Enhanced Recovery Programme Major gynaecology surgery
|
|
|
- Godfrey Harper
- 5 years ago
- Views:
Transcription
1 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Enhanced Recovery Programme Major gynaecology surgery General Surgery Department
2 When you are admitted to hospital for your surgery you will be taking part in an Enhanced Recovery Programme. This programme of care aims to help you recover quickly and safely. This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are not sure about, please ask. What is the Enhanced Recovery Programme? The aim of the programme is to get you back to full health as quickly as possible after your surgery. Research suggests the earlier you get out of bed and start eating and drinking after gynaecology surgery the better. This will speed your recovery, making it less likely that complications will develop. The programme has the following goals for a quicker and successful recovery after surgery: Reducing the stress of an operation on the body. Reducing and stopping pain or any other problems you experience after surgery. Ensuring you move around as soon as you are able, and within your normal limits. Ensure you eat and drink as soon as you are able, and within your normal limits. To ensure you benefit from all or some of the programme, we need your help and involvement. This leaflet will increase your understanding of the programme and help you to play an active role in the preparation for your surgery, and in your recovery. 2
3 Admission preparation Before your surgery it is important to look after your health, this will help you recover quicker and have fewer complications. Also, try to eat as healthily as possible and avoid putting on a lot of weight the weeks before your surgery. Ensure adequate exercise and walk whenever you can. If you are a smoker it is advisable for you to stop. Smokers are more prone to complications and chest infections after gynaecology surgery. You may wish to contact a local helpline on or if you have access to the internet log on to for help and advice in quitting smoking. It is important for you to be thinking about planning your discharge now, before you go in to hospital. When you come home from hospital you still have a lot of recovering to do and you will not be able to do everything for yourself straight away and you will tire easily. You can help yourself by arranging help and support before you come into hospital, for example: Making sure you know who will come and collect you from hospital. Please bring their contact details with you. Ask friends and relatives if they can come to stay or visit to help around the house when you get home. Arranging for a friend or relative to do some shopping for you, make extra portions of food to freeze or purchase ready meals and convenience foods that you can freeze for use in the first couple of weeks after you get home. Getting up to date on your housework before you come into hospital, this will help reduce the load when you get home. Arranging additional childcare or help with the school runs where necessary. Arranging care for your pets, if necessary. If you have any requirements that need to be put in place before you go home, or any concerns or queries, please talk to your clinical specialist nurse, key worker, pre-assessment nurse or doctor before you come into hospital. 3
4 What should I expect before my surgery? Eating and drinking It is important that you are well nourished before your surgery as this will help in the healing of your wounds; reduce the risk of infection as well as improving your general recovery. Before your surgery you would have visited the pre-assessment clinic and been asked questions about your weight, appetite and dietary intake. If you have lost weight without trying to do so or your appetite has been poor, the pre-assessment nurses will have given you some advice and written information. They may also have referred you to a dietitian and/or advised you to commence supplement drinks before your surgery. On the day before your surgery you should eat and drink as normal. In order to maximise your nutritional status we recommend you include a few extra snacks in your diet. A key aspect of your enhanced recovery programme is that you will be given a carbohydrate (sugary) drink to drink the night before your surgery and a further drink up to 2 hours before your surgery. This drink is called preload. These drinks have several benefits to your recovery. They will: Give you energy to help you recover Reduce the risk of nausea (sickness) Help your wounds to heal Reduce the risk of infection Generally aid your recovery Patients who have diabetes will be advised not to take the carbohydrate drink preload. 4
5 Admission It is usual to be admitted the day of your surgery to the Elective Surgery Unit (ESU). The ESU staff will contact you prior to your admission informing you what time to come in. When you arrive at ESU, the necessary documentation will be completed and any nursing procedures will be carried out. You will go to theatre from ESU and after your surgery you will be transferred either to the Intensive Care Unit (ICU), the Acute Dependency Unit (ADU) or directly to the main ward. Please note that your property will remain in ESU until you have returned from theatre and admitted onto a ward or unit. Therefore, it is advisable not to bring any valuables. Preparing your bowel for surgery It is sometimes necessary for the bowel to be prepared for surgery and this will depend on what operation you are due to have. Some patients may have an enema two hours before their surgery to clear the lower end of the bowel and others may not require any bowel preparation at all. This will be discussed with you in advance, prior to your admission. Preparation for surgery In order to reduce the risk of blood clots forming, you will be asked to wear below knee surgical stockings. These stockings will reduce the risk of blood clots forming in your leg veins. You will also be given a daily blood thinning injection after your surgery. Some patients will have to continue the injections for 3 4 weeks after discharge; you will be advised by the medical staff if this includes you. What can I expect after my surgery? After major gynaecology surgery some patients may be admitted to the Intensive Care Unit (ICU) or Acute Dependency Unit (ADU) to allow close post-operative monitoring. There is a higher staff ratio on these units but they are mixed sex units. We will do all we can to respect your privacy and dignity at all times, but recognise this may not be sufficient for everyone due to the mixed-sex nature of these units. Please let a member of staff know if we can do more. 5
6 Monitoring During your recovery the nurses will check you regularly because we will need to monitor: Blood pressure, pulse, respiratory rate and temperature Fluid and dietary intake Urine output When your bowels or stoma starts working Level of pain Number of times you have sat out of bed The number of walks you have taken Pain Control It is important that your pain is well controlled so that you can deep breathe, walk about, feel relaxed and sleep well. You may have a tube in your back (an epidural) which gives you continuous pain relief and is usually removed two days after surgery. Alternatively, you may have a pump connected to a button, which you can press to administer pain relief directly into your drip (Patient Controlled Analgesia PCA). This will usually be stopped one to two days after your surgery. You will also be given painkillers by mouth. Sickness Sometimes after surgery a person may feel sick or be sick. This is usually caused by the anaesthetic drugs, but you will be given medicine during surgery to help reduce this. It is important to relieve sickness in order to allow you to feel better, so that you can eat and drink normally which will aid your recovery. If you do feel sick following surgery, please speak to your nurse who will be able to provide medicine to help you. Tubes and drips During your surgery a tube (catheter) will be placed in your bladder so that we can check that your kidneys are working well and producing urine. This will be removed as soon as possible, usually within 48 hours after your surgery. You will have a drip in your arm and fluid will be given through this to ensure you get enough fluid and not become dehydrated. This should be removed once you are drinking. 6
7 Occasionally, following surgery you may have a wound drain; this is a plastic tube coming from your wound into a bottle or bag to remove any excess fluid from your wound site. Eating and drinking A few hours after your surgery, you will be able to start drinking and, if you wish eating. It is important that you eat after your surgery and we recommend you start with light meals and snacks. Your body needs the nourishment to help heal your wounds, reduce the risk of infection and help your recovery generally. We would also like you to drink at least 2 litres of fluid each day. Mobility and exercise The quicker you begin to start moving around, the quicker you may leave hospital. Your recovery starts immediately after your surgery and you should aim to start these exercises straight away after your surgery every hour that you are awake. Deep breathing exercises Take a slow deep breath in through your nose filling the very bottom of your lungs. Slowly breathe out through your mouth and relax. This should be done about three times an hour and helps reduce the risk of a chest infection. Once you have been back from surgery for more than four hours, the nursing staff will sit you fully up in the bed ( cardiac chair position). This allows your body to get used to being upright, and prepare your body for getting up and mobilising on the first morning after your surgery. On the morning after your surgery you will be expected to sit out of bed and mobilise with the assistance of the physiotherapists/ nursing staff. The mobilisation is repeated in the afternoon. You are expected to sit out for about two hours at a time on the first day. The sitting out and mobilisation is expected to progress and increase over the post-operative period. Being out of bed in a more upright position and by walking regularly improves lung function and reduces the risk of developing a chest infection. It also helps in making you feel more positive about your recovery. 7
8 Important discharge information When you leave hospital Complications do not happen very often but it is important that you know what to look out for. During the first two weeks after surgery if you are worried about any of the following please phone the telephone numbers on this leaflet. If you cannot contact the people listed then ring your GP. In order to reduce the risk of clots forming, some patients will require daily injections of Dalteparin, a blood thinning injection for up to 3 4 weeks after discharge from hospital. You will be taught how to inject the Dalteparin yourself; if you feel you will be unable to do this, please try and identify someone who can do this for you, e.g. a relative or a friend. Abdominal pain After surgery it is normal to experience some abdominal discomfort from the wound, this will gradually improve over several weeks. You should continue taking the pain relieving drugs, which have been prescribed for you at the hospital, until you feel comfortable. If you need further supplies or your pain is not adequately controlled you should see your GP. If you have severe pain lasting for more than two hours or have a fever and feel generally unwell within two weeks of your operation date, you should contact us on the telephone numbers provided. After two weeks you should speak to your GP if you have any concerns or problems. Your wound It is normal for your wound to still be slightly red and uncomfortable during the first one to two weeks. Please let us know by telephone if your wounds become inflamed, painful or swollen or to start to discharge fluid. Vaginal bleeding You should expect slight bleeding or discharge form your vagina, sanitary pads are advised BUT no tampons. Please contact a member of the health care team if the bleeding becomes heavy. 8
9 When can I return to normal activities? For the first two weeks at home you should rest and relax, but it is also important to continue to do the exercises you did in hospital. Go for a walk each day and gradually increase the amount you are doing. Regular exercise should help you to return to normal activities as soon as possible. Six to eight weeks after your operation you should be back to your normal level of activity. Do not do any heavy lifting until six weeks following surgery and avoid standing for long periods of time. Common sense will guide your exercise and rehabilitation. If your wound is uncomfortable, go easy with your exercise. Once your wound is pain free, you can undertake most activities. Work You should be able to return to work four to six weeks after your surgery depending on the type of job you do. A member of your health care team or your GP will be able to advise you. Driving You should not drive until you are confident that you can drive safely. A good indicator for this is when you have got back to most of your normal activities. Usually this will be within two to four weeks of surgery. It is important that any pain has resolved sufficiently to enable you to perform an emergency stop and turn the wheel quickly. Hobbies/activities In general, you can take up your hobbies as soon as possible after your surgery. This will benefit your convalescence. However, do not do anything that causes significant pain or involves heavy lifting avoid these activities for the first six weeks after your surgery. 9
10 Next appointment After being discharged from hospital you will be sent an appointment to meet a surgical doctor or clinical specialist nurse in clinic. This will usually be between 3 to 8 weeks after your surgery. At the clinic visit the doctor or nurse will discuss any histology test results from the laboratory and whether or not any further treatment will be recommended for you. Make sure that you write down any questions or concerns that you might have beforehand on a piece of paper and take this with you because it can be very frustrating if important questions are forgotten when you see the doctor. After they have seen you, your surgical doctor or nurse will write a letter about you to your GP so that they can continue with your medical care in the community. How can I meet the Enhanced recovery goals? Your daily diary To meet the programme goals, we would like you to complete a diary, which records whether the goals are being met. These will begin a few days before your operation, and with your help, will ensure you have a quicker and problem free recovery. You will need to complete the following sections, which start before your surgery and continue until you are discharged. We expect you to be discharged around 1 2 days after your surgery if you have robotic or laparoscopic keyhole surgery and 4 7 days if you have had open surgery. Each day that you are on a ward, please complete your personal activity plan. If you didn t achieve an activity there is space for you to document why not and also for other thoughts etc, which you may wish to write down. 10
11 The night before surgery You will be contacted by a member of staff from the hospital letting you know what time you will be admitted for your surgery. If you are not diabetic, they will also tell you what time to take your carbohydrate preload drink on the day of your surgery, this is important to ensure you gain the most benefits from this drink. All patients will have been informed if they need to take any bowel preparation the day before surgery. Please tick as appropriate: Carbohydrate Preload drink By 9pm: 2 sachets of preload mixed in with 800mls of water I am diabetic no Carbohydrate Preload drink Day of surgery If your surgery is scheduled for the morning you should have nothing to eat or drink after 2am, but you may have a small amount of water and your carbohydrate preload drink, up to 2 hours before your operation 1 sachet of preload mixed in 400mls of water, to be finished by 6am. If your surgery is scheduled for the afternoon you should have a light breakfast before 6.30am, and then have nothing except a small amount of water and your carbohydrate preload drink up to 2 hours before your operation 1 sachet of preload mixed in 400mls of water, to be finished by 10.30am. Bowel preparation (You will have been informed what you will need) None required Enema on admission Carbohydrate Preload drink If your surgery is in the morning please drink by 6am If your surgery is in the afternoon please drink by am I am diabetic no Carbohydrate Preload drink 11
12 Evening of surgery (Day 0) Date: Have you? Done your deep breathing exercises every waking hour Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat up in cardiac chair position Started drinking Eaten supper What has been your pain level today? Please indicate on the scale below: Initial when achieved (No pain) (Excruciating pain) Comments/questions 12
13 First day (Day 1) after surgery Date: Have you? Done your deep breathing exercises every waking hour Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat out of bed for 2 hours in the morning Sat out of bed for 2 hours in the afternoon Walked this morning Walked this afternoon Discussed your discharge plans with your nurse, if had robotic or laparoscopic surgery Eaten breakfast Eaten lunch Eaten supper Eaten some snacks between meals (ask your nurse for something from the kitchen) What has been your pain level today? Please indicate on the scale below: Initial when achieved (No pain) (Excruciating pain) Comments/questions 13
14 Day 2 Date: Have you? Done your deep breathing exercises every waking hour Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat out of bed in the morning for 3 hours Sat out of bed in the afternoon for 3 hours Sat out of bed in the evening for 2 hours Walked this morning Walked this afternoon Walked this evening Discussed your discharge plans with your nurse Eaten breakfast Eaten lunch Eaten supper Eaten some snacks between meals (ask your nurse for something from the kitchen) What has been your pain level today? Please indicate on the scale below: Initial when achieved (No pain) (Excruciating pain) Comments/questions 14
15 Day 3 Date: Have you? Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat out of bed in the morning for 3 hours Sat out of bed in the afternoon for 3 hours Sat out of bed in the evening for 2 hours Walked this morning Walked this afternoon (twice) Walked this evening Discussed your discharge plans with your nurse Made transport arrangements for getting home on discharge Eaten breakfast Eaten lunch Eaten supper Eaten some snacks between meals (ask your nurse for something from the kitchen) Initial when achieved Comments/questions 15
16 Day 4 Date: Have you? Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat out of bed in the morning for 3 hours Sat out of bed in the afternoon for 3 hours Sat out of bed in the evening for 2 hours Walked this morning Walked this afternoon (twice) Walked this evening Discussed your discharge plans with your nurse Made transport arrangements for getting home on discharge Eaten breakfast Eaten lunch Eaten supper Eaten some snacks between meals (ask your nurse for something from the kitchen) Initial when achieved Comments/questions 16
17 Day 5 Date: Have you? Changed your position at least every two hours to include lying tilted on your side to ensure you have relieved the pressure on your bottom Told the nurse if you have pain or nausea Sat out of bed in the morning for 3 hours Sat out of bed in the afternoon for 3 hours Sat out of bed in the evening for 2 hours Walked at least 60m Walked at least 60m Walked at least 60m Walked at least 60m Discussed your discharge plans with your nurse Made transport arrangements for getting home on discharge Eaten breakfast Eaten lunch Eaten supper Eaten some snacks between meals (ask your nurse for something from the kitchen) Initial when achieved Comments/questions 17
18 Notes & questions You may think of further questions to ask about your treatment and it is a good idea to jot these down as you think of them you could use the space below. This will help you when you next visit the hospital or your GP. References
19 Please help us to improve our care for future patients We are always trying to improve the service for future patients and your experience and opinions are appreciated, and will help us with audit and research. If you could complete the following 4 questions and bring this booklet with you to your surgical clinic follow up appointment and give your questionnaire answers to the clinic doctor or nurse to file in your medical notes. Thank you. Q1. Is there anything that we got you to do that you didn t think was necessary? Q2. Is there anything that made you feel unhappy about your patient experience? Include the bad bits or low points for you on your patient journey from your initial GP visit to your surgical follow up appointment after your operation. Q3. Is there anything that made you feel good about your experience? Include the best bits or high points for you on your patient journey from your initial GP visit to your surgical follow-up appointment after your surgery. Q4. Do you have any recommendations for how we can improve patient experience? 19
20 Contact details Important telephone numbers: Compton Ward Telephone: ext 4941 Pre-assessment Telephone: ext 4268 Royal Surrey County Hospital (RSCH) NHS Foundation Trust fully subscribes to the National Patient Safety Agency (NPSA) Being Open best practice framework, November PALS and Advocacy contact details Contact details of independent advocacy services can be provided by our Patient Advice and Liaison Service (PALS) who are located in far left corner as you enter the main reception area. PALS are also your first point of contact for health related issues, questions or concerns surrounding RSCH patient services. Telephone: Opening hours: 9.00am 4.00pm, Monday to Friday If you would like information documents in large print, on tape or in another language or form please contact PALS. Past review date: April 2016 Future review date: April 2019 Author: Angie Bates PIN a Royal Surrey County Hospital NHS Foundation Trust 2016
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet
 Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
Enhanced recovery after laparoscopic surgery (ERALS) programme. Patient information and advice
 Enhanced recovery after laparoscopic surgery (ERALS) programme Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to
Enhanced recovery after laparoscopic surgery (ERALS) programme Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet
 Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy. Information For Patients
 Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy Information For Patients 2 This information leaflet aims to help you understand the Enhanced Recovery Programme
Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy Information For Patients 2 This information leaflet aims to help you understand the Enhanced Recovery Programme
Laparoscopic (keyhole) hysterectomy: The enhanced recovery programme
 INFORMATION FOR PATIENTS Laparoscopic (keyhole) hysterectomy: The enhanced recovery programme A hysterectomy means removal of the womb. The fallopian tubes and ovaries can be removed at the same time if
INFORMATION FOR PATIENTS Laparoscopic (keyhole) hysterectomy: The enhanced recovery programme A hysterectomy means removal of the womb. The fallopian tubes and ovaries can be removed at the same time if
Elective Colorectal Surgery Enhanced Recovery Patient Diary
 How can I help reduce healthcare associated infections? Infection control is important to the well-being of our patients and for that reason we have infection control procedures in place. Keeping your
How can I help reduce healthcare associated infections? Infection control is important to the well-being of our patients and for that reason we have infection control procedures in place. Keeping your
Urology Enhanced Recovery Programme: Radical Cystectomy. Patient Information
 Urology Enhanced Recovery Programme: Radical Cystectomy Patient Information 2 This information leaflet aims to help you understand the Enhanced Recovery Programme and how you can play an active role in
Urology Enhanced Recovery Programme: Radical Cystectomy Patient Information 2 This information leaflet aims to help you understand the Enhanced Recovery Programme and how you can play an active role in
Enhanced Recovery Programme
 Enhanced Recovery Programme Page 14 Contact details South Tyneside NHS Foundation Trust Harton Lane South Shields Tyne and Wear NE34 0PL For advice please contact ward 1 on 4041001 Or ward 3 on 0191 4041003.
Enhanced Recovery Programme Page 14 Contact details South Tyneside NHS Foundation Trust Harton Lane South Shields Tyne and Wear NE34 0PL For advice please contact ward 1 on 4041001 Or ward 3 on 0191 4041003.
Enhanced Recovery Programme for Nephrectomy (Kidney Removal)
 Enhanced Recovery Programme for Nephrectomy (Kidney Removal) This information leaflet will explain what will happen when you come to the hospital for your operation. The enhanced Recovery Programme is
Enhanced Recovery Programme for Nephrectomy (Kidney Removal) This information leaflet will explain what will happen when you come to the hospital for your operation. The enhanced Recovery Programme is
Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients
 Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients Welcome to the pancreaticoduodenectomy enhanced recovery programme (PD ERP). The aim of the programme is for you to
Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients Welcome to the pancreaticoduodenectomy enhanced recovery programme (PD ERP). The aim of the programme is for you to
Radical cystectomy enhanced recovery plan. Information for patients
 Radical cystectomy enhanced recovery plan Information for patients Your doctor has recommended surgery to remove your bladder (radical cystectomy). This booklet is designed to explain the operation and
Radical cystectomy enhanced recovery plan Information for patients Your doctor has recommended surgery to remove your bladder (radical cystectomy). This booklet is designed to explain the operation and
Colorectal Surgery Enhanced Recovery Programme Preoperative Information Useful information Care
 Colorectal Surgery Enhanced Recovery Programme Preoperative Information Useful information Name:... Consultant:... Date of Surgery:... Opera on:... WPR40870 April 2014 Review date by: March 2016 Explaining
Colorectal Surgery Enhanced Recovery Programme Preoperative Information Useful information Name:... Consultant:... Date of Surgery:... Opera on:... WPR40870 April 2014 Review date by: March 2016 Explaining
Laparoscopic Radical Nephrectomy
 Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Enhanced recovery programme
 Enhanced recovery programme Gynaecological surgery Information for patients Gynaecology The aim of this leaflet is to provide you and your family with an understanding of enhanced recovery. This will prepare
Enhanced recovery programme Gynaecological surgery Information for patients Gynaecology The aim of this leaflet is to provide you and your family with an understanding of enhanced recovery. This will prepare
Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice
 Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to go home
Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to go home
Bowel Surgery Hartmann s Procedure Your operation explained
 Bowel Surgery Hartmann s Procedure Your operation explained Introduction This information is for people considering having a Hartmann s Procedure operation. It explains what is involved and some possible
Bowel Surgery Hartmann s Procedure Your operation explained Introduction This information is for people considering having a Hartmann s Procedure operation. It explains what is involved and some possible
Endometrial Cancer. Information for patients. Gynaecology Department. Feedback
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
THE ROY CASTLE LUNG CANCER FOUNDATION
 Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Patient Information Leaflet
 Patient Information Leaflet Large Bowel Resection What is the large bowel? The large bowel (also called the large intestines or colon) is the last part of the intestines. The food we eat travels from the
Patient Information Leaflet Large Bowel Resection What is the large bowel? The large bowel (also called the large intestines or colon) is the last part of the intestines. The food we eat travels from the
Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt
 Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Percutaneous Endoscopic Gastrostomy (PEG)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient Diary. Enhanced Recovery After Surgery (ERAS) Total Knee Replacement. Helping patients get better sooner after surgery.
 Contact numbers If you need any support or advice before or after surgery please do not hesitate to call us. Claire Ward enhanced recovery nurse (Monday Friday 8-4) 07816448518 Ward 12B 01494426398 How
Contact numbers If you need any support or advice before or after surgery please do not hesitate to call us. Claire Ward enhanced recovery nurse (Monday Friday 8-4) 07816448518 Ward 12B 01494426398 How
Bowel Surgery Panproctocolectomy Your operation explained
 Bowel Surgery Panproctocolectomy Your operation explained Introduction This information is for people considering having a Panproctocolectomy operation. It explains what is involved and some possible problems
Bowel Surgery Panproctocolectomy Your operation explained Introduction This information is for people considering having a Panproctocolectomy operation. It explains what is involved and some possible problems
The Gynaecology Ward, The Women s Centre. Minor Surgery. Your nursing care, recovery, and getting back to normal
 The Gynaecology Ward, The Women s Centre Minor Surgery Your nursing care, recovery, and getting back to normal Contents Admission 3 Medicines 3 Visiting Hours 3 Patientline 3 Preparation for your operation
The Gynaecology Ward, The Women s Centre Minor Surgery Your nursing care, recovery, and getting back to normal Contents Admission 3 Medicines 3 Visiting Hours 3 Patientline 3 Preparation for your operation
Partial glossectomy. Your operation explained. Information for patients Head and Neck Centre
 Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Enhanced recovery after bowel surgery
 Patient information - Bowel Pre-operative Surgery Enhanced Assessment Recovery - WLE Enhanced recovery after bowel surgery Introduction This leaflet will explain what will happen when you come to the hospital
Patient information - Bowel Pre-operative Surgery Enhanced Assessment Recovery - WLE Enhanced recovery after bowel surgery Introduction This leaflet will explain what will happen when you come to the hospital
Abdomino-perineal Resection/Excision of the Rectum
 Abdomino-perineal Resection/Excision of the Rectum What is an Abdomino-perineal Resection/Excision of Rectum? An Abdomino-perineal Resection/Excision of Rectum is the surgical removal of part of the large
Abdomino-perineal Resection/Excision of the Rectum What is an Abdomino-perineal Resection/Excision of Rectum? An Abdomino-perineal Resection/Excision of Rectum is the surgical removal of part of the large
Patient information. Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5
 Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
Nephrectomy (kidney removal): information and advice for patients on the enhanced recovery programme
 Patient information Nephrectomy (kidney removal): information and advice for patients on the enhanced recovery programme This leaflet contains information on: Introduction and reasons for surgery Types
Patient information Nephrectomy (kidney removal): information and advice for patients on the enhanced recovery programme This leaflet contains information on: Introduction and reasons for surgery Types
Patient Diary. Vascular Surgery Enhanced Recovery Programme
 2-3 days following discharge, someone from the vascular team will contact you at home. If you have any problems please do not hesitate to contact the ward. We are here to help. Please contact us on the
2-3 days following discharge, someone from the vascular team will contact you at home. If you have any problems please do not hesitate to contact the ward. We are here to help. Please contact us on the
Enhanced recovery programme
 Enhanced recovery programme Colorectal surgery Information for patients Colorectal Surgery Please bring this booklet with you to your Pre-operative Assessment appointment; when you are admitted to hospital
Enhanced recovery programme Colorectal surgery Information for patients Colorectal Surgery Please bring this booklet with you to your Pre-operative Assessment appointment; when you are admitted to hospital
A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum.
 Total Colectomy What is a Total Colectomy? A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum. Before an ileostomy
Total Colectomy What is a Total Colectomy? A Total Colectomy is the surgical removal of the entire colon (last part of the intestine/gut). It does not involve the removal of the rectum. Before an ileostomy
Preparing for Thoracic Surgery and Recovery
 Division of Thoracic Surgery Preparing for Thoracic Surgery and Recovery A Guide for Patients and Families Brigham And Women s/faulkner Hospitals Important Phone Numbers Important Phone Numbers BWH NUMBERS
Division of Thoracic Surgery Preparing for Thoracic Surgery and Recovery A Guide for Patients and Families Brigham And Women s/faulkner Hospitals Important Phone Numbers Important Phone Numbers BWH NUMBERS
Laparoscopic partial nephrectomy
 Laparoscopic partial nephrectomy This leaflet is written to give you information and answer questions you may have about your surgery. If you have any further questions, please speak to your doctor or
Laparoscopic partial nephrectomy This leaflet is written to give you information and answer questions you may have about your surgery. If you have any further questions, please speak to your doctor or
Having an open partial nephrectomy
 Having an open partial nephrectomy The aim of this information sheet is to help answer some of the questions you may have about having part of your kidney removed using conventional open surgery this is
Having an open partial nephrectomy The aim of this information sheet is to help answer some of the questions you may have about having part of your kidney removed using conventional open surgery this is
Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients
 Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
ANTERIOR RESECTION WHAT ARE THE BENEFITS OF HAVING AN ANTERIOR RESECTION?
 WHAT IS AN ANTERIOR RESECTION? ANTERIOR RESECTION This is an operation that is designed to remove part of your lower large bowel and then join the bowel ends back together again. This is called an anastamosis.
WHAT IS AN ANTERIOR RESECTION? ANTERIOR RESECTION This is an operation that is designed to remove part of your lower large bowel and then join the bowel ends back together again. This is called an anastamosis.
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Inferior Vena Cava (IVC) Filter Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
RIGHT HEMICOLECTOMY. Patient information Leaflet
 RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
You will be having surgery to remove a the distal or tail part of your pancreas.
 Distal pancreatectomy You will be having surgery to remove a the distal or tail part of your pancreas. This handout will help you learn about the surgery, how to prepare for surgery and your care after
Distal pancreatectomy You will be having surgery to remove a the distal or tail part of your pancreas. This handout will help you learn about the surgery, how to prepare for surgery and your care after
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Patient Information Varicose Vein Surgery Dr Marek Garbowski. Varicose Veins
 Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
Mediastinal Venogram and Stent Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient copy. Periurethral bulking agent for stress urinary incontinence. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay
 Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
Surgical Weight Loss at Eastern Maine Medical Center Your Inpatient Nursing Stay Dear Prospective Patient: I have recently been informed that you are considering weight loss surgery at EMMC. As you know
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Helping you to get better sooner after surgery
 Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced to provide
Guidelines for patients undergoing surgery as part of an Enhanced Recovery Programme (ERP) Helping you to get better sooner after surgery June 2012 Foreword These guidelines have been produced to provide
Enhanced Recovery Programme
 Thoracic surgery Enhanced Recovery Programme Information for patients Your Road to Recovery Choose the fast lane. page 2 What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Thoracic surgery Enhanced Recovery Programme Information for patients Your Road to Recovery Choose the fast lane. page 2 What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Mediastinal Venogram and Stent Insertion
 Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients
 Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
CONSENT FORM UROLOGICAL SURGERY
 CONSENT FORM for UROLOGICAL SURGERY (Designed in compliance with consent form 1) PATIENT AGREEMENT TO INVESTIGATION OR TREATMENT Patient Details or pre-printed label Patient s NHS Number or Hospital number
CONSENT FORM for UROLOGICAL SURGERY (Designed in compliance with consent form 1) PATIENT AGREEMENT TO INVESTIGATION OR TREATMENT Patient Details or pre-printed label Patient s NHS Number or Hospital number
Ovarian Tumor Reduction Surgery
 PATIENT EDUCATION patienteducation.osumc.edu Information About Your Your doctor found a mass in your pelvic area. Surgery is used to remove the pelvic mass and to find out if the tissue is benign (not
PATIENT EDUCATION patienteducation.osumc.edu Information About Your Your doctor found a mass in your pelvic area. Surgery is used to remove the pelvic mass and to find out if the tissue is benign (not
Your anaesthetic for a broken hip
 Your anaesthetic for a broken hip Information to help patients, relatives and carers prepare for an anaesthetic for a broken hip First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what
Your anaesthetic for a broken hip Information to help patients, relatives and carers prepare for an anaesthetic for a broken hip First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what
Enhanced Recovery after Surgery ERAS DRAFT. Hairmyres Hospital. Colorectal Surgery. Please bring this booklet with you for your admission to hospital
 Enhanced Recovery after Surgery ERAS Hairmyres Hospital Colorectal Surgery Please bring this booklet with you for your admission to hospital CONTENTS Enhanced Recovery After surgery (ERAS) 1 Diseases of
Enhanced Recovery after Surgery ERAS Hairmyres Hospital Colorectal Surgery Please bring this booklet with you for your admission to hospital CONTENTS Enhanced Recovery After surgery (ERAS) 1 Diseases of
Having an open radical nephrectomy
 Having an open radical nephrectomy Your doctor has recommended that you have a nephrectomy an operation to remove your kidney. This leaflet aims to answer your questions and explains the benefits, risks
Having an open radical nephrectomy Your doctor has recommended that you have a nephrectomy an operation to remove your kidney. This leaflet aims to answer your questions and explains the benefits, risks
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Colonoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Tenckhoff Catheter Insertion
 Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
Surgical Treatment for Cancer of the Oesophagus
 Oxford Oesophagogastric Centre Surgical Treatment for Cancer of the Oesophagus Information for patients This leaflet gives you information about your planned operation, possible risks and complications,
Oxford Oesophagogastric Centre Surgical Treatment for Cancer of the Oesophagus Information for patients This leaflet gives you information about your planned operation, possible risks and complications,
Enhanced recovery programme in head and neck Patient information
 Enhanced recovery programme in head and neck Patient information What is enhanced recovery programme? The Enhanced Recovery Programme (ERP) is a way of making sure that you receive the best preparation
Enhanced recovery programme in head and neck Patient information What is enhanced recovery programme? The Enhanced Recovery Programme (ERP) is a way of making sure that you receive the best preparation
Excision of Submandibular Gland
 Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Non-cancer related bilateral mastectomy pre-operative information sheet
 Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
What is a Mitrofanoff?
 What is a Mitrofanoff? Mitrofanoff is a surgery to make a new pathway from the bladder to the outside of the body. This pathway is used to drain urine from the bladder with a catheter. This may be easier
What is a Mitrofanoff? Mitrofanoff is a surgery to make a new pathway from the bladder to the outside of the body. This pathway is used to drain urine from the bladder with a catheter. This may be easier
Cardio Oesophagectomy
 Cardio Oesophagectomy Information for patients Excellent Care with Compassion What is a Cardio - Oesophagectomy? It is the removal of the oesophagus (gullet) where the cancer is situated. Part of the stomach
Cardio Oesophagectomy Information for patients Excellent Care with Compassion What is a Cardio - Oesophagectomy? It is the removal of the oesophagus (gullet) where the cancer is situated. Part of the stomach
General advice for going home after breast surgery
 General advice for going home after breast surgery Introduction Recovery after surgery involves healing, both physically and emotionally, and the time this takes varies from person to person. There is
General advice for going home after breast surgery Introduction Recovery after surgery involves healing, both physically and emotionally, and the time this takes varies from person to person. There is
You have been admitted with a hip fracture
 Hip fracture: Information for patients and relatives You have been admitted with a hip fracture This booklet has been designed by health professionals to provide you and your relatives with the information
Hip fracture: Information for patients and relatives You have been admitted with a hip fracture This booklet has been designed by health professionals to provide you and your relatives with the information
Laparoscopic nephrectomy surgery
 Laparoscopic nephrectomy surgery This leaflet explains more about laparoscopic nephrectomy including the benefits, risks and any alternatives, and what you can expect when your child comes in to hospital
Laparoscopic nephrectomy surgery This leaflet explains more about laparoscopic nephrectomy including the benefits, risks and any alternatives, and what you can expect when your child comes in to hospital
Having an endoscopic retrograde cholangio-pancreatograph (ERCP)
 Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Laparoscopic Radical Prostatectomy
 To learn about prostatectomy surgery, you will need to know what these words mean: The prostate is the sexual gland that makes a fluid that helps sperm move. It surrounds the urethra at the neck of the
To learn about prostatectomy surgery, you will need to know what these words mean: The prostate is the sexual gland that makes a fluid that helps sperm move. It surrounds the urethra at the neck of the
Hip fracture - DHS. Your broken hip joint - some information
 Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
Page 1 Hip Fracture - DHS Your broken hip joint - some information These notes give a guide to your stay in hospital. They also give an idea about what it will be like afterwards. They do not cover everything.
The operation will take several hours and you will stay in the recovery room until you are ready to return to the ward.
 This booklet is designed to give you information about having a free flap following a lower limb injury. We hope it will answer some of the questions that you, or those who care for you, may have at this
This booklet is designed to give you information about having a free flap following a lower limb injury. We hope it will answer some of the questions that you, or those who care for you, may have at this
Your Guide To Spine Surgery
 Your Guide To Spine Surgery Your Guide To Spine Surgery C O N T E N T S Foreword 2 Introduction 3 The Spine 4 Preparation before Surgery 5 Day of Surgery 7 After Surgery 9 Medical and Nursing Care in the
Your Guide To Spine Surgery Your Guide To Spine Surgery C O N T E N T S Foreword 2 Introduction 3 The Spine 4 Preparation before Surgery 5 Day of Surgery 7 After Surgery 9 Medical and Nursing Care in the
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients
 Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Top copy accepted by patient: yes/no (please ring)
 Consent Form 3 Patient / Parental agreement to investigation or treatment Procedures where consciousness not impaired Name of proposed procedure or course of treatment Hospital NHS Surname no: no: OUTPATIENT
Consent Form 3 Patient / Parental agreement to investigation or treatment Procedures where consciousness not impaired Name of proposed procedure or course of treatment Hospital NHS Surname no: no: OUTPATIENT
Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube Nursing and Clinical Governance The purpose of this leaflet
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube Nursing and Clinical Governance The purpose of this leaflet
INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY
 St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Advance Care Plan. Supportive & Palliative Care Team
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Advance Care Plan Supportive & Palliative Care Team Advance Care Plan A non-legally binding document to record your preferences
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Advance Care Plan Supportive & Palliative Care Team Advance Care Plan A non-legally binding document to record your preferences
PATIENT INFORMATION Anterior Resection
 PATIENT INFORMATION Anterior Resection Introduction/Procedure This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common complications
PATIENT INFORMATION Anterior Resection Introduction/Procedure This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common complications
LAPAROSCOPIC SIMPLE REMOVAL OF THE KIDNEY
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Surgery for Pneumothorax
 Oxford University Hospitals NHS Trust Thoracic Surgery Surgery for Pneumothorax Information for patients Welcome to the Oxford Heart and Lung Centre The information in this booklet will help to prepare
Oxford University Hospitals NHS Trust Thoracic Surgery Surgery for Pneumothorax Information for patients Welcome to the Oxford Heart and Lung Centre The information in this booklet will help to prepare
Having an operation. Patient information factsheet
 Having an operation Patient information factsheet The purpose of this factsheet This factsheet contains important information to prepare you for your operation at the Whittington Hospital. All patients
Having an operation Patient information factsheet The purpose of this factsheet This factsheet contains important information to prepare you for your operation at the Whittington Hospital. All patients
Recovering from a hip fracture following an accident
 South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
Abdominal Surgery. Beyond Medicine. What to Expect While You Are in the Hospital. ilearning about your health
 ilearning about your health Abdominal Surgery What to Expect While You Are in the Hospital www.cpmc.org/learning Beyond Medicine. Table of Contents On the Day of Your Surgery...3 Your Nursing Care...3
ilearning about your health Abdominal Surgery What to Expect While You Are in the Hospital www.cpmc.org/learning Beyond Medicine. Table of Contents On the Day of Your Surgery...3 Your Nursing Care...3
Parent/Carer Information Leaflet
 Circumcision Children s Ward Parent/Carer Information Leaflet Introduction Your doctor has recommended that your son has a circumcision. This means that your son will have the foreskin removed from his
Circumcision Children s Ward Parent/Carer Information Leaflet Introduction Your doctor has recommended that your son has a circumcision. This means that your son will have the foreskin removed from his
Discharge Advice Following Breast Reconstructive Surgery
 Oxford University Hospitals NHS Trust Discharge Advice Following Breast Reconstructive Surgery Information for patients This leaflet contains answers to some of the questions people most often ask when
Oxford University Hospitals NHS Trust Discharge Advice Following Breast Reconstructive Surgery Information for patients This leaflet contains answers to some of the questions people most often ask when
About your peritoneal dialysis catheter. Information for patients Sheffield Kidney Institute (Renal Unit)
 About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
About your peritoneal dialysis catheter Information for patients Sheffield Kidney Institute (Renal Unit) Introduction You will have discussed with your doctor that your kidney condition means that you
Preventing hospital-acquired blood clots
 Preventing hospital-acquired blood clots Haematology Department Patient information leaflet This leaflet explains more about blood clots, which can form after illness and surgery. What are hospital-acquired
Preventing hospital-acquired blood clots Haematology Department Patient information leaflet This leaflet explains more about blood clots, which can form after illness and surgery. What are hospital-acquired
Skin Tunnelled Catheter (STC), also known as Central line
 Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Midline. Intravenous Therapy. Patient information leaflet
 Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
Midline Intravenous Therapy Patient information leaflet 2 What is a Midline? This is a very fine flexible tube (up to 20cm length) inserted into a vein in your arm. The tip is in the vein just below your
Percutaneous nephrolithotomy (PCNL)
 Percutaneous nephrolithotomy (PCNL) This leaflet explains more about the PCNL procedure to clear kidney stones, including the benefits, risks and any alternatives and what you can expect when you come
Percutaneous nephrolithotomy (PCNL) This leaflet explains more about the PCNL procedure to clear kidney stones, including the benefits, risks and any alternatives and what you can expect when you come
Right Hemicolectomy Surgery
 Right Hemicolectomy Surgery Patient information How to contact us Oncology Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire, WD18 0HB Tel:
Right Hemicolectomy Surgery Patient information How to contact us Oncology Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire, WD18 0HB Tel:
Liver Resection. Why do I need a liver resection? This procedure is done for many reasons. Talk to your doctor about why you are having this surgery.
 Liver Resection What is a liver resection? This is a surgical procedure where the surgeon removes part of the liver. It is done under general anesthetic which means you sleep during the procedure. Why
Liver Resection What is a liver resection? This is a surgical procedure where the surgeon removes part of the liver. It is done under general anesthetic which means you sleep during the procedure. Why
About Your Colectomy
 UW MEDICINE PATIENT EDUCATION About Your Colectomy How to prepare and what to expect This handout explains a colectomy operation, including how to prepare for surgery, what to expect afterward, recovering
UW MEDICINE PATIENT EDUCATION About Your Colectomy How to prepare and what to expect This handout explains a colectomy operation, including how to prepare for surgery, what to expect afterward, recovering
Paediatric Directorate /1791
 Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Paediatric Directorate 0151 430 1627/1791 WINSTON HELEN Children Coming Into Hospital for an Operation Patient / Carer Information Leaflet Whiston Hospital Warrington Road Prescot L35 5DR Introduction
Right Hemicolectomy. Patient information - General Surgery. Right Hemicolectomy
 Right Hemicolectomy General Surgery Right Hemicolectomy Patient information - General Surgery Introduction This booklet provides information about your operation. Please do not hesitate to ask any questions
Right Hemicolectomy General Surgery Right Hemicolectomy Patient information - General Surgery Introduction This booklet provides information about your operation. Please do not hesitate to ask any questions
Laparoscopic Nissen Fundoplication
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about Laparoscopic
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about Laparoscopic
Day Case Unit/ Treatment Centre. Varicose Veins
 Day Case Unit/ Treatment Centre Varicose Veins What are varicose veins? When the superficial veins in the leg become enlarged and distorted they are said to be varicosed. They are often found in people
Day Case Unit/ Treatment Centre Varicose Veins What are varicose veins? When the superficial veins in the leg become enlarged and distorted they are said to be varicosed. They are often found in people
Hysterectomy. What is a hysterectomy? How is this procedure done?
 Hysterectomy What is a hysterectomy? A hysterectomy is a surgery that removes your uterus (womb). The uterus is one of the organs of the female reproductive system. It is about the size of your closed
Hysterectomy What is a hysterectomy? A hysterectomy is a surgery that removes your uterus (womb). The uterus is one of the organs of the female reproductive system. It is about the size of your closed
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
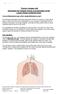 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
kidney bladder prostate Reproduced with kind permission of Health Press Ltd, Oxford
 Patient Information Radical Nephrectomy for Renal Cancer Department of Urology What is a radical nephrectomy? Removal of the kidney. Sometimes it is necessary to remove the adjoining adrenal gland and
Patient Information Radical Nephrectomy for Renal Cancer Department of Urology What is a radical nephrectomy? Removal of the kidney. Sometimes it is necessary to remove the adjoining adrenal gland and
Children s Ward Parent/Carer Information Leaflet
 Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
