Knowledge about endotracheal suctioning on the part of intensive care nursing professionals: a descriptive study
|
|
|
- Baldric Parrish
- 6 years ago
- Views:
Transcription
1 ISSN: Knowledge about endotracheal suctioning on the part of intensive care nursing professionals: a descriptive study Oleci Pereira Frota 1, Marisa Dias Rolan Loureiro 1, Adriano Menis Ferreira 1 1 Federal University of Mato Grosso do Sul ABSTRACT Aim: To evaluate the knowledge of nursing professionals in the Intensive Care Unit (ICU) about endotracheal aspiration (ETA) for open system. Method: This an exploratory descriptive study in which a quantitative approach was used, performed in July 2011 in two ICUs of a large university hospital in Mato Grosso do Sul, Brazil. Data were collected through the means of a questionnaire. The sample consisted of 27 professionals of whom 51.9% were male. Results: Globally, the knowledge of professionals was qualified as fair (73.2% correct), but worryingly, it was considered poor in five areas with differing results among the professional categories. Discussion: Taking into account that incorrect knowledge generates inappropriate behavior, it is inferred that the practice of these subjects may compromise patient safety. Conclusion: The studied individuals showed knowledge deficits in some aspects of ETA, a fact that deserves investment regarding teaching and nursing. Descriptors: Critical Care; Respiration, Artificial; Health Knowledge, Attitudes, Practice; Employee Performance Appraisal; Nursing, Team; Questionnaires. 546
2 INTRODUCTION One of the main goals of nursing is to provide evidence-based assistance in order to promote quality results for patients, families and the healthcare system. A procedure that deserves particular attention, given its direct relationship with the risk of infection, is the endotracheal aspiration (ETA) of intubated patients (1). The ETA is an essential component in airway management in patients on mechanical ventilation, being one of the most frequently performed invasive procedures in the Intensive Care Unit (ICU). Its main goal is to remove accumulated lung secretions in order to maintain the airway s permeability; provide adequate oxygenation; reduce the risk of ventilator-associated pneumonia (VAP) and prevent pulmonary consolidation and atelectasis (2). The procedure, however, is not free of risks and complications. Comorbidities such as cardiac and/or respiratory failure, hemodynamic instability, tracheobronchial injury and hypoxemia may be a result of the procedure, especially when performed incorrectly (3). Therefore, it is imperative that this procedure is performed with professional competence, which means not only having the necessary skills, but also knowledge based on updated scientific evidence, guaranteeing efficiency and the safety of the patient (4). However, research has shown that nursing practitioners do not have sufficient knowledge of the current recommendations for ETA and, according to empirical evidence, the practice is often based on rituals and traditions (4.5). Therefore, the question is: What is the knowledge of intensive care nursing professionals about the ETA procedure for open system in the light of the evidence? To answer this question we proposed this study, which aims to assess the knowledge of ICU nursing professionals relating to ETA for open systems. The justification for this study represents a diagnostic step of paramount importance. We propose to investigate and critically evaluate the knowledge of professionals and identify the skills and difficulties involved, and, based on this data, develop operational measures that contribute to improvement in the quality of the services provided. METHOD This is an exploratory, descriptive study, whose data collection was conducted in July 2011 in two ICUs (general and cardiac). These ICUs provide care for adult patients at a large university hospital in Mato Grosso do Sul. The study was approved by the Ethics Committee on Human Research of the Federal University of Mato Grosso do Sul under the protocol No. 1949/2011. The study included all the nursing professionals from the sectors investigated, so that the population was represented by 34 nurses, 18 working in the General ICU (two nurses, four nursing technicians and 12 nursing assistants) and 16 in the Cardiological ICU (two nurses, eight nursing technicians and six nursing assistants). However, we excluded the professionals who were on leave or vacation during the period of data collection and those who had less than one year of experience in the area of intensive care. Thus, the sample consisted of 27 professionals. To meet the objective of this investigation we built a structured questionnaire composed of items relating to socio-demographic data and knowledge tests. The latter was aimed at identifying the level of knowledge of participants regarding the current recommended actions before, during and after the ETA technique for open systems, as well as prevention and infection control. 547
3 In the final version, the component knowledge test consisted of 17 closed questions, as follows: 13 affirmations for which an X should be marked for one of the possible alternatives, true (T), false (F) or I do not know (it was considered as a correct question the true statements answered as T or false answered as F); three questions with multiple choice answers, in which case the assessed individual should mark an X next to the answer(s) he/ she considered correct (with these questions, all options were correct and it was considered as correct when more than 50% of the alternatives were noted), and finally; a question that dealt with the opinions of the professionals regarding their difficulties in the management of artificial airways. Note that this survey was based on the Guidelines (6) of the American Association for Respiratory Care (AARC) from 2010 and secondarily on other reference studies of the theme (1,7-9), and these were used as parameters to define what was correct or incorrect. Data was collected during working hours, in a specific room. Consultation of bibliographies or co-workers was not allowed, and there was no time limit for completing the questionnaire in order to minimize the possibility of inducing participants to answer without first reading the questionnaire properly and reflecting. Prior to the delivery of the questionnaire, a quick explanation was given to the subjects involved, especially on the objectives of the study, its relevance and method of data collection. Particular emphasis was placed on the need for collaboration and voluntary participation. After reading, signing and returning the Terms of Consent, each participant received the questionnaire. The data was collated using Microsoft Office Excel 2010 version and was analyzed using descriptive statistics. The methods of absolute and percentage distribution were employed, as well as the average and standard deviation for socio-demographics. Moreover, based on an earlier similar study (10) that was initially based on other studies, we established a conceptual assignment) in wich we made a small semantic change) to investigate and classify the variables of knowledge. Furthermore, considering all the studies analyzed on evaluation of knowledge in different areas, there was no consensus for a cut-off point, therefore empiricism and what the authors considered a suitable level of knowledge prevailed. Thus, we considered the following score diagram: equal or less than 59 points poor knowledge ; weak ; average ; good ; 90 to 99 very good and; 100 points was classified as excellent knowledge. RESULTS Of the 27 (100%) professionals investigated 11 (40.8%) worked in the General ICU (two nurses, two nursing technicians and seven nursing assistants) and 16 (59.2%) in the Cardiological ICU (two nurses, eight nursing technicians and six nursing assistants). Of this group, 14 (51.9%) subjects were male. The average age was 40.6 years ± 7 (24-55). The average time of experience in the position was 17.4 years ± 7.6 (1-30) and the average time of exercise in an adult ICU was 10.2 years ± 5.87 (1-23). Among nurses, three (75%) were post graduates in lato sensus courses and; among those at professional training levels, 16 (70%) had completed high school, six (26%) were graduates (three in nursing) and one (4%) was a post graduate in adult intensive care nursing. The evaluation of the knowledge of these professionals regarding ETA is presented in Table
4 Table 1. Characterization of nursing professionals responses (n=27) about the ETA technique. Campo Grande/MS, Brazil, 2011 Answers Variables Correct Incorrect Does not know n % n % N % Before ETA Explanation of the procedure to the patient 25 92,6 1 3,7 1 3,7 Interruption of enteral diet 23 85,2 3 11,1 1 3,7 Pre-oxygenation in order to prevent hypoxemia ,1 7 25,9 Main clinical situations that indicate the ETA 26 96,3 1 3,7 0 0 Routine AET (pre-set times) or only when needed 25 92,6 1 3,7 1 3,7 During ETA Routine instillation of SF 0.9% in the TET * 12 44, ,5 Use of suction catheter of appropriate diameter 16 59, ,8 Maximum suction time (open vacuum) 9 33, ,8 7 25,9 Monitoring of pulse oximetry 26 96,3 1 3,7 0 0 Procedure to insert the suction catheter in TET * (open or closed vacuum) 25 92,6 2 7,4 0 0 After ETA Main effects/adverse reactions related to ETA 5 18, ,5 0 0 Main parameters that should be evaluated during and after ETA 21 77,8 6 22,2 0 0 Routine hyperventilation as a way of preventing hypoxemia 12 44,5 9 31,3 6 22,2 Practices for the prevention and control of infections Hand hygiene before and after ETA, as well as the use of gloves, goggles and apron Permanence of sterility of the suction catheter 25 92,6 2 7,4 0 0 Aspiration sequence (trachea, nose and lastly the oral cavity) 22 81,5 5 18,5 0 0 Global average 19,7 73,2 4,8 17,8 2,5 9 * Endotracheal tube (orotracheal/nasotracheal tube and tracheostomy cannula) Source: Research data. Knowledge of professionals: according to the diagram score used in this study, the global knowledge of nurses was good (success rate of 85.3%); the nursing technicians it was average (success rate of 72.72%) and; the nursing assistants weak (success rate of 68.75%). Globally, however, the professionals were qualified as average (73.2% correct). Proficiency of the professionals: 12 (44.5%) expressed difficulties in at least one area of care that they provided to patients using an artificial airway. The most frequently mentioned area was the cuff pressure verification (11 times) followed by the insertion of the orotracheal tube (OTT), oral hygiene and positioning of the OTT, each was mentioned once. Twelve participants (44.5%) reported that they had never received any in-service training on ETA. DISCUSSION A worrying result was observed when we discovered that in the following five areas: routine instillation of a physiological solution (PS) 0.9% in the TET; use of aspiration catheter of appropriate diameter; maximum time of aspiration with an open void; main adverse effects/ reactions related to ETA and; routine hyperventilation as a way of preventing hypoxemia, the knowledge of the professionals was classified as poor. Considering that insufficient or incorrect knowledge leads individuals to inadequate 549
5 practices, it appears that the lack of knowledge in these areas can cause complications such as hypoxemia, infections and hemodynamic instability and thus compromise patients safety. Informing patients in advance about the procedures that will be used and encouraging their participation, aside from being a human and ethical practice is also seen as an important strategy for reducing stress and anxiety, as well as maximizing the results of ETA (4). In this research, 92.6% (n=25) of participants stated that it is necessary to explain the procedure to the patient, indicating very good knowledge on the subject. Similar results were found in a study conducted in Spain with ICU nurses, in which 100% (n=34) reported this practice and pointed out some aspects that should be addressed, such as what will be done and why, the sensations that can be felt and which concerns may be minimized with the administration of oxygen (4). The professionals were asked about the need to interrupt enteral feeding before starting the ETA. The success rate was 85.2%, showing that they had good knowledge on the subject. This precaution is necessary as it helps to reduce VAP rates, since it helps to prevent vomiting and aspiration of that content through the lower airways (7). The knowledge of the professionals on pre-oxygenation as a way of preventing hypoxemia was weak, as only 63% of respondents answered the question correctly. Despite the fact that the optimal technique (gold standard) for the provision of oxygenation in ETA (pre- -oxygenation, post-oxygenation, insufflation and hyperinsufflation, alone or in combination) remains undetermined, the last AARC Guidelines (6) recommend pre-oxygenation at 100% in pediatric and adult patients for 30 to 60 seconds (category 2B), especially in hypoxemic patients and in those whose oxygen saturation decreases during sucking. However, studies conducted with intensive care nurses showed that most of them know the importance of pre-oxygenation, but few use it routinely (4.5). Airway aspiration is required when there is a need to remove accumulated lung secretions. This can be evidenced by: 1) visible secretions in the airways; 2) the need to collect secretions for microbiological examination; 3) suspected aspiration of gastric fluid or upper airway; 4) the inability of patients to generate a spontaneous and effective cough; 5) a decrease in oxygen saturation and; 6) acute respiratory distress. The knowledge of the professionals in these areas proved to be very good, as 96.3%, reported at least three of the six possible alternatives. The first four reasons for airway aspiration were identified in the majority of cases with 27, 25, 21 and 15 records respectively and the last two with 11 and 5 records respectively were less frequently mentioned. Besides the above, there are other conditions that suggest ETA may be required, for example the presence of coarse crackles in the trachea, the standard sawtooth in the flow- -volume circuit on the monitor screen of the fan and when the inspiratory pressure peak is increased during the volume control mode or decrease of the tidal volume during the controlled pressure (6). Regarding the time it takes to aspirate the airways, that is, routinely (pre-established hours as prescribed or unit routine) or only when necessary, the knowledge of participants was also viewed as very good as 92 6% correctly indicated that the ETA should be performed only when necessary. Despite this current recommendation, literature data shows that the procedure was traditionally performed routinely every one or two hours in order to prevent the occurrence of VAP and the occlusion of TET. However, over the course of years, several randomized studies indicated that there is no benefit in periodi- 550
6 cally determined aspiration compared to that applied only when required. Furthermore, a higher number of aspirations put the patient at potential risk (9). When participants were asked about the routine instillation of PS 0.9% before the ETA, the knowledge of the professionals surveyed proved to be deficient, and was seen as poor, as only 44.5% correctly stated that it should not be applied routinely. Importantly, this procedure is the subject of much discussion, controversy and even conflicting results. The studies used in the preparation of the questionnaire were used as parameters to define what is correct or not. The use of normal saline before ETA remained traditionally stable because it was believed that its use facilitated the removal of secretions by softening and thinning lung secretions, lubricating the suction catheter and stimulating coughing, which would facilitate the mobilization of secretions into the central airways, would increase the amount of secretions removed and would improve oxygenation. However, there is insufficient evidence to support this hypothesis, since a large number of studies registered insufficiency of 0.9% physiological saline to enhance the removal of secretions. Consequently, humidifying the inspired gas and hydrating patients systemically were more acceptable measures (11). Recent literature reviews found that, in recent years, different investigations have been conducted to determine the physiological and psychological effects of the instillation of such a solution in the ETA. Based on reports of post- -extubation, gasometrical parameters, secretion removal, oxygen consumption and infection rates, the investigations included in the review showed that the procedure does not provide significant benefits. Instead, it is associated with discomfort and hemodynamic changes. In addition, this review provided evidence for asserting that the increased removal of secretions does not have clinical relevance as the amount of extra secretions removed ranged from one to two grams in the control group. Furthermore, the 0.9% physiological saline is quickly absorbed by the cardiopulmonary parenchyma and does not mix with the tracheobronchial secretions with only 18.7% of the instilled solution being recovered (12). Faced with several controversies and no tangible benefits documented for the use of 0.9% physiological saline in the ETA, the AARC Guidelines (6) do not recommend its routine use (Category 2C), since this procedure is associated with risks and complications and its use is allowed in the handling of secretions of difficult removal, as in the case of thick secretions and mucous plugs. With regards to the size of the ideal aspiration catheter, the success rate was 59.2%, indicating poor knowledge. This data is worrying because very large caliber catheters can cause considerable negative pressures to the airways, resulting, therefore, in a sudden drop in functional residual capacity, hypoxemia, atelectasis and traumas. Conversely, small caliber catheters do not provide satisfactory aspiration (13). Therefore, there is a consensus that the diameter of the catheter should be as small as possible, but large enough to facilitate the removal of secretions. Furthermore, in adults, the outer diameter of the suction catheter should occlude less than 50% of the internal diameter of the artificial airway. This allows ambient air to enter the lungs while the alveolar oxygen and other gases are being removed by the vacuum of the catheter (9). Although much discussed, there is no evidence to support the exact ratio between suction catheter and TET. However, the following formula is widely recommended to calculate the ideal caliber of the aspiration catheter: aspiration catheter caliber [Rf] = (TET Gauge [mm] - 2) x 2 (13). 551
7 Worrying data was found that stated that the duration of the suction procedure (negative pressure established) is limited to a maximum of 30 seconds. The knowledge of participants on this subject was analyzed as poor, as only 33.3% answered the question correctly. In fact, based on clinical experiences and randomized studies, the current consensus recommended that the aspiration procedure should last no longer than 15 seconds. Excessive suction time can cause hypoxemia, atelectasis and respiratory distress (6). A considerable percentage of the professionals answered correctly when they said it is true that the patient should be monitored with pulse oximetry before, during and after the procedure (96.3%) and the catheter should be inserted into the tube with the vacuum system shut (92, 6%). This knowledge was seen as very good in both areas. These practices were widely suggested and were emphasized by means of meta-analysis that aimed to clarify and analyze the effects of interventions implemented to prevent hypoxemia induced by ETA (14). Only 18.5% of respondents answered the question correctly regarding the main effects/ adverse reactions related to ETA. This result indicated poor knowledge and was at the same time alarming, considering that such professionals may underestimate the harmful effects arising from the procedure and, in practice, do not take the preventive measures recommended, which can result in mortality. The main effects/adverse reactions related to ETA include: increased blood pressure and intracranial pressure, hypoxemia, cardiac arrhythmias, cardiac and/or respiratory failure, bronchospasm, atelectasis, nosocomial infection, vagal overstimulation, damages the tracheobronchial tree, anxiety, bleeding, cardiovascular instability, neurological disorders and even death (8). With respect to the main parameters that should be evaluated during and after ETA, the success rate was 77.8%, denoting average knowledge. The patient should be monitored regarding oxygen saturation, heart rate, level of consciousness, blood pressure and their reactions to the procedure (9). The professionals were informed that hyperventilation (increase in the amount of air that ventilates the lungs, either by increasing the respiratory rate or inspiratory flow) should not be routinely used. Only 12 (44.5%) said that True was the correct answer, which was seen as poor knowledge. This result is disturbing, as this technique is not recommended as it can result in harmful effects, such as barotraumas and basic acids disorders (6) and is also not supported from an ethical point of view. Recent statements from the Regional Council of Nursing of São Paulo concluded that it is not the responsibility of the nurse to perform programming and parameter changes of Mechanic Pulmonary Ventilation devices (15:3). The professionals were asked whether the actions of hand hygiene (before and after the procedure), the use of gloves, goggles and apron were all necessary for the ETA. All (100%) participants answered the question correctly and obtained the knowledge degree rated excellent. Hand hygiene is undoubtedly the most important measure in reducing the risk of transmission of microorganisms. It must be performed before and after the contact with patients, blood, body fluids, secretions, excretions and objects contaminated by such substances. However, the use of gloves, goggles and aprons is necessary in situations where blood or secretion splashing may occur (16). Regarding the permanence of sterility of the suction catheter, 92.6% of the professionals answered the question correctly, indicating very good knowledge on the subject. In the literature, it is very well-known that the sterility of the catheter should be strictly maintained during all the steps of the ETA for open systems, in addition to the aseptic measures (17). Thus, targeting errors in this process and therefore the 552
8 VAP, the enclosed aspiration system has emerged as an alternative to the open one. However, there is no literary consensus that the closed system reduces the incidence of VAP, given the controversial results found in several investigations (9). Well-designed and robust studies, with internal and external validity, are needed not only to affirm or refute the efficacy in preventing infections, but also to stratify from which final positive expiratory pressure (PEEP) this device is indicated to maintain the oxygen fraction and pulmonary pressures stable in patients who require high pressures. Confirmation is also required of the contribution of the closed system for occupational health and whether there is a reduction in the spread of microorganisms in patients with active tuberculosis when using this system (18). In airway aspiration, it is widely accepted that professionals should respect the sequence TET, nose, and finally, the oral cavity. 81.5% of the professionals answered the question relating to this area correctly, indicating good knowledge. This care is very important, since errors in this process may culminate in nosocomial infections (1,3,4,9). The cuff pressure was the area of greatest difficulty reported by professionals in the management of artificial airways. This should be measured every eight to 12 hours, or whenever necessary, and should be maintained at between 15 and 25 mmhg (20 and 34 cmh2o). Higher values predispose to ischemic lesions and tracheal stenosis whereas lower values affect the mechanical ventilation and facilitate the aspiration of oropharyngeal secretions into the lower airways, increasing the risk of VAP (19). Faced with such problems, it is up to the nurse not only to recommend and implement preventive protocols, but also the periodic evaluation of the adherence of the proposed measures; the application of clinical indicators and; continuing education (20). Of equal importance is the commitment to quality and/ or improvement of structural and organizational issues, in addition to suitably qualified personnel and material resources. The results of this study showed that the areas where knowledge was particularly poor related to the routine use of PS 0.9%, suction catheter with proper diameter, maximum time of aspiration, main effects/adverse reactions related to the procedure and routine hyperventilation. Such results need to be analyzed and revised in teaching and nursing in the location of the research. Limitations of this research include a lack of evaluation during periods of real assistance when professionals were carrying out an actual ETA procedure and their responses during this time, which restricted the development of this study; the sample was small, although it encompassed all the professionals in the units investigated. However, generalizations of the results are fragile. CONCLUSION The nursing professionals studied presented average knowledge about the ETA technique. In addition, the findings suggest that the greater the degree of professional instruction, the better the theoretical preparation for the procedure of ETA. Therefore, nurses had higher scores than nursing technicians who, in turn, exhibited higher scores than the nursing assistants. The results suggest that there are some deficiencies in the knowledge of members of the nursing team. These results can guide the planning of strategies such as continuing education and adoption of preventative measures aimed at improving the level of knowledge of these professionals and, consequently, the quality of care provided. 553
9 554 REFERENCES 1. Kelleher S, Andrews T. An observational study on the open-system endotracheal suctioning practices of critical care nurses. J Clin Nurs. 2008; 17 (3): Seckel MA. Does the use of a closed suction system help to prevent ventilator-associated pneumonia? Crit Care Nurse. 2008; 28 (1): Davies K, Monterosso L, Leslie G. Determining standard criteria for endotracheal suctioning in the paediatric intensive care patient: an exploratory study. Intensive Crit Care Nurs. 2011; 27 (2): Ania González N, Martínez Mingo A, Eseberri Sagardoy M, Margall Coscojuela MA, Asiain Erro MC. Assessment of practice competence and scientific knowledge of ICU nurses in the tracheal suctioning. Enferm Intensiva. 2004; 15(3): Day T, Iles N, Griffiths P. Effect of performance feedback on tracheal suctioning knowledge and skills: randomized controlled trial. J Adv Nurs. 2009; 65(7): American Association of Respiratory Care. AARC clinical practice guidelines: endotracheal suctioning of mechanically ventilated patients with artificial airways Respir Care. 2010; 55 (6): Celik SA, Kanan N. A current conflict: use of isotonic sodium chloride solution on endotracheal suctioning in critically iil patients. Dimens Crit Care Nurs. 2006; 25 (1): Farias GM, Freitas MCS, Rocha KMM, Costa IKF. Pacientes sob ventilação mecânica: cuidados prestados durante a aspiração endotraqueal. Inter Science Place [Internet] Sep [cited 2012 Nov 25]; 2 (9): [about 5 p.]. Available From: org/interscienceplace/article/view/109/ Pedersen CM, Rosendahl-Nielsen M, Hjermind J, Egerod I. Endotracheal suctioning of the adult intubated patient - what is the evidence? Intensive Crit Care Nurs. 2009; 25 (1): Lourenço SA, Ohara CVS. Nurses knowledge about the insertion procedure for peripherally inserted central catheters in newborns. Rev latinoam enferm. 2010; 18 (2): Roberts FE. Consensus among physiotherapists in the United Kingdom on the use of normal saline instillation prior to endotracheal suction: a delphi study. Physiother Can. 2009; 61(2): Halm MA, Krisko-Hagel K. Instilling normal saline with suctioning: beneficial technique or potentially harmful sacred cow? Am J Crit Care. 2008; 17 (5): Day T, Farnell S, Haynes S, Wainwright S, Wilson- -Barnett J. Tracheal suctioning: an exploration of nurses knowledge and competence in acute and high dependency ward areas. J Adv Nurs. 2002; 39 (1): Oh H, Seo W. A meta-analysis of the effects of various interventions in preventing endotracheal suction-induced hypoxemia. J Clin Nurs. 2003; 12 (6): Conselho Regional de Enfermagem de São Paulo [homepage in the Internet]. Parecer n.º 046, de 06 de dezembro de Atribuições do enfermeiro e equipe de enfermagem na assistência ao paciente submetido à ventilação pulmonar mecânica [cited 2011 Sep 10]. Available From: parecer_coren_sp_2010_46_0.pdf 16. Freire ILS, Farias GM, Ramos CS. Prevenindo pneumonia nosocomial: cuidados da equipe de saúde ao paciente em ventilação mecânica invasiva. Rev eletrônica enferm. 2006; 8 (3): Jongerden IP, Rovers MM, Grypdonck MH, Bonten MJ. Open and closed endotracheal suction systems in mechanically ventilated intensive care patients: a meta-analysis. Crit Care Med. 2007; 35 (1): Ferreira AOM, Silvino ZR, Christovam BP, Lima DVM. Aspiração endotraqueal em unidade de terapia intensiva: uma revisão integrativa. Rev enferm UFPE on line [Internet]. 2013;7(7): Jerre G, Silva TJ, Beraldo MA, Gastaldi A, Kondo C, Leme F, et al. Fisioterapia no paciente sob ventilação mecânica. J bras pneumol. 2007; 33 Suppl 2: Silveira IR, Gnatta JR, Lacerda RA. Reproducibility and confiability of a processual indicator to evaluate adherence to oral hygiene in patients with orotracheal intubation. Online braz j nurs [Internet] May [cited 2012 Nov 30]; 10(1): [about 6 p.]. Available From: Received: 01/12/2012 Revised: 15/07/2013 Aproved: 23/07/2013
does staff intervene; used? If not, describe.
 Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Knowledge and Practice of ICU Nurses Regarding Endotracheal Suctioning for Mechanically Ventilated Patients in Khartoum Teaching Hospital
 American Journal of Clinical Neurology and Neurosurgery Vol. 1, No. 2, 2015, pp. 92-98 http://www.aiscience.org/journal/ajcnn Knowledge and Practice of ICU Nurses Regarding Endotracheal Suctioning for
American Journal of Clinical Neurology and Neurosurgery Vol. 1, No. 2, 2015, pp. 92-98 http://www.aiscience.org/journal/ajcnn Knowledge and Practice of ICU Nurses Regarding Endotracheal Suctioning for
A STUDY TO ASSESS THE KNOWLEDGE AND PRACTICE OF ENDOTRACHEAL SUCTIONING AMONG NEURONURSES SCTIMST
 A STUDY TO ASSESS THE KNOWLEDGE AND PRACTICE OF ENDOTRACHEAL SUCTIONING AMONG NEURONURSES SCTIMST PROJECT REPORT Submitted in partial fulfillment of the requirements For the Diploma in N euro Nursing Submitted
A STUDY TO ASSESS THE KNOWLEDGE AND PRACTICE OF ENDOTRACHEAL SUCTIONING AMONG NEURONURSES SCTIMST PROJECT REPORT Submitted in partial fulfillment of the requirements For the Diploma in N euro Nursing Submitted
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Title Nasopharyngeal Suction Standard Operating Procedure
 Document Control Title Nasopharyngeal Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health and Social Care Community Services Date Version Status
Document Control Title Nasopharyngeal Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health and Social Care Community Services Date Version Status
Saudi Journal of Medical and Pharmaceutical Sciences. DOI: /sjmps. Original Research Article
 DOI: 10.21276/sjmps Saudi Journal of Medical and Pharmaceutical Sciences Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2413-4929 (Print) ISSN 2413-4910
DOI: 10.21276/sjmps Saudi Journal of Medical and Pharmaceutical Sciences Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2413-4929 (Print) ISSN 2413-4910
Marianne Chulay is a critical care nursing/clinical research consultant in Chapel Hill, NC. The author has no financial relationships to disclose.
 VAP is a common and potentially fatal complication of ventilator care. Following the latest CDC recommendations is the best defense you can offer your patients. Marianne Chulay, RN, DNSC, FAAN Marianne
VAP is a common and potentially fatal complication of ventilator care. Following the latest CDC recommendations is the best defense you can offer your patients. Marianne Chulay, RN, DNSC, FAAN Marianne
Suctioning in Adult. Pulmonary Critical Care. 1.0 Hour
 Pulmonary Critical Care Clinical Indicators for Endotracheal Suctioning in Adult Patients Receiving Mechanical Ventilation By Mary Lou Sole, RN, PhD, CCNS, Melody Bennett, RN, MN, CCRN, and Suzanne Ashworth,
Pulmonary Critical Care Clinical Indicators for Endotracheal Suctioning in Adult Patients Receiving Mechanical Ventilation By Mary Lou Sole, RN, PhD, CCNS, Melody Bennett, RN, MN, CCRN, and Suzanne Ashworth,
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure
 Document Control Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health & Social Care Community Services Date
Document Control Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health & Social Care Community Services Date
PICU tracheostomy protocol
 PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
Title: Length of use guidelines for oxygen tubing and face mask equipment
 Title: Length of use guidelines for oxygen tubing and face mask equipment Date: September 12, 2007 Context and policy issues: There is concern that oxygen tubing and face mask equipment in the ventilator
Title: Length of use guidelines for oxygen tubing and face mask equipment Date: September 12, 2007 Context and policy issues: There is concern that oxygen tubing and face mask equipment in the ventilator
EEAN.edu.br Open system endotracheal suctioning: practices of intensive care nursing professionals
 Esc Anna Nery 2014;18(2):296-302 RESEARCH PESQUISA EEAN.edu.br Open system endotracheal suctioning: practices of intensive care nursing professionals Aspiração endotraqueal por sistema aberto: práticas
Esc Anna Nery 2014;18(2):296-302 RESEARCH PESQUISA EEAN.edu.br Open system endotracheal suctioning: practices of intensive care nursing professionals Aspiração endotraqueal por sistema aberto: práticas
Prone Ventilation of the Critically Ill Patient
 Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
COMPARISON OF AIRWAY MANAGEMENT PRACTICES BETWEEN REGISTERED NURSES AND RESPIRATORY CARE PRACTITIONERS. Pulmonary Critical Care. 1.
 Pulmonary Critical Care COMPARISON OF AIRWAY MANAGEMENT PRACTICES BETWEEN REGISTERED NURSES AND RESPIRATORY CARE PRACTITIONERS By Mary Lou Sole, RN, PhD, CCNS, and Melody Bennett, RN, MN, CCRN CNE 1. Hour
Pulmonary Critical Care COMPARISON OF AIRWAY MANAGEMENT PRACTICES BETWEEN REGISTERED NURSES AND RESPIRATORY CARE PRACTITIONERS By Mary Lou Sole, RN, PhD, CCNS, and Melody Bennett, RN, MN, CCRN CNE 1. Hour
Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 418 Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA 1. PURPOSE: To
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 418 Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA 1. PURPOSE: To
Tracheal suctioning with versus without saline instillation
 Tracheal suctioning with versus without saline instillation 1* Eman M. Zahran and 2 Ahmed A. Abd El-Razik 1 Emergency and Critical Care Nursing Dept., Faculty of Nursing, University of Alexandria, 2 Critical
Tracheal suctioning with versus without saline instillation 1* Eman M. Zahran and 2 Ahmed A. Abd El-Razik 1 Emergency and Critical Care Nursing Dept., Faculty of Nursing, University of Alexandria, 2 Critical
Respirator. Prerequisit. ive review to. Comprehensi. exam success C5, C6, C7, C8, C16) C7,C12,C15,C16, ,C18) C19, C20) C15, C18, C19, C20)
 Respirator ry Care Examinationn Preparation (RSPT 2230) Capstone Course Credit: 2 semester credit hours (2 hours lecture, 1 hour lab) Prerequisit te/co-requisite: RSPT 1113, RSPT 1207, RSPT 1261, RSPT
Respirator ry Care Examinationn Preparation (RSPT 2230) Capstone Course Credit: 2 semester credit hours (2 hours lecture, 1 hour lab) Prerequisit te/co-requisite: RSPT 1113, RSPT 1207, RSPT 1261, RSPT
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 16 Acute Trauma Management Key Points 2 16.1 Trauma in Perspective Correct management within the first few hours after the injury is vital Your hospital should
Surgical Care at the District Hospital 1 16 Acute Trauma Management Key Points 2 16.1 Trauma in Perspective Correct management within the first few hours after the injury is vital Your hospital should
VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP VAP SK-V1
 VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP Version Number V1 Date of Issue February 2018 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
VENTILATOR ASSOCIATED PNEUMONIA (VAP) SOP Version Number V1 Date of Issue February 2018 Reference Number Review Interval Approved By Name: Fionnuala O Neill Title: Nurse Practice Coordinator Authorised
Effective: Revised: April 15, 2016 SUCTIONING, MODIFIED STERILE TRACHEAL
 SUCTIONING, MODIFIED STERILE TRACHEAL Purpose: Tracheal suctioning is performed to remove secretions and maintain a patent airway. Additional Authority: Nevada Revised Statute, Nevada Nurse Practice Act,
SUCTIONING, MODIFIED STERILE TRACHEAL Purpose: Tracheal suctioning is performed to remove secretions and maintain a patent airway. Additional Authority: Nevada Revised Statute, Nevada Nurse Practice Act,
Pediatric Intensive Care Unit (PICU) Elective PL-1 Residents
 PL-1 Residents Interns are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
PL-1 Residents Interns are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
CA-1 CRITICAL CARE ROTATION University of Minnesota Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks
 CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
PROCEDURAL SEDATION AND ANALGESIA: HOSPITAL-WIDE POLICY
 CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
Case 1 Standard of Care. Disclosures. Defending Critical Care: Navigating Through the Malpractice Maze 5/9/2015. Defending Critical Care:
 Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland
 Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland Questions What was the unit length of stay and APACHE II scores for ventilated
Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland Questions What was the unit length of stay and APACHE II scores for ventilated
1. Introduction. Volume 6 Issue 4, April Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.
 Nurses Knowledge toward Essential Care for Adult Patients Undergoing Mechanical Ventilation at Critical Care Unit in Baghdad City Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.Al-Fayyadh,
Nurses Knowledge toward Essential Care for Adult Patients Undergoing Mechanical Ventilation at Critical Care Unit in Baghdad City Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.Al-Fayyadh,
Review of Clinical Practice Guidelines in Suction Therapy. Disclaimer. Suctioning the Patient in the Home Types of Suction Therapy
 Review of Clinical Practice Guidelines in Suction Therapy Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Dave Henry RRT Name of employer: DeVilbiss Healthcare Definition:
Review of Clinical Practice Guidelines in Suction Therapy Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Dave Henry RRT Name of employer: DeVilbiss Healthcare Definition:
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES. By Maureen Kroning EdD, RN
 A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
Goals & Objectives 4/17/2014 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN. Why would someone need to do this?
 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
Tube Feeding Status Critical Element Pathway
 Use this pathway for a resident who has a feeding tube. Review the Following in Advance to Guide Observations and Interviews: Most current comprehensive and most recent quarterly (if the comprehensive
Use this pathway for a resident who has a feeding tube. Review the Following in Advance to Guide Observations and Interviews: Most current comprehensive and most recent quarterly (if the comprehensive
Subacute Care. 1. Define important words in the chapter. 2. Discuss the types of residents who are in a subacute setting
 175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
Effectiveness of Video Assisted Teaching Regarding Knowledge and Practice of Intra-Venous Cannulation for Under-five Children
 IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 5, Issue 5 Ver. VII (Sep. - Oct. 26), PP 10-15 www.iosrjournals.org Effectiveness of Video Assisted Teaching
IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 5, Issue 5 Ver. VII (Sep. - Oct. 26), PP 10-15 www.iosrjournals.org Effectiveness of Video Assisted Teaching
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Human and financial costs of noninvasive mechanical ventilation in patients affected by COPD and acute respiratory failure Nava S, Evangelisti I, Rampulla C, Compagnoni M L, Fracchia C, Rubini F Record
Human and financial costs of noninvasive mechanical ventilation in patients affected by COPD and acute respiratory failure Nava S, Evangelisti I, Rampulla C, Compagnoni M L, Fracchia C, Rubini F Record
Pediatric Intensive Care Unit Rotation PL-2 Residents
 PL-2 Residents Residents are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
PL-2 Residents Residents are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
Provincial Nursing Competencies List of e-learning Modules. Updated: September 25, 2015
 Provincial Nursing Competencies List of e-learning Modules Updated: September 25, 2015 Once you sign in on the home page, you will see the following search screen on the right hand side of the page: Search:
Provincial Nursing Competencies List of e-learning Modules Updated: September 25, 2015 Once you sign in on the home page, you will see the following search screen on the right hand side of the page: Search:
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES
 UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
Practical Nursing A. Performing Medical Aseptic Procedures Notes: 1. Wash hands. 2. Follow body substance isolation (BSI)
 Name: Practical Nursing Directions: Evaluate the student by entering the appropriate number to indicate the degree of competency. The rating for each task should reflect employability readiness rather
Name: Practical Nursing Directions: Evaluate the student by entering the appropriate number to indicate the degree of competency. The rating for each task should reflect employability readiness rather
Effective: September, 2011 Revised: August 17, 2016 TRACHEOSTOMY TUBE REPLACEMENT
 TRACHEOSTOMY TUBE REPLACEMENT Purpose: Emergency tracheostomy tube replacement occurs when the tube becomes blocked, dislodged or has been unintentionally removed. Additional Authority: Nevada Revised
TRACHEOSTOMY TUBE REPLACEMENT Purpose: Emergency tracheostomy tube replacement occurs when the tube becomes blocked, dislodged or has been unintentionally removed. Additional Authority: Nevada Revised
Endotracheal Intubation Adult (April 2013)
 Endotracheal Intubation Adult (April 2013) Placement of tube into patient s trachea in order to provide pulmonary ventilation. Advanced Life Support procedure Specified in existing regulations. Not authorized
Endotracheal Intubation Adult (April 2013) Placement of tube into patient s trachea in order to provide pulmonary ventilation. Advanced Life Support procedure Specified in existing regulations. Not authorized
Ruchika D. Husa, MD, MS
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY
 POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
Abstract. Key words: Documentation, ICU, Classification systems. Masoomeh Najafi (1) Nasrin Rassoulzadeh (2) Maryam Rassouli (3)
 The Evaluation of Compliance of The Records of Nursing Care after Surgery in the Intensive Care Unit of Cardiac Surgery with Clinical Care Classification system Masoomeh Najafi (1) Nasrin Rassoulzadeh
The Evaluation of Compliance of The Records of Nursing Care after Surgery in the Intensive Care Unit of Cardiac Surgery with Clinical Care Classification system Masoomeh Najafi (1) Nasrin Rassoulzadeh
Reducing Ventilator Associated Pneumonia (V.A.P) System and Patient Tracer
 Reducing V.A.P.: SYSTEM Tracer Begin with Large Group General Questions: 1. Describe your surgical and then medical process related to the prevention of V.A.P. 2. The Team Leader will create questions
Reducing V.A.P.: SYSTEM Tracer Begin with Large Group General Questions: 1. Describe your surgical and then medical process related to the prevention of V.A.P. 2. The Team Leader will create questions
Abstract of thesis entitiled. Implementation and evaluation of evidence-based practice guidelines for open
 Abstract of thesis entitiled Implementation and evaluation of evidence-based practice guidelines for open endotracheal suctioning in mechanically-ventilated adult patients Submitted by Tang Alvin Siu Ting
Abstract of thesis entitiled Implementation and evaluation of evidence-based practice guidelines for open endotracheal suctioning in mechanically-ventilated adult patients Submitted by Tang Alvin Siu Ting
Healthcare-Associated Infections
 Healthcare-Associated Infections A healthcare crisis requiring European leadership Healthcare-associated infections (HAIs - also referred to as nosocomial infections) are defined as an infection occurring
Healthcare-Associated Infections A healthcare crisis requiring European leadership Healthcare-associated infections (HAIs - also referred to as nosocomial infections) are defined as an infection occurring
International Journal of Scientific and Research Publications, Volume 7, Issue 8, August ISSN
 International Journal of Scientific and Research Publications, Volume 7, Issue 8, August 2017 469 (Effectiveness of an Educational Program upon nurses knowledge toward The Continuous Positive Airway Pressure
International Journal of Scientific and Research Publications, Volume 7, Issue 8, August 2017 469 (Effectiveness of an Educational Program upon nurses knowledge toward The Continuous Positive Airway Pressure
Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society
 Can J Anesth/J Can Anesth (2018) Appendix 5 Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society Background Medical and surgical care has become
Can J Anesth/J Can Anesth (2018) Appendix 5 Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society Background Medical and surgical care has become
HOME MECHANICAL VENTILATION: A Guide to Invasive and Noninvasive Ventilation 1
 HOME MECHANICAL VENTILATION: A Guide to Invasive and Noninvasive Ventilation 1 As many as 1.5 million patients per year require mechanical ventilators for respiratory support. For the vast majority of
HOME MECHANICAL VENTILATION: A Guide to Invasive and Noninvasive Ventilation 1 As many as 1.5 million patients per year require mechanical ventilators for respiratory support. For the vast majority of
ROTOPRONE THERAPY SYSTEM. with people in mind.
 ROTOPRONE THERAPY SYSTEM with people in mind www.arjohuntleigh.com THE CLINICAL CHALLENGE: MINIMIZING MORTALITY AND POTENTIAL COMPLICATIONS IN ARDS PATIENTS WHILE MAKING IT EASIER TO DELIVER PRONE THERAPY
ROTOPRONE THERAPY SYSTEM with people in mind www.arjohuntleigh.com THE CLINICAL CHALLENGE: MINIMIZING MORTALITY AND POTENTIAL COMPLICATIONS IN ARDS PATIENTS WHILE MAKING IT EASIER TO DELIVER PRONE THERAPY
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland
 Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Teaching Methods. Responsibilities
 Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
ICU. Rotation Goals & Objectives for Urology Residents
 THE UNIVERSITY OF BRITISH COLUMBIA Department of Urologic Sciences Faculty of Medicine Gordon & Leslie Diamond Health Care Centre Level 6, 2775 Laurel Street Vancouver, BC, Canada V5Z 1M9 Tel: (604) 875-4301
THE UNIVERSITY OF BRITISH COLUMBIA Department of Urologic Sciences Faculty of Medicine Gordon & Leslie Diamond Health Care Centre Level 6, 2775 Laurel Street Vancouver, BC, Canada V5Z 1M9 Tel: (604) 875-4301
Patient Care. and. Transportation Standards
 Patient Care and Transportation Standards Version 2.1 Comes into force July 18, 2016 Emergency Health Services Branch Ministry of Health and Long-Term Care Patient Care Definitions Non-urgent means a request
Patient Care and Transportation Standards Version 2.1 Comes into force July 18, 2016 Emergency Health Services Branch Ministry of Health and Long-Term Care Patient Care Definitions Non-urgent means a request
ENVIRONMENT Preoperative evaluation clinic, Preoperative holding area. Preoperative evaluation clinic, Postoperative care unit, Operating room
 Goals and Objectives, Main Operating Room Anesthesia, VAMC, CA-3 year UCSD DEPARTMENT OF ANESTHESIOLOGY OPERATING ROOM CLINICAL ANESTHESIA AT VAMC GOALS AND OBJECTIVES, CA-3 YEAR PATIENT CARE: To provide
Goals and Objectives, Main Operating Room Anesthesia, VAMC, CA-3 year UCSD DEPARTMENT OF ANESTHESIOLOGY OPERATING ROOM CLINICAL ANESTHESIA AT VAMC GOALS AND OBJECTIVES, CA-3 YEAR PATIENT CARE: To provide
Do You Say. Evidence-Based Practice. Restraints. Restraint Findings. Sacred Cows in Pediatric Nursing
 Sacred Cows in Pediatric Nursing Janice Selekman DNSc, RN, NCSN, FNASN Professor University of Delaware Do You Say. But we have ALWAYS done it that way But that s the way I was taught Where did YOU go
Sacred Cows in Pediatric Nursing Janice Selekman DNSc, RN, NCSN, FNASN Professor University of Delaware Do You Say. But we have ALWAYS done it that way But that s the way I was taught Where did YOU go
Routine Practices. Infection Prevention and Control
 Routine Practices Infection Prevention and Control Routine Practices Elements of Routine Practices: Risk assessment + hand hygiene + personal protective equipment Environmental controls (patient placement,
Routine Practices Infection Prevention and Control Routine Practices Elements of Routine Practices: Risk assessment + hand hygiene + personal protective equipment Environmental controls (patient placement,
Department of Anesthesiology Anesthesia Curriculum Clinical Base Year
 Anesthesia Curriculum Clinical Base Year Description of Rotation The goal of this month long rotation is to teach the basic skills of anesthesia and to provide a foundation on which to build the initial
Anesthesia Curriculum Clinical Base Year Description of Rotation The goal of this month long rotation is to teach the basic skills of anesthesia and to provide a foundation on which to build the initial
ENVIRONMENT Preoperative evaluation clinic. Preoperative evaluation clinic. Preoperative evaluation clinic. clinic. clinic. Preoperative evaluation
 Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Respiratory Therapy Program Technical Standards
 Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
MEDICINES CONTROL COUNCIL
 MEDICINES CONTROL COUNCIL EMERGENCY PROCEDURES FOR CLINICAL TRIAL SITES This document highlights the importance of having emergency standard operating procedures in place during the conduct of clinical
MEDICINES CONTROL COUNCIL EMERGENCY PROCEDURES FOR CLINICAL TRIAL SITES This document highlights the importance of having emergency standard operating procedures in place during the conduct of clinical
Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands
 ORIGINAL ARTICLE Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands E.F.E. Wenstedt 1 *, A.J.R. De Bie Dekker 1, A.N. Roos 1, J.J.M.
ORIGINAL ARTICLE Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands E.F.E. Wenstedt 1 *, A.J.R. De Bie Dekker 1, A.N. Roos 1, J.J.M.
Subject: Skilled Nursing Facilities (Page 1 of 6)
 Subject: Skilled Nursing Facilities (Page 1 of 6) Objective: I. To ensure that Tuality Health Alliance (THA) and delegated Providence Health Plan Medicare members are appropriately placed in skilled nursing
Subject: Skilled Nursing Facilities (Page 1 of 6) Objective: I. To ensure that Tuality Health Alliance (THA) and delegated Providence Health Plan Medicare members are appropriately placed in skilled nursing
Specialized Nursing Postgraduate Diploma, Faculty of Nursing, University of Iceland, Reykjavik, Iceland
 Specialized Nursing Postgraduate Diploma, Faculty of Nursing, University of Iceland, Reykjavik, Iceland Program director: Thorunn Sch. Eliasdottir, CRNA, PhD Specialized Nursing Postgraduate Diploma Faculty
Specialized Nursing Postgraduate Diploma, Faculty of Nursing, University of Iceland, Reykjavik, Iceland Program director: Thorunn Sch. Eliasdottir, CRNA, PhD Specialized Nursing Postgraduate Diploma Faculty
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Questions. Background to the ICNARC Case Mix Programme
 Number of admissions, unit length of stay and days of mechanical ventilation for admissions with blunt chest trauma to critical care in England, Wales and Northern Ireland Questions What were the number,
Number of admissions, unit length of stay and days of mechanical ventilation for admissions with blunt chest trauma to critical care in England, Wales and Northern Ireland Questions What were the number,
Sedation/Analgesia by Non-Anesthesiologists. THE UNIVERSITY OF TOLEDO Approving Officer:
 Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
N: Emergency Nursing. Alberta Licensed Practical Nurses Competency Profile 135
 N: Emergency Nursing Alberta Licensed Practical Nurses Competency Profile 135 Competency: N-1 Multi-Systems Assessment N-1-1 N-1-2 N-1-3 N-1-4 Demonstrate knowledge and ability to apply critical thinking
N: Emergency Nursing Alberta Licensed Practical Nurses Competency Profile 135 Competency: N-1 Multi-Systems Assessment N-1-1 N-1-2 N-1-3 N-1-4 Demonstrate knowledge and ability to apply critical thinking
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Department of Emergency Medical Services
 MIAMI DADE COLLEGE MEDICAL CENTER CAMPUS SCHOOL OF HEALTH SCIENCES Department of Emergency Medical Services CLINICAL COURSE OUTLINE EMS 1431 EMERGENCY MEDICAL TECHNICIAN BASIC 1 EMS 1431 EMERGENCY MEDCIAL
MIAMI DADE COLLEGE MEDICAL CENTER CAMPUS SCHOOL OF HEALTH SCIENCES Department of Emergency Medical Services CLINICAL COURSE OUTLINE EMS 1431 EMERGENCY MEDICAL TECHNICIAN BASIC 1 EMS 1431 EMERGENCY MEDCIAL
Job Description. Job Title: (Respiratory Specialist)
 Job Title: (Respiratory Specialist) Reports to: Annette Moser Responsibility Level: Staff Direct Supervision: Respiratory Manager Job Location: UI Health Department: Respiratory Care Services Job Category:
Job Title: (Respiratory Specialist) Reports to: Annette Moser Responsibility Level: Staff Direct Supervision: Respiratory Manager Job Location: UI Health Department: Respiratory Care Services Job Category:
1 advised when using guidelines after the review date
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc.) Author: Contact Name and Job Title Guideline for Adult Nasal and Oropharyngeal Suction Eleanor Douglas, Lecturer/Practitioner
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc.) Author: Contact Name and Job Title Guideline for Adult Nasal and Oropharyngeal Suction Eleanor Douglas, Lecturer/Practitioner
Goal Elements of Performance APIC Comments APIC Recommendations
 Association for Professionals in Infection Control and Epidemiology, Inc. Comments on the Joint Commission s Proposed 2012 National Patient Safety Goals The Joint Commission Practice Guidance Team Accreditation
Association for Professionals in Infection Control and Epidemiology, Inc. Comments on the Joint Commission s Proposed 2012 National Patient Safety Goals The Joint Commission Practice Guidance Team Accreditation
PEDIATRIC ALOC Guidelines. ALOC Guidelines ALOC
 PEDIATRIC Guidelines Guidelines The Alternate Level of Care () Guidelines are intended to assist the reviewer in identifying the next safest and appropriate level of care options. They allow the reviewer
PEDIATRIC Guidelines Guidelines The Alternate Level of Care () Guidelines are intended to assist the reviewer in identifying the next safest and appropriate level of care options. They allow the reviewer
MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE
 MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE 1 INTRODUCTION Welcome to Miami Dade College Bachelor of Science in Nursing Program. The
MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE 1 INTRODUCTION Welcome to Miami Dade College Bachelor of Science in Nursing Program. The
The impact of an ICU liaison nurse service on patient outcomes
 The impact of an ICU liaison nurse service on patient outcomes Suzanne J Eliott, David Ernest, Andrea G Doric, Karen N Page, Linda J Worrall-Carter, Lukman Thalib and Wendy Chaboyer Increasing interest
The impact of an ICU liaison nurse service on patient outcomes Suzanne J Eliott, David Ernest, Andrea G Doric, Karen N Page, Linda J Worrall-Carter, Lukman Thalib and Wendy Chaboyer Increasing interest
SAN FRANCISCO EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL PERSONNEL STANDARDS & SCOPE OF PRACTICE
 SAN FRANCISCO EMERGENCY MEDICAL SERVICES AGENCY Policy Reference No.: 2000 Eff. Date: November 1, 2017 Supersedes: January 30, 2017 PREHOSPITAL PERSONNEL STANDARDS & SCOPE OF PRACTICE I. PURPOSE Define
SAN FRANCISCO EMERGENCY MEDICAL SERVICES AGENCY Policy Reference No.: 2000 Eff. Date: November 1, 2017 Supersedes: January 30, 2017 PREHOSPITAL PERSONNEL STANDARDS & SCOPE OF PRACTICE I. PURPOSE Define
Monitoring in ICU. BR Bhengu UKZN
 Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
Feedback from Anesthesia clinicians. 2.1 Intubate Patient Workflow
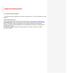 Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Standard Precautions
 Standard Precautions Speciality: Infection Control 1. Indications 1.1 Background Standard Precautions This definition broadens the coverage of the previously known Universal Precautions by recognizing
Standard Precautions Speciality: Infection Control 1. Indications 1.1 Background Standard Precautions This definition broadens the coverage of the previously known Universal Precautions by recognizing
CLINICAL SKILLS ASSESSMENT (CSA)
 CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
HEALTH SCIENCE COURSE DESCRIPTIONS
 HEALTH SCIENCE COURSE DESCRIPTIONS ECV 1114 ELECTROCARDIOGRAPHY BASIC - This eight week 64 clock hour course is designed to provide the necessary information to correctly understand and perform the twelve
HEALTH SCIENCE COURSE DESCRIPTIONS ECV 1114 ELECTROCARDIOGRAPHY BASIC - This eight week 64 clock hour course is designed to provide the necessary information to correctly understand and perform the twelve
GAMUT QI Collaborative Consensus Quality Metrics (v. 05/16/2016)
 1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
The residents will work at WVU Ruby Memorial under the supervision of departmental faculty.
 CA-2 Intermediate Clinical Training (ICT) Curriculum Department of Anesthesiology Description of Rotation The goal of this multi-month rotation is to build upon the essential skills learned in the BCT
CA-2 Intermediate Clinical Training (ICT) Curriculum Department of Anesthesiology Description of Rotation The goal of this multi-month rotation is to build upon the essential skills learned in the BCT
A survey on hand hygiene practice among anaesthetists
 A survey on hand hygiene practice among anaesthetists K Rupasingha 1 *, N Karunarathne 2 Registrar in Anaesthesiology 1, National Hospital Sri Lanka, Colombo, Sri Lanka. Consultant Anaesthetist 2, Sri
A survey on hand hygiene practice among anaesthetists K Rupasingha 1 *, N Karunarathne 2 Registrar in Anaesthesiology 1, National Hospital Sri Lanka, Colombo, Sri Lanka. Consultant Anaesthetist 2, Sri
Management for Preventing Ventilator-Associated Pneumonia at ICU Panti Rapih Hospital: A Clinical Case Study
 Nurse Media Journal of Nursing, 6 (1), 2016, 30-36 Available Online at http://ejournal.undip.ac.id/index.php/medianers Management for Preventing Ventilator-Associated Pneumonia at ICU Panti Rapih Hospital:
Nurse Media Journal of Nursing, 6 (1), 2016, 30-36 Available Online at http://ejournal.undip.ac.id/index.php/medianers Management for Preventing Ventilator-Associated Pneumonia at ICU Panti Rapih Hospital:
Anesthesia Elective Curriculum Outline
 Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
PULMONARY FUNCTION STUDIES
 Pulmonary Function StudiesApril 1, 2015 PREAMBLE PULMONARY FUNCTION STUDIES SPECIFIC ELEMENTS Pulmonary Function diagnostic procedures are divided into a professional component listed in the columns headed
Pulmonary Function StudiesApril 1, 2015 PREAMBLE PULMONARY FUNCTION STUDIES SPECIFIC ELEMENTS Pulmonary Function diagnostic procedures are divided into a professional component listed in the columns headed
A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs.
 6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
Maryland MOLST. Guide for Patients. Maryland MOLST Training Task Force
 Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
Protocol/Procedure XX. Title: Procedural Sedation/Moderate Sedation
 Protocol/Procedure XX Title: Procedural Sedation/Moderate Sedation A. DEFINITION Procedural Moderate Sedation/Analgesia is a drug-induced depression of consciousness during which patients respond purposefully
Protocol/Procedure XX Title: Procedural Sedation/Moderate Sedation A. DEFINITION Procedural Moderate Sedation/Analgesia is a drug-induced depression of consciousness during which patients respond purposefully
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE
 ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
STANDARD PRECAUTIONS POLICY Page 1 of 8 Reviewed: May 2017
 Page 1 of 8 Policy Applies to: All Mercy Staff, Credentialed Specialists, Allied Health Professionals, students, patients, visitors and contractors will be supported to meet policy requirements Related
Page 1 of 8 Policy Applies to: All Mercy Staff, Credentialed Specialists, Allied Health Professionals, students, patients, visitors and contractors will be supported to meet policy requirements Related
Pediatric Cardiology SAUDI FELLOWSHIP PROGRAM SAUDI FELLOWSHIP FINAL CLINICAL EXAMINATION OF PEDIATRIC CARDIOLOGY (2018)
 Pediatric Cardiology SAUDI FELLOWSHIP PROGRAM SAUDI FELLOWSHIP FINAL CLINICAL EXAMINATION OF PEDIATRIC CARDIOLOGY (2018) I Objectives a. Determine the ability of the candidate to practice as a specialist
Pediatric Cardiology SAUDI FELLOWSHIP PROGRAM SAUDI FELLOWSHIP FINAL CLINICAL EXAMINATION OF PEDIATRIC CARDIOLOGY (2018) I Objectives a. Determine the ability of the candidate to practice as a specialist
STATEMENT ON GRANTING PRIVILEGES FOR ADMINISTRATION OF MODERATE SEDATION TO PRACTITIONERS WHO ARE NOT ANESTHESIA PROFESSIONALS
 NOT ANESTHESIA PROFESSIONALS (Approved by the ASA House of Delegates on October 25, 2005, and amended on October 18, 2006) Outcome Indicators for Office-Based and Ambulatory Surgery (ASA Committee on Ambulatory
NOT ANESTHESIA PROFESSIONALS (Approved by the ASA House of Delegates on October 25, 2005, and amended on October 18, 2006) Outcome Indicators for Office-Based and Ambulatory Surgery (ASA Committee on Ambulatory
MODULE 4 Obstetric Anaesthesia and Analgesia
 MODULE 4 Obstetric Anaesthesia and Analgesia Duration required: A minimum 50 sessions (½ days) of clinical experience is required TE10 (2003) Recommendations for Vocational Training Programs Trainee s
MODULE 4 Obstetric Anaesthesia and Analgesia Duration required: A minimum 50 sessions (½ days) of clinical experience is required TE10 (2003) Recommendations for Vocational Training Programs Trainee s
