FAQS FOR UNIVERSITY OF SOUTH FLORIDA BUSINESS TRAVELERS
|
|
|
- Shana Austin
- 5 years ago
- Views:
Transcription
1 FAQS FOR UNIVERSITY OF SOUTH FLORIDA BUSINESS TRAVELERS How long am I covered? A: The plan covers you for trips that are taken related to USF business travel during September 1, 2017 and August 31, What is covered by the plan? A: 100% of reasonable expenses for medically necessary physician office visits, inpatient hospital services, physician and hospital outpatient services, and emergency hospital services up to a $250,000 maximum for outbound U.S. participants. Additional benefits for medically necessary services are also payable at 100% of reasonable expenses, subject to certain limitations or maximums (see the coverage overview grid below). COVERAGE Medical Benefits Period of Coverage Maximum Benefits Deductible Physician Office Visits Inpatient Hospital Services Hospital and Physician Outpatient Services Emergency Hospital Services Medical Benefit Limitations LIMITS ELIGIBLE PARTICIPANT $250,000 for Outbound U.S. Participants $0 for Outbound U.S. Participants Emergency medical treatment of pregnancy or Therapeutic termination of pregnancy Inpatient treatment of mental and nervous disorders including drug or alcohol abuse Outpatient treatment of mental and nervous disorders including drug or alcohol abuse Chiropractic Care Reasonable Expenses up $1,000 Maximum. Routine nursery care of a newborn child
2 COVERAGE Repairs to sound, natural teeth required due to an Injury Outpatient prescription drugs LIMITS ELIGIBLE PARTICIPANT ; $100 per tooth up to $500 Maximum 100% of actual charge OTHER COVERAGES Accidental Death & Dismemberment Repatriation of Remains Medical Evacuation Maximum Benefit: Principal Sum up to $25,000 for Eligible Participant 100% coverage under separate plan with UHCG 100% coverage under separate plan with UHCG Bedside Visit Emergency Response Center OTHER INCLUDED SERVICES Covered under separate plan with UHCG Emergency Medical and Travel Assistance services provided, including coordination of all evacuations and repatriations if needed Covered Medical Expenses 1. Hospital room and board expenses: the daily room rate when a Covered Person is Hospital confined; and general nursing care is provided and charged for by the Hospital. In computing the number of days payable under this benefit, the date of admission will be counted but not the date of discharge. 2. Ancillary hospital expenses: services and supplies including: operating room; laboratory tests; anesthesia; and medicines (excluding take home drugs) when Hospital confined. This does not include personal services of a non-medical nature. 3. Daily intensive care unit expenses: the daily room rate when a Covered Person is Hospital confined in a bed in the intensive care unit; and nursing services other than private duty nursing services. 4. Medical emergency care (room and supplies) expenses: incurred within 72 hours of an Accident and including: the attending Doctor s charges; X-rays; laboratory procedures; use of the emergency room; and supplies. 5. Outpatient surgical room and supply expenses for use of the surgical facility. 6. Outpatient: diagnostic x-rays; laboratory procedures; and tests. 7. Doctor non-surgical treatment/examination expenses (excluding medicines) including: the Doctor s initial visit; each Medically Necessary follow-up visit; and consultation visits when referred by the attending Doctor. 8. Doctor s surgical expenses 9. Outpatient laboratory test expenses.
3 10. Chiropractic expenses on an outpatient basis limited to one visit per day. 11. Dental expenses including dental x-rays for the repair or treatment of each injured tooth that is: whole; sound; and a natural tooth at the time of the Accident; and emergency alleviation of dental pain. 12. Air Ambulance expenses for transportation from the emergency site to the Hospital. 13. Prescription Drug Expenses including: dressings; drugs; and medicines prescribed by a Doctor. 14. Medical services and supplies: expenses for blood and blood transfusions; oxygen and its administration. 15. Expenses due to an aggravation or re-injury of a Pre-Existing Condition. 16. Emergency medical treatment of pregnancy. 17. Physical Therapy. 18. MRI/Cat scan and all other diagnostic imaging services. How do I find a covered provider/make an appointment? A: Contact UHCG s Emergency Response Center to schedule an appointment for you and arrange for direct payment to one of their doctors. The UHCG Emergency Response Center is available 24/7 by phone (call collect) or assistance@uhcglobal.com to assist you with everything from routine requests to medical emergencies. If you make your own appointment, contact the Emergency Response Center at least 24 hours prior to your appointment so UHCG can provide the doctor s office with a guarantee of payment. In many countries providers require this at the time of the visit. If this is not arranged prior to the visit, the doctor may require payment up front from you. What if I need a follow-up appointment? A: If the physician recommends a follow-up consultation, please provide this information to the UHCG Emergency Response Center in order to coordinate this appointment and arrange payment. To request these services, contact the Emergency Response Center by phone (call collect) or e- mail assistance@uhcglobal.com. What should I do in the event of a medical emergency? A: Go immediately to the nearest physician or hospital and then contact UHCG s Emergency Response Center by phone (call collect) or assistance@uhcglobal.com. UHCG coordinates emergency services with the coordination of our clinical team and a worldwide network of Physician Advisors. UHCG members in need of life-saving medical intervention are treated in Centers of Excellence around the world.
4 How do I enroll my dependent spouse or child(ren) traveling with me? A: Please call the enrollment center at to enroll your dependent spouse or child(ren). The daily rate for a dependent spouse or child is $2.58 per day. Can I extend my coverage for personal sojourns? A: Yes, please call the enrollment center at to extend your international trip coverage for up to 30 days (pre or post). The daily rate is $1.44 for students and $2.44 for employees. Are there any exclusions? A: Yes. We will not pay benefits for any loss or Injury that is caused by, or results from: 1. war or any act of war, whether declared or not. 2. piloting or serving as a crewmember. 3. commission of, or attempt to commit: a felony; an assault; or other illegal activity. 4. active participation in a riot, or insurrection. 5. flight in; boarding; or alighting from an aircraft or any craft designed to fly above the Earth s surface, except as: a) a fare-paying passenger on a regularly scheduled commercial or charter airline; b) a passenger in a non-scheduled, private aircraft used for pleasure purposes with no commercial intent during the flight; c) a passenger in a military aircraft flown by the Air Mobility Command or its foreign equivalent. 6. travel in or on any on-road or off-road motorized vehicle not requiring licensing as a motor vehicle. 7. Injury or Sickness covered by: Workers Compensation; Employer s Liability Laws; or benefits or while engaging in activity for monetary gain from sources other than the Policyholder. 8. an Accident that occurs while on active duty service in the: military; naval; or air force of any country or international organization. Upon Our receipt of proof of service, We will refund any premium paid for this time. Reserve or National Guard active duty training is not excluded unless it extends beyond 31 days. 9. Injury or Sickness where the Covered Person s Trip to the host country is undertaken for treatment or advice for such Injury or Sickness, except as provided in the Policy. 10. participation in any sports activity listed below not specifically authorized, sponsored and supervised by the Policyholder; 11. rugby; or cave diving; or rock climbing; or ice climbing; or mountain climbing; or base jumping; or bull riding; or heli-skiing; or surfing; or motorcycle racing; or climbing above 20,000 feet; including: bungee jumping; or parachuting; or skydiving; or parasailing; or hang-gliding; or caving or spelunking; or extreme skiing; or heli-skiing; or skiing outside marked trails; or mountain climbing; or ice climbing; or scuba diving; or professional or semi-professional sports; or extreme sports; or body contact sports; or hot-air ballooning; or base jumping; or sail gliding; or parakiting; or parkour; or racing including stunt show or speed test of any motorized or non-motorized vehicle; or rodeo activities
5 This insurance does not apply to the extent that trade or economic sanctions or regulations prohibit Us from providing insurance, including, but not limited to, the payment of claims. In addition to the exclusions above, We will not pay Medical Expense Benefits for any loss, treatment or services resulting from or contributed to by: 1. treatment by persons employed or retained by a Policyholder, or by any Immediate Family Member or member of the Covered Person s household. 2. treatment of: sickness; disease; or infections; except pyogenic infections or bacterial infections that result from the accidental ingestion of contaminated substances. 3. Injury or death to which a contributing cause is: the Covered Person s violation or attempt to violate any duly-enacted law; or the commission or attempt to commit an assault or a felony; or that occurs while the Covered Person is engaged in an illegal occupation. 4. Injury or death caused while: riding in or on; entering into or alighting from; or being struck by a 2 or 3-wheeled motor vehicle or a motor vehicle not designed primarily for use on public streets and highways. 5. cosmetic surgery, except for reconstructive surgery needed as the result of an Injury or Sickness. 6. Any: elective treatment; surgery; health treatment; or examination; including any: service; treatment; or supplies that: (a) are deemed by Us to be experimental; and (b) are not recognized and generally accepted medical practices in the United States. 7. treatment or service provided by a private duty nurse. 8. replacement of: artificial limbs; eyes; and larynx. 9. eye refractions or eye examinations for the purpose of prescribing corrective lenses or for the fitting thereof, unless caused by an Injury incurred while covered under the Policy. 10. conditions that are not caused by a Covered Accident or Sickness. 11. participation in any activity or hazard not specifically covered by the Policy. 12. Any: treatment; service; or supply not specifically covered by the Policy. 13. Any: treatment; services; or supplies received by the Covered Person that are incurred or received while he or she is in his or her Home Country. 14. personal comfort or convenience items. These include but are not limited to: Hospital telephone charges; television rental; or guest meals. 15. pregnancy or childbirth. This does not apply if treatment is required as a result of a Covered Accident. 16. routine nursery care. 17. routine physicals. 18. cosmetic or plastic surgery, except as a result of Injury. 19. elective surgery. 20. birth defects and congenital anomalies; or complications which arise from such conditions. 21. new eye glasses or contact lenses; eye examinations related to the correction of vision or related to the fitting of glasses or contact lenses; or repair or replacement of existing eye glasses or contact lenses. 22. routine dental care and treatment. 23. rest cures or custodial care. 24. organ or tissue transplants and related services. 25. Injury sustained while participating in professional; or semiprofessional sports.confinement or institutional care.
6 26. maternity and routine nursery care. 27. any expenses covered by any other employer or government sponsored plan for which, and to the extent that the Covered Person is eligible for reimbursement. 28. Services; supplies; or treatment including any period of Hospital confinement which were not: recommended; approved; and certified as necessary and reasonable by a Doctor; or expenses which are non-medical in nature. 29. treatment relating to: birth defects; and congenital conditions; or complications arising from those conditions. 30. sexually transmitted diseases or immune deficiency disorders and related conditions. This exclusion does not apply to the care or treatments of: Acquired Immune Deficiency Syndrome (AIDS); AIDS Related Complex (ARC); or Human Immunodeficiency Virus (HIV) infection, or any illness or disease arising from these medical conditions. 31. expenses incurred for services related to the diagnostic treatment of infertility or other problems related to the inability to conceive a child, unless such infertility is a result of a covered Injury or Sickness. 32. expenses incurred for surgical procedures and devices related to birth control. 33. nasal or sinus surgery, except surgery made necessary as the result of a covered Injury a deviated nasal septum including sub mucous resection and surgical correction thereof. 34. treatment of acne. 35. expenses incurred for Trips taken for the purpose of seeking medical care.
Security Forces SCHEDULE OF BENEFITS Participating Provider Covered Person pays:
 Benefit Local Office Visits/Physician Consultation (per visit/occurrence) Primary Care, Specialist and Walk in Clinics Security Forces Participating Provider Prescription Service rendered at a pharmacy
Benefit Local Office Visits/Physician Consultation (per visit/occurrence) Primary Care, Specialist and Walk in Clinics Security Forces Participating Provider Prescription Service rendered at a pharmacy
Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses
 Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses Extra benefits when you need them Do you have security in knowing you have help handling your medical expenses? You can with
Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses Extra benefits when you need them Do you have security in knowing you have help handling your medical expenses? You can with
Protection Series Recovery Care Insurance Plans
 Underwritten by Continental Life Insurance Company of Brentwood, Tennessee An Aetna Company Protection Series Recovery Care Insurance Plans SM Security solutions. For peace of mind protection. North Carolina
Underwritten by Continental Life Insurance Company of Brentwood, Tennessee An Aetna Company Protection Series Recovery Care Insurance Plans SM Security solutions. For peace of mind protection. North Carolina
Regence Engage Plan Highlights For Groups of /1/2016
 Plan Features Provider choice: Members have direct access to their choice of providers. Category 1 are Preferred; Category 2 are Participating; and Category 3 are Non-contracted providers. Simplicity:
Plan Features Provider choice: Members have direct access to their choice of providers. Category 1 are Preferred; Category 2 are Participating; and Category 3 are Non-contracted providers. Simplicity:
PRUPARENT/PRUHOSPITAL INCOME ROOM & BOARD/SURGICAL BENEFIT MEDICAL REPORT FORM (To be completed by Medical Attendant)
 Reg. 199002477Z PRUPARENT/PRUHOSPITAL INCOME ROOM & BOARD/SURGICAL BENEFIT MEDICAL REPORT FORM (To be completed by Medical Attendant) Policy Number Part 1 Medical Information 1. Name of Patient 2. NRIC
Reg. 199002477Z PRUPARENT/PRUHOSPITAL INCOME ROOM & BOARD/SURGICAL BENEFIT MEDICAL REPORT FORM (To be completed by Medical Attendant) Policy Number Part 1 Medical Information 1. Name of Patient 2. NRIC
Personal Accident Claim - Doctor s Statement
 Personal Accident Claim - Doctor s Statement SECTION 2 DOCTOR S STATEMENT (to be completed by the attending Doctor at claimant s expense) A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport
Personal Accident Claim - Doctor s Statement SECTION 2 DOCTOR S STATEMENT (to be completed by the attending Doctor at claimant s expense) A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport
NY EPO OA 1-09 v Page 1
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance (applies to all expenses unless otherwise stated) Maximum Out-of-Pocket Limit (per calendar year) Lifetime Maximum (per member lifetime)
PLAN FEATURES Deductible (per calendar year) Member Coinsurance (applies to all expenses unless otherwise stated) Maximum Out-of-Pocket Limit (per calendar year) Lifetime Maximum (per member lifetime)
Single/Family $2,500/$5,000 $5,000/$10,000. Single/Family $6,000/$12,000 $10,000/None. Single/Family $5,000/$10,000 $6,250/$12,500
 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Regence EmployeeChoice Plan Highlights Platinum 250, Platinum 500, Gold 500, Gold 1000, Gold 1500, Silver 2500, Bronze Essential /1/2016
 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Welcome Plan. Basic health insurance for temporary, new and returning Canadian residents
 Welcome Plan Basic health insurance for temporary, new and returning Canadian residents Help your newest plan members feel at home Recognizing the skills and fresh perspectives that a diverse organization
Welcome Plan Basic health insurance for temporary, new and returning Canadian residents Help your newest plan members feel at home Recognizing the skills and fresh perspectives that a diverse organization
MEDICAL PLAN EXCLUSIONS. For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered:
 MEDICAL PLAN EXCLUSIONS For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered: (1) Abortion. Services, supplies, care or treatment in connection with an
MEDICAL PLAN EXCLUSIONS For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered: (1) Abortion. Services, supplies, care or treatment in connection with an
Aetna Health of California, Inc.
 Easily locate PrimeCare participating providers at www.aetna.com/docfind/primecare PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral
Easily locate PrimeCare participating providers at www.aetna.com/docfind/primecare PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral
OVERVIEW OF YOUR BENEFITS
 OVERVIEW OF YOUR BENEFITS IMPORTANT PHONE NUMBERS Member Services Department (646) 473-9200 For answers to questions about your benefits or to be referred to another Benefit Fund department. Program for
OVERVIEW OF YOUR BENEFITS IMPORTANT PHONE NUMBERS Member Services Department (646) 473-9200 For answers to questions about your benefits or to be referred to another Benefit Fund department. Program for
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived 30% after deductible
 PLAN FEATURES NON- Deductible (per calendar year) $500 Individual $750 Individual $1,500 Family $2,250 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and
PLAN FEATURES NON- Deductible (per calendar year) $500 Individual $750 Individual $1,500 Family $2,250 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and
Covered Benefits Rhody Health Partners ACA Adult Expansion
 Covered s Rhody Health Partners ACA Adult Expansion Abortion Services Adult Day Services AIDS Medical and Non-Medical Case Management Alcohol and Substance Abuse Treatment Cosmetic Surgery Dental Care
Covered s Rhody Health Partners ACA Adult Expansion Abortion Services Adult Day Services AIDS Medical and Non-Medical Case Management Alcohol and Substance Abuse Treatment Cosmetic Surgery Dental Care
Single/Family $2,500/$5,000 $5,000/$10,000. Single/Family $6,000/$12,000 $10,000/None. Single/Family $5,000/$10,000 $6,250/$12,500
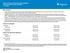 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of- Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of- Network provider, the
HEALTH SAVINGS ACCOUNT (HSA)
 HSA FEATURES Health Savings Account Amount $600 Employee $1,000 Family Amount contributed to the HSA by the employer. Funded on a quarterly basis. HSA amount reflected is on a per calendar year basis.
HSA FEATURES Health Savings Account Amount $600 Employee $1,000 Family Amount contributed to the HSA by the employer. Funded on a quarterly basis. HSA amount reflected is on a per calendar year basis.
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
Amherst Central School District First Choice Health Plan. Non-First Choice Providers and Out-of-Network Providers
 Health: Hospital Services provided by First Choice Preferred Provider Network Medical Services Radiology, Ultrasounds 20% after $500 individual or Laboratory Testing 20% after $500 individual or MRI and
Health: Hospital Services provided by First Choice Preferred Provider Network Medical Services Radiology, Ultrasounds 20% after $500 individual or Laboratory Testing 20% after $500 individual or MRI and
Covered Benefits Rhody Health Partners
 Covered s Rhody Health Partners s Covered by UnitedHealthcare Community Plan As member of UnitedHealthcare Community Plan, you are covered for the following services. (Remember to always show your current
Covered s Rhody Health Partners s Covered by UnitedHealthcare Community Plan As member of UnitedHealthcare Community Plan, you are covered for the following services. (Remember to always show your current
CA Group Business 2-50 Employees
 PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
CALIFORNIA Small Group HMO Aetna Health of California, Inc. Plan Effective Date: 04/01/2007. Aetna Value Network* HMO $30/$40
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral Requirement PHYSICIAN SERVICES CALIFORNIA Small Group HMO Primary Care Physician
PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral Requirement PHYSICIAN SERVICES CALIFORNIA Small Group HMO Primary Care Physician
PREFERRED CARE. combination of family members; however no single individual within the family will be subject to more than the individual
 PLAN FEATURES Deductible (per plan year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The family Deductible is a cumulative Deductible
PLAN FEATURES Deductible (per plan year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The family Deductible is a cumulative Deductible
PLAN FEATURES PREFERRED CARE
 PLAN DESIGN & BENEFITS - "HMO" PLAN FEATURES Deductible (per calendar year) $200 Individual $400 Family All covered expenses, excluding prescription drugs, accumulate toward the preferred Deductible. Unless
PLAN DESIGN & BENEFITS - "HMO" PLAN FEATURES Deductible (per calendar year) $200 Individual $400 Family All covered expenses, excluding prescription drugs, accumulate toward the preferred Deductible. Unless
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
Benefits are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 PLAN FEATURES Annual Deductible The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Hearing aid reimbursement does not apply to the out-of-pocket
PLAN FEATURES Annual Deductible The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Hearing aid reimbursement does not apply to the out-of-pocket
Page 1 CONTRA COSTA COMMUNITY COLLEGE DISTRICT October 2013 SUMMARY OF HEALTH PLAN BENEFITS
 Page 1 CONTRA COSTA COMMUNITY COLLEGE DISTRICT October 2013 Hospital Room Services Hospital Outpatient Surgery Maternity Skilled Nursing Facility Lab, Xray and Diagnostic Testing Home Health Care Mental
Page 1 CONTRA COSTA COMMUNITY COLLEGE DISTRICT October 2013 Hospital Room Services Hospital Outpatient Surgery Maternity Skilled Nursing Facility Lab, Xray and Diagnostic Testing Home Health Care Mental
SUMMARY OF BENEFITS. Hamilton County Department of Education Network Copay Plan. Connecticut General Life Insurance Co.
 SUMMARY OF BENEFITS Connecticut General Life Insurance Co. Hamilton County Department of Education Annual deductibles and maximums Lifetime maximum Pre-Existing Condition Limitation (PCL) Coinsurance All
SUMMARY OF BENEFITS Connecticut General Life Insurance Co. Hamilton County Department of Education Annual deductibles and maximums Lifetime maximum Pre-Existing Condition Limitation (PCL) Coinsurance All
2017 Summary of Benefits
 H5209 004_DSB9 23 16 File & Use 10/14/2016 DHS Approved 10 7 2016 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP) January 1, 2017 to December
H5209 004_DSB9 23 16 File & Use 10/14/2016 DHS Approved 10 7 2016 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP) January 1, 2017 to December
1199SEIU Greater New York Benefit Fund OVERVIEW OF YOUR BENEFITS
 1199SEIU Greater New York Benefit Fund OVERVIEW OF YOUR BENEFITS I HOSPITAL CARE This benefit is for the hospital s charge for the use of its facility only. Coverage for services rendered by doctors, labs,
1199SEIU Greater New York Benefit Fund OVERVIEW OF YOUR BENEFITS I HOSPITAL CARE This benefit is for the hospital s charge for the use of its facility only. Coverage for services rendered by doctors, labs,
SECTION II YOUR HEALTH BENEFITS
 54 SECTION II YOUR HEALTH BENEFITS A. Participating Providers Member Choice Panel Providers B. Using Your Benefits Wisely 1199SEIU Care Review Ambulatory/Outpatient Surgery Pre-Certification Managed Care
54 SECTION II YOUR HEALTH BENEFITS A. Participating Providers Member Choice Panel Providers B. Using Your Benefits Wisely 1199SEIU Care Review Ambulatory/Outpatient Surgery Pre-Certification Managed Care
BCBSM provides administrative claims services only. Your employer or plan sponsor is financially responsible for claims.
 Michigan Catholic Conference Group Number: 71755 Package Code(s): 010 Section Code(s): 1000, 2000 PPO - PPO1, Hearing, Vision ( Exam only) Effective Date: 01/01/2018 Benefits-at-a-glance This is intended
Michigan Catholic Conference Group Number: 71755 Package Code(s): 010 Section Code(s): 1000, 2000 PPO - PPO1, Hearing, Vision ( Exam only) Effective Date: 01/01/2018 Benefits-at-a-glance This is intended
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION
 Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
$10 copay. $10 copay. $10 copay $5 copay $10 copay $5 copay. $10 copay. No charge. No charge. No charge
 PLAN FEATURES * ** Deductible (per calendar ) Member Coinsurance Copay Maximum (per calendar ) Lifetime Maximum Unlimited Primary Care Physician Selection Required Upon enrollment to a Vitalidad Plus plan,
PLAN FEATURES * ** Deductible (per calendar ) Member Coinsurance Copay Maximum (per calendar ) Lifetime Maximum Unlimited Primary Care Physician Selection Required Upon enrollment to a Vitalidad Plus plan,
Chapter 12 Benefits and Covered Services
 12 Benefits and Covered Services Health Choice Generations covers the same benefits covered under Original Medicare. Sometimes Medicare adds coverage for a new service during the year. Health Choice Generations
12 Benefits and Covered Services Health Choice Generations covers the same benefits covered under Original Medicare. Sometimes Medicare adds coverage for a new service during the year. Health Choice Generations
Benefits at a Glance. Vectrus Systems Corporation Policy Number: 04804A. OAP Global Plan
 Benefits at a Glance Vectrus Systems Corporation Policy Number: 04804A OAP Global Plan Vectrus Systems Corporation Long Benefits at a Glance Policy # 04804A Effective Date January 1, 2016 Vectrus Systems
Benefits at a Glance Vectrus Systems Corporation Policy Number: 04804A OAP Global Plan Vectrus Systems Corporation Long Benefits at a Glance Policy # 04804A Effective Date January 1, 2016 Vectrus Systems
2016 Medical Plan Comparison Chart
 2016 Medical Plan Comparison Chart WellStar Health System is committed to helping you control healthcare costs while providing more choices and personal control over your healthcare coverage through the
2016 Medical Plan Comparison Chart WellStar Health System is committed to helping you control healthcare costs while providing more choices and personal control over your healthcare coverage through the
Blue Cross Premier Bronze
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within BCBSM s unsurpassed statewide PPO network including nationwide coverage.
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within BCBSM s unsurpassed statewide PPO network including nationwide coverage.
WHAT DOES MEDICALLY NECESSARY MEAN?
 WHAT DOES MEDICALLY NECESSARY MEAN? Your Primary Care Provider (PCP) will help you get the services you need that are medically necessary as defined below. Medically Necessary means appropriate and necessary
WHAT DOES MEDICALLY NECESSARY MEAN? Your Primary Care Provider (PCP) will help you get the services you need that are medically necessary as defined below. Medically Necessary means appropriate and necessary
INTRODUCING OUR RANGE OF BUSINESS HEALTH PLANS A COLLABORATION BETWEEN TWO OF THE MOST RESPECTED NAMES IN GLOBAL HEALTHCARE
 INTRODUCING OUR RANGE OF HEALTH PLANS A COLLABORATION BETWEEN TWO OF THE MOST RESPECTED NAMES IN GLOBAL HEALTHCARE 1st January 2017 TWO OF THE BIGGEST, MOST TRUSTED NAMES IN GLOBAL HEALTHCARE Bupa Global
INTRODUCING OUR RANGE OF HEALTH PLANS A COLLABORATION BETWEEN TWO OF THE MOST RESPECTED NAMES IN GLOBAL HEALTHCARE 1st January 2017 TWO OF THE BIGGEST, MOST TRUSTED NAMES IN GLOBAL HEALTHCARE Bupa Global
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Primary Care Physician Selection Optional There is no requirement for member pre-certification.
The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Primary Care Physician Selection Optional There is no requirement for member pre-certification.
Hang Seng Bank strives to provide quality health insurance services to customers and jointly offers a range of medical protection schemes with Bupa.
 1 Hang Seng Bank strives to provide quality health insurance services to customers and jointly offers a range of medical protection schemes with Bupa. A health insurance specialist in Hong Kong, Bupa is
1 Hang Seng Bank strives to provide quality health insurance services to customers and jointly offers a range of medical protection schemes with Bupa. A health insurance specialist in Hong Kong, Bupa is
BlueChoice Opt-Out Open Access
 BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay 1 Out-of-Network You Pay 1 24/7 FIRSTHELP NURSE ADVICE LINE Free advice from a registered nurse BLUE REWARDS Visit www.carefirst.com/bluerewards
BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay 1 Out-of-Network You Pay 1 24/7 FIRSTHELP NURSE ADVICE LINE Free advice from a registered nurse BLUE REWARDS Visit www.carefirst.com/bluerewards
Medi-Cal Program. Benefit. Benefits Chart
 Chart Please note that the table below is only a summary. More details about benefits can be found in the section of the Medi-Cal Evidence of Coverage booklet. All health care is arranged through your
Chart Please note that the table below is only a summary. More details about benefits can be found in the section of the Medi-Cal Evidence of Coverage booklet. All health care is arranged through your
Cigna Health and Life Insurance Company. Plan Benefits. Unlimited. Unlimited. Not applicable. Not applicable. Not applicable
 SUMMARY OF BENEFITS Client Name: Washington County Public Schools Benefit Option Name: Medicare Supplement Effective: July 1, 2018 through June 30, 2019 1 Benefit Description Lifetime Maximum Applies to
SUMMARY OF BENEFITS Client Name: Washington County Public Schools Benefit Option Name: Medicare Supplement Effective: July 1, 2018 through June 30, 2019 1 Benefit Description Lifetime Maximum Applies to
Benefit Explanation And Limitations
 Benefit Explanation And Limitations SFHP providers supply many medical benefits and services, some of which are itemized on the following pages. For specific information not covered in this table, please
Benefit Explanation And Limitations SFHP providers supply many medical benefits and services, some of which are itemized on the following pages. For specific information not covered in this table, please
Kaiser Permanente Group Plan 301 Benefit and Payment Chart
 301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
Schedule of Benefits
 3T, 09/09 Schedule of Benefits Services listed below are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and Out-of-Network. Coverage
3T, 09/09 Schedule of Benefits Services listed below are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and Out-of-Network. Coverage
T M A V e r s i o n TABLE OF CONTENTS PART DEFINITIONS
 (a) General. 1 (b) Specific definitions. 1 Abortion. 1 Absent treatment. 1 Abuse. 1 Abused dependent. 1 Accidental injury. 2 Active duty. 2 Active duty member. 2 Activities of daily living. 2 Acupuncture.
(a) General. 1 (b) Specific definitions. 1 Abortion. 1 Absent treatment. 1 Abuse. 1 Abused dependent. 1 Accidental injury. 2 Active duty. 2 Active duty member. 2 Activities of daily living. 2 Acupuncture.
Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Your Summary of Benefits ACO Flex
 Your Summary of Benefits ACO Flex Premier ACO Flex 250/15/30 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
Your Summary of Benefits ACO Flex Premier ACO Flex 250/15/30 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS
 SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS 1. General Exclusions. In addition to the Plan's other restrictions, no Plan benefit is payable for any of the following
SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS 1. General Exclusions. In addition to the Plan's other restrictions, no Plan benefit is payable for any of the following
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA HEALTH PLANS INC.
 Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN FEATURES Network Providers Annual Maximum Out-of-Pocket Amount $2,500 The maximum out-of-pocket limit applies to all
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN FEATURES Network Providers Annual Maximum Out-of-Pocket Amount $2,500 The maximum out-of-pocket limit applies to all
Schedule of Benefits-EPO
 Schedule of Benefits-EPO [Plan Information] [Health Plan:] [Ambetter Balanced Care 3 (2018)-Standard Silver On Exchange Plan] [Primary Member:] [John Doe] [Member ID:] [01213456] [Date of Birth:] [08/12/62]
Schedule of Benefits-EPO [Plan Information] [Health Plan:] [Ambetter Balanced Care 3 (2018)-Standard Silver On Exchange Plan] [Primary Member:] [John Doe] [Member ID:] [01213456] [Date of Birth:] [08/12/62]
Anthem Blue Cross Your Plan: Custom Premier HMO 25/100 admit 3 day max/100 OP Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Custom Premier HMO 25/100 admit 3 day max/100 OP Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Premier HMO 25/100 admit 3 day max/100 OP Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Vivity offered by Anthem Blue Cross Your Plan: Custom Classic HMO 25/45/500 Admit /250 OP Your Network: Vivity
 Vivity offered by Anthem Blue Cross Your Plan: Custom Classic HMO 25/45/500 Admit /250 OP Your : Vivity This summary of benefits is a brief outline of coverage, designed to help you with the selection
Vivity offered by Anthem Blue Cross Your Plan: Custom Classic HMO 25/45/500 Admit /250 OP Your : Vivity This summary of benefits is a brief outline of coverage, designed to help you with the selection
FLEX RETIREE MAP (Over 65 Flex Retirees) 2018 Benefits PROFESSIONAL SERVICES. Visit to a physician, physician assistant or nurse practitioner at a PPG
 PROFESSIONAL SERVICES Visit to a physician, physician assistant or nurse practitioner at a PPG Periodic health evaluations/preventive services - Applies when the only service(s) provided is a Medicare
PROFESSIONAL SERVICES Visit to a physician, physician assistant or nurse practitioner at a PPG Periodic health evaluations/preventive services - Applies when the only service(s) provided is a Medicare
Anthem Blue Cross Your Plan: Modified Classic HMO 15/30/250 Admit/125 OP Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Modified Classic HMO 15/30/250 Admit/125 OP Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Modified Classic HMO 15/30/250 Admit/125 OP Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Benefits are effective January 01, 2017 through December 31, 2017
 Benefits are effective January 01, 2017 through December 31, 2017 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY PLAN FEATURES Network & Out-of- Annual Deductible $0 This is the amount
Benefits are effective January 01, 2017 through December 31, 2017 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY PLAN FEATURES Network & Out-of- Annual Deductible $0 This is the amount
HOME BANK - S2395 NON-GRANDFATHERED CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET
 CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to 26 180 days from incurred Filing Limit date, except when 180 days would
CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to 26 180 days from incurred Filing Limit date, except when 180 days would
Summary of Benefits. January 1, 2018 December 31, Providence Medicare Dual Plus (HMO SNP)
 Summary of Benefits January 1, 2018 December 31, 2018 Providence Medicare Dual Plus (HMO SNP) This plan is available in Clackamas, Multnomah and Washington counties in Oregon for members who are eligible
Summary of Benefits January 1, 2018 December 31, 2018 Providence Medicare Dual Plus (HMO SNP) This plan is available in Clackamas, Multnomah and Washington counties in Oregon for members who are eligible
Vivity offered by Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your Network: Vivity
 Vivity offered by Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your : Vivity This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Vivity offered by Anthem Blue Cross Your Plan: Custom Premier HMO 10/100% Your : Vivity This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN FEATURES Network & Out-of- Annual Deductible This is the amount you have to pay out of pocket before the plan will pay
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN FEATURES Network & Out-of- Annual Deductible This is the amount you have to pay out of pocket before the plan will pay
FCPS BENEFITS COMPARISON FOR PLAN YEAR 2018 Active Employees and Retirees Under 65
 BENEFIT Medical Lifetime Maximum Unlimited Unlimited Unlimited Unlimited Unlimited Individual Annual Deductible $250 $500 $250 $500 None Family Annual Deductible $500 $1,000 $500 $1,000 None Medical Plan
BENEFIT Medical Lifetime Maximum Unlimited Unlimited Unlimited Unlimited Unlimited Individual Annual Deductible $250 $500 $250 $500 None Family Annual Deductible $500 $1,000 $500 $1,000 None Medical Plan
Covered Services List
 CAREPLUS Covered Services List For CeltiCare Health with MassHealth CarePlus Coverage This is a list of all covered services and benefits for MassHealth CarePlus enrolled in CeltiCare Health. The list
CAREPLUS Covered Services List For CeltiCare Health with MassHealth CarePlus Coverage This is a list of all covered services and benefits for MassHealth CarePlus enrolled in CeltiCare Health. The list
PLAN DESIGN AND BENEFITS - PA POS 4.2 with $5/$15/$30 RX PARTICIPATING PROVIDERS
 PLAN FEATURES Deductible (per calendar year) PHYSICIAN SERVICES Primary Care Physician Visits Specialist Office Visits Maternity OB Visits Allergy Treatment Allergy Testing PREVENTIVE CARE Routine Adult
PLAN FEATURES Deductible (per calendar year) PHYSICIAN SERVICES Primary Care Physician Visits Specialist Office Visits Maternity OB Visits Allergy Treatment Allergy Testing PREVENTIVE CARE Routine Adult
Anthem Blue Cross Your Plan: Modified Classic HMO 20/40/250 Admit /125 OP Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Modified Classic HMO 20/40/250 Admit /125 OP Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Modified Classic HMO 20/40/250 Admit /125 OP Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Services Covered by Molina Healthcare
 Services Covered by Molina Healthcare As a Molina Healthcare member, you will continue to receive all medically-necessary Medicaid-covered services at no cost to you. The following list of covered services
Services Covered by Molina Healthcare As a Molina Healthcare member, you will continue to receive all medically-necessary Medicaid-covered services at no cost to you. The following list of covered services
MEMBER CERTIFICATE BCN 1 SCHEDULE OF BENEFITS
 MEMBER CERTIFICATE BCN 1 SCHEDULE OF BENEFITS PLEASE NOTE: This Schedule of Benefits is only part of the Certificate. Please refer to it in conjunction with the Health Plan booklet entitled General Provisions.
MEMBER CERTIFICATE BCN 1 SCHEDULE OF BENEFITS PLEASE NOTE: This Schedule of Benefits is only part of the Certificate. Please refer to it in conjunction with the Health Plan booklet entitled General Provisions.
Benefit Coverage (Cal. Code Regs., tit. 22, 51328, ) (DHCS Contract , Amend. 10, Exhibit A, Attach. 11, 7)
 Revised: January 2004 Chemical Dependency Rehabilitation Benefit Coverage (Cal. Code Regs., tit. 22, 51328, 51341.1) (DHCS Contract 04-35765, Amend. 10, Exhibit A, Attach. 11, 7) Health care services necessary
Revised: January 2004 Chemical Dependency Rehabilitation Benefit Coverage (Cal. Code Regs., tit. 22, 51328, 51341.1) (DHCS Contract 04-35765, Amend. 10, Exhibit A, Attach. 11, 7) Health care services necessary
Medicare Basics. Part I of II
 Part I of II August 2013 1 What are the Four Parts of Medicare? Part A Hospital Insurance Part B Medical Insurance Part C Medicare Advantage Plans, like HMOs and PPOs Includes Part A & B and usually Part
Part I of II August 2013 1 What are the Four Parts of Medicare? Part A Hospital Insurance Part B Medical Insurance Part C Medicare Advantage Plans, like HMOs and PPOs Includes Part A & B and usually Part
SASKATCHEWAN HEALTH BENEFITS (SK HB)
 SASKATCHEWAN HEALTH BENEFITS (SK HB) Overview Updated: October 30, 2014 Eligibility If you make your home in Saskatchewan and you ordinarily live in the province at least six months a year, you are eligible
SASKATCHEWAN HEALTH BENEFITS (SK HB) Overview Updated: October 30, 2014 Eligibility If you make your home in Saskatchewan and you ordinarily live in the province at least six months a year, you are eligible
2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits
 2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits For Oregon counties: Clackamas, Clatsop, Columbia, Jackson, Josephine, Multnomah, Tillamook, Washington and Yamhill H5859_1099_CO_1018 CMS
2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits For Oregon counties: Clackamas, Clatsop, Columbia, Jackson, Josephine, Multnomah, Tillamook, Washington and Yamhill H5859_1099_CO_1018 CMS
MyHPN Solutions HMO Gold 7
 MyHPN Solutions HMO Gold 7 HIOS ID: 95865NV0030074 Attachment A Benefit Schedule Calendar Year Deductible (CYD): $3,000 of EME per Member and $6,000 of EME per family. The Calendar Year Out of Pocket Maximum
MyHPN Solutions HMO Gold 7 HIOS ID: 95865NV0030074 Attachment A Benefit Schedule Calendar Year Deductible (CYD): $3,000 of EME per Member and $6,000 of EME per family. The Calendar Year Out of Pocket Maximum
Anthem Blue Cross Your Plan: BC PPO Exclusive Plan
 Anthem Blue Cross Your Plan: BC PPO Exclusive Plan This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect each and every
Anthem Blue Cross Your Plan: BC PPO Exclusive Plan This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect each and every
RFS-7-62 ATTACHMENT E INDIANA CARE SELECT PROGRAM DESCRIPTION AND COVERED BENEFITS
 The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
New to Medicaid? 22 Medicaid Services You Should Know About
 New to Medicaid? 22 Medicaid Services You Should Know About Here Are 22 Medicaid Services You Should Know About This year Connecticut expanded Medicaid healthcare coverage (HUSKY) by raising the maximum
New to Medicaid? 22 Medicaid Services You Should Know About Here Are 22 Medicaid Services You Should Know About This year Connecticut expanded Medicaid healthcare coverage (HUSKY) by raising the maximum
GIC Employees/Retirees without Medicare
 GIC Active Employees & Retirees without Medicare 7/1/18 GIC Employees/Retirees without Medicare HMO Summary of Benefits Chart This chart provides a summary of key services offered by your Health New England
GIC Active Employees & Retirees without Medicare 7/1/18 GIC Employees/Retirees without Medicare HMO Summary of Benefits Chart This chart provides a summary of key services offered by your Health New England
Anthem Blue Cross Your Plan: Core PPO Your Network: National PPO (BlueCard PPO)
 Anthem Blue Cross Your Plan: Core PPO Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Anthem Blue Cross Your Plan: Core PPO Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
The MITRE Corporation Plan
 Benefit Type Plan Year Type Calendar Year Annual Medical Out of (for certain services) Employee Employee + 1 Family Annual Prescription Drug Out of Employee Employee + 1 Family Copayments: One copay per
Benefit Type Plan Year Type Calendar Year Annual Medical Out of (for certain services) Employee Employee + 1 Family Annual Prescription Drug Out of Employee Employee + 1 Family Copayments: One copay per
THIS INFORMATION IS NOT LEGAL ADVICE
 Medicaid Medicaid is a federal/state program that gives certain groups of people a card that can be used to get free medical care, nursing home care, and prescription drugs at reduced prices. In general,
Medicaid Medicaid is a federal/state program that gives certain groups of people a card that can be used to get free medical care, nursing home care, and prescription drugs at reduced prices. In general,
See Covered Benefits below. None. $2,000 per Member per calendar year $4,000 per family per calendar year
 Schedule of s Harvard Pilgrim Health Care, Inc. THE HARVARD PILGRIM HMO MAINE ID: MD0000002653_F2 X This Schedule of s summarizes your s under The Harvard Pilgrim HMO (the Plan) and states the Member Cost
Schedule of s Harvard Pilgrim Health Care, Inc. THE HARVARD PILGRIM HMO MAINE ID: MD0000002653_F2 X This Schedule of s summarizes your s under The Harvard Pilgrim HMO (the Plan) and states the Member Cost
Smart Start. Level of cover with Australian Unity. Cover availability. Excess options. Hospital and Extras Cover Effective from 15 December 2017 $100
 Hospital and Extras Cover Effective from 15 December 2017 Level of cover with Australian Unity Cover availability Excess options $100 HOSPITAL BASIC EXTRAS BASIC SINGLE COUPLE EXCESS Excess is waived for
Hospital and Extras Cover Effective from 15 December 2017 Level of cover with Australian Unity Cover availability Excess options $100 HOSPITAL BASIC EXTRAS BASIC SINGLE COUPLE EXCESS Excess is waived for
SERVICES COVERAGE LIMITS/ EXCLUSIONS Alcohol, Drug, and Substance Abuse Services
 SERVICES COVERAGE LIMITS/ EXCLUSIONS Alcohol, Drug, and Substance Abuse Services Alcohol, drug, and substance abuse treatment services are provided by the Department of Alcohol and Other Drug Abuse Services
SERVICES COVERAGE LIMITS/ EXCLUSIONS Alcohol, Drug, and Substance Abuse Services Alcohol, drug, and substance abuse treatment services are provided by the Department of Alcohol and Other Drug Abuse Services
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY - SELF FUNDED
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $250 Individual None Family $750 Family Unless otherwise indicated, the deductible must be met prior to benefits being
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $250 Individual None Family $750 Family Unless otherwise indicated, the deductible must be met prior to benefits being
MMA Benefits at a Glance
 MMA Benefits at a Glance You must get covered services by providers that are part of the Molina plan. You must also make sure that approval is obtained if needed. Ambulance Art Therapy Assistive Care Services
MMA Benefits at a Glance You must get covered services by providers that are part of the Molina plan. You must also make sure that approval is obtained if needed. Ambulance Art Therapy Assistive Care Services
HELPFUL INFORMATION ADDED CHOICE TRIPLE OPTION PLANS
 HELPFUL INFORMATION ADDED CHOICE TRIPLE OPTION PLANS PLEASE KEEP THIS IMPORTANT INFORMATION WELCOME TO KAISER PERMANENTE With our Added Choice Triple Option Plan, you can choose from three provider options
HELPFUL INFORMATION ADDED CHOICE TRIPLE OPTION PLANS PLEASE KEEP THIS IMPORTANT INFORMATION WELCOME TO KAISER PERMANENTE With our Added Choice Triple Option Plan, you can choose from three provider options
ST. MARY S HEALTHCARE SYSTEM, INC. Case # GA6476 BlueChoice HMO Benefit Summary Effective: January 1, 2018
 ST. MARY S HEALTHCARE SYSTEM, INC. Case # GA6476 BlueChoice HMO Benefit Summary Effective: January 1, 2018 All benefits are subject to the calendar year deductible, except those with in-network copayments,
ST. MARY S HEALTHCARE SYSTEM, INC. Case # GA6476 BlueChoice HMO Benefit Summary Effective: January 1, 2018 All benefits are subject to the calendar year deductible, except those with in-network copayments,
MEDICARE By Peter G. Pan
 Wendell K. Kimura Acting Director Research (808) 587-0666 Revisor (808) 587-0670 Fax (808) 587-0681 LEGISLATIVE REFERENCE BUREAU State of Hawaii State Capitol Honolulu, Hawaii 96813 No. 02-13 October 7,
Wendell K. Kimura Acting Director Research (808) 587-0666 Revisor (808) 587-0670 Fax (808) 587-0681 LEGISLATIVE REFERENCE BUREAU State of Hawaii State Capitol Honolulu, Hawaii 96813 No. 02-13 October 7,
Direct Care Deductible 2000 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond
 Direct Care Deductible 2000 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond The Fallon difference Direct Care is a Limited Provider Network. With Direct Care Deductible 2000 Hybrid,
Direct Care Deductible 2000 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond The Fallon difference Direct Care is a Limited Provider Network. With Direct Care Deductible 2000 Hybrid,
CHIP Perinatal Program Newborn Schedule of Benefits
 Inpatient General Acute and Inpatient Rehabilitation Hospital Services Services include: Hospital-provided Physician or Provider Semi-private room and board (or private if medically necessary as certified
Inpatient General Acute and Inpatient Rehabilitation Hospital Services Services include: Hospital-provided Physician or Provider Semi-private room and board (or private if medically necessary as certified
Annual copay maximum: Individual $500; Family $1,500 The following copay does not apply to the annual copay maximum: for infertility services
 Custom Premier HMO 30/100 (HMO 30 w/o CHIRO) Effective 07.01.2017 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan,
Custom Premier HMO 30/100 (HMO 30 w/o CHIRO) Effective 07.01.2017 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan,
Select Care Deductible 1200 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond
 Select Care Deductible 1200 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond The Fallon difference With Select Care Deductible 1200 Hybrid, you get everything you need to live a healthy
Select Care Deductible 1200 Hybrid Benefit Summary Benefits effective January 1, 2018 and beyond The Fallon difference With Select Care Deductible 1200 Hybrid, you get everything you need to live a healthy
CLASSIC BLUE SECURE/BLUE CROSS BLUE SHIELD COMPLEMENTARY Monroe County Benefit Summary/Comparison (Over 65 Retirees)
 WHO IS COVERED Enrollment Requirement Members must be enrolled in both Medicare Parts A and B Members must be enrolled in both Medicare Parts A and B Type of Tier Single only Single only Dependent/Student
WHO IS COVERED Enrollment Requirement Members must be enrolled in both Medicare Parts A and B Members must be enrolled in both Medicare Parts A and B Type of Tier Single only Single only Dependent/Student
Stanislaus County Medical Benefits EPO Option. In-Network Benefits (Stanislaus County Partners in Out-of-Network Benefits
 Stanislaus County Medical EPO Option The following summary of benefits is a brief outline of the maximum amounts or special limits that may apply to benefits payable under the Plan. For a detailed description
Stanislaus County Medical EPO Option The following summary of benefits is a brief outline of the maximum amounts or special limits that may apply to benefits payable under the Plan. For a detailed description
January 1, 2015 December 31, Maintenance Organization (HMO) offered by HEALTHNOW NEW YORK INC. with a Medicare contract)
 BLUECROSS BLUESHIELD SENIOR BLUE 601 (HMO), BLUECROSS BLUESHIELD SENIOR BLUE HMO SELECT (HMO) AND BLUECROSS BLUESHIELD SENIOR BLUE HMO 651 PARTD (HMO) (a Medicare Advantage Health Maintenance Organization
BLUECROSS BLUESHIELD SENIOR BLUE 601 (HMO), BLUECROSS BLUESHIELD SENIOR BLUE HMO SELECT (HMO) AND BLUECROSS BLUESHIELD SENIOR BLUE HMO 651 PARTD (HMO) (a Medicare Advantage Health Maintenance Organization
Your Out-of-Pocket Type of Service
 Calendar Year Deductible (CYD) 1 $3,000 single/ 3x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,200 single/ 2x family maximum. With respect to family plans,
Calendar Year Deductible (CYD) 1 $3,000 single/ 3x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,200 single/ 2x family maximum. With respect to family plans,
Schedule of Benefits
 Schedule of Benefits ANTHEM Small Business Health Options Program (SHOP) This is a brief schedule of benefits. Refer to your Anthem Certificate of Coverage (Booklet) for complete details on benefits, conditions,
Schedule of Benefits ANTHEM Small Business Health Options Program (SHOP) This is a brief schedule of benefits. Refer to your Anthem Certificate of Coverage (Booklet) for complete details on benefits, conditions,
CERTIFICATE OF INSURANCE
 AARP ESSENTIAL HEALTH INSURANCE PLAN CERTIFICATE OF INSURANCE Underwritten by United HealthCare Insurance Company Fort Washington, Pennsylvania Issued to: United HealthCare Insurance Company ( United HealthCare
AARP ESSENTIAL HEALTH INSURANCE PLAN CERTIFICATE OF INSURANCE Underwritten by United HealthCare Insurance Company Fort Washington, Pennsylvania Issued to: United HealthCare Insurance Company ( United HealthCare
Aetna Open Access POS II
 Aetna Open Access POS II The Aetna Open Access Point-of-Service (POS) II Options combine the advantages of managed healthcare with the freedom of traditional medical coverage. With the POS options, every
Aetna Open Access POS II The Aetna Open Access Point-of-Service (POS) II Options combine the advantages of managed healthcare with the freedom of traditional medical coverage. With the POS options, every
