Provider Practice Characteristics That Promote Interpersonal Continuity
|
|
|
- Baldric Barber
- 6 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Provider Practice Characteristics That Promote Interpersonal Continuity Tyler S. Mittelstaedt, MD, MPH, Motomi Mori, PhD, William E. Lambert, PhD, and John W. Saultz, MD Purpose: Becoming certified as a patient-centered medical home now requires practices to measure how effectively they provide continuity of care. To understand how continuity can be improved, we studied the association between provider practice characteristics and interpersonal continuity using the Usual Provider Continuity Index (UPC). Methods: We conducted a mixed-methods study of the relationship between provider practice characteristics and UPC in 4 university-based family medicine clinics. For the quantitative part of the study, we analyzed data extracted from monthly provider performance reports for 63 primary care providers (PCPs) between July 2009 and June We tested the association of 5 practice parameters on UPC: (1) clinic frequency; (2) panel size; (3) patient load (ratio of panel size to clinic frequency); (4) attendance ratio; and (5) duration in practice (number of years working in the current practice). Clinic, care team, provider sex, and provider type (physicians versus nonphysician providers) were analyzed as covariates. Simple and multiple linear regressions were used for statistical modeling. Findings from the quantitative part of the study were validated using qualitative data from provider focus groups that were analyzed using sequential thematic coding. Results: There were strong linear associations between UPC and both clinic frequency ( 0.94; 95% CI, ) and patient load ( 0.37; 95% CI, 0.48 to 0.26). A multiple linear regression including clinic frequency, patient load, duration in practice, and provider type explained more than 60% of the variation in UPC (adjusted R ). UPC for nurse practitioners and physician assistants was more strongly dependent on clinic frequency and was at least as high as it was for physicians. Focus groups identified 6 themes as other potential sources of variability in UPC. Conclusions: Variability in UPC between providers is strongly correlated with variables that can be modified by practice managers. Our study suggests that patients assigned to nurse practitioners and physician assistants have continuity similar to those assigned to physicians. (J Am Board Fam Med 2013; 26: ) Keywords: Continuity of Patient Care, Medical Home, Patient-Centered Care Interpersonal continuity (IC), a fundamental principle of primary care, is defined by the Institute of This article was externally peer reviewed. Submitted 15 November 2012; revised 12 March 2013; accepted 19 March From the School of Medicine, Department of Surgery (TSM); the Divisions of Biostatistics (MM) and Epidemiology (WEL), Department of Public Health & Preventive Medicine; and the Department of Family Medicine (JWS), Oregon Health & Science University, Portland. Funding: Support for the project was provided by the Departments of Family Medicine and the Public Health and Preventive Medicine, Oregon Health & Science University. Prior presentation: These results were presented as part of the master s thesis for a Master of Public Health degree (TSM). Medicine as the product of personal interactions that include trust and partnership between patients and clinicians. 1 Numerous studies have demonstrated the benefits of enhanced IC, including increased patient and provider satisfaction, 2 5 healthier patient behaviors, 6 increased receipt of preventive and screening services, 7 11 reduced hospitalization rates, 12,13 decreased emergency department and intensive care unit utilization, decreased overall Conflict of interest: none declared. Corresponding author: John W. Saultz, MD, Department of Family Medicine, Oregon Health & Science University, 3181 SW Sam Jackson Park Road, FM, Portland, OR ( saultz@ohsu.edu). 356 JABFM July August 2013 Vol. 26 No. 4
2 health costs, 17 and reduced elderly mortality. 18,19 Despite broad consensus regarding these benefits, practice characteristics that improve IC remain poorly understood, and practice trends such as remote patient interactions and team-based care are leading to new dimensions of continuity outside of traditional face-to-face encounters. 20 With the advent of formal systems to evaluate and certify patient-centered medical homes (PCMHs), primary care practices increasingly are being asked to assess and report measures of continuity of care. Decades of research have employed a variety of ways to measure IC. 21 Before electronic health records (EHRs) there were few practical methods for collecting accurate continuity data, requiring investigators to infer continuity from chart review, claims analysis, or survey data. 22 This presented barriers to accurate measurement of IC and limited investigators abilities to perform rigorous analyses. As a result, there is little consensus on how to improve continuity or whether a benchmark or target continuity rate exists. The Usual Provider Continuity Index (UPC) is a measure of how often patients see their selfidentified primary care provider (PCP). 21,23 It is calculated by first determining the population of active patients who are assigned to a particular provider. The monthly UPC for that provider then is defined as the number of monthly clinic visits during which these patients see the assigned PCP divided by their total visits to the clinic that month. Measures of UPC now are required for several systems of PCMH certification, suggesting that primary care practices will need to measure and improve performance in this area in the coming years. 24,25 In 2008, the Oregon Health & Science University (OHSU) Department of Family Medicine established a system using data from EHRs for automated monthly collection of the UPC for each provider and clinic team. This has provided a robust database of prospectively collected continuity data, allowing for analyses of the determinants of continuity that were not feasible before EHR implementation. The objective of our study was to investigate whether certain provider practice parameters are associated with higher IC, thereby suggesting ways for practices to improve continuity as they transform into PCMHs. Methods Design We conducted a sequential, explanatory, mixedmethods study 26 of the effects of several provider practice parameters on IC as measured by UPC. We used retrospective data from 12 monthly UPC reports and department personnel records for quantitative analysis. The monthly reports included information about panel size and clinic frequency as well as UPC data, and the personnel records contained information about provider sex and duration in practice; however, we also wanted to learn about other potential factors that might affect continuity of care. Therefore, we conducted provider focus groups under an expert panel paradigm for qualitative analysis after the quantitative analysis was complete, allowing us to ask providers about other factors that might impact the UPC score. Setting The OHSU Department of Family Medicine operates 4 academic family medicine clinics. These include one federally qualified health center and one rural health clinic. All the clinics are recognized as level 3 PCMHs by Oregon s designation system, 24 which is similar to that of the National Committee for Quality Assurance. 25 Each clinic is divided into care teams, which consist of physicians and mid-level providers (nurse practitioners [NPs]) and physician assistants [PAs]), residents (with the exception of the rural health clinic), nurse coordinators, medical assistants, and ancillary staff. The EPIC electronic health record is used in each of the clinics. Two years before the start of this project, each of the clinics engaged in a comprehensive quality improvement project to ensure that the PCP field in every patient s health record was accurate and up to date. To ensure correct PCP assignment data, patients are asked to identify their PCP each time they have an encounter with the clinic, including phone calls, laboratory visits, nursing visits, and provider visits. Because of this protocol, a current and accurate PCP field is verified at every patient encounter. One year before the project, the department began to track and report the UPC rate for every provider on a monthly basis. This provides a quantitative assessment of the availability of each provider to the patients for whom he or she is the doi: /jabfm Promoting Interpersonal Continuity 357
3 registered as PCP. Data are disseminated in monthly provider performance reports. Since every PCP is a member of a discrete team, the UPC for each team is also tracked monthly. Subjects for Quantitative Analysis The unit of analysis for this study was the individual provider, specifically the individual faculty physicians (MDs and DOs) and mid-level providers (NPs and PAs) at each of the 4 clinics. The study period was from July 1, 2009, to June 30, The inclusion criteria were faculty and clinical fellows who had documented clinic sessions at any of the 4 clinics and who had a registered patient panel for which they were the designated PCP during the study period. To identify all eligible providers, we searched department records of all providers who had documented clinic sessions at any of the 4 clinics during the study period; we expanded the search to include all faculty members identified by departmental personnel records. This yielded 124 potentially eligible providers. Of these 124 individuals, 61 were excluded for the following reasons: 1. Thirty-two faculty members were physicians without an assigned patient panel (15 consulting specialists, 7 locum tenens physicians, 5 nonclinical faculty, 3 exclusive residency preceptors, and 2 nonclinical fellows). 2. Two were physicians who had a mixed primary care and specialty sports medicine referral practice. 3. Five were nonphysician providers without a registered patient panel (ie, 2 acupuncturists, 2 clinical social workers, 1 PA who was assigned no patients). 4. Twenty-two were providers who left the department during the study period (5 physicians, 9 fellows who recently graduated, and 8 mid-level providers). In total, the final analysis set included 63 providers comprising 45 physicians (including 6 fellows) and 18 mid-level providers. Provider data were historic in nature and de-identified before analysis; thus an exemption was granted by the OHSU Institutional Review Board. Data Collection and Outcome Variable System-wide EHR use allowed for continuous data collection with respect to provider panel sizes, clinic frequency, and visit volumes. Our outcome variable was the mean monthly provider UPC for each provider over the 12-month study period. Predictor Variables Clinic frequency, panel size, patient load, attendance ratio, duration in practice, as well as other covariates, were the practice parameters investigated as potential independent predictors of UPC. Clinic Frequency Clinic frequency was defined as the number of monthly half-day clinic sessions for a given provider. Providers are scheduled to work in the clinics in 4-hour blocks of time, which are referred to as half-day sessions. Counts were obtained from monthly provider performance reports and averaged over the 12-month study period to yield a single mean monthly half-day count for each provider. Panel Size End-of-month patient panel size for each provider was obtained from monthly provider performance reports. Panel size values were determined from the total number of patient charts in the EHR with a given provider listed in the PCP field. Patients who had not seen their PCP in 3 or more years are dropped from the provider s panel; thus end-ofmonth panel size reflected only active patients. Patient Load Defined as the ratio of panel size to clinic frequency (panel-to-half-day ratio), the patient load variable normalizes panel size for part-time providers and was obtained by dividing the mean monthly panel size by the mean monthly half-day clinic session count for each provider. Attendance Ratio Clinic attendance ratio was calculated for each provider by dividing the mean monthly half-day session count by the expected monthly half-day count as indicated by the provider s contracted clinical full-time equivalent. A 1.0 clinical full-time equivalent corresponds to 8 clinic half-day sessions per week for mid-level providers and 7 half-day sessions per week for physicians, who have 1 half-day per week designated for resident precepting. This measure did not discriminate by reason for absence from the clinic. 358 JABFM July August 2013 Vol. 26 No. 4
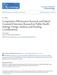
4 Duration in Practice Duration in practice for each provider was defined as the total number of years practicing in OHSU Family Medicine at the end of the study period (June 30, 2010) based on department personnel records. Other Covariates Clinic and care team assignments for each provider were obtained from monthly performance reports. Provider type (physician vs. mid-level) and sex were obtained from departmental personnel records. Statistical Analysis Stata statistical software version 11.0 (StataCorp, College Station, TX) was used for all statistical analyses. Simple linear regression was used to assess the effect of each of the individual predictors on the outcome variable (UPC). One-way analysis of variance with Bonferroni-adjusted pairwise comparisons was used to assess variability in UPC by clinic and team assignments. Two-sample t tests were used to compare UPC and predictor variables by provider type (physician vs. mid-level) and sex. Multiple linear regression modeling was performed using the backward elimination method, Mallow s criteria, and adjusted R 2 to assess multiple predictors simultaneously and to identify the best set of independent predictors for UPC. Qualitative Methods, Subjects, and Analysis The qualitative portion of our study used provider focus groups under an expert panel paradigm. 26,27 We introduced our hypotheses and proposed quantitative analysis predictor variables to provider groups to solicit their expert opinions regarding our methods and quantitative aims and to generate additional hypotheses for future study. Particular attention was paid to unique characteristics of clinics or individual providers that could limit the validity of our quantitative findings, as well as provider commentary on shifting perceptions of IC. Focus groups using a standardized script were conducted and audio-recorded by 1 of the authors (TM) during scheduled faculty meetings at each of the 4 clinics. Physician and mid-level provider participants were not formally identified at the time of the focus groups. Audio recordings were transcribed by 1 of the authors (TM), with anonymity of respondents maintained. Transcripts were independently coded into themes, subthemes, and representative quotations by 2 of the authors (TM and JS), with subsequent joint reconciliation of themes. Results Descriptive Analysis A total of 63 providers and 15 care teams from 4 clinics were included in our quantitative analysis. Among these providers, 21 were female physicians, 24 were male physicians, 16 were female mid-level providers, and 2 were male mid-level providers. Thus, 58.7% (n 37) were female and 28.6% (n 18) were mid-level providers. A descriptive summary of outcome and predictor variables is given in Table 1. There were significant differences in UPC, clinic frequency, and patient load by provider type. There were no significant differences in UPC or predictor variables by provider sex. There were no significant differences in UPC between teams in a given clinic. Clinic 1 had a significantly lower mean provider UPC relative to the other 3 clinics (56.1% vs. 65.4%; P.05). For this reason we examined whether the relationships between predictor variables and UPC differed among the clinics. Linear plots of UPC on predictor variables stratified by clinic revealed similar trends in UPC across all clinics, with the only discrepancy being a lower baseline UPC for clinic 1; thus there was no effect modification by clinic. Univariate Analysis Simple linear regressions of UPC on predictor variables are summarized in Table 2. Clinic frequency was significantly associated with increased UPC (Figure 1), whereas both panel size and patient load were significantly associated with decreased UPC (Figure 2). There was no significant association between UPC and clinic attendance ratio. Although there was no significant linear association between UPC and duration in practice, a strong association was observed between patient load and duration in practice ( 1.75; r 0.55; P.001); thus duration in practice was investigated as a potential confounder in multivariate analysis. Multivariate Analysis Multiple linear regression modeling identified a set of independent predictors: clinic frequency, doi: /jabfm Promoting Interpersonal Continuity 359
5 Table 1. Descriptive Summary of Outcome and Predictor Variables, Stratified by Provider Type Variable Mean SD Min Max P* UPC (%) All providers Physician Mid-level Clinic frequency (monthly half-day clinic sessions held) All providers Physician Mid-level Panel size (count of patients assigned to provider) All providers Physician Mid-level Patient load (ratio of panel size to half-day clinic frequency) All providers Physician Mid-level Attendance ratio All providers Physician Mid-level Duration in practice (years) All providers Physician Mid-level *Two-sample t test for difference in mean by provider type. Outcome variable: percentage of total clinic visits with assigned provider. Ratio of actual clinic frequency to expected clinic frequency. UPC, Usual Provider Continuity Index; SD, standard deviation. patient load, duration in practice, provider type, and interaction between patient load and provider type (Table 3). Clinic frequency and patient load were the primary modifiable predictors of UPC. Duration in practice was included as a significant confounder because of the association between UPC and patient load. Provider type was included as an effect modifier because the univariate analysis suggested potentially different associations between UPC and clinic frequency by provider type. The final model explains 60% of the variation in UPC across our Table 2. Simple Linear Regression of Usual Provider Continuity Index* on Predictor Variables Predictor Variable 95% CI r P Clinic Frequency Panel Size to Patient Load to Attendance Ratio to Duration in Practice to *Percentage of total clinic visits with assigned provider. Monthly half-day clinic sessions held. Count of patients assigned to provider. Ratio of panel size to clinic frequency. Ratio of actual clinic frequency to expected clinic frequency. Duration (years) in current practice. 360 JABFM July August 2013 Vol. 26 No. 4
6 Figure 1. Simple linear regression of Usual Provider Continuity Index (UPC) (percentage of total clinic visits with assigned provider) on clinic frequency (monthly half-day clinic sessions held). 90% 80% UPC % 70% 60% 50% 40% 30% Monthly Clinic Half-Days β=0.944, r=0.595 (p<0.0001) population of clinicians (adjusted R ; P.0001). Effect modification by provider type is further represented in Figure 3, which demonstrates the differential association between UPC and clinic frequency among physician and mid-level providers, holding patient load and duration in practice constant. Qualitative Analysis Physician and mid-level providers (n 35) from each of the 4 clinics participated in focus groups. Six general themes were identified during sequential coding of provider responses (Table 4). Themes 1 to 3 identify potential sources of variation in UPC that are intrinsic to specific clinics, providers, or patient populations. Themes 4 and 5 focus on alternative perceptions of IC beyond faceto-face encounters between a single patient and their personal PCP. Theme 6 addresses the potential relationship between clinic absences and IC. Discussion The purpose of our study was to (1) define baseline UPC measures for 63 providers in our 4 clinics after a full year of careful measurement and (2) understand differences in UPC among providers based on provider practice characteristics. Our findings should be useful to clinic managers and physician leaders seeking to improve IC within their practices, but this method of analysis is only valid when patients PCP assignments are known to be highly accurate and frequently updated. We identified patient load and clinic frequency as major modifiable predictors of UPC, both of which can be manipulated to achieve higher UPC. Based on our model, a provider s IC as measured by UPC can be improved by adjusting how often the provider is in the clinic and the size of his or her practice panel. A physician provider near the mean of all studied parameters (clinic frequency, 14 monthly half-days; panel size, 540 patients; patient load, 38.6; duration in practice, 7.2 years) can ex- Figure 2. Simple linear regression of Usual Provider Continuity Index (UPC) (percentage of total clinic visits with assigned provider) on patient load (panel size-to-clinic frequency ratio). 90% UPC % 80% 70% 60% 50% 40% 30% Panel-to-Half-Day Ra o β= , r=0.639 (p<0.0001) doi: /jabfm Promoting Interpersonal Continuity 361
7 Table 3. Optimal Multivariate Linear Model for Prediction of Usual Provider Continuity Index* Variables 95% CI P Clinic frequency Patient load to Duration in practice Provider type Type and patient load interaction to Intercept *Percentage of total clinic visits with assigned provider. P values reflect partial F-tests for significance of individual terms within the model. Reference group is mid-level providers (mid-level 0, physician 1). Data centered around mean clinic frequency of 16.8 monthly clinic half-days (mean clinic frequency for all providers). pect a UPC of 62.0%, nearly identical to our observed mean (61.0%). If this same provider were to add 4 half-days per month without a change in panel size, UPC would increase to 67.7%. Our qualitative analysis suggests that clinic scheduling patterns (subtheme 2.5) may account for additional unexplained variability in UPC. Providers in our focus groups believed continuity was likely to be more important for visits related to chronic or ongoing care, suggesting that these visits might be evaluated differently than acute care visits when assessing UPC (subtheme 4.1). An important finding of our study is that IC for mid-level providers as measured by UPC is at least as good as it is for physicians in this practice setting, where patients are allowed to choose physicians or mid-level providers as their PCP. Focus group participants hypothesized that intrinsic practice differences may contribute to the variability in UPC trends by provider type, including approach to patient care (subtheme 2.1), scope of practice (subtheme 2.3), and breadth of nonclinical duties (subtheme 2.4). Most of the physicians in this study perform hospital and maternity care and see patients in the office, whereas mid-level providers work only in the office setting. A specific limitation of our study is that it included only providers in academic practices, which calls into question whether our findings would be reproducible in community practices. Physicians in our practices have substantially more teaching and other academic duties than the mid-level providers. It is possible that the practices of mid-level providers in aca- Figure 3. Multivariate prediction of Usual Provider Continuity Index (UPC) (percentage of total clinic visits with assigned provider) based on clinic frequency (monthly half-day clinic sessions held), stratified by provider type (physicians vs. mid-level providers). Predicted UPC calculated at fixed values for patient load (panel-to-half-day ratio, 38.2) and duration in practice (6.35 years). Dashed lines denote data extrapolation outside of the observed range of clinic frequency for either provider type. UPC % Physician Mid-Level Monthly Clinic Half-Days 362 JABFM July August 2013 Vol. 26 No. 4
8 Table 4. Qualitative Data Summary from Focus Group Interviews Themes Subthemes Description 1. Clinic diversity 1.1 PCP assignment accuracy Clinics have different systems for ensuring that PCP fields are frequently updated and accurate. 1.2 Scheduling Clinics place variable importance on scheduling patients with their PCP rather than the first available provider. 1.3 Location/type University, FQHC, and rural clinics may have intrinsic differences in patient population and structure. 2. Provider diversity 2.1 Provider type Physician (MD/DO) and mid-level (PA/FNP) providers may have differences in both scope of practice and approach to care. 2.2 Provider sex Female and male providers may have differences in both scope of practice and approach to care. 2.3 Scope of practice Providers who provide maternity care, inpatient care, sports medicine, suboxone, resident precepting, etc., may have different UPC patterns than providers who solely conduct outpatient continuity clinics. 2.4 Nonclinical duties Providers with more academic/administrative responsibilities may have different UPC patterns than those with strictly clinical practices. 2.5 Clinic scheduling Providers with more open schedules or night/weekend clinics may have different UPC patterns than those with primarily prescheduled daytime clinics. 2.6 Location of residency Providers who trained at OHSU may have more developed panels for their year in practice than providers who trained elsewhere. 3. Patient diversity 3.1 Panel demographics SES, sex, race, ethnicity, age, medical complexity, visit frequency, and other panel demographics are likely to influence UPC for a given provider. 3.2 Importance of continuity to patient Some patients frequently change providers for a variety of reasons, making their PCP field relatively arbitrary. 4. Visit type 4.1 Acute care Acute care visits may not be as important as chronic or ongoing care in terms of actual continuity. 4.2 Nonoffice visits Current calculation of UPC does not take into account phone, , or MyChart encounters, where a meaningful interaction occurs without face-to-face contact. 5. Non-PCP continuity 5.1 Team continuity Patients may value continuity with a team of providers more than with a specific provider. 5.2 Clinic continuity Patients may value continuity with a particular clinic more than with an individual or team of providers. 5.3 Family continuity Continuity across families may be more important than continuity with individual patients. 6. Absences 6.1 Planned vs. unplanned Are all absences from clinic a diversion from continuity (eg, deliveries, inpatient), or is it just unplanned absences (eg, illness)? 6.2 New parent leave Specific extended absence that may behave differently than other absences in terms of continuity. DO, osteopathic doctor; FNP, family nurse practitioner; FQHC, federally qualified health center; MD, medical doctor; OHSU, Oregon Health & Sciences University; PA, physician assistant; PCP, primary care provider; UPC, Usual Provider Continuity Index. demic clinics may more closely resemble community-based physician practices, where physicians are less likely to have these academic responsibilities. Another key finding in our study was that longer duration in practice improves UPC, but this occurs only after adequately controlling for practice size because more experienced providers care for larger panels with fewer clinic sessions as their practices mature. Qualitative analysis suggested that providers with more years in practice might achieve continuity that is not accounted for in UPC calculations, such as during resident precepting (subtheme 2.3). In addition, providers with more mature relationships with their patients may be able to achieve the benefits of IC despite less frequent patient visits. One of the more consistent themes in our qualitative analysis was a concern about variability in UPC between providers of different sexes. Female providers in particular were concerned that different rates of maternity and well-woman visits (subtheme 2.2), as well as extended absences in the form of maternity leave (subtheme 6.2), would lead to lower UPC among female providers. Instead, our doi: /jabfm Promoting Interpersonal Continuity 363
9 quantitative analysis found no significant differences in UPC or any of our predictor variables by provider sex. The evolving nature of IC was discussed at length during the provider focus groups. Participants believed that efforts to quantify continuity should account for alternative forms of patient interactions, such as phone calls, s, or interactions through the EHR (subtheme 4.2). These were thought to be meaningful interactions enhancing IC despite the absence of a face-to-face encounter. Providers also stated that the value of IC needed to be reassessed in light of growing reliance on teambased care (subtheme 5.1) because the PCMH model emphasizes the value of team-based care. Further research is needed to investigate the value of continuity with a team of providers versus an individual provider. Conclusions Our study is a novel approach to the assessment of IC in family medicine and was made possible by our system-wide EHR, a tool that is still new for many practices. Our results improve the understanding of predictors of continuity while furthering efforts to establish benchmark UPC rates. Our methods should be reproducible in similar clinics or health systems and could be helpful to practicing family physicians as they address requirements for measuring and benchmarking continuity in the certification process to become a PCMH. Further research in this area might address how IC changes over time, how quality improvement efforts might improve continuity performance, and how clinic teams can expand on the proven value of relationship-based care in family medicine. Our mixedmethods study design allowed qualitative validation of our quantitative findings and suggests a number of key elements for future study. The authors are grateful to Ms. LeNeva Spires for editing and publication assistance. References 1. National Research Council. Primary care: America s health in a new era. Washington, DC: National Academies Press; Fan VS, Burman M, McDonell MB, Fihn SD. Continuity of care and other determinants of patient satisfaction with primary care. J Gen Intern Med 2005;20: Adler R, Vasiliadis A, Bickell N. The relationship between continuity and patient satisfaction: a systematic review. Fam Pract 2010;27: Saultz JW, Albedaiwi W. Interpersonal continuity of care and patient satisfaction: a critical review. Ann Fam Med 2004;2: Schers H, Webster S, van den Hoogen H, Avery A, Grol R, van den Bosch W. Continuity of care in general practice: a survey of patients views. Br J Gen Pract 2002;52: Berry LL, Parish JT, Janakiraman R, et al. Patients commitment to their primary physician and why it matters. Ann Fam Med 2008;6: Atlas SJ, Grant RW, Ferris TG, Chang Y, Barry MJ. Patient-physician connectedness and quality of primary care. Ann Intern Med 2009;150: Blewett LA, Johnson PJ, Lee B, Scal PB. When a usual source of care and usual provider matter: adult prevention and screening services. J Gen Intern Med 2008;23: Flores AI, Bilker WB, Alessandrini EA. Effects of continuity of care in infancy on receipt of lead, anemia, and tuberculosis screening. Pediatrics 2008;121: e Koopman RJ, Mainous AG, Baker R, Gill JM, Gilbert GE. Continuity of care and recognition of diabetes, hypertension, and hypercholesterolemia. Arch Intern Med 2003;163: Mainous AG, Kern D, Hainer B, Kneuper-Hall R, Stephens J, Geesey ME. The relationship between continuity of care and trust with stage of cancer at diagnosis. Fam Med 2004;36: Cheng SH, Chen CC, Hou YF. A longitudinal examination of continuity of care and avoidable hospitalization: evidence from a universal coverage health care system. Arch Intern Med 2010;170: Knight JC, Dowden JJ, Worrall GJ, Gadag VG, Murphy MM. Does higher continuity of family physician care reduce hospitalizations in elderly people with diabetes? Popul Health Manag 2009;12: Brousseau DC, Meurer JR, Isenberg ML, Kuhn EM, Gorelick MH. Association between infant continuity of care and pediatric emergency department utilization. Pediatrics 2004;113: Ionescu-Ittu R, McCusker J, Ciampi A, et al. Continuity of primary care and emergency department utilization among elderly people. CMAJ 2007;177: Sharma G, Freeman J, Zhang D, Goodwin JS. Continuity of care and intensive care unit use at the end of life. Arch Intern Med 2009;169: De Maeseneer JM, De Prins L, Gosset C, Heyerick J. Provider continuity in family medicine: does it make a difference for total health care costs? Ann Fam Med 2003;1: Wolinsky FD, Bentler SE, Liu L, et al. Continuity of care with a primary care physician and mortality in older adults. J Gerontol A Biol Sci Med Sci 2010;65: JABFM July August 2013 Vol. 26 No. 4
10 19. Worrall G, Knight J. Continuity of care for older patients in family practice: how important is it? Can Fam Physician 2006;52: Salisbury C, Sampson F, Ridd M, Montgomery AA. How should continuity of care in primary health care be assessed? Br J Gen Pract 2009;59:e Saultz JW. Defining and measuring interpersonal continuity of care. Ann Fam Med 2003;1: Jee SH, Cabana MD. Indices for continuity of care: a systematic review of the literature. Med Care Res Rev 2006;63: Breslau N, Reeb KG. Continuity of care in a university-based practice. J Med Educ 1975;50: Oregon.gov. Patient-centered primary care home program. Available from: oha/ohpr/pages/healthreform/pcpch/index.aspx. Accessed February 4, National Committee for Quality Assurance. Patient-centered medical home. PCMH standards and guidelines, Available from: Publications/deptCate.asp?dept_id 2&cateID 300& sortorder 796&mscssid # Accessed February 4, Creswell JW, Plano Clark VL, Gutmann ML, Hanson WE. Advanced mixed methods research designs. In: Tashakkori A, Teddlie C, editors. Handbook of mixed methods in social and behavioral research. Thousand Oaks, CA: Sage; 2003: Ivankova N, Creswell J, Stick S. Using mixed-methods sequential explanatory design: from theory to practice. Field Methods. 2006;18:3 20. doi: /jabfm Promoting Interpersonal Continuity 365
Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic
 INNOVATION AND IMPROVEMENT Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic Kathleen Heist, MD 1, Mary Guese, MD 2, Michelle Nikels, MD 1, Rachel Swigris, DO 1, and Karen Chacko,
INNOVATION AND IMPROVEMENT Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic Kathleen Heist, MD 1, Mary Guese, MD 2, Michelle Nikels, MD 1, Rachel Swigris, DO 1, and Karen Chacko,
Consistency of Care and Blood Pressure Control among Elderly African Americans and Whites with Hypertension
 Consistency of and Blood Pressure Control among Elderly s and s with Hypertension Daniel L. Howard, PhD, April P. Carson, PhD, DaJuanicia N. Holmes, MS, and Jay S. Kaufman, PhD Objective: To determine
Consistency of and Blood Pressure Control among Elderly s and s with Hypertension Daniel L. Howard, PhD, April P. Carson, PhD, DaJuanicia N. Holmes, MS, and Jay S. Kaufman, PhD Objective: To determine
Continuity of Care: An Evidence- Based Analysis (DRAFT)
 Continuity of Care: An Evidence- Based Analysis (DRAFT) Health Quality Ontario August 2012 Ontario Health Technology Assessment Series; Vol. 12: No. TBA, pp. 1 27, August 2012 Draft - Do not cite. Report
Continuity of Care: An Evidence- Based Analysis (DRAFT) Health Quality Ontario August 2012 Ontario Health Technology Assessment Series; Vol. 12: No. TBA, pp. 1 27, August 2012 Draft - Do not cite. Report
Using Data for Proactive Patient Population Management
 Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Continuity of Care to Optimize Chronic Disease Management in the Community Setting: An Evidence- Based Analysis
 Continuity of Care to Optimize Chronic Disease Management in the Community Setting: An Evidence- Based Analysis Health Quality Ontario September 2013 Ontario Health Technology Assessment Series; Vol. 13:
Continuity of Care to Optimize Chronic Disease Management in the Community Setting: An Evidence- Based Analysis Health Quality Ontario September 2013 Ontario Health Technology Assessment Series; Vol. 13:
Impact of Scribes on Performance Indicators in the Emergency Department
 CLINICAL PRACTICE Impact of Scribes on Performance Indicators in the Emergency Department Rajiv Arya, MD, Danielle M. Salovich, Pamela Ohman-Strickland, PhD, and Mark A. Merlin, DO Abstract Objectives:
CLINICAL PRACTICE Impact of Scribes on Performance Indicators in the Emergency Department Rajiv Arya, MD, Danielle M. Salovich, Pamela Ohman-Strickland, PhD, and Mark A. Merlin, DO Abstract Objectives:
Analysis of Nursing Workload in Primary Care
 Analysis of Nursing Workload in Primary Care University of Michigan Health System Final Report Client: Candia B. Laughlin, MS, RN Director of Nursing Ambulatory Care Coordinator: Laura Mittendorf Management
Analysis of Nursing Workload in Primary Care University of Michigan Health System Final Report Client: Candia B. Laughlin, MS, RN Director of Nursing Ambulatory Care Coordinator: Laura Mittendorf Management
Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service
 Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Continuity: Why It Matters and How to Build It
 Summit 2011 LEARN SHARE TRANSFORM Continuity: Why It Matters and How to Build It Clinica Family Health Services-Pecos Clinic Judy Troyer, Clinic Director Session 1B March 7,11:00 AM -12:30 PM Safety Net
Summit 2011 LEARN SHARE TRANSFORM Continuity: Why It Matters and How to Build It Clinica Family Health Services-Pecos Clinic Judy Troyer, Clinic Director Session 1B March 7,11:00 AM -12:30 PM Safety Net
A Comparison of Job Responsibility and Activities between Registered Dietitians with a Bachelor's Degree and Those with a Master's Degree
 Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 11-17-2010 A Comparison of Job Responsibility and Activities between Registered Dietitians
Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 11-17-2010 A Comparison of Job Responsibility and Activities between Registered Dietitians
Suicide Among Veterans and Other Americans Office of Suicide Prevention
 Suicide Among Veterans and Other Americans 21 214 Office of Suicide Prevention 3 August 216 Contents I. Introduction... 3 II. Executive Summary... 4 III. Background... 5 IV. Methodology... 5 V. Results
Suicide Among Veterans and Other Americans 21 214 Office of Suicide Prevention 3 August 216 Contents I. Introduction... 3 II. Executive Summary... 4 III. Background... 5 IV. Methodology... 5 V. Results
Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA
 JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
JEPM Vol XVII, Issue III, July-December 2015 1 Original Article 1 Assistant Professor, Department of Anesthesiology and Pediatrics, Duke University School of Medicine, Durham, NC, USA 2 Resident Physician,
Scottish Hospital Standardised Mortality Ratio (HSMR)
 ` 2016 Scottish Hospital Standardised Mortality Ratio (HSMR) Methodology & Specification Document Page 1 of 14 Document Control Version 0.1 Date Issued July 2016 Author(s) Quality Indicators Team Comments
` 2016 Scottish Hospital Standardised Mortality Ratio (HSMR) Methodology & Specification Document Page 1 of 14 Document Control Version 0.1 Date Issued July 2016 Author(s) Quality Indicators Team Comments
Design Principles for Learning and Caring in Patient-Centered Primary Care Homes
 The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
A mental health brief intervention in primary care: Does it work?
 A mental health brief intervention in primary care: Does it work? Author Taylor, Sarah, Briggs, Lynne Published 2012 Journal Title The Journal of Family Practice Copyright Statement 2011 Quadrant HealthCom.
A mental health brief intervention in primary care: Does it work? Author Taylor, Sarah, Briggs, Lynne Published 2012 Journal Title The Journal of Family Practice Copyright Statement 2011 Quadrant HealthCom.
Briefing: Reducing hospital admissions by improving continuity of care in general practice
 Briefing February 2017 Briefing: Reducing hospital admissions by improving continuity of care in general practice Sarah Deeny, Tim Gardner, Sally Al-Zaidy, Isaac Barker, Adam Steventon Key points Continuity
Briefing February 2017 Briefing: Reducing hospital admissions by improving continuity of care in general practice Sarah Deeny, Tim Gardner, Sally Al-Zaidy, Isaac Barker, Adam Steventon Key points Continuity
Executive Summary. This Project
 Executive Summary The Health Care Financing Administration (HCFA) has had a long-term commitment to work towards implementation of a per-episode prospective payment approach for Medicare home health services,
Executive Summary The Health Care Financing Administration (HCFA) has had a long-term commitment to work towards implementation of a per-episode prospective payment approach for Medicare home health services,
Telephone triage systems in UK general practice:
 Research Tim A Holt, Emily Fletcher, Fiona Warren, Suzanne Richards, Chris Salisbury, Raff Calitri, Colin Green, Rod Taylor, David A Richards, Anna Varley and John Campbell Telephone triage systems in
Research Tim A Holt, Emily Fletcher, Fiona Warren, Suzanne Richards, Chris Salisbury, Raff Calitri, Colin Green, Rod Taylor, David A Richards, Anna Varley and John Campbell Telephone triage systems in
Utilisation patterns of primary health care services in Hong Kong: does having a family doctor make any difference?
 STUDIES IN HEALTH SERVICES CLK Lam 林露娟 GM Leung 梁卓偉 SW Mercer DYT Fong 方以德 A Lee 李大拔 TP Lam 林大邦 YYC Lo 盧宛聰 Utilisation patterns of primary health care services in Hong Kong: does having a family doctor
STUDIES IN HEALTH SERVICES CLK Lam 林露娟 GM Leung 梁卓偉 SW Mercer DYT Fong 方以德 A Lee 李大拔 TP Lam 林大邦 YYC Lo 盧宛聰 Utilisation patterns of primary health care services in Hong Kong: does having a family doctor
Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study.
 d AUSTRALIAN CATHOLIC UNIVERSITY Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study. Sue Webster sue.webster@acu.edu.au 1 Background
d AUSTRALIAN CATHOLIC UNIVERSITY Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study. Sue Webster sue.webster@acu.edu.au 1 Background
Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN
 Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN Cheryl B. Jones, PhD, RN, FAAN; Mark Toles, PhD, RN; George J. Knafl, PhD; Anna S. Beeber, PhD, RN Research Brief,
Predicting Transitions in the Nursing Workforce: Professional Transitions from LPN to RN Cheryl B. Jones, PhD, RN, FAAN; Mark Toles, PhD, RN; George J. Knafl, PhD; Anna S. Beeber, PhD, RN Research Brief,
PCSP 2016 PCMH 2014 Crosswalk
 - Crosswalk 1 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice (PCSP) 2016 standards with NCQA s Patient-Centered Medical Home (PCMH) 2014 standards. The column on the right identifies
- Crosswalk 1 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice (PCSP) 2016 standards with NCQA s Patient-Centered Medical Home (PCMH) 2014 standards. The column on the right identifies
Determining Like Hospitals for Benchmarking Paper #2778
 Determining Like Hospitals for Benchmarking Paper #2778 Diane Storer Brown, RN, PhD, FNAHQ, FAAN Kaiser Permanente Northern California, Oakland, CA, Nancy E. Donaldson, RN, DNSc, FAAN Department of Physiological
Determining Like Hospitals for Benchmarking Paper #2778 Diane Storer Brown, RN, PhD, FNAHQ, FAAN Kaiser Permanente Northern California, Oakland, CA, Nancy E. Donaldson, RN, DNSc, FAAN Department of Physiological
Quality of Care of Medicare- Medicaid Dual Eligibles with Diabetes. James X. Zhang, PhD, MS The University of Chicago
 Quality of Care of Medicare- Medicaid Dual Eligibles with Diabetes James X. Zhang, PhD, MS The University of Chicago April 23, 2013 Outline Background Medicare Dual eligibles Diabetes mellitus Quality
Quality of Care of Medicare- Medicaid Dual Eligibles with Diabetes James X. Zhang, PhD, MS The University of Chicago April 23, 2013 Outline Background Medicare Dual eligibles Diabetes mellitus Quality
What constitutes continuity of care in schizophrenia, and is it related to outcomes? Discuss. Alastair Macdonald
 What constitutes continuity of care in schizophrenia, and is it related to outcomes? Discuss. Alastair Macdonald NICE clinical guideline 136 (2011 ) Service user experience in adult mental health: improving
What constitutes continuity of care in schizophrenia, and is it related to outcomes? Discuss. Alastair Macdonald NICE clinical guideline 136 (2011 ) Service user experience in adult mental health: improving
Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports
 Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports July 2017 Contents 1 Introduction 2 2 Assignment of Patients to Facilities for the SHR Calculation 3 2.1
Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports July 2017 Contents 1 Introduction 2 2 Assignment of Patients to Facilities for the SHR Calculation 3 2.1
The Patient-Physician Relationship, Primary Care Attributes, and Preventive Services
 22 January 2004 Family Medicine The Patient-Physician Relationship, Primary Care Attributes, and Preventive Services Michael L. Parchman, MD, MPH; Sandra K. Burge, PhD Background: The importance of a sustained
22 January 2004 Family Medicine The Patient-Physician Relationship, Primary Care Attributes, and Preventive Services Michael L. Parchman, MD, MPH; Sandra K. Burge, PhD Background: The importance of a sustained
Patient Provider Communication: Does Electronic Messaging Reduce Incoming Telephone Calls?
 ORIGINAL RESEARCH Patient Provider Communication: Does Electronic Messaging Reduce Incoming Telephone Calls? Eve N. Dexter, MS, Scott Fields, MD, MHA, Rebecca E. Rdesinski, MSW, MPH, Bhavaya Sachdeva,
ORIGINAL RESEARCH Patient Provider Communication: Does Electronic Messaging Reduce Incoming Telephone Calls? Eve N. Dexter, MS, Scott Fields, MD, MHA, Rebecca E. Rdesinski, MSW, MPH, Bhavaya Sachdeva,
Doctor Patient Gender Concordance and Patient Satisfaction in Interpreter-Mediated Consultations: An Exploratory Study
 1 ORIGINAL ARTICLES Doctor Patient Concordance and Patient Satisfaction in Interpreter-Mediated Consultations: An Exploratory Study Alexander Bischoff, PhD, RN, MPH, * Patricia Hudelson, MA, PhD, and Patrick
1 ORIGINAL ARTICLES Doctor Patient Concordance and Patient Satisfaction in Interpreter-Mediated Consultations: An Exploratory Study Alexander Bischoff, PhD, RN, MPH, * Patricia Hudelson, MA, PhD, and Patrick
Essential Skills for Evidence-based Practice: Strength of Evidence
 Essential Skills for Evidence-based Practice: Strength of Evidence Jeanne Grace Corresponding Author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
Essential Skills for Evidence-based Practice: Strength of Evidence Jeanne Grace Corresponding Author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing
 BRIEF REPORT A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing Sara Kohlbeck, MPH; Brenna Akert, BS; Caroline Pace, MD; Amy Zosel, MD, MSCS ABSTRACT
BRIEF REPORT A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing Sara Kohlbeck, MPH; Brenna Akert, BS; Caroline Pace, MD; Amy Zosel, MD, MSCS ABSTRACT
Rethinking the model of primary care. Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine
 Rethinking the model of primary care Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine Why should primary care be the foundation for any healthcare
Rethinking the model of primary care Tom Bodenheimer MD Center for Excellence in Primary Care UCSF Department of Family and Community Medicine Why should primary care be the foundation for any healthcare
CROSSWALK: CHANGE CONCEPTS FOR PRACTICE TRANSFORMATION AND 2014 NCQA PCMH TM RECOGNITION STANDARDS
 CROSSWALK: CHANGE CONCEPTS FOR PRACTICE TRANSFORMATION AND 2014 NCQA PCMH TM RECOGNITION STANDARDS 1a. Provide visible and sustained leadership to lead overall cultural change as well as specific strategies
CROSSWALK: CHANGE CONCEPTS FOR PRACTICE TRANSFORMATION AND 2014 NCQA PCMH TM RECOGNITION STANDARDS 1a. Provide visible and sustained leadership to lead overall cultural change as well as specific strategies
A comparison of two measures of hospital foodservice satisfaction
 Australian Health Review [Vol 26 No 1] 2003 A comparison of two measures of hospital foodservice satisfaction OLIVIA WRIGHT, SANDRA CAPRA AND JUDITH ALIAKBARI Olivia Wright is a PhD Scholar in Nutrition
Australian Health Review [Vol 26 No 1] 2003 A comparison of two measures of hospital foodservice satisfaction OLIVIA WRIGHT, SANDRA CAPRA AND JUDITH ALIAKBARI Olivia Wright is a PhD Scholar in Nutrition
Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease
 Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease Introduction Within the COMPASS (Care Of Mental, Physical, And
Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease Introduction Within the COMPASS (Care Of Mental, Physical, And
Research Design: Other Examples. Lynda Burton, ScD Johns Hopkins University
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Risk Adjustment Methods in Value-Based Reimbursement Strategies
 Paper 10621-2016 Risk Adjustment Methods in Value-Based Reimbursement Strategies ABSTRACT Daryl Wansink, PhD, Conifer Health Solutions, Inc. With the move to value-based benefit and reimbursement models,
Paper 10621-2016 Risk Adjustment Methods in Value-Based Reimbursement Strategies ABSTRACT Daryl Wansink, PhD, Conifer Health Solutions, Inc. With the move to value-based benefit and reimbursement models,
Factors influencing patients length of stay
 Factors influencing patients length of stay Factors influencing patients length of stay YINGXIN LIU, MIKE PHILLIPS, AND JIM CODDE Yingxin Liu is a research consultant and Mike Phillips is a senior lecturer
Factors influencing patients length of stay Factors influencing patients length of stay YINGXIN LIU, MIKE PHILLIPS, AND JIM CODDE Yingxin Liu is a research consultant and Mike Phillips is a senior lecturer
INPATIENT SURVEY PSYCHOMETRICS
 INPATIENT SURVEY PSYCHOMETRICS One of the hallmarks of Press Ganey s surveys is their scientific basis: our products incorporate the best characteristics of survey design. Our surveys are developed by
INPATIENT SURVEY PSYCHOMETRICS One of the hallmarks of Press Ganey s surveys is their scientific basis: our products incorporate the best characteristics of survey design. Our surveys are developed by
Patient Care Management Teams: Improving Continuity, Office Efficiency, and Teamwork in a Residency Clinic
 Patient Care Management Teams: Improving Continuity, Office Efficiency, and Teamwork in a Residency Clinic Tricia Hern, MD Mary Talen, PhD Christopher Babiuch, MD Ramon Durazo-Arvizu, PhD Abstract Background
Patient Care Management Teams: Improving Continuity, Office Efficiency, and Teamwork in a Residency Clinic Tricia Hern, MD Mary Talen, PhD Christopher Babiuch, MD Ramon Durazo-Arvizu, PhD Abstract Background
2014 MASTER PROJECT LIST
 Promoting Integrated Care for Dual Eligibles (PRIDE) This project addressed a set of organizational challenges that high performing plans must resolve in order to scale up to serve larger numbers of dual
Promoting Integrated Care for Dual Eligibles (PRIDE) This project addressed a set of organizational challenges that high performing plans must resolve in order to scale up to serve larger numbers of dual
time to replace adjusted discharges
 REPRINT May 2014 William O. Cleverley healthcare financial management association hfma.org time to replace adjusted discharges A new metric for measuring total hospital volume correlates significantly
REPRINT May 2014 William O. Cleverley healthcare financial management association hfma.org time to replace adjusted discharges A new metric for measuring total hospital volume correlates significantly
2017/2018. KPN Health, Inc. Quality Payment Program Solutions Guide. KPN Health, Inc. A CMS Qualified Clinical Data Registry (QCDR) KPN Health, Inc.
 2017/2018 KPN Health, Inc. Quality Payment Program Solutions Guide KPN Health, Inc. A CMS Qualified Clinical Data Registry (QCDR) KPN Health, Inc. 214-591-6990 info@kpnhealth.com www.kpnhealth.com 2017/2018
2017/2018 KPN Health, Inc. Quality Payment Program Solutions Guide KPN Health, Inc. A CMS Qualified Clinical Data Registry (QCDR) KPN Health, Inc. 214-591-6990 info@kpnhealth.com www.kpnhealth.com 2017/2018
Analyzing Readmissions Patterns: Assessment of the LACE Tool Impact
 Health Informatics Meets ehealth G. Schreier et al. (Eds.) 2016 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under the terms of the Creative
Health Informatics Meets ehealth G. Schreier et al. (Eds.) 2016 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under the terms of the Creative
Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
 HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Comparison of a clinical pharmacist managed anticoagulation service with routine medical care: impact on clinical outcomes and health care costs
ARTICLE. Influence of Medicaid Managed Care Enrollment on Emergency Department Utilization by Children
 ARTICLE Influence of Medicaid Managed Care Enrollment on Emergency Department Utilization by Children Kevin J. Dombkowski, DrPH; Rachel Stanley, MD; Sarah J. Clark, MPH Objective: To explore the association
ARTICLE Influence of Medicaid Managed Care Enrollment on Emergency Department Utilization by Children Kevin J. Dombkowski, DrPH; Rachel Stanley, MD; Sarah J. Clark, MPH Objective: To explore the association
Total Cost of Care Technical Appendix April 2015
 Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Long-Stay Alternate Level of Care in Ontario Mental Health Beds
 Health System Reconfiguration Long-Stay Alternate Level of Care in Ontario Mental Health Beds PREPARED BY: Jerrica Little, BA John P. Hirdes, PhD FCAHS School of Public Health and Health Systems University
Health System Reconfiguration Long-Stay Alternate Level of Care in Ontario Mental Health Beds PREPARED BY: Jerrica Little, BA John P. Hirdes, PhD FCAHS School of Public Health and Health Systems University
School of Public Health and Health Services Department of Prevention and Community Health
 School of Public Health and Health Services Department of Prevention and Community Health Master of Public Health and Graduate Certificate Community Oriented Primary Care (COPC) 2009-2010 Note: All curriculum
School of Public Health and Health Services Department of Prevention and Community Health Master of Public Health and Graduate Certificate Community Oriented Primary Care (COPC) 2009-2010 Note: All curriculum
Appendix 5. PCSP PCMH 2014 Crosswalk
 Appendix 5 Crosswalk NCQA Patient-Centered Medical Home 2014 July 28, 2014 Appendix 5 Crosswalk 5-1 APPENDIX 5 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice () standards with
Appendix 5 Crosswalk NCQA Patient-Centered Medical Home 2014 July 28, 2014 Appendix 5 Crosswalk 5-1 APPENDIX 5 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice () standards with
Linkage between the Israeli Defense Forces Primary Care Physician Demographics and Usage of Secondary Medical Services and Laboratory Tests
 MILITARY MEDICINE, 170, 10:836, 2005 Linkage between the Israeli Defense Forces Primary Care Physician Demographics and Usage of Secondary Medical Services and Laboratory Tests Guarantor: LTC Ilan Levy,
MILITARY MEDICINE, 170, 10:836, 2005 Linkage between the Israeli Defense Forces Primary Care Physician Demographics and Usage of Secondary Medical Services and Laboratory Tests Guarantor: LTC Ilan Levy,
T he National Health Service (NHS) introduced the first
 265 ORIGINAL ARTICLE The impact of co-located NHS walk-in centres on emergency departments Chris Salisbury, Sandra Hollinghurst, Alan Montgomery, Matthew Cooke, James Munro, Deborah Sharp, Melanie Chalder...
265 ORIGINAL ARTICLE The impact of co-located NHS walk-in centres on emergency departments Chris Salisbury, Sandra Hollinghurst, Alan Montgomery, Matthew Cooke, James Munro, Deborah Sharp, Melanie Chalder...
TC911 SERVICE COORDINATION PROGRAM
 TC911 SERVICE COORDINATION PROGRAM ANALYSIS OF PROGRAM IMPACTS & SUSTAINABILITY CONDUCTED BY: Bill Wright, PhD Sarah Tran, MPH Jennifer Matson, MPH The Center for Outcomes Research & Education Providence
TC911 SERVICE COORDINATION PROGRAM ANALYSIS OF PROGRAM IMPACTS & SUSTAINABILITY CONDUCTED BY: Bill Wright, PhD Sarah Tran, MPH Jennifer Matson, MPH The Center for Outcomes Research & Education Providence
An Overview of NCQA Relative Resource Use Measures. Today s Agenda
 An Overview of NCQA Relative Resource Use Measures Today s Agenda The need for measures of Resource Use Development and testing RRU measures Key features of NCQA RRU measures How NCQA calculates benchmarks
An Overview of NCQA Relative Resource Use Measures Today s Agenda The need for measures of Resource Use Development and testing RRU measures Key features of NCQA RRU measures How NCQA calculates benchmarks
Comparative Effectiveness Research and Patient Centered Outcomes Research in Public Health Settings: Design, Analysis, and Funding Considerations
 University of Kentucky UKnowledge Health Management and Policy Presentations Health Management and Policy 12-7-2012 Comparative Effectiveness Research and Patient Centered Outcomes Research in Public Health
University of Kentucky UKnowledge Health Management and Policy Presentations Health Management and Policy 12-7-2012 Comparative Effectiveness Research and Patient Centered Outcomes Research in Public Health
Hitting the mark... sometimes. Improve the accuracy of CPT code distribution. MGMA Connexion, Vol. 5, Issue 1, January 2005
 MGMA Connexion, Vol. 5, Issue 1, January 2005 Hitting the mark... sometimes Improve the accuracy of CPT code distribution By Margie C. Andreae, MD, associate director for clinical services, Division of
MGMA Connexion, Vol. 5, Issue 1, January 2005 Hitting the mark... sometimes Improve the accuracy of CPT code distribution By Margie C. Andreae, MD, associate director for clinical services, Division of
APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS
 Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Kerlin MP, Small DS, Cooney E, et al. A randomized trial of nighttime
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Kerlin MP, Small DS, Cooney E, et al. A randomized trial of nighttime
Cultural Transformation To Prevent Falls And Associated Injuries In A Tertiary Care Hospital p. 1
 Cultural Transformation To Prevent Falls And Associated Injuries In A Tertiary Care Hospital p. 1 2008 Pinnacle Award Application: Narrative Submission Cultural Transformation To Prevent Falls And Associated
Cultural Transformation To Prevent Falls And Associated Injuries In A Tertiary Care Hospital p. 1 2008 Pinnacle Award Application: Narrative Submission Cultural Transformation To Prevent Falls And Associated
THE HEALTH RESILIENCE PROGRAM
 THE HEALTH RESILIENCE PROGRAM A PROGRAM ASSESSMENT CONDUCTED BY: Keri Vartanian, PhD Sarah Tran, MPH Bill Wright, PhD Grace Li, PhD Megan Holtorf, MPH, CCRP Michael Levinson The Center for Outcomes Research
THE HEALTH RESILIENCE PROGRAM A PROGRAM ASSESSMENT CONDUCTED BY: Keri Vartanian, PhD Sarah Tran, MPH Bill Wright, PhD Grace Li, PhD Megan Holtorf, MPH, CCRP Michael Levinson The Center for Outcomes Research
Clinical Data acquisition and management. David A. Dorr, MD, MS Data after Dark 1/2016 OHSU
 Clinical Data acquisition and management David A. Dorr, MD, MS Data after Dark 1/2016 OHSU Clinical data: Four major points (revisited) Point Clinical data has potential to transform research across the
Clinical Data acquisition and management David A. Dorr, MD, MS Data after Dark 1/2016 OHSU Clinical data: Four major points (revisited) Point Clinical data has potential to transform research across the
Type of intervention Secondary prevention of heart failure (HF)-related events in patients at risk of HF.
 Emergency department observation of heart failure: preliminary analysis of safety and cost Storrow A B, Collins S P, Lyons M S, Wagoner L E, Gibler W B, Lindsell C J Record Status This is a critical abstract
Emergency department observation of heart failure: preliminary analysis of safety and cost Storrow A B, Collins S P, Lyons M S, Wagoner L E, Gibler W B, Lindsell C J Record Status This is a critical abstract
ENGAGED LEADERSHIP. TC-02 (Core): Defines practice organizations structure and staff responsibilities/skills to support key PCMH functions.
 Change Concepts for Practice Transformation AND 2014 NCQA PCMH Standards Crosswalk to 2017 NCQA Standards Change Concept Element 2014 NCQA PCMH Standards 2014 --> 2017 2017 NCQA Standards ENGAGED LEADERSHIP
Change Concepts for Practice Transformation AND 2014 NCQA PCMH Standards Crosswalk to 2017 NCQA Standards Change Concept Element 2014 NCQA PCMH Standards 2014 --> 2017 2017 NCQA Standards ENGAGED LEADERSHIP
Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In?
 Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In? Sue Sirlin, CPEHR Director, HIT Consulting Services Bonni Brownlee, MHA CPHQ CPEHR Principal Consultant March 15, 2013 Advancing Healthcare
Patient-Centered Medical Home: What Is It and How Do SBHCs Fit In? Sue Sirlin, CPEHR Director, HIT Consulting Services Bonni Brownlee, MHA CPHQ CPEHR Principal Consultant March 15, 2013 Advancing Healthcare
Retrospective Chart Review Studies
 Retrospective Chart Review Studies Designed to fulfill requirements for real-world evidence Retrospective chart review studies are often needed in the absence of suitable healthcare databases and/or other
Retrospective Chart Review Studies Designed to fulfill requirements for real-world evidence Retrospective chart review studies are often needed in the absence of suitable healthcare databases and/or other
ORIGINAL ARTICLE. Prevalence of nonmusculoskeletal versus musculoskeletal cases in a chiropractic student clinic
 ORIGINAL ARTICLE Prevalence of nonmusculoskeletal versus musculoskeletal cases in a chiropractic student clinic Bruce R. Hodges, DC, MS, Jerrilyn A. Cambron, DC, PhD, Rachel M. Klein, DC, Dana M. Madigan,
ORIGINAL ARTICLE Prevalence of nonmusculoskeletal versus musculoskeletal cases in a chiropractic student clinic Bruce R. Hodges, DC, MS, Jerrilyn A. Cambron, DC, PhD, Rachel M. Klein, DC, Dana M. Madigan,
Rural Health Clinics
 Rural Health Clinics * An Issue Paper of the National Rural Health Association originally issued in February 1997 This paper summarizes the history of the development and current status of Rural Health
Rural Health Clinics * An Issue Paper of the National Rural Health Association originally issued in February 1997 This paper summarizes the history of the development and current status of Rural Health
In Press at Population Health Management. HEDIS Initiation and Engagement Quality Measures of Substance Use Disorder Care:
 In Press at Population Health Management HEDIS Initiation and Engagement Quality Measures of Substance Use Disorder Care: Impacts of Setting and Health Care Specialty. Alex HS Harris, Ph.D. Thomas Bowe,
In Press at Population Health Management HEDIS Initiation and Engagement Quality Measures of Substance Use Disorder Care: Impacts of Setting and Health Care Specialty. Alex HS Harris, Ph.D. Thomas Bowe,
Managing Patients with Multiple Chronic Conditions
 Best Practices Managing Patients with Multiple Chronic Conditions Fletcher Allen Health Care Case Study Organization Profile Located in Burlington, Fletcher Allen Health Care (FAHC) is Vermont s university
Best Practices Managing Patients with Multiple Chronic Conditions Fletcher Allen Health Care Case Study Organization Profile Located in Burlington, Fletcher Allen Health Care (FAHC) is Vermont s university
Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report
 Team 10 Med-List University of Michigan Health System Program and Operations Analysis Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report To: John Clark, PharmD, MS,
Team 10 Med-List University of Michigan Health System Program and Operations Analysis Cost-Benefit Analysis of Medication Reconciliation Pharmacy Technician Pilot Final Report To: John Clark, PharmD, MS,
Robert L. Schmidt, MD, PhD, MBA, Jeanne Panlener, MT(ASCP), and Jerry W. Hussong, DDS, MS, MD
 An Analysis of Clinical Consultation Activities in Clinical Pathology Who Requests Help and Why Robert L. Schmidt, MD, PhD, MBA, Jeanne Panlener, MT(ASCP), and Jerry W. Hussong, DDS, MS, MD From the Department
An Analysis of Clinical Consultation Activities in Clinical Pathology Who Requests Help and Why Robert L. Schmidt, MD, PhD, MBA, Jeanne Panlener, MT(ASCP), and Jerry W. Hussong, DDS, MS, MD From the Department
Evaluation of an independent, radiographer-led community diagnostic ultrasound service provided to general practitioners
 Journal of Public Health VoI. 27, No. 2, pp. 176 181 doi:10.1093/pubmed/fdi006 Advance Access Publication 7 March 2005 Evaluation of an independent, radiographer-led community diagnostic ultrasound provided
Journal of Public Health VoI. 27, No. 2, pp. 176 181 doi:10.1093/pubmed/fdi006 Advance Access Publication 7 March 2005 Evaluation of an independent, radiographer-led community diagnostic ultrasound provided
SINCE 1999, EIGHT STUDIES have investigated the IMPACT OF HESI SPECIALTY EXAMS: THE NINTH HESI EXIT EXAM VALIDITY STUDY
 IMPACT OF HESI SPECIALTY EXAMS: THE NINTH HESI EXIT EXAM VALIDITY STUDY ELIZABETH L. ZWEIGHAFT, EDD, RN Using an ex post facto, nonexperimental design, this, the ninth validity study of Elsevier's HESI
IMPACT OF HESI SPECIALTY EXAMS: THE NINTH HESI EXIT EXAM VALIDITY STUDY ELIZABETH L. ZWEIGHAFT, EDD, RN Using an ex post facto, nonexperimental design, this, the ninth validity study of Elsevier's HESI
PA Education Worldwide
 Physician Assistants: Past and Future Roderick S. Hooker, PhD, MBA, PA October 205 Oregon Society of Physician Assistants PA Education Worldwide Health Workforce North America 204 US Canada Population
Physician Assistants: Past and Future Roderick S. Hooker, PhD, MBA, PA October 205 Oregon Society of Physician Assistants PA Education Worldwide Health Workforce North America 204 US Canada Population
Measuring Comprehensiveness of Primary Care: Past, Present, and Future
 Measuring Comprehensiveness of Primary Care: Past, Present, and Future Mathematica Policy Research Washington, DC June 27, 2014 Welcome Moderator Eugene Rich, M.D. Mathematica Policy Research 2 About CHCE
Measuring Comprehensiveness of Primary Care: Past, Present, and Future Mathematica Policy Research Washington, DC June 27, 2014 Welcome Moderator Eugene Rich, M.D. Mathematica Policy Research 2 About CHCE
Comparing Job Expectations and Satisfaction: A Pilot Study Focusing on Men in Nursing
 American Journal of Nursing Science 2017; 6(5): 396-400 http://www.sciencepublishinggroup.com/j/ajns doi: 10.11648/j.ajns.20170605.14 ISSN: 2328-5745 (Print); ISSN: 2328-5753 (Online) Comparing Job Expectations
American Journal of Nursing Science 2017; 6(5): 396-400 http://www.sciencepublishinggroup.com/j/ajns doi: 10.11648/j.ajns.20170605.14 ISSN: 2328-5745 (Print); ISSN: 2328-5753 (Online) Comparing Job Expectations
Supplemental materials for:
 Supplemental materials for: Ricci-Cabello I, Avery AJ, Reeves D, Kadam UT, Valderas JM. Measuring Patient Safety in Primary Care: The Development and Validation of the "Patient Reported Experiences and
Supplemental materials for: Ricci-Cabello I, Avery AJ, Reeves D, Kadam UT, Valderas JM. Measuring Patient Safety in Primary Care: The Development and Validation of the "Patient Reported Experiences and
Thank you for joining us today!
 Thank you for joining us today! Please dial 1.800.732.6179 now to connect to the audio for this webinar. To show/hide the control panel click the double arrows. 1 Emergency Room Overcrowding A multi-dimensional
Thank you for joining us today! Please dial 1.800.732.6179 now to connect to the audio for this webinar. To show/hide the control panel click the double arrows. 1 Emergency Room Overcrowding A multi-dimensional
Adopting Accountable Care An Implementation Guide for Physician Practices
 Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance
 Briefing October 2017 The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance Key points As a non-executive director, it is important to understand how data
Briefing October 2017 The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance Key points As a non-executive director, it is important to understand how data
Do patients use minor injury units appropriately?
 Journal of Public Health Medicine Vol. 18, No. 2, pp. 152-156 Printed in Great Britain Do patients use minor injury units appropriately? Jeremy Dale and Brian Dolan Abstract Background This study aimed
Journal of Public Health Medicine Vol. 18, No. 2, pp. 152-156 Printed in Great Britain Do patients use minor injury units appropriately? Jeremy Dale and Brian Dolan Abstract Background This study aimed
SEPTEMBER O NE-YEAR S URVEY SURVEY REPORT. Bachelor s Degree in Nursing Program
 SEPTEMBER 2017 O NE-YEAR S URVEY SURVEY REPORT Bachelor s Degree in Nursing Program Report of Survey Results: One-year Survey Bachelor's Degree in Nursing Report Generated: September 26, 2017 For All Graduates
SEPTEMBER 2017 O NE-YEAR S URVEY SURVEY REPORT Bachelor s Degree in Nursing Program Report of Survey Results: One-year Survey Bachelor's Degree in Nursing Report Generated: September 26, 2017 For All Graduates
Putting PCMH into Practice: A Transformation Series Care Coordination & Care Transitions (CC) September 12, 2018
 Putting PCMH into Practice: A Transformation Series Care Coordination & Care Transitions (CC) September 12, 2018 WEBINAR FACILITATOR Hannah Stanfield NCQA PCMH CCE Practice Transformation Coordinator WACMHC
Putting PCMH into Practice: A Transformation Series Care Coordination & Care Transitions (CC) September 12, 2018 WEBINAR FACILITATOR Hannah Stanfield NCQA PCMH CCE Practice Transformation Coordinator WACMHC
MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN INDIANS & ALASKA NATIVES
 American Indian & Alaska Native Data Project of the Centers for Medicare and Medicaid Services Tribal Technical Advisory Group MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN
American Indian & Alaska Native Data Project of the Centers for Medicare and Medicaid Services Tribal Technical Advisory Group MEDICARE ENROLLMENT, HEALTH STATUS, SERVICE USE AND PAYMENT DATA FOR AMERICAN
2018 MIPS Quality Performance Category Measure Information for the 30-Day All-Cause Hospital Readmission Measure
 2018 MIPS Quality Performance Category Measure Information for the 30-Day All-Cause Hospital Readmission Measure A. Measure Name 30-day All-Cause Hospital Readmission Measure B. Measure Description The
2018 MIPS Quality Performance Category Measure Information for the 30-Day All-Cause Hospital Readmission Measure A. Measure Name 30-day All-Cause Hospital Readmission Measure B. Measure Description The
How Criterion Scores Predict the Overall Impact Score and Funding Outcomes for National Institutes of Health Peer-Reviewed Applications
 RESEARCH ARTICLE How Criterion Scores Predict the Overall Impact Score and Funding Outcomes for National Institutes of Health Peer-Reviewed Applications Matthew K. Eblen *, Robin M. Wagner, Deepshikha
RESEARCH ARTICLE How Criterion Scores Predict the Overall Impact Score and Funding Outcomes for National Institutes of Health Peer-Reviewed Applications Matthew K. Eblen *, Robin M. Wagner, Deepshikha
Causes and Consequences of Regional Variations in Health Care Resources in Ontario
 Causes and Consequences of Regional Variations in Health Care Resources in Thérèse A. Stukel, Ph.D. DA Alter, R Saskin, DM Rothwell Institute for Clinical Evaluative Sciences, Health Services Restructuring
Causes and Consequences of Regional Variations in Health Care Resources in Thérèse A. Stukel, Ph.D. DA Alter, R Saskin, DM Rothwell Institute for Clinical Evaluative Sciences, Health Services Restructuring
Practice Transformation: Patient Centered Medical Home Overview
 Practice Transformation: Patient Centered Medical Home Overview Megan A. Housley, MBA Business Development Director Kentucky Regional Extension Center The Triple Aim Population Health TRIPLE AIM Per Capita
Practice Transformation: Patient Centered Medical Home Overview Megan A. Housley, MBA Business Development Director Kentucky Regional Extension Center The Triple Aim Population Health TRIPLE AIM Per Capita
MERMAID SERIES: SECONDARY DATA ANALYSIS: TIPS AND TRICKS
 MERMAID SERIES: SECONDARY DATA ANALYSIS: TIPS AND TRICKS Sonya Borrero Natasha Parekh (Adapted from slides by Amber Barnato) Objectives Discuss benefits and downsides of using secondary data Describe publicly
MERMAID SERIES: SECONDARY DATA ANALYSIS: TIPS AND TRICKS Sonya Borrero Natasha Parekh (Adapted from slides by Amber Barnato) Objectives Discuss benefits and downsides of using secondary data Describe publicly
Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System
 Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System Designed Specifically for International Quality and Performance Use A white paper by: Marc Berlinguet, MD, MPH
Case-mix Analysis Across Patient Populations and Boundaries: A Refined Classification System Designed Specifically for International Quality and Performance Use A white paper by: Marc Berlinguet, MD, MPH
How can oncology practices deliver better care? It starts with staying connected.
 How can oncology practices deliver better care? It starts with staying connected. A system rooted in oncology Compared to other EHRs that I ve used, iknowmed is the best EHR for medical oncology. Physician
How can oncology practices deliver better care? It starts with staying connected. A system rooted in oncology Compared to other EHRs that I ve used, iknowmed is the best EHR for medical oncology. Physician
Medicaid EHR Incentive Program Health Information Exchange Objective Stage 3 Updated: February 2017
 Medicaid EHR Incentive Program Health Information Exchange Objective Stage 3 Updated: February 2017 The Health Information Exchange (HIE) objective (formerly known as Summary of Care ) is required for
Medicaid EHR Incentive Program Health Information Exchange Objective Stage 3 Updated: February 2017 The Health Information Exchange (HIE) objective (formerly known as Summary of Care ) is required for
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010)
 Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Integrated care for asthma: matching care to the patient
 Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Comparison of New Zealand and Canterbury population level measures
 Report prepared for Canterbury District Health Board Comparison of New Zealand and Canterbury population level measures Tom Love 17 March 2013 1BAbout Sapere Research Group Limited Sapere Research Group
Report prepared for Canterbury District Health Board Comparison of New Zealand and Canterbury population level measures Tom Love 17 March 2013 1BAbout Sapere Research Group Limited Sapere Research Group
Comparison of Anticoagulation Clinic Patient Outcomes With Outcomes From Traditional Care in a Family Medicine Clinic
 Comparison of Anticoagulation Clinic Patient Outcomes With Outcomes From Traditional Care in a Family Medicine Clinic Marvin A. Chamberlain, RPh, MS, Nannette A. Sageser, Pharm D, and David Ruiz, MD Background:
Comparison of Anticoagulation Clinic Patient Outcomes With Outcomes From Traditional Care in a Family Medicine Clinic Marvin A. Chamberlain, RPh, MS, Nannette A. Sageser, Pharm D, and David Ruiz, MD Background:
Rural Idaho Family Physicians Scope of Practice
 Boise State University ScholarWorks Community and Environmental Health Faculty Publications and Presentations Department of Community and Environmental Health 1-1-2010 Rural Idaho Family Physicians Scope
Boise State University ScholarWorks Community and Environmental Health Faculty Publications and Presentations Department of Community and Environmental Health 1-1-2010 Rural Idaho Family Physicians Scope
Pursuing the Triple Aim: CareOregon
 Pursuing the Triple Aim: CareOregon The Triple Aim: An Introduction The Institute for Healthcare Improvement (IHI) launched the Triple Aim initiative in September 2007 to develop new models of care that
Pursuing the Triple Aim: CareOregon The Triple Aim: An Introduction The Institute for Healthcare Improvement (IHI) launched the Triple Aim initiative in September 2007 to develop new models of care that
Global Health Electives Curriculum Overview Internal Medicine Residency University of Colorado Health Sciences Center January 2007
 Global Health Electives Curriculum Overview Internal Medicine Residency University of Colorado Health Sciences Center January 2007 I. Educational Purpose and Goals Students and residents often participate
Global Health Electives Curriculum Overview Internal Medicine Residency University of Colorado Health Sciences Center January 2007 I. Educational Purpose and Goals Students and residents often participate
Supplemental materials for:
 Supplemental materials for: Krist AH, Woolf SH, Bello GA, et al. Engaging primary care patients to use a patient-centered personal health record. Ann Fam Med. 2014;12(5):418-426. ONLINE APPENDIX. Impact
Supplemental materials for: Krist AH, Woolf SH, Bello GA, et al. Engaging primary care patients to use a patient-centered personal health record. Ann Fam Med. 2014;12(5):418-426. ONLINE APPENDIX. Impact
