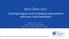
2016 Complex Case Management. Program Evaluation. Our mission is to improve the health and quality of life of our members
|
|
|
- Zoe Pierce
- 6 years ago
- Views:
Transcription
1 2016 Complex Case Management Program Evaluation Our mission is to improve the health and quality of life of our members
2 2016 Complex Case Management Program Evaluation Table of Contents Program Purpose Page 1 Goals Page 1 Objectives Page 1-2 Member Interactions Page 2 Evaluation Top 15 Primary Diagnoses in Complex Case Management Pages 2-3 Number of Referrals by Source Page 4 Complex Case Management Emergency, Admission and Readmission Utilization Pages 5 Member Discharge Status Page 6 Goals Met/ Not Met Page 7 Member Survey Results for Satisfaction with Complex Case Management Services Received Pages 8-9 Member Satisfaction Results for Improvement of Health or Quality of Life Pages Annual Review of Passport Health Plan s Total Population Pages Barriers/Opportunities Page 15 Activities Pages 16-18
3 2016 Complex Case Management Program Evaluation Program Title: Complex Case Management (CCM) Program Evaluation Evaluation Period: January 1, 2016 December 31, 2016 Program Purpose: To improve the health status and quality of life of members with multiple complex medical conditions while decreasing unnecessary hospitalizations and emergency room (ER) visits by: Improving member self-management skills Increasing adherence of members and clinicians with the evidence-based national clinical practice guidelines. To proactively provide coordination of care and services to members who have experienced a critical event or diagnosis needing the extensive use of resources and who need assistance navigating the health care system or those members with special health care needs. Program Goals: Emergency Department, Inpatient Admission, and 30-day Readmission Reduction of 20% or greater. Meet or exceed a rate of 90% of goals partially or completely met for members enrolled in CCM. To maintain a goal of 90% or above in member satisfaction with all areas of CCM services. To maintain a goal of 75% or above in member's perception of improved overall health status and quality of life at the time of discharge from CCM. Program Objectives: Provide for the collaborative process in assessing, planning, implementing, coordinating, monitoring and evaluating the options and services needed to meet the members health and human service needs. To increase the number of members who either improved or reached their optimal level of health at the time of discharge from CCM. Decrease unnecessary hospitalizations and ER visits. Improve member self-management skills and self-advocacy. Provide coordination of care and services to members who have experienced a critical event or diagnosis needing the extensive use of resources and who need assistance navigating the health care system or those members with special health care needs. 4/18/17 FINAL Page 1
4 To annually assess the characteristics of Passport Health Plan s (Passport) populations and evaluate available resources to meet the needs of these members. Member Interactions: CCM interacted with 912 members through Evaluation I. Members by Top 15 Primary Diagnoses in Complex Case Management Objective: To annually evaluate the primary diagnosis or Special Needs Category of members who trigger and enroll in CCM services to assure Passport has the appropriate staff, materials, and resources to assist members in improving their health and quality of life. 4/18/17 FINAL Page 2
5 Analysis of Findings: The graph above represents members by diagnosis enrolled into CCM. The top three diagnoses were: 1) Mood disorders 2) Other nervous system disorders 3) Other lower respiratory disease Individuals with Special Health Care Needs: Passport evaluated the population for members with Special Needs (Individuals with Special Health Care Needs or ISHCN). Members defined as having special needs are members who have or are at risk for chronic physical, developmental, behavioral, neurological, or emotional conditions and who may require a broad range of primary, specialized medical, behavioral health (BH), and/or related services. ISHCN may have an increased need for healthcare or related services due to their respective conditions; therefore Passport proactively identified, outreached, and enrolled these members into CM. In 2016, the Department of Health School Board Manager identified, assessed, planned, coordinated and implemented appropriate cost-effective health care services for individuals identified with special health care needs and medically fragile children. The manager works onsite at health departments and schools throughout the state in order to monitor the continuity and coordination of care and prevention of duplication for these children as part of the continuous quality improvement program. Medically Fragile Foster Children: Medically fragile foster care children are identified by Department of Community Based Services (DCBS) worker, DCBS service plan, and/or via a medically fragile foster care report provided monthly by the Department for Medicaid Services (DMS). All identified medically fragile foster care children are placed in CCM or Disease Management (DM). Some of them also receive case management or case consultation from the Passport BH Team. Complex Case Managers, Disease Managers, and BH Case Managers collaborate during regular integrated meetings and via ongoing contact with one another to ensure the needs of these vulnerable members are being met. Case Managers maintain regular communication with the Passport Foster Care/Adoption/Guardianship Liaison (FCL) and/or Manager of Out of Home Placements to consult as well. All Case Managers assigned to the member as well as the FCL participate in team conference calls led by the Children s Review Program (CRP) when the member s needs or presenting issues are impacting CRP s ability to locate appropriate placement for the child. 4/18/17 FINAL Page 3
6 II. Number of Referrals by Sources Objective: Identify members proactively for CM through multiple resource avenues. Analysis of Findings: The graph above represents referrals by source. The top three sources were: 1) Other 2) HRA (Health Risk Assessment) 3) Practitioner In the Other category, the 409 referrals reflect Embedded Case Management (ECM), Members Services, BH, Medical Director, Appeals and Quality. Multiple avenues are used to proactively identify members for CCM. Education and information is distributed via the Member and Provider Handbooks, Member Newsletter, New Member Packets, and Member and Provider Program brochures. Provider Referral Forms are available as well on the Passport website. Education is provided through internal department meetings and the use of internal referral forms to CCM and BH is encouraged. A daily report is obtained from the Health Information Line (24/7 Nurse Line) of identified members. Referrals are also obtained through the discharge planner at the hospitals. HRA s are utilized as a means of risk screening for the member. There was a slight decrease of 9% in returned HRA s in 2016 as compared to This allowed for prompt identification of members with conditions that qualified them for enrollment into DM and CCM services. We continue to attempt to obtain an HRA for all members with each initial contact. 4/18/17 FINAL Page 4
7 III. CCM Emergency, Admission and Readmission Utilization Goal: Emergency Department (ED), Inpatient Admission, and 30-day Readmission Reduction of 20% or greater. Analysis of Findings: This is a comparison of utilization specifically related to members in CCM. In analyzes rates of utilization prior to enrollment in CCM comparative to after. The goal of reducing ED, inpatient admission, and 30-day readmission rates by 20% or greater was met as evidenced by the data that demonstrates: A decrease of 38% in ER utilization after CCM involvement during 2016 compared to A 33% decrease in Inpatient Admission utilization after CCM involvement during 2016 compared to A decrease of 34% in Readmissions Rates after CCM involvement during 2016 compared to There was a 9% decrease in CCM membership during 2016 compared to /18/17 FINAL Page 5
8 IV. Member Discharge Status Analysis of Findings: The graph above represents reasons for member s discharge from CM during The top three reasons were: 1) Disenrolled 2) Lost contact with member 3) Other There were 157 (27%) members discharged due to Case Manager losing contact with the member; and 286 (44%) members were disenrolled. No discernable patterns were noted in this group. 4/18/17 FINAL Page 6
9 V. Goals Met / Not Met Goal: Meet or exceed a rate of 90% of goals partially or completely met for members enrolled in CM. Analysis of Findings: The graph above represents the status of goals for members enrolled in the CCM program. Result totals for 2016 for completed/partially completed was 744 goals, a 69% increase compared to There were a total of 49 goals that were not met, the same as in This represents a completion rate of 93.4% for 2016; an increase of 2.9% from The goal to meet or exceed the departmental goal of 90% was met. There are 53 ongoing goals for the members enrolled, compared to the 602 goals from 2015, a 91.2% decrease in members in progress goals. 4/18/17 FINAL Page 7
10 VI. Member Survey Results for Satisfaction with CCM Services Received Goal: Maintain or exceed the goal of 90% or above in member satisfaction with all areas of CM services. 4/18/17 FINAL Page 8
11 Analysis of Findings: The graphs above represents member satisfaction with CM. surveyed in the first graph include: 1) Frequency of contact 2) Professional manner 3) Coordination of care 4) Value of information 5) Overall effectiveness The areas The goal is 90% for each area. During 2016, 229 member surveys were distributed, of which 33 were returned yielding a 14% return rate. Results indicate 100% of members who responded to the survey reported satisfaction with frequency of contact, professional and courteous manner, ability of case manager to help coordinate their care, usefulness of information, and overall helpfulness. The goal was met in all areas. The areas surveyed in the second graph include: 1) Overall effectiveness 2) Professional manner 3) Coordination of care 4) Value of information The goal is 90% for each area. Results indicate 100% of members who responded to the survey reported satisfaction with overall effectiveness, professional and courteous manner, and ability of case manager to help coordinate their care. 92% of members who responded to the survey reported satisfaction with value of information. The goal was met in all areas. 4/18/17 FINAL Page 9
12 VII. Member Satisfaction Results for Improvement of Health or Quality of Life Goal: Maintain or exceed the goal of 75% or above in member's perception of improved overall health status and quality of life. 4/18/17 FINAL Page 10
13 Analysis of Findings: The graphs above represents the members satisfaction regarding improvement in health or quality of life. The areas surveyed in the first graph include: 1) Goals set by Case Manager and Member 2) Quality of Life 3) Overall Health 4) Control of Pain The goal is 75% for all areas. Results indicate 63% of members who responded to the survey reported improvement in quality of life, 40% reported improvement in overall health, and 40% reported better pain control. The goal was not met in all areas. However, the total number of returned surveys (33) is too small to make valid conclusions about the generalizability of the results. The areas surveyed in the second graph include: 1) Goals set by Case Manager and Member 2) Quality of Life 3) Overall Health The goal is 75% for all areas. Results indicate 85% of members who responded to the survey reported improvement in quality of life, and 77% reported improvement in overall health. The goal was met in all areas. During 2016, there were no complaints received regarding the CCM Program or the Complex Case Managers. 4/18/17 FINAL Page 11
14 VIII. Annual Review of Passport s Total Population 2015 Top 5 Primary Diagnosis Codes for All Members 2015 Top 5 Secondary Diagnosis Codes for Members Diagnosis Code Diagnosis Description ADD of Childhood with Hyperactivity Member Count Diagnosis Code 125,479 V5869 Diagnosis Description Encounter For Long-Term Use of Other Medications Member Count 60, Opioid Type Dependence Unspecified Abuse 90, Unspecified Essential Hypertension 51, Unspecified Episodic Mood Disorder Depression Disorder Not Elsewhere Classified 77, Anxiety State, Unspecified 38,070 64, Lumbago 36,478 V5869 Encounter For Long-Term Use of Other Medications 62, Nondependent Tobacco Use Disorder 33,876 4/18/17 FINAL Page 12
15 2016 Top 5 Primary Diagnosis Codes for All Members 2016 Top 5 Secondary Diagnosis Codes for Members Diagnosis Code Z00129 Diagnosis Description Encounter for routine child health examination without abnormal findings Member Count Diagnosis Code Diagnosis Description Member Count 52,026 I10 Essential (primary) hypertension 34,068 J069 Acute upper respiratory infection, unspecified 36,327 J069 Acute upper respiratory infection, unspecified 21,682 I10 Essential (primary) hypertension 34,068 R05 Cough 21,278 J029 Acute pharyngitis, unspecified 31,127 J029 Acute pharyngitis, unspecified 21,133 Z00121 Encounter for routine child health examination with abnormal findings 29,529 M545 Low back pain 21,098 4/18/17 FINAL Page 13
16 Objective: To annually assess the characteristics of Passport s populations and evaluate available resources to meet the needs of these members. Analysis of Findings: Population Analysis: At least annually, Passport assesses, analyzes, and evaluates the characteristics and needs of its member population in order to identify relevant subpopulations, revise and update its processes to meet member needs, and to assure Passport has all the needed resources to address member s needs. During 2016, Passport engaged in enrolling several subpopulations as a group into CCM services. Children were a majority of our plan enrolled population in years past; however, the adult population has increased over the past two years due to the expansion population. The adult population also tends to be the age group enrolled in CCM services. Also, as in years past, the female population is higher than the male population. Noted comorbidities of the CCM population each have specific DM programs with the exception of End Stage Renal Disease (ESRD). Members with an ESRD diagnosis tend to utilize CM services versus DM due to needing dialysis and a higher level of care coordination than typical DM programs. Therefore, Passport has made a conscious decision to keep those members in CCM. At this time, no barriers are identified thus no changes are needed at this time. Substance use as well has been noted with an increase in referrals as well. This most certainly can be contributed to House Bill I and the declination in prescribing opioids by clinicians. Member Engagement: Complex Case Managers fully engaged 129 members in This represents a 9% decrease from Complex Case Managers provide intensive proactive services and work with members with complex, multiple co-morbidities and psychosocial barriers. These case managers work to decrease readmissions and ER utilization and to increase outpatient services and compliance with treatment and care plans. 4/18/17 FINAL Page 14
17 Barriers and Opportunities Barrier: Inability to locate member for initial assessment or ongoing contact. Opportunity: Collaborate with clinicians to encourage member participation and locate additional demographics. Member education regarding the benefits of CCM through the Member Newsletter. Attempt to obtain working phone numbers through unable to contact, clinicians, pharmacies, and Tracfone. Flyer developed to encourage members to keep current addresses and phone numbers up-to-date with the State. Barrier: Member unwilling to comply with treatment plan and its completion. Opportunity: Member education regarding the benefits of CCM through the Member Newsletter. Member education regarding the benefits of CCM through individualized contact with the member. Collaborate with clinicians to encourage member participation. Barrier: Limited member response to the CCM survey. Opportunity: Encourage member response to survey at the time of discharge. Survey revised to reflect ease of answering questions and providing anonymous input. 4/18/17 FINAL Page 15
18 Activities for 2016: Provider Education: Encouraged clinician involvement with CCM. Member Education: Educated members/caregivers regarding CCM benefits and services through telephonic outreach, member newsletters, on-hold SoundCare messages, Passport s website, and member educational material. CCM identified and enrolled medically fragile foster care, and members identified as individuals with special health care needs. Updated Special Health Programs, Just for You! brochure for members on the different programs available for them to participate. Developed new Member Satisfaction Survey Postcard directing members to the Passport website to fill out their survey. There is a specific survey number based on the program the member was enrolled in. If the member would prefer to have a hard copy mailed to them, they can call into our Care Connector line and they will mail one to them to fill out and return. Screening Activities: CCM conducted depression screenings (PHQ-2) with 78 adult members with 16% of the members with a positive screening. Further depression screening (PHQ-9) was conducted with those members. CCM referred 12 members to BH services. Complex Case Managers conducted the Pediatric Symptom Checklist- 17 (PSC-17), a depression screening for children ages 4-17; 16 members were screened with 56% of the members with a positive screening. CCM referred nine (9) members to BH services. Identification Activities: Moved to new predictive modeling program to better identify high risk members appropriate for CCM Program. CCM interacted with 912 members through The CCM exhausted all measures to establish and maintain contact with members including calling clinician offices, utilizing the Medical Management System to locate current address and phone numbers, and mailing unable to contact letters with business cards attached. Reviewed the results of quarterly reporting to identify opportunities to improve the CCM process. 4/18/17 FINAL Page 16
19 Distributed the Member Satisfaction Survey to members enrolled in the CCM Program, reviewed surveys as received and conducted outreach to those members who indicate fair or poor responses on their survey (if the member completes contact information section of the survey tool) and monitored surveys for trends, none identified. Provided feedback to individual staff when appropriate and addressed any identified areas that needed improvement, none identified. Continued utilizing other reports such as ER Utilization, Kosair ER, and Hospital admission reports to identify members who could potentially benefit from CCM services. Collaborated with other departments such as UM, Member Services, and Provider Relations to identify members who could potentially benefit from CCM services. Continued to improve integration and collaboration with BH to improve overall coordination of care for members with co-existing medical and BH diagnoses/conditions. Activities for 2017: Continued Interventions: Encourage clinician involvement with CCM. Continue utilizing other reports such as ER Utilization, Kosair ER, and Hospital admission reports to identify members who could potentially benefit from CCM services. Identify and enroll medically fragile foster care, and members identified as individuals with special health care needs into CCM. Educate members/caregivers through: o Face-to-face outreach o Telephonic outreach o Member newsletters o On-hold SoundCare messages o Passport s website o Member educational materials Continue to monitor member care gaps and work with member and clinician to increase preventative health screenings. Evaluate alternate methods of communication with members for health messaging. Review the results of quarterly reporting to identify opportunities to improve the CCM process. 4/18/17 FINAL Page 17
20 Administer the PHQ-2, PHQ-9 (for adults) and PSC-17 (for children ages 4-17) to prescreen and screen for depression in members and referred members to the BH team as needed. Review surveys as received and conducted outreach to those members who indicate fair or poor responses on their survey (if the member completes contact information section of the survey tool). Monitor for trends, provide feedback both positive and negative to individual staff and address any identified areas that need improvement. Collaborate with other departments such as UM, Member Services, and Provider Relations to identify members who could potentially benefit from CCM services. Continue to improve collaboration with BH to improve overall coordination of care for members with co-existing medical and BH diagnoses. To include behavioral health/substance abuse facilities. Revise member and clinician correspondence (i.e., letters, materials, etc.) to improve member and clinician education regarding CCM services. Overall the CCM Program noted improvements in Once again, Passport noted an increase to the number of members participating in the CCM Program. Based upon the 2016 evaluation, Passport developed new and innovative initiatives to strive towards the overall goal of improving the health and quality of life for our members with complex conditions. 4/18/17 FINAL Page 18
2016 Embedded and Rapid Response Care Management
 2016 Embedded and Rapid Response Care Management Program Evaluation Our mission is to improve the health and quality of life of our members 2016 Embedded and Rapid Response Care Management Program Evaluation
2016 Embedded and Rapid Response Care Management Program Evaluation Our mission is to improve the health and quality of life of our members 2016 Embedded and Rapid Response Care Management Program Evaluation
2017 Catastrophic Care. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2017 Catastrophic Care Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Catastrophic Care Program Evaluation Table of Contents Program Purpose Page 1 Goals
2017 Catastrophic Care Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Catastrophic Care Program Evaluation Table of Contents Program Purpose Page 1 Goals
2016 Complex Case Management Program Description. Our mission is to improve the health and quality of life of our members
 2016 Complex Case Management Program Description Our mission is to improve the health and quality of life of our members Complex Case Management Program Description I. Purpose To improve the health status
2016 Complex Case Management Program Description Our mission is to improve the health and quality of life of our members Complex Case Management Program Description I. Purpose To improve the health status
2015 Congestive Heart Failure. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2015 Congestive Heart Failure Program Evaluation Our mission is to improve the health and quality of life of our members 2015 Congestive Heart Failure Program Evaluation Program Title: Congestive Heart
2015 Congestive Heart Failure Program Evaluation Our mission is to improve the health and quality of life of our members 2015 Congestive Heart Failure Program Evaluation Program Title: Congestive Heart
2017 Congestive Heart Failure. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2017 Congestive Heart Failure Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Congestive Heart Failure Program Evaluation Program Title: Congestive Heart
2017 Congestive Heart Failure Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Congestive Heart Failure Program Evaluation Program Title: Congestive Heart
2017 Quality Improvement Work Plan Summary
 Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how the member s plan works.
Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how the member s plan works.
2016 Mommy Steps Program Descriptions
 2016 Mommy Steps Program Descriptions Our mission is to improve the health and quality of life of our members Mommy Steps Program Descriptions I. Purpose Passport Health Plan (Passport) has developed approaches
2016 Mommy Steps Program Descriptions Our mission is to improve the health and quality of life of our members Mommy Steps Program Descriptions I. Purpose Passport Health Plan (Passport) has developed approaches
DISEASE MANAGEMENT PROGRAMS. Procedural Manual. CMPCN Policy #5710
 DISEASE MANAGEMENT PROGRAMS Procedural Manual CMPCN Policy #5710 Effective Date: 01/01/2012 Revision Date(s) 11/18/2012; 10/01/13 ; 01/07/14 Approval Date(s) 12/18/2012 ; 10/23/13, 05/27,14 Annotated to
DISEASE MANAGEMENT PROGRAMS Procedural Manual CMPCN Policy #5710 Effective Date: 01/01/2012 Revision Date(s) 11/18/2012; 10/01/13 ; 01/07/14 Approval Date(s) 12/18/2012 ; 10/23/13, 05/27,14 Annotated to
2013 Mommy Steps. Program Description. Our mission is to improve the health and quality of life of our members
 2013 Mommy Steps Program Description Our mission is to improve the health and quality of life of our members I. Purpose Passport Health Plan (PHP) has developed approaches to the management of members
2013 Mommy Steps Program Description Our mission is to improve the health and quality of life of our members I. Purpose Passport Health Plan (PHP) has developed approaches to the management of members
EVOLENT HEALTH, LLC. Heart Failure Program Description 2017
 EVOLENT HEALTH, LLC Heart Failure Program Description 2017 1 Evolent Health Heart Failure Program Description 2017 Table of Contents Section Page Number I. Introduction. 3 II. Program Scope. 3 III. Program
EVOLENT HEALTH, LLC Heart Failure Program Description 2017 1 Evolent Health Heart Failure Program Description 2017 Table of Contents Section Page Number I. Introduction. 3 II. Program Scope. 3 III. Program
QUALITY IMPROVEMENT. Molina Healthcare has defined the following goals for the QI Program:
 QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
EVOLENT HEALTH, LLC Diabetes Program Description 2018
 EVOLENT HEALTH, LLC Diabetes Program Description 2018 1 Evolent Health Diabetes Program Description 2018 Table of Contents Section Page Number I. Introduction... 3 II. Program Scope... 3 III. Program Goals...
EVOLENT HEALTH, LLC Diabetes Program Description 2018 1 Evolent Health Diabetes Program Description 2018 Table of Contents Section Page Number I. Introduction... 3 II. Program Scope... 3 III. Program Goals...
EVOLENT HEALTH, LLC. Asthma Program Description 2018
 EVOLENT HEALTH, LLC Asthma Program Description 2018 1 Evolent Health Asthma Program Description 2018 Table of Contents Section Page Number I. Introduction... 3 II. Program Scope... 3 III. Program Goals...
EVOLENT HEALTH, LLC Asthma Program Description 2018 1 Evolent Health Asthma Program Description 2018 Table of Contents Section Page Number I. Introduction... 3 II. Program Scope... 3 III. Program Goals...
Dual-eligible SNPs should complete and submit Attachment A and, if serving beneficiaries with end-stage renal disease (ESRD), Attachment D.
 Attachment A: Model of Care for Dual-eligible SNPs MA Contract Name: Geisinger Health Plan MA Contract Number: H3954-097 Type of Dual-eligible SNP: Full The model of care describes the MAO's approach to
Attachment A: Model of Care for Dual-eligible SNPs MA Contract Name: Geisinger Health Plan MA Contract Number: H3954-097 Type of Dual-eligible SNP: Full The model of care describes the MAO's approach to
Asthma Disease Management Program
 Asthma Disease Management Program A: Program Content GHC-SCW is committed to helping members, and their practitioners, manage chronic illness by providing tools and resources to empower members to self-manage
Asthma Disease Management Program A: Program Content GHC-SCW is committed to helping members, and their practitioners, manage chronic illness by providing tools and resources to empower members to self-manage
The Heart and Vascular Disease Management Program
 Element A: Program Content The Heart and Vascular Disease Management Program GHC-SCW is committed to helping members, and their practitioners, manage chronic illness by providing tools and resources to
Element A: Program Content The Heart and Vascular Disease Management Program GHC-SCW is committed to helping members, and their practitioners, manage chronic illness by providing tools and resources to
Integration Workgroup: Bi-Directional Integration Behavioral Health Settings
 The Accountable Community for Health of King County Integration Workgroup: Bi-Directional Integration Behavioral Health Settings May 7, 2018 1 Integrated Whole Person Care in Community Behavioral Health
The Accountable Community for Health of King County Integration Workgroup: Bi-Directional Integration Behavioral Health Settings May 7, 2018 1 Integrated Whole Person Care in Community Behavioral Health
Medical Management. G.2 At a Glance. G.3 Procedures Requiring Prior Authorization. G.5 How to Contact or Notify Medical Management
 G.2 At a Glance G.3 Procedures Requiring Prior Authorization G.5 How to Contact or Notify Medical Management G.6 When to Notify Medical Management G.11 Case Management Services G.14 Special Needs Services
G.2 At a Glance G.3 Procedures Requiring Prior Authorization G.5 How to Contact or Notify Medical Management G.6 When to Notify Medical Management G.11 Case Management Services G.14 Special Needs Services
EVOLENT HEALTH, LLC. Asthma Program Description 2017
 EVOLENT HEALTH, LLC Asthma Program Description 2017 1 Evolent Health Asthma Program Description 2017 Table of Contents Section Page Number I. Introduction.. 3 II. Program Scope 3 III. Program Goals 4 IV.
EVOLENT HEALTH, LLC Asthma Program Description 2017 1 Evolent Health Asthma Program Description 2017 Table of Contents Section Page Number I. Introduction.. 3 II. Program Scope 3 III. Program Goals 4 IV.
2016 Member Incentive. Program Descriptions. Our mission is to improve the health and quality of life of our members
 2016 Member Incentive Program Descriptions Our mission is to improve the health and quality of life of our members Member Incentive Program Descriptions I. Purpose Passport Health Plan (Passport) has developed
2016 Member Incentive Program Descriptions Our mission is to improve the health and quality of life of our members Member Incentive Program Descriptions I. Purpose Passport Health Plan (Passport) has developed
Community Care of North Carolina
 Community Care of North Carolina 2007 Community Care of North Carolina Mail Service Center 2009 Raleigh, NC 27699-2009 (919) 715-1453 www.communitycarenc.com Background Several networks in the Community
Community Care of North Carolina 2007 Community Care of North Carolina Mail Service Center 2009 Raleigh, NC 27699-2009 (919) 715-1453 www.communitycarenc.com Background Several networks in the Community
Tips for PCMH Application Submission
 Tips for PCMH Application Submission Remain calm. The certification process is not as complicated as it looks. You will probably find you are already doing many of the required processes, and these are
Tips for PCMH Application Submission Remain calm. The certification process is not as complicated as it looks. You will probably find you are already doing many of the required processes, and these are
Provider Information Guide Complex Care and Condition Care Overview
 Complex and Overview Introduction Complex and are essential components of Passport Health Plan s (Passport) Coordination services, which are used to support the practitioner-patient relationship and plan
Complex and Overview Introduction Complex and are essential components of Passport Health Plan s (Passport) Coordination services, which are used to support the practitioner-patient relationship and plan
DRUG MEDI-CAL ORGANIZED DELIVERY SYSTEM (DMC-ODS) PERFORMANCE METRICS. (version 6/23/17)
 1 Access Enrollment information to include the number of DMC-ODS beneficiaries served in the DMC-ODS program Clients Served: 1. Number of DMC-ODS beneficiaries served (admissions) by the DMC- ODS County
1 Access Enrollment information to include the number of DMC-ODS beneficiaries served in the DMC-ODS program Clients Served: 1. Number of DMC-ODS beneficiaries served (admissions) by the DMC- ODS County
Stage 2 GP longitudinal placement learning outcomes
 Faculty of Life Sciences and Medicine Department of Primary Care & Public Health Sciences Stage 2 GP longitudinal placement learning outcomes Description This block focuses on how people and their health
Faculty of Life Sciences and Medicine Department of Primary Care & Public Health Sciences Stage 2 GP longitudinal placement learning outcomes Description This block focuses on how people and their health
Medical Management. G.2 At a Glance. G.2 Procedures Requiring Prior Authorization. G.3 How to Contact or Notify Medical Management
 G.2 At a Glance G.2 Procedures Requiring Prior Authorization G.3 How to Contact or Notify G.4 When to Notify G.7 Case Management Services G.10 Special Needs Services G.12 Health Management Programs G.14
G.2 At a Glance G.2 Procedures Requiring Prior Authorization G.3 How to Contact or Notify G.4 When to Notify G.7 Case Management Services G.10 Special Needs Services G.12 Health Management Programs G.14
Department of Behavioral Health
 PROGRAM INFORMATION: Program Title: Program Description: Mental Health Service Act (MHSA) Perinatal Team The Department of Behavioral Health (DBH) Perinatal Wellness Center provides outpatient mental health
PROGRAM INFORMATION: Program Title: Program Description: Mental Health Service Act (MHSA) Perinatal Team The Department of Behavioral Health (DBH) Perinatal Wellness Center provides outpatient mental health
Tennessee Health Link Guidelines: Adults Medical Necessity Criteria
 Tennessee Health Link Guidelines: Adults Medical Necessity Criteria https://providers.amerigroup.com Program description The Health Link service model is a program created to address the diverse needs
Tennessee Health Link Guidelines: Adults Medical Necessity Criteria https://providers.amerigroup.com Program description The Health Link service model is a program created to address the diverse needs
Follow-Up after Hospitalization for Mental Illness (FUH) Improvement Strategies
 Follow-Up after Hospitalization for Mental Illness (FUH) Improvement Strategies 1. What efforts and/or strategies have you put in place to improve your plans performance on the Follow-Up After Hospitalization
Follow-Up after Hospitalization for Mental Illness (FUH) Improvement Strategies 1. What efforts and/or strategies have you put in place to improve your plans performance on the Follow-Up After Hospitalization
Healthcare Effectiveness Data and Information Set (HEDIS)
 Healthcare Effectiveness Data and Information Set (HEDIS) IlliniCare Health is a proud holder of NCQA accreditation as a managed behavioral health organization (MBHO) and prioritizes best in class performance
Healthcare Effectiveness Data and Information Set (HEDIS) IlliniCare Health is a proud holder of NCQA accreditation as a managed behavioral health organization (MBHO) and prioritizes best in class performance
Passport Advantage (HMO SNP) Model of Care Training (Providers)
 Passport Advantage (HMO SNP) Model of Care Training (Providers) 2018 Passport Advantage (HMO SNP) is an HMO Special Needs plan with a Medicare contract and an agreement with the Kentucky Department for
Passport Advantage (HMO SNP) Model of Care Training (Providers) 2018 Passport Advantage (HMO SNP) is an HMO Special Needs plan with a Medicare contract and an agreement with the Kentucky Department for
Welcome to the Cenpatico 2017 Provider Newsletter
 Improving Lives 2017 ISSUE You want to help your patients. We re here to help you. This newsletter will provide you with information regarding our clinical and operational resources, and programs, all
Improving Lives 2017 ISSUE You want to help your patients. We re here to help you. This newsletter will provide you with information regarding our clinical and operational resources, and programs, all
Quality Management and Improvement 2016 Year-end Report
 Quality Management and Improvement Table of Contents Introduction... 4 Scope of Activities...5 Patient Safety...6 Utilization Management Quality Activities Clinical Activities... 7 Timeliness of Utilization
Quality Management and Improvement Table of Contents Introduction... 4 Scope of Activities...5 Patient Safety...6 Utilization Management Quality Activities Clinical Activities... 7 Timeliness of Utilization
ProviderReport. Managing complex care. Supporting member health.
 ProviderReport Supporting member health Managing complex care Do you have patients whose conditions need complex, coordinated care they may not be able to facilitate on their own? A care manager may be
ProviderReport Supporting member health Managing complex care Do you have patients whose conditions need complex, coordinated care they may not be able to facilitate on their own? A care manager may be
Institutional Handbook of Operating Procedures Policy
 Section: Clinical Policies Institutional Handbook of Operating Procedures Policy 09.01.13 Responsible Vice President: EVP and CEO Health System Subject: Admission, Discharge, and Transfer Responsible Entity:
Section: Clinical Policies Institutional Handbook of Operating Procedures Policy 09.01.13 Responsible Vice President: EVP and CEO Health System Subject: Admission, Discharge, and Transfer Responsible Entity:
Passport Advantage Provider Manual Section 10.0 Care Management
 Passport Advantage Provider Manual Section 10.0 Care Management Table of Contents 10.1 Model of Care 10.2 Medication Therapy Management 10.3 Care Coordination 10.4 Complex Case Management Page 1 of 9 10.0
Passport Advantage Provider Manual Section 10.0 Care Management Table of Contents 10.1 Model of Care 10.2 Medication Therapy Management 10.3 Care Coordination 10.4 Complex Case Management Page 1 of 9 10.0
MHS Care Management Program 1017.PR.P.PP.1 10/17
 MHS Care Management Program 1017.PR.P.PP.1 10/17 Sample Integrated Transitional Care Model Inpatient Admission Process Admission thru discharge and beyond Goals: Ensure safe and timely transitions of care
MHS Care Management Program 1017.PR.P.PP.1 10/17 Sample Integrated Transitional Care Model Inpatient Admission Process Admission thru discharge and beyond Goals: Ensure safe and timely transitions of care
Tennessee Health Link Guidelines: Adults Medical Necessity Criteria-Final
 Tennessee Health Link Guidelines: Adults Medical Necessity Criteria-Final Program Description Tennessee Health Link service model is a program created to address the diverse needs of individuals requiring
Tennessee Health Link Guidelines: Adults Medical Necessity Criteria-Final Program Description Tennessee Health Link service model is a program created to address the diverse needs of individuals requiring
Provider Orientation to Magellan s Outpatient Behavioral Health Model
 Provider Orientation to Magellan s Outpatient Behavioral Health Model July 2017 Big-picture objectives Magellan Healthcare s outpatient care management model: Reduces provider administrative tasks Expedites
Provider Orientation to Magellan s Outpatient Behavioral Health Model July 2017 Big-picture objectives Magellan Healthcare s outpatient care management model: Reduces provider administrative tasks Expedites
Chapter 2 Provider Responsibilities Unit 6: Behavioral Health Care Specialists
 Chapter 2 Provider Responsibilities Unit 6: Health Care Specialists In This Unit Unit 6: Health Care Specialists General Information 2 Highmark s Health Programs 4 Accessibility Standards For Health Providers
Chapter 2 Provider Responsibilities Unit 6: Health Care Specialists In This Unit Unit 6: Health Care Specialists General Information 2 Highmark s Health Programs 4 Accessibility Standards For Health Providers
APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS
 Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
Model of Care Heritage Provider Network & Arizona Priority Care Model of Care 2018
 Model of Care Model of Care 2018 Learning Objectives Program participants will be able to: List two differences between the Complex Care Management (CCM), and Special Needs Program (SNP) programs. Identify
Model of Care Model of Care 2018 Learning Objectives Program participants will be able to: List two differences between the Complex Care Management (CCM), and Special Needs Program (SNP) programs. Identify
Molina Medicare Model of Care
 Molina Medicare Model of Care Provider Network Molina Healthcare 2018 1 Molina s Mission and Vision Our Vision: We envision a future where everyone receives quality health care Our Mission: To provide
Molina Medicare Model of Care Provider Network Molina Healthcare 2018 1 Molina s Mission and Vision Our Vision: We envision a future where everyone receives quality health care Our Mission: To provide
ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 SERIOUS MENTAL ILLNESS SPECIALTY PLAN
 ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 SERIOUS MENTAL ILLNESS SPECIALTY PLAN The provisions in Attachment II and the MMA Exhibit apply to this Specialty Plan, unless otherwise specified
ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 SERIOUS MENTAL ILLNESS SPECIALTY PLAN The provisions in Attachment II and the MMA Exhibit apply to this Specialty Plan, unless otherwise specified
Winter 2017 Provider Newsletter
 Winter 2017 Provider Newsletter TEXAS HEALTH STEPS (THSTEPS) ADDITIONAL MENTAL HEALTH SCREENING TOOL FOR THSTEPS CHECKUPS Effective for dates of service on or after February 1, 2017, the Pediatric Symptom
Winter 2017 Provider Newsletter TEXAS HEALTH STEPS (THSTEPS) ADDITIONAL MENTAL HEALTH SCREENING TOOL FOR THSTEPS CHECKUPS Effective for dates of service on or after February 1, 2017, the Pediatric Symptom
New York State Medicaid Value Based Payment: Data Driven Strategies. Bundled Payment Summit June 27, 2017
 New York State Medicaid Value Based Payment: Data Driven Strategies Bundled Payment Summit June 27, 2017 Panelists Moderator Paloma Hernandez Anthony Thompson Marc Berg President and CEO Urban Health Plan
New York State Medicaid Value Based Payment: Data Driven Strategies Bundled Payment Summit June 27, 2017 Panelists Moderator Paloma Hernandez Anthony Thompson Marc Berg President and CEO Urban Health Plan
PCMH 2014 Recognition Checklist
 1 PCMH1: Patient Centered Access 10.00 points Element A - Patient-Centered Appointment Access ~~ MUST PASS 4.50 points 1 Providing same-day appointments for routine and urgent care (Critical Factor) Policy
1 PCMH1: Patient Centered Access 10.00 points Element A - Patient-Centered Appointment Access ~~ MUST PASS 4.50 points 1 Providing same-day appointments for routine and urgent care (Critical Factor) Policy
Analysis of VA Health Care Utilization Among US Global War on Terrorism (GWOT) Veterans
 Analysis of VA Health Care Utilization Among US Global War on Terrorism (GWOT) Veterans Operation Enduring Freedom Operation Iraqi Freedom VHA Office of Public Health and Environmental Hazards May 2008
Analysis of VA Health Care Utilization Among US Global War on Terrorism (GWOT) Veterans Operation Enduring Freedom Operation Iraqi Freedom VHA Office of Public Health and Environmental Hazards May 2008
Statewide Inpatient Psychiatric Programs Admission Process and Level of Care Criteria. Effective August 1, 2014
 Statewide Inpatient Psychiatric Programs Admission Process and Level of Care Criteria Effective August 1, 2014 1 Table of Contents Florida Medicaid Handbook... 3 Clinical Practice Guidelines... 3 Description
Statewide Inpatient Psychiatric Programs Admission Process and Level of Care Criteria Effective August 1, 2014 1 Table of Contents Florida Medicaid Handbook... 3 Clinical Practice Guidelines... 3 Description
2015 Quality Improvement Work Plan Summary
 2015 Quality Improvement Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how
2015 Quality Improvement Project Member Service and Satisfaction Commercial Products: Commercial Project Description: To improve member service and satisfaction and increase member understanding of how
Domain 1 Patient Engagement Speed Data Reports & Schedule
 Domain 1 Patient Engagement Speed Data Reports & Schedule Suffolk Care Collaborative (SCC) Suffolk County Performing Provider System (PPS) Delivery System Reform Incentive Payment (DSRIP) Program 2 PRESENTATION
Domain 1 Patient Engagement Speed Data Reports & Schedule Suffolk Care Collaborative (SCC) Suffolk County Performing Provider System (PPS) Delivery System Reform Incentive Payment (DSRIP) Program 2 PRESENTATION
QUALITY CARE QUARTERLY
 QUALITY CARE QUARTERLY Summer 2018 - Volume 5 Your Guide to Programs and Rewards Featuring A message from Dr. Deborah Gatlin, Behavioral Health Medical Director Saint Thomas Medical Partners Sees Benefits
QUALITY CARE QUARTERLY Summer 2018 - Volume 5 Your Guide to Programs and Rewards Featuring A message from Dr. Deborah Gatlin, Behavioral Health Medical Director Saint Thomas Medical Partners Sees Benefits
Appendix 4. PCMH Distinction in Behavioral Health Integration
 Appendix 4 PCMH Distinction in Behavioral Health Integration Appendix 4 PCMH Distinction in 4-1 Distinction Purpose and Background Behavioral health conditions (mental illnesses and substance use disorders)
Appendix 4 PCMH Distinction in Behavioral Health Integration Appendix 4 PCMH Distinction in 4-1 Distinction Purpose and Background Behavioral health conditions (mental illnesses and substance use disorders)
Mental Health Inpatient Care Requirements
 Mental Health Inpatient Care Requirements These Mental Health Inpatient Care Requirements are for coordinating with our partner Mental Health Centers (MHC s) for the clinical care provided by your facility
Mental Health Inpatient Care Requirements These Mental Health Inpatient Care Requirements are for coordinating with our partner Mental Health Centers (MHC s) for the clinical care provided by your facility
ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 HIV/AIDS SPECIALTY PLAN
 ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 HIV/AIDS SPECIALTY PLAN The provisions in Attachment II and the MMA Exhibit apply to this Specialty Plan, unless otherwise specified in this
ATTACHMENT II EXHIBIT II-C Effective Date: February 1, 2018 HIV/AIDS SPECIALTY PLAN The provisions in Attachment II and the MMA Exhibit apply to this Specialty Plan, unless otherwise specified in this
HEALTHY EMPLOYEES HEALTHY EMPLOYEE BENEFIT PLAN
 HEALTHY EMPLOYEES HEALTHY EMPLOYEE BENEFIT PLAN At a point in time when many employers are forced to cut benefits healthcare costs are increasing at 3 to 4 times the rate of inflation access to quality
HEALTHY EMPLOYEES HEALTHY EMPLOYEE BENEFIT PLAN At a point in time when many employers are forced to cut benefits healthcare costs are increasing at 3 to 4 times the rate of inflation access to quality
September, James Misak, M.D. Linda Stokes, MSPH The MetroHealth System
 Better Health Greater Cleveland relies on the presenter to obtain all rights to use and display copyright-protected information. Anyone claiming a right or interest in or to any posted information should
Better Health Greater Cleveland relies on the presenter to obtain all rights to use and display copyright-protected information. Anyone claiming a right or interest in or to any posted information should
Patient Centered Medical Home 2011
 Patient Centered Medical Home 2011 NCQA Standards Rand David, MD, FACP Associate Professor of Medicine Director, Dept. of Ambulatory Care Mount Sinai School of Medicine Elmhurst Hospital Center I have
Patient Centered Medical Home 2011 NCQA Standards Rand David, MD, FACP Associate Professor of Medicine Director, Dept. of Ambulatory Care Mount Sinai School of Medicine Elmhurst Hospital Center I have
Molina Medicare Model of Care. Healthcare Services Molina Healthcare 2016
 Molina Medicare Model of Care Healthcare Services Molina Healthcare 2016 MHTPS_MOCTRN_062016 1 Molina s Mission Our mission is to provide quality health services to financially vulnerable families and
Molina Medicare Model of Care Healthcare Services Molina Healthcare 2016 MHTPS_MOCTRN_062016 1 Molina s Mission Our mission is to provide quality health services to financially vulnerable families and
UTILIZATION MANAGEMENT AND CARE COORDINATION Section 8
 Overview The focus of WellCare s Utilization Management (UM) Program is to provide members access to quality care and to monitor the appropriate utilization of services. WellCare s UM Program has five
Overview The focus of WellCare s Utilization Management (UM) Program is to provide members access to quality care and to monitor the appropriate utilization of services. WellCare s UM Program has five
NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11
 NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11 28 PCMH 1: Enhance Access and Continuity PCMH 1: Enhance Access and Continuity 20 points provides access to culturally and linguistically
NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11 28 PCMH 1: Enhance Access and Continuity PCMH 1: Enhance Access and Continuity 20 points provides access to culturally and linguistically
Access to Psychiatric Inpatient Care: Prolonged Waiting Periods in Medical Emergency Departments. Data Report for
 Access to Psychiatric Inpatient Care: Prolonged Waiting Periods in Medical Emergency Departments Data Report for 2012-2014 Prepared by: Jennifer D. Dudek, MPH 150 North 18 th Avenue, Suite 320 Phoenix,
Access to Psychiatric Inpatient Care: Prolonged Waiting Periods in Medical Emergency Departments Data Report for 2012-2014 Prepared by: Jennifer D. Dudek, MPH 150 North 18 th Avenue, Suite 320 Phoenix,
Behavioral Health Provider Training: Program Overview & Helpful Information
 Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
Section IX Special Needs & Case Management
 Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
WORK PROCESS DOCUMENT NAME: Medical Necessity Review for Behavioral Health and Substance Use Disorder REPLACES DOCUMENT: RETIRED:
 PAGE: 1 of 7 SCOPE: Coordinated Care Departments for Behavioral Health and Substance Use Disorder (SUD) Reviews for members enrolled in Integrated Managed Care and Behavioral Health Services Only PURPOSE:
PAGE: 1 of 7 SCOPE: Coordinated Care Departments for Behavioral Health and Substance Use Disorder (SUD) Reviews for members enrolled in Integrated Managed Care and Behavioral Health Services Only PURPOSE:
DSRIP Demonstration Year 1, Quarter 1-2 Domain 1 Patient Engagement Data Request
 DSRIP Demonstration Year 1, Quarter 1-2 Domain 1 Patient Engagement Data Request Webinar: Monday, October 5, 2015 Time: 1:30pm-3:00pm Presented by Suffolk Care Collaborative (SCC) Suffolk County Performing
DSRIP Demonstration Year 1, Quarter 1-2 Domain 1 Patient Engagement Data Request Webinar: Monday, October 5, 2015 Time: 1:30pm-3:00pm Presented by Suffolk Care Collaborative (SCC) Suffolk County Performing
INTEGRATED CASE MANAGEMENT ANNEX A
 INTEGRATED CASE MANAGEMENT ANNEX A NAME OF AGENCY: CONTRACT NUMBER: CONTRACT TERM: TO BUDGET MATRIX CODE: 32 This Annex A specifies the Integrated Case Management services that the Provider Agency is authorized
INTEGRATED CASE MANAGEMENT ANNEX A NAME OF AGENCY: CONTRACT NUMBER: CONTRACT TERM: TO BUDGET MATRIX CODE: 32 This Annex A specifies the Integrated Case Management services that the Provider Agency is authorized
Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum
 Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum Betsy Gornet, FACHE Chief Advanced Illness Management Executive Sutter Health / Sutter Care
Advanced Illness Management Leveraging Person Centered Care and Reengineering the Care Team Across the Continuum Betsy Gornet, FACHE Chief Advanced Illness Management Executive Sutter Health / Sutter Care
Patterns of Ambulatory Mental Health Care in Navy Clinics
 CRM D0003835.A2/Final June 2001 Patterns of Ambulatory Mental Health Care in Navy Clinics Michelle Dolfini-Reed 4825 Mark Center Drive Alexandria, Virginia 22311-1850 Approved for distribution: June 2001
CRM D0003835.A2/Final June 2001 Patterns of Ambulatory Mental Health Care in Navy Clinics Michelle Dolfini-Reed 4825 Mark Center Drive Alexandria, Virginia 22311-1850 Approved for distribution: June 2001
Behavioral Health Services
 18 Behavioral Health Services Reviewed/Revised: 10/10/2017, 02/01/2017, 02/15/2016, 08/31/2015, 09/18/2014 INTRODUCTION The State of Arizona has contracted the administration of AHCCCS mental health and
18 Behavioral Health Services Reviewed/Revised: 10/10/2017, 02/01/2017, 02/15/2016, 08/31/2015, 09/18/2014 INTRODUCTION The State of Arizona has contracted the administration of AHCCCS mental health and
Ryan White Part A. Quality Management
 Quality Management Mental Health Services Broward County/Fort Lauderdale Eligible Metropolitan Area (EMA) The creation of this public document is fully funded by a federal Ryan White CARE Act Part A grant
Quality Management Mental Health Services Broward County/Fort Lauderdale Eligible Metropolitan Area (EMA) The creation of this public document is fully funded by a federal Ryan White CARE Act Part A grant
ILLINOIS 1115 WAIVER BRIEF
 ILLINOIS 1115 WAIVER BRIEF STATE TESTING FOR THE FOLLOWING ACHIEVED RESULTS: 1. Increased rates of identification, initiation, and engagement in treatment 2. Increased adherence to and retention in treatment
ILLINOIS 1115 WAIVER BRIEF STATE TESTING FOR THE FOLLOWING ACHIEVED RESULTS: 1. Increased rates of identification, initiation, and engagement in treatment 2. Increased adherence to and retention in treatment
Interactive Voice Registration (IVR) System Manual WASHINGTON STREET, SUITE 310 BOSTON, MA (800)
 Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 (800) 495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 (800) 495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
Blending Behavioral Health and Primary Care. Cherokee Health Systems Clinical Model
 Blending Behavioral Health and Primary Care Cherokee Health Systems Clinical Model Brittany Tenbarge, Ph.D. Behavioral Health Consultant Licensed Clinical Psychologist Our Mission To improve the quality
Blending Behavioral Health and Primary Care Cherokee Health Systems Clinical Model Brittany Tenbarge, Ph.D. Behavioral Health Consultant Licensed Clinical Psychologist Our Mission To improve the quality
IV. Clinical Policies and Procedures
 A. Introduction The role of ValueOptions NorthSTAR is to coordinate the delivery of clinical services. There are three parties to this care coordination process: the Enrollee, the Provider(s), and the
A. Introduction The role of ValueOptions NorthSTAR is to coordinate the delivery of clinical services. There are three parties to this care coordination process: the Enrollee, the Provider(s), and the
Coding Guidance for HIV Clinical Practices: Care Management Services
 Coding Guidance for HIV Clinical Practices: Care Management Services HIV medical practices and clinicians provide many services outside of a face-to-face encounter with a patient. Some of these services
Coding Guidance for HIV Clinical Practices: Care Management Services HIV medical practices and clinicians provide many services outside of a face-to-face encounter with a patient. Some of these services
Appendix 5. PCSP PCMH 2014 Crosswalk
 Appendix 5 Crosswalk NCQA Patient-Centered Medical Home 2014 July 28, 2014 Appendix 5 Crosswalk 5-1 APPENDIX 5 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice () standards with
Appendix 5 Crosswalk NCQA Patient-Centered Medical Home 2014 July 28, 2014 Appendix 5 Crosswalk 5-1 APPENDIX 5 Crosswalk The table compares NCQA s Patient-Centered Specialty Practice () standards with
ALLIED PHYSICIAN IPA ADVANTAGE HEALTH NETWORK IPA ARROYO VISTA MEDICAL IPA GREATER ORANGE MEDICAL GROUP IPA GREATER SAN GABRIEL VALLEY PHYSICIANS IPA
 ALLIED PHYSICIAN IPA ADVANTAGE HEALTH NETWORK IPA ARROYO VISTA MEDICAL IPA GREATER ORANGE MEDICAL GROUP IPA GREATER SAN GABRIEL VALLEY PHYSICIANS IPA QUALITY IMPROVEMENT PROGRAM 2010 Overview The Quality
ALLIED PHYSICIAN IPA ADVANTAGE HEALTH NETWORK IPA ARROYO VISTA MEDICAL IPA GREATER ORANGE MEDICAL GROUP IPA GREATER SAN GABRIEL VALLEY PHYSICIANS IPA QUALITY IMPROVEMENT PROGRAM 2010 Overview The Quality
2015 Member Incentive. Program Evaluation. Our mission is to improve the health and quality of life of our members
 25 Member Incentive Program Evaluation Our mission is to improve the health and quality of life of our members 25 Member Incentive Program Evaluation Annual Participation Rate Program Title: Member Incentive
25 Member Incentive Program Evaluation Our mission is to improve the health and quality of life of our members 25 Member Incentive Program Evaluation Annual Participation Rate Program Title: Member Incentive
April Data Jam: Tracking Progress and Facilitating Improvement with your Data Dashboard
 April Data Jam: Tracking Progress and Facilitating Improvement with your Data Dashboard Elizabeth Arend, MPH Quality Improvement Advisor National Council for Behavioral Health CMS Change Package: Primary
April Data Jam: Tracking Progress and Facilitating Improvement with your Data Dashboard Elizabeth Arend, MPH Quality Improvement Advisor National Council for Behavioral Health CMS Change Package: Primary
Integration of Behavioral Health & Primary Care in a Homeless FQHC
 Integration of Behavioral Health & Primary Care in a Homeless FQHC AtlantiCare Health Services Mission Health Care May 2012 Bridgette Richardson, LCSW Executive Director, AtlantiCare Health Services, Mission
Integration of Behavioral Health & Primary Care in a Homeless FQHC AtlantiCare Health Services Mission Health Care May 2012 Bridgette Richardson, LCSW Executive Director, AtlantiCare Health Services, Mission
Results from the Iowa Medicaid Congestive Heart Failure Population Disease Management
 EXECUTIVE SUMMARY Study Validates Use of Technology-Based Remote Monitoring Platform to Reduce Healthcare Utilization and Cost Results from the Iowa Medicaid Congestive Heart Failure Population Disease
EXECUTIVE SUMMARY Study Validates Use of Technology-Based Remote Monitoring Platform to Reduce Healthcare Utilization and Cost Results from the Iowa Medicaid Congestive Heart Failure Population Disease
Specialty Behavioral Health and Integrated Services
 Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
Introduction Behavioral health services that are provided within primary care clinics are important to meeting our members needs. Health Share of Oregon supports the integration of behavioral health and
Model Of Care: Care Coordination Interdisciplinary Care Team (ICT)
 Cal MediConnect 2017 Model Of Care: Care Coordination Interdisciplinary Care Team (ICT) 2017 CMC Annual Training Learning Objectives Define the L.A. Care Cal MediConnect (CMC) Model of Care Describe the
Cal MediConnect 2017 Model Of Care: Care Coordination Interdisciplinary Care Team (ICT) 2017 CMC Annual Training Learning Objectives Define the L.A. Care Cal MediConnect (CMC) Model of Care Describe the
Communicator. the JUST A THOUGHT. Ensuring HEDIS-Compliant Preventive Health Services. Provider Portal Features. Peer-to-Peer Review BY DR.
 WINTER 2016 MHS NEWSLETTER FOR PHYSICIANS Ensuring HEDIS-Compliant Preventive Health Services Here are a few best practice strategies for raising HEDIS and EPSDT onsite review scores, as demonstrated by
WINTER 2016 MHS NEWSLETTER FOR PHYSICIANS Ensuring HEDIS-Compliant Preventive Health Services Here are a few best practice strategies for raising HEDIS and EPSDT onsite review scores, as demonstrated by
Behavioral Health Division JPS Health Network
 Behavioral Health Division JPS Health Network Macro Trends 1 in 5 Adults in America experience a mental illness Diversion of Behavioral Health patients from jail Federal Prisons Mental Illness State Prison
Behavioral Health Division JPS Health Network Macro Trends 1 in 5 Adults in America experience a mental illness Diversion of Behavioral Health patients from jail Federal Prisons Mental Illness State Prison
Medicare Advantage Quality Improvement Project (QIP) & Chronic Care Improvement Program (CCIP)
 Medicare Advantage Quality Improvement Project (QIP) & Chronic Care Improvement Program (CCIP) Medicare Drug and Health Plan Contract Administration Group Donna Williamson & Brandy Alston December 6, 2016
Medicare Advantage Quality Improvement Project (QIP) & Chronic Care Improvement Program (CCIP) Medicare Drug and Health Plan Contract Administration Group Donna Williamson & Brandy Alston December 6, 2016
Care Transitions Engaging Psychiatric Inpatients in Outpatient Care
 Care Transitions Engaging Psychiatric Inpatients in Outpatient Care Mark Olfson, MD, MPH Columbia University New York State Psychiatric Institute New York, NY A physician is obligated to consider more
Care Transitions Engaging Psychiatric Inpatients in Outpatient Care Mark Olfson, MD, MPH Columbia University New York State Psychiatric Institute New York, NY A physician is obligated to consider more
SECTION 3. Behavioral Health Core Program Standards. Z. Health Home
 SECTION 3 Behavioral Health Core Program Standards Z. Health Home Description Health home is a healthcare delivery approach that focuses on the whole person and provides integrated healthcare coordination
SECTION 3 Behavioral Health Core Program Standards Z. Health Home Description Health home is a healthcare delivery approach that focuses on the whole person and provides integrated healthcare coordination
Reduce Readmissions & Avoidable ED Visits: Advocate Health Care s Medically Integrated Crisis Community Support
 Reduce Readmissions & Avoidable ED Visits: Advocate Health Care s Medically Integrated Crisis Community Support by Sheri Richardt, L.C.S.W. Manager for Crisis/CL/First Access/MICCS/After Care and Shastri
Reduce Readmissions & Avoidable ED Visits: Advocate Health Care s Medically Integrated Crisis Community Support by Sheri Richardt, L.C.S.W. Manager for Crisis/CL/First Access/MICCS/After Care and Shastri
Ryan White Part A Quality Management
 Quality Management Mental Health Services Broward County/Fort Lauderdale Eligible Metropolitan Area (EMA) The creation of this public document is fully funded by a federal Ryan White CARE Act Part A grant
Quality Management Mental Health Services Broward County/Fort Lauderdale Eligible Metropolitan Area (EMA) The creation of this public document is fully funded by a federal Ryan White CARE Act Part A grant
Medical Appropriateness and Risk Adjustment
 Medical Appropriateness and Risk Adjustment Medical Appropriateness David Rzeszutko, MD Medical Director November 10, 2017 Objectives Medical necessity Value equation Medical appropriateness Why? To improve
Medical Appropriateness and Risk Adjustment Medical Appropriateness David Rzeszutko, MD Medical Director November 10, 2017 Objectives Medical necessity Value equation Medical appropriateness Why? To improve
ACOs: California Style
 ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
ACOs: California Style ACO Congress John E. Jenrette, M.D. Chief Executive Officer Sharp Community Medical Group November 2, 2011 California Style California Style A CO California Style California Style
Pain: Facility Assessment Checklists
 Pain: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to pain management in the facility, in order to identify areas
Pain: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to pain management in the facility, in order to identify areas
Behavioral Health Provider Training: Program Overview & Helpful Information
 Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
PCMH 1A Patient Centered Access
 PCMH 1A Patient Centered Access The practice has a written process and defined standards for providing access to appointments, and regularly assesses its performance on: Providing same day appointments
PCMH 1A Patient Centered Access The practice has a written process and defined standards for providing access to appointments, and regularly assesses its performance on: Providing same day appointments
STANDARDS OF CARE HIV AMBULATORY OUTPATIENT MEDICAL CARE STANDARDS I. DEFINITION OF SERVICES
 S OF CARE Oakland Transitional Grant Area Care and Treatment Services J ANUARY 2007 Office of AIDS Administration 1000 Broadway, Suite 310 Oakland, CA 94612 Tel: 510. 268.7630 Fax: 510.268-7631 AREAS OF
S OF CARE Oakland Transitional Grant Area Care and Treatment Services J ANUARY 2007 Office of AIDS Administration 1000 Broadway, Suite 310 Oakland, CA 94612 Tel: 510. 268.7630 Fax: 510.268-7631 AREAS OF
2017 EPSDT. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2017 EPSDT Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Early and Periodic Screening, Diagnosis, and Treatment Program Evaluation Program Title: Early
2017 EPSDT Program Evaluation Our mission is to improve the health and quality of life of our members 2017 Early and Periodic Screening, Diagnosis, and Treatment Program Evaluation Program Title: Early
Interactive Voice Registration (IVR) System Manual WASHINGTON STREET, SUITE 310 BOSTON, MA
 Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 1-800-495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
Interactive Voice Registration (IVR) System Manual 1000 WASHINGTON STREET, SUITE 310 BOSTON, MA 02118-5002 1-800-495-0086 www.masspartnership.com TABLE OF CONTENTS INTRODUCTION... 3 IVR INSTRUCTIONS...
MODEL OF CARE TRAINING 2018
 MDEL F CARE TRAINING 2018 Content Introduction to SNP SNP Model of Care CHMP SNP population and vulnerable population SNP Benefit Roles and Responsibility HRA ICT Team Care Transition process Provider
MDEL F CARE TRAINING 2018 Content Introduction to SNP SNP Model of Care CHMP SNP population and vulnerable population SNP Benefit Roles and Responsibility HRA ICT Team Care Transition process Provider
