Pediatrics Residents Perspectives on Family-Centered Rounds: A Qualitative Study at 2 Children s Hospitals
|
|
|
- Spencer Ball
- 6 years ago
- Views:
Transcription
1 Pediatrics Residents Perspectives on Family-Centered Rounds: A Qualitative Study at 2 Children s Hospitals Vineeta Mittal, MD Evelina Krieger, MD Benjamin C. Lee, MD Terry Kind, MD, MPH Timothy McCavit, MD Joyce Campbell, BSN, MS Mary C. Ottolini, MD, MPH Glenn Flores, MD Abstract Background Many academic hospitals have incorporated family-centered rounds, yet little is known about pediatrics residents perspectives on the educational impact of these rounds. Objective To identify pediatrics residents knowledge, attitudes, and beliefs about family-centered rounds, including perceived benefits and barriers. Methods We conducted focus groups of residents exposed to family-centered rounds at 2 universityaffiliated, freestanding children s hospitals. Focus group data were analyzed using grounded theory. Results A total of 24 residents participated in 4 focus groups. Residents reported that family-centered rounds enhance education by increasing patient encounters and improving physical exam skills, direct observation, real-time feedback, and attending role modeling; improve parent satisfaction, interpersonal and communication skills, and safety; and reduce length of stay. Physical constraints (large teams and small rooms), lack of uniform approaches to family-centered rounds, variable attending teaching styles, and specific conditions (child abuse, patients on isolation) were cited barriers. Conclusions Pediatrics residents report that wellconducted family-centered rounds improve their education and the quality of patient care, including parent satisfaction, communication with families, and patients length of stay. Standardizing family-centered rounds and reducing attending variability in teaching style might further enhance residents educational experiences. Vineeta Mittal, MD, is Associate Professor in the Division of General Pediatrics, Department of Pediatrics, University of Texas Southwestern Medical Center, and Children s Medical Center Dallas; Evelina Krieger, MD, is Assistant Professor in the Division of Hospital Medicine and the Department of Pediatrics, Children s National Medical Center, and George Washington University School of Medicine; Benjamin C. Lee, MD, is Assistant Professor in the Division of Hospital Medicine and the Department of Pediatrics, University of Texas Southwestern Medical Center, and Children s Medical Center Dallas; Terry Kind, MD, MPH, is Associate Professor in the Department of Medical Education, Children s National Medical Center, and George Washington University School of Medicine; Timothy McCavit, MD, is Assistant Professor in the Division of Hematology and Oncology and the Department of Pediatrics, University of Texas Southwestern Medical Center, and Children s Medical Center Dallas; Joyce Campbell, BSN, MS, is Senior Quality Manager in the Department of Medical Education, Children s National Medical Center; Mary C. Ottolini, MD, MPH, is Professor and Vice Chair in the Department of Medical Education, Children s National Medical Center, and George Washington University School of Medicine; and Glenn Flores, MD, is Professor, the Judith and Charles Ginsburg Endowed Chair, and Director of the Division of General Pediatrics, Department of Pediatrics, University of Texas Southwestern Medical Center, and Children s Medical Center Dallas. Funding: This work was supported in part by Children s Medical Center Dallas and the Children s Academy of Pediatric Educators. This work was presented in part as a platform presentation in July 2009 at the annual meeting of the Society of Hospitalist Medicine in Tampa, FL, and as a poster presentation in May 2010 at the annual meeting of the Pediatric Academic Societies in Vancouver, BC, Canada. Corresponding author: Vineeta Mittal, MD, Division of General Pediatrics, Department of Pediatrics, University of Texas Southwestern Medical Center, 5323 Harry Hines Boulevard, Dallas, TX , , Vineeta.Mittal@Childrens.com Editor s Note: The online version of this article contains the moderator s guide used in this study. Background Family-centered rounds (FCRs) are multidisciplinary rounds consisting of medical teams partnering with patients and families in medical decision making. 1,2 Academic hospitals are more likely to conduct FCRs. 2 Accreditation Council for Graduate Medical Education core competencies, such as professionalism and interpersonal and communication skills, ideally are taught at the bedside; FCRs allow residents to interact with patients and families under direct faculty supervision, and are valuable in teaching residents these competencies. 3,4 Implementing FCRs can be challenging in a busy inpatient environment. Although FCRs have been widely adopted, 2 7 the literature on their impact on patient care, discharge timeliness, 3 teamwork, and staff and parental Received December 15, 2011; revisions received May 14, and June 14, 2012; accepted June 25, DOI: Journal of Graduate Medical Education, March
2 satisfaction is limited, 2,5 and little is known about the educational impact of FCRs. Residents are a crucial part of FCRs; this makes it important to understand their perspectives. The study objectives were to identify pediatrics residents perceptions of FCRs, including benefits of and barriers to successful FCRs. Methods Study Design We conducted a collaborative qualitative study using focus groups 8 at Children s Medical Center Dallas (CMC) and Children s National Medical Center (CNMC). The study was conducted from November 2008 to February The study protocol was approved by both institutions Institutional Review Boards. Setting CMC and CNMC are tertiary-care, university-affiliated, freestanding children s hospitals with more than 250 beds. More than 100 trainees rotate through each hospital annually. Both centers initiated FCRs in 2007, and they share similar FCR styles, including presenting the complete case and discussion with families present, involving families in decision making, encouraging lay language, writing orders during FCRs to facilitate workflow, identifying discharge needs early, and balancing patient care and education. Daily FCRs were conducted on weekdays, but weekend FCRs were variable and attending dependent. An attending physician from a single ward rounded during FCRs for 2 weeks, and most patients were general pediatric patients. FCRs consistently included residents, students, attendings, nurses, and case managers; interpreters, nutritionists, and social workers were variably present. Participants and Inclusion Criteria Residents exposed to FCRs for at least one block (4 weeks) on a general pediatric ward were recruited via . Because interns and residents might have different FCR perspectives, participants were assigned to separate intern or senior resident focus groups. Focus Groups At each institution, we conducted 2 separate focus groups: 1 with interns and 1 with senior residents. Participants completed an anonymous questionnaire regarding sociodemographic data and received a $100 honorarium. Trained moderators conducted focus groups at each hospital using an identical moderator s guide (provided as online supplemental material). The 23-question moderator s guide addressed 8 domains: communication, parental satisfaction, outcomes, safety, efficiency, What was known Little is known about pediatrics residents perspectives on the educational impact of FCRs. What is new This is the first study, to our knowledge, to identify pediatrics residents knowledge, attitudes, and beliefs about FCRs, including perceived benefits and barriers. Limitations The single specialty limits generalizability; prior exposure to FCRs in medical school may have affected resident perceptions. Bottom line Residents report that well-conducted FCRs improve education and quality of care, including parental satisfaction, communication, and patient length of stay. coordination of care for complex medical cases, implementation barriers and benefits, and teaching and learning. Moderator s guide questions were derived from the findings of a pilot study and Consumer Assessment of Healthcare Provider and Systems questions. 9 Analysis Thematic saturation was achieved during the fourth focus group. Focus groups were audiotaped and transcribed by a professional transcriptionist unaware of the study aims and participants names. Prior to analyses, 4 authors (V.M., B.C.L., E.K., and T.K.) agreed on a uniform approach to transcript analysis using grounded theory. 10 Transcripts were margin coded, and common themes and subthemes were identified. Disagreements in coding were resolved by consensus. Results Participant Sociodemographics Of the 24 participants, 14 (9 interns and 5 senior residents) were from CMC, and 10 (5 interns and 5 senior residents) were from CNMC. Three-quarters (18 of 24) were female; the mean age was 27 years, 80% (19 of 24) were non- Hispanic white, and about two-thirds (16 of 24) were exposed to FCRs during medical school Themes Analyses identified 54 themes in 5 categories (T ABLES 1 and 2 ). Improved Trainee Education Residents stated that FCRs improve learning through increased patient volume, because they see every patient on FCRs (T ABLES 1 and 3 ). As one trainee stated, I can get information and retain it, because I have a face, family, and situation. Residents noted seeing more physical exam findings during FCRs. 82 Journal of Graduate Medical Education, March 2013
3 TABLE 1 Taxonomy of Attitudes, Beliefs, and Practices of Pediatrics Residents Regarding Family-Centered Rounds (FCRs) TABLE 1 Continued Number of pages/calls Codes Improved trainee education Increased number of patients seen on FCRs Visual and real-time learning: improved PE skills Role modeling and real-time feedback by attending Better learning about communicating with families Enhanced learning and leadership opportunities for senior resident Parental satisfaction Better information sharing and involvement in care Better understanding of medical condition Better understanding of roles of providers Reduced number of visits by providers Communication Direct communication and immediate clarification Uniform communication/all on same page Improved trainee and team communication skills More lay language Presence of bedside nurse facilitates communication Outcomes Patient safety Provides more checks on patient history Communication mistakes identified Early identification of sick kids No change in medication errors Length of stay Better discharge planning Depends on attending focus Reduced, if case manager part of FCRs Efficiency/work flow Depends on attending s rounding style Location of patient beds on multiple floors High patient census reduces efficiency Prolonged duration of rounds Increased parental questions reduce efficiency Language barriers affect flow and efficiency No change in outcomes Coordination of care for complex cases Handoffs ICU transfers Abbreviations: ICU, intensive care unit; PE, physical exam. Watching attendings interact and communicate with patients and families was cited as helpful. One trainee commented, I learned that doctors talk to doctors in a way that doctors should not talk to their patients. So, even though you mess up, there is a lot to learn. Parental Satisfaction and Communication Residents noted that FCRs improve parental satisfaction (T ABLES 1 and 3 ). They mentioned that parents are better informed and involved in decision making on FCRs. They don t get conflicting information; if they do, there is clarification, said one trainee. Residents observed that FCRs provided families with an opportunity to communicate directly with the caregivers (T ABLE 3). Having everyone on rounds got everyone on the same page. Lay language was found to be useful in improving parental understanding. Outcomes Trainees noted that FCRs improve several outcomes, including patient safety and length of stay (T ABLE 1). FCRs were noted to improve safety by providing more checks on the history and physical exam and by identifying communication errors. Better discharge planning was seen as reducing length of stay. One trainee stated, With an asthma patient, we say, Do you have a machine or inhaler? They say, we have an inhaler, but we want a machine, and the case manager is there. As opposed to, I don t know what they have at home. I will call the case manager. Residents noted that length of stay depended on the attending s focus and the presence of case managers. FCR efficiency was principally attending dependent. Patient location, a high census, increased parental questions, and language barriers were other factors affecting efficiency, including coordination of care for complex cases, medication errors, number of pages, codes, handoffs, and intensive care unit transfers. Barriers to FCRs Residents identified 6 categories of FCR barriers (TABLES 2 and 4 ). The physical environment can be an impediment. Lack of a consistent FCR approach and Journal of Graduate Medical Education, March
4 TABLE 2 Physical environment Large team size Small room size Taxonomy of Themes Regarding Barriers to Family-Centered Rounds (FCRs) as Identified by Pediatrics Residents Geographic location of beds Lack of uniformity of rounds Lack of standardization of FCR process Lack of training for trainees and of attending Variability in attending: rounding style and FCR focus Too many repeats at every level of medical hierarchy Resident-related barriers Fear of not appearing knowledgeable in front of family Distractions and interruptions Time/duration of FCRs Discomfort with FCRs Attending-specific barriers Variability in focus and practice style Lack of comfort with FCRs Varying teaching styles Family-specific barriers Language and cultural issues Participation issues Too many parental questions Medical jargon confusing Specific and sensitive patient condition and circumstances Patients on isolation STDs HIV Child abuse Abbreviation: STD, sexually transmitted disease. variability in attending rounding and teaching styles were consistently reported as major barriers. There needs to be a standard, because every attending is different, said one trainee. Residents added that training attendings and teams on conducting FCRs and having FCR rules enhance efficiency. One trainee said, We kept reiterating to present pertinent positives. No need to talk about negatives. It cuts down time and we got done. Residents cited attending teaching variability as a barrier and recommended that teaching during FCRs be in a nonlecture format involving clinical pearls, physical exam findings, and thought processes. Some attendings are very efficient. Then there are others much less efficient who repeat everything, examine every child on rounds. If the attending is not good, it makes it very difficult, said one trainee. Increased parental questions, lack of parental participation, and limited use of lay language were other FCR barriers (T ABLES 2 and 4 ). Residents noted that communicating with limited English-proficient families without interpreters was culturally insensitive. Patients with specific and sensitive conditions (eg, HIV, child abuse, and patients on isolation) were additional barriers. Discussion The study findings suggest that, if conducted well, FCRs enhance resident education and the quality of patient care, including patient satisfaction, communication, and length of stay. Physical constraints, lack of rounding uniformity, and variability in attending rounding and teaching styles were key FCR barriers. Implication for FCRs Enhanced Patient Volume and Education Programs strive to balance adequate numbers of patients across the spectrum of age and medical complexity to maximize educational experiences. 11 FCRs expose residents to more patient encounters without increasing their workload. Therefore, it is not surprising that residents identified FCRs as a valuable experience, resulting in better understanding of the decision-making process, learning about communication, and opportunities to observe more physical exams. Attending Role Modeling and Teaching Attending role modeling can improve learners skills in medical interviewing, physical exam, communication, and professionalism. 4 Medical students report effective teaching of physical exams to be least often experienced during FCRs, and they identified FCRs as a venue to teach them. 12 In this study, residents identified attending role modeling as an effective educational tool. Teachable moments identified included enhanced physical exam skills, improved communication skills, and enhanced knowledge through case-based learning. Attending role modeling may also provide opportunities to observe and learn about compassion, respect, accountability, and sensitivity with diverse populations. Direct Observation, Feedback, and Communication Skills Direct observation is considered the gold standard in assessing behavior, 13 but it is underused, because trainees 84 Journal of Graduate Medical Education, March 2013
5 TABLE 3 Representative Quotes by Pediatrics Residents on Selected Key Family-Centered Rounds (FCRs) Issues Improved trainee education I think getting the opportunity to talk to parents and update them. And, also, develop the sense of how what we are thinking medically is affecting the person, and sometimes we forget that. Sometimes we get a lot of emotional reactions from the family, and that reaction helps us be better doctors, I think. Better, because you are physically seeing and making treatment decisions versus getting a mini-lecture. As a senior, I had full leadership responsibility, of course with supervision. I really enjoyed the autonomy and them pushing me. It was pretty much me assigning things to read, teaching physical findings; I was very active too. Parental satisfaction They are more satisfied because we are informing them better; labs and test results are discussed with them every day. They know exactly who s who and what is what. You walk in, and everyone s on the same page. More satisfied because they don t have to repeat same things to four or five different people. Communication They provide an opportunity for parents to give their input. A lot of parents don t know how to advocate for them. When you go straight to them and ask them while the team is there, they feel comfortable voicing those things. With one visit, it is all said at one time - what the plan of care is - and from there on, it is gold inscribed in stone, and unless there is a change to that then, it is totally clear to the family. We all need to learn to eliminate that medical vocabulary when we are talking to families, and I think if it is done well, you can be just as efficient in your rounds, give the medical information that is needed in a way that the families can still understand. Outcomes Some attendings tend to talk more - not really explain to families - but talk more, if there is a family around, prolonging the whole rounding experience, and that diminishes work time, getting ready for sign-offs, getting things done. With complex medical cases, some parents are very knowledgeable and make contributions, and I have had parents that are totally oblivious and focused on other issues. So the whole team is not focused on the medical issues. report rarely being observed, although they value the experience. 14 Residents identified directly observing attendings as an important educational experience in learning about communication in teams and with families. FCRs also allow direct trainee observation, with real-time attending feedback. Thus, direct observation and feedback may be an effective vehicle for developing interpersonal and communication skills. FCRs, Patient Satisfaction, and Communication Effective communication between clinicians and parents is crucial to parental satisfaction. 15 FCRs improve parental satisfaction, communication, and collaboration between fellows and nurse practitioners in the neonatal intensive care unit. 16 Consistent with these findings, residents in our study reported improved parental satisfaction secondary to enhanced communication and information sharing, resulting in improved parental understanding of their child s condition and better comprehension of providers roles. Patient satisfaction is a critical outcome measure, and FCRs may be a powerful venue for future physicians to learn effective communication and information sharing. FCRs, Quality, and Outcomes FCRs improve discharge timeliness 3 and parental understanding of discharge goals. 2 Trainees in this study reported that FCRs reduce the length of stay because FCRs put everyone on the same page and often include case managers who help with discharge planning. Discharge planning during FCRs may allow residents to learn about indications for hospitalization, discharge criteria, and systems-based practices to coordinate care. What Can Residents Teach Us About How FCRs Can Be More Efficient? Lack of a consistent FCR approach and variability in attending rounding and teaching styles were key FCR barriers. On a busy general pediatric floor, conducting efficient and educational FCRs can be challenging. Thus, addressing factors identified by residents that led to inconsistent rounds may be useful. Key issues include prolonged rounding duration; variability in attending FCR practice and training about conducting FCRs; and the need for developing rounding strategies for patients with language barriers and sensitive patient conditions. Journal of Graduate Medical Education, March
6 TABLE 4 Focus Group Quotes by Pediatrics Residents on Family-Centered Rounds (FCRs) Barriers Barriers posed by physical environment I am just not convinced that family-centered rounds are most efficient way to round on 35 kids, especially if they are dispersed all over the floors of the hospital. It is physically exhausting if you are rounding for 4 4 1/2 hours Lack of uniformity of rounds We don t have it standardized here. There are no rules. I think it needs to have standard rules for everyone. I have a strong feeling that attending aren t trained in family-centered rounds. We certainly aren t trained as seniors, and interns aren t trained, either Resident-related barriers When our pages and phones are constantly ringing and we are interrupted dozens of times on rounds, it is so disruptive The most difficult aspect is learning what is appropriate to bring up during family-centered rounds and what should wait for later Attending-specific barriers Attendings should keep it concise and not go off on a half-hour lecture. I think another barrier as a senior is not having an attending that lets you lead the team Yes, there is always a fear that the attending or senior would ask something and we would just not know. And, it is fine in sit-down rounds, because I don t mind looking dumb in front of other interns, but, in front of parents, they are like, hmm, my doctor really doesn t know enough On rounds, I like to hear little tidbits, not a whole lot of information or lecture, not 80 minutes, just bam, bam, bam, this, this, and this. Physical findings or little tips, clinical hints. Things that you wouldn t know and things that you would only see if you were in the room with the patient Family-specific barriers Talking in front of a parent that doesn t understand the language, because you don t have time to get an interpreter. A lot of times parents wouldn t be there, they would be asleep or they wouldn t wake up. Specific and sensitive patient condition and circumstances We had that non-accidental trauma or a CPS [Child Protective Services] case. It is really hard to talk candidly, if at all, in the room. Suboptimal attending behaviors causing inefficient FCRs were identified by residents. Residents acknowledged that focused and timely FCRs were most efficient. Efficient teaching strategies identified by residents included: (1) demonstrating focused physical exams; (2) modeling communication skills; (3) providing clinical pearls; and (4) avoiding repetition. These findings are consistent with a recent study that showed that the most important factor associated with resident satisfaction with FCRs was the attending physician. 17 Faculty training programs to conduct effective and efficient FCRs and avoiding the aforementioned suboptimal behaviors might reduce attending variability and improve attending FCR teaching. We are currently analyzing the results of family focus groups for both limited English-proficient and English-proficient families to examine family perceptions of FCRs. Limitations Certain study limitations should be noted, including the possibility of selection bias (because not all residents in both programs participated) and the inability to compare the perspectives of participating and nonparticipating residents. A different moderator conducted the focus groups at each center, and a comparison of resident perceptions of FCRs versus other rounding modalities was not possible. Finally, it is possible that prior exposure to FCRs in medical school may have primed pediatrics residents to accept FCRs. Conclusions Our findings indicate that, if conducted well, residents perceive that FCRs improve education, quality of care, and outcomes, including parental satisfaction, communication, and length of stay. Educational benefits of FCRs include 86 Journal of Graduate Medical Education, March 2013
7 learning through increased patient encounters, attending role modeling, and direct observation and feedback. Physical constraints, lack of uniformity of rounds, and variability in attending rounding and teaching styles were reported as FCR barriers. References 1 Sisterhen LL, Blaszak RT, Woods MB, Smith CE. Defining family-centered rounds. Teach Learn Med. 2007;19(3): Mittal V, Sigrest T, Ottolini M, Rauch D, Lin H, Kit B, et al. Family-centered rounds on pediatric wards: a PRIS network survey of US and Canadian hospitalists. Pediatrics. 2010;126; Muething SE, Kotagal UR, Schoettker PJ, Gonzalez del Ray J, DeWitt TG. Family-centered bedside rounds: a new approach to patient care and teaching. Pediatrics. 2007;119(4): LaCombe MA. On bedside teaching. Ann Intern Med. 1997;126(3): Rosen P, Stenger E, Bochkoris M, Hannon MJ, Kwoh CK. Family-centered multidisciplinary rounds enhance the team approach in pediatrics. Pediatrics. 2009;123(4):e603 e Latta LC, Dick R, Parry C, Tamura GS. Parental responses to involvement in rounds on a pediatric inpatient unit at a teaching hospital: a qualitative study. Acad Med. 2008;83(3): Bergert L, Patel S. Family-centered rounds: a new twist on an old concept. Hawaii Med J. 2007;66(7): Kitizinger J. Qualitative research: introducing focus groups. Br Med J. 1995; 311: Agency for Healthcare Research and Quality. CAHPS survey and reporting kits. eng_4pt_v2.pdf. Accessed July 26, Krueger RA, Casey MA. Focus Groups: A Practical Guide for Applied Research. 4th ed. Thousand Oaks, CA: SAGE Publications Inc; Accreditation Council for Graduate Medical Education. Program Requirements for Graduate Medical Education in Child Abuse Pediatrics. ProgramRequirements/339_child_abuse_peds_ pdf. Accessed December 4, Cox ED, Schumachur JB, Young HN, Evans MD, Moreno MA, Sigrest TD. Medical student outcomes after family-centered rounds. Acad Pediatr. 2011;11(5): Bardella I, Janosky J, Elnicki M, Ploof D, Kolarik R. Observed versus reported precepting skills: teaching behaviors in a community ambulatory clerkship. Med Educ. 2005;39: Kang Y, Bardes C, Gerber L, Storey-Johnson C. Pilot of direct observation of clinical skills (DOCS) in a medicine clerkship: feasibility and relationship to clinical performance measures. Med Educ Online. 2009;14:9. med-ed-online.org. Accessed June 6, Brown J, Boles M, Mullooly J, Levinson W. Effect of clinician communication skills training on patient satisfaction. Ann Intern Med. 1999;131: Voos KC, Ross G, Ward UJ, Yohay AL, Osorio SN, Perlman JM. Effects of implementing family-centered rounds in a neonatal intensive care. J Matern Fetal Neonatal Med. 2011;24(11): Rappaport DI, Cellucci MF, Leffler MG. Implementing family-centered rounds: pediatric residents perception. Clin Pediatr. 2010;49(3): Journal of Graduate Medical Education, March
Goals. What Are Family-Centered Rounds? Disclosure. Overview of Today s Talk. Video: This Was Back Then..
 Improving Interdisciplinary Communication: Family-Centered Rounds 1 Disclosure 2 I have nothing to disclose Vineeta Mittal, MD FAAP Assistant Professor Goals 3 Overview of Today s Talk 4 Define family-centered
Improving Interdisciplinary Communication: Family-Centered Rounds 1 Disclosure 2 I have nothing to disclose Vineeta Mittal, MD FAAP Assistant Professor Goals 3 Overview of Today s Talk 4 Define family-centered
The practice of medicine is a team sport and no. How to Manage Family-Centered Rounds. family-centered rounds
 How to Manage Family-Centered Rounds Jeremy Kern, MD, Anna Gay, MD, and Vineeta Mittal, MD, MBA Abstract Objective: To present a model for operationalizing successful family-centered rounds (FCRs). Methods:
How to Manage Family-Centered Rounds Jeremy Kern, MD, Anna Gay, MD, and Vineeta Mittal, MD, MBA Abstract Objective: To present a model for operationalizing successful family-centered rounds (FCRs). Methods:
The Challenges and Strategies to Improve Family-centered Round: A Literature Review
 : A Literature Review Reni Sulung Utami, S.Kep., M.Sc, RN 1 The importance of family-centered care and the role of families in decision making are becoming more recognized today. Several studies have supported
: A Literature Review Reni Sulung Utami, S.Kep., M.Sc, RN 1 The importance of family-centered care and the role of families in decision making are becoming more recognized today. Several studies have supported
PATIENT EXPERIENCE A UNIVERSAL TRUTH
 PATIENT EXPERIENCE A UNIVERSAL TRUTH T I F F A N Y C H R I S T E N S E N - P E R S O N / P A T I E N T J O A N N E W A T S O N - P E R S O N / P H Y S I C I A N IN OUR SESSION, ATTENDEES WILL HAVE OPPORTUNITIES
PATIENT EXPERIENCE A UNIVERSAL TRUTH T I F F A N Y C H R I S T E N S E N - P E R S O N / P A T I E N T J O A N N E W A T S O N - P E R S O N / P H Y S I C I A N IN OUR SESSION, ATTENDEES WILL HAVE OPPORTUNITIES
PATIENT EXPERIENCE A UNIVERSAL TRUTH
 PATIENT EXPERIENCE A UNIVERSAL TRUTH T I F F A N Y C H R I S T E N S E N - P E R S O N / P A T I E N T J O A N N E W A T S O N - P E R S O N / P H Y S I C I A N IN OUR SESSION, ATTENDEES WILL HAVE OPPORTUNITIES
PATIENT EXPERIENCE A UNIVERSAL TRUTH T I F F A N Y C H R I S T E N S E N - P E R S O N / P A T I E N T J O A N N E W A T S O N - P E R S O N / P H Y S I C I A N IN OUR SESSION, ATTENDEES WILL HAVE OPPORTUNITIES
NURSING SPECIAL REPORT
 2017 Press Ganey Nursing Special Report The Influence of Nurse Manager Leadership on Patient and Nurse Outcomes and the Mediating Effects of the Nurse Work Environment Nurse managers exert substantial
2017 Press Ganey Nursing Special Report The Influence of Nurse Manager Leadership on Patient and Nurse Outcomes and the Mediating Effects of the Nurse Work Environment Nurse managers exert substantial
McGill University. Academic Pediatrics Fellowship Program. Program Description And Learning Objectives
 McGill University Academic Pediatrics Fellowship Program Program Description And Learning Objectives Updated May 2018 Introduction: The Pediatrics Residency Program of McGill University offers advanced
McGill University Academic Pediatrics Fellowship Program Program Description And Learning Objectives Updated May 2018 Introduction: The Pediatrics Residency Program of McGill University offers advanced
Bedside Teaching Creating Competent Physicians
 Bedside Teaching Creating Competent Physicians "The student begins with the patient, continues with the patient and ends his studies with the patient, using books and lectures as tools as means to an end
Bedside Teaching Creating Competent Physicians "The student begins with the patient, continues with the patient and ends his studies with the patient, using books and lectures as tools as means to an end
Back to the Bedside: A Primer on Effective Walk Rounds
 Back to the Bedside: A Primer on Effective Walk Rounds Maggie Benson, MD Vikram Krishnasamy, MD Melissa McNeil, MD Shanta Zimmer, MD What do YOU want to learn today? By a show of hands: Who leads walk
Back to the Bedside: A Primer on Effective Walk Rounds Maggie Benson, MD Vikram Krishnasamy, MD Melissa McNeil, MD Shanta Zimmer, MD What do YOU want to learn today? By a show of hands: Who leads walk
CAPE/COP Educational Outcomes (approved 2016)
 CAPE/COP Educational Outcomes (approved 2016) Educational Outcomes Domain 1 Foundational Knowledge 1.1. Learner (Learner) - Develop, integrate, and apply knowledge from the foundational sciences (i.e.,
CAPE/COP Educational Outcomes (approved 2016) Educational Outcomes Domain 1 Foundational Knowledge 1.1. Learner (Learner) - Develop, integrate, and apply knowledge from the foundational sciences (i.e.,
Family-Centered Rounds in the Neonatal Intensive Care Unit
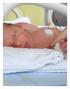 Family-Centered Rounds in the Neonatal Intensive Care Unit Gail M. Harris rs ris In neonatal intensive care units (NICUs) across the nation, true collaboration and shared decision-making with families
Family-Centered Rounds in the Neonatal Intensive Care Unit Gail M. Harris rs ris In neonatal intensive care units (NICUs) across the nation, true collaboration and shared decision-making with families
Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities
 Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities Richard J. Chung, MD Joan Jasien, MD Gary R. Maslow, MD, MPH ABSTRACT
Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities Richard J. Chung, MD Joan Jasien, MD Gary R. Maslow, MD, MPH ABSTRACT
The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults
 The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults Anna Podolsky, AB David T. Stern, MD, PhD Lauren Peccoralo, MD, MPH Abstract Background Communication and courtesy are important
The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults Anna Podolsky, AB David T. Stern, MD, PhD Lauren Peccoralo, MD, MPH Abstract Background Communication and courtesy are important
Running head: LEADERSHIP ANALYSIS: ROUNDING 1
 Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
Running head: LEADERSHIP ANALYSIS: ROUNDING 1 Leadership Analysis: Rounding Jerrene Bramble, Tara Braun, Pamela Dusseau, Angelique Kinyon, William McKinley, Noranne Morin, Nicky Reed, and Ashleigh Wash
Summary of Evidence Family Participation in Rounds
 Summary of Evidence Family Participation in Rounds By Judy E. Davidson DNP, CNS, RN, Nancy L. Falk, PhD, MBA, RN, Pat Kleba, MSN, and Jan Bull, MPA The foundational concept of family-centered care can
Summary of Evidence Family Participation in Rounds By Judy E. Davidson DNP, CNS, RN, Nancy L. Falk, PhD, MBA, RN, Pat Kleba, MSN, and Jan Bull, MPA The foundational concept of family-centered care can
COMBINED INTERNAL MEDICINE & PEDIATRICS Department of Medicine, Department of Pediatrics SCOPE OF PRACTICE PGY-1 PGY-4
 Definition and Scope of Specialty The Internal Medicine/Pediatrics residency program is a voluntary component in the continuum of the educational process of physician training; such training may take place
Definition and Scope of Specialty The Internal Medicine/Pediatrics residency program is a voluntary component in the continuum of the educational process of physician training; such training may take place
Assessing Resident Competency in an Outpatient Setting
 178 March 2004 Family Medicine Assessing Resident Competency in an Outpatient Setting Andrea L. Wendling, MD Background and Objectives: The Grand Rapids Family Practice Residency Program has been using
178 March 2004 Family Medicine Assessing Resident Competency in an Outpatient Setting Andrea L. Wendling, MD Background and Objectives: The Grand Rapids Family Practice Residency Program has been using
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP)
 BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
BUILDING BLOCKS OF PRIMARY CARE ASSESSMENT FOR TRANSFORMING TEACHING PRACTICES (BBPCA-TTP) DIRECTIONS FOR COMPLETING THE SURVEY This survey is designed to assess the organizational change of a primary
Approximately 180,000 patients die annually in the
 PRACTICE IMPROVEMENT SITUATION, BACKGROUND, ASSESSMENT, AND RECOMMENDATION GUIDED HUDDLES IMPROVE COMMUNICATION AND TEAMWORK IN THE EMERGENCY DEPARTMENT Authors: Heather A. Martin, DNP, RN, PNP-BC, and
PRACTICE IMPROVEMENT SITUATION, BACKGROUND, ASSESSMENT, AND RECOMMENDATION GUIDED HUDDLES IMPROVE COMMUNICATION AND TEAMWORK IN THE EMERGENCY DEPARTMENT Authors: Heather A. Martin, DNP, RN, PNP-BC, and
The Intimidation Factor:
 The Intimidation Factor: Workplace intimidation and its effects on wellness, morale, and patient care Disclosure Amanda Chavez, MD, UT Health SA, UHS has no relationships with commercial companies to disclose.
The Intimidation Factor: Workplace intimidation and its effects on wellness, morale, and patient care Disclosure Amanda Chavez, MD, UT Health SA, UHS has no relationships with commercial companies to disclose.
Setting: Emergency departments are high-risk contexts; they are over-crowded and
 QUALITY IMPROVEMENT STUDENT PROJECT PROPOSAL: IMPROVING HANDOFFS IN SAN FRANCISCO GENERAL HOSPTITAL S EMERGENCY DEPARTMENT TMIT Student Projects QuickStart Package 1. BACKGROUND Setting: Emergency departments
QUALITY IMPROVEMENT STUDENT PROJECT PROPOSAL: IMPROVING HANDOFFS IN SAN FRANCISCO GENERAL HOSPTITAL S EMERGENCY DEPARTMENT TMIT Student Projects QuickStart Package 1. BACKGROUND Setting: Emergency departments
Patient Payment Check-Up
 Patient Payment Check-Up SURVEY REPORT 2017 Attitudes and behavior among those billing for healthcare and those paying for it CONDUCTED BY 2017 Patient Payment Check-Up Report 1 Patient demand is ahead
Patient Payment Check-Up SURVEY REPORT 2017 Attitudes and behavior among those billing for healthcare and those paying for it CONDUCTED BY 2017 Patient Payment Check-Up Report 1 Patient demand is ahead
School of Nursing Applying Evidence to Improve Quality
 Applying Evidence to Improve Quality Linda A Dudjak PhD RN Associate Professor University of Pittsburgh School of Nursing Compare Two Alternatives Implement a Test of Change (Experiment) to Fix a Broken
Applying Evidence to Improve Quality Linda A Dudjak PhD RN Associate Professor University of Pittsburgh School of Nursing Compare Two Alternatives Implement a Test of Change (Experiment) to Fix a Broken
13th Annual Meridian Nursing Research and Evidence Based Practice Conference 2017 General Guidelines for Abstract Submission
 Hackensack Meridian Ann May Center for Nursing 13 th Annual Meridian Nursing Research and Evidence Based Practice Conference Instructions for Submission All author information and abstract contents must
Hackensack Meridian Ann May Center for Nursing 13 th Annual Meridian Nursing Research and Evidence Based Practice Conference Instructions for Submission All author information and abstract contents must
PFAC as Consultant to Hospital Initiatives
 4th Annual Patient and Family Advisory Council Conference Strengthening Patient and Family Engagement in Massachusetts Hospitals PFAC as Consultant to Hospital Initiatives Lois Erhartic, Colleen McCauley,
4th Annual Patient and Family Advisory Council Conference Strengthening Patient and Family Engagement in Massachusetts Hospitals PFAC as Consultant to Hospital Initiatives Lois Erhartic, Colleen McCauley,
Text-based Document. Developing Cultural Competence in Practicing Nurses: A Qualitative Inquiry. Edmonds, Michelle L.
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Recent changes in the delivery and financing of health
 OUTCOMES IN PRACTICE Improving Physician Satisfaction on an Academic General Medical Service Robert C. Goldszer, MD, MBA, James S. Winshall, MD, Monte Brown, MD, Shelley Hurwitz, PhD, Nancy Lee Masaschi,
OUTCOMES IN PRACTICE Improving Physician Satisfaction on an Academic General Medical Service Robert C. Goldszer, MD, MBA, James S. Winshall, MD, Monte Brown, MD, Shelley Hurwitz, PhD, Nancy Lee Masaschi,
Text-based Document. Authors Alichnie, M. Christine; Miller, Joan F. Downloaded 20-Jun :02:04.
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Pediatric Nurse Buddy Program Cohort 3 The impact of EMR on Healthcare Provider Wellness
 Pediatric Nurse Buddy Program Cohort 3 The impact of EMR on Healthcare Provider Wellness Disclosure Kayeleigh Higgerson, DO, UT Health SA, UHS has no relationships with commercial companies to disclose.
Pediatric Nurse Buddy Program Cohort 3 The impact of EMR on Healthcare Provider Wellness Disclosure Kayeleigh Higgerson, DO, UT Health SA, UHS has no relationships with commercial companies to disclose.
Improving patient satisfaction by adding a physician in triage
 ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
ORIGINAL ARTICLE Improving patient satisfaction by adding a physician in triage Jason Imperato 1, Darren S. Morris 2, Leon D. Sanchez 2, Gary Setnik 1 1. Department of Emergency Medicine, Mount Auburn
Infectious Diseases Elective PL1 Residents
 PL1 Residents The elective rotation for residents in Pediatric Infectious Disease provides a broad learning experience for residents at all levels of training through provision of care for children requiring
PL1 Residents The elective rotation for residents in Pediatric Infectious Disease provides a broad learning experience for residents at all levels of training through provision of care for children requiring
PG snapshot Nursing Special Report. The Role of Workplace Safety and Surveillance Capacity in Driving Nurse and Patient Outcomes
 PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
No Hablo Inglés: Emergency Department Experiences of Spanish-Speaking Patients
 No Hablo Inglés: Emergency Department Experiences of Spanish-Speaking Patients Team Members: Dr. Arlene Steckel RN, PhD, CPNP Danielle Bellucci RN, BSN, CEN Julie Mount RN, MS, FNP-BC, CEN, CPEN Dawn Hueber
No Hablo Inglés: Emergency Department Experiences of Spanish-Speaking Patients Team Members: Dr. Arlene Steckel RN, PhD, CPNP Danielle Bellucci RN, BSN, CEN Julie Mount RN, MS, FNP-BC, CEN, CPEN Dawn Hueber
Plan of Attack. Ambulatory Care and Education 3/19/2014. X+Y Scheduling Models for Residency Training Programs
 Plan of Attack X+Y Scheduling Models for Residency Training Programs Marc Shalaby, MD FACP Perelman School of Medicine at the University of Pennsylvania University at Buffalo Department of Pediatrics-Grand
Plan of Attack X+Y Scheduling Models for Residency Training Programs Marc Shalaby, MD FACP Perelman School of Medicine at the University of Pennsylvania University at Buffalo Department of Pediatrics-Grand
COPIC Objectives and Expectations
 COPIC Objectives and Expectations Goals: 1. Familiarize residents with how the state s medical malpractice insurer functions 2. Gain knowledge of process of malpractice claims work 3. Understand the most
COPIC Objectives and Expectations Goals: 1. Familiarize residents with how the state s medical malpractice insurer functions 2. Gain knowledge of process of malpractice claims work 3. Understand the most
Advocate Health Care Contact Hours for Continuing Nursing Education The Healthy Steps Interactive Multimedia Training and Resource Kit and The
 Advocate Health Care Contact Hours for Continuing Nursing Education The Healthy Steps Interactive Multimedia Training and Resource Kit and The Healthy Steps Interactive Multimedia Training and Resource
Advocate Health Care Contact Hours for Continuing Nursing Education The Healthy Steps Interactive Multimedia Training and Resource Kit and The Healthy Steps Interactive Multimedia Training and Resource
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Results tell the story
 Sponsor: Discover why leaders at 1400+ hospitals have made this webinar series the #1 HCAHPS education program in America! Results tell the story Webinar Series Faculty: Brian Lee, CSP Founder of CLS David
Sponsor: Discover why leaders at 1400+ hospitals have made this webinar series the #1 HCAHPS education program in America! Results tell the story Webinar Series Faculty: Brian Lee, CSP Founder of CLS David
QAPI Making An Improvement
 Preparing for the Future QAPI Making An Improvement Charlene Ross, MSN, MBA, RN Objectives Describe how to use lessons learned from implementing the comfortable dying measure to improve your care Use the
Preparing for the Future QAPI Making An Improvement Charlene Ross, MSN, MBA, RN Objectives Describe how to use lessons learned from implementing the comfortable dying measure to improve your care Use the
Improving Intimate Partner Violence Screening in the Emergency Department Setting
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Analysis of a Clinical Evaluation Tool Teresa Connolly, PhD, RN, CNRN Brenda Owen, MSN, CNM, RN Glenda Robertson, MA, RN Joan Ward, MS, RN, CNE
 HEADLINE Analysis of a Clinical Evaluation Tool Teresa Connolly, PhD, RN, CNRN Brenda Owen, MSN, CNM, RN Glenda Robertson, MA, RN Joan Ward, MS, RN, CNE Session Disclosure 1. Approval Statement: This continuing
HEADLINE Analysis of a Clinical Evaluation Tool Teresa Connolly, PhD, RN, CNRN Brenda Owen, MSN, CNM, RN Glenda Robertson, MA, RN Joan Ward, MS, RN, CNE Session Disclosure 1. Approval Statement: This continuing
Hospital pharmacists play an important role in improving
 CLINICAL PRACTICE The Invisible White Coat: Awareness of Pharmacists in a Neonatal Intensive Care Unit Rehana Bajwa, Jennifer G Kendrick, and Roxane Carr NTRODUCTION Hospital pharmacists play an important
CLINICAL PRACTICE The Invisible White Coat: Awareness of Pharmacists in a Neonatal Intensive Care Unit Rehana Bajwa, Jennifer G Kendrick, and Roxane Carr NTRODUCTION Hospital pharmacists play an important
Employers are essential partners in monitoring the practice
 Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
Jackie Loversidge, PhD, RNC-AWHC Assistant Professor of Clinical Nursing The Ohio State University College of Nursing
 Jackie Loversidge, PhD, RNC-AWHC Assistant Professor of Clinical Nursing The Ohio State University College of Nursing Examine strategies for overcoming barriers to interprofessional collaboration: The
Jackie Loversidge, PhD, RNC-AWHC Assistant Professor of Clinical Nursing The Ohio State University College of Nursing Examine strategies for overcoming barriers to interprofessional collaboration: The
Collaborative Care in Pediatric Mental Health: A Qualitative Case Study
 Collaborative Care in Pediatric Mental Health: A Qualitative Case Study Megan McLeod, M.D. Supervised by Sourav Sengupta, M.D., M.P.H. March 3 rd, 2017 Acknowledgements Thank you Dr. Sengupta Outline 1.
Collaborative Care in Pediatric Mental Health: A Qualitative Case Study Megan McLeod, M.D. Supervised by Sourav Sengupta, M.D., M.P.H. March 3 rd, 2017 Acknowledgements Thank you Dr. Sengupta Outline 1.
Oh No! I need to write an abstract! How do I start?
 Oh No! I need to write an abstract! How do I start? Why is it hard to write an abstract? Fear / anxiety about the writing process others reading what you wrote Takes time / feel overwhelmed Commits you
Oh No! I need to write an abstract! How do I start? Why is it hard to write an abstract? Fear / anxiety about the writing process others reading what you wrote Takes time / feel overwhelmed Commits you
More than 60% of elective surgery
 Benefits of Preoperative Education for Adult Elective Surgery Patients NANCY KRUZIK, MSN, RN, CNOR More than 60% of elective surgery procedures in the United States were being performed as outpatient procedures
Benefits of Preoperative Education for Adult Elective Surgery Patients NANCY KRUZIK, MSN, RN, CNOR More than 60% of elective surgery procedures in the United States were being performed as outpatient procedures
Meeting Joint Commission Standards for Health Literacy. Communication and Health Care. Multiple Players in Communication
 Meeting Joint Commission Standards for Health Literacy Christina L. Cordero, PhD, MPH Project Manager Division of Standards and Survey Methods The Joint Commission Wisconsin Literacy SW/SC Regional Health
Meeting Joint Commission Standards for Health Literacy Christina L. Cordero, PhD, MPH Project Manager Division of Standards and Survey Methods The Joint Commission Wisconsin Literacy SW/SC Regional Health
Abstract Development:
 Abstract Development: How to write an abstract Fall 2017 Sara E. Dolan Looby, PhD, ANP-BC, FAAN Assistant Professor of Medicine, Harvard Medical School Neuroendocrine Unit/Program in Nutritional Metabolism
Abstract Development: How to write an abstract Fall 2017 Sara E. Dolan Looby, PhD, ANP-BC, FAAN Assistant Professor of Medicine, Harvard Medical School Neuroendocrine Unit/Program in Nutritional Metabolism
Clinical Research: Neonatal Nurses' Perception and Experiences. [Name of the writer] [Name of the institution]
![Clinical Research: Neonatal Nurses' Perception and Experiences. [Name of the writer] [Name of the institution] Clinical Research: Neonatal Nurses' Perception and Experiences. [Name of the writer] [Name of the institution]](/thumbs/71/66083811.jpg) CLINICAL RESEARCH 1 Clinical Research: Neonatal Nurses' Perception and Experiences [Name of the writer] [Name of the institution] CLINICAL RESEARCH 2 Clinical Research: Neonatal Nurses' Perception and
CLINICAL RESEARCH 1 Clinical Research: Neonatal Nurses' Perception and Experiences [Name of the writer] [Name of the institution] CLINICAL RESEARCH 2 Clinical Research: Neonatal Nurses' Perception and
Rounds Today: A Qualitative Study of Internal Medicine and Pediatrics Resident Perceptions
 Rounds Today: A Qualitative Study of Internal Medicine and Pediatrics Resident Perceptions Raphael Rabinowitz, BA Jeanne Farnan, MD, MHPE Oliver Hulland, BA, BFA Lisa Kearns, MD, MS ABSTRACT Michele Long,
Rounds Today: A Qualitative Study of Internal Medicine and Pediatrics Resident Perceptions Raphael Rabinowitz, BA Jeanne Farnan, MD, MHPE Oliver Hulland, BA, BFA Lisa Kearns, MD, MS ABSTRACT Michele Long,
The role of end. shift verbal handover. of-shift
 The role of end end-of of-shift shift verbal handover Student - Ms. Antoinette David Supervisor- Prof. Eleanor Holroyd Supervisor- Dr. Mervyn Jackson Supervisor- Dr. Heather Pisani Australian Commission
The role of end end-of of-shift shift verbal handover Student - Ms. Antoinette David Supervisor- Prof. Eleanor Holroyd Supervisor- Dr. Mervyn Jackson Supervisor- Dr. Heather Pisani Australian Commission
AF4Q and TCAB: An Introduction
 AF4Q and TCAB: An Introduction July 13, 2011 Ellen Interlandi, MHM, RN, NE-BC Patricia Montoya, MPA, BSN 1 What is Aligning Forces for Quality? An unprecedented commitment by the Robert Wood Johnson Foundation
AF4Q and TCAB: An Introduction July 13, 2011 Ellen Interlandi, MHM, RN, NE-BC Patricia Montoya, MPA, BSN 1 What is Aligning Forces for Quality? An unprecedented commitment by the Robert Wood Johnson Foundation
Table of Contents. TeamSTEPPS Framework and Competencies Key Principles. Team Structure Multi-Team System For Patient Care
 Table of Contents TeamSTEPPS Framework and Competencies Key Principles Team Structure Multi-Team System For Patient Care Leadership Effective Team Leaders Team Events Brief Checklist Debrief Checklist
Table of Contents TeamSTEPPS Framework and Competencies Key Principles Team Structure Multi-Team System For Patient Care Leadership Effective Team Leaders Team Events Brief Checklist Debrief Checklist
A Qualitative Study of Master Patient Index (MPI) Record Challenges from Health Information Management Professionals Perspectives
 A Qualitative Study of Master Patient Index (MPI) Record Challenges from Health Information Management Professionals Perspectives by Joe Lintz, MS, RHIA Abstract This study aimed gain a better understanding
A Qualitative Study of Master Patient Index (MPI) Record Challenges from Health Information Management Professionals Perspectives by Joe Lintz, MS, RHIA Abstract This study aimed gain a better understanding
Missed Nursing Care: Errors of Omission
 Missed Nursing Care: Errors of Omission Beatrice Kalisch, PhD, RN, FAAN Titus Professor of Nursing and Chair University of Michigan Nursing Business and Health Systems Presented at the NDNQI annual meeting
Missed Nursing Care: Errors of Omission Beatrice Kalisch, PhD, RN, FAAN Titus Professor of Nursing and Chair University of Michigan Nursing Business and Health Systems Presented at the NDNQI annual meeting
Pediatric Residents. A Guide to Evaluating Your Clinical Competence. THE AMERICAN BOARD of PEDIATRICS
 2017 Pediatric Residents A Guide to Evaluating Your Clinical Competence THE AMERICAN BOARD of PEDIATRICS Published and distributed by The American Board of Pediatrics 111 Silver Cedar Court Chapel Hill,
2017 Pediatric Residents A Guide to Evaluating Your Clinical Competence THE AMERICAN BOARD of PEDIATRICS Published and distributed by The American Board of Pediatrics 111 Silver Cedar Court Chapel Hill,
Pediatric Cardiology Rotation PL-1 Residents
 PL-1 Residents The Pediatric Cardiology elective is available to residents of all levels and combines both outpatient and inpatient clinical experiences. In the outpatient setting, residents will work-up
PL-1 Residents The Pediatric Cardiology elective is available to residents of all levels and combines both outpatient and inpatient clinical experiences. In the outpatient setting, residents will work-up
A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing
 BRIEF REPORT A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing Sara Kohlbeck, MPH; Brenna Akert, BS; Caroline Pace, MD; Amy Zosel, MD, MSCS ABSTRACT
BRIEF REPORT A Multistep Approach to Address Clinician Knowledge, Attitudes, and Behavior Around Opioid Prescribing Sara Kohlbeck, MPH; Brenna Akert, BS; Caroline Pace, MD; Amy Zosel, MD, MSCS ABSTRACT
8/31/2015. Session C719 Outcomes of a Study Addressing Challenges in APRN Practice and Strategies for Success. Vanderbilt University Medical Center
 Session C719 Outcomes of a Study Addressing Challenges in APRN Practice and Strategies for Success Marilyn A. Dubree, MSN, RN, NE-BC Executive Chief Nursing Officer Vanderbilt University Medical Center
Session C719 Outcomes of a Study Addressing Challenges in APRN Practice and Strategies for Success Marilyn A. Dubree, MSN, RN, NE-BC Executive Chief Nursing Officer Vanderbilt University Medical Center
6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step
 6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step Abstract In the current model of health care delivery, the primary care physician works alone
6/5/2013 7:22:00 AM Building Teams at the Associates in Internal Medicine: The Medical Huddle as a First Step Abstract In the current model of health care delivery, the primary care physician works alone
Using Secondary Datasets for Research. Learning Objectives. What Do We Mean By Secondary Data?
 Using Secondary Datasets for Research José J. Escarce January 26, 2015 Learning Objectives Understand what secondary datasets are and why they are useful for health services research Become familiar with
Using Secondary Datasets for Research José J. Escarce January 26, 2015 Learning Objectives Understand what secondary datasets are and why they are useful for health services research Become familiar with
ROTATION DESCRIPTION FORM PGY1
 ROTATION DESCRIPTION FORM PGY1 Rotation Title Medicine Intensive Care Unit (MICU) Level of Learner PY4 PGY1 PGY2 Preceptor(s) Stacy Campbell-Bright, Brian Murray Preceptor Contact Stacy.Campbell-Bright@unchealth.unc.edu;
ROTATION DESCRIPTION FORM PGY1 Rotation Title Medicine Intensive Care Unit (MICU) Level of Learner PY4 PGY1 PGY2 Preceptor(s) Stacy Campbell-Bright, Brian Murray Preceptor Contact Stacy.Campbell-Bright@unchealth.unc.edu;
CDU. Clinical Decision Unit Ward for
 CDU Clinical Decision Unit Ward for Can t Observational Decide Medicine Unit What are observation medicine units? Observation medicine delivers intensive shortterm assessment, observation or therapy to
CDU Clinical Decision Unit Ward for Can t Observational Decide Medicine Unit What are observation medicine units? Observation medicine delivers intensive shortterm assessment, observation or therapy to
Creating An Effective Learning Environment. Lynne Yong Ee Lin, Ph.D. Licensed Clinical Psychologist Penang Adventist Hospital
 Creating An Effective Learning Environment Lynne Yong Ee Lin, Ph.D. Licensed Clinical Psychologist Penang Adventist Hospital Introduction HEALTHCARE TRAINING = APPRENTICESHIP Requires hands-on practical
Creating An Effective Learning Environment Lynne Yong Ee Lin, Ph.D. Licensed Clinical Psychologist Penang Adventist Hospital Introduction HEALTHCARE TRAINING = APPRENTICESHIP Requires hands-on practical
Original Research PRACTICE-BASED RESEARCH
 Patient-perceived value of Medication Therapy Management (MTM) services: a series of focus groups Heidi Schultz, PharmD 1 ; Sarah M. Westberg, PharmD, BCPS 2 ; Djenane Ramalho de Oliveira, PhD 1 ; and
Patient-perceived value of Medication Therapy Management (MTM) services: a series of focus groups Heidi Schultz, PharmD 1 ; Sarah M. Westberg, PharmD, BCPS 2 ; Djenane Ramalho de Oliveira, PhD 1 ; and
Communication Skills Training Curriculum for Pulmonary and Critical Care Fellows
 Online Data Supplement Communication Skills Training Curriculum for Pulmonary and Critical Care Fellows Jennifer W. McCallister, MD, Jillian Gustin, MD, Sharla Wells-Di Gregorio, PhD, David P. Way, MEd,
Online Data Supplement Communication Skills Training Curriculum for Pulmonary and Critical Care Fellows Jennifer W. McCallister, MD, Jillian Gustin, MD, Sharla Wells-Di Gregorio, PhD, David P. Way, MEd,
Course Title FUNCTIONAL ASSESSMENT OF PATIENTS WITH CARDIOVASCULAR DISEASES
 Course Title FUNCTIONAL ASSESSMENT OF PATIENTS WITH CARDIOVASCULAR DISEASES Director Judith Regensteiner, Ph.D., Professor of Medicine Director, Clinical Treadmill Laboratory, UCHSC Background & Objectives
Course Title FUNCTIONAL ASSESSMENT OF PATIENTS WITH CARDIOVASCULAR DISEASES Director Judith Regensteiner, Ph.D., Professor of Medicine Director, Clinical Treadmill Laboratory, UCHSC Background & Objectives
Children s Memorial Hermann Hospital Child Life Internship Information
 Children s Memorial Hermann Hospital Child Life Internship Information Child Life Mission Statement: We, as Child Life professionals, strive to reduce the impact of stressful or traumatic life events and
Children s Memorial Hermann Hospital Child Life Internship Information Child Life Mission Statement: We, as Child Life professionals, strive to reduce the impact of stressful or traumatic life events and
PEC GENERAL PEDIATRIC HOSPITALIST ELECTIVE
 PEC GENERAL PEDIATRIC HOSPITALIST ELECTIVE Rotation Director Jennifer Everhart, MD Introduction Welcome to the General Pediatric Hospitalist Elective at PEC! We are excited to have you join us! At the
PEC GENERAL PEDIATRIC HOSPITALIST ELECTIVE Rotation Director Jennifer Everhart, MD Introduction Welcome to the General Pediatric Hospitalist Elective at PEC! We are excited to have you join us! At the
December 16, Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC
 Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
Pharmacists in Transitions of Care: We Can All Make a Difference
 Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Preceptor Orientation 1. Department of Nursing & Allied Health RN to BSN Program. Preceptor Orientation Program
 Preceptor Orientation 1 Department of Nursing & Allied Health RN to BSN Program Preceptor Orientation Program Revised February 2014 Preceptor Orientation 2 The faculty and staff of SUNY Delhi s RN to BSN
Preceptor Orientation 1 Department of Nursing & Allied Health RN to BSN Program Preceptor Orientation Program Revised February 2014 Preceptor Orientation 2 The faculty and staff of SUNY Delhi s RN to BSN
Define the PCMH and where residents fit in
 If We Build It, Will They Come? Michael J. Rosenblum, MD, FACP Orlando Torres, MD, MS Baystate Medical Center/Tufts Univ. SOM Workshop Session III 1:30 to 3:00 p.m. Wednesday, April 28, 2010. Educational
If We Build It, Will They Come? Michael J. Rosenblum, MD, FACP Orlando Torres, MD, MS Baystate Medical Center/Tufts Univ. SOM Workshop Session III 1:30 to 3:00 p.m. Wednesday, April 28, 2010. Educational
EHR Implementation Best Practices. EHR White Paper
 EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
Building a Smarter Healthcare System The IE s Role. Kristin H. Goin Service Consultant Children s Healthcare of Atlanta
 Building a Smarter Healthcare System The IE s Role Kristin H. Goin Service Consultant Children s Healthcare of Atlanta 2 1 Background 3 Industrial Engineering The objective of Industrial Engineering is
Building a Smarter Healthcare System The IE s Role Kristin H. Goin Service Consultant Children s Healthcare of Atlanta 2 1 Background 3 Industrial Engineering The objective of Industrial Engineering is
Staffing Your TB Program
 TB Program Management San Antonio, Texas November 5-7, 2008 Staffing Your TB Program Lynelle Phillips, RN, MPH November 6, 2008 Staffing Your TB Program Lynelle Phillips RN MPH Program Manager s Course
TB Program Management San Antonio, Texas November 5-7, 2008 Staffing Your TB Program Lynelle Phillips, RN, MPH November 6, 2008 Staffing Your TB Program Lynelle Phillips RN MPH Program Manager s Course
1 - ICU EVALUATION. inconsistently synthesizes accurate, thorough histories, exams, and data to diagnose critically ill patients
 - ICU EVALUATION NOTE: LEVEL behaviors constitute critical deficiencies. Most beginning R's will be at level. Most R' will be at LEVELS -4. Graduating R's should be at LEVEL 4 across most subcompetencies.
- ICU EVALUATION NOTE: LEVEL behaviors constitute critical deficiencies. Most beginning R's will be at level. Most R' will be at LEVELS -4. Graduating R's should be at LEVEL 4 across most subcompetencies.
Optimizing Workflow with Technology and Design. Ashleigh George RN, BSN Susan Stiles RN, MHA MBA
 Optimizing Workflow with Technology and Design Ashleigh George RN, BSN Susan Stiles RN, MHA MBA December 30, 2011 Objectives Describe automating and integrating medical devices into the clinical practice
Optimizing Workflow with Technology and Design Ashleigh George RN, BSN Susan Stiles RN, MHA MBA December 30, 2011 Objectives Describe automating and integrating medical devices into the clinical practice
Piloting a Lay Navigation Program in a Community and Academic Jean B. Sellers, RN, MSN Administrative Clinical Director UNC Lineberger Comprehensive
 Piloting a Lay Navigation Program in a Community and Academic Jean B. Sellers, RN, MSN Administrative Clinical Director UNC Lineberger Comprehensive Cancer Center Chapel Hill, NC State of Navigation Today
Piloting a Lay Navigation Program in a Community and Academic Jean B. Sellers, RN, MSN Administrative Clinical Director UNC Lineberger Comprehensive Cancer Center Chapel Hill, NC State of Navigation Today
An Assessment of Community Health Centers Involvement in Health Professions and Residency Training: A Chartbook
 An Assessment of Community Health Centers Involvement in Health Professions and Residency Training: A Chartbook National Association of Community Health Centers, 2011 For more information, email research@nachc.com.
An Assessment of Community Health Centers Involvement in Health Professions and Residency Training: A Chartbook National Association of Community Health Centers, 2011 For more information, email research@nachc.com.
Experiential Education
 Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
Experiential Education Experiential Education Page 1 Experiential Education Contents Introduction to Experiential Education... 3 Experiential Education Calendar... 4 Selected ACPE Standards 2007... 5 Standard
University of Michigan Emergency Department
 University of Michigan Emergency Department Efficient Patient Placement in the Emergency Department Final Report To: Jon Fairchild, M.S., R.N. C.E.N, Nurse Manager, fairchil@med.umich.edu Samuel Clark,
University of Michigan Emergency Department Efficient Patient Placement in the Emergency Department Final Report To: Jon Fairchild, M.S., R.N. C.E.N, Nurse Manager, fairchil@med.umich.edu Samuel Clark,
For 1 hour every week my colleagues and I sit down together over lunch to discuss
 January/February 2000 Volume 3 Number 1 EFFECTIVE CLINICAL PRACTICE EDITOR H. GILBERT WELCH, MD, MPH ASSOCIATE EDITORS JOHN D. BIRKMEYER, MD WILLIAM C. BLACK, MD LISA M. SCHWARTZ, MD, MS STEVEN WOLOSHIN,
January/February 2000 Volume 3 Number 1 EFFECTIVE CLINICAL PRACTICE EDITOR H. GILBERT WELCH, MD, MPH ASSOCIATE EDITORS JOHN D. BIRKMEYER, MD WILLIAM C. BLACK, MD LISA M. SCHWARTZ, MD, MS STEVEN WOLOSHIN,
Barriers to Participation in Continuing Nursing Educational Programs among Registered Nurses in Maharashtra
 Barriers to Participation in Continuing Nursing Educational Programs among Registered Nurses in Maharashtra Mahadeo Shinde 1, Nutan Potdar 2, Sunil Kulkarni 3 1 Professor, Krishna Institute of Nursing
Barriers to Participation in Continuing Nursing Educational Programs among Registered Nurses in Maharashtra Mahadeo Shinde 1, Nutan Potdar 2, Sunil Kulkarni 3 1 Professor, Krishna Institute of Nursing
Starting with the End in Mind: UW Internal Medicine & the Next Accreditation System
 Starting with the End in Mind: UW Internal Medicine & the Next Accreditation System John H. Choe, MD, MPH Assoc. Program Director, UW Medicine Residency Dermatology Division Meeting September 13, 2013
Starting with the End in Mind: UW Internal Medicine & the Next Accreditation System John H. Choe, MD, MPH Assoc. Program Director, UW Medicine Residency Dermatology Division Meeting September 13, 2013
Conflicts of Interest Disclosure
 The Use of Innovative Educational Strategies to Increase Knowledge and Change Attitudes Regarding Children s Pain Marti Michel, MSN, RN, PCNS-BC, CPNP Kathy Haughan, MSN, RN, NE-BC Roberta Szumski, MSN,
The Use of Innovative Educational Strategies to Increase Knowledge and Change Attitudes Regarding Children s Pain Marti Michel, MSN, RN, PCNS-BC, CPNP Kathy Haughan, MSN, RN, NE-BC Roberta Szumski, MSN,
Clinical Research Proposal To the Jersey City Medical Center Institutional Review Board
 1 Clinical Research Proposal To the Jersey City Medical Center Institutional Review Board Principle Investigators: Erin Salmond BSN RN and Joanie Knuth RN BSN RN Date of Submission: Type of Proposal: Descriptive
1 Clinical Research Proposal To the Jersey City Medical Center Institutional Review Board Principle Investigators: Erin Salmond BSN RN and Joanie Knuth RN BSN RN Date of Submission: Type of Proposal: Descriptive
Revised Casey-Fink Nurse Retention Survey 2009 Kathy Casey and Regina Fink. All rights reserved.
 Revised Casey-Fink Nurse Retention Survey 2009 Kathy Casey and Regina Fink. All rights reserved. 1 I. Please answer each of the following questions by placing a mark inside the circles: DISAGREE DISAGREE
Revised Casey-Fink Nurse Retention Survey 2009 Kathy Casey and Regina Fink. All rights reserved. 1 I. Please answer each of the following questions by placing a mark inside the circles: DISAGREE DISAGREE
Inova Health System Office of Continuing Medical Education Application for Awarding Continuing Medical Education Credit for Regularly Scheduled Series
 Inova Health System Office of Continuing Medical Education Application for Awarding Continuing Medical Education Credit for Regularly Scheduled Series This application must be used to collect all of the
Inova Health System Office of Continuing Medical Education Application for Awarding Continuing Medical Education Credit for Regularly Scheduled Series This application must be used to collect all of the
Long Term Care Nurses Feelings on Communication, Teamwork and Stress in Long Term Care
 Long Term Care Nurses Feelings on Communication, Teamwork and Stress in Long Term Care Dr. Ronald M. Fuqua, Ph.D. Associate Professor of Health Care Management Clayton State University Author Note Correspondence
Long Term Care Nurses Feelings on Communication, Teamwork and Stress in Long Term Care Dr. Ronald M. Fuqua, Ph.D. Associate Professor of Health Care Management Clayton State University Author Note Correspondence
Qualitative Evidence for Practice: Why Not! Barbara Patterson, PhD, RN, ANEF Lehigh Valley Health Network Research Day 2016 October 28, 2016
 Qualitative Evidence for Practice: Why Not! Barbara Patterson, PhD, RN, ANEF Lehigh Valley Health Network Research Day 2016 October 28, 2016 OBJECTIVES At the completion of this presentation the learner
Qualitative Evidence for Practice: Why Not! Barbara Patterson, PhD, RN, ANEF Lehigh Valley Health Network Research Day 2016 October 28, 2016 OBJECTIVES At the completion of this presentation the learner
IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION
 IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION Kayla Eddins, BSN Honors Student Submitted to the School of Nursing in partial fulfillment of the requirements
IMPACT OF SIMULATION EXPERIENCE ON STUDENT PERFORMANCE DURING RESCUE HIGH FIDELITY PATIENT SIMULATION Kayla Eddins, BSN Honors Student Submitted to the School of Nursing in partial fulfillment of the requirements
MacPeds DAY FLOAT ROTATION OBJECTIVES
 MacPeds DAY FLOAT ROTATION OBJECTIVES The Royal College of Physicians and Surgeons of Canada has outlined the expectations for pediatric trainees. This rotation will enable residents to integrate many
MacPeds DAY FLOAT ROTATION OBJECTIVES The Royal College of Physicians and Surgeons of Canada has outlined the expectations for pediatric trainees. This rotation will enable residents to integrate many
Title: Training Residents in Behavioral Health Service Delivery in Primary Care: A Demonstration Project
 8716210 APPLICANT INFORMATION Applicant Name: Jeffrey Shahidullah Institution/School: Geisinger Health System Highest Degree Completed: PhD Position: Postdoc/Fellow If student, year in school: Are you
8716210 APPLICANT INFORMATION Applicant Name: Jeffrey Shahidullah Institution/School: Geisinger Health System Highest Degree Completed: PhD Position: Postdoc/Fellow If student, year in school: Are you
Developing a Curriculum in Patient Safety and Quality Improvement for Your Clerkship
 Developing a Curriculum in Patient Safety and Quality Improvement for Your Clerkship Diane Levine, Wayne State University Allison Heacock, The Ohio State University Amy Shaheen, University of North Carolina
Developing a Curriculum in Patient Safety and Quality Improvement for Your Clerkship Diane Levine, Wayne State University Allison Heacock, The Ohio State University Amy Shaheen, University of North Carolina
SPN NEWS. Column Editor: Dana Etzel-Hardman, MSN, MBA, RN, CPN
 SPN NEWS Column Editor: Dana Etzel-Hardman, MSN, MBA, RN, CPN Preparing Pediatric Nurses for the 21st Century: Perceptions of Nurse Managers, Nursing Faculty, and Staff Nurses Donna Miles Curry PhD, RN,
SPN NEWS Column Editor: Dana Etzel-Hardman, MSN, MBA, RN, CPN Preparing Pediatric Nurses for the 21st Century: Perceptions of Nurse Managers, Nursing Faculty, and Staff Nurses Donna Miles Curry PhD, RN,
OVERCOMING RESISTANCE TO RESILIENCY PROGRAMS: ONE STEP AT A TIME!
 OVERCOMING RESISTANCE TO RESILIENCY PROGRAMS: ONE STEP AT A TIME! CENTILE International Conference Washington DC, October 24, 2107 Emily Ratner, MD Director, Integrative Medicine Initiatives, MedStar Institute
OVERCOMING RESISTANCE TO RESILIENCY PROGRAMS: ONE STEP AT A TIME! CENTILE International Conference Washington DC, October 24, 2107 Emily Ratner, MD Director, Integrative Medicine Initiatives, MedStar Institute
A Roadmap for the Journey Home - A Supplemental Tool Guiding Patients from Hospital to Home
 The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-15-2017 A Roadmap
The University of San Francisco USF Scholarship: a digital repository @ Gleeson Library Geschke Center Master's Projects and Capstones Theses, Dissertations, Capstones and Projects Fall 12-15-2017 A Roadmap
Prior Assessed Learning (PAL) Application
 Prior Assessed Learning (PAL) Application 2 Identify your different work and life experiences which provide you with advanced knowledge and skills. The "job code" you assign to each experience will be
Prior Assessed Learning (PAL) Application 2 Identify your different work and life experiences which provide you with advanced knowledge and skills. The "job code" you assign to each experience will be
