Measuring Quailty of care for Medicare Advantage, Accountable Care Organizations and Insurance Companies. by James L.
|
|
|
- George Hubbard
- 5 years ago
- Views:
Transcription
1 Measuring Quailty of care for Medicare Advantage, Accountable Care Organizations and Insurance Companies by James L. Holly, MD In SETMA s February, 2015 provider training, we will continue the disucssion we briefly had on January 22 nd about the benefits SETMA receives from fulfilling a number of quality metrics which are defined by The Healthcare Effectiveness Data and Information Set ). A registered trademark of the National Committee for Qualtiy Assurance (NCQA), was originally titled the "HMO Employer Data and Information Set" as of version 1.0 of In 1993, Version 2.0 of was known as the "Health Plan Employer Data and Information Set". Version 3.0 of was released in In July 2007, NCQA announced that the meaning of " " would be changed to "Healthcare Effectiveness Data and Information Set." ) is a widely used set of performance measures which are used by over 90 health insurance programs in order to measure the whether the purchasers of healthcare, generally employers, are getting their money s worth with the services they are buying. The 75 measures are divided into six "domains of care": 1. Effectiveness of Care 2. Access/Availability of Care 3. Experience of Care 4. Utilization and Relative Resource Use 5. Health Plan Descriptive Information Only the first of these domains is directly dependent upon the healthcare provider s performance. The measures for quality performance in effectiveness of care are divided into three categories: 1. Effectiveness of Acute Care 2. Effectiveness of Preventive Care 3. Effectiveness of Chronic Care Historically, healthcare providers care was audited on the standard by companies hired by insurance carriers who did chart audits to determine how providers were performing. 1
2 Typically, providers received their results months after the audited services were delivered. While the purpose of was to measure quality, did not affect quality as very few healthcare providers knew what HEDIS measures were and being published one to two years after the care was delivered, providers largely did not care. As emphasis on quality and safety increased, and as more and more emphasis was placed on both for the purposes of payment, interest in and other quality metrics also increased. In 1999, SETMA determined that the only way we were going to sustain improvements in the quality of the care we provide was to measure that quality ourselves. In 2000, we realized that in order to improve we had to know the standard on the basis of which we were being judged. In 2005, we began tracking our performance on measures internally. In 2009, SETMA began to publicly report by provider name on our performance on measures. The following is the rationale for the above. SETMA determined that if we were going to be: 1. Given a test 2. Where the test questions were going to be given to us before the test 3. Where the test is an open book test 4. Where there is no time limited set on taking the test Why not look up the answers before the test? Furthermore, in that the purpose of the test should not only be to evaluate the one being tested but also hopefully to teach the one being tested, it is necessary for the provider to know his/her performance at the point of care. This means that if is going to affect the quality and safety of the care being given, the provider has to know how he/she is performing on at the time the care is being given. The foundation of the quality measurements for ACO payments and for enhanced payments for Medicare Advantage on the basis of the STARS rating system is This presentation summaries SETMA s deployment of all measures, of measures for ACO payments, and of measures for the STARS program. For a detailed explanation of each, see the following links to tutorials on SETMA s website: All Measures beginning with page 42 on the following tutorial: Patient-Centered Medical Home SETMA s Medical Home Coordination Review (MHCR) Tutorial Measures related to qualifying for ACO shared savings payments. Accountable Care Organization Quality Measures Performance Tool Tutorial Measures related to increasing the STAR rating for the Medicare Advantage Plan. Going from a 3.5 to a 4 STAR can mean millions of dollars of increased payments to providers for the care they provide. STARs - A Tutorial for Utilizing SETMA s Deployment of the STARS MA Program 2
3 SETMA s Deployment of The first screen of SETMA s Electronic Medical Record is seen below. In the first column is a hyperlink entitled PC-MH Coordination Review (seen outlined in Green below). When this link is activated, the Medical Home Coordination Review appears. As indicated above and as seen in the hyperlink outlined in Green below, the full measure sets is listed here. If a provider wishes to evaluate his/her own performance on all measures, it can be done so by clicking this button. If you wish to review all measures which are dependent upon the healthcare provider, you can do so by accessing this link. 3
4 The following is an example of the technical specifications of a measure. All can be reviewed by accessing each of the measures. To determine whether you have fulfilled measures you can simple use the color coding: red means the measure applies to this patient and has not been fulfilled; black means the measure applies to the patient and has been fulfilled; grey means the measure does not apply to this patient. 4
5 The following is an example of the details of a measure. To review all of the measures details see above. 5
6 ACO Metrics To review your performance on the quality metrics required in order to benefit from the Accountable Care Organziation (ACO) shared-savings plan, you can see the link on the AAA Home Temp;ate below, outlined in green. Your performance is shown on the template which pops us. The coding is the same: red applies and not done; black applies and done; grey does not apply. The details of one of the metrics are shown below. 6
7 The Medicare Advantage STARS Program quality metrics are launched below by clicking on the hyperlink outlined in green 7
8 Overview of STARS Content The Overall Star Rating combines scores for the types of services each plan offers: What is being measured? For plans covering health services, the overall score for quality of those services covers many different topics that fall into 5 categories: Staying healthy: screenings, tests, and vaccines: Includes whether members got various screening tests, vaccines, and other check-ups that help them stay healthy. Managing chronic (long-term) conditions: Includes how often members with different conditions got certain tests and treatments that help them manage their condition. Member experience with the health plan: Includes ratings of member satisfaction with the plan. Member complaints and changes in the health plan s performance: Includes how often Medicare found problems with the plan and how often members had problems with the plan. Includes how much the plan s performance has improved (if at all) over time. Health plan customer service: Includes how well the plan handles member appeals. For plans covering drug services, the overall score for quality of those services covers many different topics that fall into 4 categories: Drug plan customer service: Includes how well the plan handles member appeals. Member complaints and changes in the drug plan s performance: Includes how often Medicare found problems with the plan and how often members had problems with the plan. Includes how much the plan s performance has improved (if at all) over time. Member experience with plan s drug services: Includes ratings of member satisfaction with the plan. Drug safety and accuracy of drug pricing: Includes how accurate the plan s pricing information is and how often members with certain medical conditions are prescribed drugs in a way that is safer and clinically recommended for their condition. For plans covering health and drug services, the overall score for quality of those services covers all of the topics above. 8
9 The following gives the details of the measures which apply to the MA STARS program. The following is one details of one of the STARS metrics. 9
Medical Home Transtheoretical Model Assessment Stages of Change Tutorial
 Medical Home Transtheoretical Model Assessment Stages of Change Tutorial In the Medical Home Model of healthcare, it is imperative that the patient participates in their own care. Terms like activated,
Medical Home Transtheoretical Model Assessment Stages of Change Tutorial In the Medical Home Model of healthcare, it is imperative that the patient participates in their own care. Terms like activated,
Unique Billing for PCMH Transition of Care/HCC Risk Management
 THE MEDICAL HOME SUMMIT MARCH 23, 2015 Unique Billing for PCMH Transition of Care/HCC Risk Management JAYNE BRYANT RN, BSN THERESA BAILEY, LVN JAMES L. HOLLY, MD MARCH 23, 2015 Criteria for New Codes 2
THE MEDICAL HOME SUMMIT MARCH 23, 2015 Unique Billing for PCMH Transition of Care/HCC Risk Management JAYNE BRYANT RN, BSN THERESA BAILEY, LVN JAMES L. HOLLY, MD MARCH 23, 2015 Criteria for New Codes 2
Pharmacy Quality Measures. Presentation Developed for the Academy of Managed Care Pharmacy Updated: February 2013
 Pharmacy Quality Measures Presentation Developed for the Academy of Managed Care Pharmacy Updated: February 2013 Objectives Explain the purpose of quality measures and how they are developed Identify quality
Pharmacy Quality Measures Presentation Developed for the Academy of Managed Care Pharmacy Updated: February 2013 Objectives Explain the purpose of quality measures and how they are developed Identify quality
Medical Home Magno CMS Question Medical Home Servicers Delivered by James L Holly, MD
 Medical Home Magno CMS Question Medical Home Servicers Delivered by James L Holly, MD March 3, 2010 Ms. Linda M. Magno Medicare Demonstrations Program Group Centers for Medicare and Medicaid Services Office
Medical Home Magno CMS Question Medical Home Servicers Delivered by James L Holly, MD March 3, 2010 Ms. Linda M. Magno Medicare Demonstrations Program Group Centers for Medicare and Medicaid Services Office
How to Improve HEDIS Reporting Among Providers and Improve Your Health Plan Rankings
 How to Improve HEDIS Reporting Among Providers and Improve Your Health Plan Rankings Introduction In today s value-focused market, health plan rankings, such as those calculated by the National Committee
How to Improve HEDIS Reporting Among Providers and Improve Your Health Plan Rankings Introduction In today s value-focused market, health plan rankings, such as those calculated by the National Committee
2012 HEDIS/CAHPS Effectiveness of Care Report for 2011 Measures Oregon Commercial Business
 2012 HEDIS/CAHPS Effectiveness of Care Report for 2011 Measures Oregon Commercial Business About HEDIS The Healthcare Effectiveness Data and Information Set (HEDIS 1 ) is a widely used set of performance
2012 HEDIS/CAHPS Effectiveness of Care Report for 2011 Measures Oregon Commercial Business About HEDIS The Healthcare Effectiveness Data and Information Set (HEDIS 1 ) is a widely used set of performance
2019 Quality Improvement Program Description Overview
 2019 Quality Improvement Program Description Overview Introduction Eon/Clear Spring s Quality Improvement (QI) program guides the company s activities to improve care and treatment for the member s we
2019 Quality Improvement Program Description Overview Introduction Eon/Clear Spring s Quality Improvement (QI) program guides the company s activities to improve care and treatment for the member s we
Value-Based Payment Models, Questions for the Industry, Health Leader Media, Answers by James L. Holly, MD April 15, 2015
 Value-Based Payment Models, Questions for the Industry, Health Leader Media, Answers by James L. Holly, MD April 15, 2015 Here is the List of 8 Leftover 5 for your consideration: Why is capitation with
Value-Based Payment Models, Questions for the Industry, Health Leader Media, Answers by James L. Holly, MD April 15, 2015 Here is the List of 8 Leftover 5 for your consideration: Why is capitation with
Texas State Reportable Infectious Diseases A Systems Solution to the Problem of Reporting
 Texas State Reportable Infectious Diseases A Systems Solution to the Problem of Reporting How can healthcare providers design a solution to a complex healthcare problem, particularly when the problem is
Texas State Reportable Infectious Diseases A Systems Solution to the Problem of Reporting How can healthcare providers design a solution to a complex healthcare problem, particularly when the problem is
Accountable Care Organizations (ACO) Draft 2011 Criteria
 1 of 11 For Public Comment October 19 November 19, 2010 Comments due 5:00 pm EST Accountable Care Organizations (ACO) Draft 2011 Criteria Overview 2 of 11 Note: This publication is protected by U.S. and
1 of 11 For Public Comment October 19 November 19, 2010 Comments due 5:00 pm EST Accountable Care Organizations (ACO) Draft 2011 Criteria Overview 2 of 11 Note: This publication is protected by U.S. and
Medication Module Tutorial
 Medication Module Tutorial An Introduction to the Medication module Whether completing a clinic patient evaluation, a hospital admission history and physical, a discharge summary, a hospital order set,
Medication Module Tutorial An Introduction to the Medication module Whether completing a clinic patient evaluation, a hospital admission history and physical, a discharge summary, a hospital order set,
19. Covered California Quality Improvement Strategy (QIS) - INSTRUCTIONS FOR DATA TEMPLATE
 19. Covered California Quality Improvement Strategy (QIS) - INSTRUCTIONS FOR DATA TEMPLATE Section 19.2 of the QIS requires applicants to submit data for each initiative area. Some questions can be completed
19. Covered California Quality Improvement Strategy (QIS) - INSTRUCTIONS FOR DATA TEMPLATE Section 19.2 of the QIS requires applicants to submit data for each initiative area. Some questions can be completed
Intensive Behavioral Therapy (IBT) Obesity and Cardiovascular Disease Medicare Preventive Services
 Intensive Behavioral Therapy (IBT) Obesity and Cardiovascular Disease Medicare Preventive Services Index Stand Alone Benefit 2 G Codes for Intensive Behavioral Therapy 3 The content of the Intensive Behavioral
Intensive Behavioral Therapy (IBT) Obesity and Cardiovascular Disease Medicare Preventive Services Index Stand Alone Benefit 2 G Codes for Intensive Behavioral Therapy 3 The content of the Intensive Behavioral
MCOs Revealed: Strategies for Building Strong Hospital & Referral Relationships
 MCOs Revealed: Strategies for Building Strong Hospital & Referral Relationships June 2014 avalerehealth.net Today s Panelists John Hackett - JHackett@extendicare.com o Vice President of Strategy & Development,
MCOs Revealed: Strategies for Building Strong Hospital & Referral Relationships June 2014 avalerehealth.net Today s Panelists John Hackett - JHackett@extendicare.com o Vice President of Strategy & Development,
Humana At Home-Star Member Talking Points
 At Home-Star Member Talking Points What are the CMS Medicare Star Ratings? The Center for Medicare & Medicaid Services (CMS) is a federal agency that oversees Medicare & Medicaid, and is part of the Department
At Home-Star Member Talking Points What are the CMS Medicare Star Ratings? The Center for Medicare & Medicaid Services (CMS) is a federal agency that oversees Medicare & Medicaid, and is part of the Department
Provider Training Quality Enhancement 2016
 Provider Training Quality Enhancement 2016 1 What s Ahead? Why Are We Here? 3 NCQA Accreditation & HEDIS 4-6 Medicare Start Rating & HEDIS 7 Provider s Role and Expectation 8-11 Staying Healthy During
Provider Training Quality Enhancement 2016 1 What s Ahead? Why Are We Here? 3 NCQA Accreditation & HEDIS 4-6 Medicare Start Rating & HEDIS 7 Provider s Role and Expectation 8-11 Staying Healthy During
Passport Advantage Provider Manual Section 8.0 Quality Improvement
 Passport Advantage Provider Manual Section 8.0 Quality Improvement Table of Contents 8.1 Quality Improvement Program 8.2 Clinical Practice Guidelines 8.3 Star s 8.4 Quality of Care Concerns 8.3 Practitioner
Passport Advantage Provider Manual Section 8.0 Quality Improvement Table of Contents 8.1 Quality Improvement Program 8.2 Clinical Practice Guidelines 8.3 Star s 8.4 Quality of Care Concerns 8.3 Practitioner
Thought Leadership Series White Paper The Journey to Population Health and Risk
 AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
The Nature of Knowledge
 The Importance of Data Analytics in Physician Practice Massachusetts Medical Society March 30, 2012 James L. Holly, MD CEO, SETMA, LLP www.setma.com Adjunct Professor Department of Family and Community
The Importance of Data Analytics in Physician Practice Massachusetts Medical Society March 30, 2012 James L. Holly, MD CEO, SETMA, LLP www.setma.com Adjunct Professor Department of Family and Community
MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE
 MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE Randa Deaton, MA Corporate Director, UAW/Ford Community Healthcare Initiative Co-Executive Director, Kentuckiana Health Collaborative 1 WHO is the KHC?
MULTI-STAKEHOLDER APPROACH TO VALUE-BASED HEALTHCARE Randa Deaton, MA Corporate Director, UAW/Ford Community Healthcare Initiative Co-Executive Director, Kentuckiana Health Collaborative 1 WHO is the KHC?
Should PCMH accreditation be the next step in your quest for high-quality care delivery?
 This Web version may be reproduced for individual use. Should PCMH accreditation be the next step in your quest for high-quality care delivery? Lessons learned from one organization that achieved PCMH
This Web version may be reproduced for individual use. Should PCMH accreditation be the next step in your quest for high-quality care delivery? Lessons learned from one organization that achieved PCMH
Note: Accredited is the highest rating an exchange product can have for 2015.
 Quality Overview Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product can have for 215.
Quality Overview Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product can have for 215.
Humana Physician Quality Rewards Program 2014
 Humana Physician Quality Rewards Program 2014 Medicare Glen Champlin MSO Director March 28, 2014 1430ALL0114-B What is CMS Stars and Why Should Providers Be Concerned? CMS Program of Quality & Performance
Humana Physician Quality Rewards Program 2014 Medicare Glen Champlin MSO Director March 28, 2014 1430ALL0114-B What is CMS Stars and Why Should Providers Be Concerned? CMS Program of Quality & Performance
The New Jersey Department of Health and Senior
 The New Jersey Department of Health and Senior Services developed this report with the cooperation of the New Jersey health plans. The Department was guided by an advisory group representing health plans,
The New Jersey Department of Health and Senior Services developed this report with the cooperation of the New Jersey health plans. The Department was guided by an advisory group representing health plans,
Quality Measures for HMO s: Understanding HEDIS
 Quality Measures for HMO s: Understanding HEDIS DANE COUNTY IMMUNIZATION COALITION MEMBERSHIP MEETING November 29, 2011 Elaine Rosenblatt MSN, FNP-BC Director, Quality and Care Management UW Medical Foundation/
Quality Measures for HMO s: Understanding HEDIS DANE COUNTY IMMUNIZATION COALITION MEMBERSHIP MEETING November 29, 2011 Elaine Rosenblatt MSN, FNP-BC Director, Quality and Care Management UW Medical Foundation/
Quality Management Report 2017 Q4
 Quality Management Report 2017 Q4 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels. These activities include: CMS DHS DHS & CMS HEDIS Member Satisfaction (CAHPS
Quality Management Report 2017 Q4 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels. These activities include: CMS DHS DHS & CMS HEDIS Member Satisfaction (CAHPS
VALUE-BASED CARE REPORT
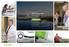 VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
MAKING PROGRESS, SEEING RESULTS
 MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
Admitting and Discharging Transient Patients
 Admitting and Discharging Transient Patients Goal: Learn to admit and discharge transient patients in CROWNWeb. Estimated Time: 25 to 30 minutes Page 1 Table of Contents Course Goals 3 Before You Begin...
Admitting and Discharging Transient Patients Goal: Learn to admit and discharge transient patients in CROWNWeb. Estimated Time: 25 to 30 minutes Page 1 Table of Contents Course Goals 3 Before You Begin...
4/18/2013. Why Quality Matters. Overview. Discussion
 Why Quality Matters Margaret E. O Kane, NCQA President April 18, 2013 Overview Who is NCQA? How do we help brokers? Employers views and quality and value About high-deductible plans Discussion 2 My Presentation,
Why Quality Matters Margaret E. O Kane, NCQA President April 18, 2013 Overview Who is NCQA? How do we help brokers? Employers views and quality and value About high-deductible plans Discussion 2 My Presentation,
The Health Services Cost Review Commission s (HSCRC) global budget revenue contracts state:
 Global Budget Revenue (GBR) Reporting on Investment in Infrastructure Background The Health Services Cost Review Commission s (HSCRC) global budget revenue contracts state: The Hospital shall provide an
Global Budget Revenue (GBR) Reporting on Investment in Infrastructure Background The Health Services Cost Review Commission s (HSCRC) global budget revenue contracts state: The Hospital shall provide an
MyHealth. results with your doctor. Talk High. to him or her about how often 3. Eat foods low in saturated 140/90 or higher
 2016 MyHealth Quarter 3 Anthem Blue Cross Cal MediConnect Plan What is blood pressure? Blood pressure is the amount of force it takes for your heart to push blood through your body. When your blood pressure
2016 MyHealth Quarter 3 Anthem Blue Cross Cal MediConnect Plan What is blood pressure? Blood pressure is the amount of force it takes for your heart to push blood through your body. When your blood pressure
Introduction to the Provider Care Management Solutions Web Interface
 Introduction to the Provider Care Management Solutions Web Interface Release 0.2 Introduction to the Provider Care Management Solutions Web Interface Purpose Provider Care Management Solutions (PCMS) is
Introduction to the Provider Care Management Solutions Web Interface Release 0.2 Introduction to the Provider Care Management Solutions Web Interface Purpose Provider Care Management Solutions (PCMS) is
Quality Improvement Program
 How we measure up At HealthKeepers, Inc., we focus on helping our Anthem HealthKeepers Plus members get healthy and stay healthy. To help us serve you the best we can, each year we look closely at the
How we measure up At HealthKeepers, Inc., we focus on helping our Anthem HealthKeepers Plus members get healthy and stay healthy. To help us serve you the best we can, each year we look closely at the
Introduction to the Provider Care Management Solutions Web Interface
 Introduction to the Provider Care Management Solutions Web Interface Release 0.2 Introduction to the Provider Care Management Solutions Web Interface Purpose Provider Care Management Solutions (PCMS) is
Introduction to the Provider Care Management Solutions Web Interface Release 0.2 Introduction to the Provider Care Management Solutions Web Interface Purpose Provider Care Management Solutions (PCMS) is
Anthem BlueCross and BlueShield
 Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Commercial HMO) Accredited Accreditation Commercial
Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Commercial HMO) Accredited Accreditation Commercial
Your health comes first
 Your health comes first Here are the many ways we re working to ensure the quality of your care At Amerigroup, our focus is on you. We want to help you get and stay healthy. That s why we have many programs
Your health comes first Here are the many ways we re working to ensure the quality of your care At Amerigroup, our focus is on you. We want to help you get and stay healthy. That s why we have many programs
Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value
 Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value Objectives Compare different primary care compensation models Identify keys to success and best methods for transitioning
Beyond RVUs: Changing Your Primary Care Compensation Plan from Volume to Value Objectives Compare different primary care compensation models Identify keys to success and best methods for transitioning
How to Document Unmade Visits
 What is an Unmade Visit? A visit is considered an unmade visit when it is not made and cannot be made up within the Medicare week. Consequently, the patient s ordered visit frequency is not met for that
What is an Unmade Visit? A visit is considered an unmade visit when it is not made and cannot be made up within the Medicare week. Consequently, the patient s ordered visit frequency is not met for that
Quality Management Report 2017 Q2
 Quality Management Report 2017 Q2 Quality Management Program CMS STAR Ratings Member Satisfaction (CAHPS & HOS) HEDIS Risk Adjustment DHS Member Incident Reporting Member Satisfaction Surveys Pay for Performance
Quality Management Report 2017 Q2 Quality Management Program CMS STAR Ratings Member Satisfaction (CAHPS & HOS) HEDIS Risk Adjustment DHS Member Incident Reporting Member Satisfaction Surveys Pay for Performance
2018 PROVIDER TOOLKIT
 1100 Circle 75 Parkway Suite 1100 Atlanta, GA 30339 2018 PROVIDER TOOLKIT Understanding the Centers for Medicare and Medicaid (CMS) Stars Rating System What is CMS Quality Star Ratings program? CMS evaluates
1100 Circle 75 Parkway Suite 1100 Atlanta, GA 30339 2018 PROVIDER TOOLKIT Understanding the Centers for Medicare and Medicaid (CMS) Stars Rating System What is CMS Quality Star Ratings program? CMS evaluates
Session 10: Integrating Data and Analytics into Provider Workflows Improves ACO Quality and Financial Performance
 Session 10: Integrating Data and Analytics into Provider Workflows Improves ACO Quality and Financial Performance Joan Valentine, MSA, RN Executive Vice President Visiting Physicians Association David
Session 10: Integrating Data and Analytics into Provider Workflows Improves ACO Quality and Financial Performance Joan Valentine, MSA, RN Executive Vice President Visiting Physicians Association David
Draft Covered California Delivery Reform Contract Provisions Comments Welcome and Encouraged
 TO: FROM: RE: State Based Marketplaces State Medicaid Directors Delivery Reform/Value Promoting Colleagues Peter V. Lee, Executive Director Draft Covered California Delivery Reform Contract Provisions
TO: FROM: RE: State Based Marketplaces State Medicaid Directors Delivery Reform/Value Promoting Colleagues Peter V. Lee, Executive Director Draft Covered California Delivery Reform Contract Provisions
Health in Handbook. a guide to Medicare rights & health in Pennsylvania #6009-8/07
 Health in Handbook a guide to Medicare rights & health in Pennsylvania #6009-8/07 Tips for Staying Healthy works hard to make sure that the health care you receive is the best care possible. There are
Health in Handbook a guide to Medicare rights & health in Pennsylvania #6009-8/07 Tips for Staying Healthy works hard to make sure that the health care you receive is the best care possible. There are
Appendix 3 Record Review Workbook Instructions
 Appendix 3 Record Review Workbook Instructions NCQA PCMH Standards and Guidelines (2017 Edition, Version 2) September 30, 2017 Appendix 3 PCMH Record Review Workbook General Instructions 3-1 APPENDIX 3
Appendix 3 Record Review Workbook Instructions NCQA PCMH Standards and Guidelines (2017 Edition, Version 2) September 30, 2017 Appendix 3 PCMH Record Review Workbook General Instructions 3-1 APPENDIX 3
Medicare Advantage Star Ratings
 Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Medicare Advantage Star Ratings December 2017 The Star Rating System measures how well Medicare Advantage (MA) and its prescription drug plans perform for consumers. As an integrated health system, Presbyterian
Value Based Care An ACO Perspective
 Value Based Care An ACO Perspective NCIOM Task Force on Accountable Care Communities January 24, 2018 Steve Neorr Chief Administrative Officer 2 3 4 5 Source: Banthin, Jessica. Healthcare Spending Today
Value Based Care An ACO Perspective NCIOM Task Force on Accountable Care Communities January 24, 2018 Steve Neorr Chief Administrative Officer 2 3 4 5 Source: Banthin, Jessica. Healthcare Spending Today
National Survey on Consumers Experiences With Patient Safety and Quality Information
 Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
Quality Management Report 2018 Q1
 Quality Management Report 2018 Q1 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels These activities include: Centers for Medicare & Medicaid Services (CMS) Department
Quality Management Report 2018 Q1 Care Wisconsin Participates in Many Quality Initiatives Across the State and Federal Levels These activities include: Centers for Medicare & Medicaid Services (CMS) Department
McLaren Health Plan Quality Improvement Update 2014
 McLaren Health Plan Quality Improvement Update 2014 Since the incorporation of McLaren Health Plan (MHP) in November 1997, the staff has continued to utilize their extensive clinical and administrative
McLaren Health Plan Quality Improvement Update 2014 Since the incorporation of McLaren Health Plan (MHP) in November 1997, the staff has continued to utilize their extensive clinical and administrative
Complex Patient Care Redesign: ThedaCare Innovation. Gregory Long, MD Chief Medical Officer
 Complex Patient Care Redesign: ThedaCare Innovation Gregory Long, MD Chief Medical Officer ThedaCare Northeastern Wisconsin An Integrated Community Health System; >7000 employees Primary service area of
Complex Patient Care Redesign: ThedaCare Innovation Gregory Long, MD Chief Medical Officer ThedaCare Northeastern Wisconsin An Integrated Community Health System; >7000 employees Primary service area of
Examining the Differences Between Commercial and Medicare ACO Models
 Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
Examining the Differences Between Commercial and Medicare ACO Models Michelle Copenhaver December 10, 2015 Agenda 1 Understanding Accountable Care Organizations 2 Moving to Accountable Care: Enhancing
2017 HIMSS DAVIES APPLICANT
 2017 HIMSS DAVIES APPLICANT Introduction of NOMS Team Members Melissa Thomas IT Project Director Joshua Frederick, CPA, MT Chief Executive Officer Jennifer Hohman, MD Executive Vice President, NOMS Healthcare
2017 HIMSS DAVIES APPLICANT Introduction of NOMS Team Members Melissa Thomas IT Project Director Joshua Frederick, CPA, MT Chief Executive Officer Jennifer Hohman, MD Executive Vice President, NOMS Healthcare
Emerging Outpatient CDI Drivers and Technologies
 7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
7th Annual Association for Clinical Documentation Improvement Specialists Conference Emerging Outpatient CDI Drivers and Technologies Elaine King, MHS, RHIA, CHP, CHDA, CDIP, FAHIMA Outpatient Payment
Colorado Choice Health Plans
 Quality Overview Health Plans Accreditation Exchange Product Accrediting Organization: Accreditation Status: URAC Health Plan Accreditation (Marketplace ) Full Full: Organization demonstrates full compliance
Quality Overview Health Plans Accreditation Exchange Product Accrediting Organization: Accreditation Status: URAC Health Plan Accreditation (Marketplace ) Full Full: Organization demonstrates full compliance
and HEDIS Measures
 1 SC Medicaid Managed Care Initiative and HEDIS Measures - 2009 Ana Lòpez De Fede, PhD Institute for Families in Society University of South Carolina Regina Young, RNC SC Department of Health and Human
1 SC Medicaid Managed Care Initiative and HEDIS Measures - 2009 Ana Lòpez De Fede, PhD Institute for Families in Society University of South Carolina Regina Young, RNC SC Department of Health and Human
 AFC HMO Provider Newsletter AFC CONNECT CONNECT Winter 2017 www.americas1stchoice.com Encouraging Active Participation in Cholesterol Management The Plan s Disease Case Managers often work with members
AFC HMO Provider Newsletter AFC CONNECT CONNECT Winter 2017 www.americas1stchoice.com Encouraging Active Participation in Cholesterol Management The Plan s Disease Case Managers often work with members
2015 Quality Improvement Work Plan Summary
 2015 Quality Improvement Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how
2015 Quality Improvement Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how
AmeriHealth Michigan Provider Overview. April, 2014
 AmeriHealth Michigan Provider Overview April, 2014 Who We Are Our Mission Dual Demonstration of Michigan AmeriHealth VIP Care Plus Agenda Our Record of Success Integrated Care Management Provider Partnerships
AmeriHealth Michigan Provider Overview April, 2014 Who We Are Our Mission Dual Demonstration of Michigan AmeriHealth VIP Care Plus Agenda Our Record of Success Integrated Care Management Provider Partnerships
Menu Item: Population Management
 Cover Page Menu Item: Population Management Name of Applicant Organization: Fremont Family Care Organization s Address: 2540 N Healthy Way, Fremont, NE 68025 Submitter s Name: Elizabeth Belmont Submitter
Cover Page Menu Item: Population Management Name of Applicant Organization: Fremont Family Care Organization s Address: 2540 N Healthy Way, Fremont, NE 68025 Submitter s Name: Elizabeth Belmont Submitter
Anthem BlueCross and BlueShield HMO
 Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: NCQA (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product
Quality Overview BlueCross and BlueShield Accreditation Exchange Product Accrediting Organization: NCQA (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product
Money and Members: Pay for Performance in a Medicaid Program
 Money and Members: Pay for Performance in a Medicaid Program IHA National Pay for Performance Summit March 9, 2010 Greg Buchert, MD, MPH Chief Operating Officer 1 AGENDA CalOptima Overview CalOptima P4P
Money and Members: Pay for Performance in a Medicaid Program IHA National Pay for Performance Summit March 9, 2010 Greg Buchert, MD, MPH Chief Operating Officer 1 AGENDA CalOptima Overview CalOptima P4P
2017 HIMSS DAVIES APPLICANT
 2017 HIMSS DAVIES APPLICANT Introduction of NOMS Team Members Melissa Thomas IT Project Director Joshua Frederick, CPA, MT Chief Executive Officer Jennifer Hohman, MD Executive Vice President, NOMS Healthcare
2017 HIMSS DAVIES APPLICANT Introduction of NOMS Team Members Melissa Thomas IT Project Director Joshua Frederick, CPA, MT Chief Executive Officer Jennifer Hohman, MD Executive Vice President, NOMS Healthcare
UPMC Health Plan. Value Based Insurance Design (VBID) Spark Your Health
 UPMC Health Plan Value Based Insurance Design (VBID) Spark Your Health Value Based Insurance Design (VBID) Spark Your Health Medicare Advantage Summit April 6, 2017 Helene Weinraub 1 The statements contained
UPMC Health Plan Value Based Insurance Design (VBID) Spark Your Health Value Based Insurance Design (VBID) Spark Your Health Medicare Advantage Summit April 6, 2017 Helene Weinraub 1 The statements contained
WHAT IT FEELS LIKE
 PCMH and PCSP WHAT IT FEELS LIKE Presentation Outline Goals of the Patient Centered Medical Home and the Patient Centered Specialty Practice Identifying the Joint Principles Recognition Programs Standards
PCMH and PCSP WHAT IT FEELS LIKE Presentation Outline Goals of the Patient Centered Medical Home and the Patient Centered Specialty Practice Identifying the Joint Principles Recognition Programs Standards
Unit 1 Introduction to the Medical Home JumpStart Program
 Objectives Overview of the Medical Home model of care and its benefits Introducing the National Committee for Quality Assurance (NCQA) recognition process Overview of the Medical Home JumpStart approach
Objectives Overview of the Medical Home model of care and its benefits Introducing the National Committee for Quality Assurance (NCQA) recognition process Overview of the Medical Home JumpStart approach
ACOs in 2012: ACO Activity Doubles in 12 Months
 Healthcare Benchmarks and Metrics July 2012 ACOs in 2012: ACO Activity Doubles in 12 Months www.hin.com The Healthcare Intelligence Network 800 State Highway 71, Suite 2 Sea Girt, NJ 08750 888-446-3530
Healthcare Benchmarks and Metrics July 2012 ACOs in 2012: ACO Activity Doubles in 12 Months www.hin.com The Healthcare Intelligence Network 800 State Highway 71, Suite 2 Sea Girt, NJ 08750 888-446-3530
Medicare Rights & Protections
 CENTERS for MEDICARE & MEDICAID SERVICES Medicare Rights & Protections This official government booklet has important information about: Your rights & protections in: Original Medicare Medicare Advantage
CENTERS for MEDICARE & MEDICAID SERVICES Medicare Rights & Protections This official government booklet has important information about: Your rights & protections in: Original Medicare Medicare Advantage
Health HAPPEN. Make. Prepare now to stay healthy during flu season. Inside
 Inside How to lower your blood pressure Make Health HAPPEN Quarter 3, 2017 www.myamerigroup.com/medicare Prepare now to stay healthy during flu season Influenza, also known as the flu, can make you feel
Inside How to lower your blood pressure Make Health HAPPEN Quarter 3, 2017 www.myamerigroup.com/medicare Prepare now to stay healthy during flu season Influenza, also known as the flu, can make you feel
Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws.
 Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Pay for Performance in the Context of the Military Patient- Centered Medical Home
 Pay for Performance in the Context of the Military Patient- Centered Medical Home Michael Dinneen, MD, PhD COL John P. Kugler, MD, MPH Department of Defense 11 March 2009 Agenda Military Health System
Pay for Performance in the Context of the Military Patient- Centered Medical Home Michael Dinneen, MD, PhD COL John P. Kugler, MD, MPH Department of Defense 11 March 2009 Agenda Military Health System
National Survey of Physician Organizations and the Management of Chronic Illness II (Independent Practice Associations)
 If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
HIT Glossary and Acronym List
 HIT Glossary and Acronym List November 2011 FACT SHEET ACA Patient Protection and Affordable Care Act (see PPACA). ACO Accountable Care Organization: A group of health care providers (e.g. primary care,
HIT Glossary and Acronym List November 2011 FACT SHEET ACA Patient Protection and Affordable Care Act (see PPACA). ACO Accountable Care Organization: A group of health care providers (e.g. primary care,
Medicare PPS Report. Self Guided Tutorial
 Medicare PPS Report Self Guided Tutorial 1 Tutorial Objectives After completing this tutorial, you will be able to: Identify the purpose of the Medicare PPS Report Access the Medicare PPS Report Customize
Medicare PPS Report Self Guided Tutorial 1 Tutorial Objectives After completing this tutorial, you will be able to: Identify the purpose of the Medicare PPS Report Access the Medicare PPS Report Customize
PCMH to ACO: Carilion Clinic s Journey
 PCMH to ACO: Carilion Clinic s Journey Michael P. Jeremiah, MD, FAAFP Chair, Department of Family and Community Medicine Carilion Clinic and the Virginia Tech-Carilion School of Medicine Patient-Centered
PCMH to ACO: Carilion Clinic s Journey Michael P. Jeremiah, MD, FAAFP Chair, Department of Family and Community Medicine Carilion Clinic and the Virginia Tech-Carilion School of Medicine Patient-Centered
Maximizing the Power of Your Data. Peggy Connorton, MS, LNFA AHCA Director, Quality and LTC Trend Tracker
 Maximizing the Power of Your Data Peggy Connorton, MS, LNFA AHCA Director, Quality and LTC Trend Tracker Objectives Explore selected LTC Trend Tracker reports & features including: re-hospitalization,
Maximizing the Power of Your Data Peggy Connorton, MS, LNFA AHCA Director, Quality and LTC Trend Tracker Objectives Explore selected LTC Trend Tracker reports & features including: re-hospitalization,
Pearls In Internal Medicine
 Pearls In Internal Medicine Transitioning From Solo or Small Group Practice to a Large Group James L. Holly, MD Adjunct Professor University of Texas Health Science Center San Antonio School of Medicine
Pearls In Internal Medicine Transitioning From Solo or Small Group Practice to a Large Group James L. Holly, MD Adjunct Professor University of Texas Health Science Center San Antonio School of Medicine
GUIDELINES FOR MARKETING AND ADVERTISING HEALTH PLAN ACCREDITATION. Table of Contents
 GUIDELINES FOR MARKETING AND ADVERTISING HEALTH PLAN ACCREDITATION Table of Contents INTRODUCTION 2 DESCRIPTIONS OF NCQA HEALTH PLAN ACCREDITATION 2 DESCRIPTIONS OF NCQA HEALTH PLAN ACCREDITATION STANDARDS
GUIDELINES FOR MARKETING AND ADVERTISING HEALTH PLAN ACCREDITATION Table of Contents INTRODUCTION 2 DESCRIPTIONS OF NCQA HEALTH PLAN ACCREDITATION 2 DESCRIPTIONS OF NCQA HEALTH PLAN ACCREDITATION STANDARDS
Reducing Hospital Admissions Through the Use of IT. Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods
 Reducing Hospital Admissions Through the Use of IT Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods Conflict of Interest Steven Milligan, MD Has no real or apparent conflicts
Reducing Hospital Admissions Through the Use of IT Steven Milligan MD Medical Director of ACO Management Colorado Health Neighborhoods Conflict of Interest Steven Milligan, MD Has no real or apparent conflicts
Medical professionals: who require the ability to scan information quickly, have consistency in how information is displayed.
 TIME-CENTERED PATIENT RECORD ABOUT THIS DESIGN We redesigned the patient record to be more user and time-centered. We took the idea that medical professionals need the ability to process lots of information
TIME-CENTERED PATIENT RECORD ABOUT THIS DESIGN We redesigned the patient record to be more user and time-centered. We took the idea that medical professionals need the ability to process lots of information
Medicare: 2018 Model of Care Training
 Medicare: 2018 Model of Care Training Training Objectives This course will describe how Centene and its contracted providers work together to successfully deliver the duals Model of Care (MOC) program.
Medicare: 2018 Model of Care Training Training Objectives This course will describe how Centene and its contracted providers work together to successfully deliver the duals Model of Care (MOC) program.
Measuring Value and Outcomes for Continuous Quality Improvement. Noelle Flaherty MS, MBA, RN, CCM, CPHQ 1. Jodi Cichetti, MS, RN, BS, CCM, CPHQ
 Noelle Flaherty MS, MBA, RN, CCM, CPHQ 1 Jodi Cichetti, MS, RN, BS, CCM, CPHQ Leslie Beck, MS 1 Amanda Abraham MS 1 Maria Uriyo, PhD, MHSA, PMP 1 1. Johns Hopkins Healthcare LLC, Baltimore Maryland Corresponding
Noelle Flaherty MS, MBA, RN, CCM, CPHQ 1 Jodi Cichetti, MS, RN, BS, CCM, CPHQ Leslie Beck, MS 1 Amanda Abraham MS 1 Maria Uriyo, PhD, MHSA, PMP 1 1. Johns Hopkins Healthcare LLC, Baltimore Maryland Corresponding
Coastal Medical, Inc.
 A Culture of Collaboration The Organization Physician-owned group Currently 19 offices across the state of Rhode Island and growing 85 physicians, 101 care providers The Challenge Implement a single, unified
A Culture of Collaboration The Organization Physician-owned group Currently 19 offices across the state of Rhode Island and growing 85 physicians, 101 care providers The Challenge Implement a single, unified
Unit 4 Evidence-Based Clinical Practice Guidelines (CPG)
 (CPG) NCQA Reference: PCMH 3 Element A Objectives Review evidence-based clinical practice guidelines Select clinical practice guidelines for JumpStart Level I Review NCQA requirements for evidence-based
(CPG) NCQA Reference: PCMH 3 Element A Objectives Review evidence-based clinical practice guidelines Select clinical practice guidelines for JumpStart Level I Review NCQA requirements for evidence-based
Principal Investigator User Guide
 INFOED ELECTRONIC RESEARCH ADMINISTRATION infoed.clemson.edu Principal Investigator User Guide November 2014 Version 1.7 i Document Revisions Date Version Number Document Changes 12/06/2013 1.0 Initial
INFOED ELECTRONIC RESEARCH ADMINISTRATION infoed.clemson.edu Principal Investigator User Guide November 2014 Version 1.7 i Document Revisions Date Version Number Document Changes 12/06/2013 1.0 Initial
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM QI PROGRAM PURPOSE The Physicians Plus Quality Improvement Program is member-centric. It is designed to deliver safe and effective medical and behavioral healthcare, at the
QUALITY IMPROVEMENT PROGRAM QI PROGRAM PURPOSE The Physicians Plus Quality Improvement Program is member-centric. It is designed to deliver safe and effective medical and behavioral healthcare, at the
PROVIDER NEWSLETTER. Illinois 2016 Issue II DISEASE MANAGEMENT IMPROVING MEMBERS HEALTH IN THIS ISSUE
 Illinois 2016 Issue II PROVIDER NEWSLETTER DISEASE MANAGEMENT IMPROVING MEMBERS HEALTH Disease Management is a no-cost, voluntary program to assist members with specific chronic conditions. A member is
Illinois 2016 Issue II PROVIDER NEWSLETTER DISEASE MANAGEMENT IMPROVING MEMBERS HEALTH Disease Management is a no-cost, voluntary program to assist members with specific chronic conditions. A member is
2016 Open Enrollment Presentation for: University of California Senior Advantage
 2016 Open Enrollment Presentation for: University of California Senior Advantage 2 Three ways we make good health easier Quality care. We do what it takes to help you get healthy, and partner with you
2016 Open Enrollment Presentation for: University of California Senior Advantage 2 Three ways we make good health easier Quality care. We do what it takes to help you get healthy, and partner with you
Payment Reform Strategies. Ann Thomas Burnett BlueCross BlueShield of South Carolina
 Payment Reform Strategies Ann Thomas Burnett BlueCross BlueShield of South Carolina Disclosure I have no relevant financial relationships with commercial interests to disclose. The Current Market Landscape
Payment Reform Strategies Ann Thomas Burnett BlueCross BlueShield of South Carolina Disclosure I have no relevant financial relationships with commercial interests to disclose. The Current Market Landscape
Tips for PCMH Application Submission
 Tips for PCMH Application Submission Remain calm. The certification process is not as complicated as it looks. You will probably find you are already doing many of the required processes, and these are
Tips for PCMH Application Submission Remain calm. The certification process is not as complicated as it looks. You will probably find you are already doing many of the required processes, and these are
Assessing the Quality of California Dual Eligible Demonstration Health Plans
 M A Y 2 0 1 2 Assessing the Quality of California Dual Eligible Demonstration Health Plans T A B L E O F C O N T E N T S Overview... 1 Introduction... 2 Table 1: Plan Rating Overview... Summary of Quality
M A Y 2 0 1 2 Assessing the Quality of California Dual Eligible Demonstration Health Plans T A B L E O F C O N T E N T S Overview... 1 Introduction... 2 Table 1: Plan Rating Overview... Summary of Quality
Standard Operating Procedure. References Physician Guideline: Chronic Pain, Management of
 Subject Chronic Pain Management Index Number GL-6171 Section Patient Care Subsection Procedures/Treatments Category Corporate Contact Holly Boisen, Ext. 55970 References Physician Guideline: Chronic Pain,
Subject Chronic Pain Management Index Number GL-6171 Section Patient Care Subsection Procedures/Treatments Category Corporate Contact Holly Boisen, Ext. 55970 References Physician Guideline: Chronic Pain,
INFORMATION ABOUT YOUR OXFORD COVERAGE REIMBURSEMENT PART I OXFORD HEALTH PLANS OXFORD HEALTH PLANS (NJ), INC.
 OXFORD HEALTH PLANS (NJ), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (NJ), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
August 8, :00pm to 1:00pm Pamela Lester, Molly Layton and Janeen Boswell
 August 8, 2013 12:00pm to 1:00pm Pamela Lester, Molly Layton and Janeen Boswell 1) NCQA PCMH Recognition, what it means and its process. 2) Understand the rationale and benefits of becoming recognized
August 8, 2013 12:00pm to 1:00pm Pamela Lester, Molly Layton and Janeen Boswell 1) NCQA PCMH Recognition, what it means and its process. 2) Understand the rationale and benefits of becoming recognized
Health Reform and Medicare: What Does it Mean for a Restructured Delivery System?
 Health Reform and Medicare: What Does it Mean for a Restructured Delivery System? Gary S. Kaplan, MD Chairman and CEO Virginia Mason Medical Center May 25, 2011 Our Strategic Plan Virginia Mason Medical
Health Reform and Medicare: What Does it Mean for a Restructured Delivery System? Gary S. Kaplan, MD Chairman and CEO Virginia Mason Medical Center May 25, 2011 Our Strategic Plan Virginia Mason Medical
Take patient engagement to the next level. INTRODUCTION BENEFITS TOOLS & SERVICES TAKE ACTION INDEX
 Take patient engagement to the next level. We share your focus on better engaging patients to improve overall health. Patients who are more actively involved in their healthcare see better health outcomes
Take patient engagement to the next level. We share your focus on better engaging patients to improve overall health. Patients who are more actively involved in their healthcare see better health outcomes
arizona health net a better decision sm Putting you at the center of everything we do.
 arizona health net a better decision sm Putting you at the center of everything we do. Nothing s more important than your health. When you re healthy, you want to stay healthy. When you re sick or have
arizona health net a better decision sm Putting you at the center of everything we do. Nothing s more important than your health. When you re healthy, you want to stay healthy. When you re sick or have
Medication Reconciliation Tutorial Systematized and Automated Philosophy and Explanation By James L. Holly, MD
 Medication Reconciliation Tutorial Systematized and Automated Philosophy and Explanation By James L. Holly, MD Introduction Philosophy and Explanation... 2 Magic and Mass 3 Physician's Role in Medication
Medication Reconciliation Tutorial Systematized and Automated Philosophy and Explanation By James L. Holly, MD Introduction Philosophy and Explanation... 2 Magic and Mass 3 Physician's Role in Medication
Anthem Blue Cross Provider Operations and Technology
 Termination of Provider Enrollee Notification Initial Policy Approval Date: 12/17/2001 Policy Review/Revision Approval Date(s): 06/17/2002, 6/16/2003, 3/29/2004, 06/19/2007 Filed DMHC, 1/17/2014 Products:
Termination of Provider Enrollee Notification Initial Policy Approval Date: 12/17/2001 Policy Review/Revision Approval Date(s): 06/17/2002, 6/16/2003, 3/29/2004, 06/19/2007 Filed DMHC, 1/17/2014 Products:
