Emergency Nursing Resource: Non-invasive Temperature Measurement in the Emergency Department
|
|
|
- Ferdinand Warren
- 6 years ago
- Views:
Transcription
1 Emergency Nursing Resource: Non-invasive Temperature Measurement in the Emergency Department What method of non-invasive body temperature measurement is the most accurate and precise for use in patients (newborn to adult) in the emergency department? Authored by the 2011 ENA Emergency Nursing Resources Development Committee: Susan Barnason, PhD, RN, APRN, CEN, CCRN, CNS, CS Jennifer Williams, MSN, RN, CEN, CCRN, CNS Jean Proehl, MN, RN, CEN, CPEN, FAEN Carla Brim, MN, RN, CEN, CNS Melanie Crowley, MSN, RN, CEN, MICN Sherry Leviner, MSN, RN, CEN Cathleen Lindauer, MSN, RN, CEN Mary Naccarato, MSN, RN, CEN, CCNS Andrew Storer, DNP, RN, ACNP, CRNP, FNP 2011 ENA Board of Directors Liaison: AnnMarie Papa, DNP, RN, CEN, NE-BC, FAEN ENA s Emergency Nursing Resources (ENRs) are developed by ENA members to provide emergency nurses with evidence-based information to utilize and implement in their care of emergency patients and families. Each ENR focuses on a clinical or practice-based issue, and is the result of a review and analysis of current information believed to be reliable. As such, information and recommendations within a particular ENR reflect the current scientific and clinical knowledge at the time of publication, are only current as of their publication date, and are subject to change without notice as advances emerge. In addition, variations in practice, which take into account the needs of the individual patient and the resources and limitations unique to the institution, may warrant approaches, treatments and/or procedures that differ from the recommendations outlined in the ENRs. Therefore, these recommendations should not be construed as dictating an exclusive course of management, treatment or care, nor does the use of such recommendations guarantee a particular outcome. ENRs are never intended to replace a practitioner s best nursing judgment based on the clinical circumstances of a particular patient or patient population. ENRs are published by ENA for educational and informational purposes only, and ENA does not approve or endorse any specific methods, practices, or sources of information. ENA assumes no liability for any injury and/or damage to persons or property arising out of or related to the use of or reliance on any ENR. Publication Date: December 2011 Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies.
2 Table of Contents Background/Significance... 1 Methodology... 1 Evidence Table and Other Resources... 2 Summary of Literature Review... 3 Description of Decision Options/Interventions and the Level of Recommendation... 8 Glossary of Terms to Describe Temperature Measurement...10 References...11 Acknowledgements...14 Page Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies.
3 Background/Significance A patient s temperature is a critical vital sign that may be used by Emergency Department (ED) clinicians to determine the degree of illness and the need for further assessment and intervention. Accurate body temperature measurement in the ED is necessary for the timely detection and management of fever or hypothermia; as well as evaluating treatment effectiveness (Crawford, Hicks, & Thompson, 2006; Sund- Levander & Grodzinsky, 2009). Pulmonary artery (PA) temperature is considered the gold standard for measuring core body temperature (Fulbrook, 1993), as mixed venous blood temperature reflects thermoregulation by the hypothalamus. Other invasive methods include esophageal, rectal and bladder measurements. Rectal temperature is considered the least invasive among these invasive temperature measures, and often is assumed to approximate core temperature (Fulbrook, 1993). Noninvasive temperature measurement methods include oral, temporal artery (TA), axillary and aural [tympanic membrane (TM)] measurements (Bridges & Thomas, 2009). All types of temperature measurements have advantages and limitations related to accuracy and precision, as well as practicality and feasibility in the ED setting (Craig, Lancaster, Taylor, Williamson, & Smyth, 2002; Fadzil, Choon, & Arumugam, 2010; Farnell, Maxwell, Tan, Rhodes, & Philips, 2005; Hooper & Andrews, 2006; Lawson et al., 2007; Lawson et al., 2007). This Emergency Nursing Resource (ENR) focuses on evidence-based practices regarding temperature measurement of patients across the lifespan in the ED setting. Methodology This ENR was created based on a thorough review and critical analysis of the literature following ENA s Guidelines for the Development of the Emergency Nursing Resources. Via a comprehensive literature search, all articles relevant to the topic were identified. The following databases were searched: PubMed, Google Scholar, MEDLINE, CINAHL, Cochrane - British Medical Journal, Agency for Healthcare Research and Quality (AHRQ; and the National Guideline Clearinghouse ( Searches were conducted using a variety of different search combinations with: temperature, measurement, methods, devices, thermometry, invasive, non-invasive, oral, rectal, tympanic, temporal, esophageal, pulmonary artery, core, body, emergency, emergency department, critical care, adults, pediatrics, children, infants and neonates. Initial searches were limited to English language articles from December 1980 October2011. In addition, the reference lists in the selected articles were hand searched for additional pertinent references. Research articles from ED settings, non-ed settings, position statements and guidelines from other sources were also reviewed. Articles that met the following criteria were chosen to formulate the ENR: research studies, metaanalyses, systematic reviews, and existing guidelines relevant to body temperature measurement. Other types of articles were reviewed and included as additional information. Articles that did not include a comparison to core temperature measurements (including rectal temperature) and/or comparison to oral temperatures were not included in the evidence summary as there was no way to determine the accuracy, precision and/or bias of temperature measurements. All temperature measurement devices described in this review are currently commercially available. The ENR authors used standardized worksheets, including the Reference Table, Evidence-Appraisal Table, Critique Worksheet and AGREE Work Sheet, to prepare tables of evidence ranking each article in terms of the level of evidence, quality of evidence, and relevance and applicability to practice. Clinical findings and levels of recommendations regarding patient management were then made by the Emergency Nursing Resource Development Committee according to the ENA s classification of levels of recommendation for practice, which include: Level A High, Level B. Moderate, Level C. Weak or Not recommended for practice (Table 1). Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 1
4 Table 1. Levels of Recommendation for Practice Level A recommendations: High Reflects a high degree of clinical certainty Based on availability of high quality level I, II and/or III evidence available using Melnyk & Fineout-Overholt grading system (Melnyk & Fineout-Overholt, 2005) Based on consistent and good quality evidence; has relevance and applicability to emergency nursing practice Is beneficial Level B recommendations: Moderate Reflects moderate clinical certainty Based on availability of Level III and/or Level IV and V evidence using Melnyk & Fineout-Overholt grading system (Melnyk & Fineout-Overholt, 2005) There are some minor or inconsistencies in quality evidence; has relevance and applicability to emergency nursing practice Is likely to be beneficial Level C recommendations: Weak Level V, VI and/or VII evidence available using Melnyk & Fineout-Overholt grading system (Melnyk & Fineout- Overholt, 2005) - Based on consensus, usual practice, evidence, case series for studies of treatment or screening, anecdotal evidence and/or opinion There is limited or low quality patient-oriented evidence; has relevance and applicability to emergency nursing practice Has limited or unknown effectiveness Not recommended for practice No objective evidence or only anecdotal evidence available; or the supportive evidence is from poorly controlled or uncontrolled studies Other indications for not recommending evidence for practice may include: o Conflicting evidence o Harmfulness has been demonstrated o Cost or burden necessary for intervention exceeds anticipated benefit o Does not have relevance or applicability to emergency nursing practice There are certain circumstances in which the recommendations stemming from a body of evidence should not be rated as highly as the individual studies on which they are based. For example: o Heterogeneity of results o Uncertainty about effect magnitude and consequences, o Strength of prior beliefs o Publication bias Evidence Table and Other Resources The articles reviewed to formulate the ENR are described in the Evidence Table. Other articles relevant to temperature measurement were reviewed and identified as additional resources (Other Resources Table). Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 2
5 Summary of Literature Review Accuracy and Precision of Temperature Measurement Methods All non-invasive methods to measure body temperature (e.g., oral, axillary, tympanic, temporal artery) have accuracy and precision variances unique to each type of method when compared to core temperature methods (e.g., rectal temperature) (Bridges & Thomas, 2009). In evaluating accuracy and precision of temperature measurement methods, it is important to note that a clinically significant difference in temperatures between core temperature measures and other non-invasive measures is considered to be 0.5 C (Sessler, Lee, & McGuire, 1991; Tayefeh, Plattner, Sessler, Ikeda, & Marder, 1998), as this reflects the range of normal circadian body temperatures. Oral Temperature Measurement Oral temperatures slightly underestimated core temperatures (PA), however, oral temperatures along with TA were the most accurate and precise compared to other non-invasive temperature measures (axillary and TM) (Lawson et al., 2007). Oral and TA temperatures had a mean difference from PA temperatures of /-0.43 C and / C respectively; as compared mean differences from PA of /-0.44 C (axillary) and /-0.56 C (TM) (Lawson et al., 2007). Oral temperatures measured by electronic thermometry in normothermic critical care (Giuliano et al., 2000) and postanesthetic adult patients (Calonder et al., 2010) were compared to core temperatures (either PA catheter or esophageal). Oral and mean core temperatures (PA) differed by to C (Giuliano et al., 2000) and oral compared to core (esophageal) temperatures had a relative bias of 0.12 C (Calonder et al., 2010); indicating oral temperatures were 0.12 C higher than core (esophageal) temperatures. Although the differences were statistically significant, these differences were not considered clinically significant since the differences were less than 0.5 C. An integrative review indicated concluded that oral temperature measurements closely reflected core temperature in the absence of a PA catheter, even among acutely ill patients receiving oxygen therapy (Hooper & Andrews, 2006). Temporal Artery Temperature Measurement Temporal artery temperatures measured in normothermic pediatric patients correlated well with core temperatures (esophageal or rectal) as measured using both rectal probes and electronic thermometer; correlations were r=0.91 (esophageal probe and TA), r=0.95 (rectal probe and TA) and r=0.88 (rectal electric and TA) (Al-Mukhaizeem et al., 2004). TA temperatures compared to rectal temperatures in pediatric patients had similar variability (precision) with rectal ( C for TA, C for core--rectal); the mean bias was C (Hebbar, Fortenberry, Rogers, Merritt, & Easley, 2005). In another study of pediatric patients (Paes, Vermeulen, Brohet, & de Winter, 2010), TA temperatures (measured using two different devices) were significantly different compared to rectal temperatures, with mean temperatures of C, C and 37.3 C for rectal, Beurer TA and Thermofocus TA temperatures respectively. The TA (infrared skin) thermometer readings had varying sensitivity from low to moderate (Beurer device=0.12 sensitivity, Thermofocus =0.64 sensitivity) (Paes et al., 2010). In a study of infants under 1 year old in the ED, TA and TM temperatures were compared to rectal temperatures (Greenes & Fleisher, 2001). Temperatures were C for rectal, C for TA Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 3
6 and C for TM; indicating the TA measurement was more accurate than TM temperatures compared to rectal. It should be noted that there were no significant differences in mean differences of TM or TA temperatures from rectal temperatures in these afebrile infants (Greenes & Fleisher, 2001). In a study of normothermic post-anesthesia adult patients where TA temperatures were compared to esophageal temperatures, there were statistically significant differences (p<0.05) with the TA temperature mean bias of 0.07 C compared to esophageal temperature. Although the differences were statistically significant, the differences were not considered clinically significant since the differences were less than 0.5 C (Calonder et al., 2010). In normothermic critically ill adults, TA temperatures were not significantly different from PA temperatures; TA temperatures had a mean difference from PA of C (Myny, De Waele, Defloor, Blot, & Colardyn, 2005). Tympanic Temperature Measurement A meta-analysis compared TM temperature measurements to rectal temperatures in pediatric patients (Craig et al., 2002). Pooled mean differences between TM and rectal temperatures was 0.29 C, with limits of agreement ranging from to C. This wide range of variance in the temperatures (limits of agreement) reflects the limits of precision using TM temperature measurement in this study (Craig et al., 2002). In adult critical care patients, TM temperatures were the least accurate and precise compared to PA temperatures with a mean difference of to C, compared to TA, oral and axillary temperatures that had a mean difference from core (PA) temperatures of: to C, 0.09 to C and 0.23 to C respectively (Lawson et al., 2007). Tympanic temperatures were significantly different from rectal temperatures among hospitalized pediatric patients with mean rectal temperature of C compared to C for TM temperatures. The TM thermometry had a sensitivity of 0.8 (Paes et al., 2010). Tympanic temperatures were less accurate than axillary temperatures among adult critical care patients, as TM temperatures had a concordance with core PA temperatures of 0.77 as compared to concordance of 0.83 for axillary (mercury-in-glass) temperatures (Moran et al., 2007). In a study of pediatric patients, ages 3 to 36 months, TM and axillary (infrared) measures were compared to rectal temperatures (Jean-Mary, Dicanzio, Shaw, & Bernstein, 2002). The TM was more accurate than axillary when compared to rectal temperatures; the TM bias was F (0.13 C) and axillary bias was F (0.18 C). In a study of intensive care pediatric patients, comparing TM, axillary, and rectal temperatures were compared to PA temperatures (Maxton, Justin, & Gillies, 2004); TM was the least accurate compared to axillary and rectal temperatures with mean differences from core (PA) temperatures of C, C and C respectively. In a study of ED patients, TM temperatures had a mean difference compared to oral (mercury-in-glass) temperature of C, with limits of agreement to C, compared to chemical oral thermometry which had a mean difference from oral temperatures of C with limits of agreement from to 0.98 C, thus indicating TM measures were more accurate and precise than chemical oral thermometry (Fadzil et al., 2010). When TM temperatures (using measurements in both ears) were compared to oral temperature measurements in both febrile and afebrile adult ED patients the mean differences were not significant, however there were significant differences (p<0.0001) between older Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 4
7 patients (65 years or older) and younger patients (under 65 years) when comparing oral to TM temperature measurements (Onur, Guneysel, Akoglu, Aydin, & Denizbasi, 2008). Integrative review analyses concluded that there is a lack of high-quality evidence to support the accuracy of temperature measurement using TM thermometers, given the variability in the accuracy and precision of TM measurements in a number of published research studies (Hooper & Andrews, 2006). Axillary Temperature Measurement Axillary mean (M) temperatures were compared to rectal and PA temperatures in pediatric patients. Axillary (M= C) and rectal (M= C) temperatures had similar variability (precision) compared to PA temperatures; axillary measurements had a mean bias was C (Hebbar et al., 2005). Among intensive care pediatric patients, TM, axillary, and rectal temperatures were compared to PA temperatures (Maxton et al., 2004). Axillary measures were more accurate than TM, but less accurate than rectal temperatures compared to PA temperatures; mean differences for axillary, TM and rectal temperature measurements were C, C, and C respectively. Among normothermic critically ill adult patients, axillary temperatures differed significantly (p<0.001) from PA temperatures, with a mean difference of / C (Myny et al., 2005). When PA temperatures were compared to axillary using gallium-in-glass (non-mercury), chemical (reactive strip) and digital measures of axillary temperatures in critically ill adults; the gallium-in-glass readings (in axilla for 12 minutes) had the most accuracy with a mean difference from core temperatures of 0.4 C, ranging from /- 1.2 C, compared to either the digital or chemical (reactive strip) axillary measurements (Rubia-Rubia, Arias, Sierra, & Aguirre-Jaime, 2011). In a study of adult trauma patients, axillary temperatures had a mean temperature difference from oral temperatures of 0.03 C, with limits of agreement ranging from to C, which was significantly better than TA mean differences from oral temperatures of 0.27 C, with limits of agreement of to C (Marable, Shaffer, Dizon, & Opalek, 2009). In both febrile and afebrile adult ED patients, oral compared to axillary temperatures were not significantly different overall. However there were significant differences (p<0.0001) by age groups of older patients (65 years or older) and younger patients (under 65 years) when comparing oral to axillary temperature measurements (Onur et al., 2008). In a meta-analysis, comparing axillary and rectal temperatures among pediatric patients, the mean differences between rectal and axillary temperature for neonates was 0.17 C (-0.15 C to+ 0.5 C) and 0.92 C (-0.15 C to C) among older children and adolescents (Craig, 2000). These wide limits of agreement (precision) between rectal and axillary temperatures may prevent low grade fever from being detected by axillary temperature measurement in pediatric patients. Chemical Thermometers A comparison of temperatures obtained by TM and chemical axillary temperature (Tempa.DOT ) methods to PA temperatures demonstrated that chemical axillary measurements (limits of agreement C) were more accurate than TM (limits of agreement -1.2 to +1.2 C) (Farnell et al., 2005). When comparing chemical axillary thermometry (Tempa.Dot Ax.), TM and PA temperatures, both TM Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 5
8 and axillary chemical mean temperatures were statistically different from PA temperatures (p< 0.05). The TM measures had a mean difference from PA readings of 0.37 to +/-0.32 C, and the axillary chemical thermometer had a mean difference from PA readings of 0.46 to +/-0.45 C. Thus, the axillary chemical was slightly less accurate and precise than TM temperatures (Fulbrook, 1993). A different chemical temperature device (3M Tempa-Dot ) was used to obtain chemical oral and axillary temperatures and comparisons were made with oral or axillary temperatures measured with an electronic device among post anesthesia patients. All temperatures were compared to operating room (OR) core temperatures (esophageal) (Washington & Matney, 2008). The chemical temperature measurements were an average of 0.57 F higher, compared to temperatures obtained with an electronic thermometer that were 0.48 F lower than OR core temperatures. Both the chemical and electronic thermometer measurements were significantly (p<0.001) correlated with OR core temperatures, with modest correlations of r=0.61 and r=0.54 respectively (Washington & Matney, 2008). Oral chemical (Nextemp ) temperature measurements were compared to both oral (mercury measured) and TM temperatures in adult ED patients (Rajee & Sultana, 2006). The chemical oral temperature modality was more precise than TM measurements when compared to oral (mercury measured) temperatures; with the chemical oral measurements within -0.6 to +0.5 C of oral (mercury in glass) temperatures as compared to TM measurements that ranged from -1.0 to +1.1 C (Rajee & Sultana, 2006). Using a chemical TA thermometer (Liquid Crystal Fever Temp Ultra ), the mean difference compared to oral (mercury in glass) temperatures was C, compared to digital oral and oral (mercury in glass) temperatures (mean difference C), and digital TM to oral (mercury in glass) temperatures (mean difference C) in ED patients indicating chemical TA thermometry had less accuracy and precision than digital oral and digital TM temperatures as compared to oral (mercury in glass) temperatures (Fadzil et al., 2010). Temperature Measurement to Detect Hyperthermia Several studies examined thermometry to detect hyperthermia in pediatric patients. In febrile (temperature than 38 C) pediatric patients younger than 24 months, TA and rectal temperature measurements were highly correlated (r=0.77) (Carr et al., 2011). The mean TA temperature was C compared to C for rectal; 94.7% of the measurements differed by less than 1 C (Carr et al., 2011). In another study of both febrile and afebrile pediatric ED patients, one to four years of age (Titus, Hulsey, Heckman, & Losek, 2009), TA temperature of 37.3 C or greater was equivalent or comparable to a rectal temperature of 38.3 C (100% sensitivity and 93.5% specificity). In febrile pediatric subjects, both TA and axillary temperatures had low sensitivity and specificity for detecting fever; neither TA or axillary temperatures were adversely influenced in the presence of shock or vasopressor use (Hebbar et al., 2005). Temporal artery (TA) temperatures of infants (age under 1 year old) with fever (rectal temperatures greater than 38 C) or high fever (rectal temperatures greater than 39 C) in the ED, were significantly more sensitive than TM temperatures (p<0.005) (Greenes & Fleisher, 2001). Professional and home models of TA measurements were compared to rectal temperatures in ED pediatric patients (Schuh et al., 2004). The TA professional thermometer accurately ruled out fever for non-febrile pediatric patients; however, it was not accurate for febrile patients (temperature over 38 Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 6
9 C), as accuracy was only 90%; and even lower with the home TA thermometer with an accuracy of 67% (Schuh et al., 2004). Thus, a temperature under 37.7 C measured by the professional TA thermometer could be accurately used as a screening mechanism to exclude fever (defined as temperature over 38.3 C rectally) in pediatric patients 3 to 24 months old (Schuh et al., 2004). In a subsample of febrile (greater than F) pediatric patients (n=63), ages one to three years, TM and axillary (infrared) measures were compared to rectal temperatures. TM bias was F (0.20 C) (sensitivity 68.3%, specificity 94.8%) compared to axillary bias of -1.2 F (0.67 C) (sensitivity 63.5%, specificity 92.6%), indicating that TM temperatures more closely correlated with rectal temperatures than axillary temperatures (Jean-Mary et al., 2002) Similarly, in a systematic review of studies examining ear-based infrared (TM) temperatures compared to rectal temperatures. Mean differences in temperature varied and ranged from C, when the rectal temperature was 38 C (Craig et al., 2002). These findings indicate that clinician could under or overtreat fever in children based on TM temperature measurement alone. Among febrile critical care adult patients, oral temperatures were more precise than TM temperatures when compared to PA temperatures, with a mean difference from PA temperatures of 0.18 to +/-0.47 C for oral and to C for TM; thus, TM temperatures underestimated PA temperatures (Giuliano et al., 2000). Temporal artery thermometry had only moderate sensitivity to detect fever (sensitivity 0.72) among neurosurgical perioperative and critical care adult patients (Kimberger, Cohen, Illievich, & Lenhardt, 2007). Both axillary and TA temperature measurements had approximately 90% or greater agreement rate of detecting fever as measured by an oral thermometer in adult trauma patients (Marable et al., 2009). Temperature Measurement to Detect Hypothermia Temporal artery thermometers had more sensitivity than oral measurements compared to PA temperatures to detect hypothermia (temperature under 35 C) in adult critical care patients (Lawson et al., 2007). Oral temperatures had a mean difference from PA of /- 0.2 C, compared to TA temperature mean difference from PA of /- 0.1 C. In another study TA temperatures had as similar level of sensitivity for detecting hypothermia (0.29 Positive Predictive value- PPV) compared to core temperature (bladder temperature measurement) (Kimberger et al., 2007). Tympanic temperatures overestimated the presence and severity of hypothermia compared to oral temperatures, with mean TM temperatures of 31.6 C and mean of 34.3 C for oral temperatures, based on readings of subjects who had been swimming in cold water (Rogers et al., 2007). Additional Information Using Rectal Temperature Measurement in ED Setting This ENR addressed only non-invasive temperature measurement. Given the limitations in accuracy and precision of non-invasive temperature measurements and lack of invasive core temperature measures for the ED patient (e.g., PA, esophageal, bladder), there are clinical situations (e.g., suspected fever) that warrant the use of rectal temperature measurement (Jensen et al., 1994; Kresovich-Wendler, Levitt, & Yearly, 1989). Specifically, only rectal temperature measurements are recommended in children 3 Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 7
10 months and younger, unless contraindicated (Jean-Mary et al., 2002). Rectal temperatures are contraindicated in neutropenic patients (Segal et al., 2008), and are not recommended in patients who have had rectal surgery/trauma or have diarrhea. Description of Decision Options/Interventions and the Level of Recommendation Temperature Measurement Device Adult Adult Febrile Adult Hypo- Thermic Adult Critically Ill /Intubated Pediatrics 0-3 Months Pediatrics 3 Months 3 Years Pediatric 3 Years 18 Years Pediatric Febrile Pediatric Hypo- Thermic Pediatric Critically Ill /Intubated Oral A A A A N/R A A A N/E N/R Tympanic I/E N/R N/E I/E N/R I/E N/R N/R N/E I/E Temporal Artery Chemical Dot A N/R N/E I/E N/R I/E A A * N/E I/E I/E I/E N/E I/E N/R N/E N/R N/R N/E N/E Axillary B N/R N/E I/E N/R I/E B N/R N/E I/E Level A (High) Recommendation: Based on consistent and good quality of evidence; has relevance and applicability to emergency nursing practice. Level B (Moderate) Recommendation: There are some minor inconsistencies in quality evidence; has relevance and applicability to emergency nursing practice. Level C (Weak) Recommendation: There is limited or low-quality patient-oriented evidence; has relevance and applicability to emergency nursing practice. N/R: Not recommended based upon current evidence. I/E: Insufficient evidence upon which to make a recommendation. N/E: No evidence upon which to make a recommendation. Evidence supporting the Level of Recommendation 1. Adult Temperature Measurement i. Oral temperature measurement ii. Temporal Artery (TA) temperature measurement iii. Axillary temperature measurement 2. Febrile Adult Temperature Measurement i. Oral temperature measurement 3. Hypothermic Adult Temperature Measurement i. Oral temperature measurement 4. Critically Ill/Intubated Adult Temperature Measurement i. Oral temperature measurement 5. Pediatrics (0 to 3 Months) Temperature Measurement i. Rectal temperature measurement * Temporal artery temperature greater than 37.3 C indicates rectal temperature of 38.3 C or greater in subjects 3-24 months (Schuh, 2004). Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 8
11 6. Pediatric (3 to 18 years) Temperature Measurement i. Oral temperature measurement ii. Temporal Artery (TA) temperature measurement iii. Axillary temperature measurement 7. Febrile Pediatric Temperature Measurement i. Oral temperature measurement ii. Temporal Artery (TA) temperature measurement Emergency Nurses Association December Please for approval to reproduce multiple copies. 9
12 Glossary of Terms to Describe Temperature Measurement Accuracy: The degree to which the means of a temperature method measures differ when compared to one or more other temperature method measures. Often the comparison temperature measurement method is the core temperature. Accuracy is reported as mean differences in temperature methods. Bias or Instrument Bias: This term is used interchangeably with accuracy. Bias or instrument bias refers to the difference between the mean of one temperature method measures compared to the mean(s) of temperature measures using different temperature method(s). Preciseness/Precision: The amount of variability (measured as the standard deviation of mean differences between temperatures) that a given temperature method measure has compared to another standard or core temperature method measure. Sensitivity: Refers to the proportion of temperature method measurements that are accurate when compared to core temperature or another standard temperature method measure. This can also be used in reference to detecting fever or hypothermia. For example, high sensitivity of a given temperature method of measurement to correctly detect fever (as measured by core temperature or another standard temperature measurement method) would indicate that a higher proportion of the patients with fever would be detected by the temperature method measure of interest. In other words the temperature measurement method of interest was accurate in predicting fever. Specificity: Refers to the proportion of temperature measurement measures that are able to discern normal temperature from an abnormal temperature (e.g., hypothermia, fever) when compared to core temperature measures or another standard temperature method measurement. For example, high specificity of a given temperature method measure of interest to accurately identify patients without fever (as measured by core temperature or another standard temperature method) would indicate a higher proportion of patients without fever would be accurately measured by the temperature method measure of interest. The emphasis of specificity is on the accuracy of the temperature measurement method on identifying when patients do not have an abnormal temperature such as fever. Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 10
13 References Al-Mukhaizeem, F., Allen, U., Komar, L., Naser, B., Roy, L., Stephens, D.,... Schuh, S. (2004). Comparison of temporal artery, rectal and esophageal core temperatures in children: Results of a pilot study. Paediatrics & Child Health, 9(7), Asher, C., & Northington, L. K. (2008). SPN news. position statement for measurement of temperature/fever in children. Journal of Pediatric Nursing, 23(3), Bridges, E., & Thomas, K. (2009). Ask the experts. noninvasive measurement of body temperature in critically ill patients. Critical Care Nurse, 29(3), Calonder, E. M., Sendelbach, S., Hodges, J. S., Gustafson, C., Machemer, C., Johnson, D., & Reiland, L. (2010). Temperature measurement in patients undergoing colorectal surgery and gynecology surgery: A comparison of esophageal core, temporal artery, and oral methods. Journal of PeriAnesthesia Nursing, 25(2), doi: /j.jopan Carr, E., A., Wilmoth, M., L., Eliades, A., Beoglos, Baker, P., J., Shelestak, D., Heisroth, K., L., & Stoner, K., H. (2011). Comparison of temporal artery to rectal temperature measurements in children up to 24 months. Journal of Pediatric Nursing, 26(3), doi: /j.pedn Craig, J. V. (2000). Temperature measured at the axilla compared with rectum in children and young people: Systematic review. BMJ: British Medical Journal (International Edition), 320(7243), Craig, J. V., Lancaster, G. A., Taylor, S., Williamson, P. R., & Smyth, R. L. (2002). Infrared ear thermometry compared with rectal thermometry in children: A systematic review. Lancet, 360(9333), 603. Crawford, D., Hicks, B., & Thompson, M. (2006). Which thermometer? factors influencing best choice for intermittent clinical temperature assessment. Journal of Medical Engineering & Technology, 30(4), doi: / Fadzil, F. M., Choon, D., & Arumugam, K. (2010). A comparative study on the accuracy of noninvasive thermometers. Australian Family Physician, 39(4), Farnell, S., Maxwell, L., Tan, S., Rhodes, A., & Philips, B. (2005). Temperature measurement: Comparison of non-invasive methods used in adult critical care. Journal of Clinical Nursing, 14(5), Fulbrook, P. (1993). Core temperature measurement in adults: A literature review. Journal of Advanced Nursing, 18(9), Giuliano, K. K., Giuliano, A. J., Scott, S. S., MacLachlan, E., Pysznik, E., Elliot, S., & Woytowicz, D. (2000). Temperature measurement in critically ill adults: A comparison of tympanic and oral methods... CE online. American Journal of Critical Care, 9(4), Greenes, D. S., & Fleisher, G. R. (2001). Accuracy of a noninvasive temporal artery thermometer for use in infants. Archives of Pediatrics & Adolescent Medicine, 155(3), Hebbar, K., Fortenberry, J. D., Rogers, K., Merritt, R., & Easley, K. (2005). Comparison of temporal artery thermometer to standard temperature measurements in pediatric intensive care unit patients. Pediatric Critical Care Medicine: A Journal of the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies, 6(5), Hooper, V. D., & Andrews, J. O. (2006). Accuracy of noninvasive core temperature measurement in acutely ill adults: The state of the science. Biological Research for Nursing, 8(1), Jean-Mary, M., Dicanzio, J., Shaw, J., & Bernstein, H. H. (2002). Limited accuracy and reliability of infrared axillary and aural thermometers in a pediatric outpatient population. Journal of Pediatrics, 141(5), Jensen, B. N., Jeppesen, L. J., Mortensen, B. B., Kjærgaard, B., Andreasen, H., & Glavind, K. (1994). The superiority of rectal thermometry to oral thermometry with regard to accuracy. Journal of Advanced Nursing, 20(4), doi: /j x Kimberger, O., Cohen, D., Illievich, U., & Lenhardt, R. (2007). Temporal artery versus bladder Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 11
14 thermometry during perioperative and intensive care unit monitoring. Anesthesia and Analgesia, 105(4), Kresovich-Wendler, K., Levitt, M. A., & Yearly, L. (1989). An evaluation of clinical predictors to determine need for rectal temperature measurement in the emergency department. The American Journal of Emergency Medicine, 7(4), Lawson, L., Bridges, E. J., Ballou, I., Eraker, R., Greco, S., Shively, J., & Sochulak, V. (2007). Accuracy and precision of noninvasive temperature measurement in adult intensive care patients. American Journal of Critical Care, 16(5), Marable, K., Shaffer, L., Dizon, V., & Opalek, J. M. (2009). Temporal artery scanning falls short as a secondary, noninvasive thermometry method for trauma patients. Journal of Trauma Nursing, 16(1), Maxton, F., Justin, L., & Gillies, D. (2004). Estimating core temperature in infants and children after cardiac surgery: A comparison of six methods. Journal of Advanced Nursing, 45(2), Moran, J. L., Peter, J. V., Solomon, P. J., Grealy, B., Smith, T., Ashforth, W.,... Peisach, A. R. (2007). Tympanic temperature measurements: Are they reliable in the critically ill? A clinical study of measures of agreement. Critical Care Medicine, 35(1), Myny, D., De Waele, J., Defloor, T., Blot, S., & Colardyn, F. (2005). Temporal scanner thermometry: A new method of core temperature estimation in ICU patients. Scottish Medical Journal, 50(1), Onur, O. E., Guneysel, O., Akoglu, H., Aydin, Y. D., & Denizbasi, A. (2008). Oral, axillary, and tympanic temperature measurements in older and younger adults with or without fever. European Journal of Emergency Medicine: Official Journal of the European Society for Emergency Medicine, 15(6), Paes, B. F., Vermeulen, K., Brohet, R. M., T, & de Winter, J. (2010). Accuracy of tympanic and infrared skin thermometers in children. Archives of Disease in Childhood, 95(12), doi: /adc Rajee, M., & Sultana, R. V. (2006). NexTemp thermometer can be used interchangeably with tympanic or mercury thermometers for emergency department use. Emergency Medicine Australasia, 18(3), Rogers, I. R., Brannigan, D., Montgomery, A., Khagure, N., Williams, A., & Jacobs, I. (2007). Tympanic thermometry is unsuitable as a screening tool for hypothermia after open water swimming. Wilderness & Environmental Medicine, 18(3), Rubia-Rubia, J., Arias, A., Sierra, A., & Aguirre-Jaime, A. (2011). Measurement of body temperature in adult patients: Comparative study of accuracy, reliability and validity of different devices. International Journal of Nursing Studies, 48(7), Schuh, S., Komar, L., Stephens, D., Chu, L., Read, S., & Allen, U. (2004). Comparison of the temporal artery and rectal thermometry in children in the emergency department. Pediatric Emergency Care, 20(11), Segal, B. H., Freifeld, A. G., Baden, L. R., Brown, A. E., Casper, C., Dubberke, E.,... The, A. S. (2008). Prevention and treatment of cancer-related infections. Journal of the National Comprehensive Cancer Network: JNCCN, 6(2), Sessler, D. I., Lee, K. A., & McGuire, J. (1991). Isoflurane anesthesia and circadian temperature cycles in humans. Anesthesiology, 75(6), Sund-Levander, M., & Grodzinsky, E. (2009). Time for a change to assess and evaluate body temperature in clinical practice. International Journal of Nursing Practice, 15(4), doi: /j x x Tayefeh, F., Plattner, O., Sessler, D. I., Ikeda, T., & Marder, D. (1998). Circadian changes in the sweatingto-vasoconstriction interthreshold range. Pflügers Archiv: European Journal of Physiology, 435(3), Emergency Nurses Association December Please Permissions@ena.org for approval to reproduce multiple copies. 12
15 Titus, M. O., Hulsey, T., Heckman, J., & Losek, J. D. (2009). Temporal artery thermometry utilization in pediatric emergency care. Clinical Pediatrics, 48(2), Washington, G. T., & Matney, J. L. (2008). Comparison of temperature measurement devices in post anesthesia patients. Journal of PeriAnesthesia Nursing, 23(1), Emergency Nurses Association December Please for approval to reproduce multiple copies. 13
16 Acknowledgements ENA would like to acknowledge the following members of the 2011 Institute for Emergency Nursing Research (IENR) Advisory Council for their review of this document: Gordon Gillespie, PhD, RN, CEN, CPEN, CCRN, FAEN Mary Johansen, PhD, MA, RN Mary Kamienski, PhD, APRN, CEN, FAEN Jane Koziol-McClain, PhD, RN Anne Manton, PhD, RN, APRN, FAEN, FAAN Lisa Wolf, PhD, RN, CEN Emergency Nurses Association December Please for approval to reproduce multiple copies. 14
Emergency Nursing Resource: Family Presence During Invasive Procedures and Resuscitation in the Emergency Department
 Emergency Nursing Resource: Family Presence During Invasive Procedures and Resuscitation in the Emergency Department Does family presence have a positive or negative influence on the patient, family and
Emergency Nursing Resource: Family Presence During Invasive Procedures and Resuscitation in the Emergency Department Does family presence have a positive or negative influence on the patient, family and
An Integrative Review Focusing on Accuracy and Reliability of Clinical Thermometers
 Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2016 An Integrative Review Focusing on Accuracy and Reliability of Clinical
Walden University ScholarWorks Walden Dissertations and Doctoral Studies Walden Dissertations and Doctoral Studies Collection 2016 An Integrative Review Focusing on Accuracy and Reliability of Clinical
Measure Abbreviation: TEMP 03 (MIPS 424)*
 Measure Abbreviation: TEMP 03 (MIPS 424)* *TEMP 03 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 424: Perioperative Temperature Management measure. MIPS measure specifications
Measure Abbreviation: TEMP 03 (MIPS 424)* *TEMP 03 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 424: Perioperative Temperature Management measure. MIPS measure specifications
Measure Abbreviation: TEMP 03 (MIPS 424)*
 Measure Abbreviation: TEMP 03 (MIPS 424)* *TEMP 03 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 424: Perioperative Temperature Management measure. MIPS measure specifications
Measure Abbreviation: TEMP 03 (MIPS 424)* *TEMP 03 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 424: Perioperative Temperature Management measure. MIPS measure specifications
Objectives. Preparing Practice Scholars: Implementing Research in the DNP Curriculum. Introduction
 Objectives Preparing Practice Scholars: Implementing Research in the DNP Curriculum 2011 Symposium Produced by Members of NONPF s Research SIG To discuss the levels of DNP research competencies currently
Objectives Preparing Practice Scholars: Implementing Research in the DNP Curriculum 2011 Symposium Produced by Members of NONPF s Research SIG To discuss the levels of DNP research competencies currently
AAENP MISSION AAENP VISION
 1 AAENP MISSION The American Academy of Emergency Nurse Practitioners promotes high quality, evidence based practice for nurse practitioners providing emergency care for patients of all ages and acuities
1 AAENP MISSION The American Academy of Emergency Nurse Practitioners promotes high quality, evidence based practice for nurse practitioners providing emergency care for patients of all ages and acuities
Nursing skill mix and staffing levels for safe patient care
 EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
The How to Guide for Reducing Surgical Complications
 The How to Guide for Reducing Surgical Complications Post operative wound (surgical site) infections Maintaining perioperative normothermia Main contacts for Reducing Surgical Complications Campaign Director:
The How to Guide for Reducing Surgical Complications Post operative wound (surgical site) infections Maintaining perioperative normothermia Main contacts for Reducing Surgical Complications Campaign Director:
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form
 Last Updated: Version 3.2 NQF-ENORSE VOLUNTARY CONSENSUS STANARS FOR HOSPITAL CARE Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure I#: SCIP- Performance Measure
Last Updated: Version 3.2 NQF-ENORSE VOLUNTARY CONSENSUS STANARS FOR HOSPITAL CARE Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure I#: SCIP- Performance Measure
Systematic Review. Request for Proposal. Grant Funding Opportunity for DNP students at UMDNJ-SN
 Systematic Review Request for Proposal Grant Funding Opportunity for DNP students at UMDNJ-SN Sponsored by the New Jersey Center for Evidence Based Practice At the School of Nursing University of Medicine
Systematic Review Request for Proposal Grant Funding Opportunity for DNP students at UMDNJ-SN Sponsored by the New Jersey Center for Evidence Based Practice At the School of Nursing University of Medicine
Evaluating the Use of a Topical Vapocoolant to Reduce Pain during Intravenous Insertions: The Patients' and Nurses' Perspectives
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Nurses are Knowledge Workers
 The Nurse as Scholar: Promoting Evidence- Based Nursing Practice Among Direct Care Nurses Elizabeth W. Bayley, PhD, RN Louanne A. Stratton, PhD, RN Nemours Strategic Plan for Research and Scholarly Activity
The Nurse as Scholar: Promoting Evidence- Based Nursing Practice Among Direct Care Nurses Elizabeth W. Bayley, PhD, RN Louanne A. Stratton, PhD, RN Nemours Strategic Plan for Research and Scholarly Activity
Clinical Practice Guideline: Gastric Tube Placement Verification Full Version [Formerly known as Emergency Nursing Resource (ENR)]
![Clinical Practice Guideline: Gastric Tube Placement Verification Full Version [Formerly known as Emergency Nursing Resource (ENR)] Clinical Practice Guideline: Gastric Tube Placement Verification Full Version [Formerly known as Emergency Nursing Resource (ENR)]](/thumbs/79/79169986.jpg) Clinical Practice Guideline: Gastric Tube Placement Verification Full Version [Formerly known as Emergency Nursing Resource (ENR)] In patients having gastric tubes inserted in the emergency department
Clinical Practice Guideline: Gastric Tube Placement Verification Full Version [Formerly known as Emergency Nursing Resource (ENR)] In patients having gastric tubes inserted in the emergency department
Faculty Awareness when Teaching Transforming Evidence-based Literature into Practice
 Faculty Awareness when Teaching Transforming Evidence-based Literature into Practice Guillermo Valdes, DNP, RN-BC, Patricia R. Messmer, PhD, RN-BC, FAAN Benjamín León School of Nursing, Miami Dade College,
Faculty Awareness when Teaching Transforming Evidence-based Literature into Practice Guillermo Valdes, DNP, RN-BC, Patricia R. Messmer, PhD, RN-BC, FAAN Benjamín León School of Nursing, Miami Dade College,
Objectives. EBP: A Definition. EBP: A Definition. Evidenced-Based Practice and Research: The Fundamentals. EBP: The Definition
 Objectives Evidenced-Based Practice and Research: The Fundamentals March 22, 2011 EBP Boot Camp Presentation by Cynthia A. Oster, PhD, MBA, RN, CNS-BC, ANP Upon completion of this educational activity,
Objectives Evidenced-Based Practice and Research: The Fundamentals March 22, 2011 EBP Boot Camp Presentation by Cynthia A. Oster, PhD, MBA, RN, CNS-BC, ANP Upon completion of this educational activity,
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES
 UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
Evidence-Based Practice Pulling the pieces together. Lynette Savage, RN, PhD, COI March 2017
 Evidence-Based Practice Pulling the pieces together Lynette Savage, RN, PhD, COI March 2017 Learning Objectives Delineate the differences between Quality Improvement (QI), Evidence Based Practice (EBP),
Evidence-Based Practice Pulling the pieces together Lynette Savage, RN, PhD, COI March 2017 Learning Objectives Delineate the differences between Quality Improvement (QI), Evidence Based Practice (EBP),
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Shared Decision Making, Ethics, and Shared Responsibility
 Shared Decision Making, Ethics, and Shared Responsibility Ben Moulton, JD, MPH Senior Legal Advisor Lecturer in Health Law, Harvard School of Public Health September 29, 2011 Shared Decision Making (SDM)
Shared Decision Making, Ethics, and Shared Responsibility Ben Moulton, JD, MPH Senior Legal Advisor Lecturer in Health Law, Harvard School of Public Health September 29, 2011 Shared Decision Making (SDM)
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU. Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia
 CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
Preparing and Registering S.T.A.B.L.E. Support Instructors
 Preparing and Registering S.T.A.B.L.E. Support Instructors If a person is unable to attend an official National or Private Instructor course, but they wish to co-teach a S.T.A.B.L.E. Learner course with
Preparing and Registering S.T.A.B.L.E. Support Instructors If a person is unable to attend an official National or Private Instructor course, but they wish to co-teach a S.T.A.B.L.E. Learner course with
This article is Part 1 of a two-part series designed. Evidenced-Based Case Management Practice, Part 1. The Systematic Review
 CE Professional Case Management Vol. 14, No. 2, 76 81 Copyright 2009 Wolters Kluwer Health Lippincott Williams & Wilkins Evidenced-Based Case Management Practice, Part 1 The Systematic Review Terry Throckmorton,
CE Professional Case Management Vol. 14, No. 2, 76 81 Copyright 2009 Wolters Kluwer Health Lippincott Williams & Wilkins Evidenced-Based Case Management Practice, Part 1 The Systematic Review Terry Throckmorton,
Rapid Review Evidence Summary: Manual Double Checking August 2017
 McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
A National Job Analysis of the Critical Care Nurse Specializing in Cardiac Surgery
 APPLIED MEASUREMENT PROFESSIONALS, INC. A National Job Analysis of the Critical Care Nurse Specializing in Cardiac Surgery Conducted for the American Association of Critical-Care Nurses Certification Corporation
APPLIED MEASUREMENT PROFESSIONALS, INC. A National Job Analysis of the Critical Care Nurse Specializing in Cardiac Surgery Conducted for the American Association of Critical-Care Nurses Certification Corporation
ECLEPS CEL Workshop July 16, 2008 Evidence Based Practice (EBP)
 ECLEPS CEL Workshop July 16, 2008 Evidence Based Practice (EBP) Definition: Evidence Based Practice Evidence based nursing practice is the conscientious, explicit and judicious use of theoryderived, research-based
ECLEPS CEL Workshop July 16, 2008 Evidence Based Practice (EBP) Definition: Evidence Based Practice Evidence based nursing practice is the conscientious, explicit and judicious use of theoryderived, research-based
Best Evidence Statement (BESt)
 Date: May 30, 2012 Title: Timing of Patient/Family Preoperative Education and its Relationship to Retention of Information Clinical Question: P (population/problem) I (intervention) C (comparison) O (outcome)
Date: May 30, 2012 Title: Timing of Patient/Family Preoperative Education and its Relationship to Retention of Information Clinical Question: P (population/problem) I (intervention) C (comparison) O (outcome)
Evidence Based Practice Template: Rotating PIV Sites in Adults
 Professional Nursing Staff Organization Evidence Based Practice Template: Rotating PIV Sites in Adults Statement of problem/issue: Rotation of peripheral intravenous catheter sites in the adult population
Professional Nursing Staff Organization Evidence Based Practice Template: Rotating PIV Sites in Adults Statement of problem/issue: Rotation of peripheral intravenous catheter sites in the adult population
Clinical Development Process 2017
 InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
Access to Health Care Services in Canada, 2003
 Access to Health Care Services in Canada, 2003 by Claudia Sanmartin, François Gendron, Jean-Marie Berthelot and Kellie Murphy Health Analysis and Measurement Group Statistics Canada Statistics Canada Health
Access to Health Care Services in Canada, 2003 by Claudia Sanmartin, François Gendron, Jean-Marie Berthelot and Kellie Murphy Health Analysis and Measurement Group Statistics Canada Statistics Canada Health
SYSTEMATIC REVIEW METHODS. Unit 1
 SYSTEMATIC REVIEW METHODS Unit 1 GETTING STARTED Introduction Schedule Ground rules EVALUATION Class Participation (20%) Contribution to class discussions Evidence of critical thinking Engagement in learning
SYSTEMATIC REVIEW METHODS Unit 1 GETTING STARTED Introduction Schedule Ground rules EVALUATION Class Participation (20%) Contribution to class discussions Evidence of critical thinking Engagement in learning
Critical appraisal of systematic reviewsijn_1863
 414..418 International Journal of Nursing Practice 2010; 16: 414 418 TIPS AND TRICKS Critical appraisal of systematic reviewsijn_1863 Dónal P O Mathúna PhD Senior Lecturer in Ethics, Decision-Making and
414..418 International Journal of Nursing Practice 2010; 16: 414 418 TIPS AND TRICKS Critical appraisal of systematic reviewsijn_1863 Dónal P O Mathúna PhD Senior Lecturer in Ethics, Decision-Making and
Emergency department rectal temperatures in over 10 years: A retrospective observational study
 Emergency department rectal temperatures in over 10 years: A retrospective observational study The Harvard community has made this article openly available. Please share how this access benefits you. Your
Emergency department rectal temperatures in over 10 years: A retrospective observational study The Harvard community has made this article openly available. Please share how this access benefits you. Your
Exploring the Science of Evidence Based Nursing. Presented by Geneva Craig, PhD, RN
 Exploring the Science of Evidence Based Nursing Presented by Geneva Craig, PhD, RN Exploring To make a careful investigation or study of something Making a careful search Searching for the purpose of discovery
Exploring the Science of Evidence Based Nursing Presented by Geneva Craig, PhD, RN Exploring To make a careful investigation or study of something Making a careful search Searching for the purpose of discovery
Evidence-Based Nursing Practice. Day 1: Intro To EBNP
 Evidence-Based Nursing Practice Day 1: Intro To EBNP Dec 11, 2015 Francesca Frati, BFA, MLIS Julia Kleinberg, BA, MLIS EBNP for infection prevention & control Two day-long workshops designed to help develop
Evidence-Based Nursing Practice Day 1: Intro To EBNP Dec 11, 2015 Francesca Frati, BFA, MLIS Julia Kleinberg, BA, MLIS EBNP for infection prevention & control Two day-long workshops designed to help develop
RESEARCH PROTOCOL M MED (ANAESTHESIOLOGY) DEPARTMENT OF ANAESTHESIOLOGY, UNIVERSITY OF LIMPOPO (MEDUNSA CAMPUS)
 RESEARCH PROTOCOL M MED (ANAESTHESIOLOGY) DEPARTMENT OF ANAESTHESIOLOGY, UNIVERSITY OF LIMPOPO (MEDUNSA CAMPUS) TITLE: AN AUDIT OF PREOPERATIVE EVALUATION OF GENERAL SURGERY PATIENTS AT DR GEORGE MUKHARI
RESEARCH PROTOCOL M MED (ANAESTHESIOLOGY) DEPARTMENT OF ANAESTHESIOLOGY, UNIVERSITY OF LIMPOPO (MEDUNSA CAMPUS) TITLE: AN AUDIT OF PREOPERATIVE EVALUATION OF GENERAL SURGERY PATIENTS AT DR GEORGE MUKHARI
Implementation Model. Levels of Evidence 3/9/2011. Strategies to get Evidence into Practice EXTRACTING. Elizabeth Bridges PhD RN CCNS, FCCM, FAAN
 Implementation Model Strategies to get Evidence into Practice Extracting Summarizing Embedding g g Elizabeth Bridges PhD RN CCNS, FCCM, FAAN Clinical Nurse Researcher University of Washington Medical Center
Implementation Model Strategies to get Evidence into Practice Extracting Summarizing Embedding g g Elizabeth Bridges PhD RN CCNS, FCCM, FAAN Clinical Nurse Researcher University of Washington Medical Center
Contents. Contributors. Introduction Kathleen M. White, PhD, RN, NEA-BC, FAAN and Ann O Sullivan, MSN, RN, NE-BC, CNE
 Contents Contributors Introduction Kathleen M. White, PhD, RN, NEA-BC, FAAN and Ann O Sullivan, MSN, RN, NE-BC, CNE xi xiv Chapter 1 Nursing s Social Policy Statement 1 Catherine E. Neuman, MSN, RN, NEA-BC
Contents Contributors Introduction Kathleen M. White, PhD, RN, NEA-BC, FAAN and Ann O Sullivan, MSN, RN, NE-BC, CNE xi xiv Chapter 1 Nursing s Social Policy Statement 1 Catherine E. Neuman, MSN, RN, NEA-BC
Objectives. Brief Review: EBP vs Research. APHON/Mattie Miracle Cancer Foundation EBP Grant Program Webinar 3/5/2018
 APHON/Mattie Miracle Cancer Foundation EBP Grant Program Webinar Mary Baron Nelson, PhD RN Katherine Patterson Kelly, PhD RN Objectives Identify the process for submitting a LOI for an APHON EBP grant,
APHON/Mattie Miracle Cancer Foundation EBP Grant Program Webinar Mary Baron Nelson, PhD RN Katherine Patterson Kelly, PhD RN Objectives Identify the process for submitting a LOI for an APHON EBP grant,
Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence
 CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
Reducing Fever and Improving Outcomes In The Neurologically Compromised Patient
 Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Reducing Fever and Improving Outcomes In The Neurologically Compromised Patient Rachel Gross RN Lehigh Valley Health Network,
Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Reducing Fever and Improving Outcomes In The Neurologically Compromised Patient Rachel Gross RN Lehigh Valley Health Network,
Evidence-based Practice, Research, and Quality Improvement What s the Difference?
 Evidence-based Practice, Research, and Quality Improvement What s the Difference? Susan B Stillwell, DNP, RN, CNE, ANEF, FAAN Associate Professor School of Nursing University of Portland Portland, OR Quality
Evidence-based Practice, Research, and Quality Improvement What s the Difference? Susan B Stillwell, DNP, RN, CNE, ANEF, FAAN Associate Professor School of Nursing University of Portland Portland, OR Quality
The Essentials of Maintaining Patient Normothermia
 1 The Essentials of Maintaining Patient Normothermia Copyright 2011 by Virgo Publishing. http://www.infectioncontroltoday.com/ By: Posted on: 02/22/2010 http://www.infectioncontroltoday.com/articles/2010/02/the-essentials-of-maintainingpatient-normothermi.aspx
1 The Essentials of Maintaining Patient Normothermia Copyright 2011 by Virgo Publishing. http://www.infectioncontroltoday.com/ By: Posted on: 02/22/2010 http://www.infectioncontroltoday.com/articles/2010/02/the-essentials-of-maintainingpatient-normothermi.aspx
Best Evidence Statement (BESt)
 Best Evidence Statement (BESt) Date: December 22, 2011 Title: Child Life Support During Medical Procedures Clinical Question: P (population) I (intervention) C (comparison) O (outcome) T (time) Among pediatric
Best Evidence Statement (BESt) Date: December 22, 2011 Title: Child Life Support During Medical Procedures Clinical Question: P (population) I (intervention) C (comparison) O (outcome) T (time) Among pediatric
ENVIRONMENT Preoperative evaluation clinic. Preoperative evaluation clinic. Preoperative evaluation clinic. clinic. clinic. Preoperative evaluation
 Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
FANNP 28TH NATIONAL NNP SYMPOSIUM: CLINICAL UPDATE AND REVIEW OCTOBER 17-21, 2017
 How Can NNPs Perform Evidence-Based Practice at the Bedside? Bobby B. Bellflower, DNSc, APRN-BC, NNP-BC Associate Professor, Director of DNP Programs University of Tennessee Health Science Center Neonatal
How Can NNPs Perform Evidence-Based Practice at the Bedside? Bobby B. Bellflower, DNSc, APRN-BC, NNP-BC Associate Professor, Director of DNP Programs University of Tennessee Health Science Center Neonatal
University of Minnesota Anesthesiology Residency Program PEDIATRIC ANESTHESIA ROTATION GOALS AND OBJECTIVES
 University of Minnesota Anesthesiology Residency Program PEDIATRIC ANESTHESIA ROTATION GOALS AND OBJECTIVES Goals: The overall goal of the rotation is to provide an introduction and understanding of the
University of Minnesota Anesthesiology Residency Program PEDIATRIC ANESTHESIA ROTATION GOALS AND OBJECTIVES Goals: The overall goal of the rotation is to provide an introduction and understanding of the
Effectiveness and safety of intravenous therapy at home for children and adolescents with acute and chronic illnesses: a systematic review protocol
 Effectiveness and safety of intravenous therapy at home for children and adolescents with acute and chronic illnesses: a systematic review protocol Helena Hansson 1 Anne Brødsgaard 2 1 Department of Paediatric
Effectiveness and safety of intravenous therapy at home for children and adolescents with acute and chronic illnesses: a systematic review protocol Helena Hansson 1 Anne Brødsgaard 2 1 Department of Paediatric
December 16, Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC
 Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
A Comparison of Different Methods of Temperature Measurements in Sick Newborns
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 57, NO. 6, 2011 A Comparison of Different Methods of Temperature Measurements in Sick Newborns by Sinan Uslu, 1,2 Hamus Ozdemir, 2 Ali Bulbul, 1 Serdar Comert, 1 Fatih
JOURNAL OF TROPICAL PEDIATRICS, VOL. 57, NO. 6, 2011 A Comparison of Different Methods of Temperature Measurements in Sick Newborns by Sinan Uslu, 1,2 Hamus Ozdemir, 2 Ali Bulbul, 1 Serdar Comert, 1 Fatih
Creating Care Pathways Committees
 Presentation Creating Care Title Pathways Committees December 12, 2012 December 12, 2012 Creating Care Pathways Committees LeadingAge Indiana Integrated Care & Payment Executive Series 1 2012 Health Dimensions
Presentation Creating Care Title Pathways Committees December 12, 2012 December 12, 2012 Creating Care Pathways Committees LeadingAge Indiana Integrated Care & Payment Executive Series 1 2012 Health Dimensions
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Malnutrition Screening Pathway v.1.1
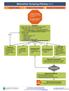 Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
Clinical guideline Published: 23 April 2008 nice.org.uk/guidance/cg65
 Hypothermia: prevention ention and management in adults having surgery Clinical guideline Published: 23 April 2008 nice.org.uk/guidance/cg65 NICE 20. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Hypothermia: prevention ention and management in adults having surgery Clinical guideline Published: 23 April 2008 nice.org.uk/guidance/cg65 NICE 20. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Shannon Moreland, DNP, FNP, CEN University of Rochester School of Nursing Strong Memorial Hospital Rochester, NY
 Practice Innovation Committee: Fostering the Use of Evidence-Based Practice in the Emergency Department Shannon Moreland, DNP, FNP, CEN University of Rochester School of Nursing Strong Memorial Hospital
Practice Innovation Committee: Fostering the Use of Evidence-Based Practice in the Emergency Department Shannon Moreland, DNP, FNP, CEN University of Rochester School of Nursing Strong Memorial Hospital
NURSING - GRADUATE (NGRD)
 Nursing - Graduate (NGRD) 1 NURSING - GRADUATE (NGRD) Courses NGRD 500. Gerontological Health and Wellness. 2 Continues development of the advanced practice role of health promotion, maintenance, and management.
Nursing - Graduate (NGRD) 1 NURSING - GRADUATE (NGRD) Courses NGRD 500. Gerontological Health and Wellness. 2 Continues development of the advanced practice role of health promotion, maintenance, and management.
Goals and Objectives. Assessment Methods/Tools
 CA-2 PEDIATRIC ANESTHESIA ROTATION Minneapolis Children s Hospital and Clinics (MCHC) Rotation Site Director: Dr. Chris Altman Rotation Duration: 6 weeks Introduction: In the CA-2 year residents have the
CA-2 PEDIATRIC ANESTHESIA ROTATION Minneapolis Children s Hospital and Clinics (MCHC) Rotation Site Director: Dr. Chris Altman Rotation Duration: 6 weeks Introduction: In the CA-2 year residents have the
Version 1.0 (posted Aug ) Aaron L. Leppin. Background. Introduction
 Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
PROCEDURAL SEDATION AND ANALGESIA: HOSPITAL-WIDE POLICY
 CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
Institutional Handbook of Operating Procedures Policy
 Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Clinical Practice Guideline Development Manual
 Clinical Practice Guideline Development Manual Publication Date: September 2016 Review Date: September 2021 Table of Contents 1. Background... 3 2. NICE accreditation... 3 3. Patient Involvement... 3 4.
Clinical Practice Guideline Development Manual Publication Date: September 2016 Review Date: September 2021 Table of Contents 1. Background... 3 2. NICE accreditation... 3 3. Patient Involvement... 3 4.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Single Technology Appraisal (STA)
 Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective on the technology
Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective on the technology
Written and verbal information versus verbal information only for patients being discharged from acute hospital settings to home: systematic review
 HEALTH EDUCATION RESEARCH Vol.20 no.4 2005 Theory & Practice Pages 423 429 Advance Access publication 30 November 2004 Written and verbal information versus verbal information only for patients being discharged
HEALTH EDUCATION RESEARCH Vol.20 no.4 2005 Theory & Practice Pages 423 429 Advance Access publication 30 November 2004 Written and verbal information versus verbal information only for patients being discharged
Evidence-Based Practice for Nursing
 Evidence-Based Practice for Nursing The Essentials of Baccalaureate Education for Professional Nursing Practice Pages 15-20 in: http://www.aacn.nche.edu/educationresources/baccessentials08.pdf AACN Essential
Evidence-Based Practice for Nursing The Essentials of Baccalaureate Education for Professional Nursing Practice Pages 15-20 in: http://www.aacn.nche.edu/educationresources/baccessentials08.pdf AACN Essential
The Effects of Preceptor Training on New Graduate Registered Nurse Transition Experiences and Organizational Outcomes
 The Effects of Preceptor Training on New Graduate Registered Nurse Transition Experiences and Organizational Outcomes Carina J. Piccinini, MSN, RN; Nancy Hudlun, MSN, RN, CCRN; Karen Branam, MSN, RN; and
The Effects of Preceptor Training on New Graduate Registered Nurse Transition Experiences and Organizational Outcomes Carina J. Piccinini, MSN, RN; Nancy Hudlun, MSN, RN, CCRN; Karen Branam, MSN, RN; and
Survey of Nurse Employers in California 2014
 Survey of Nurse Employers in California 2014 Conducted by UCSF Philip R. Lee Institute for Health Policy Studies, California Institute for Nursing & Health Care, and the Hospital Association of Southern
Survey of Nurse Employers in California 2014 Conducted by UCSF Philip R. Lee Institute for Health Policy Studies, California Institute for Nursing & Health Care, and the Hospital Association of Southern
Anesthesia Elective Curriculum Outline
 Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
Department of Internal Medicine Texas Tech University Health Sciences Center Odessa, Texas Anesthesia Elective Curriculum Outline Revision Date: July 10, 2006 Approved by Curriculum Meeting September 19,
Hospital data to improve the quality of care and patient safety in oncology
 Symposium QUALITY AND SAFETY IN ONCOLOGY NURSING: INTERNATIONAL PERSPECTIVES Hospital data to improve the quality of care and patient safety in oncology Dr Jean-Marie Januel, PhD, MPH, RN MER 1, IUFRS,
Symposium QUALITY AND SAFETY IN ONCOLOGY NURSING: INTERNATIONAL PERSPECTIVES Hospital data to improve the quality of care and patient safety in oncology Dr Jean-Marie Januel, PhD, MPH, RN MER 1, IUFRS,
How to Find and Evaluate Pertinent Research. Levels and Types of Research Evidence
 AACN Advanced Critical Care Volume 24, Number 4, pp. 416-420 2013 AACN Clinical Inquiry Bradi B. Granger, RN, PhD Department Editor How to Find and Evaluate Pertinent Research Adrianne Leonardelli, MLIS
AACN Advanced Critical Care Volume 24, Number 4, pp. 416-420 2013 AACN Clinical Inquiry Bradi B. Granger, RN, PhD Department Editor How to Find and Evaluate Pertinent Research Adrianne Leonardelli, MLIS
CA-1 CRITICAL CARE ROTATION University of Minnesota Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks
 CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland
 Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Draft National Quality Assurance Criteria for Clinical Guidelines
 Draft National Quality Assurance Criteria for Clinical Guidelines Consultation document July 2011 1 About the The is the independent Authority established to drive continuous improvement in Ireland s health
Draft National Quality Assurance Criteria for Clinical Guidelines Consultation document July 2011 1 About the The is the independent Authority established to drive continuous improvement in Ireland s health
A Comparison of Job Responsibility and Activities between Registered Dietitians with a Bachelor's Degree and Those with a Master's Degree
 Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 11-17-2010 A Comparison of Job Responsibility and Activities between Registered Dietitians
Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 11-17-2010 A Comparison of Job Responsibility and Activities between Registered Dietitians
ASCO s Quality Training Program
 ASCO s Quality Training Program Project Title: Treatment of febrile neutropenia at the University of Virginia Presenter s Name: Tri Le, MD, Tanya Thomas, RN, Michael Keng, MD Institution: University of
ASCO s Quality Training Program Project Title: Treatment of febrile neutropenia at the University of Virginia Presenter s Name: Tri Le, MD, Tanya Thomas, RN, Michael Keng, MD Institution: University of
Bid Bridging i the know-do gap in primary. promote effective practice. Director, London School of Hygiene and Tropical Medicine
 Bid Bridging i the know-do gap in primary care an overview of strategies to promote effective practice Andy Haines Director, London School of Hygiene and Tropical Medicine Niccolo Machiavelli in the The
Bid Bridging i the know-do gap in primary care an overview of strategies to promote effective practice Andy Haines Director, London School of Hygiene and Tropical Medicine Niccolo Machiavelli in the The
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary
 TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary Inclusion Criteria Age 0-17 years Gastrostomy tube insertions
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary Inclusion Criteria Age 0-17 years Gastrostomy tube insertions
Quality ID #424 (NQF 2681): Perioperative Temperature Management National Quality Strategy Domain: Patient Safety
 Quality ID #424 (NQF 2681): Perioperative Temperature Management National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #424 (NQF 2681): Perioperative Temperature Management National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
2010 PQRI REPORTING OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #193: Perioperative Temperature Management 2010 PQRI REPTING OPTIONS F INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage of patients, regardless of age, undergoing surgical or therapeutic
Measure #193: Perioperative Temperature Management 2010 PQRI REPTING OPTIONS F INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage of patients, regardless of age, undergoing surgical or therapeutic
Disclosures. The Nuts and Bolts of Orthopaedic Nursing Research. Objectives. Learner Outcome 12/7/2016
 The Nuts and Bolts of Orthopaedic Nursing Research Dawn Denny, PhD, RN, ONC Disclosures Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect of my current personal or professional
The Nuts and Bolts of Orthopaedic Nursing Research Dawn Denny, PhD, RN, ONC Disclosures Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect of my current personal or professional
Institution Degree Year University of Texas Houston Doctorate of Nursing Practice 2012 Health Science Center School of Nursing Houston, TX
 Melissa Dawn McLenon, DNP, APRN, ACNP-BC Acute Care Nurse Practitioner Cardiothoracic Transplant Surgery University of Maryland Medical Center 22 South Green St. Baltimore, MD 21201 (410) 599-5420 (mobile)
Melissa Dawn McLenon, DNP, APRN, ACNP-BC Acute Care Nurse Practitioner Cardiothoracic Transplant Surgery University of Maryland Medical Center 22 South Green St. Baltimore, MD 21201 (410) 599-5420 (mobile)
Symptom Management? Complex cases? Difficult decisions?
 Symptom Management? Complex cases? Difficult decisions? What can help us to help our patients? Who can help us to help our patients? Anita Margulies BSN RN 1 Zürich, Switzerland EBM, EBN, Evidence-based
Symptom Management? Complex cases? Difficult decisions? What can help us to help our patients? Who can help us to help our patients? Anita Margulies BSN RN 1 Zürich, Switzerland EBM, EBN, Evidence-based
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
NURSING (MN) Nursing (MN) 1
 Nursing (MN) 1 NURSING (MN) MN501: Advanced Nursing Roles This course explores skills and strategies essential to successful advanced nursing role implementation. Analysis of existing and emerging roles
Nursing (MN) 1 NURSING (MN) MN501: Advanced Nursing Roles This course explores skills and strategies essential to successful advanced nursing role implementation. Analysis of existing and emerging roles
Critical Appraisal of a Therapy Paper (Randomized Controlled Trial)
 Critical Appraisal of a Therapy Paper (Randomized Controlled Trial) Goal: Participants will be able to critically appraise an article addressing therapy. Objectives: 1. Learn how build a PICO question
Critical Appraisal of a Therapy Paper (Randomized Controlled Trial) Goal: Participants will be able to critically appraise an article addressing therapy. Objectives: 1. Learn how build a PICO question
19th Annual. Challenges. in Critical Care
 19th Annual Challenges in Critical Care A Multidisciplinary Approach Friday August 22, 2014 The Hotel Hershey 100 Hotel Road Hershey, Pennsylvania 17033 A continuing education service of Penn State College
19th Annual Challenges in Critical Care A Multidisciplinary Approach Friday August 22, 2014 The Hotel Hershey 100 Hotel Road Hershey, Pennsylvania 17033 A continuing education service of Penn State College
The Effect Of Preoperative Reflective Hats And Jackets, And Intraoperative Reflective Blankets On Perioperative Temperature
 ISPUB.COM The Internet Journal of Anesthesiology Volume 6 Number 2 The Effect Of Preoperative Reflective Hats And Jackets, And Intraoperative Reflective Blankets On Perioperative Temperature Y Sheng, F
ISPUB.COM The Internet Journal of Anesthesiology Volume 6 Number 2 The Effect Of Preoperative Reflective Hats And Jackets, And Intraoperative Reflective Blankets On Perioperative Temperature Y Sheng, F
MASTER OF SCIENCE IN NURSING (MSN)
 Master of Science in Nursing (MSN) MASTER OF SCIENCE IN NURSING (MSN) https://nursing.case.edu/msn/ Phone: 6.68.888 Latina Brooks, PhD, CNP, Program Director latina.brooks@case.edu The Master of Science
Master of Science in Nursing (MSN) MASTER OF SCIENCE IN NURSING (MSN) https://nursing.case.edu/msn/ Phone: 6.68.888 Latina Brooks, PhD, CNP, Program Director latina.brooks@case.edu The Master of Science
Review: Measuring the Impact of Interprofessional Education (IPE) on Collaborative Practice and Patient Outcomes
 Review: Measuring the Impact of Interprofessional Education (IPE) on Collaborative Practice and Patient Outcomes Valentina Brashers MD, FACP, FNAP Professor of Nursing & Woodard Clinical Scholar Attending
Review: Measuring the Impact of Interprofessional Education (IPE) on Collaborative Practice and Patient Outcomes Valentina Brashers MD, FACP, FNAP Professor of Nursing & Woodard Clinical Scholar Attending
C. Agency for Healthcare Research and Quality
 Page 1 of 7 C. Agency for Healthcare Research and Quality Draft Guidelines for Ensuring the Quality of Information Disseminated to the Public Contents I. Agency Mission II. Scope and Applicability of Guidelines
Page 1 of 7 C. Agency for Healthcare Research and Quality Draft Guidelines for Ensuring the Quality of Information Disseminated to the Public Contents I. Agency Mission II. Scope and Applicability of Guidelines
CLOSING THE GAP: EVIDENCE TO ACTION
 CLOSING THE GAP: EVIDENCE TO ACTION DR. SALIZAR MOHAMED LUDIN RN (PPUM), CRIT CARE (PPUM), BNSc (Teaching)(UM), MN (Crit.Care) (AUS), PhD (AUS) AGM, Malaysian Nurses Association, Pahang Branch, Gambang
CLOSING THE GAP: EVIDENCE TO ACTION DR. SALIZAR MOHAMED LUDIN RN (PPUM), CRIT CARE (PPUM), BNSc (Teaching)(UM), MN (Crit.Care) (AUS), PhD (AUS) AGM, Malaysian Nurses Association, Pahang Branch, Gambang
13th Annual Meridian Nursing Research and Evidence Based Practice Conference 2017 General Guidelines for Abstract Submission
 Hackensack Meridian Ann May Center for Nursing 13 th Annual Meridian Nursing Research and Evidence Based Practice Conference Instructions for Submission All author information and abstract contents must
Hackensack Meridian Ann May Center for Nursing 13 th Annual Meridian Nursing Research and Evidence Based Practice Conference Instructions for Submission All author information and abstract contents must
Transcending Boundaries to Transform Healthcare through Intervention Research and Evidence-based Practice
 Transcending Boundaries to Transform Healthcare through Intervention Research and Evidence-based Practice Bernadette Mazurek Melnyk, PhD, CPNP/PMHNP, FAANP, FAAN Associate Vice President for Health Promotion
Transcending Boundaries to Transform Healthcare through Intervention Research and Evidence-based Practice Bernadette Mazurek Melnyk, PhD, CPNP/PMHNP, FAANP, FAAN Associate Vice President for Health Promotion
Pediatric Skin Integrity Practice Guideline for Institutional Use: A Quality Improvement Project
 St. John Fisher College Fisher Digital Publications Nursing Faculty Publications Wegmans School of Nursing 7-2014 Pediatric Skin Integrity Practice Guideline for Institutional Use: A Quality Improvement
St. John Fisher College Fisher Digital Publications Nursing Faculty Publications Wegmans School of Nursing 7-2014 Pediatric Skin Integrity Practice Guideline for Institutional Use: A Quality Improvement
Assessing competence during professional experience placements for undergraduate nursing students: a systematic review
 University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
During the hospital medicine rotation, residents will focus on the following procedures as permitted by case mix:
 Educational Goals & Objectives The Inpatient Family Medicine rotation will provide the resident with an opportunity to evaluate and manage patients with common acute medical conditions. Training will focus
Educational Goals & Objectives The Inpatient Family Medicine rotation will provide the resident with an opportunity to evaluate and manage patients with common acute medical conditions. Training will focus
S T A B L E INSTRUCTOR COURSE WITH CARDIAC MODULE OCTOBER 1-3, 2007 SPONSORED BY
 SUGAR TEMPERATURE AIRWAY BLOOD PRESSURE LAB WORK EMOTIONAL SUPPORT S T A B L E INSTRUCTOR COURSE WITH CARDIAC MODULE OCTOBER 1-3, 2007 AKRON CHILDREN S HOSPITAL WILLIAM H. CONSIDINE PROFESSIONAL BUILDING
SUGAR TEMPERATURE AIRWAY BLOOD PRESSURE LAB WORK EMOTIONAL SUPPORT S T A B L E INSTRUCTOR COURSE WITH CARDIAC MODULE OCTOBER 1-3, 2007 AKRON CHILDREN S HOSPITAL WILLIAM H. CONSIDINE PROFESSIONAL BUILDING
Technology Overview. Issue 13 August A Clinical and Economic Review of Telephone Triage Services and Survey of Canadian Call Centre Programs
 Technology Overview Issue 13 August 2004 A Clinical and Economic Review of Telephone Triage Services and Survey of Canadian Call Centre Programs Publications can be requested from: CCOHTA 600-865 Carling
Technology Overview Issue 13 August 2004 A Clinical and Economic Review of Telephone Triage Services and Survey of Canadian Call Centre Programs Publications can be requested from: CCOHTA 600-865 Carling
Scaling Up and Validating a Nursing Acuity Tool to Ensure Synergy in Pediatric Critical Care
 Scaling Up and Validating a Nursing Acuity Tool to Ensure Synergy in Pediatric Critical Care Jean Connor PhD, RN, CPNP, FAAN Director of Nursing Research, Cardiovascular and Critical Care Services Boston
Scaling Up and Validating a Nursing Acuity Tool to Ensure Synergy in Pediatric Critical Care Jean Connor PhD, RN, CPNP, FAAN Director of Nursing Research, Cardiovascular and Critical Care Services Boston
IMCI at the Referral Level: Hospital IMCI
 Integrated Management of Childhood Illness (IMCI) Implementation in the Western Pacific Region IMCI at the Referral Level: Hospital IMCI 6 IMCI at the Referral Level: Hospital IMCI Hospital referral care:
Integrated Management of Childhood Illness (IMCI) Implementation in the Western Pacific Region IMCI at the Referral Level: Hospital IMCI 6 IMCI at the Referral Level: Hospital IMCI Hospital referral care:
Effectively implementing multidisciplinary. population segments. A rapid review of existing evidence
 Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
Effectively implementing multidisciplinary teams focused on population segments A rapid review of existing evidence October 2016 Francesca White, Daniel Heller, Cait Kielty-Adey Overview This review was
PHARMACOLOGY An Evidence-Based Practice Conference for Advanced Practice Clinicians
 Seventh Annual FOCUS ON PHARMACOLOGY An Evidence-Based Practice Conference for Advanced Practice Clinicians Saturday April 16, 2016 Sheraton Harrisburg Hershey Hotel 4650 Lindle Road, Harrisburg, PA 17111
Seventh Annual FOCUS ON PHARMACOLOGY An Evidence-Based Practice Conference for Advanced Practice Clinicians Saturday April 16, 2016 Sheraton Harrisburg Hershey Hotel 4650 Lindle Road, Harrisburg, PA 17111
