Donald Robinson, MD, is a family
|
|
|
- Heather Sullivan
- 6 years ago
- Views:
Transcription
1 GETTING REWARDS FOR YOUR RESULTS: PAY-FOR-PERFORMANCE PROGRAMS More and more health plans are paying physicians for quality. Here s what you need to know about these, and how to get involved. Scott Endsley MD, MSc, Margaret Kirkegaard, MD, MPH, Geoffrey Baker and Anita C. Murcko, MD ILLUSTRATION BY RANDY LYHUS Donald Robinson, MD, is a family physician in private practice in Hamburg, N.Y., a blue-collar suburb of Buffalo, and has been practicing medicine since For the past five years, he has participated with the three largest HMOs in the Buffalo area in pay-for-performance. From one managed care plan alone, Independent Health, he earned $20,000 in incentive bonus payments in 2002 for achieving targets in five areas: patient satisfaction, access to care, emergency room utilization, mammography rates and colorectal cancer screening rates. To meet the quality targets of the managed care plans with which he works, Robinson has had to shift his way of practicing medicine and cultivate a new mindset and skill set. He has developed computerized patient registries to track his patients. He employs two part-time staffers to send reminder notices to patients and maintain his patient registry. He has also partnered with his managed care plans, which provide him with lists of his patients in need of services as well as flow sheets, guidelines, patient education materials and other tools. Robinson monitors his own preventive care outcomes, such as colonoscopy and mammography rates, and has dedicated special attention to improving the Dr. Endsley, a family physician, is medical director of system design for the Health Services Advisory Group in Phoenix. Dr. Kirkegaard is with the Department of Family Medicine, Chicago College of Osteopathic Medicine, Midwestern University, in Downers Grove, Ill. Geoffrey Baker is with Med-Vantage Inc., San Francisco. Dr. Murcko is chief medical officer of the Health Services Advisory Group. Conflicts of interest: none reported. Downloaded from the Family Practice Management Web site at March 2004 Copyright American /fpm FAcademy A M I L Y of P RFamily A C T IPhysicians. C E M A N For A G the E M private, E N T 45 noncommercial use of one individual user of the Web site. All other rights reserved. Contact copyrights@aafp.org for copyright questions and/or permission requests.
2 SPEEDBAR Pay-for-performance helped family physician Donald Robinson earn $20,000 in bonuses for achieving specific quality targets. Improving quality of care requires a shift in the way physicians are accustomed to practicing medicine. Current payment methods provide physicians with little incentive to improve quality of care and may even prevent such actions, according to the Institute of Medicine. More than 35 health plans representing 30 million members now offer pay-for-performance, and those numbers are expected to grow. outcomes of his adult patients with diabetes and his pediatric patients with asthma. These changes in his practice have paid off. He receives bonuses from his managed care plans that have increased his earnings by approximately 6 percent. This additional money has enabled him to hire more staff, build and maintain a patient registry (the centerpiece of his practice improvement efforts), conduct a series of quality improvement projects in his practice and take home more money each year. He admits practice improvement is hard work, but it s worth the effort. It s not the profit that interests me, he says. It s the quality. I feel like I am stamping out disease. The basics of pay for performance Current payment methods provide physicians with little incentive to improve quality of care. Even among health professionals motivated to provide the best care possible, the structure of payment incentives may not facilitate the actions needed to systematically improve the quality of care, and may even prevent such actions, according to the Institute of Medicine (IOM). 1 The IOM has called for broad-based reform of the health care payment system and strengthening of existing payment methods that provide physicians with greater financial incentives for quality improvement. More than 35 health plans representing 30 million members now offer pay-forperformance (see the table on page 47). Based on current growth trends, at least 80 health plans are expected to offer such by 2006, covering some 60 million members. 2 Pay-for-performance have four essential elements that physicians should be aware of before participating. (See the tool for evaluating pay-for-performance on page 49.) The first element is the set of performance measures being used. Performance measures fall into several categories: Utilization/cost management (e.g., average number of emergency department visits per patient per year), Clinical quality/effectiveness (e.g., the percentage of patients with asthma on controller medications), KEY POINTS Thirty-five health plans covering some 30 million patients now offer pay-for-performance. Participating physicians receive an average of 10 percent of annual income by meeting specified quality measures. Practices that succeed at pay-for-performance continuously experiment with new ideas for improving their care, service and efficiency. Patient satisfaction (e.g., the percentage of patients who would recommend the physician to a family member or friend), Administrative (e.g., the practice s level of information technology), Patient safety (e.g., the percentage of patients questioned about allergic drug reactions). These measures may be developed locally by the health plan or purchaser or may come from nationally recognized sources, such as Health Plan Employer Data and Information Set HEDIS ( /hedis/index.htm) or the Consumer Assessment of Health Plans ( ahcpr.gov/qual/ cahps/dept1.htm). A recent study by Med-Vantage found that 71 percent of health plans with pay-for-performance use some subset of HEDIS measures. 2 The second element to be aware of is how the health plan collects the performance data. Performance data can be derived from the health plan s administrative data, claims data for medical services or encounter data from the physician s practice. Administrative and claims data have the advantage of ease of collection for the health plan; encounter data has the advantage of greater clinical detail, which improves validity of the measurement but can be difficult for physician offices to supply. Web-based electronic health records would enable family physicians to engage health plans more actively in performance measurement; however, some groups are finding creative solutions even without fully functioning electronic health records. For example, the Employers Coalition on Current payment methods provide physicians with little incentive to improve quality of care. 46 F A M I L Y P R A C T I C E M A N A G E M E N T /fpm March 2004
3 P A Y F O R P E R F O R M A N C E HEALTH PLANS OFFERING PAY-FOR-PERFORMANCE PROGRAMS SPEEDBAR More than 35 health plans, covering some 30 million members, now offer pay-for-performance. Plan Name Aetna Anthem Blue Cross Blue Shield of New Hampshire Anthem Blue Cross Blue Shield of Ohio Anthem Blue Cross Blue Shield of Kentucky Program Name, and Quality Enhancement Common performance measures focus on utilization, clinical quality, patient satisfaction, administrative issues and patient safety. Blue Cross Blue Shield of Alabama Blue Cross Blue Shield of Hawaii (HMSA) Quality and Service Recognition Program Blue Cross Blue Shield of Illinois Blue Cross Blue Shield of Massachusetts Blue Cross Blue Shield of Michigan Blue Cross Blue Shield of Missouri Blue Cross Blue Shield of Western New York HMO Blue Group Performance Incentive Program and Rewarding Results Physician Group Partners Program Quality Incentives A majority of health plans with pay-forperformance use some subset of HEDIS measures. Blue Cross of California and PPO Physician Quality and Incentive Program Blue Shield of California Care First Blue Cross Blue Shield of the Mid-Atlantic Cigna Healthcare of California Empire Blue Cross Blue Shield of New York Excellus Blue Cross Blue Shield of Rochester Harvard Pilgrim Healthcare Health Partners (Minnesota) Health Net of California Primary Care Physician Recognition Program Rewarding Results and Value of Care (IPA) Quality Incentives and Outcomes Recognition Program Performance data can be derived from the health plan s administrative data, claims data for medical services or encounter data from the physician s practice. Highmark Blue Cross Blue Shield of Pennsylvania Quality Incentive Payment System HIP of New York PCP Incentive Plan Horizon Blue Cross Blue Shield of New Jersey Humana Independence Blue Cross of Pennsylvania Independent Health of Buffalo, N.Y. Massachusetts Health Quality Partners PacifiCare Presbyterian Health Plan of New Mexico Priority Health Quality Incentive Payment System Quality Management Incentive Awards Program Rewarding Results Physician Incentive Program Promina Cigna (Georgia) Reward for Quality Touchpoint Healthplan of Wisconsin Trigon Blue Cross Blue Shield of Virginia Performance Extra Tufts Health Plan of Massachusetts United Healthcare Univera/Excellus Blue Cross Blue Shield of Buffalo Western Health Advantage Encounter data offer greater clinical detail, which improves validity of the measurement, but can be difficult for physician offices to supply. March /fpm F A M I L Y P R A C T I C E M A N A G E M E N T 47
4 SPEEDBAR Health plans compare physicians either to others participating in the program or to national benchmarks. The two most common incentives are quality bonuses and reimbursement at risk (or withholds). Quality bonuses are preferable for physicians, as they involve no financial risk. Payments for performance range from 1 percent to 40 percent of a practice s total annual revenue, with an average of a 10-percent bonus or withhold. Health (ECOH) in Rockford, Ill., has distributed to physicians a software system called Project in a Box, developed by the Illinois quality improvement organization ( The software helps standardize the collection of data on diabetes and preventive care, which are used in ECOH s pay-for-performance program. Third, physicians should understand how the health plan determines its performance targets or benchmarks. Some compare the IMPROVEMENT IDEAS FROM THE FPM ARCHIVES To achieve the required outcomes for pay-for-performance, your practice may need to improve its current care processes. You can find improvement ideas through the Family Practice Management archives, available online at Quality improvement Holding the Gains in Quality Improvement. Giovino JM. May 1999: A Team Approach to Quality Improvement. Schwarz M, Landis SE, Rowe JE. April 1999: Quality Improvement: First Steps. Coleman MT, Endsley S. March 1999: System redesign The KISS Principle in Family Practice: Keep It Simple and Systematic. Solberg LI. July/August 2003: Starting a Revolution in Office-Based Care. White B. October 2001: Chronic disease care improvement Thirteen Months of Quality Improvement: Did it Work? White B. January 2001: Making Diabetes Checkups More Fruitful. White B. September 2000: Using Flow Sheets to Improve Diabetes Care. White B. June 2000: Helping Patients Take Charge of Their Chronic Illnesses. Funnell MM. March 2000: Building a Patient Registry From the Ground Up. White B. November/December 1999: Improving Chronic Disease Care in the Real World: A Step-by-Step Approach. White B. October 1999: Practice measurement/assessment Putting Measurement Into Practice With a Clinical Instrument Panel. Endsley S. February 2003: The Family Practice Management Practice Self-Test. Edsall R, Backer L, Bush J, White B, Maresh O, Hocker K. February 2001: participant group to itself and establish a defined subset as the target (e.g., two standard deviations from the mean, the top quartile or the 90th percentile). Others compare the participant group to an external benchmark (e.g., data from other health plans, national surveys or specialty society goals). Finally, physicians should understand how the health plan will reward them for meeting or exceeding performance targets. Typically, health plans combine a physician s performance ratings on individual measures into a single value to determine whether the physician qualifies for rewards. A number of financial incentives exist, 3 but the two most common incentives are quality bonuses (in which physicians receive an annual payment for meeting performance targets) and reimbursement at risk (in which the health plan withholds 5 percent to 10 percent of reimbursement and pays it back to the physician for meeting minimum requirements). The most desirable will use bonuses, which physicians prefer because no financial risk is involved. The Med-Vantage study of pay-forperformance found that payments for performance ranged from 1 percent to 40 percent of a practice s total annual revenue, with an average of a 10-percent bonus or withhold. National demonstration projects Currently, two high-profile national demonstration projects are in the early stages of testing whether pay-for-performance significantly contribute to improved health care outcomes. Rewarding Results is an $8.8 million initiative of the Robert Wood Johnson Foundation and the California HealthCare Foundation. The grantees include Blue Cross Blue Shield of Michigan, Blue 48 F A M I L Y P R A C T I C E M A N A G E M E N T /fpm March 2004
5 P A Y F O R P E R F O R M A N C E PAY-FOR-PERFORMANCE EVALUATION TOOL SPEEDBAR The spreadsheet shown here can help you evaluate pay-for-performance available to you. The best will offer financial bonuses of adequate size to be worthwhile, incentives based on welltested and valid measures, and assistance in collecting data and improving care. To download a working copy of the spreadsheet, visit this article online at Two high-profile national demonstration projects are testing whether pay-for-performance contribute to improved health care outcomes. The author s pay-forperformance evaluation tool can help you judge whether a program is worth your consideration. The best pay-for-performance will include financial incentives of adequate size to be worthwhile, incentives based on well-tested and valid measures, and health plan assistance in improving care. Cross of California, Excellus Health Plan, Integrated Healthcare Association (IHA) and Massachusetts Health Quality Partners. The largest of these is IHA, a coalition of seven health care plans (Aetna of California, Blue Cross of California, Blue Shield of California, CIGNA Healthcare of California, Health Net of California, PacifiCare and Western Health Advantage). In early 2003, participating physicians submitted data on patient satisfaction, investment in information technology and six clinical indicators: childhood immunization status, cervical cancer screening, breast cancer screening, use of appropriate medication for people with asthma, LDL- C screening after cardiovascular event, and A 1c testing in diabetes. The first bonuses will be paid in mid-2004., funded by Robert Wood Johnson and supported by the Center for Medicare & Medicaid Services, is an initiative of large employers (General Electric Company, Procter and Gamble, Verizon Communications, Raytheon Company, UPS, Humana, Ford Motor Company and Cincinnati Children s Hospital Medical Center), health plans (Aetna, Anthem Blue Cross Blue Shield of Ohio and Kentucky, Blue Cross Blue Shield of Illinois, Alabama and Massachusetts, Tufts Health Plan, United Healthcare, Harvard Pilgrim Your decision to participate in pay-forperformance will also depend on whether you have the commitment, staff and resources to devote to improving quality of care in your practice. March /fpm F A M I L Y P R A C T I C E M A N A G E M E N T 49
6 SPEEDBAR If your health plans do not currently offer payfor-performance, let them know you are interested and look for opportunities to shape these in your area. Pay-for-performance are not one size fits all. To reach your performance goals, look for improvement opportunities sponsored by reputable organizations or initiate your own. Most importantly, start improving your practice right now; don t put it off until tomorrow. Healthcare and Humana) and physician groups in the three large urban markets of Boston, Cincinnati and Louisville. It seeks improvements in three areas: diabetes care, cardiovascular care and patient care management systems. The diabetes component of this initiative is modeled on the American Diabetes Association/National Committee for Quality Assurance s Physician Recognition Program. Incentives of up to 10 percent of annual income will be paid to physicians who achieve targets in these three areas. Getting involved with pay for performance If you are ready to change your mind-set and skill set, pay-for-performance are a rapidly growing opportunity to work on your practice, deliver the highest attainable quality of care to your patients and strengthen your financial performance. As Dr. Robinson described, attaining new levels of performance in your practice can be hard work but well worth the effort. Step 1: Decide whether pay for performance is right for you. Do you have the commitment, staff and resources to devote to improving quality of care in your practice? Is your practice free from relationships that would impair your improvement efforts (e.g., being owned by a larger health system not committed to quality improvement)? Are the typical pay-for-performance measures applicable to your patient population (e.g., pneumococcal immunization rates in a younger population)? Does your practice have adequate information systems or data collection capacity, or are you willing to acquire it? Do you have the patience to achieve the outcomes that reap higher financial bonuses? Don t underestimate how much hard work it will take. Step 2: Look for health plans offering pay-for-performance. The table on page 47 lists more than 35 health plans that reported pay-for-performance in the Med-Vantage study. Discuss these with representatives from the health plans with which you currently contract, and talk with your colleagues about their experiences. If your health plans do not currently offer pay-for-performance, let them know you are interested 50 F A M I L Y P R A C T I C E M A N A G E M E N T /fpm March 2004 and look for opportunities to shape these in your area. Step 3: Evaluate the pay-for-performance available to you. Pay-for-performance are not one size fits all. Available in your local health care market may vary and may not fit your practice s needs and capabilities for performance improvement. Use the spreadsheet tool shown on page 49 to assess how a health plan s pay-for-performance program fits with your practice s needs. The key criteria to look for include financial incentives of adequate size to be worthwhile, incentives based on welltested and valid measures, and health plan assistance in improving care. Step 4: Find improvement opportunities to help you reach your performance goals. Opportunities include improvement projects and collaboratives sponsored by local health plans, national health care organizations such as the AAFP ( or the Institute for Healthcare Improvement ( or your state quality improvement organization (for a directory, visit qio.jsp?pageid=4). You can also initiate your own improvement projects. Continuously look for new ideas that will help you improve patient care, service or efficiency. (See the FPM reading list on page 48 for some ideas.) Test the ideas on a small scale, adapt them as needed and keep only what works. When you find good ideas, steal shamelessly and share openly. Step 5: Get started now. When you find good ideas, steal shamelessly and share openly. Send comments to fpmedit@aafp.org. 1. Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: The National Academies Press; National Study of Provider Pay-for-Performance Programs: Lessons Learned. San Francisco: Med-Vantage Inc.; Bailit Health Purchasing, LLC. Provider Incentive Models for Improving Quality of Care. Washington, DC: National Health Care Purchasing Institute; 2002.
California Pay for Performance: A Case Study with First Year Results. Tom Williams Integrated Healthcare Association (IHA) March 17, 2005
 California Pay for Performance: A Case Study with First Year Results Tom Williams Integrated Healthcare Association (IHA) March 17, 2005 Agenda National Perspective California Program Overview Data Collection
California Pay for Performance: A Case Study with First Year Results Tom Williams Integrated Healthcare Association (IHA) March 17, 2005 Agenda National Perspective California Program Overview Data Collection
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction
 FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association 1 Agenda Incentives in PPS: what does
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association 1 Agenda Incentives in PPS: what does
10/6/2017. FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction. Agenda. Incentives in PPS: what does excludable mean?
 FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association Agenda Incentives in PPS: what does excludable
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association Agenda Incentives in PPS: what does excludable
National Survey of Physician Organizations and the Management of Chronic Illness II (Independent Practice Associations)
 If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
Holding the Line: How Massachusetts Physicians Are Containing Costs
 Holding the Line: How Massachusetts Physicians Are Containing Costs 2017 Massachusetts Medical Society. All rights reserved. INTRODUCTION Massachusetts is a high-cost state for health care, and costs continue
Holding the Line: How Massachusetts Physicians Are Containing Costs 2017 Massachusetts Medical Society. All rights reserved. INTRODUCTION Massachusetts is a high-cost state for health care, and costs continue
Money and Members: Pay for Performance in a Medicaid Program
 Money and Members: Pay for Performance in a Medicaid Program IHA National Pay for Performance Summit March 9, 2010 Greg Buchert, MD, MPH Chief Operating Officer 1 AGENDA CalOptima Overview CalOptima P4P
Money and Members: Pay for Performance in a Medicaid Program IHA National Pay for Performance Summit March 9, 2010 Greg Buchert, MD, MPH Chief Operating Officer 1 AGENDA CalOptima Overview CalOptima P4P
Pay for Performance and the Integrated Healthcare Association. Tom Williams Dolores Yanagihara April 23, 2007
 Pay for Performance and the Integrated Healthcare Association Tom Williams Dolores Yanagihara April 23, 2007 Agenda Why Community Collaboration? Case Study: California P4P Program Structure Program Governance
Pay for Performance and the Integrated Healthcare Association Tom Williams Dolores Yanagihara April 23, 2007 Agenda Why Community Collaboration? Case Study: California P4P Program Structure Program Governance
Physician Compensation for Quality Within Groups: Complying with Stark and State of The Art. Traditional Physician Compensation Models
 Physician Compensation for Quality Within Groups: Complying with Stark and State of The Art Alice G. Gosfield, Esq. Medicare and Medicaid Institute American Health Lawyers Association March 29, 2012 c.2012,
Physician Compensation for Quality Within Groups: Complying with Stark and State of The Art Alice G. Gosfield, Esq. Medicare and Medicaid Institute American Health Lawyers Association March 29, 2012 c.2012,
Intelligent Healthcare. Intelligent Solutions for Achieving Clinical Integration & Accountable Care. Case Study: Advocate Physician Partners
 Solutions for Achieving Clinical Integration & Accountable Care Case Study: Advocate Physician Partners Provide physicians with the right information, and they will make the right decisions. Paul Katz,
Solutions for Achieving Clinical Integration & Accountable Care Case Study: Advocate Physician Partners Provide physicians with the right information, and they will make the right decisions. Paul Katz,
MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE
 MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE Randa Deaton, MA Corporate Director, UAW/Ford Community Healthcare Initiative Co-Executive Director, Kentuckiana Health Collaborative 1 WHO is the KHC?
MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE Randa Deaton, MA Corporate Director, UAW/Ford Community Healthcare Initiative Co-Executive Director, Kentuckiana Health Collaborative 1 WHO is the KHC?
Brave New World: The Effects of Health Reform Legislation on Hospitals. HFMA Annual National Meeting, Las Vegas, Nevada
 Brave New World: The Effects of Health Reform Legislation on Hospitals HFMA Annual National Meeting, Las Vegas, Nevada Highlights of PPACA Requires most Americans to have health insurance Expands coverage
Brave New World: The Effects of Health Reform Legislation on Hospitals HFMA Annual National Meeting, Las Vegas, Nevada Highlights of PPACA Requires most Americans to have health insurance Expands coverage
Issue Brief February 2015 Affordable Care Act Funding:
 CENTER FOR HEALTHCARE RESEARCH & TRANSFORMATION Issue Brief February 2015 Affordable Care Act Funding: An Analysis of Grant Programs under Health Care Reform FY2010- The Patient Protection and Affordable
CENTER FOR HEALTHCARE RESEARCH & TRANSFORMATION Issue Brief February 2015 Affordable Care Act Funding: An Analysis of Grant Programs under Health Care Reform FY2010- The Patient Protection and Affordable
1998 AAPA Census Report
 Section I. General Information about Respondents Table 1. Distribution of Respondents by Sex Respondents... 15716 100.0% Male... 7413 47.2% Female... 8303 52.8% Table 2. Distribution of Respondents by
Section I. General Information about Respondents Table 1. Distribution of Respondents by Sex Respondents... 15716 100.0% Male... 7413 47.2% Female... 8303 52.8% Table 2. Distribution of Respondents by
HOME HEALTH AIDE TRAINING REQUIREMENTS, DECEMBER 2016
 BACKGROUND HOME HEALTH AIDE TRAINING REQUIREMENTS, DECEMBER 2016 Federal legislation (42 CFR 484.36) requires that Medicare-certified home health agencies employ home health aides who are trained and evaluated
BACKGROUND HOME HEALTH AIDE TRAINING REQUIREMENTS, DECEMBER 2016 Federal legislation (42 CFR 484.36) requires that Medicare-certified home health agencies employ home health aides who are trained and evaluated
ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM. Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017
 ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017 1 DISCLAIMER The enclosed materials are highly sensitive, proprietary and confidential.
ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017 1 DISCLAIMER The enclosed materials are highly sensitive, proprietary and confidential.
1 Title Improving Wellness and Care Management with an Electronic Health Record System
 HIMSS Stories of Success! Graybill Medical Group 1 Title Improving Wellness and Care Management with an Electronic Health Record System 2 Background Knowledge It is widely understood that providers wellness
HIMSS Stories of Success! Graybill Medical Group 1 Title Improving Wellness and Care Management with an Electronic Health Record System 2 Background Knowledge It is widely understood that providers wellness
When Aetna recently agreed to stop bundling
 Same-Day E/M Services: What to Do When a Health Plan Won t Pay These ideas will help you deal with the difficult consequences of this common policy. Cindy Hughes, CPC When Aetna recently agreed to stop
Same-Day E/M Services: What to Do When a Health Plan Won t Pay These ideas will help you deal with the difficult consequences of this common policy. Cindy Hughes, CPC When Aetna recently agreed to stop
A legacy of primary care support underscores Priority Health s leadership in accountable care
 Priority Health has been at the forefront of supporting primary care, driving accountability, improving quality and improving care for patients. A legacy of primary care support underscores Priority Health
Priority Health has been at the forefront of supporting primary care, driving accountability, improving quality and improving care for patients. A legacy of primary care support underscores Priority Health
Patient-Centered Medical Home Best Practices: Case Study Examples
 Patient-Centered Medical Home Best Practices: Case Study Examples Mona Chitre, PharmD, CGP Director of Clinical Services, Strategy, and Policy FLRx Pharmacy Management Excellus Health Plans Disclosures
Patient-Centered Medical Home Best Practices: Case Study Examples Mona Chitre, PharmD, CGP Director of Clinical Services, Strategy, and Policy FLRx Pharmacy Management Excellus Health Plans Disclosures
The Pennsylvania Chronic Care Initiative
 The Pennsylvania Chronic Care Initiative Richard L. Snyder, M.D. Senior Vice President Chief Medical Officer Independence Blue Cross William J. Warning II, M.D. Program Director Crozer-Keystone Family
The Pennsylvania Chronic Care Initiative Richard L. Snyder, M.D. Senior Vice President Chief Medical Officer Independence Blue Cross William J. Warning II, M.D. Program Director Crozer-Keystone Family
Table 4.2c: Hours Worked per Week for Primary Clinical Employer by Respondents Who Worked at Least
 CONTENTS INTRODUCTION HIGHLIGHTS OF NATIONAL STATISTICS SECTION 1: CHARACTERISTICS OF 2009 AAPA CENSUS RESPONDENTS Table 1.1: Number and Percent Distribution of Census Respondents by State Where Employed...
CONTENTS INTRODUCTION HIGHLIGHTS OF NATIONAL STATISTICS SECTION 1: CHARACTERISTICS OF 2009 AAPA CENSUS RESPONDENTS Table 1.1: Number and Percent Distribution of Census Respondents by State Where Employed...
Improving Care for Dual Eligibles through Health IT
 Los Angeles, October 31, 2012 Presentation Improving Care for Dual Eligibles through Health IT The National Dual Eligibles Summit Duals Market is sizable Medicare and Medicaid Populations Medicaid Total
Los Angeles, October 31, 2012 Presentation Improving Care for Dual Eligibles through Health IT The National Dual Eligibles Summit Duals Market is sizable Medicare and Medicaid Populations Medicaid Total
Valuing the Invaluable: A New Look at State Estimates of the Economic Value of Family Caregiving (Data Update)
 Valuing the Invaluable: A ew Look at State Estimates of the Economic Value of Family Caregiving (Data Update) This update includes comparisons to FY 2006 Medicaid. At the time of the original release,
Valuing the Invaluable: A ew Look at State Estimates of the Economic Value of Family Caregiving (Data Update) This update includes comparisons to FY 2006 Medicaid. At the time of the original release,
Transforming Physician Practices: Evolution of ACOs in California. National Association of ACOs - Washington, DC October 2015
 Transforming Physician Practices: Evolution of ACOs in California National Association of ACOs - Washington, DC October 2015 Integrated Healthcare Association Statewide multi-stakeholder leadership group
Transforming Physician Practices: Evolution of ACOs in California National Association of ACOs - Washington, DC October 2015 Integrated Healthcare Association Statewide multi-stakeholder leadership group
2001 AAPA Physician Assistant Census Report 1. Respondents % Male % Female %
 1 Section I. Personal Characteristics of Respondents* Table 1. Distribution of Respondents by Sex Respondents... 19786 100.0% Male... 8603 43.5% Female... 11183 56.5% Table 2. Distribution of Respondents
1 Section I. Personal Characteristics of Respondents* Table 1. Distribution of Respondents by Sex Respondents... 19786 100.0% Male... 8603 43.5% Female... 11183 56.5% Table 2. Distribution of Respondents
As part of the Patient Protection and Affordable Care Act
 CENTER FOR HEALTHCARE RESEARCH & TRANSFORMATION Issue Brief February 2016 Affordable Care Act Funding: An Analysis of Grant Programs under Health Care Reform FY2010-FY2015 Spending Provisions...2 Spending
CENTER FOR HEALTHCARE RESEARCH & TRANSFORMATION Issue Brief February 2016 Affordable Care Act Funding: An Analysis of Grant Programs under Health Care Reform FY2010-FY2015 Spending Provisions...2 Spending
 3+ 3+ N = 155, 442 3+ R 2 =.32 < < < 3+ N = 149, 685 3+ R 2 =.27 < < < 3+ N = 99, 752 3+ R 2 =.4 < < < 3+ N = 98, 887 3+ R 2 =.6 < < < 3+ N = 52, 624 3+ R 2 =.28 < < < 3+ N = 36, 281 3+ R 2 =.5 < < < 7+
3+ 3+ N = 155, 442 3+ R 2 =.32 < < < 3+ N = 149, 685 3+ R 2 =.27 < < < 3+ N = 99, 752 3+ R 2 =.4 < < < 3+ N = 98, 887 3+ R 2 =.6 < < < 3+ N = 52, 624 3+ R 2 =.28 < < < 3+ N = 36, 281 3+ R 2 =.5 < < < 7+
Moving Toward Systemness: Creating Accountable Care Systems
 Moving Toward Systemness: Creating Accountable Care Systems Stephen M. Shortell, Ph.D. Blue Cross of California Distinguished Professor of Health Policy and Management Dean, School of Public Health University
Moving Toward Systemness: Creating Accountable Care Systems Stephen M. Shortell, Ph.D. Blue Cross of California Distinguished Professor of Health Policy and Management Dean, School of Public Health University
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by February 2018 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.1 19 Alabama 3.7 33 Ohio 4.5 2 New Hampshire 2.6 19 Missouri 3.7 33 Rhode Island 4.5
States Ranked by February 2018 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.1 19 Alabama 3.7 33 Ohio 4.5 2 New Hampshire 2.6 19 Missouri 3.7 33 Rhode Island 4.5
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by November 2015 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.7 19 Indiana 4.4 37 Georgia 5.6 2 Nebraska 2.9 20 Ohio 4.5 37 Tennessee 5.6
States Ranked by November 2015 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.7 19 Indiana 4.4 37 Georgia 5.6 2 Nebraska 2.9 20 Ohio 4.5 37 Tennessee 5.6
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by April 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Colorado 2.3 17 Virginia 3.8 37 California 4.8 2 Hawaii 2.7 20 Massachusetts 3.9 37 West Virginia
States Ranked by April 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Colorado 2.3 17 Virginia 3.8 37 California 4.8 2 Hawaii 2.7 20 Massachusetts 3.9 37 West Virginia
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by August 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.3 18 Maryland 3.9 36 New York 4.8 2 Colorado 2.4 18 Michigan 3.9 38 Delaware 4.9
States Ranked by August 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.3 18 Maryland 3.9 36 New York 4.8 2 Colorado 2.4 18 Michigan 3.9 38 Delaware 4.9
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by March 2016 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 South Dakota 2.5 19 Delaware 4.4 37 Georgia 5.5 2 New Hampshire 2.6 19 Massachusetts 4.4 37 North
States Ranked by March 2016 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 South Dakota 2.5 19 Delaware 4.4 37 Georgia 5.5 2 New Hampshire 2.6 19 Massachusetts 4.4 37 North
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by September 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.4 17 Indiana 3.8 36 New Jersey 4.7 2 Colorado 2.5 17 Kansas 3.8 38 Pennsylvania
States Ranked by September 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.4 17 Indiana 3.8 36 New Jersey 4.7 2 Colorado 2.5 17 Kansas 3.8 38 Pennsylvania
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by December 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.0 16 South Dakota 3.5 37 Connecticut 4.6 2 New Hampshire 2.6 20 Arkansas 3.7 37 Delaware
States Ranked by December 2017 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.0 16 South Dakota 3.5 37 Connecticut 4.6 2 New Hampshire 2.6 20 Arkansas 3.7 37 Delaware
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by September 2015 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.8 17 Oklahoma 4.4 37 South Carolina 5.7 2 Nebraska 2.9 20 Indiana 4.5 37 Tennessee
States Ranked by September 2015 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.8 17 Oklahoma 4.4 37 South Carolina 5.7 2 Nebraska 2.9 20 Indiana 4.5 37 Tennessee
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by November 2014 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.7 19 Pennsylvania 5.1 35 New Mexico 6.4 2 Nebraska 3.1 20 Wisconsin 5.2 38 Connecticut
States Ranked by November 2014 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 North Dakota 2.7 19 Pennsylvania 5.1 35 New Mexico 6.4 2 Nebraska 3.1 20 Wisconsin 5.2 38 Connecticut
Unemployment Rate (%) Rank State. Unemployment
 States Ranked by July 2018 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.1 19 Massachusetts 3.6 37 Kentucky 4.3 2 Iowa 2.6 19 South Carolina 3.6 37 Maryland 4.3
States Ranked by July 2018 Unemployment Rate Seasonally Adjusted Unemployment Unemployment Unemployment 1 Hawaii 2.1 19 Massachusetts 3.6 37 Kentucky 4.3 2 Iowa 2.6 19 South Carolina 3.6 37 Maryland 4.3
Medicare Physician Group Practice Demonstration
 Medicare Physician Group Practice Demonstration Disease Management Colloquium Philadelphia, Pennsylvania June 23, 2005 John Pilotte Senior Research Analyst Medicare Demonstrations Program Group Centers
Medicare Physician Group Practice Demonstration Disease Management Colloquium Philadelphia, Pennsylvania June 23, 2005 John Pilotte Senior Research Analyst Medicare Demonstrations Program Group Centers
ARL ACADEMIC HEALTH SCIENCES LIBRARY STATISTICS
 ASSOCIATION OF RESEARCH LIBRARIES WASHINGTON, D.C. 2006 ARL ACADEMIC HEALTH SCIENCES LIBRARY STATISTICS 2004-05 Compiled and Edited by MARK YOUNG MARTHA KYRILLIDOU Downloaded from publications.arl.org
ASSOCIATION OF RESEARCH LIBRARIES WASHINGTON, D.C. 2006 ARL ACADEMIC HEALTH SCIENCES LIBRARY STATISTICS 2004-05 Compiled and Edited by MARK YOUNG MARTHA KYRILLIDOU Downloaded from publications.arl.org
The Significant Lack of Alignment Across State and Regional Health Measure Sets: An Analysis of 48 State and Regional Measure Sets, Presentation
 The Significant Lack of Alignment Across State and Regional Health Measure Sets: An Analysis of 48 State and Regional Measure Sets, Presentation Kate Reinhalter Bazinsky Michael Bailit September 10, 2013
The Significant Lack of Alignment Across State and Regional Health Measure Sets: An Analysis of 48 State and Regional Measure Sets, Presentation Kate Reinhalter Bazinsky Michael Bailit September 10, 2013
TABLE 3c: Congressional Districts with Number and Percent of Hispanics* Living in Hard-to-Count (HTC) Census Tracts**
 living Alaska 00 47,808 21,213 44.4 Alabama 01 20,661 3,288 15.9 Alabama 02 23,949 6,614 27.6 Alabama 03 20,225 3,247 16.1 Alabama 04 41,412 7,933 19.2 Alabama 05 34,388 11,863 34.5 Alabama 06 34,849 4,074
living Alaska 00 47,808 21,213 44.4 Alabama 01 20,661 3,288 15.9 Alabama 02 23,949 6,614 27.6 Alabama 03 20,225 3,247 16.1 Alabama 04 41,412 7,933 19.2 Alabama 05 34,388 11,863 34.5 Alabama 06 34,849 4,074
2015 State Hospice Report 2013 Medicare Information 1/1/15
 2015 State Hospice Report 2013 Medicare Information 1/1/15 www.hospiceanalytics.com 2 2013 Demographics & Hospice Utilization National Population 316,022,508 Total Deaths 2,529,792 Medicare Beneficiaries
2015 State Hospice Report 2013 Medicare Information 1/1/15 www.hospiceanalytics.com 2 2013 Demographics & Hospice Utilization National Population 316,022,508 Total Deaths 2,529,792 Medicare Beneficiaries
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
Aetna at a Glance. Over 35,000 Aetna employees worldwide million medical members million dental members million pharmacy members
 Aetna s Pay for Performance Initiatives Driving Improvement Opportunities Aetna at a Glance People Membership Over 35,000 Aetna employees worldwide 17.467 million medical members 14.166 million dental
Aetna s Pay for Performance Initiatives Driving Improvement Opportunities Aetna at a Glance People Membership Over 35,000 Aetna employees worldwide 17.467 million medical members 14.166 million dental
Medicare Advantage PFFS Products HFMA 2008 Spring Education Conference Kiet Lam Senior Manager, Triage Consulting Group
 Medicare Advantage PFFS Products HFMA 2008 Spring Education Conference Kiet Lam Senior Manager, Triage Consulting Group In the news Medicare Audits Show Problems in Private Plans NY Times (Oct 2007) Medicare
Medicare Advantage PFFS Products HFMA 2008 Spring Education Conference Kiet Lam Senior Manager, Triage Consulting Group In the news Medicare Audits Show Problems in Private Plans NY Times (Oct 2007) Medicare
Value Based P4P Program Updates MY 2017 & MY 2018
 Value Based P4P Program Updates MY 2017 & MY 2018 January 31, 2018 Lindsay Erickson, Director Ginamarie Gianandrea, Senior Program Coordinator Thien Nguyen, Project Manager Brandi Melville, Health Care
Value Based P4P Program Updates MY 2017 & MY 2018 January 31, 2018 Lindsay Erickson, Director Ginamarie Gianandrea, Senior Program Coordinator Thien Nguyen, Project Manager Brandi Melville, Health Care
CONNECTICUT: ECONOMIC FUTURE WITH EDUCATIONAL REFORM
 CONNECTICUT: ECONOMIC FUTURE WITH EDUCATIONAL REFORM This file contains detailed projections and information from the article: Eric A. Hanushek, Jens Ruhose, and Ludger Woessmann, It pays to improve school
CONNECTICUT: ECONOMIC FUTURE WITH EDUCATIONAL REFORM This file contains detailed projections and information from the article: Eric A. Hanushek, Jens Ruhose, and Ludger Woessmann, It pays to improve school
Pioneer Accountable Care Organization Model: General Fact Sheet May 22, 2012
 Pioneer Accountable Care Organization Model: General Fact Sheet May 22, 2012 The Pioneer ACO Model is a CMS Innovation Center initiative designed to support organizations with experience operating as Accountable
Pioneer Accountable Care Organization Model: General Fact Sheet May 22, 2012 The Pioneer ACO Model is a CMS Innovation Center initiative designed to support organizations with experience operating as Accountable
Critical Access Hospitals and HCAHPS
 Critical Access Hospitals and HCAHPS Michelle Casey, MS Senior Research Fellow and Deputy Director University of Minnesota Rural Health Research Center June 12, 2012 Overview of Presentation Why is HCAHPS
Critical Access Hospitals and HCAHPS Michelle Casey, MS Senior Research Fellow and Deputy Director University of Minnesota Rural Health Research Center June 12, 2012 Overview of Presentation Why is HCAHPS
TABLE 3b: Congressional Districts Ranked by Percent of Hispanics* Living in Hard-to- Count (HTC) Census Tracts**
 Rank State District Count (HTC) 1 New York 05 150,499 141,567 94.1 2 New York 08 133,453 109,629 82.1 3 Massachusetts 07 158,518 120,827 76.2 4 Michigan 13 47,921 36,145 75.4 5 Illinois 04 508,677 379,527
Rank State District Count (HTC) 1 New York 05 150,499 141,567 94.1 2 New York 08 133,453 109,629 82.1 3 Massachusetts 07 158,518 120,827 76.2 4 Michigan 13 47,921 36,145 75.4 5 Illinois 04 508,677 379,527
Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value
 Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value Objectives Compare different primary care compensation models Identify keys to success and best methods for transitioning
Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value Objectives Compare different primary care compensation models Identify keys to success and best methods for transitioning
DOCTORAL/RESEARCH INSTITUTIONS RECEIVING FULBRIGHT AWARDS FOR
 DOCTORAL/RESEARCH INSTITUTIONS RECEIVING FULBRIGHT AWARDS FOR 2015-2016 Those institutions highlighted in blue are listed in the Chronicle of Higher Education Institution State Grants Applications Harvard
DOCTORAL/RESEARCH INSTITUTIONS RECEIVING FULBRIGHT AWARDS FOR 2015-2016 Those institutions highlighted in blue are listed in the Chronicle of Higher Education Institution State Grants Applications Harvard
PRESS RELEASE Media Contact: Joseph Stefko, Director of Public Finance, ;
 PRESS RELEASE Media Contact: Joseph Stefko, Director of Public Finance, 585.327.7075; jstefko@cgr.org Highest Paid State Workers in New Jersey & New York in 2010; Lowest Paid in Dakotas and West Virginia
PRESS RELEASE Media Contact: Joseph Stefko, Director of Public Finance, 585.327.7075; jstefko@cgr.org Highest Paid State Workers in New Jersey & New York in 2010; Lowest Paid in Dakotas and West Virginia
Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director
 Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director AMGA Pre-conference Workshop 1 April 14, 2011 Washington, D.C. Disclosure Nothing in Today
Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director AMGA Pre-conference Workshop 1 April 14, 2011 Washington, D.C. Disclosure Nothing in Today
Medi-Cal Value Payments
 Medi-Cal Value Payments P4P Program Overview Joel Gray joel.gray@anthem.com Linkedin.com/in/jgray123 4/26/2018 Anthem Blue Cross CA Medicaid Plan 1.2M Members 29 Counties 2 VBP/P4P Challenge Design a new
Medi-Cal Value Payments P4P Program Overview Joel Gray joel.gray@anthem.com Linkedin.com/in/jgray123 4/26/2018 Anthem Blue Cross CA Medicaid Plan 1.2M Members 29 Counties 2 VBP/P4P Challenge Design a new
FDA s Sentinel Initiative A National Strategy for Monitoring Medical Product Safety
 FDA s Sentinel Initiative A National Strategy for Monitoring Medical Product Safety Judy Racoosin, MD, MPH Sentinel Initiative Scientific Lead US Food and Drug Administration 1 Sentinel Initiative Develop
FDA s Sentinel Initiative A National Strategy for Monitoring Medical Product Safety Judy Racoosin, MD, MPH Sentinel Initiative Scientific Lead US Food and Drug Administration 1 Sentinel Initiative Develop
About the Pacific Business Group on Health. Prepared By: Diane Stewart Senior Manager Pacific Business Group on Health
 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% HbA1c < 9.0 HbA1c Test 2003 LDL
100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% HbA1c < 9.0 HbA1c Test 2003 LDL
ARL ACADEMIC LAW LIBRARY STATISTICS
 ASSOCIATION OF RESEARCH LIBRARIES WASHINGTON, D.C. 2006 ARL ACADEMIC LAW LIBRARY STATISTICS 2004-05 Compiled and Edited by MARK YOUNG MARTHA KYRILLIDOU Downloaded from publications.arl.org ARL Academic
ASSOCIATION OF RESEARCH LIBRARIES WASHINGTON, D.C. 2006 ARL ACADEMIC LAW LIBRARY STATISTICS 2004-05 Compiled and Edited by MARK YOUNG MARTHA KYRILLIDOU Downloaded from publications.arl.org ARL Academic
Table 8 Online and Telephone Medicaid Applications for Children, Pregnant Women, Parents, and Expansion Adults, January 2017
 Table 8 Online and Telephone Medicaid Applications for Children, Pregnant Women, Parents, and Expansion Adults, January 2017 State Applications Can be Submitted Online at the State Level 1 < 25% 25% -
Table 8 Online and Telephone Medicaid Applications for Children, Pregnant Women, Parents, and Expansion Adults, January 2017 State Applications Can be Submitted Online at the State Level 1 < 25% 25% -
PRIMARY CARE EXTENSION PROGRAM for ILLINOIS: History and Vision. Margaret Gadon MD MPH
 PRIMARY CARE EXTENSION PROGRAM for ILLINOIS: History and Vision. Margaret Gadon MD MPH Implementing system change is never easy. But with the lack of value in the current healthcare system, change is essential.
PRIMARY CARE EXTENSION PROGRAM for ILLINOIS: History and Vision. Margaret Gadon MD MPH Implementing system change is never easy. But with the lack of value in the current healthcare system, change is essential.
Medicaid 101: The Basics
 Medicaid 101: The Basics April 9, 2018 Miranda Motter President and CEO Gretchen Blazer Thompson Director of Govt. Affairs Angela Weaver Director of Regulatory Affairs OAHP Overview Who We Are: The Ohio
Medicaid 101: The Basics April 9, 2018 Miranda Motter President and CEO Gretchen Blazer Thompson Director of Govt. Affairs Angela Weaver Director of Regulatory Affairs OAHP Overview Who We Are: The Ohio
Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives. Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018
 Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018 Why Standardization? MEDI-CAL CROSS PRODUCT San Francisco Health
Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018 Why Standardization? MEDI-CAL CROSS PRODUCT San Francisco Health
Interstate Turbine Advisory Council (CESA-ITAC)
 Interstate Turbine Advisory Council (CESA-ITAC) Mark Mayhew NYSERDA for Val Stori Clean Energy States Alliance SWAT 4/25/12 Today CESA ITAC, LLC - What, who and why The Unified List - What, why, how and
Interstate Turbine Advisory Council (CESA-ITAC) Mark Mayhew NYSERDA for Val Stori Clean Energy States Alliance SWAT 4/25/12 Today CESA ITAC, LLC - What, who and why The Unified List - What, why, how and
Aligning Physician Groups to Maximize Managed Care Performance
 Aligning Physician Groups to Maximize Managed Care Performance Presented to: 2016 Spring Managed Care Forum Friday, April 22, 2016 Introduction Today s speaker Page 1 Craig D. Pederson Principal Insight
Aligning Physician Groups to Maximize Managed Care Performance Presented to: 2016 Spring Managed Care Forum Friday, April 22, 2016 Introduction Today s speaker Page 1 Craig D. Pederson Principal Insight
Evolution of ACOs in California. Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D.
 Evolution of ACOs in California Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D. Integrated Healthcare Association Statewide multi stakeholder leadership group that promotes quality
Evolution of ACOs in California Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D. Integrated Healthcare Association Statewide multi stakeholder leadership group that promotes quality
IMPROVING THE QUALITY OF CARE IN SOUTH CAROLINA S MEDICAID PROGRAM
 IMPROVING THE QUALITY OF CARE IN SOUTH CAROLINA S MEDICAID PROGRAM VICE PRESIDENT, PUBLIC POLICY & EXTERNAL RELATIONS October 16, 2008 Who is NCQA? TODAY Why measure quality? What is the state of health
IMPROVING THE QUALITY OF CARE IN SOUTH CAROLINA S MEDICAID PROGRAM VICE PRESIDENT, PUBLIC POLICY & EXTERNAL RELATIONS October 16, 2008 Who is NCQA? TODAY Why measure quality? What is the state of health
The American Legion NATIONAL MEMBERSHIP RECORD
 The American Legion NATIONAL MEMBERSHIP RECORD www.legion.org 2016 The American Legion NATIONAL MEMBERSHIP RECORD 1920-1929 Department 1920 1921 1922 1923 1924 1925 1926 1927 1928 1929 Alabama 4,474 3,246
The American Legion NATIONAL MEMBERSHIP RECORD www.legion.org 2016 The American Legion NATIONAL MEMBERSHIP RECORD 1920-1929 Department 1920 1921 1922 1923 1924 1925 1926 1927 1928 1929 Alabama 4,474 3,246
FY 2014 Per Capita Federal Spending on Major Grant Programs Curtis Smith, Nick Jacobs, and Trinity Tomsic
 Special Analysis 15-03, June 18, 2015 FY 2014 Per Capita Federal Spending on Major Grant Programs Curtis Smith, Nick Jacobs, and Trinity Tomsic 202-624-8577 ttomsic@ffis.org Summary Per capita federal
Special Analysis 15-03, June 18, 2015 FY 2014 Per Capita Federal Spending on Major Grant Programs Curtis Smith, Nick Jacobs, and Trinity Tomsic 202-624-8577 ttomsic@ffis.org Summary Per capita federal
State (and U. S. Territorial) Health Department Request for Technical Assistance (RTA): Applications due: (December 1, 2014) at 11:59 pm ET
 State (and U. S. Territorial) Health Department Request for Technical Assistance (RTA): Million Hearts Stakeholders Workshop Applications due: (December 1, 2014) at 11:59 pm ET I. Purpose: The purpose
State (and U. S. Territorial) Health Department Request for Technical Assistance (RTA): Million Hearts Stakeholders Workshop Applications due: (December 1, 2014) at 11:59 pm ET I. Purpose: The purpose
2009 AAPA Physician Assistant Census National Report
 Report # CENS2009-01 January 2010 2009 AAPA Physician Assistant Census National Report Introduction The American Academy of Physician Assistants (AAPA) was founded in 1968 and is the only national organization
Report # CENS2009-01 January 2010 2009 AAPA Physician Assistant Census National Report Introduction The American Academy of Physician Assistants (AAPA) was founded in 1968 and is the only national organization
Utilizing Grants to Achieve Your Farm Objectives
 Utilizing Grants to Achieve Your Farm Objectives Ohio Ecological Food and Farm Association Annual Conference- Granville, OH February 13, 2010 Mike Hogan Extension Educator & Associate Professor Sustainable
Utilizing Grants to Achieve Your Farm Objectives Ohio Ecological Food and Farm Association Annual Conference- Granville, OH February 13, 2010 Mike Hogan Extension Educator & Associate Professor Sustainable
COMMUNITY PARAMEDICINE MOBILE INTEGRATED HEALTHCARE STAKEHOLDERS MEETING
 COMMUNITY PARAMEDICINE MOBILE INTEGRATED HEALTHCARE STAKEHOLDERS MEETING July 18, 2014 WHAT IS COMMUNITY PARAMEDICINE & MOBILE INTEGRATED HEALTHCARE (MIH) CP/MIHC programs use EMS practitioners and other
COMMUNITY PARAMEDICINE MOBILE INTEGRATED HEALTHCARE STAKEHOLDERS MEETING July 18, 2014 WHAT IS COMMUNITY PARAMEDICINE & MOBILE INTEGRATED HEALTHCARE (MIH) CP/MIHC programs use EMS practitioners and other
2014 ACEP URGENT CARE POLL RESULTS
 2014 ACEP URGENT CARE POLL RESULTS PREPARED FOR: PREPARED BY: 2014 Marketing General Incorporated 625 North Washington Street, Suite 450 Alexandria, VA 22314 800.644.6646 toll free 703.739.1000 telephone
2014 ACEP URGENT CARE POLL RESULTS PREPARED FOR: PREPARED BY: 2014 Marketing General Incorporated 625 North Washington Street, Suite 450 Alexandria, VA 22314 800.644.6646 toll free 703.739.1000 telephone
engineering salary guide
 engineering salary guide At a time when lean practices and agile teams create the expectation of doing more with less, employers need to develop new strategies to attract and retain the best employees
engineering salary guide At a time when lean practices and agile teams create the expectation of doing more with less, employers need to develop new strategies to attract and retain the best employees
MAP 1: Seriously Delinquent Rate by State for Q3, 2008
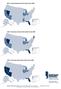 MAP 1: Seriously Delinquent Rate by State for Q3, 2008 Seriously Delinquent Rate Greater than 6.93% 5.18% 6.93% 0 5.17% Source: MBA s National Deliquency Survey MAP 2: Foreclosure Inventory Rate by State
MAP 1: Seriously Delinquent Rate by State for Q3, 2008 Seriously Delinquent Rate Greater than 6.93% 5.18% 6.93% 0 5.17% Source: MBA s National Deliquency Survey MAP 2: Foreclosure Inventory Rate by State
Table 1 Elementary and Secondary Education. (in millions)
 Revised February 22, 2005 WHERE WOULD THE CUTS BE MADE UNDER THE PRESIDENT S BUDGET? Data Table 1 Elementary and Secondary Education Includes Education for the Disadvantaged, Impact Aid, School Improvement
Revised February 22, 2005 WHERE WOULD THE CUTS BE MADE UNDER THE PRESIDENT S BUDGET? Data Table 1 Elementary and Secondary Education Includes Education for the Disadvantaged, Impact Aid, School Improvement
Provider Services and Network Management Newsletter
 A healthier you. A healthier community. In this Issue: Provider Services and Network Management Newsletter Fall 2017, Volume2 : Issue2 We won the RFP... Pg. 1 Care Management... Pg. 2 CAHPS... Pg. 3 Incentives...
A healthier you. A healthier community. In this Issue: Provider Services and Network Management Newsletter Fall 2017, Volume2 : Issue2 We won the RFP... Pg. 1 Care Management... Pg. 2 CAHPS... Pg. 3 Incentives...
The US health care system falls far short
 Q Manage Health Care Vol. 14, No. 2, pp. 66 79 c 2005 Lippincott Williams & Wilkins, Inc. Paying for Performance: Implementing a Statewide Project in California Cheryl L. Damberg, PhD; Kristiana Raube,
Q Manage Health Care Vol. 14, No. 2, pp. 66 79 c 2005 Lippincott Williams & Wilkins, Inc. Paying for Performance: Implementing a Statewide Project in California Cheryl L. Damberg, PhD; Kristiana Raube,
PATIENT-FOCUSED CARE PROGRAMS in Select Metro Service Areas (MSAs)
 PATIENT-FOCUSED CARE PROGRAMS in Select Metro Service Areas (MSAs) Providence-New Bedford-Fall River Rhode Island-Massachusetts Blue Cross and Blue Shield of Rhode Island BCBSRI Shared Savings Program
PATIENT-FOCUSED CARE PROGRAMS in Select Metro Service Areas (MSAs) Providence-New Bedford-Fall River Rhode Island-Massachusetts Blue Cross and Blue Shield of Rhode Island BCBSRI Shared Savings Program
DataArts and the New CDP
 DataArts and the New CDP October 26, 2016 PRESENTED BY Mary Garcia Charumilind Senior Business Development Associate Overview Agenda Agenda 1 2 3 4 5 About DataArts The DataArts Platform The New Cultural
DataArts and the New CDP October 26, 2016 PRESENTED BY Mary Garcia Charumilind Senior Business Development Associate Overview Agenda Agenda 1 2 3 4 5 About DataArts The DataArts Platform The New Cultural
Enhancing Outcomes with Quality Improvement (QI) October 29, 2015
 Enhancing Outcomes with Quality Improvement (QI) October 29, 2015 Learning Objectives! Introduce Quality Improvement (QI)! Explain Clinical Performance Person-Centered Medical Home (PCMH) Measures! Implement
Enhancing Outcomes with Quality Improvement (QI) October 29, 2015 Learning Objectives! Introduce Quality Improvement (QI)! Explain Clinical Performance Person-Centered Medical Home (PCMH) Measures! Implement
Aiming Higher. A State Scorecard on Health System Performance. Joel C. Cantor and Dina Belloff
 Rutgers Center for State Health Policy Aiming Higher A State Scorecard on Health System Performance Joel C. Cantor and Dina Belloff Rutgers Center for State Health Policy Cathy Schoen, Sabrina K.H. How,
Rutgers Center for State Health Policy Aiming Higher A State Scorecard on Health System Performance Joel C. Cantor and Dina Belloff Rutgers Center for State Health Policy Cathy Schoen, Sabrina K.H. How,
Benefits by Service: Inpatient Hospital Services, other than in an Institution for Mental Diseases (October 2006) Definition/Notes
 Page 1 of 9 Benefits by Service: Inpatient Hospital Services, other than in an Institution for Mental Diseases (October 2006) Definition/Notes Note: Totals include 50 states and D.C. "Benefits Covered"
Page 1 of 9 Benefits by Service: Inpatient Hospital Services, other than in an Institution for Mental Diseases (October 2006) Definition/Notes Note: Totals include 50 states and D.C. "Benefits Covered"
Provider Incentives to Improve Accountability
 Provider Incentives to Improve Accountability Friday, October 26, 2007 1:00 pm EDT This audioconference is sponsored by a generous grant from the Robert Wood Johnson Foundation, through the Forum for State
Provider Incentives to Improve Accountability Friday, October 26, 2007 1:00 pm EDT This audioconference is sponsored by a generous grant from the Robert Wood Johnson Foundation, through the Forum for State
Physician Compensation for Quality Within Groups: Complying with Stark and The State of The Art. Alice G. Gosfield
 Physician Compensation for Quality Within Groups: Complying with Stark and The State of The Art Alice G. Gosfield Alice G. Gosfield and Associates, PC 2309 Delancey Place Philadelphia PA 19103 (215) 735-2384
Physician Compensation for Quality Within Groups: Complying with Stark and The State of The Art Alice G. Gosfield Alice G. Gosfield and Associates, PC 2309 Delancey Place Philadelphia PA 19103 (215) 735-2384
Ethnic Studies Asst 54, ,315-3, ,229 6,229. Gen Honors/UC Asso 64, ,402-4, ,430 24,430
 A&S Prof 99,280 157 110,954-11,674-10.52 1,832,807 2,010,866 Asso 70,144 112 73,921-3,777-5.11 422,998 603,376 Asst 60,165 82 62,465-2,300-3.68 188,570 269,597 Total 80,845 351 87,809-6,964-7.93 2,444,375
A&S Prof 99,280 157 110,954-11,674-10.52 1,832,807 2,010,866 Asso 70,144 112 73,921-3,777-5.11 422,998 603,376 Asst 60,165 82 62,465-2,300-3.68 188,570 269,597 Total 80,845 351 87,809-6,964-7.93 2,444,375
Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In?
 Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In? Sue Sirlin, CPEHR Director, HIT Consulting Services Bonni Brownlee, MHA CPHQ CPEHR Principal Consultant March 15, 2013 Advancing Healthcare
Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In? Sue Sirlin, CPEHR Director, HIT Consulting Services Bonni Brownlee, MHA CPHQ CPEHR Principal Consultant March 15, 2013 Advancing Healthcare
Piloting Performance Measurement of Physician Organizations in Medi-Cal Managed Care: Findings and Implications
 Issue Brief No. 13 January 2015 Piloting Performance Measurement of Physician Organizations in Medi-Cal Managed Care: Findings and Implications Ann Hardesty, Project Manager Jill Yegian, Senior Vice President,
Issue Brief No. 13 January 2015 Piloting Performance Measurement of Physician Organizations in Medi-Cal Managed Care: Findings and Implications Ann Hardesty, Project Manager Jill Yegian, Senior Vice President,
INTRODUCTION. The system seems backwards. Doctors only get paid when people get sick so they have no incentive to keep people healthy.
 Year ONE 2 0 0 9 INTRODUCTION Dr. John Yindra prepared to see his next patient, who was referred to him because of a leg infection. He saw that she had diabetes, but he didn t have any other information
Year ONE 2 0 0 9 INTRODUCTION Dr. John Yindra prepared to see his next patient, who was referred to him because of a leg infection. He saw that she had diabetes, but he didn t have any other information
STATE ENTREPRENEURSHIP INDEX
 University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln Business in Nebraska Bureau of Business Research 12-2013 STATE ENTREPRENEURSHIP INDEX Eric Thompson University of Nebraska-Lincoln,
University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln Business in Nebraska Bureau of Business Research 12-2013 STATE ENTREPRENEURSHIP INDEX Eric Thompson University of Nebraska-Lincoln,
Judith Schaefer, MPH MacColl Institute Missouri Foundation for Health September 27, 2010
 Patient Centered Medical Home Judith Schaefer, MPH MacColl Institute Missouri Foundation for Health September 27, 2010 What is the Medical Home? History of Medical Home Pediatrics -Started as a movement
Patient Centered Medical Home Judith Schaefer, MPH MacColl Institute Missouri Foundation for Health September 27, 2010 What is the Medical Home? History of Medical Home Pediatrics -Started as a movement
Revenues, Expenses, and Operating Profits of U. S. Lotteries, FY 2002
 Revenues, Expenses, and Operating Profits of U. S. Lotteries, APPENDIX A Table A.1: Lottery Sales Excluding Sales From Video Lottery Terminals, Table A.2: Sales from Video Lottery Terminals Table A.3:
Revenues, Expenses, and Operating Profits of U. S. Lotteries, APPENDIX A Table A.1: Lottery Sales Excluding Sales From Video Lottery Terminals, Table A.2: Sales from Video Lottery Terminals Table A.3:
2016 INCOME EARNED BY STATE INFORMATION
 BY STATE INFORMATION This information is being provided to assist in your 2016 tax preparations. The information is also mailed to applicable Columbia fund non-corporate shareholders with their year-end
BY STATE INFORMATION This information is being provided to assist in your 2016 tax preparations. The information is also mailed to applicable Columbia fund non-corporate shareholders with their year-end
Kaiser Permanente Overview: Innovation, Integration, Information Technology, and System-ness in Health Care
 Kaiser Permanente Overview: Innovation, Integration, Information Technology, and System-ness in Health Care Bernadette Loftus, MD Associate Executive Director, The Permanente Medical Group Executive Medical
Kaiser Permanente Overview: Innovation, Integration, Information Technology, and System-ness in Health Care Bernadette Loftus, MD Associate Executive Director, The Permanente Medical Group Executive Medical
Fiscal Year 1999 Comparisons. State by State Rankings of Revenues and Spending. Includes Fiscal Year 2000 Rankings for State Taxes Only
 Fiscal Year 1999 Comparisons State by State Rankings of Revenues and Spending Includes Fiscal Year 2000 Rankings for State Taxes Only January 2002 1 2 published annually by: The Minnesota Taxpayers Association
Fiscal Year 1999 Comparisons State by State Rankings of Revenues and Spending Includes Fiscal Year 2000 Rankings for State Taxes Only January 2002 1 2 published annually by: The Minnesota Taxpayers Association
Anthem BlueCross and BlueShield
 Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Commercial HMO) Accredited Accreditation Commercial
Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Commercial HMO) Accredited Accreditation Commercial
Healthcare Hot Spotting: Variation in Quality and Resource Use in California
 Issue Brief No. 19 July 2015 Healthcare Hot Spotting: Variation in Quality and Resource Use in California Kelly Miller, Project Manager Jill Yegian, Ph.D., Senior Vice President, Programs and Policy Dolores
Issue Brief No. 19 July 2015 Healthcare Hot Spotting: Variation in Quality and Resource Use in California Kelly Miller, Project Manager Jill Yegian, Ph.D., Senior Vice President, Programs and Policy Dolores
THE STATE OF GRANTSEEKING FACT SHEET
 1 THE STATE OF GRANTSEEKING FACT SHEET ORG ANIZATIONAL COMPARISO N BY C ENSUS DIV ISION S PRING 2013 The State of Grantseeking Spring 2013 is the sixth semi-annual informal survey of nonprofits conducted
1 THE STATE OF GRANTSEEKING FACT SHEET ORG ANIZATIONAL COMPARISO N BY C ENSUS DIV ISION S PRING 2013 The State of Grantseeking Spring 2013 is the sixth semi-annual informal survey of nonprofits conducted
W. Douglas Weaver, MD, MACC. American College of Cardiology SENATE FINANCE COMMITTEE
 Statement of W. Douglas Weaver, MD, MACC On behalf of the American College of Cardiology Presented to the SENATE FINANCE COMMITTEE Roundtable on Medicare Physician Payments: Perspectives from Physicians
Statement of W. Douglas Weaver, MD, MACC On behalf of the American College of Cardiology Presented to the SENATE FINANCE COMMITTEE Roundtable on Medicare Physician Payments: Perspectives from Physicians
