding guidelines Supporting positive change in communities April 2018 March 2019 Tudor makes grants to smaller community-led groups that support people at the margins of society. Tudor s trustees are
Responding to Patients and Families that Want Everything Done
 Responding to Patients and Families that Want Everything Done Steven Pantilat, MD Professor of Clinical Medicine Alan M. Kates and John M. Burnard Endowed Chair in Palliative Care Director, Palliative
Responding to Patients and Families that Want Everything Done Steven Pantilat, MD Professor of Clinical Medicine Alan M. Kates and John M. Burnard Endowed Chair in Palliative Care Director, Palliative
Station Name: Mrs. Smith. Issue: Transitioning to comfort measures only (CMO)
 Station Name: Mrs. Smith Issue: Transitioning to comfort measures only (CMO) Presenting Situation: The physician will meet with Mrs. Smith s children to update them on her condition and determine the future
Station Name: Mrs. Smith Issue: Transitioning to comfort measures only (CMO) Presenting Situation: The physician will meet with Mrs. Smith s children to update them on her condition and determine the future
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM FMD. Patient s first names.
 Patient identifier/label: Page 1 of 6 Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
Patient identifier/label: Page 1 of 6 Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
1. Guidance notes. Social care (Adults, England) Knowledge set for end of life care. (revised edition, 2010) What are knowledge sets?
 Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PAZOPANIB. Patient s first names.
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PAZOPANIB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM PAZOPANIB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas
End of Life Care in the Acute Hospital Setting. Dr Adam Brown Consultant in Palliative Medicine
 End of Life Care in the Acute Hospital Setting Dr Adam Brown Consultant in Palliative Medicine Learning objectives Understanding a patient's priorities for end of life care How to work with the 5 priorities
End of Life Care in the Acute Hospital Setting Dr Adam Brown Consultant in Palliative Medicine Learning objectives Understanding a patient's priorities for end of life care How to work with the 5 priorities
Colorectal Multi Disciplinary Team
 Colorectal Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with Colorectal Cancer. There are many people involved in providing cancer health
Colorectal Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with Colorectal Cancer. There are many people involved in providing cancer health
We need to talk about Palliative Care. The Care Inspectorate
 We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
Ready Today for The Future of Health Care and Optimal Hospice Care
 Ready Today for The Future of Health Care and Optimal Hospice Care Aetna Compassionate Care SM Program End of life care current state There is a great divide separating the kind of care Americans say they
Ready Today for The Future of Health Care and Optimal Hospice Care Aetna Compassionate Care SM Program End of life care current state There is a great divide separating the kind of care Americans say they
Health and Social Care Alliance Scotland Carer Responses Analysis: Summary of Findings
 Health and Social Care Alliance Scotland Carer Responses Analysis: Summary of Findings 1. Introduction Professors Jane Joy, University Teacher, Nursing and Health Care and her colleague Diane Willis, University
Health and Social Care Alliance Scotland Carer Responses Analysis: Summary of Findings 1. Introduction Professors Jane Joy, University Teacher, Nursing and Health Care and her colleague Diane Willis, University
Worcestershire Hospices
 Worcestershire Hospices Our lives are a story and the ending matters. Dr Atul Gawande Worcestershire Hospices our year in numbers Support over 4,638 patients & loved ones Employ over 300+ staff Cost 10.2m
Worcestershire Hospices Our lives are a story and the ending matters. Dr Atul Gawande Worcestershire Hospices our year in numbers Support over 4,638 patients & loved ones Employ over 300+ staff Cost 10.2m
PATIENT AGREEMENT TO SYSTEMIC THERAPY: GENERIC CONSENT FORM. Patient s first names. Date of birth. Job title
 Patient identifier/label: Page 1 of 5 GENERIC CONSENT FORM Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other identifier) Male Female Special requirements
Patient identifier/label: Page 1 of 5 GENERIC CONSENT FORM Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other identifier) Male Female Special requirements
Information for patients with gynaecological cancer. Departments of gynaecology, oncology and gynaecological oncology
 Information for patients with gynaecological cancer Departments of gynaecology, oncology and gynaecological oncology This booklet gives further information about cancers of the female reproductive system
Information for patients with gynaecological cancer Departments of gynaecology, oncology and gynaecological oncology This booklet gives further information about cancers of the female reproductive system
The Oncology Project Year 3
 The Oncology Project Year 3 Dr Alison Brewster Consultant Clinical Oncologist, Velindre Hospital Introduction to the Oncology Project Why is it important? Learning objectives Process Tutorials Patient
The Oncology Project Year 3 Dr Alison Brewster Consultant Clinical Oncologist, Velindre Hospital Introduction to the Oncology Project Why is it important? Learning objectives Process Tutorials Patient
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth
 Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM WEEKLY RITUXIMAB. Patient s first names. Date of birth
 Page 1 of 5 FORM WEEKLY RITUXIMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
Page 1 of 5 FORM WEEKLY RITUXIMAB Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s Hospital St. Thomas Hospital King s College Hospital Lewisham Hospital NHS number
Why Is it so Diffi cult to Die?
 Why Is it so Diffi cult to Die? Note Health care practice and knowledge are constantly changing and developing as new research and treatments, changes in procedures, drugs and equipment become available.
Why Is it so Diffi cult to Die? Note Health care practice and knowledge are constantly changing and developing as new research and treatments, changes in procedures, drugs and equipment become available.
Chapter 13. Death, Dying, Bereavement, And Widowhood. Sociology 431
 Chapter 13 Death, Dying, Bereavement, And Widowhood Sociology 431 The Changing Context of Dying Many Americans are uncomfortable talking about death, especially the prospect of their own. People use euphemisms
Chapter 13 Death, Dying, Bereavement, And Widowhood Sociology 431 The Changing Context of Dying Many Americans are uncomfortable talking about death, especially the prospect of their own. People use euphemisms
ILLINOIS Advance Directive Planning for Important Health Care Decisions
 ILLINOIS Advance Directive Planning for Important Health Care Decisions CaringInfo 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CaringInfo, a program of the National Hospice
ILLINOIS Advance Directive Planning for Important Health Care Decisions CaringInfo 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CaringInfo, a program of the National Hospice
VICTORIA HOSPICE & PALLIATIVE CARE
 D R. G. M I C H A E L D OWNING C L I N I C A L A S S O C I AT E P R O F E S S O R PA L L I AT I V E M E D I C I N E D I R E C T O R O F R E S E A R C H & D E V E LO P M E N T V I C T O R I A H O S P I
D R. G. M I C H A E L D OWNING C L I N I C A L A S S O C I AT E P R O F E S S O R PA L L I AT I V E M E D I C I N E D I R E C T O R O F R E S E A R C H & D E V E LO P M E N T V I C T O R I A H O S P I
Oral Ibrutinib (single agent)
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM IBRUTINIB Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM IBRUTINIB Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other
Paediatric Directorate /1791
 Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
You can complete this survey online at Patient Feedback Fill in this survey and help us improve hospital services
 Patient Feedback Fill in this survey and help us improve hospital services Patient Survey Help us improve hospital services What is the survey about? This survey is about your most recent stay as an inpatient
Patient Feedback Fill in this survey and help us improve hospital services Patient Survey Help us improve hospital services What is the survey about? This survey is about your most recent stay as an inpatient
Three steps to success
 Inpatient care for people with diabetes at Russells Hall Hospital (The Dudley Group NHS Foundation Trust) Three steps to success The ThinkGlucose team at Russells Hall Hospital developed a three-stage
Inpatient care for people with diabetes at Russells Hall Hospital (The Dudley Group NHS Foundation Trust) Three steps to success The ThinkGlucose team at Russells Hall Hospital developed a three-stage
