Gastrostomy Tube Placement: Pre-op Phase v2.0
|
|
|
- Earl Shields
- 6 years ago
- Views:
Transcription
1 Gastrostomy Tube Placement: Pre-op Phase v2.0 Executive Summary Explanation of Evidence Ratings Citation Information Summary of Version Changes Recommendations Prophylactic fundoplication is not recommended for any patient population. Gastrostomy tube placement alone will be done only if the patient demonstrates tolerance of nasogastric feeds. Patients under 1 year of age who are unable to demonstrate tolerance of nasogastric feeds (due to physiologic regurgitation) and who are unable to protect their airway may be considered for fundoplication with gastrostomy tube placement Fundoplication with gastrostomy tube placement may be considered in patients with progressive neurologic disorders. Avoidance of gastrojejunostomy tube placement should be considered in cases where families have difficulty accessing adequate medical care secondary to geography or other environmental circumstances. Inclusion Criteria All patients anticipated to receive primary gastrostomy tube, primary gastrojejunostomy tube or gastrostomy with fundoplication Exclusion Criteria Patients scheduled for concurrent major surgical interventions Patients undergoing gastrostomy tube change, repair, or g to j tube advancement Gastrostomy tube readiness Checklist completed? Yes, schedule procedure Procedure Scheduled Patient arrives to pre-op area Pre-Op Phase ordered and initiated by proceduralist Perioperative abx Pre-op Universal time out OR Default to General Surgery Placement Children < 4 kg Children at high-risk for forceful gastrostomy pulling Children with anatomic anomalies Kyphoscoliosis Hiatal hernia Children with prior abdominal operations precluding percutaneous placement Concomitant other operation No! Do not schedule IR ONLY IR Pre-op Phase ordered and initiated by IR service Recommendations Place a gastrostomy tube through the rectus abdominis midway between the umbilicus and costal margin, in the antrum of the stomach away from the pylorus Intra Op Tube lot number and brand recorded 16 french gastrostomy tube will be placed Transfer to PACU! Signout must occur from proceduralist to admitting team prior to transfer from PACU PACU manangement Pain: IV morphine NPO, IVF orders Signout from Proceduralist to Admitting service Post-Op Phase ordered and initiated by proceduralist Discharge from PACU Criteria Patient stable, pain controlled Signout to admitting team is completed by proceduralist For questions concerning this pathway, contact: gastrostomytubeplacement@seattlechildrens.org 2015 Seattle Children s Spine, all rights reserved, Medical Disclaimer Last Updated: March 2015 Next Expected Revision: May 2016
2 Gastrostomy Tube Placement: Inpatient Phase v2.0 Inpatient Management POD #0 Admit to: Medical Home service or Medical Hospitalist if no medical home identified NPO except for medications via gastrostomy 6 hours post-op. Use liquid medication when available. For patients with gastrojejunostomy, g tube to be used for medications. Standardized, age/developmentally appropriate pain scores (N-PASS, FLACC) will be used to assess pain. Every four hours in addition to before and after pain medication delivery. Patients will receive acetaminophen around-the-clock in addition to narcotics and ibuprofen as needed for breakthrough pain. On the day of surgery, intravenous morphine can be used, on subsequent days patients will be transitioned to enteral oxycodone If not tolerating enteral medications, IV toradol and rectal acetaminophen can be used Consider concurrent procedures when assessing pain. Nursing orders: routine VS, strict I&O, IV maintenance fluids, Feeding tube to be vented NOT clamped Contact proceduralist for specific questions/concerns regarding the recently placed tube. Care coordination notified! Nutrition consult ordered Stop feeds and notify provider for pain with feeding, vomiting, abdominal distention, fresh bleeding, or Inpatient Management POD #1 external leakage of gastric contents Admitting provider to assess patient prior to initiation of feeds. Any concerns about the patient assessment or initiation of feeds should be discussed with the proceduralist care team. Start full strength feeds the morning following tube placement at 50% goal volume. For bolus feeds, advance to full feed volume over 3 boluses. For continuous feeds, advance volume q 1 hour to goal volume feeds by 6 hours. If not tolerating feeds, contact admitting provider for further assessment and plans Pain control :Patients greater than 6 months old will be transitioned to enteral oxycodone and scheduled acetaminophen and ibuprofen. Patients less than 6 months old will not receive ibuprofen Nursing orders: routine VS, strict I&O, q 4 hr pain assessment with N-PASS, FLACC scores in addition to pre and post pain medication administration, call for pain with feeding, vomiting, abdominal distention, fresh bleeding, or leaking at tube site Contact proceduralist for specific questions/concerns regarding the recently placed tube Assess discharge criteria Discharge Criteria Tolerance of pre-operative feeding volume Tolerance of pre-operative medication regimen Adequate pain control and tolerance of post-operative pain medications Passage of stool or flatus Completion of home teaching Home health follow-up plans arranged Availability of home equipment Follow up appointments with primary dietitian and proceduralist service scheduled Temp < 38c x 12 hrs, no incision redness or pain, UOP > 0.5 ml/kg/hr if > 2years old, >1ml/kg/hr if < 2 years old Yes, discharge No Discharge Instructions Follow up with proceduralist in days Follow up with primary dietitian and medical home in 4 weeks Yes, however patient to remain hospitalized for ongoing management of comorbidities Off Pathway Continued inpatient management per admitting service Contact proceduralist for specific questions/concerns regarding the recently placed tube For questions concerning this pathway, contact: gastrostomytubeplacement@seattlechildrens.org 2015 Seattle Children s Spine, all rights reserved, Medical Disclaimer Last Updated: March 2015 Next Expected Revision: May 2016
3 Gastrostomy Tube Readiness Checklist All parts of this form must be completed prior to scheduling of surgery. This is ordered through Ad hoc Charting.. This form can be ordered by licensed independent providers and IR (e.g. Kirby Meyer PA, Amy Skjonsberg IR Nurse Coordinator) 1. Nasogastric/nasoduodenal feeding trial successfully completed (at goal feeding regimen)? Yes 2. Upper GI study completed and ligament of Treitz is in correct position? Yes 3. Feed Tube home identified? Yes Feed Tube home (Provider name and service, if provider is not on staff at SCH, please specify phone number) 4. Nutrition/tube feeding plan determined (including goals and timelines)? Yes 5. Is patient followed by dietitian at Seattle Children s? Yes Who? (use provider selector box) No Other (community-based) dietitians: (optional field) 6. Is patient already followed by a Seattle Children s feeding therapist (OT/PT/SLP)? Yes Who? Other feeding therapists: (optional field) 7. Family social/psych readiness assessed? Yes 8. Home health care company identified? Yes Who? 9. Based on the questions above, is patient ready to be scheduled for gastrostomy tube placement? Yes
4 Executive Summary Return to Home Cont. to Pg 2
5 Executive Summary, cont. Return to Home Cont. to Pg 3
6 Executive Summary Return to Home Cont. to Pg 4
7 Executive Summary Return to Home
8 Return to Home
9 Inpatient Phase
10 Evidence Ratings We used the GRADE method of rating evidence quality. Evidence is first assessed as to whether it is from randomized trial, or observational studies. The rating is then adjusted in the following manner: Quality ratings are downgraded if studies: Have serious limitations Have inconsistent results If evidence does not directly address clinical questions If estimates are imprecise OR If it is felt that there is substantial publication bias Quality ratings can be upgraded if it is felt that: The effect size is large If studies are designed in a way that confounding would likely underreport the magnitude of the effect OR If a dose-response gradient is evident Quality of Evidence: High quality Moderate quality Low quality Very low quality Expert Opinion (E) Reference: Guyatt G et al. J Clin Epi 2011: To Bibliography Return to Home
11 Summary of Version Changes Version 1.0 (5/28/13): Go live Version 2.0 (3/16/15): Updates to the Readiness Checklist and reformatted to meet new CSW standards/formats Return to Home
12 Medical Disclaimer Medicine is an ever-changing science. As new research and clinical experience broaden our knowledge, changes in treatment and drug therapy are required. The authors have checked with sources believed to be reliable in their efforts to provide information that is complete and generally in accord with the standards accepted at the time of publication. However, in view of the possibility of human error or changes in medical sciences, neither the authors nor Seattle Children s Healthcare System nor any other party who has been involved in the preparation or publication of this work warrants that the information contained herein is in every respect accurate or complete, and they are not responsible for any errors or omissions or for the results obtained from the use of such information. Readers should confirm the information contained herein with other sources and are encouraged to consult with their health care provider before making any health care decision. Return to Home
13 Bibliography Studies were identified by searching electronic databases using search strategies developed and executed by a medical librarian, Susan Klawansky. Searches were performed in April, The following databases were searched on the Ovid platform: Medline (2002 to date), Cochrane Database of Systematic Reviews (2005 to date); elsewhere Embase (2002 to date), Clinical Evidence, National Guideline Clearinghouse, TRIP and Cincinnati Children s Evidence-Based Care Guidelines. Retrieval was limited to children (0-18 years of age) and English language. In Medline and Embase, appropriate Medical Subject Headings (MeSH) and Emtree headings were used respectively, along with text words, and the search strategy was adapted for other databases as appropriate. Concepts searched were enteral nutrition, gastrointestinal intubation, gastrostomy and associated terms for various types of feeding tubes. All retrieval was further limited to certain evidence categories, such as relevant publication types, index terms for study types and other similar limits. Susan Klawansky, MLS, AHIP June 21, 2012 Identification 973 records identified through database searching 10 additional records identified through other sources Screening 747 records after duplicates removed 747 records screened 719 records excluded Elgibility 28 full-text articles assessed for eligibility 13 full-text articles excluded, 13 did not answer clinical question 0 did not meet quality threshold Included 15 studies included in pathway Flow diagram adapted from Moher D et al. BMJ 2009;339:bmj.b2535 To Bibliography, Pg 1 Return to Home
14 Bibliography Barnhart. Effectiveness of fundoplication at the time of gastrostomy in neurologically impaired infants. JAMA-Pediatrics accepted, publication pending. Bankhead,R.;Boullata,J.;Brantley,S.;et al.enteral nutrition practice recommendations.jpen: Journal of Parenteral & Enteral Nutrition2009, 33, 2, Burd RS.; Price, MR.; Whalen, TV.; The Role of Protective Antireflux Procedures in Neurologically Impaired Children: A Decision Analysis. J Pediatr Surg 2002 Mar; 37 (3): Chao,N.S.Y.; Leung,M.W.Y.; Poon,M.; Wong,B.P.Y.; Chung,K.W.; Kwok,W.K.; Liu,K.K.W. Fundoplication in children with neurological impairment: A worthwhile surgical treatment? Hong Kong J.Paediatr., 2009, 14, 3, Cheung,K.M.; Tse,H.W.; Tse,P.W.; Chan,K.H. Nissen fundoplication and gastrostomy in severely neurologically impaired children with gastroesophageal reflux. Hong Kong Med.J., 2006, 12, 4, Harrington,J.W.; Brand,D.A.; Edwards,K.S. Seizure disorder as a risk factor for gastroesophageal reflux in children with neurodevelopmental disabilities. Clin.Pediatr.(Phila), 2004, 43, 6, Kawahara,H.; Okuyama,H.; Kubota,A.; Oue,T.; Tazuke,Y.; Yagi,M.; Okada,A. Can laparoscopic antireflux surgery improve the quality of life in children with neurologic and neuromuscular handicaps?. J.Pediatr.Surg., 2004, 39, 12, Kuenzler KA. Gastric Volvulus After Laparoscopic Nissen Fundoplication With Gastrostomy. J Pediatr Surg 2003 Aug:38 (3): Partrick DA. Gastrointestinal tract feeding access and the role of fundoplication in combination with gastrostomy. Curr Opin Pediatr Jun; 19 (3):333-7 Rapid Response Report: Early Detection of Complications after gastrostomy Source: National Patient Safety Agency, NHS United Kingdom, March 2010 Sjovie,H.; Larsson,L.T.; Arnbjornsson,E. Postoperative gastrostomy site leakage correlated to the dimension of the gastrostomy button in children Gastroenterol.Insights, 2010, 2, 1, Srivastava,R.; Downey,E.C.; O'Gorman,M.; Feola,P.; Samore,M.; Holubkov,R.; Mundorff,M.; James,B.C.; Rosenbaum,P.; Young,P.C.; Dean,J.M. Impact of fundoplication versus gastrojejunal feeding tubes on mortality and in preventing aspiration pneumonia in young children with neurologic impairment who have gastroesophageal reflux disease. Pediatrics, 2009, 123, 1, VernonRoberts,Angharad; Sullivan, Peter B. Fundoplication versus post-operative medication for gastrooesophageal reflux in children with neurological impairment undergoing gastrostomy.cochrane Database of Systematic Reviews, 2009, 4 Viswanath,N.; Wong,D.; Channappa,D.; Kukkady,A.; Brown,S.; Samarakkody,U. Is prophylactic fundoplication necessary in neurologically impaired children?. Eur.J.Pediatr.Surg., 2010, 20, 4, Wales, PW.; Diamond, IR.; Dutta, S.; et al. Fundoplication and Gastrostomy Versus Image-Guided Gastrojejunal Tube for Enteral Feeding in Neurologically Impaired Children With Gastroesophageal Reflux. J Pediatr Surg 2002 Mar; 37 (3): Return to Home
15 Title: Gastrostomy Tube Placement Authors: Seattle Children s Hospital Adam Goldin Jeffrey Foti Caren Goldenberg Jocelyn Hayes Kristi Klee Jenny Kreiss Michael Leu David Suskind Date: May 2013 Gastrostomy Tube Placement Citation Retrieval Website: Example: Seattle Children s Hospital, Goldin A, Foti J, Goldenberg C, Hayes J, Klee K, Kreiss J, Leu M, Suskind D May. Gastrostomy Tube Placement Pathway. Available from: Return to Home
Malnutrition Screening Pathway v.1.1
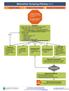 Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
Malnutrition Screening Pathway v.1.1 Approval & Citation Summary of Version Changes Explanation of Evidence Ratings Inclusion Criteria Inpatients age 1 month and older Exclusion Criteria
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary
 TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary Inclusion Criteria Age 0-17 years Gastrostomy tube insertions
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Postoperative Gastrostomy Tube Management Evidence-Based Practice Course Evidence Summary Inclusion Criteria Age 0-17 years Gastrostomy tube insertions
Clinical Pathway: TICKER Short Stay (Expected LOS 5 days) For Patients not eligible for other TICKER Clinical Pathways
 Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: TICKER Short Stay (Expected LOS 5 days) For Patients not eligible for other TICKER Clinical Pathways Notes: (1) This pathway
Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: TICKER Short Stay (Expected LOS 5 days) For Patients not eligible for other TICKER Clinical Pathways Notes: (1) This pathway
Button, Button. Where s The Button?
 Button, Button. Where s The Button? A Discussion of Gastrostomy Tubes Elizabeth Paton, RN, MSN, PNP, FAEN OBJECTIVES Discuss History of Gastrostomy Tubes in Pediatrics List Types of Gastrostomy Tubes Troubleshoot
Button, Button. Where s The Button? A Discussion of Gastrostomy Tubes Elizabeth Paton, RN, MSN, PNP, FAEN OBJECTIVES Discuss History of Gastrostomy Tubes in Pediatrics List Types of Gastrostomy Tubes Troubleshoot
Clinical Pathway: Ventricular Septal Defect (VSD) or Atrial Septal Defect (ASD) Repair
 Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: Ventricular Septal Defect (VSD) or Atrial Septal Defect (ASD) Repair Notes: (1) This pathway is a general guideline and does
Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: Ventricular Septal Defect (VSD) or Atrial Septal Defect (ASD) Repair Notes: (1) This pathway is a general guideline and does
Tube Feeding at Home A Guidebook for Patients and Caregivers
 Tube Feeding at Home A Guidebook for Patients and Caregivers This manual provides information on the following: What is Tube Feeding? How to Flush Your Feeding Tube Problems That May Occur With Tube Feeds
Tube Feeding at Home A Guidebook for Patients and Caregivers This manual provides information on the following: What is Tube Feeding? How to Flush Your Feeding Tube Problems That May Occur With Tube Feeds
Pediatric Surgery Curriculum Clinical Base Year
 Pediatric Surgery Curriculum Clinical Base Year Collaborating Faculty: Cindi Graves, MD Residency Program Director Department of Surgery Purpose and Educational Value The purpose of the Pediatric Surgery
Pediatric Surgery Curriculum Clinical Base Year Collaborating Faculty: Cindi Graves, MD Residency Program Director Department of Surgery Purpose and Educational Value The purpose of the Pediatric Surgery
PLACEMENT. Disclaimer
 1 TITLE: GUIDELINE FOR PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE Disclaimer PLACEMENT The Canadian Society of Gastroenterology Nurses and Associates (CSGNA) presents this guideline to be used as a reference
1 TITLE: GUIDELINE FOR PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE Disclaimer PLACEMENT The Canadian Society of Gastroenterology Nurses and Associates (CSGNA) presents this guideline to be used as a reference
Creating Clinical Pathways
 Creating Clinical Pathways Michael Stifelman, MD Professor and Chairman of Urology Director, Urologic Oncology & Courtney DiBona, MSN, RN-BC Nurse Manager: Urology Why create clinical pathways? Institute
Creating Clinical Pathways Michael Stifelman, MD Professor and Chairman of Urology Director, Urologic Oncology & Courtney DiBona, MSN, RN-BC Nurse Manager: Urology Why create clinical pathways? Institute
Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology
 Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology Your healthcare team recommended that you undergo gastrojejunostomy tube (GJ tube) placement. This procedure will be
Placement and Care of Your Gastrojejunostomy Tube (GJ Tube) Interventional Radiology Your healthcare team recommended that you undergo gastrojejunostomy tube (GJ tube) placement. This procedure will be
SURGICAL RESIDENT CURRICULUM FOR THE DIVISION OF GENERAL and PEDIATRIC SURGERY
 SURGICAL RESIDENT CURRICULUM FOR THE DIVISION OF GENERAL and PEDIATRIC SURGERY I. The Clinical Mission of the Division of Pediatric Surgery The clinical mission of the Division of Pediatric Surgery at
SURGICAL RESIDENT CURRICULUM FOR THE DIVISION OF GENERAL and PEDIATRIC SURGERY I. The Clinical Mission of the Division of Pediatric Surgery The clinical mission of the Division of Pediatric Surgery at
9/29/2017. Enhanced Recovery After Surgery at the University of Virginia Medical Center. Disclosures. Objectives. None
 Enhanced Recovery After Surgery at the University of Virginia Medical Center Bethany Sarosiek, RN, MSN, MPH, CNL University of Virginia Health System Charlottesville, VA ErasRN@virginia.edu Disclosures
Enhanced Recovery After Surgery at the University of Virginia Medical Center Bethany Sarosiek, RN, MSN, MPH, CNL University of Virginia Health System Charlottesville, VA ErasRN@virginia.edu Disclosures
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES
 UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
Enhanced Recovery After Surgery in OB/GYN
 Enhanced Recovery After Surgery in OB/GYN Audra Williams, MD Ashley Wright, MD University of Alabama at Birmingham Department of OB/GYN Women s Reproductive Healthcare Division Outline Brief background
Enhanced Recovery After Surgery in OB/GYN Audra Williams, MD Ashley Wright, MD University of Alabama at Birmingham Department of OB/GYN Women s Reproductive Healthcare Division Outline Brief background
DEPARTMENT OF SURGERY SECTION OF PEDIATRIC SURGERY PEDIATRIC SURGERY ROTATION (DSP)
 DEPARTMENT OF SURGERY SECTION OF PEDIATRIC SURGERY PEDIATRIC SURGERY ROTATION (DSP) C.S. Mott Children s Hospital Von Voigtlander Women s Hospital House Officer I House Officer II House Officer III Curriculum/Rotation
DEPARTMENT OF SURGERY SECTION OF PEDIATRIC SURGERY PEDIATRIC SURGERY ROTATION (DSP) C.S. Mott Children s Hospital Von Voigtlander Women s Hospital House Officer I House Officer II House Officer III Curriculum/Rotation
Care of your Radiologically Inserted Gastrostomy (RIG) Tube
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Care of your Radiologically Inserted Gastrostomy (RIG) Tube Nursing and Clinical Governance The purpose of this leaflet is
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Care of your Radiologically Inserted Gastrostomy (RIG) Tube Nursing and Clinical Governance The purpose of this leaflet is
Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure
 Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence
 CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
SCIP-Inf-2, SCIP-Inf-3, SCIP-Inf-4, SCIP-Inf- 9, SCIP-Inf-10, SCIP-VTE-1, SCIP-VTE-2 Anesthesia End Time 5
 Release Notes: Alphabetical Data Dictionary Version 3.3 Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Release Notes: Alphabetical Data Dictionary Version 3.3 Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01
 Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Trust Standard for the Assessment and Management of Physical Health Practice Guidance Note Enteral Tube Feeding Overview V01 Date Issued Planned Review PGN No: Issue 1 Aug 16 Issue 2 Nov 16 Aug 19 AMPH-PGN-02
Surgical Care, Centered on You
 General Surgery Surgical Care, Centered on You Having surgery is an important decision, and so is choosing where to have surgery. At Woman s, your surgery will be performed by experienced specialists and
General Surgery Surgical Care, Centered on You Having surgery is an important decision, and so is choosing where to have surgery. At Woman s, your surgery will be performed by experienced specialists and
Tube Feeding Status Critical Element Pathway
 Use this pathway for a resident who has a feeding tube. Review the Following in Advance to Guide Observations and Interviews: Most current comprehensive and most recent quarterly (if the comprehensive
Use this pathway for a resident who has a feeding tube. Review the Following in Advance to Guide Observations and Interviews: Most current comprehensive and most recent quarterly (if the comprehensive
TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines
 TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines DATE: 05 June 2015 CONTEXT AND POLICY ISSUES Breaking drug tablets is a common practice referred to as pill
TITLE: Pill Splitting: A Review of Clinical Effectiveness, Cost-Effectiveness, and Guidelines DATE: 05 June 2015 CONTEXT AND POLICY ISSUES Breaking drug tablets is a common practice referred to as pill
DK3M 04 (SFH CHS17) Carry Out Extended Feeding Techniques to Ensure Individuals Nutritional and Fluid Intake
 DK3M 04 (SFH CHS17) Carry Out Extended Feeding Techniques to Ensure Individuals Nutritional and Fluid Intake Overview This standard covers feeding individuals using techniques other than oral feeding.
DK3M 04 (SFH CHS17) Carry Out Extended Feeding Techniques to Ensure Individuals Nutritional and Fluid Intake Overview This standard covers feeding individuals using techniques other than oral feeding.
TITLE: Double Gloves for Prevention of Transmission of Blood Borne Pathogens to Patients: A Review of the Clinical Evidence
 TITLE: Double Gloves for Prevention of Transmission of Blood Borne Pathogens to Patients: A Review of the Clinical Evidence DATE: 27 March 2012 CONTEXT AND POLICY ISSUES As concern surrounding the risk
TITLE: Double Gloves for Prevention of Transmission of Blood Borne Pathogens to Patients: A Review of the Clinical Evidence DATE: 27 March 2012 CONTEXT AND POLICY ISSUES As concern surrounding the risk
Clinical Pathway: Tetralogy of Fallot (TOF) Repair
 Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: Tetralogy of Fallot (TOF) Repair Notes: (1) This pathway is a general guideline and variations can occur based on professional
Project TICKER Teamwork to Improve Cardiac Kids End Results Clinical Pathway: Tetralogy of Fallot (TOF) Repair Notes: (1) This pathway is a general guideline and variations can occur based on professional
Percutaneous Endoscopic Gastrostomy (PEG)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
National Priorities for Improvement:
 National Priorities for Improvement: Standardization of Performance Measures, Data Collection, and Analysis Dale W. Bratzler, DO, MPH Principal Clinical Coordinator Oklahoma Foundation Contracting for
National Priorities for Improvement: Standardization of Performance Measures, Data Collection, and Analysis Dale W. Bratzler, DO, MPH Principal Clinical Coordinator Oklahoma Foundation Contracting for
Institutional Handbook of Operating Procedures Policy
 Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
TUBE FEEDING WITH NUTRICIA CHOICE
 TUBE FEEDING WITH NUTRICIA CHOICE NURSE SUPPORT FLEXIBLE DELIVERIES OUT OF HOURS SUPPORT ENTERAL FEEDING PUMP SUPPORTING ALL YOUR TUBE FEEDING NEEDS EASY TO ORDER & PAY COMPREHENSIVE TUBE FEED PACKAGE
TUBE FEEDING WITH NUTRICIA CHOICE NURSE SUPPORT FLEXIBLE DELIVERIES OUT OF HOURS SUPPORT ENTERAL FEEDING PUMP SUPPORTING ALL YOUR TUBE FEEDING NEEDS EASY TO ORDER & PAY COMPREHENSIVE TUBE FEED PACKAGE
2/13/2018. Enhanced Recovery after Surgery (ERAS) in Gynecology
 Enhanced Recovery after Surgery (ERAS) in Gynecology J. Michael Straughn, Jr., MD Professor, Gynecologic Oncology University of Alabama at Birmingham Outline What is Enhanced Recovery after Surgery (ERAS)?
Enhanced Recovery after Surgery (ERAS) in Gynecology J. Michael Straughn, Jr., MD Professor, Gynecologic Oncology University of Alabama at Birmingham Outline What is Enhanced Recovery after Surgery (ERAS)?
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion
 Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Nursing skill mix and staffing levels for safe patient care
 EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
C. difficile Infection and C. difficile Lab ID Reporting in NHSN
 C. difficile Infection and C. difficile Lab ID Reporting in NHSN MARY ANDRUS, BA, RN, CIC Infection Preventionist Consultant Learning Objectives Review the structure and of the MDRO/CDAD Module within
C. difficile Infection and C. difficile Lab ID Reporting in NHSN MARY ANDRUS, BA, RN, CIC Infection Preventionist Consultant Learning Objectives Review the structure and of the MDRO/CDAD Module within
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta
 Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta Abstract Introduction: Day care units are playing an increasingly important role in healthcare provision,
Delayed discharges and unplanned admissions from the Day Care Unit at Mater Dei Hospital, Malta Abstract Introduction: Day care units are playing an increasingly important role in healthcare provision,
Protocol: Name of supervising ED provider: Name of RDTC Faculty: Disposition: Date: / / Time: : (military)
 RDTC TRACKING SHEET Record patient information in top right corner When completed, place in RDTC binder at A-pod Faculty desk Name: MR# Stamp OR write patient information above ED provider (i.e. faculty/pa/resident
RDTC TRACKING SHEET Record patient information in top right corner When completed, place in RDTC binder at A-pod Faculty desk Name: MR# Stamp OR write patient information above ED provider (i.e. faculty/pa/resident
QUALITY NET REPORTING
 5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER. Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow
 SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
SURGICAL RESIDENT CURRICULUM FOR NORTH CAROLINA JAYCEE BURN CENTER Residency years included: PGY1 _X PGY2 PGY3 _X PGY4 PGY5 Fellow I. Clinical Mission of the North Carolina Jaycee Burn Center The clinical
A Guide to Your Child s Hospital Stay
 A Guide to Your Child s Hospital Stay Thank you for choosing Blank Children s Hospital for your child s care. Our mission is to provide the Best Outcome, Every Patient, Every Time. As a parent or caregiver
A Guide to Your Child s Hospital Stay Thank you for choosing Blank Children s Hospital for your child s care. Our mission is to provide the Best Outcome, Every Patient, Every Time. As a parent or caregiver
3 SCIP-Inf-2, SCIP-Inf-3, SCIP-Inf-4, SCIP-Inf-9, SCIP-Inf-10, SCIP-VTE-1, SCIP-VTE-2 Anesthesia End Time
 Release Notes: Alphabetical Data Dictionary Version 3.0b Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Release Notes: Alphabetical Data Dictionary Version 3.0b Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
ABG QCDR MEASURES LIST 2017
 2017-2018 Anesthesia Business Group, LLC All Rights Reserved. ABG QCDR MEASURES LIST 2017 ** Labor Epidurals are excluded from the definition of cases in operating rooms/procedure rooms. Measure # Measure
2017-2018 Anesthesia Business Group, LLC All Rights Reserved. ABG QCDR MEASURES LIST 2017 ** Labor Epidurals are excluded from the definition of cases in operating rooms/procedure rooms. Measure # Measure
SFHCHS17 Carry out extended feeding techniques to ensure individuals nutritional and fluid intake
 Carry out extended feeding techniques to ensure individuals nutritional Overview This standard covers feeding individuals using techniques other than oral feeding. These methods include Percutaneous Endoscopic
Carry out extended feeding techniques to ensure individuals nutritional Overview This standard covers feeding individuals using techniques other than oral feeding. These methods include Percutaneous Endoscopic
1. CRITICAL CARE. Preamble. Adult and Pediatric Critical Care
 1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
1. CRITICAL CARE Complete understanding of the following paragraphs is essential to appropriate billing of the critical care fees. Members of the team billing the Critical Care Payment Schedule can not
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay
 Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
UNMH Critical Care Clinical Privileges. Name: Effective Dates: From To
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective November 17, 2016: INSTRUCTIONS: Applicant: Check off the requested box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective November 17, 2016: INSTRUCTIONS: Applicant: Check off the requested box for each privilege requested.
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #427: Post-Anesthetic Transfer of Care: Use of Checklist or Protocol for Direct Transfer of Care from Procedure Room to Intensive Care Unit (ICU) National Quality Strategy Domain: Communication
Quality ID #427: Post-Anesthetic Transfer of Care: Use of Checklist or Protocol for Direct Transfer of Care from Procedure Room to Intensive Care Unit (ICU) National Quality Strategy Domain: Communication
UNM SRMC CRITICAL CARE PRIVILEGES
 UNM SRMC INSTRUCTIONS All new applicants must meet the following requirements as approved by the UNM SRMC Board of Directors effective May 24, 2017 Applicant: Check off the "Requested" box for each privilege
UNM SRMC INSTRUCTIONS All new applicants must meet the following requirements as approved by the UNM SRMC Board of Directors effective May 24, 2017 Applicant: Check off the "Requested" box for each privilege
Best Practice Guidelines BPG 2 Enteral Feeding
 Best Practice Guidelines BPG 2 Enteral Feeding Wolverhampton Clinical Commissioning Group Best Practice Guideline BPG 2 - Enteral Feeding 1 DOCUMENT STATUS: Approved DATE ISSUED: 10 th November 2015 DATE
Best Practice Guidelines BPG 2 Enteral Feeding Wolverhampton Clinical Commissioning Group Best Practice Guideline BPG 2 - Enteral Feeding 1 DOCUMENT STATUS: Approved DATE ISSUED: 10 th November 2015 DATE
General OR-Stanford-CA-1 revised: Tuesday, February 02, 2016
 Stanford University Anesthesiology Residency Program Rotation specific goals and objectives for residents Core Curriculum for PGY 1 Surgery Residents on the Anesthesia Rotation Description: The General
Stanford University Anesthesiology Residency Program Rotation specific goals and objectives for residents Core Curriculum for PGY 1 Surgery Residents on the Anesthesia Rotation Description: The General
Policies and Procedures. Title:
 Policies and Procedures Title: PATIENT CONTROLLED ANALGESIA (PCA) LPN Additional Competency: Patient Controlled Analgesia with an Established Plan of Care RN Entry-Level Competency Authorization: [X] Former
Policies and Procedures Title: PATIENT CONTROLLED ANALGESIA (PCA) LPN Additional Competency: Patient Controlled Analgesia with an Established Plan of Care RN Entry-Level Competency Authorization: [X] Former
Surgical H&P and Consultations Daily Progress Notes and Presentations Post-Operative Notes What should I be doing throughout the day?
 Surgical H&P and Consultations Daily Progress Notes and Presentations Post-Operative Notes What should I be doing throughout the day? Surgical H&P s and Consultations For this and all other clerkships,
Surgical H&P and Consultations Daily Progress Notes and Presentations Post-Operative Notes What should I be doing throughout the day? Surgical H&P s and Consultations For this and all other clerkships,
Adult Patient Controlled Analgesia (PCA)
 Contents... 1 Policy... 1 Scope/Audience... 1 Associated Documents... 1 Statement... 2 Criteria... 2 Patient and Whanau Education... 2 Procedural Considerations... 3 Pre Administration... 3 Patient Monitoring...
Contents... 1 Policy... 1 Scope/Audience... 1 Associated Documents... 1 Statement... 2 Criteria... 2 Patient and Whanau Education... 2 Procedural Considerations... 3 Pre Administration... 3 Patient Monitoring...
CLINICAL PATHWAY. Surgical Services. Recurring Ventral Hernia
 CLINICAL PATHWAY Surgical Services Recurring Ventral Hernia Recurring Ventral Hernia Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of this Pathway 1 Pathway Contacts 1 CLINICAL PATHWAY 3
CLINICAL PATHWAY Surgical Services Recurring Ventral Hernia Recurring Ventral Hernia Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of this Pathway 1 Pathway Contacts 1 CLINICAL PATHWAY 3
You will be having surgery to remove a the distal or tail part of your pancreas.
 Distal pancreatectomy You will be having surgery to remove a the distal or tail part of your pancreas. This handout will help you learn about the surgery, how to prepare for surgery and your care after
Distal pancreatectomy You will be having surgery to remove a the distal or tail part of your pancreas. This handout will help you learn about the surgery, how to prepare for surgery and your care after
SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: POST ANESTHESIA CARE UNITS (PACU) EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: Job Title of
PS1070 SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: POST ANESTHESIA CARE UNITS (PACU) EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: Job Title of
Beth Israel Deaconess Medical Center Perioperative Services Manual. Guidelines for Perioperative Handoffs from OR to receiving units.
 Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Beth Israel Deaconess Medical Center Perioperative Services Manual Title: Guidelines for Perioperative Handoffs from OR to receiving units. Policy #: PSM 100-102A Purpose: This guideline provides a standard
Final scope for the systematic review of the clinical and cost effectiveness evidence for the prevention of ventilator-associated pneumonia (VAP)
 Final scope for the systematic review of the clinical and cost effectiveness evidence for the prevention of ventilator-associated pneumonia (VAP) Contents 1. AIM...2 2. BACKGROUND...2 3. INTERVENTIONS...3
Final scope for the systematic review of the clinical and cost effectiveness evidence for the prevention of ventilator-associated pneumonia (VAP) Contents 1. AIM...2 2. BACKGROUND...2 3. INTERVENTIONS...3
Pediatric Private Duty Nursing Qualification Assessment Background. Section 1. Section 2
 Background The Pediatric Private Duty Nursing Qualification Assessment tool is designed to accurately determine a client s need for private duty nursing hours, while considering all conditions which require
Background The Pediatric Private Duty Nursing Qualification Assessment tool is designed to accurately determine a client s need for private duty nursing hours, while considering all conditions which require
Your Hospital Stay After Iliac Crest Free Flap Surgery
 Your Hospital Stay After Iliac Crest Free Flap Surgery What to expect This handout explains what to expect during your hospital stay after your iliac crest free flap surgery. It includes where you will
Your Hospital Stay After Iliac Crest Free Flap Surgery What to expect This handout explains what to expect during your hospital stay after your iliac crest free flap surgery. It includes where you will
Long-term outcome of percutaneous endoscopic gastrostomy feeding in patients with dysphagic stroke
 Age and Ageing 998; 7: 67-676 998, British Geriatrics Society Long-term outcome of percutaneous endoscopic gastrostomy feeding in patients with dysphagic stroke ANTHONY JAMES, KAPIL KAPUR, A. BARNEY HAWTHORNE
Age and Ageing 998; 7: 67-676 998, British Geriatrics Society Long-term outcome of percutaneous endoscopic gastrostomy feeding in patients with dysphagic stroke ANTHONY JAMES, KAPIL KAPUR, A. BARNEY HAWTHORNE
Pause for PEG Best Practices in Patients with Advanced Dementia
 Pause for PEG Best Practices in Patients with Advanced Dementia Deborah Conley, MSN, APRN-CNS, GCNS-BC, FNGNA Geriatric Service Line Director Amy Hessel, MS-CCC/SPL Speech Language Pathologist Methodist
Pause for PEG Best Practices in Patients with Advanced Dementia Deborah Conley, MSN, APRN-CNS, GCNS-BC, FNGNA Geriatric Service Line Director Amy Hessel, MS-CCC/SPL Speech Language Pathologist Methodist
The Assessment of Postoperative Vital Signs: Clinical Effectiveness and Guidelines
 CADTH RAPID RESPONSE REPORT: REFERENCE LIST The Assessment of Postoperative Vital Signs: Clinical Effectiveness and Guidelines Service Line: Rapid Response Service Version: 1.0 Publication Date: February
CADTH RAPID RESPONSE REPORT: REFERENCE LIST The Assessment of Postoperative Vital Signs: Clinical Effectiveness and Guidelines Service Line: Rapid Response Service Version: 1.0 Publication Date: February
You and your gastrostomy feeding tube
 The Clatterbridge Cancer Centre NHS Foundation Trust You and your gastrostomy feeding tube Rehabilitation and Support A guide for patients and carers Contents Skin care...1 Daily tube care...2 Feeding
The Clatterbridge Cancer Centre NHS Foundation Trust You and your gastrostomy feeding tube Rehabilitation and Support A guide for patients and carers Contents Skin care...1 Daily tube care...2 Feeding
During the hospital medicine rotation, residents will focus on the following procedures as permitted by case mix:
 Educational Goals & Objectives The Inpatient Family Medicine rotation will provide the resident with an opportunity to evaluate and manage patients with common acute medical conditions. Training will focus
Educational Goals & Objectives The Inpatient Family Medicine rotation will provide the resident with an opportunity to evaluate and manage patients with common acute medical conditions. Training will focus
Based on the comprehensive assessment of a resident, the facility must ensure that:
 7. QUALITY OF CARE Each resident must receive, and the facility must provide, the necessary care and services to attain or maintain the highest practicable physical, mental and psychosocial wellbeing,
7. QUALITY OF CARE Each resident must receive, and the facility must provide, the necessary care and services to attain or maintain the highest practicable physical, mental and psychosocial wellbeing,
Strategy/Driver Prevention Strategies Action Strategies
 I. Hospital executive leadership commitment to prevention of surgical site infections 1. Establish Surgical Site Infection prevention as a strategic priority 2. Develop and implement business/strategic
I. Hospital executive leadership commitment to prevention of surgical site infections 1. Establish Surgical Site Infection prevention as a strategic priority 2. Develop and implement business/strategic
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #426: Post-Anesthetic Transfer of Care Measure: Procedure Room to a Post Anesthesia Care Unit (PACU) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL
Quality ID #426: Post-Anesthetic Transfer of Care Measure: Procedure Room to a Post Anesthesia Care Unit (PACU) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL
PRE OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS
 Before the Operating Room: PRE OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS Presenters: Anjna Melwani, MD Sonaly McClymont, MD David Rappaport, MD Sarah Denniston, MD David Pressel, MD Amy Vinson, MD
Before the Operating Room: PRE OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS Presenters: Anjna Melwani, MD Sonaly McClymont, MD David Rappaport, MD Sarah Denniston, MD David Pressel, MD Amy Vinson, MD
In recent years, the use of enteral feeding tubes has become increasingly common in the community for those unable to swallow.
 1. Introduction In recent years, the use of enteral feeding tubes has become increasingly common in the community for those unable to swallow. The most common type in use is percutaneous endoscopic gastrostomy
1. Introduction In recent years, the use of enteral feeding tubes has become increasingly common in the community for those unable to swallow. The most common type in use is percutaneous endoscopic gastrostomy
THE SUPPORTING ROLE IT PLAYS FOR THE CHILD, PARENT AND CAREGIVER
 THE WOMEN S AND CHILDREN S HOSPITAL HOME ENTERAL NUTRITION SERVICE: THE SUPPORTING ROLE IT PLAYS FOR THE CHILD, PARENT AND CAREGIVER DANA WRIGHT RN, BNg, Grad. Cert. Health (CCAFHN) Clinical Nurse - Home
THE WOMEN S AND CHILDREN S HOSPITAL HOME ENTERAL NUTRITION SERVICE: THE SUPPORTING ROLE IT PLAYS FOR THE CHILD, PARENT AND CAREGIVER DANA WRIGHT RN, BNg, Grad. Cert. Health (CCAFHN) Clinical Nurse - Home
Inguinal hernia repair integrated care pathway (ICP)
 Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
Name Ward Hosp no DOB Affix patient label Inguinal hernia repair integrated care pathway (ICP) Inclusion criteria Patients undergoing inguinal hernia repair aged under 3 months corrected gestational age
TOTAL HIP REPLACEMENT FLOW SHEET
 TOTAL HIP REPLACEMENT FLOW SHEET Before Surgery: Nothing to eat or drink after midnight the night before surgery. Make sure you have a bowel movement the day before surgery. Be sure to attend your pre-op
TOTAL HIP REPLACEMENT FLOW SHEET Before Surgery: Nothing to eat or drink after midnight the night before surgery. Make sure you have a bowel movement the day before surgery. Be sure to attend your pre-op
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee
 TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
Medical Review Criteria Skilled Nursing Facility & Subacute Care
 Medical Review Criteria Skilled Nursing Facility & Care Subject: Skilled Nursing Facility and Care Background: Skilled nursing facilities () provide facility-based skilled nursing care and related services
Medical Review Criteria Skilled Nursing Facility & Care Subject: Skilled Nursing Facility and Care Background: Skilled nursing facilities () provide facility-based skilled nursing care and related services
Post-operative "Fast-Track" pathways for lung resection. Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic
 Post-operative "Fast-Track" pathways for lung resection Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic Post-operative "Fast-Track" pathways for lung resection Dennis A. Wigle Division of Thoracic
Post-operative "Fast-Track" pathways for lung resection Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic Post-operative "Fast-Track" pathways for lung resection Dennis A. Wigle Division of Thoracic
TRAUMA AND EMERGENCY SURGERY CORE OBJECTIVES: PGY 4
 TRAUMA AND EMERGENCY SURGERY CORE OBJECTIVES: PGY 4 GOALS Through rotation on the trauma and emergency surgery service, residents shall attain the following goals: I. Patient Care A. Trauma Resuscitations
TRAUMA AND EMERGENCY SURGERY CORE OBJECTIVES: PGY 4 GOALS Through rotation on the trauma and emergency surgery service, residents shall attain the following goals: I. Patient Care A. Trauma Resuscitations
G: Surgical. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67
 G: Surgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67 Major Competency Area: G Surgical Competency: G-1 Surgical Nursing Date: June 1, 2015 G-1-1 G-1-2 G-1-3
G: Surgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67 Major Competency Area: G Surgical Competency: G-1 Surgical Nursing Date: June 1, 2015 G-1-1 G-1-2 G-1-3
Policies & Procedures
 Policies & Procedures Title: ENTERAL FEEDING TUBE WITH A STYLET: ASSISTING WITH INSERTION OF: CARE OF, REMOVAL OF Authorization [X] SHR Nursing Practice Committee ID Number: 1109 Source: Nursing Date Reaffirmed:
Policies & Procedures Title: ENTERAL FEEDING TUBE WITH A STYLET: ASSISTING WITH INSERTION OF: CARE OF, REMOVAL OF Authorization [X] SHR Nursing Practice Committee ID Number: 1109 Source: Nursing Date Reaffirmed:
ENVIRONMENT Preoperative evaluation clinic. Preoperative evaluation clinic. Preoperative evaluation clinic. clinic. clinic. Preoperative evaluation
 Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool
 Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Policy for Admission to Adult Critical Care Services
 Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
POST OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS
 After the Operating Room: POST OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS Presenters: Sonaly McClymont, MD Anjna Melwani, MD David Rappaport, MD Rebecca Rosenberg, MD Sarah Denniston, MD Moises Auron,
After the Operating Room: POST OPERATIVE MANAGEMENT FOR PEDIATRIC HOSPITALISTS Presenters: Sonaly McClymont, MD Anjna Melwani, MD David Rappaport, MD Rebecca Rosenberg, MD Sarah Denniston, MD Moises Auron,
Version 1.0 (posted Aug ) Aaron L. Leppin. Background. Introduction
 Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Clinical Development Process 2017
 InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
InterQual Clinical Development Process 2017 InterQual Overview Thousands of people in hospitals, health plans, and government agencies use InterQual evidence-based clinical decision support content to
Your Hospital Stay After Fibular Free Flap Surgery
 Your Hospital Stay After Fibular Free Flap Surgery What to expect This handout explains what to expect during your hospital stay after your fibular free flap surgery. It includes where you will stay after
Your Hospital Stay After Fibular Free Flap Surgery What to expect This handout explains what to expect during your hospital stay after your fibular free flap surgery. It includes where you will stay after
Implementing a Regional Dysphagia Management Strategy. Practical Considerations
 Implementing a Regional Dysphagia Management Strategy Practical Considerations Acknowledgements This publication, Implementing a Regional Dysphagia Management Strategy: Practical Considerations, owes its
Implementing a Regional Dysphagia Management Strategy Practical Considerations Acknowledgements This publication, Implementing a Regional Dysphagia Management Strategy: Practical Considerations, owes its
Standard methods for preparation of evidence reports
 University of Pennsylvania Health System Center for Evidence-based Practice Standard methods for preparation of evidence reports January 2018 The University of Pennsylvania Health System (UPHS) Center
University of Pennsylvania Health System Center for Evidence-based Practice Standard methods for preparation of evidence reports January 2018 The University of Pennsylvania Health System (UPHS) Center
Goals and Objectives. Assessment Methods/Tools
 CA-2 PEDIATRIC ANESTHESIA ROTATION Minneapolis Children s Hospital and Clinics (MCHC) Rotation Site Director: Dr. Chris Altman Rotation Duration: 6 weeks Introduction: In the CA-2 year residents have the
CA-2 PEDIATRIC ANESTHESIA ROTATION Minneapolis Children s Hospital and Clinics (MCHC) Rotation Site Director: Dr. Chris Altman Rotation Duration: 6 weeks Introduction: In the CA-2 year residents have the
Rapid Review Evidence Summary: Manual Double Checking August 2017
 McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
McGill University Health Centre: Nursing Research and MUHC Libraries What evidence exists that describes whether manual double checks should be performed independently or synchronously to decrease the
General Surgery Clinical Privileges
 Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE
 ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
December 16, Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC
 Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
Thoracostomy Tube Removal Procedural Pain Practice Guideline Implementation Lisa M. Ring, DNP, CPNP, AC-PC Objectives Nature and scope of the project Literature review and analysis Project methods Results
of the respiratory checklist from July1, April 30, Measures were evaluated monthly. Primary measures:
 Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
Surfactant Administration and Respiratory Care During the Golden Hour Adia Stokes MD, Bushra Saleem, MD, Melissa Oh, MD, Natalie Davis, MD and Sara Mola, MD University of Maryland Medical Center Primary
Your Hospital Stay For patients receiving treatment for head and neck cancer
 Patient Education Your Hospital Stay For patients receiving treatment for head and neck cancer This section of the Guide to Your Head and Neck Cancer Treatment explains what will happen while you are at
Patient Education Your Hospital Stay For patients receiving treatment for head and neck cancer This section of the Guide to Your Head and Neck Cancer Treatment explains what will happen while you are at
How do we know the surgical checklist is making a meaningful. impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010
 How do we know the surgical checklist is making a meaningful impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010 1 Show Me the Evidence You simply have to MEASURE! 2 Why Measure?
How do we know the surgical checklist is making a meaningful impact in surgical care? Virginia Flintoft, MSc, BN Vancouver, BC March 9, 2010 1 Show Me the Evidence You simply have to MEASURE! 2 Why Measure?
Surgical Oncology Manual: Patient Protocols: Daily Rounds:
 Surgical Oncology Manual: Patient Protocols: Daily Rounds: All inpatients must be seen by the chief resident or fellow prior to that day s OR cases. Multidisciplinary notes are to be completed for every
Surgical Oncology Manual: Patient Protocols: Daily Rounds: All inpatients must be seen by the chief resident or fellow prior to that day s OR cases. Multidisciplinary notes are to be completed for every
Care of a Freka Percutaneous Endoscopic Gastrostomy (PEG)
 Care of a Freka Percutaneous Endoscopic Gastrostomy (PEG) Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets
Care of a Freka Percutaneous Endoscopic Gastrostomy (PEG) Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets
Internal Medicine Curriculum Gastroenterology/Hepatology Rotation
 Internal Medicine Curriculum Gastroenterology/Hepatology Rotation Contact Person: Educational Purpose Gastrointestinal and hepatic disorders frequently cause patients to seek medical attention. Abdominal
Internal Medicine Curriculum Gastroenterology/Hepatology Rotation Contact Person: Educational Purpose Gastrointestinal and hepatic disorders frequently cause patients to seek medical attention. Abdominal
