ROUNDTABLE. Value-based Care programs are driving improvements in quality and people s health. sponsored by
|
|
|
- Collin Robinson
- 6 years ago
- Views:
Transcription
1 ROUNDTABLE Value-based Care programs are driving improvements in quality and people s health sponsored by
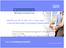
2 ROUNDTABLE CityBusiness Executive Roundtable Tuesday December 13, 2016 in the office of UnitedHealthcare, 3838 North Causeway Boulevard, Suite 2600, Metairie, Louisiana. Value-based Care is creating the personal connection for the consumer, really putting that patient in the middle. What a lot of people don t know is Value-based Care can come in many different arrangements -- through an incentive-based plan with primary care physicians; a set of payments for bundled and episodic services or in the form of an Accountable Care Organization (ACO). Accountable Care Organization starts with high performing network providers. And through those high performing providers and Insurance Carriers, they are focused on managing a population. Through UnitedHealthCare and partners like Ochsner Health Network, we define quality metrics. Manage population according to those quality metrics to demonstrate savings and improved outcomes for the patients. It s about rewarding our partners in regards to value based outcomes versus fee for service. If you deliver Value-based Care well, by keeping that patient at the center, you hit the triple aim; that is, driving high quality, low cost, and better health outcomes. NATALIE CHANDLER MODERATOR CityBusiness Editor MEETING PARTICIPANTS DAVID CARMOUCHE CHRISTINE O BRIEN JOE OCHIPINTI WARNER THOMAS MD, Sr. VP and President, Ochsner Health Network VP of Key Account Sales and Account Management, UnitedHealthcare Gulf States President and CEO, UnitedHealthCare Gulf States President and CEO, Ochsner Health System CHANDLER: Why have you selected Ochsner s Health Network to partner with on an ACO? MD, Sr. Medical Director, UnitedHealthcare-Southeast Region Ochsner Health Network. I like to think about it as being proactive versus reactive. Historically in healthcare, we ve been reactive. For example, we wait for patients to come to the physician s office or to come to the emergency department. Today, we view it as being much more proactive. Conducting outreach to make sure people are getting their screenings and looking at it as a partnership with our patients to make sure they are working to live healthier more productive lives. We are working hard at a federal and state level to see the governmental programs change to embrace this type of pan mechanism with all insurers, including UnitedHealthcare, to try and change the way healthcare is reimbursed and to reward organizations that take this type of approach. Our partners across the Ochsner Health Network -- St. Tammany Parish Hospital, Slidell Memorial, Lafayette General Health and then Terrebonne General -- are all coming together to try and drive that agenda across the state for more affordable, better access and higher quality healthcare in the state. OCHIPINTI: UnitedHealthcare has been very fortunate to have a long-term relationship with Ochsner Health System. When I think about the three things I want in a successful relationship, not only in healthcare but primarily in driving Value-based Care, it is to be able to collaborate, create and connect. I ve only been in this role a little under a year, but I can tell you the collaboration from Dr. Carmouche, Warner and the Ochsner team has been terrific. Together we have created an integrated model and have been able to connect in the community. Now we have roughly over 25,000 members in our UnitedHealthcare Ochsner Health Network ACO. And we just happen to be in Louisiana, a state that when you look at the America s Health Rankings Report, which evaluates economics, public policy, healthcare and population, it continuously ranks in the bottom. So it s the ability to get out and help people live healthier lives, which is our mission at UnitedHealthcare, and I know a lot of what Ochsner Health Network The Value-Based Care Spectrum is focused on. Performance-Based CHANDLER: Warner, what should people in our region know Fee-for-Service about Ochsner Health Network? THOMAS: At Ochsner, we re focused on two particular things: One is to be a destination center for healthcare, a place that people travel far and wide to receive high-end quaternary care. Last year, we saw people from every parish in Louisiana, every state in the U.S. and 80 countries from around the world. These are services that people travel to New Orleans to receive this type of destination care. The second is being a Center of Excellence for population health and being an ACO which we re doing in conjunction with our partners through the PENNY S. WALKER Bundled Payments Accountable Care Programs Amount of Financial Accountability for Providers Key Characteristics Degree of Integration Between Provider and Health Plan Pay for Volume Performance-based contracts for doctors and hospitals Primary Care incentives Episode-based payments for specific conditions or medical specialties Accountable Care Organizations Capitation Sharing savings and/or risk
3 ROUNDTABLE CHANDLER: Dr. Carmouche, what should people in the region know about Ochsner Health Network? CARMOUCHE: When Warner asked me to take a leadership role at Ochsner Health Network, I was really gratified that they had picked the exact partners across each of their metro service areas in Louisiana that I would have chosen had I put a network together. First of all, I think we ve got a set of tremendously aligned partners -- aligned culturally and in our vision of what we re trying to deliver for Louisiana. None of us like the 50th health outcomes that we unfortunately suffer here. Most of us live here and raise our children here and want a better state. We view the network as a change agent and positive force for improving health. Secondly, we want people to view us as a partner to do this type of work with and it s a journey. What we like about our relationship with UnitedHealthcare and where we re going is that they re seeking to align the payment with what we re trying to do so that when we re successful at delivering better health outcomes at a lower price point, we win, UnitedHealthcare wins and UnitedHealthcare policyholders win. I think that s what excites us about this. CHANDLER: Joe, how many members and spending does UnitedHealthcare have under Value-based Care nationally and locally in Louisiana? OCHIPINTI: When you think about Value-based Care, you have to think of it in several different arrangements: primary care physician Value-Based Care Puts Consumers at the Center Health CONSUMER incentives; bundling episodic payments; and then the more comprehensive Accountable Care Organization. When you think of UnitedHealthcare nationally, you think of commercial and group insurance, Medicaid and Medicare. When you tie all that together, we are servicing about 15 million members under Value-based Care and that equates to about 52 billion dollars worth of total payment under Value-based Care. In Louisiana, Mississippi and the Gulf South region, we have just under 500,000 lives that we treat under a Value-based Care arrangement. That s about 850 million dollars worth of spend tied to value-based incentives. CHANDLER: Are there specific categories that UnitedHealthcare is focused on how Value-based Care gets delivered? OCHIPINTI: If you focus on what s core for an Accountable Care Organization, it s making sure the primary care physician and specialists are driving the care, while making sure we strengthen the personal connection between these physicians and the consumer. We want to simplify the interactions through technology, whether that s, integrating different systems to give that primary care physician or specialist a full view of that patients care, allowing them to provide the right care at the right time. When you tie the interactions together through technology, you empower the physicians and improve the consumer experience, and that s what I think we ve created here with our ACO with Ochsner Health Network. Care Value-based care is health care that works smarter and better to help people live healthier lives. This new model of health care promotes better health, better care and lower costs through innovative partnerships with care providers and consumers. 15 MILLION accustomed with working with in the past two years. In 2016, we launched three of the four: Gulf South Quality Network (April 2016), Hattiesburg Clinic (September 2016) in Mississippi and most recently, Franciscan Missionaries of Our Lady (FMOL) Health Leaders Network (October 2016). Each of these ACO s are establishing a personal connection with the patient. We are seeing Employer Groups sign up in these geographies to provide their employees greater access to care. We hope to see increased satisfaction between Providers, Employers and consumers through higher quality care, while seeing costs go down and improved outcomes on quality metrics defined in each of these ACO s. UnitedHealthcare members benefit from value-based programs. CHANDLER: Christine, how is your vision of an ACO product different from products that have been offered in the past? O BRIEN: Our ACO members will have a better overall healthcare experience and they re going to start with choosing a primary care physician for themselves and their family members. The primary care physician and the Ochsner physicians exclusively will help the patient and their families, guide them to make sure that they are proactively receiving care. Our members will receive timely and appropriate healthcare screenings and avoid the duplicate healthcare screenings that occur a lot of times when you re seeing multiple different providers in multiple different systems. And lastly, the primary care providers are going to help members manage chronic diseases such as diabetes, heart disease, and arthritis. We think in the end overall this will offer a better healthcare experience at a better cost and better care for the patient. CHANDLER: Is there a proven track record that demonstrates that ACOs perform better than non-acos? Health Physicians encourage patients to be active in their health care and to engage in dialogue about their diagnosis and treatment options. Actionable data shared with physicians makes it easier for them to close gaps in care with individual patients, such as a missed screening or follow-up appointment. Premium Tier 1 physicians assure consumers of measurably stronger outcomes. CHANDLER: How many ACOs and Value-based Care arrangements have you implemented in Louisiana and what do you hope to achieve? OCHIPINTI: There are several different arrangements. Within UnitedHealthcare in Louisiana when you think of primary care incentives, bundled payments and Accountable Care Organizations, we have over 300 arrangements that we have established today that span over about 191 hospital or physician contracts. Taking that to a more granular level, we really have four primary Accountable Care Organizations that provide coverage across the entire state of LA and Southern MS. Our first one launched in 2014 with Ochsner Health Network. That s been the more mature ACO that we ve been experienced and O BRIEN: Yes, there is. Commercial ACOs perform better than non-acos on 83 percent of the most common quality measures that we monitor. And ACOs have been proven to have fewer hospital admissions as well as fewer emergency room visits. The top ten percent of ACOs closed 74.7 of the care opportunities identified for patients versus 56 percent for non-acos. So this translates into better health for the patient, better care for the patient, as well as lower cost for both the patient and the employer. THOMAS: David, could you comment on the care gaps? CARMOUCHE: We have about 25 registries -- a conditioned defined list of patients who fall within a care gap and meet certain criteria -- that are live within our Epic (electronic medical record system) environment. For example, we populated our diabetes registry primarily patients receiving primary care at Ochsner Health System not including the network level -- and when we turned it on we identified about 46,000 care gaps. That could be a lab that hasn t been done on time or a patient who hasn t had an office visit in a reasonable period of time; a number of different things. What we re able to do now is create processes to conduct proactive outreach. We can do bulk orders; communicate via our secure portal, MyOchsner, that patients have
4 ROUNDTABLE access to; do direct mailings or text messages to outpatients to identify these care gaps. And when we did that, we expected about a 15 percent care gap closure. However, we were pleasantly surprised we had an 85 percent care gap closure. This is an incredible way for us to kind of keep track of patients who frequently just lose track themselves. I think we all have the experience through other industries, but frequently we don t get those kinds of reminders from the healthcare system. I think Ochsner has tried to correct that now. For 25 of the more common chronic conditions that we re interested in closing care gaps for, we have these registries and programs built and I think it s totally transformed how we think about patients. CHANDLER: To that point, how does Ochsner create and integrate its technology to offer integrated care? CARMOUCHE: It starts with Epic. Ochsner s made a major investment in one of the leading system wide electronic medical record systems in the country that we use in our hospital environment and in our ambulatory environment across all of Ochsner Health System and several of our partners who have chosen to go on our instance of Epic. I think that s allowed us to conduct numerous efforts like this proactive outreach and create care pathways and standardized care based on evidence-based medicine to reduce this kind of unnecessary variation that can exist in healthcare to drive better outcomes. We also extend that to our patients and some of the community physicians so patients have access through MyOchsner in order to be able to see their own office notes, go online to schedule their own appointments, review reminders and message their physician. There s a communication element to technology that I think goes a long way to putting the patient at the center of what we do. Additionally, technology that integrates with Epic allows us to deliver innovated care. For example, we have a hypertension program for patients who have poorly controlled blood pressure after so many months of routine care that we can refer patients to. It involves them having a Bluetooth-enabled mobile home blood pressure monitor that uploads blood pressures to an Apple phone into the cloud and into Epic so that a care team using an algorithm can in real time send prompts to patients and adjust medications based on these algorithms. We ve been very successful and about 80 percent of those patients are controlled at six months versus about 25 percent being controlled if they had stayed in their usual environment. Across the system and our whole network, we have providers who are on disparate electronic medical records systems (not Epic). We would like to connect the entire network and pair all claims data with clinical data so we ve made an investment to partner with IBM to use their Explorys product. We re in the process right now of taking in claims data from UnitedHealthcare and other payers and marrying that up with clinical data from different types of electronic medical records to see views of populations to help us drive performance across a much broader network. Those are just some of the examples that come to mind. But there s a lot of technology investment required to be a proactive healthcare system and be successful in this Value-based Care world. THOMAS: This goes back to regardless of which hospital, which clinic location, which imaging center you go to at Ochsner, all of your hospital and clinic data is in one location. As David indicated, we have now extended Epic to St. Tammany Parish Hospital and we re getting ready to install that at Premium Tier 1 physicians assure consumers of measurably stronger outcomes. Care Care providers have a complete view of patients health by sharing information among every health professional involved in an individual s treatment, from primary care physicians to specialists; from the ER to the local walk-in clinic. Consumers build stronger connections with their physicians, find it easier to access care (including home visits in some cases) and have more information at their fingertips. Care providers receive the time and compensation to provide more coordinated care which ultimately can reduce costs by minimizing unnecessary care such as re-hospitalization and redone procedures. Terrebonne General Medical Center and Slidell Memorial Hospital in We re really trying to be a much more consumer-focused organization because our patients are consumers, consumers of healthcare. CARMOUCHE: To add to that, I think the next iteration of how technology transforms healthcare is in telemedicine. Ochsner has been a leader in telemedicine -- telemedicine being hospital-to-hospital services in Louisiana. For example, we provide emergency room telestroke services to about 50 hospitals across the state and that s powerful. That allows these hospitals to have 24/7 access to a highly trained and skilled neurologist who can assess a patient in a remote emergency room somewhere and make a determination as to whether that patient may be appropriate to have a medication administered that could really reverse a stroke. It s a very time sensitive approach needed so that patients can have the best outcome. This has allowed many patients to stay and thrive in their local community hospital; whereas in the past, they would have probably not been assessed, not been offered that treatment, and been transferred to a center like Ochsner but outside a window where we could have really impacted them. It s about bringing healthcare to people where they are, where they work and at home through direct to consumer telemedicine. We re very excited that UnitedHealthcare is a big supporter of that. We all live on our smartphone and if we can deliver some services in a more convenient, safe and effective way, we certainly want to do that. And I think you ll continue to see us making those significant investments in CHANDLER: How does United share data with providers to impact clinical outcomes? WALKER: We receive data from laboratories, pharmacy claims and some actual claims, and we package that information for our physicians so that they can identify gaps in care, like those already mentioned, to help close those gaps. It helps compare themselves to their peers. Every specialty has things that they are supposed to do for the patients that they are seeing, so they can see if they are in line with that and also in line with the costs. The other thing that we do is we have real time data where we share ER visits and discharges from the hospital and that helps us activate our care coordination program and also helps us share that information with both physicians and hospitals so they can help prevent further ER visits. CHANDLER: What is UnitedHealthcare doing to support the most commonly cited challenges in value-based programs? WALKER: This is threefold. We definitely need to have a primary care focus. The primary care doctor is the coordinator of all the care. They can help the patient avoid admissions and make sure they have gaps in their care closed. Primary care physicians really need to be a champion in an ACO. When we have a physician champion, we ve seen the results like Christine and Dr. Carmouche mentioned. The second part of the ACO that we have noticed is data. It s very data driven, so we have provided daily reports, weekly reports, monthly reports, and quarterly reports, especially the real time reports and the ER information that is very important. Then, as you move further along, we help close gaps in care such as mammograms, colonoscopies, immunizations, things that patients wouldn t normally even think about. And then the third part is it s very important to have both the physician and executive champions. When a physician champion and an executive champion all meet up, it really helps provide that leadership that keeps an ACO functioning and very fruitful. CARMOUCHE: One study said that only about 50 percent of the care that an individual person should be getting based on the current evidence in their age and their conditions is actually being provided in the United States. That means
5 ROUNDTABLE reduce costs by minimizing unnecessary care such as re-hospitalization and redone procedures. Mobile tools and more transparent information make it easier to research and compare quality, cost and provider-specific information. Financial incentives reward consumers for choosing high-performing doctors who are identified as having measurably stronger outcomes. Learn more about UnitedHealthcare's approach to value-based care at about half the things that the best practices would suggest any individual should be doing or getting doesn t happen in this country. That is why we ve developed the registries mentioned earlier to hopefully better close those gaps in care. We also agree that the relationship between a personal physician or a primary care physician and a patient is critical to success. But physicians alone in traditional practices can t do this work. If you take all of the wellness needs of a population and then add in all the chronic disease needs of a population and then try to manage all the acute care needs walk-ins or urgent needs of a population, it would take about 16 hours a day for a typical panel size. When you start to understand that and when you start to have tools like Epic that allow you to identify all these care gaps, you rapidly start to realize that you need a care team who is jointly responsible for patients in making sure that we bring more than 50 percent of the appropriate care to these patients. It s not just about care gaps; it s about the care team and how we transformed our design of delivery care practices to become successful. CHANDLER: If you look a few years down the road, what do you see being offered in collaboration with Ochsner and UnitedHealthcare? OCHIPINTI: UnitedHealthcare brings national resources to our care provider relationships to strengthen how care is delivered locally. We have tremendous assets with technology and our Optum brand. We need to continue to collaborate on the learnings of how we re addressing the gaps in care and how we re integrating new areas like telemedicine. We need to maintain the strengths of Ochsner, FMOL, GSQN or Hattiesburg Clinic and together we can increase quality, drive down costs and create better outcomes to our consumers and employers. Employers want more access at affordable prices, consumers know their PCP and they have trust with their PCP. I expect to see more Value-based Care programs putting PCP s at the front entrance, but allowing consumers more flexibility in the ACO, while the care provider uses social media and interactive applications to engage with consumers at the right time and how they want to be engaged. THOMAS: The way I look at this is we need to make healthcare better in Louisiana and in the whole Gulf South. Ochsner Health System can t do it alone. And that s why Ochsner Health Network was created to bring in other like-minded organizations across the entire state so that we can change healthcare and change it to improve qualities, improve access to care and make healthcare more affordable. Ochsner Health System can t do that alone. The Ochsner Health Network with organizations like UnitedHealthcare and the other major insurers in the state -- Blue Cross, Humana and others -- all have to work together. Because at the end of the day, we re here -- we at Ochsner are here to serve the community. We re a not-for-profit organization. We give back to the community. The relationships like what we re talking about with UnitedHealthcare are important to allow us to make sure we have the right financial models set up that facilitate all the things we talked about today with care gaps, with proactive versus reactive type of care. We have to work together to engage employers and their employees in a very different conversation so that they can. People want to be healthy, but we have to remind them, make it obvious and handle this in a different way. I think one of our key goals is to also engage more with employers to help them think about how they can do this with their employee base. We re a healthcare provider, but we re also the largest private employer in the State of Louisiana employing over 17,000 people so we really kind of look at it on both sides. How do we help our own employees live healthier lives and take the strategies and ideas we have there and bring them to other employers? At the end of the day, it s about making healthcare better and relationships like what we have with Joe and with UnitedHealthcare are critical to that. We need to continue to build our relationships with our partners in Ochsner Health Network. Together, we can and will change healthcare in the state and that is our goal over the next couple of years. CARMOUCHE: I d like to just pick up a little bit on what Warner said about our thoughts around employers and how we want to work with employers. I think the fact of the matter is most people access healthcare services through their insurance products. I think if you think about it, all of the great things that we ve talked about that Ochsner s investing in and doing are sometimes not easily translated to the actual individual consumer who s purchasing an insurance product that then allows them access to healthcare services. So from our perspective, the value proposition of working as an ACO with UnitedHealthcare is to hopefully have those folks help bring our story to employers who are offering insurance benefits to their employees. The types of products that have been sold in Louisiana traditionally have been broad access products. I think what all of us are recognizing is that if we really want to create the optimal care experience, an organized experience, a coordinated experience where the information flows to patients and across providers, we can t do that easily in broad networks. So I think for Ochsner what we d like to see from UnitedHealthcare is assistance in translating what they know as to be good work and a better care experience and better health outcomes into the insurance products that they sell to employers. I think if we re successful at doing our part, then we would hope that our partners can help better position us with employers who are increasingly looking to avoid a 10 percent annual increase in their premium or increasingly looking to these new types of relationships and narrower higher performing network type products to drive value for their employees. THOMAS: The other thing is this is not just Ochsner Clinic physicians. Within Ochsner Health Network, we have hundreds of community physicians that we re working with. For example, St. Tammany Parish Hospital has partnered with their physicians to create St. Tammany Quality Network who are many community physicians that are coming together along with these same goals of improving quality, improving access, reducing cost. Ochsner is partnering with hundreds of community physicians to help them understand and create models that work for them and really continue to make sure we re proactive within our entire network, not just in the Ochsner Clinic. I was sitting here thinking about how do we know we re successful when we re really making progress here. To me when we are successful, we re going to have people come up to us saying, Thank you for helping me or my husband keep his blood pressure under control or Thank you for helping my wife keep her diabetes under control. We ll be successful when we are making sure we re addressing chronic disease in the right way. Part of our job is to make sure that we re continuing to communicate and educate our patients and the insurer, the employer, and the individual to make sure they re being proactive to deal with these preventative challenges. We re human and we forget about these things sometimes, but it s so important: the wellness activities, the being proactive around your health and your own life. That would be great success and I think that s coming in the near future. O BRIEN: We continue to work very closely with Ochsner and the other ACO partner s that Joe mentioned to use data to offer ACO-type products and develop plan designs that Employers want in the marketplace. If you offer a benefit design that supports an integrated experience for the consumer, greater access to care and that model offers an affordable plan and coverage to a family and to an employer, it is a win for all parties involved. CHANDLER: Thank you all so much for participating in this round table discussion. CHANDLER: Does anybody else have anything to add?
6 Consumers are at the center with Value-based Care Value-based Care is health care that works smarter and better to help people live healthier lives. It s a health care model that promotes better health, better care and lower costs through innovative partnerships with care providers and consumers. 15 MILLION UnitedHealthcare members benefit from value-based programs. Health Consumer Care Health Physicians encourage patients to be active in their health care and to be engaged in their diagnosis and treatment options. Actionable data shared with physicians, such as a missed screening or follow-up appointment, makes it easier to close gaps in care with individual patients. Premium Tier 1 physicians assure consumers of measurably stronger outcomes. Care Care providers have a complete view of patients health by sharing information among every health professional involved in an individual s treatment, from a doctor at a walk-in clinic to a specialist. Consumers build stronger connections with their physicians, find it easier to access care (including home visits in some cases) and have more information at their fingertips. Care providers receive the time and compensation to provide more coordinated care which ultimately can reduce costs by minimizing unnecessary care such as re-hospitalization and redone procedures. Mobile tools and more transparent information make it easier to research and compare quality, cost and provider-specific information. Financial incentives reward consumers for choosing high-performing doctors who are identified as having measurably stronger outcomes. Learn more about UnitedHealthcare s approach to Value-based Care at uhc.com/valuebasedcare Insurance coverage provided by or through UnitedHealthcare Insurance Company or its affiliates. Administrative services provided by United HealthCare Services, Inc. or their affiliates. MT / United HealthCare Services, Inc
Collaborative and Coordinated:
 Collaborative and Coordinated: How Value-Based Care Programs are Driving Improvements in Quality and People s Health ISSUE DATE: NOVEMBER 2016 INTRODUCTION How the Shift from Volume to Value is Driving
Collaborative and Coordinated: How Value-Based Care Programs are Driving Improvements in Quality and People s Health ISSUE DATE: NOVEMBER 2016 INTRODUCTION How the Shift from Volume to Value is Driving
Value-based Care Report. February How Value-based Care is improving quality and health.
 Value-based Care Report February 2018 How Value-based Care is improving quality and health. 1 Value-based Care means better health, better care and lower costs. Placing greater emphasis on value in health
Value-based Care Report February 2018 How Value-based Care is improving quality and health. 1 Value-based Care means better health, better care and lower costs. Placing greater emphasis on value in health
Value-based Care. Fact Sheet. How Value-based Care is improving quality and health.
 How is improving quality and health. Working Smarter and Better to Help People Live Healthier Lives can help you lead the healthiest life possible. Imagine every health care professional you see understanding
How is improving quality and health. Working Smarter and Better to Help People Live Healthier Lives can help you lead the healthiest life possible. Imagine every health care professional you see understanding
Health plans for New Hampshire small businesses Available through the Health Insurance Marketplace
 Health plans for New Hampshire small businesses Available through the Health Insurance Marketplace 1 38476NHEENABS Rev. 09/14 We can help you navigate the health care road We re here to help. In fact,
Health plans for New Hampshire small businesses Available through the Health Insurance Marketplace 1 38476NHEENABS Rev. 09/14 We can help you navigate the health care road We re here to help. In fact,
All ACO materials are available at What are my network and plan design options?
 ACO Toolkit: A Roadmap for Employers What is an ACO? Is an ACO strategy right for my company? Which ACOs are ready? All ACO materials are available at www.businessgrouphealth.org What are my network and
ACO Toolkit: A Roadmap for Employers What is an ACO? Is an ACO strategy right for my company? Which ACOs are ready? All ACO materials are available at www.businessgrouphealth.org What are my network and
POPULATION HEALTH PLAYBOOK. Mark Wendling, MD Executive Director LVPHO/Valley Preferred 1
 POPULATION HEALTH PLAYBOOK Mark Wendling, MD Executive Director LVPHO/Valley Preferred www.populytics.com 1 Today s Agenda Outline LVHN, LVPHO and Populytics Overview Population Health Approach Population
POPULATION HEALTH PLAYBOOK Mark Wendling, MD Executive Director LVPHO/Valley Preferred www.populytics.com 1 Today s Agenda Outline LVHN, LVPHO and Populytics Overview Population Health Approach Population
Value-based Care Report. February How Value-based Care is improving quality and health.
 Value-based Care Report February 2018 How Value-based Care is improving quality and health. Value-based Care delivers: Value-based Care means better health, better care and lower costs. Placing greater
Value-based Care Report February 2018 How Value-based Care is improving quality and health. Value-based Care delivers: Value-based Care means better health, better care and lower costs. Placing greater
PATH Program. Getting Started Guide
 PATH Program Getting Started Guide We have a BIG opportunity. Together, we can empower and encourage people to take an active role in their health. Preventive health care services help people find and
PATH Program Getting Started Guide We have a BIG opportunity. Together, we can empower and encourage people to take an active role in their health. Preventive health care services help people find and
Integrated Health System
 Integrated Health System Please note that the views expressed are those of the conference speakers and do not necessarily reflect the views of the American Hospital Association and Health Forum. Page 2
Integrated Health System Please note that the views expressed are those of the conference speakers and do not necessarily reflect the views of the American Hospital Association and Health Forum. Page 2
Using Data for Proactive Patient Population Management
 Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
UnitedHealth Center for Health Reform & Modernization September 2014
 Health Reform & Modernization September 2014 2014 UnitedHealth Group. Any use, copying or distribution without written permission from UnitedHealth Group is prohibited. Overview Why Focus on Primary Care?
Health Reform & Modernization September 2014 2014 UnitedHealth Group. Any use, copying or distribution without written permission from UnitedHealth Group is prohibited. Overview Why Focus on Primary Care?
Patient-Centered Medical Home 101: General Overview
 Patient-Centered Medical Home 101: General Overview Publicly Available Slide Deck Last Updated: January 2015 Suggested Citation: PCPCC Map Tools. (2015). Patient-Centered Medical Home 101: General Overview.
Patient-Centered Medical Home 101: General Overview Publicly Available Slide Deck Last Updated: January 2015 Suggested Citation: PCPCC Map Tools. (2015). Patient-Centered Medical Home 101: General Overview.
Managing Population Health in Northeast Georgia: One Medical Group's Experience
 September 21, 2013 Managing Population Health in Northeast Georgia: One Medical Group's Experience By Mark Hagland Northeast Georgia Physicians Group (NGPG), based in Gainesville, Georgia, a suburb of
September 21, 2013 Managing Population Health in Northeast Georgia: One Medical Group's Experience By Mark Hagland Northeast Georgia Physicians Group (NGPG), based in Gainesville, Georgia, a suburb of
A strategy for building a value-based care program
 3M Health Information Systems A strategy for building a value-based care program How data can help you shift to value from fee-for-service payment What is value-based care? Value-based care is any structure
3M Health Information Systems A strategy for building a value-based care program How data can help you shift to value from fee-for-service payment What is value-based care? Value-based care is any structure
Value-Based Contracting
 Value-Based Contracting AUTHOR Melissa Stahl Research Manager, The Health Management Academy 2018 Lumeris, Inc 1.888.586.3747 lumeris.com Introduction As the healthcare industry continues to undergo transformative
Value-Based Contracting AUTHOR Melissa Stahl Research Manager, The Health Management Academy 2018 Lumeris, Inc 1.888.586.3747 lumeris.com Introduction As the healthcare industry continues to undergo transformative
Central Ohio Primary Care (COPC) Spotlight on Innovation
 Central Ohio Primary Care (COPC) Spotlight on Innovation BY BETTER MEDICARE ALLIANCE MARCH 2017 Central Ohio Primary Care Spotlight on Innovation 1 Central Ohio Primary Care (COPC) Spotlight on Innovation
Central Ohio Primary Care (COPC) Spotlight on Innovation BY BETTER MEDICARE ALLIANCE MARCH 2017 Central Ohio Primary Care Spotlight on Innovation 1 Central Ohio Primary Care (COPC) Spotlight on Innovation
Value-Based Care Contracting and Legal Issues
 Session 4b Value-Based Care Contracting and Legal Issues Presented by: Janet Walker Farrer General Counsel and Insurance Legal Department Chair Ascension Health Leah Stewart Associate Vice President for
Session 4b Value-Based Care Contracting and Legal Issues Presented by: Janet Walker Farrer General Counsel and Insurance Legal Department Chair Ascension Health Leah Stewart Associate Vice President for
Disconnects in Transforming Health Care Delivery. How Executives, Clinical Leaders, and Clinicians Must Bridge Their Divide and Move Forward Together
 Disconnects in Transforming Health Care Delivery How Executives, Clinical Leaders, and Must Bridge Their Divide and Move Forward Together Disconnects in Transforming Health Care Delivery 2 Over the past
Disconnects in Transforming Health Care Delivery How Executives, Clinical Leaders, and Must Bridge Their Divide and Move Forward Together Disconnects in Transforming Health Care Delivery 2 Over the past
Program Overview
 2015-2016 Program Overview 04HQ1421 R03/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health Service
2015-2016 Program Overview 04HQ1421 R03/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health Service
ACOs: California Style
 ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
Healthcare 2015: Win-win or lose-lose?
 IBM Institute for Business Value Healthcare 2015: Win-win or lose-lose? A portrait and a path to successful transformation Presented at Disease Management Colloquium May 19, 2008 Jim Adams, IBM Center
IBM Institute for Business Value Healthcare 2015: Win-win or lose-lose? A portrait and a path to successful transformation Presented at Disease Management Colloquium May 19, 2008 Jim Adams, IBM Center
Sample Exam Case Studies/Questions
 Module II of the CHFP Program: HFMA's Operational Excellence exam Sample Exam Case Studies/Questions The intent of the Operational Excellence exam is for you to exhibit your mastery of the information
Module II of the CHFP Program: HFMA's Operational Excellence exam Sample Exam Case Studies/Questions The intent of the Operational Excellence exam is for you to exhibit your mastery of the information
Decreasing Medical. Costs. Are your members listening to you? PRESENTED BY: September 22, 2016
 Decreasing Medical Costs Are your members listening to you? PRESENTED BY: Aaron Crowell, Executive Vice President, MTM, Inc. Gary Jacobs, Executive Vice President, CareCentrix Dan Masciopinto, SVP of Product,
Decreasing Medical Costs Are your members listening to you? PRESENTED BY: Aaron Crowell, Executive Vice President, MTM, Inc. Gary Jacobs, Executive Vice President, CareCentrix Dan Masciopinto, SVP of Product,
OVERVIEW. Helping people live healthier lives and helping make the health system work better for everyone
 OVERVIEW Helping people live healthier lives and helping make the health system work better for everyone About UnitedHealth Group UnitedHealth Group helps drive positive change in health care in the United
OVERVIEW Helping people live healthier lives and helping make the health system work better for everyone About UnitedHealth Group UnitedHealth Group helps drive positive change in health care in the United
MAKING PROGRESS, SEEING RESULTS
 MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
Population Health. Driving local and population health. Being the trusted partner for doctors and health care systems, we re changing how
 02 Population Health Driving local and population health Being the trusted partner for doctors and health care systems, we re changing how people interact with the system to make it easier to navigate
02 Population Health Driving local and population health Being the trusted partner for doctors and health care systems, we re changing how people interact with the system to make it easier to navigate
Telehealth: Overcoming the challenges of implementing innovative health care solutions
 Telehealth: Overcoming the challenges of implementing innovative health care solutions NRTRC 5 TH ANNUAL CONFERENCE MARCH 22, 2016 ROKI CHAUHAN, MD, FAAFP Disclaimer 2 The material presented here is being
Telehealth: Overcoming the challenges of implementing innovative health care solutions NRTRC 5 TH ANNUAL CONFERENCE MARCH 22, 2016 ROKI CHAUHAN, MD, FAAFP Disclaimer 2 The material presented here is being
Managing Patients with Multiple Chronic Conditions
 Best Practices Managing Patients with Multiple Chronic Conditions Fletcher Allen Health Care Case Study Organization Profile Located in Burlington, Fletcher Allen Health Care (FAHC) is Vermont s university
Best Practices Managing Patients with Multiple Chronic Conditions Fletcher Allen Health Care Case Study Organization Profile Located in Burlington, Fletcher Allen Health Care (FAHC) is Vermont s university
Examining the Differences Between Commercial and Medicare ACO Models
 Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
Payer Perspectives On Value-based Contracting
 Payer Perspectives On Value-based Contracting Miles Snowden, MD, MPH, CEBS Chief Medical Officer 1 A simple goal Making the health system work better for everyone 2 Optum serves 60,000,000+ individuals
Payer Perspectives On Value-based Contracting Miles Snowden, MD, MPH, CEBS Chief Medical Officer 1 A simple goal Making the health system work better for everyone 2 Optum serves 60,000,000+ individuals
Medicare Quality Payment Program: Deep Dive FAQs for 2017 Performance Year Hospital-Employed Physicians
 Medicare Quality Payment Program: Deep Dive FAQs for 2017 Performance Year Hospital-Employed Physicians This document supplements the AMA s MIPS Action Plan 10 Key Steps for 2017 and provides additional
Medicare Quality Payment Program: Deep Dive FAQs for 2017 Performance Year Hospital-Employed Physicians This document supplements the AMA s MIPS Action Plan 10 Key Steps for 2017 and provides additional
Long term commitment to a new vision. Medical Director February 9, 2011
 ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
Accountable Care: Clinical Integration is the Foundation
 Solutions for Value-Based Care Accountable Care: Clinical Integration is the Foundation CLINICAL INTEGRATION CARE COORDINATION ACO INFORMATION TECHNOLOGY FINANCIAL MANAGEMENT The Accountable Care Organization
Solutions for Value-Based Care Accountable Care: Clinical Integration is the Foundation CLINICAL INTEGRATION CARE COORDINATION ACO INFORMATION TECHNOLOGY FINANCIAL MANAGEMENT The Accountable Care Organization
Introduction for New Mexico Providers. Corporate Provider Network Management
 Introduction for New Mexico Providers Corporate Provider Network Management Overview New Mexico snapshot. Who we are. Why Medicaid managed care? Why AmeriHealth Caritas? Why partner with us? Medical Management
Introduction for New Mexico Providers Corporate Provider Network Management Overview New Mexico snapshot. Who we are. Why Medicaid managed care? Why AmeriHealth Caritas? Why partner with us? Medical Management
ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods
 A unique vision for an ever-changing healthcare environment ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods Presented by Joe Laden, President, ORVA, LLC The Environment
A unique vision for an ever-changing healthcare environment ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods Presented by Joe Laden, President, ORVA, LLC The Environment
Population Health or Single-payer The future is in our hands. Robert J. Margolis, MD
 Population Health or Single-payer The future is in our hands Robert J. Margolis, MD Today s problems Interim steps Population health Alternatives Conclusions Outline $3,000,000,000,000 $1,000,000,000,000
Population Health or Single-payer The future is in our hands Robert J. Margolis, MD Today s problems Interim steps Population health Alternatives Conclusions Outline $3,000,000,000,000 $1,000,000,000,000
YOUR TRUSTED HEALTH COMPANION. A plan for life.
 YOUR TRUSTED HEALTH COMPANION A plan for life. Being healthy is about more than preventing illness. It s achieving the best possible quality of life, physically and emotionally. That s what CDPHP is all
YOUR TRUSTED HEALTH COMPANION A plan for life. Being healthy is about more than preventing illness. It s achieving the best possible quality of life, physically and emotionally. That s what CDPHP is all
3 Ways to Increase Patient Visits
 3 Ways to Increase Patient Visits 3 Ways to Increase Patient Visits www.kareo.com kareo.com Table of Contents Introduction 03 Create an Effective Recall/Recare Program 04 Build and Manage Your Online Presence
3 Ways to Increase Patient Visits 3 Ways to Increase Patient Visits www.kareo.com kareo.com Table of Contents Introduction 03 Create an Effective Recall/Recare Program 04 Build and Manage Your Online Presence
THE NEW IMPERATIVE: WHY HEALTHCARE ORGANIZATIONS ARE SEEKING TRANSFORMATIONAL CHANGE AND HOW THEY CAN ACHIEVE IT
 Today s challenges are not incremental, but transformational; across the country, many CEOs and executives in healthcare see the need not merely to improve traditional ways of doing business, but to map
Today s challenges are not incremental, but transformational; across the country, many CEOs and executives in healthcare see the need not merely to improve traditional ways of doing business, but to map
Adopting a Care Coordination Strategy
 Adopting a Care Coordination Strategy Authors: Henna Zaidi, Manager, and Catherine Castillo, Senior Consultant Current state of health care The traditional approach to health care delivery is quickly becoming
Adopting a Care Coordination Strategy Authors: Henna Zaidi, Manager, and Catherine Castillo, Senior Consultant Current state of health care The traditional approach to health care delivery is quickly becoming
Creating a Patient-Centered Payment System to Support Higher-Quality, More Affordable Health Care. Harold D. Miller
 Creating a Patient-Centered Payment System to Support Higher-Quality, More Affordable Health Care Harold D. Miller First Edition October 2017 CONTENTS EXECUTIVE SUMMARY... i I. THE QUEST TO PAY FOR VALUE
Creating a Patient-Centered Payment System to Support Higher-Quality, More Affordable Health Care Harold D. Miller First Edition October 2017 CONTENTS EXECUTIVE SUMMARY... i I. THE QUEST TO PAY FOR VALUE
TKG Health Systems Advisory Panel Meeting. Healthcare in 2017: Trends & Hot Topics. Tuesday, March 24 th, 2017 Gaylord Texan Resort, Grapevine, TX
 TKG Health Systems Advisory Panel Meeting Healthcare in 2017: Trends & Hot Topics Tuesday, March 24 th, 2017 Gaylord Texan Resort, Grapevine, TX Executive Summary Key Trends The transition to value-based
TKG Health Systems Advisory Panel Meeting Healthcare in 2017: Trends & Hot Topics Tuesday, March 24 th, 2017 Gaylord Texan Resort, Grapevine, TX Executive Summary Key Trends The transition to value-based
The influx of newly insured Californians through
 January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
Improvement Happens: An Interview with Deeb Salem, MD and Brian Cohen, MD
 INNOVATION AND IMPROVEMENT Improvement Happens: An Interview with Deeb Salem, MD and Brian Cohen, MD Matthew J. Press, MD, MSc Departments of Public Health and Medicine, Weill Cornell Medical College,
INNOVATION AND IMPROVEMENT Improvement Happens: An Interview with Deeb Salem, MD and Brian Cohen, MD Matthew J. Press, MD, MSc Departments of Public Health and Medicine, Weill Cornell Medical College,
Health plans for Maine small businesses Available through the Health Insurance Marketplace
 Health plans for Maine small businesses Available through the Health Insurance Marketplace Effective January 1, 2016 We can help you navigate the health care road We re here to help. In fact, for more
Health plans for Maine small businesses Available through the Health Insurance Marketplace Effective January 1, 2016 We can help you navigate the health care road We re here to help. In fact, for more
Prevea Health Automates Population Health Management and Improves Health Outcomes
 CASE STUDY Prevea Health Prevea Health Automates Population Health Management and Improves Health Outcomes After adopting the patient-centered medical home care delivery model to improve the health and
CASE STUDY Prevea Health Prevea Health Automates Population Health Management and Improves Health Outcomes After adopting the patient-centered medical home care delivery model to improve the health and
The Digital Transformation Of Healthcare. Warner Thomas, President & CEO Ochsner Health System
 The Digital Transformation Of Healthcare Warner Thomas, President & CEO Ochsner Health System Ochsner Health System Our Mission is to Serve, Heal, Lead, Educate, and Innovate Largest Health System In Gulf
The Digital Transformation Of Healthcare Warner Thomas, President & CEO Ochsner Health System Ochsner Health System Our Mission is to Serve, Heal, Lead, Educate, and Innovate Largest Health System In Gulf
REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN
 REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN Supporting Collaborative Regional Approaches to Sustainable High-Value Healthcare Harold D. Miller President and CEO Center for Healthcare
REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN Supporting Collaborative Regional Approaches to Sustainable High-Value Healthcare Harold D. Miller President and CEO Center for Healthcare
CPC+ CHANGE PACKAGE January 2017
 CPC+ CHANGE PACKAGE January 2017 Table of Contents CPC+ DRIVER DIAGRAM... 3 CPC+ CHANGE PACKAGE... 4 DRIVER 1: Five Comprehensive Primary Care Functions... 4 FUNCTION 1: Access and Continuity... 4 FUNCTION
CPC+ CHANGE PACKAGE January 2017 Table of Contents CPC+ DRIVER DIAGRAM... 3 CPC+ CHANGE PACKAGE... 4 DRIVER 1: Five Comprehensive Primary Care Functions... 4 FUNCTION 1: Access and Continuity... 4 FUNCTION
Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model. The New Accountable Care Business Model
 Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model Michael C. Tobin, D.O., M.B.A. Interim Chief medical Officer Health Networks February 12, 2011 2011 North Iowa
Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model Michael C. Tobin, D.O., M.B.A. Interim Chief medical Officer Health Networks February 12, 2011 2011 North Iowa
Patient Engagement in the Population Health Management Era
 Patient Engagement in the Population Health Management Era Creagh Milford, DO, MPH President, Population Health Services A Catholic healthcare ministry serving Ohio and Kentucky Agenda Agenda I. Overview
Patient Engagement in the Population Health Management Era Creagh Milford, DO, MPH President, Population Health Services A Catholic healthcare ministry serving Ohio and Kentucky Agenda Agenda I. Overview
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP)
 BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
Curley s Secret of Life : VBID and Payment Reform
 1 Curley s Secret of Life : VBID and Payment Reform Lewis G. Sandy MD SVP, Clinical Advancement, UnitedHealth Group UnitedHealth Center for Health Reform and Modernization University of Michigan Center
1 Curley s Secret of Life : VBID and Payment Reform Lewis G. Sandy MD SVP, Clinical Advancement, UnitedHealth Group UnitedHealth Center for Health Reform and Modernization University of Michigan Center
Executive Summary 1. Better Health. Better Care. Lower Cost
 Executive Summary 1 To build a stronger Michigan, we must build a healthier Michigan. My vision is for Michiganders to be healthy, productive individuals, living in communities that support health and
Executive Summary 1 To build a stronger Michigan, we must build a healthier Michigan. My vision is for Michiganders to be healthy, productive individuals, living in communities that support health and
Draft Covered California Delivery Reform Contract Provisions Comments Welcome and Encouraged
 TO: FROM: RE: State Based Marketplaces State Medicaid Directors Delivery Reform/Value Promoting Colleagues Peter V. Lee, Executive Director Draft Covered California Delivery Reform Contract Provisions
TO: FROM: RE: State Based Marketplaces State Medicaid Directors Delivery Reform/Value Promoting Colleagues Peter V. Lee, Executive Director Draft Covered California Delivery Reform Contract Provisions
CoxHealth: A Case Study in Launching a Co-Branded Medicare Advantage Plan
 CoxHealth: A Case Study in Launching a Co-Branded Medicare Advantage Plan Guiding a Health System s Journey to Value with a Collaborative Payer Partner Situation $1.3 billion, five-hospital system in the
CoxHealth: A Case Study in Launching a Co-Branded Medicare Advantage Plan Guiding a Health System s Journey to Value with a Collaborative Payer Partner Situation $1.3 billion, five-hospital system in the
Medicaid Payment Reform at Scale: The New York State Roadmap
 Medicaid Payment Reform at Scale: The New York State Roadmap ASTHO Technical Assistance Call June 22 nd 2015 Greg Allen Policy Director New York State Medicaid Overview Background and Brief History Delivery
Medicaid Payment Reform at Scale: The New York State Roadmap ASTHO Technical Assistance Call June 22 nd 2015 Greg Allen Policy Director New York State Medicaid Overview Background and Brief History Delivery
Thought Leadership Series White Paper The Journey to Population Health and Risk
 AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
Technology Driven Strategies for Enhancing Patient Engagement Within an ACO Model. ACO Congress November 5, 2013 Charles Kennedy
 Technology Driven Strategies for Enhancing Patient Engagement Within an ACO Model ACO Congress November 5, 2013 Charles Kennedy Aetna s values drive ACS strategy apple 2 Changing the emphasis from volume
Technology Driven Strategies for Enhancing Patient Engagement Within an ACO Model ACO Congress November 5, 2013 Charles Kennedy Aetna s values drive ACS strategy apple 2 Changing the emphasis from volume
Coastal Medical, Inc.
 A Culture of Collaboration The Organization Physician-owned group Currently 19 offices across the state of Rhode Island and growing 85 physicians, 101 care providers The Challenge Implement a single, unified
A Culture of Collaboration The Organization Physician-owned group Currently 19 offices across the state of Rhode Island and growing 85 physicians, 101 care providers The Challenge Implement a single, unified
Jumpstarting population health management
 Jumpstarting population health management Issue Brief April 2016 kpmg.com Table of contents Taking small, tangible steps towards PHM for scalable achievements 2 The power of PHM: Five steps 3 Case study
Jumpstarting population health management Issue Brief April 2016 kpmg.com Table of contents Taking small, tangible steps towards PHM for scalable achievements 2 The power of PHM: Five steps 3 Case study
Better, Smarter, Healthier: In historic announcement, HHS sets clear goals and timeline for shifting Medicare reimbursements from volume to value
 Page 1 of 5 HHS.gov U.S. Department of Health & Human Services FOR IMMEDIATE RELEASE January 26, 2015 Contact: HHS Press Office 202-690-6343 Better, Smarter, Healthier: In historic announcement, HHS sets
Page 1 of 5 HHS.gov U.S. Department of Health & Human Services FOR IMMEDIATE RELEASE January 26, 2015 Contact: HHS Press Office 202-690-6343 Better, Smarter, Healthier: In historic announcement, HHS sets
Patient Payment Check-Up
 Patient Payment Check-Up SURVEY REPORT 2017 Attitudes and behavior among those billing for healthcare and those paying for it CONDUCTED BY 2017 Patient Payment Check-Up Report 1 Patient demand is ahead
Patient Payment Check-Up SURVEY REPORT 2017 Attitudes and behavior among those billing for healthcare and those paying for it CONDUCTED BY 2017 Patient Payment Check-Up Report 1 Patient demand is ahead
Executive Summary. Leadership Toolkit for Redefining the H: Engaging Trustees and Communities
 Executive Summary Leadership Toolkit for Redefining the H: Engaging Trustees and Communities Report produced by the AHA Committee on Research and Committee on Performance Improvement 2015 Executive Summary
Executive Summary Leadership Toolkit for Redefining the H: Engaging Trustees and Communities Report produced by the AHA Committee on Research and Committee on Performance Improvement 2015 Executive Summary
For fully insured groups of 100 or more eligible employees. HealthyOutcomes. A fully-integrated health management solution that works for you
 For fully insured groups of 100 or more eligible employees HealthyOutcomes wellness case management condition care maternity A fully-integrated health management solution that works for you HealthyOutcomes
For fully insured groups of 100 or more eligible employees HealthyOutcomes wellness case management condition care maternity A fully-integrated health management solution that works for you HealthyOutcomes
Building the Universal Roadmap to Population Health Management
 Building the Universal Roadmap to Population Health Management Executive Webinar January 21, 2016 Karen Handmaker, MPP, PCMH CCE IBM Watson Health House Keeping 1. Using the control panel Use the control
Building the Universal Roadmap to Population Health Management Executive Webinar January 21, 2016 Karen Handmaker, MPP, PCMH CCE IBM Watson Health House Keeping 1. Using the control panel Use the control
 As healthcare moves toward value-based care and risk-sharing payment models, many hospitals are taking a new look at ambulatory surgery centers (ASCs) as a transformational outpatient strategy with potential
As healthcare moves toward value-based care and risk-sharing payment models, many hospitals are taking a new look at ambulatory surgery centers (ASCs) as a transformational outpatient strategy with potential
Improving Diabetes Care in 75 Minutes. Moderator: Jerry Penso, M.D., M.B.A., President & CEO, AMGA
 Improving Diabetes Care in 75 Minutes Moderator: Jerry Penso, M.D., M.B.A., President & CEO, AMGA SESSION OBJECTIVES 1. Identify specific tactics that health care delivery systems can implement to improve
Improving Diabetes Care in 75 Minutes Moderator: Jerry Penso, M.D., M.B.A., President & CEO, AMGA SESSION OBJECTIVES 1. Identify specific tactics that health care delivery systems can implement to improve
The Evolution of ASC Joint Ventures: Key Trends for Value-Based Care
 The Evolution of ASC Joint Ventures: Key Trends for Value-Based Care The Evolution of ASC Joint Ventures: Key Trends for Value-Based Care By Laura Dyrda As healthcare moves toward value-based care and
The Evolution of ASC Joint Ventures: Key Trends for Value-Based Care The Evolution of ASC Joint Ventures: Key Trends for Value-Based Care By Laura Dyrda As healthcare moves toward value-based care and
Low Income Pool (LIP) Tier One Milestone (STC-61) Application for Enhancement Projects. Submitted by:
 2012-2013 Low Income Pool (LIP) Tier One Milestone (STC-61) Application for Enhancement Projects Submitted by: Florida Health Sciences Center, Inc. d/b/a Tampa General Hospital July 31, 2012 1 1. Applicant:
2012-2013 Low Income Pool (LIP) Tier One Milestone (STC-61) Application for Enhancement Projects Submitted by: Florida Health Sciences Center, Inc. d/b/a Tampa General Hospital July 31, 2012 1 1. Applicant:
Event Summary The State of Adoption in Value-Based Health Care
 Event Summary The State of Adoption in Value-Based Health Care 2015 Sponsored by THE STATE OF ADOPTION IN VALUE-BASED HEALTH CARE FEATURING Michael E. Porter, Bishop William Lawrence University Professor,
Event Summary The State of Adoption in Value-Based Health Care 2015 Sponsored by THE STATE OF ADOPTION IN VALUE-BASED HEALTH CARE FEATURING Michael E. Porter, Bishop William Lawrence University Professor,
Roadmap for Transforming America s Health Care System
 Roadmap for Transforming America s Health Care System America s health care system requires transformational change to provide all health care participants with broader access and choice, improved quality
Roadmap for Transforming America s Health Care System America s health care system requires transformational change to provide all health care participants with broader access and choice, improved quality
ACO Practice Transformation Program
 ACO Overview ACO Practice Transformation Program PROGRAM OVERVIEW As healthcare rapidly transforms to new value-based payment systems, your level of success will dramatically improve by participation in
ACO Overview ACO Practice Transformation Program PROGRAM OVERVIEW As healthcare rapidly transforms to new value-based payment systems, your level of success will dramatically improve by participation in
CEOCFO Magazine. Andy Reeves, RPh Chief Executive Officer OptiMed Specialty Pharmacy
 CEOCFO Magazine ceocfointerviews.com All rights reserved! Issue: October 30, 2017 Q&A with Andy Reeves, RPh, CEO of OptiMed Specialty Pharmacy, a National Specialty and Infusion Pharmacy dedicated to Managing
CEOCFO Magazine ceocfointerviews.com All rights reserved! Issue: October 30, 2017 Q&A with Andy Reeves, RPh, CEO of OptiMed Specialty Pharmacy, a National Specialty and Infusion Pharmacy dedicated to Managing
TELEHEALTH INDEX: 2015 PHYSICIAN SURVEY
 TELEHEALTH INDEX: 2015 PHYSICIAN SURVEY Overview Telehealth is accelerating in 2015. As many as 37% of hospital systems have at least one type of telemedicine solution to meet a variety of objectives,
TELEHEALTH INDEX: 2015 PHYSICIAN SURVEY Overview Telehealth is accelerating in 2015. As many as 37% of hospital systems have at least one type of telemedicine solution to meet a variety of objectives,
Healthy Aging Recommendations 2015 White House Conference on Aging
 Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
Health Information Technology
 ACO Congress Oct 25, 2010 Los Angeles, CA Patient Centered Medical Home and Accountable Care Organizations Health Information Technology David K. Nace MD, Medical Director, McKesson Corporation Co-Chair,
ACO Congress Oct 25, 2010 Los Angeles, CA Patient Centered Medical Home and Accountable Care Organizations Health Information Technology David K. Nace MD, Medical Director, McKesson Corporation Co-Chair,
Bundled Payments. AMGA September 25, 2013 AGENDA. Who Are We. Our Business Challenge. Episode Process. Experience
 Bundled Payments AMGA September 25, 2013 Who Are We AGENDA Our Business Challenge Episode Process Experience 1 Cleveland Clinic is transforming Fee for service Fee for value 3 Fast Facts 41,200 employees
Bundled Payments AMGA September 25, 2013 Who Are We AGENDA Our Business Challenge Episode Process Experience 1 Cleveland Clinic is transforming Fee for service Fee for value 3 Fast Facts 41,200 employees
Challenges and Opportunities for Improving Health and Healthcare in Ohio through Technology
 Challenges and Opportunities for Improving Health and Healthcare in Ohio through Technology Ohio Health IT Advocacy Day Craig Brammer, CEO cbrammer@healthbridge.org @CraigABrammer Challenge #1: Information
Challenges and Opportunities for Improving Health and Healthcare in Ohio through Technology Ohio Health IT Advocacy Day Craig Brammer, CEO cbrammer@healthbridge.org @CraigABrammer Challenge #1: Information
Physician Engagement
 Pathways for Successful Accountable Care Organizations: Physician Engagement Thomas Kloos, MD Jim Barr, MD Atlantic ACO & Optimus Healthcare Partners ACO Helping providers Care Better for their patients.
Pathways for Successful Accountable Care Organizations: Physician Engagement Thomas Kloos, MD Jim Barr, MD Atlantic ACO & Optimus Healthcare Partners ACO Helping providers Care Better for their patients.
CONNECTED SM. Blue Care Connection SIMPLY AN ACTIVE APPROACH TO INTEGRATED HEALTH MANAGEMENT
 SIMPLY CONNECTED SM Blue Care Connection AN ACTIVE APPROACH TO INTEGRATED HEALTH MANAGEMENT Jeanine Patterson, MS, RN, HSMI Clinical Account Consultant July 23, 2013 Blue Cross and Blue Shield of Illinois,
SIMPLY CONNECTED SM Blue Care Connection AN ACTIVE APPROACH TO INTEGRATED HEALTH MANAGEMENT Jeanine Patterson, MS, RN, HSMI Clinical Account Consultant July 23, 2013 Blue Cross and Blue Shield of Illinois,
Pricing Transparency and Patient Education
 Pricing Transparency and Patient Education Ochsner Health System Wendy Burns and Katherine Cardwell January 22, 2018 Agenda OHS Background Revenue Cycle Structure Consumerism at OHS Patient Education Initiatives
Pricing Transparency and Patient Education Ochsner Health System Wendy Burns and Katherine Cardwell January 22, 2018 Agenda OHS Background Revenue Cycle Structure Consumerism at OHS Patient Education Initiatives
Health Care Reform An Integrated Health Care Delivery System Perspective
 Health Care Reform Insights Health Care Reform An Integrated Health Care Delivery System Perspective Andrew McCulloch A national imperative: True health care reform requires innovation and integration
Health Care Reform Insights Health Care Reform An Integrated Health Care Delivery System Perspective Andrew McCulloch A national imperative: True health care reform requires innovation and integration
Building & Strengthening Patient Centered Medical Homes in the Safety Net
 Blue Shield of California Foundation County Coverage Expansion Planning Workshop #2 Building & Strengthening Patient Centered Medical Homes in the Safety Net July 8, 2011 Presented by: Kathryn Phillips,
Blue Shield of California Foundation County Coverage Expansion Planning Workshop #2 Building & Strengthening Patient Centered Medical Homes in the Safety Net July 8, 2011 Presented by: Kathryn Phillips,
What is a Pathways HUB?
 What is a Pathways HUB? Q: What is a Community Pathways HUB? A: The Pathways HUB model is an evidence-based community care coordination approach that uses 20 standardized care plans (Pathways) as tools
What is a Pathways HUB? Q: What is a Community Pathways HUB? A: The Pathways HUB model is an evidence-based community care coordination approach that uses 20 standardized care plans (Pathways) as tools
Coordinated Care: Key to Successful Outcomes
 Coordinated Care: Key to Successful Outcomes Best practices in care coordination improve health, lower costs and increase patient satisfaction 402 Lippincott Drive Marlton, NJ 08053 856.782.3300 www.continuumhealth.net
Coordinated Care: Key to Successful Outcomes Best practices in care coordination improve health, lower costs and increase patient satisfaction 402 Lippincott Drive Marlton, NJ 08053 856.782.3300 www.continuumhealth.net
Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network
 Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network Kim Cox Vice President, Provider Network, Optum Kim Cox is Vice President of Provider Network. She joined Optum in February
Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network Kim Cox Vice President, Provider Network, Optum Kim Cox is Vice President of Provider Network. She joined Optum in February
TRANSFORMING HEALTHCARE DELIVERY A Pathway to Affordable, High-Quality Care in America
 TRANSFORMING HEALTHCARE DELIVERY A Pathway to Affordable, High-Quality Care in America TABLE OF CONTENTS Executive Summary... 3 A Pathway to Affordable, High-Quality Care in America... 7 Appendix... 18
TRANSFORMING HEALTHCARE DELIVERY A Pathway to Affordable, High-Quality Care in America TABLE OF CONTENTS Executive Summary... 3 A Pathway to Affordable, High-Quality Care in America... 7 Appendix... 18
Future of Community Healthcare Providers. Author: Mr. Raj Shah, CEO, CTIS Inc.
 Author: Mr. Raj Shah, CEO, CTIS Inc. Healthcare providers range from government to commercial sectors. In the government sector, this includes both civilian and military hospitals, academic medical and
Author: Mr. Raj Shah, CEO, CTIS Inc. Healthcare providers range from government to commercial sectors. In the government sector, this includes both civilian and military hospitals, academic medical and
Welcome to Regence! Meet your employer health plan
 is an Independent Licensee of the Blue Cross and Blue Shield Association Regence BlueCross BlueShield of Utah Welcome to Regence! Meet your employer health plan 1 Health insurance is a big, wonderful benefit.
is an Independent Licensee of the Blue Cross and Blue Shield Association Regence BlueCross BlueShield of Utah Welcome to Regence! Meet your employer health plan 1 Health insurance is a big, wonderful benefit.
Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws.
 Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Austin Regional Clinic Seton Health Alliance
 Austin Regional Clinic Seton Health Alliance Clinical Integration Through the Eyes of an Independent Multispecialty Physician Group AMGA Annual Conference March 14, 2013 Norman H. Chenven, M.D. Founder
Austin Regional Clinic Seton Health Alliance Clinical Integration Through the Eyes of an Independent Multispecialty Physician Group AMGA Annual Conference March 14, 2013 Norman H. Chenven, M.D. Founder
NACDD and CDC Health Payer 101 Webinar Series. Webinar #4: Contracting 101
 NACDD and CDC Health Payer 101 Webinar Series Webinar #4: Contracting 101 Jennifer Nolty, Director, Innovative Primary Care National Association of Community Health Centers June 30, 2016 Contracting 101
NACDD and CDC Health Payer 101 Webinar Series Webinar #4: Contracting 101 Jennifer Nolty, Director, Innovative Primary Care National Association of Community Health Centers June 30, 2016 Contracting 101
Value-Based Readiness: Setting the Right Pace
 HEALTHLEADERS MEDIA INTELLIGENCE REPORT MAY 2017 Value-Based Readiness: Setting the Right Pace An Independent HealthLeaders Media Report Supported by: An Independent HealthLeaders Media Report Powered
HEALTHLEADERS MEDIA INTELLIGENCE REPORT MAY 2017 Value-Based Readiness: Setting the Right Pace An Independent HealthLeaders Media Report Supported by: An Independent HealthLeaders Media Report Powered
Person-Centered Accountable Care
 Person-Centered Accountable Care Nelly Ganesan, MPH, Senior Director, Avalere s Evidence, Translation and Implementation Practice October 12, 2017 avalere.com @NGanesanAvalere @avalerehealth Despite Potential
Person-Centered Accountable Care Nelly Ganesan, MPH, Senior Director, Avalere s Evidence, Translation and Implementation Practice October 12, 2017 avalere.com @NGanesanAvalere @avalerehealth Despite Potential
Risk Adjustment Methods in Value-Based Reimbursement Strategies
 Paper 10621-2016 Risk Adjustment Methods in Value-Based Reimbursement Strategies ABSTRACT Daryl Wansink, PhD, Conifer Health Solutions, Inc. With the move to value-based benefit and reimbursement models,
Paper 10621-2016 Risk Adjustment Methods in Value-Based Reimbursement Strategies ABSTRACT Daryl Wansink, PhD, Conifer Health Solutions, Inc. With the move to value-based benefit and reimbursement models,
Bright Spots in primary care
 Bright Spots in primary care A High- Performing Teaching Practice: Site Visit to Oregon Health & Science University s (OHSU) Family Medicine Clinic at Gabriel Park General information Tom Bodenheimer MD
Bright Spots in primary care A High- Performing Teaching Practice: Site Visit to Oregon Health & Science University s (OHSU) Family Medicine Clinic at Gabriel Park General information Tom Bodenheimer MD
Patient Centered Medical Home The next generation in patient care
 Patient Centered Medical Home The next generation in patient care Provider Training Module I OBJECTIVE To explain... What Patient Centered Medical Home is How it works Why it s important Where to begin
Patient Centered Medical Home The next generation in patient care Provider Training Module I OBJECTIVE To explain... What Patient Centered Medical Home is How it works Why it s important Where to begin
STAYING THE COURSE ON VALUE
 32 % of respondents say the fee-for-service payment model is least effective in quality and cost improvements INTELLIGENCE REPORT MAY/JUNE 2018 STAYING THE COURSE ON VALUE ANALYSIS... 2 SURVEY RESULTS...
32 % of respondents say the fee-for-service payment model is least effective in quality and cost improvements INTELLIGENCE REPORT MAY/JUNE 2018 STAYING THE COURSE ON VALUE ANALYSIS... 2 SURVEY RESULTS...
Aligning Physician Groups to Maximize Managed Care Performance
 Aligning Physician Groups to Maximize Managed Care Performance Presented to: 2016 Spring Managed Care Forum Friday, April 22, 2016 Introduction Today s speaker Page 1 Craig D. Pederson Principal Insight
Aligning Physician Groups to Maximize Managed Care Performance Presented to: 2016 Spring Managed Care Forum Friday, April 22, 2016 Introduction Today s speaker Page 1 Craig D. Pederson Principal Insight
