Integrated Health System
|
|
|
- Hilary Strickland
- 5 years ago
- Views:
Transcription
1
2 Integrated Health System Please note that the views expressed are those of the conference speakers and do not necessarily reflect the views of the American Hospital Association and Health Forum. Page 2
3 Integrated Health System: U of U Health $281 Million+ Grants in FY2016 1,250 Health Care Providers Trained Annually Over 1,400 Providers HOSPITALS & CLINICS EDUCATION RESEARCH PYSICIANS Page 3
4 Audience Question Which bests fits your perspective? a. Hospital b. Physician c. Insurance Carrier d. Pharmacy Page 4
5 Audience Question As a percentage, how much of your budget is spent on employee health care coverage? a. 0% b. 0-5% c. 5-10% d % e. I don t know Page 5
6 National Average Page 6
7 Think Like an Employer Employer demands to keep costs down UM & Prior-Authorizations Requirement Page 7
8 Unsustainability of Health Care Page 8
9 Unsustainability of Health Care Page 9
10 Cost Shift to Employees Page 10
11 How Health Systems Measure Quality Page 11
12 How Employers and Patients Measure Quality Page 12
13 What Patients Really Value is Affordability and Access Register for White Paper at: UofUHealth.org/ValueSurvey Page 13
14 Most Valued Select five (5) statements from the list below that best reflect what you value most when getting services from a health care provider. A health care provider is someone who is licensed to provide health services, including doctors, nurses, physicians assistants, nurse practitioners, etc. 45% 39% 38% 36% 36% 34% 33% 32% Percent Selected 31% 45% - My out-of-pocket cost is affordable 39% - I m able to schedule a timely appointment 26% 25% 25% 24% 21% 17% 15% 12% 10% My out-ofpocket cost is affordable I'm able to schedule a timely appointment I'm confident in the provider's expertise The office is conveniently located The provider knows and cares about me The provider reviews the results of exams, labs, and imaging with me The staff are friendly and helpful My health improves The wait time at the office is reasonable The provider includes me in choosing treatment options The provider knows and considers my insurance plan when providing treatment I don't experience complications or medical errors Enough time is spent with the provider I can easily communicate with my provider between appointments I get specific treatments I want (like antibiotics or an MRI) My mental health needs are considered in my treatment plan The provider reviews my prescription medications and discusses their cost The provider has extended office hours (nights and weekends) Total sample; Weight: final; base n = 5031; effective sample size = 3416 (68%) 14
15 Responsibility Who s primarily responsible for ensuring that Me (the patient) My health care provider My health care system My insurance company My employer I don't experience complications or medical errors The wait time at the office is reasonable The staff are friendly and helpful The provider reviews the results of exams, labs, and imaging with me The provider has extended office hours (nights and weekends) I get specific treatments I want (like antibiotics or an MRI) Enough time is spent with the provider The provider knows and cares about me The provider knows and considers my insurance plan when providing My out-of-pocket cost is affordable The provider includes me in choosing treatment options The provider reviews my prescription medications and discusses their cost My mental health needs are considered in my treatment plan I can easily communicate with my provider between appointments My health improves I'm confident in the provider's expertise I'm able to schedule a timely appointment The office is conveniently located 0% 10% 20% 30% 40% 50% 60% 70% 80% 90% 100% Total sample; Weight: final; base n = from 488 to 2338; total n = 5031; 4543 missing; effective sample size = 1546 (66%) 15
16 Audience Question What is the average margin of a health insurance company is? a. 0% b. 0-5% c. 5-10% d % e % Page 16
17 How Can We Work Together Efficiently? Hospital Physician Patient Pharmacy Insurance Employer Page 17
18 How Can We Work Together Page 18
19 Q & A Break Page 19
20 Managing Risk from a CMO Perspective COST - Managing the Population s Health Care Management Integration with Clinicians Our approach to Population Health REVENUE - Risk Adjustment Overview Strategies for optimization Page 20
21 Care Management The Evidence Randomized trial 174,120 people to telephone-based care management or non-intervention Followed for 1 year Total costs $7.96 (3.6%) PMPM lower in the care managed group Cost of program $2.00 PMPM 10.1% reduction in hospital admissions accounted for majority of savings N Engl J Med 2010;363: Page 21
22 Total Cost of Care (PMPM) Group Nonintervention Care Managed $ Difference % Difference Chronic Conditions at the top 10% of financial risk $1,659 $1,576 -$84-5% Care Gaps $502 $678 +$ % Only a select group of individuals benefit from care management How do we find those people? N Engl J Med 2010;363: Page 22
23 Culling Candidates for Care Management Page 23
24 Production Methodology Predicting Intervenable Risk Initial Filter RISK STRATIFICATION FLAG SCORE Number and severity of chronic diseases ED visits Inpatient Hospitalizations Risk score migration- Higher prospective than concurrent Mental Health Diagnosis Page 24
25 Validity of Stratification Model Page 25
26 Risk Stratification 0-2 flags 3 flags 4 flags >5 flags <1% 2% 9% 6% 9% 26% 87% 59% % of Membership % of Cost Page 26
27 Next Step: Integration Getting Data to Our Providers We work with providers to create an efficient care pathway Other Carriers Page 27
28 Lessons Learned 1. Our tool is too blunt. Touching too many lives to find a patient suitable for care management. Can big data solutions help? Lots of vendors seem to think so. 2. Data to the provider isn t very useful unless it integrates with clinician s workflow. Implementing Epic Caboodle which will allow integration of health plan claims into clinical workflow. 3. Is data alone enough? A prelude to Alternative Payment Methodologies. Page 28
29 Our Approach to Population Health Building Blocks Page 29
30 Something is Working 20% Reduction in ED visits ED visits per 1000 members 30% Reduction in inpatient admissions Inpatient Admits per 1000 members Page 30
31 Revenue Capturing Risk Premium Page 31
32 Managed Risk Isn t all Bad MLR by HCC Chronic Conditions Categories Chronic Heart Disease Cancers HIV Mental Health No HCC's Student Athletes Page 32
33 Risk Adjustment Medicare Advantage CMS-HCC model Prospective Model: This year s claims used to determine next years capitated rate for each member. Individual and Small Group Exchange HHS-HCC model Concurrent Model: This year s claims used to determine risk transfer for current year. Zero Sum: Transfers are made between carriers in each state. Carrier with healthier members pay carriers with sicker members. Medicaid Varies by state Generally CDPS prospective model Page 33
34 How it Works - NOW Each diagnosis code billed in the calendar year is grouped into disease categories Each Condition Category is given a weight Rules in place to prevent duplication- (Hierarchical) For example: Breast cancer and metastatic cancer are different HCC s. Coding metastatic cancer will negate the breast cancer HCC. Medicare: Average beneficiary has risk score of 1 Exchange: Built on commercial data and calibrated to 1 National Average 2015 = 1.62 (Range ) CMS: Summary Report on Transitional Reinsurance Payments and Permanent Risk Adjustment Transfers for the 2015 Benefit Year Page 34
35 Common HCCs Diagnosis HCC Category 2014 Weight Chronic Hepatitis B, C Acute Hepatitis, or unspecified None None Diabetes, Uncomplicated Diabetes with Complications Morbidly Obesity, BMI > Page 35
36 CMS HCC Example No Diagnoses 80 y/o Male Medicaid Eligible Total Risk PMPM $557 Annual Reimbursement $6,682 Some Diagnoses 80 y/o Male Medicaid Eligible Diabetes (250.0) Peripheral Vascular Dz Total Risk PMPM $815 Annual Reimbursement $9,788 Specific Diagnoses 80 y/o Male Medicaid Eligible DM with Vascular Complications Peripheral Vascular Dz CHF Interaction CHF- DM Total Risk PMPM $1,315 Annual Reimbursement $15,788 Page 36
37 Improving your Risk Score 37 % of patients with major chronic conditions go uncoded* *Optum: Accurate coding: the foundation of accountable care accessed online June 7, 2017 Page 37
38 Is This Allowable? We do not believe there is anything inappropriate, unethical or otherwise wrong with hospitals taking full advantage of coding opportunities to maximize Medicare payment that is supported by documentation in the medical record. CMS 2008 IPPS Final Rule, p. 208 Medicare Payment Advisory Commission: Letter to Acting Administrator Leslie Norwalk, June 11, 2007, page 12. Page 38
39 Risk Adjustment Visits Provider is given a list of suspected diagnoses based on historical claims and other triggers Page 39
40 HCC Scout Creeps through text looking for diagnoses which were not billed Page 40
41 The Bottom Line Page 41
42 Q & A Break Page 43
43 Alternative Payment Models Better Care, Smarter Spending, Healthier People Background Fully at-risk for Medicaid Future of health care industry Commitment to ACO principles Improved care coordination and clinical outcomes Improved access and member/patient satisfaction Controlled cost aligning payment and incentives Practice with integrated system safe environment before rolling out to other practices and payers Page 44
44 Alternative Payment Models Maturity of Payment Risk Fee for Service Gain Sharing Bundle Specific/ Partial Capitation Global Capitation No Risk Increasing Risk Full Risk Value Based Payment July 2013 Modeled Pediatric Health Management July 2016 Page 45
45 Membership & Dollars Under Alternative Payment Models MEDICAID MEMBERSHIP Fee for service Gain Sharing Capitation 25.20% MEDICAID PAID DOLLARS Fee for service Gain Sharing Capitation 10.70% 64.10% 10.70% 33.60% 55.70% Page 46
46 The Starting Point 2013 Membership Member Concentration 31% 9% 7% 9% 52% 2% 15% 75% Medicaid Dual Eligible Employee Plan TPA U Health Care Clinic 2 Clinic 3 Clinic 4 Page 47
47 Gain Sharing Value Based Payment Model Attribution based model Fee for service Enhanced payments Thin cap Shared savings based on Financial baseline Quality measures Data analytics and reporting Shared care management Page 48
48 Capitation Pediatric Health Management Model UUHP Medicaid 33,000 children PSS Capitation model Pediatric sub-specialty care UUMG pediatric subspecialists Primary Children s Budgeted Capitation Payment Model Based on defined pediatric services and historical claims trend UUHP passes two-sided risk for defined sub-specialty care, in-scope services Provider risk exposure mitigated Large dollar carve-out Risk corridor High-cost drug carve-out Physician/Hospital shared risk Page 49
49 Status of Models Financial Results PROVIDER PAYMENT Gain Sharing Focus Level of on-going provider risk Data sharing parameters and best venue Care management collaboration Page 50
50 Lessons Learned Control is key Physicians more comfortable with controlling quality than cost Unanticipated costs are barriers to engagement $625,000-$750,000 First Year $1,000 a pill (daily) New York Times, Costly Drug for Fatal Muscular Disease Wins F.D.A. Approval, December 30, 2016 New York Times, How Much Should Hepatitis C Treatment Cost?, March 15, 2014 Page 51
51 Lessons Learned Control is key Physicians more comfortable with controlling quality than cost Unanticipated costs are barriers to engagement Phase-in approach Timing and scope KPMG/AMA MACRA Survey, Are physicians ready for MACRA/QPP?, June 2017 Page 52
52 Lessons Learned Control is key Physicians more comfortable with controlling quality than cost Unanticipated costs are barriers to engagement Phase-in approach Timing and scope Making data available isn t enough Analytics of data high risk and clinical priority Operationalize changes within practice useable data integrated in work flow Understand impact to financial outcomes actuarial support Page 53
53 Reporting & Analytics Page 54
54 Lessons Learned Control is key Physicians more comfortable with controlling quality than cost Unanticipated costs are barriers to engagement Phase-in approach Timing and scope Making data available isn t enough Analytics of data high risk and clinical priority Operationalize changes within practice useable data integrated in work flow Understand impact to financial outcomes actuarial support Shared care management approach is worth the effort Page 55
55 Collaboration of Care Management Provider UUHP Patients in defined risk stratification categories Patients with ED visits >= 5 in 12 months Patients discharged from inpatient hospitalization Ambulatory sensitive conditions U Baby Program participants Restricted Healthy U Medicaid members Who bears the risk? High cost/catastrophic Notification of University hospitalizations Page 56
56 Q & A Break Page 57
Describe the process for implementing an OP CDI program
 1 Outpatient CDI: The Marriage of MACRA and HCCs Marion Kruse, RN, MBA Founding Partner LYM Consulting Columbus, OH Learning Objectives At the completion of this educational activity, the learner will
1 Outpatient CDI: The Marriage of MACRA and HCCs Marion Kruse, RN, MBA Founding Partner LYM Consulting Columbus, OH Learning Objectives At the completion of this educational activity, the learner will
Adopting Accountable Care An Implementation Guide for Physician Practices
 Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Adopting Accountable Care An Implementation Guide for Physician Practices EXECUTIVE SUMMARY November 2014 A resource developed by the ACO Learning Network www.acolearningnetwork.org Executive Summary Our
Medical Appropriateness and Risk Adjustment
 Medical Appropriateness and Risk Adjustment Medical Appropriateness David Rzeszutko, MD Medical Director November 10, 2017 Objectives Medical necessity Value equation Medical appropriateness Why? To improve
Medical Appropriateness and Risk Adjustment Medical Appropriateness David Rzeszutko, MD Medical Director November 10, 2017 Objectives Medical necessity Value equation Medical appropriateness Why? To improve
Population Health or Single-payer The future is in our hands. Robert J. Margolis, MD
 Population Health or Single-payer The future is in our hands Robert J. Margolis, MD Today s problems Interim steps Population health Alternatives Conclusions Outline $3,000,000,000,000 $1,000,000,000,000
Population Health or Single-payer The future is in our hands Robert J. Margolis, MD Today s problems Interim steps Population health Alternatives Conclusions Outline $3,000,000,000,000 $1,000,000,000,000
Next Generation Physician Compensation Design in a Schizophrenic Payer Environment
 Next Generation Physician Compensation Design in a Schizophrenic Payer Environment Presented to: 2015 Spring Managed Care Forum Friday, April 24, 2015 Today s agenda Setting the Stage Why are we Here?
Next Generation Physician Compensation Design in a Schizophrenic Payer Environment Presented to: 2015 Spring Managed Care Forum Friday, April 24, 2015 Today s agenda Setting the Stage Why are we Here?
Using Data for Proactive Patient Population Management
 Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Using Data for Proactive Patient Population Management Kate Lichtenberg, DO, MPH, FAAFP October 16, 2013 Topics Review population based care Understand the use of registries Harnessing the power of EHRs
Rethinking annual assessments: Identifying and closing gaps in care
 Rethinking annual assessments: Identifying and closing gaps in care Expert presenters Curtis A. Mock, MD, MBA, National Medical Director, Complex Population Management Annual in-home assessments provide
Rethinking annual assessments: Identifying and closing gaps in care Expert presenters Curtis A. Mock, MD, MBA, National Medical Director, Complex Population Management Annual in-home assessments provide
Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks
 Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks Agenda Define ACO, CIN, and Coordinated Care Review ACO/CIN
Healthcare Financial Management Association October 13 th, 2016 Introduction to Accountable Care Organizations and Clinically Integrated Networks Agenda Define ACO, CIN, and Coordinated Care Review ACO/CIN
POPULATION HEALTH PLAYBOOK. Mark Wendling, MD Executive Director LVPHO/Valley Preferred 1
 POPULATION HEALTH PLAYBOOK Mark Wendling, MD Executive Director LVPHO/Valley Preferred www.populytics.com 1 Today s Agenda Outline LVHN, LVPHO and Populytics Overview Population Health Approach Population
POPULATION HEALTH PLAYBOOK Mark Wendling, MD Executive Director LVPHO/Valley Preferred www.populytics.com 1 Today s Agenda Outline LVHN, LVPHO and Populytics Overview Population Health Approach Population
Risk Adjusted Diagnosis Coding:
 Risk Adjusted Diagnosis Coding: Reporting ChronicDisease for Population Health Management Jeri Leong, R.N., CPC, CPC-H, CPMA, CPC-I Executive Director 1 Learning Objectives Explain the concept Medicare
Risk Adjusted Diagnosis Coding: Reporting ChronicDisease for Population Health Management Jeri Leong, R.N., CPC, CPC-H, CPMA, CPC-I Executive Director 1 Learning Objectives Explain the concept Medicare
Understanding Risk Adjustment in Medicare Advantage
 Understanding Risk Adjustment in Medicare Advantage ISSUE BRIEF JUNE 2017 Risk adjustment is an essential mechanism used in health insurance programs to account for the overall health and expected medical
Understanding Risk Adjustment in Medicare Advantage ISSUE BRIEF JUNE 2017 Risk adjustment is an essential mechanism used in health insurance programs to account for the overall health and expected medical
Healthcare Reimbursement Change VBP -The Future is Now
 Healthcare Reimbursement Change VBP -The Future is Now 1 On the Move Volume/ Fee-for-Service Fee-for-service reimbursement High quality not rewarded No shared financial risk Stand-alone systems can thrive
Healthcare Reimbursement Change VBP -The Future is Now 1 On the Move Volume/ Fee-for-Service Fee-for-service reimbursement High quality not rewarded No shared financial risk Stand-alone systems can thrive
A Care Coordination Model for Value-Based Performance Programs
 A Care Coordination Model for Value-Based Performance Programs Richard S. Chung, MD Chief Clinical Officer APS Healthcare 8th National Pay for Performance (P4P) Summit February 20, 2013 Hyatt Regency Hotel,
A Care Coordination Model for Value-Based Performance Programs Richard S. Chung, MD Chief Clinical Officer APS Healthcare 8th National Pay for Performance (P4P) Summit February 20, 2013 Hyatt Regency Hotel,
REPORT OF THE BOARD OF TRUSTEES
 REPORT OF THE BOARD OF TRUSTEES B of T Report 21-A-17 Subject: Presented by: Risk Adjustment Refinement in Accountable Care Organization (ACO) Settings and Medicare Shared Savings Programs (MSSP) Patrice
REPORT OF THE BOARD OF TRUSTEES B of T Report 21-A-17 Subject: Presented by: Risk Adjustment Refinement in Accountable Care Organization (ACO) Settings and Medicare Shared Savings Programs (MSSP) Patrice
SUCCESS IN A VALUE - BASED PAYMENT ARRANGMENT
 SUCCESS IN A VALUE - BASED PAYMENT ARRANGMENT October 3 rd, 2017 David Evangelista MediSys Health Network 1 Who is MediSys? Jamaica Hospital is a 431-bed not-for profit teaching hospital. Jamaica is a
SUCCESS IN A VALUE - BASED PAYMENT ARRANGMENT October 3 rd, 2017 David Evangelista MediSys Health Network 1 Who is MediSys? Jamaica Hospital is a 431-bed not-for profit teaching hospital. Jamaica is a
ENHANCING PRESCRIBER RELATIONSHIPS: MAKING IT A WIN-WIN JULY 12, :00 5:00 PM
 ENHANCING PRESCRIBER RELATIONSHIPS: MAKING IT A WIN-WIN JULY 12, 2017 3:00 5:00 PM ACPE UAN: 0107-9999-17-105-L04-P 0.2 CEU/2.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists: Upon
ENHANCING PRESCRIBER RELATIONSHIPS: MAKING IT A WIN-WIN JULY 12, 2017 3:00 5:00 PM ACPE UAN: 0107-9999-17-105-L04-P 0.2 CEU/2.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists: Upon
Connected Care Partners
 Connected Care Partners Our Discussion Today Introducing the Connected Care Partners CIN What is a Clinically Integrated Network (CIN) and why is the time right to join the Connected Care Partners CIN?
Connected Care Partners Our Discussion Today Introducing the Connected Care Partners CIN What is a Clinically Integrated Network (CIN) and why is the time right to join the Connected Care Partners CIN?
Emerging Outpatient CDI Drivers and Technologies
 7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
the role of HCCs in a value-based payment system
 REPRINT October 2017 Donna M. Smith L. Gordon Moore healthcare financial management association hfma.org the role of HCCs in a value-based payment system Appropriate documentation and coding of hierarchical
REPRINT October 2017 Donna M. Smith L. Gordon Moore healthcare financial management association hfma.org the role of HCCs in a value-based payment system Appropriate documentation and coding of hierarchical
Bundled Payments. AMGA September 25, 2013 AGENDA. Who Are We. Our Business Challenge. Episode Process. Experience
 Bundled Payments AMGA September 25, 2013 Who Are We AGENDA Our Business Challenge Episode Process Experience 1 Cleveland Clinic is transforming Fee for service Fee for value 3 Fast Facts 41,200 employees
Bundled Payments AMGA September 25, 2013 Who Are We AGENDA Our Business Challenge Episode Process Experience 1 Cleveland Clinic is transforming Fee for service Fee for value 3 Fast Facts 41,200 employees
Total Cost of Care Technical Appendix April 2015
 Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Getting Ready for the Maryland Primary Care Program
 Getting Ready for the Maryland Primary Care Program Presentation to Maryland Academy of Nutrition and Dietetics March 19, 2018 Maryland Department of Health All-Payer Model: Performance to Date Performance
Getting Ready for the Maryland Primary Care Program Presentation to Maryland Academy of Nutrition and Dietetics March 19, 2018 Maryland Department of Health All-Payer Model: Performance to Date Performance
Session 74 PD, Innovative Uses of Risk Adjustment. Moderator: Joan C. Barrett, FSA, MAAA
 Session 74 PD, Innovative Uses of Risk Adjustment Moderator: Joan C. Barrett, FSA, MAAA Presenters: Jill S. Herbold, FSA, MAAA Robert Anders Larson, FSA, MAAA Erica Rode, ASA, MAAA SOA Antitrust Disclaimer
Session 74 PD, Innovative Uses of Risk Adjustment Moderator: Joan C. Barrett, FSA, MAAA Presenters: Jill S. Herbold, FSA, MAAA Robert Anders Larson, FSA, MAAA Erica Rode, ASA, MAAA SOA Antitrust Disclaimer
Paying for Primary Care: Is There A Better Way?
 Paying for Primary Care: Is There A Better Way? Robert A. Berenson, M.D. Senior Fellow, The Urban Institute CHCS Regional Quality Improvement Initiative, Providence, R.I., July 25, 2007 1 Medicare Challenges
Paying for Primary Care: Is There A Better Way? Robert A. Berenson, M.D. Senior Fellow, The Urban Institute CHCS Regional Quality Improvement Initiative, Providence, R.I., July 25, 2007 1 Medicare Challenges
Session #6: Population Health Must Haves Care Coordination
 Session #6: Population Health Must Haves Care Coordination Presenter: Robert Wieland, M.D. Arbor Lakes Saturday, Jan. 7, 2017 11:15 a.m. 12:15 p.m. Robert A. Wieland, M.D. Robert A. Wieland, M.D. (Bob)
Session #6: Population Health Must Haves Care Coordination Presenter: Robert Wieland, M.D. Arbor Lakes Saturday, Jan. 7, 2017 11:15 a.m. 12:15 p.m. Robert A. Wieland, M.D. Robert A. Wieland, M.D. (Bob)
ENGAGING PHYSICIANS FOR IMPROVED OUTCOMES: CLINICAL DOCUMENTATION, FINANCIAL & PATIENT CARE
 ENGAGING PHYSICIANS FOR IMPROVED OUTCOMES: CLINICAL DOCUMENTATION, FINANCIAL & PATIENT CARE Northeast Ohio HFMA GHALI May 20, 2016 James Begley, MD, MS Physician Champion, ICD-10 & Medical Records Committee
ENGAGING PHYSICIANS FOR IMPROVED OUTCOMES: CLINICAL DOCUMENTATION, FINANCIAL & PATIENT CARE Northeast Ohio HFMA GHALI May 20, 2016 James Begley, MD, MS Physician Champion, ICD-10 & Medical Records Committee
From Reactive to Proactive: Creating a Population Management Platform
 Session D9 / E9 From Reactive to Proactive: Creating a Population Management Platform Richard Gitomer, MD Director, Brigham and Women s Primary Care Center of Excellence Vice Chair, Primary Care, Dept.
Session D9 / E9 From Reactive to Proactive: Creating a Population Management Platform Richard Gitomer, MD Director, Brigham and Women s Primary Care Center of Excellence Vice Chair, Primary Care, Dept.
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers
 Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
The Patient-Centered Medical Home Model of Care
 The Patient-Centered Medical Home Model of Care May 11, 2017 Louise Bryde Principal Presentation Outline Imperatives for Change Overview: What Is a Patient-Centered Medical Home? The Medical Neighborhood
The Patient-Centered Medical Home Model of Care May 11, 2017 Louise Bryde Principal Presentation Outline Imperatives for Change Overview: What Is a Patient-Centered Medical Home? The Medical Neighborhood
Healthy Aging Recommendations 2015 White House Conference on Aging
 Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT
 ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT The Centers for Medicare and Medicaid Services Kate Goodrich, MD MHS Director, Clinical Standards & Quality Chief Medical Officer 1 DISCLAIMERS
ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT The Centers for Medicare and Medicaid Services Kate Goodrich, MD MHS Director, Clinical Standards & Quality Chief Medical Officer 1 DISCLAIMERS
A Model for Value-Based Provider/Payer Partnerships
 A Model for Value-Based Provider/Payer Partnerships Page 1 With the recent spotlight on accountable care, payer and provider organizations are seeing an opportunity to collaborate to drive down medical
A Model for Value-Based Provider/Payer Partnerships Page 1 With the recent spotlight on accountable care, payer and provider organizations are seeing an opportunity to collaborate to drive down medical
The Influence of Health Policy on Clinical Practice. Dr. Kim Kuebler, DNP, APRN, ANP-BC Multiple Chronic Conditions Resource Center
 The Influence of Health Policy on Clinical Practice Dr. Kim Kuebler, DNP, APRN, ANP-BC Multiple Chronic Conditions Resource Center Disclaimer Director: Multiple Chronic Conditions Resource Center www.multiplechronicconditions.org
The Influence of Health Policy on Clinical Practice Dr. Kim Kuebler, DNP, APRN, ANP-BC Multiple Chronic Conditions Resource Center Disclaimer Director: Multiple Chronic Conditions Resource Center www.multiplechronicconditions.org
Rural and Independent Primary Care.
 Rural and Independent Primary Care www.caravanhealth.com Agenda 2015 Results from Rural ACO Participants Fundamental population health programs. Overview of additional rural value-based payments Opportunities
Rural and Independent Primary Care www.caravanhealth.com Agenda 2015 Results from Rural ACO Participants Fundamental population health programs. Overview of additional rural value-based payments Opportunities
Medicaid Practice Benchmark Report
 Issue Brief Medicaid Practice Benchmark Report Overview In 2015, the Maine Health Management Coalition (MHMC) distributed its first Medicaid Practice Benchmark Report to over 300 pediatric and adult practices,
Issue Brief Medicaid Practice Benchmark Report Overview In 2015, the Maine Health Management Coalition (MHMC) distributed its first Medicaid Practice Benchmark Report to over 300 pediatric and adult practices,
WPS Integrated Care Management Improving health, one member at a time
 WPS Integrated Care Management Improving health, one member at a time Integrated Care Management supports and promotes member health Looking for more from your group health insurance for your employees?
WPS Integrated Care Management Improving health, one member at a time Integrated Care Management supports and promotes member health Looking for more from your group health insurance for your employees?
Improve Your Revenue for the Services Your Provide with Proper Coding and Documentation. by Christina Rock, BSN, RN Supervisor, Clinical Education
 Improve Your Revenue for the Services Your Provide with Proper Coding and Documentation by Christina Rock, BSN, RN Supervisor, Clinical Education Objectives Awareness of resources and reference materials
Improve Your Revenue for the Services Your Provide with Proper Coding and Documentation by Christina Rock, BSN, RN Supervisor, Clinical Education Objectives Awareness of resources and reference materials
Physician Engagement
 Pathways for Successful Accountable Care Organizations: Physician Engagement Thomas Kloos, MD Jim Barr, MD Atlantic ACO & Optimus Healthcare Partners ACO Helping providers Care Better for their patients.
Pathways for Successful Accountable Care Organizations: Physician Engagement Thomas Kloos, MD Jim Barr, MD Atlantic ACO & Optimus Healthcare Partners ACO Helping providers Care Better for their patients.
Risk Adjustment Medicare and Commercial
 Risk Adjustment Medicare and Commercial 900 1671 0416 Transform your thinking about Introduction In a time of continual regulatory reform and the evolution of payer/provider reimbursement models, are you
Risk Adjustment Medicare and Commercial 900 1671 0416 Transform your thinking about Introduction In a time of continual regulatory reform and the evolution of payer/provider reimbursement models, are you
CMS Oncology Care Model s Standards for Patient Navigation
 CMS Oncology Care Model s Standards for Patient Navigation Nikolas Buescher Executive Director of Cancer Services Penn Medicine, Lancaster November 13, 2017 Ann B Barshinger Health Cancer Institute scale
CMS Oncology Care Model s Standards for Patient Navigation Nikolas Buescher Executive Director of Cancer Services Penn Medicine, Lancaster November 13, 2017 Ann B Barshinger Health Cancer Institute scale
A Practical Approach Toward Accountable Care and Risk-Based Contracting: Design to Implementation
 A Practical Approach Toward Accountable Care and Risk-Based Contracting: Design to Implementation Daniel J. Marino, President/CEO, Health Directions Asad Zaman, MD June 19, 2013 Session Objectives Establish
A Practical Approach Toward Accountable Care and Risk-Based Contracting: Design to Implementation Daniel J. Marino, President/CEO, Health Directions Asad Zaman, MD June 19, 2013 Session Objectives Establish
An Overview of NCQA Relative Resource Use Measures. Today s Agenda
 An Overview of NCQA Relative Resource Use Measures Today s Agenda The need for measures of Resource Use Development and testing RRU measures Key features of NCQA RRU measures How NCQA calculates benchmarks
An Overview of NCQA Relative Resource Use Measures Today s Agenda The need for measures of Resource Use Development and testing RRU measures Key features of NCQA RRU measures How NCQA calculates benchmarks
CMS Quality Payment Program: Performance and Reporting Requirements
 CMS Quality Payment Program: Performance and Reporting Requirements Session #QU1, February 19, 2017 Kristine Martin Anderson, Executive Vice President, Booz Allen Hamilton Colleen Bruce, Lead Associate,
CMS Quality Payment Program: Performance and Reporting Requirements Session #QU1, February 19, 2017 Kristine Martin Anderson, Executive Vice President, Booz Allen Hamilton Colleen Bruce, Lead Associate,
Accountable Care and Governance Challenges Under the Affordable Care Act
 Accountable Care and Governance Challenges Under the Affordable Care Act The First National Congress on Healthcare Clinical Innovations, Quality Improvement and Cost Containment October 26, 2011 Doug Hastings
Accountable Care and Governance Challenges Under the Affordable Care Act The First National Congress on Healthcare Clinical Innovations, Quality Improvement and Cost Containment October 26, 2011 Doug Hastings
Alternative Payment Models and Health IT
 Alternative Payment Models and Health IT Health DataPalooza Preconference May 8, 2016 Kelly Cronin, MS, MPH, Director, Office of Care Transformation, ONC/HHS HHS Goals for Medicare Payment Reform In January
Alternative Payment Models and Health IT Health DataPalooza Preconference May 8, 2016 Kelly Cronin, MS, MPH, Director, Office of Care Transformation, ONC/HHS HHS Goals for Medicare Payment Reform In January
From Risk Scores to Impactability Scores:
 From Risk Scores to Impactability Scores: Innovations in Care Management Carlos T. Jackson, Ph.D. September 14, 2015 Outline Population Health What is Impactability? Complex Care Management Transitional
From Risk Scores to Impactability Scores: Innovations in Care Management Carlos T. Jackson, Ph.D. September 14, 2015 Outline Population Health What is Impactability? Complex Care Management Transitional
What s Next for CMS Innovation Center?
 What s Next for CMS Innovation Center? A Guide to Building Successful Value-Based Payment Models Given CMMI s New Focus on Voluntary, Home-Grown Initiatives W W W. H E A L T H M A N A G E M E N T. C O
What s Next for CMS Innovation Center? A Guide to Building Successful Value-Based Payment Models Given CMMI s New Focus on Voluntary, Home-Grown Initiatives W W W. H E A L T H M A N A G E M E N T. C O
ACOs: California Style
 ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
Moving the Dial on Quality
 Moving the Dial on Quality Washington State Medical Oncology Society November 1, 2013 Nancy L. Fisher, MD, MPH CMO, Region X Centers for Medicare and Medicaid Serving Alaska, Idaho, Oregon, Washington
Moving the Dial on Quality Washington State Medical Oncology Society November 1, 2013 Nancy L. Fisher, MD, MPH CMO, Region X Centers for Medicare and Medicaid Serving Alaska, Idaho, Oregon, Washington
Preventable Readmissions
 Preventable Readmissions Strategy to reduce readmissions and increase quality needs to have the following elements A tool to identify preventable readmissions Payment incentives Public reporting Quality
Preventable Readmissions Strategy to reduce readmissions and increase quality needs to have the following elements A tool to identify preventable readmissions Payment incentives Public reporting Quality
Transitions of Care: Primary Care Perspective. Patrick Noonan, DO
 Transitions of Care: Primary Care Perspective Patrick Noonan, DO Disclosures None Bio Outpatient primary care internist at New Pueblo Medicine Completed residency at the University of Iowa Graduated from
Transitions of Care: Primary Care Perspective Patrick Noonan, DO Disclosures None Bio Outpatient primary care internist at New Pueblo Medicine Completed residency at the University of Iowa Graduated from
COLLABORATING FOR VALUE. A Winning Strategy for Health Plans and Providers in a Shared Risk Environment
 COLLABORATING FOR VALUE A Winning Strategy for Health Plans and Providers in a Shared Risk Environment Collaborating for Value Executive Summary The shared-risk payment models central to health reform
COLLABORATING FOR VALUE A Winning Strategy for Health Plans and Providers in a Shared Risk Environment Collaborating for Value Executive Summary The shared-risk payment models central to health reform
Succeeding in a New Era of Health Care Delivery
 March 14, 2012 Succeeding in a New Era of Health Care Delivery Building Value-Based Partnerships LeadingAge Pennsylvania Kathleen Griffin, PhD, National Director Post-Acute and Senior Services 1 Your Presenter
March 14, 2012 Succeeding in a New Era of Health Care Delivery Building Value-Based Partnerships LeadingAge Pennsylvania Kathleen Griffin, PhD, National Director Post-Acute and Senior Services 1 Your Presenter
ACO Practice Transformation Program
 ACO Overview ACO Practice Transformation Program PROGRAM OVERVIEW As healthcare rapidly transforms to new value-based payment systems, your level of success will dramatically improve by participation in
ACO Overview ACO Practice Transformation Program PROGRAM OVERVIEW As healthcare rapidly transforms to new value-based payment systems, your level of success will dramatically improve by participation in
Reforming Health Care with Savings to Pay for Better Health
 Reforming Health Care with Savings to Pay for Better Health Mark McClellan, MD PhD Director, Initiative on Health Care Value and Innovation Senior Fellow, Economic Studies October 2014 National Forum on
Reforming Health Care with Savings to Pay for Better Health Mark McClellan, MD PhD Director, Initiative on Health Care Value and Innovation Senior Fellow, Economic Studies October 2014 National Forum on
Using An APCD to Inform Healthcare Policy, Strategy, and Consumer Choice. Maine s Experience
 Using An APCD to Inform Healthcare Policy, Strategy, and Consumer Choice Maine s Experience What I ll Cover Today Maine s History of Using Health Care Data for Policy and System Change Health Data Agency
Using An APCD to Inform Healthcare Policy, Strategy, and Consumer Choice Maine s Experience What I ll Cover Today Maine s History of Using Health Care Data for Policy and System Change Health Data Agency
Generations Advantage Focus DC (HMO SNP) Diabetes Care Special Needs Plan GENERAL MODEL OF CARE (MOC) TRAINING
 Generations Advantage Focus DC (HMO SNP) Diabetes Care Special Needs Plan GENERAL MODEL OF CARE (MOC) TRAINING Through this training you will learn: What is a SNP? What is Martin s Point Generations Advantage
Generations Advantage Focus DC (HMO SNP) Diabetes Care Special Needs Plan GENERAL MODEL OF CARE (MOC) TRAINING Through this training you will learn: What is a SNP? What is Martin s Point Generations Advantage
What Have we Learned from the Pioneer ACO Model?
 What Have we Learned from the Pioneer ACO Model? Sherly Binu, CMMI December 7, 2016 Disclaimers 2 This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose
What Have we Learned from the Pioneer ACO Model? Sherly Binu, CMMI December 7, 2016 Disclaimers 2 This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose
The Pain or the Gain?
 The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
Goals & Challenges for Outpatient Quality Directors. Quality HealthCare Consulting, LLC CEO: Jennifer O'Donnell, MHA, PCMH-CCE
 Goals & Challenges for Outpatient Quality Directors Quality HealthCare Consulting, LLC CEO: Jennifer O'Donnell, MHA, PCMH-CCE Objectives Learn a practical way for Quality Directors to align Quality Measures
Goals & Challenges for Outpatient Quality Directors Quality HealthCare Consulting, LLC CEO: Jennifer O'Donnell, MHA, PCMH-CCE Objectives Learn a practical way for Quality Directors to align Quality Measures
Payer s Perspective on Clinical Pathways and Value-based Care
 Payer s Perspective on Clinical Pathways and Value-based Care Faculty Stephen Perkins, MD Chief Medical Officer Commercial & Medicare Services UPMC Health Plan Pittsburgh, Pennsylvania perkinss@upmc.edu
Payer s Perspective on Clinical Pathways and Value-based Care Faculty Stephen Perkins, MD Chief Medical Officer Commercial & Medicare Services UPMC Health Plan Pittsburgh, Pennsylvania perkinss@upmc.edu
Understanding Insurance Models For Risk Adjustment
 Understanding Insurance Models For Risk Adjustment For Healthcare Professionals Education provided by: Brian Boyce, BSHS, CPC, CPC-I CEO, Proprietor & Managing Consultant, ionhealthcare, LLC 1 No part
Understanding Insurance Models For Risk Adjustment For Healthcare Professionals Education provided by: Brian Boyce, BSHS, CPC, CPC-I CEO, Proprietor & Managing Consultant, ionhealthcare, LLC 1 No part
Alternative Managed Care Reimbursement Models
 Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
Population Health and the Accelerating Leap to Outcomes-Based Reimbursement. Craig J. Wilson
 Population Health and the Accelerating Leap to Outcomes-Based Reimbursement Craig J. Wilson Agenda / Goals Define Population Health Management Review emerging reimbursement landscape eg MACRA Review why
Population Health and the Accelerating Leap to Outcomes-Based Reimbursement Craig J. Wilson Agenda / Goals Define Population Health Management Review emerging reimbursement landscape eg MACRA Review why
State Leadership for Health Care Reform
 State Leadership for Health Care Reform Mark McClellan, MD, PhD Director, Engelberg Center for Health Care Reform Senior Fellow, Economic Studies Leonard D. Schaeffer Chair in Health Policy Studies Brookings
State Leadership for Health Care Reform Mark McClellan, MD, PhD Director, Engelberg Center for Health Care Reform Senior Fellow, Economic Studies Leonard D. Schaeffer Chair in Health Policy Studies Brookings
THE BUSINESS OF PEDIATRICS: BETTER CARE = BETTER PAYMENT. 19 th CNHN Pediatric Practice Management Seminar Thursday, December 6, 2016
 THE BUSINESS OF PEDIATRICS: BETTER CARE = BETTER PAYMENT 19 th CNHN Pediatric Practice Management Seminar Thursday, December 6, 2016 SMALLER VS BIGGER? WHAT PRACTICE SIZE IS JUST RIGHT? Mark Weissman,
THE BUSINESS OF PEDIATRICS: BETTER CARE = BETTER PAYMENT 19 th CNHN Pediatric Practice Management Seminar Thursday, December 6, 2016 SMALLER VS BIGGER? WHAT PRACTICE SIZE IS JUST RIGHT? Mark Weissman,
UnitedHealth Center for Health Reform & Modernization September 2014
 Health Reform & Modernization September 2014 2014 UnitedHealth Group. Any use, copying or distribution without written permission from UnitedHealth Group is prohibited. Overview Why Focus on Primary Care?
Health Reform & Modernization September 2014 2014 UnitedHealth Group. Any use, copying or distribution without written permission from UnitedHealth Group is prohibited. Overview Why Focus on Primary Care?
Long term commitment to a new vision. Medical Director February 9, 2011
 ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease
 Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease Introduction Within the COMPASS (Care Of Mental, Physical, And
Guidance for Developing Payment Models for COMPASS Collaborative Care Management for Depression and Diabetes and/or Cardiovascular Disease Introduction Within the COMPASS (Care Of Mental, Physical, And
Prior to implementation of the episode groups for use in resource measurement under MACRA, CMS should:
 Via Electronic Submission (www.regulations.gov) March 1, 2016 Andrew M. Slavitt Acting Administrator Centers for Medicare and Medicaid Services 7500 Security Boulevard Baltimore, MD episodegroups@cms.hhs.gov
Via Electronic Submission (www.regulations.gov) March 1, 2016 Andrew M. Slavitt Acting Administrator Centers for Medicare and Medicaid Services 7500 Security Boulevard Baltimore, MD episodegroups@cms.hhs.gov
June 25, Dear Administrator Verma,
 June 25, 2018 Seema Verma Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services Room 445 G, Hubert H. Humphrey Building 200 Independence Avenue SW Washington,
June 25, 2018 Seema Verma Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services Room 445 G, Hubert H. Humphrey Building 200 Independence Avenue SW Washington,
Keenan Pharmacy Care Management (KPCM)
 Keenan Pharmacy Care Management (KPCM) This program is an exclusive to KPS clients as an additional layer of pharmacy benefit management by engaging physicians and members directly to ensure that the best
Keenan Pharmacy Care Management (KPCM) This program is an exclusive to KPS clients as an additional layer of pharmacy benefit management by engaging physicians and members directly to ensure that the best
4/9/2016. The changing health care market THE CHANGING HEALTH CARE MARKET. CPAs & ADVISORS
 CPAs & ADVISORS experience support // ADVANCED PAYMENT MODELS: CJR Eric. M. Rogers MEd. RT(R) Managing Consultant The changing health care market THE CHANGING HEALTH CARE MARKET HHS goal of 30% of traditional
CPAs & ADVISORS experience support // ADVANCED PAYMENT MODELS: CJR Eric. M. Rogers MEd. RT(R) Managing Consultant The changing health care market THE CHANGING HEALTH CARE MARKET HHS goal of 30% of traditional
Prepared for North Gunther Hospital Medicare ID August 06, 2012
 Prepared for North Gunther Hospital Medicare ID 000001 August 06, 2012 TABLE OF CONTENTS Introduction: Benchmarking Your Hospital 3 Section 1: Hospital Operating Costs 5 Section 2: Margins 10 Section 3:
Prepared for North Gunther Hospital Medicare ID 000001 August 06, 2012 TABLE OF CONTENTS Introduction: Benchmarking Your Hospital 3 Section 1: Hospital Operating Costs 5 Section 2: Margins 10 Section 3:
Medicaid Payment Reform at Scale: The New York State Roadmap
 Medicaid Payment Reform at Scale: The New York State Roadmap ASTHO Technical Assistance Call June 22 nd 2015 Greg Allen Policy Director New York State Medicaid Overview Background and Brief History Delivery
Medicaid Payment Reform at Scale: The New York State Roadmap ASTHO Technical Assistance Call June 22 nd 2015 Greg Allen Policy Director New York State Medicaid Overview Background and Brief History Delivery
Patient-centered medical homes (PCMH): eligible providers.
 ACTION: Final DATE: 09/21/2018 3:40 PM 5160-1-71 Patient-centered medical homes (PCMH): eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model led by primary
ACTION: Final DATE: 09/21/2018 3:40 PM 5160-1-71 Patient-centered medical homes (PCMH): eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model led by primary
Telehealth: Overcoming the challenges of implementing innovative health care solutions
 Telehealth: Overcoming the challenges of implementing innovative health care solutions NRTRC 5 TH ANNUAL CONFERENCE MARCH 22, 2016 ROKI CHAUHAN, MD, FAAFP Disclaimer 2 The material presented here is being
Telehealth: Overcoming the challenges of implementing innovative health care solutions NRTRC 5 TH ANNUAL CONFERENCE MARCH 22, 2016 ROKI CHAUHAN, MD, FAAFP Disclaimer 2 The material presented here is being
Section 7. Medical Management Program
 Section 7. Medical Management Program Introduction Molina Healthcare maintains a medical management program to ensure patient safety as well as detect and prevent fraud, waste and abuse in its programs.
Section 7. Medical Management Program Introduction Molina Healthcare maintains a medical management program to ensure patient safety as well as detect and prevent fraud, waste and abuse in its programs.
Surviving and thriving in the time of MACRA: What you need to know now to optimize your future.
 Surviving and thriving in the time of MACRA: What you need to know now to optimize your future. Risk Adjustment in the Resource Use Performance Measures 2017 SGIM Annual Meeting Thursday, April 20, 2017
Surviving and thriving in the time of MACRA: What you need to know now to optimize your future. Risk Adjustment in the Resource Use Performance Measures 2017 SGIM Annual Meeting Thursday, April 20, 2017
Physician Compensation in an Era of New Reimbursement Models
 2014 IHA Annual Membership Meeting Physician Compensation in an Era of New Reimbursement Models Taryn E. Stone Ice Miller LLP (317) 236-5872 taryn.stone@ Agenda Background New Reimbursement Models Trends
2014 IHA Annual Membership Meeting Physician Compensation in an Era of New Reimbursement Models Taryn E. Stone Ice Miller LLP (317) 236-5872 taryn.stone@ Agenda Background New Reimbursement Models Trends
Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System
 Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System Karen Davis President, The Commonwealth Fund IOM Workshop Series: The Policy Agenda September
Eliminating Excessive, Unnecessary, and Wasteful Expenditures: Getting to a High Performance U.S. Health System Karen Davis President, The Commonwealth Fund IOM Workshop Series: The Policy Agenda September
March Data Jam: Using Data to Prepare for the MACRA Quality Payment Program
 March Data Jam: Using Data to Prepare for the MACRA Quality Payment Program Elizabeth Arend, MPH Quality Improvement Advisor National Council for Behavioral Health CMS Change Package: Primary and Secondary
March Data Jam: Using Data to Prepare for the MACRA Quality Payment Program Elizabeth Arend, MPH Quality Improvement Advisor National Council for Behavioral Health CMS Change Package: Primary and Secondary
MACRA Frequently Asked Questions
 Following the release of the Quality Payment Program Interim Final Rule, the American Medical Association (AMA) conducted numerous informational and training sessions for physicians and medical societies.
Following the release of the Quality Payment Program Interim Final Rule, the American Medical Association (AMA) conducted numerous informational and training sessions for physicians and medical societies.
Maryland s Integrated Care Network. Heading into Year Three
 Maryland s Integrated Care Network Heading into Year Three Facilitator David Finney Chief of Staff, CRISP Partner, Leap Orbit Learning Objectives At the end of this session, you will be able to Explain
Maryland s Integrated Care Network Heading into Year Three Facilitator David Finney Chief of Staff, CRISP Partner, Leap Orbit Learning Objectives At the end of this session, you will be able to Explain
Medicare Advantage Star Ratings
 Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Disease Management at Anthem West Or: what have we learned in trying to design these programs?
 Disease Management at Anthem West Or: what have we learned in trying to design these programs? Lisa M. Latts, MD, MSPH Regional Medical Director May 12, 2003 Anthem Inc. Anthem Inc. Headquarters: Indianapolis
Disease Management at Anthem West Or: what have we learned in trying to design these programs? Lisa M. Latts, MD, MSPH Regional Medical Director May 12, 2003 Anthem Inc. Anthem Inc. Headquarters: Indianapolis
Hospital Inpatient Quality Reporting (IQR) Program
 Clinical Episode-Based Payment (CEBP) Measures Questions & Answers Moderator Candace Jackson, RN Project Lead, Hospital IQR Program Hospital Inpatient Value, Incentives, and Quality Reporting (VIQR) Outreach
Clinical Episode-Based Payment (CEBP) Measures Questions & Answers Moderator Candace Jackson, RN Project Lead, Hospital IQR Program Hospital Inpatient Value, Incentives, and Quality Reporting (VIQR) Outreach
7/7/17. Value and Quality in Health Care. Kevin Shah, MD MBA. Overview of Quality. Define. Measure. Improve
 Value and Quality in Health Care Kevin Shah, MD MBA 1 Overview of Quality Define Measure 2 1 Define Health care reform is transitioning financing from volume to value based reimbursement Today Fee for
Value and Quality in Health Care Kevin Shah, MD MBA 1 Overview of Quality Define Measure 2 1 Define Health care reform is transitioning financing from volume to value based reimbursement Today Fee for
Examining the Differences Between Commercial and Medicare ACO Models
 Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
TO BE RESCINDED Patient-centered medical homes (PCMH): eligible providers.
 ACTION: Final DATE: 09/21/2018 3:40 PM TO BE RESCINDED 5160-1-71 Patient-centered medical homes (PCMH): eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model
ACTION: Final DATE: 09/21/2018 3:40 PM TO BE RESCINDED 5160-1-71 Patient-centered medical homes (PCMH): eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model
Calendar Year 2014 Medicare Physician Fee Schedule Final Rule
 Calendar Year 2014 Medicare Physician Fee Schedule Final Rule Non-Facility Cap After receiving many negative comments on this issue from physician groups, along with the House GOP Doctors Caucus letter
Calendar Year 2014 Medicare Physician Fee Schedule Final Rule Non-Facility Cap After receiving many negative comments on this issue from physician groups, along with the House GOP Doctors Caucus letter
Reducing Hospital Admissions Through the Use of IT. Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods
 Reducing Hospital Admissions Through the Use of IT Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods Conflict of Interest Steven Milligan, MD Has no real or apparent conflicts
Reducing Hospital Admissions Through the Use of IT Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods Conflict of Interest Steven Milligan, MD Has no real or apparent conflicts
WHITE PAPER. The Shift to Value-Based Care: 9 Steps to Readiness.
 The Shift to Value-Based Care: Table of Contents Overview 1 Value Based Care Is it here to stay? 1 1. Determine your risk tolerance 2 2. Know your cost structure 3 3. Establish your care delivery network
The Shift to Value-Based Care: Table of Contents Overview 1 Value Based Care Is it here to stay? 1 1. Determine your risk tolerance 2 2. Know your cost structure 3 3. Establish your care delivery network
Reinventing Health Care: Health System Transformation
 Reinventing Health Care: Health System Transformation Aspen Institute Patrick Conway, M.D., MSc CMS Chief Medical Officer Director, Center for Clinical Standards and Quality Acting Director, Center for
Reinventing Health Care: Health System Transformation Aspen Institute Patrick Conway, M.D., MSc CMS Chief Medical Officer Director, Center for Clinical Standards and Quality Acting Director, Center for
Healthcare 2015: Win-win or lose-lose?
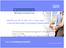 IBM Institute for Business Value Healthcare 2015: Win-win or lose-lose? A portrait and a path to successful transformation Presented at Disease Management Colloquium May 19, 2008 Jim Adams, IBM Center
IBM Institute for Business Value Healthcare 2015: Win-win or lose-lose? A portrait and a path to successful transformation Presented at Disease Management Colloquium May 19, 2008 Jim Adams, IBM Center
WELCOME. Kate Gainer, PharmD Executive Vice President and CEO Iowa Pharmacy Association
 WHAT IS MACRA? WELCOME Kate Gainer, PharmD Executive Vice President and CEO Iowa Pharmacy Association WELCOME Anthony Pudlo, PharmD, MBA, BCACP Vice President of Professional Affairs Iowa Pharmacy Association
WHAT IS MACRA? WELCOME Kate Gainer, PharmD Executive Vice President and CEO Iowa Pharmacy Association WELCOME Anthony Pudlo, PharmD, MBA, BCACP Vice President of Professional Affairs Iowa Pharmacy Association
Brave New World: The Effects of Health Reform Legislation on Hospitals. HFMA Annual National Meeting, Las Vegas, Nevada
 Brave New World: The Effects of Health Reform Legislation on Hospitals HFMA Annual National Meeting, Las Vegas, Nevada Highlights of PPACA Requires most Americans to have health insurance Expands coverage
Brave New World: The Effects of Health Reform Legislation on Hospitals HFMA Annual National Meeting, Las Vegas, Nevada Highlights of PPACA Requires most Americans to have health insurance Expands coverage
Collaborative and Coordinated:
 Collaborative and Coordinated: How Value-Based Care Programs are Driving Improvements in Quality and People s Health ISSUE DATE: NOVEMBER 2016 INTRODUCTION How the Shift from Volume to Value is Driving
Collaborative and Coordinated: How Value-Based Care Programs are Driving Improvements in Quality and People s Health ISSUE DATE: NOVEMBER 2016 INTRODUCTION How the Shift from Volume to Value is Driving
Patient-centered medical homes (PCMH): Eligible providers.
 ACTION: Final DATE: 09/20/2016 8:11 AM 5160-1-71 Patient-centered medical homes (PCMH): Eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model led by primary
ACTION: Final DATE: 09/20/2016 8:11 AM 5160-1-71 Patient-centered medical homes (PCMH): Eligible providers. (A) A Patient-centered medical home (PCMH) is a team-based care delivery model led by primary
Health Care Evolution
 Health Care Evolution Patient-Centered Medical Home to Clinical Integration & Accountable Care Ken Bertka, MD bertka@mindspring.com 419-346-8719 Agenda Top 3 Challenges of Health Care Reform PCMH & ACO
Health Care Evolution Patient-Centered Medical Home to Clinical Integration & Accountable Care Ken Bertka, MD bertka@mindspring.com 419-346-8719 Agenda Top 3 Challenges of Health Care Reform PCMH & ACO
