GASTROSCOPY. Travelling to London Bridge Hospital A GUIDE FOR PATIENTS. Please ensure you read this booklet as it contains important information
|
|
|
- Pearl Harris
- 6 years ago
- Views:
Transcription
1 Travelling to London Bridge Hospital Directions: London Bridge Hospital is situated on the south side of the River Thames. We are next to London Bridge mainline and underground stations with easy access to the City. Train: London Bridge Station is serviced by trains from Kent and Surrey and offers direct connections to Charing Cross, Cannon Street, Waterloo East and Blackfriars Stations. Trains also connect directly on the Thameslink line. Underground: London Bridge Station is on the Jubilee Line and Northern Line (Bank Branch). Please take the Tooley Street exit, located opposite the London Dungeons. By Car: There are no car parking facilities available at the hospital. There is limited parking nearby. Patients can be dropped off and collected by car or taxi outside the main door of the hospital, where 15 minutes parking is available. Taxi: The hospital reception can book taxis for patients and visitors through our local taxi company, alternatively black cabs are available at London Bridge Station. GASTROSCOPY A GUIDE FOR PATIENTS Buses: There are numerous buses that pass by the hospital on Tooley Street, from London Bridge, or from outside the main entrance of the London Bridge Station Tooley Street, London SE1 2PR Tel: Web: Please ensure you read this booklet as it contains important information
2 Welcome You have been advised to have a investigation on the upper gastrointestinal tract (Gastroscopy). This booklet gives information about the procedure. We will do everything we can to make your stay as comfortable as possible and prepare you for your visit. Please take the time to read this booklet, as it contains important information about: How to prepare yourself for your procedure. What to expect during your stay. Being discharged home. Advice for carers Your formal consent is required before carrying out this examination. This booklet explains how the examination is carried out and what the risks are. This will help you to make an informed decision in agreeing to the examination and having sedation. If there is anything you do not understand, or anything further you wish to discuss please call either your Consultant or the Endoscopy Department. The purpose of this information booklet is as a guide for your procedure. Your Consultant may have given you specific instructions to follow. Please then follow your Consultant s requests.
3 Before you come into hospital Please bring in with you: You will have already seen a doctor in an outpatient clinic and they have decided that you require this procedure as a day case. If you have been sent a Patient Self Assessment form, or admission/registration form, please complete it making sure all details are correct. If you do not think either document will reach us in time for your admission, please bring the form with you. Prior to admission, it is imperative that you advise your insurance company of your admission to gain pre-authorisation. If you are self-funding, full payment must be made prior to admission. If you have any questions about your insurance or payment methods, you can contact our Pre-Admissions Officer on If the intended operation or procedure is being carried out under general anaesthetic or sedation, you must make arrangements in advance for somebody to take you home and also stay with you overnight. Your procedure may not go ahead if you have not made suitable or safe discharge arrangements. If you have any queries about your admission date or time, please contact your Consultant, your Consultant s secretary or our Reservations Department. Telephone or /2180. Privacy and accommodation In the Day Surgery Unit, all rooms are shared. Each room will accommodate two to four patients. The bed spaces are separated by curtains and partitions to provide some privacy. Each room will only ever be single-sex. All tablets, medications, inhalers that you are currently taking in the original packaging or any prescriptions you have. Please do not bring in your dosette box. Any toiletries you require. Glasses/contact lenses, cases and solutions. Something to help you pass the time, such as books, magazines, puzzles etc. X-rays, scans and any other appropriate reports or letters. Insurance documents. HCA Hospital ID Card if you have been a patient of an HCA hospital before. Credit/debit card or other payment method. Valuables Please do not bring jewellery or large sums of money. If this is unavoidable, please ask a relative or friend to look after them. London Bridge Hospital cannot be held responsible for any loss or damage to property brought into the hospital. In the Day Surgery Unit, you will have a locker next to your bed space for your personal possessions. This will be locked and the nurse will look after the key for you whilst you are having your procedure. This space is limited; please only bring with you what you will need. What should I wear? Wear loose, comfortable clothes, cotton underwear and flat or low-heeled shoes. 2
4 What to expect during your stay Waiting time Although you will have been given a provisional time for your procedure, the order of the operating list is not confirmed until the day of admission by the Consultant. Any investigation time may also be subject to change. On the day of your procedure, you must allow time for the admission process, procedure and your recovery time. You should expect to spend up to three hours with us. If you feel that you want to discuss your proposed treatment in a more private place, ask the nurse assigned to you. Please do not hesitate to contact us if you have any questions you wish to discuss further with a nurse prior to your admission. Do I keep taking my normal medication? Your routine medication should be taken. If your appointment is in the morning your medication should be taken at 6am with a little water, however if your appointment is in the afternoon your medication should be taken by 8am. If you are presently taking tablets to reduce the acid in your stomach please discuss this with your Consultant. Your Consultant may wish for you to discontinue them. If you are having a follow up gastroscopy to check for healing of an ulcer found during the last two-three months, then please continue your acid reducing medications right up to the day before your repeat endoscopy. If you are diabetic and taking medication (either tablets or insulin), you will have to reduce/modify your tablets or insulin dose when you start avoiding solid food as below. You should test your blood or urine for glucose before you start your bowel preparation, and then at least every four hours until you leave home for your appointment. If the result is higher than 10mmol/L, continue with your medication. You may drink sugary drinks to maintain your blood sugar level up to two hours before your appointment time. If it is lower than 10mmol/L, delay your medication until you start eating again. You may need to take just your normal dosage of medication according to blood sugar level. If you take Warfarin, Aspirin, Clopidrogrel (Plavix), any anti-inflammatory tablet or Heparin, you may continue them. However, you should discuss this with your consultant. For example if you have a known colonic polyp which will need to be removed then you must discontinue the blood thinning medication. Please remember to tell the staff about the drug before your test. Dietary Advice You must not have anything to eat for six hours before and drink two hours before the procedure; it is essential that your stomach is empty, as you may be sedated. If your stomach is not empty there is a risk of aspiration (vomit inhaled into the lungs). This can be a very serious complication. Furthermore having your stomach empty allows a clear view during the procedure. Intravenous Sedation Please note that if you are given sedation a responsible adult must accompany you home and you must have someone to stay with you overnight. You may wake up fairly quickly or more slowly each person reacts differently. You will probably remain on the unit for about two hours, but the effects of the sedation will last for much longer, up to 24 hours. Your thinking processes and movements will be slower than usual. It is very likely that you will not remember anything about the examination afterwards.
5 What happens when I arrive You will be asked to arrive at London Bridge Hospital one hour before your scheduled procedure time to allow the administrative and nursing staff ample time to complete your admission and any pre-test tasks. You will see a member of staff from the accounts team. They will check your admission and account details with you. You will then be sent up to the appropriate ward area, where you will be greeted by a member of the nursing team. They will show you to your room or bed space. A nurse will complete the admission process with you. This will include confirming your identity, completing paperwork, asking you questions about yourself and your health, (this is made shorter if you complete the Self Assessment Booklet), taking your blood pressure, pulse and temperature. You will be given two hospital identity bracelets with your name and details on them. If you are allergic to anything such as some foods, types of medication or latex, please tell your nurse and a red allergy bracelet will be used. You will be asked to wear a hospital gown. You will see your Consultant prior to your procedure. Feel free to ask any questions at this time. You will then sign a consent form, unless you have already done so in your outpatients clinic. You will be given a copy of the consent form for your own records by your Consultant or nurse. The nurse will also ask you about your arrangements for getting home reminding you of the importance of having someone accompanying you if you have had sedation. What is a Gastroscopy? This test is a very accurate way of looking at the lining of your upper digestive tract: the oesophagus (gullet), stomach and duodenum (first part of the small bowel), to establish whether there is any disease present. The instrument used in this investigation is called a gastroscope. It is flexible and has a diameter less than that of a little finger. The end of the gastroscope contains a light which enables light to be directed onto the lining of your upper digestive tract and a camera which relays pictures back to the endoscopist onto a television screen. During the investigation, the doctor may need to take some tissue samples (biopsies) from the lining of your upper digestive tract for analysis: this is painless. The samples will be retained and sent for analysis. A photograph of the inside of your bowel may also be taken. It will be kept in your medical records and sent with your biopsy and can be shown to you later to help you understand the findings of your test. Why do I need a Gastroscopy? A Gastroscopy is usually carried out to investigate symptoms such as: swallowing difficulties, nausea, vomiting, reflux, bleeding, indigestion, abdominal pain or chest pain or as a follow-up inspection of a previous known disease/problem. The results will help your consultant to decide on the best treatment for your problem or whether to carry out any further examinations The nurse will check your personal details again before taking you to the endoscopy room. Why do you keep asking me the same questions? We have to confirm certain details are correct as part of our checking procedure. This is standard practice for any patient having a procedure as we have to ensure the correct procedure is carried out. We do know who you are and why you are in hospital, but we want to double check our information.
6 What are the risks? According to the British Society of Gastroenterology the main risks for Gastroscopy are: Perforation: a tear of the linings of the stomach or oesophagus which could entail you being admitted to hospital. Although perforation generally requires surgery to repair the hole, certain cases may be treated conservatively with antibiotics and intravenous fluids. Bleeding: this may occur at the site of a biopsy. This is usually very minor and stops of its own accord. Damage to teeth, crowns or bridgework: utmost care is taken to protect any teeth or dental work by use of a mouthguard. This occurs very rarely. Reaction to sedation: problems with breathing, heart rate and blood pressure happen occasionally. If any of these problems do occur, they are normally short lived. Careful monitoring by a fully trained endoscopy nurse ensures that any potential problems can be identified and treated rapidly. These risks do increase for elderly patients and those who have significant health problems. Allergic reactions to sedation are very rare. Aspiration pneumonia: Vomit inhaled into lungs. This occurs very rarely in patients. What happens during a Gastrosocopy?. You will be taken to an examination room for the procedure. Once sat on the trolley the nurse or doctor may spray your throat with a local anaesthetic. This makes your throat go numb quite quickly and you may start to feel as if you can t swallow. Don t panic, you can swallow just not feel it. The nurses will ask you to lie down in the correct position resting on your left side with your knees slightly bent. A nurse will stay with you throughout the test. To keep your mouth slightly open, a plastic mouthpiece will also be placed between your teeth. A sedative drug will be injected via the cannula into your arm. This is not a full anaesthetic but it will make you very relaxed and sleepy. You may also be given analgesia (pain relieving drugs) via the cannula to ensure any discomfort you might feel during the procedure is minimised. Alternatively, a throat spray can be used to make the back of your throat numb, but you will have an opportunity to discuss this with your Consultant when you attend. A fine soft tube will be placed into both nostrils to give you a little extra oxygen to breathe and a small device will be attached to you finger or thumb to monitor your pulse rate and oxygen levels during the test. Once you are sedated or had throat spray the test will be carried out as follows: 1. Firstly, the endoscope is gently passed through your mouth into your stomach. This will not cause you any pain nor will it interfere with your breathing. 2. The lining of the oesophagus (gullet), stomach and duodenum (small bowel) will then be examined closely. Air will be passed through to distend the stomach to give a clear view of the lining. This air is sucked out at the end of the test. 3. If the doctor finds any change in tissue, a tiny piece may be removed (biopsy) using instruments passed through the endoscope. Any samples of tissues removed are sent to the laboratory for specialist examination. When the procedure is complete, the tube is removed quickly and easily. You will then be returned to the ward for your recovery.
7 What happens after the procedure? After the test you will return to the Day Surgery Unit on your trolley to continue your recovery. The nursing staff will check your pulse, blood pressure and oxygen levels, and generally assess how you have recovered from the test. You may feel a little bloated and experience wind pains, due to the air passed into the stomach, please don t feel embarrassed if you need to belch, this will help relieve the discomfort quite quickly. If you are in pain, please inform your nurse as soon as possible. You will be given something to eat and drink about an hour after returning to the ward. Your Consultant will explain what was seen during the examination either before you leave or in your follow up appointment. If you haven t already got a follow up appointment this is when you will discuss this with your Consultant. Discharge Advice Side effects The effect of the sedative can last up to 24 hours. It can make you forgetful and drowsy even though you may feel fully alert. Once home, it is important to rest quietly for the remainder of the day. You may suffer from a sore throat which should last no longer than hours. Furthermore you should avoid the following activities for at least 24 hours after the procedure: going to work driving operating machinery drinking alcohol signing any legally binding documents carrying out any activities involving heights caring for young children (sole responsibility) Queries and concerns If you have problems you wish to discuss following your procedure, please telephone the ward where you were cared for. You will be given this number on discharge. If you require advice out of hours (between 9pm and 7am), please telephone and ask to speak to the site bleep holder (on 000 ). This connects you to the senior nurse in charge of the hospital who can assist you. If you feel you need to be seen by a doctor in an emergency, please contact your Consultant, GP or go to your nearest Accident and Emergency Department.
8 Fire At London Bridge Hospital we take the safety of our patients, visitors and staff very seriously. Our staff undergo regular training, we have the latest evacuation equipment, our buildings are constructed to the very highest standards and are subject to frequent and regular external inspection. Test and drills Alarms are tested every Tuesday starting at 10.00am, and drills are conducted annually. Your nursing staff will inform you when a drill is taking place; you will not be expected to participate. In the unlikely event of a fire, we would like you to observe the following procedure: On discovering fire raise the alarm by either informing a member of staff or by using a break glass alarm and shouting fire, fire. Then contain the fire by shutting the nearest fire rated door and evacuate the immediate area. On hearing a continuous alarm this indicates that the fire is in your area. Your visitors and non-essential personnel will be evacuated to an assembly area outside the hospital. You are to remain in place until a member of the nursing staff evacuates you to a place of safety. On hearing the intermittent alarm this indicates that the fire is in your building but not in your area. Again, your visitors and non-essential personnel will be evacuated to an assembly area outside the hospital. Remain in your room until a senior member of the nursing staff tells you what to do. PLEASE DO NOT ATTEMPT TO LEAVE THE BUILDING UNLESS DIRECTED TO DO SO BY A MEMBER OF STAFF. Visitors and Escorts There are no restrictions on visiting times, but please remember that other patients may wish to rest or sleep. However, in consideration for other patients, please restrict your visitors to a maximum of two at any one time. Children are welcome to visit, but must be supervised by an adult at all times. Calls from friends or relatives can be made to the private phone by your bed. Please ask your callers to call the ward you are staying in, and a nurse will put them through (see useful telephone numbers at the back of this booklet). Alternatively, they can call the main switchboard on and ask to be put through to the room. The person taking you home is welcome to phone the hospital to check what time you will be ready to go home. Telephone: Comments, suggestions and complaints We welcome your views on our services to help us meet patients needs. We hope that your hospital visit will be a pleasant one and our staff will do all they can to ensure that this is the case. If you have a comment, suggestion or complaint about any aspect of our service, please approach a member of staff in the department and they will attempt to resolve things as quickly as possible. You will be given a Patient Feedback booklet to complete and we encourage your participation. Useful telephone numbers Main Reception Patient Accounts /2395/2061/2946 Day Surgery Unit /2631 Middle East Department X-ray Outpatients
9 Diagram of Digestive Tract Oesophagus Stomach Transverse colon Ascending colon Caecum Duodenum Small Intestine Descending colon Sigmoid colon Rectum Anus
Having a Gastroscopy. A guide to the test. Information for patients
 Having a Gastroscopy A guide to the test Information for patients Your doctor has recommended that you have a gastrointestinal endoscopy, this is sometimes called a Gastroscopy or Endoscopy. This leaflet
Having a Gastroscopy A guide to the test Information for patients Your doctor has recommended that you have a gastrointestinal endoscopy, this is sometimes called a Gastroscopy or Endoscopy. This leaflet
Gastroscopy. Please bring this booklet with you to your appointment. Oesophago-gastro duodenoscopy (OGD)
 Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
If you have any questions about the risks of this procedure please ask the endoscopist doing the test or the person who has referred you.
 What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
Having a Push Enteroscopy
 Endoscopy Unit Having a Push Enteroscopy A guide to the test Outpatient information 2 Your doctor has recommended that you have a Push Enteroscopy. This leaflet will explain the procedure and what to expect
Endoscopy Unit Having a Push Enteroscopy A guide to the test Outpatient information 2 Your doctor has recommended that you have a Push Enteroscopy. This leaflet will explain the procedure and what to expect
Upper GI Endoscopy a guide for patients and carers
 Upper GI Endoscopy a guide for patients and carers Welcome to the Endoscopy Unit. This information leaflet is intended to provide you with information about an upper endoscopy. It is not expected to cover
Upper GI Endoscopy a guide for patients and carers Welcome to the Endoscopy Unit. This information leaflet is intended to provide you with information about an upper endoscopy. It is not expected to cover
Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis
 South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South Tyneside and Sunderland.
South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South Tyneside and Sunderland.
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Colonoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Having an endoscopic retrograde cholangio-pancreatograph (ERCP)
 Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Endoscopy Unit Having an EUS
 Endoscopy Unit Having an EUS Information for patients 2 Your doctor has recommended that you have an Endoscopic Ultrasound. This leaflet will explain the procedure and what to expect on the day of your
Endoscopy Unit Having an EUS Information for patients 2 Your doctor has recommended that you have an Endoscopic Ultrasound. This leaflet will explain the procedure and what to expect on the day of your
Endoscopic Ultrasound (EUS) or Endosonography
 Endoscopic Ultrasound (EUS) or Endosonography This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment
Endoscopic Ultrasound (EUS) or Endosonography This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment
Double Balloon Enteroscopy
 Endoscopy Unit Double Balloon Enteroscopy A guide to the test Outpatient information Your doctor has recommended that you have a Double Balloon Enteroscopy. This leaflet will explain the procedure and
Endoscopy Unit Double Balloon Enteroscopy A guide to the test Outpatient information Your doctor has recommended that you have a Double Balloon Enteroscopy. This leaflet will explain the procedure and
HAVING A GASTROSCOPY. ENDOSCOPY DEPARTMENT Patient Information
 ENDOSCOPY DEPARTMENT Patient Information HAVING A GASTROSCOPY Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large print,
ENDOSCOPY DEPARTMENT Patient Information HAVING A GASTROSCOPY Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large print,
Gastroscopy - Inpatients
 PATIENT INFORMATION Gastroscopy - Inpatients Welcome to the Endoscopy Unit You have been referred by your doctor to have a Gastroscopy. This booklet has been written to explain the procedure. This will
PATIENT INFORMATION Gastroscopy - Inpatients Welcome to the Endoscopy Unit You have been referred by your doctor to have a Gastroscopy. This booklet has been written to explain the procedure. This will
Gastroscopy and Dilatation
 i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation
 Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation This leaflet provides information about the Endoscopy and Dilation procedure. It aims to answer any questions you may have
Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation This leaflet provides information about the Endoscopy and Dilation procedure. It aims to answer any questions you may have
PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL)
 PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Gastroscopy? A gastroscopy (or simple endoscopy) is a test which allows the Endoscopist to look
PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Gastroscopy? A gastroscopy (or simple endoscopy) is a test which allows the Endoscopist to look
Having a gastroscopy
 Other formats Having a gastroscopy Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on If you need this information in another format such as audio tape or
Other formats Having a gastroscopy Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on If you need this information in another format such as audio tape or
Diagnostic Upper Gastrointestinal Endoscopy
 Diagnostic Upper Gastrointestinal Endoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a gastroscopy, including the benefits, risks and any alternatives and
Diagnostic Upper Gastrointestinal Endoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a gastroscopy, including the benefits, risks and any alternatives and
Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients
 Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients i Introduction We hope that this booklet will help you to understand more about the procedure and the care that you
Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients i Introduction We hope that this booklet will help you to understand more about the procedure and the care that you
FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE
 DAY SURGERY UNIT FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a flexible sigmoidoscopy?
DAY SURGERY UNIT FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a flexible sigmoidoscopy?
Upper gastro-intestinal (GI) endoscopy
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. You have been advised by your doctor
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. You have been advised by your doctor
Patient Information Leaflet. Gastroscopy. Prepared by Endoscopy Department
 Patient Information Leaflet Gastroscopy Prepared by Endoscopy Department February 2013 Review due February 2016 1 If you require this leaflet in another language, large print or another format, please
Patient Information Leaflet Gastroscopy Prepared by Endoscopy Department February 2013 Review due February 2016 1 If you require this leaflet in another language, large print or another format, please
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Sigmoidoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Sigmoidoscopy Gastroenterology Unit patient information booklet What is sigmoidoscopy? Sigmoidoscopy is a camera procedure used to examine
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Sigmoidoscopy Gastroenterology Unit patient information booklet What is sigmoidoscopy? Sigmoidoscopy is a camera procedure used to examine
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion
 Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Gastroscopy and Flexible Sigmoidoscopy
 Gastroscopy and Flexible Sigmoidoscopy Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment An appointment
Gastroscopy and Flexible Sigmoidoscopy Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment An appointment
Having a Gastroscopy Information for Patients
 Endoscopy Team Information for Patients Having a Gastroscopy Information for Patients What is a Gastroscopy? You have been advised to have a gastroscopy to help find the cause of your symptoms. A gastroscopy
Endoscopy Team Information for Patients Having a Gastroscopy Information for Patients What is a Gastroscopy? You have been advised to have a gastroscopy to help find the cause of your symptoms. A gastroscopy
Colonoscopy. Patient Information. Introduction
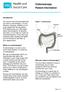 Colonoscopy Patient Information Introduction Your doctor has recommended that you have a colonoscopy. It is your decision, however, whether or not to go ahead with the procedure. This leaflet gives you
Colonoscopy Patient Information Introduction Your doctor has recommended that you have a colonoscopy. It is your decision, however, whether or not to go ahead with the procedure. This leaflet gives you
Having an Oesophageal Dilatation
 Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Northumbria Healthcare NHS Foundation Trust. Your guide to having a combined Gastroscopy and Colonoscopy. Issued by the Endoscopy Team
 Northumbria Healthcare NHS Foundation Trust Your guide to having a combined Gastroscopy and Colonoscopy Issued by the Endoscopy Team You have been referred for a combined gastroscopy and colonoscopy. This
Northumbria Healthcare NHS Foundation Trust Your guide to having a combined Gastroscopy and Colonoscopy Issued by the Endoscopy Team You have been referred for a combined gastroscopy and colonoscopy. This
Antegrade Double Balloon Enteroscopy Endoscopy Unit
 Manchester Royal Infirmary Antegrade Double Balloon Enteroscopy Endoscopy Unit Information For Patients 2 You have been advised to have an antegrade double balloon enteroscopy. This booklet has been prepared
Manchester Royal Infirmary Antegrade Double Balloon Enteroscopy Endoscopy Unit Information For Patients 2 You have been advised to have an antegrade double balloon enteroscopy. This booklet has been prepared
Endoscopy Unit. Having a Colonoscopy. A guide to the test. Outpatient information
 Endoscopy Unit Having a Colonoscopy A guide to the test Outpatient information Your doctor has recommended that you have a colonoscopy. This leaflet will explain the procedure and what to expect on the
Endoscopy Unit Having a Colonoscopy A guide to the test Outpatient information Your doctor has recommended that you have a colonoscopy. This leaflet will explain the procedure and what to expect on the
Endoscopy Unit Having an Oesophageal Stent insertion
 Endoscopy Unit Having an Oesophageal Stent insertion Information for patients Your doctor has recommended that you have an Oesophageal Stent Insertion. This leaflet will explain the procedure and what
Endoscopy Unit Having an Oesophageal Stent insertion Information for patients Your doctor has recommended that you have an Oesophageal Stent Insertion. This leaflet will explain the procedure and what
Having a lower gastrointestinal endoscopy (colonoscopy)
 Having a lower gastrointestinal endoscopy (colonoscopy) Patient name Appointment date Arrival time Endoscopy sessions run from 9am to 1pm and 1.30pm to 5pm. Every effort will be made to see you promptly
Having a lower gastrointestinal endoscopy (colonoscopy) Patient name Appointment date Arrival time Endoscopy sessions run from 9am to 1pm and 1.30pm to 5pm. Every effort will be made to see you promptly
Percutaneous Endoscopic Gastrostomy (PEG)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Having a Gastroscopy Information for Patients
 909170-WZZ 1044.qxp 27/01/2017 15:56 Page 1 Amersham Stoke Mandeville Wycombe Title of leaflet: Having a Gastroscopy information for Patients Compiled by: Sisters Sue Kenny & Deborah Coles Endoscopy Services,
909170-WZZ 1044.qxp 27/01/2017 15:56 Page 1 Amersham Stoke Mandeville Wycombe Title of leaflet: Having a Gastroscopy information for Patients Compiled by: Sisters Sue Kenny & Deborah Coles Endoscopy Services,
Endoscopy Suite Patient Information
 Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
Transnasal Endoscopy (TNE)
 Transnasal Endoscopy (TNE) Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other
Transnasal Endoscopy (TNE) Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other
Flexible Sigmoidoscopy Inpatients
 PATIENT INFORMATION Flexible Sigmoidoscopy Inpatients Your doctor has requested this procedure to help investigate your medical condition to aid your diagnosis and management. This booklet has been written
PATIENT INFORMATION Flexible Sigmoidoscopy Inpatients Your doctor has requested this procedure to help investigate your medical condition to aid your diagnosis and management. This booklet has been written
Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure
 Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for parents This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about a colonoscopy
Information for parents This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about a colonoscopy
Gastroscopy and Colonoscopy
 Patient Information Gastroscopy and Colonoscopy Endoscopy Department Shrewsbury and Telford Hospital NHS Trust What is a Gastroscopy and Colonoscopy? Gastroscopy and Colonoscopy is a combined procedure
Patient Information Gastroscopy and Colonoscopy Endoscopy Department Shrewsbury and Telford Hospital NHS Trust What is a Gastroscopy and Colonoscopy? Gastroscopy and Colonoscopy is a combined procedure
Having a Colonoscopy Information for Patients
 Endoscopy Team Information for Patients Having a Colonoscopy Information for Patients What is a Colonoscopy? A colonoscopy is a technique to look directly at the lining of the large bowel (colon) to try
Endoscopy Team Information for Patients Having a Colonoscopy Information for Patients What is a Colonoscopy? A colonoscopy is a technique to look directly at the lining of the large bowel (colon) to try
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment 1 2 Your appointment
Flexible Sigmoidoscopy This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment 1 2 Your appointment
Flexible sigmoidoscopy and rectal bleeding clinic
 Flexible sigmoidoscopy and rectal bleeding clinic This leaflet will explain what will happen when you come to attend the One-stop Rectal Bleed Clinic. If you have any questions or concerns, please speak
Flexible sigmoidoscopy and rectal bleeding clinic This leaflet will explain what will happen when you come to attend the One-stop Rectal Bleed Clinic. If you have any questions or concerns, please speak
Having a flexible sigmoidoscopy
 Having a flexible sigmoidoscopy +/- banding of haemorrhoids Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on Other formats If you need this information
Having a flexible sigmoidoscopy +/- banding of haemorrhoids Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on Other formats If you need this information
COLONOSCOPY. Travelling to London Bridge Hospital A GUIDE FOR PATIENTS. Please ensure you read this booklet as it contains important information
 Travelling to London Bridge Hospital Directions: London Bridge Hospital is situated on the south side of the River Thames. We are next to London Bridge mainline and underground stations with easy access
Travelling to London Bridge Hospital Directions: London Bridge Hospital is situated on the south side of the River Thames. We are next to London Bridge mainline and underground stations with easy access
FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL)
 PATIENT PROCEDURE INFORMATION LEAFLET FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Flexible Sigmoidoscopy? A flexible sigmoidoscopy is a test which allows the Endoscopist to look directly at the
PATIENT PROCEDURE INFORMATION LEAFLET FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Flexible Sigmoidoscopy? A flexible sigmoidoscopy is a test which allows the Endoscopist to look directly at the
PATIENT INFORMATION FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED
 PATIENT INFORMATION ON FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED Page 1 of 8 Page 2 of 8 Your consultant has recommended that you have a flexible sigmoidoscopy to view the left side of your large
PATIENT INFORMATION ON FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED Page 1 of 8 Page 2 of 8 Your consultant has recommended that you have a flexible sigmoidoscopy to view the left side of your large
Endoscopy Department Patient Information Leaflet
 Having a Colonoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Having a Colonoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Having a flexible sigmoidoscopy A guide for patients and their carers
 Having a flexible sigmoidoscopy A guide for patients and their carers Your information checklist: flexible sigmoidoscopy It is very important that you read this booklet. If you need further information
Having a flexible sigmoidoscopy A guide for patients and their carers Your information checklist: flexible sigmoidoscopy It is very important that you read this booklet. If you need further information
Endoscopy Department Patient Information Leaflet
 Having a flexible sigmoidoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Having a flexible sigmoidoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Flexible Sigmoidoscopy with an Enema
 Flexible Sigmoidoscopy with an Enema You must read this booklet at least seven days before your test Contents Page What is a flexible sigmoidoscopy? 1 Preparing yourself for a flexible sigmoidoscopy 2
Flexible Sigmoidoscopy with an Enema You must read this booklet at least seven days before your test Contents Page What is a flexible sigmoidoscopy? 1 Preparing yourself for a flexible sigmoidoscopy 2
Gastroscopy and Varices
 Gastroscopy and Varices Patient information Leaflet October 2013 What is a Gastroscopy? The doctor is going to carry out a procedure called a gastroscopy to look at your gullet (food pipe) and stomach,
Gastroscopy and Varices Patient information Leaflet October 2013 What is a Gastroscopy? The doctor is going to carry out a procedure called a gastroscopy to look at your gullet (food pipe) and stomach,
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Gastroscopy. What is a Gastroscopy? Website: Tel:
 Gastroscopy (Oesophago-Gastro Duodenoscopy, or OGD) This booklet contains advice for patients and carers about having a Gastroscopy or OGD Endoscopy Department Website: www.rbch.nhs.uk Tel: 01202 704668
Gastroscopy (Oesophago-Gastro Duodenoscopy, or OGD) This booklet contains advice for patients and carers about having a Gastroscopy or OGD Endoscopy Department Website: www.rbch.nhs.uk Tel: 01202 704668
Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy
 Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy A guide to the test Information for patients Endoscopy Welcome to The Endoscopy Unit Sheffield Teaching Hospitals NHS Foundation Trust has
Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy A guide to the test Information for patients Endoscopy Welcome to The Endoscopy Unit Sheffield Teaching Hospitals NHS Foundation Trust has
ERCP CONSENT TO EXAMINATION AND TREATMENT
 ENDOSCOPY DEPARTMENT Patient Information ERCP CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information
ENDOSCOPY DEPARTMENT Patient Information ERCP CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information
Northumbria Healthcare NHS Foundation Trust. Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team
 Northumbria Healthcare NHS Foundation Trust Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team This leaflet is to inform you about having a gastroscopy. Purpose of the
Northumbria Healthcare NHS Foundation Trust Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team This leaflet is to inform you about having a gastroscopy. Purpose of the
Having an operation as a day patient (under a general or local anaesthetic)
 Having an operation as a day patient (under a general or local anaesthetic) Information for patients Telephone numbers of day centres Unit Name Channel Day Surgery Centre William Harvey Hospital Ashford
Having an operation as a day patient (under a general or local anaesthetic) Information for patients Telephone numbers of day centres Unit Name Channel Day Surgery Centre William Harvey Hospital Ashford
Flexible - Sigmoidoscopy Essential information for patients
 Flexible - Sigmoidoscopy Essential information for patients Flexible Sigmoidoscopy It is an examination, which allows the doctor to look directly at the lining of the lower part (rectum and sigmoid colon)
Flexible - Sigmoidoscopy Essential information for patients Flexible Sigmoidoscopy It is an examination, which allows the doctor to look directly at the lining of the lower part (rectum and sigmoid colon)
Colonoscopy. Endoscopy Department. Patient information leaflet
 Colonoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a colonoscopy, including the benefits, risks and any alternatives and what you can expect when you come
Colonoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a colonoscopy, including the benefits, risks and any alternatives and what you can expect when you come
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy The procedure explained Please read this information leaflet carefully and bring it with you to your next appointment. Version Number: 3 Created: September 2014 Author: K Bridwell
Flexible Sigmoidoscopy The procedure explained Please read this information leaflet carefully and bring it with you to your next appointment. Version Number: 3 Created: September 2014 Author: K Bridwell
Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test)
 South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
COLONOSCOPY With Moviprep CONSENT TO EXAMINATION AND TREATMENT
 ENDOSCOPY DEPARTMENT Patient Information COLONOSCOPY With Moviprep CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If
ENDOSCOPY DEPARTMENT Patient Information COLONOSCOPY With Moviprep CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If
OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL
 OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL Ospidéal Naomh Séamus, Sráid Shéamais, Baile Átha Cliath 8. St. James s Hospital, James s Street, Dublin 8. + 353 1 410 3000 xxx.stjames.ie Endoscopy Unit Route
OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL Ospidéal Naomh Séamus, Sráid Shéamais, Baile Átha Cliath 8. St. James s Hospital, James s Street, Dublin 8. + 353 1 410 3000 xxx.stjames.ie Endoscopy Unit Route
Direct access flexible sigmoidoscopy
 Direct access flexible sigmoidoscopy What to expect Information for patients Endoscopy Why has my GP referred me for a direct access flexible sigmoidoscopy? Your General Practitioner (GP) has referred
Direct access flexible sigmoidoscopy What to expect Information for patients Endoscopy Why has my GP referred me for a direct access flexible sigmoidoscopy? Your General Practitioner (GP) has referred
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Colonoscopy. Please bring this booklet to your appointment with you.
 i Colonoscopy This booklet contains details about your appointment, information about the examination and preparation. Please bring this booklet to your appointment with you. If you need this information
i Colonoscopy This booklet contains details about your appointment, information about the examination and preparation. Please bring this booklet to your appointment with you. If you need this information
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Colonoscopy Essential information for patients
 Colonoscopy Essential information for patients Colonoscopy A colonoscopy is a procedure that allows the endoscopist to look directly at the lining of the large bowel or (colon). It is performed using a
Colonoscopy Essential information for patients Colonoscopy A colonoscopy is a procedure that allows the endoscopist to look directly at the lining of the large bowel or (colon). It is performed using a
Colonoscopy A Guide to the Test
 Colonoscopy A Guide to the Test Name: Who to contact and how: Notes: Diana, Princess of Wales Scartho Road Grimsby DN33 2BA 03033 306999 www.nlg.nhs.uk Scunthorpe General Hospital Cliff Gardens Scunthorpe
Colonoscopy A Guide to the Test Name: Who to contact and how: Notes: Diana, Princess of Wales Scartho Road Grimsby DN33 2BA 03033 306999 www.nlg.nhs.uk Scunthorpe General Hospital Cliff Gardens Scunthorpe
Oesophago-Gastro Duodenoscopy (OGD) with PEG feeding tube insertion. Patient information. Endoscopy Unit,
 Oesophago-Gastro Duodenoscopy (OGD) with PEG feeding tube insertion Patient information Endoscopy Unit, The Royal Infirmary of Edinburgh Endoscopy Nurses: 0131 242 1600 Endoscopy Booking Line: 0131 536
Oesophago-Gastro Duodenoscopy (OGD) with PEG feeding tube insertion Patient information Endoscopy Unit, The Royal Infirmary of Edinburgh Endoscopy Nurses: 0131 242 1600 Endoscopy Booking Line: 0131 536
Endoscopy Unit Colonic Stent insertion
 Endoscopy Unit Colonic Stent insertion Information for patients Your doctor has recommended that you have a Colonic Stent Insertion. This leaflet will explain the procedure and what to expect on the day
Endoscopy Unit Colonic Stent insertion Information for patients Your doctor has recommended that you have a Colonic Stent Insertion. This leaflet will explain the procedure and what to expect on the day
Colonoscopy with Extended Bowel Preparation
 Colonoscopy with Extended Bowel Preparation Name: Who to contact and how: Notes: Diana, Princess of Wales Scartho Road Grimsby DN33 2BA 03033 306999 www.nlg.nhs.uk Scunthorpe General Hospital Cliff Gardens
Colonoscopy with Extended Bowel Preparation Name: Who to contact and how: Notes: Diana, Princess of Wales Scartho Road Grimsby DN33 2BA 03033 306999 www.nlg.nhs.uk Scunthorpe General Hospital Cliff Gardens
Your Anesthesiologist, Anesthesia and Pain Control
 You can reduce your pain level after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in
You can reduce your pain level after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in
A Patient s Guide to Surgery
 A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
ERCP (Endoscopic Retrograde Cholangiopancreatography)
 Patient & Family Guide 2018 ERCP (Endoscopic Retrograde Cholangiopancreatography) Aussi disponible en français : CPRE (Cholangiopancréatographie rétrograde endoscopique) (FF85-1503) Also available in Arabic:
Patient & Family Guide 2018 ERCP (Endoscopic Retrograde Cholangiopancreatography) Aussi disponible en français : CPRE (Cholangiopancréatographie rétrograde endoscopique) (FF85-1503) Also available in Arabic:
Hip fracture - DHS. Your broken hip joint - some information
 Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Anal fissure. (lateral sphincterotomy) Information for patients General Surgery
 Anal fissure (lateral sphincterotomy) Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre
Anal fissure (lateral sphincterotomy) Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre
PEG Tube (Percutaneous Endoscopic Gastrostomy)
 Patient & Family Guide 2017 PEG Tube (Percutaneous Endoscopic Gastrostomy) www.nshealth.ca PEG Tube What is a PEG tube? A PEG tube is a type of feeding tube. It is inserted (put in) by a GI specialist
Patient & Family Guide 2017 PEG Tube (Percutaneous Endoscopic Gastrostomy) www.nshealth.ca PEG Tube What is a PEG tube? A PEG tube is a type of feeding tube. It is inserted (put in) by a GI specialist
Fistula in ano. Information for patients General Surgery
 Fistula in ano Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre Admissions Unit
Fistula in ano Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre Admissions Unit
Functional Endoscopic Sinus Surgery (FESS)
 Patient information Functional Endoscopic Sinus Surgery (FESS) Ear, Nose and Throat Directorate PIF 232 V7 Your Consultant / Doctor has advised you to have Functional Endoscopic Sinus Surgery (FESS). What
Patient information Functional Endoscopic Sinus Surgery (FESS) Ear, Nose and Throat Directorate PIF 232 V7 Your Consultant / Doctor has advised you to have Functional Endoscopic Sinus Surgery (FESS). What
HOW TO CARE FOR YOUR DIALYSIS CATHETER
 RENAL PATIENT INFORMATION HOW TO CARE FOR YOUR DIALYSIS CATHETER Advice for patients with a dialysis tunnelled catheter How to care for your dialysis line What is a haemodialysis line? A dialysis line
RENAL PATIENT INFORMATION HOW TO CARE FOR YOUR DIALYSIS CATHETER Advice for patients with a dialysis tunnelled catheter How to care for your dialysis line What is a haemodialysis line? A dialysis line
UW MEDICINE PATIENT EDUCATION. Angiography: Percutaneous or Transjugular Liver Biopsy. How to prepare and what to expect. What is a liver biopsy?
 UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients
 Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients i The prostate The prostate is a small gland, which is found only men. It is found at the base of the
Having a Day Case TRUS Biopsy (General Anaesthetic) Department of Urology Information for patients i The prostate The prostate is a small gland, which is found only men. It is found at the base of the
Radical cystectomy enhanced recovery plan. Information for patients
 Radical cystectomy enhanced recovery plan Information for patients Your doctor has recommended surgery to remove your bladder (radical cystectomy). This booklet is designed to explain the operation and
Radical cystectomy enhanced recovery plan Information for patients Your doctor has recommended surgery to remove your bladder (radical cystectomy). This booklet is designed to explain the operation and
Stapling / Repair of Pharyngeal Pouch
 Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
Rectal prolapse. Information for patients General Surgery
 Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
ABOUT YOUR GASTROSCOPY
 ABOUT YOUR GASTROSCOPY Dear Patient: Your physician has referred you for an exam of your upper digestive tract, which is called a gastroscopy. Sometimes it is called an EGD or an upper endoscopy. The purpose
ABOUT YOUR GASTROSCOPY Dear Patient: Your physician has referred you for an exam of your upper digestive tract, which is called a gastroscopy. Sometimes it is called an EGD or an upper endoscopy. The purpose
Patient Information. Having a Laparoscopy
 Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Paediatric Directorate /1791
 Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Children s Ward Parent/Carer Information Leaflet
 Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
Cardiac catheterisation. Cardiology Department Patient Information Leaflet
 Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Patient Information Leaflet. Tennis Elbow. Produced By: Orthopaedic Department
 Patient Information Leaflet Tennis Elbow Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another format, please
Patient Information Leaflet Tennis Elbow Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another format, please
UW MEDICINE PATIENT EDUCATION. How to prepare and what to expect DRAFT. What is an IVC filter?
 UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
Your Anesthesiologist, Anesthesia and Pain Control
 You should avoid having pain after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in advance.
You should avoid having pain after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in advance.
Having a blue light cystoscopy
 Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for Patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about paracentesis
Information for Patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about paracentesis
Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case)
 Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case) Department of Urology Information for patients i What is a Trans Urethral Resection of Bladder Tumour (TURBT)? Your recent cystoscopy has shown
Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case) Department of Urology Information for patients i What is a Trans Urethral Resection of Bladder Tumour (TURBT)? Your recent cystoscopy has shown
