Perioperative Fluid Utilization Variability and Association With Outcomes
|
|
|
- Andrew Cannon
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Perioperative Fluid Utilization Variability and Association With Outcomes Considerations for Enhanced Recovery Efforts in Sample US Surgical Populations Julie K. M. Thacker, MD, William K. Mountford, PhD,y Frank R. Ernst, PharmD, MS,z Michelle R. Krukas, MA,z and Michael (Monty) G. Mythen, MBBS, MD, FRCA, FFICM, FCAI (Hon) Objectives: To study current perioperative fluid administration and associated outcomes in common surgical cohorts in the United States. Background: An element of enhanced recovery care protocols, optimized perioperative fluid administration may be associated with improved outcomes; however, there is currently no consensus in the United States on fluid use or the effects on outcomes of this use. Methods: The study included all inpatients receiving colon, rectal, or primary hip or knee surgery, 18 years of age or older, who were discharged from a hospital between January 1, 2008 and June, in the Premier Research Database. Patient outcomes and intravenous fluid utilization on the day of surgery were summarized for each surgical cohort. Regression models were developed to evaluate associations of high or low day-of-surgery fluids with the likelihood of increased hospital length of stay (LOS), total costs, or postoperative ileus. Results: The study showed significant associations between high fluid volume given on the day of surgery with both increased LOS (odds ratio ) and increased total costs (odds ratio ). High fluid utilization was associated with increased presence of postoperative ileus for both rectal and colon surgery patients. Low fluid utilization was also associated with worse outcomes. Conclusions: According to results from this review of current practice in US hospitals, fluid optimization would likely lead to decreased variability and improved outcomes. Keywords: enhanced recovery, intraoperative fluid use, perioperative fluid, surgical costs, surgical outcomes (Ann Surg 2016;263: ) Despite improvements in surgical technique, anesthesia, and perioperative care, colorectal operations are plagued with morbidity and complicated postsurgical inpatient courses. In addition, orthopedic procedures are carried out more frequently each year, with significant costs. Any effort to avoid complications or unnecessary hospital days in these populations is warranted. Throughout the 1990s and early 2000s, the benefits of concerted From the Department of Surgery, Duke University School of Medicine, Durham, NC; ydepartment of Research Quintiles, Durham, NC; zdepartment of Research Premier, Inc, Charlotte, NC; and Surgical Outcomes Research Centre (SOuRCe), University College London Hospitals National Institute of Health Research Biomedical Research Centre, London, UK. Disclosure: Supported by funding from Deltex Medical (to W.M., F.E., and M.K.). The authors declare no conflicts of interest. Supplemental digital content is available for this article. Direct URL citations appear in the printed text and are provided in the HTML and PDF versions of this article on the journal s Web site ( Reprints: Julie K. M. Thacker, MD, Department of Surgery, Duke University School of Medicine, Durham, NC, USA julie.thacker@duke.edu. Copyright ß 2015 Wolters Kluwer Health, Inc. All rights reserved. ISSN: /14/ DOI: /SLA efforts to implement multimodal perioperative care methods were reported. 1 Described as Enhanced Recovery After Surgery (ERAS), fast-track surgery, perioperative goal-directed therapy, or perioperative care mapping, these efforts represent multidisciplinary preoperative, intraoperative, and postoperative care pathways. 2,3 The primary aim of this multimodal approach to perioperative care is to reduce the length of hospitalization following elective surgery by maintaining preoperative organ function and reducing postsurgical stress. The key elements of evidence-based, multimodal, perioperative care in Europe have been summarized in Consensus Guidelines established in 2009, 4 and subsequently updated in The 20 or so elements defined in these consensus statements include preoperative assessment and education, optimal perioperative fluid maintenance, standardized regimens for analgesia and anesthesia, and early mobilization. Although such a perioperative regimen has been shown to decrease length of stay (LOS) and improve outcomes, the successful implementation of these protocols requires patient engagement and multidisciplinary teamwork. 6 Acceptance and implementation of enhanced recovery principles has not been swift or widespread in the United States. The team approach to managing outcomes with multiple causative factors has been a challenge to gaining wide adoption of these principles. Elsewhere, however, the payment structure of the healthcare system has facilitated change. Implementation in England, for example, was first established as a National Health Service (NHS) project. 7 The success of the British effort is measured as a marker of acceptance; those centers with proof of adoption have shown expected improvements. 8 Postoperative elements have been electively supported at random US centers, although no nation-wide analysis or implementation effort has occurred. Evidence-based postoperative care programs have been defined in the US literature as enhanced recovery, whereas the intraoperative elements are less often reported. The anesthesia literature abounds with discussion of intraoperative fluid management regimens, but these are largely divorced from postoperative fluid management strategies or enhanced recovery efforts. When both the perioperative surgeon-driven elements and the intraoperative pain and fluid management anesthesia-driven elements are combined, the benefits of enhanced recovery are maximized. 4,5 One outcome addressed by enhanced recovery efforts in colorectal surgery (CRS) is postoperative ileus (POI). Often a driver of postoperative LOS, POI develops less frequently in CRS populations with directed perioperative fluid management protocols. 6 Postoperative ileus also occurs after orthopedic operations. Although POI is considered a medical complication to the orthopedic patient and a surgical complication to the gastrointestinal surgery patient, the effect of POI on LOS and postoperative recovery is the same. Attributing complications of an orthopedic patient or bowel surgery patient to perioperative fluid management is not definitively Annals of Surgery Volume 263, Number 3, March 2016
2 Annals of Surgery Volume 263, Number 3, March 2016 Perioperative Fluid Utilization Variability supported in the literature; however, a general understanding that algorithm-led hemodynamic management including individualized goal-directed fluid management may yield improved outcomes is reported. 3 To best extrapolate a proposed perioperative fluid management protocol, an understanding of current perioperative fluid management is necessary. With acknowledgment of the paucity of published data on the impact of intraoperative and perioperative fluid management on surgical outcomes from these common procedures in the United States, this study was designed to summarize intravenous fluid utilization, in particular on the day of surgery (DOS), and patient outcomes, including the presence of POI, hospital LOS, in-hospital mortality, total hospital costs, and hospital readmissions (30, 60, and 90 days following index discharge) among adult inpatients receiving elective colon surgery, rectal surgery, or hip or knee replacement procedures. We hypothesized that there would be substantial variation in fluid utilization on the DOS and associations between both high- and low-volume usage and increased LOS, hospital costs, and POI. METHODS Data Source The Premier Research Database 9 contains information on over 67 million inpatient hospital discharges (6 million discharges per year) one-fifth of all annual US acute care hospitalizations from the year 2000 to the present. The database contains standard hospital discharge files that include patient demographic information. Patients can be tracked across the inpatient and hospital-based outpatient settings, as well as across visits with a unique identifier. In addition to the data elements available in most standard hospital discharge files, the Premier database contains a date-stamped record of all charge master items, including procedures, medications, laboratory and diagnostic services, and therapeutic services at the individual patient level. Drug utilization information is available by day of stay and includes quantity, dosing, strength, and cost. Costs are those reported by the hospital, and represent the hospital s internal perspective; they are not the charge to a payer and are not the amount reimbursed to the hospital. Patient Population This retrospective, observational, database analysis included inpatients, 18 years of age or older, who were discharged from 524 contributing hospitals between January 1, 2008, and June 30, Patients of interest had procedure codes from the International Classification of Diseases 9th Revision, Clinical Modification (ICD-9) signifying colon, rectal, or hip or knee replacement procedures (see Supplemental Digital Content Appendix, available at To increase the likelihood that the hospital visit was directly related to the surgical procedure, patients were required to have the identifying ICD-9 procedure code(s) of interest occur on the day of hospital admission. Furthermore, patients with hospital admissions that were not listed as elective were excluded. The colon surgery population was subcategorized by open versus laparoscopic procedures, which was defined by the ICD-9 code used to identify the patient. When both open and laparoscopic ICD-9 procedure codes for the same surgical procedure were present on the day of admission, the patient was removed from the subgroup evaluations to maintain clear separation between the subgroups. Patient Outcomes The main outcomes of interest were hospital LOS, in-hospital mortality, total hospital costs, intravenous fluid utilization, presence of POI (identified by ICD-9 diagnosis codes and 997.4x), and all-cause hospital readmissions (30, 60, and 90 days following index discharge, where the patient was alive at discharge). Fluid utilization was defined using the charge master data, which were provided at the day of service level. Therefore, fluids were summarized for the total duration of the index hospital stay and stratified by time period: during the DOS or on days postsurgery (DPS). Considerable variation was defined as being below the 25th percentile (low volume quartile) or above the 75th percentile (high volume quartile). Thus, within each surgery type, patients in the middle between the 25th and 75th percentiles (reference volume) were compared to those in the lowest and highest quartiles. Statistical Analysis All analyses were stratified by surgical cohort: colon, rectal, and hip/knee replacement. Descriptive analyses were conducted to characterize the patient population by patient, clinical, and hospital attributes. Data measured on a continuous scale were expressed as mean, standard deviation, median, and interquartile range (IQR) (25th percentile [Q1] to 75th percentile [Q3]). Categorical data were expressed as counts/percentages in the categories. Student t tests were used for comparisons of continuous measures such as age, and x 2 tests were used for categorical variables. All statistical tests were two sided and significance was indicated by P-values less than Logistic regression modeling was conducted to evaluate the relationship between the volume of fluids received by patients on the DOS and key outcomes, including LOS, total hospital costs, and occurrence of POI. The volume of fluids received on the DOS was categorized into 3 levels: within the IQR (values lying between the 25th and 75th percentile); within Quartile 1 (Q1, defined as being in the lower 25th percentile of volume amounts), referred to as low; and within Quartile 4 (Q4, defined as being in the upper 25th percentile), referred to as high. The moderate IQR was designated as the referent level in all logistic models. Separate logistic regression models were developed for the following outcomes: excess LOS (top 25%), excess total hospital costs (top 25%), and presence of POI. Models were created to compute both unadjusted and adjusted results where, in the latter case, multivariable adjustment was made for patient and hospital covariates. The covariates varied by model, but generally included age, race, sex, Charlson Comorbidity Index (CCI), Medicare Severity Diagnosis Related Groups (MS-DRG), 10 and hospital teaching status, location (urban versus rural), US Census region, and number of beds. For each adjusted model, covariates eligible for inclusion in the models were selected using a stepwise selection method until all variables remaining in the model were significant at P 0.1. RESULTS Patient Characteristics The study included 3 groups: 84,722 colon, 22,178 rectal, and 548,526 primary hip or knee replacement surgical patients (Table 1). Overall, the study population had a mean age >60 years, with more females as compared to males, and a larger percentage of white race for all surgical cohorts. The most common insurance providers were Medicare (43%) and managed care (30%). The study population had geographic representation from all US regions. Furthermore, the study population included admissions from urban (89%) and rural (7%) hospitals, teaching and nonteaching (55%) hospitals, and small (<100 hospital beds), medium, and large (500þ hospital beds) hospitals. Unadjusted Outcomes Mean (SD) DOS fluid use was L (median 3.1, IQR 1.7 5) for patients undergoing colon surgery, L (median ß 2015 Wolters Kluwer Health, Inc. All rights reserved
3 Thacker et al Annals of Surgery Volume 263, Number 3, March 2016 TABLE 1. Patient and Hospital Characteristics by Surgical Cohort Surgical Cohort Colon Rectal Hip/Knee N (%) N (%) N (%) Total patients 84, , , Patient demographics Age, yr , , , , , , , , þ , Mean (SD) 62.3 (14.2) 61.4 (14.2) 65.7 (11) Median (IQR) 63 (53 73) 62 (52 72) 66 (58 74) Sex Female 45, , , Male 38, , , Race/ethnicity Black , Hispanic Other 12, , White 62, , , Primary payer Commercial , Managed care 30, , Medicaid , Medicare 39, , Other , Charlson Comorbidity Index Mean (SD) 3.8 (3) 4.1 (3) 1.9 (1.5) Median (IQR) 3 (2 5) 3 (2 8) 1 (1 2) Hospital characteristics Provider region Midwest 16, , Northeast 15, , South 36, , West 16, , Population served Rural , Urban 75, , , Teaching status y No 51, , , Yes 33, , Hospital bed size , , , , , , þ 27, , Provider region as defined by US Census: yteaching hospital or nonteaching hospital, as defined by CMS to mean, a hospital engaged in an approved graduate medical examination (GME) residency program in medicine, osteopathy, dentistry, or podiatry. IQR indicates interquartile range; SD, standard deviation. 3.3, IQR ) for rectal surgery patients, and L (median 3, IQR ) for hip/knee replacement patients (Table 2). Average (SD) DPS fluid use was L (median 6.6, IQR ) for patients receiving colon surgery, L (median 7.1, IQR ) for rectal surgery patients, and L (median 1.5, IQR 1 3) for hip/knee replacement patients. Mean LOS was 6.3 days (median 5, IQR 4 7) for patients receiving colon surgery, 7.0 days (median 6, IQR 4 8) for rectal surgery patients, and 3.3 days (median 3, IQR 3 4) for hip/knee replacement patients. Average total hospital costs were $15,069 (median $12,485, IQR $9576 $16,822) for colon surgery, $17,284 (median $14,401, IQR $10,821 $19,882) for rectal surgery, and $16,397 (median $15,287, IQR $12,632 $18,898) for hip/ knee replacement. Postoperative ileus was diagnosed in approximately 18% of both colon surgery and rectal surgery cohorts, but was found in <1% of hip/knee replacement patients. The rate of colon surgery patients with readmissions for colon surgery patients ranged from 10.2% within 30 days to 14.7% within 90 days. For rectal surgery patients, readmissions ranged from 14.5% within 30 days to 24.6% within 90 days. Hip/knee replacement patients were readmitted within 30 days 9.5% of the time and 12.8% of the time within 90 days. Death during the index hospitalization was rare (<1%) for all surgical groups ß 2015 Wolters Kluwer Health, Inc. All rights reserved.
4 Annals of Surgery Volume 263, Number 3, March 2016 Perioperative Fluid Utilization Variability TABLE 2. Patient Outcomes and Fluid Utilization by Surgical Cohort Surgical Cohort Colon Rectal Hip/Knee N (%) N (%) N (%) Total patients 84, , , Length of stay (d) Mean (SD) 6.3 (5.8) 7 (5.8) 3.3 (1.6) Median (IQR) 5 (4 7) 6 (4 8) 3 (3 4) Inhospital mortality Yes Postoperative ileus Yes 14, Inpatient hospital readmissions Readmission 30-d , d 10, , d 12, , Total length of stay (index plus readmit within 30 d) N , Mean (SD) 16.3 (13.3) 16.9 (13.2) 11.7 (6.4) Median (IQR) 13 (9 19) 14 (9 20) 10 (8 14) Total length of stay (index plus readmit within 60 d) N 10, , Mean (SD) 16.7 (13.8) 16.6 (13.1) 11.3 (7) Median (IQR) 13 (9 20) 13 (9 20) 10 (7 14) Total length of stay (index plus readmit within 90 d) N 12, , Mean (SD) 16.9 (14.5) 16.7 (13.4) 11 (7.4) Median (IQR) 13 (9 20) 13 (9 20) 9 (6 14) Hospitalization cost outcomes ($) Total cost N 83, , , Mean (SD) $15,069 ($10,036) $17,284 ($11,350) $16,397 ($5,897) Median (IQR) $12,485 ($9,576 $16,822) $14,401 ($10,821 $19,882) $15,287 ($12,632 $18,898) ICU day(s) cost N 11, , Mean (SD) $18,159 ($19,021) $18,438 ($16,979) $16,835 ($13,092) Median (IQR) $12,524 ($8,418 $19,895) $13,869 ($9,284 $20,824) $14,536 ($7,804 $21,301) Non-ICU day(s) cost N 83, , , Mean (SD) $12,760 ($6,813) $14,373 ($8,311) $16,083 ($5,736) Median (IQR) $11,478 ($8,659 $15,263) $12,937 ($9,303 $17,566) $15,148 ($12,491 $18,695) Fluid utilization outcomes (L) Total fluid use N 77, , , Mean (SD) 11.5 (14.2) 12.7 (13.8) 4.6 (14.1) Median (IQR) 9.6 (5 14.6) 10.3 (5 16.5) 4 (2 6.1) Day of surgery fluid use N 70, , , Mean (SD) 3.5 (2.4) 3.8 (2.7) 3 (2) Median (IQR) 3.1 (1.7 5) 3.3 ( ) 3 ( ) Day(s) postsurgery fluid use total N 70, , , Mean (SD) 8.4 (7.9) 9.3 (9.1) 2.2 (2.4) Median (IQR) 6.6 (3.2 11) 7.1 ( ) 1.5 (1 3) IQR indicates interquartile range; L, liters, SD, standard deviation. Compared with patients having laparoscopic colon surgery, patients with open colon procedures tended to have greater unadjusted average LOS ( vs days; P < ), greater unadjusted average total costs ($15,675 10,980 vs $13, ; P < ), and poorer patient-level outcomes, as measured by POI (19.8% vs 13.2%; P < ) and readmissions (11.6% vs 7.5% at 30 days; P < ) (Table 3). Despite statistically significant differences in all unadjusted outcomes between open and laparoscopic colon surgeries, the DOS fluid volume did not substantially vary between open and laparoscopic cases (median 3.1 L, mean 3.5 L for both groups; P ¼ ). ß 2015 Wolters Kluwer Health, Inc. All rights reserved
5 Thacker et al Annals of Surgery Volume 263, Number 3, March 2016 TABLE 3. Patient Outcomes and Fluid Utilization by Surgery Type for Colon Procedures Colon Surgeries Open Laparoscopic N (%) N (%) P Total patients 48, , Percentage of surgery type Length of stay (d) Mean (SD) 7.1 (6.6) 4.9 (3.8) < Median (IQR) 6 (4 8) 4 (3 5) Inhospital mortality Yes < Postoperative ileus Yes < Inpatient hospital readmissions Readmission 30-d < d < d < Total length of stay (index plus readmit within 30 d) N Mean (SD) 17.4 (13.8) 13.5 (10.9) < Median (IQR) 13 (9 21) 10 (7 16) Total length of stay (index plus readmit within 60 d) N Mean (SD) 17.7 (14.3) 13.9 (11.4) < Median (IQR) 13 (9 21) 10 (7 16) Total length of stay (index plus readmit within 90 d) N Mean (SD) 18 (15.2) 14 (11.6) < Median (IQR) 13 (9 21) 10 (7 17) Hospitalization cost outcomes ($) Total cost N 47, , Mean (SD) $15,675 ($10,980) $13,582 ($7890) < Median (IQR) $12,617 ($9563 $17,503) $11,900 ($9330 $15,377) ICU day(s) cost N Mean (SD) $18,398 ($19,523) $16,584 ($17,162) < Median (IQR) $12,502 ($8302 $20,315) $11,830 ($8456 $17,862) Non-ICU day(s) cost N 47, , Mean (SD) $12,729 ($7148) $12,395 ($5988) < Median (IQR) $11,294 ($8409 $15,302) $11,383 ($8809 $14,690) Fluid utilization outcomes (ml) Total fluid use N 43, , Mean (SD) 12.7 (16) 9.4 (9.8) < Median (IQR) 10.8 ( ) 8.1 ( ) Day of surgery fluid use total N 40, , Mean (SD) 3.5 (2.4) 3.5 (2.3) Median (IQR) 3.1 (1.5 5) 3.1 (2 5) Day(s) postsurgery fluid use total N 40, , Mean (SD) 9.3 (8.4) 6.6 (6.4) < Median (IQR) 7.5 (4 12.2) 5 (3 8.2) IQR indicates interquartile range; L, liters; SD, standard deviation. Among the colon surgical cohort, we found a statistically significant association between fluid volumes received after the first postoperative day (Table 2, DPS) and the volume of fluids received on the DOS (Table 2, DOS). In particular, the mean DPS fluid volume on DOS increased from 6.7 L among patients in the lowest quartile of DOS fluids to 10.0 L in DPS fluids among patients in the highest quartile of DOS fluids (Table 4; P < ). In other words, patients who tended to receive lesser DOS fluids also tended to receive lesser DPS fluids and those with higher DOS fluids also tended to receive higher DPS fluids ß 2015 Wolters Kluwer Health, Inc. All rights reserved.
6 Annals of Surgery Volume 263, Number 3, March 2016 Perioperative Fluid Utilization Variability TABLE 4. Postsurgical Fluid Utilization by Day-of-surgery Quartile for Colon Surgery Cohort DOS Fluid Quartile Mean DPS Fluids (L) Q Q Q Q Linear trend test P < Modeled Outcomes The multivariable (adjusted) odds ratios (ORs) and corresponding 95% confidence intervals (CIs) describing the relationship between DOS fluids with LOS, total hospital costs, and POI are displayed in Figure 1. ORs from the univariable models were consistently similar to those in the multivariable models and, therefore, are not presented (available upon request). In colon surgery patients, both low and high fluid volumes were often associated with worse outcomes. Low fluid volume (Q1) was associated with 9% greater odds (OR 1.09, 95% CI ) of prolonged LOS than moderate fluids (Q2 Q3), when controlling for patient and hospital covariates, whereas high fluid volume (Q4) was associated with 25% greater odds (OR 1.25, 95% CI ) of longer LOS. Low fluid volume (Q1) was also associated with 17% greater odds (OR 1.17, 95% CI ) of higher hospitalization costs, and high fluid volume (Q4) was associated with 30% greater odds (OR 1.30, 95% CI ) of higher costs. In addition, low fluid volume (Q1) was associated with 12% greater odds (OR 1.12, 95% CI ) of having POI, whereas high fluid volume (Q4) was associated with 10% greater odds (OR 1.10, 95% CI ) of POI. In rectal surgery patients, both low and high fluid volumes were often associated with worse outcomes. Specifically, low fluid volume (Q1) was associated with 7% greater odds (OR 1.07, 95% CI ) of prolonged LOS than moderate fluids (Q2 Q3), which was not statistically significant when controlling for patient and hospital covariates. By contrast, high fluid volume (Q4) was associated with 41% greater odds (OR 1.41, 95% CI ) of longer LOS. Low fluid volume (Q1) was also associated with 3% greater odds (OR 1.03, 95% CI ) of higher hospitalization costs, which was not statistically significant. However, high fluid volume (Q4) was associated with 53% greater odds (OR 1.53, 95% CI ) of higher costs, which was significant. In addition, low fluid volume (Q1) was associated with 16% greater odds (OR 1.16, 95% CI ) of having POI, whereas high fluid volume (Q4) was associated with 26% greater odds (OR 1.26, 95% CI ) of POI. In hip/knee surgery patients as well, both low and high fluid volumes were often associated with worse outcomes. In particular, low fluid volume (Q1) was associated with 14% greater odds (OR 1.14, 95% CI ) of prolonged LOS than moderate fluids (Q2 Q3), when controlling for patient and hospital covariates. High fluid volume (Q4) was associated with 3% greater odds (OR 1.03, 95% CI ) of longer LOS. Low fluid volume (Q1) was also associated with 12% greater odds (OR 1.12, 95% CI ) of higher hospitalization costs, and high fluid volume (Q4) was associated with 26% greater odds (OR 1.26, 95% CI ) of higher costs. Low fluid volume (Q1) was associated with 10% greater odds (OR 1.10, 95% CI ) of having POI, whereas high fluid volume (Q4) was associated with 4% greater odds (OR 1.04, 95% CI ) of POI, but both were insignificant differences. Open Versus Laparoscopic Colon Surgery Additional models were developed to evaluate the relationship between DOS fluids and outcomes by open versus laparoscopic surgeries. No statistically significant differences in LOS, costs, or risk of POI were detected between open and laparoscopic surgical approaches, as shown by the overlapping 95% CIs at the bottom of Figure 1. In particular, low fluid volume (Q1) was associated with 10% greater (OR , 95% CI ) odds of prolonged LOS among the open colon surgery patients compared to 9% greater odds (OR 1.09, 95% CI ) among the laparoscopic colon surgery patients. For high fluid-volume colon surgery patients, increased LOS was 26% more likely (OR 1.26, 95% CI ) for open surgery, versus 23% more likely (OR 1.23, 95% CI ) for laparoscopic surgery. Low fluid volume (Q1) in open colon surgery cases was associated with 16% greater odds (OR 1.16, 95% CI ) of higher costs, compared to 23% greater odds (OR 1.23, 95% CI ) among the laparoscopic colon surgery patients. High fluid volume (Q4) in open colon surgery cases was associated with 35% greater odds (OR 1.35, 95% CI ) of higher costs, compared to 19% greater odds (OR 1.19, 95% CI ) among the laparoscopic colon surgery patients. Then, finally, low fluid volume (Q1) in open colon surgery cases was associated with 14% greater odds (OR , 95% CI ) of POI, compared to 12% greater odds (OR 1.12, 95% CI ) among the laparoscopic colon surgery patients. High fluid volume (Q4) in open colon surgery cases was associated with 13% greater odds (OR , 95% CI ) of POI, compared to 8% greater odds (OR 1.08, 95% CI ) among the laparoscopic colon surgery patients. DISCUSSION The fluid utilization and associated outcomes of 3 common US surgical patient populations were evaluated by retrospective analysis of the Premier database. From this approach, we studied fluid given on DOS in a demographically diverse patient cohort, well represented in our large patient population from a range of hospital types. The first aim of this study was to characterize the current DOS intravenous fluid use during colon, rectal, and hip/knee operations. A wide range of fluid given on DOS is observed, as shown in Table 2. For example, 25% of patients received less than the following DOS amounts: 1.7 L for colon, 1.5 L for rectal, and 1.3 L for hip/knee surgeries. Another 25% of patients received more than 5.0 L for colon, 5.4 L for rectal, and 4.1 L for hip/knee surgeries on the DOS. Furthermore, 25% of patients received less than the following DPS amounts: 3.2 L for colon, 3.1 L for rectal, and 1.0 L for hip/knee surgeries. Moreover, 25% of patients received more than 11.0 L for colon, 12.3 L for rectal, and 3.0 L for hip/knee surgery patients in the days following surgery. The significant variability of DOS fluid administration corresponds to our background impression that protocoled/goal-directed fluid management and enhanced recovery pathways are not routinely followed in the United States. The second aim was to define associations between DOS fluid use and outcomes. In every group, we identified an association between receiving the greatest amount of fluid and worse outcomes. High (Q4) DOS fluid patients had increased likelihood of longer LOS, increased POI, and increased cost compared to patients with DOS fluids in the second and third quartiles. Although the overall LOS and POI incidence are consistent with those reported in the literature, 11 we have shown an association with the amount of fluid given on the DOS. In all instances, adjusted and unadjusted, worse outcomes are seen in the extremes of fluid administration. By defining quartiles 2 and 3 as presumptively optimal with improved ß 2015 Wolters Kluwer Health, Inc. All rights reserved
7 Thacker et al Annals of Surgery Volume 263, Number 3, March 2016 FIGURE 1. Odds of increased/decreased (% and 95% confidence intervals) outcomes (length of stay, cost, or ileus) comparing reference group of patients (quartiles 2 and 3) to those who received lower (Q1) and higher (Q4) volumes of fluid on the day of surgery ß 2015 Wolters Kluwer Health, Inc. All rights reserved.
8 Annals of Surgery Volume 263, Number 3, March 2016 Perioperative Fluid Utilization Variability FIGURE 1. (Continued). outcomes over the extremes, we conclude that variation in intraoperative fluid delivery impacts surgical outcomes. It is important to note the independence of the impact of fluids given and MS-DRG and CCI. The association of improved outcomes with our defined optimal range of fluid given is maintained while controlling for every level of patient severity of illness and baseline comorbidity status. Regardless of procedure category or comorbidity index, patients receiving fluids in the second and third quartile ranges had better outcomes and lower costs. Our results suggest that an applicable, protocoled approach toward optimal fluid management may improve outcomes. In the orthopedic cohort, the variability of fluid use was less than in the colorectal cohorts. Despite this, and the categorization by the Charlson index and MS-DRG, the orthopedic cohort experienced the best outcomes in our defined optimal fluid categories. The association of improved surgical outcomes with amount of intraoperative fluid is independent of MS-DRG. In other words, even in the defined healthier populations, intraoperative optimized fluid strategies may positively impact outcomes. Similarly, we note a difference in outcomes between the laparoscopic and open colorectal groups. Consistent with the previous literature, surgical outcomes are improved with laparoscopic approaches to surgery. Again, we report the association between fluid administration and improved outcomes is seen in each group, with multivariable analysis. Within the laparoscopic group and within the open group, patients with high or low DOS fluids tended to have poorer outcomes, regardless of surgical approach. Adoption and application of patient-centered care pathways and protocols can reduce variability and improve outcomes. Recent meta-analyses emphasized that goal-directed fluid protocols are associated with reduced variability in fluid management and better outcomes. 3,12 Goal-directed fluid therapy (GDFT) utilizes a cardiac output monitor to individualize fluid therapy and aims to restrict volume therapy to the minimum required to maintain central euvolemia. Background crystalloid infusion rates ( maintenance fluid ) may also be dramatically reduced. The relative contributions of fluid restriction and the use of vasoactive drugs to increase oxygen delivery remain uncertain, but flow-guided algorithms for fluid management are associated with improved outcomes with little or any evidence of harm. 13 Although some degree of uncertainty exists about the need for GDFT when considering low-risk patients undergoing laparoscopic procedures in enhanced recovery care programs, our observations support the importance of avoiding either excessive fluid restriction or overload in all our patients. 6,13 The primary strengths of our study are the size of our patient sample and the availability of data allowing multivariable analysis. With the diversity of hospital size, patient characteristics, and patient comorbidities represented in our sample, we combat the biases of individual or hospital patient case complexity and outlier provider variables. We did not account for biases introduced by nonrandomization of treatment, such as with propensity score methods. Instead, we observed variability in real-world use of fluids in our study and applied multivariable regression techniques to account for confounding factors. Because the granularity of the Premier database permits no finer analyses of timing than a calendar day, our study was not able to distinguish the fluids used during surgery (intraoperative time) versus perioperatively (preoperative, intraoperative, and postoperative time). However, we were able to separate the day of a surgical procedure from days following surgery. The hospital cost data in our analysis were captured from financial information gathered by the hospitals during the course of treatment. The limitations of this approach are the possible underreporting of clinical outcomes of interest, and the reliance on ICD-9 coding to identify clinically related information such as procedures and diagnosed comorbid conditions. For example, a diagnosis of POI may be underreported due to the lack of consistent documentation in patient medical records, whereas a readmission is increasingly unlikely to be missed. However, this limitation should have minimal impact on our conclusion given that over- or under-reporting would likely be consistent within institutions and, therefore, consistent in effect. In conclusion, we analyzed differences in outcomes as they may relate to the volume of fluid given on the DOS. Based on the poorer outcomes observed in patients receiving both restricted and liberal amounts of fluid, we advocate continued examination of the effect of patient-centered care pathways that incorporate protocolized optimal intraoperative intravenous fluid management to enhance surgical recovery. REFERENCES 1. Kehlet H. Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth. 1997;78: Grocott MP, Dushianthan A, Hamilton MA, et al. Perioperative increase in global blood flow to explicit defined goals and outcomes following surgery. Cochrane Database Syst Rev. 2012;11:CD Spanjersberg WR, Reurings J, Keus F, et al. Fast track surgery versus conventional recovery strategies for colorectal surgery. Cochrane Database Syst Rev. 2011;2:CD Lassen K, Soop M, Nygren J, et al. Consensus review of optimal perioperative care in colorectal surgery: Enhanced Recovery After Surgery (ERAS) Group recommendations. Arch Surg. 2009;144: Gustafsson UO, Scott MJ, Schwenk W, et al. Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS(R)) Society recommendations. Clin Nutr. 2012;31: ß 2015 Wolters Kluwer Health, Inc. All rights reserved
9 Thacker et al Annals of Surgery Volume 263, Number 3, March Miller TE, Thacker JK, White WD, et al. Reduced length of hospital stay in colorectal surgery after implementation of an enhanced recovery protocol. Anesth Analg. 2014;118: Mythen MG. Spread and adoption of enhanced recovery from elective surgery in the English National Health Service. Can J Anaesth. 2015;62: Knott A, Pathak S, McGrath JS, et al. Consensus views on implementation and measurement of enhanced recovery after surgery in England: Delphi study. BMJ open. 2012;2:e Premier database. Premier Inc. (Charlotte, NC). Available at: mierinc.com/transforming-healthcare/healthcare-performance-improvement/ premier-research-services/. Accessed 5 February, Medicare Program; Changes to the Hospital Inpatient Prospective Payment Systems and Fiscal Year 2008 Rates; Final Rule. Available at: PPS/IPPS-Regulations-and-Notices-Items/CMS html. 11. Chapuis PH, Bokey L, Keshava A, et al. Risk factors for prolonged ileus after resection of colorectal cancer: an observational study of 2400 consecutive patients. Ann Surg. 2013;257: Pearse RM, Harrison DA, MacDonald N, et al. Effect of a perioperative, cardiac output-guided hemodynamic therapy algorithm on outcomes following major gastrointestinal surgery: a randomized clinical trial and systematic review. JAMA. 2014;311: Bennett-Guerrero E. Hemodynamic goal-directed therapy in high-risk surgical patients. JAMA. 2014;311: ß 2015 Wolters Kluwer Health, Inc. All rights reserved.
Understanding Readmissions after Cancer Surgery in Vulnerable Hospitals
 Understanding Readmissions after Cancer Surgery in Vulnerable Hospitals Waddah B. Al-Refaie, MD, FACS John S. Dillon and Chief of Surgical Oncology MedStar Georgetown University Hospital Lombardi Comprehensive
Understanding Readmissions after Cancer Surgery in Vulnerable Hospitals Waddah B. Al-Refaie, MD, FACS John S. Dillon and Chief of Surgical Oncology MedStar Georgetown University Hospital Lombardi Comprehensive
9/29/2017. Enhanced Recovery After Surgery at the University of Virginia Medical Center. Disclosures. Objectives. None
 Enhanced Recovery After Surgery at the University of Virginia Medical Center Bethany Sarosiek, RN, MSN, MPH, CNL University of Virginia Health System Charlottesville, VA ErasRN@virginia.edu Disclosures
Enhanced Recovery After Surgery at the University of Virginia Medical Center Bethany Sarosiek, RN, MSN, MPH, CNL University of Virginia Health System Charlottesville, VA ErasRN@virginia.edu Disclosures
Minority Serving Hospitals and Cancer Surgery Readmissions: A Reason for Concern
 Minority Serving Hospitals and Cancer Surgery : A Reason for Concern Young Hong, Chaoyi Zheng, Russell C. Langan, Elizabeth Hechenbleikner, Erin C. Hall, Nawar M. Shara, Lynt B. Johnson, Waddah B. Al-Refaie
Minority Serving Hospitals and Cancer Surgery : A Reason for Concern Young Hong, Chaoyi Zheng, Russell C. Langan, Elizabeth Hechenbleikner, Erin C. Hall, Nawar M. Shara, Lynt B. Johnson, Waddah B. Al-Refaie
Total Joint Partnership Program Identifies Areas to Improve Care and Decrease Costs Joseph Tomaro, PhD
 WHITE PAPER Accelero Health Partners, 2013 Total Joint Partnership Program Identifies Areas to Improve Care and Decrease Costs Joseph Tomaro, PhD ABSTRACT The volume of total hip and knee replacements
WHITE PAPER Accelero Health Partners, 2013 Total Joint Partnership Program Identifies Areas to Improve Care and Decrease Costs Joseph Tomaro, PhD ABSTRACT The volume of total hip and knee replacements
Cost Effectiveness of Physician Anesthesia J.P. Abenstein, M.S.E.E., M.D. Mayo Clinic Rochester, MN
 Mayo Clinic Rochester, MN Introduction The question of whether anesthesiologists are cost-effective providers of anesthesia services remains an open question in the minds of some of our medical colleagues,
Mayo Clinic Rochester, MN Introduction The question of whether anesthesiologists are cost-effective providers of anesthesia services remains an open question in the minds of some of our medical colleagues,
Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients?
 Research Article Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients? R Mallick *, Z Magama, C Neophytou, R Oliver, F Odejinmi Barts Health NHS Trust, Whipps Cross
Research Article Nurse Led Follow Up: Is It The Best Way Forward for Post- Operative Endometriosis Patients? R Mallick *, Z Magama, C Neophytou, R Oliver, F Odejinmi Barts Health NHS Trust, Whipps Cross
Supplementary Online Content
 Supplementary Online Content Kaukonen KM, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000-2012.
Supplementary Online Content Kaukonen KM, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000-2012.
Long-Stay Alternate Level of Care in Ontario Mental Health Beds
 Health System Reconfiguration Long-Stay Alternate Level of Care in Ontario Mental Health Beds PREPARED BY: Jerrica Little, BA John P. Hirdes, PhD FCAHS School of Public Health and Health Systems University
Health System Reconfiguration Long-Stay Alternate Level of Care in Ontario Mental Health Beds PREPARED BY: Jerrica Little, BA John P. Hirdes, PhD FCAHS School of Public Health and Health Systems University
Surgical Care for the Underserved: US We have our own problems
 Surgical Care for the Underserved: US We have our own problems Gregg Marshall Grand Rounds February 27, 2012 Outline Introduction US Statistics Underserved populations in the US Global Health Lack of infrastructure
Surgical Care for the Underserved: US We have our own problems Gregg Marshall Grand Rounds February 27, 2012 Outline Introduction US Statistics Underserved populations in the US Global Health Lack of infrastructure
Frequently Asked Questions (FAQ) Updated September 2007
 Frequently Asked Questions (FAQ) Updated September 2007 This document answers the most frequently asked questions posed by participating organizations since the first HSMR reports were sent. The questions
Frequently Asked Questions (FAQ) Updated September 2007 This document answers the most frequently asked questions posed by participating organizations since the first HSMR reports were sent. The questions
Community Performance Report
 : Wenatchee Current Year: Q1 217 through Q4 217 Qualis Health Communities for Safer Transitions of Care Performance Report : Wenatchee Includes Data Through: Q4 217 Report Created: May 3, 218 Purpose of
: Wenatchee Current Year: Q1 217 through Q4 217 Qualis Health Communities for Safer Transitions of Care Performance Report : Wenatchee Includes Data Through: Q4 217 Report Created: May 3, 218 Purpose of
How to Win Under Bundled Payments
 How to Win Under Bundled Payments Donald E. Fry, M.D., F.A.C.S. Executive Vice-President, Clinical Outcomes MPA Healthcare Solutions Chicago, Illinois Adjunct Professor of Surgery Northwestern University
How to Win Under Bundled Payments Donald E. Fry, M.D., F.A.C.S. Executive Vice-President, Clinical Outcomes MPA Healthcare Solutions Chicago, Illinois Adjunct Professor of Surgery Northwestern University
Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study
 Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study PI/senior researcher: Richard Falcone Jr. MD, MPH Co-primary investigator: Stephanie Polites MD, MPH; Juan Gurria MD My
Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study PI/senior researcher: Richard Falcone Jr. MD, MPH Co-primary investigator: Stephanie Polites MD, MPH; Juan Gurria MD My
Evidence for Accreditation in Bariatric Surgery Hospitals
 Evidence for Accreditation in Bariatric Surgery Hospitals John Morton, MD, MPH, FASMBS, FACS Chief, Bariatric and Minimally Invasive Surgery Stanford School of Medicine President,American Society for Metabolic
Evidence for Accreditation in Bariatric Surgery Hospitals John Morton, MD, MPH, FASMBS, FACS Chief, Bariatric and Minimally Invasive Surgery Stanford School of Medicine President,American Society for Metabolic
Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service
 Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Enhanced Recovery in NSQIP (ERIN): an update on the collaborative. Julie Thacker, LianeFeldman, and Julia Berian ACS NSQIP National Conference 2015
 Enhanced Recovery in NSQIP (ERIN): an update on the collaborative Julie Thacker, LianeFeldman, and Julia Berian ACS NSQIP National Conference 2015 No disclosures ERIN, ERAS, and ERP ERIN-Enhanced Recovery
Enhanced Recovery in NSQIP (ERIN): an update on the collaborative Julie Thacker, LianeFeldman, and Julia Berian ACS NSQIP National Conference 2015 No disclosures ERIN, ERAS, and ERP ERIN-Enhanced Recovery
Advisor Live Enhanced surgical recovery with perioperative goal-direcred therapy. October 16, #AdvisorLive
 Advisor Live Enhanced surgical recovery with perioperative goal-direcred therapy October 16, 2015 @PremierHA #AdvisorLive Download today s slides at www.premierinc.com/events Logistics Audio Use your computer
Advisor Live Enhanced surgical recovery with perioperative goal-direcred therapy October 16, 2015 @PremierHA #AdvisorLive Download today s slides at www.premierinc.com/events Logistics Audio Use your computer
Perioperative Surgical Home
 None Disclosures Debnath Chatterjee, M.D. Associate Professor of Anesthesiology CRASH 2015 - Vail, Colorado 2 Learning Objectives What is the PSH model? Describe the concept of the Perioperative Surgical
None Disclosures Debnath Chatterjee, M.D. Associate Professor of Anesthesiology CRASH 2015 - Vail, Colorado 2 Learning Objectives What is the PSH model? Describe the concept of the Perioperative Surgical
The number of patients admitted to acute care hospitals
 Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
Over the past decade, the number of quality measurement programs has grown
 Performance improvement Surgeon sees standardization and data as keys to higher value healthcare Over the past decade, the number of quality measurement programs has grown exponentially as hospitals respond
Performance improvement Surgeon sees standardization and data as keys to higher value healthcare Over the past decade, the number of quality measurement programs has grown exponentially as hospitals respond
Improving Hospital Performance Through Clinical Integration
 white paper Improving Hospital Performance Through Clinical Integration Rohit Uppal, MD President of Acute Hospital Medicine, TeamHealth In the typical hospital, most clinical service lines operate as
white paper Improving Hospital Performance Through Clinical Integration Rohit Uppal, MD President of Acute Hospital Medicine, TeamHealth In the typical hospital, most clinical service lines operate as
Malnutrition is a serious problem among hospitalized patients. A growing
 Credible Evidence in Nutrition Health Economics Outcomes Research: The Effects of Oral Nutritional Tomas J. Philipson, PhD (with Julia Thornton Snider, PhD, Darius N. Lakdawalla, PhD, Benoit Stryckman,
Credible Evidence in Nutrition Health Economics Outcomes Research: The Effects of Oral Nutritional Tomas J. Philipson, PhD (with Julia Thornton Snider, PhD, Darius N. Lakdawalla, PhD, Benoit Stryckman,
The Pain or the Gain?
 The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
Impact of Financial and Operational Interventions Funded by the Flex Program
 Impact of Financial and Operational Interventions Funded by the Flex Program KEY FINDINGS Flex Monitoring Team Policy Brief #41 Rebecca Garr Whitaker, MSPH; George H. Pink, PhD; G. Mark Holmes, PhD University
Impact of Financial and Operational Interventions Funded by the Flex Program KEY FINDINGS Flex Monitoring Team Policy Brief #41 Rebecca Garr Whitaker, MSPH; George H. Pink, PhD; G. Mark Holmes, PhD University
3M Health Information Systems. 3M Clinical Risk Groups: Measuring risk, managing care
 3M Health Information Systems 3M Clinical Risk Groups: Measuring risk, managing care 3M Clinical Risk Groups: Measuring risk, managing care Overview The 3M Clinical Risk Groups (CRGs) are a population
3M Health Information Systems 3M Clinical Risk Groups: Measuring risk, managing care 3M Clinical Risk Groups: Measuring risk, managing care Overview The 3M Clinical Risk Groups (CRGs) are a population
Enhanced Recovery: Measurement for Improvement Monthly Data Submission Guidance. Version 1.0
 Enhanced Recovery: Measurement for Improvement Monthly Data Submission Guidance Version 1.0 Document Control Version Version 1.0 Date Issued January 2014 Document To provide guidance for the monthly collection
Enhanced Recovery: Measurement for Improvement Monthly Data Submission Guidance Version 1.0 Document Control Version Version 1.0 Date Issued January 2014 Document To provide guidance for the monthly collection
Variation in length of stay within and between hospitals
 ORIGINAL ARTICLE Variation in length of stay within and between hospitals Thom Walsh 1, 2, Tracy Onega 2, 3, 4, Todd Mackenzie 2, 3 1. The Dartmouth Center for Health Care Delivery Science, Lebanon. 2.
ORIGINAL ARTICLE Variation in length of stay within and between hospitals Thom Walsh 1, 2, Tracy Onega 2, 3, 4, Todd Mackenzie 2, 3 1. The Dartmouth Center for Health Care Delivery Science, Lebanon. 2.
Enhanced recovery after surgery: the role of the PACU & Pre-op
 Enhanced recovery after surgery: the role of the PACU & Pre-op Magnus K. Teig BSc (Hons.) MBChB MRCP FRCA EDIC FFICM Assistant Professor Anesthesia & Neurosurgery Director UH PACU University of Michigan
Enhanced recovery after surgery: the role of the PACU & Pre-op Magnus K. Teig BSc (Hons.) MBChB MRCP FRCA EDIC FFICM Assistant Professor Anesthesia & Neurosurgery Director UH PACU University of Michigan
With healthcare spending continuing to increase while
 Predictive Factors of Discharge Navigation Lag Time CHARLES WALKER, MD; SAYEH BOZORGHADAD, BS; LEAH SCHOLTIS, PA-C; CHUNG-YIN SHERMAN, CRNP; JAMES DOVE, BA; MARIE HUNSINGER, RN, BSHS; JEFFREY WILD, MD;
Predictive Factors of Discharge Navigation Lag Time CHARLES WALKER, MD; SAYEH BOZORGHADAD, BS; LEAH SCHOLTIS, PA-C; CHUNG-YIN SHERMAN, CRNP; JAMES DOVE, BA; MARIE HUNSINGER, RN, BSHS; JEFFREY WILD, MD;
Medicare P4P -- Medicare Quality Reporting, Incentive and Penalty Programs
 Medicare P4P -- Medicare Quality Reporting, Incentive and Penalty Programs Presenter: Daniel J. Hettich King & Spalding; Washington, DC dhettich@kslaw.com 1 I. Introduction Evolution of Medicare as a Purchaser
Medicare P4P -- Medicare Quality Reporting, Incentive and Penalty Programs Presenter: Daniel J. Hettich King & Spalding; Washington, DC dhettich@kslaw.com 1 I. Introduction Evolution of Medicare as a Purchaser
Prepared for North Gunther Hospital Medicare ID August 06, 2012
 Prepared for North Gunther Hospital Medicare ID 000001 August 06, 2012 TABLE OF CONTENTS Introduction: Benchmarking Your Hospital 3 Section 1: Hospital Operating Costs 5 Section 2: Margins 10 Section 3:
Prepared for North Gunther Hospital Medicare ID 000001 August 06, 2012 TABLE OF CONTENTS Introduction: Benchmarking Your Hospital 3 Section 1: Hospital Operating Costs 5 Section 2: Margins 10 Section 3:
ICU Research Using Administrative Databases: What It s Good For, How to Use It
 ICU Research Using Administrative Databases: What It s Good For, How to Use It Allan Garland, MD, MA Associate Professor of Medicine and Community Health Sciences University of Manitoba None Disclosures
ICU Research Using Administrative Databases: What It s Good For, How to Use It Allan Garland, MD, MA Associate Professor of Medicine and Community Health Sciences University of Manitoba None Disclosures
Admissions and Readmissions Related to Adverse Events, NMCPHC-EDC-TR
 Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
The Role of Analytics in the Development of a Successful Readmissions Program
 The Role of Analytics in the Development of a Successful Readmissions Program Pierre Yong, MD, MPH Director, Quality Measurement & Value-Based Incentives Group Centers for Medicare & Medicaid Services
The Role of Analytics in the Development of a Successful Readmissions Program Pierre Yong, MD, MPH Director, Quality Measurement & Value-Based Incentives Group Centers for Medicare & Medicaid Services
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU. Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia
 CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
June 25, Shamis Mohamoud, David Idala, Parker James, Laura Humber. AcademyHealth Annual Research Meeting
 Evaluation of the Maryland Health Home Program for Medicaid Enrollees with Severe Mental Illnesses or Opioid Substance Use Disorder and Risk of Additional Chronic Conditions June 25, 2018 Shamis Mohamoud,
Evaluation of the Maryland Health Home Program for Medicaid Enrollees with Severe Mental Illnesses or Opioid Substance Use Disorder and Risk of Additional Chronic Conditions June 25, 2018 Shamis Mohamoud,
Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN
 Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN Cheryl B. Jones, PhD, RN, FAAN; Mark Toles, PhD, RN; George J. Knafl, PhD; Anna S. Beeber, PhD, RN Research Brief,
Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN Cheryl B. Jones, PhD, RN, FAAN; Mark Toles, PhD, RN; George J. Knafl, PhD; Anna S. Beeber, PhD, RN Research Brief,
OFF-HOURS ADMISSION AND MORTALITY IN THE PEDIATRIC INTENSIVE CARE UNIT MICHAEL CONOR MCCRORY, M.D. A Thesis Submitted to the Graduate Faculty of
 OFF-HOURS ADMISSION AND MORTALITY IN THE PEDIATRIC INTENSIVE CARE UNIT BY MICHAEL CONOR MCCRORY, M.D. A Thesis Submitted to the Graduate Faculty of WAKE FOREST UNIVERSITY GRADUATE SCHOOL OF ARTS AND SCIENCES
OFF-HOURS ADMISSION AND MORTALITY IN THE PEDIATRIC INTENSIVE CARE UNIT BY MICHAEL CONOR MCCRORY, M.D. A Thesis Submitted to the Graduate Faculty of WAKE FOREST UNIVERSITY GRADUATE SCHOOL OF ARTS AND SCIENCES
Research Design: Other Examples. Lynda Burton, ScD Johns Hopkins University
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Scottish Hospital Standardised Mortality Ratio (HSMR)
 ` 2016 Scottish Hospital Standardised Mortality Ratio (HSMR) Methodology & Specification Document Page 1 of 14 Document Control Version 0.1 Date Issued July 2016 Author(s) Quality Indicators Team Comments
` 2016 Scottish Hospital Standardised Mortality Ratio (HSMR) Methodology & Specification Document Page 1 of 14 Document Control Version 0.1 Date Issued July 2016 Author(s) Quality Indicators Team Comments
Outpatient Hospital Facilities
 Outpatient Hospital Facilities Chapter 6 Chapter Outline Introduce students to 1. Different outpatient facilities 2. Different departments involved in the reimbursement process 3. The Chargemaster 4. Terminology
Outpatient Hospital Facilities Chapter 6 Chapter Outline Introduce students to 1. Different outpatient facilities 2. Different departments involved in the reimbursement process 3. The Chargemaster 4. Terminology
Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System
 Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System Designed Specifically for International Quality and Performance Use A white paper by: Marc Berlinguet, MD, MPH
Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System Designed Specifically for International Quality and Performance Use A white paper by: Marc Berlinguet, MD, MPH
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings
 Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings Executive Summary The Alliance for Home Health Quality and
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings Executive Summary The Alliance for Home Health Quality and
ORIGINAL ARTICLE. Evaluating Popular Media and Internet-Based Hospital Quality Ratings for Cancer Surgery
 ORIGINAL ARTICLE Evaluating Popular Media and Internet-Based Hospital Quality Ratings for Cancer Surgery Nicholas H. Osborne, MD; Amir A. Ghaferi, MD; Lauren H. Nicholas, PhD; Justin B. Dimick; MD MPH
ORIGINAL ARTICLE Evaluating Popular Media and Internet-Based Hospital Quality Ratings for Cancer Surgery Nicholas H. Osborne, MD; Amir A. Ghaferi, MD; Lauren H. Nicholas, PhD; Justin B. Dimick; MD MPH
Improving patient satisfaction by adding a physician in triage
 ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
ORIGINAL ARTICLE. Inpatient Hospital Admission and Death After Outpatient Surgery in Elderly Patients
 ORIGINAL ARTICLE Inpatient Hospital Admission and Death After Outpatient Surgery in Elderly Patients Importance of Patient and System Characteristics and Location of Care Lee A. Fleisher, MD; L. Reuven
ORIGINAL ARTICLE Inpatient Hospital Admission and Death After Outpatient Surgery in Elderly Patients Importance of Patient and System Characteristics and Location of Care Lee A. Fleisher, MD; L. Reuven
Factors that Impact Readmission for Medicare and Medicaid HMO Inpatients
 The College at Brockport: State University of New York Digital Commons @Brockport Senior Honors Theses Master's Theses and Honors Projects 5-2014 Factors that Impact Readmission for Medicare and Medicaid
The College at Brockport: State University of New York Digital Commons @Brockport Senior Honors Theses Master's Theses and Honors Projects 5-2014 Factors that Impact Readmission for Medicare and Medicaid
The Determinants of Patient Satisfaction in the United States
 The Determinants of Patient Satisfaction in the United States Nikhil Porecha The College of New Jersey 5 April 2016 Dr. Donka Mirtcheva Abstract Hospitals and other healthcare facilities face a problem
The Determinants of Patient Satisfaction in the United States Nikhil Porecha The College of New Jersey 5 April 2016 Dr. Donka Mirtcheva Abstract Hospitals and other healthcare facilities face a problem
PG snapshot Nursing Special Report. The Role of Workplace Safety and Surveillance Capacity in Driving Nurse and Patient Outcomes
 PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
Cause of death in intensive care patients within 2 years of discharge from hospital
 Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland
 Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Objectives 2/23/2011. Crossing Paths Intersection of Risk Adjustment and Coding
 Crossing Paths Intersection of Risk Adjustment and Coding 1 Objectives Define an outcome Define risk adjustment Describe risk adjustment measurement Discuss interactive scenarios 2 What is an Outcome?
Crossing Paths Intersection of Risk Adjustment and Coding 1 Objectives Define an outcome Define risk adjustment Describe risk adjustment measurement Discuss interactive scenarios 2 What is an Outcome?
Pricing and funding for safety and quality: the Australian approach
 Pricing and funding for safety and quality: the Australian approach Sarah Neville, Ph.D. Executive Director, Data Analytics Sean Heng Senior Technical Advisor, AR-DRG Development Independent Hospital Pricing
Pricing and funding for safety and quality: the Australian approach Sarah Neville, Ph.D. Executive Director, Data Analytics Sean Heng Senior Technical Advisor, AR-DRG Development Independent Hospital Pricing
Final Report No. 101 April Trends in Skilled Nursing Facility and Swing Bed Use in Rural Areas Following the Medicare Modernization Act of 2003
 Final Report No. 101 April 2011 Trends in Skilled Nursing Facility and Swing Bed Use in Rural Areas Following the Medicare Modernization Act of 2003 The North Carolina Rural Health Research & Policy Analysis
Final Report No. 101 April 2011 Trends in Skilled Nursing Facility and Swing Bed Use in Rural Areas Following the Medicare Modernization Act of 2003 The North Carolina Rural Health Research & Policy Analysis
POST-ACUTE CARE Savings for Medicare Advantage Plans
 POST-ACUTE CARE Savings for Medicare Advantage Plans TABLE OF CONTENTS Homing In: The Roles of Care Management and Network Management...3 Care Management Opportunities...3 Identify the Most Efficient Care
POST-ACUTE CARE Savings for Medicare Advantage Plans TABLE OF CONTENTS Homing In: The Roles of Care Management and Network Management...3 Care Management Opportunities...3 Identify the Most Efficient Care
Increased mortality associated with week-end hospital admission: a case for expanded seven-day services?
 Increased mortality associated with week-end hospital admission: a case for expanded seven-day services? Nick Freemantle, 1,2 Daniel Ray, 2,3,4 David Mcnulty, 2,3 David Rosser, 5 Simon Bennett 6, Bruce
Increased mortality associated with week-end hospital admission: a case for expanded seven-day services? Nick Freemantle, 1,2 Daniel Ray, 2,3,4 David Mcnulty, 2,3 David Rosser, 5 Simon Bennett 6, Bruce
Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA
 JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
BUILDING THE PATIENT-CENTERED HOSPITAL HOME
 WHITE PAPER BUILDING THE PATIENT-CENTERED HOSPITAL HOME A New Model for Improving Hospital Care Authors Sonya Pease, MD Chief Medical Officer TeamHealth Anesthesia Kurt Ehlert, MD National Director, Orthopaedics
WHITE PAPER BUILDING THE PATIENT-CENTERED HOSPITAL HOME A New Model for Improving Hospital Care Authors Sonya Pease, MD Chief Medical Officer TeamHealth Anesthesia Kurt Ehlert, MD National Director, Orthopaedics
Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR)
 Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR) The table below summarizes the specific provisions noted in the Medicare
Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR) The table below summarizes the specific provisions noted in the Medicare
Supplementary Online Content
 Supplementary Online Content Colla CH, Wennberg DE, Meara E, et al. Spending differences associated with the Medicare Physician Group Practice Demonstration. JAMA. 2012;308(10):1015-1023. eappendix. Methodologic
Supplementary Online Content Colla CH, Wennberg DE, Meara E, et al. Spending differences associated with the Medicare Physician Group Practice Demonstration. JAMA. 2012;308(10):1015-1023. eappendix. Methodologic
Background and Issues. Aim of the Workshop Analysis Of Effectiveness And Costeffectiveness. Outline. Defining a Registry
 Aim of the Workshop Analysis Of Effectiveness And Costeffectiveness In Patient Registries ISPOR 14th Annual International Meeting May, 2009 Provide practical guidance on suitable statistical approaches
Aim of the Workshop Analysis Of Effectiveness And Costeffectiveness In Patient Registries ISPOR 14th Annual International Meeting May, 2009 Provide practical guidance on suitable statistical approaches
Healthcare- Associated Infections in North Carolina
 2018 Healthcare- Associated Infections in North Carolina Reference Document Revised June 2018 NC Surveillance for Healthcare-Associated and Resistant Pathogens Patient Safety Program NC Department of Health
2018 Healthcare- Associated Infections in North Carolina Reference Document Revised June 2018 NC Surveillance for Healthcare-Associated and Resistant Pathogens Patient Safety Program NC Department of Health
Peri-operative Pain Management - a multi-disciplinary team-based approach
 Peri-operative Pain Management - a multi-disciplinary team-based approach Dr Steven Wong Chief of Service Department of Anaesthesiology & OT Services Queen Elizabeth Hospital Outline Development of postoperative
Peri-operative Pain Management - a multi-disciplinary team-based approach Dr Steven Wong Chief of Service Department of Anaesthesiology & OT Services Queen Elizabeth Hospital Outline Development of postoperative
Enhanced Recovery After Surgery (ERAS) for Elective Colon Resection Surgery at Vancouver General Hospital. What is Possible?
 Enhanced Recovery After Surgery (ERAS) for Elective Colon Resection Surgery at Vancouver General Hospital What is Possible? BC Provincial Collaborative November 25, 2014 Disclosure Statement I do not have
Enhanced Recovery After Surgery (ERAS) for Elective Colon Resection Surgery at Vancouver General Hospital What is Possible? BC Provincial Collaborative November 25, 2014 Disclosure Statement I do not have
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings
 Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings May 11, 2009 Avalere Health LLC Avalere Health LLC The intersection
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings May 11, 2009 Avalere Health LLC Avalere Health LLC The intersection
Death and readmission after intensive care the ICU might allow these patients to be kept in ICU for a further period, to triage the patient to an appr
 British Journal of Anaesthesia 100 (5): 656 62 (2008) doi:10.1093/bja/aen069 Advance Access publication April 2, 2008 CRITICAL CARE Predicting death and readmission after intensive care discharge A. J.
British Journal of Anaesthesia 100 (5): 656 62 (2008) doi:10.1093/bja/aen069 Advance Access publication April 2, 2008 CRITICAL CARE Predicting death and readmission after intensive care discharge A. J.
TC911 SERVICE COORDINATION PROGRAM
 TC911 SERVICE COORDINATION PROGRAM ANALYSIS OF PROGRAM IMPACTS & SUSTAINABILITY CONDUCTED BY: Bill Wright, PhD Sarah Tran, MPH Jennifer Matson, MPH The Center for Outcomes Research & Education Providence
TC911 SERVICE COORDINATION PROGRAM ANALYSIS OF PROGRAM IMPACTS & SUSTAINABILITY CONDUCTED BY: Bill Wright, PhD Sarah Tran, MPH Jennifer Matson, MPH The Center for Outcomes Research & Education Providence
Work In Progress August 24, 2015
 Presenter Sarah Wilson MSOTR/L, CHT, CLT 4 th year PhD student at NOVA Southeastern University Practicing OT for 14 years Have worked for Washington Orthopedics and Sports Medicine for the last 8 years
Presenter Sarah Wilson MSOTR/L, CHT, CLT 4 th year PhD student at NOVA Southeastern University Practicing OT for 14 years Have worked for Washington Orthopedics and Sports Medicine for the last 8 years
Hospital Strength INDEX Methodology
 2017 Hospital Strength INDEX 2017 The Chartis Group, LLC. Table of Contents Research and Analytic Team... 2 Hospital Strength INDEX Summary... 3 Figure 1. Summary... 3 Summary... 4 Hospitals in the Study
2017 Hospital Strength INDEX 2017 The Chartis Group, LLC. Table of Contents Research and Analytic Team... 2 Hospital Strength INDEX Summary... 3 Figure 1. Summary... 3 Summary... 4 Hospitals in the Study
MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN INDIANS & ALASKA NATIVES
 American Indian & Alaska Native Data Project of the Centers for Medicare and Medicaid Services Tribal Technical Advisory Group MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN
American Indian & Alaska Native Data Project of the Centers for Medicare and Medicaid Services Tribal Technical Advisory Group MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN
IMPACT OF RN HYPERTENSION PROTOCOL
 1 IMPACT OF RN HYPERTENSION PROTOCOL Joyce Cheung, RN, Marie Kuzmack, RN Orange County Hypertension Team Kaiser Permanente, Orange County Joyce.m.cheung@kp.org and marie-aline.z.kuzmack@kp.org Cell phone:
1 IMPACT OF RN HYPERTENSION PROTOCOL Joyce Cheung, RN, Marie Kuzmack, RN Orange County Hypertension Team Kaiser Permanente, Orange County Joyce.m.cheung@kp.org and marie-aline.z.kuzmack@kp.org Cell phone:
National Priorities for Improvement:
 National Priorities for Improvement: Standardization of Performance Measures, Data Collection, and Analysis Dale W. Bratzler, DO, MPH Principal Clinical Coordinator Oklahoma Foundation Contracting for
National Priorities for Improvement: Standardization of Performance Measures, Data Collection, and Analysis Dale W. Bratzler, DO, MPH Principal Clinical Coordinator Oklahoma Foundation Contracting for
Burnout in ICU caregivers: A multicenter study of factors associated to centers
 Burnout in ICU caregivers: A multicenter study of factors associated to centers Paolo Merlani, Mélanie Verdon, Adrian Businger, Guido Domenighetti, Hans Pargger, Bara Ricou and the STRESI+ group Online
Burnout in ICU caregivers: A multicenter study of factors associated to centers Paolo Merlani, Mélanie Verdon, Adrian Businger, Guido Domenighetti, Hans Pargger, Bara Ricou and the STRESI+ group Online
Predicting use of Nurse Care Coordination by Patients in a Health Care Home
 Predicting use of Nurse Care Coordination by Patients in a Health Care Home Catherine E. Vanderboom PhD, RN Clinical Nurse Researcher Mayo Clinic Rochester, MN USA 3 rd Annual ICHNO Conference Chicago,
Predicting use of Nurse Care Coordination by Patients in a Health Care Home Catherine E. Vanderboom PhD, RN Clinical Nurse Researcher Mayo Clinic Rochester, MN USA 3 rd Annual ICHNO Conference Chicago,
Enhanced Recovery Implementing Meaningful Change
 Enhanced Recovery Implementing Meaningful Change Jeff Simmons MD Associate Professor UAB Department of Anesthesiology and Perioperative Medicine I have no relevant financial relationships to disclose.
Enhanced Recovery Implementing Meaningful Change Jeff Simmons MD Associate Professor UAB Department of Anesthesiology and Perioperative Medicine I have no relevant financial relationships to disclose.
Hospital Inpatient Quality Reporting (IQR) Program
 Clinical Episode-Based Payment (CEBP) Measures Questions & Answers Moderator Candace Jackson, RN Project Lead, Hospital IQR Program Hospital Inpatient Value, Incentives, and Quality Reporting (VIQR) Outreach
Clinical Episode-Based Payment (CEBP) Measures Questions & Answers Moderator Candace Jackson, RN Project Lead, Hospital IQR Program Hospital Inpatient Value, Incentives, and Quality Reporting (VIQR) Outreach
Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence
 CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
Quality Based Impacts to Medicare Inpatient Payments
 Quality Based Impacts to Medicare Inpatient Payments Overview New Developments in Quality Based Reimbursement Recap of programs Hospital acquired conditions Readmission reduction program Value based purchasing
Quality Based Impacts to Medicare Inpatient Payments Overview New Developments in Quality Based Reimbursement Recap of programs Hospital acquired conditions Readmission reduction program Value based purchasing
Introduction and Executive Summary
 Introduction and Executive Summary 1. Introduction and Executive Summary. Hospital length of stay (LOS) varies markedly and persistently across geographic areas in the United States. This phenomenon is
Introduction and Executive Summary 1. Introduction and Executive Summary. Hospital length of stay (LOS) varies markedly and persistently across geographic areas in the United States. This phenomenon is
ACS NSQIP Pediatric Participant Use Data File (PUF)
 ACS NSQIP Pediatric Participant Use Data File (PUF) Christine L. Sullivan, MBA, MS Continuous Quality Improvement, Division of Research and Optimal Patient Care American College of Surgeons July 22, 2017
ACS NSQIP Pediatric Participant Use Data File (PUF) Christine L. Sullivan, MBA, MS Continuous Quality Improvement, Division of Research and Optimal Patient Care American College of Surgeons July 22, 2017
The Basics: Disease-Specific Care Certification Clinical Practice Guidelines and Performance Measures
 The Basics: Disease-Specific Care Certification Clinical Practice Guidelines and Performance Measures June 21, 2017 Caroline Isbey, RN, MSN, CDE Associate Director, Certification David Eickemeyer, MBA
The Basics: Disease-Specific Care Certification Clinical Practice Guidelines and Performance Measures June 21, 2017 Caroline Isbey, RN, MSN, CDE Associate Director, Certification David Eickemeyer, MBA
National Hospice and Palliative Care OrganizatioN. Facts AND Figures. Hospice Care in America. NHPCO Facts & Figures edition
 National Hospice and Palliative Care OrganizatioN Facts AND Figures Hospice Care in America 2017 Edition NHPCO Facts & Figures - 2017 edition Table of Contents 2 Introduction 2 About this report 2 What
National Hospice and Palliative Care OrganizatioN Facts AND Figures Hospice Care in America 2017 Edition NHPCO Facts & Figures - 2017 edition Table of Contents 2 Introduction 2 About this report 2 What
Hip Hemi-Arthroplasty vs Total Hip Replacement for Displaced Intra-Capsular Hip Fractures: Retrospective Age and Sex Matched Cohort Study
 Ulster Med J 28;87():7-2 Clinical Paper Hip Hemi-Arthroplasty vs Total Hip Replacement for Displaced Intra-Capsular Hip Fractures: Retrospective Age and Sex Matched Cohort Study Daniel Dawson, David Milligan,
Ulster Med J 28;87():7-2 Clinical Paper Hip Hemi-Arthroplasty vs Total Hip Replacement for Displaced Intra-Capsular Hip Fractures: Retrospective Age and Sex Matched Cohort Study Daniel Dawson, David Milligan,
Telephone triage systems in UK general practice:
 Research Tim A Holt, Emily Fletcher, Fiona Warren, Suzanne Richards, Chris Salisbury, Raff Calitri, Colin Green, Rod Taylor, David A Richards, Anna Varley and John Campbell Telephone triage systems in
Research Tim A Holt, Emily Fletcher, Fiona Warren, Suzanne Richards, Chris Salisbury, Raff Calitri, Colin Green, Rod Taylor, David A Richards, Anna Varley and John Campbell Telephone triage systems in
Low Molecular Weight Heparins
 ril 2014 Low Molecular Weight Heparins FINAL CONSOLIDATED COMPREHENSIVE RESEARCH PLAN September 2015 FINALCOMPREHENSIVE RESEARCH PLAN 2 A. Introduction The objective of the drug class review on LMWH is
ril 2014 Low Molecular Weight Heparins FINAL CONSOLIDATED COMPREHENSIVE RESEARCH PLAN September 2015 FINALCOMPREHENSIVE RESEARCH PLAN 2 A. Introduction The objective of the drug class review on LMWH is
Bundled Payments to Align Providers and Increase Value to Patients
 Bundled Payments to Align Providers and Increase Value to Patients Stephanie Calcasola, MSN, RN-BC Director of Quality and Medical Management Baystate Health Baystate Medical Center Baystate Health Is
Bundled Payments to Align Providers and Increase Value to Patients Stephanie Calcasola, MSN, RN-BC Director of Quality and Medical Management Baystate Health Baystate Medical Center Baystate Health Is
Version 1.0 (posted Aug ) Aaron L. Leppin. Background. Introduction
 Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
From Risk Scores to Impactability Scores:
 From Risk Scores to Impactability Scores: Innovations in Care Management Carlos T. Jackson, Ph.D. September 14, 2015 Outline Population Health What is Impactability? Complex Care Management Transitional
From Risk Scores to Impactability Scores: Innovations in Care Management Carlos T. Jackson, Ph.D. September 14, 2015 Outline Population Health What is Impactability? Complex Care Management Transitional
Association between organizational factors and quality of care: an examination of hospital performance indicators
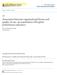 University of Iowa Iowa Research Online Theses and Dissertations 2010 Association between organizational factors and quality of care: an examination of hospital performance indicators Smruti Chandrakant
University of Iowa Iowa Research Online Theses and Dissertations 2010 Association between organizational factors and quality of care: an examination of hospital performance indicators Smruti Chandrakant
Oscar Guillamondegui, MD, MPH, FACS Associate Professor of Surgery Tennessee Surgical Quality Collaborative
 Oscar Guillamondegui, MD, MPH, FACS Associate Professor of Surgery Tennessee Surgical Quality Collaborative NSQIP 2014 A Collaborative that has Reduced Surgical Site Infections Tennessee Surgical Quality
Oscar Guillamondegui, MD, MPH, FACS Associate Professor of Surgery Tennessee Surgical Quality Collaborative NSQIP 2014 A Collaborative that has Reduced Surgical Site Infections Tennessee Surgical Quality
NUTRITION SCREENING SURVEYS IN HOSPITALS IN NORTHERN IRELAND,
 NUTRITION SCREENING SURVEYS IN HOSPITALS IN NORTHERN IRELAND, 2007-2011 A report based on the amalgamated data from the four Nutrition Screening Week surveys undertaken by BAPEN in 2007, 2008, 2010 and
NUTRITION SCREENING SURVEYS IN HOSPITALS IN NORTHERN IRELAND, 2007-2011 A report based on the amalgamated data from the four Nutrition Screening Week surveys undertaken by BAPEN in 2007, 2008, 2010 and
Chapter 39 Bed occupancy
 National Institute for Health and Care Excellence Final Chapter 39 Bed occupancy Emergency and acute medical care in over 16s: service delivery and organisation NICE guideline 94 March 218 Developed by
National Institute for Health and Care Excellence Final Chapter 39 Bed occupancy Emergency and acute medical care in over 16s: service delivery and organisation NICE guideline 94 March 218 Developed by
September 6, RE: CY 2017 Hospital Outpatient Prospective Payment and Ambulatory Surgical Center Payment Systems Proposed Rule
 September 6, 2016 VIA E-MAIL FILING Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-1656-P P.O. Box 8013 Baltimore, MD 21244-1850 RE: CY 2017 Hospital Outpatient
September 6, 2016 VIA E-MAIL FILING Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-1656-P P.O. Box 8013 Baltimore, MD 21244-1850 RE: CY 2017 Hospital Outpatient
Comparison of Care in Hospital Outpatient Departments and Physician Offices
 Comparison of Care in Hospital Outpatient Departments and Physician Offices Final Report Prepared for: American Hospital Association February 2015 Berna Demiralp, PhD Delia Belausteguigoitia Qian Zhang,
Comparison of Care in Hospital Outpatient Departments and Physician Offices Final Report Prepared for: American Hospital Association February 2015 Berna Demiralp, PhD Delia Belausteguigoitia Qian Zhang,
Integrated care for asthma: matching care to the patient
 Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Reliability of Evaluating Hospital Quality by Surgical Site Infection Type. ACS NSQIP Conference July 22, 2012
 Reliability of Evaluating Hospital Quality by Surgical Site Infection Type ACS NSQIP Conference July, 01 Surgical Site Infection Common cause of patient morbidity 5%-6% for colorectal procedures Significant
Reliability of Evaluating Hospital Quality by Surgical Site Infection Type ACS NSQIP Conference July, 01 Surgical Site Infection Common cause of patient morbidity 5%-6% for colorectal procedures Significant
? Prehab, immunonutrition. Safe surgical principles. Optimizing Preoperative Evaluation
 Optimizing Preoperative Evaluation Timothy Geiger, MD, MMHC Associate Professor of Surgery Executive Medical Director, Surgery Patient Care Center Chief, Division of General Surgery Director, Colon and
Optimizing Preoperative Evaluation Timothy Geiger, MD, MMHC Associate Professor of Surgery Executive Medical Director, Surgery Patient Care Center Chief, Division of General Surgery Director, Colon and
Linking Supply Chain, Patient Safety and Clinical Outcomes
 Premier s Vision for High Performing Healthcare Organizations: Linking Supply Chain, Patient Safety and Clinical Outcomes Joe M. Pleasant Sr. VP and CIO Premier Inc. Global GS1 Conference Hong Kong October
Premier s Vision for High Performing Healthcare Organizations: Linking Supply Chain, Patient Safety and Clinical Outcomes Joe M. Pleasant Sr. VP and CIO Premier Inc. Global GS1 Conference Hong Kong October
A Regional Payer/Provider Partnership to Reduce Readmissions The Bronx Collaborative Care Transitions Program: Outcomes and Lessons Learned
 A Regional Payer/Provider Partnership to Reduce Readmissions The Bronx Collaborative Care Transitions Program: Outcomes and Lessons Learned Stephen Rosenthal, MBA President and COO, Montefiore Care Management
A Regional Payer/Provider Partnership to Reduce Readmissions The Bronx Collaborative Care Transitions Program: Outcomes and Lessons Learned Stephen Rosenthal, MBA President and COO, Montefiore Care Management
The introduction of the first freestanding ambulatory
 Epidemiology of Ambulatory Anesthesia for Children in the United States: and 1996 Jennifer A. Rabbitts, MB, ChB,* Cornelius B. Groenewald, MB, ChB,* James P. Moriarty, MSc, and Randall Flick, MD, MPH*
Epidemiology of Ambulatory Anesthesia for Children in the United States: and 1996 Jennifer A. Rabbitts, MB, ChB,* Cornelius B. Groenewald, MB, ChB,* James P. Moriarty, MSc, and Randall Flick, MD, MPH*
