Stimulus-response time to invasive blood pressure alarms: implications for the safety of critical-care patients
|
|
|
- Brett Miller
- 5 years ago
- Views:
Transcription
1 Original article Stimulus-response time to invasive blood pressure alarms: implications for the safety of critical-care patients Revista Gaúcha de Enfermagem Tempo estímulo-resposta aos alarmes de pressão arterial invasiva: implicações para a segurança do paciente crítico Tiempo estímulo-respuesta de alarmas de promedio de la presión arterial invasiva: implicaciones para la seguridad del paciente crítico Adele Kuckartz Pergher a Roberto Carlos Lyra da Silva b DOI: ABSTRACT Observational, descriptive, exploratory, case study with the objective of measuring the stimulus-response time of the team to alarms monitoring invasive blood pressure (IBP) and analyzing the implications of this time for the safety of the patient. From January to March 2013, 60 hours of structured observation were conducted with registration of the alarms activated by IBP monitors in an adult ICU at a military hospital in the city of Rio de Janeiro. 76 IBP alarms were recorded (1.26 alarms/hour), 21 of which (28%) were attended to and 55 (72%) considered as fatigued. The average response time to the alarms was 2 min. 45 sec. The deficit in human resource and physical layout were factors determining the delay in response to the alarms. The increase in response times to these alarms may compromise the safety of patients with hemodynamic instability, especially in situations such as shock and the use of vasoactive drugs. Descriptors: Clinical alarms. Fatigue. Patient safety. Intensive care. RESUMO Estudo observacional, descritivo, exploratório, do tipo estudo de caso. Teve como objetivos medir o tempo estímulo-resposta da equipe aos alarmes de monitorização da pressão arterial invasiva (PAI) e analisar as implicações desse tempo para a segurança do paciente. De janeiro a março de 2013, foram realizadas 60 horas de observação estruturada e registro de alarmes disparados por monitores de PAI em uma UTI para adultos de um hospital militar da cidade do Rio de Janeiro. Foram registrados 76 alarmes de PAI (1,26 alarmes/ hora), dos quais 21 alarmes (28%) foram atendidos e 55 (72%) considerados fatigados. O tempo médio de resposta aos alarmes foi 2 minutos e 45 seg.undos O déficit de recursos humanos e a planta física foram fatores determinantes no retardo da resposta aos alarmes. O alargamento do tempo de resposta a esses alarmes pode comprometer a segurança do paciente com instabilidade hemodinâmica, especialmente em situações de choque e uso de drogas vasoativas. Descritores: Alarmes clínicos. Fadiga. Segurança do paciente. Terapia intensiva. a Master in nursing from the Federal University of the State of Rio de Janeiro UNIRIO. Intensive Care Nurse from the University of the State of Rio de Janeiro- UERJ. Officer in the Brazilian Air Force. Rio de Janeiro (RJ), Brazil. b Doctor of Nursing. Associate Professor at the Basic Nursing Department at the Alfredo Pinto Nursing School-EEAP/UNIRIO. Researcher at the CNPq. Rio de Janeiro (RJ), Brazil. RESUMEN Estudio de caso observacional, descriptivo y exploratorio. Dirigido para medir el tiempo del equipo de estímulo y respuesta a las alarmas de monitoreo de la presión arterial invasiva (PAI) y analizar las implicaciones de este periodo la seguridad del paciente. Desde enero hasta marzo de 2013, hemos llevado a cabo 60 horas de observación estructurada y registro de alarmas disparadas por los monitores de MAP en una UCI de adultos de un hospital militar en la ciudad de Río de Janeiro. Se registraron 76 alarmas PAI (1,26 alarmas / hora), de los cuales 21 alarmas (28 %) fueron ingresados y 55 (72 %) considera fatigado. El tiempo promedio de respuesta fue 2 minutos y 45 segundos. La falta de recursos humanos y la planta física fueron los factores de respuesta tardía a las alarmas. La prórroga del plazo para responder a estas alarmas puede comprometer la seguridad de los pacientes con inestabilidad hemodinámica, especialmente en situaciones de shock y fármacos vasoactivos. Descriptores: Alarmas clínicas. Fatiga. Seguridad del paciente. Cuidados intensivos. Versão on-line Português/Inglês:
2 Pergher AK, Silva RCL INTRODUCTION The measurement and continual monitoring of invasive blood pressure (IBP) are fundamentally important accompanying critical patients, especially during continuous infusion of vasoactive drugs, given its importance (1). The Brazilian consensus for monitoring and hemodynamic support recommends that IBP monitoring be undertaken on patients in hypertensive emergency situations, states of shock, during the use of vasoactive amines, patients during and immediately after cardiac and neurological surgery or other conditions in which hypotension cannot be tolerated or sharp cariations in blood pressure (1). The use of these drugs requires constant vigilance, as small variations in the dose or blood pressure will require immediate professional intervention (2). In this perspective, the multi-parametric monitoring systems enable real time monitoring and alarm systems capable of calling the attention of the team to possible changes in the patient s clinical status. The development and incorporation of new monitoring equipment and advanced life support at Intensive Care Units (ICU) has been contributing more and more to increasing the number of sound and visual alarms, all with the intention of alerting professionals about the conditions of the patients and faults in the equipment, ensuring the safety and quality of care (3). Around 40 different types of alarms can be heard at intensive care units, especially those generated by monitors (electrocardiogram, respiratory frequency, IBP, pulse oximetry), infusion pumps, dialysis machines, ventilators, etc. (4) This amount of alarms, which are not always correct or relevant, provokes a true cacophony of noise, hindering the identification of those that really require an immediate response and consequently increasing the response time of the health team (5). We reiterate that nurses have a prominent role in relation to patient safety, as these professionals spend 24 hours monitoring their condition (3). Although the alarms are important for saving lives, they may also compromise the safety of the patient when frequently ignored (3,6). This problem gave rise to the concept of alarm fatigue, a phenomenon frequently observed in ICUs which is characterized by the excessive number of alarm signals, desensitization of professionals and delayed response times (7). The central theme of this study is the phenomenon of alarm fatigue and the objective under investigation is the stimulus-response time of the team to the audio alarms set off by the monitors during invasive blood pressure monitoring. In 2010 a study demonstrated that 85% of the alarms that occur in the ICU are false or have limited utility (8). False alarms are irritating and can interfere in care and normally do not result from an adverse event related to it (7). The World Health Organization defines an adverse event as undesirable complications resulting from the care provided to patients, not attributed to the natural evolution of the base disease (9). In 2012 and 2013 the Emergency Care Research Institute considered alarms as number 1 on its list of 10 hazards for technologies used in healthcare (6). In the national setting, the National Sanitary Surveillance Agency (ANVISA) estimates that one in ten patients attended to at hospitals will suffer some kind of adverse event, such as fall, incorrect administration of medication, identification failures, errors in surgical procedures, infections or misuse of medical devices and equipment. It is estimated that 66.7% of these events are avoidable (10). In this context, in 2013 the Collegiate Directorship published Resolution (RDC) 36/2013 instituting the National Patient Safety Program, with the objective of contributing to improving the care processes and use of health technologies (10). In 2012, one of the first national works dealing with alarm fatigue was published, studying pulse oximetry alarms at a neonatal intensive care unit (11). In this study 81 alarms (37%) were attended to by health professionals with a maximum time of 14 min. and 43 sec., while another 138 (63%) of alarms were not responded to or were considered as alarm fatigue. The safety of patients with hemodynamic instability is strongly related to the professional s response time to IBP alarms (12). This study had the objective of measuring the stimulus-response time of the team to alarms activated by the monitor during invasive blood pressure monitoring and analyzing the implications of this time for patient safety at intensive care units. This work is expected to contribute to testing and research in nursing and, above all, to patient safety at intensive care units. METHOD This is an observational, descriptive and exploratory case study based on descriptive statistics for the treatment and organization of data, which was analyzed within the theoretical framework of alarm fatigue and patient safety. The case study is an investigation into an institute that enables phenomenon to be explored but not exhaustively studied, generating hypotheses to be tested in subsequent research (13). For the collection of data a structured observation technique was used which includes the use of instruments and protocols about what should be observed, the time the obser- 136
3 Stimulus-response time to invasive blood pressure alarms: implications for the safety of critical-care patients vation should ensure and how the data should be recorded (13). This technique may generate behavioral distortions owing to the presence of the observed, a problem known as reactivity (13). The project was approved by the Research Ethics Committee at the Federal University of the State of Rio de Janeiro-UNIRIO on 17/08/2012 under number The research was conducted at an adult ICU at a military hospital in the city of Rio de Janeiro. The unit has 14 beds with an occupation rate of 86.01%, attends clinical and surgical patients and counts on a multidisciplinary team composed of physicians, medical residents, medical and physiotherapy students, nurses, nursing technicians, dentists and pharmacist. In relation to the material resources, all of the bed spaces include multi-parametric monitors, mechanical ventilators, automatic beds and infusion pumps. The monitors are connected to a monitoring station located at the nursing workbench to facilitate the surveillance of patients. When an alarm is activated, the monitor emits a visual and audio alarm. The alarm may be silenced for 2 minutes, but the visual signal will remain on the monitor. Only the visual signal appears on the monitoring station. In relation to human resources, the nursing team is composed of two nurses and six nursing technicians during day shifts (from 7 am to 7 pm) and one nurse and five nursing technicians on night shifts (from 7 pm to 7 am). The medical team is composed by five physicians in the morning period, and two physicians on duty during the afternoon and nighttime. There is always a resident physician on duty 24 hours per day. There is a physiotherapist at the unit from 7.45 am to 5.15 pm. The inclusion criteria for the participants were: being on duty at the intensive care unit at the times chosen for observation and agreeing to participate in the study. The inclusion criteria for the beds/patients were: use of invasive blood pressuring monitoring during the onsite observation periods, which occurred between January and June Before starting the observation, the professionals in the multidisciplinary team were invited to participate in the study after its objectives were explained. After accepting, they completed the declaration of free and clarified consent, authorizing observation during their work activities in accordance with the ethical and legal precepts inherent in scientific research. Before starting each observation shift, which took place between 7 am and 7 pm, it was verified which patients were being monitored for invasive blood pressure and if they were using vasoactive medication. The researcher observed and recorded the alarms using the monitoring station at the nursing post. These resources enable the observation of 14 boxes, given that the visual observation of all beds is not possible at any point in the unit. When an IBP alarm sounded stimulus-response time was measured with a timer, which was activated as soon as the alarm was activated, and paused when the professional went to the patient s bed, regardless of the conduct established. If the alarm stopped before being attended to it was considered as having no response and being a case of alarm fatigue. In these situations, the blood pressure values returned to normal values before any intervention by the professional. Alarms that sounded uninterruptedly in the same box and for the same cause that were not attended to within 10 minutes did not have their time restarted but were considered as a single alarm generated. During the observation there was no situation in which two alarms in different boxes sounded at the same time. Alarms that were not attended to after 10 minutes were also considered as being alarm fatigue. The 10 minute limit was defined considering that when dealing with cardiorespiratory arrest, the greater the response time to the alarm and implementation of actions, the worse the neurological outcome and there are recommendations for the start of cardiocerebral resuscitation should be less than 4 minutes (14). The definition of this limit has the intention of demonstrating the impact of alarm fatigue, and how this has contributed to enlarging the response time to the alarms beyond that enabling a satisfactory neurological outcome. RESULTS 60 hours of observation were conducted during the daily shifts (between 7 am and 7 pm), divided into 19 trips to the site. Thirty-seven professionals agreed to participate in the study: 28 from the nursing team, 05 from the medical team and 4 physiotherapists. The distribution of the number of participants per professional category is presented in Figure 1. Note that (75%) of the participants are from the nursing team. The significant number of participants in this professional category corroborates the importance of these professionals in patient surveillance and safety (3). During each observation shift there was an average of eleven patients hospitalized at the ICU, with four (36%) having the IBP monitored. Approximately half of them were surgical patients and used vasoactive medication at the time of observation. 76 alarms for invasive arterial pressure were recorded, generating an average of 1.26 IBP alarms per hour, i.e. ap- 137
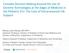
4 Pergher AK, Silva RCL proximately one alarm per hour. 21 (28%) of the alarms were observed, with an average response time of 2.45 min. The lowest response time was 20 seconds and the highest was 8 minutes. Figure 2 demonstrates the IBP alarms that were attended to each minute. Fifteen alarms (71.4% of the alarms attended to, 20% of the total alarms) were attended to in the first 3 minutes after sounding. This response time seems appropriate to prevent complications in critical patients, however, only 20% of the IBP alarms were attended to in this interval, while the others had a larger response time or were not dealt with. Fifty-five (72%) alarms were categorized under alarm fatigue, given that they remain without a response for more than 10 minutes, or stopped sounding before the professional could attend to them. The relationship between the alarms attended to and alarm fatigue is illustrated in Figure 3. DISCUSSION Although the results could, in principle, demonstrate that the number of audio alarms set off at the unit was not Distribution of participants according to professional category Number of participants 30 75% Nurse 14% 11% Physician Physiotherapy Professional category Figure 1. Distribution of participants according to professional category. Rio de Janeiro, RJ, January 2013 to March Source: Research data. 10 Response time to PAM alarms Number of alarms attended to in the interval :01 01:00 01:01 02:00 02:01 03:00 03:01 04:00 04:01 05:00 05:01 06:00 06:01 07:00 07:01 08:00 Interval in min. to attend to the alarms Figure 2. IBP alarms attended to each minute. Rio de Janeiro, RJ, January 2013 to March Source: Research data. 138
5 Stimulus-response time to invasive blood pressure alarms: implications for the safety of critical-care patients Figure 3. Number of alarms attended to and alarm fatigue recorded at the unit. Rio de Janeiro, RJ, January 2013 to March Source: Research data. Alarms with alarm fatigue 55 (72%) Alarms attended 21 (28%) high, we should consider that in this study only those relating to invasive blood pressure were recorded. IBP alarms can vary from 10 to 23% of all alarms set off at the unit by the multi-parametric monitors (5). In this sense, we can discover how common it is for one of these alarms to go off and how this can contribute to raising the number of alarms activated at the ICU. The risk of occurrences of incidents related to blood pressure variations may be very high, given the elevated number of alarms no responded to (72%), although this is within the average reveled by other studies (3-7,11,16). In individuals with hemodynamic instability rapid intervention is necessary and may change the prognosis and development of symptoms (14). In the case of hypotension, the persistent shock generates an inadequate tissue perfusion, the systems begin to decompensate owing to the lack of blood supply, compromising organs and the patient s failure to respond to treatment (2). Maintenance of a state of shock for more than 24 hours is responsible for a poor prognosis, raising the death rate to 60 to 70% (14). In serious cases of hypertension, there may be damage to target organs, such as encephalopathy, acute myocardial infarction, unstable angina, acute pulmonary edema, eclampsia and stroke (2). In the occurrence of cardiorespiratory arrest (which could be verified using IBP monitoring), the response time to the alarms becomes imperative, with the recommendation to start maneuvers already in the 1 st minute increasing the survival of patients, mainly in relation to neurological damage (14). Permanent neurological damage is the most feared complication of cardiac resuscitation or when it does not take place early. The high energy needs of the brain become especially vulnerable in situations of ischemia, in 5 minutes of complete cerebral anoxia, reducing the oxygen supply to below critical levels, when secondary alterations to ischemia start to develop (15). Neural activity cease, and if the oxygen supply is not restored the cell dies, causing hypoxic-ischemic brain damage (15). Therefore, taking into consideration that in 5 minutes ischemic damage may already occur, we can consider that the criteria of 10 minutes with no response to classify alarm fatigue is a highly extended time. Research conducted at a hospital in the city of Rio de Janeiro recoded 227 alarms, resulting in an average of 5.7 alarms per hour. In the daytime service, 64.15% of all alarms observed were categorized as alarm fatigue. The average stimulus-response time was 4 minutes and 54 seconds (5). The author also used the 10 minute criterion as a limit to consider the alarm as being attended to, therefore, our study found similar results when specifically observing IBP alarms. In other research conducted at an ICU with 24 beds in the same city, 17 alarms IBP alarms were recorded, all considered as alarm fatigue, which was concerning to the author in respect to patient safety (16). It should be reiterated that the alarms are cumulative in the environment and the noise level is negative for patients and the team. Thus, every time there is a delay in the response time to an alarm, it adds to this accumulation as another alarm could be triggered before responding to the previous one. Some strategies could be used to analyze the errors related to alarms. One of these is a fault tree (17) that indicates factors contributing to not respond promptly to an alarm: team too busy to respond; team deliberating ignoring the alarm; not seeing/hearing the alarm; and confusion in the identification of which alarm of which patient is sounding. In the scenario studied, it was possible to observe the presence of all these factors. The first two related to staffing deficits, and the latter to the physical layout and excess noise at the unit. In relation to the physical layout, it can be noted that there is a difficult in identifying some beds, which impedes the alarm being head. All of the monitors are connected to a monitoring station, however, when the alarm goes off at the bed only a visual signal is shown at the station. Thus, the distance between the beds and the nursing post hinders the identification of the alarm that is sounding and consequently a reaction by the professional to correct it and ensure the safety of the patient. 139
6 Pergher AK, Silva RCL In relation to the personnel deficit, the number on the nursing team at the unit was identified as diverging from that foreseen in RDC nº 26, May 11 th This resolution includes a minimum of 01 clinical nurse for every 10 beds or fraction thereof on each shift, and 01 nursing technician for every 02 beds per shift (18). According to the Resolution, this ICU should have a minimum of 02 clinical nurses and 07 nursing technicians on each shift. Therefore, the number is not being complied with at the unit. If we take into consideration the Federal Nursing Council Resolution (COFEN) nº 293/2004 which forecasts 52 to 56% nurses for intensive care, the discrepancy becomes even greater (19). The professional in the setting studied passes the majority of their time occupied, providing care to patients, frequently interrupting this to render another type of care, such as attending to the alarms. These interruptions to healthcare have a series of consequences, as they interrupt the sequence of planned work, changing the team s work process and interfering in the professional s capacity to concentrate, which can lead to errors (5). In 2004 a study observed the alarms and conducts in an ICU destined for neonatal patients, and revealed that alarms were set off per hour (20). Despite representing different circumstances from a unit for adult patients, it draws attention for taking into consideration the amount of patients and the time required to deal with each alarm. The authors concluded that if the nurses responded to all of the alarms, it would be practically impossible to carry out any other routine task. Therefore, it is a challenge for the nursing team to respond to all the alarms sounding at the unit, especially when considering the nurse-patient ratio imposed by RDC 26. Therefore, we should seek alternatives that enable safer and more effective use of the alarm systems. Thus we have demonstrated, as also discussed in the literature, that it is the nursing team that monitors the patients 24 hours and that interacts most with the patient monitoring system and alarms of these systems, and is therefore the category most involved in the alarm fatigue phenomenon (6-7). FINAL CONSIDERATIONS This study was the first experiment with the phenomenon, especially in relation to the occurrence of the phenomenon during invasive blood pressure monitoring. It did not take into consideration, for example, the borderline values that were adjusted for each patient in their monitors, therefore, there could be some relevant situations that were not detected after the activation of audio alarms. This research, although diagnostic in nature, has the potential for formulating hypotheses that could result in future studies for proposing measures for reducing the number of alarms and, consequently, alarm fatigue. In this sense, the training of the team could be tested, for example, to see if individualized adjustment of the borderline values would present satisfactory results in reducing the number of alarms activated and a positive impact on patient safety IBP alarms were detected per hour, therefore, although these alarms do not represent a large number in the context of the ICU, they concur with the phenomenon of alarm fatigue. This phenomenon has shown itself to be a current issue that has not been widely studied in Brazil. This lack of knowledge could be related to the large number of studies focused on adverse events related to health professionals, instead of those related to the use of technology/ equipment and its consequence on patient safety. The results encountered point out the need for electrical medical equipment to be maintained by all members of the health team. Adequate programming of alarms to the needs of patients needs to be incorporated in the nursing routine, as patient safety is also dependent on this. Unadjusted, disconnected or low volume alarms may lead to adverse events with a very unfavorable clinical outcome. In this context, the deficit in human resources should be considered as a contributing factor not only to alarm fatigue by also patient safety as a whole. In this study, 72% of the alarms were considered as cases of alarm fatigue, causing concern in relation to patient safety. There is therefore a need to always question if it is necessary and safe for the patient to enable more than one alarm, which may be unnecessary within their clinical diagnosis. REFERENCES 1. Dias FS, Rezende E, Mendes CL, Réa-Neto A, David CM, Schettino G, et al. Parte II: monitorização hemodinâmica básica e cateter de artéria pulmonar. Rev Bras Ter Intensiva. 2006;18(1): Cheregatti AL, Amorim CP Enfermagem em terapia intensiva. 1. ed. São Paulo: Martinari; Korniewicz DM, Clark T, David Y. A national online survey on the effectiveness of clinical alarms. Am J Crit Care Jan;17: Chambrin MC, Ravaux P, Calvelo-Aros D, Jaborska A, Chopin C, Boniface B. Multicentric study of monitoring alarms in the adult intensive care unit (ICU): a descriptive analysis. Intensive Care Med [Internet] Dec [citado 2012 nov 20];25(12): Available in: s Bridi, AC. Fatores determinantes do tempo estímulo-resposta da equipe de enfermagem aos alarmes dos monitores multiparamétricos em terapia intensiva: 140
7 Stimulus-response time to invasive blood pressure alarms: implications for the safety of critical-care patients implicações para a segurança do paciente grave [dissertação]. Rio de Janeiro (RJ): Programa de Pós-Graduação Mestrado em Enfermagem, Universidade Federal do Estado do Rio de Janeiro; Cvach M. Monitor alarm fatigue: an integrative review. Biomed Instrum Technol [Internet] Jul-Aug [citado 2012 nov 20];46(4): Available in: 7. Graham KC, Cvach M. Monitor alarm fatigue: standardizing use of physiological monitors and decreasing nuisance alarms. Am J Crit Care [Internet] Jan [citado 2012 out 15];19(1): Available in: content/19/1/28.full.pdf+html 8. Siebig S, Kuhls S, Imhoff M, Gather U, Schölmerich J, Wrede CE. Collection of annotated data in a critical validation study for alarm algorithms in intensive care: a methodologic framework. J Crit Care [Internet] Mar [citado 2012 nov 20];25(1): Available in: 9. World Health Organization [Internet]. Conceptual framework for the international classification for patient safety: final technical report [and technical annexes] [citado 2010 abr 22]. Available in: Ministério da Saúde (BR), Agência Nacional de Vigilância Sanitária. Portaria Nº 529, de 01 de abril de Institui o Programa Nacional de Segurança do Paciente (PNSP). Brasília (DF); Monteiro, JLS. Tempo estímulo-resposta aos alarmes de oxímetros de pulso em unidade de terapia intensiva neonatal: implicações para a segurança do paciente [dissertação]. Rio de Janeiro (RJ): Programa de Pós-Graduação Mestrado em Enfermagem, Universidade Federal do Estado do Rio de Janeiro; Pergher, AK. Tempo estímulo-resposta aos alarmes de monitorização invasiva da pressão arterial: contribuições para a segurança do paciente em unidade de cuidados intensivos [dissertação]. Rio de Janeiro (RJ): Programa de Pós-Graduação Mestrado em Enfermagem, Universidade Federal do Estado do Rio de Janeiro; Polit DF, Beck CT. Fundamentos de pesquisa em enfermagem: avaliação de evidências para a prática da enfermagem. Porto Alegre: Artmed; Ferrari D. Choque. In: Ferrari D. Terapia intensiva moderna [Internet]. São Paulo: IBRATI; [citado 2013 ago 09]. Available in: Rech TH, Vieira S R R, BRAUNER JS. Valor da enolase específica do neurônio como indicador de prognóstico pós-parada cardiorrespiratória. Rev Bras Ter Intensiva. 2006;18(4): Santos F. O tempo estímulo-resposta na predisposição a fadiga de alarmes de ventiladores mecânicos: implicações para a segurança do paciente [dissertação]. Rio de Janeiro (RJ): Programa de Pós-Graduação em Enfermagem, Universidade Federal do Estado do Rio de Janeiro; Hyman, WA, Johnson E. Fault tree analysis of clinical alarms. J Clin Eng Apr/Jun 33(2): Ministério da Saúde (BR), Agência Nacional de Vigilância Sanitária. Resolução RDC nº 26 de 11 de maio de Brasília (DF); Conselho Federal de Enfermagem (BR). Resolução COFEN-293/2004 de 21 de setembro de Fixa e estabelece parâmetros para o dimensionamento do quadro de profissionais de enfermagem nas unidades assistenciais das instituições de saúde e assemelhados. Rio de Janeiro (RJ); Bitan Y, Meyer J, Shinar D, Zmora E. Nurses reaction to alarms in a neonatal intensive care unit. Cogn Tech Work Nov;6(4): Author s address: Roberto Carlos Lyra da Silva Rua Dr. Xavier Sigaud, 290, Urca , Rio de Janeiro, RJ proflyra@gmail.com Received: Approved:
ISSN DOI: / v7i
 Alarmes de monitorização invasiva da pressão arterial: damos a atenção necessária? Alarm of monitoring invasive of blood pressure: are we giving the attention required? Monitoreo de alarma arterial invasiva
Alarmes de monitorização invasiva da pressão arterial: damos a atenção necessária? Alarm of monitoring invasive of blood pressure: are we giving the attention required? Monitoreo de alarma arterial invasiva
Stimulus-response time to alarms of the intra-aortic balloon pump: safe care practices
 RESEARCH Stimulus-response time to alarms of the intra-aortic balloon pump: safe care practices Tempo estímulo-resposta aos alarmes do balão intraórtico: práticas para cuidado seguro El tempo estíulo-respuesta
RESEARCH Stimulus-response time to alarms of the intra-aortic balloon pump: safe care practices Tempo estímulo-resposta aos alarmes do balão intraórtico: práticas para cuidado seguro El tempo estíulo-respuesta
Assessment of a neonatal unit nursing staff: Application of the Nursing Activities Score
 Rev. Latino-Am. Enfermagem 2013 Jan.-Feb.;21(1):348-55 Original Article Assessment of a neonatal unit nursing staff: Application of the Nursing Activities Score Bruna Kosar Nunes 1 Edi Toma 2 Objective:
Rev. Latino-Am. Enfermagem 2013 Jan.-Feb.;21(1):348-55 Original Article Assessment of a neonatal unit nursing staff: Application of the Nursing Activities Score Bruna Kosar Nunes 1 Edi Toma 2 Objective:
Reaction time of a health care team to monitoring alarms in the intensive care unit: implications for the safety of seriously ill patients
 ORIGINAL ARTICLE Adriana Carla Bridi 1, Roberto Carlos Lyra da Silva 1, Carolina Correa Pinto de Farias 1, Andrezza Serpa Franco 1, Viviane de Lima Quintas dos Santos 1 Reaction time of a health care team
ORIGINAL ARTICLE Adriana Carla Bridi 1, Roberto Carlos Lyra da Silva 1, Carolina Correa Pinto de Farias 1, Andrezza Serpa Franco 1, Viviane de Lima Quintas dos Santos 1 Reaction time of a health care team
Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring
 Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring Israeli Society of Internal Medicine Meeting July 5, 2013 Eyal Zimlichman MD,
Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring Israeli Society of Internal Medicine Meeting July 5, 2013 Eyal Zimlichman MD,
Non-Profit Academic Project, developed under the Open Acces Initiative
 Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version Simão, Carla Maria Fonseca; Caliri, Maria Helena Larcher; Santos, Claudia Benedita
Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version Simão, Carla Maria Fonseca; Caliri, Maria Helena Larcher; Santos, Claudia Benedita
Monitoring in ICU. BR Bhengu UKZN
 Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
Monitoring in ICU BR Bhengu UKZN What monitoring entails Intermittent (regular or irregular) series of observations Observations are systematic and purposeful Gather information on all aspects of the patient
Nursing work at night in palliative oncology care 1
 Rev. Latino-Am. Enfermagem 2013 May-June;21(3):773-9 Original Article Nursing work at night in palliative oncology care 1 Marcelle Miranda da Silva 2 Marleá Chagas Moreira 3 Joséte Luzia Leite 4 Alacoque
Rev. Latino-Am. Enfermagem 2013 May-June;21(3):773-9 Original Article Nursing work at night in palliative oncology care 1 Marcelle Miranda da Silva 2 Marleá Chagas Moreira 3 Joséte Luzia Leite 4 Alacoque
THE COMMUNICATION BETWEEN NURSE AND THE BINOMIAL CHILD/FAMILY IN PEDIATRIC UNIT 1
 THE COMMUNICATION BETWEEN NURSE AND THE BINOMIAL CHILD/FAMILY IN PEDIATRIC UNIT 1 BARROS, Camilla Silva de 2 ; NEVES, Eliane Tatsch 3 ; ZAMBERLAN, Kellen Cervo 4 ; ABSTRACT It is an experience report about
THE COMMUNICATION BETWEEN NURSE AND THE BINOMIAL CHILD/FAMILY IN PEDIATRIC UNIT 1 BARROS, Camilla Silva de 2 ; NEVES, Eliane Tatsch 3 ; ZAMBERLAN, Kellen Cervo 4 ; ABSTRACT It is an experience report about
TRENDS IN LABOR CONTRACTING IN THE FAMILY HEALTH PROGRAM IN BRAZIL: A TELEPHONE SURVEY
 Cah. Socio. Démo. Méd., XXXXVIIIème année, n 2, p. (Avril-Juin 2008) Cah. Socio. Démo. Méd., 48 (2) : (April-June 2008) TRENDS IN LABOR CONTRACTING IN THE FAMILY HEALTH PROGRAM IN BRAZIL: A TELEPHONE SURVEY
Cah. Socio. Démo. Méd., XXXXVIIIème année, n 2, p. (Avril-Juin 2008) Cah. Socio. Démo. Méd., 48 (2) : (April-June 2008) TRENDS IN LABOR CONTRACTING IN THE FAMILY HEALTH PROGRAM IN BRAZIL: A TELEPHONE SURVEY
The Problem of Alarm Fatigue
 Priority #1: The Problem of Alarm Fatigue wwhen entering a busy labor and delivery unit or neonatal intensive care unit, the first thing people usually notice is the sheer volume of activity. Nurses hurry
Priority #1: The Problem of Alarm Fatigue wwhen entering a busy labor and delivery unit or neonatal intensive care unit, the first thing people usually notice is the sheer volume of activity. Nurses hurry
GAMUT QI Collaborative Consensus Quality Metrics (v. 05/16/2016)
 1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
Non-Profit Academic Project, developed under the Open Acces Initiative
 Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version Polidoro Dini, Ariane; dos Santos Alves, Daniela Fernanda; Ceretta Oliveira,
Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version Polidoro Dini, Ariane; dos Santos Alves, Daniela Fernanda; Ceretta Oliveira,
Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support
 Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support Mithya Lewis-Newby, MD MPH Assistant Professor, Division
Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support Mithya Lewis-Newby, MD MPH Assistant Professor, Division
ENVIRONMENT Preoperative evaluation clinic. Preoperative evaluation clinic. Preoperative evaluation clinic. clinic. clinic. Preoperative evaluation
 Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Educational strategies to improve adherence to patient identification
 Original article Educational strategies to improve adherence to patient identification Revista Gaúcha de Enfermagem Estratégias educativas para melhorar a adesão à identificação do paciente Estrategias
Original article Educational strategies to improve adherence to patient identification Revista Gaúcha de Enfermagem Estratégias educativas para melhorar a adesão à identificação do paciente Estrategias
Recognising a Deteriorating Patient. Study guide
 Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Recognising a Deteriorating Patient Study guide Recognising a deteriorating patient Recognising and responding to clinical deterioration Background Clinical deterioration can occur at any time in a patient
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue. The Development and Implementation of a Rapid Response Program at a Regional Facility
 Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
Rapid Assessment and Treatment (R.A.T.) Team to the Rescue The Development and Implementation of a Rapid Response Program at a Regional Facility Dynamics 2013 Lethbridge Chinook Regional Hospital 276 Bed
EMS System for Metropolitan Oklahoma City and Tulsa 2017 Medical Control Board Treatment Protocols
 PROTOCOL 17A: Adult General Medical s Adult General Medical s Four (4) Levels of General Medical s Priority I and II Priority III No Will time and distance to the hospital of choice be detrimental to the
PROTOCOL 17A: Adult General Medical s Adult General Medical s Four (4) Levels of General Medical s Priority I and II Priority III No Will time and distance to the hospital of choice be detrimental to the
Pediatric Intensive Care Unit Rotation PL-2 Residents
 PL-2 Residents Residents are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
PL-2 Residents Residents are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
King Saud University. Updated Study Plan. Prince Sultan Bin Abdulaziz College for EMS. Bachelor of Science Program, Emergency Medical Services
 2013 King Saud University Prince Sultan Bin Abdulaziz College for EMS Bachelor of Science Program, Emergency Medical Services Updated Study Plan 1433 ه 1434- Prince Sultan Bin Abdulaziz College for EMS,
2013 King Saud University Prince Sultan Bin Abdulaziz College for EMS Bachelor of Science Program, Emergency Medical Services Updated Study Plan 1433 ه 1434- Prince Sultan Bin Abdulaziz College for EMS,
SURGICAL SAFETY CHECKLIST
 SURGICAL SAFETY CHECKLIST WHY: INFORMATION, RATIONALE, AND FAQ May 2009 Building a safer health system INFORMATION, RATIONALE, AND FAQ May 2009 - Version 1.0 The aim of this document is to provide information
SURGICAL SAFETY CHECKLIST WHY: INFORMATION, RATIONALE, AND FAQ May 2009 Building a safer health system INFORMATION, RATIONALE, AND FAQ May 2009 - Version 1.0 The aim of this document is to provide information
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience. Presented by: Fadwa Jabboury, RN, MSN
 Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
New Monitoring Alarm Challenges and Opportunities for Collaborative Progress
 New Monitoring Alarm Challenges and Opportunities for Collaborative Progress AAMI Alarms Summit October 4-5, 2011 Joseph J. Frassica, MD VP and Chief Medical Information Officer - Philips Healthcare NEW
New Monitoring Alarm Challenges and Opportunities for Collaborative Progress AAMI Alarms Summit October 4-5, 2011 Joseph J. Frassica, MD VP and Chief Medical Information Officer - Philips Healthcare NEW
Acute Care Workflow Solutions
 Acute Care Workflow Solutions 2016 North American General Acute Care Workflow Solutions Product Leadership Award The Philips IntelliVue Guardian solution provides general floor, medical-surgical units,
Acute Care Workflow Solutions 2016 North American General Acute Care Workflow Solutions Product Leadership Award The Philips IntelliVue Guardian solution provides general floor, medical-surgical units,
PATIENT RIGHTS, PRIVACY, AND PROTECTION
 REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
Web-based simulation: a tool to teach critical care nursing
 Universidade Federal de São Paulo Programa de Pós-Graduação em Enfermagem Web-based simulation: a tool to teach critical care nursing Sayonara de Fátima F. Barbosa Heimar de Fátima Marin Introduction The
Universidade Federal de São Paulo Programa de Pós-Graduação em Enfermagem Web-based simulation: a tool to teach critical care nursing Sayonara de Fátima F. Barbosa Heimar de Fátima Marin Introduction The
Technovigilance and risk management as tools to improve patient safety in Colombian health care institutions
 Revista Ingeniería Biomédica ISSN 1909-9762 / Volumen 11 / Número 21 / Enero-junio de 2017 / pp. 57-64 Universidad EIA-Universidad CES / Envigado, Colombia Technovigilance and risk management as tools
Revista Ingeniería Biomédica ISSN 1909-9762 / Volumen 11 / Número 21 / Enero-junio de 2017 / pp. 57-64 Universidad EIA-Universidad CES / Envigado, Colombia Technovigilance and risk management as tools
Running head: FAILURE TO RESCUE 1
 Running head: FAILURE TO RESCUE 1 Failure to Rescue Susan Headley Ferris State University FAILURE TO RESCUE 2 Introduction Quality improvement in healthcare is a continuous process that evaluates care
Running head: FAILURE TO RESCUE 1 Failure to Rescue Susan Headley Ferris State University FAILURE TO RESCUE 2 Introduction Quality improvement in healthcare is a continuous process that evaluates care
Policy for Admission to Adult Critical Care Services
 Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
CA-1 CRITICAL CARE ROTATION University of Minnesota Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks
 CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
As Introduced. 132nd General Assembly Regular Session S. B. No Senator Skindell Cosponsor: Senator Williams A B I L L
 132nd General Assembly Regular Session S. B. No. 55 2017-2018 Senator Skindell Cosponsor: Senator Williams A B I L L To amend sections 3727.50, 3727.51, 3727.52, and 3727.53 and to enact sections 3727.80
132nd General Assembly Regular Session S. B. No. 55 2017-2018 Senator Skindell Cosponsor: Senator Williams A B I L L To amend sections 3727.50, 3727.51, 3727.52, and 3727.53 and to enact sections 3727.80
Preventing Medical Errors
 Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
Presents Preventing Medical Errors Contact Hours: 2 First Published: March 31, 2017 This Course Expires on: March 31, 2019 Course Objectives Upon completion of this course, the nurse will be able to: 1.
Transition of Care Practices. Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI
 Transition of Care Practices Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI Objectives Pharmacist 1. Describe transition of care opportunities 2. Explain ways to use pharmacist extenders
Transition of Care Practices Nancy MacDonald, PharmD, BCPS, FASHP Henry Ford Hospital Detroit, MI Objectives Pharmacist 1. Describe transition of care opportunities 2. Explain ways to use pharmacist extenders
Creating and validating an instrument to identify the workload at an Oncology and Hematology Outpatient Service
 ORIGINAL ARTICLE Creating and validating an instrument to identify the workload at an Oncology and Hematology Outpatient Service Construção e validação de instrumento para identificação de carga de trabalho
ORIGINAL ARTICLE Creating and validating an instrument to identify the workload at an Oncology and Hematology Outpatient Service Construção e validação de instrumento para identificação de carga de trabalho
Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that
 Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that hospital. 1 2 3 Note that an actual variance occurs when
Thanks to Anne C. Byrne, RN, Medical Monitor at Northwest Georgia Regional Hospital. This presentation was developed from one she designed for that hospital. 1 2 3 Note that an actual variance occurs when
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
An Evaluative Study of Practices Related to Administration of Vasoactive Drugs by Nurses
 IOSR Journal of Nursing and Health Science (IOSRJNHS) eissn: 3 959.p ISSN: 3 9 Volume 3, Issue Ver. III (MarApr. ), PP 9 An Evaluative Study of Practices Related to Administration of Vasoactive Drugs by
IOSR Journal of Nursing and Health Science (IOSRJNHS) eissn: 3 959.p ISSN: 3 9 Volume 3, Issue Ver. III (MarApr. ), PP 9 An Evaluative Study of Practices Related to Administration of Vasoactive Drugs by
The Importance of Nonverbal Communication During the Preanesthesia Period
 Sawada, N.O.; Mendes, I.A.C.; Galvão, C.M., Trevizan, M.A. The Importance of Nonverbal Communication During the Preanesthesia Period. Clinical Nursing Research, v.01, n.2, p.207-213, 1992. The Importance
Sawada, N.O.; Mendes, I.A.C.; Galvão, C.M., Trevizan, M.A. The Importance of Nonverbal Communication During the Preanesthesia Period. Clinical Nursing Research, v.01, n.2, p.207-213, 1992. The Importance
Cost Effectiveness of Physician Anesthesia J.P. Abenstein, M.S.E.E., M.D. Mayo Clinic Rochester, MN
 Mayo Clinic Rochester, MN Introduction The question of whether anesthesiologists are cost-effective providers of anesthesia services remains an open question in the minds of some of our medical colleagues,
Mayo Clinic Rochester, MN Introduction The question of whether anesthesiologists are cost-effective providers of anesthesia services remains an open question in the minds of some of our medical colleagues,
Pediatric Intensive Care Unit (PICU) Elective PL-1 Residents
 PL-1 Residents Interns are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
PL-1 Residents Interns are required to have sufficient knowledge of their patients in order to present them to the team on rounds, and to construct a differential diagnosis and treatment plan. They are
Teaching Methods. Responsibilities
 Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Performance Scorecard 2013
 NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2013 updated May 2013 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality health care through
NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2013 updated May 2013 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality health care through
Diagnostics for Patient Safety and Quality of Care. Vulnerable System Syndrome
 Diagnostics for Patient Safety and Quality of Care Carol Haraden, PhD APAC Forum This presenter has nothing to disclose. Vulnerable System Syndrome Three core pathologies - Blame - Denial - And the pursuit
Diagnostics for Patient Safety and Quality of Care Carol Haraden, PhD APAC Forum This presenter has nothing to disclose. Vulnerable System Syndrome Three core pathologies - Blame - Denial - And the pursuit
Analysis of adverse events in patients admitted to an intensive care unit
 Original Article Analysis of adverse events in patients admitted to an intensive care unit Análise de eventos adversos em pacientes internados em unidade de terapia intensiva Daniela Benevides Ortega 1,2
Original Article Analysis of adverse events in patients admitted to an intensive care unit Análise de eventos adversos em pacientes internados em unidade de terapia intensiva Daniela Benevides Ortega 1,2
Adverse effects in surgical patients: knowledge of the nursing professionals
 Original Article Adverse effects in surgical patients: knowledge of the nursing professionals Eventos adversos em pacientes cirúrgicos: conhecimento dos profissionais de enfermagem Elena Bohomol 1 Juliana
Original Article Adverse effects in surgical patients: knowledge of the nursing professionals Eventos adversos em pacientes cirúrgicos: conhecimento dos profissionais de enfermagem Elena Bohomol 1 Juliana
Body mobilization for prevention of pressure ulcers: direct labor costs
 RESEARCH Body mobilization for prevention of pressure ulcers: direct labor costs Mobilização corporal para prevenção de úlceras por pressão: custo direto com pessoal Movilización para la prevención de
RESEARCH Body mobilization for prevention of pressure ulcers: direct labor costs Mobilização corporal para prevenção de úlceras por pressão: custo direto com pessoal Movilización para la prevención de
Lost in translation: challenges in handing over critical care
 Lost in translation: challenges in handing over critical care Andre Amaral, MD Assistant Professor Interdepartmental Division of Critical Care Medicine University of Toronto Sunnybrook Health Sciences
Lost in translation: challenges in handing over critical care Andre Amaral, MD Assistant Professor Interdepartmental Division of Critical Care Medicine University of Toronto Sunnybrook Health Sciences
HONG KONG SANATORIUM AND HOSPITAL INTENSIVE CARE UNIT (ICU) GUIDELINES ON ADMISSIONS AND DISCHARGES
 HONG KONG SANATORIUM AND HOSPITAL INTENSIVE CARE UNIT (ICU) GUIDELINES ON ADMISSIONS AND DISCHARGES I. Principle The intensive care unit is operated on the principles of high turnover; ready accessibility
HONG KONG SANATORIUM AND HOSPITAL INTENSIVE CARE UNIT (ICU) GUIDELINES ON ADMISSIONS AND DISCHARGES I. Principle The intensive care unit is operated on the principles of high turnover; ready accessibility
PROCEDURAL SEDATION AND ANALGESIA: HOSPITAL-WIDE POLICY
 CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
Self-care assessment as an indicator for clinical supervision in nursing
 DOI: 10.15253/2175-6783.2016000300008 www.revistarene.ufc.br Original Article Self-care assessment as an indicator for clinical supervision in nursing Avaliação do autocuidado como indicador para supervisão
DOI: 10.15253/2175-6783.2016000300008 www.revistarene.ufc.br Original Article Self-care assessment as an indicator for clinical supervision in nursing Avaliação do autocuidado como indicador para supervisão
C. difficile Infection and C. difficile Lab ID Reporting in NHSN
 C. difficile Infection and C. difficile Lab ID Reporting in NHSN MARY ANDRUS, BA, RN, CIC Infection Preventionist Consultant Learning Objectives Review the structure and of the MDRO/CDAD Module within
C. difficile Infection and C. difficile Lab ID Reporting in NHSN MARY ANDRUS, BA, RN, CIC Infection Preventionist Consultant Learning Objectives Review the structure and of the MDRO/CDAD Module within
Theoretical model of critical thinking in diagnostic processes in nursing
 Theoretical model of critical thinking in diagnostic processes in nursing Greicy Kelly Gouveia Dias Bittencourt 1, Maria da Graça Oliveira Crossetti 2 1 Federal University of Paraíba 2 Federal University
Theoretical model of critical thinking in diagnostic processes in nursing Greicy Kelly Gouveia Dias Bittencourt 1, Maria da Graça Oliveira Crossetti 2 1 Federal University of Paraíba 2 Federal University
CARE OF THE PATIENT REQUIRING CONTINUOUS FLOLAN INFUSION GUIDELINE
 Page Number: 1 of 5 TITLE: CARE OF THE PATIENT REQUIRING CONTINUOUS FLOLAN INFUSION GUIDELINE PURPOSE: To provide guidelines for the nursing care of the patient with a Flolan infusion delivered thru continuous
Page Number: 1 of 5 TITLE: CARE OF THE PATIENT REQUIRING CONTINUOUS FLOLAN INFUSION GUIDELINE PURPOSE: To provide guidelines for the nursing care of the patient with a Flolan infusion delivered thru continuous
The model adopted for the hospital accreditation
 1.0 ANCC CONTACT HOUR Quality of Electronic Nursing Records The Impact of Educational Interventions During a Hospital Accreditation Process Aline Tsuma Gaedke Nomura, MS, RN, Lisiane Pruinelli, PhD, RN,
1.0 ANCC CONTACT HOUR Quality of Electronic Nursing Records The Impact of Educational Interventions During a Hospital Accreditation Process Aline Tsuma Gaedke Nomura, MS, RN, Lisiane Pruinelli, PhD, RN,
NORTHWESTERN LAKE FOREST HOSPITAL. Scorecard updated September 2012
 NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2012 updated September 2012 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality healthcare through
NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2012 updated September 2012 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality healthcare through
Pediatric Neonatology Sub I
 Course Goals Goals 1. Provide patient care that is compassionate, appropriate and effective for the treatment of health problems. 2. Recommend and interpret common diagnostic tests and vital signs. 3.
Course Goals Goals 1. Provide patient care that is compassionate, appropriate and effective for the treatment of health problems. 2. Recommend and interpret common diagnostic tests and vital signs. 3.
Making the Stars Align When Time Matters: Leveraging Actionable Data to Combat Sepsis
 Making the Stars Align When Time Matters: Leveraging Actionable Data to Combat Sepsis Licking Memorial Health Systems Patient Impact Where did we begin? EDUCATION EDUCATION EDUCATION EDUCATION EDUCATION
Making the Stars Align When Time Matters: Leveraging Actionable Data to Combat Sepsis Licking Memorial Health Systems Patient Impact Where did we begin? EDUCATION EDUCATION EDUCATION EDUCATION EDUCATION
Complications Associated with Anesthesia for Gynecology: A Prospective Survey in Oran Algeria
 ISPUB.COM The Internet Journal of Health Volume 6 Number 2 Complications Associated with Anesthesia for Gynecology: A Prospective Survey in Oran Algeria M Khdidja Citation M Khdidja. Complications Associated
ISPUB.COM The Internet Journal of Health Volume 6 Number 2 Complications Associated with Anesthesia for Gynecology: A Prospective Survey in Oran Algeria M Khdidja Citation M Khdidja. Complications Associated
Organ Recovery Services
 Title: Donation After Circulatory Death Associated Departments: Medical Director, VP Operations, Hospital Development Release Date: Approver: Alison Smith Revision History Revision Date Revision Description
Title: Donation After Circulatory Death Associated Departments: Medical Director, VP Operations, Hospital Development Release Date: Approver: Alison Smith Revision History Revision Date Revision Description
The curriculum is based on achievement of the clinical competencies outlined below:
 ANESTHESIOLOGY CRITICAL CARE MEDICINE FELLOWSHIP Program Goals and Objectives The curriculum is based on achievement of the clinical competencies outlined below: Patient Care Fellows will provide clinical
ANESTHESIOLOGY CRITICAL CARE MEDICINE FELLOWSHIP Program Goals and Objectives The curriculum is based on achievement of the clinical competencies outlined below: Patient Care Fellows will provide clinical
BMHI Internship Presentation. Saba Akbar UNC Chapel Hill Apr 11, 2018
 BMHI Internship Presentation Saba Akbar UNC Chapel Hill Apr 11, 2018 2 Centre for Healthcare Resilience and Implementation Science Centre for Health Informatics Centre for Health Systems and Safety Research
BMHI Internship Presentation Saba Akbar UNC Chapel Hill Apr 11, 2018 2 Centre for Healthcare Resilience and Implementation Science Centre for Health Informatics Centre for Health Systems and Safety Research
Using Predictive Analytics to Improve Sepsis Outcomes 4/23/2014
 Using Predictive Analytics to Improve Sepsis Outcomes 4/23/2014 Ryan Arnold, MD Department of Emergency Medicine and Value Institute Christiana Care Health System, Newark, DE Susan Niemeier, RN Chief Nursing
Using Predictive Analytics to Improve Sepsis Outcomes 4/23/2014 Ryan Arnold, MD Department of Emergency Medicine and Value Institute Christiana Care Health System, Newark, DE Susan Niemeier, RN Chief Nursing
Kate Beaumont. Strategy Advisor, NPSA Head of Clinical Interventions, National Patient Safety Campaign.
 Why Safety Matters Kate Beaumont Strategy Advisor, NPSA Head of Clinical Interventions, National Patient Safety Campaign Catherine.beaumont@npsa.nhs.uk www.npsa.nhs.uk About the NPSA What we are: Arm s
Why Safety Matters Kate Beaumont Strategy Advisor, NPSA Head of Clinical Interventions, National Patient Safety Campaign Catherine.beaumont@npsa.nhs.uk www.npsa.nhs.uk About the NPSA What we are: Arm s
Principles In developing these recommendations the Consensus Panel first established the following principles for anesthesia outcomes capture:
 Outcomes of Anesthesia: Core Measures The following Core Measures are the consensus recommendations of the Anesthesia Quality Institute (AQI) and the Multicenter Perioperative Outcomes Group (MPOG). They
Outcomes of Anesthesia: Core Measures The following Core Measures are the consensus recommendations of the Anesthesia Quality Institute (AQI) and the Multicenter Perioperative Outcomes Group (MPOG). They
MEDICAL POLICY No R2 TELEMEDICINE
 Summary of Changes Clarifications: Page 1, Section I. A 6, additional language added for clarification. Deletions: Additions Page 4, Section IV, Description, additional language added in regards to telemedicine.
Summary of Changes Clarifications: Page 1, Section I. A 6, additional language added for clarification. Deletions: Additions Page 4, Section IV, Description, additional language added in regards to telemedicine.
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA
 Review PS18 (2008) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA The terms Anaesthetist, medical practitioner and practitioner
Review PS18 (2008) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS ON MONITORING DURING ANAESTHESIA The terms Anaesthetist, medical practitioner and practitioner
Element(s) of Performance for DSPR.1
 Prepublication Issued Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Prepublication Issued Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
NORTHWESTERN LAKE FOREST HOSPITAL. Scorecard updated May 2011
 NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2011 updated May 2011 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality health care through
NORTHWESTERN LAKE FOREST HOSPITAL Performance Scorecard 2011 updated May 2011 Northwestern Lake Forest Hospital is committed to providing the communities we serve the highest quality health care through
The Institute of Medicine concluded that medical
 Hosp Pharm 2015;50(2):113 117 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-113 Original Article Optimizing Smart Pump Technology by Increasing Critical Safety Alerts
Hosp Pharm 2015;50(2):113 117 2015 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj5002-113 Original Article Optimizing Smart Pump Technology by Increasing Critical Safety Alerts
Anesthesia Elective Curriculum Outline
 Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
Cause of death in intensive care patients within 2 years of discharge from hospital
 Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Using Clinical Criteria for Evaluating Short Stays and Beyond. Georgeann Edford, RN, MBA, CCS-P. The Clinical Face of Medical Necessity
 Using Clinical Criteria for Evaluating Short Stays and Beyond Georgeann Edford, RN, MBA, CCS-P The Clinical Face of Medical Necessity 1 The Documentation Faces of Medical Necessity ç3 Setting the Stage
Using Clinical Criteria for Evaluating Short Stays and Beyond Georgeann Edford, RN, MBA, CCS-P The Clinical Face of Medical Necessity 1 The Documentation Faces of Medical Necessity ç3 Setting the Stage
MBQIP Measures Fact Sheets December 2017
 December 2017 This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant number U1RRH29052, Rural Quality
December 2017 This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant number U1RRH29052, Rural Quality
BEDSIDE NURSES KNOW: The Patient Safety Act. Fewer Patients = Better Healthcare. A Toolkit for Massachusetts RNs. How you can help make safe limits
 The Patient Safety Act BEDSIDE NURSES KNOW: Fewer Patients = Better Healthcare A Toolkit for Massachusetts RNs How you can help make safe limits on RN patient loads a reality This booklet provides you
The Patient Safety Act BEDSIDE NURSES KNOW: Fewer Patients = Better Healthcare A Toolkit for Massachusetts RNs How you can help make safe limits on RN patient loads a reality This booklet provides you
1. Create a heightened awareness of clinical risks and enterprise-wide challenges associated with misuse of copy and paste.
 1 2 Disclaimer The information, examples and suggestions presented in this material have been developed from sources believed to be reliable, but they should not be construed as legal or other professional
1 2 Disclaimer The information, examples and suggestions presented in this material have been developed from sources believed to be reliable, but they should not be construed as legal or other professional
PROMOVING SPACES FOR THE COLLECTIVE CONSTRUCTION OF KNOWLEDGE IN THE FAMILY HEALTH STRATEGY PROGRAM 1
 PROMOVING SPACES FOR THE COLLECTIVE CONSTRUCTION OF KNOWLEDGE IN THE FAMILY HEALTH STRATEGY PROGRAM 1 QUADROS, Jacqueline Silveira de²; MUNHOZ, Cloris Ineu 3 ; COLOMÉ, Juliana Silveira 4. ABSTRACT This
PROMOVING SPACES FOR THE COLLECTIVE CONSTRUCTION OF KNOWLEDGE IN THE FAMILY HEALTH STRATEGY PROGRAM 1 QUADROS, Jacqueline Silveira de²; MUNHOZ, Cloris Ineu 3 ; COLOMÉ, Juliana Silveira 4. ABSTRACT This
Nursing approaches for pain diagnosis and classification of outcomes*
 ORIGINAL ARTICLE Nursing approaches for pain diagnosis and classification of outcomes* Condutas de enfermagem no diagnóstico da dor e a classificação dos resultados Simone Regina Alves de Freitas Barros
ORIGINAL ARTICLE Nursing approaches for pain diagnosis and classification of outcomes* Condutas de enfermagem no diagnóstico da dor e a classificação dos resultados Simone Regina Alves de Freitas Barros
PHARMACY SERVICES/MEDICATION USE
 25.01. 10 Drug Reactions & Administration Errors & Incompatibilities. Drug administration errors, adverse drug reactions and incompatibilities must be immediately reported to the attending physician and
25.01. 10 Drug Reactions & Administration Errors & Incompatibilities. Drug administration errors, adverse drug reactions and incompatibilities must be immediately reported to the attending physician and
Serious Incident Report Public Board Meeting 26 November 2015
 Serious Incident Report Public Board Meeting 26 November 2015 Presented for: Presented by: Author Previous Committees Governance Yvette Oade, Chief Medical Officer Craig Brigg, Director of Quality None
Serious Incident Report Public Board Meeting 26 November 2015 Presented for: Presented by: Author Previous Committees Governance Yvette Oade, Chief Medical Officer Craig Brigg, Director of Quality None
Structural elements of critical thinking of nurses in emergency care
 Original article Structural elements of critical thinking of nurses in emergency care Revista Gaúcha de Enfermagem Elementos estruturais do pensamento crítico de enfermeiros atuantes em emergências Elementos
Original article Structural elements of critical thinking of nurses in emergency care Revista Gaúcha de Enfermagem Elementos estruturais do pensamento crítico de enfermeiros atuantes em emergências Elementos
Association between workload of the nursing staff and patient safety outcomes
 Original Article DOI: http://dx.doi.org/10.1590/s1980-220x2016021203255 Association between workload of the nursing staff and patient safety outcomes Associação entre carga de trabalho da equipe de enfermagem
Original Article DOI: http://dx.doi.org/10.1590/s1980-220x2016021203255 Association between workload of the nursing staff and patient safety outcomes Associação entre carga de trabalho da equipe de enfermagem
Acta Paulista de Enfermagem ISSN: Escola Paulista de Enfermagem Brasil
 Acta Paulista de Enfermagem ISSN: 0103-2100 ape@unifesp.br Escola Paulista de Enfermagem Brasil Medina Valadares, Alessandra Freire; da Silva Magro, Marcia Cristina Opinião dos estudantes de enfermagem
Acta Paulista de Enfermagem ISSN: 0103-2100 ape@unifesp.br Escola Paulista de Enfermagem Brasil Medina Valadares, Alessandra Freire; da Silva Magro, Marcia Cristina Opinião dos estudantes de enfermagem
Asian Journal of Business and Management Sciences ISSN: January, 2016 Vol. 4 No. 09[16-23]
![Asian Journal of Business and Management Sciences ISSN: January, 2016 Vol. 4 No. 09[16-23] Asian Journal of Business and Management Sciences ISSN: January, 2016 Vol. 4 No. 09[16-23]](/thumbs/83/87289717.jpg) OPENING AND CLOSING OF COMPANIES IN A BRAZILIAN CITY OF SÃO PAULO STATE: AN ANALYSIS FROM 2010 TO 20 Bruno Celestino Mateus Bachelor in Business Administration FHO Uniararas E-mail: bmateus.89@hotmail.com
OPENING AND CLOSING OF COMPANIES IN A BRAZILIAN CITY OF SÃO PAULO STATE: AN ANALYSIS FROM 2010 TO 20 Bruno Celestino Mateus Bachelor in Business Administration FHO Uniararas E-mail: bmateus.89@hotmail.com
Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients
 UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology
 CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology Description of Rotation or Educational Experience This rotation is a continuation of the CA-2 Cardiothoracic
CA-3 Curriculum for Cardiac Anesthesia West Virginia University Department of Anesthesiology Description of Rotation or Educational Experience This rotation is a continuation of the CA-2 Cardiothoracic
Telenursing in Primary Health Care: Report of Experience in Southern Brazil
 202 Connecting Health and Humans K. Saranto et al. (Eds.) IOS Press, 2009 2009 The authors and IOS Press. All rights reserved. doi:10.2/978-1-60750-024-7-202 Telenursing in Primary Health Care: Report
202 Connecting Health and Humans K. Saranto et al. (Eds.) IOS Press, 2009 2009 The authors and IOS Press. All rights reserved. doi:10.2/978-1-60750-024-7-202 Telenursing in Primary Health Care: Report
Identifying patient risks during hospitalization
 Original Article Identifying patient risks during hospitalization Identificando os riscos do paciente hospitalizado Lucélia Ferreira Lima 1, Lucila Coca Leventhal 2, Maria da Piedade do Pilar Fernandes
Original Article Identifying patient risks during hospitalization Identificando os riscos do paciente hospitalizado Lucélia Ferreira Lima 1, Lucila Coca Leventhal 2, Maria da Piedade do Pilar Fernandes
Prepublication Requirements
 Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Fundamental Critical Care Support (FCCS)
 Provided By: Fundamental Critical Care Support (FCCS) Center for Advanced Medical Learning and Simulation (CAMLS) 124 S. Franklin, Tampa, Florida 33602 Needs Statement and Educational Gap: Early identification
Provided By: Fundamental Critical Care Support (FCCS) Center for Advanced Medical Learning and Simulation (CAMLS) 124 S. Franklin, Tampa, Florida 33602 Needs Statement and Educational Gap: Early identification
Non-Profit Academic Project, developed under the Open Acces Initiative
 Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version de Souza, Sabrina; Kuerten Rocha, Patrícia; de Almeida Cabral, Patrícia Fernanda;
Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Sistema de Información Científica English version de Souza, Sabrina; Kuerten Rocha, Patrícia; de Almeida Cabral, Patrícia Fernanda;
Admissions and Readmissions Related to Adverse Events, NMCPHC-EDC-TR
 Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
Admissions and Readmissions Related to Adverse Events, 2007-2014 By Michael J. Hughes and Uzo Chukwuma December 2015 Approved for public release. Distribution is unlimited. The views expressed in this
Select Medical TRANSITIONS OF CARE & CARE COORDINATION
 Select Medical TRANSITIONS OF CARE & CARE COORDINATION Agenda Select Medical Overview Transitions of Care Right Patient, Right Level of Care,Right Time Chronic Critical Illness Syndrome Role of Long Term
Select Medical TRANSITIONS OF CARE & CARE COORDINATION Agenda Select Medical Overview Transitions of Care Right Patient, Right Level of Care,Right Time Chronic Critical Illness Syndrome Role of Long Term
Telemedicine: Solving the Root Causes for Preventable 30-day Readmissions in SNF Settings
 For Immediate Release: 05/11/18 Written By: Scott Whitaker Telemedicine: Solving the Root Causes for Preventable 30-day Readmissions in SNF Settings Outlining the Problem: Reducing preventable 30-day hospital
For Immediate Release: 05/11/18 Written By: Scott Whitaker Telemedicine: Solving the Root Causes for Preventable 30-day Readmissions in SNF Settings Outlining the Problem: Reducing preventable 30-day hospital
St. Antonius Hospital reduces non-actionable ICU alarms by 40% to improve patient care and staff satisfaction
 Clinical Transformation and Education Who ICU Department, St. Antonius Hospital, Nieuwegein, The Netherlands Ineke van de Pol, project champion and ICU nurse practitioner Dr. J.W. Wirds, anesthesiologist
Clinical Transformation and Education Who ICU Department, St. Antonius Hospital, Nieuwegein, The Netherlands Ineke van de Pol, project champion and ICU nurse practitioner Dr. J.W. Wirds, anesthesiologist
ROTATION DESCRIPTION FORM PGY1
 ROTATION DESCRIPTION FORM PGY1 Rotation Title Medicine Intensive Care Unit (MICU) Level of Learner PY4 PGY1 PGY2 Preceptor(s) Stacy Campbell-Bright, Brian Murray Preceptor Contact Stacy.Campbell-Bright@unchealth.unc.edu;
ROTATION DESCRIPTION FORM PGY1 Rotation Title Medicine Intensive Care Unit (MICU) Level of Learner PY4 PGY1 PGY2 Preceptor(s) Stacy Campbell-Bright, Brian Murray Preceptor Contact Stacy.Campbell-Bright@unchealth.unc.edu;
Assessment and Reassessment of Patients
 Approved by: Assessment and Reassessment of Patients Senior Director, Operations, Emergency, Medicine, Critical Care & Respiratory - GNCH Senior Director, Operations, Emergency, Medicine, Critical Care
Approved by: Assessment and Reassessment of Patients Senior Director, Operations, Emergency, Medicine, Critical Care & Respiratory - GNCH Senior Director, Operations, Emergency, Medicine, Critical Care
RADIOLOGICAL MONITORING AND SURVEYS
 Radiological Monitoring Surveys Page 1 of 9 RADIOLOGICAL MONITORING AND SURVEYS 1.0 Objective The objective of this surveillance is to verify that the laboratory has established and implemented an effective
Radiological Monitoring Surveys Page 1 of 9 RADIOLOGICAL MONITORING AND SURVEYS 1.0 Objective The objective of this surveillance is to verify that the laboratory has established and implemented an effective
The Multidisciplinary aspects of JCI accreditation
 The Multidisciplinary aspects of JCI accreditation Saleem Kiblawi MD, FCCP, Physician consultant, Joint Commission International Oakbrook, Illinois USA Lebanese American University April 15, 2016 Beirut,
The Multidisciplinary aspects of JCI accreditation Saleem Kiblawi MD, FCCP, Physician consultant, Joint Commission International Oakbrook, Illinois USA Lebanese American University April 15, 2016 Beirut,
