Health Policy Brief. Better Outcomes, Lower Costs: Palliative Care Program Reduces Stress, Costs of Care for Children With Life-Threatening Conditions
|
|
|
- Katrina Watts
- 6 years ago
- Views:
Transcription
1 Health Policy Brief August 2012 Better Outcomes, Lower Costs: Palliative Care Program Reduces Stress, Costs of Care for Children With Life-Threatening Conditions Daphna Gans, Gerald F. Kominski, Dylan H. Roby, Allison L. Diamant, Xiao Chen, Wenjiao Lin and Nina Hohe for Children Partners improved quality of life for the child and family. SUMMARY: This policy brief examines the Partners for Children (PFC) program California s public pediatric community-based palliative care benefit to children living with life-threatening conditions and their families. Preliminary analysis of administrative and survey data indicates that participation in the PFC program improves quality of life for the child and family. In addition, participation in the program resulted in a one-third reduction in the average number of days spent in the hospital. Shifting care from a hospital setting to in-home community-based care resulted in cost savings of $1,677 per child per month on average an 11% decrease in spending on a traditionally high-cost population. As the three-year pilot program draws to an end, policymakers are considering the advisability of extending the program beyond the 11 counties that now participate. This policy brief provides recommendations that policymakers, families and advocates should consider to ensure sustainability and successful expansion of the program. Supported by the Children s Hospice & Palliative Care Coalition (CHPCC). California is one of the few states to offer a public community-based pediatric palliative care benefit to children living with life-threatening conditions and their families that is available earlier than the last six months of life. Through the Partners for Children (PFC) program, eligible children receive in-home coordinated family-centered care including pain and symptom management, access to a 24/7 nurse line, family education, respite care, expressive therapies and family counseling. Currently, the number of children living with a life-threatening condition and receiving treatment in community settings is estimated at half a million a year nationally. 1,2 What Is Pediatric Palliative Care? Pediatric palliative care seeks to relieve symptoms associated with a serious medical condition or its treatment and to enhance the quality of life for children and their families, addressing their unique psychological, social and spiritual needs. Source: The Institute of Medicine (IOM) 3 California s Response to the Need for Pediatric Palliative Care California was one of the first states to respond to the need for comprehensive pediatric palliative care. The Nick Snow Children s
2 2 UCLA CENTER FOR HEALTH POLICY RESEARCH Exhibit 1 Exhibit 2 Counties Participating in the Partners for Children (PFC) Program* Monterey San Diego Santa Clara Santa Cruz Marin Alameda Per Enrollee Per Month Medical Expenditures Before Enrollment in the PFC Program by Type of Service Outpatient 26% Pharmacy 9% Inpatient 65% Source: UCLA Center for Health Policy Research preliminary analysis based on MIS/DSS claims, MEDS and CMS Net data from 2009 until September Per Enrollee Per Month Medical Expenditures During Enrollment in the PFC Program by Type of Service Outpatient 39% Pharmacy 14% Inpatient 47% Orange San Francisco Sonoma Los Angeles Fresno * Due to a lack of providers, Alameda and Fresno counties are currently not serving clients. Source: UCLA Center for Health Policy Research preliminary analysis based on MIS/DSS claims, MEDS and CMS Net data from 2009 until September Hospice and Palliative Care Act of 2006 (bill number AB 1745) required the California State Department of Health Care Services (DHCS) to develop a pediatric palliative care benefit for children eligible for Medi- Cal alongside curative care and regardless of the child s life expectancy. Approved as a three-year pilot program in 2008, PFC was implemented in January The objective of the program is to improve the quality of life for the child or teen participant and his or her family through the provision of supportive home-based services and to minimize costly hospital stays. As of March 2012, there are 123 participants in the program from seven counties, ranging in age from less than 1 to 20 years old. Sixtynine percent of the children are male, 71% are Hispanic/Latino, 12% are non-latino Caucasian and the remaining 17% are from other ethnic or racial backgrounds. About half report speaking Spanish at home. The eligible life-threatening conditions of the participants include neurologic (29%), cancer (20%), pulmonary (16%), neuromuscular (10%), gastrointestinal (6%), cardiac (4%) and others that meet medical eligibility (15%). There are 45 children on wait lists in different counties, the majority of whom are unable to participate due to the lack of participating care agencies in the area or the lack of space at the currently participating care agencies. The program was considered highly innovative given that before the enactment of the Patient Protection and Affordable Care Act (ACA) in 2010, children with life-limiting health conditions under Medicaid were eligible for a hospice benefit only in the last six months of their life. Additionally, to receive the benefit, families had to end all curative treatment for the child s life-limiting condition, a choice many found difficult to make. The American Academy of Pediatrics recommends that pediatric palliative care, as defined by the Institute of Medicine (IOM), begin upon the diagnosis of a child s lifethreatening condition, and continue for the
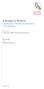
3 UCLA CENTER FOR HEALTH POLICY RESEARCH 3 Change in Per Enrollee Per Month Cost in U.S. Dollars From Pre- to Post-Enrollment in the PFC Program by Type of Service Exhibit 3 $2,000 $1,000 $0 -$1,000 -$2,000 -$3,000 -$4,000 Inpatient Outpatient Pharmacy Total Source: UCLA Center for Health Policy Research preliminary analysis based on MIS/DSS claims, MEDS and CMS Net data from 2009 until September duration of the disease and alongside curative care or life-saving treatment. 5 Additionally, the IOM recommends that such care be included in both public and private insurance plans. 3 With the passage of the ACA, including the new Concurrent Care for Children Requirement (CCCR Section 2302), state Medicaid programs were required to provide hospice care alongside curative treatment for qualifying children. However, the eligibility requirement that a child has at most six months to live was not changed. In contrast, the PFC program provides access to comprehensive in-home palliative care services as early as at the time of diagnosis and throughout the course of the disease. Assessing the PFC Program: Preliminary Findings One-Third Reduction in Hospital Days One of the PFC program s goals is to minimize hospitalization through the use of community-based care. Based on preliminary data, there was a 32% reduction in the average number of days spent in the hospital per member per month from 4.0 to Before participation in the program, the majority of the medical expenditures (65%) occurred in the inpatient hospital setting, with a smaller proportion in the community: 26% in outpatient settings (e.g., doctors offices, clinics) accompanied by 9% in pharmaceutical costs (Exhibit 1). After enrollment, only about half of the expenditures (47%) occurred in the inpatient setting with a larger share in community settings: 39% in outpatient settings (including added PFC services such as expressive therapy sessions and care coordination) and 14% in pharmaceutical costs (Exhibit 2). 7 11% Reduction in Spending The average total medical expenditures per enrollee per month after enrollment ($13,976) were $1,677 lower than expenditures before program participation ($15,653) an 11% reduction in average costs. For the first 18 months of the program operation from January 2010 to September 2011, these cost savings amounted to nearly $1 million. Cost savings were driven by reductions in the volume of inpatient care, in which postenrollment expenditures were $3,571 lower than before enrollment a 35% reduction in hospital stay costs. However, these cost savings were partially offset by increases in expenditures on services outside the hospital, most notably a 34% increase ($1,398) in outpatient costs and a 35% increase ($495) in outpatient pharmaceutical costs (Exhibit 3). 8 Despite the offset, the overall cost savings suggest that the PFC program appears to be reducing expensive inpatient care and replacing it with less expensive communitybased and outpatient care. reduction in There was a one-third hospital days per child.
4 4 UCLA CENTER FOR HEALTH POLICY RESEARCH How the Partners for Children Program Works The PFC program provides the following services: (1) care coordination of services across settings bringing together PFC, Medi-Cal, and other medical and community services to ensure that all of the child s and family s needs are addressed; (2) expressive therapies including art, music, play and massage for the child; (3) family education, providing instruction to families regarding the care of the child and operation of medical equipment; (4) respite care both in and out of the home to provide needed rest for the primary caregivers; (5) family counseling and bereavement counseling after the death of a child, if needed; and (6) pain and symptom management. In addition, the hospice and home health agencies offer 24/7 on-call nursing support providing advice on urgent care questions. In order to be enrolled in the PFC program, children and young adults up to 20 years old must meet certain financial and medical criteria, and must reside in one of the 11 counties participating in the program. 9 The program is built on collaboration among DHCS Children s Medical Services, California Children s Services (CCS) program at the state and county levels, special care centers where children receive curative treatment, and local licensed private home health agencies, hospices or contracted agencies that have voluntarily decided to participate in the program. To start the process, children can be referred by a physician or another health care provider, self refer or be identified by a California Children s Services Nurse Liaison (CCSNL). The county CCSNL serves as the liaison among all state, local and private agencies involved in the child s care. Each child and his or her family are assigned a care coordinator and a multidisciplinary team of providers at the contracted care agency. The care coordinator, in collaboration with the child and family, completes a comprehensive Family-Centered Action Plan (F-CAP) highlighting their needs and desires and updates this plan bimonthly. PFC families felt more confident in their ability to care for their child. Families Quality of Life Caregiving for a child with a life-threatening illness can have a devastating effect on the well-being and confidence of parents and other primary caregivers. A survey of 33 families enrolled in the PFC program was conducted at the time of enrollment (baseline) before receipt of services and after about six months of enrollment (follow up). The survey indicated a decrease in reported frequency of having difficulty sleeping; feeling nervous or tense; and feeling worried. Families also reported an increase in the frequency of feeling confident in their ability to care for their child (Exhibit 4). Notably, all surveyed families reported that care coordination, family education and the 24/7 nurse line were helpful in reducing stress and worry and in increasing confidence in managing their child s condition. Massage therapy for the affected children was noted by all families as helpful in reducing stress, and child life therapy was reported by all families as helpful in reducing worry. Family and Staff Satisfaction With the PFC Program Survey data showed high satisfaction with the program overall and with each of the individual services among both families and providers. When asked to rate the PFC
5 UCLA CENTER FOR HEALTH POLICY RESEARCH 5 Change in Stress, Worry and Confidence Levels Before and After PFC Services Exhibit 4 All the Time Most of the Time Sometimes Occasionally Never Baseline Follow up Difficulty sleeping Worried Nervous/tense Confidence Source: A survey developed by the UCLA Center for Health Policy Research and administered to families by California Children s Services Nurse Liaisons at baseline (enrollment) and follow up (six months after enrollment). Based on 33 surveyed families. program overall on a scale from zero to 10, where 10 indicates excellent care, families and the California Children s Services Nurse Liaisons (CCSNLs) (the liaisons among all agencies involved in the program) rated the PFC services at close to 10 (average 9.6 and 9.8, respectively). Home health agency and hospice representatives rated the PFC program lower at 7.8 on the 10-point scale. However, it should be noted that during the analysis period, only five providers were actively participating in the program and only four of those participated in the survey. It is possible that this rating is affected by what these providers perceive as lower than adequate reimbursement rates for services, an issue that came up in their survey responses as a barrier to provider participation in the PFC program. Nonetheless, ratings of all individual services were high and 97% of the families reported that they would recommend the program to a friend or family member in need. Conclusion and Recommendations Based on preliminary results, there is evidence that the PFC program has reduced costs and improved quality of life. In particular, PFC has had success replacing costly hospital care with less expensive community-based services, a notable accomplishment in this high-needs population. However, these preliminary results must be interpreted with caution until a full analysis at the end of the three-year program is conducted because of the small number of participants and the wide variability of cost among children. Nonetheless, these promising results indicate that the PFC program is providing cost-effective, beneficial services to a vulnerable group of children and their families. Given existing demand, and demand generated should the program expand beyond the current 11 counties, Nearly all PFC families would recommend the program to a friend or family member.
6 6 UCLA CENTER FOR HEALTH POLICY RESEARCH beneficial PFC provides cost-effective, services to a vulnerable group of children. planning to accommodate a larger volume of children and families is needed. In order to ensure the sustainability of the PFC program, policymakers, families and advocates should consider the following recommendations: Encourage the participation of hospice and home health agencies. Availability of providers is key to the PFC program s success. Efforts to retain current providers and recruit new ones should be prioritized. Reimbursement structures, timely reimbursement for services and other potential factors associated with agencies decisions to participate should be examined. For example, currently Medi-Cal reimburses only for the cost of actual service provision. However, service providers incur additional costs in the form of provider training, billing and other administrative expenses. An additional reimbursement to support the agencies administrative costs may provide some incentive to participate. Given the potentially significant cost savings of this program, enhancing reimbursement would still be cost effective. Continue education efforts across settings regarding pediatric palliative care. To ensure referral of children living with a lifethreatening condition, who will be expected to require significant utilization of health services, concentrated efforts should be made to educate the medical community regarding the fairly new practice of community-based pediatric palliative care and the availability of PFC services in participating counties. Starting care earlier on in the continuum of care will improve quality of life and will likely contribute to lowering the cost of care for the child. Develop collaborations and share best practices to simplify referral and enrollment processes. As the program expands, it is important to build on existing partnerships and develop new ones among the state and county California Children s Services (CCS) programs, specialty care centers, other medical and community services, and hospice and home health agencies. Along with planning for CCS staffing needs, sharing best practices among the partners will lead to simplified referral protocols across medical settings and enrollment procedures at the county level, and will develop infrastructure for successful expansion. Methods The cost analyses reported in this policy brief are based on medical costs as measured by standard cost accounting systems using MIS/DSS claims, MEDS and CMS Net data from 2009 until September In order to promote complete claims information, a six-month claims run-out was used. However, unbilled or unpaid claims may be excluded from this analysis, potentially leading to a bias overestimating savings in the program. Analyses are based on 74 children. Due to the preliminary nature of these analyses, the results should be interpreted with caution. To validate these preliminary results, an analysis at the end of the three years operation of the program should be conducted with a difference-in-differences design using full administrative data. The quality of life and family satisfaction analyses reported in this brief are based on surveys developed by the UCLA Center for Health Policy Research and administered by CCSNLs upon enrollment (baseline) and six months after enrollment (follow up). There were 33 families participating in the follow-up survey. The satisfaction of providers analyses reported in this brief are based on a provider survey developed by the UCLA Center for Health Policy Research and administered online. There were nine CCSNL respondents and four home health/hospice agency respondents. Responses may be biased due to the nature of voluntary self-reported data. Author Information Daphna Gans is a research scientist at the UCLA Center for Health Policy Research. Gerald F. Kominski is the director of the UCLA Center for Health Policy Research and a professor in the UCLA Fielding School of Public Health. Dylan H. Roby is the director of the Health Economics and Evaluation Research Program at the UCLA Center for Health Policy Research and an assistant professor in the UCLA Fielding School of Public Health. Allison L. Diamant, MD, MSHS, is a professor in the Division of General Internal Medicine and Health Services Research at the David Geffen School of Medicine at UCLA and a faculty associate at the UCLA Center for Health Policy Research. Xiao Chen is a senior statistician at the UCLA Center for Health Policy Research. Wenjiao Lin is a statistician at the UCLA
7 UCLA CENTER FOR HEALTH POLICY RESEARCH 7 Center for Health Policy Research. Nina Hohe is a public administration analyst at the UCLA Center for Health Policy Research. The UCLA Center for Health Policy Research is one of the nation s leading health policy research centers and the premier source of health policy information for California. Established in 1994, the UCLA Center for Health Policy Research is based in the UCLA Fielding School of Public Health and affiliated with the UCLA Luskin School of Public Affairs. The UCLA Center for Health Policy Research improves the public s health by advancing health policy through research, public service, community partnership and education. Acknowledgments The authors wish to acknowledge Dr. Jill Abramson, Devon Dabbs, Gwendolyn Driscoll, Livier Cabezas and Greg Watson for their helpful reviews. We wish to acknowledge Mark Ramirez of the UCLA Fielding School of Public Health for his work on the PFC Evaluation, Denis Hulett of the California Medicaid Research Institute for his assistance in administrative Medi-Cal data collection, and Brenda Washington and Scott Schmolke of the DHCS Children s Medical Services for their assistance in compiling CCS administrative data and survey data delivery. Funding Information Development of this policy brief was supported by the Children s Hospice & Palliative Care Coalition (CHPCC), which is supported by the California HealthCare Foundation (CHCF). Children s Hospice & Palliative Care Coalition is a nonprofit organization committed to pursuing and implementing cost-effective strategies that ensure a high quality of care for children living with lifethreatening conditions. CHPCC represents children, parents, families and health care providers in its collaboration with community leaders, government officials, legislators and social advocates to improve health care systems. Founded in 2001, CHPCC has successfully initiated programs and policies at the state and local levels that address critical gaps in community-based services for children and their families, including California s new Pediatric Palliative Care Benefit. Endnotes 1 Elias, ER, Murphy, NA, The Council on Children With Disabilities. Home care of children and youth with complex health care needs and technology dependencies. Pediatrics 2012;129(5): Himelstein, BP, et al. Pediatric palliative care. New England Journal of Medicine 2004;350(17): Committee on Palliative and End-of-Life Care for Children and Their Families, Board on Health Sciences Policy, Institute of Medicine. When Children Die: Improving Palliative and End-of-Life Care for Children and their Families. Washington, D.C.: National Academic Press, (c) Home & Community-Based Waivers. 2008; hcbswaivers-section1915(c).asp 5 American Academy of Pediatrics, Committee on Bioethics, Committee on Hospital Care. Palliative care for children. Pediatrics 2000;106(2): Preliminary analysis is based on administrative data for 74 children participating in the program by September The post-enrollment period for each child is composed of the time he or she spent enrolled in the program between January 2010 and September The pre-enrollment period is the 12 months before the child s enrollment. 7 For this population, visits to the emergency room represent a very small expenditure: $4 per member per month (PMPM) before the program, versus $6 PMPM during PFC. Considering this small number and the very minor change between pre- to post-enrollment, the numbers are not included in the exhibits in the brief. 8 In addition, there was a minor ($2) increase in emergency room costs (not shown). 9 Counties were enrolled yearly on a rolling basis from year one to year three (see sidebar for participating counties). Financial eligibility is granted for children with fullscope Medi-Cal coverage. Medical eligibility is decided based on the existence of qualifying California Children s Services (CCS) health condition as well as a set of other more specific medical criteria. The medical eligibility was expanded in 2010 to include children with all CCS eligible life-threatening conditions who are expected to have at least 30 days total per year of hospital service use. Conditions that may qualify a child to receive services include, for example, neoplasm, cardiac, gastrointestinal, neuromuscular, neurological, or pulmonary and other conditions that meet level of care. For more details, please visit the DHCS website at ppc/pages/default.aspx Suggested Citation Gans D, Kominski GF, Roby DH, Diamant AL, Chen X, Lin W and Hohe N. Better Outcomes, Lower Costs: Palliative Care Program Reduces Stress, Costs of Care for Children With Life-Threatening Conditions. Los Angeles, CA: UCLA Center for Health Policy Research, 2012.
8 UCLA CENTER FOR HEALTH POLICY RESEARCH Wilshire Blvd., Suite 1550 Los Angeles, California The UCLA Center for Health Policy Research is affiliated with the UCLA Fielding School of Public Health and the UCLA Luskin School of Public Affairs. The analyses, interpretations, conclusions and views expressed in this policy brief are those of the authors and do not necessarily represent the UCLA Center for Health Policy Research, the Regents of the University of California, DHCS, CHPCC, CHCF or any collaborating organizations or funders. PB Copyright 2012 by the Regents of the University of California. All Rights Reserved. Editor-in-Chief: Gerald F. Kominski, PhD Phone: Fax: Read this publication online
California s Pediatric Palliative Care. Jill Abramson, MD, MPH November 1, 2012
 California s Pediatric Palliative Care Jill Abramson, MD, MPH November 1, 2012 Outline How a program can change a life Pediatric Palliative Care PFC Overview PFC Results Challenges PFC in the future Case
California s Pediatric Palliative Care Jill Abramson, MD, MPH November 1, 2012 Outline How a program can change a life Pediatric Palliative Care PFC Overview PFC Results Challenges PFC in the future Case
Community Health Centers (CHCs)
 Health Policy Brief May 2014 Ready for ACA? How Community Health Centers Are Preparing for Health Care Reform Nadereh Pourat, Max W. Hadler Two in five CHCs have made significant progress toward ACA readiness.
Health Policy Brief May 2014 Ready for ACA? How Community Health Centers Are Preparing for Health Care Reform Nadereh Pourat, Max W. Hadler Two in five CHCs have made significant progress toward ACA readiness.
Center for Labor Research and Education University of California, Berkeley Center for Health Policy Research University of California, Los Angeles
 Center for Labor Research and Education University of California, Berkeley Center for Health Policy Research University of California, Los Angeles School of Public Health University of California, Berkeley
Center for Labor Research and Education University of California, Berkeley Center for Health Policy Research University of California, Los Angeles School of Public Health University of California, Berkeley
Low-Income Health Program (LIHP) Evaluation Proposal
 Low-Income Health Program (LIHP) Evaluation Proposal UCLA Center for Health Policy Research & The California Medicaid Research Institute Background In November of 2010, California s Bridge to Reform 1115
Low-Income Health Program (LIHP) Evaluation Proposal UCLA Center for Health Policy Research & The California Medicaid Research Institute Background In November of 2010, California s Bridge to Reform 1115
Low-Income Health Program (LIHP) Evaluation Proposal
 Low-Income Health Program (LIHP) Evaluation Proposal UCLA Center for Health Policy Research & The California Medicaid Research Institute BACKGROUND In November of 2010, California s Bridge to Reform 1115
Low-Income Health Program (LIHP) Evaluation Proposal UCLA Center for Health Policy Research & The California Medicaid Research Institute BACKGROUND In November of 2010, California s Bridge to Reform 1115
Appendix 11 CCS Physician Survey Tool. CCS Provider Survey
 CCS Provider Survey Q58 The California Children s Services program (otherwise known as CCS), is an important program serving some of our state s most vulnerable children. Federal requirements stipulate
CCS Provider Survey Q58 The California Children s Services program (otherwise known as CCS), is an important program serving some of our state s most vulnerable children. Federal requirements stipulate
1331 Garden Highway Sacramento, CA
 Fiscal Impact of AB 415: Potential Cost Savings from Expansion of Telehealth Matthew Newman & Trisha McMahon, Blue Sky Consulting September 30, 2011 A fiscal analysis of AB 415, The Telehealth Advancement
Fiscal Impact of AB 415: Potential Cost Savings from Expansion of Telehealth Matthew Newman & Trisha McMahon, Blue Sky Consulting September 30, 2011 A fiscal analysis of AB 415, The Telehealth Advancement
California Children s Services Program Redesign:
 California Children s Services Program Redesign: Vision, Goals and Groundwork for the Stakeholder Process September 26, 2014 Agenda 9:30-9:35 Welcome and Introductions Dylan Roby, UCLA 9:35-9:45 Opening
California Children s Services Program Redesign: Vision, Goals and Groundwork for the Stakeholder Process September 26, 2014 Agenda 9:30-9:35 Welcome and Introductions Dylan Roby, UCLA 9:35-9:45 Opening
Whole Person Care Pilots & the Health Home Program
 Whole Person Care Pilots & the Health Home Program Molly Brassil, MSW Director of Behavioral Health Integration, Harbage Consulting December 13, 2016 Presentation Overview Delivery System Reform in California
Whole Person Care Pilots & the Health Home Program Molly Brassil, MSW Director of Behavioral Health Integration, Harbage Consulting December 13, 2016 Presentation Overview Delivery System Reform in California
DMC-ODS. System Transformation. Presented at DHCS 2017 Annual Conference. Elizabeth Stanley-Salazar, MPH Doug Bond Lisa Garcia, LCSW
 DMC-ODS System Transformation Presented at DHCS 2017 Annual Conference Elizabeth Stanley-Salazar, MPH Doug Bond Lisa Garcia, LCSW Objectives Understand managed care principles applied to DMC-ODS Waiver
DMC-ODS System Transformation Presented at DHCS 2017 Annual Conference Elizabeth Stanley-Salazar, MPH Doug Bond Lisa Garcia, LCSW Objectives Understand managed care principles applied to DMC-ODS Waiver
State of California Health and Human Services Agency Department of Health Care Services
 State of California Health and Human Services Agency Department of Health Care Services TOBY DOUGLAS Director EDMUND G. BROWN JR. Governor DATE: OCTOBER 28, 2013 ALL PLAN LETTER 13-014 SUPERSEDES ALL PLAN
State of California Health and Human Services Agency Department of Health Care Services TOBY DOUGLAS Director EDMUND G. BROWN JR. Governor DATE: OCTOBER 28, 2013 ALL PLAN LETTER 13-014 SUPERSEDES ALL PLAN
Heart of Hope Asian America Hospice Care 希望之 心安寧醫護關懷中 心
 Heart of Hope Asian America Hospice Care 希望之 心安寧醫護關懷中 心 Teleconference 2017.01.19 Prepared by: Che-Fai Au (fai@mac.com) Hospice Care through Medicare, Medi-Cal, and Private Insurance Hospice care is a
Heart of Hope Asian America Hospice Care 希望之 心安寧醫護關懷中 心 Teleconference 2017.01.19 Prepared by: Che-Fai Au (fai@mac.com) Hospice Care through Medicare, Medi-Cal, and Private Insurance Hospice care is a
California s Current Section 1115 Waiver & Its Impact on the Public Hospital Safety Net
 February 2010 California s Current Section 1115 Waiver & Its Impact on the Public Hospital Safety Net Executive Summary The current Section 1115 Medicaid waiver, which was intended to stabilize California
February 2010 California s Current Section 1115 Waiver & Its Impact on the Public Hospital Safety Net Executive Summary The current Section 1115 Medicaid waiver, which was intended to stabilize California
Department of Health Care Services
 State of California Department of Health Care Services Streamlining the Cal MediConnect Voluntary Enrollment Experience April 2016 This is one of three documents released by the Department of Health Care
State of California Department of Health Care Services Streamlining the Cal MediConnect Voluntary Enrollment Experience April 2016 This is one of three documents released by the Department of Health Care
A Bridge to Reform: California s Medicaid Section 1115 Waiver
 A Bridge to Reform: California s Medicaid Section 1115 Waiver Prepared for California HealthCare Foundation By Peter Harbage and Meredith Ledford King October 2012 About the Authors Peter Harbage, MPP,
A Bridge to Reform: California s Medicaid Section 1115 Waiver Prepared for California HealthCare Foundation By Peter Harbage and Meredith Ledford King October 2012 About the Authors Peter Harbage, MPP,
The Budget: Maximizing Federal Reimbursement For Parolee Mental Health Care Summary
 The 2013-14 Budget: Maximizing Federal Reimbursement For Parolee Mental Health Care MAC Taylor Legislative Analyst MAY 6, 2013 Summary Historically, the state has spent tens of millions of dollars annually
The 2013-14 Budget: Maximizing Federal Reimbursement For Parolee Mental Health Care MAC Taylor Legislative Analyst MAY 6, 2013 Summary Historically, the state has spent tens of millions of dollars annually
Hospital Specialist Palliative Care Service
 Hospital Specialist Palliative Care Service What is palliative care? Palliative care is an approach that aims to improve the quality of life for patients facing a serious illness and their familes, through
Hospital Specialist Palliative Care Service What is palliative care? Palliative care is an approach that aims to improve the quality of life for patients facing a serious illness and their familes, through
Introduction. Summary of Approved WPC Pilots
 The California Whole Person Care Pilot Program: County Partnerships to Improve the Health of Medi-Cal Beneficiaries Prepared by Lucy Pagel, Tanya Schwartz and Jennifer Ryan with support from The California
The California Whole Person Care Pilot Program: County Partnerships to Improve the Health of Medi-Cal Beneficiaries Prepared by Lucy Pagel, Tanya Schwartz and Jennifer Ryan with support from The California
Overview and Current Status of Program of All-inclusive Care for the Elderly (PACE) Dr. Cheryl Phillips, M.D. Chief Medical Officer, On Lok Lifeways
 Overview and Current Status of Program of All-inclusive Care for the Elderly (PACE) Dr. Cheryl Phillips, M.D. Chief Medical Officer, On Lok Lifeways 1 What is On Lok? Original Vision: Help the low-income
Overview and Current Status of Program of All-inclusive Care for the Elderly (PACE) Dr. Cheryl Phillips, M.D. Chief Medical Officer, On Lok Lifeways 1 What is On Lok? Original Vision: Help the low-income
California Program on Access to Care Findings
 C P A C February California Program on Access to Care Findings 2008 Increasing Health Care Access for the Medically Underserved in Four California Counties Annette Gardner, PhD, MPH Some of the most active
C P A C February California Program on Access to Care Findings 2008 Increasing Health Care Access for the Medically Underserved in Four California Counties Annette Gardner, PhD, MPH Some of the most active
Cindy Cameron Senior Director of Finance & Reimbursement LightBridge Hospice, LLC
 Cindy Cameron Senior Director of Finance & Reimbursement LightBridge Hospice, LLC Kristina Runnels Director Patient Financial Services VITAS Healthcare Corp Medi-Cal Managed Care Program The 3 models of
Cindy Cameron Senior Director of Finance & Reimbursement LightBridge Hospice, LLC Kristina Runnels Director Patient Financial Services VITAS Healthcare Corp Medi-Cal Managed Care Program The 3 models of
hospic Hospice Care 1 Hospice care is a medical multidisciplinary care designed to meet the unique needs of terminally ill individuals.
 Hospice Care 1 Hospice care is a medical multidisciplinary care designed to meet the unique needs of terminally ill individuals. Hospice care is used to alleviate pain and suffering, and treat symptoms
Hospice Care 1 Hospice care is a medical multidisciplinary care designed to meet the unique needs of terminally ill individuals. Hospice care is used to alleviate pain and suffering, and treat symptoms
Long Term Care. Lecture for HS200 Nov 14, 2006
 Long Term Care Lecture for HS200 Nov 14, 2006 Steven P. Wallace, Ph.D. Professor, Dept. Community Health Sciences, SPH and Associate Director, UCLA Center for Health Policy Research What is long-term care
Long Term Care Lecture for HS200 Nov 14, 2006 Steven P. Wallace, Ph.D. Professor, Dept. Community Health Sciences, SPH and Associate Director, UCLA Center for Health Policy Research What is long-term care
Health Home Program (HHP)
 Comparison of California s, Whole Person Care Pilot, Program, and March 16, 2016 This document summarizes and compares four major California initiatives: 1) the Health Homes for Patients with Complex Needs
Comparison of California s, Whole Person Care Pilot, Program, and March 16, 2016 This document summarizes and compares four major California initiatives: 1) the Health Homes for Patients with Complex Needs
(d) (1) Any managed care contractor serving children with conditions eligible under the CCS
 Department of Health Care Services California Children s Services (CCS) Redesign Proposed Statutory Changes July 17, 2015 Proposed Language in Black Text, Bold Underline August 20, 2015 Additional Language
Department of Health Care Services California Children s Services (CCS) Redesign Proposed Statutory Changes July 17, 2015 Proposed Language in Black Text, Bold Underline August 20, 2015 Additional Language
As Reported by the House Aging and Long Term Care Committee. 132nd General Assembly Regular Session Sub. H. B. No
 132nd General Assembly Regular Session Sub. H. B. No. 286 2017-2018 Representative LaTourette Cosponsors: Representatives Arndt, Schaffer, Schuring A B I L L To amend section 3712.01 and to enact sections
132nd General Assembly Regular Session Sub. H. B. No. 286 2017-2018 Representative LaTourette Cosponsors: Representatives Arndt, Schaffer, Schuring A B I L L To amend section 3712.01 and to enact sections
The Honorable Diana Dooley Secretary, California Health and Human Services Agency 1600 Ninth Street, Room 460 Sacramento, CA 95814
 Sutter Health Sutter Medical Center, Sacramento We Plus You 5151 F Street Sacramento, CA 95819 916.733.1038 April 14, 2015 The Honorable Diana Dooley Secretary, California Health and Human Services Agency
Sutter Health Sutter Medical Center, Sacramento We Plus You 5151 F Street Sacramento, CA 95819 916.733.1038 April 14, 2015 The Honorable Diana Dooley Secretary, California Health and Human Services Agency
s n a p s h o t Medi-Cal at a Crossroads: What Enrollees Say About the Program
 s n a p s h o t Medi-Cal at a Crossroads: What Enrollees Say About the Program May 2012 Introduction Medi-Cal, which currently provides health and long term care coverage for more than 7.5 million Californians,
s n a p s h o t Medi-Cal at a Crossroads: What Enrollees Say About the Program May 2012 Introduction Medi-Cal, which currently provides health and long term care coverage for more than 7.5 million Californians,
SECTION 7. The Changing Health Care Marketplace
 SECTION 7 The Changing Health Care Marketplace This section provides an overview of the health care markets in and the, including data on HMO enrollment, trends and information about hospitals and nursing
SECTION 7 The Changing Health Care Marketplace This section provides an overview of the health care markets in and the, including data on HMO enrollment, trends and information about hospitals and nursing
Client-Provider Interactions About Screening and Referral to Primary Care Services and Health Insurance Programs
 Research Brief on Client-Provider Interactions About Screening and Referral to Primary Care Services and Health Insurance Programs March 2014 Suggested citation: Sara Daniel, MPH; Antonia Biggs, PhD; Jan
Research Brief on Client-Provider Interactions About Screening and Referral to Primary Care Services and Health Insurance Programs March 2014 Suggested citation: Sara Daniel, MPH; Antonia Biggs, PhD; Jan
FEE FOR SERVICE MEASURES
 FEE FOR SERVICE MEASURES Fee for Service (FFS) Measures provide a single payment incentive to PCP sites in exchange for performing a service or activity. All 2018 measures require providers to submit a
FEE FOR SERVICE MEASURES Fee for Service (FFS) Measures provide a single payment incentive to PCP sites in exchange for performing a service or activity. All 2018 measures require providers to submit a
State of California Health and Human Services Agency Department of Health Care Services
 State of California Health and Human Services Agency Department of Health Care Services TOBY DOUGLAS Director EDMUND G. BROWN JR. Governor DATE: JUNE 26, 2014 ALL PLAN LETTER 14-007 TO: ALL MEDI-CAL MANAGED
State of California Health and Human Services Agency Department of Health Care Services TOBY DOUGLAS Director EDMUND G. BROWN JR. Governor DATE: JUNE 26, 2014 ALL PLAN LETTER 14-007 TO: ALL MEDI-CAL MANAGED
Medi-cal Part 2 Provider Manual For Soc Billing Instructions
 Medi-cal Part 2 Provider Manual For Soc Billing Instructions Medi-Cal Provider Manual Contents 7,265 Bytes How to Use This Manual (0Bhwtouse) 18,979 Bytes Contents (Part 2 Medi-Cal Billing and Policy):
Medi-cal Part 2 Provider Manual For Soc Billing Instructions Medi-Cal Provider Manual Contents 7,265 Bytes How to Use This Manual (0Bhwtouse) 18,979 Bytes Contents (Part 2 Medi-Cal Billing and Policy):
Medicare. Costs and Financing of Medicare Enrollees Living with HIV/AIDS in California by June Eichner and James G. Kahn
 August 2001 No. 8 Medicare Brief Costs and Financing of Medicare Enrollees Living with HIV/AIDS in California by June Eichner and James G. Kahn Summary Because Medicare does not cover a large part of the
August 2001 No. 8 Medicare Brief Costs and Financing of Medicare Enrollees Living with HIV/AIDS in California by June Eichner and James G. Kahn Summary Because Medicare does not cover a large part of the
Same Disease, Different Care: How Patient Health Coverage Drives Treatment Patterns in California. The analysis includes:
 Same Disease, Different Care: How Patient Health Coverage Drives Treatment Patterns in California C A L I FOR N I A HEALTHCARE FOUNDATION Introduction As shown in The 2005 Dartmouth Atlas of Health Care,
Same Disease, Different Care: How Patient Health Coverage Drives Treatment Patterns in California C A L I FOR N I A HEALTHCARE FOUNDATION Introduction As shown in The 2005 Dartmouth Atlas of Health Care,
Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps
 I S S U E P A P E R kaiser commission on medicaid and the uninsured March 2004 Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps In 2000, over 7 million people were dual eligibles, low-income
I S S U E P A P E R kaiser commission on medicaid and the uninsured March 2004 Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps In 2000, over 7 million people were dual eligibles, low-income
Medi-Cal and the Safety Net California Association of Health Plans Seminar Series Medi-Cal at its Core
 Medi-Cal and the Safety Net California Association of Health Plans Seminar Series Medi-Cal at its Core August 3, 2017 Deborah Kelch Executive Director Insure the Uninsured Project 1 Safety-Net Definitions
Medi-Cal and the Safety Net California Association of Health Plans Seminar Series Medi-Cal at its Core August 3, 2017 Deborah Kelch Executive Director Insure the Uninsured Project 1 Safety-Net Definitions
Hospice Care for anyone considering hospice
 A decision aid for Care for anyone considering hospice You or a loved one have been diagnosed with a serious illness that might not be curable. Many people find this scary or confusing. Some people feel
A decision aid for Care for anyone considering hospice You or a loved one have been diagnosed with a serious illness that might not be curable. Many people find this scary or confusing. Some people feel
Improving Access to Specialty Care. Janet M. Coffman, MPP, PhD Center for the Health Professions Philip R. Lee Institute for Health Policy Studies
 Improving Access to Specialty Care Janet M. Coffman, MPP, PhD Center for the Health Professions Philip R. Lee Institute for Health Policy Studies Outline State of access to specialty care for low-income
Improving Access to Specialty Care Janet M. Coffman, MPP, PhD Center for the Health Professions Philip R. Lee Institute for Health Policy Studies Outline State of access to specialty care for low-income
CALIFORNIA HEALTHCARE FOUNDATION. Medi-Cal Versus Employer- Based Coverage: Comparing Access to Care JULY 2015 (REVISED JANUARY 2016)
 CALIFORNIA HEALTHCARE FOUNDATION Medi-Cal Versus Employer- Based Coverage: Comparing Access to Care JULY 2015 (REVISED JANUARY 2016) Contents About the Authors Tara Becker, PhD, is a statistician at the
CALIFORNIA HEALTHCARE FOUNDATION Medi-Cal Versus Employer- Based Coverage: Comparing Access to Care JULY 2015 (REVISED JANUARY 2016) Contents About the Authors Tara Becker, PhD, is a statistician at the
FACT SHEET Low Income Assistance: Cal MediConnect (E-004) p. 1 of 6
 FACT SHEET Low Income Assistance: Cal MediConnect (E-004) p. 1 of 6 Low Income Assistance: Cal MediConnect What is Cal MediConnect? California is one of 12 states that has signed a Memorandum of Understanding
FACT SHEET Low Income Assistance: Cal MediConnect (E-004) p. 1 of 6 Low Income Assistance: Cal MediConnect What is Cal MediConnect? California is one of 12 states that has signed a Memorandum of Understanding
FACT SHEET Low Income Assistance: Cal MediConnect(E-004) p. 1 of 6
 FACT SHEET Low Income Assistance: Cal MediConnect(E-004) p. 1 of 6 Low Income Assistance: Cal MediConnect What is Cal MediConnect? California is 1 of 15 states that has signed a Memorandum of Understanding
FACT SHEET Low Income Assistance: Cal MediConnect(E-004) p. 1 of 6 Low Income Assistance: Cal MediConnect What is Cal MediConnect? California is 1 of 15 states that has signed a Memorandum of Understanding
Variables that impact the cost of delivering SB 1004 palliative care services. Kathleen Kerr, BA Kerr Healthcare Analytics September 28, 2017
 Variables that impact the cost of delivering SB 1004 palliative care services Kathleen Kerr, BA Kerr Healthcare Analytics September 28, 2017 SB 1004 Palliative Care SB 1004 (Hernandez, Chapter 574, Statutes
Variables that impact the cost of delivering SB 1004 palliative care services Kathleen Kerr, BA Kerr Healthcare Analytics September 28, 2017 SB 1004 Palliative Care SB 1004 (Hernandez, Chapter 574, Statutes
I. Coordinating Quality Strategies Across Managed Care Plans
 Jennifer Kent Director California Department of Health Care Services 1501 Capitol Avenue Sacramento, CA 95814 SUBJECT: California Department of Health Care Services Medi-Cal Managed Care Quality Strategy
Jennifer Kent Director California Department of Health Care Services 1501 Capitol Avenue Sacramento, CA 95814 SUBJECT: California Department of Health Care Services Medi-Cal Managed Care Quality Strategy
ACOs: California Style
 ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
ECONOMIC EVALUATION OF PALLIATIVE CARE IN IRELAND
 ECONOMIC EVALUATION OF PALLIATIVE CARE IN IRELAND 2015 AUTHORS Aoife Brick, Charles Normand, Sinéad O Hara, Samantha Smith Evidence from this study shows that more developed palliative care reduces the
ECONOMIC EVALUATION OF PALLIATIVE CARE IN IRELAND 2015 AUTHORS Aoife Brick, Charles Normand, Sinéad O Hara, Samantha Smith Evidence from this study shows that more developed palliative care reduces the
Senate Bill No. 586 CHAPTER 625
 Senate Bill No. 586 CHAPTER 625 An act to amend Sections 123835 and 123850 of the Health and Safety Code, and to amend Sections 14093.06, 14094.2, and 14094.3 of, and to add Article 2.985 (commencing with
Senate Bill No. 586 CHAPTER 625 An act to amend Sections 123835 and 123850 of the Health and Safety Code, and to amend Sections 14093.06, 14094.2, and 14094.3 of, and to add Article 2.985 (commencing with
Re: California Health+ Advocates opposes the proposed state budget changes to the 340B program
 May 2, 2017 René Mollow, Deputy Director Health Care Benefits and Eligibility Department of Health Care Services 1501 Capitol Avenues, MS 0007 P.O. Box 997413 Sacramento, CA 95899-7413 Re: California Health+
May 2, 2017 René Mollow, Deputy Director Health Care Benefits and Eligibility Department of Health Care Services 1501 Capitol Avenues, MS 0007 P.O. Box 997413 Sacramento, CA 95899-7413 Re: California Health+
Medi-Cal s Most Costly FFS Populations
 Medi-Cal s Most Costly FFS Populations A Look At The Population, Costs, And Diseases Prepared by DHCS Research and Analytical Studies Section 1 Which Populations Drive Medi-Cal FFS Provider Payments? The
Medi-Cal s Most Costly FFS Populations A Look At The Population, Costs, And Diseases Prepared by DHCS Research and Analytical Studies Section 1 Which Populations Drive Medi-Cal FFS Provider Payments? The
Federal Legislation to Address the Opioid Crisis: Medicaid Provisions in the SUPPORT Act
 October 2018 Issue Brief Federal Legislation to Address the Opioid Crisis: Medicaid Provisions in the SUPPORT Act MaryBeth Musumeci and Jennifer Tolbert On October 3, 2018, the Senate overwhelmingly passed
October 2018 Issue Brief Federal Legislation to Address the Opioid Crisis: Medicaid Provisions in the SUPPORT Act MaryBeth Musumeci and Jennifer Tolbert On October 3, 2018, the Senate overwhelmingly passed
Provider Relations Training
 Cal MediConnect Provider Relations Training Presented by Victor Gonzalez and George Scolari Provider Relations Training Agenda Overview of Cal MediConnect Eligibility & Exclusions Enrollment & Disenrollment
Cal MediConnect Provider Relations Training Presented by Victor Gonzalez and George Scolari Provider Relations Training Agenda Overview of Cal MediConnect Eligibility & Exclusions Enrollment & Disenrollment
DHCS Update: Major Initiatives and Strategies Towards Standardization
 DHCS Update: Major Initiatives and Strategies Towards Standardization Javier Portela, Division Chief Managed Care Operations Department of Health Care Services ICE 2016 Annual Conference December 2016
DHCS Update: Major Initiatives and Strategies Towards Standardization Javier Portela, Division Chief Managed Care Operations Department of Health Care Services ICE 2016 Annual Conference December 2016
MHP Work Plan: 1 Behavioral Health Integrated Access
 PROGRAM INFORMATION: Program Title: Youth Wellness Center Provider: Department of Behavioral Health Program Description: The Department of Behavioral Health (DBH) Youth Wellness Center is designed to improve
PROGRAM INFORMATION: Program Title: Youth Wellness Center Provider: Department of Behavioral Health Program Description: The Department of Behavioral Health (DBH) Youth Wellness Center is designed to improve
CHAPTER 7 CONTEXTUAL ANALYSIS OF CARVE-OUT POLICY
 CHAPTER 7 CONTEXTUAL ANALYSIS OF CARVE-OUT POLICY As discussed in Chapter 4 (Research Design and Methods), the contextual analysis of the carve-out policy examines the experiences and observations of CCS
CHAPTER 7 CONTEXTUAL ANALYSIS OF CARVE-OUT POLICY As discussed in Chapter 4 (Research Design and Methods), the contextual analysis of the carve-out policy examines the experiences and observations of CCS
About the National Standards for CYSHCN
 National Standards for Systems of Care for Children and Youth with Special Health Care Needs: Crosswalk to National Committee for Quality Assurance Primary Care Medical Home Recognition Standards Kate
National Standards for Systems of Care for Children and Youth with Special Health Care Needs: Crosswalk to National Committee for Quality Assurance Primary Care Medical Home Recognition Standards Kate
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction
 FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association 1 Agenda Incentives in PPS: what does
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association 1 Agenda Incentives in PPS: what does
10/6/2017. FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction. Agenda. Incentives in PPS: what does excludable mean?
 FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association Agenda Incentives in PPS: what does excludable
FQHC Incentive Payments: A Critical Practice for Quality and Patient Satisfaction Meaghan McCamman Assistant Director of Policy California Primary Care Association Agenda Incentives in PPS: what does excludable
Appendix 3: PPACA Provider Questions and Answers from CMS
 Appendix 3: PPACA Provider Questions and Answers from CMS Patient Protection and Affordable Care Act (PPACA) Section 2302: Concurrent Care for Children PROVIDER QUESTIONS AND ANSWERS FROM CMS FEBRUARY
Appendix 3: PPACA Provider Questions and Answers from CMS Patient Protection and Affordable Care Act (PPACA) Section 2302: Concurrent Care for Children PROVIDER QUESTIONS AND ANSWERS FROM CMS FEBRUARY
HEALTHY FAMILIES PROGRAM TRANSITION TO MEDI-CAL
 HEALTHY FAMILIES PROGRAM TRANSITION TO MEDI-CAL NETWORK ADEQUACY ASSESSMENT REPORT PHASE 1 November 1, 2012 Submitted by the California Department of Managed Health Care in Fulfillment of the Requirements
HEALTHY FAMILIES PROGRAM TRANSITION TO MEDI-CAL NETWORK ADEQUACY ASSESSMENT REPORT PHASE 1 November 1, 2012 Submitted by the California Department of Managed Health Care in Fulfillment of the Requirements
Sutter Health Sutter Maternity & Surgery Center of Santa Cruz
 Sutter Health Sutter Maternity & Surgery Center of Santa Cruz 2016 2018 Implementation Strategy Responding to the 2016 Community Health Needs Assessment Sutter Maternity & Surgery Center of Santa Cruz
Sutter Health Sutter Maternity & Surgery Center of Santa Cruz 2016 2018 Implementation Strategy Responding to the 2016 Community Health Needs Assessment Sutter Maternity & Surgery Center of Santa Cruz
HOSPICE IN MINNESOTA: A RURAL PROFILE
 JUNE 2003 HOSPICE IN MINNESOTA: A RURAL PROFILE Background Numerous national polls have found that when asked, most people would prefer to die in their own homes. 1 Contrary to these wishes, 75 percent
JUNE 2003 HOSPICE IN MINNESOTA: A RURAL PROFILE Background Numerous national polls have found that when asked, most people would prefer to die in their own homes. 1 Contrary to these wishes, 75 percent
2015 Summary of Benefits
 2015 Summary of Benefits Health Net Cal MediConnect Plan (Medicare-Medicaid Plan) Los Angeles County, CA H3237_2015_0291 CMS Accepted 09082014 Health Net Cal MediConnect Summary of Benefits! This is a
2015 Summary of Benefits Health Net Cal MediConnect Plan (Medicare-Medicaid Plan) Los Angeles County, CA H3237_2015_0291 CMS Accepted 09082014 Health Net Cal MediConnect Summary of Benefits! This is a
National Hospice and Palliative Care OrganizatioN. Facts AND Figures. Hospice Care in America. NHPCO Facts & Figures edition
 National Hospice and Palliative Care OrganizatioN Facts AND Figures Hospice Care in America 2017 Edition NHPCO Facts & Figures - 2017 edition Table of Contents 2 Introduction 2 About this report 2 What
National Hospice and Palliative Care OrganizatioN Facts AND Figures Hospice Care in America 2017 Edition NHPCO Facts & Figures - 2017 edition Table of Contents 2 Introduction 2 About this report 2 What
Impact of Enrolling in Health Insurance on Low-Income Children that Enrolled for a Medical Reason
 Impact of Enrolling in Health Insurance on Low-Income Children that Enrolled for a Medical Reason Prepared for: Prepared by Moira Inkelas and Patricia Barreto The University of California at Los Angeles
Impact of Enrolling in Health Insurance on Low-Income Children that Enrolled for a Medical Reason Prepared for: Prepared by Moira Inkelas and Patricia Barreto The University of California at Los Angeles
Partnering with Hospice: Reducing Skilled Nursing Facility to Hospital Readmissions
 Partnering with Hospice: Reducing Skilled Nursing Facility to Hospital Readmissions Scott Lavis, LICSW, CT Community Liaison Kline Galland Hospice Objectives for Today Quick review of regulations that
Partnering with Hospice: Reducing Skilled Nursing Facility to Hospital Readmissions Scott Lavis, LICSW, CT Community Liaison Kline Galland Hospice Objectives for Today Quick review of regulations that
Medi-Cal Managed Care Time and Distance Standards for Providers
 California s protection & advocacy system Medi-Cal Managed Care Time and Distance Standards for Providers May 2018, Pub. #5610.01 Medi-Cal Managed Care Time and Distance Standards for Providers To ensure
California s protection & advocacy system Medi-Cal Managed Care Time and Distance Standards for Providers May 2018, Pub. #5610.01 Medi-Cal Managed Care Time and Distance Standards for Providers To ensure
MHP Work Plan: 4-Behavioral health clinical care
 PROGRAM INFORMATION: Program Title: School Based Metro (MHSA) Provider: Department of Behavioral Health The Department of Behavioral Health (DBH) Metro School Based Team (MSBT) is designed to deliver outpatient
PROGRAM INFORMATION: Program Title: School Based Metro (MHSA) Provider: Department of Behavioral Health The Department of Behavioral Health (DBH) Metro School Based Team (MSBT) is designed to deliver outpatient
Local Solutions for Serving the Remaining Uninsured: Benefits and Financing
 Local Solutions for Serving the Remaining Uninsured: Benefits and Financing Presenters: Bob Brownstein, Working Partnerships USA Cynthia Carmona, Community Clinic Association of Los Angeles County David
Local Solutions for Serving the Remaining Uninsured: Benefits and Financing Presenters: Bob Brownstein, Working Partnerships USA Cynthia Carmona, Community Clinic Association of Los Angeles County David
State Policy Report #47. October Health Center Payment Reform: State Initiatives to Meet the Triple Aim. Introduction
 Health Center Payment Reform: State Initiatives to Meet the Triple Aim State Policy Report #47 October 2013 Introduction Policymakers at both the federal and state levels are focusing on how best to structure
Health Center Payment Reform: State Initiatives to Meet the Triple Aim State Policy Report #47 October 2013 Introduction Policymakers at both the federal and state levels are focusing on how best to structure
California s Coordinated Care Initiative: An Update
 California s Coordinated Care Initiative: An Update Background On April 1, 2014, health plans in selected counties began enrolling beneficiaries as part of the Coordinated Care Initiative. This fact sheet
California s Coordinated Care Initiative: An Update Background On April 1, 2014, health plans in selected counties began enrolling beneficiaries as part of the Coordinated Care Initiative. This fact sheet
Personal Responsibility in Medicaid
 Personal Responsibility in Medicaid Chris Perrone Director, Improving Access HMA Conference 2017 The Future of Medicaid Is Here September 12, 2017 3 Questions Context: What problems are we trying to solve?
Personal Responsibility in Medicaid Chris Perrone Director, Improving Access HMA Conference 2017 The Future of Medicaid Is Here September 12, 2017 3 Questions Context: What problems are we trying to solve?
Alternative Managed Care Reimbursement Models
 Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
California Children s Services (CCS) Program Medi-Cal Managed Care CCS Whole-Child Model Comparison Chart January 6, 2016
 California Children s Services (CCS) Program Medi-Cal Managed Care CCS Whole-Child Model Comparison Chart January 6, 2016 Authorization for Services Plan to adjudicate authorization request. Authorization
California Children s Services (CCS) Program Medi-Cal Managed Care CCS Whole-Child Model Comparison Chart January 6, 2016 Authorization for Services Plan to adjudicate authorization request. Authorization
Today s Agenda. Morning. Afternoon
 Today s Agenda Morning Background and Introductions State and Local Policy Updates Break Lessons Learned from the Teen Health Care Pipeline Program in South Los Angeles Break The Full Restoration of Adult
Today s Agenda Morning Background and Introductions State and Local Policy Updates Break Lessons Learned from the Teen Health Care Pipeline Program in South Los Angeles Break The Full Restoration of Adult
Navigating the Hospital Readmission Reduction Program
 Navigating the Hospital Readmission Reduction Program Since the Affordable Care Act passed in 2010, a hospital s 30-day readmission rate has become synonymous with quality of care. Beginning in 2012, the
Navigating the Hospital Readmission Reduction Program Since the Affordable Care Act passed in 2010, a hospital s 30-day readmission rate has become synonymous with quality of care. Beginning in 2012, the
CARE COORDINATION PROJECT
 CARE COORDINATION PROJECT Improving Care Coordination for Patients Diagnosed with Congestive Heart Failure, Diabetes and Hypertension History Objectives CONTENTS Implementation and Information Technology
CARE COORDINATION PROJECT Improving Care Coordination for Patients Diagnosed with Congestive Heart Failure, Diabetes and Hypertension History Objectives CONTENTS Implementation and Information Technology
HEALTH CARE TEAM SACRAMENTO S MENTAL HEALTH CRISIS
 Team Leader/Issue Contact: HEALTH CARE TEAM Laura Niznik Williams, UC Davis Health System, (916) 276-9078, ljniznik@ucdavis.edu SACRAMENTO S MENTAL HEALTH CRISIS Requested Action: Evaluate the Institutions
Team Leader/Issue Contact: HEALTH CARE TEAM Laura Niznik Williams, UC Davis Health System, (916) 276-9078, ljniznik@ucdavis.edu SACRAMENTO S MENTAL HEALTH CRISIS Requested Action: Evaluate the Institutions
The Status of the Implementation of Medi-Cal Mental Health Services
 FEBRUARY 2015 The Status of the Implementation of Medi-Cal Mental Health Services Background: Implementing Expanded Mental Health Services for Medi-Cal Beneficiaries Mental Health and Substance Use Disorder
FEBRUARY 2015 The Status of the Implementation of Medi-Cal Mental Health Services Background: Implementing Expanded Mental Health Services for Medi-Cal Beneficiaries Mental Health and Substance Use Disorder
Central Ohio Primary Care (COPC) Spotlight on Innovation
 Central Ohio Primary Care (COPC) Spotlight on Innovation BY BETTER MEDICARE ALLIANCE MARCH 2017 Central Ohio Primary Care Spotlight on Innovation 1 Central Ohio Primary Care (COPC) Spotlight on Innovation
Central Ohio Primary Care (COPC) Spotlight on Innovation BY BETTER MEDICARE ALLIANCE MARCH 2017 Central Ohio Primary Care Spotlight on Innovation 1 Central Ohio Primary Care (COPC) Spotlight on Innovation
MINUTES. Santa Clara County Health Authority Annual Governing Board Retreat
 Board members present: Ms. Michele Lew Dr. Dale Rai Dr. Wally Wenner Ms. Emily Harrison Ms. Laura Jones Mr. Daniel Peddycord Ms. Linda Williams Ms. Pattie DeMellopine Ms. Liz Kniss Ms. Dolores Alvarado
Board members present: Ms. Michele Lew Dr. Dale Rai Dr. Wally Wenner Ms. Emily Harrison Ms. Laura Jones Mr. Daniel Peddycord Ms. Linda Williams Ms. Pattie DeMellopine Ms. Liz Kniss Ms. Dolores Alvarado
Administrators. Medical Directors. 61% The negative impact on our hospital-based program s. 44% We will need to consider the most appropriate or most
 2016 This annual survey, which began in 2009, provides key insight into nationwide developments in the business of cancer care. To better capture information from its multidisciplinary membership, this
2016 This annual survey, which began in 2009, provides key insight into nationwide developments in the business of cancer care. To better capture information from its multidisciplinary membership, this
Medi-Cal Eligibility: History, ACA Changes and Challenges
 Medi-Cal Eligibility: History, ACA Changes and Challenges PRESENTATION TO CAHP SEMINAR CATHY SENDERLING-MCDONALD, CWDA FEBRUARY 26, 2015 1 Presentation Overview What is CWDA? Medi-Cal Eligibility Overview
Medi-Cal Eligibility: History, ACA Changes and Challenges PRESENTATION TO CAHP SEMINAR CATHY SENDERLING-MCDONALD, CWDA FEBRUARY 26, 2015 1 Presentation Overview What is CWDA? Medi-Cal Eligibility Overview
The influx of newly insured Californians through
 January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
Medicaid Efficiency and Cost-Containment Strategies
 Medicaid Efficiency and Cost-Containment Strategies Medicaid provides comprehensive health services to approximately 2 million Ohioans, including low-income children and their parents, as well as frail
Medicaid Efficiency and Cost-Containment Strategies Medicaid provides comprehensive health services to approximately 2 million Ohioans, including low-income children and their parents, as well as frail
Survey of Ontario Clinics Providing Concussion Services
 Survey of Ontario Clinics Providing Concussion Services Conducted by the Institute for Social Research, York University, for the Ontario Neurotrauma Foundation 2016 Purpose Characterize concussion care
Survey of Ontario Clinics Providing Concussion Services Conducted by the Institute for Social Research, York University, for the Ontario Neurotrauma Foundation 2016 Purpose Characterize concussion care
End of Life Care. LONDON: The Stationery Office Ordered by the House of Commons to be printed on 24 November 2008
 End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
End of Life Care LONDON: The Stationery Office 14.35 Ordered by the House of Commons to be printed on 24 November 2008 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1043 Session 2007-2008 26 November
SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program
 California s Protection & Advocacy System Toll-Free (800) 776-5746 SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program December 2013, Pub #F077.01 SB 468 1 creates a state-wide
California s Protection & Advocacy System Toll-Free (800) 776-5746 SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program December 2013, Pub #F077.01 SB 468 1 creates a state-wide
California Community Clinics
 California Community Clinics A Financial and Operational Profile, 2008 2011 Prepared by Sponsored by Blue Shield of California Foundation and The California HealthCare Foundation TABLE OF CONTENTS Introduction
California Community Clinics A Financial and Operational Profile, 2008 2011 Prepared by Sponsored by Blue Shield of California Foundation and The California HealthCare Foundation TABLE OF CONTENTS Introduction
CA1 Enhanced Supportive Care for Advanced Cancer Patients
 CA1 Enhanced Supportive Care for Advanced Cancer Patients Scheme Name QIPP Reference Eligible Providers CA1 Enhanced Supportive Care (ESC) Access for Advanced Cancer Patients QIPP 16-17 S23- Cancer Cancer
CA1 Enhanced Supportive Care for Advanced Cancer Patients Scheme Name QIPP Reference Eligible Providers CA1 Enhanced Supportive Care (ESC) Access for Advanced Cancer Patients QIPP 16-17 S23- Cancer Cancer
Physician Participation in Medi-Cal,
 Physician Participation in Medi-Cal, 1996 1998 February 2002 Andrew B. Bindman, M.D. William Huen Karen Vranizan, M.A. Jean Yoon, M.H.S. Kevin Grumbach, M.D. Center for California Health Workforce Studies
Physician Participation in Medi-Cal, 1996 1998 February 2002 Andrew B. Bindman, M.D. William Huen Karen Vranizan, M.A. Jean Yoon, M.H.S. Kevin Grumbach, M.D. Center for California Health Workforce Studies
UPDATE ON THE IMPLEMENTATION OF CALIFORNIA S COORDINATED CARE INITIATIVE
 UPDATE ON THE IMPLEMENTATION OF CALIFORNIA S COORDINATED CARE INITIATIVE Eileen Kunz Chief of Government Affairs & Compliance On Lok Carol Hubbard Executive Director of Home & Community Services St. Paul
UPDATE ON THE IMPLEMENTATION OF CALIFORNIA S COORDINATED CARE INITIATIVE Eileen Kunz Chief of Government Affairs & Compliance On Lok Carol Hubbard Executive Director of Home & Community Services St. Paul
Department of Health & Human Services Division of Behavioral Health Services Alcohol & Drug Services. Uma K. Zykofsky, LCSW Behavioral Health Director
 Department of Health & Human Services Division of Behavioral Health Services Alcohol & Drug Services April 24, 2017 Presentation to Geographic Managed Care Providers Uma K. Zykofsky, LCSW Behavioral Health
Department of Health & Human Services Division of Behavioral Health Services Alcohol & Drug Services April 24, 2017 Presentation to Geographic Managed Care Providers Uma K. Zykofsky, LCSW Behavioral Health
HPSM Medi-Cal Benefits A Guide on How to Get Your Health Care
 HPSM Medi-Cal Benefits A Guide on How to Get Your Health Care Health care and insurance benefits can be difficult to understand. This guide introduces you to your basic Medi-Cal benefits, to the Health
HPSM Medi-Cal Benefits A Guide on How to Get Your Health Care Health care and insurance benefits can be difficult to understand. This guide introduces you to your basic Medi-Cal benefits, to the Health
Undocumented Latinos in the San Joaquin Valley: Health Care Access and the Impact on Safety Net Providers
 Undocumented Latinos in the San Joaquin Valley: Health Care Access and the Impact on Safety Net Providers John A. Capitman, PhD Diana Traje, MPH Tania L. Pacheco, ABD California Program on Access to Care
Undocumented Latinos in the San Joaquin Valley: Health Care Access and the Impact on Safety Net Providers John A. Capitman, PhD Diana Traje, MPH Tania L. Pacheco, ABD California Program on Access to Care
A Health Care Innovation Grant Project: A Collaboration of Contra Costa County EHSD Aging & Adult Services Bureau and the Contra Costa Health Plan
 A Health Care Innovation Grant Project: A Collaboration of Contra Costa County EHSD Aging & Adult Services Bureau and the Contra Costa Health Plan La Valda R. Marshall EXECUTIVE SUMMARY Teamwork is the
A Health Care Innovation Grant Project: A Collaboration of Contra Costa County EHSD Aging & Adult Services Bureau and the Contra Costa Health Plan La Valda R. Marshall EXECUTIVE SUMMARY Teamwork is the
Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum
 Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum Betsy Gornet, FACHE Chief Advanced Illness Management Executive Sutter Health / Sutter Care
Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum Betsy Gornet, FACHE Chief Advanced Illness Management Executive Sutter Health / Sutter Care
RESPITE CARE LEGACY HOSPICE
 RESPITE CARE LEGACY HOSPICE THE BASICS OF RESPITE CARE WHAT IS RESPITE? Short-term inpatient care provided only when necessary to relieve the family members or other persons caring for the individual at
RESPITE CARE LEGACY HOSPICE THE BASICS OF RESPITE CARE WHAT IS RESPITE? Short-term inpatient care provided only when necessary to relieve the family members or other persons caring for the individual at
Member Services Director
 Central Coast Alliance for Health September 2006 Duty Statement page 1 Member Services Director 1. Responsible for senior management and strategic planning for the Member Services Department, including
Central Coast Alliance for Health September 2006 Duty Statement page 1 Member Services Director 1. Responsible for senior management and strategic planning for the Member Services Department, including
SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program
 California s Protection & Advocacy System Toll-Free (800) 776-5746 SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program December 2013, Pub #F077.01 SB 468 1 creates a state-wide
California s Protection & Advocacy System Toll-Free (800) 776-5746 SB 468 (Emmerson/Beall/Mitchell/Chesbro) Statewide Self-Determination Program December 2013, Pub #F077.01 SB 468 1 creates a state-wide
Evolution of ACOs in California. Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D.
 Evolution of ACOs in California Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D. Integrated Healthcare Association Statewide multi stakeholder leadership group that promotes quality
Evolution of ACOs in California Accountable Care Congress Los Angeles November 11, 2014 Jill Yegian, Ph.D. Integrated Healthcare Association Statewide multi stakeholder leadership group that promotes quality
