Discharge Care Pathway for Infants from Neonatal Unit, CAH
|
|
|
- MargaretMargaret Chapman
- 6 years ago
- Views:
Transcription
1 Title: Author: Designation: Speciality / Division: CLINICAL GUIDELINES ID TAG Discharge care pathway for infants from the neonatal unit, Craigavon Area Hospital Una Toland Lead Nurse for Neonatal Services, SHSCT Neonatal Directorate: CYP Date Uploaded: 24 th November 2014 Review Date: 1 st November 2017 Clinical Guideline ID CG0052 Discharge Care Pathway for Infants from Neonatal Unit, CAH
2 Discharge Care Pathway for Infants from Neonatal Unit, CAH PURPOSE The purpose of this pathway is to facilitate the safe and effective discharge of infants from the neonatal unit to: The home environment where there are no safeguarding concerns or complex medical/nursing needs. The home environment where there are safeguarding concerns. The home environment requiring home oxygen therapy and input from children s nursing team. The home environment requiring enteral feeding and input from community children s nursing team. The postnatal ward. Another Neonatal Unit for ongoing care. The discharge needs of the infant will be assessed on an individual basis and should be carefully planned. This will ensure continuity of care in the hospital, between hospitals and in the community setting. SCOPE This pathway applies to all neonatal nursing and medical staff and midwives and any other members of the multidisciplinary team inputting into the care of infants in neonatal setting.
3 INFANTS DISCHARGED FROM THE NEONATAL UNIT TO THE HOME ENVIRONMENT WHO DO NOT HAVE SAFE GUARDING CONCERNS OR COMPLEX MEDICAL / NURSING NEEDS DISCHARGE CRITIERIA Assessment of infants for discharge should include Thermoregulation- adequate maintenance of normal body temperature fully clothed in an open cot Feeding/ nutrition Cardio respiratory stability Colonisation / Infection risk Family readiness for discharge. Family training / education Availability of community support Gestational age ideally have reached 34 weeks corrected age or more Weight gain (ideally minimum weight of 1800grams and showing sustained pattern of weight gain, < 1800grams is at consultant discretion ) Screening tests ( to include ROP screening follow up ) Immunisation status DECISION TO DISCHARGE Consultant Paediatrician/Neonatologist in consultation with senior nurse in charge and ANNP. Medical and nursing staff to agree a date of discharge with parents /carers with parental responsibility. Nursing team will perform majority of discharge requirements. DISCHARGE CHECKLIST Where appropriate, the following should be achieved before discharge with the input from language support / interpreter if required. All parents should be offered to room in overnight with infant.
4 Parental competencies Administration of medications to include instruction on storage, dosage, timing and administration. Baby cares (nappy change, top and tail bathing, bathing). Feeding Parental education Consider the need for resuscitation training and give BLISS DVD and practical demonstration as required. Information on respiratory syncytial virus if applicable (give BLISS leaflet). Prevention of SIDs (give information leaflet). Storage of breast milk and cleaning of breast pump equipment if appropriate (give written information leaflet). Preparation of powdered infant formula feeds (give written information leaflet). Discuss tips for keeping infant safe from infection in home environment, proper positioning during sleep and use of car seats. Procedures and Investigations Check all new-born blood spot screening tests completed to date and any follow up tests communicated to community team. When immunisations not complete, send copy of immunisations received to date to GP, HV and Child Health. Arrange BCG if required. Arrange audiology screening if required. Arrange ophthalmology screening follow up if required ( <32weeks gestation and or < 1501grams). Professional Communication Check home and discharge addresses and confirm name of GP. Complete NIMATS or CHS3b discharge documentation and send copy to Child Health/ Health visitor/ GP/ Community Children s Nursing Team. Complete admission/ discharge ledger. Contact Community midwife / Health visitor on day of discharge (if weekend discharge inform on next working day). Complete daily stats book. Inform TAMBA HV link if applicable. Update on line Regional Neonatal cot locator. Give parents copy of Your experience of neonatal care survey to complete.
5 Medical/ ANNP team Perform and record discharge examination Complete Part A and Part B of Infant PCHR Red Book Check Hip referral sent if required Ensure prescription for take home medications written, sent to pharmacy and drugs available in ward on day of discharge Complete discharge summary on Badger Check all follow up appointment s made Follow up appointments Ensure these are written on discharge summary. Likely appointments may include Neonatal outpatient clinic Ophthalmology clinic Audiology referral Cranial ultrasound Brain MRI Physiotherapy Hip referral Dietitian Child developmental clinic BCG immunisation or Palivizumab Planned review for blood taking, weight check at Rainbow Clinic Tertiary consultant out patients
6 INFANTS DISCHARGED FROM NEONATAL UNIT TO THE HOME ENVIRONMENT ABOUT WHOM THERE ARE SAFE GUARDING CONCERNS DISCHARGE CRITIERIA Discharge planning meeting should take place as soon as reasonably possible in conjunction with all relevant professionals involved in the infants hospital care and care in the community. Consider the need for input from language support/ interpreter if required. Ensure that no infant about whom there are safe guarding concerns is discharged from hospital back into the community without an identified GP and a full assessment of home circumstances. Ensure all actions following discharge planning meeting are completed before infant is discharged from neonatal unit. If applicable, facilitation of Adoption / Foster carers should be coordinated as advised by hospital social work team. Professionals who may be invited to attend the discharge planning meeting pending the circumstances include (see attached template for preparation for discharge meeting re infant about whom there are safe guarding concerns appendix 1). GP Health Visitor Community midwife Children s community nurse Hospital social worker Community social worker Hospital Safe guarding lead Member of neonatal medical team Member of neonatal nursing team Assessment of infants for discharge should include Thermoregulation- adequate maintenance of normal body temperature fully clothed in an open cot Cardio respiratory stability Colonisation /Infection risk Gestational age ideally have reached 34 weeks corrected age or more Weight gain (ideally minimum weight of 1800grams and showing sustained pattern of weight gain, < 1800grams is at Consultant discretion ) Family readiness for discharge. Family training / education Availability of community support Screening tests ( to include ROP screening follow up ) Immunisation status
7 DECISION TO DISCHARGE Consultant paediatrician/neonatologist in consultation with senior nurse in charge and ANNP. Medical and nursing staff to agree a date of discharge with parents /carers with parental responsibility. Nursing team will perform majority of discharge requirements. DISCHARGE CHECKLIST Where appropriate the following should be achieved before discharge. All parents should be offered to room in overnight with infant. Parental / Carer competencies Administration of medications to include instruction on storage, dosage, timing and administration Baby cares (nappy change, top and tail bathing, bathing) Feeding Parental /Carer education Consider the need for resuscitation training and give BLISS DVD and practical demonstration as required. Information on Respiratory syncytial virus if applicable (give BLISS leaflet). Prevention of SIDS (give information leaflet). Storage of breast milk and cleaning of breast pump equipment if appropriate (give written information leaflet). Preparation of powdered infant formula feeds (give written information leaflet). Discuss tips for keeping infant safe from infection in home environment, proper positioning during sleep and use of car seats. Procedures and Investigations Check all new-born blood spot screening tests completed to date and any follow up tests communicated to community team When immunisations not complete ensure send copy of immunisation received to date to GP, HV and Child Health. Arrange BCG if required. Arrange audiology screening if required. Arrange ophthalmology screening follow up if required ( <32weeks gestation and or < 1501grams).
8 Professional Communication The social worker will normally provide transport for the infant on the day of discharge from Neonatal to the home of Foster / Adoptive parents. Check home and discharge addresses and confirm name of GP. Complete NIMATS or CHS3b discharge documentation and send copy to Child Health/ Health visitor/ GP/ Community Children s Nursing Team. Complete admission/ discharge ledger. Contact Community Midwife /Health visitor on day of discharge (if week end discharge inform on next working day). Complete daily stats book. Inform TAMBA HV link if applicable. Update on line Regional Neonatal cot locator. Give parents copy of Your experience of neonatal care survey to complete. Complete Child Protection Discharge Checklist (ref: SHSCT Assessment, admission and Discharge Policy and Procedures for Children and Young People under the age of 18 years about whom there are Safe guarding Concerns within Acute Services). Send copy of completed Child Protection Discharge checklist to hospital social work team. Medical/ ANNP team Perform and record discharge examination Complete Part A and Part B of Infant PCHR Red Book Check Hip referral sent if required Ensure prescription for take home medications written, sent to pharmacy and drugs available in ward on day of discharge Complete discharge summary on Badger Check all follow up appointment s made Follow up appointments Ensure these are written on discharge summary. Likely appointments may include Neonatal outpatient clinic Ophthalmology clinic Audiology referral Cranial ultrasound Brain MRI Physiotherapy Hip referral Die titian Child developmental clinic BCG immunisation or Palivizumab Planned review for blood taking, weight check at Rainbow Clinic Tertiary consultant out patients
9 Addressograph APPENDIX 1 Template for preparation for multidisciplinary meeting in preparation for discharge of infant with complex needs and or Safe guarding concerns DATE OF MEETING TIME OF MEETING VENUE FOR MEETING NURSING SUMMARY ON INFANT PROGRESS READY FOR MEETING MEDICAL SUMMARY ON INFANT PROGRESS READY FOR MEETING PLANNED DATE OF DISCHARGE FOR INFANT Professional Group Named representative Contact number Attendance confirmed or alternative representative designated to attend NEONATAL NURSE NEONATAL MEDICAL REPRESENTATIVE GP HEALTH VISITOR COMMUNITY MIDWIFE COMMUNITY CHILDRENS NURSE SOCIAL WORKER HOSPITAL BASED SOCAIL WORKER COMMUNITY BASED SAFE GUARDING NURSE PARENTS/CARERS OTHERS
10 Summary of key actions to be taken forward by key staff following meeting ACTION KEY PROFESSIONAL RESPONSIBLE FOR FOLLOW UP
11 INFANTS DISCHARGED FROM NEONATAL TO THE HOME ENVIRONMENT REQUIRING HOME OXYGEN THERAPY AND INPUT FROM CHILDRENS NURSING TEAM INDICATIONS FOR HOME OXYGEN Chronic lung disease and other neonatal lung condition at Consultant discretion. DISCHARGE CRITIERIA Be clinically stable or improving No significant cyanotic or apnoeic episodes in preceding 2 weeks Discharge planning meeting should take place as soon as reasonably possible in conjunction with all relevant professionals involved in the infants hospital care and care in the community. Consider the need for input from language support / interpreter if required. Ideal timing of discharge should be start of week so that staff are available in event of problems. Liaison with Children s Community Nursing team is vital approaching discharge so that on site visit to meet parents/ carers / infant pre discharge can be organised and home visit on day of discharge can be facilitated. Professionals who may be invited to attend the discharge planning meeting pending the circumstances include (see attached template for preparation for discharge meeting re infant with complex needs). GP Health Visitor Community midwife Children s community nurse Hospital social worker Community social worker Hospital Safe guarding lead Member of neonatal medical team Member of neonatal nursing team Assessment of infants for discharge should include: An agreement on the need for continuous or intermittent pulse- oximetry. An agreement on saturation levels for infant in the home environment Plan for management of low saturation at home Thermoregulation- adequate maintenance of normal body temperature fully clothed in an open cot. Feeding /nutrition
12 Cardio respiratory stability Colonisation / Infection risk Family readiness for discharge. Family training / education Availability of community support Gestational age ideally have reached 34 weeks corrected age or more. Weight gain (ideally minimum weight of 1800grams and showing sustained pattern of weight gain. < 1800grams is at Consultant discretion ) Screening tests ( to include ROP screening follow up ) Immunisation status DECISION TO DISCHARGE Consultant Paediatrician/Neonatologist in consultation with senior nurse in charge and ANNP. Medical and nursing staff to agree a date of discharge with parents /carers with parental responsibility. Nursing team will perform majority of discharge requirements. DISCHARGE CHECKLIST All parents / carers should be offered to room in overnight with infant. Parents/ carers must ensure they contact Home and Car Insurance companies and alert them of need for home oxygen need. Complete HOOF (HOME OXYGEN ORDER FORM) and fax to appropriate department as indicated on form, indicating need for concentrator, ambulatory oxygen for car/buggy etc. Once the HOOF form is submitted to the home oxygen provider for the local area, a representative will contact parents/carers to arrange delivery and installation of oxygen supply in the home. Medical staff to dictate a written prescription indicating clinical diagnosis, amount of oxygen required for infant and a letter should be forwarded to oxygen supplier. Ensure parents/carers have a list of emergency telephone numbers in event of breakdown of equipment. Parents /carers should have a supply of accessories required for delivery of oxygen, nasal cannulae, fixation pads, etc appropriate to needs of infant, be trained in use of all equipment, be able to trouble shoot and know who to contact in an emergency and for replenishment of stock.
13 Where appropriate the following should be achieved before discharge Parental /Carer competencies Administration of medications to include instruction on storage, dosage, timing and administration. Baby cares (nappy change, top and tail bathing, bathing). Feeding Parental /Carer education Check home and discharge addresses and confirm name of GP. Provide resuscitation training and give BLISS DVD and practical demonstration as required. Information on Respiratory syncytial virus if applicable (give BLISS leaflet). Prevention of SIDS (give information leaflet). Storage of breast milk and cleaning of breast pump equipment if appropriate (give written information leaflet). Preparation of powdered infant formula feeds (give written information leaflet). Discuss tips for keeping infant safe from infection in home environment, proper positioning during sleep and use of car seats. Equipment operation, maintenance and problem solving for each device needed. Face to face training on use of home oxygen, set up, monitoring, adjusting oxygen, safety precautions etc. Compliment with BLISS GOING HOME ON OXYGEN booklet. Use of oxygen nasal cannulae and care of same. Application of saturation probe, interpretation of monitor readings. Identification of cyanosis without using pulse-oximetry. Safety issues associated with oxygen in the home, naked flames, open fires, candles, birthday cakes, smoking etc. Procedures and Investigations Check all new-born blood spot screening tests completed to date and any follow up tests communicated to community team When immunisations not complete ensure send copy of immunisation received to date to GP, HV and Child Health. Arrange BCG if required. Arrange audiology screening if required. Arrange ophthalmology screening follow up if required ( <32weeks and or <1501grams).
14 Professional Communication Check home and discharge addresses and confirm name of GP Complete NIMATS or CHS3b discharge documentation and send copy to Child Health/ Health visitor/ GP/ Community Children s Nursing Team. Complete admission/ discharge ledger Contact Community Midwife /Health visitor on day of discharge (if week end discharge inform on next working day). Complete daily stats book Inform TAMBA HV link if applicable Update on line Regional Neonatal cot locator Give parents copy of Your experience of neonatal care survey to complete Medical/ ANNP team Perform and record discharge examination Complete Part A and Part B of Infant PCHR Red Book Check Hip referral sent if required Ensure prescription for take home medications written, sent to pharmacy and available in ward on day of discharge. Complete discharge summary on Badger Check all follow up appointment s made Follow up appointments Ensure these are written on discharge summary. Likely appointments may include Neonatal outpatient clinic Ophthalmology clinic Audiology referral Cranial ultrasound Brain MRI Physiotherapy Hip referral Dietician Child developmental clinic BCG immunisation or Palivizumab Open access to Children s ward Planned review for blood taking, weight check at Rainbow Clinic Tertiary consultant out patients
15 INFANTS DISCHARGED FROM NEONATAL TO THE HOME ENVIRONMENT WHO REQUIRE TUBE FEEDING AND INPUT FROM COMMUNITY CHILDRENS NURSING TEAM DISCHARGE CRITIERIA Assessment of infants for discharge should include Thermoregulation- adequate maintenance of normal body temperature fully clothed in an open cot Cardio respiratory stability Colonisation / Infection risk Family readiness for discharge. Family training / education Gestational age ideally have reached 34 weeks corrected age or more. Weight gain (ideally minimum weight of 1800grams and showing sustained pattern of weight gain. < 1800grams is at Consultant discretion ) Availability of community support Screening tests ( to include ROP screening follow up ) Immunisation status DECISION TO DISCHARGE Consultant Paediatrician/Neonatologist in consultation with senior nurse in charge and ANNP. Medical and nursing staff to agree a date of discharge with parents /carers with parental responsibility. Nursing team will perform majority of discharge requirements. DISCHARGE CHECKLIST Where appropriate the following should be achieved before discharge with the input from language support / interpreter if required. Discharge planning meeting should take place as soon as reasonably possible in conjunction with all relevant professionals involved in the infants hospital care and care in the community. Agree a plan of action for parents if feeding tube is dislodged out of hours and ensure parents/carers aware of who to contact and where to go to have tube replaced. If infant is able to suck some feeds and has stable blood sugars, it may not be appropriate to come to Paediatric ward in middle of night for tube replaced. This may be left until the next morning.
16 Professionals who may be invited to attend the discharge planning meeting pending the circumstances include (see attached template for preparation for discharge meeting re infant with complex needs appendix 1). GP Health Visitor Community midwife Children s community nurse Member of neonatal medical team Member of neonatal nursing team dietician All parents should be offered to room in overnight with infant. Parents /carers should have a supply of enteral feeding equipment appropriate to needs of infant, be trained in use of all equipment, be able to trouble shoot and know who to contact in an emergency and for replenishment of stock. Parental competencies Administration of medications to include instruction on storage, dosage, timing and administration. Baby cares (nappy change, top and tail bathing, bathing). Tube Feeding training and competency assessment and parents feel confident in administration of tube feed. Parental education Consider the need for resuscitation training and give BLISS DVD and practical demonstration as required. Information on respiratory syncytial virus if applicable (give BLISS leaflet). Prevention of SIDS (give information leaflet). Storage of breast milk and cleaning of breast pump equipment if appropriate (give written information leaflet). Cleaning and storage of enteral feeding equipment. Preparation of powdered infant formula feeds (give written information leaflet). Discuss tips for keeping infant safe from infection in home environment,, proper positioning during sleep and use of car seats.
17 Procedures and Investigations Check all new-born blood spot screening tests completed to date and any follow up tests communicated to community team When immunisations not complete ensure GP, HV and Child Health informed on discharge Arrange IF BCG required Arrange audiology screening Arrange ophthalmology screening follow up Professional Communication Check home and discharge addresses and confirm name of GP. Complete NIMATS or CHS3b discharge documentation and send copy to Child Health/ Health visitor/ GP/ Community Children s Nursing Team. Complete admission/ discharge ledger. Contact Health visitor on day of discharge (if weekend discharge inform on next working day). Complete daily stats book Inform TAMBA if applicable HV link Update on line Regional Neonatal cot locator Give parents copy of Your experience of neonatal care survey to complete Medical/ ANNP team Perform and record discharge examination Complete Part A and Part B of Infant PCHR Red Book Check Hip referral sent if required Ensure prescription for take home medications written and sent to pharmacy Complete discharge summary on Badger Check all follow up appointment s made Follow up appointments Ensure these are written on discharge summary. Likely appointments may include Neonatal outpatient clinic Physiotherapy Ophthalmology clinic Hip referral Audiology referral Die titian Cranial ultrasound Child developmental clinic Brain MRI BCG immunisation or Palivizumab
18 Open access to Children s ward Tertiary consultant out patients Planned review for blood taking, weight check at Rainbow Clinic INFANTS DISCHARGED FROM NEONATAL TO THE POST NATAL WARD DISCHARGE CRITIERIA Assessment of infants for discharge to post natal ward should include Thermoregulation- adequate maintenance of normal body temperature fully clothed in an open cot Feeding/ nutrition Cardio respiratory stability Colonisation / Infection risk Need for intravenous drugs (antibiotics) Follow up blood tests and investigations still required Mother still an in patient Procedures and Investigations Check all new-born blood spot screening tests completed to date and any follow up tests communicated to midwifery team Arrange IF BCG required Make arrangements for follow up blood tests /investigations Professional Communication Complete admission/ discharge ledger Complete daily stats book Inform TAMBA if applicable HV link Update on line Regional Neonatal cot locator Neonatal nurse should contact postnatal ward and debrief named midwife on planned transfer to ward. Neonatal nurse should accompany the infant from Neonatal to Postnatal ward and give verbal handover to Named midwife and both staff should carry out an armband check on transfer. This infant should be discussed on the postnatal ward round. Inform social work team and safe guarding nurse if there are any safe guarding concerns. Medical/ ANNP team Record any relevant information in Part A and Part B of Infant PCHR Red Book.
19 Ensure medical summary/ transfer examination and care plan completed in neonatal combined medical notes. Check Hip referral sent if required Complete discharge summary on Badger Check all follow up appointment s made Follow up appointments Ensure these are written on discharge summary. Likely appointments may include Neonatal outpatient clinic Ophthalmology clinic Audiology referral Cranial ultrasound Brain MRI Physiotherapy Hip referral
20 INFANTS DISCHARGED FROM NEONATAL TO ANOTHER NEONATAL UNIT FOR ONGOING CARE DISCHARGE CRITIERIA Assessment of infants for discharge to another neonatal unit should include Availability of a cot in the appropriate neonatal unit for repatriation care or for intensive care input in Regional Neonatal Unit (see attached appendix re repatriation care services available in each neonatal unit in Northern Ireland). Clinical stability of infant requiring transfer. Availability of key transport staff to facilitate the transfer, either local neonatal skilled team or regional transport team. Availability of maternal bed if required. Procedures and Investigations Check pre transfusion blood spot screening card completed before transfer if applicable and ensure card accompanies infant to transferring until if transfer occurring before infant has Day 5 test completed. Check all new-born blood spot screening tests completed to date and any follow up tests communicated to receiving unit team. Record all relevant up to date blood test results and results of any relevant other investigations. Professional Communication Complete the NI Paediatric Transfer form detailing all blood tests, investigations, nursing requirements, travel arrangements for parents,, fluid balance observations, vital signs, drugs and personal data set details. Complete the Neonatal Network Northern Ireland NNNI Neonate Notification of alert organism status form. Complete the neonatal transfer out of unit proforma for monthly data collation. Update on line Regional Neonatal cot locator. Photocopy and attach copies of any relevant laboratory results. Photocopy ROP examination record sheet if applicable. Photocopy drug kardex Enclose a copy of Badger electronic centile chart. Complete admission/ discharge ledger
21 Complete daily stats book Inform TAMBA if applicable HV link If safe guarding issue, inform safe guarding nurse and social work team in both transferring and receiving unit. If required neonatal staff should liaise with both transferring unit and receiving unit maternity staff to ascertain if maternal bed required and available. Inform parents if not present of transfer details as soon as possible. Medical/ ANNP team Medical staff should communicate directly with receiving unit and confirm arrangements for discharge of infant and provide verbal medical summary. Ensure Badger electronic medical summary updated and print copy for receiving unit. Infants who are being discharged home for follow-up in their local hospital should have a nominated consultant for follow-up before discharge and the discharge summary plus other pertinent information must be addressed prior to discharge with parental involvement.
22 Neonatal Care Pathway - Unit Specification Trust BHSCT WHSCT NHSCT SEHSCT SHSCT Area RJMH - NICU Altnagelvin - LNU SWAH- SCBU Antrim- LNU Ulster -LNU (Inc. DP & LV MLUs Craigavon - LNU Daisy Hill - SCBU Gestational range after consultant paediatrician to consultant neonatologist discussion*, 24 weeks onwards. We currently look after babies of all gestations. Babies between may be transferred in utero if there is cot available in RJMH. 34 weeks and above 27 completed weeks and above. Capable of caring for 24-26wks gestation if NNU RJMH is unable to accept. In utero or post delivery transfer to RJMH requested at this extreme prematurity. 28 weeks onwards 28+ wks 27+ wks following discussion with Consultant 34+ weeks and above; 32 weeks to 34 weeks following discussion with Consultant Criteria for care at Hospital what are you routinely providing currently? Ventilation what type long term, short term Short and long term. Short and long term. Less than 1 day Short and long term Short and long term Short and long term Short term HFOV yes yes no yes No Yes no Nitric Oxide yes No no no No No no Non invasive resp. support yes Yes yes yes Yes Yes Yes CPAP 24 hrs limit TPN yes Yes yes yes Yes Yes Yes Surgery include. NEC yes No no no No No no Therapeutic hypothermia yes Yes no yes Yes Yes Passive only until transfer out Transfer and repatriation If a baby from your Trust is resident in another unit. If a baby from another Trust is resident in your unit. A Belfast Trust baby born elsewhere will be accepted when a cot is available. Repatriation will be anticipated once the baby is clinically stable and meets the clinical pathway threshold for the local unit. WHSCT all babies born elsewhere will be accepted when a cot is available. Repatriation will be anticipated once the baby is clinically stable and meets the clinical pathway threshold for their local unit/ special care unit A southern sector western trust baby will be accepted back from another hospital when not ventilated and a cot available. Uncommon Repatriation once Meeting clinical / infection control criteria for Northern Trust and cot and isolation room available. The Neonatal Chief / Clinical Team will override isolation in a side room criterion depending on case mix and NNNI requirements Repatriation will be anticipated once the baby is clinically stable and meets the clinical pathway threshold/ cot available in accepting Local Unit Repatriation to SET when cot available and clinical criteria for SET met. Once the baby is clinically stable and cot available in the local unit A Southern trust baby born elsewhere will be accepted back when an isolation room cot is available Repatriation will be anticipated once the baby is clinically stable and meets the clinical pathway threshold for NNUCAH A Southern trust baby born elsewhere will be accepted back when an isolation room cot is available Repatriation will be anticipated once the baby is clinically stable and meets the clinical pathway threshold for SCBU
23
PROTOCOL FOR DISCHARGING A BABY
 PROTOCOL FOR DISCHARGING A BABY Parents of babies who stay on the neonatal unit are fully supported during their baby s admission and the unit promotes a philosophy of family-centred care. Families often
PROTOCOL FOR DISCHARGING A BABY Parents of babies who stay on the neonatal unit are fully supported during their baby s admission and the unit promotes a philosophy of family-centred care. Families often
Staffordshire, Shropshire & Black Country Newborn and Maternity Network. Neonatal Care Pathways 2015
 Staffordshire, Shropshire & Black Country Newborn and Maternity Network Neonatal Care Pathways 2015 1 Introduction This is a revision to the original Staffordshire, Shropshire and Black Country Newborn
Staffordshire, Shropshire & Black Country Newborn and Maternity Network Neonatal Care Pathways 2015 1 Introduction This is a revision to the original Staffordshire, Shropshire and Black Country Newborn
CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES
 CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES STANDARD OPERATING PROCEDURES Ysbyty Glan Clwyd Telephone No: 01745 534686 Fax No: 01745 534681 Date: June 2015 Authors: Neonatal Transport
CYMRU INTER HOSPITAL ACUTE NEONATAL TRANSFER SERVICE - NORTH WALES STANDARD OPERATING PROCEDURES Ysbyty Glan Clwyd Telephone No: 01745 534686 Fax No: 01745 534681 Date: June 2015 Authors: Neonatal Transport
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care
 Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Quality Surveillance Team. Neonatal Critical Care (NCC) Quality Indicators
 Quality Surveillance Team Neonatal Critical Care (NCC) Quality Indicators Neonatal Critical Care Quality Indicators Introduction These neonatal critical care quality indicators have been developed using
Quality Surveillance Team Neonatal Critical Care (NCC) Quality Indicators Neonatal Critical Care Quality Indicators Introduction These neonatal critical care quality indicators have been developed using
Burton Hospitals NHS Foundation Trust. On: 24 October Review Date: October Corporate / Directorate. Clinical / Non Clinical
 POLICY DOCUMENT Burton Hospitals NHS Foundation Trust DISCHARGE POLICY Approved by: Trust Executive Committee On: 24 October 2017 Review Date: October 2020 Corporate / Directorate Clinical / Non Clinical
POLICY DOCUMENT Burton Hospitals NHS Foundation Trust DISCHARGE POLICY Approved by: Trust Executive Committee On: 24 October 2017 Review Date: October 2020 Corporate / Directorate Clinical / Non Clinical
Trust Guideline for the Management of Postnatal Care: Planning, Information and Discharge Guideline
 Trust Guideline for the Management of Postnatal Care: Planning, A Clinical Guideline recommended for use In: Women s health - Obstetrics By: For: Key words: Written by: Obstetricians, Midwives, Paediatricians
Trust Guideline for the Management of Postnatal Care: Planning, A Clinical Guideline recommended for use In: Women s health - Obstetrics By: For: Key words: Written by: Obstetricians, Midwives, Paediatricians
^Çãáëëáçå=íç=íÜÉ=kÉçå~í~ä=råáí==
 tljbkûpeb^iqe j^qbokfqvrkfq ^ÇãáëëáçåíçíÜÉkÉçå~í~äråáí ^ãéåçãéåíë Date Page(s) Comments Approved by July 2012 Whole Document Document Reviewed Women s Health Guidelines Group Jan 2013 Admission to SCU
tljbkûpeb^iqe j^qbokfqvrkfq ^ÇãáëëáçåíçíÜÉkÉçå~í~äråáí ^ãéåçãéåíë Date Page(s) Comments Approved by July 2012 Whole Document Document Reviewed Women s Health Guidelines Group Jan 2013 Admission to SCU
Certificate of Need (CON) Review Standards for NICU Beds & Special Newborn Nursery Services Effective March 3, 2014
 + Certificate of Need (CON) Review Standards for NICU Beds & Special Newborn Nursery Services Effective March 3, 2014 Northern Michigan Perinatal Summit July 23, 2014 Tulika Bhattacharya, CON Michigan
+ Certificate of Need (CON) Review Standards for NICU Beds & Special Newborn Nursery Services Effective March 3, 2014 Northern Michigan Perinatal Summit July 23, 2014 Tulika Bhattacharya, CON Michigan
Craigavon Area Hospital Profile
 Craigavon Area Hospital Profile 2012 Craigavon Area Hospital Profile Craigavon Area Hospital is located in Craigavon, County Armagh and is an essential part of the hospital network provided by the Southern
Craigavon Area Hospital Profile 2012 Craigavon Area Hospital Profile Craigavon Area Hospital is located in Craigavon, County Armagh and is an essential part of the hospital network provided by the Southern
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY V2. Transfer Policy for Neonates, Infants and Children Page 1 of 36
 TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
TRANSFER POLICY FOR NEONATES, INFANTS AND CHILDREN MAY 2015 Page 1 of 36 Title: Transfer Policy for Neonates, Infants and Children Author(s): Mary McKenna, Head of Acute & Community Paediatrics and Neonatal
Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport
 Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport Transport Service Facilities 1. Access to 24/7 Cheshire and Merseyside Perinatal Cot Bureau and Data Management
Carol Jackson Cheshire and Merseyside Neonatal Network Nurse Consultant for Neonatal Transport Transport Service Facilities 1. Access to 24/7 Cheshire and Merseyside Perinatal Cot Bureau and Data Management
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) E8a SSNDS 23
 E8a 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
E8a 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
Clinical Director for Women s and Children s Directorate
 FEEDING PRETERM AND SMALL FOR GESTATIONAL AGE INFANTS ON THE POSTNATAL WARD CLINICAL GUIDELINES Register No: 08094 Status: Public Developed in response to: Contributes to CQC Regulation 9,11 Intrapartum
FEEDING PRETERM AND SMALL FOR GESTATIONAL AGE INFANTS ON THE POSTNATAL WARD CLINICAL GUIDELINES Register No: 08094 Status: Public Developed in response to: Contributes to CQC Regulation 9,11 Intrapartum
Every Child Counts. Regional Audit of the Child Health Promotion Programme Health Visiting and School Nursing Service
 Every Child Counts Regional Audit of the Child Health Promotion Programme Health Visiting and School Nursing Service March 2016 Contents Page Introduction 3 Background 3 Aim 5 Objectives 5 Standards 5
Every Child Counts Regional Audit of the Child Health Promotion Programme Health Visiting and School Nursing Service March 2016 Contents Page Introduction 3 Background 3 Aim 5 Objectives 5 Standards 5
PROCEDURE FOR RECORD KEEPING FOR HEALTH VISITING
 PROCEDURE FOR RECORD KEEPING FOR HEALTH VISITING Issue History Issue Version One Purpose of Issue/Description of Change Planned Review Date To promote safe and effective record keeping for all staff working
PROCEDURE FOR RECORD KEEPING FOR HEALTH VISITING Issue History Issue Version One Purpose of Issue/Description of Change Planned Review Date To promote safe and effective record keeping for all staff working
Outline. Case 1. Progress 4/23/2013. From hospital to hospice or home How the neonatal team can enable palliative care
 Outline From hospital to hospice or home How the neonatal team can enable palliative care Dr Sharon English Lead Clinician Neonatal Services Leeds Teaching Hospitals NHS Trust Case stories Background Practicalities
Outline From hospital to hospice or home How the neonatal team can enable palliative care Dr Sharon English Lead Clinician Neonatal Services Leeds Teaching Hospitals NHS Trust Case stories Background Practicalities
Best Practice Guidance for Supplementary Prescribing by Nurses Within the HPSS in Northern Ireland. patient CMP
 Best Practice Guidance for Supplementary Prescribing by Nurses Within the HPSS in Northern Ireland patient CMP nurse doctor For further information relating to Nurse Prescribing please contact the Nurse
Best Practice Guidance for Supplementary Prescribing by Nurses Within the HPSS in Northern Ireland patient CMP nurse doctor For further information relating to Nurse Prescribing please contact the Nurse
SCHEDULE 2 THE SERVICES. A. Service Specifications
 Appendix 2 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E08/S/a Neonatal Critical Care (Intensive Care, HDU
Appendix 2 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E08/S/a Neonatal Critical Care (Intensive Care, HDU
Daisy Hill Hospital Profile
 Daisy Hill Hospital Profile 2012 Daisy Hill Hospital Profile Mairead McAlinden, Southern Trust Chief Executive, and Chair Roberta Brownlee welcome Health Minister Edwin Poots on a recent visit to Daisy
Daisy Hill Hospital Profile 2012 Daisy Hill Hospital Profile Mairead McAlinden, Southern Trust Chief Executive, and Chair Roberta Brownlee welcome Health Minister Edwin Poots on a recent visit to Daisy
MIDWIFE AND HEALTH VISITOR COMMUNICATION PROCEDURE
 Appendix 2a of the Health Visiting Overarching Policy MIDWIFE AND HEALTH VISITOR COMMUNICATION PROCEDURE 1. Introduction 1.1. This procedure sets out standards of best practice regarding communication
Appendix 2a of the Health Visiting Overarching Policy MIDWIFE AND HEALTH VISITOR COMMUNICATION PROCEDURE 1. Introduction 1.1. This procedure sets out standards of best practice regarding communication
Neo-natal Jaundice Guidelines
 SH CP 53 Version: 3 Summary: Keywords (minimum of 5): (To assist policy search engine) Target Audience: This document defines the guideline for management of jaundice and the early identification of liver
SH CP 53 Version: 3 Summary: Keywords (minimum of 5): (To assist policy search engine) Target Audience: This document defines the guideline for management of jaundice and the early identification of liver
Inguinal hernia repair integrated care pathway (ICP)
 Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Clinical Skills Passport for Relief and Temporary Staff in Neonatal Units
 Clinical Skills Passport for Relief and Temporary Staff in Neonatal Units This work is drawn from the Scottish Neonatal Nurses Group document The Competency Framework and Core Clinical Skills for Neonatal
Clinical Skills Passport for Relief and Temporary Staff in Neonatal Units This work is drawn from the Scottish Neonatal Nurses Group document The Competency Framework and Core Clinical Skills for Neonatal
Policy Checklist. Working Group: Administration of Infusion of Intravenous Fluids & Medicines in Neonates (Chairperson: Dr Hogan) YES
 Policy Checklist Name of Policy: Purpose of Policy: Directorate responsible for Policy Name & Title of Author: Does this meet criteria of a Policy? Staff side consultation? Policy for the administration
Policy Checklist Name of Policy: Purpose of Policy: Directorate responsible for Policy Name & Title of Author: Does this meet criteria of a Policy? Staff side consultation? Policy for the administration
ESSENTIAL NEWBORN CARE: INTRODUCTION
 ESSENTIAL NEWBORN CARE: INTRODUCTION Essential Newborn Care Implementation Toolkit 2013 The Introduction defines Essential Newborn Care and provides an overview of Newborn Care in South Africa and how
ESSENTIAL NEWBORN CARE: INTRODUCTION Essential Newborn Care Implementation Toolkit 2013 The Introduction defines Essential Newborn Care and provides an overview of Newborn Care in South Africa and how
Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee
 The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
The Delivery Suite Shift Co-ordinator: Roles and Responsibilities (GL819) This document forms appendix 4 of the Policy document Delivery Suite Staffing (Obstetric, Anaesthetic, Paediatric and Midwifery
Critical Care in Obstetrics Guideline
 This is an official Northern Trust policy and should not be edited in any way Critical Care in Obstetrics Guideline Reference Number: NHSCT/12/515 Target audience: This guideline is directed to all obstetricians,
This is an official Northern Trust policy and should not be edited in any way Critical Care in Obstetrics Guideline Reference Number: NHSCT/12/515 Target audience: This guideline is directed to all obstetricians,
Use of Intravenous devices for administration of fluid therapy in Neonates
 This is an official Northern Trust policy and should not be edited in any way Use of Intravenous devices for administration of fluid therapy in Neonates Reference Number: NHSCT/12/534 Target audience:
This is an official Northern Trust policy and should not be edited in any way Use of Intravenous devices for administration of fluid therapy in Neonates Reference Number: NHSCT/12/534 Target audience:
Welcome to the Neonatal Unit at the Royal Oldham Hospital. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Welcome to the Neonatal Unit at the Royal Oldham Hospital An information guide Welcome to the Neonatal Unit at the Royal Oldham Hospital
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Welcome to the Neonatal Unit at the Royal Oldham Hospital An information guide Welcome to the Neonatal Unit at the Royal Oldham Hospital
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012
 Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
Policy on Admission of Children To The Acute Children s Wards Within the WHSCT August 2012 Page 1 of 9 Title Acute Children s Wards Within the WHSCT Reference Number WC12/007 Implementation Date August
South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines. Version 1.0
 South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines Version 1.0 Ratified: 28 th August 2018 Date for Review: 28 th August 2019 Suzanne.sweeney@uclpartners.com South London
South London Neonatal Network Hypoxic Ischemic Encephalopathy Transfer Guidelines Version 1.0 Ratified: 28 th August 2018 Date for Review: 28 th August 2019 Suzanne.sweeney@uclpartners.com South London
Assignment 2: KMC Global: Ghana
 Assignment 2: KMC Global: Ghana Ghana o Household About 1/3 are women 40% of Ghanaian population is under age 15 Families often live with extended family members Tradition of either move in to live with
Assignment 2: KMC Global: Ghana Ghana o Household About 1/3 are women 40% of Ghanaian population is under age 15 Families often live with extended family members Tradition of either move in to live with
North York General Hospital Policy Manual
 ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
Mapping maternity services in Australia: location, classification and services
 Accessory publication Mapping maternity services in Australia: location, classification and services Caroline S. E. Homer 1,4 RM, MMedSci(ClinEpi), PhD, Professor of Midwifery Janice Biggs 2 BA(Hons),
Accessory publication Mapping maternity services in Australia: location, classification and services Caroline S. E. Homer 1,4 RM, MMedSci(ClinEpi), PhD, Professor of Midwifery Janice Biggs 2 BA(Hons),
North West London Perinatal Network (NWLPODN) Induction Package. NWLPODN March
 North West London Perinatal Network (NWLPODN) Induction Package NWLPODN March 2015 1 Introduction This package is for staff working within the 7 NWLPODN hospitals: To explain how the NWLPODN functions
North West London Perinatal Network (NWLPODN) Induction Package NWLPODN March 2015 1 Introduction This package is for staff working within the 7 NWLPODN hospitals: To explain how the NWLPODN functions
Neonatal Intensive Care Unit (NICU) Level of Care Authorization and Reimbursement Policy
 In the event of conflict between a Clinical Payment and Coding Policy and any plan document under which a member is entitled to Covered Services, the plan document will govern. Plan documents include,
In the event of conflict between a Clinical Payment and Coding Policy and any plan document under which a member is entitled to Covered Services, the plan document will govern. Plan documents include,
South Central Neonatal Network
 South Central Neonatal Network Education and training strategy: Continuing education and professional development Authored by Sue Turrill, School of Healthcare, University of Leeds, February 2012 Final
South Central Neonatal Network Education and training strategy: Continuing education and professional development Authored by Sue Turrill, School of Healthcare, University of Leeds, February 2012 Final
KANGAROO MOTHER CARE PROGRESS MONITORING TOOL (Version 4)
 MRC Research Unit for Maternal and Infant Health Care Strategies, 2002, 2004, 2007, 2009 University of Pretoria and Kalafong Hospital PO Box 667, Pretoria 0001, South Africa KANGAROO MOTHER CARE PROGRESS
MRC Research Unit for Maternal and Infant Health Care Strategies, 2002, 2004, 2007, 2009 University of Pretoria and Kalafong Hospital PO Box 667, Pretoria 0001, South Africa KANGAROO MOTHER CARE PROGRESS
Changing for the Better 5 Year Strategic Plan
 Quality Care - for you, with you 5 Year Strategic Plan Contents: Section 1: Vision and Priorities for Change 3 Section 2: About the Trust 5 Section 3: Promoting Health & Wellbeing and Primary Care 6 Section
Quality Care - for you, with you 5 Year Strategic Plan Contents: Section 1: Vision and Priorities for Change 3 Section 2: About the Trust 5 Section 3: Promoting Health & Wellbeing and Primary Care 6 Section
Examination of the Newborn by Registered Midwives Protocol (CG484)
 Examination of the Newborn by Registered Midwives Protocol (CG484) Approval and Authorisation Approved by Maternity Clinical Governance Committee Job Title or Chair of Committee Chair, Maternity Clinical
Examination of the Newborn by Registered Midwives Protocol (CG484) Approval and Authorisation Approved by Maternity Clinical Governance Committee Job Title or Chair of Committee Chair, Maternity Clinical
What You Need To Know When Your Child Is Having Craniofacial Surgery
 What You Need To Know When Your Child Is Having Craniofacial Surgery Main Hospital Number 01 878 4200 Craniofacial Office 01 878 4883 email; craniofacial@cuh.ie Pre Operative (Surgery) Assessment Appointment
What You Need To Know When Your Child Is Having Craniofacial Surgery Main Hospital Number 01 878 4200 Craniofacial Office 01 878 4883 email; craniofacial@cuh.ie Pre Operative (Surgery) Assessment Appointment
Organization: Adventist Healthcare Shady Grove Medical Center
 Organization: Adventist Healthcare Shady Grove Medical Center Title: A Team-Based, Innovative Approach to Providing Safer Care by Reducing the Incidence of Chronic Lung Disease in the Premature Newborn
Organization: Adventist Healthcare Shady Grove Medical Center Title: A Team-Based, Innovative Approach to Providing Safer Care by Reducing the Incidence of Chronic Lung Disease in the Premature Newborn
Review by RQIA of Northern Ireland Single Assessment Tool Stage One
 Review by RQIA of Northern Ireland Single Assessment Tool Stage One Overview Report October 2011 Section 1 Contents Page 1.0 The Regulation and Quality Improvement Authority 1 2.0 Context for the Review
Review by RQIA of Northern Ireland Single Assessment Tool Stage One Overview Report October 2011 Section 1 Contents Page 1.0 The Regulation and Quality Improvement Authority 1 2.0 Context for the Review
Standard of Care for MTC inpatients
 Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
Consulted With Post/Committee/Group Date Dr Agrawal
 DRUG AND ALCOHOL MISUSE IN PREGNANCY CLINICAL GUIDELINES Register No: 06056 Status: Public Developed in response to: Contributes to CQC Outcome 4 Intrapartum NICE Guidelines RCOG guideline Consulted With
DRUG AND ALCOHOL MISUSE IN PREGNANCY CLINICAL GUIDELINES Register No: 06056 Status: Public Developed in response to: Contributes to CQC Outcome 4 Intrapartum NICE Guidelines RCOG guideline Consulted With
Micro-Preemies.Macro Outcomes Keywords: Background: Global AIM: Secondary Aims: Golden Hour Charter (Focus on thermoregulation): Respiratory Charter
 Micro-Preemies.Macro Outcomes Carey Gaede, NNP-BC; Mary Jane Zonfrilli, NNP-BC; Stephanie King, RRT; Sara Dalbey, NNP-BC; Lisa Davis, NNP-BC; William Stratton, MD Primary: Carey Gaede, NNP-BC; e-mail:
Micro-Preemies.Macro Outcomes Carey Gaede, NNP-BC; Mary Jane Zonfrilli, NNP-BC; Stephanie King, RRT; Sara Dalbey, NNP-BC; Lisa Davis, NNP-BC; William Stratton, MD Primary: Carey Gaede, NNP-BC; e-mail:
MEETING THE NEONATAL CHALLENGE. Dr.B.Kishore Assistant Commissioner (CH), GoI New Delhi November 14, 2009
 MEETING THE NEONATAL CHALLENGE Dr.B.Kishore Assistant Commissioner (CH), GoI New Delhi November 14, 2009 Presentation Outline 1. Background 2. Key Initiatives of GoI 3. Progress 4. Major challenges & way
MEETING THE NEONATAL CHALLENGE Dr.B.Kishore Assistant Commissioner (CH), GoI New Delhi November 14, 2009 Presentation Outline 1. Background 2. Key Initiatives of GoI 3. Progress 4. Major challenges & way
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW)
 APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW) 1 ST0217/01 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Assistant,
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW) 1 ST0217/01 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Assistant,
SCHEDULE 2 THE SERVICES
 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service E08/S/b Neonatal Intensive Care Transport Commissioner Lead Provider Lead Period Date of Review 12 Months 1. Population
SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service E08/S/b Neonatal Intensive Care Transport Commissioner Lead Provider Lead Period Date of Review 12 Months 1. Population
Annie Hunter Head of Midwifery Isle of Wight NHS
 Annie Hunter Head of Midwifery Isle of Wight NHS The Isle of Wight has a population of 140,500, this doubles in the holiday season with the Island receiving approximately 2.8 million visitors each year.
Annie Hunter Head of Midwifery Isle of Wight NHS The Isle of Wight has a population of 140,500, this doubles in the holiday season with the Island receiving approximately 2.8 million visitors each year.
Paper 5.0 SHAPING A HEALTHIER FUTURE PAEDIATRIC TRANSITION: ANTICIPATED BENEFITS OF THE TRANSITION AND PROPOSED MODEL OF CARE.
 SHAPING A HEALTHIER FUTURE PAEDIATRIC TRANSITION: ANTICIPATED BENEFITS OF THE TRANSITION AND PROPOSED MODEL OF CARE December 2015 Version 2.2 Paper 5.0 1 Purpose This document sets out the proposed new
SHAPING A HEALTHIER FUTURE PAEDIATRIC TRANSITION: ANTICIPATED BENEFITS OF THE TRANSITION AND PROPOSED MODEL OF CARE December 2015 Version 2.2 Paper 5.0 1 Purpose This document sets out the proposed new
CLINICAL PROTOCOL FOR THE HEALTHY CHILD PROGRAMME
 CLINICAL PROTOCOL FOR THE HEALTHY CHILD PROGRAMME RATIONALE In establishing the foundations of good health, the Healthy Child Programme (HCP) makes a crucial contribution to the Every Child Matters outcomes
CLINICAL PROTOCOL FOR THE HEALTHY CHILD PROGRAMME RATIONALE In establishing the foundations of good health, the Healthy Child Programme (HCP) makes a crucial contribution to the Every Child Matters outcomes
MULTIDISCIPLINARY MEETINGS FOR COMMUNITY HOSPITALS POLICY
 MULTIDISCIPLINARY MEETINGS FOR COMMUNITY HOSPITALS POLICY (To be read in conjunction with Handover Policy) Version: 3 Ratified by: Date ratified: August 2015 Title of originator/author: Title of responsible
MULTIDISCIPLINARY MEETINGS FOR COMMUNITY HOSPITALS POLICY (To be read in conjunction with Handover Policy) Version: 3 Ratified by: Date ratified: August 2015 Title of originator/author: Title of responsible
Health Visiting Implementation Programme for Herefordshire. Marcia Perry Service Unit Manager Integrated Family Health Services 11 th October 2012
 Health Visiting Implementation Programme for Herefordshire Marcia Perry Service Unit Manager Integrated Family Health Services 11 th October 2012 Local Demography Strengths and Challenges Large geographical
Health Visiting Implementation Programme for Herefordshire Marcia Perry Service Unit Manager Integrated Family Health Services 11 th October 2012 Local Demography Strengths and Challenges Large geographical
OXYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0
 OYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline 1.1 To provide guidance on the assessment and management of infants requiring oxygen therapy
OYGEN THERAPY AND SATURATION MONITORING OF THE NEONATE - CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline 1.1 To provide guidance on the assessment and management of infants requiring oxygen therapy
Examination of the newborn competency tool
 Examination of the newborn competency tool This tool can be used as a guide to assessment of clinical competence (minimal competence level to be achieved by midwives is four) or simply as a checklist for
Examination of the newborn competency tool This tool can be used as a guide to assessment of clinical competence (minimal competence level to be achieved by midwives is four) or simply as a checklist for
Parental Views on Maternity Services
 www.patientclientcouncil.hscni.net Parental Views on Maternity Services Parents Views on the Review of Maternity Services for Northern Ireland Your voice in health and social care 1 This information is
www.patientclientcouncil.hscni.net Parental Views on Maternity Services Parents Views on the Review of Maternity Services for Northern Ireland Your voice in health and social care 1 This information is
ECMO a parent and family guide
 ECMO a parent and family guide This leaflet aims to provide you with some basic information about ECMO, and will hopefully answer some questions that you may have in helping to decide on ECMO for your
ECMO a parent and family guide This leaflet aims to provide you with some basic information about ECMO, and will hopefully answer some questions that you may have in helping to decide on ECMO for your
STUDENT OVERVIEW AT A GLANCE
 STUDENT OVERVIEW AT A GLANCE Great North Children s Hospital and New Victoria Wing are home to the department of paediatric and teenage oncology. This consists of a children s inpatient unit (Ward 4),
STUDENT OVERVIEW AT A GLANCE Great North Children s Hospital and New Victoria Wing are home to the department of paediatric and teenage oncology. This consists of a children s inpatient unit (Ward 4),
VERIFICATION OF LIFE EXTINCT POLICY DECEMBER Verification of Life Extinct Policy December 2009 Page 1 of 18
 VERIFICATION OF LIFE EXTINCT POLICY DECEMBER 2009 Page 1 of 18 POLICY TITLE: Verification of Life Extinct Policy POLICY REFERENCE NUMBER: Med01/009 IMPLEMENTATION DATE: December 2009 REVIEW DATE: December
VERIFICATION OF LIFE EXTINCT POLICY DECEMBER 2009 Page 1 of 18 POLICY TITLE: Verification of Life Extinct Policy POLICY REFERENCE NUMBER: Med01/009 IMPLEMENTATION DATE: December 2009 REVIEW DATE: December
Preparing and Registering S.T.A.B.L.E. Support Instructors
 Preparing and Registering S.T.A.B.L.E. Support Instructors If a person is unable to attend an official National or Private Instructor course, but they wish to co-teach a S.T.A.B.L.E. Learner course with
Preparing and Registering S.T.A.B.L.E. Support Instructors If a person is unable to attend an official National or Private Instructor course, but they wish to co-teach a S.T.A.B.L.E. Learner course with
Your Health Visiting Service
 Your Health Visiting Service Information for new parents Welcome to the Health Visiting Service in Lothian We would like to take this opportunity to welcome you to the Health Visiting Service in Lothian.
Your Health Visiting Service Information for new parents Welcome to the Health Visiting Service in Lothian We would like to take this opportunity to welcome you to the Health Visiting Service in Lothian.
STUDENTS WELCOME TO YOUR PLACEMENT. On the. Neonatal Unit, RHCH
 STUDENTS WELCOME TO YOUR PLACEMENT On the Neonatal Unit, RHCH Dear Student Welcome to Hampshire Hospitals NHS Foundation Trust. We hope you find your placement at HHFT rewarding and enjoyable and your
STUDENTS WELCOME TO YOUR PLACEMENT On the Neonatal Unit, RHCH Dear Student Welcome to Hampshire Hospitals NHS Foundation Trust. We hope you find your placement at HHFT rewarding and enjoyable and your
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW)
 APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW) 1 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Assistant, Mental
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (HCSW) 1 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Assistant, Mental
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (SHCSW)
 APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (SHCSW) 1 ST0217/02 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Support
APPRENTICESHIP STANDARD FOR SENIOR HEALTHCARE SUPPORT WORKER (SHCSW) 1 ST0217/02 Typical job titles: Senior Healthcare Support Worker, Senior Healthcare Assistant, Maternity Support Worker, Theatre Support
The Management of Child Protection Medicals for All Children. And Procedures for the Discharge of Children Under 2 Years of Age
 The Management of Child Protection Medicals for All Children And Procedures for the Discharge of Children Under 2 Years of Age 1. Child safeguarding concern in the community 1.1 Follow guidance in Working
The Management of Child Protection Medicals for All Children And Procedures for the Discharge of Children Under 2 Years of Age 1. Child safeguarding concern in the community 1.1 Follow guidance in Working
User Requirements Specification. Family Health Assessment. For. Version v.10. Prepared by BSO. December FHA URS v 10 MC
 User Requirements Specification For Family Health Assessment Version v.10 Prepared by BSO December 2010 2010-12-03 FHA URS v 10 MC Page ii Table of Contents Table of Contents... ii Revision History...
User Requirements Specification For Family Health Assessment Version v.10 Prepared by BSO December 2010 2010-12-03 FHA URS v 10 MC Page ii Table of Contents Table of Contents... ii Revision History...
1. CRITICAL CARE. Preamble. Adult and Pediatric Critical Care
 1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
Maternal Child Adolescent Health Program Assessment. Rebecca Scherr, MD February 26, 2015
 Maternal Child Adolescent Health Program Assessment Rebecca Scherr, MD February 26, 2015 Programs Community Health Nursing/MCAH Kids Clinic (clinical-exams for children) Refugee Health program (screening
Maternal Child Adolescent Health Program Assessment Rebecca Scherr, MD February 26, 2015 Programs Community Health Nursing/MCAH Kids Clinic (clinical-exams for children) Refugee Health program (screening
YOU RE IN GOOD HANDS THANK YOU FOR CHOOSING ST VINCENT S PRIVATE HOSPITAL WERRIBEE
 YOU RE IN GOOD HANDS THANK YOU FOR CHOOSING ST VINCENT S PRIVATE HOSPITAL WERRIBEE Welcome to St Vincent s Private Hospital werribee From the moment you step through our doors we re looking out for you
YOU RE IN GOOD HANDS THANK YOU FOR CHOOSING ST VINCENT S PRIVATE HOSPITAL WERRIBEE Welcome to St Vincent s Private Hospital werribee From the moment you step through our doors we re looking out for you
Neonatal Implementation. TRANSPORT PATHWAYS (Logistics)
 Neonatal Implementation TRANSPORT PATHWAYS (Logistics) The plan is to transfer the longer term and complex neonatal intensive care to the Neonatal Intensive Care Unit (NICU) in Arrowe Park from January
Neonatal Implementation TRANSPORT PATHWAYS (Logistics) The plan is to transfer the longer term and complex neonatal intensive care to the Neonatal Intensive Care Unit (NICU) in Arrowe Park from January
The New NCCMDS, Neonatal HRGs 2016 and Reference Costs. A Guide for Clinicians
 The New NCCMDS, Neonatal HRGs 2016 and Reference Costs A Guide for Clinicians Aim To help clinicians involved in neonatal care to understand the changes that have taken place to the NCCMDS dataset the
The New NCCMDS, Neonatal HRGs 2016 and Reference Costs A Guide for Clinicians Aim To help clinicians involved in neonatal care to understand the changes that have taken place to the NCCMDS dataset the
Serious Incident Report Public Board Meeting 28 July 2016
 Serious Incident Report Public Board Meeting 28 July 2016 Presented for: Presented by: Author Previous Committees Governance Dr Yvette Oade, Chief Medical Officer Louise Povey, Serious Incidents Investigations
Serious Incident Report Public Board Meeting 28 July 2016 Presented for: Presented by: Author Previous Committees Governance Dr Yvette Oade, Chief Medical Officer Louise Povey, Serious Incidents Investigations
Patient Self Administration of Intravenous (IV) Antibiotics at Home
 Trust Policy Document Ref. No: PP(16)319 Patient Self Administration of Intravenous (IV) Antibiotics at Home For use in: For use by: For use for: Document owner: Status: Clinical Areas Clinical Staff Patient
Trust Policy Document Ref. No: PP(16)319 Patient Self Administration of Intravenous (IV) Antibiotics at Home For use in: For use by: For use for: Document owner: Status: Clinical Areas Clinical Staff Patient
SCHEDULE 2 THE SERVICES. A. Service Specifications. E07/S/c Paediatric Long Term Ventilation
 Appendix 2 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E07/S/c Paediatric Long Term Ventilation 1. Population
Appendix 2 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E07/S/c Paediatric Long Term Ventilation 1. Population
An investigation of breastfeeding support in Coventry November 2012
 An investigation of breastfeeding support in Coventry November 2012 Responses received 1 LINk s Recommendations 1. Commissioners ensure adequate provision of antenatal support for women in pregnancy regarding
An investigation of breastfeeding support in Coventry November 2012 Responses received 1 LINk s Recommendations 1. Commissioners ensure adequate provision of antenatal support for women in pregnancy regarding
Wales Critical Care & Trauma Network (North)
 Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
Wales Critical Care & Trauma Network (North) CRITICAL CARE ADMISSION & DISCHARGE GUIDELINES Revised 2016 1 CONTENTS: 1.0 Introduction 1.1 Scope of the Guideline 1.2 Levels of Care 2.0 Admission Guidance
SCBU Escalation Policy & Procedure
 Page 1 of 6 AGENDA ITEM: 5(d) SCBU Escalation Policy & Procedure Page 2 of 6 The Special Care Baby Unit at Colchester General Hospital admits over 500 babies each year and has a capacity of 18 cots within
Page 1 of 6 AGENDA ITEM: 5(d) SCBU Escalation Policy & Procedure Page 2 of 6 The Special Care Baby Unit at Colchester General Hospital admits over 500 babies each year and has a capacity of 18 cots within
Patient Transfer Policy
 Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
Handover of Care (Maternity) Guidelines Author s job title Lead Clinical Midwife Department Ladywell Unit. Comment / Changes / Approval
 Document Control Title Author Directorate Surgery Date Version Issued 0.1 Oct 2009 0.2 Nov 2009 1.0 Nov 2009 1.1 Feb 2010 2.0 Feb 2010 2.1 Aug 2011 2.2 Oct 2011 Handover of Care (Maternity) Guidelines
Document Control Title Author Directorate Surgery Date Version Issued 0.1 Oct 2009 0.2 Nov 2009 1.0 Nov 2009 1.1 Feb 2010 2.0 Feb 2010 2.1 Aug 2011 2.2 Oct 2011 Handover of Care (Maternity) Guidelines
April Authors. Directorate responsible for this Document Date of Issue April 2014 Review Date April 2016 Version 3
 ASSESSMENT, ADMISSION AND DISCHARGE POLICY AND PROCEDURES FOR CHILDREN AND YOUNG PEOPLE UNDER THE AGE OF 18 YEARS ABOUT WHOM THERE ARE SAFEGUARDING CONCERNS WITHIN ACUTE SERVICES (Version 3) April 2014
ASSESSMENT, ADMISSION AND DISCHARGE POLICY AND PROCEDURES FOR CHILDREN AND YOUNG PEOPLE UNDER THE AGE OF 18 YEARS ABOUT WHOM THERE ARE SAFEGUARDING CONCERNS WITHIN ACUTE SERVICES (Version 3) April 2014
Acutely ill patients in hospital
 Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
Issue date: July 2007 Acutely ill patients in hospital Recognition of and response to acute illness in adults in hospital Developed by the Centre for Clinical Practice at NICE Contents Key priorities for
6: What care is available?
 6: What care is available? This section identifies and explains the types of care on offer at end of life and who is involved. The following information is an extracted section from our full guide End
6: What care is available? This section identifies and explains the types of care on offer at end of life and who is involved. The following information is an extracted section from our full guide End
South Canterbury District Health Board
 South Canterbury District Health Board - Timaru Hospital Introduction This report records the results of a Surveillance Audit of a provider of hospital services against the Health and Disability Services
South Canterbury District Health Board - Timaru Hospital Introduction This report records the results of a Surveillance Audit of a provider of hospital services against the Health and Disability Services
Greater Manchester Neuro-Rehabilitation Services information for patients and carers
 THIS BOOKLET IS BEING TRIALLED Greater Manchester Neuro-Rehabilitation Services information for patients and carers Greater Manchester Neuro-Rehabilitation Services gmnrodn@srft.nhs.uk All Rights Reserved
THIS BOOKLET IS BEING TRIALLED Greater Manchester Neuro-Rehabilitation Services information for patients and carers Greater Manchester Neuro-Rehabilitation Services gmnrodn@srft.nhs.uk All Rights Reserved
Catherine Hughson Kathryn Kearney Number of supervisors relinquishing role since last report:
 Name of Local Supervising Authority: Western Isles Health Board Period of report: 2005/2006 Date: September 2006 1. Supervision of Midwives and Midwifery Practice 1.1 Designated Local Supervising Authority
Name of Local Supervising Authority: Western Isles Health Board Period of report: 2005/2006 Date: September 2006 1. Supervision of Midwives and Midwifery Practice 1.1 Designated Local Supervising Authority
Nursing staff requirements for neonatal intensive
 54 Archives of Disease in Childhood 199; 68: 54-58 ORIGINAL ARTICLES Mersey Regional Neonatal Intensive Care Unit, Liverpool Maternity Hospital, Oxford Street, Liverpool L7 7BN S Williams A Whelan A M
54 Archives of Disease in Childhood 199; 68: 54-58 ORIGINAL ARTICLES Mersey Regional Neonatal Intensive Care Unit, Liverpool Maternity Hospital, Oxford Street, Liverpool L7 7BN S Williams A Whelan A M
Pregnancy Information Sharing Pathway for Safeguarding Children (Midwifery, Health Visiting and Primary Care)
 Pregnancy Information Sharing Pathway for Safeguarding Children (Midwifery, Health Visiting and Primary Care) July 2010 Originator: Women and Child Health /Primary Care/Safeguarding Team Submitted by:
Pregnancy Information Sharing Pathway for Safeguarding Children (Midwifery, Health Visiting and Primary Care) July 2010 Originator: Women and Child Health /Primary Care/Safeguarding Team Submitted by:
Clinical Care Pathway for BRAIN TUMOURS in Childhood.
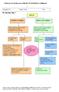 - 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
- 1 - Pre Operation Page 1 Referral Unstable or ventilated Stable or non ventilated Discuss with on-call Consultant Neurosurgeon & PICU Imagelink scans if possible Discuss with on-call Consultant Neurosurgeon
MATERNITY UNIT.
 MATERNITY UNIT www.ahmedalkadi.com Rooming-In Ahmed Al-Kadi Private Hospital practices rooming-in. This allows mothers and babies to remain together 24 hours a day. Rooming-in helps mothers bond with their
MATERNITY UNIT www.ahmedalkadi.com Rooming-In Ahmed Al-Kadi Private Hospital practices rooming-in. This allows mothers and babies to remain together 24 hours a day. Rooming-in helps mothers bond with their
IV. Global Summit for Preemies
 The importance of mental support for parents during NICU and beyond Dora Monostori (Hungary) 1, University of Szeged, Faculty of Health and Social Care 2, University of Pécs, Faculty of Health Sciences,
The importance of mental support for parents during NICU and beyond Dora Monostori (Hungary) 1, University of Szeged, Faculty of Health and Social Care 2, University of Pécs, Faculty of Health Sciences,
Managing Emergency Pressures Within The Neonatal Unit. Escalation Policy. V3
 Managing Emergency Pressures Within The Neonatal Unit. Escalation Policy. V3 Lead Person(s) : Ian MacLennan, Nurse Manager. Centre : Women and Children s First developed : March 2012 Last updated : March
Managing Emergency Pressures Within The Neonatal Unit. Escalation Policy. V3 Lead Person(s) : Ian MacLennan, Nurse Manager. Centre : Women and Children s First developed : March 2012 Last updated : March
Integrated Comfort Care Pathway (ICCP) - Newborn*
 Integrated Comfort Care Pathway (ICCP) - Newborn* Parent name & contact details.. Relationship to newborn Parental responsibility Parent name & contact details.. Relationship to newborn Parental responsibility
Integrated Comfort Care Pathway (ICCP) - Newborn* Parent name & contact details.. Relationship to newborn Parental responsibility Parent name & contact details.. Relationship to newborn Parental responsibility
Cover for pregnancy and childbirth
 Cover for pregnancy and childbirth 2017 How we cover pregnancy and childbirth in 2017 The Maternity Benefit covers day-to-day and in-hospital medical expenses for expectant mothers and newborns. Overview
Cover for pregnancy and childbirth 2017 How we cover pregnancy and childbirth in 2017 The Maternity Benefit covers day-to-day and in-hospital medical expenses for expectant mothers and newborns. Overview
Family Birth Place at Baptist Hospital
 Family Birth Place at Baptist Hospital Pregnancy Is a Stage of Parenthood The birth of a baby is an exciting time perhaps one of life s most special events. This booklet has been designed to give you
Family Birth Place at Baptist Hospital Pregnancy Is a Stage of Parenthood The birth of a baby is an exciting time perhaps one of life s most special events. This booklet has been designed to give you
Audit on Record Keeping in the Acute Hospital Setting Final report produced: 2 September 2015
 Audit on Record Keeping in the Acute Hospital Setting Final report produced: 2 September 2015 Audit on Record Keeping in the Acute Hospital Setting Page 1 of 71 Contents Introduction Background to the
Audit on Record Keeping in the Acute Hospital Setting Final report produced: 2 September 2015 Audit on Record Keeping in the Acute Hospital Setting Page 1 of 71 Contents Introduction Background to the
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation
 Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Specialised Services Commissioning Policy: CP160 Specialised Paediatric Neurological Rehabilitation April 2018 Version 4.0 Document information Document purpose Document name Author Policy Specialised
Advanced Neonatal Nurse Practitioner Medway NHS Foundation Trust
 Advanced Neonatal Nurse Practitioner Medway NHS Foundation Trust Come and join us at Medway NHS FT Whether you re a porter or a nurse, a pharmacist or a housekeeper, a doctor or an IT expert, you can have
Advanced Neonatal Nurse Practitioner Medway NHS Foundation Trust Come and join us at Medway NHS FT Whether you re a porter or a nurse, a pharmacist or a housekeeper, a doctor or an IT expert, you can have
JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach.
 JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach. JOB TITLE: GRADE: BASE: MANAGED BY: Advanced Neonatal Nurse Practitioner Band 8a Homerton
JOB DESCRIPTION Safe, compassionate, effective care provided to our communities with a transparent, open approach. JOB TITLE: GRADE: BASE: MANAGED BY: Advanced Neonatal Nurse Practitioner Band 8a Homerton
