Hickman line insertion and caring for your line
|
|
|
- Melvin Terry
- 5 years ago
- Views:
Transcription
1 Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your line. If you have any more questions, please do not hesitate to speak to the nurses or doctors caring for you. Confirming your identity Before you have a treatment or procedure, our staff will ask you your name and date of birth and check your ID band. If you don t have an ID band we will also ask you to confirm your address. If we don t ask these questions, then please ask us to check. Ensuring your safety is our primary concern.
2 What is a Hickman line? It is a long, thin silicone tube that is tunnelled under your skin and into a large vein in your chest. You have this procedure under local anaesthetic. You can go home with it in and it can be left in place for weeks or months while you are having your treatment. The line has two or three separate openings called lumen. These allow you to be given different treatments at the same time. Each lumen is clamped with a clip midway along the line and then sealed with a needle-free device, a cap, a connector or a bung, to keep your line closed when it is not being used (see diagram on the right/above/below). There is a small cuff around the Hickman line. You can feel this under your skin, just above the area where it leaves your body (exit site). The cuff stops your line from falling out. It takes about three weeks for the tissue under your skin to grow around this cuff and hold your line in place. You may also hear a Hickman line called a central line, a tunnelled line or a central venous access device. Why do I need a Hickman line? It is used to give medicines and treatments such as blood transfusions, chemotherapy and stem cells safely and reliably directly into your vein. It can also be used to take blood samples. 2
3 What are the benefits of having a Hickman line? You do not need to keep on having needles put in every time you have treatment. It can be very useful if doctors and nurses find it difficult to put a needle into your veins, or if the walls of your veins have been hardened by previous chemotherapy treatment. What are the risks when having it put it in? Pneumothorax: this happens when your lung is accidentally punctured, allowing air to get between your lung and chest wall. It is very rare (1:1,000 risk). The doctor putting in your line will be able to see if this has happened using real-time x-rays. Sometimes, only a small amount of air gets in, so your body can take care of it on its own and you do not need to be admitted to hospital. But if there is more air, you will have to be admitted to hospital to have it taken out. Bleeding: you may have a small amount of blood oozing out where the line is put in and/or comes out. What are the risks after it has been put in? Although most patients do not have any problems with their Hickman line, it is important that you know the potential risks. Loose or disconnected needle-free device: this can cause air to move into the line. If the device is loose, tighten it. If it has come off or is missing, check the line is still clamped and go to your local Haematology outpatient department (out of hours, go to your nearest Accident and Emergency) to get the device replaced. Cough, chest pain, shortness of breath and/or throat irritation within hours of having your line put in: if you have any of these, check that all the lumens are clamped and the needle freedevices are in place and go to your local Haematology outpatient 3
4 department (out of hours, go to your nearest Accident and Emergency) to get the line checked. Thrombosis (blood clot): as the Hickman line is in one of your veins, there is a risk you can develop a blood clot. Symptoms include: swelling around your line swelling/discomfort in the arm, hand and neck on the side of your Hickman line blocked line. If you have a blood clot, your line may be taken out and you will be given medication to help break it down. Bruising, pain and/or discomfort: it is common to have some bruising, pain and/or discomfort where the line tunnels under the skin for a few days after its insertion. You can take a mild painkiller such as paracetamol to ease this. Bleeding: many people have a small amount of bleeding after the line has been put in. This should stop after a few hours. Severe bleeding is very rare. If you are taking any medications that can affect the way your blood clots, or you have a history of abnormal bleeding, you must let us know before the day of the procedure (see What happens before the procedure, page 6. Infection: you can develop an infection either inside the Hickman line lumens or around the area where the line leaves your body (exit site). Your immune system may be weakened due to your illness or chemotherapy treatment and this makes you more likely to develop an infection. You must seek medical help straight away if you have any of the following symptoms: 4
5 redness, oozing and/or soreness around the exit site hot flushes or shivering before or after your line has been accessed/used for treatment temperature above 38ºC. A small round dressing that is impregnated with an antiseptic solution ( called a biopatch) will be applied at the line exit site to help minimise the risk of infection here. Lumen problems: one or more of the lumens of your line can become blocked. To stop this from happening, they need to be flushed with saline (salt solution) regularly and promptly when you have finished an infusion. Are there any alternatives? Having a needle put in to a vein in your arm or hand every time you have treatment. Having another type of central venous access device put in, such as a PICC line, which has similar benefits and risks to a Hickman Line. But a PICC line has only two lumens and you may need three to have your treatment, which is why your doctors have asked you to have a Hickman line put in. Please ask your doctor or nurse for more information about these alternatives Consent We must by law obtain your written consent to any operation and some other procedures beforehand. Staff will explain the risks, benefits and alternatives before they ask you to sign a consent form. If you are unsure of any aspect of the treatment proposed, please do not hesitate to speak with a senior member of the staff again. 5
6 How a Hickman line is put in What happens before the procedure? Blood clotting medications: if you are taking any medications that affect how your blood clots, or you have a history of abnormal bleeding, please tell your doctor or clinical nurse specialist when they confirm the date of your procedure. They may ask you to stop taking these for a short while before you have the line put in. Preventing infection: we will give you an antibacterial liquid called Hibiscrub that you need to wash with instead of soap or shower gel the night before and on the morning of the procedure. This is an important step in reducing the risk of infection. Your procedure will be cancelled if you have not completed this step. Eating and drinking: you can eat and drink normally before having the line put in you do not need to fast. Where will I have the procedure? If you are having this as an outpatient procedure, please come to the Supportive Therapy Unit on the ground floor of the Cheyne Wing. You will then be taken to the Interventional Radiology (IR) department to have the line put in. This is because x-rays and ultrasound imaging are used to place your line in exactly the right place. If you are an inpatient, you will be taken to the IR department to have your line put in. What happens during the procedure? The line will be put in by a specialist doctor called a radiologist. Before the procedure, they will explain the risks and benefits of the procedure and ask for your consent. 6
7 If you agree to go ahead with the procedure, a nurse will take you to the IR theatre and ask you to lie on the x-ray table. They will connect you to monitoring equipment and check your pulse and blood pressure during the procedure. There will also be a radiographer in the theatre to control the x-ray imaging. The doctor will find a suitable vein in your neck, near your collarbone, using an ultrasound machine. They will then use antiseptic to clean the area of skin where your line is going to be put in and cover you with a sterile cloth which partly covers your face. Next they will inject local anaesthetic into your neck and chest area. This may sting a little as it goes in. After this, the area will be numb and you should feel only pressure, not pain. If you do feel any discomfort during the procedure, tell the doctor as they can give you more local anaesthetic. The doctor will make a small cut in the skin in your neck. This is the insertion site. Using ultrasound images, they will gently guide the tip of the line into a large vein (jugular), towards your heart. Next they will tunnel the other end of the line under the skin of your chest. The line then reaches the exit site, where it comes out of your body, so you will also have a small cut here, too. The diagram above shows the position of the central line. 7
8 The doctor will close the small cuts in your neck and chest with stitches and cover them with dressings. How long does the procedure take? The procedure usually takes about 30 minutes. What happens after the procedure? After the procedure, you will be taken back to the Supportive Therapy Unit or back to your ward bed. If the procedure is being done as a day case, you can go home later that day after xx hours of observation in Supportive Therapy. Before you leave hospital a nurse will check your Hickman line and put on new dressings, if needed. They will also book an appointment for the next day to have your dressing changed and your line flushed. The stitches in your neck are taken out after 7 10 days and those in your chest are taken out after 21 days. Looking after your Hickman line On the day you have it put in After your procedure you will return to the Supportive Therapy Unit for about 2 hours of observation prior to discharge home. Your nurse will arrange a further appointment for the following day to have your dressing changed and Hickman line flushed. Every week You will attend either King s or your local Haematology outpatients at least once a week to have your Hickman line cleaned and dressing changed, and to have new needle-free devices attached and flushed. This makes you less likely to get an infection and makes sure the line does not become blocked. 8
9 The bung on each of the lumens on your Hickman line is also changed once a week at the same time as the dressing. If your line is not being used regularly, a weak solution of heparin will be injected into all the lumens to help stop the line becoming blocked. How to minimise the risk of infection Take your temperature every evening, or at other times if you feel unwell. If it is above 38ºC you must seek medical help as soon as possible (see Infection, page 4). Shower or wash daily, making sure you keep the area where the line has been put in and the line itself dry. Do not touch or play with your Hickman line. Make sure your line is cleaned and the dressing changed each week. What should I do if I have a problem with the dressing? If you get a rash, or have blistering, itching or redness under the dressing, tell your doctor or nurse. They can put on a different type of dressing. What should I do if the line falls out? It is rare for a line to fall out because it is held in place by a cuff under your skin. If it does happen, you should: Lie or sit down and quickly press on the site using a clean towel/ tissues Contact your local Haematology outpatient department or go to your nearest Accident and Emergency straight away. How do I wash? You can shower and have shallow baths but you must keep the area where the line has been put in and the line itself dry. Your dressings are splash-proof but do not get them wet or soak 9
10 them. If you do, you need to get a new one put on at your local haematology outpatient department. Can I exercise with a Hickman line? Avoid strenuous exercise such as running or tennis because this can cause your Hickman line to come out. You must not swim because you must not immerse your Hickman line in water. Gentle exercise such as walking is ideal. When and how will my Hickman line taken out? How long you have your Hickman line depends on your individual needs. It will be taken out if: You no longer need it It becomes infected It becomes blocked or damaged. It is usually taken out and the entry and exit sites stitched in the Haematology outpatient department by one of the Haematology doctors. You will have an appointment to have the stitches removed seven 10 days later. Who can I contact with queries and concerns? Haematology outpatient department, Monday to Friday, 8am 8pm (not bank holidays) Tel: or Haematology registrar, out of hours Tel: main switchboard, , and ask for the on-call haematology registrar. 10
11 Sharing your information We have teamed up with Guy s and St Thomas Hospitals in a partnership known as King s Health Partners Academic Health Sciences Centre. We are working together to give our patients the best possible care, so you might find we invite you for appointments at Guy s or St Thomas. To make sure everyone you meet always has the most up-to-date information about your health, we may share information about you between the hospitals. Care provided by students We provide clinical training where our students get practical experience by treating patients. Please tell your doctor or nurse if you do not want students to be involved in your care. Your treatment will not be affected by your decision. PALS The Patient Advice and Liaison Service (PALS) offers support, information and assistance to patients, relatives and visitors. They can also provide help and advice if you have a concern or complaint that staff have not been able to resolve for you. The PALS office is located on the ground floor of the Hambleden Wing, near the main entrance on Bessemer Road - staff will be happy to direct you. PALS at King s College Hospital, Denmark Hill, London SE5 9RS Tel: kch-tr.pals@nhs.net You can also contact us by using our online form at If you would like the information in this leaflet in a different language or format, please contact PALS on
12 PL798.1 November 2017 Networked Care Review date November 2020 Corporate Comms: 1740
Hickman line insertion in the interventional radiology department
 Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Skin Tunnelled Catheter (STC), also known as Central line
 Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Cheekbone (isolated zygomatic arch) fracture surgery
 Ambulatory Care & Local Networks Cheekbone (isolated zygomatic arch) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone. This
Ambulatory Care & Local Networks Cheekbone (isolated zygomatic arch) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone. This
Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients
 Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients What is a tunnelled central venous catheter (CVC)? A CVC is a long, narrow tube (catheter) that is put
Vascular Access Department Insertion of a tunnelled Central Venous Catheter Information for patients What is a tunnelled central venous catheter (CVC)? A CVC is a long, narrow tube (catheter) that is put
Having a portacath insertion in the x-ray department
 Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Insertion of a Hickman Line Information for parents and carers
 Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Care of Your Peripherally Inserted Central Catheter
 Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Peripherally Inserted Central Catheter (PICC)
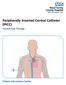 Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients
 Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients page 2 What is a peripherally inserted central catheter (PICC)? A PICC is a narrow, hollow tube
Vascular Access Department Insertion of a peripherally inserted central catheter Information for patients page 2 What is a peripherally inserted central catheter (PICC)? A PICC is a narrow, hollow tube
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath
 You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
Haemorrhoidectomy. Information for day surgery patients
 Haemorrhoidectomy Information for day surgery patients This booklet explains haemorrhoids, the symptoms and why a procedure is undertaken. An explanation of the benefits, alternatives, consent and the
Haemorrhoidectomy Information for day surgery patients This booklet explains haemorrhoids, the symptoms and why a procedure is undertaken. An explanation of the benefits, alternatives, consent and the
Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line
 Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line Department of Radiology Information for Patients i Radiology Leaflet No. 85 University Hospitals of Leicester NHS Trust Referral
Insertion of a PICC (Peripherally Inserted Central Catheter) / Mid Line Department of Radiology Information for Patients i Radiology Leaflet No. 85 University Hospitals of Leicester NHS Trust Referral
About your PICC line. Information for patients Weston Park Hospital
 About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
Laparoscopic cholecystectomy
 Laparoscopic cholecystectomy Information for day surgery patients at King s College Hospital only This leaflet answers some of the questions you may have about having a laparoscopic cholecystectomy. It
Laparoscopic cholecystectomy Information for day surgery patients at King s College Hospital only This leaflet answers some of the questions you may have about having a laparoscopic cholecystectomy. It
Peripherally Inserted Central Catheter (PICC Line)
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Peripherally inserted central catheter (PICC line) Information to accompany consent
 Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
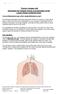 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Peripherally Inserted Central Catheter (PICC)
 University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
Chest Drain Insertion
 Chest Drain Insertion Information for Patients What is a chest drain? The insertion of a chest drain is a sterile procedure that involves placing a small drain through your skin into the space between
Chest Drain Insertion Information for Patients What is a chest drain? The insertion of a chest drain is a sterile procedure that involves placing a small drain through your skin into the space between
Inferior Vena Cava (IVC) Filter Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Home Intravenous Therapy Team - PICC and Midline. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - PICC and Midline An information guide Home Intravenous Therapy Team - PICC and Midline What is intravenous
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - PICC and Midline An information guide Home Intravenous Therapy Team - PICC and Midline What is intravenous
Midline. Intravenous Therapy. Patient information leaflet
 Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
Having an Oesophageal Dilatation
 Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Peripherally Inserted Central Catheter
 UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
Mediastinal Venogram and Stent Insertion
 Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Information for Patients
 Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
About your peritoneal dialysis catheter. Information for patients Sheffield Kidney Institute (Renal Unit)
 About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
Information for Patients Central Venous Catheter (Haemodialysis Catheter)
 Information for Patients Central Venous Catheter (Haemodialysis Catheter) Going Home with a Haemodialysis Catheter? Important facts you must know. Haemodialysis Treatment 29/07/2018 Page 1 In order to
Information for Patients Central Venous Catheter (Haemodialysis Catheter) Going Home with a Haemodialysis Catheter? Important facts you must know. Haemodialysis Treatment 29/07/2018 Page 1 In order to
Know about your tunnelled Central Venous Catheter (CVC)
 Know about your tunnelled Central Venous Catheter (CVC) Information for patients and families Read this resource to learn: What a tunnelled CVC is What to expect when getting your tunnelled CVC How to
Know about your tunnelled Central Venous Catheter (CVC) Information for patients and families Read this resource to learn: What a tunnelled CVC is What to expect when getting your tunnelled CVC How to
All about Your Implanted Venous Access Device (IVAD, Port )
 All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
Bone marrow aspiration and biopsy
 Bone marrow aspiration and biopsy Haematology Oncology Team Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called bone marrow aspiration and a biopsy. It
Bone marrow aspiration and biopsy Haematology Oncology Team Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called bone marrow aspiration and a biopsy. It
Pleural procedures and thoracic ultrasound British Thoracic Society Pleural Disease Guideline 2010
 Pleural procedures and thoracic ultrasound British Thoracic Society Pleural Disease Guideline 2010 Tom Havelock, Richard Teoh, Diane Laws, Fergus Gleeson On behalf of the BTS Pleural Disease Guideline
Pleural procedures and thoracic ultrasound British Thoracic Society Pleural Disease Guideline 2010 Tom Havelock, Richard Teoh, Diane Laws, Fergus Gleeson On behalf of the BTS Pleural Disease Guideline
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
National Hospital for Neurology and Neurosurgery. About plasma exchange Plasma Exchange Service
 National Hospital for Neurology and Neurosurgery About plasma exchange Plasma Exchange Service If you would like this document in another language or format, or require the services of an interpreter,
National Hospital for Neurology and Neurosurgery About plasma exchange Plasma Exchange Service If you would like this document in another language or format, or require the services of an interpreter,
patientinformation Peripherally inserted central catheter (PICC) Vascular Access The Rotherham NHS Foundation Trust
 The Rotherham NHS Foundation Trust Peripherally inserted central catheter (PICC) Vascular Access patientinformation Your health, your life, your choice, our passion Bring your medicines when you come into
The Rotherham NHS Foundation Trust Peripherally inserted central catheter (PICC) Vascular Access patientinformation Your health, your life, your choice, our passion Bring your medicines when you come into
Venous Sampling. Information for patients
 Venous Sampling Information for patients What is Venous Sampling? What is Venous Sampling? Venous sampling is a procedure that involves inserting a catheter (thin tube) into a specific vein or veins, taking
Venous Sampling Information for patients What is Venous Sampling? What is Venous Sampling? Venous sampling is a procedure that involves inserting a catheter (thin tube) into a specific vein or veins, taking
Tenckhoff Catheter Insertion
 Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
HOW TO CARE FOR YOUR DIALYSIS CATHETER
 RENAL PATIENT INFORMATION HOW TO CARE FOR YOUR DIALYSIS CATHETER Advice for patients with a dialysis tunnelled catheter How to care for your dialysis line What is a haemodialysis line? A dialysis line
RENAL PATIENT INFORMATION HOW TO CARE FOR YOUR DIALYSIS CATHETER Advice for patients with a dialysis tunnelled catheter How to care for your dialysis line What is a haemodialysis line? A dialysis line
Haemodialysis service
 Liver, Renal & Surgery Haemodialysis service Information for patients attending King s College Hospital main and satellite haemodialysis units Welcome to the King s haemodialysis service. This booklet
Liver, Renal & Surgery Haemodialysis service Information for patients attending King s College Hospital main and satellite haemodialysis units Welcome to the King s haemodialysis service. This booklet
UW MEDICINE PATIENT EDUCATION. Angiography: Percutaneous or Transjugular Liver Biopsy. How to prepare and what to expect. What is a liver biopsy?
 UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology
 Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology Your healthcare team recommended that you undergo gastrojejunostomy tube (GJ tube) placement. This procedure will be
Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology Your healthcare team recommended that you undergo gastrojejunostomy tube (GJ tube) placement. This procedure will be
Home Intravenous Therapy HOPT (Home / Outpatient Parenteral Therapy)
 Home Intravenous Therapy HOPT (Home / Outpatient Parenteral Therapy) Intermediate Care 0161 206 7017 All Rights Reserved 2017. Document for issue as handout. This booklet has been given to you because
Home Intravenous Therapy HOPT (Home / Outpatient Parenteral Therapy) Intermediate Care 0161 206 7017 All Rights Reserved 2017. Document for issue as handout. This booklet has been given to you because
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your doctor has recommended you have
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your doctor has recommended you have
UW MEDICINE PATIENT EDUCATION. Right Heart Catheterization. How to prepare and what to expect DRAFT. Your Appointment
 UW MEDICINE PATIENT EDUCATION Right Heart Catheterization How to prepare and what to expect This handout explains how to prepare and what to expect when you are scheduled for a right heart catheterization
UW MEDICINE PATIENT EDUCATION Right Heart Catheterization How to prepare and what to expect This handout explains how to prepare and what to expect when you are scheduled for a right heart catheterization
Department of Colorectal Surgery Pilonidal Sinus Operation
 What is a pilonidal sinus? Department of Colorectal Surgery Pilonidal Sinus Operation A pilonidal sinus is an inflamed sinus tract (or tracts, as there can be more than one) which leads to a cavity under
What is a pilonidal sinus? Department of Colorectal Surgery Pilonidal Sinus Operation A pilonidal sinus is an inflamed sinus tract (or tracts, as there can be more than one) which leads to a cavity under
Treatment of non-muscle invasive bladder cancer with BCG and EMDA MMC
 Treatment of non-muscle invasive bladder cancer with BCG and EMDA MMC This information sheet has been given to you to explain the combined use of BCG and EMDA MMC to treat your non-muscle invasive bladder
Treatment of non-muscle invasive bladder cancer with BCG and EMDA MMC This information sheet has been given to you to explain the combined use of BCG and EMDA MMC to treat your non-muscle invasive bladder
Inferior Vena Cava (IVC) Filter Retrieval with the Endovascular Laser Sheath
 If you have any questions, ask your doctor or nurse. Inferior Vena Cava (IVC) Filter Retrieval with the Endovascular Laser Sheath The inferior vena cava (IVC) is a large vein in your abdomen that brings
If you have any questions, ask your doctor or nurse. Inferior Vena Cava (IVC) Filter Retrieval with the Endovascular Laser Sheath The inferior vena cava (IVC) is a large vein in your abdomen that brings
Dacryocystorhinostomy (DCR)
 Dacryocystorhinostomy (DCR) This leaflet explains about dacryocystorhinostomy (DCR) including the benefits, risks and any alternatives, together with what you can expect when you come to hospital. If you
Dacryocystorhinostomy (DCR) This leaflet explains about dacryocystorhinostomy (DCR) including the benefits, risks and any alternatives, together with what you can expect when you come to hospital. If you
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
University College London Hospital. Stereotactic Vacuum Assisted Biopsy (VAB) of the Breast. Imaging Department
 University College London Hospital Stereotactic Vacuum Assisted Biopsy (VAB) of the Breast Imaging Department If you would like this document in another language or format, or require the services of an
University College London Hospital Stereotactic Vacuum Assisted Biopsy (VAB) of the Breast Imaging Department If you would like this document in another language or format, or require the services of an
Totally Implantable Venous Access Devices (port) Information for patients. Cross section of a port
 Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
Morton s neuroma. If you have any further questions, please speak to a doctor or nurse caring for you.
 Morton s neuroma This leaflet aims to answer your questions about having surgery for Morton s neuroma. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Morton s neuroma This leaflet aims to answer your questions about having surgery for Morton s neuroma. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Emergency Department (ED)
 Emergency Department (ED) Information for patients This leaflet explains how the Emergency Department (ED) works and what to expect when you come in. Confirming your identity Before you have a treatment
Emergency Department (ED) Information for patients This leaflet explains how the Emergency Department (ED) works and what to expect when you come in. Confirming your identity Before you have a treatment
Bimaxillary surgery: before and after your operation
 Ambulatory Care & Local Networks Bimaxillary surgery: before and after your operation Information for patients This leaflet explains what happens before and after surgery to reset both jaw bones (bimaxillary
Ambulatory Care & Local Networks Bimaxillary surgery: before and after your operation Information for patients This leaflet explains what happens before and after surgery to reset both jaw bones (bimaxillary
Complaints procedure.
 Complaints procedure This leaflet explains what to do if you have a complaint about any aspect of our service. We treat all complaints seriously and aim to resolve them as quickly and fully as we can.
Complaints procedure This leaflet explains what to do if you have a complaint about any aspect of our service. We treat all complaints seriously and aim to resolve them as quickly and fully as we can.
Your child s minor operation under a general anaesthetic. Information for parents and carers
 Your child s minor operation under a general anaesthetic Information for parents and carers The problem that is being treated:... Your child s doctor will discuss your child s condition with you and why
Your child s minor operation under a general anaesthetic Information for parents and carers The problem that is being treated:... Your child s doctor will discuss your child s condition with you and why
Local Anaesthesia for your eye operation. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Local Anaesthesia for your eye operation An information guide Local Anaesthesia for your eye operation Introduction You and your doctor
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Local Anaesthesia for your eye operation An information guide Local Anaesthesia for your eye operation Introduction You and your doctor
Heart Rhythm Program, St. Paul s Hospital Lead Extraction
 Heart Rhythm Program, St. Paul s Hospital Lead Extraction FD.723.P114.PHC (R.Feb-18) What is a lead? A cardiac lead is a special wire that sends energy from a pacemaker or implantable cardioverter defibrillator
Heart Rhythm Program, St. Paul s Hospital Lead Extraction FD.723.P114.PHC (R.Feb-18) What is a lead? A cardiac lead is a special wire that sends energy from a pacemaker or implantable cardioverter defibrillator
Vertebroplasty. Exceptional healthcare, personally delivered
 Vertebroplasty Exceptional healthcare, personally delivered Your Doctor has requested that you have a vertebroplasty. We hope the following information will answer some of the questions you may have about
Vertebroplasty Exceptional healthcare, personally delivered Your Doctor has requested that you have a vertebroplasty. We hope the following information will answer some of the questions you may have about
Transjugular Liver Biopsy About your procedure
 Patient Education Transjugular Liver Biopsy About your procedure This handout explains what a transjugular liver biopsy is and what to expect when you have this procedure. What is a liver biopsy? In a
Patient Education Transjugular Liver Biopsy About your procedure This handout explains what a transjugular liver biopsy is and what to expect when you have this procedure. What is a liver biopsy? In a
Contents. Welcome to the Cath Lab P4/5
 Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Laparoscopic Radical Nephrectomy
 Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
UW MEDICINE PATIENT EDUCATION. How to prepare and what to expect DRAFT. What is an IVC filter?
 UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
Diagnostic shoulder arthroscopy
 Diagnostic shoulder arthroscopy The aim of this leaflet is to help answer some of the questions you may have about having a diagnostic shoulder arthroscopy. It explains the benefits, risks and alternatives
Diagnostic shoulder arthroscopy The aim of this leaflet is to help answer some of the questions you may have about having a diagnostic shoulder arthroscopy. It explains the benefits, risks and alternatives
Having a Vena Cava Filter
 Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
ICD and CRT-D Generator Replacement. Information for patients
 ICD and CRT-D Generator Replacement Information for patients Your doctor has recommended that your ICD or CRT-D generator needs to be replaced, in order to keep your ICD or CRT-D working. What happens
ICD and CRT-D Generator Replacement Information for patients Your doctor has recommended that your ICD or CRT-D generator needs to be replaced, in order to keep your ICD or CRT-D working. What happens
Recovering from a hip fracture following an accident
 South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
Going home with a redivac drain after surgery
 Going home with a redivac drain after surgery This leaflet explains about going home with a redivac drain following your surgery. If you have any further questions, please speak to the nurse or doctor
Going home with a redivac drain after surgery This leaflet explains about going home with a redivac drain following your surgery. If you have any further questions, please speak to the nurse or doctor
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients
 Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
A lifetime of specialist care. Managing your chest drain at home
 A lifetime of specialist care Managing your chest drain at home Contents Introduction 3 Patient details 3 How to contact us 4 Going home with a chest drain 5 How do I look after my chest drain? 5 General
A lifetime of specialist care Managing your chest drain at home Contents Introduction 3 Patient details 3 How to contact us 4 Going home with a chest drain 5 How do I look after my chest drain? 5 General
Top copy accepted by patient: yes/no (please ring)
 Consent Form 3 Patient / Parental agreement to investigation or treatment Procedures where consciousness not impaired Name of proposed procedure or course of treatment Hospital NHS Surname no: no: OUTPATIENT
Consent Form 3 Patient / Parental agreement to investigation or treatment Procedures where consciousness not impaired Name of proposed procedure or course of treatment Hospital NHS Surname no: no: OUTPATIENT
Hernia. Information for patients General Surgery
 Hernia Information for patients General Surgery page 2 of 8 What is a hernia? A hernia is a bulge or weakness in the muscles which form the front of the body wall. They are very common and easily treated,
Hernia Information for patients General Surgery page 2 of 8 What is a hernia? A hernia is a bulge or weakness in the muscles which form the front of the body wall. They are very common and easily treated,
Percutaneous Liver Biopsy
 PATIENT INFORMATION Royal Devon and Exeter NHS Foundation Trust Percutaneous Liver Biopsy Introduction This leaflet tells you about the procedure known as percutaneous liver biopsy. It explains what is
PATIENT INFORMATION Royal Devon and Exeter NHS Foundation Trust Percutaneous Liver Biopsy Introduction This leaflet tells you about the procedure known as percutaneous liver biopsy. It explains what is
E1 Ocean Ward Information Booklet
 Southampton University Hospitals NHS Trust E1 Ocean Ward Information Booklet for young people Help you prepare for your hospital stay This booklet has been written to help you prepare for your hospital
Southampton University Hospitals NHS Trust E1 Ocean Ward Information Booklet for young people Help you prepare for your hospital stay This booklet has been written to help you prepare for your hospital
Inferior Vena Cava (IVC) Filter Placement
 If you have any questions, ask your doctor or nurse. Filters may also be used. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower part of
If you have any questions, ask your doctor or nurse. Filters may also be used. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower part of
Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients
 Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients i The prostate The prostate is a small gland, which is found only men. It is found at the base of the
Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients i The prostate The prostate is a small gland, which is found only men. It is found at the base of the
Excision of Submandibular Gland
 Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Percutaneous Gastrostomy G-tube, or stomach feeding tube
 Patient Education Percutaneous Gastrostomy G-tube, or stomach feeding tube This handout explains what percutaneous gastrostomy is and what to expect when you have one. What is a gastrostomy tube? A gastrostomy
Patient Education Percutaneous Gastrostomy G-tube, or stomach feeding tube This handout explains what percutaneous gastrostomy is and what to expect when you have one. What is a gastrostomy tube? A gastrostomy
Oxford Orthoptic Service, Oxford Eye Hospital Children s Day Care Ward, The Children s Hospital. Squint surgery for children
 Oxford Orthoptic Service, Oxford Eye Hospital Children s Day Care Ward, The Children s Hospital Squint surgery for children This leaflet has been written to give you information about surgical correction
Oxford Orthoptic Service, Oxford Eye Hospital Children s Day Care Ward, The Children s Hospital Squint surgery for children This leaflet has been written to give you information about surgical correction
Having trabeculectomy surgery
 Having trabeculectomy surgery This leaflet aims to answer some of the questions you may have about having trabeculectomy surgery. It explains the benefits, risks and alternatives of the procedure as well
Having trabeculectomy surgery This leaflet aims to answer some of the questions you may have about having trabeculectomy surgery. It explains the benefits, risks and alternatives of the procedure as well
Breast Enlargement (augmentation)
 Patient information Breast Enlargement (augmentation) Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed: May 2015 Next review: May
Patient information Breast Enlargement (augmentation) Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed: May 2015 Next review: May
Non-cancer related bilateral mastectomy pre-operative information sheet
 Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
Carbapenemase-Producing Enterobacteriaceae (CPE) and Carbapenemase-Producing Organisms (CPO)
 Carbapenemase-Producing Enterobacteriaceae (CPE) and Carbapenemase-Producing Organisms (CPO) Information for patients and visitors This leaflet explains how we test for, treat and prevent the spread of
Carbapenemase-Producing Enterobacteriaceae (CPE) and Carbapenemase-Producing Organisms (CPO) Information for patients and visitors This leaflet explains how we test for, treat and prevent the spread of
Rectal prolapse. Information for patients General Surgery
 Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet
 Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Patient information. Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5
 Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt
 Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Treating a Bartholin s cyst or abscess
 Treating a Bartholin s cyst or abscess The aim of this information leaflet is to help answer some of the questions you may have about the treatment of a Bartholin s cyst or abscess. If you have any questions
Treating a Bartholin s cyst or abscess The aim of this information leaflet is to help answer some of the questions you may have about the treatment of a Bartholin s cyst or abscess. If you have any questions
Adult Strabismus Surgery Operation on the Eye Muscles
 Adult Strabismus Surgery Operation on the Eye Muscles Information for patients, relatives and carers Department of Ophthalmology For more information, please contact: The Eye Clinic Tel: 01904 726758 The
Adult Strabismus Surgery Operation on the Eye Muscles Information for patients, relatives and carers Department of Ophthalmology For more information, please contact: The Eye Clinic Tel: 01904 726758 The
You and your gastrostomy feeding tube
 The Clatterbridge Cancer Centre NHS Foundation Trust You and your gastrostomy feeding tube Rehabilitation and Support A guide for patients and carers Contents Skin care...1 Daily tube care...2 Feeding
The Clatterbridge Cancer Centre NHS Foundation Trust You and your gastrostomy feeding tube Rehabilitation and Support A guide for patients and carers Contents Skin care...1 Daily tube care...2 Feeding
Ophthalmology. Cataract Surgery. Information
 Ophthalmology Cataract Surgery Information Welcome to Spencer Ward We would hope your stay with us will meet your expectations. We have compiled this booklet to help answer any questions you may have regarding
Ophthalmology Cataract Surgery Information Welcome to Spencer Ward We would hope your stay with us will meet your expectations. We have compiled this booklet to help answer any questions you may have regarding
RIGHT HEMICOLECTOMY. Patient information Leaflet
 RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
Enhanced recovery programme
 Enhanced recovery programme Colorectal surgery Information for patients Colorectal Surgery Please bring this booklet with you to your Pre-operative Assessment appointment; when you are admitted to hospital
Enhanced recovery programme Colorectal surgery Information for patients Colorectal Surgery Please bring this booklet with you to your Pre-operative Assessment appointment; when you are admitted to hospital
Percutaneous Endoscopic Gastrostomy (PEG)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Implantable Loop Recorder (ILR)
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your doctor has advised you have an
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your doctor has advised you have an
Cardiac catheterisation. Cardiology Department Patient Information Leaflet
 Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Endometrial Cancer. Information for patients. Gynaecology Department. Feedback
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
