Effective communication is essential to maintain a
|
|
|
- Clementine Dixon
- 6 years ago
- Views:
Transcription
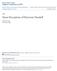
1 JNPD Journal for Nurses in Professional Development & Volume 30, Number 4, 166Y173 & Copyright B 2014 Wolters Kluwer Health Lippincott Williams & Wilkins Improving Client and Nurse Satisfaction Through the Utilization of Bedside Report 2.8 ANCC Contact Hours Mary M. Vines, MN, RN, CMSRN, CHES ƒ Alice E. Dupler, JD, APRN-BC ƒ Catherine R. Van Son, PhD, RN ƒ Ginny W. Guido, JD, MSN, RN, FAAN Bedside reporting improves client safety and trust and facilitates nursing teamwork and accountability; however, many nurses do not consider it best practice when caring for their clients. A literature review was conducted to determine whether bedside report is an essential shift handover process that promotes both client and nursing satisfaction. Implications for nurses in professional development are discussed, and strategies for developing and implementing bedside report using Lewin s theory of planned change are provided. Effective communication is essential to maintain a safe and trusting environment for clients. Eighty percent of medical errors are attributed to miscommunication among caregivers (American Nurses Association, 2012). Miscommunication is also a leading contributor of patient harm, identified in more than 80% of medical malpractice lawsuits (Lang, 2012). Thus, increased emphasis has been placed on effective communication strategies that promote client safety and facilitate nursing teamwork. The purpose of this article is to evaluate one such strategy, bedside report, to determine whether evidence supports its use as an essential shift handover practice that promotes safety and facilitates client and nurse satisfaction within an adult clinical care environment. Implications for nurses in professional development are discussed, and Mary M. Vines, MN, RN, CMSRN, CHES, is an Adjunct Nursing Instructor at Columbia Basin College, Richland, Washington, and a Surgical Staff Nurse at Kadlec Regional Medical Center, Richland, Washington. Alice E. Dupler, JD, APRN-BC, is an Associate Professor at the School of Nursing and Human Physiology, Gonzaga University and a Clinical Associate Professor at College of Nursing, Washington State University, Spokane. Catherine R. Van Son, PhD, RN, is an Assistant Professor at College of Nursing, Washington State University, Spokane. Ginny W. Guido, JD, MSN, RN, FAAN, is the Regional Director of Nursing and Assistant Dean at College of Nursing, Washington State University, Vancouver. The authors have disclosed that they have no significant relationship with, or financial interest in, any commercial companies pertaining to this article. ADDRESS FOR CORRESPONDENCE: Mary Vines, MN, RN, CMSRN, CHES, College of Nursing, Washington State University, P.O. Box 1495, Spokane, WA (e<mail: mvines12@hotmail.com). DOI: /NND strategies for developing and implementing bedside report using Lewin s theory of planned change are provided. BACKGROUND Communication errors can be verbal or written and involve all members of the healthcare team. It can be a failure to relay critical laboratory results or medication information to another caregiver, resulting in preventable complications (Agency for Healthcare Research and Quality, 2003). Although it can occur at any time during client care, the greatest risk for miscommunication is during shift handover (Sand-Jecklin & Sherman, 2013). The standardization of shift handovers was identified as one of the 2009 National Client Safety Goals from The Joint Commission (TJC). Shift handovers must include up-to-date information about the care, treatment, current condition, and recent or anticipated changes in the client. It should also encourage client involvement in their care (TJC, 2008). Employing a standardized bedside report as a universal handover process is one strategy that in part meets the requirements of these goals. Anderson and Mangino (2006) identified specific motivating factors to support the need for bedside reporting. Today, clients are more informed consumers, accessing the Internet to gain knowledge about their conditions and treatment options. Educated clients desire a collaborative model of care to be involved in their plan of care and to be kept informed of their condition and treatment options. Although the intent of bedside report is to provide the oncoming nurse with pertinent up-to-date information on the client s clinical course and plan of care, it also allows an opportunity for clients and family members to contribute their input and desires, opening the lines of communication (Griffin, 2010; Tobiano, Chaboyer, & McMurray, 2013). Bedside report increases client safety and satisfaction; creates trust between the nurse and client; reduces communication errors; and promotes accountability, teamwork, and respect among staff (Cairns, Dudjak, Hoffman, & Lorenz, 2013; Reinbeck & Fitzsimmons, 2013; Sand-Jecklin & Sherman, 2013). Nevertheless, Cairns et al. (2013) indicated that shift reports are occurring away from the client s bedside, with increased length of time, disorganization of July/August 2014
2 content, and interruptions. Verbal report alone, without the client s collaboration, can impact safety if information is incomplete or communicated poorly because of interruptions or distractions (Anderson & Mangino, 2006; Cairns et al., 2013). Regardless of the evidence, nurses are hesitant to adopt bedside report as a standard of care for client handover (Caruso, 2007; Sand-Jecklin & Sherman, 2013; Wakefield, Ragan, Brandt, & Tregnago, 2013). One obstacle results from the responsibility to protect client confidentiality, which is at risk when patients are sharing semiprivate rooms (Sand-Jecklin & Sherman, 2013; Wakefield, et al., 2012). Medical information can be unintentionally disclosed during bedside report, and staff may be concerned that this is a violation of the Health Insurance Portability and Accountability Act (HIPAA). However, the HIPAA Privacy Rule permits certain incidental uses and disclosures of protected health information to occur when the covered entity has in place reasonable safeguards and minimum necessary policies and procedures to protect an individual s privacy (Office for Civil Rights, 2002, para. 1). Therefore, the apprehension to provide bedside reporting related to protecting client confidentiality can be overstated, given that it is already incorporated within the HIPAA Privacy Rule. THEORETICAL FRAMEWORKS Hildegard Peplau s theory of interpersonal relations and Kurt Lewin s theory of planned change are two theoretical frameworks that are applicable to the bedside report process. Peplau focused on the interactions between the nurse and the client in an attempt to establish a therapeutic and trusting relationship. Bedside report is an essential component to building this relationship, and Peplau s theory provides the conceptual framework to help guide caregivers to succeed (Radtke, 2013). Peplau identified three phases within the theory of interpersonal relations: orientation, working, and termination. Clients are the main focus of the first phase, orientation. During bedside report, the nurse introduces himself or herself, explains the process of bedside report, obtains the client s permission, and then proceeds. During the second phase, working, caregivers and clients collaborate to identify needs and determine methods to accomplish them, developing and initiating a plan of care. During the third phase, termination, when the needs of the client are met, the relationship comes to an end (McCarthy & Aquino-Russell, 2009). Lewin s theory of planned change can be used as a foundation to facilitate and implement education for staff about the use of bedside report as a fundamental handover practice (Caruso, 2007; Chaboyer, McMurray, & Wallis, 2009; Costello, 2010; Hagman, Oman, Kleiner, Johnson, & Nordhagen, 2013; McMurray, Chaboyer, Wallis, & Fetherston, 2010). There are three stages to the change theory: unfreezing, moving, and refreezing. These stages outline the activities related to educating and informing to change perspective, inspiring and directing new activities, and codifying and establishing a new set of norms postadoption. During the unfreezing phase, the proposed change of bedside report, the reasoning behind it, and the anticipated outcomes are presented and explained to the staff. A force field analysis should also be conducted to determine motivating and restraining forces, which may assist or impede the change. By addressing and overcoming the restraining forces, motivating forces increase and enable the individualtoprogressintothesecond stage, which is moving (Costello, 2010). It is during the moving stage that the process of initiating and conducting bedside report begins. Lastly, the final stage, refreezing, is accomplished when bedside report is considered the exclusive handover process, utilized at every shift change (Kassean & Jagoo, 2005). LITERATURE REVIEW Methods A review of literature served as a foundation to establish whether or not bedside report is an essential handover practice to facilitate client and nurse satisfaction. Using keywords client satisfaction, nursing satisfaction, bedside report, bedside handoff, shift report, andshift handoff, a literature search was conducted in Academic Search Complete, ArticleFirst, CINAHL, the Cochrane Library, MEDLINE, PubMed, and WorldCat databases. Ninety-five publications were retrieved; the results were then limited by date (2006 to present), setting (hospital/adult clinical care), population (adult), and relevance to purpose statement. Subsequently, nine articles were chosen for this review and were categorized into two sections: client satisfaction and nursing satisfaction (see Figure 1). These categories provided the organizational framework for this article and were examined in detail. Findings Client satisfaction The Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) is a 27-item survey, which measures client perceptions of their hospital experience (Centers for Medicare & Medicaid Services, 2014). One focus of the HCAHPS survey is nursing communication. Clients are asked how often nurses listened carefully to them, whether nurses explain things in a way they could understand, and if nurses treat them with courtesy and respect. Respondents answer these questions on a 4-point rating scale of never, sometimes, usually, andalways. Higher scores signify higher satisfaction with communication (Centers for Medicare & Medicaid Services, 2013). Lack of communication between nurses and clients has been verified through the HCAHPS surveys. Often, clients feel excluded from information and decisions related to Journal for Nurses in Professional Development 167
3 FIGURE 1 Literature review. their health and hospitalization (Radtke, 2013). Bedside report can contribute to an increase in satisfaction and HCAHPS communication scores, as it assists in keeping clients informed and involved in their plan of care (Cairns et al., 2013; Maxson, Derby, Wrobleski, & Foss, 2012; McMurray, Chaboyer, Wallis, Johnson, & Gehrke, 2011; Radtke, 2013). It also allows clients to address problems or concerns and correct inaccuracies (Maxson et al., 2012) July/August 2014
4 The traditional taped or verbal report can result in a communication failure among staff members, increasing errors and decreasing client safety. These factors were cited by Anderson and Mangino (2006) as driving forces behind the implementation of bedside report on a 32-bed surgical unit utilizing a client-centered care delivery model. In preparation for implementation, the staff received classroom education, with written handouts. Upon admission to the unit, clients received information regarding the expectations of bedside report. Eight months after initiation, results obtained from informal rounds conducted by unit managers, as well as HCAHPS scores, were analyzed and compared to the preimplementation data. Results showed that bedside report increased in client satisfaction within three key areas of communication: (1) nurses kept me informed (56%Y99%), (2) staff worked well together to provide care (98%Y99%), and (3) staff included me in decisions regarding my treatment (58%Y97%; Anderson & Mangino, 2006). Freitag and Carroll (2011) described an analysis of shift handoffs conducted on a 24-bed telemetry unit. After examining the current process, it was determined that the best method for improving and facilitating client communication and participation was to relocate nurse-to-nurse handoff to the bedside. Over a 3-month period, a pilot study was conducted on the unit, employing both bedside report and the Situation, Background, Assessment, Recommendation (SBAR) handoff tool. Using PressYGaney client satisfaction scores to measure outcomes, initiation of bedside report contributed to a 4.4% increase in overall client satisfaction and a 5.5% increase in client perceptions of being informed (2011). Reinbeck and Fitzsimmons (2013) observed similar results when a 592-bed acute care hospital initiated bedside report to enhance client safety and experiences through communication. To make the report concise, the staff chose to utilize the SBAR handoff tool. Within 6 months of implementation, HCAHPS scores within nursing communication increased from 74 to 80, an 8% change as compared to baseline, confirming the positive influence that bedside report has on client satisfaction (Reinbeck & Fitzsimmons, 2013). Sand-Jecklin and Sherman (2013) discussed the introduction of bedside report on a medical surgical unit in a large teaching hospital. Using Cronbach s alpha to determine and establish reliability, the Client Views on Nursing Care survey (Sand-Jecklin & Sherman, 2013) was selected to gather data. The survey contained 17 questions characteristic of nursing care, including respect, listening, communication, and teaching. Data were collected from 232 clients and 70 family members before initiation and from 178 clients and 72 family members 3 months after implementation. Utilizing independent t tests, the research team determined that bedside report significantly impacted responses; clients and family members reported that nurses made sure they knew who their nurse was (p =.029)and included them in shift report discussions (p =.017) (Sand- Jecklin & Sherman, 2013, p. 4). A 20-bed health center in the Midwest transitioned to bedside report with the intention of improving client satisfaction (Wakefield et al., 2012). Before the changeover, an analysis was conducted on the existing report process, collecting baseline data through nurse surveys and client communication scores. For 6 months after implementation, monthly client satisfaction scores, obtained through the PressYGaney survey instrument, increased by an average of 11.1 points (range, 8.7Y14.0), as compared to preimplementation. Longitudinal results, which were observed 23 months after initiation, showed an increase of 6.9 points (range, 5.5Y7.6). In addition, during this time, 43 client interviews were conducted in an attempt to determine the client s perceptions of bedside report and how satisfied they were with the process. Seventy-two percent of surveyed clients indicated that they were very satisfied with bedside report. Nursing satisfaction Researchers have identified positive nursing perceptions toward bedside report. Nurses utilizing bedside report stated that it reduced communication errors among staff; promoted accountability; and enhanced teamwork, collaboration, and respect (Anderson & Mangino, 2006; Cairns et al., 2013; Reinbeck & Fitzsimmons, 2013; Sand-Jecklin & Sherman, 2013). Bedside report allows for immediate visualization of the client during shift change, facilitating the prioritization of care (Anderson & Mangino, 2006; Jeffs et al., 2013; Maxson et al., 2012). In addition, it encourages experiential learning and improves the accuracy and efficacy of shift report (Anderson & Mangino, 2006; Sand-Jecklin & Sherman, 2013). Nurses at a large academic hospital expressed concerns over disorganization, length, and accuracy of shift reporting. As a result, the hospital launched bedside reporting on a 23-bed trauma unit to improve efficiency and value of the handover process (Cairns et al., 2013). Anonymous surveys were completed by staff 3 months prior to and following the implementation of bedside reporting. The survey tool was developed by an investigator, tested on nursing management to determine clarity, and then uploaded to Survey Monkey. Using a 5-point Likert scale (1 = strongly agree to 5 =strongly disagree), nurses were asked to rank the current automated method based on conciseness of the report, accuracy of information, nurse availability after report, and excessive time spent on report. Three months following the initiation of bedside report, nursing satisfaction increased in several areas; positive change was identified in conciseness of the report (38% [n = 29] to 77.8% [n = 18]), accuracy of information (72.4% [n = 29] to 83.4% [n =18]),andnurse availability after report (75.9% [n = 29] to 88.9% [n =18]). Journal for Nurses in Professional Development 169
5 Nurses reported that time spent on report decreased from 48.2% (n = 29) to 38.9% (n = 18). In addition, the nurses believed that bedside report generated more staff accountability and provided a greater sense of confidence in themselves while providing client care (Cairns et al., 2013). Chaboyer et al. (2010) conducted a descriptive study in six medical and surgical units in two hospitals that focused on the components and processes of bedside report in relation to nurse perceptions and outcomes. The components of bedside report consisted of the oncoming team, as well as the outgoing team leader, the client, a handover sheet, which included the client s demographics, diagnosis, history, and clinical condition, and the bedside chart containing medication records and risk assessment charts. The processes were identified as three phases: before, during, and after handover. Before handover, involved staff updating the computer generated handover sheet and informing the client about the upcoming shift change. During handover, information was reviewed and communicated at the bedside, allowing for client contributions. Perceived outcomes of bedside handover and its components and processes were identified through interviews with 34 nurses. Nurses acknowledged that bedside report improved accuracy, accountability, delivery, preparation, and communication, and it encouraged client-centered care (Chaboyer et al., 2010). The initiation of bedside report on a 32-bed medicaly surgical unit was the result of nurse dissatisfaction (Evans, Grunawalt, McClish, Wood, & Friese, 2012). Literature on best practices for handover was reviewed by the unit manager, nurse specialist, nurse supervisor, and clinical educator. It was determined that bedside report may resolve some of the issues with the current handover process, such as the lack of client involvement. Preimplementation data were collected to establish a baseline, and postimplementation data were collected 6 months after to evaluate effectiveness. After transferring handover to the bedside, nurse satisfaction scores increased from a baseline of 37% to 78%. Having the ability to assess the client immediately while conducting a report and then clarify or ask questions with the outgoing shift contributed to this increase in satisfaction (Evans et al., 2012). Maxsonetal.(2012)conductedresearchinasmall 11-bed acute care unit to determine whether bedside report increased communication, accountability, and prioritization among nursing staff and, therefore, increased nursing satisfaction. Using a survey developed by an investigator with a 5-point Likert scale (1 = strongly agree to 5 = strongly disagree), 15 nurses participated in a pre- and post- bedside report survey focused on the connection between handover and the hypothesized benefits. Baseline scores had been between 2 (agree)and 4(disagree). Every question on the post-bedside report survey scored a 1, indicating the nurses strongly agreed that bedside report increased accountability, communication, and prioritization. In addition, nurses stated they felt more prepared to speak to physicians about their clients after utilizing bedside report (Maxson et al., 2012). IMPLICATIONS FOR THE NURSES IN PROFESSIONAL DEVELOPMENT The reviewed studies provide evidence that supports using bedside report as an essential shift handover practice within an adult clinical care environment, with improvements in client and nurse satisfaction determined repeatedly. It is integral to the development of best practices that this current evidence is included. Bedside reports, modified to meet client preferences and values when exercising clinical judgment, facilitates patient-centered care. Lewin s theory of planned change was cited in the reviewed literature as the foundation for transforming nurse attitudes and shift handovers to the bedside (Caruso, 2007; Chaboyer et al., 2009; Costello, 2010; Hagman et al., 2013; McMurray et al., 2010). Implications and suggestions for developing and initiating an educational inservice for staff on bedside report utilizing Lewin s theory as well as recommendations for maintaining the new handover process are described below. Implementing Bedside Report Using Lewin s Theory of Planned Change Lewin s theory of planned change can provide the foundational framework to achieve success when implementing bedside report (see Figure 2). Unfreezing phase. The purpose of the unfreezing phase is to confront and challenge existing staff attitudes and beliefs toward bedside report. Despite research and documentation of the benefits of bedside reporting, numerous barriers are cited in the opposition against implementing it into standard practice. Although the barriers related to nurses comfort level can vary in origin and validity, it is understood that nurses are generally supportive of change if it improves client care and outcomes (McMurray et al., 2010). Appealing to this favorability is critical in unfreezing the challenge to change. Using valid and reliable evidence retrieved from literature and TJC recommendations for best practice, a committee composed of staff nurses, unit managers, and clinical educators who support bedside report can lead the change process, providing information to the staff behind the need for change to bedside handover. Informational meetings with open forums can allow staff to ask questions, receive answers, and express concerns about the impending change in a nonjudgmental environment (Burke & McLaughlin, 2012; Caruso, 2007; Grant & Colello, 2009). Moving phase. In the moving phase, the process of bedside report is introduced, with a focus on achieving staff acceptance. To begin, the committee should explore current July/August 2014
6 FIGURE 2 Implementing bedside report: Strategies for nurse educators. literature on standard scripts used during bedside report. Existing handover scripts such as SBAR, AIDET (acknowledge, introduce, duration, explanation, and thank you), and ISHAPED (introduction, story, history, assessment, plan, error prevention, and dialogue) have been widely accepted and useful for communicating essential elements during handover (Friesen, Herbst, Turner, Speroni, & Robinson, 2013; McMurray et al., 2010; Reinbeck & Fitzsimmons, 2013; Sand-Jecklin & Sherman, 2013). Ultimately, however, the final script selection should be made by the affected staff (Costello, 2010; Risenberg, Leitzch, & Cunningham, 2010). Staff should participate in determining the actual process of the bedside report. Chaboyer et al. (2009) outlined that important components of the process should include who will be involved in the handoff (oncoming and off-going nurse, nursing assistant, lead nurse) and what information should be covered (vital signs, flow sheet, medications, plan of care). Safety checks, including addressing clientcontrolled analgesics (PCA) and intravenous fluids, should be included (Costello, 2010), as well as a nonmedication review, including a room check, quick access to oxygen, tubing, suction, and an Ambu bag. Once the components and processes have been determined, an educational inservice should be conducted to present and discuss expectations, address concerns that were identified during the unfreezing phase, and reiterate the importance behind bedside report. Another aspect of the inservice is the enhancement of communication skills, which contributes to client satisfaction (McMurray et al., 2011). Role-playing can provide an opportunity to cultivate and improve communication skills, while easing anxiety and increasing confidence in the ability to perform bedside report (Burke & McLaughlin, 2013; Cairns et al., 2013; Caruso, 2007). Novice nurses may need guidance on what material should be communicated during report, whereas veteran nurses may need reminders on what is appropriate for the bedside versus what should be communicated elsewhere. Role-playing can be especially beneficial when handling difficult situations and clients (Hagman et al., 2013). Using nonmedical terminology during handover should also be emphasized, as it enables clients to comprehend their plan of care more thoroughly, providing them with the opportunity to share their opinions and expectations (McMurray et al., 2011). Refreezing phase. In the refreezing phase, bedside report has been incorporated into daily practice and has become the primary handover method utilized at every shift change. Evaluations, anonymous surveys, debriefing Journal for Nurses in Professional Development 171
7 sessions, and monthly meetings can identify unresolved issues or concerns with the new process. Obtaining continuous staff feedback allows for modifications and generates greater nurse satisfaction and adherence (Anderson & Mangino, 2006; Caruso, 2007; Costello, 2010). Sharing (HCAHPS) scores with staff can also provide tangible evidence of client satisfaction, providing the encouragement needed to sustain the change (Baker, 2010). Mandatory continuing education and annual performance competencies for staff may be necessary to maintain the new practice. In addition, new staff orientation should include training on bedside report, so individuals are aware of the expectations for handover (Chaboyer et al., 2009; McMurray et al., 2010). RECOMMENDATIONS FOR FUTURE RESEARCH Although there are several handoff methods in use, bedside report certainly seems to warrant further study to continue to demonstrate the opportunities to improve client satisfaction, nursing satisfaction, and client outcomes. Athwal, Fields, and Wagnell (2009) stated that shift reports that lack a formal structure and guidelines can lead to inefficiencies and the sharing of irrelevant and inadequate information (p. 143). The connection between the use of a standardized script or handoff tool during bedside report and its correlation to an increase in client and nurse satisfaction should be further examined. In addition, use of whiteboards in conjunction with bedside report can be further tested to assure that conveyed information is relevant, accurate, consistent, and easy for staff to use (Sehgal, Green, Vidyarthi, Blegen, & Wachte, 2010). Investigating a connection between whiteboard use during bedside report and client and nurse satisfaction should be further examined. Further investigation into the role of bedside report and its connection to client outcomes is warranted. Current research suggests that initiating bedside reports is correlated with a decrease in client falls during shift change (Athwal et al., 2009; Frietag & Carroll, 2011) and a decrease in medication errors (Sand-Jecklin & Sherman, 2013). Others have also suggested that the relationship between bedside report and activation of rapid response or code teams should also be analyzed to examine its effect on adverse or sentinel events. CONCLUSION The greatest risk for miscommunication within the healthcare environment is during shift handover (Sand- Jecklin & Sherman, 2013). In an effort to eliminate this risk, TJC recognized the need to standardize shift handovers and involve the client during the interaction (Joint Commission on Accreditation of Healthcare Organizations, 2008). Employing bedside report as a universal handover process is one strategy that in part meets these provisions. The purpose of this article was to determine whether bedside report is an essential handover practice that facilitates both client and nursing satisfaction in care settings. Evidence showed a direct correlation between this handover and increased satisfaction in both groups, validating the importance of shifting the process to the bedside. The nurse in professional development can be the primary facilitator for change, making bedside report an effective communication tool for the shift change process. References Agency for Healthcare Research and Quality. (2003). AHRQ s client safety initiative: Building foundations, reducing risk. Interim report to the Senate Committee on Appropriations (AHRQ Publication No. 04-RG005). Rockville, MD. American Nurses Association. (2012, October 5). Tackling miscommunication among caregivers. Retrievedfrom Anderson, C., & Mangino, R. (2006). Nurse shift report: Who says you can t talk in front of the client? Nursing Administration Quarterly, 30(2), 112Y122. Athwal, P., Fields, W., & Wagnell, E. (2009). Standardization of change-of-shift report. Journal of Nursing Care Quality, 24(2), 143Y147. Baker, S. (2010). Bedside shift report improves patient safety and nurse accountability. Journal of Emergency Nursing, 36(4), 355Y358. Burke, W., & McLaughlin, D. (2012). (2013). Partnering for change. American Journal of Nursing, 113(2), 47Y51. Cairns, L., Dudjak, L., Hoffman, R., & Lorenz, H. (2013). Utilizing bedside shift report to improve the effectiveness of shift handoff. Journal of Nursing Administration, 43(3), 160Y165. Caruso, E. (2007). The evolution of nurse-to-nurse bedside report on a medical-surgical cardiology unit. Medical Surgical Nursing, 16(1), 17Y22. Centers for Medicare & Medicaid Services. (2013, August). HCAHPS fact sheet. Retrieved from Centers for Medicare & Medicaid Services. (2014, March). Standard HCAHPS survey. Retrieved from instrument.aspx Chaboyer, W., McMurray, A., Johnson, J., Hardy, L., Wallis, M., & Chu, F. (2009). Bedside handover: Quality improvement strategy to transform care at the bedside. Journal of Nursing Care Quality, 24(2), 136Y142. Chaboyer, W., McMurray, A., & Wallis, M. (2010). Bedside nursing handover: A case study. International Journal of Nursing Practice, 16, 27Y34. Costello, M. (2010). Changing handoffs: The shift is on. Nursing Management, 41(10), 39Y42. Evans, D., Grunawalt, J. McClish, D., Wood, W., & Friese, C. (2012). Bedside shift-to-shift nursing report: Implementation and outcomes. MedSurg Nursing, 21(5), 281Y292. Freitag, M., & Carroll, V. (2011). Handoff communication: Using failure modes and effects analysis to improve the transition in care process. Quality Management in Health Care, 20(2), 103Y109. doi: /QMH.0b013e f58 Friesen, M., Herbst, A., Turner, J., Speroni, K., & Robinson, J. (2013). Developing a client-centered ISHAPED handoff with client/family and parent advisory councils. Journal of Nursing Care Quality, 28(3), 208Y216. Grant, B., & Colello, S. (2009). Engaging the client in handoff communication at the bedside. Nursing, 39(10), 22Y24. Griffin, T. (2010). Bringing change-of-shift report to the bedside: A client- and family-centered approach. Journal of Perinatal and Neonatal Nursing, 24(4), 348Y July/August 2014
8 Hagman, J., Oman, K., Kleiner, C., Johnson, E., & Nordhagen, J. (2013). Lessons learned from the implementation of a bedside handoff model. Journal of Nursing Administration, 43(6), 315Y317. Jeffs, L., Acott, A., Simpson, E., Campbell, H., Irwin, T., Lo, J., I Cardoso, R. (2013). The value of bedside shift reporting: Enhancing nurse surveillance, accountability, and client safety. Journal of Nursing Care Quality, 28(3), 229Y232. Joint Commission on Accreditation of Healthcare Organizations. (2008) National Client Safety Goals. Joint Commission Perspectives, 28(7), 11Y14. Kassean, H., & Jagoo, Z. (2005). Managing change in the nursing handover from traditional to bedside handoverva case study from Mauritius. BioMed Central Nursing, 4(1), 1Y6. doi: / Lang, E. (2012). A better client experience through better communication. Journal of Radiology Nursing, 31(4), 114Y119. doi: /j.jradnu Maxson, P., Derby, K., Wrobleski, D., & Foss, D. (2012). Bedside nurse-to-nurse handoff promotes client safety. MEDSURG Nursing, 21(3), 140Y145. McCarthy, C., & Aquino-Russell, C. (2009). A comparison of two nursing theories in practice: Peplau and Parse. Nursing Science Quarterly, 22(1), 34Y40. McMurray, A., Chaboyer, W., Wallis, M., & Fetherston, C. (2010). Implementing bedside handover: Strategies for change management. Journal of Clinical Nursing, 19, 2580Y2589. McMurray, A., Chaboyer, W., Wallis, M., Johnson, J., & Gehrke, T. (2011). Clients perspectives of bedside nursing handover. Collegian, 18(1), 19Y26. Office for Civil Rights. (2002). HIPAA Privacy: Incidental uses and disclosures [45 CFR (a)(1)(iii)]. U.S. Department of Health and Human Services. Retrieved from hipaa/understanding/coveredentities/incidentalusesand disclosures.htm Radtke, K. (2013). Improving client satisfaction with nursing communication using bedside shift report. Journal for Advanced Nursing Practice, 27(1), 19Y25. Reinbeck, D., & Fitzsimons, V. (2013). Improving the client experience through bedside shift report. Nursing Management, 44(2), 16Y17. Risenberg, L., Leitzch, J., & Cunningham, J. (2010). Nursing handoffs: A systemic review of literature. American Journal of Nursing, 110(4), 24Y34. Sand-Jecklin, K., & Sherman, J. (2013). Incorporating bedside report into nursing handoff: Evaluation of change in practice. Journal of Nursing Care Quality, 28(2), 186Y194. doi: /NCQ.0b013e31827a4795 Sehgal, N., Green, A., Vidyarthi, A., Blegen, M., & Wachter, R. (2010). Client whiteboards as a communication tool in the hospital setting: A survey of practices and recommendations. Journal of Hospital Medicine, 5(4), 234Y239. Tobiano, G., Chaboyer, W., & McMurray A. (2013). Family members perceptions of the nursing bedside handover. Journal of Clinical Nursing, 22(1Y2), 192Y200. doi: /j x Wakefield, D., Ragan, R., Brandt, J., & Tregnago, M. (2012). Making the transition to nursing bedside shift reports. The Joint Commission Journal on Quality and Client Safety, 38(6), 243Y253. For more than 21 additional continuing education articles related to professional development, go to NursingCenter.com\CE. Journal for Nurses in Professional Development 173
IMPROVING COMMUNICATION IN THE CLINICAL ENVIRONMENT THROUGH BEDSIDE SHIFT REPORT (BSR): A QUALITY IMPROVEMENT PROJECT. Karen Burk
 IN THE CLINICAL ENVIRONMENT THROUGH BEDSIDE SHIFT REPORT (BSR): A QUALITY IMPROVEMENT PROJECT by Karen Burk MARYLEE BRESSIE, DNP, Faculty Mentor and Chair JOHN SCHMIDT, DNP, Committee Member ANITA GRIMES,
IN THE CLINICAL ENVIRONMENT THROUGH BEDSIDE SHIFT REPORT (BSR): A QUALITY IMPROVEMENT PROJECT by Karen Burk MARYLEE BRESSIE, DNP, Faculty Mentor and Chair JOHN SCHMIDT, DNP, Committee Member ANITA GRIMES,
Sustaining Bedside Report. Collaborative Outcomes Council Update September, 2016
 Sustaining Bedside Report Collaborative Outcomes Council Update September, 2016 Background A well-established best practice that improves communication, supports patient safety and patient satisfaction
Sustaining Bedside Report Collaborative Outcomes Council Update September, 2016 Background A well-established best practice that improves communication, supports patient safety and patient satisfaction
Text-based Document. Improving Transitions of Care with Bedside Report. Authors Lehmer, Joshua S. Downloaded 26-Apr :02:57
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Implementing Bedside Shift Report: An Evaluation of Change in Practice
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2015 Implementing Bedside Shift Report: An Evaluation of Change in Practice
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2015 Implementing Bedside Shift Report: An Evaluation of Change in Practice
RUNNING HEAD: HANDOVER 1
 RUNNING HEAD: HANDOVER 1 Evidence-Based Practice Project: Implementing Bedside Nursing Handover Jane Jones, BSN RN Austin State Univeristy August 18, 2017 RUNNING HEAD: HANDOVER 2 I. Introduction The purpose
RUNNING HEAD: HANDOVER 1 Evidence-Based Practice Project: Implementing Bedside Nursing Handover Jane Jones, BSN RN Austin State Univeristy August 18, 2017 RUNNING HEAD: HANDOVER 2 I. Introduction The purpose
Text-based Document. Improving Patient Satisfaction with Nursing Communication in an Acute Care Setting. Downloaded 8-Apr :05:11
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Bedside Shift Handoff
 Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Bedside Shift Handoff Amelia Bard BSN, RN Lehigh Valley Health Network Tyler McLean BSN, RN Lehigh Valley Health Network
Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Bedside Shift Handoff Amelia Bard BSN, RN Lehigh Valley Health Network Tyler McLean BSN, RN Lehigh Valley Health Network
Nurse Shift Handoff Report at the Patient's Bedside: Improving Nurse-to-Nurse Communication
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-16-2016 Nurse
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-16-2016 Nurse
Development of a Bedside Shift Report Policy and Guidelines to Assist Nurses with Patient Care
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies 2016 Development of a Bedside Shift Report Policy and Guidelines to Assist Nurses with Patient Care Cynthia Snedecor Walden University
Walden University ScholarWorks Walden Dissertations and Doctoral Studies 2016 Development of a Bedside Shift Report Policy and Guidelines to Assist Nurses with Patient Care Cynthia Snedecor Walden University
Standardizing the Bedside Shift Report Process to Improve Communication and Promote Patient Safety
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Summer 8-9-2017 Standardizing
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Summer 8-9-2017 Standardizing
The role of end. shift verbal handover. of-shift
 The role of end end-of of-shift shift verbal handover Student - Ms. Antoinette David Supervisor- Prof. Eleanor Holroyd Supervisor- Dr. Mervyn Jackson Supervisor- Dr. Heather Pisani Australian Commission
The role of end end-of of-shift shift verbal handover Student - Ms. Antoinette David Supervisor- Prof. Eleanor Holroyd Supervisor- Dr. Mervyn Jackson Supervisor- Dr. Heather Pisani Australian Commission
Nurse Perceptions of Electronic Handoff
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 2016 Nurse Perceptions
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 2016 Nurse Perceptions
Nurse-To-Nurse End of Shift Report
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Nurse-To-Nurse End of Shift Report Winifred N. Nzeribe Walden University
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Nurse-To-Nurse End of Shift Report Winifred N. Nzeribe Walden University
Examining Nurse Satisfaction with a Bedside Handover Report Process
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Examining Nurse Satisfaction with a Bedside Handover Report Process Imelda
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Examining Nurse Satisfaction with a Bedside Handover Report Process Imelda
University of Arkansas, Fayetteville. Win Szeto University of Arkansas, Fayetteville
 University of Arkansas, Fayetteville ScholarWorks@UARK The Eleanor Mann School of Nursing Undergraduate Honors Theses The Eleanor Mann School of Nursing 12-2014 A Qualitative Study Evaluating Bedside Reporting
University of Arkansas, Fayetteville ScholarWorks@UARK The Eleanor Mann School of Nursing Undergraduate Honors Theses The Eleanor Mann School of Nursing 12-2014 A Qualitative Study Evaluating Bedside Reporting
HANDOFFS, the transfer of responsibility
 J Nurs Care Qual Vol. 32, No. 1, pp. 15 24 Copyright c 2017 Wolters Kluwer Health, Inc. All rights reserved. Patients Perceptions of Bedside Handoff Further Evidence to Support a Culture of Always Yvonne
J Nurs Care Qual Vol. 32, No. 1, pp. 15 24 Copyright c 2017 Wolters Kluwer Health, Inc. All rights reserved. Patients Perceptions of Bedside Handoff Further Evidence to Support a Culture of Always Yvonne
Evaluating the Effects and Process of Nurse Bedside Shift Report on Nurse s Perceptions of
 i Evaluating the Effects and Process of Nurse Bedside Shift Report on Nurse s Perceptions of Communication Patterns, Nurse Satisfaction, and Patient Involvement Final Defense Heidi M. Shank University
i Evaluating the Effects and Process of Nurse Bedside Shift Report on Nurse s Perceptions of Communication Patterns, Nurse Satisfaction, and Patient Involvement Final Defense Heidi M. Shank University
School of Nursing Applying Evidence to Improve Quality
 Applying Evidence to Improve Quality Linda A Dudjak PhD RN Associate Professor University of Pittsburgh School of Nursing Compare Two Alternatives Implement a Test of Change (Experiment) to Fix a Broken
Applying Evidence to Improve Quality Linda A Dudjak PhD RN Associate Professor University of Pittsburgh School of Nursing Compare Two Alternatives Implement a Test of Change (Experiment) to Fix a Broken
Face to Face Nursing the Bedside
 Face to Face Nursing Report @ the Bedside Contact: Mary Kunkel, RN kunkelme@upmc.edu Campus: Shadyside "Patient Safety First...Care Always..." Project Aim Statement Improve Press Ganey survey scores from
Face to Face Nursing Report @ the Bedside Contact: Mary Kunkel, RN kunkelme@upmc.edu Campus: Shadyside "Patient Safety First...Care Always..." Project Aim Statement Improve Press Ganey survey scores from
A Nurse's Perception of Hand-Off Communication Before and After Utilization of the I-5 Verification of Information Tool
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2016 A Nurse's Perception of Hand-Off Communication Before and After Utilization
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2016 A Nurse's Perception of Hand-Off Communication Before and After Utilization
Patient and Family Engagement: Mount Carmel New Albany s Journey. Susan Schultz, MSN, RN, FACHE July 16, 2017
 Patient and Family Engagement: Mount Carmel New Albany s Journey Susan Schultz, MSN, RN, FACHE July 16, 2017 Mount Carmel New Albany Surgical Hospital Built in 2003 as New Albany Surgical Hospital (NASH)
Patient and Family Engagement: Mount Carmel New Albany s Journey Susan Schultz, MSN, RN, FACHE July 16, 2017 Mount Carmel New Albany Surgical Hospital Built in 2003 as New Albany Surgical Hospital (NASH)
Bedside Nursing Handover and Multidisciplinary Whiteboard Assisted Communication
 Research Centre for Clinical and Community Practice Innovation Bedside Nursing Handover and Multidisciplinary Public Report on Pilot Study as part of the National Clinical Handover Initiative Professor
Research Centre for Clinical and Community Practice Innovation Bedside Nursing Handover and Multidisciplinary Public Report on Pilot Study as part of the National Clinical Handover Initiative Professor
IMPROVING BEDSIDE SHIFT-TO-SHIFT NURSING REPORT PROCESS
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-14-2015 IMPROVING
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-14-2015 IMPROVING
Improving Nurse-patient Communication about New Medicines
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Summer 8-17-2015 Improving
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Summer 8-17-2015 Improving
Merced College Registered Nursing 34: Advanced Medical/Surgical Nursing and Pediatric Nursing
 Merced College Registered Nursing 34: Advanced Medical/Surgical Nursing and Pediatric Nursing Course Description, Student Learning Outcomes and Competencies, Clinical Evaluation Tool, and Clinical Activities
Merced College Registered Nursing 34: Advanced Medical/Surgical Nursing and Pediatric Nursing Course Description, Student Learning Outcomes and Competencies, Clinical Evaluation Tool, and Clinical Activities
Drivers of HCAHPS Performance from the Front Lines of Healthcare
 Drivers of HCAHPS Performance from the Front Lines of Healthcare White Paper by Baptist Leadership Group 2011 Organizations that are successful with the HCAHPS survey are highly focused on engaging their
Drivers of HCAHPS Performance from the Front Lines of Healthcare White Paper by Baptist Leadership Group 2011 Organizations that are successful with the HCAHPS survey are highly focused on engaging their
Text-based Document. Implementing Strategies to Improve Patient Perception of Nursing Communication. Dunbar, Ghada; Nagar, Stacey
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Running head: HANDOFF REPORT 1
 Running head: HANDOFF REPORT 1 Exposing Students to Handoff Report Abby L. Shipley University of Southern Indiana HANDOFF REPORT 2 Abstract The topic selected for the educational project was Exposing Students
Running head: HANDOFF REPORT 1 Exposing Students to Handoff Report Abby L. Shipley University of Southern Indiana HANDOFF REPORT 2 Abstract The topic selected for the educational project was Exposing Students
Standardized Communication at the Bedside: A Review for Reimplementation
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Standardized Communication at the Bedside: A Review for Reimplementation
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2017 Standardized Communication at the Bedside: A Review for Reimplementation
Approximately 180,000 patients die annually in the
 PRACTICE IMPROVEMENT SITUATION, BACKGROUND, ASSESSMENT, AND RECOMMENDATION GUIDED HUDDLES IMPROVE COMMUNICATION AND TEAMWORK IN THE EMERGENCY DEPARTMENT Authors: Heather A. Martin, DNP, RN, PNP-BC, and
PRACTICE IMPROVEMENT SITUATION, BACKGROUND, ASSESSMENT, AND RECOMMENDATION GUIDED HUDDLES IMPROVE COMMUNICATION AND TEAMWORK IN THE EMERGENCY DEPARTMENT Authors: Heather A. Martin, DNP, RN, PNP-BC, and
Barriers & Incentives to Obtaining a Bachelor of Science Degree in Nursing
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 4-2011 Barriers & Incentives to Obtaining a Bachelor of Science Degree in Nursing Tiffany Boring Brianna Burnette
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 4-2011 Barriers & Incentives to Obtaining a Bachelor of Science Degree in Nursing Tiffany Boring Brianna Burnette
Exploring Socio-Technical Insights for Safe Nursing Handover
 Context Sensitive Health Informatics: Redesigning Healthcare Work C. Nøhr et al. (Eds.) 2017 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under
Context Sensitive Health Informatics: Redesigning Healthcare Work C. Nøhr et al. (Eds.) 2017 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under
HCAHPS, HSOPS, HACs and HIQRP Connecting the Dots
 HCAHPS, HSOPS, HACs and HIQRP Connecting the Dots Sharon Burnett, R.N., BSN, MBA Vice President of Clinical and Regulatory Affairs Missouri Hospital Association Objectives Discuss how the results of the
HCAHPS, HSOPS, HACs and HIQRP Connecting the Dots Sharon Burnett, R.N., BSN, MBA Vice President of Clinical and Regulatory Affairs Missouri Hospital Association Objectives Discuss how the results of the
PG snapshot Nursing Special Report. The Role of Workplace Safety and Surveillance Capacity in Driving Nurse and Patient Outcomes
 PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
Practice Problems. Managing Registered Nurses with Significant PRACTICE GUIDELINE
 PRACTICE GUIDELINE Managing Registered Nurses with Significant Practice Problems Practice Problems May 2012 (1/17) Mission The Nurses Association of New Brunswick is a professional regulatory organization
PRACTICE GUIDELINE Managing Registered Nurses with Significant Practice Problems Practice Problems May 2012 (1/17) Mission The Nurses Association of New Brunswick is a professional regulatory organization
International Journal of Caring Sciences September-December 2014 Volume 7 Issue 3 823
 International Journal of Caring Sciences September-December 2014 Volume 7 Issue 3 823 O R I G I N A L P A P E R Nursing Bedside Handover does not Influence Cardiovascular Surgery Patients Participation
International Journal of Caring Sciences September-December 2014 Volume 7 Issue 3 823 O R I G I N A L P A P E R Nursing Bedside Handover does not Influence Cardiovascular Surgery Patients Participation
Original Article Rural generalist nurses perceptions of the effectiveness of their therapeutic interventions for patients with mental illness
 Blackwell Science, LtdOxford, UKAJRAustralian Journal of Rural Health1038-52822005 National Rural Health Alliance Inc. August 2005134205213Original ArticleRURAL NURSES and CARING FOR MENTALLY ILL CLIENTSC.
Blackwell Science, LtdOxford, UKAJRAustralian Journal of Rural Health1038-52822005 National Rural Health Alliance Inc. August 2005134205213Original ArticleRURAL NURSES and CARING FOR MENTALLY ILL CLIENTSC.
Nursing education at the point of care can be an
 JNPD Journal for Nurses in Professional Development & Volume 33, Number 4, E1YE5 & Copyright B 2017 Wolters Kluwer Health, Inc. All rights reserved. Peer Education Versus -Based Education Improve Utilization
JNPD Journal for Nurses in Professional Development & Volume 33, Number 4, E1YE5 & Copyright B 2017 Wolters Kluwer Health, Inc. All rights reserved. Peer Education Versus -Based Education Improve Utilization
Nurse Author & Editor
 Nurse Author & Editor Leslie H. Nicoll, PhD, MBA, RN, FAAN Editor-in-Chief Menu FEBRUARY 20, 2015 EDIT Engaging Clinical Nurses Engaging Clinical Nurses in Manuscript Preparation and Publication NURSE
Nurse Author & Editor Leslie H. Nicoll, PhD, MBA, RN, FAAN Editor-in-Chief Menu FEBRUARY 20, 2015 EDIT Engaging Clinical Nurses Engaging Clinical Nurses in Manuscript Preparation and Publication NURSE
Ó Journal of Krishna Institute of Medical Sciences University 74
 ISSN 2231-4261 ORIGINAL ARTICLE Effects of Situation, Background, Assessment, and Recommendation (SBAR) Usage on Communication Skills among Nurses in a Private Hospital in Kuala Lumpur 1* 1 1 Ho Siew Eng,
ISSN 2231-4261 ORIGINAL ARTICLE Effects of Situation, Background, Assessment, and Recommendation (SBAR) Usage on Communication Skills among Nurses in a Private Hospital in Kuala Lumpur 1* 1 1 Ho Siew Eng,
The American Occupational Therapy Association Advisory Opinion for the Ethics Commission Ethical Issues Concerning Payment for Services
 The American Occupational Therapy Association Advisory Opinion for the Ethics Commission Ethical Issues Concerning Payment for Services The current health care environment has created the potential for
The American Occupational Therapy Association Advisory Opinion for the Ethics Commission Ethical Issues Concerning Payment for Services The current health care environment has created the potential for
The Effects of a Care Delivery Model Change on Nursing Staff and Patient Satisfaction
 Gardner-Webb University Digital Commons @ Gardner-Webb University Nursing Theses and Capstone Projects Hunt School of Nursing 2013 The Effects of a Care Delivery Model Change on Nursing Staff and Patient
Gardner-Webb University Digital Commons @ Gardner-Webb University Nursing Theses and Capstone Projects Hunt School of Nursing 2013 The Effects of a Care Delivery Model Change on Nursing Staff and Patient
IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION
 IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION Kayla Eddins, BSN Honors Student Submitted to the School of Nursing in partial fulfillment of the requirements
IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION Kayla Eddins, BSN Honors Student Submitted to the School of Nursing in partial fulfillment of the requirements
CAPE/COP Educational Outcomes (approved 2016)
 CAPE/COP Educational Outcomes (approved 2016) Educational Outcomes Domain 1 Foundational Knowledge 1.1. Learner (Learner) - Develop, integrate, and apply knowledge from the foundational sciences (i.e.,
CAPE/COP Educational Outcomes (approved 2016) Educational Outcomes Domain 1 Foundational Knowledge 1.1. Learner (Learner) - Develop, integrate, and apply knowledge from the foundational sciences (i.e.,
Factors Influencing Acceptance of Electronic Health Records in Hospitals 1
 Factors Influencing Acceptance of Electronic Health Records in Hospitals 1 Factors Influencing Acceptance of Electronic Health Records in Hospitals by Melinda A. Wilkins, PhD, RHIA Abstract The study s
Factors Influencing Acceptance of Electronic Health Records in Hospitals 1 Factors Influencing Acceptance of Electronic Health Records in Hospitals by Melinda A. Wilkins, PhD, RHIA Abstract The study s
The Structure of Multidisciplinary Rounds and the Effects on Patient Perceptions
 Gardner-Webb University Digital Commons @ Gardner-Webb University Nursing Theses and Capstone Projects Hunt School of Nursing 7-2016 The Structure of Multidisciplinary Rounds and the Effects on Patient
Gardner-Webb University Digital Commons @ Gardner-Webb University Nursing Theses and Capstone Projects Hunt School of Nursing 7-2016 The Structure of Multidisciplinary Rounds and the Effects on Patient
Text-based Document. Bedside Shift Report: A Patient-Centered Approach to Improving Satisfaction Scores. Downloaded 9-May :22:54
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Research Paper: The Effect of Shift Reporting Training Using the SBAR Tool on the Performance of Nurses Working in Intensive Care Units
 February 2017. Volume 3. Number 1 Research Paper: The Effect of Shift Reporting Training Using the SBAR Tool on the Performance of Nurses Working in Intensive Care Units Azade Inanloo 1, Nooredin Mohammadi
February 2017. Volume 3. Number 1 Research Paper: The Effect of Shift Reporting Training Using the SBAR Tool on the Performance of Nurses Working in Intensive Care Units Azade Inanloo 1, Nooredin Mohammadi
Running head: MEDICATION ERRORS 1. Medications Errors and Their Impact on Nurses. Kristi R. Rittenhouse. Kent State University College of Nursing
 Running head: MEDICATION ERRORS 1 Medications Errors and Their Impact on Nurses Kristi R. Rittenhouse Kent State University College of Nursing MEDICATION ERRORS 2 Abstract One in five medication dosages
Running head: MEDICATION ERRORS 1 Medications Errors and Their Impact on Nurses Kristi R. Rittenhouse Kent State University College of Nursing MEDICATION ERRORS 2 Abstract One in five medication dosages
Educational Innovation Brief: Educating Graduate Nursing Students on Value Based Purchasing
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2014 Educational
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2014 Educational
DEVELOPMENT, VALIDITY AND TESTING OF PATIENT HANDOVER DOCUMENTATION TOOL
 DEVELOPMENT, VALIDITY AND TESTING OF PATIENT HANDOVER DOCUMENTATION TOOL Jaspreet Kaur Sodhi 1, Kapil Sharma 2, Jaspreet Kaur 3, Manpreet Kaur Brar 4 Abstract: The aim of this study was to develop and
DEVELOPMENT, VALIDITY AND TESTING OF PATIENT HANDOVER DOCUMENTATION TOOL Jaspreet Kaur Sodhi 1, Kapil Sharma 2, Jaspreet Kaur 3, Manpreet Kaur Brar 4 Abstract: The aim of this study was to develop and
Communication Challenges Overcoming the Barriers to Improve Quality. Presented by: Christy Brinkman LNHA Laura Seleen RN
 Communication Challenges Overcoming the Barriers to Improve Quality Presented by: Christy Brinkman LNHA Laura Seleen RN 6-16-16 Objectives The participant will be able to identify a process to follow to
Communication Challenges Overcoming the Barriers to Improve Quality Presented by: Christy Brinkman LNHA Laura Seleen RN 6-16-16 Objectives The participant will be able to identify a process to follow to
Accountable Care Organizations. What the Nurse Executive Needs to Know. Rebecca F. Cady, Esq., RNC, BSN, JD, CPHRM
 JONA S Healthcare Law, Ethics, and Regulation / Volume 13, Number 2 / Copyright B 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Accountable Care Organizations What the Nurse Executive Needs
JONA S Healthcare Law, Ethics, and Regulation / Volume 13, Number 2 / Copyright B 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Accountable Care Organizations What the Nurse Executive Needs
Domain: Clinical Skills and Knowledge A B C D E Self Assessment NURSING PROCESS Assessment. Independently and consistently
 Domain: Clinical Skills and Knowledge A B C D E Self Assessment NURSING PROCESS Assessment Performs assessment & identifies appropriate nursing diagnosis and/or patient care standard with assistance. Performs
Domain: Clinical Skills and Knowledge A B C D E Self Assessment NURSING PROCESS Assessment Performs assessment & identifies appropriate nursing diagnosis and/or patient care standard with assistance. Performs
Organization Review Process Guide Perinatal Care Certification
 Organization Review Process Guide Perinatal Care Certification 2016 Perinatal Care Certification Review Process Guide for Health Care Organizations 2016 What s New? Review process and contents of this
Organization Review Process Guide Perinatal Care Certification 2016 Perinatal Care Certification Review Process Guide for Health Care Organizations 2016 What s New? Review process and contents of this
An analysis of service quality at a student health center
 at a student health center Cem Canel Associate Professor of Operations Management, Department of Information Systems and Operations Management, Cameron School of Business, The University of North Carolina
at a student health center Cem Canel Associate Professor of Operations Management, Department of Information Systems and Operations Management, Cameron School of Business, The University of North Carolina
Measuring Patient Safety Culture Manual, Part I: Getting Started & Planning Your Survey Process
 The Armstrong Institute for Patient Safety and Quality Measuring Patient Safety Culture Manual, Part I: Getting Started & Planning Your Survey Process This manual has been adapted from the publically available
The Armstrong Institute for Patient Safety and Quality Measuring Patient Safety Culture Manual, Part I: Getting Started & Planning Your Survey Process This manual has been adapted from the publically available
Entrustable Professional Activities (EPAs) for Psychiatry
 Professional Activities (EPAs) for Psychiatry These summaries describing the various EPAs can be used to formulate entrustability decisions and feedback comments on the clinic card. A student can be assessed
Professional Activities (EPAs) for Psychiatry These summaries describing the various EPAs can be used to formulate entrustability decisions and feedback comments on the clinic card. A student can be assessed
Prospectus Summary Brief: NICU Communication Improvement
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Spring 5-22-2015 Prospectus
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Spring 5-22-2015 Prospectus
Nurse to Nurse Handoff Report
 Patient Safety Exceeding Expectations Nurse to Nurse Handoff Report 6 Main Why are we here today? Patient Safety is at risk. 3 hour time gap of patients not being seen during report time. The most dangerous
Patient Safety Exceeding Expectations Nurse to Nurse Handoff Report 6 Main Why are we here today? Patient Safety is at risk. 3 hour time gap of patients not being seen during report time. The most dangerous
JENNIFER A. SPECHT, PHD, RN
 MENTORING RELATIONSHIPS AND THE LEVELS OF ROLE CONFLICT AND ROLE AMBIGUITY EXPERIENCED BY NOVICE NURSING FACULTY JENNIFER A. SPECHT, PHD, RN This study explored the effect of mentoring on the levels of
MENTORING RELATIONSHIPS AND THE LEVELS OF ROLE CONFLICT AND ROLE AMBIGUITY EXPERIENCED BY NOVICE NURSING FACULTY JENNIFER A. SPECHT, PHD, RN This study explored the effect of mentoring on the levels of
Your Results for: "NCLEX Review"
 Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
Pediatric Residents. A Guide to Evaluating Your Clinical Competence. THE AMERICAN BOARD of PEDIATRICS
 2017 Pediatric Residents A Guide to Evaluating Your Clinical Competence THE AMERICAN BOARD of PEDIATRICS Published and distributed by The American Board of Pediatrics 111 Silver Cedar Court Chapel Hill,
2017 Pediatric Residents A Guide to Evaluating Your Clinical Competence THE AMERICAN BOARD of PEDIATRICS Published and distributed by The American Board of Pediatrics 111 Silver Cedar Court Chapel Hill,
at OU Medicine Leadership Development Institute August 6, 2010
 Effective Patient Handovers at OU Medicine Leadership Development Institute August 6, 2010 Quality and Patient Safety Realize OU Medicine s position with respect to a culture of safety and quality. Improve
Effective Patient Handovers at OU Medicine Leadership Development Institute August 6, 2010 Quality and Patient Safety Realize OU Medicine s position with respect to a culture of safety and quality. Improve
Occupation Description: Responsible for providing nursing care to residents.
 NOC: 3152 (2011 NOC is 3012) Occupation: Registered Nurse Occupation Description: Responsible for providing nursing care to residents. Key essential skills are: Document Use, Oral Communication, Problem
NOC: 3152 (2011 NOC is 3012) Occupation: Registered Nurse Occupation Description: Responsible for providing nursing care to residents. Key essential skills are: Document Use, Oral Communication, Problem
RUNNING HEAD: SHARED GOVERNANCE IN A CLINIC SYSTEM Meyers 1. Shared Governance in a Clinic System
 RUNNING HEAD: SHARED GOVERNANCE IN A CLINIC SYSTEM Meyers 1 Shared Governance in a Clinic System Michelle M. Meyers, RN, CCRN, DNP Student, Creighton University, 2500 California Plaza, Omaha NE 68102,
RUNNING HEAD: SHARED GOVERNANCE IN A CLINIC SYSTEM Meyers 1 Shared Governance in a Clinic System Michelle M. Meyers, RN, CCRN, DNP Student, Creighton University, 2500 California Plaza, Omaha NE 68102,
Invited Speech: Evidence Based Practice: Acuity Based Care and Research Practice Change
 Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2014 Invited Speech: Evidence Based Practice: Acuity Based Care and Research Practice Change Carolyn Lindgren
Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2014 Invited Speech: Evidence Based Practice: Acuity Based Care and Research Practice Change Carolyn Lindgren
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Running head: Evidence Based 1. Evidence Based Practice Paper. Natalie Russell. Ferris State University
 Running head: Evidence Based 1 Evidence Based Practice Paper Natalie Russell Ferris State University Evidence Based 2 Abstract There has been debate in the field of nursing regarding the benefit of performing
Running head: Evidence Based 1 Evidence Based Practice Paper Natalie Russell Ferris State University Evidence Based 2 Abstract There has been debate in the field of nursing regarding the benefit of performing
INSERT ORGANIZATION NAME
 INSERT ORGANIZATION NAME Quality Management Program Description Insert Year SAMPLE-QMProgramDescriptionTemplate Page 1 of 13 Table of Contents I. Overview... Purpose Values Guiding Principles II. III.
INSERT ORGANIZATION NAME Quality Management Program Description Insert Year SAMPLE-QMProgramDescriptionTemplate Page 1 of 13 Table of Contents I. Overview... Purpose Values Guiding Principles II. III.
Employers are essential partners in monitoring the practice
 Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
CHAPTER 3. Research methodology
 CHAPTER 3 Research methodology 3.1 INTRODUCTION This chapter describes the research methodology of the study, including sampling, data collection and ethical guidelines. Ethical considerations concern
CHAPTER 3 Research methodology 3.1 INTRODUCTION This chapter describes the research methodology of the study, including sampling, data collection and ethical guidelines. Ethical considerations concern
The Use of a Standardized System of Communication to Change the Perception of Handoff Communication in a Psychiatric Setting
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2015 The Use of a Standardized System of Communication to Change the Perception
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2015 The Use of a Standardized System of Communication to Change the Perception
DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING
 DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING Jenny Gilmore, BSN, RN, CMSRN Jana Jacobs, BSN, RN, CMSRN Maine Medical Center Portland, ME Objectives Describe Partnership Rounding for the staff
DEVELOPING A CULTURE OF NURSE LED PARTNERSHIP ROUNDING Jenny Gilmore, BSN, RN, CMSRN Jana Jacobs, BSN, RN, CMSRN Maine Medical Center Portland, ME Objectives Describe Partnership Rounding for the staff
How many times have you watched a change
 J O U R N A L F O R N U R S E S I N S T A F F D E V E L O P M E N T Volume 24, Number 4, 176 184 Copyright A 2008 Wolters Kluwer Health Lippincott Williams & Wilkins Change Management Magic or Mayhem?
J O U R N A L F O R N U R S E S I N S T A F F D E V E L O P M E N T Volume 24, Number 4, 176 184 Copyright A 2008 Wolters Kluwer Health Lippincott Williams & Wilkins Change Management Magic or Mayhem?
HCAHPS: Background and Significance Evidenced Based Recommendations
 HCAHPS: Background and Significance Evidenced Based Recommendations Susan T. Bionat, APRN, CNS, ACNP-BC, CCRN Education Leader, Nurse Practitioner Program Objectives Discuss the background of HCAHPS. Discuss
HCAHPS: Background and Significance Evidenced Based Recommendations Susan T. Bionat, APRN, CNS, ACNP-BC, CCRN Education Leader, Nurse Practitioner Program Objectives Discuss the background of HCAHPS. Discuss
Program Director Dr. Leonard Friedman
 School of Public Health and Health Services Department of Health Services and Leadership Master of Health Services Administration 2011-2012 Note: All curriculum revisions will be updated immediately on
School of Public Health and Health Services Department of Health Services and Leadership Master of Health Services Administration 2011-2012 Note: All curriculum revisions will be updated immediately on
Exploring Nurses Feelings On Floating: A Phenomenological Study
 Exploring Nurses Feelings On Floating: A Phenomenological Study Marie-Paule M. Lafontant, EdD/CI, MSN, RN-BC Clinical Nurse Educator II South Miami Hospital Miami Cardiac and Vascular Institute Cardiac
Exploring Nurses Feelings On Floating: A Phenomenological Study Marie-Paule M. Lafontant, EdD/CI, MSN, RN-BC Clinical Nurse Educator II South Miami Hospital Miami Cardiac and Vascular Institute Cardiac
TrainingABC Patient Rights Made Simple Support Materials
 TrainingABC 2017 Patient Rights Made Simple Support Materials Video Transcript The Patient Bill of Rights is a list of rights first developed in 1973 and then revised in 1992, by the American Hospital
TrainingABC 2017 Patient Rights Made Simple Support Materials Video Transcript The Patient Bill of Rights is a list of rights first developed in 1973 and then revised in 1992, by the American Hospital
Innovation Diffusion: The start of a good idea, initiating a fall prevention teach back tool.
 It Takes a Village: Turning a Pilot Project into Part of the Culture Jennifer P Colwill MSN, APRN, CCNS, PCCN Dianna Copley MSN, APRN, ACCNS-AG, CCRN Shannon Rives, MSN, APRN, ACNS-BC, CCRN, CMSRN Innovation
It Takes a Village: Turning a Pilot Project into Part of the Culture Jennifer P Colwill MSN, APRN, CCNS, PCCN Dianna Copley MSN, APRN, ACCNS-AG, CCRN Shannon Rives, MSN, APRN, ACNS-BC, CCRN, CMSRN Innovation
Mandatory Public Reporting of Hospital Acquired Infections
 Mandatory Public Reporting of Hospital Acquired Infections The non-profit Consumers Union (CU) has recently sent a letter to every member of the Texas Legislature urging them to pass legislation mandating
Mandatory Public Reporting of Hospital Acquired Infections The non-profit Consumers Union (CU) has recently sent a letter to every member of the Texas Legislature urging them to pass legislation mandating
Table of. Clinical Manual. Dalhousie University School of Nursing
 Table of Clinical Manual Dalhousie University School of Nursing 1 2 Table of Contents Preamble 4 Introduction 5 BScN Program Clinical Course Descriptions 5 Year One Clinical Courses 5 Year Two Clinical
Table of Clinical Manual Dalhousie University School of Nursing 1 2 Table of Contents Preamble 4 Introduction 5 BScN Program Clinical Course Descriptions 5 Year One Clinical Courses 5 Year Two Clinical
CHAPTER 1. Documentation is a vital part of nursing practice.
 CHAPTER 1 PURPOSE OF DOCUMENTATION CHAPTER OBJECTIVE After completing this chapter, the reader will be able to identify the importance and purpose of complete documentation in the medical record. LEARNING
CHAPTER 1 PURPOSE OF DOCUMENTATION CHAPTER OBJECTIVE After completing this chapter, the reader will be able to identify the importance and purpose of complete documentation in the medical record. LEARNING
Kurt A. Patton, MS, RPh with a foreword by Thanasekaran Sinnathamby, MD Handoff Communication Handoff Handoff Communication, Global Edition:
 Handoff Contents About the author......................................... v Foreword............................................... vii Introduction............................................. xii Chapter
Handoff Contents About the author......................................... v Foreword............................................... vii Introduction............................................. xii Chapter
Standards of Practice for Professional Ambulatory Care Nursing... 17
 Table of Contents Scope and Standards Revision Team..................................................... 2 Introduction......................................................................... 5 Overview
Table of Contents Scope and Standards Revision Team..................................................... 2 Introduction......................................................................... 5 Overview
December 16, Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC
 Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists
 EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists Micah Hata, PharmD, a Roger Klotz, BSPharm, a Rick Sylvies, PharmD, b Karl Hess, PharmD, a Emmanuelle Schwartzman,
EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists Micah Hata, PharmD, a Roger Klotz, BSPharm, a Rick Sylvies, PharmD, b Karl Hess, PharmD, a Emmanuelle Schwartzman,
Barriers to a Positive Safety Culture. Donna Zankowski MPH RN
 Barriers to a Positive Safety Culture Donna Zankowski MPH RN What we ll talk about: 1. The Importance of Institutional Leadership 2. The Issue of Underreporting 3. Incident Reporting Tools 4. Employee
Barriers to a Positive Safety Culture Donna Zankowski MPH RN What we ll talk about: 1. The Importance of Institutional Leadership 2. The Issue of Underreporting 3. Incident Reporting Tools 4. Employee
Ethics for Professionals Counselors
 Ethics for Professionals Counselors PREAMBLE NATIONAL BOARD FOR CERTIFIED COUNSELORS (NBCC) CODE OF ETHICS The National Board for Certified Counselors (NBCC) provides national certifications that recognize
Ethics for Professionals Counselors PREAMBLE NATIONAL BOARD FOR CERTIFIED COUNSELORS (NBCC) CODE OF ETHICS The National Board for Certified Counselors (NBCC) provides national certifications that recognize
Running head: LEADERSHIP ANALYSIS: ROUNDING 1
 Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016
 UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016 Department Name: Department of Pharmacy Department Director: Steve Rough, MS,
UNIVERSITY OF WISCONSIN HOSPITAL AND CLINICS DEPARTMENT OF PHARMACY SCOPE OF PATIENT CARE SERVICES FY 2017 October 1 st, 2016 Department Name: Department of Pharmacy Department Director: Steve Rough, MS,
Running Head: READINESS FOR DISCHARGE
 Running Head: READINESS FOR DISCHARGE Readiness for Discharge Quantitative Review Melissa Benderman, Cynthia DeBoer, Patricia Kraemer, Barbara Van Der Male, & Angela VanMaanen. Ferris State University
Running Head: READINESS FOR DISCHARGE Readiness for Discharge Quantitative Review Melissa Benderman, Cynthia DeBoer, Patricia Kraemer, Barbara Van Der Male, & Angela VanMaanen. Ferris State University
The act of purposeful rounding,
 1.5 CONTACT HOURS HCAHPS Series Part 2 Does purposeful leader ro By Melissa Winter, MSN, RN, NEA-BC, and Linda Tjiong, MSN, DBA, RN, NE-BC In part 1 of our 3-part HCAHPS series, we looked at the new Care
1.5 CONTACT HOURS HCAHPS Series Part 2 Does purposeful leader ro By Melissa Winter, MSN, RN, NEA-BC, and Linda Tjiong, MSN, DBA, RN, NE-BC In part 1 of our 3-part HCAHPS series, we looked at the new Care
Submission Form Deadline: November 9, 2015
 Submission Form Deadline: November 9, 2015 Organization: Sinai Hospital Contact Person: Pat Moloney-Harmon, MS, RN, CCNS, FAAN Title: Clinical Outcomes Specialist, Children s Services Address: 2401 W.
Submission Form Deadline: November 9, 2015 Organization: Sinai Hospital Contact Person: Pat Moloney-Harmon, MS, RN, CCNS, FAAN Title: Clinical Outcomes Specialist, Children s Services Address: 2401 W.
PGY1 Medication Safety Core Rotation
 PGY1 Medication Safety Core Rotation Preceptor: Mike Wyant, RPh Hours: 0800 to 1730 M-F Contact: (541)789-4657, michael.wyant@asante.org General Description This rotation is a four week rotation in duration.
PGY1 Medication Safety Core Rotation Preceptor: Mike Wyant, RPh Hours: 0800 to 1730 M-F Contact: (541)789-4657, michael.wyant@asante.org General Description This rotation is a four week rotation in duration.
General Eligibility Requirements
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 Overview General Eligibility Requirements Clinical Care Program Certification (CCPC)
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 Overview General Eligibility Requirements Clinical Care Program Certification (CCPC)
Keeping Kids Safe TeamSTEPPS Essentials
 Keeping Kids Safe TeamSTEPPS Essentials TeamSTEPPS Leadership Team Michelle (Mickey) Ryerson, DNP, RN, NEA BC Glen Medellin, MD Michelle Arandes, MD Stacey Denver, DNP, FNP BC Rachael Bridwell, MSN, RN
Keeping Kids Safe TeamSTEPPS Essentials TeamSTEPPS Leadership Team Michelle (Mickey) Ryerson, DNP, RN, NEA BC Glen Medellin, MD Michelle Arandes, MD Stacey Denver, DNP, FNP BC Rachael Bridwell, MSN, RN
Critical Thinking Indicators (CTIs)
 Critical Thinking Indicators (CTIs) 2009-2010 Evidence-Based Version. Available at: www.alfaroteachsmart.com Rosalinda Alfaro-LeFevre RN, MSN, ANEF Teaching Smart / Learning Easy 6161 S.E. Landing Way
Critical Thinking Indicators (CTIs) 2009-2010 Evidence-Based Version. Available at: www.alfaroteachsmart.com Rosalinda Alfaro-LeFevre RN, MSN, ANEF Teaching Smart / Learning Easy 6161 S.E. Landing Way
The Patient Experience at Florida Hospital Learning Module for Students
 The Patient Experience at Florida Hospital Learning Module for Students 1 Introduction Adventist Health System and its East Florida Region hospitals welcome the privilege to provide a wellrounded learning
The Patient Experience at Florida Hospital Learning Module for Students 1 Introduction Adventist Health System and its East Florida Region hospitals welcome the privilege to provide a wellrounded learning
Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor
 Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2008 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution
Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2008 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution
