Policy on Correct Site Surgery Policy and Procedures for Pre-operative Marking. (Local Safety Standards for Invasive Procedures)
|
|
|
- Neal Barnett
- 6 years ago
- Views:
Transcription
1 Policy on Correct Site Surgery Policy and Procedures for Pre-operative Marking (Local Safety Standards for Invasive Procedures)
2 Policy Title: Executive Summary: Supersedes: Description of Amendment(s): Policy on Correct Site Surgery/ LocSSIPs This policy/ standard provides guidance to all staff responsible for preoperative skin site marking. Supersedes Version 3 to reflect changes in practice, surgical checklists and review of the National Safety Standards for Invasive Procedures (NATSSIPs) Supersedes Version 3 to reflect recommendations in National Safety Standards for Invasive Procedures (NATSSIPs) and updated surgical safety checklist This policy will impact on: Patients Any Clinician or Practitioner responsible for correct site marking prior to surgical procedures Clinicians and Practitioners working within the Radiology Department where specialist preoperative marking may be required Financial Implications: Limited financial impact. Policy Area: Trust Wide Document Reference: ECT Version Number: 4:0 Effective Date: July 2017 Issued By: Mike Cawley Theatre Manager Review Date: Jan 2020 Author: (Full Job title ) Mike Cawley Theatre Manager Janet Hatton Theatre Practice Development Nurse Sam Leonard Matron surgery Impact Assessment Date: March 2017 APPROVAL RECORD COMMITTEES / GROUP DATE Consultation: Planned Care SQS 25 th March 2017 Approved by Director: Received for information: Director of Nursing, Quality and Performance Professional Forum Directorate SQS meetings 25 th March th March 2017 MC/JH/SL review of policy March17 2
3 Contents - Pages Policy Statement Planning and Implementation Circumstances where marking may not be appropriate Patient Refusal of Pre-operative Skin Marking (appendix 3) Marking to promote correct site surgery Standard pre-operative marking using a marking pen Marking using other techniques in specialist departments such as Radiology Surgical Safety Checklist Risk Management Pre-Operative Marking (Procedure 1, Appendix 1) How to mark Where to mark Who marks With whom Time and place Verify (Appendix 2) Organisational Responsibilities Measuring performance Review 9 Appendix 1 - Procedure for Pre-operative Marking 10 Appendix 2 - The Pre-Operative Surgical Safety Checklist 11 Appendix 3 WHO safety checklist (theatre) 12 Appendix 4 Patient Refusal Form MC/JH/SL review of policy March17 3
4 1.0 POLICY STATEMENT The national Patient Safety Agency (NPSA) issued alert No. 06 in March 2005 with regard to pre-operative marking recommendations, which East Cheshire NHS Trust adopted. In January 2009 the World Health Organisation (WHO) reviewed the 2008 version of the guidance and recommendation made within Safe Surgery Saves Lives Challenge document. The purpose of the World Health Organisation (WHO) Safe Surgery Saves Lives recommended the use of a universal WHO Patient Safety Checklist to facilitate improved patient safety and the provision of evidence based guidance to inform health care establishments worldwide to Firstly, to do no harm. The aim therefore of the WHO Patient Safety Checklist was to define a core set of safety standards that could be applied in all countries and healthcare settings to reduce the adverse consequences of wrong site, wrong patient surgical procedures In September 2015 National Safety Standards for Invasive Procedures (NATSSIPs) was published by NHS England. These standards set out key steps necessary to deliver safe care for patients undergoing invasive procedures and include steps for procedural verification of site marking. The Trust policy has been reviewed and updated to ensure that local standards are compliant with these national standards This Policy has been updated to reflect the recommendations made by WHO 2009, NATSSIPs 2015 and ECNHST s valued-based behaviours. It applies to all clinical staff employed by East Cheshire NHS Trust either temporarily or permanently who are responsible for providing compassionate care to our patients and their families. This policy has been impact assessed with regards to dignity, equality and diversity and there are no areas in the policy that contravene equality and diversity guidance. For further information please contact ecn-tr.policycoordination@nhs.net. 2.0 PLANNING AND IMPLEMENTATION Surgical site marking is mandatory for all procedures for which it is possible (NATSSIPs 2015) Non operative side must NEVER be marked even with statements such as not on this side (NATSSIPs 2015) 2.1 Circumstances where marking may not be appropriate a) Emergency surgery should not be delayed due to lack of pre-operative marking b) Teeth and mucous membranes c) Cases of bilateral organ surgery such as bilateral tonsillectomy, squint surgery d) Situations where the laterality of surgery needs to be confirmed following examination in theatre such as revision of squints 2.2 Patient Refusal of pre-operative skin marking Where a patient refuses to have their skin marked before surgery, the risks of wrong-site surgery should be explained to them by a suitably qualified healthcare professional. A clear and accurate entry must be made in the patient s clinical records in accordance with the professional s regulatory body and ECNHST Clinical Records Management Policy. MC/JH/SL review of policy March17 4
5 The patient should be asked to sign a Patient Refusal to have skin marked prior to their operation form, which is witnessed by any relative present/ and or operating doctor or deputy (please refer to appendix 4) It may be appropriate in such instances and in agreement with the patient to mark the site of the intended operation by using alternative means such as marking the antiembolic stocking or theatre gown, attaching a label to a digit, attaching a patient identification wrist band on the wrist of the correct site to be operated on or stick a paper tape to the correct site and mark this. It is not acceptable in such instances to do nothing. As an individual you must make the care of a patient your first concern and ensure their safety. Careful explanations of the reasons why marking for surgery is indicated may be enough for the patient to change their mind and accept skin marking. Equally, however, the patient s wishes or personal beliefs must be respected and supported by the healthcare worker acknowledging their right to accept or decline treatment or care. You must not allow their belief to prejudice the care you provide for them promoting dignity and respect at all times. In some instances a patient may not have the capacity to make an informed decision about skin marking. You must ensure that patients who lack capacity are fully safeguarded and seek further advice regarding mental capacity assessment. 2.3 Marking to promote correct site surgery Pre-operative marking has a significant role in promoting correct site surgery, including operating on the correct side of the patient and/ or the correct anatomical location or level (such as the correct finger on the correct hand). In all instances you must ensure the patient is wearing a printed or legible patient identification (ID) wristband with the correct details included as detailed in ECNHST Patient ID Policy. 2.4 Standard pre-operative marking using a marking pen The patient should be informed of, and agree of the requirement to mark the correct operation site at the point of access nearest to the surgery and prior to seeking their allergy status e.g. marking is usually undertaken on admission to the ward, day case unit or surgical admission lounge. It is advised that the patient has showered on the day of attendance to hospital before the pre-operative marking is applied to the skin area. The patient should be assured that the ink will wash off fairly quickly. It is the responsibility of the admitting nurse to confirm that the patient has showered prior to attendance and if not provide an opportunity for the patient to at the earliest opportunity. This must be documented as cited on the Surgical Safety Checklist. Pre-operative marking for patients who are due major bowel surgery are usually seen in the Bowel Screening Assessment Clinic on Friday afternoon prior to admission where preoperative marking is applied to the skin area. On the day of admission to hospital it is the responsibility of the admitting nurse to ensure that the patient has a shower using Chlorhexdine solution. The nurse must clearly document and sign the Surgical Safety Checklist as part of the procedure. 3.0 MARKING USING OTHER TECHNIQUES IN SPECIALIST DEPARTMENTS SUCH AS RADIOLOGY Patients may undergo other kinds of pre-operative marking such as for impalpable breast lesions where marking is made using ultrasound or guide wires inserted under X-ray control. In such circumstances additional marking by pen is unnecessary and potentially dangerous. MC/JH/SL review of policy March17 5
6 4.0 SURGICAL SAFETY CHECKLIST The WHO checklist has been adapted for use by ECNHST to incorporate the Pre- Operative Checklist and on the reverse of the form the Surgical Safety Checklist, the completion of which is mandatory for each patient undergoing a surgical procedure in theatres. The checklist is printed on pink paper to align itself with the surgical notes which are also printed on pink paper. A new checklist must be fixed to the patient s clinical records and a separate checklist should be completed for each new surgical procedure. The surgical checklists are available from the photocopying room, code: CPY787 (pink). All checklists must be filed in the appropriate section of the patient s clinical records together with the theatre records. 5.0 RISK MANAGEMENT If failure of any pre-operative check occurs the Surgeon in Charge should be informed immediately. (S)He will assess the situation in discussion with the patient. A decision to either continue with the planned surgery or return the patient to the ward/day case area or surgical admission lounge for the procedure to be rescheduled will be made. It is the Surgeon in Charge s responsibility to ensure that a clear and accurate entry is documented in the patient s clinical records that a decision to proceed at risk was taken in accordance with GMC standards, guidance and patient consent. A patient safety incident report (Datix form) must be completed even if the decision to proceed with the operation is made. The reason for failure of any pre-operative checks must be clearly documented. If the patient is returned to the ward/ day care area a patient safety incident report (Datix) must be completed in line with local governance procedures even if the operation did not take place. A senior member of staff should offer an explanation and apology to the patient and carer. If the patient s next of kin or carer is not within the hospital every effort should be made to make contact by telephone in order to explain the reasons why the procedure has not been undertaken and allow the family member/carer with an opportunity to visit outside of normal visiting hours. If surgery is carried out on the incorrect site or incorrect patient, a Datix incident form must be completed and investigation initiated as per national Never Event Policy and the trust s Incident Reporting Policy (SIRI). In addition, verbal escalation of the incident to clinical risk management and senior line management is required. The most senior responsible clinician must also comply with the Duty of Candour Being Open Policy. Action plans resulting from investigations must be implemented within the agreed time-scales and will be monitored by directorate SQS Sub-committees and Serious Incident Review Sub-committee. 6.0 PRE-OPERATIVE MARKING (PROCEDURE 1, APPENDIX 1) 6.1 How to mark a) Specialist Marking Specialist pre-operative marking procedures may be carried out where simple marking by indelible ink pen is not enough. For example, following discussion and agreement with patients with impalpable breast lesions, the operation site will be marked in the X-ray department by ultra sound or guide wire. It is not necessary to carry out any further marking MC/JH/SL review of policy March17 6
7 prior to theatre. The practitioner carrying out the procedure will document in the patient medical records. b) Indelible marker pen An indelible marker pen should be used., the ink of which is not easily removed with alcoholic solutions (NATSSIPs 2015) The mark should be an arrow that extends to or near to the incision site and remain visible after the application of the skin preparation. It is desirable that the mark should also remain visible after the application of theatre drapes. Advice from The Infection Prevention and Control Team confirms that risk of cross infections is minimal from the same pen used on many patients. Pre-operative preparation of skin in theatre should be sufficient to clean the marked skin. 6.2 Where to mark Ascertain intended surgical site from reliable documentation and images. Surgical operations involving side (laterality) should be marked at, or near, the intended incision. For digits on the hand and foot the mark should extend to the correct specific digit. The mark must be placed such that it will remain visible in the operative field after preparation of the patient and application of drapes (NATSSIPs 2015) For procedures during which the patients position is changed, marking must be applied such that it is visible at all times. when the patients position is changed during a procedure,the surgical site should be verified and the surgical mark checked(natssips 2015) 6.3 Who marks? Marking should be undertaken by the operating surgeon, or nominated deputy (see note below) who will be present in the operating theatre at the time of the patient s procedure. (NATSSIPs 2015). The Consultant remains responsible in law for the management of the patient s total care and treatment. Competence and training A nominated deputy may include the Peri-operative Specialist Practitioners and Surgical Care Practitioner, after appropriate training, assessment of competency and written approval from the relevant Consultant. 6.4 With whom The process of pre-operative marking of the intended site should involve the patient and/ or family members/ significant others wherever possible 7.0 TIME AND PLACE The procedural site must be marked shortly before the procedure but not in the anaesthetic or procedure room (NATSSIPs, 2015) The surgical site should, ideally be marked on the ward or day care area prior to patient transfer to the operating theatre. Marking should take place before pre-medication. 8.0 VERIFY (APPENDIX 2) The surgical site mark should be checked with the patient at the first nursing pre-operative check on the ward and against reliable documentation (including medical notes, consent form, X-rays) to confirm it is (a) correctly located, and (b) still legible, using the Preoperative Checklist (Pink Form) CPY787. Checking should occur at each transfer of the patient s care; MC/JH/SL review of policy March17 7
8 prior to leaving the ward (Refer to appendix 2) In the anaesthetic room The SIGN IN must be undertaken before induction on anaesthesia and carried out by the ODP and anaesthetist as per checklist (refer to appendix 3) The TIME OUT must be undertaken and carried out by the team members (circulator, ODP, nurse, anaesthetist and surgeon) before the start of the surgical intervention e.g. skin incision checking that marking is correct and the correct procedure is identified The SIGN OUT must be undertaken and carried out by the circulator, ODP, nurse, anaesthetist and surgeon before team members leave the operating theatre-.confirming that the procedure has been performed on the correct site and side( NATSSIPs 2015) It is imperative that the whole team are present and complies with the TIME OUT and SIGN OUT procedure as referred to in Appendix 3 Surgical Safety Checklist and documentation of sign in,,time out, and sign out is completed (NATSSIPs 2015) 9.0 ORGANISATIONAL RESPONSIBILITIES The responsibility for pre-operative correct site surgery marking will be the operating surgeon or designated deputy, who will be present in the theatre at the time of the Patient s procedure. The pre-operative checklist will be the responsibility of the responsible (checking) nurse. In theatre the operating surgeon and theatre staff directly involved in the intended operative procedure will be responsible for the required pre-operative checks. This Policy will be the responsibility of the Theatre Services Manager and Service Managers in Surgery, Orthopaedics and Radiology MEASURING PERFORMANCE Compliance with this policy will be monitored through the following: WHO checklist (Quality and Performance Balanced Scorecard) Independent observational audit of processes annual by a nominated member of the the Governance Department 11.0 REVIEW This policy will be reviewed every 2 years through the Planned Care Services Safety and Quality Standards Sub-committee, unless other recommendations or guidelines are released. MC/JH/SL review of policy March17 8
9 Appendix 1 POLICY FOR PRE-OPERATIVE MARKING CORRECT SITE SURGERY Procedure 1: Marking of Operation Site This procedure excludes specialist marking (e.g. in X-ray Department by guide wire or ultrasound). In all cases the surgeon performing the surgery must check the marking prior to anaesthesia. When marking a site or limb please ensure the following: The patient is able to identify the affected limb/area for surgery The notes, x-rays, consent form, patient understanding and operation list must all agree In the event of a confused/ unconscious patient, a relative, nurse or doctor must be a second witness to the marking with reference to the above The mark must be made using a permanent marker The mark should clearly identify the area of concern by an arrow or the use of accepted abbreviation on the site/ limb itself (i.e. Total Hip Replacement) A mark must be made even on a plastered or dressed area as this will be removed in the anaesthetic room The marker should avoid vulnerable areas (i.e. bruising/ tibial crest in malnourished individuals, friable skin in patients taking steroids) The marker should take note of allergy-prone individuals The mark should be applied as close to the procedure as is practical The mark must be placed such that it will remain visible in the operative field after preparation of the patient and application of drapes For procedures during which the patients position is changed, marking must be applied such that it is visible at all times. when the patients position is changed during a procedure,the surgical site should be verified and the surgical maker checked The mark should be made by a member of the team performing the surgery (i.e. the operating surgeon or nominated deputy) The marker should ask the patient/ nurse/carer to report if the mark is washed off preoperatively so that it may be re-applied Non operative side must never be marked even with statements such as not on this side (NATSSIPs 2015) MC/JH/SL review of policy March17 9
10 Name: Unit number : NHS Number: D.O.B. : THIS FORM MUST BE COMPLETED BY THE RESPONSIBLE NURSE BEFORE A PATIENT IS SENT TO THE OPERATING THEATRE. THE SITE OF OPERATION MUST BE MARKED BEFORE LEAVING THE WARD Blood Pressure Pulse Temperature (>36 C)* Respiratory rate Weight (kg) Blood Glucose (if diabetic) Consent form correctly completed and signed by patient Site of operation marked (COMPULSORY) Allergies/sensitivities Patient has taken usual prescribed medication/s Yes No Notes/ prescription sheet enclosed X-rays/scans/ test results enclosed Possum Score result in notes for laparotomy patients Yes No Patient Identity band checked with patient and notes VTE Risk assessed and appropriate measures taken Time patient last ate: Time patient last drank: All patients pre-op shower: YesNo Major bowel patients have showered with Chlorhexidine: Yes No In women of reproductive age: Could you be pregnant? Yes No Has a repeat G&S been done: not required Yes No Hearing aid removed and put away safely Dentures/plates removed Any loose teeth? Please state where Caps/crowns in situ Jewellery/body piercing/makeup/ hairgrips - removed taped False /Gel nails removed Yes No N/A Contact lenses/ prosthesis - removed Valuables secured Mobility assessed: state how travelling to theatre (walk/trolley/bed) If assessed as able to walk to theatre patient has given their consent: Yes No If travelling on trolley or bed safety rails in situ Yes No Waterlow >10 or at risk of pressure sore: Yes No ODA/ODP Receiving patient Print Name: Responsible Nurse Print Name: Responsible Nurse Signature: Signature: Date Date/Time: * Follow NICE guidance for SSI (CG74) and Peri-operative Care (CG65) CPY787 Updated March 17. Shared/surgical specialities/policies/preop chcklist
11 SIGN IN (ODP & Anaesthetist) BEFORE INDUCTION ON ANAESTHESIA Has the patient confirmed his/her identity, site, procedure and consent? Yes Is the surgical site marked? Yes Not applicable Is the anaesthesia machine and medication check complete? Yes Is the pulse oximeter on the patient and functioning? Yes Does the patient have a : Known allergy? No Yes Difficult airway or aspiration risk? No Yes, and equipment/assistance available Risk of >500ml blood loss (7ml/kg in children)? No Yes Blood products available/g&s two IVs/central venous access Need for Active Warning? No Yes TIME OUT (Circulator, ODP, Nurse, Anaesthetist and Surgeon) BEFORE SKIN INCISION Confirm all team members have introduced themselves by name and role Confirm the patient s name, procedure and where the incision will be made Has antibiotics prophylaxis been given within the last 60 minutes Yes Not applicable Has VTE prophylaxis been undertaken? Yes Not applicable Anticipated Critical Events To Surgeon: What are the critical or non-routine steps? How long will case take? What is anticipated blood loss? To Anaesthetist: Are there any patient specific concerns? To Nursing Team: Has sterility (including indicator results) been confirmed? Are there any equipment issues or any concerns? Is essential imaging displayed? Yes Not applicable SIGN OUT (Circulator, ODP, Nurse, Anaesthetist & Surgeon) BEFORE PATIENT LEAVES OPERATING ROOM Scrub nurse verbally confirms with the team: The name of the procedure Completion of instruments, sponge and needle counts Specimen labelling (read specimen labels aloud, including patient name) Whether there are any equipment problems to be addressed Surgeon, anaesthetist and scrub nurse: What are the key concerns for recovery and management of this patient?
12 POLICY FOR PRE-OPERATIVE MARKING CORRECT SITE SURGERY PATIENT REFUSAL TO HAVE SKIN MARKED BEFORE THEIR OPERATION I (full name):.... Hospital Number:... Address: OPERATION: Do not want my skin to be marked for the correct operation site prior to my operation I have been informed clearly of the risks I am taking by this refusal I understand and accept the risks and wish the operation to proceed without the marks Signature of patient:.. Witness 1:... (relative) Witness 2:... (Operating Surgeon or operating deputy) Date:. This form must be filed in the medical record with the theatre notes
Patient safety alert 06
 Immediate action Action Update Information request Correct site surgery Surgery performed at the incorrect anatomical site is rare. However, it can be devastating for patients. Correct site surgery (CSS)
Immediate action Action Update Information request Correct site surgery Surgery performed at the incorrect anatomical site is rare. However, it can be devastating for patients. Correct site surgery (CSS)
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Pre-Operative Marking
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Pre-Operative Marking Version.: 6.1 Effective From: 01 April 2015 Expiry Date: 01 April 2018 Date Ratified: 17 December 2014 Ratified By: Theatre
The Newcastle upon Tyne Hospitals NHS Foundation Trust Pre-Operative Marking Version.: 6.1 Effective From: 01 April 2015 Expiry Date: 01 April 2018 Date Ratified: 17 December 2014 Ratified By: Theatre
Policy for Patient Identification. Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead:
 CONTROLLED DOCUMENT Policy for Patient Identification CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead: Approved By:
CONTROLLED DOCUMENT Policy for Patient Identification CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled Document Lead: Approved By:
Implementation of Surgical Safety Checklist
 Implementation of Surgical Safety Checklist The World Health Organisation has identified through consultation with surgeons, anaesthetists and nurses a checklist of critical steps that are common to all
Implementation of Surgical Safety Checklist The World Health Organisation has identified through consultation with surgeons, anaesthetists and nurses a checklist of critical steps that are common to all
Five Steps to Safer Surgical Interventions
 Five Steps to Safer Surgical Interventions Local Safety Standards for Invasive Procedures 1 Policy Title: Five Steps to Safer Surgical Interventions Executive Summary: A definitive policy for the roles
Five Steps to Safer Surgical Interventions Local Safety Standards for Invasive Procedures 1 Policy Title: Five Steps to Safer Surgical Interventions Executive Summary: A definitive policy for the roles
Admission Record IVF/Gynae
 Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
Admission Record IVF/Gynae Surgeon: Operation : of Admission: Please state your full name and date of birth - correct Nurse Checklist Yes No Please tell me your full address - correct Consent form signed,
Patient Transfer Policy
 Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
Patient Transfer Policy Policy Title: Executive Summary: Patient Transfer Policy All patients within East Cheshire NHS Trust that require transfer from one area to another either internally or externally
SURGICAL SAFETY CHECKLIST
 SURGICAL SAFETY CHECKLIST WHY: INFORMATION, RATIONALE, AND FAQ May 2009 Building a safer health system INFORMATION, RATIONALE, AND FAQ May 2009 - Version 1.0 The aim of this document is to provide information
SURGICAL SAFETY CHECKLIST WHY: INFORMATION, RATIONALE, AND FAQ May 2009 Building a safer health system INFORMATION, RATIONALE, AND FAQ May 2009 - Version 1.0 The aim of this document is to provide information
Nursing Practice Committee
 Nursing Practice Committee Standard Operating Procedure on Patient preparation and Admission to Operating Theatre Author: Emma Cooney CNM 3 & Rosemary Clerkin CNF Issue Date: March 2010 Review Date: March
Nursing Practice Committee Standard Operating Procedure on Patient preparation and Admission to Operating Theatre Author: Emma Cooney CNM 3 & Rosemary Clerkin CNF Issue Date: March 2010 Review Date: March
Patient information. Ankle Arthroscopy. Trauma and Orthopaedic Directorate PIF 713 / V4
 Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Accreditation Program: Hospital Chapter: National Patient Safety Goals
 Universal Protocol Accreditation Program: Hospital Chapter: National Patient Safety Goals The organization meets the expectations of the Universal Protocol. UP.01.01.01 Conduct a pre-procedure verification
Universal Protocol Accreditation Program: Hospital Chapter: National Patient Safety Goals The organization meets the expectations of the Universal Protocol. UP.01.01.01 Conduct a pre-procedure verification
How important is verification of correct site surgery marking?
 How important is verification of correct site surgery marking? By Veronica Mac-Quarshie Moteclife UK June,2008 PLAN Definitions Background Risk Factors Causes of wrong site surgery Effects on patient and
How important is verification of correct site surgery marking? By Veronica Mac-Quarshie Moteclife UK June,2008 PLAN Definitions Background Risk Factors Causes of wrong site surgery Effects on patient and
Procedure. Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013. Title: Universal Protocol / Time Out
 Title: Universal Protocol / Time Out Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013 Procedure Patient Age Group: ( ) N/A (X) All Ages ( ) Newborns ( ) Pediatric
Title: Universal Protocol / Time Out Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013 Procedure Patient Age Group: ( ) N/A (X) All Ages ( ) Newborns ( ) Pediatric
Recommendations from National Patient Safety Agency alerts that remain relevant to the Never Events list 2018
 Recommendations from National Patient Safety Agency alerts that remain relevant to the Never Events list 2018 January 2018 We support providers to give patients safe, high quality, compassionate care within
Recommendations from National Patient Safety Agency alerts that remain relevant to the Never Events list 2018 January 2018 We support providers to give patients safe, high quality, compassionate care within
Inguinal hernia repair integrated care pathway (ICP)
 Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Hip fracture - DHS. Your broken hip joint - some information
 Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
Surgery Road Map. General practices. Road map sections
 Surgery Road Map MHA s road maps provide hospitals and health systems with evidence-based recommendations and standards for the development of topic-specific prevention and quality improvement programs,
Surgery Road Map MHA s road maps provide hospitals and health systems with evidence-based recommendations and standards for the development of topic-specific prevention and quality improvement programs,
Z: Perioperative Nursing Specialty
 Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
DOCUMENT CONTROL Patient Identification Policy 6 CL001
 Title: Version: Reference Number: Scope: DOCUMENT CONTROL Patient Identification Policy 6 CL001 This policy applies to all staff who work in an inpatient setting and staff accessing inpatient wards. Purpose:
Title: Version: Reference Number: Scope: DOCUMENT CONTROL Patient Identification Policy 6 CL001 This policy applies to all staff who work in an inpatient setting and staff accessing inpatient wards. Purpose:
High 5s Project: Action on Patient Safety. SOP Flow Charts. 20 th International Forum on Quality and Safety in Healthcare April 2015 London, UK
 High 5s Project: Action on Patient Safety SOP Flow Charts 20 th International Forum on Quality and Safety in Healthcare 21-24 April 2015 London, UK Performance of Correct Procedure at Correct Body Site
High 5s Project: Action on Patient Safety SOP Flow Charts 20 th International Forum on Quality and Safety in Healthcare 21-24 April 2015 London, UK Performance of Correct Procedure at Correct Body Site
Implementation Manual for the World Health Organization Surgical Safety Checklist (First Edition)
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Implementation Manual for the World Health Organization Surgical Safety Checklist (First Edition) Author : SAGES
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Implementation Manual for the World Health Organization Surgical Safety Checklist (First Edition) Author : SAGES
Management of Reported Medication Errors Policy
 Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
Management of Reported Medication Errors Policy Approved By: Policy & Guideline Committee Date of Original 6 October 2008 Approval: Trust Reference: B45/2008 Version: 4 Supersedes: 3 February 2015 Trust
South Tyneside NHS Foundation Trust. Clinical Policy. Chaperoning Policy. Review Date June 2011
 South Tyneside NHS Foundation Trust Clinical Policy Chaperoning Policy Date Approved by Version Issue Date June 2009 2 June Executive 2009 Director of Nursing & Clinical Services Procedure /Policy number
South Tyneside NHS Foundation Trust Clinical Policy Chaperoning Policy Date Approved by Version Issue Date June 2009 2 June Executive 2009 Director of Nursing & Clinical Services Procedure /Policy number
PATIENT IDENTIFICATION POLICY
 PATIENT IDENTIFICATION POLICY DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Effectiveness Committee Date ratified: 12 th January 2012 Name of originator/author: Clinical Policy Advisor Name of responsible
PATIENT IDENTIFICATION POLICY DOCUMENT CONTROL: Version: 1 Ratified by: Clinical Effectiveness Committee Date ratified: 12 th January 2012 Name of originator/author: Clinical Policy Advisor Name of responsible
Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital
 Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital Name: Start Date:. Mentor:. Introduction My name is Helen McCallum; I am the Clinical Skills Facilitator for St Marys Theatres. I would
Introduction to Gynaecology & Obstetrics Theatres St Marys Hospital Name: Start Date:. Mentor:. Introduction My name is Helen McCallum; I am the Clinical Skills Facilitator for St Marys Theatres. I would
UNIVERSAL PROTOCOL POLICY FOR CORRECT SITE IDENTIFICATION (VERIFICATION OF CORRECT SITE FOR INVASIVE, HIGHRISK, OR SURGICAL PROCEDURES)
 UNIVERSAL PROTOCOL POLICY FOR CORRECT SITE IDENTIFICATION (VERIFICATION OF CORRECT SITE FOR INVASIVE, HIGHRISK, OR SURGICAL PROCEDURES) PURPOSE: To promote patient safety by providing guidelines for verification
UNIVERSAL PROTOCOL POLICY FOR CORRECT SITE IDENTIFICATION (VERIFICATION OF CORRECT SITE FOR INVASIVE, HIGHRISK, OR SURGICAL PROCEDURES) PURPOSE: To promote patient safety by providing guidelines for verification
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Spire Wellesley Hospital Eastern Avenue, Southend-on-Sea, SS2
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Spire Wellesley Hospital Eastern Avenue, Southend-on-Sea, SS2
Same Day Admission (in A.M.)
 Same Day Admission (in A.M.) Patient Information Booklet Pre-Operative Assessment Clinic Please bring this book to your admission to the Hospital and to all of your appointments For information call 613-721-2000
Same Day Admission (in A.M.) Patient Information Booklet Pre-Operative Assessment Clinic Please bring this book to your admission to the Hospital and to all of your appointments For information call 613-721-2000
Patient Information Leaflet. Tennis Elbow. Produced By: Orthopaedic Department
 Patient Information Leaflet Tennis Elbow Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another format, please
Patient Information Leaflet Tennis Elbow Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another format, please
PLANNED CARE THEATRE OPERATIONAL POLICY
 PLANNED CARE THEATRE OPERATIONAL POLICY Review date: April 2021 Mr U Khan : Clinical Director Mr M Brown :Associate Director Planned Care Mr M Cawley : Theatre Manager Theatre Operational Policy V4.1 Policy
PLANNED CARE THEATRE OPERATIONAL POLICY Review date: April 2021 Mr U Khan : Clinical Director Mr M Brown :Associate Director Planned Care Mr M Cawley : Theatre Manager Theatre Operational Policy V4.1 Policy
Day Surgery. Patient Information Booklet Pre-Operative Assessment Clinic
 Day Surgery Patient Information Booklet Pre-Operative Assessment Clinic Please bring this book to your admission to the Hospital and to all of your appointments For information call 613-721-2000 extension
Day Surgery Patient Information Booklet Pre-Operative Assessment Clinic Please bring this book to your admission to the Hospital and to all of your appointments For information call 613-721-2000 extension
Patient Identification
 Patient Identification Reference No: Version: 5 Ratified by: P_CS_24 LCHS Trust Board Date ratified: 10 th April 2018 Name of originator/author: Name of approving committee/responsible individual: Date
Patient Identification Reference No: Version: 5 Ratified by: P_CS_24 LCHS Trust Board Date ratified: 10 th April 2018 Name of originator/author: Name of approving committee/responsible individual: Date
Assessment criteria for obtaining a venous blood sample
 Core blood competencies assessment framework Assessment criteria for obtaining a venous blood sample This framework is for assessing the candidates ability in obtaining a venous blood sample for transfusion.
Core blood competencies assessment framework Assessment criteria for obtaining a venous blood sample This framework is for assessing the candidates ability in obtaining a venous blood sample for transfusion.
Title: VERIFICATION OF PROCEDURES TO BE PERFORMED
 Approved By: Garren Colvin, EVP/COO Responsible Parties: Alicia Humphrey, Director Outpatient Surgery Tracie Shelton, Director Patient Safety & Accreditation Policy No.: ACLIN-V-01 Originated: 01/01/11
Approved By: Garren Colvin, EVP/COO Responsible Parties: Alicia Humphrey, Director Outpatient Surgery Tracie Shelton, Director Patient Safety & Accreditation Policy No.: ACLIN-V-01 Originated: 01/01/11
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients
 Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Accreditation Program: Office-Based Surgery
 ccreditation Program: Office-Based Surgery National Patient Safety Goals indicates scoring category ; indicates scoring category ; indicates situational decision rules apply; indicates 2009 The Joint ommission
ccreditation Program: Office-Based Surgery National Patient Safety Goals indicates scoring category ; indicates scoring category ; indicates situational decision rules apply; indicates 2009 The Joint ommission
TRUST POLICY AND PROCEDURES FOR PATIENT IDENTIFICATION
 TRUST POLICY AND PROCEDURES FOR PATIENT IDENTIFICATION Reference Number POL-RKM/2133/08 Version: 4 Status: Final Author: Sandra Mir Job Title: Patient Safety and Risk Manager Version / Amendment History
TRUST POLICY AND PROCEDURES FOR PATIENT IDENTIFICATION Reference Number POL-RKM/2133/08 Version: 4 Status: Final Author: Sandra Mir Job Title: Patient Safety and Risk Manager Version / Amendment History
Surgical Technology Patient Care Skills Preop Routine Objectives:
 Surgical Technology 8-Jul-09 Patient Care Skills Preop Routine Objectives: 1) Discuss why preop preparation of the patient is important a) Preparing the patient decreases impact and potential risks of
Surgical Technology 8-Jul-09 Patient Care Skills Preop Routine Objectives: 1) Discuss why preop preparation of the patient is important a) Preparing the patient decreases impact and potential risks of
POLICY NO.: POLICY AND PROCEDURE Subject: Patient Identification and Wrist Bands SUPERSEDES: ORIGINAL DATE: PAGE: I. POLICY: II. DEFINITIONS: PC_01
 POLICY AND PROCEDURE Subject: Patient Identification and Wrist Bands POLICY NO.: PC_01 ORIGINAL DATE: SUPERSEDES: PAGE: 04/01/1998 12/2012 1 of 6 Key Words: Color Coded Alert, ID Applies to: Inpatient:
POLICY AND PROCEDURE Subject: Patient Identification and Wrist Bands POLICY NO.: PC_01 ORIGINAL DATE: SUPERSEDES: PAGE: 04/01/1998 12/2012 1 of 6 Key Words: Color Coded Alert, ID Applies to: Inpatient:
PATIENT ASSESSMENT POLICY Page 1 of 7
 Page 1 of 7 Policy applies to: All staff and allied health professionals involved in patient care delivery at Mercy Hospital including Manaaki. Related Standards: Health & Disability Services (core) Standards
Page 1 of 7 Policy applies to: All staff and allied health professionals involved in patient care delivery at Mercy Hospital including Manaaki. Related Standards: Health & Disability Services (core) Standards
What will I do? Our HCSWs fall into three groups:
 As an HCSW, you will be a valued member of your team. Your focus will be on keeping patients at the centre of all we do, providing high quality care and living our Trust values: Together - Safe Kind Excellent.
As an HCSW, you will be a valued member of your team. Your focus will be on keeping patients at the centre of all we do, providing high quality care and living our Trust values: Together - Safe Kind Excellent.
Enhancing Patient Safety through Team Work and Communication Strategies
 Enhancing Patient Safety through Team Work and Communication Strategies St. Joseph Medical Center- Towson Maryland Program/Project Description. In July 2009, Catholic Health Initiatives, of which St Joseph
Enhancing Patient Safety through Team Work and Communication Strategies St. Joseph Medical Center- Towson Maryland Program/Project Description. In July 2009, Catholic Health Initiatives, of which St Joseph
Patient Safety (PS) 1) A collaborative process is used to develop policies and/or procedures that address the accuracy of patient identification.
 Patient Safety (PS) Standard PS.1 [Patient identification] The organization has established procedures for accurately identifying patients. Intent of PS.1 Wrong-patient errors occur in virtually all aspects
Patient Safety (PS) Standard PS.1 [Patient identification] The organization has established procedures for accurately identifying patients. Intent of PS.1 Wrong-patient errors occur in virtually all aspects
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
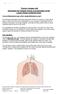 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
National Patient Safety Goals Effective January 1, 2016
 National Patient Safety Goals Effective January 1, 2016 Goal 1 Improve the accuracy of patient identification. NPSG.01.01.01 Office-Based Surgery ccreditation Program Use at least two patient identifiers
National Patient Safety Goals Effective January 1, 2016 Goal 1 Improve the accuracy of patient identification. NPSG.01.01.01 Office-Based Surgery ccreditation Program Use at least two patient identifiers
Excision of Submandibular Gland
 Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery
 CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
CLINICAL GUIDELINE Perioperative management of the higher risk surgical patient with an acute surgical abdomen undergoing emergency surgery CG10214-2 For use in (clinical areas): For use by (staff groups):
POLICY. The purpose of this policy is to establish Saskatoon Health Region s (SHR s) communication requirements for all surgical patients.
 POLICY Number: 7311-60-026 Title: Surgical Safety Checklist Authorization [ ] President and CEO [ X] Vice President, Finance and Corporate Services Source: Chair(s), Surgical Operations Committee Cross
POLICY Number: 7311-60-026 Title: Surgical Safety Checklist Authorization [ ] President and CEO [ X] Vice President, Finance and Corporate Services Source: Chair(s), Surgical Operations Committee Cross
The Regulation and Quality Improvement Authority
 The Regulation and Quality Improvement Authority Review of Theatre Practice in Health and Social Care Trusts in Northern Ireland Overview report June 2014 Assurance, Challenge and Improvement in Health
The Regulation and Quality Improvement Authority Review of Theatre Practice in Health and Social Care Trusts in Northern Ireland Overview report June 2014 Assurance, Challenge and Improvement in Health
Wrong site interventions
 Publication Ref: I2017/004/1 Wrong site interventions 27 November 2017 This interim bulletin contains facts which have been determined up to the time of issue. It is published to inform the NHS and the
Publication Ref: I2017/004/1 Wrong site interventions 27 November 2017 This interim bulletin contains facts which have been determined up to the time of issue. It is published to inform the NHS and the
Reducing the Risk of Wrong Site Surgery
 Joint Commission Center for Transforming Healthcare Reducing the Risk of Wrong Site Surgery Wrong Site Surgery Project Participants The Joint Commission s Center for Transforming Healthcare aims to solve
Joint Commission Center for Transforming Healthcare Reducing the Risk of Wrong Site Surgery Wrong Site Surgery Project Participants The Joint Commission s Center for Transforming Healthcare aims to solve
Patient copy. Periurethral bulking agent for stress urinary incontinence. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
COMPETENCIES FOR HEALTHCARE ASSISTANT IN SEXUAL HEALTH (BAND 3)
 COMPETENCIES FOR HEALTHCARE ASSISTANT IN SEXUAL HEALTH (BAND 3) Dimension Level Indicators Areas of application to nursing practice Achieved - Signature and Date 1. Communication Level 2 Communicate with
COMPETENCIES FOR HEALTHCARE ASSISTANT IN SEXUAL HEALTH (BAND 3) Dimension Level Indicators Areas of application to nursing practice Achieved - Signature and Date 1. Communication Level 2 Communicate with
Health Care Support Worker. Job description
 Health Care Support Worker Job description Date: December 2015 Context Barts Health NHS Trust is one of Britain s leading healthcare providers and the largest trust in the NHS. It was created on 1 April
Health Care Support Worker Job description Date: December 2015 Context Barts Health NHS Trust is one of Britain s leading healthcare providers and the largest trust in the NHS. It was created on 1 April
CLINICAL EXAMINATION INSTRUCTIONS FOR CANDIDATES
 POLICY ROYAL AUSTRALASIAN COLLEGE OF SURGEONS Division: Education Development & Assessment Ref. No. EDA-EXA-004 Department: Examinations Title: Conduct of the SET Clinical Examination SCHEDULE 1 ROYAL
POLICY ROYAL AUSTRALASIAN COLLEGE OF SURGEONS Division: Education Development & Assessment Ref. No. EDA-EXA-004 Department: Examinations Title: Conduct of the SET Clinical Examination SCHEDULE 1 ROYAL
Policy for Venous Thromboembolism Prevention and Treatment
 Policy for Venous Thromboembolism Prevention and Treatment Start date: May 2013 Next Review: May 2015 Committee approval: Endorsed by: Distribution: Location Thrombosis and Thromboprophylaxis Steering
Policy for Venous Thromboembolism Prevention and Treatment Start date: May 2013 Next Review: May 2015 Committee approval: Endorsed by: Distribution: Location Thrombosis and Thromboprophylaxis Steering
Prescribing Policy between Nottinghamshire Commissioning Organisations and local providers of NHS Services
 Prescribing Policy between Nottinghamshire Commissioning Organisations and local providers of NHS Services Document Purpose Version 2.2 To detail the specific contractual issues associated with prescribing
Prescribing Policy between Nottinghamshire Commissioning Organisations and local providers of NHS Services Document Purpose Version 2.2 To detail the specific contractual issues associated with prescribing
Patient Information Varicose Vein Surgery Dr Marek Garbowski. Varicose Veins
 Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Fitzwilliam Hospital Milton Way, South Bretton, Peterborough,
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Fitzwilliam Hospital Milton Way, South Bretton, Peterborough,
Medical Staff Rules & Regulations Last Updated: October University Hospital Medical Staff. Rules & Regulations
 University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
Day Surgery/Endoscopy Unit
 Day Surgery/Endoscopy Unit Information for Day Surgery Patient information Leaflet Your Consultant Surgeon has decided that you need an operation/procedure. Because your operation/procedure requires only
Day Surgery/Endoscopy Unit Information for Day Surgery Patient information Leaflet Your Consultant Surgeon has decided that you need an operation/procedure. Because your operation/procedure requires only
The How to Guide for Reducing Surgical Complications
 The How to Guide for Reducing Surgical Complications Post operative wound (surgical site) infections Maintaining perioperative normothermia Main contacts for Reducing Surgical Complications Campaign Director:
The How to Guide for Reducing Surgical Complications Post operative wound (surgical site) infections Maintaining perioperative normothermia Main contacts for Reducing Surgical Complications Campaign Director:
ACUTE CARE BUSINESS UNIT THEATRE OPERATIONAL POLICY
 ACUTE CARE BUSINESS UNIT THEATRE OPERATIONAL POLICY Review date: October 2017 Mr U Khan : Clinical Director Mrs G Bird : Directorate Manager Critical Care Mr M Cawley : Theatre Manager Theatre Operational
ACUTE CARE BUSINESS UNIT THEATRE OPERATIONAL POLICY Review date: October 2017 Mr U Khan : Clinical Director Mrs G Bird : Directorate Manager Critical Care Mr M Cawley : Theatre Manager Theatre Operational
How do we know the surgical checklist is making a meaningful. impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010
 How do we know the surgical checklist is making a meaningful impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010 1 Show Me the Evidence You simply have to MEASURE! 2 Why Measure?
How do we know the surgical checklist is making a meaningful impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010 1 Show Me the Evidence You simply have to MEASURE! 2 Why Measure?
Register No: Status: Public on ratification
 Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
Private Patient Policy Type: Policy Register No: 12024 Status: Public on ratification Developed in response to: Service Development Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group
POLICY FOR TAKING BLOOD CULTURES
 Sponsor: Reviewer(s): Dr Roberta Parnaby (Consultant Microbiologist) Dr Alicja Baczynska (F2 Microbiology) Dr Chris Gordon (Medical Director) Dr Roberta Parnaby Dr Matthew Dryden (Consultant Microbiologists)
Sponsor: Reviewer(s): Dr Roberta Parnaby (Consultant Microbiologist) Dr Alicja Baczynska (F2 Microbiology) Dr Chris Gordon (Medical Director) Dr Roberta Parnaby Dr Matthew Dryden (Consultant Microbiologists)
Serious Incident Report Public Board Meeting 28 July 2016
 Serious Incident Report Public Board Meeting 28 July 2016 Presented for: Presented by: Author Previous Committees Governance Dr Yvette Oade, Chief Medical Officer Louise Povey, Serious Incidents Investigations
Serious Incident Report Public Board Meeting 28 July 2016 Presented for: Presented by: Author Previous Committees Governance Dr Yvette Oade, Chief Medical Officer Louise Povey, Serious Incidents Investigations
Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1
 Managing medicines in care homes Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Managing medicines in care homes Social care guideline Published: 14 March 2014 nice.org.uk/guidance/sc1 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Spire Gatwick Park Hospital Povey Cross Road, Horley, RH6 0BB
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Spire Gatwick Park Hospital Povey Cross Road, Horley, RH6 0BB
Choice on Discharge Policy
 Choice on Discharge Policy Reference No: P_CIG_19 Version 1 Ratified by: LCHS Trust Board Date ratified: 13 th September 2016 Name of originator / author: Sarah McKown Name of responsible committee / Individual
Choice on Discharge Policy Reference No: P_CIG_19 Version 1 Ratified by: LCHS Trust Board Date ratified: 13 th September 2016 Name of originator / author: Sarah McKown Name of responsible committee / Individual
PLASTER CASTS, APPLIANCES OR BRACES
 PRESSURE DAMAGE: POLICY FOR PREVENTION IN PATIENTS WITH PLASTER CASTS, APPLIANCES OR BRACES To be read in conjunction with the Pressure Ulceration Policy and DVT and PE Policy Version: 2 Ratified by: Date
PRESSURE DAMAGE: POLICY FOR PREVENTION IN PATIENTS WITH PLASTER CASTS, APPLIANCES OR BRACES To be read in conjunction with the Pressure Ulceration Policy and DVT and PE Policy Version: 2 Ratified by: Date
USING FRAM IN A CHILDREN S SURGICAL UNIT
 USING FRAM IN A CHILDREN S SURGICAL UNIT TO UNDERSTAND WORKFLOW AND DESIGN SOLUTIONS TO DAMPEN VARIABILITY Dr Danielle Franklin BM BSc FRCA Safety- II in Practice 14-15 June 2018 Supported by Ernest Leach
USING FRAM IN A CHILDREN S SURGICAL UNIT TO UNDERSTAND WORKFLOW AND DESIGN SOLUTIONS TO DAMPEN VARIABILITY Dr Danielle Franklin BM BSc FRCA Safety- II in Practice 14-15 June 2018 Supported by Ernest Leach
Patient Weighing Scales Policy
 Patient Weighing Scales Policy Policy Title: Executive Summary: Patient Weighing Scales Policy East Cheshire NHS Trust is committed to the health safety and welfare of all of the patients it treats. The
Patient Weighing Scales Policy Policy Title: Executive Summary: Patient Weighing Scales Policy East Cheshire NHS Trust is committed to the health safety and welfare of all of the patients it treats. The
DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY
 DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY (To be read in conjunction with Diagnostic Imaging Requesting and Interpreting Radiographs by Non Medical Practitioners Policy, Consent
DIAGNOSTIC CLINICAL TESTS AND SCREENING PROCEDURES MANAGEMENT POLICY (To be read in conjunction with Diagnostic Imaging Requesting and Interpreting Radiographs by Non Medical Practitioners Policy, Consent
The University Hospital Medical Staff. Rules And Regulations
 The University Hospital Medical Staff Rules And Regulations - 1 - UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement
The University Hospital Medical Staff Rules And Regulations - 1 - UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement
Research Article WHO Surgical Checklist and Its Practical Application in Plastic Surgery
 Plastic Surgery International Volume 2011, Article ID 579579, 5 pages doi:10.1155/2011/579579 Research Article WHO Surgical Checklist and Its Practical Application in Plastic Surgery Shady Abdel-Rehim,
Plastic Surgery International Volume 2011, Article ID 579579, 5 pages doi:10.1155/2011/579579 Research Article WHO Surgical Checklist and Its Practical Application in Plastic Surgery Shady Abdel-Rehim,
Medicines Reconciliation Policy
 Medicines Reconciliation Policy Lead executive Medical Director Authors details Senior Clinical Pharmacy Technician - 01244 39 7494 Document level: Trustwide (TW) Code: MP19 Issue number: 3 Type of document
Medicines Reconciliation Policy Lead executive Medical Director Authors details Senior Clinical Pharmacy Technician - 01244 39 7494 Document level: Trustwide (TW) Code: MP19 Issue number: 3 Type of document
Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) Policy
 Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) Policy 1 Policy Title: Executive Summary: Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) Policy Cardiopulmonary resuscitation (CPR) can be attempted
Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) Policy 1 Policy Title: Executive Summary: Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) Policy Cardiopulmonary resuscitation (CPR) can be attempted
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition
 Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Chapter 3M Specialty Nursing Competencies Perioperative (Recovery) Nursing Competency Workbook 6th Edition The Royal Children's Hospital (RCH) Nursing Competency Workbook is a dynamic document that will
Issue Date Review Date Version July 2017 July 2022 V6
 Trust Policy Instrument Counts during Invasive Procedures Purpose Issue Date Review Date Version July 2017 July 2022 V6 This policy identifies the correct procedure for counting instruments and bio-medical
Trust Policy Instrument Counts during Invasive Procedures Purpose Issue Date Review Date Version July 2017 July 2022 V6 This policy identifies the correct procedure for counting instruments and bio-medical
Patient information. Plaque Radiotherapy. St. Paul s Eye Unit PIF 529 V8
 Patient information Plaque Radiotherapy St. Paul s Eye Unit PIF 529 V8 Your Consultant / Doctor has advised you to have Plaque Radiotherapy. What is Plaque Radiotherapy? It is radiotherapy used to treat
Patient information Plaque Radiotherapy St. Paul s Eye Unit PIF 529 V8 Your Consultant / Doctor has advised you to have Plaque Radiotherapy. What is Plaque Radiotherapy? It is radiotherapy used to treat
QUALITY NET REPORTING
 5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
A PATIENT S GUIDE TO PREPARE FOR SAME DAY ADMISSION SURGERY
 A PATIENT S GUIDE TO PREPARE FOR SAME DAY ADMISSION SURGERY Surgery Date The hospital will call with your arrival time 2 days prior to surgery. QHC#391 (Revised April 2015) 1 General Instructions Notify
A PATIENT S GUIDE TO PREPARE FOR SAME DAY ADMISSION SURGERY Surgery Date The hospital will call with your arrival time 2 days prior to surgery. QHC#391 (Revised April 2015) 1 General Instructions Notify
Your Guide To Spine Surgery
 Your Guide To Spine Surgery Your Guide To Spine Surgery C O N T E N T S Foreword 2 Introduction 3 The Spine 4 Preparation before Surgery 5 Day of Surgery 7 After Surgery 9 Medical and Nursing Care in the
Your Guide To Spine Surgery Your Guide To Spine Surgery C O N T E N T S Foreword 2 Introduction 3 The Spine 4 Preparation before Surgery 5 Day of Surgery 7 After Surgery 9 Medical and Nursing Care in the
Wrong Site, Wrong Procedure, Wrong Person Surgery
 Back to Basics Seventh in a Series Patient Safety Wrong Site, Wrong Procedure, Wrong Person Surgery By Alecia Cooper, RN, BS, MBA, CNOR An alarming occurrence affecting perioperative patient safety: According
Back to Basics Seventh in a Series Patient Safety Wrong Site, Wrong Procedure, Wrong Person Surgery By Alecia Cooper, RN, BS, MBA, CNOR An alarming occurrence affecting perioperative patient safety: According
Guidance for Fellows in implementing surgical safety checklists for radiological procedures
 Radiology Guidance for Fellows in implementing surgical safety checklists for radiological procedures Board of the Faculty of Clinical Radiology The Royal College of Radiologists Contents Introduction
Radiology Guidance for Fellows in implementing surgical safety checklists for radiological procedures Board of the Faculty of Clinical Radiology The Royal College of Radiologists Contents Introduction
About your peritoneal dialysis catheter. Information for patients Sheffield Kidney Institute (Renal Unit)
 About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
Hickman line insertion in the interventional radiology department
 Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Morton s neuroma. If you have any further questions, please speak to a doctor or nurse caring for you.
 Morton s neuroma This leaflet aims to answer your questions about having surgery for Morton s neuroma. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Morton s neuroma This leaflet aims to answer your questions about having surgery for Morton s neuroma. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Preventing Wrong-Site Surgery Through Implementation of Evidenced-Based Best Practices
 Preventing Wrong-Site Surgery Through Implementation of Evidenced-Based Best Practices Robert Yonash, RN, CPPS Pennsylvania Patient Safety Authority Patient Safety Liaison, Southwest Region Objectives
Preventing Wrong-Site Surgery Through Implementation of Evidenced-Based Best Practices Robert Yonash, RN, CPPS Pennsylvania Patient Safety Authority Patient Safety Liaison, Southwest Region Objectives
JOB DESCRIPTION. Ward/dept Queen Victoria Hospital, East Grinstead
 JOB DESCRIPTION Job Title: Staff Nurse Intensive care Band: 5 Base: Division / Department: Ward/dept Queen Victoria Hospital, East Grinstead Nursing and Quality Hours: Reports to: Accountable to: Ward
JOB DESCRIPTION Job Title: Staff Nurse Intensive care Band: 5 Base: Division / Department: Ward/dept Queen Victoria Hospital, East Grinstead Nursing and Quality Hours: Reports to: Accountable to: Ward
Neurosurgical Unit Day Case Surgery
 Information for patients Neurosurgical Unit Day Case Surgery Your admission to the neurosurgical unit day case procedure Thank you for attending Pre-assessment Clinic. Following your appointment, providing
Information for patients Neurosurgical Unit Day Case Surgery Your admission to the neurosurgical unit day case procedure Thank you for attending Pre-assessment Clinic. Following your appointment, providing
Having an Oesophageal Dilatation
 Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
ECT Reference: Version 4 Effective Date: 28/02/2017. Date
 Chaperone Policy Policy Title: Executive Summary: Chaperone Policy This policy sets out guidance on the use of chaperones within the Trust and is based on recommendations from the General Medical Council,
Chaperone Policy Policy Title: Executive Summary: Chaperone Policy This policy sets out guidance on the use of chaperones within the Trust and is based on recommendations from the General Medical Council,
bpas JOB OUTLINE AND PERSON SPECIFICATION
 bpas JOB OUTLINE AND PERSON SPECIFICATION Role: Responsible to: Surgeon - Termination of Pregnancy Unit Manager Purpose To provide safe, effective and comprehensive surgical and medical terminations of
bpas JOB OUTLINE AND PERSON SPECIFICATION Role: Responsible to: Surgeon - Termination of Pregnancy Unit Manager Purpose To provide safe, effective and comprehensive surgical and medical terminations of
Acute Medical Unit (AMU)
 Acute Medical Unit (AMU) Contents What is the Acute Medical Unit? 3 What happens when I come to the unit? 3 What if I need to stay in the unit? 4 What if I need to be admitted to hospital? 5 What happens
Acute Medical Unit (AMU) Contents What is the Acute Medical Unit? 3 What happens when I come to the unit? 3 What if I need to stay in the unit? 4 What if I need to be admitted to hospital? 5 What happens
Stapling / Repair of Pharyngeal Pouch
 Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
Hepatitis B Immunisation procedure SOP
 Hepatitis B Immunisation Procedure SOP Standard Operating Procedure (SOP) Ref No: 1992 Version: 3 Prepared by: Karen Bennett Presented to: Care and Clinical Policies Sub Group Ratified by: Care and Clinical
Hepatitis B Immunisation Procedure SOP Standard Operating Procedure (SOP) Ref No: 1992 Version: 3 Prepared by: Karen Bennett Presented to: Care and Clinical Policies Sub Group Ratified by: Care and Clinical
Appendix 1. Policy on the Dissemination, Implementation and Monitoring of National Clinical Guidance
 Appendix 1 Policy on the Dissemination, Implementation and Monitoring of National Clinical Guidance Policy Title: Executive Summary: Policy on the dissemination, implementation and monitoring of national
Appendix 1 Policy on the Dissemination, Implementation and Monitoring of National Clinical Guidance Policy Title: Executive Summary: Policy on the dissemination, implementation and monitoring of national
Standard Operating Procedure
 Standard Operating Procedure Title of Standard Operation Procedure: Delivering Enhanced Care Reference Number: Version No: 6 Issue Date: April 2016 Review Date: April 2018 Purpose and Background Vulnerable
Standard Operating Procedure Title of Standard Operation Procedure: Delivering Enhanced Care Reference Number: Version No: 6 Issue Date: April 2016 Review Date: April 2018 Purpose and Background Vulnerable
