CPD: The non-pharmacological nursing management of dyspnoea in end-stage respiratory disease and palliative care populations
|
|
|
- Adrian Parks
- 5 years ago
- Views:
Transcription
1 CPD: The non-pharmacological nursing management of dyspnoea in end-stage respiratory disease and palliative care populations David Stephenson, Flinders University and Annie McHugh, Southern Adelaide Palliative & Support Services After reading this article it is anticipated that the reader will be able to identify 1. Current care pathways for the treatment of dyspnoea in the palliative setting. 2. Discuss current practice trends associated with nurse-led dyspnoea clinics. 3. Outline the components of the interventions of the dyspnoea. Breathing is truly a strange phenomenon of life, caught midway between the conscious and the unconscious and particularly sensitive to both. (Richards 1953 p.15) Defining dyspnoea The urge to breathe is one of the strongest impulses we experience. Dyspnoea occurs when the act of breathing does not satisfy the urge to breathe (Adams & Gus 1996 p.11). In ways that closely parallel good definitions of pain, dyspnoea needs to be understood as both a subjective sensation and an experience that can be compounded or ameliorated by a wide range of social, emotional, spiritual and environmental factors. For people living with end-stage respiratory disease or advanced malignancy, dyspnoea is frequently a multi-factorial symptom in which the awareness of effort seems to be common to all circumstances and dominant in most (Adams & Gus 1996 p.11). The American Thoracic Society (1999) reiterates this point in their definition of dyspnoea as a subjective experience of breathing discomfort that consists of qualitatively distinct sensations that vary in intensity (p321). David Stephenson RN BN MPallC MRCNA Clinical Nurse, Southern Adelaide Palliative & Supportive Services Senior Lecturer, School of Nursing & Midwifery, Flinders University Annie McHugh RN, Grad. Cert Respiratory Nursing, Grad Cert in Health (Palliative Care) Grad. Cert (Coronary Care). Clinical Nurse, Southern Adelaide Palliative & Supportive Services Incidence in palliative care populations Although the incidence and degree of distress associated with dyspnoea increase when patients are afflicted with primary or secondary malignancy affecting the lungs or respiratory tract, dyspnoea can affect between 50-70% of all patients with malignant disease (Heyse-Moore, Ross et al. 1991; Bailey 1997; Dudgeon & Lertzman 1998; Corner & O Driscoll 1999; Bruera, Schmitz et al. 2000; Edmonds, Higginson et al. 2000). Chan, Sham et al. (2004) and Dudgeon & Lertzman (1998) report that between 19-55% and 28-50% respectively, grade their experience of this symptom as moderate to severe. Other authors put this figure as high as 90% during the period leading up to death (Muers & Round 1993; Tarzain 2000). Ripamonti & Bruera (1997) note that 24% of all dyspnoeic cancer patients do not have any cardiac or pulmonary pathology. For many patients with a life-limiting illness arising from malignancy, the onset of dyspnoea as a new symptom can be a very frighting marker of disease progression and a dreaded portent of things to come. Paradoxically, mild dyspnoea, not unlike mild pain, can often be masked by patients and easy for clinicians to ignore. Prompt recognition and early discussion and intervention are therefore vital in offsetting the fear this symptom creates and the creeping burden it places on patients and their carers when left unrecognised and untreated. A broad reading of the literature supports Roberts, Thorne et al s (1993) observation that patients generally receive little or no emotional support during acute episodes of dyspnoea and inadequate practical education at other times to assist them to take control over dyspnoea. Dyspnoea in end-stage respiratory disease For patients with chronic respiratory diseases, dyspnoea is often insidious in onset, and with years of adaptation to the experience, breathlessness, even beyond a moderate form, can easily be overlooked by clinicians, carers and patients alike. By the end-stages of chronic respiratory disease, clinicians, by and large, expect that patients have assumed the enormous symptom burden associated with dyspnoea, and have learned, as much as is possible, to live with the limitations and frustrations that such a symptom imposes. The end stage of these diseases are characterised by increasingly frequent episodes of acute exacerbation requiring hospitalisation and active intervention and symptom management. In general terms, severe refractory dyspnoea, cachexia, increasingly frequent exacerbations, longer hospital admissions with Collegian Vol 11 No
2 diminishing return of functional status, together herald the onset of the terminal stages of these diseases. The challenges of managing dyspnoea Dyspnoea as a symptom continues to rank highly in the top ten symptoms reported by terminally ill patients and is as difficult to manage now as it was 20 years ago (cf incidences cited by Wilkes in 1974 quoted in Enck (1989) with those cited by Rawlinson (2000). Current management Despite a large and growing body of literature pertaining to the pathophysiology associated with dyspnoea, Madjar (1998) states that we still remain ignorant as to its causes and why some patients display more distress than others. Much of the effort to manage breathlessness has thus far focused on the treatment of underlying causes or on pharmacological strategies. Drings (1997) and Chan, Sham et al. (2004) amongst others provide a comprehensive guide to the interventions that are available to investigate and alleviate dyspnoea in cancer patients. Many are of course not without risk of increased morbidity and mortality, and Booth (1998a; 1998b) reminds us that the general condition and nearness to death should dictate the suitability of such interventions. A more global perspective and approach is required to properly balance out the needs, benefits and burdens associated with the range of possible interventions that are available for the investigation and treatment of the causes of dyspnoea (as cited by Drings). So too will such considerations also dictate the appropriateness of the range of non-pharmacological nursing interventions described below. Primary causes of dyspnoea in the palliative population: (adapted from Chan & Sham p 590) Pulmonary: Lung malignancy Airway collapse Bronchial obstruction Consolidation Infection Fibrosis Lymphangitis Embolism Radiation damage Cardiac: Ischaemic heart disease Cardiac failure Pericardial disease SVC obstruction Pleural: Embolism Pneumothorax Effusion Psychological: Anxiety Panic Hyperventilation Other: Anaemia Diaphragmatic (tumour or ascites) Cachexia Ripamonti (1999) surveyed the literature on breathlessness in palliative care populations, and listed many causes. Some are associated with the disease or its treatment, but many (eg. Asthma, COPD and heart failure) co-exist with the diagnosis of cancer (Reuben & Mor 1986). A full assessment, including history taking and clinical examination, can elicit information leading to diagnosis of the cause of breathlessness. Medical interventions such as radiotherapy and chemotherapy can provide excellent temporary relief, as can paracentesis and blood transfusion. (Higginson & McCarthy 1989; Chan, Sham et al. 2004). Beyond the role of radiotherapy however, much of the current clinical management literature continues to focus on the limited array of pharmacological management strategies, namely: Opioids to reduce the sensation of breathlessness Bronchodilators to improve air entry Steroids to reduce bronchospasm and obstructive inflammation Antibiotics to combat infection Anxiolytics to reduce panic Oxygen to relieve hypoxia (Bruera, Macmillan et al. 1990; Hanratty & Higginson 1994; Davis 1997; Brant 1998; Le Grand & Walsh 1999; Ripamonti 1999; Rousseau 2002; Chan, Sham et al. 2004) Despite the frequency and severity of irreversible dyspnoea in palliative care, clinical management practices have not yet become standardised across the international palliative community. In a recent International Palliative Care Conference (Palliative Care in Respiratory Care 2001 Mexico) Manning, quoted by Levy (2001) suggested that from an evidence-based perspective only opioids and supplemental oxygen have been demonstrated to have a significant beneficial effect on dyspnoea. While the role and efficacy of bronchodilators have been well established in COPD, their effect has been poorly researched within palliative care populations. A single arm study within this population found that 49% of the trial participants had reversible airflow obstruction, yet only 5% were using bronchodilator therapy (Congleton & Muers 1995) When comparing the transformation in pain management practices, with the opening up of an array of new pharmacotherapeutic fronts, and considerable investment in receptor modelling, efficacy studies and large multi-centre randomised controlled effectiveness studies that have taken place over recent decades, meagre progress has been made in advancing our understanding and management of dyspnoea. As suggested earlier, the symptom is approached both conceptually and clinically in much the same way as it was 20 years ago; opioids, oxygen and benzodiazepines continue to be reiterated as the mainstay of treatment (Davis 1997; Le Grand & Walsh 1999; Rousseau 2002). The nursing approach Cox (2002) asserts that most of the interventions associated with the management of dyspnoea are based on a medical model in which they are mostly done to the patient, with the patient in a compliant role and the nurse supporting that role (p.33). Holistic models of nursing, as described by McMahon (1991) amongst many, places the patient in an active partnership with nurses, who use their skills creatively to assist the patient in his or her quest for health (Cox 2002 p.33). In the context of end-stage respiratory disease and palliative care populations, health is constructed as the ability to live well within the limits and confines of her or his capacity and disease (Cox p33). As Krishnasamy, Corner et al (2001) state;... although there has been a recognition of a psychological or emotional component [in the management of dyspnoea] this is often presented as being something separate or distinct from the symptom as physiologically defined... in other words, breathlessness has predominantly been approached through a reductionist perspective, an approach increasingly recognised as being of limited value in minimizing the distress caused by this complex problem (p.3) 38 Collegian Vol 11 No
3 CPD: The non-pharmacological nursing management of dyspnoea in end-stage respiratory disease and palliative care populations The development of nurse-lead dyspnoea clinics as a non-pharmacological nursing intervention The forerunner of the new nurse-lead dyspnoea clinics that are now firmly established across the UK lay in the work of pulmonary rehabilitation programs and the clinics designed to follow up and help maintain COPD patients post rehabilitation (Corner, Plant et al. 1996). The principal goals of pulmonary rehabilitation are to reduce symptoms, improve quality of life and increase physical and emotional participation in everyday activities. To accomplish these goals pulmonary rehabilitation covers a range of non-pulmonary problems including exercise deconditioning, relative social isolation, altered mood states (especially depression), muscle wasting and weight loss. These rehabilitation programs focussed on utilised breathing retraining, relaxation, adaptation and coping strategies along with counselling support (Gift, Moore et al. 1992). Meta analyses by Devine & Pearcy (2002) and Guell, Casan et al. (2000) report that A-level evidence exists for a reduction in dyspnoea, an increase in exercise tolerance and improved quality of life. The GOLD study (1996; Pauwels, Buist et al. 2001) suggests that these benefits can be maintained for at least two years post rehabilitation providing regular follow up through a respiratory nursing clinic or physician clinic is maintained. Despite this efficacy evidence, effectiveness of this intervention in the UK has been marginalised by lack of uptake. Pauwels, Buist et al. (2001) reported that in that year fewer than 2% of COPD patients undertake respiratory rehabilitation, and The British Thoracic Society (2002) also found that 60% of GPs had no understanding of such rehabilitation programs. The extent of uptake of respiratory rehabilitation programs fro COPD patients in the Australian setting has not been documented. Drawing on the experiences of respiratory nurses, COPD patients and these pulmonary rehabilitation programs Corner et al (1996) undertook a study into non-pharmacological interventions for breathlessness in lung cancer patients. The intervention was designed to draw on conceptual relationship between shared decision-making and enhanced patient education leading to increased self-care of symptoms and greater patient and carer empowerment, as promoted by theorists and authors such as Grahn (1998) and Benor et al (1999). Randomisation during the initial study was halted at the request of nursing and medical staff, who noted clear benefits for the patients receiving the intervention. Although the truncated sample size was small (intervention n=11, control n=9) analysis of available data found that after 12 weeks of weekly clinic visits, the intervention group experienced median improvements from baseline of 35% for breathlessness at worst, 53% for dyspnoea induced distress, 17% for functional capacity along with a 21% reduction in difficulty performing ADLs. The scores for the control group either remained static or worsened over the length of the study period. In the second phase of this research program Bredin, Corner et al (1999) went on to preform a multi-centre RCT, which lead to the incorporation of the results these two studies into the Macmillan Practice Development Unit project titled Managing Breathlessness in Lung Cancer. Bredin, Corner et al s (1999) randomised control trial involved 119 patients from 6 UK hospitals where clinics were led by specialist cancer nurses including Macmillan Nurses. The patients all had a diagnosis of either mesothelioma or small cell or non-small cell lung cancer, had completed first-line treatment for their disease, and reported breathlessness. Patients enrolled in the intervention arm were seen at a nurse-led clinic, while the control group were given standard care. The levels of dyspnoea, and its effects on the lifestyle and functional status of the sample were monitored for 8 weeks. At the start of the trial participants in both arms reported high levels of dyspnoea-related distress and functional impairment. Although there was no difference in overall survival, global quality of life scores, or scores for dyspnoea at worst and psychological distress between the two groups at the end of the 8 week period, the intervention group showed significant improvement in scores for dyspnoea at best, WHO performance status, depression, physical symptom distress. The intervention also resulted in slight improvements in dyspnoea induced distress and levels of anxiety. Corner et al s original 1996 study assessed patients from remission to end-stage disease, and found that elements of the nursing interventions could be used at all stages. This is a crucial finding, given the reported under-utilisation of such non-pharmacological interventions during the terminal care phase where such measures as positioning and fan therapy and when pharmacotherapy is often seen as an easy option for a difficult and intractable symptom. From research to practice: the interventions of the dyspnoea clinic. The experience of the nurse-led dyspnoea clinics involved in these two research initiatives was instrumental in the development and role out of the subsequent train-the-trainer courses throughout the United Kingdom which followed on from the successes of the second phase of the research. Unique to these nursing clinics is the integrative model of breathlessness, in which the emotional experience of breathlessness is considered inseparable from the sensory experience and the biological mechanisms. The experiences of nurses working in the dyspnoea clinics confirms the extent to which, anticipatory anxiety and the emotional flow on the experience of breathlessness have a profound influence on how dyspnoea is managed in practice (Krishnasamy, Corner et al. 2001). Bailey (1995) argues that; symptoms are sometimes generalized too much. Experience is particular, not universal, and an open, accepting and therapeutic approach to managing illness has to be involved with messy and sometimes frightening emotions (p.187) Unlike much of the research literature surrounding dyspnoea management, Cox (2002) Bredin et al(1999), and (Bredin 2003) provide much needed description of the interventions and the rationale behind their use. The suite of interventions that form the basis of the work carried out by specialist nurses in dyspnoea clinics are founded on the following: A detailed physical assessment focussing on breathlessness, its qualitative and quantitative features and its ameliorating and exacerbating factors. Advice and support for patients and their families on ways of managing breathlessness. Training in breathing control techniques, progressive muscle relaxation, and distraction exercises. Collegian Vol 11 No
4 Goal setting to complement breathing and relaxation techniques, to help in the management of functional and social activities, and to support the development and adoption of coping strategies. Early recognition of problems warranting pharmacological or medical intervention. Exploration of the meaning of breathlessness, their disease, and feelings about and plans for the future. These concepts can be explained in a more fundamental way by the formation of a more readily accessible tool devised by the authors of this paper. The mnemonic BREATHE is described simply as: BREATHE Breathing retraining Relaxation techniques Energy expenditure modification Anxiety management: Tools dysponea measurement scales and patient education diaries Help or hinder (ameliorating or exacerbating factors) Emergency plan McHugh and Stephenson, 2004 The subtle complexity of dyspnoea as both a symptom for patients and a clinical management challenge for nurses has prompted authors such as Connolly & O Neill (1999), Krishnasamy (2001) and Cox (2002) to stress the expertise and advanced nature of the practice of the specialist nurses working in dyspnoea clinic. Cox (2002) also notes the extent to which the lack of detailed description and advanced training in the integration of those interventions cited above represent the greatest barriers to informed practice and improved care outcomes for patients with dyspnoea. Review comments I agree that this would be a fantastic advancement and achievement for the nursing-led management of dyspnoea, and would very much represent evidence-based best practice. The health context in the UK is of course different to here in Australia, and the funding for such clinics will not be easily established. There are people also within the nursing profession who are warning of being too specialised, and would argue that this role should be a part of a specialist palliative care nurse role in both the inpatient and community setting. A good article with much merit. Mr Mark Cockayne RN Palliative Care Nurse Cabrini Palliative Care Service, Prahran Reviewers comments There is little doubt that dyspnoea in end-stage disease must rank as highly as pain in terms of its potential for causing severe distress for both patients and their families and confronts nurses with a major clinical challenge in attempting to effectively manage dyspnoea and its sequalae. David Stephenson and Annie McHugh provide us with a brief yet valuable insight into the practice of specialist nurses in respiratory palliative care and the unique contributions that are emerging from this practice area. The concept of specialist nurse led clinics, Conclusion The research reviewed in the above section points to the reproducible success of the nurse-led dyspnoea nursing clinics as an effective means of achieving substantial and sustained improvement in dyspnoea in people with end-stage chronic and malignant respiratory disease It is not difficult to conclude, on the basis of a review of the research literature and the reported practice experiences of clinic nurses in the field, that it is the nurse-led clinic itself that is the critical component in the intervention. The presence of a nurse-led clinic, staffed by expert specialist nurses who provide care, education, guidance and support to dyspnoeic patients along with clinical advice and consultation to other care providers, represents the most important innovation in this area of care. In order to respond adequately to the unmet needs of people with end-stage chronic and malignant respiratory disease, three things are required in the Australian context. 1. Dyspnoea clinics need to be elevated to the status of a firstline clinical management strategy rather than a tertiary component of care. 2. Healthcare systems planners need to invested resources and vision in the development and support of dyspnoea nurse specialists and the organisational infrastructure and material support necessary for the implementation of these clinics. 3. Nurses need to respond to the challenge implicit in the best-available evidence, forge a path toward clinical excellence and take on leadership roles in the innovation of new models and practices on dyspnoea management in the Australian context. whilst not new, remains an exciting area of practice development with potential for making significant positive contributions to patient care. The authors provide a valuable overview of the aetiology and treatment of dyspnoea in both malignant disease and in end-stage respiratory disease. I m not sure that I completely agree with the dichotomous presentation of the medical/symptomatic/ pharmacological treatment of dyspnoea with that of the holistic nursing approach as presented in the article. I accept that for the purposes of differentiation the dichotomy may be useful however I suspect that the differences may not generally be as marked. The evidence for the effectiveness of nurse led clinics appears robust and there is no doubt that there is a need in this country for such services as there is for pulmonary rehabilitation programs. These needs will only increase with the changing demography and disease profiles occurring in Australia. I believe that the authors make a convincing case for the establishment of nurse led dyspnoea clinics that have the potential to provide a valuable service to respiratory patients. I think that they also highlight the need to continue to build the research evidence of the effectiveness of such clinics and I look forward to reading the much-needed future research in this area. Associate Professor Nick Santamaria Principal Research Scientist, Ambulatory and Community Services The Alfred Hospital and University of Melbourne 40 Collegian Vol 11 No
5 References Adams, L. & Gus, A. (1996). Respiratory Sensation. New York: Marcel Dekker Inc. ATS (1999). Dyspnoea. Mechanisms, Assessment and Management: A Consensus Statement. American Journal of Respiratory and Critical Care Medicine 159: Bailey, C. (1995). Nursing as Therapy in the Management of Breathlessness in Lung Cancer. European Journal of Cancer Care 4(4): Bailey, C. (1997). Palliative Care: Breathlessness. Nursing Times: Learning Curve 1(6): 1-4. Benor, D., Delbar, V. & Krulik, T. (1998). Measuring the Impact of Nursing Intervention on Cancer Patients Ability to Control Symptoms. Cancer Nursing 21: Booth, S. (1998a). Management of Dyspnoea in Advanced Cancer. British Journal of Therapy and Rehabilitation 5(6): 282. Booth, S. (1998b). The Management of Dyspnoea in Advanced Cancer. Hospital Medicine (London) 59(5): Brant, J. (1998). The Art of Palliative Care: Living with Hope, Dying with Dignity. Oncology Nursing Forum 25(6): Bredin, M. (2003). Breathlessness. Palliative Care Nursing: A Guide To Practice. Aranda, S. & O Connor, M. Melbourne: Ausmed Publications. Bredin, M., Corner, J., Krishnasamy, M., et al. (1999). Multicentre Randomised Controlled Trial of Nursing Interventions for Breathlessness in Patients with Lung Cancer. British Medical Journal 318(7188): Bruera, E., Macmillan, K., Pither, J., et al. (1990). Effects of Morphine on the Dyspnoea of the Terminal Cancer Patient. Journal of Pain and Symptom Management 5(6): Bruera, E., Schmitz, B., Pither, J., et al. (2000). The Frequency and Correlates of Dyspnoea in Patients with Advanced Cancer. Journal of Pain and Symptom Management 19(5): Chan, K.-S., Sham, M., Tse, D., et al. (2004). Palliative Medicine in Malignant Respiratory Diseases. The Oxford Textbook of Palliative Medicine. Doyle, D., Hanks, G., Cherny, N. & Calman, K. Oxford: Oxford University Press. Congleton, J. & Muers, M. (1995). The Incidence of Airflow Obstruction in Bronchial Carcinoma, Its Relation to Breathlessness, and Response to Bronchodilator Therapy. Respiratory Medicine 89(4): Connolly, M. & O Neill, J. (1999). Teaching a Research-based Approach to the Management of Breathlessness in Patients with Lung Cancer. European Journal of Cancer Care 8(30-36). Corner, J. & O Driscoll, M. (1999). Development of a Breathlessness Assessment Guide for Use in Lung Cancer. Palliative Medicine 13: Corner, J., Plant, H., A Hern, R., et al. (1996). Non-pharmacological Intervention for Breathlessness in Lung Cancer. Palliative Medicine 10(4): Cox, C. (2002). Non-pharmacological treatment of breathlessness. Nursing Standard 16(24): Davis, C. (1997). ABC of Palliative Care: Breathlessness, Cough, and Other Respiratory Problems. British Medical Journal 315(7113): Devine, E. & Pearcy, J. (2002). Meta-analysis of the Effects of Psychoeducational Care in Adults with Chronic Obstructive Pulmonary Disease. Database of Abstracts of Reviews of Effectiveness: December. Drings, P. (1997). Dyspnoea and Cancer: Support in Agonizing Conditions. Supportive Care in Cancer 5(2): Dudgeon, D. & Lertzman, M. (1998). Dyspnoea in the Advanced Cancer Patient. Journal of Pain and Symptom Management 26(4): Edmonds, P., Higginson, I., Altmann, D., et al. (2000). Is the Presence of Dyspnoea a Risk Factor for Morbidity in Cancer Patients? Journal of Pain and Symptom Management 19(1): Enck, R. (1989). The Management of Dyspnea. American Journal of Hospice and Palliative Care 6(4): Gift, A., Moore, T. & Seoken, K. (1992). Relaxation to Reduce Dyspnoea and Anxiety in COPD Patients. Nursing Research 41(4): Grahn, G. (1996). Patient Information as a Necessary Therapeutic Intervention. European Journal of Cancer Care 5(1): 1-8. Guell, G., Casan, P., Belda, J., et al. (2000). Long-term Effects of Outpatient Rehabilitation of COPD: A Randomised Trial. Chest 7(4): Hanratty, J. & Higginson, I. (1994). Palliative Care in Terminal Illness. Oxford: Radcliffe Medical Press. Heyse-Moore, L., Ross, V. & Mullee, M. (1991). How Much of a Problem is Dyspnoea in Advanced Cancer? Palliative Medicine 5(20-26). Higginson, I. & McCarthy, M. (1989). Measuring Symptoms in Terminal Cancer: Are Pain and Dyspnoea Controlled. Journal of the Royal Society of Medicine 82( ). Krishnasamy, M., Corner, J., Bredin, M., et al. (2001). Cancer Nursing Practice Development: Understanding Breathlessness. Journal of Clinical Nursing 10(1): Le Grand, S. & Walsh, D. (1999). Palliative Management of Dyspnoea in Advanced Cancer. Current Opinion in Oncology 11(4): Levy, M. (2001). Palliaitve Care in Respiratory Care: Mexico Conference Summary. 2002: Madjar, I. (1998). The Body in Health, Illness and Pain. The Body in Nursing. Lawler, J. Melbourne: Churchill Livingstone: McMahon, R. (1991). Therapeutic Nursing: Theory, Issues and Practice. Nursing as Therapy. McMahon R & Pearson, A. London: Chapman and Hall. Muers, M. & Round, C. (1993). Palliation of Symptoms in Non-small Cell Lung Cancer: A Study by The Yorkshire Regional Cancer Organisation Thoracic Group. Thorax 48(4): Pauwels, R., Buist, A., Calverley, P., et al. (2001). Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease: National Heart, Lung, and Blood Institute and World Health Organization Global Initiative for Chronic Obstructive Lung Disease (GOLD): Executive Summary. 2002: Rawlinson, F. (2000). Dyspnoea and Cough. European Journal of Palliative Care 7(5): Reuben, D. & Mor, V. (1986). Dyspnoea in Terminally Ill Cancer Patients. Chest 89: Richards, D. (1953). The Nature of Cardiac and Pulmonary Dyspnea. Circulation 7: Ripamonti, C. (1999). Management of Dyspnoea in Advanced Cancer Patients. Supportive Care in Cancer 7(4): Ripamonti, C. & Bruera, E. (1997). Dyspnea: Pathophysiology and Assessment. Journal of Pain and Symptom Management 13: Roberts, D., Thorne, S. & Person, C. (1993). The Experience of Dyspnoea in Late Stage Cancer: Patients and Nurses Perspectives. Cancer Nursing 16(4): Rousseau, P. (2002). Non-pain Symptom Control in the Dying Patient. Hospital Physician 38(2): Tarzain, A. (2000). Caring for Dying Patients Who Have Air Hunger. Journal of Nursing Scholarship 32(2): Collegian Vol 11 No
COPD Management in the community
 COPD Management in the community Anne Jones Independent Respiratory Nurse Consultant RN,BSc(Hons),PGDip(RespMed)/MA Content of session Will consider the impact of COPD COPD Strategy recommendations and
COPD Management in the community Anne Jones Independent Respiratory Nurse Consultant RN,BSc(Hons),PGDip(RespMed)/MA Content of session Will consider the impact of COPD COPD Strategy recommendations and
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Guidelines for the appointment of. General Practitioners with Special Interests in the Delivery of Clinical Services. Respiratory Medicine
 Guidelines for the appointment of General Practitioners with Special Interests in the Delivery of Clinical Services Respiratory Medicine April 2003 Respiratory Medicine This General Practitioner with a
Guidelines for the appointment of General Practitioners with Special Interests in the Delivery of Clinical Services Respiratory Medicine April 2003 Respiratory Medicine This General Practitioner with a
Respiratory Nursing 2015
 QRC: 2208 Price One Day : $363 inc. GST Two Days: $490 inc. GST Date 25-26 May 2015 Venue Hotel IBIS - Therry Street 15-21 Therry Street, Melbourne, VI, 3000 CPD Hours 12 Hours 0 Mins Respiratory Nursing
QRC: 2208 Price One Day : $363 inc. GST Two Days: $490 inc. GST Date 25-26 May 2015 Venue Hotel IBIS - Therry Street 15-21 Therry Street, Melbourne, VI, 3000 CPD Hours 12 Hours 0 Mins Respiratory Nursing
Evaluation Tool* Clinical Standards ~ March 2010 Chronic Obstructive Pulmonary Disease** Services
 Evaluation Tool* Clinical Standards ~ March 2010 Chronic Obstructive Pulmonary Disease** Services *Formerly known as Self-Assessment Framework ** Chronic Obstructive Pulmonary Disease (COPD) Standard 1:
Evaluation Tool* Clinical Standards ~ March 2010 Chronic Obstructive Pulmonary Disease** Services *Formerly known as Self-Assessment Framework ** Chronic Obstructive Pulmonary Disease (COPD) Standard 1:
Breathlessness and the Family
 Breathlessness and the Family International Breathlessness Conference: Developing treatments for breathlessness Copenhagen - 7th May 2015 Dr Morag Farquhar (edited version of slides for web) Impact of
Breathlessness and the Family International Breathlessness Conference: Developing treatments for breathlessness Copenhagen - 7th May 2015 Dr Morag Farquhar (edited version of slides for web) Impact of
National Standards Assessment Program. Quality Report
 National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
Introduction to the lung cancer multi disciplinary team (MDT)
 Royal Berkshire NHS Foundation Trust London Road Reading Berkshire RG1 5AN 0118 322 51111 (Switchboard) www.royalberkshire.nhs.uk This document can be made available in other languages and formats upon
Royal Berkshire NHS Foundation Trust London Road Reading Berkshire RG1 5AN 0118 322 51111 (Switchboard) www.royalberkshire.nhs.uk This document can be made available in other languages and formats upon
A nursing intervention to assist in the management of breathlessness Meeting with Community Partners, Bayshore Friday November 9 th, 2007 Cathy
 A nursing intervention to assist in the management of breathlessness Meeting with Community Partners, Bayshore Friday November 9 th, 2007 Cathy Kiteley Sharilee Cox-Arseneault Jennifer Parkins Welcome
A nursing intervention to assist in the management of breathlessness Meeting with Community Partners, Bayshore Friday November 9 th, 2007 Cathy Kiteley Sharilee Cox-Arseneault Jennifer Parkins Welcome
Alberta Breathes: Proposed Standards for Respiratory Health of Albertans
 Alberta Breathes: Proposed Standards for Respiratory Health of Albertans The concept of Alberta Breathes and these standards was developed in consultation with over 150 health professionals and stakeholders
Alberta Breathes: Proposed Standards for Respiratory Health of Albertans The concept of Alberta Breathes and these standards was developed in consultation with over 150 health professionals and stakeholders
Module 2 Excellence in practice
 Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
Module 2 Excellence in practice This module sets out the key skills required by specialist nurses caring for patients with metastatic breast cancer. It also examines key interventions undertaken by nurses
DRAFT Optimal Care Pathway
 DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
DRAFT Optimal Care Pathway 1. Introduction... 3 1.1 Background... 3 1.2 Intent of the Optimal Care Pathways... 3 1.3 Key principles of care... 3 2. Steps in the care of patients with x cancer... 4 Step
Baseline. Eight Months later
 Baseline Eight Months later 12 months later later Minimal Dependency Unit I feel absolutely wretched as though all my available energy has almost run out Diagnosis & Co-morbidities Bronchoscopy* Bespoke
Baseline Eight Months later 12 months later later Minimal Dependency Unit I feel absolutely wretched as though all my available energy has almost run out Diagnosis & Co-morbidities Bronchoscopy* Bespoke
INTERNAL MEDICINE RESPIRATORY MEDICINE ROTATION OBJECTIVES
 INTERNAL MEDICINE RESPIRATORY MEDICINE ROTATION OBJECTIVES A. The following goals/objectives cover the breadth of respirology for an internal medicine residency. While many objectives may be covered during
INTERNAL MEDICINE RESPIRATORY MEDICINE ROTATION OBJECTIVES A. The following goals/objectives cover the breadth of respirology for an internal medicine residency. While many objectives may be covered during
Professor Lutz Beckert. Dr Amanda Landers. 12:00-12:30 Identifying Milestones in Severe COPD to Initiate End of Life Discussions -
 Professor Lutz Beckert Department of Respiratory Medicine University of Otago, Christchurch Dr Amanda Landers Palliative Care Specialist University of Otago 12:00-12:30 Identifying Milestones in Severe
Professor Lutz Beckert Department of Respiratory Medicine University of Otago, Christchurch Dr Amanda Landers Palliative Care Specialist University of Otago 12:00-12:30 Identifying Milestones in Severe
End of Life Care. LONDON: The Stationery Office Ordered by the House of Commons to be printed on 24 November 2008
 End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
providing an overview of what an integrated system can offer its respiratory population both in and out of hospital
 PRIMARY CARE R E S P I R AT O R Y S O C I E T Y U K A population-focused respiratory service framework providing an overview of what an integrated system can offer its respiratory population both in and
PRIMARY CARE R E S P I R AT O R Y S O C I E T Y U K A population-focused respiratory service framework providing an overview of what an integrated system can offer its respiratory population both in and
North Central London Sustainability and Transformation Plan. A summary
 Sustainability and Transformation Plan A summary N C L Introduction Hospitals, local authorities, GPs, commissioners, and mental health trusts across north central London have all come together to transform
Sustainability and Transformation Plan A summary N C L Introduction Hospitals, local authorities, GPs, commissioners, and mental health trusts across north central London have all come together to transform
Service Mapping Report
 Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Alfred Health, Cabrini Health,
Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Alfred Health, Cabrini Health,
HS&DR Programme Application Plain English Summaries
 HS&DR Programme Application Plain English Summaries To assist applicants to the HS&DR programme, the following three recently funded project Plain English Summaries are provided. These were highlighted
HS&DR Programme Application Plain English Summaries To assist applicants to the HS&DR programme, the following three recently funded project Plain English Summaries are provided. These were highlighted
Heading Towards a COPD Care Pathway
 June 20, 2013 Heading Towards a COPD Care Pathway Dr Luc Van Zandweghe Pulmonologist Head Nurse AZ Sint-Blasius Dendermonde Belgium 1 AZ Sint-Blasius Where We Are Located Dendermonde Zele AZ Sint-Blasius
June 20, 2013 Heading Towards a COPD Care Pathway Dr Luc Van Zandweghe Pulmonologist Head Nurse AZ Sint-Blasius Dendermonde Belgium 1 AZ Sint-Blasius Where We Are Located Dendermonde Zele AZ Sint-Blasius
We need to talk about Palliative Care. The Care Inspectorate
 We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
NHSGGC Respiratory Managed Clinical Network Annual Report 2010/11 Executive Summary and Table of Contents
 NHSGGC Respiratory Managed Clinical Network Annual Report 2010/11 Executive Summary and Table of Contents The full report is available on the Respiratory MCN Website www.nhsggc.org.uk/respmcn 1. Executive
NHSGGC Respiratory Managed Clinical Network Annual Report 2010/11 Executive Summary and Table of Contents The full report is available on the Respiratory MCN Website www.nhsggc.org.uk/respmcn 1. Executive
National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI)
 October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart
 CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
CLINICAL PROTOCOL National Early Warning Score (NEWS) Observation Chart November 2014 1 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
Service Mapping Report
 Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Service Mapping Report Background and purpose One of the roles of the Southern Melbourne Integrated Cancer Service (SMICS) is to map cancer services provided to adults by Bayside Health, Cabrini Health,
Framework for Cancer CNS Development (Band 7)
 Framework for Cancer CNS Development (Band 7) Opening Statement This framework provides a common understanding of the CNS role across the London Cancer Alliance and will be used to support the development
Framework for Cancer CNS Development (Band 7) Opening Statement This framework provides a common understanding of the CNS role across the London Cancer Alliance and will be used to support the development
Contents. Introduction 3. Required knowledge and skills 4. Section One: Knowledge and skills for all nurses and care staff 6
 Decision-making frameworks in advanced dementia: Links to improved care project. Page 2 of 17 Contents Introduction 3 Required knowledge and skills 4 Section One: Knowledge and skills for all nurses and
Decision-making frameworks in advanced dementia: Links to improved care project. Page 2 of 17 Contents Introduction 3 Required knowledge and skills 4 Section One: Knowledge and skills for all nurses and
Effectively implementing multidisciplinary. population segments. A rapid review of existing evidence
 Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Safety reporting in multi-site clinical trials in Palliative Care
 Safety reporting in multi-site clinical trials in Palliative Care Belinda Fazekas Linda Devilee Zac Vandersman David Currow Flinders University receives funding for PaCCSC from the Australian Government
Safety reporting in multi-site clinical trials in Palliative Care Belinda Fazekas Linda Devilee Zac Vandersman David Currow Flinders University receives funding for PaCCSC from the Australian Government
Division of Clinical Psychology Faculty of Clinical Health Psychology. Briefing Paper No. 27 Clinical Health Psychologists in the NHS
 Division of Clinical Psychology Faculty of Clinical Health Psychology Briefing Paper No. 27 Clinical Health Psychologists in the NHS January 2008 Briefing Paper No. 27 Clinical Health Psychologists in
Division of Clinical Psychology Faculty of Clinical Health Psychology Briefing Paper No. 27 Clinical Health Psychologists in the NHS January 2008 Briefing Paper No. 27 Clinical Health Psychologists in
Introduction to Population Health Healthcare Public Health
 Introduction to Population Health Healthcare Public Health Dr Jason Horsley Senior Clinical Lecturer in Public Health, ScHARR Consultant in Public Health, Sheffield City Council j.horsley@sheffield.ac.uk
Introduction to Population Health Healthcare Public Health Dr Jason Horsley Senior Clinical Lecturer in Public Health, ScHARR Consultant in Public Health, Sheffield City Council j.horsley@sheffield.ac.uk
One Chance to Get it Right:
 One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
1. Guidance notes. Social care (Adults, England) Knowledge set for end of life care. (revised edition, 2010) What are knowledge sets?
 Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
End of Life Care Strategy
 End of Life Care Strategy 2016-2020 Foreword Southern Health NHS Foundation Trust is committed to providing the highest quality care for patients, their families and carers. Therefore, I am pleased to
End of Life Care Strategy 2016-2020 Foreword Southern Health NHS Foundation Trust is committed to providing the highest quality care for patients, their families and carers. Therefore, I am pleased to
Hayward House Macmillan Specialist Palliative Care Cancer Unit. Resuscitation Policy for Inpatients
 Hayward House Macmillan Specialist Palliative Care Cancer Unit Resuscitation Policy for Inpatients Introduction Hayward House cares for patients with advanced cancer or motor neurone disease and aims to
Hayward House Macmillan Specialist Palliative Care Cancer Unit Resuscitation Policy for Inpatients Introduction Hayward House cares for patients with advanced cancer or motor neurone disease and aims to
Hospice Isle of Man Education Prospectus 2018
 Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Your Results for: "NCLEX Review"
 Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
INTRODUCTION. LEARNING OBJECTIVES (CanMEDS)
 OVERVIEW The Thoracic Surgery selective is based at Health Sciences Centre. Students participate in the surgical management of patients with lung cancer and esophageal cancer, as well as other conditions
OVERVIEW The Thoracic Surgery selective is based at Health Sciences Centre. Students participate in the surgical management of patients with lung cancer and esophageal cancer, as well as other conditions
Supportive Care Roundtable
 Supportive Care Roundtable Brussels, 20 February 2018 1 Preface Cancer supportive care is the prevention and management of the symptoms and side effects of cancer and its treatment across the cancer continuum
Supportive Care Roundtable Brussels, 20 February 2018 1 Preface Cancer supportive care is the prevention and management of the symptoms and side effects of cancer and its treatment across the cancer continuum
Together for Health A Respiratory Health Delivery Plan. A Delivery Plan up to 2017 for the NHS and its partners
 Together for Health A Respiratory Health Delivery Plan A Delivery Plan up to 2017 for the NHS and its partners Date of Issue: 29 April 2014 Digital ISBN 978 1 4734 1110 4 Crown copyright 2014 WG21465 CONTENTS
Together for Health A Respiratory Health Delivery Plan A Delivery Plan up to 2017 for the NHS and its partners Date of Issue: 29 April 2014 Digital ISBN 978 1 4734 1110 4 Crown copyright 2014 WG21465 CONTENTS
The National Healthcare Group Advance Care Programme (NHG ACP)
 1 The National Healthcare Group Advance Care Programme (NHG ACP) An end-of-life care programme for advanced COPD, end-stage heart failure & end-stage renal failure 2 How it all started Concept of Chronic
1 The National Healthcare Group Advance Care Programme (NHG ACP) An end-of-life care programme for advanced COPD, end-stage heart failure & end-stage renal failure 2 How it all started Concept of Chronic
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth
 Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Criteria and Guidance for referral to Specialist Palliative Care Services
 Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Living With Long Term Conditions A Policy Framework
 April 2012 Living With Long Term Conditions A Policy Framework Living with Long Term Conditions Contents Page Number Minister s Foreword 3 Introduction 4 Principles 13 Chapter 1 Working in partnership
April 2012 Living With Long Term Conditions A Policy Framework Living with Long Term Conditions Contents Page Number Minister s Foreword 3 Introduction 4 Principles 13 Chapter 1 Working in partnership
Executive Summary 10 th September Dr. Richard Wagland. Dr. Mike Bracher. Dr. Ana Ibanez Esqueda. Professor Penny Schofield
 Experiences of Care of Patients with Cancer of Unknown Primary (CUP): Analysis of the 2010, 2011-12 & 2013 Cancer Patient Experience Survey (CPES) England. Executive Summary 10 th September 2015 Dr. Richard
Experiences of Care of Patients with Cancer of Unknown Primary (CUP): Analysis of the 2010, 2011-12 & 2013 Cancer Patient Experience Survey (CPES) England. Executive Summary 10 th September 2015 Dr. Richard
A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland
 A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland The aim of this session To refresh our memories about what a competency is To give a bit
A Specialist Palliative Care Nurses Competency Framework Helen Butler Education Team Leader Mercy Hospice Auckland The aim of this session To refresh our memories about what a competency is To give a bit
DRAFT. Rehabilitation and Enablement Services Redesign
 DRAFT Rehabilitation and Enablement Services Redesign Services Vision Statement Inverclyde CHP is committed to deliver Adult rehabilitation services that are easily accessible, individually tailored to
DRAFT Rehabilitation and Enablement Services Redesign Services Vision Statement Inverclyde CHP is committed to deliver Adult rehabilitation services that are easily accessible, individually tailored to
UK HEALERS - Quality Criteria Training
 This document defines the minimum training standards for healers in member organisations accredited by UK Healers to ensure that healers registered with UK Healers have undergone a procedure of training,
This document defines the minimum training standards for healers in member organisations accredited by UK Healers to ensure that healers registered with UK Healers have undergone a procedure of training,
Payment Reforms to Improve Care for Patients with Serious Illness
 Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Scottish Medicines Consortium. A Guide for Patient Group Partners
 Scottish Medicines Consortium Advising on new medicines for Scotland www.scottishmedicines.org page 1 Acknowledgements Some of the information in this booklet is adapted from guidance produced by the HTAi
Scottish Medicines Consortium Advising on new medicines for Scotland www.scottishmedicines.org page 1 Acknowledgements Some of the information in this booklet is adapted from guidance produced by the HTAi
Coordinated cancer care: better for patients, more efficient. Background
 the voice of NHS leadership briefing June 2010 Issue 203 Coordinated cancer care: Key points There are two million people with cancer in the UK. It is suggested that by 2030 there will be over four million
the voice of NHS leadership briefing June 2010 Issue 203 Coordinated cancer care: Key points There are two million people with cancer in the UK. It is suggested that by 2030 there will be over four million
National Stroke Nursing Forum Nurse Staffing of Stroke Early Supported Discharge Teams A Position Statement for Guidance of Service Developments
 National Stroke Nursing Forum Nurse Staffing of Stroke Early Supported Discharge Teams A Position Statement for Guidance of Service Developments Introduction This paper is a position statement from the
National Stroke Nursing Forum Nurse Staffing of Stroke Early Supported Discharge Teams A Position Statement for Guidance of Service Developments Introduction This paper is a position statement from the
End of Life PSP Module. Case Study: Mr. James Lee
 Case Study: Mr. James Lee Mr. James Lee is a 74 yr old retired electrician. He is married to Mary with two children in their 30 s. They have been in Canada for 35 years and are fluent in English and Cantonese.
Case Study: Mr. James Lee Mr. James Lee is a 74 yr old retired electrician. He is married to Mary with two children in their 30 s. They have been in Canada for 35 years and are fluent in English and Cantonese.
COPD Dyspnea Palliation Project: Dyspnea Palliation in End-Stage COPD Patients
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Doctor of Nursing Practice (DNP) Projects College of Nursing 2014 COPD Dyspnea Palliation Project: Dyspnea Palliation in End-Stage COPD Patients
University of Massachusetts Amherst ScholarWorks@UMass Amherst Doctor of Nursing Practice (DNP) Projects College of Nursing 2014 COPD Dyspnea Palliation Project: Dyspnea Palliation in End-Stage COPD Patients
Do Not Attempt Resuscitation Policy
 Do Not Attempt Resuscitation Policy PROV 27 March 2009 1 Document Management Title of document Do Not Attempt Resuscitation Policy Type of document Policy PROV 27 Description To ensure that do not resuscitate
Do Not Attempt Resuscitation Policy PROV 27 March 2009 1 Document Management Title of document Do Not Attempt Resuscitation Policy Type of document Policy PROV 27 Description To ensure that do not resuscitate
Improving family experiences in ICU. Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU
 Improving family experiences in ICU Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU Family Burden in icu:- Incidence of anxiety symptoms range from 21% to 60.4% (median 40%) from ICU admission
Improving family experiences in ICU Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU Family Burden in icu:- Incidence of anxiety symptoms range from 21% to 60.4% (median 40%) from ICU admission
Independent investigation into the death of Mr Stephen Keogh a prisoner at HMP Manchester on 24 April 2016
 Independent investigation into the death of Mr Stephen Keogh a prisoner at HMP Manchester on 24 April 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr Stephen Keogh a prisoner at HMP Manchester on 24 April 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms
 Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms Guide for setting up IAPT-LTC services 1. Aims The
Psychological Therapies for Depression and Anxiety Disorders in People with Longterm Physical Health Conditions or with Medically Unexplained Symptoms Guide for setting up IAPT-LTC services 1. Aims The
Job Description. Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7. Department: Cancer Services Hours: 30
 Job Description Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 30 Reports to: Lead Nurse for Cancer We are a pioneering research active organisation and
Job Description Job title: Gynae-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 30 Reports to: Lead Nurse for Cancer We are a pioneering research active organisation and
Quality and Leadership: Improving outcomes
 Quality and Leadership: Improving outcomes Podiatry Managers/Allied Health Managers and Leaders 5 March 2014 Shelagh Morris OBE Acting Chief Allied Health Professions Officer 2 http://www.nhsemployers.org/aboutus/latest-news/pages/the-new-nhs-in-2013-infographic.aspx
Quality and Leadership: Improving outcomes Podiatry Managers/Allied Health Managers and Leaders 5 March 2014 Shelagh Morris OBE Acting Chief Allied Health Professions Officer 2 http://www.nhsemployers.org/aboutus/latest-news/pages/the-new-nhs-in-2013-infographic.aspx
QUALIFICATION HANDBOOK
 QUALIFICATION HANDBOOK Level 2, 3 & 5 Awards and Certificates in End of Life Care (3571-02-03-04-05) May 2013 Version 5.0 Qualification at a glance Subject area City & Guilds number 3571 End of life care
QUALIFICATION HANDBOOK Level 2, 3 & 5 Awards and Certificates in End of Life Care (3571-02-03-04-05) May 2013 Version 5.0 Qualification at a glance Subject area City & Guilds number 3571 End of life care
Eastern Palliative Care. Model of care
 Eastern Palliative Care Model of care 2009 Model of Care At EPC we actively engage with people and their families to develop a therapeutic relationship. We journey with them, recognising the essence of
Eastern Palliative Care Model of care 2009 Model of Care At EPC we actively engage with people and their families to develop a therapeutic relationship. We journey with them, recognising the essence of
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT)
 TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
Core Domain You will be able to: You will know and understand: Leadership, Management and Team Working
 DEGREE APPRENTICESHIP - REGISTERED NURSE 1 ST0293/01 Occupational Profile: A career in nursing is dynamic and exciting with opportunities to work in a range of different roles as a Registered Nurse. Your
DEGREE APPRENTICESHIP - REGISTERED NURSE 1 ST0293/01 Occupational Profile: A career in nursing is dynamic and exciting with opportunities to work in a range of different roles as a Registered Nurse. Your
Range of Variables Statements and Evidence Guide. December 2010
 Range of Variables Statements and Evidence Guide December 2010 Unit 1 Demonstrates knowledge sufficient to ensure safe practice. Each of the competency elements in this unit needs to be reflected in the
Range of Variables Statements and Evidence Guide December 2010 Unit 1 Demonstrates knowledge sufficient to ensure safe practice. Each of the competency elements in this unit needs to be reflected in the
Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016
 Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
Independent investigation into the death of Mr David Adkins a prisoner at HMP Whatton on 14 September 2016 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence
National care of the dying audit for hospitals, England Executive summary May 2014
 National care of the dying audit for hospitals, England Executive summary May 2014 Foreword We only have one chance to get end of life care right and sadly sometimes we don t. There are few surprises in
National care of the dying audit for hospitals, England Executive summary May 2014 Foreword We only have one chance to get end of life care right and sadly sometimes we don t. There are few surprises in
Challenging The 2015 PH Guidelines - comments from the Nurses. Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust
 Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
The latest information and insight for inspired nursing care
 The latest information and insight for inspired nursing care The essential information resource for the whole nursing team RCNi is a wholly-owned part of the Royal College of Nursing, one of the world
The latest information and insight for inspired nursing care The essential information resource for the whole nursing team RCNi is a wholly-owned part of the Royal College of Nursing, one of the world
Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy
 Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy 2016-2017 Contents Acknowledgements Subject Page Number 1. Introduction 4 2. Vision 5 3. National policy Context 5-6 4. Local
Calderdale and Huddersfield NHS Foundation Trust End of Life Care Strategy 2016-2017 Contents Acknowledgements Subject Page Number 1. Introduction 4 2. Vision 5 3. National policy Context 5-6 4. Local
End of Life Care Review Case Review Audit
 Case Review Audit : : Version: 1 NHS Wales (Intranet) / Public Health Wales (Intranet) Purpose and summary of document: This document is for use by general practices who are engaged in providing services
Case Review Audit : : Version: 1 NHS Wales (Intranet) / Public Health Wales (Intranet) Purpose and summary of document: This document is for use by general practices who are engaged in providing services
Table S1 KEYWORDS USED TO SEARCH THE LITERATURE
 Table S1 KEYWORDS USED TO SEARCH THE LITERATURE COPD, CHRONIC OBSTRUCTIVE PULMONARY DIS*", CHRONIC OBSTRUCTIVE AIRWAY DIS*, CHRONIC LUNG DIS*, CHRONIC LUNG ILLNESS, CHRONIC PULMONARY ILLNESS, CHRONIC PULMONARY
Table S1 KEYWORDS USED TO SEARCH THE LITERATURE COPD, CHRONIC OBSTRUCTIVE PULMONARY DIS*", CHRONIC OBSTRUCTIVE AIRWAY DIS*, CHRONIC LUNG DIS*, CHRONIC LUNG ILLNESS, CHRONIC PULMONARY ILLNESS, CHRONIC PULMONARY
Stockport Strategic Vision. for. Palliative Care and End of Life Care Services. Final Version. Ratified by the End of Life Care Programme Board
 Stockport Strategic Vision for Palliative Care and End of Life Care Services Final Version Ratified by the End of Life Care Programme Board on 8 th February 2012 Clinical Commissioning Pathfinder Contents
Stockport Strategic Vision for Palliative Care and End of Life Care Services Final Version Ratified by the End of Life Care Programme Board on 8 th February 2012 Clinical Commissioning Pathfinder Contents
Coding Guidelines for Certain Respiratory Care Services January 2018 (updates in red)
 Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
Theory Application: Theory of Comfort. RobERT Pinkston. Old Dominion University
 Running head: THEORY OF COMFORT 1 Theory Application: Theory of Comfort RobERT Pinkston Old Dominion University THEORY OF COMFORT 2 THEORY APPLICATION: THEORY OF COMFORT The Theory of Comfort was developed
Running head: THEORY OF COMFORT 1 Theory Application: Theory of Comfort RobERT Pinkston Old Dominion University THEORY OF COMFORT 2 THEORY APPLICATION: THEORY OF COMFORT The Theory of Comfort was developed
Quick guide: planning for increased seasonal demand in respiratory illness
 Quick guide: planning for increased seasonal demand in respiratory illness Published by NHS England and NHS Improvement December 2017 The British Thoracic Society is pleased to endorse this quick guide,
Quick guide: planning for increased seasonal demand in respiratory illness Published by NHS England and NHS Improvement December 2017 The British Thoracic Society is pleased to endorse this quick guide,
Bratislava
 Practice consultant at the local hospital Herlev Practice consultant in the municipality of Gladsaxe Early detection, management and pulmonary rehabilitation of COPD How can general practice and specialist
Practice consultant at the local hospital Herlev Practice consultant in the municipality of Gladsaxe Early detection, management and pulmonary rehabilitation of COPD How can general practice and specialist
If patient is 24 hour dependent on NIV and decides to discontinue it, support and forward planning are essential
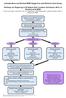 Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY
 THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
THE VIRTUAL WARD MANAGING THE CARE OF PATIENTS WITH CHRONIC (LONG-TERM) CONDITIONS IN THE COMMUNITY An Economic Assessment of the South Eastern Trust Virtual Ward Introduction and Context Chronic (long-term)
PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS. Dawn Chaitram BSW, RSW, MA Psychosocial Specialist
 PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS Dawn Chaitram BSW, RSW, MA Psychosocial Specialist WRHA Palliative Care Program April 19, 2017 OUTLINE Vulnerability and Compassion Addressing
PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS Dawn Chaitram BSW, RSW, MA Psychosocial Specialist WRHA Palliative Care Program April 19, 2017 OUTLINE Vulnerability and Compassion Addressing
Job Description. Job title: Uro-Oncology Clinical Nurse Specialist Band: 7
 Job Description Job title: Uro-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 37.5 (min 22.5 hrs) Reports to: Lead Nurse for Cancer We are a pioneering research active organisation
Job Description Job title: Uro-Oncology Clinical Nurse Specialist Band: 7 Department: Cancer Services Hours: 37.5 (min 22.5 hrs) Reports to: Lead Nurse for Cancer We are a pioneering research active organisation
Routine Dyspnea Assessment on Unit Admission
 CE 2.4 HOURS Continuing Education Routine Dyspnea Assessment on Unit Admission Is it feasible for nurses to quantify and document this important prognostic marker? OVERVIEW: Dyspnea assessment is valuable
CE 2.4 HOURS Continuing Education Routine Dyspnea Assessment on Unit Admission Is it feasible for nurses to quantify and document this important prognostic marker? OVERVIEW: Dyspnea assessment is valuable
Planning and Organising End of Life Care
 GUIDE Palliative Care Network Planning and Organising End of Life Care A Guide for Clinical Model Development Collaboration. Innovation. Better Healthcare. The Agency for Clinical Innovation (ACI) works
GUIDE Palliative Care Network Planning and Organising End of Life Care A Guide for Clinical Model Development Collaboration. Innovation. Better Healthcare. The Agency for Clinical Innovation (ACI) works
Coordinated Veterans Care (CVC) Toolkit Questionnaires for use in a comprehensive needs assessment
 Coordinated Veterans Care (CVC) Toolkit Questionnaires for use in a comprehensive needs assessment This resource is a guide to conducting a comprehensive needs assessment for the Coordinated Veterans Care
Coordinated Veterans Care (CVC) Toolkit Questionnaires for use in a comprehensive needs assessment This resource is a guide to conducting a comprehensive needs assessment for the Coordinated Veterans Care
End of Life Care A National Policy Perspective
 End of Life Care A National Policy Perspective END OF LIFE CARE A NATIONAL POLICY PERSPECTIVE Dr Matthew Anstey I n t ensive C a r e P h ysician S i r C h arles G a i r dner H o s p ital M e d i cal A
End of Life Care A National Policy Perspective END OF LIFE CARE A NATIONAL POLICY PERSPECTIVE Dr Matthew Anstey I n t ensive C a r e P h ysician S i r C h arles G a i r dner H o s p ital M e d i cal A
Integrated respiratory action network for patients with COPD
 Integrated respiratory action network for patients with COPD In this Future Hospital Programme case study Dr Helen Ward describes how a team from The Royal Wolverhampton NHS Trust established a respiratory
Integrated respiratory action network for patients with COPD In this Future Hospital Programme case study Dr Helen Ward describes how a team from The Royal Wolverhampton NHS Trust established a respiratory
Return to independent living Self manage breathing techniques, secretion clearance Recognize early symptoms of COPD exacerbation
 CLINICAL PATHWAY Chronic Obstructive Pulmonary Disease Exacerbation (COPD-E) Civic General Clinical Frailty Scale (At baseline, at least 2 weeks before hospitalization) Init. Diagram Frailty Scale Description
CLINICAL PATHWAY Chronic Obstructive Pulmonary Disease Exacerbation (COPD-E) Civic General Clinical Frailty Scale (At baseline, at least 2 weeks before hospitalization) Init. Diagram Frailty Scale Description
Palliative and Hospice Care In the United States Jean Root, DO
 Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Serious Medical Treatment Decisions. BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE
 Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
Serious Medical Treatment Decisions BEST PRACTICE GUIDANCE FOR IMCAs END OF LIFE CARE Contents Introduction... 3 End of Life Care (EoLC)...3 Background...3 Involvement of IMCAs in End of Life Care...4
Improving General Practice for the People of West Cheshire
 Improving General Practice for the People of West Cheshire Huw Charles-Jones (GP Chair, West Cheshire Clinical Commissioning Group) INTRODUCTION There is a growing consensus that the current model of general
Improving General Practice for the People of West Cheshire Huw Charles-Jones (GP Chair, West Cheshire Clinical Commissioning Group) INTRODUCTION There is a growing consensus that the current model of general
Alison Hunter. Improvement Advisor, Acute Adult Safety Programme. Healthcare Improvement Scotland
 Alison Hunter Improvement Advisor, Acute Adult Safety Programme Healthcare Improvement Scotland Acute Adult 2008 what we did Leadership Medicines Perioperative Critical Care Reduce Mortality & Harm General
Alison Hunter Improvement Advisor, Acute Adult Safety Programme Healthcare Improvement Scotland Acute Adult 2008 what we did Leadership Medicines Perioperative Critical Care Reduce Mortality & Harm General
End Of Life Decision Making - Who s Decision Is It Anyway?
 End Of Life Decision Making - Who s Decision Is It Anyway? Kara Livy RN MN NP Critical Care Nurse Practitioner Royal Alexandra Hospital Edmonton, Alberta Kara.livy@albertahealthservices.ca End-Of-Life
End Of Life Decision Making - Who s Decision Is It Anyway? Kara Livy RN MN NP Critical Care Nurse Practitioner Royal Alexandra Hospital Edmonton, Alberta Kara.livy@albertahealthservices.ca End-Of-Life
Core competencies* for undergraduate students in clinical associate, dentistry and medical teaching and learning programmes in South Africa
 Core competencies* for undergraduate students in clinical associate, dentistry and medical teaching and learning programmes in South Africa Developed by the Undergraduate Education and Training Subcommittee
Core competencies* for undergraduate students in clinical associate, dentistry and medical teaching and learning programmes in South Africa Developed by the Undergraduate Education and Training Subcommittee
Competency Asse ssment Tool for Care of Febrile Neutropenia 2009
 Competency Asse ssment Tool for Care of Febrile Neutropenia 2009 Guidelines for use: In assessing competence, a combination of assessment methods may be utilised including clinical questioning/ interview
Competency Asse ssment Tool for Care of Febrile Neutropenia 2009 Guidelines for use: In assessing competence, a combination of assessment methods may be utilised including clinical questioning/ interview
Stage 2 GP longitudinal placement learning outcomes
 Faculty of Life Sciences and Medicine Department of Primary Care & Public Health Sciences Stage 2 GP longitudinal placement learning outcomes Description This block focuses on how people and their health
Faculty of Life Sciences and Medicine Department of Primary Care & Public Health Sciences Stage 2 GP longitudinal placement learning outcomes Description This block focuses on how people and their health
 FACULTY of health sciences www.acu.edu.au/health_sciences Faculty of health sciences I like ACU because it supports and encourages students to actively participate in projects that are in line with the
FACULTY of health sciences www.acu.edu.au/health_sciences Faculty of health sciences I like ACU because it supports and encourages students to actively participate in projects that are in line with the
NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting
 NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting 1. Introduction To standardise the type and frequency of observations to be taken on adult
NHS LOTHIAN Standard Operating Procedure: EHSCP Physiological Observations of Patients in the Community Setting 1. Introduction To standardise the type and frequency of observations to be taken on adult
Community Health Services in Bristol Community Learning Disabilities Team
 Community Health Services in Bristol 2014 Community Learning Disabilities Team This provides specialist community based services for adults with learning difficulties and help to promote equal access to
Community Health Services in Bristol 2014 Community Learning Disabilities Team This provides specialist community based services for adults with learning difficulties and help to promote equal access to
Service Specification. Service to Manage COPD Exacerbations
 Service Specification Service to Manage COPD Exacerbations 1 DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development Finance Planning
Service Specification Service to Manage COPD Exacerbations 1 DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development Finance Planning
