2.2. Preoperative preparation: Ensure that the child/young person is fit for surgery. If there is any doubt consult the anaesthetist.
|
|
|
- Gregory Cunningham
- 5 years ago
- Views:
Transcription
1 Clinical guideline for the supportive care and insertion of skin tunnelled catheters (Hickman lines) and totally implantable devices (Portacaths) in children and young people on the CLIC Unit at RCHT. 1. Aim/Purpose of this Guideline 1.1. This guideline aims to give clear information for supportive care for the insertion of skin tunneled catheters (Hickman lines) and totally implantable devices (Portacaths) in children and young on the CLIC Unit at RCHT. 2. The Guidance 2.1. Skin tunnelled catheters (Hickman lines) and fully implantable devices (Portacaths) are routinely used on the CLIC Unit. In the majority of cases the devices are inserted at Bristol Royal Hospital for Children. Occasionally the devices are inserted at Royal Cornwall Hospitals NHS Trust (RCHT) following discussion and under the care of the vascular surgeons Preoperative preparation: Ensure that the child/young person is fit for surgery. If there is any doubt consult the anaesthetist. The anaesthetist will review the child/young person prior to the procedure. Preparation and education should be provided to the child/young adult and family prior to the procedure e.g. Wiggly Colouring Book, BRHC Information pack for parents, Play Specialists. Bloods should be checked prior to the procedure (e.g. FBC, clotting screen, G&S). It is generally accepted that the platelet count should be > /litre prior to the insertion of the catheter other than a PICC, and the INR <1.5. Ensure that surgeon is aware of the results. The procedure is performed in general theatres under a general anaesthetic. Skin cleansing is the most important part of care for prevention of infection before catheter insertion. The number of lumina and diameter of catheters should be kept to a minimum. The surgeon will consent the child/young person for the procedure and discuss the device placement with the child/young adult and family. Page 1 of 12
2 2.3. Antibiotic prophylais: Prophylactic antibiotics should not be routinely used. Antibiotic cover may be appropriate if there is simultaneous removal and insertion of catheters in a proven case of catheter-related sepsis. In this circumstance antibiotics are continued for a minimum of 48 hours post insertion of the new catheter unless microbiologist advises a longer course. The antibiotics may be given via the new catheter in most cases Postoperative: Following insertion of the device the patient should be carefully monitored. This includes postoperative monitoring of temperature, pulse, BP, respiratory rate, oygen saturation as well as observation of central venous catheter (CVC) eit site, skin tunnel, and insertion site. There are a number of potential post-operative complications following insertion of a CVC. Appropriate supportive care must be commenced immediately if any complications are suspected. Pneumothora Cardiac tamponade Arterial puncture Haemorrhage Haemothora Hydrothora Air embolus Brachial pleus injury Thoracic duct injury Occlusion Thrombosis Fracture Infection Misplacement of central venous catheter The child/young person may have an infusion running into the new line on return from theatre. The child/young adult may be fit for discharge later that day Dressings: The dressing is checked for signs of bleeding and should be changed if bleeding has occurred. Otherwise the dressing is changed hours after the catheter insertion and weekly thereafter (sooner if dressing is no longer intact or if moisture has collected underneath). A sterile gauze type dressing may be used if there is bleeding or oozing post insertion of catheter. When gauze dressings are used the eit site and dressing must be assessed and changed daily. Page 2 of 12
3 Until wound healing has occurred a sterile dressing change procedure should be used (for the first 28 days after CVC insertion). Then aseptic non touch technique (ANTT) should be followed. The recommended dressing is transparent and semi-occlusive eg Opsite fleigrid, C-view film. This ensures that the device is secure and permits visual inspection of the catheter site. A review has found no consistent benefit for any type of dressing and the choice of dressing may be a matter of preference. Skin-tunnelled dressings may not require a dressing once the wound has healed. However on the CLIC Unit we prefer to use dressings. Nylon fiation sutures may be routinely removed after 4 weeks if: The cuff is securely fied within the skin tunnel The sutures irritate the skin or provide a focus for infection or debris collection The suture is too tight and causing CVC occlusion Steri-strips should be removed after 7-10 days. Routine cleaning of the eit site is not required for established lines. However if the eit site, skin and CVC under the dressing is damp or soiled then the area should be cleaned using non touch technique with a single use 2% chloheidine gluconate in 70% alcohol applicator eg Enturia Chloraprep Check catheter placement: Do not use the new central venous line without ensuring the position of the line has been confirmed. The device position is checked in theatre and recorded in the theatre notes (checked on image intensifier). If it is not clear from the operation note that the device position has been confirmed then tip placement should be checked by X-ray prior to use and the position of the catheter tip should be documented in the patient s notes. The best tip position is the distal vena cava or the upper right atrium Long term catheter care: In order to reduce the risks and prevent complications associated with the use of long term catheters only those trained and assessed as competent should be involved in accessing and caring for these devices. Securing the skin tunnelled CVC is essential to prevent accidental dislodgement or removal especially in the first 4 weeks, until fibrin has collected around the Dacron cuff. The end of the skin tunnelled catheter CVC should be looped and secured to the chest wall under the clear dressing. Fiation tape is used to reduce pull on the CVC and maintain stability eg mepore tape. LOOP IT OR LOSE IT Catheter patency is maintained by flushing with the correct solutions according to the manufacturers recommendations. The flush technique should involve push-pause action to create turbulence within the catheter lumen, removing debris from the internal catheter wall. Page 3 of 12
4 When locking the CVC between uses a positive pressure technique should be used in order to prevent reflu of blood into the catheter. Due to the risk of catheter damage from ecessive pressure syringes smaller than 10ml should not be used. The use of heparin flushes vs. normal saline intermittent flushes remains controversial. A review of the current evidence has concluded that heparin doses of 10 units/ml are no more beneficial than flushing with normal saline alone. Some manufacturers and clinicians recommend heparin flushes when catheters are used infrequently. Eposure to heparin should be minimized. CVCs that are accessed frequently will not need to be locked with heparinised saline after each access At RCHT CLIC Unit the current advice for lock solutions is: Line Solution frequency Skin-tunnelled (Hickman, Cook, Broviac) Ports 5-10mls sodium chloride 0.9% +/- 3-5mls heparinised saline (10 units/ml) 5-10mls sodium chloride 0.9% +/- 4-6mls heparinised saline (100 units/ml) After each access or weekly After each access or monthly 2.9. Swimming Swimming must be avoided with any eternal catheter in order to prevent colonisation by Gram-negative organisms e.g. Pseudomonas spp Bathing and showering The eternal CVC is held in position by tissue growth into the Dacron cuff under the skin. Until this occurs (usually about 4 weeks after insertion) dressings and tapes are important in securing the CVC and should be kept dry. After 4 weeks normal showering or bathing can be resumed. However neither the CVC nor the eit site should be submerged under water for any length of time Bathing The eit site and eternal CVC should be kept out of the water during bathing. If the dressing becomes wet or dislodged during bathing then the eit site should be dried with sterile gauze and a new dressing applied Showering Showering can resume after the eit site has healed (about 4 weeks after insertion of the eternal CVC). The dressing should be removed prior to showering. Do not use soap or shower gel near the eit site. After showering the eit site should be dried with sterile gauze and a new dressing applied. Page 4 of 12
5 2.13. Ports Patients with a Port can swim or shower as long as the port is not accessed with a gripper needle Damage or accidental removal of CVC Patients and carers must be aware of who to contact should a problem arise related to the device (The CLIC Unit ). They should receive education and training in the risks associated with a CVC and the appropriate monitoring and care of the device. A CVC Safety Pack (from CLIC Unit) should be provided, with training, so that the carer or child/young adult knows what to do in an emergency. The CVC Safety Pack consists of: Sterile gauze 2 clamps (gate or peripheral adaptor clamps) Dressings Accidental removal of CVC Apply pressure to the eit site in order to stop bleeding. The patient should be assessed by a doctor. Document the incident in patient s notes Damage to CVC The patient should have a CVC Safety Pack with them at all times. Plastic clamps should be applied proimal to the damaged area of the CVC. If only sterile clamps are available then the CVC must be protected by wrapping sterile gauze around the site to be clamped. Apply a sterile dressing to the damaged area of the CVC for protection prior to assessment for repair Repair of CVCs Long term CVCs that are split, leaking or damaged may be able to be repaired. If possible CVCs should be repaired within 24 hours to reduce the risk of infection. Assessment should be made by a competent member of staff that it is practical for a repair to be done. Only members of staff who are trained and assessed as competent should carry out a CVC repair. Hickman line repair kits are available in the store cupboard on CLIC Unit or General Theatres. Document the repair in the patient s notes. Page 5 of 12
6 3. Monitoring compliance and effectiveness Element to be monitored Lead Tool Frequency Reporting arrangements Acting on recommendations and Lead(s) Compliance with all elements of guideline Audit lead Dr.Katrina MacDonald Paediatric oncology team Audit and annual review Peer review- annually Annually or earlier if required Paediatric oncology team Department audit and guidelines meeting Paediatric oncology team Department audit and guidelines meeting Required actions will be identified and completed in 3-6 months Change in practice and lessons to be shared Required changes to practice will be identified and actioned within3-6 months. A lead member of the team will be identified to take each change forward where appropriate. Lessons will be shared with all the relevant stakeholders 4. Equality and Diversity 4.1. This document complies with the Royal Cornwall Hospitals NHS Trust service Equality and Diversity statement Equality Impact Assessment The Initial Equality Impact Assessment Screening Form is at Appendi 2. Page 6 of 12
7 Appendi 1. Governance Information Document Title Clinical Guideline for supportive care for the insertion of skin tunnelled catheters (Hickman Lines) and totally implantable devices (Portacaths) in children and young people on the CLIC unit at RCHT. Date Issued/Approved: February 2014 Date Valid From: February 2014 Date Valid To: February 2017 etended to August 2017 Directorate / Department responsible (author/owner): Contact details: Brief summary of contents Suggested Keywords: Target Audience Eecutive Director responsible for Policy: Dr. K.Macdonald-Associate specialist Sue Turk- CLIC Sargent outreach nurse Sabrina Teirney- senior paediatric pharmacist Clear guidance for supportive care for the insertion of skin tunnelled catheters (Hickman Lines) and totally implantable devices (Portacaths) in children and young people on the CLIC unit at RCHT. Children Oncology Paedaitrics Portacath Hickman line RCHT PCH CFT KCCG Eecutive Director Date revised: December 2013 This document replaces (eact title of previous version): Approval route (names of committees)/consultation: Guideline for supportive care for the insertion of skin tunnelled catheters (Hickman lines) and totally implantable devices (Portacaths) in children and young adults on the CLIC Unit at RCHT Paediatric oncology team Department audit and guidelines meeting Divisional Manager confirming approval processes Sheena Wallace Page 7 of 12
8 Name and Post Title of additional signatories Signature of Eecutive Director giving approval Publication Location (refer to Policy on Policies Approvals and Ratification): Document Library Folder/Sub Folder Links to key eternal standards Not Required {Original Copy Signed} Internet & Intranet Paediatrics none Intranet Only RCHT GEN 57 Central Venous Catheter (CVC) Guidelines (ecluding dialysis catheters) Bristol Royal Hospital for Children Clinical Guideline November Central Venous Catheter Guidelines. BCSH (British Committee for Standards in Haematology) for Guidelines on the insertion and management of central venous access devices (2006) Related Documents: Guidelines on the insertion and management of central venous access devices in adults (International Journal of Laboratory Haematology 2007) Ansell et al 2004, Douketis, Johnson & Turpie 2004 Farkas et al 1992, Dezfulian et al 2003 Knutstad, Hager & Hauser 2003 O Grady et al 2002, Pratt et al 2001 Gillies et al 2003 Morris et al 1995, O Grady et al 2002 Fletcher & Bodenham 2000 Pellowe et al 2004 Training Need Identified? No Page 8 of 12
9 Version Control Table Date Versio n No Summary of Changes Changes Made by (Name and Job Title) Feb 12 V1.0 Initial Issue Feb 2014 V2.0 Review and re format Dr.N.Gilbertson-paediatric consultant Dr.K.Macdonald- Assosciate specialist Sue Turk-CLIC sargent outreach nurse Sabrina Tierney-senior paediatric pharmacist. Dr.K.Macdonald- Assosciate specialist Sue Turk-CLIC sargent outreach nurse Tabitha Fergus-Deputy ward manager format only Sabrina Tierney-senior All or part of this document can be released under the Freedom of Information Act 2000 This document is to be retained for 10 years from the date of epiry. This document is only valid on the day of printing Controlled Document This document has been created following the Royal Cornwall Hospitals NHS Trust Policy on Document Production. It should not be altered in any way without the epress permission of the author or their Line Manager. Page 9 of 12
10 Appendi 2. Initial Equality Impact Assessment Form Name of the strategy / policy /proposal / service function to be assessed (hereafter referred to as policy) (Provide brief description): Clinical Guideline for supportive care for the insertion of skin tunnelled catheters (Hickman Lines) and totally implantable devices (Portacaths) in children and young people on the CLIC unit at RCHT. Directorate and service area: child health Is this a new or eisting Policy? eisting Name of individual completing assessment: t.fergus 1. Policy Aim* Who is the strategy / policy / proposal / service function aimed at? Telephone: Clear guidance for supportive care for the insertion of skin tunnelled catheters (Hickman Lines) and totally implantable devices 2. Policy Objectives* Clear guidance for supportive care for the insertion of skin tunnelled catheters (Hickman Lines) and totally implantable devices 3. Policy intended Outcomes* 4. *How will you measure the outcome? 5. Who is intended to benefit from the policy? 6a) Is consultation required with the workforce, equality groups, local interest groups etc. around this policy? Evidence based and standardised practice. audit Children and families no b) If yes, have these *groups been consulted? C). Please list any groups who have been consulted about this procedure. Page 10 of 12
11 7. The Impact Please complete the following table. Are there concerns that the policy could have differential impact on: Equality Strands: Yes No Rationale for Assessment / Eisting Evidence Age Se (male, female, transgender / gender reassignment) Race / Ethnic communities /groups Disability - learning disability, physical disability, sensory impairment and mental health problems Religion / other beliefs Marriage and civil partnership Pregnancy and maternity Seual Orientation, Biseual, Gay, heteroseual, Lesbian You will need to continue to a full Equality Impact Assessment if the following have been highlighted: You have ticked Yes in any column above and No consultation or evidence of there being consultation- this ecludes any policies which have been identified as not requiring consultation. or Major service redesign or development 8. Please indicate if a full equality analysis is recommended. Yes No 9. If you are not recommending a Full Impact assessment please eplain why. No areas indicated Signature of policy developer / lead manager / director.t.fergus Date of completion and submission5/2/14 Names and signatures of members carrying out the Screening Assessment Keep one copy and send a copy to the Human Rights, Equality and Inclusion Lead, c/o Royal Cornwall Hospitals NHS Trust, Human Resources Department, Knowledge Spa, Truro, Cornwall, TR1 3HD Page 11 of 12
12 A summary of the results will be published on the Trust s web site. Signed T.Fergus Date 5/2/14 Page 12 of 12
CLINICAL GUIDELINE FOR THE USE OF INTRAVENOUS SLIDING SCALE REGIMEN FOR ADULTS 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR THE USE OF INTRAVENOUS SLIDING SCALE REGIMEN FOR ADULTS 1. Aim/Purpose of this Guideline This guideline is for the management of for the management of Adult patients with Mellitus
CLINICAL GUIDELINE FOR THE USE OF INTRAVENOUS SLIDING SCALE REGIMEN FOR ADULTS 1. Aim/Purpose of this Guideline This guideline is for the management of for the management of Adult patients with Mellitus
2.1. Applicable areas: Royal Cornwall Hospitals Trust; Neonatal Unit and Delivery Suite
 ADVANCED NEONATAL NURSE PRACTITIONERS (ANNPs) BLOOD COMPONENT AND BLOOD PRODUCT REQUESTING PROTOCOL NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1 The purpose of this protocol is to guide
ADVANCED NEONATAL NURSE PRACTITIONERS (ANNPs) BLOOD COMPONENT AND BLOOD PRODUCT REQUESTING PROTOCOL NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1 The purpose of this protocol is to guide
Clinical Guideline for Post-Operative Nausea and Vomiting 1. Aim/Purpose of this Guideline
 Clinical Guideline for Post-Operative Nausea and Vomiting 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to provide anaesthetists with an algorithm to work with when dealing with
Clinical Guideline for Post-Operative Nausea and Vomiting 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to provide anaesthetists with an algorithm to work with when dealing with
CLINICAL GUIDELINE FOR THE MANAGEMENT OF SEPSIS IN ADULT PATIENTS 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR THE MANAGEMENT OF SEPSIS IN ADULT PATIENTS 1. Aim/Purpose of this Guideline 1.1. This guideline aims to improve outcomes for patients presenting with sepsis or developing sepsis
CLINICAL GUIDELINE FOR THE MANAGEMENT OF SEPSIS IN ADULT PATIENTS 1. Aim/Purpose of this Guideline 1.1. This guideline aims to improve outcomes for patients presenting with sepsis or developing sepsis
CLINICAL GUIDELINE FOR REFERRAL TO PAIN SERVICE 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR REFERRAL TO PAIN SERVICE 1. Aim/Purpose of this Guideline To provide guidance for appropriate referral to the acute pain service for in-patient review. 2. The Guidance PAIN SERVICES
CLINICAL GUIDELINE FOR REFERRAL TO PAIN SERVICE 1. Aim/Purpose of this Guideline To provide guidance for appropriate referral to the acute pain service for in-patient review. 2. The Guidance PAIN SERVICES
MANAGEMENT OF HEREDITARY SPHEROCYTOSIS IN THE NEONATAL PERIOD CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline
 MANAGEMENT OF HEREDITARY SPHEROCYTOSIS IN THE NEONATAL PERIOD CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1 This guideline aimed at all clinical staff responsible for the management of infants
MANAGEMENT OF HEREDITARY SPHEROCYTOSIS IN THE NEONATAL PERIOD CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1 This guideline aimed at all clinical staff responsible for the management of infants
CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline 1.1. Guidelines for the use of rectus sheath catheters for the management of pain following laparotomy
CLINICAL GUIDELINE FOR THE USE OF RECTUS SHEATH CATHETERS IN CHILDREN. 1. Aim/Purpose of this Guideline 1.1. Guidelines for the use of rectus sheath catheters for the management of pain following laparotomy
Loading Dose Worksheet for Oral Amiodarone
 This applies to adult patients only Key: General Notes ED/MAU/SRU/Acute GP/Amb-Care GP/SWASFT In-patient wards Start Prescribe as per loading dose worksheet below End 1. Aim/Purpose of this Guideline 1.1.
This applies to adult patients only Key: General Notes ED/MAU/SRU/Acute GP/Amb-Care GP/SWASFT In-patient wards Start Prescribe as per loading dose worksheet below End 1. Aim/Purpose of this Guideline 1.1.
ESCALATION PLAN PAEDIATRICS AND NEONATAL UNIT 1. Aim/Purpose of this Guideline
 ESCALATION PLAN PAEDIATRICS AND NEONATAL UNIT 1. Aim/Purpose of this Guideline 1.1. This guidance is designed to aid staff to monitor capacity and staffing in Child Health. 2. The Guidance 2.1. The majority
ESCALATION PLAN PAEDIATRICS AND NEONATAL UNIT 1. Aim/Purpose of this Guideline 1.1. This guidance is designed to aid staff to monitor capacity and staffing in Child Health. 2. The Guidance 2.1. The majority
School Vision Screening Policy V2.0
 School Vision Screening Policy V2.0 05 April 2016 Summary. Vision screening test in school PASS Visual acuity LogMAR 0.2 both eyes Kays 0.1 both eyes Outcome letter sent home Test result information put
School Vision Screening Policy V2.0 05 April 2016 Summary. Vision screening test in school PASS Visual acuity LogMAR 0.2 both eyes Kays 0.1 both eyes Outcome letter sent home Test result information put
Clinical Guideline for Nurse-Led Indocyanine Green Angiography Summary.
 Clinical Guideline for Nurse-Led Indocyanine Green Angiography Summary. Obtain brief medical history including allergies & renal function. Informed verbal consent gained and documented and procedure and
Clinical Guideline for Nurse-Led Indocyanine Green Angiography Summary. Obtain brief medical history including allergies & renal function. Informed verbal consent gained and documented and procedure and
This guideline is for nursing staff within the Pain Services assisting with the administration of botulinum toxin.
 CLINICAL GUIDELINE FOR THE SAFE ADMINISTRATION OF BOTULINUM NEURO TOIN FOR INJECTION within the PAIN SERVICE. Botox and eomin (trade names) 1. Aim/Purpose of this Guideline This guideline is for nursing
CLINICAL GUIDELINE FOR THE SAFE ADMINISTRATION OF BOTULINUM NEURO TOIN FOR INJECTION within the PAIN SERVICE. Botox and eomin (trade names) 1. Aim/Purpose of this Guideline This guideline is for nursing
Policy for the authorising of blood components by the Haematology Clinical Nurse Specialist V1.0
 Policy for the authorising of blood components by the Haematology Clinical Nurse Specialist V1.0 January 2016 Summary. This policy applies only to selected staff within the Haematology Department at the
Policy for the authorising of blood components by the Haematology Clinical Nurse Specialist V1.0 January 2016 Summary. This policy applies only to selected staff within the Haematology Department at the
PRESCRIBING, DISPENSING AND ADMINISTRATION OF CHEMOTHERAPY TO CHILDREN AND YOUNG PEOPLE - CLINICAL GUIDELINE V4.0
 PRESCRIBING, DISPENSING AND ADMINISTRATION OF CHEMOTHERAPY TO CHILDREN AND YOUNG PEOPLE - CLINICAL GUIDELINE V4.0 Clinical Guideline Template Page 1 of 14 1. Aim/Purpose of this Guideline 1.1. This guideline
PRESCRIBING, DISPENSING AND ADMINISTRATION OF CHEMOTHERAPY TO CHILDREN AND YOUNG PEOPLE - CLINICAL GUIDELINE V4.0 Clinical Guideline Template Page 1 of 14 1. Aim/Purpose of this Guideline 1.1. This guideline
CLINICAL GUIDELINE FOR THE ASSESSMENT AND DOCUMENTATION OF PAIN (ADULTS)
 CLINICAL GUIDELINE FOR THE ASSESSMENT AND DOCUMENTATION OF PAIN (ADULTS) 1. Aim/Purpose of this Guideline 1.1. Pain is whatever the experiencing person says it is, existing whenever the experiencing person
CLINICAL GUIDELINE FOR THE ASSESSMENT AND DOCUMENTATION OF PAIN (ADULTS) 1. Aim/Purpose of this Guideline 1.1. Pain is whatever the experiencing person says it is, existing whenever the experiencing person
CLINICAL GUIDELINE FOR: Management of low-risk upper GI haemorrhage. Page 1 of 10. Management of low-risk upper GI haemorrhage
 CLINICAL GUIDELINE FOR: Page 1 of 10 Summary AGE
CLINICAL GUIDELINE FOR: Page 1 of 10 Summary AGE
A list of authorised referrers will be retained by the Colposcopy team and the Clinical Imaging Department.
 Clinical Guideline for Clinical Imaging Referral Protocol for Nurse Colposcopist within Colposcopy Dept. Royal Cornwall Hospital 1. Aim/Purpose of this Guideline 1.1 This protocol applies to Nurse Colposcopist
Clinical Guideline for Clinical Imaging Referral Protocol for Nurse Colposcopist within Colposcopy Dept. Royal Cornwall Hospital 1. Aim/Purpose of this Guideline 1.1 This protocol applies to Nurse Colposcopist
CLINICAL GUIDELINE FOR USE OF BED AND CHAIR SENSOR ALARM MATS FOR PREVENTING FALLS IN ADULT PATIENTS
 CLINICAL GUIDELINE FOR USE OF BED AND CHAIR SENSOR ALARM MATS FOR PREVENTING FALLS IN ADULT PATIENTS 1. Aim/Purpose of this Guideline This guideline is to support the use of bed and chair sensor alarm
CLINICAL GUIDELINE FOR USE OF BED AND CHAIR SENSOR ALARM MATS FOR PREVENTING FALLS IN ADULT PATIENTS 1. Aim/Purpose of this Guideline This guideline is to support the use of bed and chair sensor alarm
PARACETAMOL PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline
 PARACETAMOL PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical staff in the Child Health Department and its
PARACETAMOL PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical staff in the Child Health Department and its
CLINICAL GUIDELINE FOR IPRATROPIUM BROMIDE NEBULISER INHALER PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR IPRATROPIUM BROMIDE NEBULISER INHALER PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical
CLINICAL GUIDELINE FOR IPRATROPIUM BROMIDE NEBULISER INHALER PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical
CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0
 CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0 Page 1 of 13 Abbreviation (P/A)HDU (P/A)ICU GCS IPPV CPAP BiPAP DKA Reg Meaning (Paediatric/Adult) High Dependency
CLINICAL GUIDELINE FOR THE ADMISSION OF PATIENTS TO PAEDIATRIC HIGH DEPENDANCY UNIT V4.0 Page 1 of 13 Abbreviation (P/A)HDU (P/A)ICU GCS IPPV CPAP BiPAP DKA Reg Meaning (Paediatric/Adult) High Dependency
Policy on Governance Arrangements Relating to Medicines V2.0
 V2.0 August 2015 Summary. The policy outlines the governance arrangements for medicines within the Trust, specifically; 1. The committee structure in the Trust and the county for medicine related matters
V2.0 August 2015 Summary. The policy outlines the governance arrangements for medicines within the Trust, specifically; 1. The committee structure in the Trust and the county for medicine related matters
CLINICAL GUIDELINE FOR CLINICAL IMAGING REFERRAL PROTOCOL FOR NURSE SPECIALISTS IN HEART FUNCTION WITHIN RCHT Summary. Start
 CLINICAL GUIDELINE FOR CLINICAL IMAGING REFERRAL PROTOCOL FOR NURSE SPECIALISTS IN HEART FUNCTION WITHIN RCHT Summary. Start The non-medical practitioner has received sufficient training to make clinical
CLINICAL GUIDELINE FOR CLINICAL IMAGING REFERRAL PROTOCOL FOR NURSE SPECIALISTS IN HEART FUNCTION WITHIN RCHT Summary. Start The non-medical practitioner has received sufficient training to make clinical
Diagnostic Test Reporting & Acknowledgement Procedures. - Pathology & Clinical Imaging
 Diagnostic Test Reporting & Acknowledgement Procedures V2.0 November 2014 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5.
Diagnostic Test Reporting & Acknowledgement Procedures V2.0 November 2014 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5.
IBUPROFEN PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline
 IBUPROFEN PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical staff in the Child Health Department and its
IBUPROFEN PATIENT GROUP DIRECTION CHILD HEALTH 1. Aim/Purpose of this Guideline 1.1. This Patient Group Direction (PGD) applies to all nursing and clinical staff in the Child Health Department and its
Diagnostic Testing Procedures in Urodynamics V3.0
 V3.0 09 01 18 Table of Contents Summary.... 1. Introduction... 3 1.1. Diagnostic testing information... 3 2. Purpose of this Policy/Procedure... 3 2.1. Approved Document Process... 3 3. Scope... 3 3.1.
V3.0 09 01 18 Table of Contents Summary.... 1. Introduction... 3 1.1. Diagnostic testing information... 3 2. Purpose of this Policy/Procedure... 3 2.1. Approved Document Process... 3 3. Scope... 3 3.1.
1.3 Referrer: in the context of this protocol the term referrer refers to a health care worker who is authorised to refer individuals for X-rays.
 Clinical Guideline for Clinical Imaging Referral Protocol for Nurse Endoscopist (Lower GI) within the Royal Cornwall Hospitals Trust 1. Aim/Purpose of this Guideline 1.1 This protocol applies to Nurse
Clinical Guideline for Clinical Imaging Referral Protocol for Nurse Endoscopist (Lower GI) within the Royal Cornwall Hospitals Trust 1. Aim/Purpose of this Guideline 1.1 This protocol applies to Nurse
CLINICAL GUIDELINE FOR THE EMERGENCY DEFILL OF AN ADJUSTABLE GASTRIC BAND
 CLINICAL GUIDELINE FOR THE EMERGENCY DEFILL OF AN ADJUSTABLE GASTRIC BAND 1. Aim/Purpose of this Guideline The aim of this guideline to enable the effective care of patients needing emergency defill of
CLINICAL GUIDELINE FOR THE EMERGENCY DEFILL OF AN ADJUSTABLE GASTRIC BAND 1. Aim/Purpose of this Guideline The aim of this guideline to enable the effective care of patients needing emergency defill of
Clinical Guideline for Clinical Imaging Referral Protocol for Upper & Lower GI Non medical Endoscopist within RCHT. 1. Aim/Purpose of this Guideline
 Clinical Guideline for Clinical Imaging Referral Protocol for Upper & Lower GI Non medical Endoscopist. 1. Aim/Purpose of this Guideline 1.1 This protocol applies to upper & lower GI Non medical Endoscopist
Clinical Guideline for Clinical Imaging Referral Protocol for Upper & Lower GI Non medical Endoscopist. 1. Aim/Purpose of this Guideline 1.1 This protocol applies to upper & lower GI Non medical Endoscopist
Procedure for the Application of a Cast and its subsequent care V1.3
 Procedure for the Application of a Cast and its subsequent care V1.3 May 2015 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary...
Procedure for the Application of a Cast and its subsequent care V1.3 May 2015 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary...
CEREBRAL FUNCTION MONITORING (aeeg). NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline
 CEREBRAL FUNCTION MONITORING (aeeg). NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide guidance on the operation and interpretation of Cerebral Function Monitoring (CFM) in neonates.
CEREBRAL FUNCTION MONITORING (aeeg). NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide guidance on the operation and interpretation of Cerebral Function Monitoring (CFM) in neonates.
CLINICAL IMAGING REFERRAL PROTOCOL FOR REGISTERED NURSE PRACTITIONERS IN THE EMERGENCY DEPARTMENT, URGENT CARE CENTRE AND AMBULATORY CARE
 CLINICAL IMAGING REFERRAL PROTOCOL FOR REGISTERED NURSE PRACTITIONERS IN THE EMERGENCY DEPARTMENT, URGENT CARE CENTRE AND AMBULATORY CARE CLINICAL GUIDELINE V4. Summary. Start The non-medical practitioner
CLINICAL IMAGING REFERRAL PROTOCOL FOR REGISTERED NURSE PRACTITIONERS IN THE EMERGENCY DEPARTMENT, URGENT CARE CENTRE AND AMBULATORY CARE CLINICAL GUIDELINE V4. Summary. Start The non-medical practitioner
The initial care and management of patients admitted to RCHT with a Ventricular Assist Device (VAD). V2.0
 The initial care and management of patients admitted to RCHT with a Ventricular Assist Device (VAD). V2.0 October 2016 Summary. Start See section 6.2 of this document for important information regarding
The initial care and management of patients admitted to RCHT with a Ventricular Assist Device (VAD). V2.0 October 2016 Summary. Start See section 6.2 of this document for important information regarding
OXYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0
 OYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline 1.1 To provide guidance on the assessment and management of infants requiring oxygen therapy
OYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline 1.1 To provide guidance on the assessment and management of infants requiring oxygen therapy
Safe Bathing Policy V1.3
 V1.3 April 2018 Summary Safe hot water temperatures The hot water distribution temperatures, which are required for the control and prevention of Legionella, can lead to discharge temperatures in excess
V1.3 April 2018 Summary Safe hot water temperatures The hot water distribution temperatures, which are required for the control and prevention of Legionella, can lead to discharge temperatures in excess
Intravenous Medication Administration via a Central Venous Line
 Standard Operating Procedure 11 (SOP 11) Intravenous Medication Administration via a Central Venous Line Why we have a procedure? This procedure is to assist/ inform healthcare professionals on how to
Standard Operating Procedure 11 (SOP 11) Intravenous Medication Administration via a Central Venous Line Why we have a procedure? This procedure is to assist/ inform healthcare professionals on how to
WARD CLOSURE POLICY V
 WARD CLOSURE POLICY V3.0 29.07.15 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 4 5.1.
WARD CLOSURE POLICY V3.0 29.07.15 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 4 5.1.
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath
 You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
Tissue Viability Referral Pathway. April 2017
 Tissue Viability Referral Pathway V4 April 2017 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities...
Tissue Viability Referral Pathway V4 April 2017 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities...
Care of Your Peripherally Inserted Central Catheter
 Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Totally Implantable Venous Access Devices (port) Information for patients. Cross section of a port
 Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
Peripherally inserted central catheter (PICC line) Information to accompany consent
 Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Risk Assessment Form HS 9 (1)
 s Full Name: Date of Birth: NHS Number 1. The fully implanted port system Sitimplant is not regularly used in the community and nursing staff may be unfamiliar with the recommended care of this system
s Full Name: Date of Birth: NHS Number 1. The fully implanted port system Sitimplant is not regularly used in the community and nursing staff may be unfamiliar with the recommended care of this system
Central Venous Access Devices (CVADs)
 Contents Purpose... 1 Policy... 1 Scope... 2 Associated documents... 2 1 Insertion of CVADs... 2 2 Endorsement/Certification... 2 3 Procedural Considerations... 3 3.1 Checking and Identification requirements...
Contents Purpose... 1 Policy... 1 Scope... 2 Associated documents... 2 1 Insertion of CVADs... 2 2 Endorsement/Certification... 2 3 Procedural Considerations... 3 3.1 Checking and Identification requirements...
2.1. It is essential that promoting and safeguarding the welfare of children and young people is integral to all NHS Trust policies and procedures.
 Was Not Brought, Cancellation and Refusal of Appointments Policy for Children and Young People up to the Age of 18 Years (up to the age of 25 years for people with a Learning Disability) 1. Aim/Purpose
Was Not Brought, Cancellation and Refusal of Appointments Policy for Children and Young People up to the Age of 18 Years (up to the age of 25 years for people with a Learning Disability) 1. Aim/Purpose
Hickman line insertion in the interventional radiology department
 Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Peripherally Inserted Central Catheter (PICC)
 University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
Diagnostic Testing Procedures in Neurophysiology V1.0
 V1.0 10 September 2012 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 3 5.2. Role of the
V1.0 10 September 2012 Table of Contents 1. Introduction... 3 2. Purpose of this Policy/Procedure... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 3 5.2. Role of the
See Policy #1302 (Nursing Student Privileges and Limitations) for full details. Central Line dressing care, declotting and discontinuation may ONLY
 To assure a standardized knowledge base related to CVL Care and CLABSI prevention, ProMedica requires all Instructors/Faculty on adult and pediatric units to complete this educational module. This content
To assure a standardized knowledge base related to CVL Care and CLABSI prevention, ProMedica requires all Instructors/Faculty on adult and pediatric units to complete this educational module. This content
Central Venous Access Devices (CVAD) Procedures
 SH CP 138 Central Venous Access Devices (CVAD) Procedures (e.g. Peripherally Inserted Central Catheter ( PICC lines) and Skin Tunnelled Central lines) Version:2 Summary: Keywords (minimum of 5): (To assist
SH CP 138 Central Venous Access Devices (CVAD) Procedures (e.g. Peripherally Inserted Central Catheter ( PICC lines) and Skin Tunnelled Central lines) Version:2 Summary: Keywords (minimum of 5): (To assist
CENTRAL VENOUS ACCESS DEVICE POLICY
 CENTRAL VENOUS ACCESS DEVICE POLICY Version: 1 Date of Issue: April 2018 Review Date: April 2021 Applies to: All clinical staff who care for patients with Central Venous Access Devices (CVADs) as part
CENTRAL VENOUS ACCESS DEVICE POLICY Version: 1 Date of Issue: April 2018 Review Date: April 2021 Applies to: All clinical staff who care for patients with Central Venous Access Devices (CVADs) as part
Hickman line insertion and caring for your line
 Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
Venous Access Devices. Management of Central Venous Access Devices (CVADs) Central Venous Catheters. Outline. Implantable Port
 Management of Central Venous Access Devices (CVADs) Bangkok June 2015 Venous Access Devices Implantable Port Central Venous Catheter (CVC) Boviac /Hickman catheters Margaret Conway BSN, RN, CPON Peripherally
Management of Central Venous Access Devices (CVADs) Bangkok June 2015 Venous Access Devices Implantable Port Central Venous Catheter (CVC) Boviac /Hickman catheters Margaret Conway BSN, RN, CPON Peripherally
Having a portacath insertion in the x-ray department
 Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
About your PICC line. Information for patients Weston Park Hospital
 About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
Information for Patients Central Venous Catheter (Haemodialysis Catheter)
 Information for Patients Central Venous Catheter (Haemodialysis Catheter) Going Home with a Haemodialysis Catheter? Important facts you must know. Haemodialysis Treatment 29/07/2018 Page 1 In order to
Information for Patients Central Venous Catheter (Haemodialysis Catheter) Going Home with a Haemodialysis Catheter? Important facts you must know. Haemodialysis Treatment 29/07/2018 Page 1 In order to
NURSING POLICIES, PROCEDURES & PROTOCOLS
 Page 1 of 10 NURSING POLICIES, PROCEDURES & PROTOCOLS CENTRAL VENOUS ACCESS DEVICE (CVAD) HEMODIALYSIS CATHETERS: DRESSING CHANGE, INITIATING OR DISCONTINUING AN INFUSION NO.: 00056 (Formerly NSG2146)
Page 1 of 10 NURSING POLICIES, PROCEDURES & PROTOCOLS CENTRAL VENOUS ACCESS DEVICE (CVAD) HEMODIALYSIS CATHETERS: DRESSING CHANGE, INITIATING OR DISCONTINUING AN INFUSION NO.: 00056 (Formerly NSG2146)
Peripherally Inserted Central Catheter (PICC)
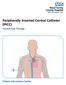 Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Insertion of a Hickman Line Information for parents and carers
 Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Newborn Hearing Screening Programme Policy
 Newborn Hearing Screening Programme Policy V3.0 December 2015 Page 1 of 16 Summary - Screening Pathway for Newborn Hearing Screening Newborn hearing screening Check eligibility Eligible for screening Not
Newborn Hearing Screening Programme Policy V3.0 December 2015 Page 1 of 16 Summary - Screening Pathway for Newborn Hearing Screening Newborn hearing screening Check eligibility Eligible for screening Not
Skin Tunnelled Catheter (STC), also known as Central line
 Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients
 Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients page 2 What is a peripherally inserted central catheter (PICC)? A PICC is a narrow, hollow tube
Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients page 2 What is a peripherally inserted central catheter (PICC)? A PICC is a narrow, hollow tube
MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa
 MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling
MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling
Safeguarding Children Supervision Policy V4.0. November 2016
 Safeguarding Children Supervision Policy V4.0 November 2016 Page 1 of 20 Summary Part 1 Part 2 Safeguarding supervision for Nursing and Midwifery staff, Paediatricians, Medical Staff and other Allied Health
Safeguarding Children Supervision Policy V4.0 November 2016 Page 1 of 20 Summary Part 1 Part 2 Safeguarding supervision for Nursing and Midwifery staff, Paediatricians, Medical Staff and other Allied Health
Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients
 Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients What is a tunnelled central venous catheter (CVC)? A CVC is a long, narrow tube (catheter) that is put
Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients What is a tunnelled central venous catheter (CVC)? A CVC is a long, narrow tube (catheter) that is put
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa
 CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling Vascular Access
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling Vascular Access
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Vascuport in Children for Routine Flushing and Administration of Medication
 Standard Operating Procedure 6 (SOP 6) Vascuport in Children for Routine Flushing and Administration of Medication Why we have a procedure? This guidance is to assist/ inform healthcare professionals on
Standard Operating Procedure 6 (SOP 6) Vascuport in Children for Routine Flushing and Administration of Medication Why we have a procedure? This guidance is to assist/ inform healthcare professionals on
Peripherally Inserted Central Catheter
 UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure
 Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Quality and Standards Group Date
Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Quality and Standards Group Date
Home Intravenous Therapy Team - PICC and Midline. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - PICC and Midline An information guide Home Intravenous Therapy Team - PICC and Midline What is intravenous
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - PICC and Midline An information guide Home Intravenous Therapy Team - PICC and Midline What is intravenous
CLINICAL GUIDELINE FOR MAXIMUM SURGICAL BLOOD ORDER SCHEDULE (MSBOS) Summary.
 CLINICAL GUIDELINE FOR MAXIMUM SURGICAL BLOOD ORDER SCHEDULE (MSBOS) Summary. Start Elective procedure identified, blood requirement listed in guideline Patient attends PAC and has a group and screen (G&S)
CLINICAL GUIDELINE FOR MAXIMUM SURGICAL BLOOD ORDER SCHEDULE (MSBOS) Summary. Start Elective procedure identified, blood requirement listed in guideline Patient attends PAC and has a group and screen (G&S)
RN Entry Level Competency
 Policies & Procedures Title: CENTRAL VENOUS CATHETERS BLOOD WITHDRAWAL (, SHORT TERM, TUNNELED, IMPLANTED) LPN Additional Competency (LPNAC) Central Venous Catheters - Blood Withdrawal from with an Established
Policies & Procedures Title: CENTRAL VENOUS CATHETERS BLOOD WITHDRAWAL (, SHORT TERM, TUNNELED, IMPLANTED) LPN Additional Competency (LPNAC) Central Venous Catheters - Blood Withdrawal from with an Established
1. Nurses may remove non-tunneled catheters upon the order of a physician. Physicians remove tunneled catheters.
 Removal of Non-Tunneled Central Venous Catheter (CVC) (Approved Aug 15, 2011/Rev Dec 16, 2011/Rev Jun 13, 2012) Vascular Access Guideline Table of Contents This procedure is posted on the BC Provincial
Removal of Non-Tunneled Central Venous Catheter (CVC) (Approved Aug 15, 2011/Rev Dec 16, 2011/Rev Jun 13, 2012) Vascular Access Guideline Table of Contents This procedure is posted on the BC Provincial
Diagnostic Testing Procedures for Ophthalmic Science
 V4.0 01/08/17 Table of Contents 1. Introduction... 3 2. Purpose of this Policy... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 3 5.2. Role of the Managers... 3 5.3.
V4.0 01/08/17 Table of Contents 1. Introduction... 3 2. Purpose of this Policy... 3 3. Scope... 3 4. Definitions / Glossary... 3 5. Ownership and Responsibilities... 3 5.2. Role of the Managers... 3 5.3.
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
Know about your tunnelled Central Venous Catheter (CVC)
 Know about your tunnelled Central Venous Catheter (CVC) Information for patients and families Read this resource to learn: What a tunnelled CVC is What to expect when getting your tunnelled CVC How to
Know about your tunnelled Central Venous Catheter (CVC) Information for patients and families Read this resource to learn: What a tunnelled CVC is What to expect when getting your tunnelled CVC How to
Aseptic Technique Policy
 Post holder responsible for Policy Author of Policy Division/ Department responsible for Procedural Document Contact details Judy Potter, Lead Nurse/Director Infection Prevention& Control Judy Potter,
Post holder responsible for Policy Author of Policy Division/ Department responsible for Procedural Document Contact details Judy Potter, Lead Nurse/Director Infection Prevention& Control Judy Potter,
Peripherally Inserted Central Catheter (PICC Line)
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
CENTRAL VENOUS LINES: REMOVAL
 [Type text] KINGSTON HEALTH SCIENCES CENTRE Kingston General Hospital site CENTRAL VENOUS LINES: REMOVAL LEARNING GUIDE FOR REGISTERED NURSES Prepared by: Nursing Education Services Date: 1993 December
[Type text] KINGSTON HEALTH SCIENCES CENTRE Kingston General Hospital site CENTRAL VENOUS LINES: REMOVAL LEARNING GUIDE FOR REGISTERED NURSES Prepared by: Nursing Education Services Date: 1993 December
Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line
 Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line Department of Radiology Information for Patients i Radiology Leaflet No. 85 University Hospitals of Leicester NHS Trust Referral
Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line Department of Radiology Information for Patients i Radiology Leaflet No. 85 University Hospitals of Leicester NHS Trust Referral
Section G - Aseptic Technique. Version 5
 Section G - Aseptic Technique Version 5 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you must
Section G - Aseptic Technique Version 5 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you must
HHVNA Infusion Therapy MIDLINE CATHETER
 CONSIDERATIONS: 1. This midline procedure includes procedural steps for: a. Catheter Insertion b. Flushing c. Site care and dressing change d. Cap change e. Blood Draw f. Management of complications 2.
CONSIDERATIONS: 1. This midline procedure includes procedural steps for: a. Catheter Insertion b. Flushing c. Site care and dressing change d. Cap change e. Blood Draw f. Management of complications 2.
All about Your Implanted Venous Access Device (IVAD, Port )
 All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy
 Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy (Note: See Separate Policy for Port-a-Cath Care and Management) DOCUMENT CONTROL: Version: v2 Ratified by: Quality
Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy (Note: See Separate Policy for Port-a-Cath Care and Management) DOCUMENT CONTROL: Version: v2 Ratified by: Quality
Limitations and Guidelines Revised for Elastomeric Devices and IV Supplies and Equipment
 Limitations and Guidelines Revised for Elastomeric Devices and IV Supplies and Equipment Information posted January 8, 2007 Effective for dates of service on or after March 1, 2007, benefit limitations
Limitations and Guidelines Revised for Elastomeric Devices and IV Supplies and Equipment Information posted January 8, 2007 Effective for dates of service on or after March 1, 2007, benefit limitations
Policy for the Care of Patients with Central Venous Catheters (CVC)
 Policy Type: Definition: Owner Group: Clinical Policy Operations Cli nic al G u ide lin e Clinical Policy Policy for the Care of Patients with Central Venous Catheters (CVC) Applicable To: Communication
Policy Type: Definition: Owner Group: Clinical Policy Operations Cli nic al G u ide lin e Clinical Policy Policy for the Care of Patients with Central Venous Catheters (CVC) Applicable To: Communication
CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES
 CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES Lauren E.B. Stone, MSN, RN, VA-BC Nurse Manager IV Team and Blood Donor Center Boston Children's Hospital
CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES Lauren E.B. Stone, MSN, RN, VA-BC Nurse Manager IV Team and Blood Donor Center Boston Children's Hospital
Medication Administration Using the Home Pump (Eclipse)
 Medication Administration Using the Home Pump (Eclipse) Phone Number: Nurse/Contact: Receiving IV Therapy in the Home Your doctor has ordered for you to receive your IV medication at home. Receiving IV
Medication Administration Using the Home Pump (Eclipse) Phone Number: Nurse/Contact: Receiving IV Therapy in the Home Your doctor has ordered for you to receive your IV medication at home. Receiving IV
21 st Century Health Care Consultants
 21 st Century Health Care Consultants Presents 1 Investing in your Infusion Specialty Program Presented by: Rhonda Surgnier RN Becky Tolson RN David Kachel CRNI INFUSION THERAPY OBJECTIVES 2 At the completion
21 st Century Health Care Consultants Presents 1 Investing in your Infusion Specialty Program Presented by: Rhonda Surgnier RN Becky Tolson RN David Kachel CRNI INFUSION THERAPY OBJECTIVES 2 At the completion
SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY
 PS1006 SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY TITLE: INFECTION PREVENTION FOR INTRAVASCULAR Job Title of Responsible Owner: Executive Director, Quality POLICY #: EFFECTIVE DATE: REVIEWED/REVISED
PS1006 SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY TITLE: INFECTION PREVENTION FOR INTRAVASCULAR Job Title of Responsible Owner: Executive Director, Quality POLICY #: EFFECTIVE DATE: REVIEWED/REVISED
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Injectable Medicines Policy
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Injectable Medicines Policy Version No.: 4.3 Effective From: 24 March 2017 Expiry Date: 21 January 2019 Date Ratified: 11 January 2017 Ratified By:
The Newcastle upon Tyne Hospitals NHS Foundation Trust Injectable Medicines Policy Version No.: 4.3 Effective From: 24 March 2017 Expiry Date: 21 January 2019 Date Ratified: 11 January 2017 Ratified By:
patientinformation Peripherally inserted central catheter (PICC) Vascular Access The Rotherham NHS Foundation Trust
 The Rotherham NHS Foundation Trust Peripherally inserted central catheter (PICC) Vascular Access patientinformation Your health, your life, your choice, our passion Bring your medicines when you come into
The Rotherham NHS Foundation Trust Peripherally inserted central catheter (PICC) Vascular Access patientinformation Your health, your life, your choice, our passion Bring your medicines when you come into
Hand Hygiene Policy V2.1
 V2.1 October 2017 Summary. Effective hand hygiene is shown to significantly reduce the carriage of potential pathogens and decrease the risk and occurrence of healthcare associated infections. Each individual
V2.1 October 2017 Summary. Effective hand hygiene is shown to significantly reduce the carriage of potential pathogens and decrease the risk and occurrence of healthcare associated infections. Each individual
Patient Experience Strategy
 POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
Information for Patients
 Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
Health and Safety Policy and Guidance for Staff Working During Night Time Hours V2.0
 Health and Safety Policy and Guidance for Staff Working During Night Time Hours V2.0 January 2016 Summary Purpose of the document: The purpose of this policy is to provide an outline of the requirements
Health and Safety Policy and Guidance for Staff Working During Night Time Hours V2.0 January 2016 Summary Purpose of the document: The purpose of this policy is to provide an outline of the requirements
STANDARDIZED PROCEDURE HEPATIC ARTERY INFUSION OF CHEMOTHERAPY (Adults, Peds)
 I. Definition Hepatic arterial infusion (HAI) of chemotherapy is accomplished by a small drug delivery system or pump that is implanted in a subcutaneous pocket in the lower abdomen. The pump reservoir
I. Definition Hepatic arterial infusion (HAI) of chemotherapy is accomplished by a small drug delivery system or pump that is implanted in a subcutaneous pocket in the lower abdomen. The pump reservoir
Midline. Intravenous Therapy. Patient information leaflet
 Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS ACCESS DEVICE PORTS FOR ADULTS
 PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS FOR ADULTS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To ensure a safe and effective procedure for the
PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS FOR ADULTS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To ensure a safe and effective procedure for the
