A short stay unit decreased mean length of stay in a
|
|
|
- Sheena Paul
- 5 years ago
- Views:
Transcription
1 Original Article A short stay unit decreased mean length of stay in a hospital in south Brazil Tania Weber Furlanetto 1,2,3, Daniel de Souza Barcelos 1, Gustavo Adolpho Moreira Faulhaber 1,4 ABSTRACT Introduction Public health services in Brazil are periodically overcrowded. Since reducing the length of stay (LOS) could increase the availability of hospital beds, this study evaluated the impact of a short stay unit (SSU) on LOS, early readmission rates, and intra-hospital mortality rates. Methods Data were evaluated retrospectively in the 12 months before and after the establishment of a multidisciplinary SSU in a tertiary care hospital in south Brazil. All admissions of adult patients through the Emergency Department for causes in nine groups of the World Health Organization International Code of Diseases-10 were included. Results Mean LOS decreased 1.42 days in the first year after the implementation of a SSU with no change in 7-day readmission rates or intra-hospital mortality rates. This decrease may be partially explained by the decrease in the mean LOS in other areas of the hospital, although the amount of hospital-bed days saved in the second year was 5,668 days in the Internal Medicine Division and 1,595 days in all other clinical or surgical areas. Mortality rates after discharge were not evaluated. Conclusions A SSU decreased mean LOS of selected patients admitted through the Emergency Department without increasing 7-day readmission rates or intra-hospital mortality. Keywords: Health care surveys; quality improvement; length of stay Higher life expectancy and better management of chronic conditions have caused an increased demand for health services in Brazil. Bed shortage is common 1 and emergency rooms are often overcrowded 2. In the Hospital de Clínicas de Porto Alegre, a tertiary care, academic, public hospital in south Brazil, patients are admitted majorly through the Emergency Department, and their data are registered in electronic files. When admission to hospital is indicated, and there are no available beds in the inpatient area, patients stay in the Emergency Department until discharge. During the epidemics of H1N1 influenza in 2009, a multidisciplinary short stay unit (SSU) was implemented in the Internal Medicine Division, with criteria for early discharge of convalescent patients. Patients had a low mean length of stay (LOS), and no one needed early readmission (unpublished data). Based on these results, a SSU with 18 beds was created in the Internal Medicine Division to treat acute clinical patients and to allow for early discharge of convalescent patients. As decreased LOS could be associated with worse outcomes, including early readmission rates, the aim of this study was to evaluate the impact of the SSU on LOS, early readmission rates, and intrahospital mortality rates. Clin Biomed Res. 2014;34(4): Programa de Pós-Graduação em Medicina: Ciências Médicas, Universidade Federal do Rio Grande do Sul (UFRGS). Porto Alegre, RS, Brazil. 2 Serviço de Medicina Interna, Hospital de Clínicas de Porto Alegre (HCPA). Porto Alegre, RS, Brazil. 3 Pesquisadora do CNPq. Porto Alegre, RS, Brazil. 4 Faculdade de Medicina, Universidade Federal do Rio Grande do Sul (UFRGS). Porto Alegre, RS, Brazil. Corresponding author: Tania Weber Furlanetto taniafurlanetto@gmail.com Serviço de Medicina Interna, Hospital de Clínicas de Porto Alegre Rua Ramiro Barcelos, 2350/ , Porto Alegre, RS, Brasil METHODS Our study was conducted at HCPA, a large public hospital in south Brazil, which has an Internal Medicine Division with approximately 100 beds for inpatients. Clin Biomed Res 2014;34(4) 381
2 Furlanetto et al. Data were obtained using in-house software. The groups of diseases that caused the greatest number of admissions to the SSU were selected, according to the World Health Organization International Code of Diseases-10: influenza and pneumonia (J09-J18); chronic lower respiratory diseases (J40-J47); other diseases of urinary system (N30-N39); other forms of heart disease (I30-I52); cerebrovascular diseases (I60-I69); human immunodeficiency virus disease (B20-B24); malignant neoplasms of digestive organs (C15-C26); other bacterial diseases (A30-A49); and diabetes mellitus (E10-E14). All admissions through the Emergency Department due to these diseases in two years were included: before (December 1, 2008-November 30, 2009) and after the establishment of the SSU (December 1, November 30, 2010). When hospital beds were available, patients were transferred to the Internal Medicine Division or any other clinical or surgical area of the hospital, or they remained in the Emergency Department until discharge. The SSU had 18 beds, 9 for each sex. Patients were treated by two teams; each team included one senior internist, two resident physicians, and two medical students. When the emergency physicians, in the first evaluation, believed a patient had an acute condition that would require hospitalization for ten days or less, he/she was admitted, if there was a bed available, to one of the two teams, which cared for nine patients each. After admission to the SSU, patients were evaluated by a nurse, and subsequently by a medical resident or medical student, who collected data and formulated the investigation, treatment, and discharge plans. If social problems were identified, which could hinder the discharge process, an early intervention of the social services was requested. There were two medical rounds a day, coordinated by one senior internist (at least once a day) or a second- or third-year medical resident. Every day there was also a short round including nurses, social work assistants, psychologists, dietitians, pharmacists, and managers, for problem solving to decrease the LOS. Outpatient follow-up in the first 7 days after discharge was available if needed. The primary outcomes were LOS as the primary efficiency outcome and 7-day readmission rates 3 and intra-hospital mortality rates as safety endpoints. The mean LOS was calculated for patients discharged alive. This study was approved by the Health Research Ethics Board at the Hospital de Clínicas de Porto Alegre and the need for patient informed consent was waived. Data were analyzed with the Mann-Whitney test or chi square test, as indicated, using the software SPSS 18.0 (Chicago, IL, EUA). Differences were considered significant when the two-sided P value was less than RESULTS During the two years, 11,040 adult patients, 5,289 in the first and 5,751 in the second year, were admitted to the hospital through the Emergency Department. Admissions for diseases other than those previously mentioned were excluded (1,489 in the first year and 1,793 in the second year), so 7,758 admissions were evaluated: 2,129 to the Internal Medicine Division (779 in the first year and 1,350 in the second year), 2,500 to other hospital departments (1,340 in the first year and 1,160 in the second year), and 3,129 patients who remained in the Emergency Department until discharge (1,681 in the first year and 1,448 in the second year). These data are shown in Figure 1. As expected, the proportion of patients admitted to the Internal Medicine Division with the selected diagnosis increased after the implementation of the SSU (before: 20.5%, after: 34.1%, p<0.001); a decrease in the proportion of patients remaining in the Emergency Department (before: 44.2%, after: 36.6%, p<0.001) or admitted to other areas (before: 35.3%, after: 29.3%, p<0.001) was also observed. These data are shown in Table 1. There was a decrease in the mean LOS of all patients admitted to the hospital for the selected causes through the Emergency Department and discharged alive after the establishment of the SSU (before: 10.89±13.17 days, after: 9.47±11.24 days, p=0.006), as well as a marked decrease in the LOS of patients admitted to the Internal Medicine Division [before (n=680): 14.33±14.57 days, after (n=1243): 9.77±10.62 days, p<0.001] and to other hospital departments [before (n=1,142): 18.95±15.22 days, after (n=938): 17.25±14.23 days, p=0.014]. Conversely, mean LOS did not change for patients remaining in the Emergency Department [before (n=1,547): 3.42±2.21 days, after (n=1,310): 3.61±2.61 days, p=0.856]. These data are shown in Figure 2. The number of hospital-bed days saved in the second year was 5,668 days in the Internal Medicine Division and 1,595 days in other clinical or surgical areas. There was no change in the intra-hospital mortality rates of all patients admitted for the selected causes [before (n=3,800): 11.3%, after (n=3,958): 11.8% p=0.53] or in their 7-day readmission rates [before (n=3,369): 7.2%, after (n=3,491): 6.7%, p=0.41] after the implementation of the SSU. 382 Clin Biomed Res 2014;34(4)
3 Short stay unit and length of stay Figure 1: Study flow diagram. *Admissions due to diseases in the following groups of the WHO ICD-10: J09-J018: influenza and pneumonia, J40-J47: chronic lower respiratory diseases, N30-N39: other diseases of urinary system, I30-I52: other forms of heart disease, I60-I69: cerebrovascular diseases, B20-B24: human immunodeficiency virus disease, C15-C26: malignant neoplasms of digestive organs, A30-A49: other bacterial diseases, and E10-E14: diabetes mellitus. Emergency: patients remaining in the Emergency Department for more than 24 hours until discharge; Others: other clinical or surgical areas; HCPA: Hospital de Clínicas de Porto Alegre. Table 1: Selected causes* of adult patients admission, before (12/01/ /30/2009) and after (12/01/ /30/2010) the implementation of a short stay unit in the Internal Medicine Division, according to the admission area. December 1, 2008-November 30,2009 n (%) December 1, 2009-November 30, 2010 n (%) All 3,800 (100) 3,958 (100) Emergency 1,681 (44.2) 1,448 (36.6) <0.001 Internal Medicine 779 (20.5) 1,350 (34.1) <0.001 Other clinical or surgical areas 1,340 (35.3) 1,160 (29.3) <0.001 *Groups J09-J018, J40-J47, N30-N39, I30-I52, I60-I69, B20-B24, C15-C26, A30-A49, and E10-E14, of the WHO ICD-10. Emergency: patients remaining in the Emergency Department for 24 hours or more until discharge p DISCUSSION In this study, mean LOS of patients admitted to a tertiary care hospital through the Emergency Department with selected diagnosis decreased 1.42 days in the year following the implementation of a SSU in the Internal Medicine Division, with no change in 7-day readmission rates or intra-hospital mortality rates. This decrease may be partially explained by the decrease in the mean LOS of patients admitted to other clinical or surgical areas of the hospital. The larger number of hospital-bed days saved in the Internal Medicine Division (5,668 days) as compared with the other areas (1,595 days) and the increase in the number of patients admitted to the Internal Medicine Division after SSU implementation indicate that the SSU contributed greatly to this decrease. Several factors have been associated to a trend to decrease LOS, as the judicious use of diagnostic tests, allowing earlier and more precise diagnosis, more effective drugs and procedures, and others Clin Biomed Res 2014;34(4) 383
4 Furlanetto et al. Figure 2: Mean length of stay of patients discharged alive after being admitted for selected causes (WHO ICD-10 groups J09-J018, J40-J47, N30-N39, I30-I52, I60-I69, B20-B24, C15-C26, A30-A49, and E10-E14) to a tertiary care hospital, before (December, 2008-November, 2009) and after (December, 2009-November, 2010) the implementation of a short stay unit in the Internal Medicine Division, according to the area of admission. Emergency: patients remaining in the Emergency Department for 24 hours or more until discharge; Others: other clinical or surgical area. The mean LOS was days before and 9.47 days after the SSU implementation for all patients; 3.42 days before and 3.61 days after SSU implementation for patients in the Emergency Department; days before and 9.77 days after the SSU implementation for patients in the Internal Medicine Unit; and days before and days after the SSU implementation for patients in other areas. Data are shown as mean±se of the mean.*p=0.006; **p<0.001; ***p= The effect of interventions to decrease LOS has also been studied. Moher et al. randomized clinical patients to two groups: one received standard treatment, while the other had also a medical team coordinator, whose role was to facilitate administrative tasks such as discharge planning, to coordinate tests and procedures, and to collect and collate patient information. The authors observed a decrease in LOS, with no significant difference in the 14-day readmission rate 11. In patients with pneumonia, the use of multidisciplinary rounds decreased LOS 12. Home treatment supported by respiratory nurses allowed early discharge of patients with acute exacerbations of chronic obstructive pulmonary disease uncomplicated by acidotic respiratory failure or other medical problems, with no increase in readmission, additional hospital days, and deaths within 60 days of initial admission 13. Lim at al. compared the effect of two discharge protocols on consecutive patients admitted for acute severe exacerbations of bronchial asthma after remission of signs and symptoms or after improvement but before complete remission of signs and symptoms. They concluded that the release of asthmatics who responded promptly to intensive treatment and were compliant with medication despite incomplete resolution of symptoms, signs and peak expiratory flow rates at the time of discharge from hospital, may not be associated with increased risk of early relapse 14. Another study including patients with exacerbated chronic obstructive pulmonary disease, comparing early discharged patients with nurse supervision at home with those receiving the standard treatment, found no increase in the rate of hospital readmissions 15. In a quasi-experimental study that compared usual care with usual care plus nurse practitioner/physician management of hospital care, multidisciplinary team-based planning, expedited discharge, and assessment after discharge, Cowan et al. observed a decrease in the LOS with no differences in mortality or 4-month readmissions 16. Recently, McAlister et al. described the effect of an initiative comprising four actions (demand capacity realignment, team integration and culture change, implementation of best practices, and transition optimizations) on LOS, readmission rates, and intrahospital mortality, with substantial reductions in LOS without increasing post-discharge events 17. In our study, the decrease in LOS was probably the result of the combination of several actions: development of an investigation plan and establishment of treatment goals in the first 24 hours, review of 384 Clin Biomed Res 2014;34(4)
5 Short stay unit and length of stay clinical conditions and results of exams twice a day, early identification of psychosocial problems, actions of the multidisciplinary team to decrease LOS, as well as the availability of outpatient follow-up in the first 7 days after discharge. Although our results are impressive, this study has some flaws: mortality rates after discharge were not evaluated, and the results were not adjusted for risk factors. Nevertheless, we tried to control for some of these factors, as well as seasonality of diseases, by including all the admissions during two whole years, the first one immediately before, and the second one immediately after the implementation of the SSU. Other limitations that could not be addressed were a change in pathogens causing infectious diseases in different years, as well as changes in medical residents working in the SSU. In conclusion, a SSU in the Internal Medicine Division decreased mean LOS of patients admitted to the hospital for the selected diagnosis without increasing 7-day readmission rates or intra-hospital mortality. Disclaimer The authors had full access to and take full responsibility for the integrity of the data. The views expressed in this article are those of the authors and do not necessarily represent the views of the UFRGS and HCPA. Conflicts of interest All authors declare no conflict of interests. Funding Conselho Nacional de Desenvolvimento Científico e Tecnológico, CNPq, Brazil. Institution where the study was performed: Hospital de Clínicas de Porto Alegre, Brazil References 1. Gonçalves EL, Dias MJM, Mattos HB. Assistência hospitalar no âmbito da previdência social no Estado de Sâo Paulo, Brasil. Rev Saude Publica. 1972;6(1): PMid: Brick A. The stretchers from Emergency Room (ER. Rev Bras Cir Cardiovasc. 2009;24(1): PMid: Heggestad T, Lilleeng SE. Measuring readmissions: focus on the time factor. Int J Qual Health Care. 2003;15(2): org/ /intqhc/mzg019. PMid: Kaboli PJ, Go JT, Hockenberry J, Glasgow JM, Johnson SR, Rosenthal GE, et al. Associations between reduced hospital length of stay and 30-day readmission rate and mortality: 14-year experience in 129 Veterans Affairs hospitals. Ann Intern Med. 2012;157(12): org/ / PMid: Baker DW, Einstadter D, Husak SS, Cebul RD. Trends in postdischarge mortality and readmissions: has length of stay declined too far? Arch Intern Med. 2004;164(5): dx.doi.org/ /archinte PMid: Harrison ML, Graff LA, Roos NP, Brownell MD. Discharging patients earlier from Winnipeg hospitals: does it adversely affect quality of care? CMAJ. 1995;153(6): PMid: Cabre M, Bolivar I, Pera G, Pallares R, Pneumonia Study Collaborative Group. Factors influencing length of hospital stay in communityacquired pneumonia: a study in 27 community hospitals. Epidemiol Infect. 2004;132(5): org/ /s PMid: Capelastegui A, España PP, Quintana JM, Gallarreta M, Gorordo I, Esteban C, et al. Declining length of hospital stay for pneumonia and postdischarge outcomes. Am J Med. 2008;121(10): org/ /j.amjmed PMid: Bittar OJ. [Hospital productivity in the light of hospital indicators]. Rev Saude Publica. 1996;30(1): PMid: André C, Py MO, Mariño RG. [Causes of unjustified hospital stay following cerebral infarction]. Arq Neuropsiquiatr. 1997;55(3B): PMid: Moher D, Weinberg A, Hanlon R, Runnalls K. Effects of a medical team coordinator on length of hospital stay. CMAJ. 1992;146(4): PMid: O Mahony S, Mazur E, Charney P, Wang Y, Fine J. Use of multidisciplinary rounds to simultaneously improve quality outcomes, enhance resident education, and shorten length of stay. J Gen Intern Med. 2007;22(8): PMid: Cotton MM, Bucknall CE, Dagg KD, Johnson MK, MacGregor G, Stewart C, et al. Early discharge for patients with exacerbations of chronic obstructive pulmonary disease: a randomized controlled trial. Thorax. 2000;55(11): org/ /thorax PMid: Lim TK, Chin NK, Lee KH, Stebbings AM. Early discharge of patients hospitalized with acute asthma: a controlled study. Respir Med. 2000;94(12): org/ /rmed PMid: Sala E, Alegre L, Carrera M, Ibars M, Orriols FJ, Blanco ML, et al. Supported discharge shortens hospital stay in patients hospitalized because Clin Biomed Res 2014;34(4) 385
6 Furlanetto et al. of an exacerbation of COPD. Eur Respir J. 2001;17(6): dx.doi.org/ / PMid: Cowan MJ, Shapiro M, Hays RD, Afifi A, Vazirani S, Ward CR, et al. The effect of a multidisciplinary hospitalist/ physician and advanced practice nurse collaboration on hospital costs. J Nurs Adm. 2006;36(2): PMid: McAlister FA, Bakal JA, Majumdar SR, Dean S, Padwal RS, Kassam N, et al. Safely and effectively reducing inpatient length of stay: a controlled study of the General Internal Medicine Care Transformation Initiative. BMJ Qual Saf. 2014;23(6): bmjqs PMid: Received: 09/10/14 Accepted: 19/11/ Clin Biomed Res 2014;34(4)
Running head: LEADERSHIP ANALYSIS: ROUNDING 1
 Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
Utilizing a Pharmacist and Outpatient Pharmacy in Transitions of Care to Reduce Readmission Rates. Disclosures. Learning Objectives
 Utilizing a Pharmacist and Outpatient Pharmacy in Transitions of Care to Reduce Readmission Rates. Disclosures Rupal Mansukhani declares grant support from the Foundation for. Rupal Mansukhani, Pharm.D.
Utilizing a Pharmacist and Outpatient Pharmacy in Transitions of Care to Reduce Readmission Rates. Disclosures Rupal Mansukhani declares grant support from the Foundation for. Rupal Mansukhani, Pharm.D.
Analyzing Readmissions Patterns: Assessment of the LACE Tool Impact
 Health Informatics Meets ehealth G. Schreier et al. (Eds.) 2016 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under the terms of the Creative
Health Informatics Meets ehealth G. Schreier et al. (Eds.) 2016 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under the terms of the Creative
Thank you for joining us today!
 Thank you for joining us today! Please dial 1.800.732.6179 now to connect to the audio for this webinar. To show/hide the control panel click the double arrows. 1 Emergency Room Overcrowding A multi-dimensional
Thank you for joining us today! Please dial 1.800.732.6179 now to connect to the audio for this webinar. To show/hide the control panel click the double arrows. 1 Emergency Room Overcrowding A multi-dimensional
Supported discharge shortens hospital stay in patients hospitalized because of an exacerbation of COPD
 Eur Respir J 2001; 17: 1138 1142 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 Supported discharge shortens hospital stay in patients hospitalized
Eur Respir J 2001; 17: 1138 1142 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 Supported discharge shortens hospital stay in patients hospitalized
Cause of death in intensive care patients within 2 years of discharge from hospital
 Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W
 Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
OP ED-THROUGHPUT GENERAL DATA ELEMENT LIST. All Records
 Material inside brackets ( [ and ] ) is new to this Specifications Manual version. HOSPITAL OUTPATIENT QUALITY MEASURES ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Material inside brackets ( [ and ] ) is new to this Specifications Manual version. HOSPITAL OUTPATIENT QUALITY MEASURES ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Optimizing Care for Complex Patients with COPD
 Optimizing Care for Complex Patients with COPD Janice Gasaway, RN, MN, Director Quality & Safety Elvin Perkins, MBA, Chronic Disease Project Manager 1 Cone Health System: Who We Are Regional Health System
Optimizing Care for Complex Patients with COPD Janice Gasaway, RN, MN, Director Quality & Safety Elvin Perkins, MBA, Chronic Disease Project Manager 1 Cone Health System: Who We Are Regional Health System
Quick guide: planning for increased seasonal demand in respiratory illness
 Quick guide: planning for increased seasonal demand in respiratory illness Published by NHS England and NHS Improvement December 2017 The British Thoracic Society is pleased to endorse this quick guide,
Quick guide: planning for increased seasonal demand in respiratory illness Published by NHS England and NHS Improvement December 2017 The British Thoracic Society is pleased to endorse this quick guide,
Safely and effectively reducing inpatient length of stay: a controlled study of the General Internal Medicine Care Transformation Initiative
 ORIGINAL RESEARCH Editor s choice Scan to access more free content Additional material is published online only. To view please visit the journal online (http://dx.doi.org/10.1136/bmjqs- 2013-002289).
ORIGINAL RESEARCH Editor s choice Scan to access more free content Additional material is published online only. To view please visit the journal online (http://dx.doi.org/10.1136/bmjqs- 2013-002289).
Specifications Manual for National Hospital Inpatient Quality Measures Discharges (1Q17) through (4Q17)
 Last Updated: Version 5.2a EMERGENCY DEPARTMENT (ED) NATIONAL HOSPITAL INPATIENT QUALITY MEASURES ED Measure Set Table Set Measure ID # ED-1a ED-1b ED-1c ED-2a ED-2b ED-2c Measure Short Name Median Time
Last Updated: Version 5.2a EMERGENCY DEPARTMENT (ED) NATIONAL HOSPITAL INPATIENT QUALITY MEASURES ED Measure Set Table Set Measure ID # ED-1a ED-1b ED-1c ED-2a ED-2b ED-2c Measure Short Name Median Time
OP ED-THROUGHPUT GENERAL DATA ELEMENT LIST. All Records
 Material inside brackets ( [ and ] ) is new to this Specifications Manual version. HOSPITAL OUTPATIENT QUALITY MEASURES ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Material inside brackets ( [ and ] ) is new to this Specifications Manual version. HOSPITAL OUTPATIENT QUALITY MEASURES ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Hot Spotter Report User Guide
 PATIENT-CENTERED CARE Hot Spotter Report User Guide Overview The Hot Spotter Report is designed to give providers and care team members a heads up when their attributed patients appear to be at risk for
PATIENT-CENTERED CARE Hot Spotter Report User Guide Overview The Hot Spotter Report is designed to give providers and care team members a heads up when their attributed patients appear to be at risk for
OP ED-Throughput General Data Element List. All Records All Records. All Records All Records All Records. All Records. All Records.
 Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures ED-Throughput Set Measure ID # OP-18 OP-20 OP-22 Measure Short Name Median Time from
Outpatient management of community acquired pneumonia
 Outpatient management of community acquired pneumonia Wei Shen Lim Consultant Respiratory Physician Honorary Professor of Medicine (University of Nottingham) Nottingham University Hospitals NHS Trust What
Outpatient management of community acquired pneumonia Wei Shen Lim Consultant Respiratory Physician Honorary Professor of Medicine (University of Nottingham) Nottingham University Hospitals NHS Trust What
Community nurse specialists and prevention of readmissions in older patients with chronic lung disease and cardiac failure
 HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Key Messages 1. A post-discharge follow-up by community nurses significantly reduced length of stay in acute hospital and accident and emergency
HEALTH SERVICES RESEARCH FUND HEALTH CARE AND PROMOTION FUND Key Messages 1. A post-discharge follow-up by community nurses significantly reduced length of stay in acute hospital and accident and emergency
O U T C O M E. record-based. measures HOSPITAL RE-ADMISSION RATES: APPROACH TO DIAGNOSIS-BASED MEASURES FULL REPORT
 HOSPITAL RE-ADMISSION RATES: APPROACH TO DIAGNOSIS-BASED MEASURES FULL REPORT record-based O U Michael Goldacre, David Yeates, Susan Flynn and Alastair Mason National Centre for Health Outcomes Development
HOSPITAL RE-ADMISSION RATES: APPROACH TO DIAGNOSIS-BASED MEASURES FULL REPORT record-based O U Michael Goldacre, David Yeates, Susan Flynn and Alastair Mason National Centre for Health Outcomes Development
Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS
 Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS Safe and timely discharge of patients from hospitals helps ensure patients well-being
Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS Safe and timely discharge of patients from hospitals helps ensure patients well-being
La Rabida Inpatient Rotation PL2 Residents
 PL2 Residents Residents rotate through the inpatient service at La Rabida Children s Hospital and Research Center over 1-2 months during the second year of residency. The inpatient service is separated
PL2 Residents Residents rotate through the inpatient service at La Rabida Children s Hospital and Research Center over 1-2 months during the second year of residency. The inpatient service is separated
National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI)
 October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
Reducing Readmissions: Potential Measurements
 Reducing Readmissions: Potential Measurements Avoid Readmissions Through Collaboration October 27, 2010 Denise Remus, PhD, RN Chief Quality Officer BayCare Health System Overview Why Focus on Readmissions?
Reducing Readmissions: Potential Measurements Avoid Readmissions Through Collaboration October 27, 2010 Denise Remus, PhD, RN Chief Quality Officer BayCare Health System Overview Why Focus on Readmissions?
Level of acuity in pediatric patients with recurrent emergency department visits
 ORIGINAL ARTICLE Level of acuity in pediatric patients with recurrent emergency department visits Ilene Claudius, Chun Nok Lam LAC+USC, Department of Emergency Medicine, Keck School of Medicine, USA Correspondence:
ORIGINAL ARTICLE Level of acuity in pediatric patients with recurrent emergency department visits Ilene Claudius, Chun Nok Lam LAC+USC, Department of Emergency Medicine, Keck School of Medicine, USA Correspondence:
Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national COPD audits of 2003 and 2008
 Q J Med 2011; 104:859 866 doi:10.1093/qjmed/hcr083 Advance Access Publication 26 May 2011 Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national
Q J Med 2011; 104:859 866 doi:10.1093/qjmed/hcr083 Advance Access Publication 26 May 2011 Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national
Improving patient satisfaction by adding a physician in triage
 ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
Accepted Manuscript. Hospitalists, Medical Education, and US Health Care Costs,
 Accepted Manuscript Hospitalists, Medical Education, and US Health Care Costs, James E. Dalen MD, MPH, ScD (hon), Kenneth J Ryan MD, Anna L Waterbrook MD, Joseph S Alpert MD PII: S0002-9343(18)30503-5
Accepted Manuscript Hospitalists, Medical Education, and US Health Care Costs, James E. Dalen MD, MPH, ScD (hon), Kenneth J Ryan MD, Anna L Waterbrook MD, Joseph S Alpert MD PII: S0002-9343(18)30503-5
Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service
 Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
The Heart of Care Redesign; Care Protocols. Paul N. Casale, MD, FACC Chief, Division of Cardiology Lancaster General Health
 The Heart of Care Redesign; Care Protocols Paul N. Casale, MD, FACC Chief, Division of Cardiology Lancaster General Health Lancaster General Health By the Numbers (Fiscal Year 2012) Beds: 631 in service
The Heart of Care Redesign; Care Protocols Paul N. Casale, MD, FACC Chief, Division of Cardiology Lancaster General Health Lancaster General Health By the Numbers (Fiscal Year 2012) Beds: 631 in service
The impact of nighttime intensivists on medical intensive care unit infection-related indicators
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Factors that Impact Readmission for Medicare and Medicaid HMO Inpatients
 The College at Brockport: State University of New York Digital Commons @Brockport Senior Honors Theses Master's Theses and Honors Projects 5-2014 Factors that Impact Readmission for Medicare and Medicaid
The College at Brockport: State University of New York Digital Commons @Brockport Senior Honors Theses Master's Theses and Honors Projects 5-2014 Factors that Impact Readmission for Medicare and Medicaid
Washtenaw Community College Comprehensive Report. NUR 123 Medical Surgical Nursing I Effective Term: Winter 2017
 Washtenaw Community College Comprehensive Report NUR 123 Medical Surgical Nursing I Effective Term: Winter 2017 Course Cover Division: Health Sciences Department: Nursing & Health Science Discipline: Nursing
Washtenaw Community College Comprehensive Report NUR 123 Medical Surgical Nursing I Effective Term: Winter 2017 Course Cover Division: Health Sciences Department: Nursing & Health Science Discipline: Nursing
Measuring Harm. Objectives and Overview
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3. Measuring Harm
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
A Virtual Ward to prevent readmissions after hospital discharge
 A Virtual Ward to prevent readmissions after hospital discharge Irfan Dhalla MD MSc FRCPC Departments of Medicine and Health Policy, Management and Evaluation, University of Toronto Keenan Research Centre,
A Virtual Ward to prevent readmissions after hospital discharge Irfan Dhalla MD MSc FRCPC Departments of Medicine and Health Policy, Management and Evaluation, University of Toronto Keenan Research Centre,
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings
 Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings Executive Summary The Alliance for Home Health Quality and
Medicare Spending and Rehospitalization for Chronically Ill Medicare Beneficiaries: Home Health Use Compared to Other Post-Acute Care Settings Executive Summary The Alliance for Home Health Quality and
CDU. Clinical Decision Unit Ward for
 CDU Clinical Decision Unit Ward for Can t Observational Decide Medicine Unit What are observation medicine units? Observation medicine delivers intensive shortterm assessment, observation or therapy to
CDU Clinical Decision Unit Ward for Can t Observational Decide Medicine Unit What are observation medicine units? Observation medicine delivers intensive shortterm assessment, observation or therapy to
About the Data: Adult Health and Disease - Chronic Illness 2016/17, 2014/15 (archived) Last Updated: August 29, 2018
 About the Data: Adult Health and Disease - Chronic Illness 2016/17, 2014/15 (archived) Last Updated: August 29, 2018 Adult Health and Disease: 2016/17 Denominator: Ontario Ministry of Health and Long-Term
About the Data: Adult Health and Disease - Chronic Illness 2016/17, 2014/15 (archived) Last Updated: August 29, 2018 Adult Health and Disease: 2016/17 Denominator: Ontario Ministry of Health and Long-Term
Dashboard Review First Quarter of FY-2017 Joe Selby, MD, MPH
 Dashboard Review First Quarter of FY-217 Joe Selby, MD, MPH Executive Director 1 Board of Governors Dashboard First Quarter FY-217 (As of 12/31/216) Our Goals: Increase Information, Speed Implementation,
Dashboard Review First Quarter of FY-217 Joe Selby, MD, MPH Executive Director 1 Board of Governors Dashboard First Quarter FY-217 (As of 12/31/216) Our Goals: Increase Information, Speed Implementation,
Introduction. Singapore. Singapore and its Quality and Patient Safety Position 11/9/2012. National Healthcare Group, SIN
 Introduction Singapore and its Quality and Patient Safety Position Singapore 1 Singapore 2004: Top 5 Key Risk Factors High Body Mass (11.1%; 45,000) Physical Inactivity (3.8%; 15,000) Cigarette Smoking
Introduction Singapore and its Quality and Patient Safety Position Singapore 1 Singapore 2004: Top 5 Key Risk Factors High Body Mass (11.1%; 45,000) Physical Inactivity (3.8%; 15,000) Cigarette Smoking
2017 Quality Reporting: Claims and Administrative Data-Based Quality Measures For Medicare Shared Savings Program and Next Generation ACO Model ACOs
 2017 Quality Reporting: Claims and Administrative Data-Based Quality Measures For Medicare Shared Savings Program and Next Generation ACO Model ACOs June 15, 2017 Rabia Khan, MPH, CMS Chris Beadles, MD,
2017 Quality Reporting: Claims and Administrative Data-Based Quality Measures For Medicare Shared Savings Program and Next Generation ACO Model ACOs June 15, 2017 Rabia Khan, MPH, CMS Chris Beadles, MD,
Beyond the Hospital Walls: Impact of a SNFist Practice Model
 Beyond the Hospital Walls: Impact of a SNFist Practice Model Aaron Snyder, MD Vice President, US Acute Care Solutions Kim Repac Chief Financial Officer, WMHS Aging Population 50 Million Distribution
Beyond the Hospital Walls: Impact of a SNFist Practice Model Aaron Snyder, MD Vice President, US Acute Care Solutions Kim Repac Chief Financial Officer, WMHS Aging Population 50 Million Distribution
Boarding Impact on patients, hospitals and healthcare systems
 Boarding Impact on patients, hospitals and healthcare systems Dan Beckett Consultant Acute Physician NHSFV National Clinical Lead Whole System Patient Flow Project Scottish Government May 2014 Important
Boarding Impact on patients, hospitals and healthcare systems Dan Beckett Consultant Acute Physician NHSFV National Clinical Lead Whole System Patient Flow Project Scottish Government May 2014 Important
Sepsis Screening Tools
 ICU Rounds Amanda Venable MSN, RN, CCRN Case Mr. H is a 67-year-old man status post hemicolectomy four days ago. He was transferred from the ICU to a medical-surgical floor at 1700 last night. Overnight
ICU Rounds Amanda Venable MSN, RN, CCRN Case Mr. H is a 67-year-old man status post hemicolectomy four days ago. He was transferred from the ICU to a medical-surgical floor at 1700 last night. Overnight
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center
 Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Reducing Hospital Readmissions
Maryland Patient Safety Center s Annual MEDSAFE Conference: Taking Charge of Your Medication Safety Challenges November 3, 2011 The Conference Center at the Maritime Institute Reducing Hospital Readmissions
TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate
 TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate Heidi Luder, PharmD, MS, BCACP Assistant Professor of Pharmacy Practice University
TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate Heidi Luder, PharmD, MS, BCACP Assistant Professor of Pharmacy Practice University
Predictors of In-Hospital vs Postdischarge Mortality in Pneumonia
 CHEST Original Research Predictors of In-Hospital vs Postdischarge Mortality in Pneumonia Mark L. Metersky, MD, FCCP; Grant Waterer, MBBS; Wato Nsa, MD, PhD; and Dale W. Bratzler, DO, MPH CHEST INFECTIONS
CHEST Original Research Predictors of In-Hospital vs Postdischarge Mortality in Pneumonia Mark L. Metersky, MD, FCCP; Grant Waterer, MBBS; Wato Nsa, MD, PhD; and Dale W. Bratzler, DO, MPH CHEST INFECTIONS
4/10/2013. Learning Objective. Quality-Based Payment Models
 Creating Best in Class Perioperative Services under Accountable Care and Value- Based Purchasing Becker s Healthcare Jeffry Peters Learning Objective How ACA/VBP changes how we measure surgical services
Creating Best in Class Perioperative Services under Accountable Care and Value- Based Purchasing Becker s Healthcare Jeffry Peters Learning Objective How ACA/VBP changes how we measure surgical services
*Your Name *Nursing Facility. radiation therapy. SECTION 2: Acute Change in Condition and Factors that Contributed to the Transfer
 Gaining information about resident transfers is an important goal of the OPTIMISTC project. CMS also requires us to report these data. This form is where data relating to long stay transfers are to be
Gaining information about resident transfers is an important goal of the OPTIMISTC project. CMS also requires us to report these data. This form is where data relating to long stay transfers are to be
C hronic obstructive pulmonary disease (COPD) is one of
 837 CHRONIC OBSTRUCTIVE PULMONARY DISEASE UK National COPD Audit 2003: impact of hospital resources and organisation of care on patient outcome following admission for acute COPD exacerbation L C Price,
837 CHRONIC OBSTRUCTIVE PULMONARY DISEASE UK National COPD Audit 2003: impact of hospital resources and organisation of care on patient outcome following admission for acute COPD exacerbation L C Price,
Health Literacy. Definition & Controversies
 Health Literacy Definition & Controversies Michael Wolf, MA MPH PhD Assistant Professor of Medicine and Learning Sciences Director, Center for Communication in Healthcare Feinberg School of Medicine School
Health Literacy Definition & Controversies Michael Wolf, MA MPH PhD Assistant Professor of Medicine and Learning Sciences Director, Center for Communication in Healthcare Feinberg School of Medicine School
January 1, 20XX through December 31, 20XX. LOINC(R) is a registered trademark of the Regenstrief Institute.
 e Title Median Time from ED Arrival to ED Departure for Admitted ED Patients e Identifier ( Authoring Tool) 55 e Version number 5.1.000 NQF Number 0495 GUID 9a033274-3d9b- 11e1-8634- 00237d5bf174 ment
e Title Median Time from ED Arrival to ED Departure for Admitted ED Patients e Identifier ( Authoring Tool) 55 e Version number 5.1.000 NQF Number 0495 GUID 9a033274-3d9b- 11e1-8634- 00237d5bf174 ment
Northern Ireland COPD Audit
 Northern Ireland COPD Audit A regional audit of chronic obstructive pulmonary disease (COPD) care September 2017 www.rqia.org.uk Assurance, Challenge and Improvement in Health and Social Care Contents
Northern Ireland COPD Audit A regional audit of chronic obstructive pulmonary disease (COPD) care September 2017 www.rqia.org.uk Assurance, Challenge and Improvement in Health and Social Care Contents
Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge
 Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge Julianna Burton, Pharm.D., BCPS, BCACP, FCSHP Assistant Chief, Ambulatory Clinical Services
Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge Julianna Burton, Pharm.D., BCPS, BCACP, FCSHP Assistant Chief, Ambulatory Clinical Services
Community Performance Report
 : Wenatchee Current Year: Q1 217 through Q4 217 Qualis Health Communities for Safer Transitions of Care Performance Report : Wenatchee Includes Data Through: Q4 217 Report Created: May 3, 218 Purpose of
: Wenatchee Current Year: Q1 217 through Q4 217 Qualis Health Communities for Safer Transitions of Care Performance Report : Wenatchee Includes Data Through: Q4 217 Report Created: May 3, 218 Purpose of
W e were aware that optimising medication management
 207 QUALITY IMPROVEMENT REPORT Improving medication management for patients: the effect of a pharmacist on post-admission ward rounds M Fertleman, N Barnett, T Patel... See end of article for authors affiliations...
207 QUALITY IMPROVEMENT REPORT Improving medication management for patients: the effect of a pharmacist on post-admission ward rounds M Fertleman, N Barnett, T Patel... See end of article for authors affiliations...
HIMSS ASIAPAC 11 CONFERENCE & LEADERSHIP SUMMIT SEPTEMBER 2011 MELBOURNE, AUSTRALIA
 HIMSS ASIAPAC 11 CONFERENCE & LEADERSHIP SUMMIT 20 23 SEPTEMBER 2011 MELBOURNE, AUSTRALIA INTRODUCTION AND APPLICATION OF A CODING QUALITY TOOL PICQ JOE BERRY OPERATIONS AND PROJECT MANAGER, PAVILION HEALTH
HIMSS ASIAPAC 11 CONFERENCE & LEADERSHIP SUMMIT 20 23 SEPTEMBER 2011 MELBOURNE, AUSTRALIA INTRODUCTION AND APPLICATION OF A CODING QUALITY TOOL PICQ JOE BERRY OPERATIONS AND PROJECT MANAGER, PAVILION HEALTH
REDUCING READMISSIONS through TRANSITIONS IN CARE
 REDUCING READMISSIONS through TRANSITIONS IN CARE Christina R. Whitehouse, PhD, CRNP, CDE Postdoctoral Research Fellow NewCourtland Center for Transitions and Health University of Pennsylvania School of
REDUCING READMISSIONS through TRANSITIONS IN CARE Christina R. Whitehouse, PhD, CRNP, CDE Postdoctoral Research Fellow NewCourtland Center for Transitions and Health University of Pennsylvania School of
Using Facets of Midas+ Hospital Case Management to Support Transitions of Care. Barbara Craig, Midas+ SaaS Advisor
 Using Facets of Midas+ Hospital Case Management to Support Transitions of Care Barbara Craig, Midas+ SaaS Advisor What does Transitional Care Include? Transitional Care is the smooth conversion of a patient
Using Facets of Midas+ Hospital Case Management to Support Transitions of Care Barbara Craig, Midas+ SaaS Advisor What does Transitional Care Include? Transitional Care is the smooth conversion of a patient
Admissions and Readmissions Related to Adverse Events, NMCPHC-EDC-TR
 Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
Rural-Relevant Quality Measures for Critical Access Hospitals
 Rural-Relevant Quality Measures for Critical Access Hospitals Ira Moscovice PhD Michelle Casey MS University of Minnesota Rural Health Research Center Minnesota Rural Health Conference Duluth, Minnesota
Rural-Relevant Quality Measures for Critical Access Hospitals Ira Moscovice PhD Michelle Casey MS University of Minnesota Rural Health Research Center Minnesota Rural Health Conference Duluth, Minnesota
Standard of Care for MTC inpatients
 Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
Standard of Care for MTC inpatients The following document is intended to summarise the model of care for patients admitted under the care of the Leeds Major Trauma System. It will outline expected duties
National Early Warning Scoring System
 National Early Warning Scoring System A common language for health care The deteriorating patient Professor Derek Bell January 2013 Adult National Early Warning Score Background Overview of NEWS Next Steps
National Early Warning Scoring System A common language for health care The deteriorating patient Professor Derek Bell January 2013 Adult National Early Warning Score Background Overview of NEWS Next Steps
Integrated respiratory action network for patients with COPD
 Integrated respiratory action network for patients with COPD In this Future Hospital Programme case study Dr Helen Ward describes how a team from The Royal Wolverhampton NHS Trust established a respiratory
Integrated respiratory action network for patients with COPD In this Future Hospital Programme case study Dr Helen Ward describes how a team from The Royal Wolverhampton NHS Trust established a respiratory
Disclosure. SwedishAmerican Hospital A Division of UW Health. Learning Objectives. Medication History. Medication History 2/2/2017
 Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
The model adopted for the hospital accreditation
 1.0 ANCC CONTACT HOUR Quality of Electronic Nursing Records The Impact of Educational Interventions During a Hospital Accreditation Process Aline Tsuma Gaedke Nomura, MS, RN, Lisiane Pruinelli, PhD, RN,
1.0 ANCC CONTACT HOUR Quality of Electronic Nursing Records The Impact of Educational Interventions During a Hospital Accreditation Process Aline Tsuma Gaedke Nomura, MS, RN, Lisiane Pruinelli, PhD, RN,
Operational Focus: Performance
 Operational Focus: Performance Sandra Iskander Changes for 2015/16 Change of focus of 18-weeks and A&E 4-hour wait targets as recommended by Sir Bruce Keogh, Medical Director, NHS England. 18-weeks to
Operational Focus: Performance Sandra Iskander Changes for 2015/16 Change of focus of 18-weeks and A&E 4-hour wait targets as recommended by Sir Bruce Keogh, Medical Director, NHS England. 18-weeks to
Readmissions Moving beyond blame to fill the patient needs. Jackie Conrad RN, MBA, RCC Cynosure Health
 Readmissions Moving beyond blame to fill the patient needs Jackie Conrad RN, MBA, RCC Cynosure Health jconrad@cynosurehealth.org 1 51 year old male with 3 acute care admissions and 2 ED visits in the past
Readmissions Moving beyond blame to fill the patient needs Jackie Conrad RN, MBA, RCC Cynosure Health jconrad@cynosurehealth.org 1 51 year old male with 3 acute care admissions and 2 ED visits in the past
SPECIALTY SPECIFIC OBJECTIVES
 Family Medicine Residency Internal Medicine In-house II Rotation Rotation Goal Admission, evaluation, treatment and appropriate specialty consultation of adult hospitalized patients from either the ER,
Family Medicine Residency Internal Medicine In-house II Rotation Rotation Goal Admission, evaluation, treatment and appropriate specialty consultation of adult hospitalized patients from either the ER,
2017 LEAPFROG TOP HOSPITALS
 2017 LEAPFROG TOP HOSPITALS METHODOLOGY AND DESCRIPTION In order to compare hospitals to their peers, Leapfrog first placed each reporting hospital in one of the following categories: Children s, Rural,
2017 LEAPFROG TOP HOSPITALS METHODOLOGY AND DESCRIPTION In order to compare hospitals to their peers, Leapfrog first placed each reporting hospital in one of the following categories: Children s, Rural,
A Tool for Improving Patient Discharge Process and Hospital Communication Practices: the Patient Tracker
 A Tool for Improving Patient Discharge Process and Hospital Communication Practices: the Patient Tracker Christopher G. Maloney MD PhD 1, Douglas Wolfe MBA 2, Per H. Gesteland MD MS 1, Joe W. Hales PhD
A Tool for Improving Patient Discharge Process and Hospital Communication Practices: the Patient Tracker Christopher G. Maloney MD PhD 1, Douglas Wolfe MBA 2, Per H. Gesteland MD MS 1, Joe W. Hales PhD
Key Scientific Publications
 Key Scientific Publications Introduction This document provides a list of over 60 key scientific publications for those interested in hand hygiene improvement. For a comprehensive list of pertinent publications,
Key Scientific Publications Introduction This document provides a list of over 60 key scientific publications for those interested in hand hygiene improvement. For a comprehensive list of pertinent publications,
Case study O P E N A C C E S S
 O P E N A C C E S S Case study Discharge against medical advice in a pediatric emergency center in the State of Qatar Hala Abdulateef 1, Mohd Al Amri 1, Rafah F. Sayyed 1, Khalid Al Ansari 1, *, Gloria
O P E N A C C E S S Case study Discharge against medical advice in a pediatric emergency center in the State of Qatar Hala Abdulateef 1, Mohd Al Amri 1, Rafah F. Sayyed 1, Khalid Al Ansari 1, *, Gloria
Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
 Journal of Pharmacy and Pharmacology 2 (2014) 731-738 doi: 10.17265/2328-2150/2014.12.006 D DAVID PUBLISHING Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
Journal of Pharmacy and Pharmacology 2 (2014) 731-738 doi: 10.17265/2328-2150/2014.12.006 D DAVID PUBLISHING Reducing Readmission Rates in Heart Failure and Acute Myocardial Infarction by Pharmacy Intervention
9/8/14. Re-hospitalizations among patients in the Medicare Fee-for-service Program
 Rachael Ali-Permell, BS, RT, RRT-NPS, ACCS, AE-C Manager Respiratory Therapy Department Bayhealth Milford Memorial Hospital, Delaware Faculty Quinones Healthcare Seminars, LLC Hospital Readmission Reduction
Rachael Ali-Permell, BS, RT, RRT-NPS, ACCS, AE-C Manager Respiratory Therapy Department Bayhealth Milford Memorial Hospital, Delaware Faculty Quinones Healthcare Seminars, LLC Hospital Readmission Reduction
Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON
 Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON SCHOOL OF PHARMACY Conflicts of Interest I have no conflicts
Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON SCHOOL OF PHARMACY Conflicts of Interest I have no conflicts
Patients Not Included in Medical Audit Have a Worse Outcome Than Those Included
 Pergamon International Journal for Quality in Health Care, Vol. 8, No. 2, pp. 153-157, 1996 Copyright
Pergamon International Journal for Quality in Health Care, Vol. 8, No. 2, pp. 153-157, 1996 Copyright
BUILDING BRIDGES: SUCCESSFUL TRANSITIONS FROM HOSPITAL TO HOME FOR OLDER ADULTS
 BUILDING BRIDGES: SUCCESSFUL TRANSITIONS FROM HOSPITAL TO HOME FOR OLDER ADULTS Senior s Month Education 2013 Sponsored by Regional Geriatric Program central (RGPc) Committee for the Enhancement of Elder
BUILDING BRIDGES: SUCCESSFUL TRANSITIONS FROM HOSPITAL TO HOME FOR OLDER ADULTS Senior s Month Education 2013 Sponsored by Regional Geriatric Program central (RGPc) Committee for the Enhancement of Elder
Nursing skill mix and staffing levels for safe patient care
 EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
Quality Based Impacts to Medicare Inpatient Payments
 Quality Based Impacts to Medicare Inpatient Payments Overview New Developments in Quality Based Reimbursement Recap of programs Hospital acquired conditions Readmission reduction program Value based purchasing
Quality Based Impacts to Medicare Inpatient Payments Overview New Developments in Quality Based Reimbursement Recap of programs Hospital acquired conditions Readmission reduction program Value based purchasing
Malnutrition Screening Pathway v.1.1
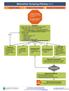 Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
Open versus Closed Sandwich Wound Dressing Method in Burn Children.
 http://www.bioline.org.br/js Open versus Closed Sandwich Wound Dressing Method in Burn Children. 8 P. Oduor, MMed Surgery, FCS(ECSA) Surgeon, Rift Valley Provincial General Hospital, Nakuru, Kenya. Email:
http://www.bioline.org.br/js Open versus Closed Sandwich Wound Dressing Method in Burn Children. 8 P. Oduor, MMed Surgery, FCS(ECSA) Surgeon, Rift Valley Provincial General Hospital, Nakuru, Kenya. Email:
Improving Transitions of Care
 Improving Transitions of Care Mark V. Williams, MD, FACP, FHM Professor & Chief, Division of Hospital Medicine Northwestern University Feinberg School of Medicine Principal Investigator, Project BOOST
Improving Transitions of Care Mark V. Williams, MD, FACP, FHM Professor & Chief, Division of Hospital Medicine Northwestern University Feinberg School of Medicine Principal Investigator, Project BOOST
The Development of the Oncology Symptom Management Clinic
 The Development of the Oncology Symptom Management Clinic Submitted by: Catherine Brady-Copertino BSN, MS, OCN Executive Director Anne Arundel Medical Center s Geaton and JoAnn DeCesaris Cancer Institute
The Development of the Oncology Symptom Management Clinic Submitted by: Catherine Brady-Copertino BSN, MS, OCN Executive Director Anne Arundel Medical Center s Geaton and JoAnn DeCesaris Cancer Institute
Papers. Hospital bed utilisation in the NHS, Kaiser Permanente, and the US Medicare programme: analysis of routine data. Abstract.
 Hospital bed utilisation in the NHS, Kaiser Permanente, and the US Medicare programme: analysis of routine data Chris Ham, Nick York, Steve Sutch, Rob Shaw Abstract Objective To compare the utilisation
Hospital bed utilisation in the NHS, Kaiser Permanente, and the US Medicare programme: analysis of routine data Chris Ham, Nick York, Steve Sutch, Rob Shaw Abstract Objective To compare the utilisation
The Effect of an Interprofessional Heart Failure Education Program on Hospital Readmissions
 1 The Effect of an Interprofessional Heart Failure Education Program on Hospital Readmissions Julia N. Clarkson, Susan D. Schaffer, Joshua J. Clarkson Heart failure (HF) is a pressing concern to public
1 The Effect of an Interprofessional Heart Failure Education Program on Hospital Readmissions Julia N. Clarkson, Susan D. Schaffer, Joshua J. Clarkson Heart failure (HF) is a pressing concern to public
OVERALL GOALS & OBJECTIVES FOR EACH RESIDENT LEVEL FIRST-YEAR RESIDENT. Patient Care
 OVERALL GOALS & OBJECTIVES FOR EACH RESIDENT LEVEL FIRST-YEAR RESIDENT Patient Care 1) Demonstrate proficiency in the preoperative and postoperative care of surgical patients. 2) Demonstrate thorough,
OVERALL GOALS & OBJECTIVES FOR EACH RESIDENT LEVEL FIRST-YEAR RESIDENT Patient Care 1) Demonstrate proficiency in the preoperative and postoperative care of surgical patients. 2) Demonstrate thorough,
Carthage Area Hospital, Inc.
 Carthage Area Hospital, Inc. 1. Mission: Carthage Area Hospital provides quality comprehensive healthcare services in a community setting. 2. Service Area: Located in Northern New York, Carthage Area Hospital
Carthage Area Hospital, Inc. 1. Mission: Carthage Area Hospital provides quality comprehensive healthcare services in a community setting. 2. Service Area: Located in Northern New York, Carthage Area Hospital
Maroon Inpatient Rotation PL-1 Residents
 PL-1 Residents The Inpatient Maroon experience has been designed to develop the needed competencies for an intern to manage patients with a wide array of conditions requiring hospitalization, from the
PL-1 Residents The Inpatient Maroon experience has been designed to develop the needed competencies for an intern to manage patients with a wide array of conditions requiring hospitalization, from the
HAI Learning and Action Network February 11, 2015 Monthly Call. Overview of HAI LAN
 HAI Learning and Action Network February 11, 2015 Monthly Call 1 Overview of HAI LAN CLABSI, CAUTI, CDI, VAE Conferred Rights through NHSN Monthly meetings/webex/teleconferences Antimicrobial Stewardship
HAI Learning and Action Network February 11, 2015 Monthly Call 1 Overview of HAI LAN CLABSI, CAUTI, CDI, VAE Conferred Rights through NHSN Monthly meetings/webex/teleconferences Antimicrobial Stewardship
Health System Performance and Accountability Division MOHLTC. Transitional Care Program Framework
 Transitional Care Program Framework August, 2010 1 Table of Contents 1. Context... 3 2. Transitional Care Program Framework... 4 3. Transitional Care Program in the Hospital Setting... 5 4. Summary of
Transitional Care Program Framework August, 2010 1 Table of Contents 1. Context... 3 2. Transitional Care Program Framework... 4 3. Transitional Care Program in the Hospital Setting... 5 4. Summary of
HAI Learning and Action Network January 8, 2015 Monthly Call
 HAI Learning and Action Network January 8, 2015 Monthly Call GPQIN Website greatplainsqin.org PATH: Website Initiatives Reducing HAI in Hospitals 2 HAI Page 3 4 5 Patient and Family Engagement Why should
HAI Learning and Action Network January 8, 2015 Monthly Call GPQIN Website greatplainsqin.org PATH: Website Initiatives Reducing HAI in Hospitals 2 HAI Page 3 4 5 Patient and Family Engagement Why should
Inpatient Care in a Community Hospital: Comparing Length of Stay and Costs Among Teaching, Hospitalist, and Community Services
 Vol. 40, No. 2 119 Health Services Research Inpatient Care in a Community Hospital: Comparing Length of Stay and Costs Among Teaching, Hospitalist, and Community Services Peter J. Carek, MD, MS; Holly
Vol. 40, No. 2 119 Health Services Research Inpatient Care in a Community Hospital: Comparing Length of Stay and Costs Among Teaching, Hospitalist, and Community Services Peter J. Carek, MD, MS; Holly
Community Health Needs Assessment Mercy Hospital Ardmore 2012
 Community Health Needs Assessment Mercy Hospital Ardmore 2012 Contents Table of Contents Introduction... 2 Description and Basic Community Demographics... 2 Who was Involved in Assessment?... 2 Community
Community Health Needs Assessment Mercy Hospital Ardmore 2012 Contents Table of Contents Introduction... 2 Description and Basic Community Demographics... 2 Who was Involved in Assessment?... 2 Community
CKHA Quality Improvement Plan (QIP) Scorecard
 CKHA Quality Improvement Plan () Scorecard 217-18 Quality dimension Performance Indicator 217-18 Performance Goals results where available Current Value Page Safety Medication Reconciliation completed
CKHA Quality Improvement Plan () Scorecard 217-18 Quality dimension Performance Indicator 217-18 Performance Goals results where available Current Value Page Safety Medication Reconciliation completed
April Clinical Governance Corporate Report Narrative
 April 14 - Clinical Governance Corporate Report Narrative ITEM 7B Narrative has been provided where there is something of note in relation to a specific metric; this could be positive improvement, decline
April 14 - Clinical Governance Corporate Report Narrative ITEM 7B Narrative has been provided where there is something of note in relation to a specific metric; this could be positive improvement, decline
Chronic Disease Management: Implications for LTC homes
 Chronic Disease Management: Implications for LTC homes George A Heckman MD MSc FRCPC Schlegel Research Chair in Geriatric Medicine Associate Professor, School of Public Health and Health Systems February
Chronic Disease Management: Implications for LTC homes George A Heckman MD MSc FRCPC Schlegel Research Chair in Geriatric Medicine Associate Professor, School of Public Health and Health Systems February
MEDICAL POLICY No R1 TELEMEDICINE
 Summary of Changes MEDICAL POLICY TELEMEDICINE Effective Date: March 1, 2016 Review Dates: 12/12, 12/13, 11/14, 11/15 Date Of Origin: December 12, 2012 Status: Current Clarifications: Deletions: Pg. 4,
Summary of Changes MEDICAL POLICY TELEMEDICINE Effective Date: March 1, 2016 Review Dates: 12/12, 12/13, 11/14, 11/15 Date Of Origin: December 12, 2012 Status: Current Clarifications: Deletions: Pg. 4,
Challenging The 2015 PH Guidelines - comments from the Nurses. Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust
 Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
Integrated respiratory care
 Integrated respiratory care what s the best model? Georges Ng Man Kwong Pennine Lung Service key components outcomes leadership & team future The optimal model of integrated respiratory care that provides
Integrated respiratory care what s the best model? Georges Ng Man Kwong Pennine Lung Service key components outcomes leadership & team future The optimal model of integrated respiratory care that provides
Using Quality Improvement to Optimize Pediatric Discharge Efficiency
 This presenter has nothing to disclose Using Quality Improvement to Optimize Pediatric Discharge Efficiency Christine White MD, MAT Associate Professor-Hospital Medicine Cincinnati Children s Hospital
This presenter has nothing to disclose Using Quality Improvement to Optimize Pediatric Discharge Efficiency Christine White MD, MAT Associate Professor-Hospital Medicine Cincinnati Children s Hospital
