Medical Device Interoperability: to Enable System Solutions at the Sharp Edge of Healthcare Delivery
|
|
|
- Cori Knight
- 6 years ago
- Views:
Transcription
1 C I M I T White House Homeland Security Council Biodefense Directorate Conference April 1-2, Medical Device Interoperability: to Enable System Solutions at the Sharp Edge of Healthcare Delivery Julian M. Goldman, MD Anesthesiologist, Massachuse7s General Hospital / Harvard Medical School Medical Director, Partners HealthCare System Biomedical Engineering Founding Director, CIMIT Program on Medical Device Plug and Play Interoperability (MD PnP) Boston, Massachuse7s Contact information: 1
2 Scenario Population exposure to CBW or H5N1 pandemic May produce large numbers affected civilians in severe acute respiratory failure Mass respiratory support with mechanical ventilation Could require care by minimally skilled individuals in non-healthcare settings (e.g. high school gymnasiums) Scenario presented to CDC NCPHI BSC 20Nov08 2
3 Current Plans BARDA - Biomedical Advanced Research and Development Authority is working on Non- Pharmacologic Respiratory Countermeasures RFP* for low-cost ventilators < $2000/each for Strategic National Stockpile, with ability to ramp-up to 10,000 units in 6 months Other early planning may be addressing less expensive devices and far greater quantities *Advanced Development of Next Generation Portable VentilatorsSolicitation Number: PreSol-HHS-BARDA
4 Use Case: Flu/CBW > Respiratory Failure Acute Respiratory Failure Data General status Devices Monitoring equipment ambulance Data General status Vital signs Devices Monitoring equipment Command and Control M&S etc. Treatment at School Gymnasium by? Data Vital signs MedicaMons Procedures Devices Monitoring equipment VenMlator Decision Support? Diagnosis? Natural History? Caregiver support
5 Needs Connecting ventilators, monitors, etc. in local networks would support above and enable local care of patients, for decision support, alarms, etc. Also need for resource management Development of an open platform approach could support or automate some of these needs. 5
6 Proximity Tiers I-II (Local and regional) Local (gymnasium, field): Decision support, smart alarms, closed loop control (O 2, infusion, etc.), resource management Regional (town, etc) : Resource allocation, regional data analysis, data reduction 6
7 Proximity Tier III (remote) Remote: Means to permit population surveillance connectivity of devices and monitors at local level for remote data access Remote: Means to monitor natural history of disease and to asses treatment efficacy in near real-time Improve? Deteriorate? Management Problems? (with secretions, pulmonary barotraumas, or hypoxemia?) Is therapy effective? 7
8 High Level Problem statement Improvements in patient safety, patient care, and healthcare efficiency require systems solutions cannot be implemented due to the lack of interoperability of medical devices and systems, especially in high-acuity clinical settings. Need for interoperable systems will increase with distributed/remote care and innovative care models Ability to integrate the clinical environment is an essential step to create error-resistant systems Requirement: medical device system integration. Medical device interoperability is a key enabling capability. 8 8
9 Forward-area OR in Iraq ICU This is the current state 9
10 OR How do we prevent errors and Injuries? 10
11 How do we connect Data integramon is hard! medical devices to the EMR? Example of cables required to connect devices to the Hint: We don t use TCP/IP over Ethernet Anesthesia EMR The cables represent one aspect of the interoperability barrier
12 Examples of 4 clinical procedures and associated safety issues > (From the MD PnP Clinical Scenarios Repository) 12
13 Scenario: Surgical Fires
14 Airway Laser + O 2 > Fire O 2 enriched respiratory gas supports combusmon Surgical team must remember to minimize O 2 prior to airway laser use (dependent upon teamwork and communicamon) Tracheal Tube
15 Airway Laser O 2 Interlock Measure O 2 during anesthesia Prevent acmvamon of airway laser if inspired O 2 > ~25% Tracheal Tube Solution requires connecting laser equipment and anesthetic equipment / O 2 monitor NOT Commercially AVAILABLE Proposed and published by Sem Lampotang, PhD, Univ. of Florida, Gainesville
16 Scenario: Failure to venmlate #1 16
17 Cardio Pulmonary Bypass or Normal routine: Switch from anesthesia machine ventilator to cardiopulmonary (heart-lung) bypass machine, and back to ventilator (after bypass) 17
18 Failure to VenMlate Adverse AnestheMc Outcomes Arising from Gas Delivery Equipment: A Closed Claims Analysis. Anesthesiology. 87(4): , October Years In the second case, the anesthesiologist forgot to resume venmlamon aher separamon from cardiopulmonary bypass. The delayed detecmon of apnea was a7ributed to the fact that the audible alarms for the pulse oximeter and capnograph had been disabled during bypass and had not been reacmvated. Both paments sustained permanent brain damage. clinicians report problem, but solutions are not proposed or developed 18
19 Cardio Pulmonary Bypass NOT AVAILABLE Should alarm if both off Smart system would provide warning if both ventilator and bypass pump are off. Almost every surgical team has experienced this error! 19
20 Scenario: Failure to venmlate #2 20
21 Example: Cholecystectomy (gall bladder removal) w/ intraop cholangiography (bile duct x-ray) Workflow: 1. Ventilation is stopped 2. Intraoperative cholangeogram is performed with contrast to identify internal structures. Breath pause -> improve x-ray quality. X-ray Ventilator 21
22 With the advent of sophismcated anesthesia machines incorporamng comprehensive monitoring, it is easy to forget that serious anesthesia mishaps smll can and do occur. APSF Newsle<er Winter 2005 A 32-year-old woman had a laparoscopic cholecystectomy performed under general anesthesia. At the surgeon s request, a plane film x-ray was shot during a cholangiogram. The anesthesiologist stopped the ventilator for the film. The x-ray technician was unable to remove the film because of its position beneath the table. The anesthesiologist attempted to help her, but found it difficult because the gears on the table had jammed. Finally, the x-ray was removed, and the surgical procedure recommenced. At some point, the anesthesiologist glanced at the EKG and noticed severe bradycardia. He realized he had never restarted the ventilator. This patient ultimately expired. 22
23 What are the root causes? Inadequate alarms? Inadequate vigilance? At its root, this is a medical device system problem, because the vendlator never should have been turned off it should have been synchronized with the x ray 23
24 Synchronize x ray with expiramon: cholangiogram, roumne chest radiograph NOT COMMERCIALLY AVAILABLE Integration of imaging devices into a networked, smarter system can improve safety by avoiding ventilator shut-off, improve image quality (especially on serial images), and decrease re-imaging. Synchronization of Radiograph Film Exposure with the Inspiratory Pause Am. J. Respir. Crit. Care Med., Volume 160, Number 6, December 1999, years 24 Solution has been demonstrated in MD PnP Lab
25 End to End Approach of analyzing and prototyping X Ray VenMlator Use Case 1. Elicited clinical scenario (STA 2005 conference) 2. Analyzed requirements and workflow (MD PnP mulminsmtumonal interdisciplinary team) 3. Ve7ed by vendor, engineers 4. Use Case development / UML 5. Rapid prototype in lab 6. Iterate Design Engineers Clinical Engineers Clinicians 25 Clinical Scenario Clinical Workflow Use Cases Logic Map/Key State Diagram Technical Solution and Clinical Implementation
26 VenMlator Xray SimulaMon at ASA ScienMfic Exhibit October 15,
27 ImplicaMons of unmet needs IntegraMon of operamng room monitors for development of a smart alarm system (Navabi/Mylrea 1990) A system for opmmized design of fluid resuscitamon in trauma (1991) OR: 70% of anesthesiologists disable clinical alarms (Block, NuuMnen, Ballast 1995) ICU: 86% false alarms (Tsien, Fackler CCM 1997) 27
28 Application of novel devices and treatments CCAT example: improving alarm sensitivity and specificity with dual oximetry ICE facilitates novel annunciation strategies 28
29 29
30 Typical PCA System Patient can call to request more analgesia, but, cannot call for help when over-medicated. PCA Pump (With patient button) Patient Nurse call PCA = Patient-Controlled Analgesia 30
31 APSF PCA RecommendaMons A parmcularly a7racmve feature may be the ability to automamcally terminate or reduce PCA infusions when monitoring technology suggests the presence of opioid induced respiratory depression. To facilitate such capabilimes, we strongly endorse the efforts to develop internamonal standards for device interoperability and device device communicamon 31
32 Smart PCA monitoring system American Society of Anesthesiologists ScienMfic Exhibit October 2007 Plug-and-play detection of monitors connected to patient, Permits selection of best supervisory algorithm at point of care Exhibit recognized with First Place award 32
33 How urgent is the problem? To Err is Human IOM ,000 preventable hospital deaths annually HealthGrades PaMent Safety in American Hospitals ,000 preventable deaths annually These studies only address current pracmce models 33
34 The sharp edge of acute health care delivery: Why Focus on Medical Device Interoperability? The namonal focus has been on one way data transfer to the EMR, but Medical Devices have a unique place in the interoperability ecosystem 1. DATA Medical Devices are key data sources ( to EMR). Data obtained via current interfaces may not be complete or accurate 2. CARE DELIVERY Medical devices can be be7er umlized to improve health care delivery (fluid, medicamon, energy, measurement) 3. INJURIES Adverse Events/Near Misses that involve medical devices can be mimgated using medical devices as part of system solumons 34
35 Overview of the Medical Device Plug-and-Play Interoperability Standardization Program (MD PnP) MGH and CIMIT, with TATRC support, initiated the MD PnP program in 2004 to lead the adoption of open standards and technology for medical device interoperability to improve patient safety. More than 85 companies and institutions and > 700 experts (clinicians and engineers) have participated in four plenary conferences, working group meetings, and clinical focus groups to shape the mission and strategy and identify clinical requirements. 35
36 MD PnP stakeholder community 2004: key issues must be addressed for adopdon of interoperability: Must be clinical requirements based Regulatory obstacles Liability concerns Unclear business case No widely adopted standards In summary: Interoperability requires many elements to be aligned 36
37 Goals of the MD PnP Program 1. Lead the adopmon of open standards and related technology to support medical device interoperability and system solumons 2. Define a regulatory pathway in partnership with the FDA and other regulatory agencies 3. Elicit clinical requirements for the proposed interoperable solumons to maintain focus on pament safety. 4. Use our vendor neutral laboratory to: evaluate interoperability standards and solumons model clinical use cases (in simulamon environment) serve as a resource for medical device interoperability 5. InvesMgate safety of proposed engineering solumons 37
38 MD PnP Program collaborators NSF Philips Healthcare Lockheed MarMn and others 38
39 MD PnP Program Projects Clinical Scenarios/Use Cases Society Endorsements Standards ICE and others FDA posimon/projects Healthcare provider purchasing language MD FIRE 39
40 Clinical Requirements STA SAGES others AAMI Clinical Scenarios Focus groups: Provide examples of how interoperability could improve safety or efficiency. Design Engineers Clinical Engineers Clinicians 40 Clinical Scenario Clinical Workflow Use Cases Logic Map/Key State Diagram Technical Solution and Clinical Implementation
41 MD FIRE Medical Device Free Interoperability Requirements for the Enterprise Interoperability RFP and Contract samples Developed by MGH, Partners, Hopkins, Kaiser Conveys healthcare needs to industry, and simplify purchasing specificamons Released for public use Oct 17, Stakeholder groups from each organization: Purchasing/materials management, BME, IS, Clinical, Legal Download MD FIRE from 41
42 MD FIRE Our collaboration through the Medical Device Plug-and-Play (MD PnP) program over the last four years leads us to conclude that Healthcare Delivery Organizations (HDOs) must lead a nationwide call to action for interoperability of medical devices and systems. One way that HDOs can effect this change is by including medical device interoperability as an essential element in the procurement process and in vendor selection criteria. Signed: MGH, PHS, Hopkins, Kaiser October 2008 Download:
43 MD FIRE Recommendations: (from page 2) We strongly encourage HDOs to adopt medical device interoperability as an essential element of their procurement process. We have drafted sample medical device interoperability requirements and would encourage HDOs and vendors to use such requirements in their procurement process, including their requests for proposals (RFPs) and contracts. You can find the sample language attached as an Appendix to this document and available at We expect that the sample requirements and contracting language will evolve over time based on use. We believe that changing the way in which we procure medical devices to integrate requirements for interoperability will provide a way for us to ensure patient safety, improve healthcare quality, reduce healthcare costs, and provide for more comprehensive and secure management of health information 43
44 MD FIRE RFP Examples (MD FIRE pages 4-5) (section headings and excerpts) A. Request for Specific Functionality and Interoperability Capabilities Note: Requests a complete description of specific functionality and interoperability capabilities. The text shown is an example only, and should be greatly expanded by the HDO. This may be used if the HDO knows what interoperability capabilities it is seeking, what product functions support that interoperability, and which standards are to be implemented. B. Description of All Interoperability Capabilities and Related Functionality Note: Requests a complete description of the Product interoperability, but does not call for any particular function or standard. C. Description of Technology Supporting Interoperability Note: Requests a complete description of the Product technology. This should be used only if the Customer intends to evaluate the Product s technology and implementation D. Description of Vendor s Past Support for Interoperability Note: Requests a complete description of the vendor s corporate activities related to interoperability but not directly related to the Product itself. This should be used only if the Customer intends to evaluate vendors past commitment and contributions to interoperability. 44
45 MD FIRE: CONTRACT TERMS EXAMPLES (MD FIRE pages 6-8) (section headings and excerpts) Option 1: Complete Interoperability Note: The purpose of this section is to provide an example of terms for complete interoperability. Language in square brackets [this or that] should be selected as appropriate by the Healthcare Delivery Organization (referred to herein as Customer or HDO ). Option 2: Independent lab testing of interfaces Supplier agrees to have each interface tested and verified by an independent lab approved by Supplier and Customer. All costs from the Supplier and other third parties for independent lab testing and certification shall be listed separately [and paid by Supplier]. Supplier also agrees to obtain any applicable consortia certification for Product interfaces, including without limitation, USB, WiFi, ZigBee, Bluetooth, HL7 and Continua. Option 3: Connectivity by Clinical Domain Note: This section provides a means to add requirements by clinical domain. Customer should consider selecting a specific domain if needed. 45
46 MD FIRE: CONTRACT TERMS EXAMPLES pages (6-8) Option 4: Request for Conformance to Specific Standards Note: This section provides a means to add conformance to specific standards if not required by other sections. Option 5: Commitment to Work towards Interoperability Purpose: This section is to be used when the Supplier is expected to make a best effort to achieve interoperability, and at the same time to inform the Customer of any issues, barriers, or problems with the current set of standards. Option 6: Customer Requirements-Gathering Example This is a placeholder for the Customer to define its program/project timeline with respect to gathering requirements for interoperable interfaces. It is referenced in the Agreement terms 46
47 VHA PresentaMon on MD FIRE Presented March 18, 2009 to supply chain management via webinar (VHA Dallas studio) VHA serves more than 1,400 not for profit hospital and more than 21,000 non acute health care facilimes in 47 states and the District of Columbia. VHA's membership includes approximately 28 percent of the namon's community owned, not for profit hospitals. 140 hospitals connected to webinar
48 Financial ImplicaMons of Med Dev Interop Kaiser Permanente 2006 Analysis med device > EMR integramon costs with and without interop standards Analysis excludes safety and workflow benefits Results: standard interfaces would reduce integramon costs 30% Savings: $12M annually 48
49 Clinical Society Requirements We believe that intercommunicamon and interoperability of electronic medical devices could lead to important advances in pament safety and pament care, and that the standards and protocols to allow such seamless intercommunicamon should be developed fully with these advances in mind as of Nov 2008: Anesthesia Patient Safety Foundation Society for Technology in Anesthesia Society of American Gastrointestinal Endoscopic Surgeons World Federation of Societies of Anesthesiologists American Society of Anesthesiologists 49 Massachusetts Medical Society
50 Scope of ASTM ICE Part I From final draft, ASTM ICE part I This standard specifies general requirements for integramng equipment to create a Integrated Clinical Environment (ICE), as defined in 3.6. This standard specifies the characterismcs necessary for the safe integramon of medical devices and other equipment, via an electronic interface, from different manufacturers into a single medical system for the care of a single high acuity pament. This standard establishes requirements for a medical system that is intended to have greater error resistance and improved pament safety, treatment efficacy and workflow efficiency than can be achieved with independently used medical devices. 50
51 ICE Standard Integrated Clinical Environment ASTM F 2761 New medical device standard describes requirements for safe and effecmve plug and play integramon of devices in high acuity environments Developed by CIMIT/MGH MD PnP Program wrimng group convened under the authority of ASTM InternaMonal Commi7ee F29* First drah 2006 prepared for ISO/IEC ASTM version inimated 2007 PublicaMon expected April *ASTM F29.21 Devices in the Integrated Clinical Environment 51
52 Annex B Clinical context and clinical scenarios 1. Safety Interlock (PCA)* 2. SynchronizaMon with safety interlock (X ray venmlator synchronizamon)* 3. Process control/workflow (Heparin monitoring via PTT tesmng) 4. Smart alarm system (annunciate alarm when venmlator not re started aher cardiopulmonary bypass)* 5. Decision support (integrate bedside data and observamons to acmvate Rapid Response Team) 6. Physiological Closed Loop Control (armficial pancreas via intravenous infusions) 52 *Discussed today
53 DefiniMon 3.6 INTEGRATED CLINICAL ENVIRONMENT (ICE) An Integrated Clinical Environment is an environment where monitoring, treatment or diagnosis is performed on a single PATIENT, with interconnected medical devices and other equipment While many of the elements of a clinical environment exist in a bounded physical space containing the pament (e.g., an operamng room, intensive care unit, field hospital, ambulance, or other acute care environments), they need not all be within that physical space. Some of the operators, some pieces of equipment (e.g., control consoles), or databases can be located at remote locamons. An Integrated Clinical Environment is pament centric. As a pament moves among different venues (e.g., operamng room, ICU, emergency department, transport, home) the ICE moves with the pament; however some of the elements of the ICE can change. 53
54 ICE Part I Clinical Scenarios Listed in Annex B Six scenarios all high acuity care / documented preventable adverse events ICE based solumon pathway aligned with HHS Common Device ConnecMvity requirements 54
55 Functional Elements of the Integrated Clinical Environment Key 1 patient 2 medical device 3 Equipment 4 ice interface 5 ice network controller 6 data logger 7 ice supervisor 8 ice manager 9 operator (clinician) 10 ICE 11 external interface From ASTM Draft ICE Part I ICE can serve as a collaboration framework 55
56 The ICE supervisor supports the following capabilimes of the integrated clinical environment Provide safety interlocks Distribute integrated alarm condimons to relevant operators Provide context aware clinical decision support Set command input variables of other medical devices, per operatordefined, context appropriate rules in order to manage their operamon (e.g. change NIBP cycle interval) Assess the readiness of medical devices in a clinical environment to support specified funcmons or clinical workflow Perform integramon of alarm condimons from mulmple medical devices Perform automated record keeping Support integrated control* of devices Perform data reducmon with pointers for EMR Control of those features made available through the ICE interface (box #4) From draft ICE Part I 56
57 Functional Elements of the Integrated Clinical Environment Key 1 patient 2 medical device 3 Equipment 4 ice interface 5 ice network controller 6 data logger 7 ice supervisor 8 ice manager 9 operator (clinician) 10 ICE 11 external interface From draft ASTM ICE Part I Current draft: 57
58 The ICE network controller supports the following capabilimes of the integrated clinical environment Provide Plug and Play connecmvity with medical devices and other devices Interface with equipment that contains an ice equipment interface Provide data logs for forensic analysis (flight recorder) Perform network control funcmons independently of the underlying data communicamon mechanizamon Provide relevant informamon to support a healthcare equipment management system Also provides a common Mme base and binding of data to pament idenmty Also can provide and retrieve relevant clinical data to a healthcare informamon system/electronic medical record/electronic health record (HIS/EMR/EHR) From draft ICE Part I 58
59 Functional Elements of the Integrated Clinical Environment Key 1 patient 4 medical device 5 Equipment 6 ice interface 7 ice network controller 8 data logger 9 ice supervisor 10 ice manager 11 operator (clinician) 12 ICE 13 external interface From ASTM Draft ICE Part I ICE leaves many elements unspecified Can serve as a collaboration framework 59
60 The ICE supervisor supports the following pament centric capabilimes of the integrated clinical environment Provide safety interlocks Distribute integrated alarm condimons to relevant operators Provide context aware clinical decision support Set command input variables of other medical devices, per operatordefined, context appropriate rules in order to manage their operamon (e.g. change NIBP cycle interval) Assess the readiness of medical devices in a clinical environment to support specified funcmons or clinical workflow Perform integramon of alarm condimons from mulmple medical devices Perform automated record keeping Support integrated control* of devices Control of those features made available through the ICE interface (box #4) From draft ICE Part I 60
61 Functional Elements of the Integrated Clinical Environment Key 1 patient 4 medical device 5 Equipment 6 ice interface 7 ice network controller 8 data logger 9 ice supervisor 10 ice manager 11 operator (clinician) 12 ICE 13 external interface From draft ASTM ICE Part I Current draft: 61
62 The ICE network controller supports the following pament centric capabilimes of the integrated clinical environment Provide Plug and Play (PnP) connecmvity with medical devices and other devices Interface with equipment that contains an ice equipment interface Provide data logs for forensic analysis (flight recorder) Perform network control funcmons independently of the underlying data communicamon mechanizamon Provide relevant informamon to support a healthcare equipment management system Also provides a common Mme base and binding of data to pament idenmty Also can provide and retrieve relevant clinical data to a healthcare informamon system/electronic medical record/electronic health record (HIS/EMR/EHR) From draft ICE Part I 62
63 ICE in clinical data context MedicaMon List Lab Summary Historical Vitals Imaging Summary Summary of Medical History Discharge Summary Physician Notes Lab Results Imaging Results Historical PaMent Data Current Network Medical Data Monitoring of real Mme data subset Summarized Real Time Data (Flow Sheet) Clinical InformaMon System Order Data Image Data Lab Results Notes MedicaMon ReconciliaMon Admit Discharge Transfer Real Time Physiological Data In PaMent Historical Data Clinical ObservaMon Real Time Laboratory Environmental Data Alarms MedicaMon Data 63 63
64 Common Device ConnecMvity Drah AHIC Extension/Gap Dec 2008 C. The ability to communicate measurement information to the EHR for effective patient monitoring and management. D. The ability to uniquely identify a device and related components, communicate device setting and detailed device information associated with each measurement value, to the EHR. E. The ability to communicate and manage measurement intervals and device setting information within the EHR. F. The ability to query for additional device information captured by the device that may not have been communicated to the EHR. I. The ability to set and communicate limits and safeguards for device settings from the EHR to a device. 64
65 AdopMon of medical device interoperability (standards and technologies) will support: 1. Complete, accurate electronic medical records 2. Rapid deployment of devices in makeshih emergency care se{ngs 3. Clinical decision support systems and smart clinical alarms 4. Support of remote healthcare delivery 5. flight data recorder to facilitate adverse events analysis 6. Automated system readiness assessment (prior to starmng invasive clinical procedures or crimcal care transport) 7. Reduce cost of devices and their integramon, and reduce EMRadopMon costs 8. Closed loop control of therapeumc devices and safety interlocks (e.g. venmlamon, medicamon and fluid delivery) 9. Pathway for innovamve medical applicamons 65
66 Will we reach the Mpping point? Clinical Push (Societies) Hospital Demand (MD FIRE) Technology / Platform* Standards* Regulatory (FDA) interoperability Document Clinical Need / IOM Alignment with Federal HIT initiatives* * Greatest gaps 66 adoption
67 The MD PnP Vision Improve safety and efficiency by changing expectations; changing technology; changing healthcare
68 Contact info: MD PnP Program: Kurashiki, Japan 68
The anesthesiologist switches the patient from the ventilator to the cardiopulmonary
 Technology for surgery Integrating devices for patient safety The anesthesiologist switches the patient from the ventilator to the cardiopulmonary bypass machine but forgets to resume ventilation after
Technology for surgery Integrating devices for patient safety The anesthesiologist switches the patient from the ventilator to the cardiopulmonary bypass machine but forgets to resume ventilation after
Vision on Medical Device Plug and Play. Qixin Wang Assistant Professor, Dept. of Computing, The Hong Kong Polytechnic University June 21, 2009
 Vision on Medical Device Plug and Play Qixin Wang Assistant Professor, Dept. of Computing, The Hong Kong Polytechnic University Contents Demand Existing Efforts Vision and Roadmap 2 Contents Demand Existing
Vision on Medical Device Plug and Play Qixin Wang Assistant Professor, Dept. of Computing, The Hong Kong Polytechnic University Contents Demand Existing Efforts Vision and Roadmap 2 Contents Demand Existing
Medical devices are pervasive throughout modern
 Plug-and-Play for Medical Devices: Experiences from a Case Study David Arney, Sebastian Fischmeister, Julian M. Goldman, Insup Lee, Robert Trausmuth Medical devices are pervasive throughout modern healthcare,
Plug-and-Play for Medical Devices: Experiences from a Case Study David Arney, Sebastian Fischmeister, Julian M. Goldman, Insup Lee, Robert Trausmuth Medical devices are pervasive throughout modern healthcare,
Advanced Medical Technology Training and the APSF Recommendations: Perspectives from my Vantage Point
 Sept 16 2013 APSF, Phoenix, Az Advanced Medical Technology Training and the APSF Recommendations: Perspectives from my Vantage Point Julian M. Goldman, MD Member, APSF Committee on Technology (COT) Medical
Sept 16 2013 APSF, Phoenix, Az Advanced Medical Technology Training and the APSF Recommendations: Perspectives from my Vantage Point Julian M. Goldman, MD Member, APSF Committee on Technology (COT) Medical
Survey on ASA Standards and APSF Recommendations
 Physician-Patient Alliance for Health & Safety Improving Health & Safety Through Innovation and Awareness Survey on ASA Standards and APSF Recommendations Mike Wong Physician-Patient Alliance for Health
Physician-Patient Alliance for Health & Safety Improving Health & Safety Through Innovation and Awareness Survey on ASA Standards and APSF Recommendations Mike Wong Physician-Patient Alliance for Health
D Bringing you closer to your patients PATIENT MONITORING AND IT SOLUTIONS
 D-41011-2012 Bringing you closer to your patients PATIENT MONITORING AND IT SOLUTIONS 02 How can I D-41498-2012 spend more time with my patients? 03 D-40970-2012 D-40373-2012 D-41225-2012 Patient monitoring
D-41011-2012 Bringing you closer to your patients PATIENT MONITORING AND IT SOLUTIONS 02 How can I D-41498-2012 spend more time with my patients? 03 D-40970-2012 D-40373-2012 D-41225-2012 Patient monitoring
Masimo Patient SafetyNet
 Masimo Patient SafetyNet Remote Monitoring and Clinician Notification System When You Leave the Room, You ll Still Be There * The use of the trademark Patient SafetyNet is under license from University
Masimo Patient SafetyNet Remote Monitoring and Clinician Notification System When You Leave the Room, You ll Still Be There * The use of the trademark Patient SafetyNet is under license from University
STATEMENT. JEFFREY SHUREN, M.D., J.D. Director, Center for Devices and Radiological Health Food and Drug Administration
 STATEMENT JEFFREY SHUREN, M.D., J.D. Director, Center for Devices and Radiological Health Food and Drug Administration Institute of Medicine Committee on Patient Safety and Health Information Technology
STATEMENT JEFFREY SHUREN, M.D., J.D. Director, Center for Devices and Radiological Health Food and Drug Administration Institute of Medicine Committee on Patient Safety and Health Information Technology
RescueNet Dispatch, epcr, Care Exchange. HL7 v2. Ellkay LK EMR-Archive Smart on FHIR SAML Ellkay to Epic
 Use Case Title: Heart Attack Overview: Morgan is 40 years old and is experiencing chest pains. A 911 call is placed. Emergency Medical Services arrives and Morgan is evaluated. The decision comes down
Use Case Title: Heart Attack Overview: Morgan is 40 years old and is experiencing chest pains. A 911 call is placed. Emergency Medical Services arrives and Morgan is evaluated. The decision comes down
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Saving Lives In the Medical Surgical Unit and Establishing a Successful Capnography Monitoring Program For Patients Receiving Opioid Medications
 Saving Lives In the Medical Surgical Unit and Establishing a Successful Capnography Monitoring Program For Patients Receiving Opioid Medications March 14, 2016 AAMI Foundation Vision: To drive the safe
Saving Lives In the Medical Surgical Unit and Establishing a Successful Capnography Monitoring Program For Patients Receiving Opioid Medications March 14, 2016 AAMI Foundation Vision: To drive the safe
The Solution to Medical Device Security Also Could Save Tens of Thousands of Lives and Millions of Dollars
 The Solution to Medical Device Security Also Could Save Tens of Thousands of Lives and Millions of Dollars February 24, 2017 Evolver, Inc. The Solution to Medical Device Security Could Save Tens of Thousands
The Solution to Medical Device Security Also Could Save Tens of Thousands of Lives and Millions of Dollars February 24, 2017 Evolver, Inc. The Solution to Medical Device Security Could Save Tens of Thousands
Patient Safety and Interoperability: Are We There Yet?
 2006 HCC, Inc. CD000000-0000XX Patient Safety and Interoperability: Are We There Yet? David C Classen MD, MS Associate Professor of Medicine University of Utah and CMIO Pascal Metrics October 2, 2012 Slide
2006 HCC, Inc. CD000000-0000XX Patient Safety and Interoperability: Are We There Yet? David C Classen MD, MS Associate Professor of Medicine University of Utah and CMIO Pascal Metrics October 2, 2012 Slide
VENTILATION SERVO-U THE NEW POWER OF YOU
 VENTILATION SERVO-U THE NEW POWER OF YOU Critical Care SERVO-U 3 SERVO-U THE NEW POWER OF YOU SERVO-U delivers many effective options for protective ventilation. All of them more accessible, under standable
VENTILATION SERVO-U THE NEW POWER OF YOU Critical Care SERVO-U 3 SERVO-U THE NEW POWER OF YOU SERVO-U delivers many effective options for protective ventilation. All of them more accessible, under standable
QA offers significant economic benefits!
 and Safety Systems in the USA J. Tobey Clark, MSEE, CCE, SASHE University of Vermont, USA Definitions Quality assurance Planned and systematic actions that can be demonstrated to provide confidence that
and Safety Systems in the USA J. Tobey Clark, MSEE, CCE, SASHE University of Vermont, USA Definitions Quality assurance Planned and systematic actions that can be demonstrated to provide confidence that
Optum Anesthesia. Completely integrated anesthesia information management system
 Optum Anesthesia Completely integrated anesthesia information management system 2 Completely integrated anesthesia information management system Optum Anesthesia Information Management System (AIMS) helps
Optum Anesthesia Completely integrated anesthesia information management system 2 Completely integrated anesthesia information management system Optum Anesthesia Information Management System (AIMS) helps
GE Healthcare. B40 Patient Monitor Connecting intelligence and care
 GE Healthcare B40 Patient Monitor Connecting intelligence and care Simple. The B40 Monitor provides versatile clinical capabilities to help you monitor a wide range of patients. From ambulatory surgery
GE Healthcare B40 Patient Monitor Connecting intelligence and care Simple. The B40 Monitor provides versatile clinical capabilities to help you monitor a wide range of patients. From ambulatory surgery
National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI)
 October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
Keep watch and intervene early
 IntelliVue GuardianSoftware solution Keep watch and intervene early The earlier, the better Intervene early, by recognizing subtle signs Clinical realities on the general floor and in the emergency department
IntelliVue GuardianSoftware solution Keep watch and intervene early The earlier, the better Intervene early, by recognizing subtle signs Clinical realities on the general floor and in the emergency department
IMPROVING EFFICIENCY AND COST SAVINGS. Technology Solutions for NHS Hospitals
 SM IMPROVING EFFICIENCY AND COST SAVINGS Technology Solutions for NHS Hospitals IMPROVING EFFICIENCY IN A CHANGING HEALTHCARE TECHNOLOGY ENVIRONMENT NHS hospitals and their managing trusts are challenged
SM IMPROVING EFFICIENCY AND COST SAVINGS Technology Solutions for NHS Hospitals IMPROVING EFFICIENCY IN A CHANGING HEALTHCARE TECHNOLOGY ENVIRONMENT NHS hospitals and their managing trusts are challenged
ENVIRONMENT Preoperative evaluation clinic, Preoperative holding area. Preoperative evaluation clinic, Postoperative care unit, Operating room
 Goals and Objectives, Main Operating Room Anesthesia, VAMC, CA-3 year UCSD DEPARTMENT OF ANESTHESIOLOGY OPERATING ROOM CLINICAL ANESTHESIA AT VAMC GOALS AND OBJECTIVES, CA-3 YEAR PATIENT CARE: To provide
Goals and Objectives, Main Operating Room Anesthesia, VAMC, CA-3 year UCSD DEPARTMENT OF ANESTHESIOLOGY OPERATING ROOM CLINICAL ANESTHESIA AT VAMC GOALS AND OBJECTIVES, CA-3 YEAR PATIENT CARE: To provide
Using CAST for Adverse Event Investigation in Hospitals
 Using CAST for Adverse Event Investigation in Hospitals Meaghan O Neil March 27, 2014 Motivation As many as 98,000 people, die in hospitals each year as a result of medical errors that could have been
Using CAST for Adverse Event Investigation in Hospitals Meaghan O Neil March 27, 2014 Motivation As many as 98,000 people, die in hospitals each year as a result of medical errors that could have been
Acute Care Workflow Solutions
 Acute Care Workflow Solutions 2016 North American General Acute Care Workflow Solutions Product Leadership Award The Philips IntelliVue Guardian solution provides general floor, medical-surgical units,
Acute Care Workflow Solutions 2016 North American General Acute Care Workflow Solutions Product Leadership Award The Philips IntelliVue Guardian solution provides general floor, medical-surgical units,
Feedback from Anesthesia clinicians. 2.1 Intubate Patient Workflow
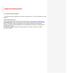 Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Alaris Products. Protecting patients at the point of care
 Alaris Products Protecting patients at the point of care Overview The medication process is the largest source of medical errors 1 with medication errors costing an estimated $3.5 billion yearly in hospitals.
Alaris Products Protecting patients at the point of care Overview The medication process is the largest source of medical errors 1 with medication errors costing an estimated $3.5 billion yearly in hospitals.
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
SURVEYOR CENTRAL MONITORING SYSTEM
 SURVEYOR CENTRAL MONITORING SYSTEM how logical... Patient Monitors from a Company Dedicated to the Science of ECG It s really quite simple when it comes to patient monitors. It s all about your patient.
SURVEYOR CENTRAL MONITORING SYSTEM how logical... Patient Monitors from a Company Dedicated to the Science of ECG It s really quite simple when it comes to patient monitors. It s all about your patient.
AirStrip ONE Cardiology
 AirStrip ONE Cardiology A Synchronized View of the Vital Patient Data Needed to Improve Care Heart disease is the leading cause of death in the U.S. The associated costs exceed $100 billion annually. AirStrip
AirStrip ONE Cardiology A Synchronized View of the Vital Patient Data Needed to Improve Care Heart disease is the leading cause of death in the U.S. The associated costs exceed $100 billion annually. AirStrip
You ll love the Vue. Philips IntelliVue Information Center ix
 You ll love the Vue Philips IntelliVue Information Center ix IT Director It has to fit into our IT infrastructure and integrate easily with our EMR and HIS. Clinical Engineering Make it easy to support.
You ll love the Vue Philips IntelliVue Information Center ix IT Director It has to fit into our IT infrastructure and integrate easily with our EMR and HIS. Clinical Engineering Make it easy to support.
EMR Surveillance Intervenes to Reduce Risk Adjusted Mortality March 2, 2016 Katherine Walsh, MS, DrPH, RN, NEA-BC Vice President of Operations,
 EMR Surveillance Intervenes to Reduce Risk Adjusted Mortality March 2, 2016 Katherine Walsh, MS, DrPH, RN, NEA-BC Vice President of Operations, Houston Methodist Hospital Michael Rothman, PhD, Chief Science
EMR Surveillance Intervenes to Reduce Risk Adjusted Mortality March 2, 2016 Katherine Walsh, MS, DrPH, RN, NEA-BC Vice President of Operations, Houston Methodist Hospital Michael Rothman, PhD, Chief Science
APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that apply)
 POLICY NAME: ANESTHESIA PAYMENT POLICY POLICY NUMBER: ISSUING DEPT.: Claims EFFECTIVE DATE: 9/25/2017 APPROVED BY: APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that
POLICY NAME: ANESTHESIA PAYMENT POLICY POLICY NUMBER: ISSUING DEPT.: Claims EFFECTIVE DATE: 9/25/2017 APPROVED BY: APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that
EMS Subspecialty Certification Review Course. Learning Objectives. Scope of Practice
 EMS Subspecialty Certification Review Course 2.3.1 Scope of Practice Models 2.3.1.1 Military/federal government medical personnel 2.3.1.2 State vs. national scope of practice model 2.3.1.2.1 Levels of
EMS Subspecialty Certification Review Course 2.3.1 Scope of Practice Models 2.3.1.1 Military/federal government medical personnel 2.3.1.2 State vs. national scope of practice model 2.3.1.2.1 Levels of
Surgery Road Map. General practices. Road map sections
 Surgery Road Map MHA s road maps provide hospitals and health systems with evidence-based recommendations and standards for the development of topic-specific prevention and quality improvement programs,
Surgery Road Map MHA s road maps provide hospitals and health systems with evidence-based recommendations and standards for the development of topic-specific prevention and quality improvement programs,
CDRL A006 Training Manual User's Guide for STAT! TM EMEDS ICU Serious Medical Game. Release v November 26, 2014
 CDRL A006 Training Manual User's Guide for STAT! TM EMEDS ICU Serious Medical Game Copyright 2014 Vcom3D, Inc. Release v1.0.0 - November 26, 2014 Sponsored by Air Force Research Laboratory (AFRL) Prepared
CDRL A006 Training Manual User's Guide for STAT! TM EMEDS ICU Serious Medical Game Copyright 2014 Vcom3D, Inc. Release v1.0.0 - November 26, 2014 Sponsored by Air Force Research Laboratory (AFRL) Prepared
Rethinking Telemetry and Its Impact on Healthcare. Wireless technology that improves care and reduces costs
 Rethinking Telemetry and Its Impact on Healthcare Wireless technology that improves care and reduces costs Thinking differently about telemetry. You know it better than anyone the challenge of improving
Rethinking Telemetry and Its Impact on Healthcare Wireless technology that improves care and reduces costs Thinking differently about telemetry. You know it better than anyone the challenge of improving
APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER
 APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER We are carrying out a survey to establish the quality of anaesthesia care provided to Obstetric patients in East Africa. We therefore
APPENDIX I QUESTIONNAIRE FOR INTERVIEWING THE ANAESTHESIA PROVIDER We are carrying out a survey to establish the quality of anaesthesia care provided to Obstetric patients in East Africa. We therefore
Guidance for Medication Reconciliation and System Integration Process
 Guidance for Medication Reconciliation and System Integration Process Identifying points of failure within the medication reconciliation process and determining systematic approaches (via health IT) to
Guidance for Medication Reconciliation and System Integration Process Identifying points of failure within the medication reconciliation process and determining systematic approaches (via health IT) to
Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society
 Can J Anesth/J Can Anesth (2018) Appendix 5 Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society Background Medical and surgical care has become
Can J Anesth/J Can Anesth (2018) Appendix 5 Position Paper on Anesthesia Assistants: An Official Position Paper of the Canadian Anesthesiologists Society Background Medical and surgical care has become
"Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics"
 "Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics" Healthcare Transformation Services Lisa Pahl, MSN, Principal, Practice Lead Alarm Management May, 2017 Data,
"Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics" Healthcare Transformation Services Lisa Pahl, MSN, Principal, Practice Lead Alarm Management May, 2017 Data,
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
The Ohio State University Department of Orthopaedics. Residency Curriculum. PGY1 Rotations
 The Ohio State University Department of Orthopaedics Residency Curriculum PGY1 Rotations Goals and Objectives Anesthesiology Rotation PGY1 Level I. Core Competency Areas By the end of the PGY1 rotation
The Ohio State University Department of Orthopaedics Residency Curriculum PGY1 Rotations Goals and Objectives Anesthesiology Rotation PGY1 Level I. Core Competency Areas By the end of the PGY1 rotation
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Anesthesia
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Anesthesia 1. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Anesthesia 1. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation.
STATEMENT ON GRANTING PRIVILEGES FOR ADMINISTRATION OF MODERATE SEDATION TO PRACTITIONERS WHO ARE NOT ANESTHESIA PROFESSIONALS
 NOT ANESTHESIA PROFESSIONALS (Approved by the ASA House of Delegates on October 25, 2005, and amended on October 18, 2006) Outcome Indicators for Office-Based and Ambulatory Surgery (ASA Committee on Ambulatory
NOT ANESTHESIA PROFESSIONALS (Approved by the ASA House of Delegates on October 25, 2005, and amended on October 18, 2006) Outcome Indicators for Office-Based and Ambulatory Surgery (ASA Committee on Ambulatory
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
The residents will work at WVU Ruby Memorial under the supervision of departmental faculty.
 CA-2 Intermediate Clinical Training (ICT) Curriculum Department of Anesthesiology Description of Rotation The goal of this multi-month rotation is to build upon the essential skills learned in the BCT
CA-2 Intermediate Clinical Training (ICT) Curriculum Department of Anesthesiology Description of Rotation The goal of this multi-month rotation is to build upon the essential skills learned in the BCT
Recognising a Deteriorating Patient. Study guide
 Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
GE integrates with ELLKAY; GE integrates with Cerner HIE; GE Media Manager IHE PDQ, IHE XDS, HL7 CDA. ELLKAY LKeMPI IHE PDQ
 Use Case Title: Battlefield to Bedside Overview: Shane is injured in combat, is triaged and treated at an Army field hospital unit, and eventually discharged to return home. Some time later he has follow
Use Case Title: Battlefield to Bedside Overview: Shane is injured in combat, is triaged and treated at an Army field hospital unit, and eventually discharged to return home. Some time later he has follow
EMERGING TRENDS WHAT I WILL COVER INCREASED INTEREST DEVICES ARE MIGRATING SAFE AND RELIABLE DEVICES LEAD TO LIVING WELL
 SAFE AND RELIABLE DEVICES LEAD TO LIVING WELL THE HOME AND MEDICAL DEVICE TECHNOLOGY Presented by Mary Weick-Brady, MSN, RN April 20, 2012 Great Lakes Biomedical Conference on Home and Mobile Health WHAT
SAFE AND RELIABLE DEVICES LEAD TO LIVING WELL THE HOME AND MEDICAL DEVICE TECHNOLOGY Presented by Mary Weick-Brady, MSN, RN April 20, 2012 Great Lakes Biomedical Conference on Home and Mobile Health WHAT
At your side in intensive care
 D-18925-2010 At your side in intensive care 2 Providing quality care in this stressful environment is anything but easy. * Technology at its best Today s ICU technology faces incredible pressure to perform.
D-18925-2010 At your side in intensive care 2 Providing quality care in this stressful environment is anything but easy. * Technology at its best Today s ICU technology faces incredible pressure to perform.
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES
 UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY
 POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center
 Engaging the team: Steps to Reduce Complications Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center Safety
Engaging the team: Steps to Reduce Complications Susan Moffatt-Bruce, MD, PhD Chief Quality and Patient Safety Officer Associate Professor of Surgery The Ohio State University s Wexner Medical Center Safety
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #427: Post-Anesthetic Transfer of Care: Use of Checklist or Protocol for Direct Transfer of Care from Procedure Room to Intensive Care Unit (ICU) National Quality Strategy Domain: Communication
Quality ID #427: Post-Anesthetic Transfer of Care: Use of Checklist or Protocol for Direct Transfer of Care from Procedure Room to Intensive Care Unit (ICU) National Quality Strategy Domain: Communication
ISANSYS LIFECARE LTD CLOUD COMPUTING TECHNOLOGY TO MONITOR PATIENTS VITAL SIGNS
 MONITOR PATIENTS VITAL SIGNS 34 KEY DATA: FACT FILE Technology Vital signs monitoring Established 2010 Type Start up Location Milton, Oxford Employees 14 CEO and Co-Founder Dr Keith Errey A serial entrepreneur,
MONITOR PATIENTS VITAL SIGNS 34 KEY DATA: FACT FILE Technology Vital signs monitoring Established 2010 Type Start up Location Milton, Oxford Employees 14 CEO and Co-Founder Dr Keith Errey A serial entrepreneur,
Healthcare without Bounds: Trends in Clinical Surveillance and Analytics 2018
 Trends in Clinical Surveillance and Analytics 2018 1 of 6 Healthcare without Bounds: Trends in Clinical Surveillance and Analytics 2018 TITLE: Trends in Clinical Surveillance and Analytics 2018 AUTHOR:
Trends in Clinical Surveillance and Analytics 2018 1 of 6 Healthcare without Bounds: Trends in Clinical Surveillance and Analytics 2018 TITLE: Trends in Clinical Surveillance and Analytics 2018 AUTHOR:
Integrated Nurse Call Solutions
 Integrated Nurse Call Solutions INTEGRATED NURSE CALL SOLUTIONS Making Your Work Day Easier Streamlined Workflows Tools for Improving Patient Satisfaction and Safety Wireless Communications Connects Patients
Integrated Nurse Call Solutions INTEGRATED NURSE CALL SOLUTIONS Making Your Work Day Easier Streamlined Workflows Tools for Improving Patient Satisfaction and Safety Wireless Communications Connects Patients
CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology
 CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology Description of Rotation or Educational Experience This rotation is a continuation of the CA-2 Cardiothoracic
CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology Description of Rotation or Educational Experience This rotation is a continuation of the CA-2 Cardiothoracic
A Centralized Monitoring Approach to Pulse Oximetry for Patients on Opioids
 A Centralized Monitoring Approach to Pulse Oximetry for Patients on Opioids Phyllis J. Miller About the Author Phyllis J. Miller, MS, RN, FHCE, is an independent nursing consultant. At the time this article
A Centralized Monitoring Approach to Pulse Oximetry for Patients on Opioids Phyllis J. Miller About the Author Phyllis J. Miller, MS, RN, FHCE, is an independent nursing consultant. At the time this article
Simulation Design Template
 Simulation Design Template Date: May 7/8, 2008 File Name: Discipline: RN, Charge nurse, medical radiology, pharmacy tech, social work, medicine (whatever is available at the institution) Student Level:
Simulation Design Template Date: May 7/8, 2008 File Name: Discipline: RN, Charge nurse, medical radiology, pharmacy tech, social work, medicine (whatever is available at the institution) Student Level:
Component Description Unit Topics 1. Introduction to Healthcare and Public Health in the U.S. 2. The Culture of Healthcare
 Component Description (Each certification track is tailored for the exam and will only include certain components and units and you can find these on your suggested schedules) 1. Introduction to Healthcare
Component Description (Each certification track is tailored for the exam and will only include certain components and units and you can find these on your suggested schedules) 1. Introduction to Healthcare
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #426: Post-Anesthetic Transfer of Care Measure: Procedure Room to a Post Anesthesia Care Unit (PACU) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL
Quality ID #426: Post-Anesthetic Transfer of Care Measure: Procedure Room to a Post Anesthesia Care Unit (PACU) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL
Improving the Safe Use of Multiple IV Infusions
 QUICK GUIDE Improving the Safe Use of Multiple IV Infusions The AAMI Foundation is grateful to its collaborating partners in the National Coalition for Infusion Therapy Safety: Acknowledgements The AAMI
QUICK GUIDE Improving the Safe Use of Multiple IV Infusions The AAMI Foundation is grateful to its collaborating partners in the National Coalition for Infusion Therapy Safety: Acknowledgements The AAMI
Patient Safety Course Descriptions
 Adverse Events Antibiotic Resistance This course will teach you how to deal with adverse events at your facility. You will learn: What incidents are, and how to respond to them. What sentinel events are,
Adverse Events Antibiotic Resistance This course will teach you how to deal with adverse events at your facility. You will learn: What incidents are, and how to respond to them. What sentinel events are,
How Pharmacy Informatics and Technology are Evolving to Improve Patient Care
 How Pharmacy Informatics and Technology are Evolving to Improve Patient Care HealthcareIS.com 2 Table of Contents 3 Impact of Emerging Technologies 3 CPOE 5 Automated Dispensing Machines 6 Barcode Medication
How Pharmacy Informatics and Technology are Evolving to Improve Patient Care HealthcareIS.com 2 Table of Contents 3 Impact of Emerging Technologies 3 CPOE 5 Automated Dispensing Machines 6 Barcode Medication
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC
 Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
UNDERSTANDING THE CONTENT OUTLINE/CLASSIFICATION SYSTEM
 BOARD OF PHARMACY SPECIALTIES CRITICAL CARE PHARMACY SPECIALIST CERTIFICATION CONTENT OUTLINE/CLASSIFICATION SYSTEM FINALIZED SEPTEMBER 2017/FOR USE ON FALL 2018 EXAMINATION AND FORWARD UNDERSTANDING THE
BOARD OF PHARMACY SPECIALTIES CRITICAL CARE PHARMACY SPECIALIST CERTIFICATION CONTENT OUTLINE/CLASSIFICATION SYSTEM FINALIZED SEPTEMBER 2017/FOR USE ON FALL 2018 EXAMINATION AND FORWARD UNDERSTANDING THE
Digitizing healthcare Digital Innovation Forum Henk van Houten Chief Technology Officer, Philips
 Digitizing healthcare Digital Innovation Forum 2017 Henk van Houten Chief Technology Officer, Philips Digitization is transforming every industry The digital revolution: how photography evolved Mechanization
Digitizing healthcare Digital Innovation Forum 2017 Henk van Houten Chief Technology Officer, Philips Digitization is transforming every industry The digital revolution: how photography evolved Mechanization
HL7 v2 IEEE and DoseLink. HIMSS Interoperability Showcase Page 1 of 11
 Use Case Title: Cardiovascular Diabetes Risk Overview: Francine, a 65-year-old, has diabetes is exhibiting cardiovascular risks for which she needs immediate observation monitoring. She is eventually put
Use Case Title: Cardiovascular Diabetes Risk Overview: Francine, a 65-year-old, has diabetes is exhibiting cardiovascular risks for which she needs immediate observation monitoring. She is eventually put
The History of Emergency Medicine in Rwanda
 The History of Emergency Medicine in Rwanda Laura Janneck, MD, MPH sidharte Rwanda Country Director Emergency Medicine in the Tropics Kigali, Rwanda August 22, 2016 From the beginning 1952- Maurice Ellis
The History of Emergency Medicine in Rwanda Laura Janneck, MD, MPH sidharte Rwanda Country Director Emergency Medicine in the Tropics Kigali, Rwanda August 22, 2016 From the beginning 1952- Maurice Ellis
Safety Innovations FOUNDATIONHTSI. Healthcare Alarm Safety What We Can Learn From Military Alarm Management Strategies
 FOUNDATIONHTSI Healthcare Technology Safety Institute Safety Innovations Healthcare Alarm Safety What We Can Learn From Military Alarm Management Strategies Lockheed Martin (LM) Advanced Technology Laboratories
FOUNDATIONHTSI Healthcare Technology Safety Institute Safety Innovations Healthcare Alarm Safety What We Can Learn From Military Alarm Management Strategies Lockheed Martin (LM) Advanced Technology Laboratories
making technology talk
 REPRINT May 2016 Ed Cantwell Kerry McDermott healthcare financial management association hfma.org making technology talk how interoperability can improve care, drive efficiency, and reduce waste The abundance
REPRINT May 2016 Ed Cantwell Kerry McDermott healthcare financial management association hfma.org making technology talk how interoperability can improve care, drive efficiency, and reduce waste The abundance
at OU Medicine Leadership Development Institute August 6, 2010
 Effective Patient Handovers at OU Medicine Leadership Development Institute August 6, 2010 Quality and Patient Safety Realize OU Medicine s position with respect to a culture of safety and quality. Improve
Effective Patient Handovers at OU Medicine Leadership Development Institute August 6, 2010 Quality and Patient Safety Realize OU Medicine s position with respect to a culture of safety and quality. Improve
Digistat Patient Watch
 Digistat Patient Watch The patient bedside at your fingertips gehealthcare.com The patient bedside at your fingertips Quality care depends on relevant patient information, sent to the right caregiver,
Digistat Patient Watch The patient bedside at your fingertips gehealthcare.com The patient bedside at your fingertips Quality care depends on relevant patient information, sent to the right caregiver,
Continuity of Care Record (CCR)
 Continuity of Care Record (CCR) William R. Braithwaite, MD, PhD Treasurer, HL7 Board of Directors Member, CCR Steering Committee www.hl7.org CCR Sponsors ASTM International Voluntary consensus standards
Continuity of Care Record (CCR) William R. Braithwaite, MD, PhD Treasurer, HL7 Board of Directors Member, CCR Steering Committee www.hl7.org CCR Sponsors ASTM International Voluntary consensus standards
OHTAC Recommendation. Implementation and Use of Smart Medication Delivery Systems
 OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
OHTAC Recommendation Implementation and Use of Smart Medication Delivery Systems July 2009 Background The Ontario Health Technology Advisory Committee (OHTAC) engaged the University Health Network s (UHN)
Smart Personal Health. the state of the art. Chris Johnson Berlin, September 2010
 1 Smart Personal Health Interoperability of personal health systems the state of the art Chris Johnson www.chrisjohnson.nl Berlin, September 2010 2 About your presenter Vice President Cypak since 2007:
1 Smart Personal Health Interoperability of personal health systems the state of the art Chris Johnson www.chrisjohnson.nl Berlin, September 2010 2 About your presenter Vice President Cypak since 2007:
Commission on Accreditation of Allied Health Education Programs
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 Commission on Accreditation of Allied Health
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 Commission on Accreditation of Allied Health
Chuck Campbell, SES, Military Health System Chief Information Officer. Using Service Oriented Architecture to Support Meaningful Use
 Chuck Campbell, SES, Military Health System Chief Information Officer Using Service Oriented Architecture to Support Meaningful Use 07/14/10 0 Agenda Military Health System (MHS) Military s Electronic
Chuck Campbell, SES, Military Health System Chief Information Officer Using Service Oriented Architecture to Support Meaningful Use 07/14/10 0 Agenda Military Health System (MHS) Military s Electronic
Quality Improvement in the ICU: A Way Forward
 Quality Improvement in the ICU: A Way Forward Ognjen Gajic M.D. Mayo Clinic Rochester MN, USA Multidisciplinary Epidemiology and Translational Research in Intensive Care, Emergency and Perioperative Medicine
Quality Improvement in the ICU: A Way Forward Ognjen Gajic M.D. Mayo Clinic Rochester MN, USA Multidisciplinary Epidemiology and Translational Research in Intensive Care, Emergency and Perioperative Medicine
Nurse Call System. A Voice over IP Based Solution for Streamlined Communication, Alerting and Workflow
 790 Nurse Call System A Voice over IP Based Solution for Streamlined Communication, Alerting and Workflow 790 Focused on Patient The needs of patients are increasingly complex which places even greater
790 Nurse Call System A Voice over IP Based Solution for Streamlined Communication, Alerting and Workflow 790 Focused on Patient The needs of patients are increasingly complex which places even greater
Department of Anesthesiology Anesthesia Curriculum Clinical Base Year
 Anesthesia Curriculum Clinical Base Year Description of Rotation The goal of this month long rotation is to teach the basic skills of anesthesia and to provide a foundation on which to build the initial
Anesthesia Curriculum Clinical Base Year Description of Rotation The goal of this month long rotation is to teach the basic skills of anesthesia and to provide a foundation on which to build the initial
Alabama Trauma Center Designation Criteria
 2 Alabama Trauma Center Designation Criteria Office of Emergency Medical Services Master Checklist Alabama Trauma Center Designation Trauma Center Criteria: APPENDIX A Trauma Rules The following table
2 Alabama Trauma Center Designation Criteria Office of Emergency Medical Services Master Checklist Alabama Trauma Center Designation Trauma Center Criteria: APPENDIX A Trauma Rules The following table
GENERAL PROGRAM GOALS AND OBJECTIVES
 BENJAMIN ATWATER RESIDENCY TRAINING PROGRAM DIRECTOR UCSD MEDICAL CENTER DEPARTMENT OF ANESTHESIOLOGY 200 WEST ARBOR DRIVE SAN DIEGO, CA 92103-8770 PHONE: (619) 543-5297 FAX: (619) 543-6476 Resident Orientation
BENJAMIN ATWATER RESIDENCY TRAINING PROGRAM DIRECTOR UCSD MEDICAL CENTER DEPARTMENT OF ANESTHESIOLOGY 200 WEST ARBOR DRIVE SAN DIEGO, CA 92103-8770 PHONE: (619) 543-5297 FAX: (619) 543-6476 Resident Orientation
SPOK MESSENGER. Improving Staff Efficiency and Patient Care With Timely Communications and Critical Connectivity
 SM SPOK MESSENGER Improving Staff Efficiency and Patient Care With Timely Communications and Critical Connectivity THE CHALLENGE OF PROVIDING PATIENT CARE WHILE MAINTAINING EFFICIENCY Many hospitals today
SM SPOK MESSENGER Improving Staff Efficiency and Patient Care With Timely Communications and Critical Connectivity THE CHALLENGE OF PROVIDING PATIENT CARE WHILE MAINTAINING EFFICIENCY Many hospitals today
Ontario Shores Journey to EMRAM Stage 7. October 21, 2015
 Ontario Shores Journey to EMRAM Stage 7 October 21, 2015 ICE BREAKER Agenda System overview & pervasiveness of use Review Clinical Practice Guideline implementation Discuss Patient Portal implementation
Ontario Shores Journey to EMRAM Stage 7 October 21, 2015 ICE BREAKER Agenda System overview & pervasiveness of use Review Clinical Practice Guideline implementation Discuss Patient Portal implementation
Monitoring in ICU. BR Bhengu UKZN
 Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
IV-EHR Interoperability
 IV-EHR Interoperability Some Things Work Better Together Your smart pumps help enhance safety through guidance at the bedside. Your barcode system, connected to electronic health records (EHR), electronically
IV-EHR Interoperability Some Things Work Better Together Your smart pumps help enhance safety through guidance at the bedside. Your barcode system, connected to electronic health records (EHR), electronically
Mobile Communications
 Mobile Communications Speakers Brett Moran, MD, BCIM, BCCI Associate Chief Medical Officer and CMIO About me Former Professor of Internal Medicine where he practiced academic medicine at UTSW for 19 years
Mobile Communications Speakers Brett Moran, MD, BCIM, BCCI Associate Chief Medical Officer and CMIO About me Former Professor of Internal Medicine where he practiced academic medicine at UTSW for 19 years
D Pure possibilities. Dräger perseus A500
 D-91730-2013 Pure possibilities Dräger perseus A500 02 How about more workspace? D-91310-2013 D-91554-2013 Great expectations Today s perioperative environment presents new challenges. As caseloads increase
D-91730-2013 Pure possibilities Dräger perseus A500 02 How about more workspace? D-91310-2013 D-91554-2013 Great expectations Today s perioperative environment presents new challenges. As caseloads increase
Bridging the Gap Between Clinicians and HTM Staff
 Bridging the Gap Between Clinicians and HTM Staff James H. Philip MEE MD CCE, Professor of Anaesthesia, Harvard Medical School, Anesthesiologist and Medical Liaison for Anesthesia, Department of Biomedical
Bridging the Gap Between Clinicians and HTM Staff James H. Philip MEE MD CCE, Professor of Anaesthesia, Harvard Medical School, Anesthesiologist and Medical Liaison for Anesthesia, Department of Biomedical
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
HL7 v2 IEEE OBIX Perinatal Data System
 Use Case Title: Labor and Delivery Overview: Ariana, a 40-year-old, is pregnant. She has a history of arrhythmia so hers is a high-risk pregnancy. She arrives at the hospital for delivery ahead of her
Use Case Title: Labor and Delivery Overview: Ariana, a 40-year-old, is pregnant. She has a history of arrhythmia so hers is a high-risk pregnancy. She arrives at the hospital for delivery ahead of her
For some years, the automation of hospital administrative
 An Introduction to IEC 80001: Aiming for Patient Safety in the Networked Healthcare Environment Sherman Eagles Editor s note: At press time, the second draft of IEC/CD2 80001, Application of risk management
An Introduction to IEC 80001: Aiming for Patient Safety in the Networked Healthcare Environment Sherman Eagles Editor s note: At press time, the second draft of IEC/CD2 80001, Application of risk management
Profiles in CSP Insourcing: Tufts Medical Center
 Profiles in CSP Insourcing: Tufts Medical Center Melissa A. Ortega, Pharm.D., M.S. Director, Pediatrics and Inpatient Pharmacy Operations Tufts Medical Center Hospital Profile Tufts Medical Center (TMC)
Profiles in CSP Insourcing: Tufts Medical Center Melissa A. Ortega, Pharm.D., M.S. Director, Pediatrics and Inpatient Pharmacy Operations Tufts Medical Center Hospital Profile Tufts Medical Center (TMC)
General OR-Stanford-CA-1 revised: Tuesday, February 02, 2016
 Stanford University Anesthesiology Residency Program Rotation specific goals and objectives for residents Core Curriculum for PGY 1 Surgery Residents on the Anesthesia Rotation Description: The General
Stanford University Anesthesiology Residency Program Rotation specific goals and objectives for residents Core Curriculum for PGY 1 Surgery Residents on the Anesthesia Rotation Description: The General
Using Telemedicine to Enhance Meaningful Use Qualification
 Beth DeStasio Director, Regulatory Affairs & Strategy, REACH Health September 2014 Copyright 2014 REACH Health, Inc. All rights Reserved Key Takeaways 1. As of September 4, 2014, the Center for Medicare
Beth DeStasio Director, Regulatory Affairs & Strategy, REACH Health September 2014 Copyright 2014 REACH Health, Inc. All rights Reserved Key Takeaways 1. As of September 4, 2014, the Center for Medicare
Utah DOH (CDC) Michigan DHHS (CDC) EDEN EDRS. IHE VRDR: QRPH-47 (FHIR), QRPH 38 JDI ( HL7 v2.6) HIMSS Interoperability Showcase 2018
 Use Case Title: Reporting Overview: 11-month-old Ravi is diagnosed with Pertussis, a reportable condition. An initial Case Report is triggered, evaluated for reportability and sent to public health. health
Use Case Title: Reporting Overview: 11-month-old Ravi is diagnosed with Pertussis, a reportable condition. An initial Case Report is triggered, evaluated for reportability and sent to public health. health
EDEN EDRS. Utah DOH (CDC) Michigan DHHS (CDC) IHE VRDR: QRPH-47 (FHIR), QRPH 38 JDI ( HL7 v2.6)
 Use Case Title: Reporting Overview: 11-month-old Ravi is diagnosed with Pertussis, a reportable condition. An initial Case Report is triggered, evaluated for reportability and sent to public health. health
Use Case Title: Reporting Overview: 11-month-old Ravi is diagnosed with Pertussis, a reportable condition. An initial Case Report is triggered, evaluated for reportability and sent to public health. health
Plum 360 TM Infusion System with Full IV-EHR Interoperability
 Plum 360 TM Infusion System with Full IV-EHR Interoperability Your Direct Connection To Clinical Excellence > Air management that doesn t require disconnecting from the patient > A secondary line that
Plum 360 TM Infusion System with Full IV-EHR Interoperability Your Direct Connection To Clinical Excellence > Air management that doesn t require disconnecting from the patient > A secondary line that
Preventing Medical Errors
 Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
