Postdischarge Follow-Up Visits for Medical and Pharmacy Students on an Inpatient Medicine Clerkship
|
|
|
- Angelina Jenkins
- 6 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Postdischarge Follow-Up Visits for Medical and Pharmacy Students on an Inpatient Medicine Clerkship Cindy J. Lai, MD 1 Heather E. Nye, MD, PhD 1 Thomas Bookwalter, PharmD 2 Anson Kwan, BA 1 Karen E. Hauer, MD 1 1 Department of Medicine, School of Medicine, University of California, San Francisco, California 2 Department of Pharmaceutical Services, Department of Clinical Pharmacy, School of Pharmacy, University of California, San Francisco, California BACKGROUND: Teaching medical and pharmacy students to collaborate on discharge planning for chronically ill patients may facilitate their ability to provide quality care. OBJECTIVE: To determine whether a discharge curriculum would improve students attitudes and self-assessed skills in interdisciplinary collaboration and transitional care for chronically ill patients. DESIGN: The discharge curriculum of an inpatient medicine clerkship focused on safe patient transitions after hospitalization. Curricular components included an interdisciplinary workshop, follow-up visits with discharged patients, a final group debriefing, and letters to patients primary care providers. Preassigned medical and pharmacy student partners coordinated discharges and conducted postdischarge visits. The change in students attitudes and skills in interdisciplinary collaboration and discharge planning was assessed using a 5-point Likert-scaled survey given before and after the curriculum, and students reported their satisfaction using additional Likert-scaled and open-ended questions. RESULTS: The program was completed by 97% of students (37 of 39 medical, 22 of 22 pharmacy). The postcurriculum survey response rates were 92% and 86%, respectively; matched response rates were 58% and 59%. The attitudes and selfassessed skills of both medical and pharmacy students significantly improved for most survey items after the curriculum. Students also reported that the curriculum had a favorable impact on their learning about interdisciplinary care (4.3, SD 0.72), humanism (4.3, SD 0.63), and discharge planning (4.4, SD 0.70). Ninety-three percent reported that the curriculum was valuable to their education. CONCLUSIONS: A clinically oriented curriculum with postdischarge visits improved students attitudes and self-assessed skills in interdisciplinary collaboration and transitional care and fostered a patient-centered approach to care. Journal of Hospital Medicine 2008;3: Society of Hospital Medicine. KEYWORDS: interdisciplinary, home visit, transitional care, medical student, pharmacy student. Supported by a UCSF Academy of Medical Educators Innovations Funding grant. This work was presented in part as an innovations poster at the 29th Annual Society of General Internal Medicine Meeting, Los Angeles, April 2006, and at the Annual Society of Hospital Medicine Meeting, Washington, DC, May The authors gratefully acknowledge Deborah Airo for editorial review and Kathleen Kerr for statistical support. The increasing burden of chronic illness has prompted concerns about the traditional education model that focuses on management of acute disease. 1 3 Chronic illness has replaced acute disease as the major cause of disability and total national health care expenditures. 4 6 Medical educators have called for improved chronic disease curricula, 2,3 and the Institute of Medicine has asserted that health professions, including medicine and pharmacy, must reexamine how students are educated to manage patients with complex illnesses. 7,8 Despite the rising prevalence of chronic illness, the positive attitudes of medical students toward Society of Hospital Medicine DOI /jhm.264 Published online in Wiley InterScience (
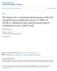
2 providing care to such patients decline during training. 2,9 One theory is that the current model of core clerkship training excessively exposes students to highly complex, seriously ill hospitalized patients. Students may become disillusioned and overwhelmed by these encounters, particularly without the opportunity to see improvement or thriving in the outpatient setting. 2 There are few curricula on how to transition chronically ill patients from an inpatient to an outpatient setting and the inherent safety risks of this transition. For these patients, the posthospital discharge period is particularly confusing because of the sudden change in health status and new medication regimens It is very likely that communication among providers and patients will be insufficient during the discharge process, 11,13 15 yet physicians tend to overestimate patients understanding of postdischarge treatment plans and thereby underanticipate problems. 16 One intervention to address these concerns is a postdischarge visit. Home visits have been shown to improve students understanding of continuity of care and of the impact of chronic illness on their patients medical and psychosocial situations There is scant structured teaching of third-year medical students about another critical aspect of transitional care: the role of different health care disciplines. Although research about the impact of undergraduate interdisciplinary education on patient outcomes is limited, training students in interdisciplinary collaboration may improve their ability to provide quality care Multiple disciplines are critical for a smooth transition of chronically ill patients from an inpatient to an outpatient setting. In particular, pharmacist involvement in a predischarge medication review, patient counseling, and telephone follow-up has been associated with improved outcomes. 11,12,23,24 Early introduction of interdisciplinary team training can improve student attitudes about working within a team. 25 To teach the importance of safe discharges and interdisciplinary collaboration in caring for chronically ill patients, we developed an inpatient medicine clerkship curriculum for medical and pharmacy students that included postdischarge visits to students own team patients. The purpose of the study was to assess the impact of this didactic and experiential curriculum on students attitudes and self-assessed skills in the interdisciplinary care and transitional care of chronically ill patients. We hypothesized that the discharge curriculum would improve student attitudes and self-assessed skills in these domains. Finally, we hypothesized that visiting a patient s home would highlight for students the potential challenges of care transitions for patients. METHODS Participants and Setting Participants were third-year medical students on an 8-week internal medicine (IM) clerkship and fourth-year pharmacy students on a 6-week pharmacy practice clerkship at a tertiary-care university-based hospital between April 2005 and April The hospital is 1 of 3 IM clerkship sites for medical students and 1 of 9 for pharmacy students. This site was selected because it included both medical and pharmacy students on most inpatient teams. Clerkship students were assigned to all 7 medical teams, each consisting of an attending physician, a senior IM resident (postgraduate year 2 or 3), 2 IM interns (postgraduate year 1), 1 or 2 medical students, and up to 1 pharmacy student. Hospitalists covered 52% of inpatient months, with the remainder staffed by faculty primary care physicians, specialists, or chief residents. Although only three-quarters of the medical teams were randomly assigned a pharmacy student at any given point, each team had a pharmacy student for a portion of time that overlapped with the rotation of the medical students. Over the year, 8-10 medical students rotated on the service during each of 6 blocks, and 4-6 pharmacy students and 1 pharmacy practice resident rotated during each of 8 blocks. The pharmacy students rotated on a different schedule than the medical students, and thus the curriculum was scheduled around the medical students clerkship. The Institutional Review Board of the University of California at San Francisco approved the study. Intervention (Curriculum Description) We developed a 3-part pilot interdisciplinary curriculum (Fig. 1). During the first 2 weeks of the IM clerkship, interdisciplinary faculty, including 3 pharmacists, 2 hospitalists, and occasionally a social worker and geriatric clinical nurse specialist, led a 1-hour interactive workshop on transitional care. The 3 workshop topics were: roles that various disciplines such as social work and pharmacy play in discharge care; the challenges a patient faces Postdischarge Follow-Up Visits for Medical/Pharmacy Students / Lai et al. 21
3 FIGURE 1. Discharge curriculum for medical and pharmacy students on an inpatient medicine clerkship. around the time of discharge, using a typical case; and discussion of elements of a postdischarge visit. Medical and pharmacy students were partnered based on clerkship team assignments in teams of up to 3 student partners (1 or 2 medical students and 1 pharmacy student). Partners were advised to select a consenting patient known to them from the ward team for 1 postdischarge visit. Suggested selection criteria were at least 1 chronic illness, 1 prior hospitalization, and older than age 65 because patients fitting these criteria are most at risk for readmission or adverse outcomes following discharge. 15,26,27 The student partners scheduled a postdischarge visit by the end of the rotation to the patient s home, nursing home, or subacute care facility. Each patient and the patient s primary care provider (PCP) gave informed consent. During the postdischarge visit, student partners assessed medication discrepancies, environmental safety, and clinical status using structured data collection protocols developed by the investigators after review of the literature. 28,29 After the visit, students reported back to the ward teams on the patient s status and wrote a visit summary letter to the patient s PCP. The letter described the patient s clinical status and home environment, any medication discrepancies, and follow-up plans and included a reflection piece. Reflection questions included, How did the visit change your perspective of patient discharge? What were the most critical aspects of this or any discharge? How do you think this experience will affect your future practice? What was the best thing about this experience? During the last 2 weeks of the rotation, all student participants met with faculty preceptors for an hour-long group debriefing session on the postdischarge visits. Survey Instrument and Procedure Students were asked to complete a presurvey at the beginning of the first workshop and a postsurvey at the end of the second (debriefing) workshop. The surveys contained self-assessment questions on attitudes and skills in 3 domains: interdisciplinary care, chronic illness management, and transitional care. Questions were developed and tested with IM faculty with experience in student education and with ineligible students on previous rotations, and questions were revised for clarity and comprehensiveness. Students had the option to write a 4-digit identifier on the pre- and postsurveys to allow matched analysis. The 10-item presurvey contained 4 items on interdisciplinary care and 3 each on chronic care and follow-up visits. We reviewed surveys in the literature regarding home care and chronic illness to inform the development of our survey. 30,31 Students rated each item on a 5-point Likert scale, ranging from 1 (strongly disagree) to 5 (strongly agree). The 22-item postsurvey included the same 10 items and additional Likert-scaled questions on satisfaction with the curriculum. Two open-ended questions solicited opinions about the value of the program and lessons learned for future patient encounters. Statistical Analysis We assessed the mean Likert score ( SD) for each presurvey and postsurvey question and compared means ( SD). We evaluated the differences between medical students and for pharmacy students in mean Likert score on the surveys using a dependent-samples t test and set the level of significance at Journal of Hospital Medicine Vol 3/No 1/Jan/Feb 2008
4 Change in scores between pre post survey variables were calculated overall and within student type (medicine vs. pharmacy). Because no intercorrelations and possible patterns indicating a structure were found, a factor analysis was not conducted. Two investigators (C.L., H.N.) read all written responses to the open-ended questions and independently generated a list of themes. The list was reconciled through discussion and was used to code all comments in order to determine the frequency of each theme. Discrepancies were discussed until consensus was reached. RESULTS Participants Ninety-seven percent of eligible students (37 of 39 medical students and 22 of 22 pharmacy students) completed the curriculum. Two medical students did not complete the home visit because their patients did not keep the appointment. The presurvey response was 100% for medical students and 91% for pharmacy students. The postsurvey response was 92% for medical students and 86% for pharmacy students; 58% of medical students and 59% of pharmacy students wrote in matching pre post survey identifiers for statistical analysis. Pre post survey responses showed an increase for both student groups in positive attitudes and self-assessed skill in interdisciplinary collaboration, chronic illness management, and transitional care. Trends over time were highly significant for individual items on matched surveys (P 0.05; Table 1a,b). Twenty-two student partners of 1 or 2 medical students and 1 pharmacy student visited 22 patients (64% women; mean age 71 years). Most visits (91%) occurred at patients homes. Students were satisfied with the curriculum (Table 2). Both the medical and the pharmacy students perceived the 2 most valuable components to be the interdisciplinary collaboration on patient care and the postdischarge visit, followed by the debriefing session. The least useful were the initial workshop on interdisciplinary roles and the writeup to the PCP. Ninety-one percent of students agreed that they learned skills valuable for future patient care (medical students 4.4, SD 0.61; pharmacy students 4.1, SD 0.62; Table 3). Most students agreed that the program enhanced their learning about interdisciplinary care (4.3, SD 0.72), discharge planning (4.4, SD 0.70), and humanism (4.4, SD 0.63). Ninety-three percent agreed that this curriculum was valuable to their education. Open-Ended Comments on Educational Value Twenty-nine medical students and 15 pharmacy students wrote responses to the open-ended questions. Students identified the most valuable component of the curriculum as seeing patients at home in their social context (30 total comments). In the reflection write-up, one student explained, I was unaware of the types of living conditions many patients face, especially in the setting of chronic disease. In the future I will try to gain a more detailed understanding of my patients social situations in order to help identify and anticipate problems in the management of their medical issues. Thirteen students commented that working as an interdisciplinary team was a valuable experience. Eight students expressed appreciation at learning about transitional care and the components of discharge planning. I was a little surprised during this home visit to find how much Ms. C had altered her medication regimen. She didn t like how she was feeling on the higher blood pressure medications, so she halved them. She doesn t really like taking pills, in general, so she stopped taking the aspirin, Senna, and Colace. I suppose something that might have made this discharge more successful would have been if we had really elicited her preferences regarding medications while she was in the hospital, such that we could have been more selective in what we prescribed and very clear with her with respect to what exactly we were hoping to accomplish with each. During group debriefing, students reinforced the themes in their written comments and shared additional reflections. Students observed a shift in dynamics between patient and student provider; the patients appeared more comfortable in familiar settings. Students were also surprised that many of their patients did not have a clear understanding of medication regimens at home. In addition, they discussed the importance of communicating with patients PCPs about the hospital course and follow-up. Also during the debriefing, students expressed the value of the postdischarge visit and interdisciplinary collaboration. Medical students appreciated seeing how the pharmacy students reviewed medications and taught patients how to use their medications. However, the students thought that prep- Postdischarge Follow-Up Visits for Medical/Pharmacy Students / Lai et al. 23
5 TABLE 1 Attitudes and Self-Rated Skills of Medical and Pharmacy Students in Interdisciplinary Care, Transitional Care, and Chronic Illness Management Before and After a Discharge Planning Curriculum Medical students (matched respondents n 23) Pharmacy students (matched respondents n 13) Question Presurvey, mean (SD) Postsurvey, mean (SD) Mean difference P value Effect size Presurvey, mean (SD) Postsurvey, mean (SD) Mean difference P value Effect size 1. I am able to state the various roles of the pharmacy students and/or pharmacists (or medical students and/or physicians) in taking care of hospitalized patients (0.89) 4.35 (0.57) * (0.63) 4.15 (0.38) * I am able to state the various roles of the case manager and/or social worker in taking care of hospitalized patients (0.78) 3.91 (0.42) * (0.83) 3.54 (0.97) * I am confident in my ability to work with a pharmacy student or pharmacist (or medical student and/or physician) in taking care of inpatients with chronic illness (1.00) 4.52 (0.51) * (0.87) 4.23 (0.44) * I am confident in my ability to work with a case manager and/or social worker in taking care of inpatients with chronic illness (0.71) 3.96 (0.56) * (0.95) 3.38 (0.87) I am confident in my ability to involve patients in making a plan for their care (0.62) 4.26 (0.54) * (0.60) 4.15 (0.55) * I am able to assist patients in solving problems they encounter in selfmanagement of their chronic illness (0.70) 3.91 (0.60) * (0.87) 3.92 (0.49) I am confident in my ability to review patients medications and side effects (0.85) 3.70 (0.76) * (0.76) 4.46 (0.52) * I am able to review the goals of a followup visit with a patient (0.95) 4.43 (0.51) * (0.76) 3.62 (0.77) I can identify factors that may facilitate or impede a patient s transition to an outpatient setting (0.51) 4.35 (0.49) * (0.82) 3.85 (0.69) * I can identify several topics for review at a follow-up visit to confirm a safe transition to an outpatient setting (0.94) 4.52 (0.59) * (0.73) 3.77 (0.73) Likert scale: 1 strongly disagree, 2 disagree, 3 neutral, 4 agree, 5 strongly agree; *statistically significant. TABLE 2 Satisfaction of Medical and Pharmacy Students with a Discharge Planning Curriculum Component Mean score* (SD) Rated very good or excellent (%) Joint patient care with medical/pharmacy student 4.5 (1.04) 94% Postdischarge visit 4.3 (0.68) 91% Debriefing session 3.9 (1.04) 75% Team presentation after patient visit 3.7 (1.32) 63% Case-based workshop 3.6 (1.18) 54% Write-up on experience 3.4 (0.81) 48% Overall program 4.1 (1.14) 86% All respondents: n 53; medical students n 35, pharmacy students n 18. *Likert scale: 1 poor, 2 fair, 3 good, 4 very good, 5 excellent. 24 Journal of Hospital Medicine Vol 3/No 1/Jan/Feb 2008
6 TABLE 3 Student Assessment of Impact of a Discharge Curriculum Medical students (n 35) Pharmacy students (n 18) All students (n 53) Mean score* (SD) Agree/strongly agree (%) Mean score (SD) Agree/strongly agree (%) Mean score (SD) Agree/strongly agree (%) I have learned skills from this program that I plan to apply to future patient care experiences. 4.4 (0.61) 94% 4.1 (0.62) 84% 4.3 (0.63) 91% This program added to my learning about an interdisciplinary approach to patient care beyond the other experiences of this clerkship. 4.3 (0.74) 91% 4.2 (0.71) 84% 4.3 (0.72) 89% This program added to my learning about discharge planning and transitional care beyond the other experiences of this clerkship. 4.4 (0.66) 91% 4.2 (0.79) 89% 4.4 (0.70) 91% This program added to my understanding of a patient as a whole person beyond the other experiences of this clerkship. 4.3 (0.69) 89% 4.5 (0.51) 100% 4.4 (0.63) 93% This program was valuable to my medical education. 4.3 (0.74) 91% 4.4 (0.60) 95% 4.4 (0.68) 93% *Likert scale: 1 strongly disagree, 2 disagree, 3 neutral, 4 agree, 5 strongly agree. aration of paperwork prior to the visit and the write-up seemed less valuable. DISCUSSION A discharge curriculum that included a postdischarge visit to a recently hospitalized patient improved the attitudes and self-assessed skills of third-year medical students and fourth-year pharmacy students about interdisciplinary collaboration and transitions in care. It also deepened their appreciation of the impact of chronic illness on individual patients. To our knowledge, this is the first study to report an interdisciplinary curriculum with postdischarge home visits for students on their inpatient medicine clerkship. Our curriculum was unique because its activities were linked to patients the students had cared for in the inpatient setting, a relationship that was key to students accepting the curriculum, as was the autonomy they had in selecting one of their patients for a visit. Although home visits are often part of medical school training, they generally occur in the preclinical years 5,19 or during third-year primary care rotations, during which students are assigned patients at home or in outpatient facilities. 17,32 Home visits have been qualitatively reported to be a valuable aspect of geriatric, primary care, and other ambulatory-based rotations of medical students. 17,19,32 Postdischarge visits in graduate medical education have been shown to improve residents awareness of and skills with transitions in care. 28,33,34 Another novel aspect of this curriculum was the interdisciplinary collaboration in discharge planning and postdischarge visits. Although educators have implemented conferences on interdisciplinary education in preclinical medical education, patient-centered curricula in real-time allow realistic interdisciplinary collaboration between medical and pharmacy students in their core clerkships. In our study, quantitative and qualitative data showed that the student partners valued each other s expertise in the context of a clinically relevant activity discharge planning and a follow-up home visit. Students reported confidence in their collaborative abilities after completing the curriculum, and comments supported a broadened understanding of other professionals roles in patient care. Given that pharmacist involvement in discharge planning has been shown to improve patient outcomes, 11,24 our study supports the idea that medical educators should develop structured curricula on interdisciplinary training in core clerkships. By evaluating the impact of hospitalization and chronic illness on their patients after discharge, our students developed an appreciation for safe transitions and opportunities to improve patients health and level of function. We observed that students also appreciated the positive effect of the home environment on patient health and well-being. From their postdischarge visit, students also became aware of the need for communication with primary care providers, particularly for patients with comorbidities. This type of transitional care Postdischarge Follow-Up Visits for Medical/Pharmacy Students / Lai et al. 25
7 experience may help to counter the negative attitudes toward chronic illness that students typically develop during clerkships. 2,9,38,39 Of note, although pharmacy students reported improvement in their attitudes and skills with transitional care, the trend toward significance was less than that for medical students. This difference was consistent with the broader rotation goals of each group. At the end of the curriculum, the pharmacy students expressed more comfort with medication review than did medical students, although the latter were better able to conduct transitional care including postdischarge visits and identification of barriers or facilitators to a safe discharge. Another interesting note is that pharmacy students came into the curriculum with a better understanding of the roles of physicians, whereas the medical students had a less clear idea of the pharmacist s role. A possible explanation is that pharmacy students are better trained in their preclinical years to work as a team with medical personnel. The pharmacy school curriculum places an emphasis on independent learning and interdisciplinary collaboration, which may lead to the greater comfort felt by the pharmacy students. This study had several limitations. The absolute number of visits was small overall; however, nearly all student partners completed their visits. Although the response rate to the postcurriculum survey was high, the response rate to matched pre post surveys was lower. In addition, the survey questions were not validated. Further, although there was significant improvement in students attitudes and self-assessed skills after completion of the curriculum, we cannot be certain whether this improvement was a result of the curriculum or of other rotation experiences. We attempted to clarify this effect by asking if the curriculum added to their learning beyond other clerkship experiences, and students perceived that our curriculum was responsible for the positive effect. Also, the curriculum was used at 1 academic site and may not be generalizable to other hospitals, student populations, or team structures. The patients were selected by students, and thus the results may not be reproducible for every population; in some situations, students had to ask several patients until a patient consented to a postdischarge visit. In implementing this interdisciplinary curriculum, we were challenged by the discordant schedules of the medical and pharmacy students. Initially, it was also difficult to overcome students concerns about adding an additional expectation to an already busy rotation. The medical students, in particular, voiced concerns about having to leave the hospital during their inpatient rotation. However, this has become much less of an issue with time as the value of the postdischarge visit has become clear to students and team members, with the latter now aware of and supportive of the program. This discharge curriculum represents a clinically relevant experience that addresses national educational mandates regarding interdisciplinary care and chronic illness across care settings. We are now expanding the curriculum from the original site to our other clerkship sites and are evaluating its impact on patient safety and clinical outcomes. Future research should focus on whether these interdisciplinary postdischarge patient visits lead to improved attitudes and skills during residency training or practice and whether, ultimately, they lead to improved patient outcomes. Address for correspondence and reprint requests: Cindy J. Lai, MD, University of California, San Francisco, 505 Parnassus, M1078, Box 0120, San Francisco, CA 94143; Fax: (415) ; clai@medicine.ucsf.edu Received 10 April 2007; revision received 1 July 2007; accepted 9 July REFERENCES 1. Fitzpatrick SB, O Donnell R, Getson P, Sahler OJ, Goldberg R, Greenberg LW. Medical students experiences with and perceptions of chronic illness prior to medical school. Med Educ. 1993;27: Davis BE, Nelson DB, Sahler OJ, McCurdy FA, Goldberg R, Greenberg LW. Do clerkship experiences affect medical students attitudes toward chronically ill patients? Acad Med. 2001;76: Darer JD, Hwang W, Pham H, Bass EB, Anderson G. More training needed in chronic care: a survey of US physicians. Acad Med. 2004;79: Holman, H. Chronic disease the need for a new clinical education. JAMA. 2004;292: Wagner PJ, Jester DM, Moseley GC. Medical students as health coaches. Acad Med. 2002;77: Hoffman C, Rice D, Sung HY. Persons with chronic conditions. Their prevalence and costs. JAMA. 1996;276: Kohn LT, Corrigan JM, Donaldson MS. To Err Is Human. Washington, DC: National Academy Press; Institute of Medicine. Health Professions Education: A Bridge to Quality. Washington DC: National Academy Press; Griffith CH, Wilson JF. The loss of student idealism in the 3rd-year clinical clerkships. Eval Health Prof. 2001:24: Forster AJ, Murff HJ, Peterson JF, Gandhi TK, Bates DW. Adverse drug events occurring following hospital discharge. J Gen Intern Med. 2005;20: Journal of Hospital Medicine Vol 3/No 1/Jan/Feb 2008
8 11. Schnipper JL, Kirwin JL, Cotugno MC, et al. Role of pharmacist counseling in preventing adverse drug events after hospitalization. Arch Intern Med. 2006;166: Crotty M, Rowett D, Spurling L, Giles LC, Phillips PA. Does the addition of a pharmacist transition coordinator improve evidence-based medication management and health outcomes in older adults moving from the hospital to a longterm care facility? Results of a randomized, controlled trial. Am J Geriatr Pharmacother. 2004;2: Forster AJ, Murff HJ, Peterson JF, Gandhi TK, Bates DW. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med. 2003;138: Coleman EA, Smith JD, Raha D, Min SJ. Posthospital medication discrepancies: Prevalence and contributing factors. Arch Intern Med. 2005;165: Forster AJ, Clark HD, Menard A, et al. Adverse events among medical patients after discharge from hospital. CMAJ. 2004; 170: Calkins DR, Davis RB, Reiley P, et al. Patient-physician communication at hospital discharge and patients understanding of the postdischarge treatment plan. Arch Intern Med. 1997;157: Yuen JK, Breckman R, Adelman RD, Capello CF, Lofaso V, Carrington Reid M. Reflections of medical students on visiting chronically ill older patients in the home. J Am Geriatr Soc. 2006;54: Levine SA, Boal J, Boling PA. Home care. JAMA. 2003;290: Medina-Walpole A, Heppard B, Clark NS, Markakis K, Tripler S, Quill T. Mi casa o su casa? Assessing function and values in the home. J Am Geriatr Soc. 2005;53: Hall P, Weaver L. Interdisciplinary education, and teamwork: a long and winding road. Med Educ. 2001;35: Fineberg IC, Wenger NS, Forrow L. Interdisciplinary education: evaluation of a palliative care training intervention for pre-professionals. Acad Med. 2004;79: Gilkey MB, Earp JA. Effective interdisciplinary training: Lessons from the University of North Carolina s Student Health Action Coalition. Acad Med. 2006;81: Dudas V, Bookwalter T, Kerr KM, Pantilat SZ. The impact of follow-up telephone calls to patients after hospitalization. Am J Med. 2001;111(9B):26S 30S. 24. Kaboli PJ, Hoth AB, McClimon BJ, Schnipper JL. Clinical pharmacists and inpatient medical care: A systematic review. Arch Intern Med. 2006;166: Cooper H, Carlisle C, Gibbs T, Watkins C. Developing an evidence base for interdisciplinary learning: a systematic review. J Adv Nurs. 2001;35: Marcantonio ER, McKean S, Goldfinger M, Kleefield S, Yurkofsky M, Brennan TA. Factors associated with unplanned hospital readmission among patients 65 years of age and older in a Medicare managed care plan. Am J Med. 1999;107: Reed RL, Pearlman RA, Buchner DM. Risk factors for early unplanned hospital readmission in the elderly. J Gen Intern Med. 1991;6: Matter CA, Speice JA, McCann JR, et al. Hospital to home: Improving internal medicine residents understanding of the needs of older persons after a hospital stay. Acad Med. 2003;78: Coleman, E. Care transitions program. University of Colorado at Denver, Health Sciences Center. Available at: Accessed April 9, Boal J, Fabacher D, Miller R, Siu A, Kantor B, Flaherty J. Validation of an instrument designed to assess medical student attitudes toward home care. J Am Geriatr Soc. 2001;49: Patient Assessment of Chronic Illness Care (PACIC) from Improving Chronic Illness Care, a national program of the Robert Wood Johnson Foundation. Available at: Accessed April 9, Flaherty JH, Fabacher DA, Miller R, Fox A, Boal J. The determinants of attitudinal change among medical students participating in home care training: A multi-center study. Acad Med. 2002;77: Laditka SB, Fischer M, Mathews KB, Sadlik JM, Warfel ME. There s no place like home: Evaluating family medicine residents training in home care. Home Health Care Serv Q. 2002;21: Hansen FR, Spedtsberg K, Schrool M. Geriatric follow-up by home visits after discharge from hospital: a randomized controlled trial. Age Ageing. 1992;21: Horsburgh M, Lamdin R, Williamson E. Multiprofessional learning: the attitudes of medical nursing, and pharmacy students to shared learning. Med Educ. 2001;35: Harward DH, Tresolini CP, Davis WA. Can participation in a health affairs interdisciplinary case conference improve medical students knowledge and attitudes? Acad Med. 2006; 81: Hope JM, Lugassy D, Meyer R, et al. Bringing interdisciplinary and multicultural team building to health care education: the Downstate Team-Building Initiative. Acad Med. 2005;80: Turner J, Pugh J and Budiani MA. It s always continuing : First year medical students perspectives on chronic illness and the care of chronically ill patients. Acad Med. 2005;80: Pham HH, Simonson L, Elnicki DM, Fried LP, Goroll AH, Bass EB. Training U.S. medical students to care for the chronically ill. Acad Med. 2004;79: Postdischarge Follow-Up Visits for Medical/Pharmacy Students / Lai et al. 27
INSTRUCTIONAL DESIGN AND ASSESSMENT Peer-to-Peer Interprofessional Health Policy Education for Medicare Part D
 INSTRUCTIONAL DESIGN AND ASSESSMENT Peer-to-Peer Interprofessional Health Policy Education for Medicare Part D Helene L. Lipton, PhD, a,b Cindy J. Lai, MD, c Timothy W. Cutler, PharmD, a Amanda R. Smith,
INSTRUCTIONAL DESIGN AND ASSESSMENT Peer-to-Peer Interprofessional Health Policy Education for Medicare Part D Helene L. Lipton, PhD, a,b Cindy J. Lai, MD, c Timothy W. Cutler, PharmD, a Amanda R. Smith,
Physician Use of Advance Care Planning Discussions in a Diverse Hospitalized Population
 J Immigrant Minority Health (2011) 13:620 624 DOI 10.1007/s10903-010-9361-5 BRIEF COMMUNICATION Physician Use of Advance Care Planning Discussions in a Diverse Hospitalized Population Sonali P. Kulkarni
J Immigrant Minority Health (2011) 13:620 624 DOI 10.1007/s10903-010-9361-5 BRIEF COMMUNICATION Physician Use of Advance Care Planning Discussions in a Diverse Hospitalized Population Sonali P. Kulkarni
Objectives. Prevalence of Non-Adherence. Medications and Care Transitions. The Cost of Readmissions. The Pharmacist s Role in Improving Care 4/22/2015
 MEDS TO BEDS: DELIVERING REDUCED READMISSIONS, LOWER COSTS, AND IMPROVED QUALITY Laura S. Carr PharmD, Senior Attending Pharmacist, Transitional Care Massachusetts General Hospital Ed Cohen, PharmD, FAPhA
MEDS TO BEDS: DELIVERING REDUCED READMISSIONS, LOWER COSTS, AND IMPROVED QUALITY Laura S. Carr PharmD, Senior Attending Pharmacist, Transitional Care Massachusetts General Hospital Ed Cohen, PharmD, FAPhA
Improving Transitions to Home & Community- Based Care Settings
 This presenter has nothing to disclose. Improving Transitions to Home & Community- Based Care Settings Eric Coleman September 29, 2015 Session Objectives Participants will be able to: Describe the role
This presenter has nothing to disclose. Improving Transitions to Home & Community- Based Care Settings Eric Coleman September 29, 2015 Session Objectives Participants will be able to: Describe the role
INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism
 INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism Bonnie Brehm, PhD, a Phyllis Breen, MA, b Bethanne Brown, PharmD, c Lisa Long, MS, a Rebecca Smith, MEd,
INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism Bonnie Brehm, PhD, a Phyllis Breen, MA, b Bethanne Brown, PharmD, c Lisa Long, MS, a Rebecca Smith, MEd,
Bringing the Clinical Mindset to the Retail Pharmacist
 Bringing the Clinical Mindset to the Retail Pharmacist Sarah Griffin, Pharm.D. Harding University College of Pharmacy White County Medical Center Objectives Describe challenging situations faced by pharmacists
Bringing the Clinical Mindset to the Retail Pharmacist Sarah Griffin, Pharm.D. Harding University College of Pharmacy White County Medical Center Objectives Describe challenging situations faced by pharmacists
SO YOU WANT TO IMPROVE THE DISCHARGE PROCESS?
 Who are we? Why are we here? SO YOU WANT TO IMPROVE THE DISCHARGE PROCESS? Michelle Mourad MD Arpana Vidyarthi Ellen Kynoch Oh Betty Why Betty? pulmonary edema sodium intake & daily weights What makes
Who are we? Why are we here? SO YOU WANT TO IMPROVE THE DISCHARGE PROCESS? Michelle Mourad MD Arpana Vidyarthi Ellen Kynoch Oh Betty Why Betty? pulmonary edema sodium intake & daily weights What makes
Pharmacists Role in Care Transitions
 Pharmacists Role in Care Transitions SHE A FA NNING, PHA RMD, PGY 1 PHA RMA C Y RE SIDENT ST. PETER S HOSPITAL HE LE NA, MT Disclosures Co-investigators: Thomas Richardson, PharmD, BCPS AQ-ID; Brad Hornung,
Pharmacists Role in Care Transitions SHE A FA NNING, PHA RMD, PGY 1 PHA RMA C Y RE SIDENT ST. PETER S HOSPITAL HE LE NA, MT Disclosures Co-investigators: Thomas Richardson, PharmD, BCPS AQ-ID; Brad Hornung,
Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic
 INNOVATION AND IMPROVEMENT Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic Kathleen Heist, MD 1, Mary Guese, MD 2, Michelle Nikels, MD 1, Rachel Swigris, DO 1, and Karen Chacko,
INNOVATION AND IMPROVEMENT Impact of 4+1 Block Scheduling on Patient Care Continuity in Resident Clinic Kathleen Heist, MD 1, Mary Guese, MD 2, Michelle Nikels, MD 1, Rachel Swigris, DO 1, and Karen Chacko,
Marshall Digital Scholar. Marshall University. Brittany Snodgrass. Charles K. Babcock Marshall University,
 Marshall University Marshall Digital Scholar Pharmacy Practice & Administration Faculty Research 2013 The impact of a community pharmacist conducted comprehensive medication review (CMR) on 30-day re-admission
Marshall University Marshall Digital Scholar Pharmacy Practice & Administration Faculty Research 2013 The impact of a community pharmacist conducted comprehensive medication review (CMR) on 30-day re-admission
10/27/10. Michelle Mourad MD Arpana Vidyarthi Ellen Kynoch. pulmonary edema. sodium intake & daily weights
 Michelle Mourad MD Arpana Vidyarthi Ellen Kynoch pulmonary edema sodium intake & daily weights 1 What makes her at risk for readmission? Why didn t she listen to her doctors about her salt intake? Did
Michelle Mourad MD Arpana Vidyarthi Ellen Kynoch pulmonary edema sodium intake & daily weights 1 What makes her at risk for readmission? Why didn t she listen to her doctors about her salt intake? Did
Optimizing Patient Outcomes at the Transition of Care: From Inpatient to Skilled Nursing Facility
 Optimizing Patient Outcomes at the Transition of Care: From Inpatient to Skilled Nursing Facility Cynthia Williams, B.S.Pharm, FASHP Vice President/Chief Pharmacy Officer Riverside Health System, Newport
Optimizing Patient Outcomes at the Transition of Care: From Inpatient to Skilled Nursing Facility Cynthia Williams, B.S.Pharm, FASHP Vice President/Chief Pharmacy Officer Riverside Health System, Newport
EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists
 EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists Micah Hata, PharmD, a Roger Klotz, BSPharm, a Rick Sylvies, PharmD, b Karl Hess, PharmD, a Emmanuelle Schwartzman,
EXPERIENTIAL EDUCATION Medication Therapy Management Services Provided by Student Pharmacists Micah Hata, PharmD, a Roger Klotz, BSPharm, a Rick Sylvies, PharmD, b Karl Hess, PharmD, a Emmanuelle Schwartzman,
Note EDUCATION. Keywords: Pharmacists Patient Care Process, faculty development, video
 Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Are We a Team of Experts or an Expert Team?
 Are We a Team of Experts or an Expert Team? BEST PRACTICES: Care for the Complex Community Dwelling Older Adult July 11 12, 2008 NEBGEC Annual Conference Katherine Jones, PT, PhD kjonesj@unmc.edu Objectives
Are We a Team of Experts or an Expert Team? BEST PRACTICES: Care for the Complex Community Dwelling Older Adult July 11 12, 2008 NEBGEC Annual Conference Katherine Jones, PT, PhD kjonesj@unmc.edu Objectives
Community Care Coordination Cross Continuum Care IHC Medical Home Conference September 5, 2012 Des Moines IA
 Community Care Coordination Cross Continuum Care IHC Medical Home Conference September 5, 2012 Des Moines IA Peg Bradke, RN, MA Director of Heart Care Services St. Luke s Hospital, Cedar Rapids, IA Session
Community Care Coordination Cross Continuum Care IHC Medical Home Conference September 5, 2012 Des Moines IA Peg Bradke, RN, MA Director of Heart Care Services St. Luke s Hospital, Cedar Rapids, IA Session
Academic medical centers are under considerable pressure to reduce costs Caregiver Perceptions of the Reasons for Delayed Hospital Discharge
 ORIGINAL ARTICLE TRACEY M. MINICHIELLO, MD ANDREW D. AUERBACH, MD, MPH ROBERT M. WACHTER, MD University of California, San Francisco San Francisco, Calif Eff Clin Pract. 2001;4:250 255. Caregiver Perceptions
ORIGINAL ARTICLE TRACEY M. MINICHIELLO, MD ANDREW D. AUERBACH, MD, MPH ROBERT M. WACHTER, MD University of California, San Francisco San Francisco, Calif Eff Clin Pract. 2001;4:250 255. Caregiver Perceptions
Journal of the Association of American Medical Colleges ACCEPTED
 Journal of the Association of American Medical Colleges Uncomposed, edited manuscript published online ahead of print. This published ahead-of-print manuscript is not the final version of this article,
Journal of the Association of American Medical Colleges Uncomposed, edited manuscript published online ahead of print. This published ahead-of-print manuscript is not the final version of this article,
Medication Reconciliation for Older Adults Transitioning from. Long-Term Care to Home. Allison (Leverett) Kackman
 Medication Reconciliation for Older Adults Transitioning from Long-Term Care to Home By Allison (Leverett) Kackman Washington State University Spokane. Riverpoint campus Ubrary P.O. Box 1495 Spokane, WA
Medication Reconciliation for Older Adults Transitioning from Long-Term Care to Home By Allison (Leverett) Kackman Washington State University Spokane. Riverpoint campus Ubrary P.O. Box 1495 Spokane, WA
Avoiding Errors During Transitions of Care: Medication Reconciliation
 in in Practice Avoiding Errors During Transitions of Care: Medication Reconciliation When medication errors occur, they often are the result of discrepancies in medication information during transitions
in in Practice Avoiding Errors During Transitions of Care: Medication Reconciliation When medication errors occur, they often are the result of discrepancies in medication information during transitions
Definitions. Using Physician Extenders on Inpatient Resident Teams to help meet. Kathleen Finn, MD. ACGME Requirements. Physician Extenders
 Using Physician Extenders on Inpatient Resident Teams to help meet ACGME Requirements Kathleen Finn, MD John Moriarty, MD Definitions ACGME Requirements Physician Extenders Clerical Assistants Nurse Practitioners
Using Physician Extenders on Inpatient Resident Teams to help meet ACGME Requirements Kathleen Finn, MD John Moriarty, MD Definitions ACGME Requirements Physician Extenders Clerical Assistants Nurse Practitioners
Improving Transitions of Care
 Improving Transitions of Care Mark V. Williams, MD, FACP, FHM Professor & Chief, Division of Hospital Medicine Northwestern University Feinberg School of Medicine Principal Investigator, Project BOOST
Improving Transitions of Care Mark V. Williams, MD, FACP, FHM Professor & Chief, Division of Hospital Medicine Northwestern University Feinberg School of Medicine Principal Investigator, Project BOOST
Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON
 Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON SCHOOL OF PHARMACY Conflicts of Interest I have no conflicts
Pharmacist Led Transitions of Care in an Indigent Population JEANNA SEWELL, PHARMD, BCACP CLINICAL ASSISTANT PROFESSOR AUBURN UNIVERSITY HARRISON SCHOOL OF PHARMACY Conflicts of Interest I have no conflicts
Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge
 Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge Julianna Burton, Pharm.D., BCPS, BCACP, FCSHP Assistant Chief, Ambulatory Clinical Services
Evaluation of a Pharmacist-Led Bedside Medication Delivery Service for Cardiology Patients at Hospital Discharge Julianna Burton, Pharm.D., BCPS, BCACP, FCSHP Assistant Chief, Ambulatory Clinical Services
Medication Reconciliation in Transitions of Care
 Medication Reconciliation in Transitions of Care Jeff West, RN MPH June 18th, 2015 Adverse Drug Events & Readmissions For every 1,000 hospital admissions, medication reconciliation could prevent 14 adverse
Medication Reconciliation in Transitions of Care Jeff West, RN MPH June 18th, 2015 Adverse Drug Events & Readmissions For every 1,000 hospital admissions, medication reconciliation could prevent 14 adverse
Poor admission medication reconciliation can follow
 Importance of Medication Reconciliation in the Continuum of Care Cynthia R. Hennen, BS, RPh; and James A. Jorgenson, RPh, MS, FASHP Specialty Healthcare Benefits Council Poor admission medication reconciliation
Importance of Medication Reconciliation in the Continuum of Care Cynthia R. Hennen, BS, RPh; and James A. Jorgenson, RPh, MS, FASHP Specialty Healthcare Benefits Council Poor admission medication reconciliation
Health Care Reform s BOOST to Reducing Readmissions
 Health Care Reform s BOOST to Reducing Readmissions Mark V. Williams, MD, FHM Professor & Chief, Division of Hospital Medicine Principal Investigator, Project BOOST Why the Focus on Care Transitions? n
Health Care Reform s BOOST to Reducing Readmissions Mark V. Williams, MD, FHM Professor & Chief, Division of Hospital Medicine Principal Investigator, Project BOOST Why the Focus on Care Transitions? n
TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate
 TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate Heidi Luder, PharmD, MS, BCACP Assistant Professor of Pharmacy Practice University
TransitionRx: Impact of a Community Pharmacy Post-Discharge Medication Therapy Management Program on Hospital Readmission Rate Heidi Luder, PharmD, MS, BCACP Assistant Professor of Pharmacy Practice University
Key Words: Transitions of care, care coordination, medication management, drug therapy problem
 Implementing a Pharmacist-Led Medication Management Pilot to Improve Care Transitions Rachel Root, PharmD, MS* 1, Pamela Phelps, PharmD, FASHP 2, Amanda Brummel, PharmD 2, and Craig Else, PharmD, MBA 3
Implementing a Pharmacist-Led Medication Management Pilot to Improve Care Transitions Rachel Root, PharmD, MS* 1, Pamela Phelps, PharmD, FASHP 2, Amanda Brummel, PharmD 2, and Craig Else, PharmD, MBA 3
IMPROVING INPATIENT TO OUTPATIENT TRANSITION FOR GENERAL MEDICINE CLINIC PATIENTS
 IMPROVING INPATIENT TO OUTPATIENT TRANSITION FOR GENERAL MEDICINE CLINIC PATIENTS JULIE GILBREATH, MD, FACP; RAMON GALLEGOS, RN; PATRICIA REYES 8/2016-1/2017 1 THE TEAM CSE Participants: Julie Gilbreath,
IMPROVING INPATIENT TO OUTPATIENT TRANSITION FOR GENERAL MEDICINE CLINIC PATIENTS JULIE GILBREATH, MD, FACP; RAMON GALLEGOS, RN; PATRICIA REYES 8/2016-1/2017 1 THE TEAM CSE Participants: Julie Gilbreath,
Who Cares About Medication Reconciliation? American Pharmacists Association American Society of Health-system Pharmacists The Joint Commission Agency
 The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
The Impact of Medication Reconciliation Jeffrey W. Gower Pharmacy Resident Saint Alphonsus Regional Medical Center Objectives Understand the definition and components of effective medication reconciliation
Impact of Experiential Education on Pharmacy Students Perceptions of Health Roles
 Impact of Experiential Education on Pharmacy Students Perceptions of Health Roles Kimberly S. Plake and Alan P. Wolfgang School of Pharmacy and Pharmacal Sciences, Purdue University, 1335 R. Heine Pharmacy
Impact of Experiential Education on Pharmacy Students Perceptions of Health Roles Kimberly S. Plake and Alan P. Wolfgang School of Pharmacy and Pharmacal Sciences, Purdue University, 1335 R. Heine Pharmacy
Understanding and improving the quality of medication use: Research in Clinical Pharmacy starting from Academia. Anne Spinewine
 Understanding and improving the quality of medication use: Research in Clinical Pharmacy starting from Academia Clinical Pharmacy Research Group (CLIP) Anne Spinewine 1 04.10.2011 WBI- UCL Research activities
Understanding and improving the quality of medication use: Research in Clinical Pharmacy starting from Academia Clinical Pharmacy Research Group (CLIP) Anne Spinewine 1 04.10.2011 WBI- UCL Research activities
Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS
 Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS Safe and timely discharge of patients from hospitals helps ensure patients well-being
Chapter 14 Regina Qu Appelle Regional Health Authority Safe and Timely Discharge of Hospital Patients 1.0 MAIN POINTS Safe and timely discharge of patients from hospitals helps ensure patients well-being
TRANSITIONS of CARE. Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine
 TRANSITIONS of CARE Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine 5-15-15 Objectives At the conclusion of the presentation, the participant will be able to: 1. Improve
TRANSITIONS of CARE Francis A. Komara, D.O. Michigan State University College of Osteopathic Medicine 5-15-15 Objectives At the conclusion of the presentation, the participant will be able to: 1. Improve
Assessing Resident Competency in an Outpatient Setting
 178 March 2004 Family Medicine Assessing Resident Competency in an Outpatient Setting Andrea L. Wendling, MD Background and Objectives: The Grand Rapids Family Practice Residency Program has been using
178 March 2004 Family Medicine Assessing Resident Competency in an Outpatient Setting Andrea L. Wendling, MD Background and Objectives: The Grand Rapids Family Practice Residency Program has been using
Safe Medication Reconciliation: An Intervention to Improve Residents Medication Reconciliation Skills
 Safe Medication Reconciliation: An Intervention to Improve Residents Medication Reconciliation Skills Cherinne Arundel, MD Jessica Logan, MD Ribka Ayana, MD Jacqueline Gannuscio, DNP, ACNP, AACC Jennifer
Safe Medication Reconciliation: An Intervention to Improve Residents Medication Reconciliation Skills Cherinne Arundel, MD Jessica Logan, MD Ribka Ayana, MD Jacqueline Gannuscio, DNP, ACNP, AACC Jennifer
Improving Emergency Department Transitions of Care Can It Help with ED Overcrowding? Stephen V. Cantrill, MD, FACEP Denver Health Medical Center
 Improving Emergency Department Transitions of Care Can It Help with ED Overcrowding? Stephen V. Cantrill, MD, FACEP Denver Health Medical Center Improving Emergency Department Transitions of Care: Can
Improving Emergency Department Transitions of Care Can It Help with ED Overcrowding? Stephen V. Cantrill, MD, FACEP Denver Health Medical Center Improving Emergency Department Transitions of Care: Can
Physician Advocacy: What is it and how do we train for it? Anastasia Coutinho MD MHS, Christina Kelly MD, Jeff Haney MD.
 Physician Advocacy: What is it and how do we train for it? Anastasia Coutinho MD MHS, Christina Kelly MD, Jeff Haney MD Objectives Differentiate between a health care agent and a health care advocate Define
Physician Advocacy: What is it and how do we train for it? Anastasia Coutinho MD MHS, Christina Kelly MD, Jeff Haney MD Objectives Differentiate between a health care agent and a health care advocate Define
The Care Transitions Intervention
 The Care Transitions Intervention Kimberly Irby, MPH Colorado Foundation for Medical Care www.cfmc.org/integratingcare Acknowledgments: Objectives To provide an overview of the Care Transitions Intervention
The Care Transitions Intervention Kimberly Irby, MPH Colorado Foundation for Medical Care www.cfmc.org/integratingcare Acknowledgments: Objectives To provide an overview of the Care Transitions Intervention
INSTRUCTIONAL DESIGN AND ASSESSMENT An Advanced Pharmacy Practice Experience in Community Engagement
 INSTRUCTIONAL DESIGN AND ASSESSMENT An Advanced Pharmacy Practice Experience in Community Engagement Ann M. Ryan Haddad, PharmD, Kelli L. Coover, PharmD, Kimberley J. Begley, PharmD, and Jennifer A. Tilleman,
INSTRUCTIONAL DESIGN AND ASSESSMENT An Advanced Pharmacy Practice Experience in Community Engagement Ann M. Ryan Haddad, PharmD, Kelli L. Coover, PharmD, Kimberley J. Begley, PharmD, and Jennifer A. Tilleman,
The Case for Home Care Medicine: Access, Quality, Cost
 The Case for Home Care Medicine: Access, Quality, Cost 1. Background Long term care: community models vs. institutional care Compared with most industrialized nations the US relies more on institutional
The Case for Home Care Medicine: Access, Quality, Cost 1. Background Long term care: community models vs. institutional care Compared with most industrialized nations the US relies more on institutional
Patient Satisfaction with Medical Student Participation in the Private OB/Gyn Ambulatory Setting
 Patient Satisfaction with Medical Student Participation in the Private OB/Gyn Ambulatory Setting Katie G. Mellington, MD Faculty Mentor: Benjie B. Mills, MD Disclosure The authors have no meaningful conflicts
Patient Satisfaction with Medical Student Participation in the Private OB/Gyn Ambulatory Setting Katie G. Mellington, MD Faculty Mentor: Benjie B. Mills, MD Disclosure The authors have no meaningful conflicts
Using Data to Inform Quality Improvement
 20 15 10 5 0 Using Data to Inform Quality Improvement Ethan Kuperman, MD FHM Aparna Kamath, MD MS Justin Glasgow, MD PhD Disclosures None of the presenters today have relevant personal or financial conflicts
20 15 10 5 0 Using Data to Inform Quality Improvement Ethan Kuperman, MD FHM Aparna Kamath, MD MS Justin Glasgow, MD PhD Disclosures None of the presenters today have relevant personal or financial conflicts
Medication Use in the Transition from Hospital to Home
 136 Medication Use after Hospital Discharge Yvette M Cua and Sunil Kripalani Commentary Medication Use in the Transition from Hospital to Home Yvette M Cua, 1 MD, Sunil Kripalani, 2 MD, MSc Abstract After
136 Medication Use after Hospital Discharge Yvette M Cua and Sunil Kripalani Commentary Medication Use in the Transition from Hospital to Home Yvette M Cua, 1 MD, Sunil Kripalani, 2 MD, MSc Abstract After
Pharmacists in Transitions of Care: We Can All Make a Difference
 Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Pharmacists in Transitions of Care: We Can All Make a Difference Disclosure The speakers of this panel have no actual or potential conflict of interest in relation to this program to disclose. Kenda Germain,
Effective Care Transitions to Reduce Hospital Readmissions
 Effective Care Transitions to Reduce Hospital Readmissions November 8, 2017 Anchorage, Alaska The vicious cycle of readmissions What is Care Transitions? The movement of patients across settings, referred
Effective Care Transitions to Reduce Hospital Readmissions November 8, 2017 Anchorage, Alaska The vicious cycle of readmissions What is Care Transitions? The movement of patients across settings, referred
ORIGINAL STUDIES. Participants: 100 medical directors (50% response rate).
 ORIGINAL STUDIES Profile of Physicians in the Nursing Home: Time Perception and Barriers to Optimal Medical Practice Thomas V. Caprio, MD, Jurgis Karuza, PhD, and Paul R. Katz, MD Objectives: To describe
ORIGINAL STUDIES Profile of Physicians in the Nursing Home: Time Perception and Barriers to Optimal Medical Practice Thomas V. Caprio, MD, Jurgis Karuza, PhD, and Paul R. Katz, MD Objectives: To describe
National Survey on Consumers Experiences With Patient Safety and Quality Information
 Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
Summary and Chartpack The Kaiser Family Foundation/Agency for Healthcare Research and Quality/Harvard School of Public Health National Survey on Consumers Experiences With Patient Safety and Quality Information
The influx of newly insured Californians through
 January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
January 2016 Managing Cost of Care: Lessons from Successful Organizations Issue Brief The influx of newly insured Californians through the public exchange and Medicaid expansion has renewed efforts by
9/23/2015. Jackie F. Webb, DNP, FNP-BC Assistant Professor Linfield College
 Jackie F. Webb, DNP, FNP-BC Assistant Professor Linfield College Participants will understand differences between traditional care vs. group care Participants will describe effective components of group
Jackie F. Webb, DNP, FNP-BC Assistant Professor Linfield College Participants will understand differences between traditional care vs. group care Participants will describe effective components of group
Community Health Network of San Francisco Committee on Interdisciplinary Practice
 Community Health Network of San Francisco Committee on Interdisciplinary Practice Title: Pain Consultation Service - Clinical Pharmacist I. Policy Statement A. It is the policy of the Community Health
Community Health Network of San Francisco Committee on Interdisciplinary Practice Title: Pain Consultation Service - Clinical Pharmacist I. Policy Statement A. It is the policy of the Community Health
A Framework for the Evaluation of Medication Errors in the Inpatient Setting
 University of Connecticut DigitalCommons@UConn Master's Theses University of Connecticut Graduate School 5-5-2015 A Framework for the Evaluation of Medication Errors in the Inpatient Setting Alaina J.
University of Connecticut DigitalCommons@UConn Master's Theses University of Connecticut Graduate School 5-5-2015 A Framework for the Evaluation of Medication Errors in the Inpatient Setting Alaina J.
Reducing Avoidable Readmissions Within 30 Days of Discharge
 Reducing Avoidable Readmissions Within 30 Days of Discharge What We Know About Hospital Readmissions Approximately 20% of Medicare hospital discharges are followed by readmission within 30 days. 90% of
Reducing Avoidable Readmissions Within 30 Days of Discharge What We Know About Hospital Readmissions Approximately 20% of Medicare hospital discharges are followed by readmission within 30 days. 90% of
The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults
 The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults Anna Podolsky, AB David T. Stern, MD, PhD Lauren Peccoralo, MD, MPH Abstract Background Communication and courtesy are important
The Courteous Consult: A CONSULT Card and Training to Improve Resident Consults Anna Podolsky, AB David T. Stern, MD, PhD Lauren Peccoralo, MD, MPH Abstract Background Communication and courtesy are important
Evidence-Based Quality Improvement: A recipe for improving medication safety and handover of care Smeulers, Marian
 UvA-DARE (Digital Academic Repository) Evidence-Based Quality Improvement: A recipe for improving medication safety and handover of care Smeulers, Marian Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Evidence-Based Quality Improvement: A recipe for improving medication safety and handover of care Smeulers, Marian Link to publication Citation for published version
Differences of Job stress, Burnout, and Mindfulness according to General Characteristics of Clinical Nurses
 , pp.191-195 http://dx.doi.org/10.14257/astl.2015.88.40 Differences of Job stress, Burnout, and Mindfulness according to General Characteristics of Clinical Nurses Jung Im Choi 1, Myung Suk Koh 2 1 Sahmyook
, pp.191-195 http://dx.doi.org/10.14257/astl.2015.88.40 Differences of Job stress, Burnout, and Mindfulness according to General Characteristics of Clinical Nurses Jung Im Choi 1, Myung Suk Koh 2 1 Sahmyook
Breaking Down Silos of Care: Integration of Social Support Services with Health Care Delivery
 Breaking Down Silos of Care: Integration of Social Support Services with Health Care Delivery Betty Shephard Lead VP, Care Management HealthCare Partners National Health Policy Forum October 19, 2012 HCP
Breaking Down Silos of Care: Integration of Social Support Services with Health Care Delivery Betty Shephard Lead VP, Care Management HealthCare Partners National Health Policy Forum October 19, 2012 HCP
BACKGROUND: Ineffective communication of hospital discharge instructions may
 ORIGINAL RESEARCH Hospital Discharge Information and Older Patients: Do They Get What They Need? Jonathan Flacker, MD 1,3 Wansoo Park, PhD 2 Addie Sims, MSW 3 1 Division of Geriatric Medicine and Gerontology,
ORIGINAL RESEARCH Hospital Discharge Information and Older Patients: Do They Get What They Need? Jonathan Flacker, MD 1,3 Wansoo Park, PhD 2 Addie Sims, MSW 3 1 Division of Geriatric Medicine and Gerontology,
Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting
 Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting Natalie McMurtry, BSc Pharm, Sr. Medication Consultant; Vanessa Moorgen,
Medication Reconciliation Project Edmonton Zone Steps To MedRec Success Across Multiple Programs and Sites in a Large Urban Setting Natalie McMurtry, BSc Pharm, Sr. Medication Consultant; Vanessa Moorgen,
Educating Physicians-in-Training About Resource Utilization and Their Own Outcomes of Care in the Inpatient Setting
 Educating Physicians-in-Training About Resource Utilization and Their Own Outcomes of Care in the Inpatient Setting C. Jessica Dine, MD, MSHPR Jean Miller, MD Alexander Fuld, MD Lisa M. Bellini, MD Theodore
Educating Physicians-in-Training About Resource Utilization and Their Own Outcomes of Care in the Inpatient Setting C. Jessica Dine, MD, MSHPR Jean Miller, MD Alexander Fuld, MD Lisa M. Bellini, MD Theodore
There are more than 3 million hospital readmissions per
 Cost-Effectiveness of Pharmacist Postdischarge Follow-Up to Prevent Medication-Related Admissions BRENNAN SPIEGEL, MD, MSHS; RITA SHANE, PHARMD; KATHERINE PALMER, PHARMD; AND DUONG DONNA LUONG, PHARMD
Cost-Effectiveness of Pharmacist Postdischarge Follow-Up to Prevent Medication-Related Admissions BRENNAN SPIEGEL, MD, MSHS; RITA SHANE, PHARMD; KATHERINE PALMER, PHARMD; AND DUONG DONNA LUONG, PHARMD
As the U.S. population of older adults continues
 Facilitating Interdisciplinary Practice Through Mobile Service Provision to the Rural Older Adult Karen S. Hayward, PhD, RN, SANE-A Reaching the older adult in the rural communities in which they reside
Facilitating Interdisciplinary Practice Through Mobile Service Provision to the Rural Older Adult Karen S. Hayward, PhD, RN, SANE-A Reaching the older adult in the rural communities in which they reside
It is well established that group
 Evaluation of Prenatal and Pediatric Group Visits in a Residency Training Program Cristen Page, MD, MPH; Alfred Reid, MA; Laura Andrews, Julea Steiner, MPH BACKGROUND: It is well established that group
Evaluation of Prenatal and Pediatric Group Visits in a Residency Training Program Cristen Page, MD, MPH; Alfred Reid, MA; Laura Andrews, Julea Steiner, MPH BACKGROUND: It is well established that group
Care Transitions in Behavioral Health
 Janssen Pharmaceuticals, Inc. Presents: Care Transitions in Behavioral Health Chuck Ingoglia, MSW Senior Vice President, Policy and Practice Improvement, National Council for Behavioral Health Nina Marshall,
Janssen Pharmaceuticals, Inc. Presents: Care Transitions in Behavioral Health Chuck Ingoglia, MSW Senior Vice President, Policy and Practice Improvement, National Council for Behavioral Health Nina Marshall,
A Structured Workshop to Improve the Quality of Resident Discharge Summaries
 A Structured Workshop to Improve the Quality of Resident Discharge Summaries Jaideep S. Talwalkar, MD Jason R. Ouellette, MD Shawnette Alston, MD Gregory K. Buller, MD Daniel Cottrell, MD Thomas Genese,
A Structured Workshop to Improve the Quality of Resident Discharge Summaries Jaideep S. Talwalkar, MD Jason R. Ouellette, MD Shawnette Alston, MD Gregory K. Buller, MD Daniel Cottrell, MD Thomas Genese,
The number of patients admitted to acute care hospitals
 Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
Accepted Manuscript. Hospitalists, Medical Education, and US Health Care Costs,
 Accepted Manuscript Hospitalists, Medical Education, and US Health Care Costs, James E. Dalen MD, MPH, ScD (hon), Kenneth J Ryan MD, Anna L Waterbrook MD, Joseph S Alpert MD PII: S0002-9343(18)30503-5
Accepted Manuscript Hospitalists, Medical Education, and US Health Care Costs, James E. Dalen MD, MPH, ScD (hon), Kenneth J Ryan MD, Anna L Waterbrook MD, Joseph S Alpert MD PII: S0002-9343(18)30503-5
Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities
 Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities Richard J. Chung, MD Joan Jasien, MD Gary R. Maslow, MD, MPH ABSTRACT
Resident Dyads Providing Transition Care to Adolescents and Young Adults With Chronic Illnesses and Neurodevelopmental Disabilities Richard J. Chung, MD Joan Jasien, MD Gary R. Maslow, MD, MPH ABSTRACT
Evolving Roles of Pharmacists: Integrating Medication Management Services
 Evolving Roles of Pharmacists: Integrating Management Services Marie Smith, PharmD, FNAP Palmer Professor and Assistant Dean, Practice and Policy Partnerships UCONN School of Pharmacy (marie.smith@uconn.edu)
Evolving Roles of Pharmacists: Integrating Management Services Marie Smith, PharmD, FNAP Palmer Professor and Assistant Dean, Practice and Policy Partnerships UCONN School of Pharmacy (marie.smith@uconn.edu)
Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination
 Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Quality ID #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
THE BEST OF TIMES: PHARMACY IN AN ERA OF
 OBJECTIVES THE BEST OF TIMES: PHARMACY IN AN ERA OF ACCOUNTABLE CARE Toni Fera, BS, PharmD October 17, 2014 1. Describe the role of pharmacists in accountable care organizations (ACO). 2. List four key
OBJECTIVES THE BEST OF TIMES: PHARMACY IN AN ERA OF ACCOUNTABLE CARE Toni Fera, BS, PharmD October 17, 2014 1. Describe the role of pharmacists in accountable care organizations (ACO). 2. List four key
Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination
 Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
Using a Resident Discharge Clinic for Resident Education and Patient Care: A Feasibility Study
 Using a Resident Discharge Clinic for Resident Education and Patient Care: A Feasibility Study Katrina A. Booth, MD Lisa M. Vinci, MD Julie L. Oyler, MD Amber T. Pincavage, MD Abstract Background Many
Using a Resident Discharge Clinic for Resident Education and Patient Care: A Feasibility Study Katrina A. Booth, MD Lisa M. Vinci, MD Julie L. Oyler, MD Amber T. Pincavage, MD Abstract Background Many
Introduction. 1 Health Professions Regulatory Advisory Council. (2015) Registered Nurse Prescribing Referral, A Preliminary Literature
 RN Prescribing Home Care Ontario & Ontario Community Support Association Submission to the Health Professions Regulatory Advisory Committee February 2016 Introduction The Ontario government has confirmed
RN Prescribing Home Care Ontario & Ontario Community Support Association Submission to the Health Professions Regulatory Advisory Committee February 2016 Introduction The Ontario government has confirmed
Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service
 Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Hospital Pharmacy Volume 36, Number 11, pp 1164 1169 2001 Facts and Comparisons PEER-REVIEWED ARTICLE Performance Measurement of a Pharmacist-Directed Anticoagulation Management Service Jon C. Schommer,
Improving Sign-Outs in Hospital Medicine
 Improving Sign-Outs in Hospital Medicine Arpana R. Vidyarthi, MD Assistant Professor of Medicine Division of Hospital Medicine Director of Quality, Division of Hospital Medicine Director, Patient Safety
Improving Sign-Outs in Hospital Medicine Arpana R. Vidyarthi, MD Assistant Professor of Medicine Division of Hospital Medicine Director of Quality, Division of Hospital Medicine Director, Patient Safety
Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination
 Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Measure #46 (NQF 0097): Medication Reconciliation Post-Discharge National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Transitions of Care: An opportunity to improve care, experience and reduce waste
 Transitions of Care: An opportunity to improve care, experience and reduce waste Dr. Paresh Dawda, Visiting Fellow, Australian Primary Health Care Research Institute, ANU Adjunct Associate Professor, University
Transitions of Care: An opportunity to improve care, experience and reduce waste Dr. Paresh Dawda, Visiting Fellow, Australian Primary Health Care Research Institute, ANU Adjunct Associate Professor, University
Addressing Cost Barriers to Medications: A Survey of Patients Requesting Financial Assistance
 http://www.ajmc.com/journals/issue/2014/2014 vol20 n12/addressing cost barriers to medications asurvey of patients requesting financial assistance Addressing Cost Barriers to Medications: A Survey of Patients
http://www.ajmc.com/journals/issue/2014/2014 vol20 n12/addressing cost barriers to medications asurvey of patients requesting financial assistance Addressing Cost Barriers to Medications: A Survey of Patients
Pediatric Hospitalists: Training, Current Practice, and Career Goals. OBJECTIVE: To determine the range and frequency of experiences, clinical and
 ORIGINAL RESEARCH Pediatric Hospitalists: Training, Current Practice, and Career Goals Gary L. Freed, MD, MPH 1,2 Kelly M. Dunham, MPP 1,2 Research Advisory Committee of the American Board of Pediatrics
ORIGINAL RESEARCH Pediatric Hospitalists: Training, Current Practice, and Career Goals Gary L. Freed, MD, MPH 1,2 Kelly M. Dunham, MPP 1,2 Research Advisory Committee of the American Board of Pediatrics
UNIVERSITY OF CALIFORNIA
 UNIVERSITY OF CALIFORNIA Report on Nursing Programs Enrollment Levels, FY 2008-09 2008-09 Legislative Session Budget and Capital Resources Budget and Capital Resources UNIVERSITY OF CALIFORNIA Report
UNIVERSITY OF CALIFORNIA Report on Nursing Programs Enrollment Levels, FY 2008-09 2008-09 Legislative Session Budget and Capital Resources Budget and Capital Resources UNIVERSITY OF CALIFORNIA Report
PERFORMANCE MEASURE DATE / RESULTS / ANALYSIS FOLLOW-UP / ACTION PLAN
 Resident-to-Resident Assaults AIM: To decrease incidents of Resident to Residents assaults by 5% in the Fiscal Year (FY) 2011-2012. MONITORING: Data is collected from all instances in which State of California
Resident-to-Resident Assaults AIM: To decrease incidents of Resident to Residents assaults by 5% in the Fiscal Year (FY) 2011-2012. MONITORING: Data is collected from all instances in which State of California
NURSING SPECIAL REPORT
 2017 Press Ganey Nursing Special Report The Influence of Nurse Manager Leadership on Patient and Nurse Outcomes and the Mediating Effects of the Nurse Work Environment Nurse managers exert substantial
2017 Press Ganey Nursing Special Report The Influence of Nurse Manager Leadership on Patient and Nurse Outcomes and the Mediating Effects of the Nurse Work Environment Nurse managers exert substantial
Evaluating the Impact of Pain Management (PM) Education on Physician Practice Patterns A Continuing Medical Education (CME) Outcomes Study
 J Canc Educ (2010) 25:224 228 DOI 10.1007/s13187-010-0040-y Evaluating the Impact of Pain Management (PM) Education on Physician Practice Patterns A Continuing Medical Education (CME) Outcomes Study L.
J Canc Educ (2010) 25:224 228 DOI 10.1007/s13187-010-0040-y Evaluating the Impact of Pain Management (PM) Education on Physician Practice Patterns A Continuing Medical Education (CME) Outcomes Study L.
Project Title: Improving Pain Management at Hospital Admission and Discharge: Implementing an Interdisciplinary Evidence-Based Approach
 Project Title: Improving Pain Management at Hospital Admission and Discharge: Implementing an Interdisciplinary Evidence-Based Approach Principal Investigators: Wendy Anderson, MD, MS University of California,
Project Title: Improving Pain Management at Hospital Admission and Discharge: Implementing an Interdisciplinary Evidence-Based Approach Principal Investigators: Wendy Anderson, MD, MS University of California,
Novel combined patient instruction and discharge summary tool improves timeliness of documentation and outpatient provider satisfaction
 701053SMO0010.1177/2050312117701053SAGE Open MedicineGilliam et al. research-article2017 Original Article SAGE Open Medicine Novel combined patient instruction and discharge summary tool improves timeliness
701053SMO0010.1177/2050312117701053SAGE Open MedicineGilliam et al. research-article2017 Original Article SAGE Open Medicine Novel combined patient instruction and discharge summary tool improves timeliness
How to Improve the Discharge Process. Michelle Mourad, MD Ryan Greysen, MD
 How to Improve the Discharge Process Michelle Mourad, MD Ryan Greysen, MD Who are we? Why are we here? I mean BOB is the reason we are all really here. Do you have a BOB where you are? Or perhaps you like
How to Improve the Discharge Process Michelle Mourad, MD Ryan Greysen, MD Who are we? Why are we here? I mean BOB is the reason we are all really here. Do you have a BOB where you are? Or perhaps you like
McGill University. Academic Pediatrics Fellowship Program. Program Description And Learning Objectives
 McGill University Academic Pediatrics Fellowship Program Program Description And Learning Objectives Updated May 2018 Introduction: The Pediatrics Residency Program of McGill University offers advanced
McGill University Academic Pediatrics Fellowship Program Program Description And Learning Objectives Updated May 2018 Introduction: The Pediatrics Residency Program of McGill University offers advanced
The BOOST California Collaborative
 The BOOST California Collaborative California HealthCare Foundation Hospital Association of Southern California LA Care Health Plan The John A. Hartford Foundation Objectives for the Day Review the rationale
The BOOST California Collaborative California HealthCare Foundation Hospital Association of Southern California LA Care Health Plan The John A. Hartford Foundation Objectives for the Day Review the rationale
New York State Department of Health Dementia Grants Program Grant Funded Project
 New York State Department of Health Dementia Grants Program 2003-2005 Grant Funded Project Improving Continuity of Care and Medication Management When Nursing Home Residents are Discharged to and Admitted
New York State Department of Health Dementia Grants Program 2003-2005 Grant Funded Project Improving Continuity of Care and Medication Management When Nursing Home Residents are Discharged to and Admitted
What is Transition of Care?
 Transitions of Care and Reducing Readmissions Jackie Vance, RN, CDONA, FACDONA Director of Clinical Affairs and Industry Relations, AMDA NTOCC is chaired and coordinated by CMSA in partnership with sanofi
Transitions of Care and Reducing Readmissions Jackie Vance, RN, CDONA, FACDONA Director of Clinical Affairs and Industry Relations, AMDA NTOCC is chaired and coordinated by CMSA in partnership with sanofi
Reduced Anxiety Improves Learning Ability of Nursing Students Through Utilization of Mentoring Triads
 Reduced Anxiety Improves Learning Ability of Nursing Students Through Utilization of Mentoring Triads Keywords: Anxiety, Nursing Students, Mentoring Tamara Locken Heather Norberg College of Nursing Brigham
Reduced Anxiety Improves Learning Ability of Nursing Students Through Utilization of Mentoring Triads Keywords: Anxiety, Nursing Students, Mentoring Tamara Locken Heather Norberg College of Nursing Brigham
Appendix D. Measuring Humanism. Created by: Anandi Law. April 16, 2009
 Appendix D Measuring Humanism Created by: Anandi Law April 16, 2009 Due to the broad, complex and ambiguous definitions of humanism in the medical field, research to find faculty perspectives in humanism
Appendix D Measuring Humanism Created by: Anandi Law April 16, 2009 Due to the broad, complex and ambiguous definitions of humanism in the medical field, research to find faculty perspectives in humanism
FOSTERING INTERPROFESSIONAL EDUCATION (IPE) IN A NON TEACHING COMMUNITY HOSPITAL
 FOSTERING INTERPROFESSIONAL EDUCATION (IPE) IN A NON TEACHING COMMUNITY HOSPITAL Rebecca Margevicius, PharmD, BCPS rmargevicius@swgeneral.com Laura Stasiak, PharmD, BCPS lstasiak@swgeneral.com Pharmacist
FOSTERING INTERPROFESSIONAL EDUCATION (IPE) IN A NON TEACHING COMMUNITY HOSPITAL Rebecca Margevicius, PharmD, BCPS rmargevicius@swgeneral.com Laura Stasiak, PharmD, BCPS lstasiak@swgeneral.com Pharmacist
Medication Assisted Treatment for Opioid Use Disorders Reporting Requirements
 This document is scheduled to be published in the Federal Register on 09/27/2016 and available online at https://federalregister.gov/d/2016-23277, and on FDsys.gov DEPARTMENT OF HEALTH AND HUMAN SERVICES
This document is scheduled to be published in the Federal Register on 09/27/2016 and available online at https://federalregister.gov/d/2016-23277, and on FDsys.gov DEPARTMENT OF HEALTH AND HUMAN SERVICES
Impact of a Pharmacist-managed, Studentsupported Inpatient Warfarin Education Program on HCAHPS Scores in a Community Teaching Hospital
 Impact of a Pharmacist-managed, Studentsupported Inpatient Warfarin Education Program on HCAHPS Scores in a Community Teaching Hospital Submitted by: Daniel T. Abazia, Pharm.D., BCPS, Clinical Pharmacist
Impact of a Pharmacist-managed, Studentsupported Inpatient Warfarin Education Program on HCAHPS Scores in a Community Teaching Hospital Submitted by: Daniel T. Abazia, Pharm.D., BCPS, Clinical Pharmacist
Electronic medical records have introduced. Patients Perceptions of Clinical Scribe Use in Outpatient Physician Practices
 Original Research Patients Perceptions of Clinical Scribe Use in Outpatient Physician Practices Alan Leahey, MD; Susan Bethel, MSN, RN, NE-BC; Julie Summey, EdD; and Smith Heavner, BSN, RN, PCCN From the
Original Research Patients Perceptions of Clinical Scribe Use in Outpatient Physician Practices Alan Leahey, MD; Susan Bethel, MSN, RN, NE-BC; Julie Summey, EdD; and Smith Heavner, BSN, RN, PCCN From the
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010)
 Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
