GUIDELINE FOR CLINICAL STAFF ON THE CARE OF : IMPLANTABLE PORTS
|
|
|
- Trevor McBride
- 6 years ago
- Views:
Transcription
1 GUIDELINE FOR CLINICAL STAFF ON THE CARE OF : IMPLANTABLE PORTS Version Number V2 Date of Issue December 2016 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised By Name: Rachel Kenna Title: Director for Nursing Author/s Location of Copies CVADIP V1 3 yearly Signature: Date: December 2016 Signature: Date: December 2016 Name: Fionnuala O Neill Title: Nurse Practice Coordinator On Hospital Intranet and locally in department Document Review History Review Date Reviewed By Signature 2019 Document Change History Change to Document Reason for Change
2 Date of Issue: November 2016 Page 2 of 13 Central Venous Access Devices (CVAD), is a broad term used to include many catheter types which are inserted into a peripheral/central vein in the body to deliver medications or other therapies to children. A catheter has one end positioned outside the body while a port is surgically placed under the skin and requires a special needle to access it. The most common CVADs include: Peripherally Inserted Central Catheter inserted into one of the peripheral veins in the upper arm. Central Venous Catheter Implanted ports inserted into the subclavian or vein or jugular and attached to a fluid reservoir placed in a surgically created subcutaneous pocket in the upper chest or into an arm vein. Hickman/Broviac catheter Permcath Catheter Umbilical Venous Catheter
3 Date of Issue: November 2016 Page 3 of 13 CONTENTS Page Number Introduction CVADs Commonly used reference tables Table 3 Blood discard volumes and Flush volumes for CVADS 2.0 Description General Principles for the care of Implantable Ports Port Access Insertion of a Cytocan/Gripper Needle and Flushing of Implantable Port Procedure Troubleshooting Definition 7.2 Port Occlusion 7.3 Port Erosion, Splitting of the catheter 7.4 Port Pocket Infection Appendix 1 - If needle not in situ 9 Appendix 2 If need in situ 9 References
4 Date of Issue: November 2016 Page 4 of Commonly used reference tables Table 3. Flush volumes for CVADS Line type Age Blood discard volume Suggested Flush volume for pre and post line use Heparin dose PICC/Midlines It is not possible to withdraw blood from a 1-2fr PICC < 1 year 1ml 0.5ml 10 units/ml 1-3 years 2.5ml units/ml > 3 years 3.5ml units/ml Central Venous Catheters < 1 year 1 ml 0.5-1ml 10 units/ml 1-3 years 2.5ml 1-2.5mls 10 units/ml > 3 years 3-5ml 3-5 mls 10 units/ml Hickman/Broviac < 1 year 1 ml As per surgeons 10 units/ml 1-3 years 2 ml As per surgeons 10 units/ml > 3 years 3-5 ml As per surgeons 10 units/ml Implantofix In some cases it may be requested that blood is withdrawn from an Implantofix. Umbilical Venous Catheters Permcath-Vascath < 1 year N/A 1ml -2.5 mls 10 units/ml 1-3 years N/A 1ml- 2.5mls 10 units/ml but Use 100units/ml when on discharge for patients with CF > 3 years N/A 1ml-2.5mls 10 units/ml < 1 year 1ml 0.5-1ml 10 units/ml 1-3 years N/A N/A 10 units/ml > 3 years N/A N/A 10 units/ml < 1 year 1ml 0.5-1ml See guideline 1-3 years N/A N/A See guideline > 3 years N/A N/A See guideline 2.0 Description Antibiotic locks must be given using the Pharmacy guideline as per OLCHC formulary app An implanted venous access device consists of a portal body attached to a silicone catheter. It is implanted subcutaneously in a convenient but inconspicuous location on the body, usually on the chest. Implanted ports require little care of the site because of the intact skin layer over the accessible port. They also require minimal flushing and permit easy access for fluids and/or medications. There is less interference with daily activities and body image is not threatened by the presence of a catheter. The catheter is inserted under general anaesthetic. A semi-circular incision is made to create the pouch to hold the port and a separate incision usually in the neck is made to locate the vein into which the
5 Date of Issue: November 2016 Page 5 of 13 catheter will be placed. After one end of the catheter is placed in a suitable vein the other end is locked to the port and fluid is injected to ensure the system is working properly. The port is then placed in the skin pocket and secured in place with stitches. The port may be used immediately following insertion. There are two basic parts to the system: The port A small plastic chamber sealed at the top by a rubber disc (septum) designed to withstand multiple punctures. A thin catheter one end is placed into a vein inside the body and the other end firmly attached to the portal with a special lock. 3.0 General Principles for the care of Implantable Ports Flushing and Maintaining Patency Prior to accessing the port for flushing and taking blood sampling, the documented port volume plus needle volume should be obtained from the patient s healthcare records. Note: same general principles regarding flushing and maintaining patency as Hickman catheter applies to Port -A - Cath. *Note: Parents are taught to do this at home in some situations. 100 units per ml of Heparinised saline are recommended to flush the Port- A-Cath if the device will not be used for 4 weeks to maintain patency. 10 units per ml of Heparinised saline can be used after more frequent drug administration or infusion. 4.0 Port Access Local anaesthetic cream e.g. Amethocaine 4% w/w (Huband & Trigg 2011) may be used prior to accessing the port. The skin should be washed with soap and water first to remove the ointment based anaesthetic cream, followed by cleaning with an antibacterial agent such as Chlorhexidine or Disposable disinfection wipes (70% v/v Isopropyl alcohol and 2% w/v Chlorhexidine gluconate) before accessing the port. A Huber point (non-coring) needle and a 10ml syringe (or larger) should always be used to access the port. In OLCHC a Cytocan or Gripper needle is inserted through the skin and silicone rubber septum into the portal chamber for repeated venous access e.g. for antibiotic therapy. Practitioners who have received specific education and training should access a port. (Please refer to the protocol for insertion of Cytocan/Gripper Needle and Flushing of Implanted ports section in the next page) The needle may remain in place for up to two weeks. The needle should remain in-situ using an occlusive dressing to avoid needle dislodgement e.g. Tegaderm Opsite dressing. An advantage of a port is that, when the port is not required the needle access is removed.
6 Date of Issue: November 2016 Page 6 of 13 The disadvantages of a port are the discomfort associated with accessing the port (especially if placed deeply or in a difficult area to access). This can be overcome with the use of topical anaesthetic cream. However, it still requires the insertion of a needle and for some children this may be unacceptable. 5.0 Insertion of a Cytocan / Gripper Needle and Flushing of Implantable Port DECONTAMINATE HANDS and collect the following: Requirements Sterile gloves x 1 pair Needle free device x 1 10 ml syringe x 2 Gauze x 1 packet Filter Straw x 2 Non-coring Huber needle with extension set (size individual to child) Heparin Sodium Flushing Solution (10 units/ml) x 3ml 0.9% sodium chloride solution 10ml Disposable disinfection wipes x 3 Clear dressing i.e. Tegaderm, Opsite Clean Tray 6.0 Procedure Explain the procedure to the patient and the parent. Apply Ametop cream 45 minutes prior to procedure if requested by the patient. Remove Tegaderm and Ametop from patient s skin. Wash skin with soap and water to remove the residue. Follow Universal precautions of hand washing and collect the following equipment prior to starting procedure. Prepare the sterile field by opening the sterile gloves packet onto tray and using the glove packet as a sterile field. Open all sterile equipment onto the sterile field. Bring the tray, vials of Heparinised Sodium Flushing Solution (10 units/ml) and 0.9% sodium chloride. solution (10ml) to the child s bedside Check expiry date of 0.9% Sodium Chloride and Heparinised sodium 10 units/ml vial clean the neck of vial with Disinfection wipe and dry it for a minimum of 30secs. Break off the top and leave it on a flat surface beside your sterile field.
7 Date of Issue: November 2016 Page 7 of 13 Decontaminate hands with antiseptic solution and put on sterile gloves. Draw up 0.9% Sodium Chloride and Heparinised sodium 10 units/ml into two separate syringes using ampoule straw, remove ampoule straw, expel any air bubbles and place the syringes in the tray. Unfold Disposable disinfection wipes. Connect needle free device to the Huber needle extension set. Prime the extension line using a syringe prepared with 0.9% sodium chloride solution and place on sterile field. Clean the port site and surrounding skin using disposable disinfection wipes. Working in a clockwise direction clean from the centre outwards for at least 10cm (4 inches). Use each swab once in one direction only. Pick up Huber Needle and syringe in right hand and remove guard from needle. Using left hands palpate the edges of the port and hold the outer edge through the skin ensuring port is secure & non-mobile. Put the needle firmly through the skin and port at a 90 degree angle until it hits the bottom of the port chamber. Check for blood return. Open clamp and flush the line with 10ml of 0.9% sodium chloride solution and remove syringe from needle free device. Attach the syringe containing Heparinised saline to the Needle free device. Open clamp and inject the heparin solution, closing the clamp as the last 0.5ml is being injected. Removing Huber needle: Whilst withdrawing the needle it is important to maintain positive pressure by pressing down on the port with two fingers as the last 0.5 ml of flush is infused. Apply pressure if oozing. Site may be left exposed following removal of the Huber needle or covered with a dry dressing. IF leaving Huber Needle in situ: Cover and secure it with a Tegaderm dressing. If needle is not flush with skin place a small piece of keyhole cut gauze between the skin and needle housing. Once accessed the Huber needle may remain in situ for up to 14 days or as per local policy. Sterile technique must be adhered to while accessing the port with a hubar needle. Once accessed and a Needle free bung is applied, strict non-touch technique is sufficient and the Port is managed as per Hickman Policy. Ensure that the child is comfortable and that the line is well secured.
8 Date of Issue: November 2016 Page 8 of 13 Dispose of all equipment appropriately. Decontaminate hands with antiseptic solution. Document procedure in patient s healthcare records. 7.0 Troubleshooting Port-A-Cath Infection 7.1 Definition A documented rise in temperature in a clinically well child following flushing of the catheter associated with a chill/rigor and transient constitutional disturbance e.g. fatigue or decreased activity that settles spontaneously or with antipyretic measures. (Please follow the same protocol as for the management of Hickman Catheter Line Infections) 7.2 Port Occlusion Obstruction secondary to thrombus formation is one of the complications associated with implantable Ports. Do not attempt to unblock totally occluded ports unless trained to do so as it may dislodge a catheter embolus. Contact OLCHC, Haematology/Oncology medical team who may decide that Urokinase may need to be prescribed to unblock the line occlusion. Implantable Port 5,000 Units of Urokinase (Syner-KINASE brand) in 1ml of saline Note: Please follow the Protocol for instillation of Urokinase into a Blocked Hickman Catheter. The same protocol applies to port occlusion also. 7.3 Port Erosion, Splitting of the catheter If skin breaks down over the port reservoir seek advice from the Haematology/Oncology Team in OLCHC supervising the child s care. Once port erosion occurs the device usually requires removal. If there is a suspected break on the internal part of the catheter seek advice from the Haematology/Oncology team in OLCHC. The child may need a lineogram to confirm the breakage. 7.4 Port Pocket Infection Swelling, tenderness and redness at the port site or along the catheter tract suggests port pocket infection. Please follow the action procedure in the next page when needle not in-situ and needle insitu.
9 Date of Issue: November 2016 Page 9 of 13 Appendix 1 If needle not in situ ACTION If possible avoid accessing the Port RATIONALE If needle is inserted through the skin into the Port, infection may be introduced into the Port and catheter. If child s condition dictates or no other venous access available it may be preferable to access the Port. If this action is taken ensure blood cultures are obtained and IV antibiotics are commenced. Contact the medical team at OLCHC supervising the child s treatment. Culture any purulent discharge Give IV antibiotics via peripheral cannula for 48 hours Access the Port after 48 hours. If the infection is responding to IV antibiotics the Port may be accessed and antibiotics continued via Port. Check Port daily for signs of skin breakdown To identify cause of infection To clear Port pocket infection Once infection is treated Port may be used. This is advisable if skin infection has cleared to treat any infection that may have entered the Port To identify Port erosion. If Port erosion presents contact OLCHC medical team supervising the child s treatment as device may require removal. Appendix 2 If needle in situ ACTION Do not remove the needle Continue to give IV antibiotics via the port for 48 hours If no improvement after 48hours remove the needle and continue IV antibiotics peripherally If improvement in the condition of the skin continue to treat through the port RATIONALE It has provided a conduit for the infection which may already have entered the port To treat infection if it has tracked through to the port To rest skin. Port has received some treatment with antibiotics Treatment is effective References
10 Date of Issue: November 2016 Page 10 of 13 American College of Chest Physicans (ACCP) (2012) Antithrombotic therapy in neonates and children: antithrombotic therapy and prevention of thrombosis, 9 th Edition. Chest, 141: e737s-e801s. Ball, J.W. Bindler, R.C. and Cowen, K. (2013) Child Health Nursing: Partnering with Children and Families, 3rd Edition. Pearson: London. BBraun (2011) Air Embolism: Risk Prevention in Infusion Therapy. BBraun: Melsungen, Germany. Available online: (Accessed April 27 th 2016). Boer, W.H. and Hene, R.J. (1999) Lethal air embolism following removal of a double lumen jugular vein catheter. Nephrology Dialysis Transplantation. 14(8): Brockmeyer, J. Simon, T. Seery, J. Johnson, E. and Armstrong, P. (2009) Cerebral air embolism following removal of central venous catheter. Military Medicine, 174(8): Carrett, L. Reverdy, M.E. Lafforgue, C. Falson, F. Fleurette, J. and Freney, J. (1997) Kinetics of chlorhexidine on intact skin following a single application. Pathology Biology 54(9): Chen, Z. (2014) Evidence Summary: Central Venous Access Device (CAVD), Removal. The Joanna Briggs Institute: Adelaide. Department of Health (2007) Saving Lives: Reducing Infection, Delivering Clean and Safe Care. High Impact Intervention No 1: Central venous Catheter Care Bundle. Department of Health: London. Available online: (Accessed April 25 th 2016). Department of Health (2010) Clean Safe Care. High Impact Interventions: Central Venous Catheter Care Bundle and Peripheral IV Cannula Care Bundle. Department of Health, London. Department of Health and Children (2002) Segetation Packaging and Storage Guidelines for Healthcare Risk Waste. Department of Health and Children: Dublin. Drewett. S.R. (2000a) Central venous catheter removal: procedures and rationale. British Journal of Nursing 9(22): Drewett, S.R. (2000b) Complications of central venous catheters: nursing care. British Journal of Nursing, 9(8): Dougherty, L. (2015) How to remove a non-tunnelled central venous catheter. Nursing Standard, 30(16-18): Dougherty, L. and Lister, S (eds) (2015) The Royal Marsden Hospital Manual of Clinical Nursing Procedures, 9 th Edition. Wiley-Blackwell: Chichester. Dumont, C. (2001) Procedures nurse use to remove central venous catheters and complications they observe: A pilot study. American Journal of Critical Care 10(3): Feil, M. (2012) Risking risk of air embolism associated with central venous devices. Pennsylvania Patient Safety, 9(2): Available online: (Accessed 27 th April 2016). Hadaway, L.C. (2010) Anatomy and Physiology Related to Infusion Therapy. In Infusion Nurse Society, Alexandra, M. Corrigan, A. Gorski, L. HANKINS, j. AND Perucca, R. Infusion Nursing: An Evidencebased Approach, 3 rd Edition. Saunders Elsevier: St Louis,
11 Date of Issue: November 2016 Page 11 of 13 HCAI / Royal College of Physicians of Ireland/ HSE (2014) Prevention of Intravascular Catheterrelated Infections in Ireland: Update of 2009 National Guidelines. Available online: (Accessed 22 nd April 2016). Hockenberry, M.J. and Wilson, D. (eds) (2015) Wong s Essentials of Pediatric Nursing, 10 th Edition. Mosby: St Louis. Ingram P. Sinclair L. and Edwards T. (2006) The safe removal of central venous catheters. Nursing Standard 20(49): INS (2011) Infusion nursing standards of practice, Journal of Infusion Nursing 34(1): supplement. Joanna Briggs Institute (2013) Central Venous Access Device (CAVD): Removal. The Joanna Briggs Institute; Adelaide. Kim, D.K. Gottesman, M.H. Forero, A. Han, D. Myers, D.W. Forienza, R. and Golzarian, J. (1998) The CVC removal distress syndrome: an unappreciated complication of central venous line removal. American Journal of Surgery, 64(4): Lloyd-Jones, M. (2004) Minimizing pain at dressing changes. Nursing Standard 18(24): Long, K.D.L. (2015) Central Venous Catheter (CVC): Dressing and Flushing. The Joanna Briggs Institute: Adelaide. Loveday, H.P. Wilson, J.A. Pratt, R.J. Golsorkhi, M. Ingle, A. Bak, J. Browne, J. Prieto, J. Wilcox, M. (2014) Epic3: National evidence-based guidelines for preventing healthcare-associated infections in NHS hospital in England. Journal of Hospital Medicine, 8651: s1 s70. Luettel, d. (2011) Avoiding air embolism when removing CVCs. Nursing Times, 107(43): 23. Maki, D.G. Kluger, D.M. Cmich, C.J. (2006) The risk of bloodstream infection in adults with different intravascular devices: a systematic review of 200 published prospective studies. Mayo Clin Proc., 81(9): Meggiolaro, M. Roman-Pognuz, E. Baritussio, A, and Scatto, A. (2013) Air embolism after central venous catheter removal; Fibrin sheath at the portal of persistant air entry. Case Reports in Critical Care, 2013, Article ID , 1-3. Available online: (Accessed April 27 th 2016). Morgan, B. (2013) Procedure for Removal of Central Venous Catheters (Jugular, Subclavian and Femoral.) London Health Sciences Centre. Available online: (Accessed April 26 th 2016). National Institute for Health and Clinical Excellence (NICE) (2012) Healthcare Associated Infection : Prevention and Control in Primary and Community Care. NICE: London. NMBI (2015a) Recording Clinical Practice, 2 nd Edition. Nursing and Midwifery Board of Ireland: Dublin. NMBI (2015b) Scope of Nursing and Midwifery Practice Framework, 2 nd Edition. Nursing and Midwifery Board of Ireland: Dublin.
12 Date of Issue: November 2016 Page 12 of 13 NPSA (2011) Risk of Air Embolism When Removing Central Lines / Signal. National Patient Safety Agency. Available online: (Accessed April 27 th 2016). Nolan, T. and Berwick, D.M. (2006) All or none measurement raises the bar on performance. JAMA, 295(10): O Grady, N.P. Alexander, M. Burns, L.A. Dellinger, E.P. garland, J. Heard, S.O. Lipsett, P.A. Masur, H. Mermel, L.A. Person, M.L. Raad, I.I. Randolph, A. Rupp, M.E. Saint, S. and Healthcare Infection Control Practices and Advisory Committee (HICPAC) (2011) Guidelines for Prevention of Intravascular Catheter-related Infection. (CDC) / HICPAC. Available online: (Accessed 22 nd April 2016). OLCHC (2008) Infection Control / Waste Policy, Our Lady s Children s Hospital, Crumlin: Dublin. OLCHC (2010a) Guideline for Hand Hygiene, Our Lady s Children s Hospital Crumlin: Dublin. OLCHC (2010b) Hospital Formulary. Our Lady s Children s Hospital, Crumlin, Dublin. OLCHC (2011) Standard Universal Precautions. Our Lady s Children s Hospital, Crumlin: Dublin. OLCHC (2012a) Skin Asepsis Prior to Peripheral and Central Line Insertion. Our Lady s Children s Hospital, Crumlin: Dublin. OLCHC (2012b) Anti Thrombotic Central Line Guidelines. Our Lady s Children s Hospital, Crumlin: Dublin. OLCHC (2013) Aseptic Non-touch Technique, OLCHC Reference Guide. Our Lady s Children s Hospital, Crumlin: Dublin. OLCHC (2015) Guidelines on Care Bundles in Our Lady s Children s Hospital Crumlin (OLCHC). Our Lady s Children s Hospital, Crumlin: Dublin. Peter, D.A. and Saxman, C. (2003) Preventing air embolism when removing cvcs: An evidence-based approach to changing practice. Medsurg Nursing 12(4): Phifer, T.J. Bridges, M.Conrad, S.A. (1991) The residual central venous catheter track- an occult source of lethal air embolism: case report. Journal of Trauma 31(11): Porritt, K. (2016) Central Venous Access Device (CAVD): Dressing Change. The Joanna Briggs Institute: Adalaide. Pronovost, P. Needham, D. Berenholtz, S. Sinopoli, D. Chu, H. Cosgrove, S. Sexton, B. Hyzy, R. Welsh, R. Roth, G. Bander, J. Kepros, J. and Goeschel, C. (2006) An intervention to decrease catheter-related bloodstream infections in the ICU. New England Journal of Medicine, 355(26): Resar, R. Griffin, F.A. Haraden, C. and Nolan, T.W. (2012) Using Care Bundles to Improve Healthcare Quality. IHI Innovative Series White paper. Institute for Healthcare Improvement (IHI); Cambridge, MA. Available online: (Accessed April 22 nd 2016). Royal College of Nurses (2010) Standards for Infusion Therapy, 3 rd Edition. RCN: London. Available online: (Accessed 26 th April 2016).
13 Date of Issue: November 2016 Page 13 of 13 SARI Infection Control Sub Committee (2009) A Strategy for the Control of Antimicrobial Resistance in Ireland (SARI): Guidelines for Hand Hygiene in Irish healthcare Settings. Health Service Executive (HSE) / Health Protection Surveillance Centre (HPSC). Stephenson, M. (2016) Evidence Summary: Central Venous Catheter (CVC), Dressing of Insertion Site. The Joanna Briggs Institute: Adelaide. Van Matre, J.G. (2006) All or none measurement of healthcare quality. JAMA, 296(4): 392. Disclaimer 2016, Our Lady s Children s Hospital Crumlin, Dublin 12. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system or transmitted in any form or by any means without the prior written permission of the copyright holder. Every effort has been made to ensure that the information provided is accurate and in accord with standards accepted at the time of printing OLCHC.
NURSING GUIDELINES ON TAKING BLOOD CULTURES FROM PERIPHERAL OR CENTRAL VENOUS ACCESS DEVICE
 NURSING GUIDELINES ON TAKING BLOOD CULTURES FROM PERIPHERAL OR CENTRAL VENOUS ACCESS DEVICE Version Number V22 Date of Issue June 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill
NURSING GUIDELINES ON TAKING BLOOD CULTURES FROM PERIPHERAL OR CENTRAL VENOUS ACCESS DEVICE Version Number V22 Date of Issue June 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill
Intravenous Medication Administration via a Central Venous Line
 Standard Operating Procedure 11 (SOP 11) Intravenous Medication Administration via a Central Venous Line Why we have a procedure? This procedure is to assist/ inform healthcare professionals on how to
Standard Operating Procedure 11 (SOP 11) Intravenous Medication Administration via a Central Venous Line Why we have a procedure? This procedure is to assist/ inform healthcare professionals on how to
Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy
 Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy (Note: See Separate Policy for Port-a-Cath Care and Management) DOCUMENT CONTROL: Version: v2 Ratified by: Quality
Central Venous Access Devices (CVADs) Hickman/Broviac and PICC Care Management Policy (Note: See Separate Policy for Port-a-Cath Care and Management) DOCUMENT CONTROL: Version: v2 Ratified by: Quality
Vascuport in Children for Routine Flushing and Administration of Medication
 Standard Operating Procedure 6 (SOP 6) Vascuport in Children for Routine Flushing and Administration of Medication Why we have a procedure? This guidance is to assist/ inform healthcare professionals on
Standard Operating Procedure 6 (SOP 6) Vascuport in Children for Routine Flushing and Administration of Medication Why we have a procedure? This guidance is to assist/ inform healthcare professionals on
Totally Implantable Venous Access Devices (port) Information for patients. Cross section of a port
 Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
Cystic Fibrosis Unit, Ward 26 0121 424 2000 Information for Patients Totally Implantable Venous Access Devices (port) Information for patients This leaflet tells you about the procedures for Totally Implantable
PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS ACCESS DEVICE PORTS FOR ADULTS
 PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS FOR ADULTS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To ensure a safe and effective procedure for the
PROCEDURE FOR FLUSHING TOTALLY IMPLANTED INTRAVENOUS FOR ADULTS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To ensure a safe and effective procedure for the
Central Venous Access Devices (CVAD) Procedures
 SH CP 138 Central Venous Access Devices (CVAD) Procedures (e.g. Peripherally Inserted Central Catheter ( PICC lines) and Skin Tunnelled Central lines) Version:2 Summary: Keywords (minimum of 5): (To assist
SH CP 138 Central Venous Access Devices (CVAD) Procedures (e.g. Peripherally Inserted Central Catheter ( PICC lines) and Skin Tunnelled Central lines) Version:2 Summary: Keywords (minimum of 5): (To assist
ASEPTIC TECHNIQUE LEARNING PACKAGE
 ASEPTIC TECHNIQUE LEARNING PACKAGE Staff Name:... Date:... Table of Contents What is Aseptic technique? 3 Core infection control components 3 Key parts 5 References 6 Aseptic technique questionnaire 7
ASEPTIC TECHNIQUE LEARNING PACKAGE Staff Name:... Date:... Table of Contents What is Aseptic technique? 3 Core infection control components 3 Key parts 5 References 6 Aseptic technique questionnaire 7
References and Bibliography
 References and Bibliography References and Bibliography ANTT Theoretical Framework for Clinical Practice V4.0 2015. Association for Safe Aseptic Practice (ASAP) www.antt.org. BNF (2015) British National
References and Bibliography References and Bibliography ANTT Theoretical Framework for Clinical Practice V4.0 2015. Association for Safe Aseptic Practice (ASAP) www.antt.org. BNF (2015) British National
NASAL ENDOSCOPY IN THE OUTPATIENTS DEPARTMENT (OPD)
 NASAL ENDOSCOPY IN THE OUTPATIENTS DEPARTMENT (OPD) Version Number V2 Date of Issue January 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
NASAL ENDOSCOPY IN THE OUTPATIENTS DEPARTMENT (OPD) Version Number V2 Date of Issue January 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
RN Entry Level Competency
 Policies & Procedures Title: CENTRAL VENOUS CATHETERS BLOOD WITHDRAWAL (, SHORT TERM, TUNNELED, IMPLANTED) LPN Additional Competency (LPNAC) Central Venous Catheters - Blood Withdrawal from with an Established
Policies & Procedures Title: CENTRAL VENOUS CATHETERS BLOOD WITHDRAWAL (, SHORT TERM, TUNNELED, IMPLANTED) LPN Additional Competency (LPNAC) Central Venous Catheters - Blood Withdrawal from with an Established
Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure
 Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Quality and Standards Group Date
Administration of IV Medication in the Community by the Children s Community Nursing Team Standard Operating Procedure DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Quality and Standards Group Date
NURSING POLICIES, PROCEDURES & PROTOCOLS
 Page 1 of 10 NURSING POLICIES, PROCEDURES & PROTOCOLS CENTRAL VENOUS ACCESS DEVICE (CVAD) HEMODIALYSIS CATHETERS: DRESSING CHANGE, INITIATING OR DISCONTINUING AN INFUSION NO.: 00056 (Formerly NSG2146)
Page 1 of 10 NURSING POLICIES, PROCEDURES & PROTOCOLS CENTRAL VENOUS ACCESS DEVICE (CVAD) HEMODIALYSIS CATHETERS: DRESSING CHANGE, INITIATING OR DISCONTINUING AN INFUSION NO.: 00056 (Formerly NSG2146)
DISTRICT NURSING and INTERMEDIATE CARE
 CLINICAL GUIDELINES DISTRICT NURSING and INTERMEDIATE CARE Schedule of guidelines attached: DNICT03 Community Procedure for the Administration of Intravenous Drugs via Bolus The guidelines scheduled above
CLINICAL GUIDELINES DISTRICT NURSING and INTERMEDIATE CARE Schedule of guidelines attached: DNICT03 Community Procedure for the Administration of Intravenous Drugs via Bolus The guidelines scheduled above
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa
 CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling Vascular Access
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling Vascular Access
CENTRAL VENOUS ACCESS DEVICE POLICY
 CENTRAL VENOUS ACCESS DEVICE POLICY Version: 1 Date of Issue: April 2018 Review Date: April 2021 Applies to: All clinical staff who care for patients with Central Venous Access Devices (CVADs) as part
CENTRAL VENOUS ACCESS DEVICE POLICY Version: 1 Date of Issue: April 2018 Review Date: April 2021 Applies to: All clinical staff who care for patients with Central Venous Access Devices (CVADs) as part
Procedure for Eye Examination for Retinopathy of Prematurity (ROP) in the Out Patients Department (OPD)
 Procedure for Eye Examination for Retinopathy of Prematurity (ROP) in the Version Number 03 STANDARD OPERATING PROCEDURE Date of Issue January 2015 Reference Number Review Interval Approved By Name: Fionnuala
Procedure for Eye Examination for Retinopathy of Prematurity (ROP) in the Version Number 03 STANDARD OPERATING PROCEDURE Date of Issue January 2015 Reference Number Review Interval Approved By Name: Fionnuala
MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa
 MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling
MARSHALLTOWN MEDICAL & SURGICAL CENTER Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.37 Subject: Implanted Venous Access Device (Infus-A-Port), Nursing Management Of (Indwelling
Implementation Guide for Central Line Associated Blood Stream Infection
 Implementation Guide for Central Line Associated Blood Stream Infection March 27, 2013 Contents 1. Introduction... 3 2. Central Line Associated Blood Stream Infection Prevention Evidence-Based Practices...
Implementation Guide for Central Line Associated Blood Stream Infection March 27, 2013 Contents 1. Introduction... 3 2. Central Line Associated Blood Stream Infection Prevention Evidence-Based Practices...
Developed in response to: Best Practice Health and Social Act 2008 CQC Fundamental Standards: 12
 ASEPTIC TECHNIQUE AND ASEPTIC NON- TOUCH TECHNIQUE Clinical Guideline Register No: 08038 Status : Public Developed in response to: Best Practice Health and Social Act 2008 CQC Fundamental Standards: 12
ASEPTIC TECHNIQUE AND ASEPTIC NON- TOUCH TECHNIQUE Clinical Guideline Register No: 08038 Status : Public Developed in response to: Best Practice Health and Social Act 2008 CQC Fundamental Standards: 12
Central Venous Access Devices (CVADs)
 Contents Purpose... 1 Policy... 1 Scope... 2 Associated documents... 2 1 Insertion of CVADs... 2 2 Endorsement/Certification... 2 3 Procedural Considerations... 3 3.1 Checking and Identification requirements...
Contents Purpose... 1 Policy... 1 Scope... 2 Associated documents... 2 1 Insertion of CVADs... 2 2 Endorsement/Certification... 2 3 Procedural Considerations... 3 3.1 Checking and Identification requirements...
Registered Nurse Intravenous Therapy and Peripheral Cannulation Competency Framework
 Registered Nurse Intravenous Therapy and Peripheral Cannulation Competency Framework Name: Location: Date commenced: Contents Competency: Page No: Page 1. Core: Introduction Demonstrate knowledge that
Registered Nurse Intravenous Therapy and Peripheral Cannulation Competency Framework Name: Location: Date commenced: Contents Competency: Page No: Page 1. Core: Introduction Demonstrate knowledge that
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath
 You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
Nursing Guidelines on the Administration of Coagulation Factor Concentrate
 Nursing Guidelines on the Administration of Coagulation Factor Concentrate Version Number 2 Date of Issue 2 nd April 2014 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Chairperson
Nursing Guidelines on the Administration of Coagulation Factor Concentrate Version Number 2 Date of Issue 2 nd April 2014 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Chairperson
CENTRAL LINE ASSOCIATED BLOOD STREAM INFECTIONS (CLABSI)
 CENTRAL LINE ASSOCIATED BLOOD STREAM INFECTIONS (CLABSI) A Step-by- Step Approach 1 Evidence Based Recommendations for the Prevention of CLABSI 2013 CLABSI FACTS An estimated 41,000 central line-associated
CENTRAL LINE ASSOCIATED BLOOD STREAM INFECTIONS (CLABSI) A Step-by- Step Approach 1 Evidence Based Recommendations for the Prevention of CLABSI 2013 CLABSI FACTS An estimated 41,000 central line-associated
1. Nurses may remove non-tunneled catheters upon the order of a physician. Physicians remove tunneled catheters.
 Removal of Non-Tunneled Central Venous Catheter (CVC) (Approved Aug 15, 2011/Rev Dec 16, 2011/Rev Jun 13, 2012) Vascular Access Guideline Table of Contents This procedure is posted on the BC Provincial
Removal of Non-Tunneled Central Venous Catheter (CVC) (Approved Aug 15, 2011/Rev Dec 16, 2011/Rev Jun 13, 2012) Vascular Access Guideline Table of Contents This procedure is posted on the BC Provincial
ASEPTIC & CLEAN (NON TOUCH TECHNIQUE) POLICY
 ASEPTIC & CLEAN (NON TOUCH TECHNIQUE) POLICY First Issued by/date Issue Version Purpose of Issue/Description of Change Planned Review Date 4 Update September 2012 Named Responsible Officer:- Approved by
ASEPTIC & CLEAN (NON TOUCH TECHNIQUE) POLICY First Issued by/date Issue Version Purpose of Issue/Description of Change Planned Review Date 4 Update September 2012 Named Responsible Officer:- Approved by
Peripherally Inserted Central Catheter (PICC)
 University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
393 PICC INSERTION USING ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1
 393 ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1 POLICY: General Information: 1. RN s validated to insert PICCs with the additional training in the use of ultrasonography (U/S) and microintroduction
393 ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1 POLICY: General Information: 1. RN s validated to insert PICCs with the additional training in the use of ultrasonography (U/S) and microintroduction
Section G - Aseptic Technique. Version 5
 Section G - Aseptic Technique Version 5 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you must
Section G - Aseptic Technique Version 5 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you must
Nottingham Renal and Transplant Unit
 Nottingham Renal and Transplant Unit GUIDELINES FOR THE COMMENCEMENT AND TERMINATION OF EXTRA CORPOREAL THERAPIES VIA A CENTRAL VENOUS CATHETER (TUNNELLED AND NON TUNNELLED) USING CITRATE 46.7% LOCKING
Nottingham Renal and Transplant Unit GUIDELINES FOR THE COMMENCEMENT AND TERMINATION OF EXTRA CORPOREAL THERAPIES VIA A CENTRAL VENOUS CATHETER (TUNNELLED AND NON TUNNELLED) USING CITRATE 46.7% LOCKING
Wyoming STATE BOARD OF NURSING
 David D. Freudenthal Governor Wyoming STATE BOARD OF NURSING Mary Kay Goetter, PhD, RNC, NEA-BC Executive Director 1810 Pioneer Avenue Cheyenne, Wyoming 82002 Phone: 307-777-7601 FAX: 307-777-3519 http://nursing.state.wy.us
David D. Freudenthal Governor Wyoming STATE BOARD OF NURSING Mary Kay Goetter, PhD, RNC, NEA-BC Executive Director 1810 Pioneer Avenue Cheyenne, Wyoming 82002 Phone: 307-777-7601 FAX: 307-777-3519 http://nursing.state.wy.us
1. Communicate to the UAP any special information needed prior to the administration of the medication.
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by intradermal injection. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by intradermal injection. 2. document medication administration in the client
See Policy #1302 (Nursing Student Privileges and Limitations) for full details. Central Line dressing care, declotting and discontinuation may ONLY
 To assure a standardized knowledge base related to CVL Care and CLABSI prevention, ProMedica requires all Instructors/Faculty on adult and pediatric units to complete this educational module. This content
To assure a standardized knowledge base related to CVL Care and CLABSI prevention, ProMedica requires all Instructors/Faculty on adult and pediatric units to complete this educational module. This content
CENTRAL VENOUS LINES: REMOVAL
 [Type text] KINGSTON HEALTH SCIENCES CENTRE Kingston General Hospital site CENTRAL VENOUS LINES: REMOVAL LEARNING GUIDE FOR REGISTERED NURSES Prepared by: Nursing Education Services Date: 1993 December
[Type text] KINGSTON HEALTH SCIENCES CENTRE Kingston General Hospital site CENTRAL VENOUS LINES: REMOVAL LEARNING GUIDE FOR REGISTERED NURSES Prepared by: Nursing Education Services Date: 1993 December
Patient Self Administration of Intravenous (IV) Antibiotics at Home
 Trust Policy Document Ref. No: PP(16)319 Patient Self Administration of Intravenous (IV) Antibiotics at Home For use in: For use by: For use for: Document owner: Status: Clinical Areas Clinical Staff Patient
Trust Policy Document Ref. No: PP(16)319 Patient Self Administration of Intravenous (IV) Antibiotics at Home For use in: For use by: For use for: Document owner: Status: Clinical Areas Clinical Staff Patient
All about Your Implanted Venous Access Device (IVAD, Port )
 All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
Best Practice Guidelines BPG 5 Catheter Care
 Best Practice Guidelines BPG 5 Catheter Care BGP 5 1 DOCUMENT STATUS: Reviewed DATE ISSUED: March 2014 DATE TO BE REVIEWED: 13.10.17 AMENDMENT HISTORY VERSION DATE AMENDMENT HISTORY V1 March 2014 New Guideline
Best Practice Guidelines BPG 5 Catheter Care BGP 5 1 DOCUMENT STATUS: Reviewed DATE ISSUED: March 2014 DATE TO BE REVIEWED: 13.10.17 AMENDMENT HISTORY VERSION DATE AMENDMENT HISTORY V1 March 2014 New Guideline
Practice Guideline: Approval Date: May 11, 2017
 Page 1 of 7 1. PURPOSE To provide a safe, standardized, evidence-informed process, for Central Vascular Access Device (CVAD) dressing changes. This practice guideline does not include dialysis catheters.
Page 1 of 7 1. PURPOSE To provide a safe, standardized, evidence-informed process, for Central Vascular Access Device (CVAD) dressing changes. This practice guideline does not include dialysis catheters.
NORTH SHORE MEDICAL CENTER NURSING PROCEDURE
 NORTH SHORE MEDICAL CENTER NURSING PROCEDURE TITLE: IMPLANTED VASCULAR ACCESS DEVICE (VAD): DEVICE ACCESS, ADMINISTRATION OF IV FLUID OR MEDICATION, DRAWING BLOOD SPECIMENS AND REMOVAL OF NON-CORING RIGHT
NORTH SHORE MEDICAL CENTER NURSING PROCEDURE TITLE: IMPLANTED VASCULAR ACCESS DEVICE (VAD): DEVICE ACCESS, ADMINISTRATION OF IV FLUID OR MEDICATION, DRAWING BLOOD SPECIMENS AND REMOVAL OF NON-CORING RIGHT
Having a portacath insertion in the x-ray department
 Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
Blood Culture Policy
 Policy No: IC27 Version: 5.0 Name of Policy: Blood Culture Policy Effective From: 21/09/2015 Date Ratified 15/09/2015 Ratified Infection Prevention and Control Committee Review Date 01/09/2017 Sponsor
Policy No: IC27 Version: 5.0 Name of Policy: Blood Culture Policy Effective From: 21/09/2015 Date Ratified 15/09/2015 Ratified Infection Prevention and Control Committee Review Date 01/09/2017 Sponsor
Venous Access Devices. Management of Central Venous Access Devices (CVADs) Central Venous Catheters. Outline. Implantable Port
 Management of Central Venous Access Devices (CVADs) Bangkok June 2015 Venous Access Devices Implantable Port Central Venous Catheter (CVC) Boviac /Hickman catheters Margaret Conway BSN, RN, CPON Peripherally
Management of Central Venous Access Devices (CVADs) Bangkok June 2015 Venous Access Devices Implantable Port Central Venous Catheter (CVC) Boviac /Hickman catheters Margaret Conway BSN, RN, CPON Peripherally
The Nurse s Role in Preventing CLABSI
 The Nurse s Role in Preventing CLABSI This course has been awarded one (1.0) contact hour. This course expires on February 28, 2020 Copyright 2017 by RN.com. All Rights Reserved. Reproduction and distribution
The Nurse s Role in Preventing CLABSI This course has been awarded one (1.0) contact hour. This course expires on February 28, 2020 Copyright 2017 by RN.com. All Rights Reserved. Reproduction and distribution
ASEPTIC TECHNIQUE POLICY
 SECTION 3b ASEPTIC TECHNIQUE POLICY INFECTION CONTROL MANUAL Read in conjunction with: o Hand hygiene policy (also section 3) o Standard (Universal) Precautions policy (section 4) o Decontamination policy
SECTION 3b ASEPTIC TECHNIQUE POLICY INFECTION CONTROL MANUAL Read in conjunction with: o Hand hygiene policy (also section 3) o Standard (Universal) Precautions policy (section 4) o Decontamination policy
VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP VAP SK-V1
 VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP Version Number V1 Date of Issue February 2018 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP Version Number V1 Date of Issue February 2018 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
Mid-line Vascular Access Device Policy (Adults) and Procedures/Guideline
 Mid-line Vascular Access Device Policy (Adults) and Procedures/Guideline October 2016 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
Mid-line Vascular Access Device Policy (Adults) and Procedures/Guideline October 2016 Document Profile Type i.e. Strategy, Policy, Procedure, Guideline, Protocol Title Category i.e. organisational, clinical,
STANDARDIZED PROCEDURE HEPATIC ARTERY INFUSION OF CHEMOTHERAPY (Adults, Peds)
 I. Definition Hepatic arterial infusion (HAI) of chemotherapy is accomplished by a small drug delivery system or pump that is implanted in a subcutaneous pocket in the lower abdomen. The pump reservoir
I. Definition Hepatic arterial infusion (HAI) of chemotherapy is accomplished by a small drug delivery system or pump that is implanted in a subcutaneous pocket in the lower abdomen. The pump reservoir
HHVNA Infusion Therapy MIDLINE CATHETER
 CONSIDERATIONS: 1. This midline procedure includes procedural steps for: a. Catheter Insertion b. Flushing c. Site care and dressing change d. Cap change e. Blood Draw f. Management of complications 2.
CONSIDERATIONS: 1. This midline procedure includes procedural steps for: a. Catheter Insertion b. Flushing c. Site care and dressing change d. Cap change e. Blood Draw f. Management of complications 2.
STANDARDIZED PROCEDURE CENTRAL LINE PLACEMENT and TEMPORARY NONTUNNELLED CENTRAL VENOUS DIALYSIS CATHETER INSERTION (Adult, Peds)
 I. Definition: This protocol covers the task of central (venous) catheter placement and temporary nontunnelled central venous dialysis catheters by the Advanced Health Practitioner. The purpose of this
I. Definition: This protocol covers the task of central (venous) catheter placement and temporary nontunnelled central venous dialysis catheters by the Advanced Health Practitioner. The purpose of this
TRUST DELIVERY GROUP: 22 AUGUST 2017 FOR: APPROVAL DISCUSSION INFORMATION. Acting Chief Nurse & Director of Patient Experience
 TRUST DELIVERY GROUP: 22 AUGUST 2017 FOR: APPROVAL DISCUSSION INFORMATION ITEM Lead: Designation: Jim Murray Acting Chief Nurse & Director of Patient Experience TRUST POLICY AND PROCEDURES FOR ASEPTIC
TRUST DELIVERY GROUP: 22 AUGUST 2017 FOR: APPROVAL DISCUSSION INFORMATION ITEM Lead: Designation: Jim Murray Acting Chief Nurse & Director of Patient Experience TRUST POLICY AND PROCEDURES FOR ASEPTIC
Community Intravenous Therapy Referral Standards
 pecialist harmacy ervice Medicines Use and afety Community Intravenous Therapy Referral tandards Background A multi-centred audit of prescribing and administration of community IV therapy across East and
pecialist harmacy ervice Medicines Use and afety Community Intravenous Therapy Referral tandards Background A multi-centred audit of prescribing and administration of community IV therapy across East and
MIDLINES/EXTENDED DWELL
 MIDLINES/EXTENDED DWELL Peripheral venous access devices 3-8 inserted within 1.5 above or below antecubital fossa, tip terminates below axilla Therapies 2-4 weeks ideally, if no complications may extend
MIDLINES/EXTENDED DWELL Peripheral venous access devices 3-8 inserted within 1.5 above or below antecubital fossa, tip terminates below axilla Therapies 2-4 weeks ideally, if no complications may extend
Administering Cytarabine to Children in the Community Setting
 Standard Operating Procedure 18 (SOP 18) Administering Cytarabine to Children in the Community Setting Why we have a procedure? Cytarabine is a chemotherapy drug which is prescribed for some children as
Standard Operating Procedure 18 (SOP 18) Administering Cytarabine to Children in the Community Setting Why we have a procedure? Cytarabine is a chemotherapy drug which is prescribed for some children as
CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES
 CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES Lauren E.B. Stone, MSN, RN, VA-BC Nurse Manager IV Team and Blood Donor Center Boston Children's Hospital
CHILDREN SUPPORTED BY MEDICAL TECHNOLOGY IN SCHOOLS: CARE AND MAINTENANCE OF CENTRAL VENOUS LINES Lauren E.B. Stone, MSN, RN, VA-BC Nurse Manager IV Team and Blood Donor Center Boston Children's Hospital
21 st Century Health Care Consultants
 21 st Century Health Care Consultants Presents 1 Investing in your Infusion Specialty Program Presented by: Rhonda Surgnier RN Becky Tolson RN David Kachel CRNI INFUSION THERAPY OBJECTIVES 2 At the completion
21 st Century Health Care Consultants Presents 1 Investing in your Infusion Specialty Program Presented by: Rhonda Surgnier RN Becky Tolson RN David Kachel CRNI INFUSION THERAPY OBJECTIVES 2 At the completion
Hickman line insertion and caring for your line
 Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE BLOOD CULTURE COLLECTION PROCEDURE (spe20) DATE: REVIEWED: PAGES: 6/10 9/18 1 of 6 PS1094 ISSUED FOR: Nursing/Lab RESPONSIBILITY: RN, LPN II, select
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE BLOOD CULTURE COLLECTION PROCEDURE (spe20) DATE: REVIEWED: PAGES: 6/10 9/18 1 of 6 PS1094 ISSUED FOR: Nursing/Lab RESPONSIBILITY: RN, LPN II, select
Northeast Hospitals Infection Control Policy and Procedure Manual
 Northeast Hospitals Infection Control Policy and Procedure Manual Subject: Prevention/Control of Healthcare Associated Infections (HAI) Date Effective: 8/07 Date Revised: 3/11 Key Contact: Infection Prevention
Northeast Hospitals Infection Control Policy and Procedure Manual Subject: Prevention/Control of Healthcare Associated Infections (HAI) Date Effective: 8/07 Date Revised: 3/11 Key Contact: Infection Prevention
Venepuncture, obtaining blood cultures and managing blood samples
 Venepuncture, obtaining blood cultures and managing blood samples Aims To ensure that students are able to demonstrate the safe and correct technique for venepuncture, obtaining blood cultures and managing
Venepuncture, obtaining blood cultures and managing blood samples Aims To ensure that students are able to demonstrate the safe and correct technique for venepuncture, obtaining blood cultures and managing
ENDOSCOPY MICROBIOLOGY ALERTS PROCEDURE STANDARD OPERATING PROCEDURE
 ENDOSCOPY MICROBIOLOGY ALERTS PROCEDURE STANDARD OPERATING PROCEDURE Version Number V1 Date of Issue December 2017 Reference Number Review Interval Approved By Name: Seamus Hussey Title: Chairperson Endoscopy
ENDOSCOPY MICROBIOLOGY ALERTS PROCEDURE STANDARD OPERATING PROCEDURE Version Number V1 Date of Issue December 2017 Reference Number Review Interval Approved By Name: Seamus Hussey Title: Chairperson Endoscopy
New research: Change peripheral intravenous catheters only as clinically
 Content page New research: Change peripheral intravenous catheters only as clinically indicated, not routinely. The results of a nurse led and nationally funded multicentre, randomised equivalence trial
Content page New research: Change peripheral intravenous catheters only as clinically indicated, not routinely. The results of a nurse led and nationally funded multicentre, randomised equivalence trial
About your PICC line. Information for patients Weston Park Hospital
 About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
ADMINISTRATION OF MEDICATED EYE DROPS PRIOR TO EYE EXAMINATION FOR NURSING STAFF IN THE OPHTHALMOLOGY DEPARTMENT
 ADMINISTRATION OF MEDICATED EYE DROPS PRIOR TO EYE EXAMINATION FOR NURSING STAFF IN THE OPHTHALMOLOGY DEPARTMENT Version Number V2 Date of Issue April 2018 Reference Number Review Interval Approved By
ADMINISTRATION OF MEDICATED EYE DROPS PRIOR TO EYE EXAMINATION FOR NURSING STAFF IN THE OPHTHALMOLOGY DEPARTMENT Version Number V2 Date of Issue April 2018 Reference Number Review Interval Approved By
Peripherally Inserted Central Catheter
 UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
1. Infection Control, Centers for Disease Control and Prevention (CDC). (2002). Guideline for hand hygiene in health-care settings
 HOSPITAL CORPSMAN SKILLS BASIC (HMSB) MAY 8 Checklist (PCL) Clinical Skill: Intravenous Therapy Circle One: Initial Evaluation Re-Evaluation Command: A. INTRODUCTION Upon successful completion of this
HOSPITAL CORPSMAN SKILLS BASIC (HMSB) MAY 8 Checklist (PCL) Clinical Skill: Intravenous Therapy Circle One: Initial Evaluation Re-Evaluation Command: A. INTRODUCTION Upon successful completion of this
IV 03 CRAIG HOSPITAL POLICY/PROCEDURE
 CRAIG HOSPITAL POLICY/PROCEDURE Approved: NPC, P&P 12/06; P&T 2/07; Effective Date: 10/78 IC, MEC 03/07; NPC, P&P 08/09; MEC 9/09 P&T 12/10; MEC, P&P 01/11, 04/11; NPC, P&P 06/12, 06/15, 12/15 ; NPC, P&T,
CRAIG HOSPITAL POLICY/PROCEDURE Approved: NPC, P&P 12/06; P&T 2/07; Effective Date: 10/78 IC, MEC 03/07; NPC, P&P 08/09; MEC 9/09 P&T 12/10; MEC, P&P 01/11, 04/11; NPC, P&P 06/12, 06/15, 12/15 ; NPC, P&T,
POLICY FOR ASEPTIC TECHNIQUE AND ASEPTIC NON TOUCH TECHNIQUE
 POLICY FOR ASEPTIC TECHNIQUE AND ASEPTIC NON TOUCH TECHNIQUE Please be aware that this printed version of the Policy may NOT be the latest version. Staff are reminded that they should always refer to the
POLICY FOR ASEPTIC TECHNIQUE AND ASEPTIC NON TOUCH TECHNIQUE Please be aware that this printed version of the Policy may NOT be the latest version. Staff are reminded that they should always refer to the
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Blood Culture Collection Policy SUMMARY
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Blood Culture Collection Policy Version No.: 1.2 Effective From: 14 December 2017 Expiry Date: 14 December 2020 Date Ratified: 08 December 2017 Ratified
The Newcastle upon Tyne Hospitals NHS Foundation Trust Blood Culture Collection Policy Version No.: 1.2 Effective From: 14 December 2017 Expiry Date: 14 December 2020 Date Ratified: 08 December 2017 Ratified
CLABSI: Beyond the Policy and Procedure
 CLABSI: Beyond the Policy and Procedure This course has been awarded one (1.0) contact hour. This course expires on July 31, 2017. Copyright 2014 by RN.com. All Rights Reserved. Reproduction and distribution
CLABSI: Beyond the Policy and Procedure This course has been awarded one (1.0) contact hour. This course expires on July 31, 2017. Copyright 2014 by RN.com. All Rights Reserved. Reproduction and distribution
Peripherally Inserted Central Catheter (PICC)
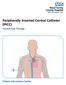 Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Peripherally inserted central catheter (PICC line) Information to accompany consent
 Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Peripherally inserted central catheter (PICC line) Information to accompany consent Exceptional healthcare, personally delivered What is a PICC line? PICC stands for peripherally inserted central venous
Chapter 10. medical and Surgical Asepsis. safe, effective Care environment. Practices that Promote Medical Asepsis
 chapter 10 Unit 1 Section Chapter 10 safe, effective Care environment safety and Infection Control medical and Surgical Asepsis Overview Asepsis The absence of illness-producing micro-organisms. Asepsis
chapter 10 Unit 1 Section Chapter 10 safe, effective Care environment safety and Infection Control medical and Surgical Asepsis Overview Asepsis The absence of illness-producing micro-organisms. Asepsis
Policy for the Care of Patients with Central Venous Catheters (CVC)
 Policy Type: Definition: Owner Group: Clinical Policy Operations Cli nic al G u ide lin e Clinical Policy Policy for the Care of Patients with Central Venous Catheters (CVC) Applicable To: Communication
Policy Type: Definition: Owner Group: Clinical Policy Operations Cli nic al G u ide lin e Clinical Policy Policy for the Care of Patients with Central Venous Catheters (CVC) Applicable To: Communication
ADMINISTRATION BY INJECTION POLICY INTRAVENOUS, INTRAMUSCULAR and SUBCUTANEOUS
 ADMINISTRATION BY INJECTION POLICY INTRAVENOUS, INTRAMUSCULAR and SUBCUTANEOUS This policy should be read in conjunction with the Syringe Driver Policy and the Medicines Policy Version: 6 Date of Issue:
ADMINISTRATION BY INJECTION POLICY INTRAVENOUS, INTRAMUSCULAR and SUBCUTANEOUS This policy should be read in conjunction with the Syringe Driver Policy and the Medicines Policy Version: 6 Date of Issue:
Objectives. Vessel Health and Preservation: Disclosure. Ms. Moureau has disclosed the following: Angiodynamics, Genentech
 Vessel Health and Preservation: What is the Right Line for the Right Patient at the Right Time? Nancy Moureau, BSN, RN, CRNI, CPUI, VA-BC This program is sponsored by Teleflex Saxe Communications 2012
Vessel Health and Preservation: What is the Right Line for the Right Patient at the Right Time? Nancy Moureau, BSN, RN, CRNI, CPUI, VA-BC This program is sponsored by Teleflex Saxe Communications 2012
Kevin Chapman Tissue Viability - Modern Matron
 Tissue Viability Policy - Practice Guidance Note Aseptic Non Touch Technique V01 Date issued Issue 1 Jan 16 Planned review January 2019 TV-PGN-03 Part of NTW(C)18 Tissue Viability Policy Author/Designation
Tissue Viability Policy - Practice Guidance Note Aseptic Non Touch Technique V01 Date issued Issue 1 Jan 16 Planned review January 2019 TV-PGN-03 Part of NTW(C)18 Tissue Viability Policy Author/Designation
Peripherally Inserted Central Catheter (PICC Line)
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Care of Your Peripherally Inserted Central Catheter
 Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
PC EP 4; PC EP 7. (Outpatient Only) If nutritional screen positive, plans for follow-up documented.
 Dialysis - Patient Documentation & Observation Tool Data Definition Tool This audit is to be completed by the manager or designee on a monthly basis. "Dialysis - Patient Documentation & Observation Tool"
Dialysis - Patient Documentation & Observation Tool Data Definition Tool This audit is to be completed by the manager or designee on a monthly basis. "Dialysis - Patient Documentation & Observation Tool"
NURSING GUIDELINE ON PERFORMING A WOUND SWAB
 NURSING GUIDELINE ON PERFORMING A WOUND SWAB Version Number 3 Date of Issue 9 th January 2014 Reference Number Review Interval NGPWS-12-2013-CH-V3 3 yearly or more regularly if international evidence indicates
NURSING GUIDELINE ON PERFORMING A WOUND SWAB Version Number 3 Date of Issue 9 th January 2014 Reference Number Review Interval NGPWS-12-2013-CH-V3 3 yearly or more regularly if international evidence indicates
Lincolnshire Partnership NHS Foundation Trust (LPFT) Title of Policy
 Lincolnshire Partnership NHS Foundation Trust (LPFT) Title of Policy REF: 7n DOCUMENT VERSION CONTROL Document Type and Title: Correct Use of Personal Protective Environment Authorised Document Folder:
Lincolnshire Partnership NHS Foundation Trust (LPFT) Title of Policy REF: 7n DOCUMENT VERSION CONTROL Document Type and Title: Correct Use of Personal Protective Environment Authorised Document Folder:
A new option for you. What is the Primo Port?
 Totally Implantable Port Patient Information Synchronizing Medical Innovation with Global Markets A new option for you Your treatment may require frequent injections of medicine, or other IV fluids directly
Totally Implantable Port Patient Information Synchronizing Medical Innovation with Global Markets A new option for you Your treatment may require frequent injections of medicine, or other IV fluids directly
Medication Administration Using the Home Pump (Eclipse)
 Medication Administration Using the Home Pump (Eclipse) Phone Number: Nurse/Contact: Receiving IV Therapy in the Home Your doctor has ordered for you to receive your IV medication at home. Receiving IV
Medication Administration Using the Home Pump (Eclipse) Phone Number: Nurse/Contact: Receiving IV Therapy in the Home Your doctor has ordered for you to receive your IV medication at home. Receiving IV
B.S.N., M.S., CRNI, CNSN
 Central Line Infection: Improving our Surveillance, Treatment and Prevention in the Home Setting By Susan Poole, B.S.N., M.S., CRNI, CNSN For as long as patients have had central venous catheters (CVCs),
Central Line Infection: Improving our Surveillance, Treatment and Prevention in the Home Setting By Susan Poole, B.S.N., M.S., CRNI, CNSN For as long as patients have had central venous catheters (CVCs),
Patricia Church, MSN, RN, PCNS-BC, CPON Bernice Mowery, PhD, PNP, RN
 Beyond the Bundle: Strategies to Prevent Catheter Related Blood Stream Infections in a Pediatric Oncology In- Patient Unit Patricia Church, MSN, RN, PCNS-BC, CPON Bernice Mowery, PhD, PNP, RN Objectives
Beyond the Bundle: Strategies to Prevent Catheter Related Blood Stream Infections in a Pediatric Oncology In- Patient Unit Patricia Church, MSN, RN, PCNS-BC, CPON Bernice Mowery, PhD, PNP, RN Objectives
INFECTION CONTROL SURVEYOR WORKSHEET
 Attachment 2 Exhibit 351 INFECTION CONTROL SURVEYOR WORKSHEET Instructions: The following is a list of items that must be assessed during the on-site survey, in order to determine compliance with the infection
Attachment 2 Exhibit 351 INFECTION CONTROL SURVEYOR WORKSHEET Instructions: The following is a list of items that must be assessed during the on-site survey, in order to determine compliance with the infection
GUIDELINE ON ROUTINE TRACHEOSTOMY TUBE CHANGE GRTTC RMSF-V2
 GUIDELINE ON ROUTINE TRACHEOSTOMY TUBE CHANGE Version Number V2 Date of Issue July 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Development Coordinator
GUIDELINE ON ROUTINE TRACHEOSTOMY TUBE CHANGE Version Number V2 Date of Issue July 2017 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Development Coordinator
Infection Prevention and Control. Approval Process. Executive Director of Nursing and Operations, DIPC. Distribution IPC Governance Meeting Members
 Title Trust Ref No 766-37839 Local Ref (optional) Main points the document covers Who is the document aimed at? Author Approved by (Committee/Director) Document Details Aseptic Technique Policy This policy
Title Trust Ref No 766-37839 Local Ref (optional) Main points the document covers Who is the document aimed at? Author Approved by (Committee/Director) Document Details Aseptic Technique Policy This policy
Andrew Kingsley, Clinical Manager Infection Control & Tissue Liability
 Report to Trust Board Date 22nd July 2008 Agenda Item Title Sponsor Prepared by Presented by P2 Intravascular Device Policy Carolyn Mills, Director of Nursing Andrew Kingsley, Clinical Manager Infection
Report to Trust Board Date 22nd July 2008 Agenda Item Title Sponsor Prepared by Presented by P2 Intravascular Device Policy Carolyn Mills, Director of Nursing Andrew Kingsley, Clinical Manager Infection
Healthcare-Associated Infections: What all doctors must know and do
 Policy Group on Healthcare-Associated Infection Healthcare-Associated Infections: What all doctors must know and do June 2011 1 2 The Importance of Healthcare-Associated Infections 1(a-d) Healthcare associated
Policy Group on Healthcare-Associated Infection Healthcare-Associated Infections: What all doctors must know and do June 2011 1 2 The Importance of Healthcare-Associated Infections 1(a-d) Healthcare associated
Giving Intravenous (IV) Nutrition Through a Central Line with a CADD Pump
 Home Care Services Giving Intravenous (IV) Nutrition Through a Central Line with a CADD Pump Receiving medicine and supplies When you receive a shipment, make sure you have the correct medicine and supplies.
Home Care Services Giving Intravenous (IV) Nutrition Through a Central Line with a CADD Pump Receiving medicine and supplies When you receive a shipment, make sure you have the correct medicine and supplies.
Department Policy. Code: D: MM Entity: Fairview Pharmacy Services. Department: Fairview Home Infusion. Manual: Policy and Procedure Manual
 Department Policy Code: D: MM-5615 Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Chemotherapy Purpose: Ensure
Department Policy Code: D: MM-5615 Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Chemotherapy Purpose: Ensure
PICU tracheostomy protocol
 PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
Section Z - Blood Culture Policy. Version 4
 Section Z - Blood Culture Policy Version 4 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you
Section Z - Blood Culture Policy Version 4 Important: This document can only be considered valid when viewed on the Trust s Intranet. If this document has been printed or saved to another location, you
Insertion of a Hickman Line Information for parents and carers
 Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Oxford University Hospitals NHS Trust Children s Hospital, Kamran s Ward Insertion of a Hickman Line Information for parents and carers This leaflet explains: what a Hickman line is why one is necessary
Central Venous Access Devices (CVAD) Management (Adult) Resource Package
 Nursing and Midwifery Professional Stream 121/RP Vascular Access Surveillance and Education Central Venous Access Devices (CVAD) Management (Adult) Resource Package Completion of this package, if relevant
Nursing and Midwifery Professional Stream 121/RP Vascular Access Surveillance and Education Central Venous Access Devices (CVAD) Management (Adult) Resource Package Completion of this package, if relevant
Outpatient intravenous antibiotic therapy
 Oxford Centre for Respiratory Medicine Churchill Hospital Outpatient intravenous antibiotic therapy Patient Held Record Contents Page Introduction for patients 3 Introduction for the doctor or nurse 3
Oxford Centre for Respiratory Medicine Churchill Hospital Outpatient intravenous antibiotic therapy Patient Held Record Contents Page Introduction for patients 3 Introduction for the doctor or nurse 3
