PC EP 2 & 6 PC EP 4 & 5
|
|
|
- Letitia Hoover
- 5 years ago
- Views:
Transcription
1 Record Review Inpatient Only 3/10/2016 Data Definition Tool The Tracer Packet is to be completed in each inpatient unit by the manager or designee on a monthly basis. It is suggested that the manager does not complete a packet for his/her own area. Tracers are due on the last day of the month following the review (example: July Tracer due July 31). Instructions: Indicate Yes, No, NA (Not Applicable) for each question below. Inpatient Units: Monitor at least 1 patient record per month using the Tracer Record Review Inpatient Tool. Standard Location YES ADMISSION 1 Medical Record Number: 2 Initial nursing history completed within 24 hours of admission EP 2 & 6 HED: 1) Admission History tab (nurseries); 2) StarPanel starform for all Inpt. units that document in HED except nurseries; 3)StarPanel PDF of VPIMS Periop Nursing documentation for Periop staff; 4) StarPanel PDF for Cath Lab Nursing documentation; 5)paper record Admission /History/ Discharge form if completed during downtime or by an area where none of these electronic options is available. All components completed & signed by RN w/in timeframe as indicated on (1) Time of Medipac transaction to admit; (2) Time order written in CPOE; or (3) Time on Nursing Admission History 3 Provider history and physical (H&P) completed and. (May use previous H&P within 30 days prior or 24 hours after admission or registration that includes an update. The update includes an examination and any changes to the patient's condition.) & 5 H& P form or Star Panel H&P time on record w/in appropriate timeframes which are up to 24 hrs including: Previous H&P within 30 days prior or 24 hours after admission or registration that includes an update. The update includes an examination and any changes to the patient's condition.
2 4 Nursing physical assessment completed on admission? PC EP 6 Assessment/Intervention tab age appropriate First assessment completed w/in 8 hrs of admit time as indicated on (1) Time of Medipac transaction to admit; (2) Time order written in CPOE; or (3) Time on Nursing Admission History 5 Functional screen complete? PC ; EP 8 6 If functional screen positive, plans for follow-up PC Nutritional screen complete PC ; EP 7 8 Pain screen complete PC EP1 & 2 9 If pain screen positive, plans for follow-up PC EP 23; PC Abuse screen complete PC If abuse screen positive, plans for follow-up 12 Suicide Risk screen completed (including the environment) for patients with primary diagnosis of emotional or behavioral disorders? PC , 6, & 7 NPSG ) Admission History StarForm in StarPanel for units that chart in HED (nurseries do not complete Functional Screen on newborns); 2) paper admission history if completed in area that does not document in HED Admission History Admission History/Discharge Plan Nursing Assessment in HED Nursing Assessment in HED Admission History Admission History age appropriate tab VPH documents suicide risk screen in HED. In other areas, it's part of safety assessment in age appropriate assessment interventions tab. Functional Screen complete within 24 hours. Positive screen & provider contacted, MD notified as free text note. NA=negative screen OR preexisting condition (i.e., blind, cerebral palsy, or ADHD) Nutritional screen completed within 8 hours Pain screen completed within 8 hours Positive screen follow up of initial screen completed or negative screen = NA Social Work screen completed; NA is inappropriate answer for inpatients Positive screen & check in "social work ordered" box or negative screen = NA Patients with emotional or behavioral disorder diagnosis has completed assessment. (Children's 8C when applicable and all VPH) 13 If Suicide Risk screen positive, follow-up includes NPSG. provider assessment and environmental assessment Learning needs/education screen complete PC NA is inappropriate answer for inpatients., 4 & 5 15 Preferred language for discussing health care. PC VPH - in suicide screen section. Other HED areas - in Safety interventions. Provider assessment would be in StarPanel. Admission History tab (IP) In admission history Nursing environmental assessment and provider assessment is. Learning needs completed within 8 hours Documented
3 16 Discharge planning initiated within 24 hours of admission Alcohol and Substance Abuse Disorders 17 Assessment includes the following: * patient's religion and spiritual beliefs, values and preferences; * living situation; * leisure and recreational activities; * military service history; * peer group; * social factors; * ethnic & cultural factors; * financial status; * vocational or educational background; * legal history; * communication skills. 18 Assessment includes the following: * history of physical or sexual abuse as either the abuser or the abused; * Sexual history and identification; * Childhood history; * Emotional and health issues: * Visual - motor function; * Self-care. PC PC PC EP 6 19 Assessment includes the patient's family PC circumstances including the composition of the family EP 7 group and the need for their participation in the patient's care. Emotional and Behavioral Disorders 20 Assessment includes the following: * patient's religion and spiritual beliefs, values and preferences; * living situation; * leisure and recreational activities; * military service history; * peer group; * social factors; * ethnic & cultural factors; * financial status; * vocational or educational background; * legal history; * communication skills. PC Plan of Care VPH Psychosocial Assessment & VPH Nursing Admission History & Psychiatric Admission Evaluation (starpanel) and/or Crisis Assessment (paper record) VPH Psychosocial Assessment & VPH Nursing Admission History & Psychiatric Admission Evaluation (starpanel) and/or Crisis Assessment (paper record) VPH Pscyhosocial Assessment and Psychiatric Admission Evaluation (Starpanel) VPH Psychosocial Assessment & VPH Nursing Admission History & Psychiatric Admission Evaluation (starpanel) and/or Crisis Assessment (paper record) Plan initiated w/in timeframe or Case Management & Socical Work screen negataive
4 21 Assessment includes the following: * history of physical or sexual abuse as either the abuser or the abused; * Sexual history; * Childhood history; * Emotional and healthcare issues: * Visual - motor function; * Self-care. 22 Assessment includes the following: * patient's family circumstances including the composition of the family group; *Community Resources currently used by the patient; and *The need for their participation in the patient's care. PC EP4 PC VPH Psychosocial Assessment & VPH Nursing Admission History & Psychiatric Admission Evaluation (starpanel) and/or Crisis Assessment (paper record) VPH Pscyhosocial Assessment and Psychiatric Admission Evaluation (Starpanel) 23 Assessment includes the following: * Psychiatric evaluation; * Pscyhological assessments including intellectual projective neuropsychological and personality testing; * Complete neurological examination, when indicated. PC EP6 Psychiatric Admission Evaluation (Starpanel) ADVANCE DIRECTIVES (IP Only) 24 Advance Directives Progress Notes (MC# 4137) signed and completed? 25 Copy in chart or substance of directive in physician's progress notes or on Advance Directives Progress Notes (MC#4137) RC RI EP 9 RI EP 9 & 11 Advance Directives Progress Notes and HED Admission / History Extended Data (both completed) Clear plastic advance directive sleeve at the front of the chart (1st item) or on Advance Directives Progress Notes or physician progress notes or scanned in star panel under legal documents and in HED Adm/History extended data Both Advance Directives Progress Notes form and HED data completed to be Yes. Choice of: - Copy present or directive signed by physician OR - Copy in STAR Panel from previous admission under "ALL" and then "legal Documents" OR - Answer "NA" if patient has no Advance Directive
5 NURSING ASSESSMENT (IP Only) 26 Physical assessment per shift or unit standard? PC EP 23; 27 Each patient is reassessed as necessary based on his or her plan for care or changes in his or her condition. 28 Pain assessment at least every shift; when there is a change in patient condition or primary caregiver. PC Interventions r/t pain management are PC Pain is reassessed after administration of pain med/comfort measures PC PATIENT EDUCATION 31 Pain management addressed, as appropriate PC All "teaching/education" fields complete, as appropriate (excluding pain management) 33 Documentation by all disciplines involved in the patient's care, treatment or services. MEDICATION ADMINISTRATION 34 "Do Not Use" Abbreviations are NOT found in the MR on date of review? 35 Supporting documentation (diagnosis, condition, or indication for use) exists for every order for "current" medications. PC PC IM MM EP 9 Assessment/Intervention age appropriate tab Assessment/Intervention age appropriate tab Assessment/ Intervention age appropriate or Pain tab Assessment/Intervention age appropriate tab or Pain tab Assessment/Intervention age appropriate tab or pain tab and/or Controlled Drug Record HED Education Tab Education Record "other" or HED Education Tab Same as above. Paper and individual discipline notes; Electronic documentation available via OPC Assessment Section. All entries in the medical record on date of review including medication orders, MAR, problem list, flowsheets, progress notes,etc. Physician orders, H&P, progress notes Date, nurse signatuare & title, time and initials are and check mark placed beside "Standards Met" or "Except as Noted" for each section. Date, nurse signatuare & title, time and initials are and check mark placed beside "Standards Met" or "Except as Noted" for each section. Time, Date, Pain Score/indicators are Interventions, post time, relief, initials are. Interventions, date time, pain score, and initials are within 2 hrs of intervention. Exception: PCA or continuous infusion IV analgesia assessment every 4 hrs. All teaching fields specific to pain are completed. All teaching fields are appropriately completed except pain management teaching. Signature(s) & initials are present for appropriate disciplines. No " Do Not Use" abbreviations are found in the medical record on the date of review. Diagnosis, condition or indications for use are anywhere in the medical record including the H&P
6 36 Are orders for PRN medications specific such that there is no therapeutic duplicatoin (multiple options for a specific indication? Medications list Review patient's current PRN medication orders for therapeutic duplication. There should not be two orders that have the same instructions for when to administer (e.g., prn pain, prn nausea, prn for agitation).
7 DISCHARGE (IP Only) 37 Discharge plan reviewed every 24 hours. PC Discharge instructions completed upon discharge. PC EP 8 39 For patients admitted with primary diagnosis of emotional or behavioral disorders, discharge instructions include suicide prevention information such as crisis hot line number. OPERATIVE & OTHER PROCEDURES NPSG Consent form present and signed, dated and timed? RI Provider history and physical (H&P) completed and prior to procedure? (May use previous H&P within 30 days prior or 24 hours after admission or registration that includles an update. The update includes an examination and any changes to the patient's condition.) Plan of Care tab 1) Discharge Process tool document saved to StarPanel. 2) Paper Discharge Instructions sheet scanned into StarPanel if pt. discharged during HEO/Wiz downtime or Discharge Process tool not used. WIZ or paper Patient Discharge Instructions or discharge letters per speciality Consent Form H& P form Check box on Plan of Care/Discharge Plan tab for "done" Discharge letter complete and in StarPanel Discharge instructions includes suicide prevention information consent form present and signed, dated and timed H&P on record prior to procedure/ surgery and w/in appropriate timeframes: 42 Pre-procedural education before operative or high-risk procedures or before moderate or deep sedation or anesthesia. 43 Patient's condition is re-evaluated before administering moderate or deep sedation or anesthesia. PC PC EP 8 44 Pre-procedure checklist is completed. UP EP 2 45 "Time Out" before procedure. UP Preop Nursing Record (PDF in Starpanel) Sedation & Analgesia Record, Anesthesia record Pre-procedure checklist Area Specific documentation systems. Sedation/ Analgesia form. Documented ASA class and Pre-Sedation Status completed for moderate or deep sedation. For OR area Anesthesia Care Record ASA score prior to induction completed. All fields completed, as appropriate. Completed including date and time.
8 46 Immediate Post Operative/procedural Note is present RC and includes the following: EP 7 1. Name of surgeon, proceduralist and assistants; 2. Procedure(s) performed and description of the procedure; 3. Findings; 4. Estimated blood loss; 5. Specimen(s) removed, if any. 6. Postoperative diagnosis. Post surgical progress notes All elements are in the record before the patient moves to the next level of care irregardless of physical location. Exception: if the proceduralist accompanies the patient from the procedure room to the next level of care, the note can be written in that unit or area of care. 47 The Operative/Procedural report is dictated or electronically entered in the pt record within 24 hrs of the procedure and includes: 1. Patient s name and medical record number; 2. Name and date of procedure; 3. Name of surgeon, proceduralists and assistants; 4. Pre-operative diagnosis, 5. Postoperative diagnosis; 6. Anesthetic agent used; 7. Description of the techniques and procedure; 8. Description of the findings; 9. Estimated blood loss; 10. Specimen(s) removed, if any; 11. Any laboratory or diagnostic procedure ordered; 12. Complications, if any; 13. Condition of patient. RC , 6 & 7 CMS (b) Surgical / procedure Report All elements are in the report and dictated or electronically entered within 24 hours of the procedure. The attending physician has signed the report within 14 days of the procedure. 48 For operative or high-risk procedures and/or the administration of moderate or deep sedation or anesthesia, patients are discharged from recovery area by LIP or by criteria. (Operative/Procedural Areas) PC Discharge Criteria documentation Discharge criteria
IP = Inpatient OP = Outpatient Standard Location YES No. HED: Admission History tab or paper record Admission /History/ Discharge form
 Tracer Record Review - ECT-Periop Only 9-30-2016 Data Definition Tool The Tracer Packet is to be completed in each Periop area by the manager or designee on a monthly basis. It is suggested that the manager
Tracer Record Review - ECT-Periop Only 9-30-2016 Data Definition Tool The Tracer Packet is to be completed in each Periop area by the manager or designee on a monthly basis. It is suggested that the manager
Standard Location YES. Activities of Daily Living section completed. VMG Clinic Intake Form
 Tracer Record Review - Outpatient Only updated: 3/21/2016 Data Definition Tool The Tracer Packet is to be completed in each outpatient area by the manager or designee on a monthly basis. It is suggested
Tracer Record Review - Outpatient Only updated: 3/21/2016 Data Definition Tool The Tracer Packet is to be completed in each outpatient area by the manager or designee on a monthly basis. It is suggested
PC EP 4; PC EP 7. (Outpatient Only) If nutritional screen positive, plans for follow-up documented.
 Dialysis - Patient Documentation & Observation Tool Data Definition Tool This audit is to be completed by the manager or designee on a monthly basis. "Dialysis - Patient Documentation & Observation Tool"
Dialysis - Patient Documentation & Observation Tool Data Definition Tool This audit is to be completed by the manager or designee on a monthly basis. "Dialysis - Patient Documentation & Observation Tool"
Joint Commission quarterly update Medical record documentation guide and medical record reviews
 April 2016 HIM Briefings Joint Commission quarterly update Medical record documentation guide and medical record reviews Jean S. Clark, RHIA, CSHA Our readers have been asking for an updated medical record
April 2016 HIM Briefings Joint Commission quarterly update Medical record documentation guide and medical record reviews Jean S. Clark, RHIA, CSHA Our readers have been asking for an updated medical record
Institutional Handbook of Operating Procedures Policy
 Section: Clinical Policies Subject: General Procedures Institutional Handbook of Operating Procedures Policy 09.13.09 Responsible Vice President: EVP and CEO Health System Responsible Entity: UTMB Health
Section: Clinical Policies Subject: General Procedures Institutional Handbook of Operating Procedures Policy 09.13.09 Responsible Vice President: EVP and CEO Health System Responsible Entity: UTMB Health
EP Review Project: The Joint Commission Deletes 225 Hospital Requirements
 PR Review Project: The Joint Commission Deletes 225 Hospital Requirements Project REFRESH (see related articles on pages 1 and 3) includes a project first announced in the December 2015 Perspectives: the
PR Review Project: The Joint Commission Deletes 225 Hospital Requirements Project REFRESH (see related articles on pages 1 and 3) includes a project first announced in the December 2015 Perspectives: the
Community Health Network, Inc. MEDICAL STAFF POLICIES & PROCEDURES
 Community East Community South Community North TITLE: Medical Record Chart Requirements The medical record of care comprises all the data and information about a patient s visit. It functions as both a
Community East Community South Community North TITLE: Medical Record Chart Requirements The medical record of care comprises all the data and information about a patient s visit. It functions as both a
The University Hospital Medical Staff. Rules And Regulations
 The University Hospital Medical Staff Rules And Regulations - 1 - UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement
The University Hospital Medical Staff Rules And Regulations - 1 - UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement
Medical Staff Rules & Regulations Last Updated: October University Hospital Medical Staff. Rules & Regulations
 University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
STANFORD HEALTH CARE Medical Staff Rules and Regulations. Last Approval Date: December 2017
 STANFORD HEALTH CARE Medical Staff Rules and Regulations Last Approval Date: December 2017 The Medical Staff is responsible to the Stanford Healthcare (SHC) Board of Directors for the professional medical
STANFORD HEALTH CARE Medical Staff Rules and Regulations Last Approval Date: December 2017 The Medical Staff is responsible to the Stanford Healthcare (SHC) Board of Directors for the professional medical
CRAIG HOSPITAL POLICY/PROCEDURE
 CRAIG HOSPITAL POLICY/PROCEDURE Approved: P&T, MEC, NPC, P&P 03/09 Effective Date: 02/95 P&T, MEC, P&P 08/09; P&P 08/10; P&T, MEC 10/10, P&T, P&P 12/10 ; MEC 01/11; P&T, MEC 02/11, 04/11 ; P&T, P&P 12/11
CRAIG HOSPITAL POLICY/PROCEDURE Approved: P&T, MEC, NPC, P&P 03/09 Effective Date: 02/95 P&T, MEC, P&P 08/09; P&P 08/10; P&T, MEC 10/10, P&T, P&P 12/10 ; MEC 01/11; P&T, MEC 02/11, 04/11 ; P&T, P&P 12/11
ENVIRONMENT Preoperative evaluation clinic. Preoperative evaluation clinic. Preoperative evaluation clinic. clinic. clinic. Preoperative evaluation
 Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Goals and Objectives, Preoperative Evaluation Clinic Rotation, CA-1 and CA-2 year UCSD DEPARTMENT OF ANESTHESIOLOGY PREOPERATIVE EVALUATION CLINIC ROTATION GOALS AND OBJECTIVES, CA-1 and CA-2 YEAR PATIENT
Ask the Expert Webinar
 Copyright, The Joint Commission Ask the Expert Webinar Answers to the Most Frequently Asked Questions (FAQs) From Nursing Care Centers Presenter: Lynette Gibbney, RN Associate Director, Standards Interpretation
Copyright, The Joint Commission Ask the Expert Webinar Answers to the Most Frequently Asked Questions (FAQs) From Nursing Care Centers Presenter: Lynette Gibbney, RN Associate Director, Standards Interpretation
RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF UNIVERSITY OF NORTH CAROLINA HOSPITALS
 RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF UNIVERSITY OF NORTH CAROLINA HOSPITALS Approved by the Executive Committee of the Medical Staff, November 5, 2001. Approved and adopted by the Board
RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF UNIVERSITY OF NORTH CAROLINA HOSPITALS Approved by the Executive Committee of the Medical Staff, November 5, 2001. Approved and adopted by the Board
High 5s Project: Action on Patient Safety. SOP Flow Charts. 20 th International Forum on Quality and Safety in Healthcare April 2015 London, UK
 High 5s Project: Action on Patient Safety SOP Flow Charts 20 th International Forum on Quality and Safety in Healthcare 21-24 April 2015 London, UK Performance of Correct Procedure at Correct Body Site
High 5s Project: Action on Patient Safety SOP Flow Charts 20 th International Forum on Quality and Safety in Healthcare 21-24 April 2015 London, UK Performance of Correct Procedure at Correct Body Site
CHILDREN'S MENTAL HEALTH ACT
 40 MINNESOTA STATUTES 2013 245.487 CHILDREN'S MENTAL HEALTH ACT 245.487 CITATION; DECLARATION OF POLICY; MISSION. Subdivision 1. Citation. Sections 245.487 to 245.4889 may be cited as the "Minnesota Comprehensive
40 MINNESOTA STATUTES 2013 245.487 CHILDREN'S MENTAL HEALTH ACT 245.487 CITATION; DECLARATION OF POLICY; MISSION. Subdivision 1. Citation. Sections 245.487 to 245.4889 may be cited as the "Minnesota Comprehensive
CAMH February 2005 Update HIGHLIGHTS
 CAMH February 2005 Update HIGHLIGHTS STANDARD UP 1. How to Use Manual Multiple changes to scoring, category changes and Measure of Success (MOS) designation removed 2. Accreditation Policies & Procedures
CAMH February 2005 Update HIGHLIGHTS STANDARD UP 1. How to Use Manual Multiple changes to scoring, category changes and Measure of Success (MOS) designation removed 2. Accreditation Policies & Procedures
CPAN / CAPA Examination Study Plan
 CPAN / CAPA Examination Study Plan Candidates should prepare thoroughly prior to taking the CPAN and/or CAPA examinations. This Study Plan is based on the CPAN and CAPA Test Blueprints and a weekly learning
CPAN / CAPA Examination Study Plan Candidates should prepare thoroughly prior to taking the CPAN and/or CAPA examinations. This Study Plan is based on the CPAN and CAPA Test Blueprints and a weekly learning
Patient Age Group: ( ) N/A (X) All Ages ( ) Newborns ( ) Pediatric ( ) Adult
 Title: Documentation of Clinical Activities by UNMH Medical Staff and House Staff Applies To: UNM Hospitals Responsible Department: Office of Clinical Affairs Updated: 05/2016 Policy Patient Age Group:
Title: Documentation of Clinical Activities by UNMH Medical Staff and House Staff Applies To: UNM Hospitals Responsible Department: Office of Clinical Affairs Updated: 05/2016 Policy Patient Age Group:
CRITICAL ACCESS HOSPITALS
 Are anesthesia services and post-anesthesia services medical director(s) qualified in terms of education, experience and competency as determined by the hospital medical staff and appointed by the governing
Are anesthesia services and post-anesthesia services medical director(s) qualified in terms of education, experience and competency as determined by the hospital medical staff and appointed by the governing
PACU PRE-OP. Demographics
 Table of Contents Can you find this information that the Joint Commission will ask to see? Remember there may be multiple paths to locate the below information. Any route that you know will be fine! PRE-OP
Table of Contents Can you find this information that the Joint Commission will ask to see? Remember there may be multiple paths to locate the below information. Any route that you know will be fine! PRE-OP
CHEYENNE REGIONAL MEDICAL CENTER AREA: TITLE: TrueConnect Downtime/Recovery Procedure. Page 1 of 1 NUMBER: ADMIN-IM-32 ORIGINATOR: CMIO
 ORIGINATOR: CMIO Page 1 of 1 POLICY APPLIES TO: Cheyenne Regional APPROVED BY: CEO: COO: CHRO: CNO: CMIO: REVISION DATE: N/A new policy EFFECTIVE DATE: March 2013 POLICY REVIEW COMMITTEE (PRC) REVIEW DATE:
ORIGINATOR: CMIO Page 1 of 1 POLICY APPLIES TO: Cheyenne Regional APPROVED BY: CEO: COO: CHRO: CNO: CMIO: REVISION DATE: N/A new policy EFFECTIVE DATE: March 2013 POLICY REVIEW COMMITTEE (PRC) REVIEW DATE:
The Joint Commission Standards and the Patients
 The Joint Commission Standards and the Patients 23 rd Annual National Forum on Quality Improvement in Health Care December 7, 2011 Orlando, Florida Pat Adamski, RN, MS, MBA Director, Standards Interpretation
The Joint Commission Standards and the Patients 23 rd Annual National Forum on Quality Improvement in Health Care December 7, 2011 Orlando, Florida Pat Adamski, RN, MS, MBA Director, Standards Interpretation
Sec Disconnect Go to End Forward Sec Next Report Go To
 Effective 3/15/04 escription DICTATION SYSTEM FOR INPATIENT HISTORY & PHYSICALS, DISCHARGE SUMMARIES, DELIVERY (NORMAL) NOTES OPERATIVE REPORTS DIAL 3-4000 LISTEN FOR VERBAL PROMPTS. ENTER: First 5 digits
Effective 3/15/04 escription DICTATION SYSTEM FOR INPATIENT HISTORY & PHYSICALS, DISCHARGE SUMMARIES, DELIVERY (NORMAL) NOTES OPERATIVE REPORTS DIAL 3-4000 LISTEN FOR VERBAL PROMPTS. ENTER: First 5 digits
Clinical Utilization Management Guideline
 Clinical Utilization Management Guideline Subject: Therapeutic Behavioral On-Site Services for Recipients Under the Age of 21 Years Status: New Current Effective Date: January 2018 Description Last Review
Clinical Utilization Management Guideline Subject: Therapeutic Behavioral On-Site Services for Recipients Under the Age of 21 Years Status: New Current Effective Date: January 2018 Description Last Review
Patient Safety Course Descriptions
 Adverse Events Antibiotic Resistance This course will teach you how to deal with adverse events at your facility. You will learn: What incidents are, and how to respond to them. What sentinel events are,
Adverse Events Antibiotic Resistance This course will teach you how to deal with adverse events at your facility. You will learn: What incidents are, and how to respond to them. What sentinel events are,
Prepublication Requirements
 Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY
 POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
Prepublication Requirements
 Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program)
 Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program) (SEE NY Public Health Law 2500f for HIV testing of newborns FOR STATUTE)
Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program) (SEE NY Public Health Law 2500f for HIV testing of newborns FOR STATUTE)
2012 Medical Staff Update 2011 CHALLENGING STANDARDS/NPSGS
 2012 Medical Staff Update Laurel McCourt, M.D. TJC Surveyor: Hospital and Office-Based Surgery Programs, and Special Survey Unit 2011 CHALLENGING STANDARDS/NPSGS 2 Standard/NPSG 2010 Non Compliance 3 2011
2012 Medical Staff Update Laurel McCourt, M.D. TJC Surveyor: Hospital and Office-Based Surgery Programs, and Special Survey Unit 2011 CHALLENGING STANDARDS/NPSGS 2 Standard/NPSG 2010 Non Compliance 3 2011
Surgical Technology Patient Care Skills Preop Routine Objectives:
 Surgical Technology 8-Jul-09 Patient Care Skills Preop Routine Objectives: 1) Discuss why preop preparation of the patient is important a) Preparing the patient decreases impact and potential risks of
Surgical Technology 8-Jul-09 Patient Care Skills Preop Routine Objectives: 1) Discuss why preop preparation of the patient is important a) Preparing the patient decreases impact and potential risks of
Institutional Handbook of Operating Procedures Policy
 Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
Section: Admission, Discharge, and Transfer Institutional Handbook of Operating Procedures Policy 9.1.29 Responsible Vice President: EVP & CEO Health System Subject: Admission, Discharge, and Transfer
*OB/Gyn. Hospital Billing. April 2, 2014 Erika Bloomquist, CPC
 OB/Gyn Hospital Billing April 2, 2014 Erika Bloomquist, CPC Initial Date Diagnoses Billing Level Code Patient Label ZK 3/1 1,2 A1 Or two patient identifiers BB 3/2 1,2 S2 TS 3/3 1,2 D1 Inpt. Obs Transfer
OB/Gyn Hospital Billing April 2, 2014 Erika Bloomquist, CPC Initial Date Diagnoses Billing Level Code Patient Label ZK 3/1 1,2 A1 Or two patient identifiers BB 3/2 1,2 S2 TS 3/3 1,2 D1 Inpt. Obs Transfer
59G Preadmission Screening and Resident Review.
 59G-1.040 Preadmission Screening and Resident Review. (1) Purpose. This rule applies to all Florida Medicaid-certified nursing facilities (NF), regardless of payer source; all providers rendering NF services
59G-1.040 Preadmission Screening and Resident Review. (1) Purpose. This rule applies to all Florida Medicaid-certified nursing facilities (NF), regardless of payer source; all providers rendering NF services
Procedure. Applies To: UNM Hospitals Responsible Department: Quality Revised: 03/2014
 Procedure Patient Age Group: ( ) N/A ( ) All Ages ( ) Newborns (X) Pediatric (x ) Adult DESCRIPTION/OVERVIEW UNM Hospitals (UNMH) is recognized as a large academic health care system providing services
Procedure Patient Age Group: ( ) N/A ( ) All Ages ( ) Newborns (X) Pediatric (x ) Adult DESCRIPTION/OVERVIEW UNM Hospitals (UNMH) is recognized as a large academic health care system providing services
Introduction to Perioperative Nursing
 C H A P T E R 1 Introduction to Perioperative Nursing LEARNER OBJECTIVES 1. Define the three phases of the surgical experience. 2. Describe the scope of perioperative nursing practice. 3. Discuss application
C H A P T E R 1 Introduction to Perioperative Nursing LEARNER OBJECTIVES 1. Define the three phases of the surgical experience. 2. Describe the scope of perioperative nursing practice. 3. Discuss application
The Joint Commission 2007 Requirements Related to the Provision of Culturally and Linguistically Appropriate Health Care May 2007
 The Joint Commission 2007 Requirements Related to the Provision of Culturally and Linguistically Appropriate Health Care May 2007 The Joint Commission views the issue of the provision of culturally and
The Joint Commission 2007 Requirements Related to the Provision of Culturally and Linguistically Appropriate Health Care May 2007 The Joint Commission views the issue of the provision of culturally and
Covered Service Codes and Definitions
 Covered Service Codes and Definitions [01] Assessment Assessment services include the systematic collection and integrated review of individualspecific data, such as examinations and evaluations. This
Covered Service Codes and Definitions [01] Assessment Assessment services include the systematic collection and integrated review of individualspecific data, such as examinations and evaluations. This
Inpatient Rehabilitation. Scope of Services
 Inpatient Rehabilitation Scope of Services Inpatient Rehabilitation is a 12-bed inpatient unit located within Nationwide Children s Hospital. Nationwide Children s is a 451-bed, Level I Trauma Center.
Inpatient Rehabilitation Scope of Services Inpatient Rehabilitation is a 12-bed inpatient unit located within Nationwide Children s Hospital. Nationwide Children s is a 451-bed, Level I Trauma Center.
SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: POST ANESTHESIA CARE UNITS (PACU) EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: Job Title of
PS1070 SARASOTA MEMORIAL HOSPITAL PERIOPERATIVE DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: POST ANESTHESIA CARE UNITS (PACU) EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: Job Title of
Beltway Surgery Centers, L.L.C.
 MEDICAL STAFF RULES AND REGULATIONS ARTICLE I. PROFESSIONALISM 1.1 These rules and regulations are intended to provide comprehensive information to members of the Ambulatory Surgery Center in order for
MEDICAL STAFF RULES AND REGULATIONS ARTICLE I. PROFESSIONALISM 1.1 These rules and regulations are intended to provide comprehensive information to members of the Ambulatory Surgery Center in order for
QUALITY NET REPORTING
 5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
5/18/15% A webinar series that keeps you in the know Brought to you by Progressive QUALITY NET REPORTING Sarah Martin, MBA, RN, CASC Progressive Huddle May 18, 2015 ASCQR ASC Quality Reporting started
Nurse Practitioner - Outpatient Lung Transplant (1.0 FTE, Days)
 Nurse Practitioner - Outpatient Lung Transplant (1.0 FTE, Days) Category: Nursing Advance Practice Job Type: Full-Time Shift: Days Location: Palo Alto, CA, United States Req: 5609 FTE: 1 Nursing Advance
Nurse Practitioner - Outpatient Lung Transplant (1.0 FTE, Days) Category: Nursing Advance Practice Job Type: Full-Time Shift: Days Location: Palo Alto, CA, United States Req: 5609 FTE: 1 Nursing Advance
STROKE REHAB PROGRAM
 STROKE REHAB PROGRAM Allied Rehab Hospital is part of Allied Services Integrated Health System, the premier post-acute health-care system in Northeast Pennsylvania, and is the region s leading provider
STROKE REHAB PROGRAM Allied Rehab Hospital is part of Allied Services Integrated Health System, the premier post-acute health-care system in Northeast Pennsylvania, and is the region s leading provider
SCIP-Inf-2, SCIP-Inf-3, SCIP-Inf-4, SCIP-Inf- 9, SCIP-Inf-10, SCIP-VTE-1, SCIP-VTE-2 Anesthesia End Time 5
 Release Notes: Alphabetical Data Dictionary Version 3.3 Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Release Notes: Alphabetical Data Dictionary Version 3.3 Surgical Care Improvement Project (SCIP) - Data Dictionary The General Abstraction Guidelines explain the different sections of the data element
Impact of Medicare COP Changes on HIM
 Impact of Medicare COP Changes on HIM Audio Seminar/Webinar March 29, 2007 Practical Tools for Seminar Learning Copyright 2007 American Health Information Management Association. All rights reserved. Disclaimer
Impact of Medicare COP Changes on HIM Audio Seminar/Webinar March 29, 2007 Practical Tools for Seminar Learning Copyright 2007 American Health Information Management Association. All rights reserved. Disclaimer
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Proposed Standards Revisions Related to Pain Assessment and Management
 Leadership (LD) Chapter LD.0001 Proposed Standards Revisions Related to Pain Assessment and Management 1 2 Leaders establish priorities for performance improvement. (Refer to the "Performance Improvement"
Leadership (LD) Chapter LD.0001 Proposed Standards Revisions Related to Pain Assessment and Management 1 2 Leaders establish priorities for performance improvement. (Refer to the "Performance Improvement"
907 KAR 15:080. Coverage provisions and requirements regarding outpatient chemical dependency treatment center services.
 907 KAR 15:080. Coverage provisions and requirements regarding outpatient chemical dependency treatment center services. RELATES TO: KRS 205.520, 42 U.S.C. 1396a(a)(10)(B), 1396a(a)(23) STATUTORY AUTHORITY:
907 KAR 15:080. Coverage provisions and requirements regarding outpatient chemical dependency treatment center services. RELATES TO: KRS 205.520, 42 U.S.C. 1396a(a)(10)(B), 1396a(a)(23) STATUTORY AUTHORITY:
G: Surgical. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67
 G: Surgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67 Major Competency Area: G Surgical Competency: G-1 Surgical Nursing Date: June 1, 2015 G-1-1 G-1-2 G-1-3
G: Surgical College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 67 Major Competency Area: G Surgical Competency: G-1 Surgical Nursing Date: June 1, 2015 G-1-1 G-1-2 G-1-3
INPATIENT PROGRAM ENVIRONMENT Brain Injury Specialty Program
 INPATIENT PROGRAM ENVIRONMENT Brain Injury Specialty Program INPATIENT PROGRAM ENVIRONMENT Upon admission, patients and families are oriented to the Rehabilitation Program, and are involved in an evaluation
INPATIENT PROGRAM ENVIRONMENT Brain Injury Specialty Program INPATIENT PROGRAM ENVIRONMENT Upon admission, patients and families are oriented to the Rehabilitation Program, and are involved in an evaluation
University of Mississippi Medical Center University of Mississippi Health Care. Pharmacy and Therapeutics Committee Medication Use Evaluation
 University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation TJC Standards for Medication Management March 2012 Purpose The
MENTAL HEALTH NURSING ORIENTATION. (2) Alleviating disabling symptoms of mental disorders.
 Page 1 of 6 1. Mission Statement MENTAL HEALTH NURSING ORIENTATION a. The mission of mental health services is to provide constitutionally adequate care. Mental health care is provided to assist the inmate
Page 1 of 6 1. Mission Statement MENTAL HEALTH NURSING ORIENTATION a. The mission of mental health services is to provide constitutionally adequate care. Mental health care is provided to assist the inmate
Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid
 Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid Information posted on October 8, 2010 Effective for dates of service on or after December 1, 2010, the benefit criteria
Benefit Criteria for Outpatient Observation Services to Change for Texas Medicaid Information posted on October 8, 2010 Effective for dates of service on or after December 1, 2010, the benefit criteria
WakeMed Rehab Spinal Cord Injury Scope of Service
 WakeMed Rehab Spinal Cord Injury Scope of Service The WakeMed Rehab Continuum provides an integrated, comprehensive delivery of rehabilitation services utilizing evidence-based practice directed toward
WakeMed Rehab Spinal Cord Injury Scope of Service The WakeMed Rehab Continuum provides an integrated, comprehensive delivery of rehabilitation services utilizing evidence-based practice directed toward
Inpatient orders and Physician Certification MUST BE authenticated PRIOR to discharge No EXCEPTIONS.
 2 Midnight Rule for InPatient Admission On August 2, 2013 the Centers for Medicare & Medicaid Services (CMS) issued a final rule (CMS- 1599-F) updating Medicare payment policies which modifies and clarifies
2 Midnight Rule for InPatient Admission On August 2, 2013 the Centers for Medicare & Medicaid Services (CMS) issued a final rule (CMS- 1599-F) updating Medicare payment policies which modifies and clarifies
LOUISIANA MEDICAID PROGRAM ISSUED: 02/01/12 REPLACED: 02/01/94 CHAPTER 5: PROFESSIONAL SERVICES SECTION 5.1: COVERED SERVICES PAGE(S) 11
 Anesthesia Services Surgical anesthesia services may be provided by anesthesiologists or certified registered nurse anesthetists (CRNAs). Maternity-related anesthesia services may be provided by anesthesiologists,
Anesthesia Services Surgical anesthesia services may be provided by anesthesiologists or certified registered nurse anesthetists (CRNAs). Maternity-related anesthesia services may be provided by anesthesiologists,
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Respite Care DEFINITION
 DEFINITION Respite Care programs provide temporary relief to caregivers with responsibility for the care and supervision of adults or children who: have physical, emotional, developmental, cognitive, behavioural,
DEFINITION Respite Care programs provide temporary relief to caregivers with responsibility for the care and supervision of adults or children who: have physical, emotional, developmental, cognitive, behavioural,
Child and Family Development and Support Services
 Child and Services DEFINITION Child and Services address the needs of the family as a whole and are based in the homes, neighbourhoods, and communities of families who need help promoting positive development,
Child and Services DEFINITION Child and Services address the needs of the family as a whole and are based in the homes, neighbourhoods, and communities of families who need help promoting positive development,
Sedation/Analgesia by Non-Anesthesiologists. THE UNIVERSITY OF TOLEDO Approving Officer:
 Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
CAH PREPARATION ON-SITE VISIT
 CAH PREPARATION ON-SITE VISIT Illinois Department of Public Health, Center for Rural Health This day is yours and can be flexible to the timetable of hospital staff. An additional visit can also be arranged
CAH PREPARATION ON-SITE VISIT Illinois Department of Public Health, Center for Rural Health This day is yours and can be flexible to the timetable of hospital staff. An additional visit can also be arranged
Florida Medicaid. Statewide Inpatient Psychiatric Program Coverage Policy
 Florida Medicaid Statewide Inpatient Psychiatric Program Coverage Policy Agency for Health Care Administration December 2015 Table of Contents 1.0 Introduction... 1 1.1 Description... 1 1.2 Legal Authority...
Florida Medicaid Statewide Inpatient Psychiatric Program Coverage Policy Agency for Health Care Administration December 2015 Table of Contents 1.0 Introduction... 1 1.1 Description... 1 1.2 Legal Authority...
APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that apply)
 POLICY NAME: ANESTHESIA PAYMENT POLICY POLICY NUMBER: ISSUING DEPT.: Claims EFFECTIVE DATE: 9/25/2017 APPROVED BY: APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that
POLICY NAME: ANESTHESIA PAYMENT POLICY POLICY NUMBER: ISSUING DEPT.: Claims EFFECTIVE DATE: 9/25/2017 APPROVED BY: APPLIES TO: x SummaCare, Inc. x Apex Health Solutions PRODUCT LINE(S): (Check all that
Prepublication Requirements
 Prepublication Requirements Standards Revisions for Swing Bed Final Rule in Critical Access Hospitals The Joint Commission has approved the following revisions for prepublication. While revised requirements
Prepublication Requirements Standards Revisions for Swing Bed Final Rule in Critical Access Hospitals The Joint Commission has approved the following revisions for prepublication. While revised requirements
Anesthesia Services Policy
 Anesthesia Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare Medicare
Anesthesia Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare Medicare
WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service
 WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service WakeMed Rehab Hospital provides an integrated, comprehensive delivery of rehabilitation services utilizing evidenced-based practice directed
WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service WakeMed Rehab Hospital provides an integrated, comprehensive delivery of rehabilitation services utilizing evidenced-based practice directed
244 CMR: BOARD OF REGISTRATION IN NURSING
 244 CMR 4.00: THE PRACTICE OF NURSING IN THE EXPANDED ROLE Section 4.01: Authority 4.02: Purpose 4.03: Citation 4.04: Scope 4.05: Definitions 4.06: Gender of Pronouns 4.07: Number (4.08 through 4.10: Reserved)
244 CMR 4.00: THE PRACTICE OF NURSING IN THE EXPANDED ROLE Section 4.01: Authority 4.02: Purpose 4.03: Citation 4.04: Scope 4.05: Definitions 4.06: Gender of Pronouns 4.07: Number (4.08 through 4.10: Reserved)
Comprehensive Community Services (CCS) File Review Checklist Comprehensive
 This is a sample form developed by the "CCS Statewide QA/QI Work Group", and is available to CCS sites as a sample for consideration of use, modification, and customization. There is no implicit or explicit
This is a sample form developed by the "CCS Statewide QA/QI Work Group", and is available to CCS sites as a sample for consideration of use, modification, and customization. There is no implicit or explicit
Designated Record Set Health Record The health information described below may be maintained in any medium (paper, electronic, digital, etc)
 Designated Record Set Health Record The health information described below may be maintained in any medium (paper, electronic, digital, etc) DEFINITION Designated Record Set A group of records (recorded
Designated Record Set Health Record The health information described below may be maintained in any medium (paper, electronic, digital, etc) DEFINITION Designated Record Set A group of records (recorded
Medicare Behavioral Health Authorization List Effective 5/26/18
 100 All inclusive room and board 101 All inclusive room and board 104 Anesthesia, ECT 114 Room and Board- private psychiatric 116 Room and Board- private room detoxification 118 Room and Board- private
100 All inclusive room and board 101 All inclusive room and board 104 Anesthesia, ECT 114 Room and Board- private psychiatric 116 Room and Board- private room detoxification 118 Room and Board- private
Acute. Proposing Surgical Procedure Orders and Orders. Surgical Procedure Orders and Orders Affiliated. Requesting a Surgical Encounter FIN#:
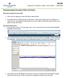 Acute Surgical Procedure Orders and Orders Affiliated Proposing Surgical Procedure Orders and Orders Requesting a Surgical Encounter FIN#: 1. Office calls Pre-registration at 801-387-7646 or 800-624-3972.
Acute Surgical Procedure Orders and Orders Affiliated Proposing Surgical Procedure Orders and Orders Requesting a Surgical Encounter FIN#: 1. Office calls Pre-registration at 801-387-7646 or 800-624-3972.
Interpretation of The Joint Commission Standards Related to Pain Management. Agenda. The Joint Commission Mission 9/6/2012
 Interpretation of The Joint Commission Standards Related to Pain Management ASPMN 22 nd National Conference Baltimore, MD September 13, 2012 Pat Adamski, RN, MS, MBA, FACHE Director, Standards Interpretation
Interpretation of The Joint Commission Standards Related to Pain Management ASPMN 22 nd National Conference Baltimore, MD September 13, 2012 Pat Adamski, RN, MS, MBA, FACHE Director, Standards Interpretation
CAMH. Table of Changes CAMH Update 1, March 2011
 Comprehensive Accreditation Manual for Hospitals: The Official Handbook Table of Changes To update your manual, please remove and recycle the pages listed in this table of changes and insert the replacement
Comprehensive Accreditation Manual for Hospitals: The Official Handbook Table of Changes To update your manual, please remove and recycle the pages listed in this table of changes and insert the replacement
11/1/2016. Hospital Breakfast Briefing: Provision of Care, Treatment & Services. Publications and Record Restrictions.
 Hospital Breakfast Briefing: Provision of Care, Treatment & Services November 3, 2016 Steve Chinn, DPM, MS, MBA Consultant Joint Commission Resources 1 Hospital Breakfast Briefings Part 10 Disclosure Statement
Hospital Breakfast Briefing: Provision of Care, Treatment & Services November 3, 2016 Steve Chinn, DPM, MS, MBA Consultant Joint Commission Resources 1 Hospital Breakfast Briefings Part 10 Disclosure Statement
OBSTETRICAL ANESTHESIA
 DEPARTMENT OF ANESTHESIA RESIDENCY TRAINING PROGRAM UNIVERSITY OF MANITOBA OBSTETRICAL ANESTHESIA INTRODUCTION Residents will have the opportunity to gain experience in Obstetrical anesthesia in the course
DEPARTMENT OF ANESTHESIA RESIDENCY TRAINING PROGRAM UNIVERSITY OF MANITOBA OBSTETRICAL ANESTHESIA INTRODUCTION Residents will have the opportunity to gain experience in Obstetrical anesthesia in the course
NURSING GUIDELINES TO PROCEDURAL SEDATION Finalized 1/18/2012 Procedural Sedation Task Force
 Intention (responsiveness) Responds normally to commands Responds purposefully to verbal commands/or light touch DEEP Responds to pain Reflex withdrawal No response Anticipated Outcomes (Airway, Cardiovascular)
Intention (responsiveness) Responds normally to commands Responds purposefully to verbal commands/or light touch DEEP Responds to pain Reflex withdrawal No response Anticipated Outcomes (Airway, Cardiovascular)
Adult: Any person eighteen years of age or older, or emancipated minor.
 Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3)
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Post Anesthesia Care Unit (CA-1, CA-2, CA-3) Goals GOALS AND OBJECTIVES To analyze and interpret
Goals & Objectives. Name of Rotation: Pediatric Anesthesia Rotation: UCSF/Moffitt-Long. Supervisor: Marla Ferschl and Pediatric Anesthesia Faculty
 Goals & Objectives Name of Rotation: Pediatric Anesthesia Rotation: UCSF/Moffitt-Long Supervisor: Marla Ferschl and Pediatric Anesthesia Faculty Rotation Description: This is a month-long rotation for
Goals & Objectives Name of Rotation: Pediatric Anesthesia Rotation: UCSF/Moffitt-Long Supervisor: Marla Ferschl and Pediatric Anesthesia Faculty Rotation Description: This is a month-long rotation for
9/17/2018. Place of Service Type of Service Patient Status
 Place of Service Type of Service Patient Status 1 The first factor you must consider in code assingment is the place of service. Office Hospital Emergency Department Nursing Home Type of service is the
Place of Service Type of Service Patient Status 1 The first factor you must consider in code assingment is the place of service. Office Hospital Emergency Department Nursing Home Type of service is the
Nursing Documentation 101
 Nursing Documentation 101 Module 5: Applying Knowledge Part I Handout 2014 College of Licensed Practical Nurses of Alberta. All Rights Reserved. Nursing Documentation 101 Module 5: Applying Knowledge Part
Nursing Documentation 101 Module 5: Applying Knowledge Part I Handout 2014 College of Licensed Practical Nurses of Alberta. All Rights Reserved. Nursing Documentation 101 Module 5: Applying Knowledge Part
State of Connecticut REGULATION of. Department of Social Services. Payment of Behavioral Health Clinic Services
 R-39 Rev. 03/2012 (Title page) Page 1 of 17 IMPORTANT: Read instructions on back of last page (Certification Page) before completing this form. Failure to comply with instructions may cause disapproval
R-39 Rev. 03/2012 (Title page) Page 1 of 17 IMPORTANT: Read instructions on back of last page (Certification Page) before completing this form. Failure to comply with instructions may cause disapproval
Standards of Practice for Hospice Programs (2010) (Veteran-related Standards)
 Standards of Practice for Hospice Programs (2010) (Veteran-related Standards) National Hospice and Palliative Care Organizations (NHPCO) Standards of Practice for Hospice Programs (2010) is a valuable
Standards of Practice for Hospice Programs (2010) (Veteran-related Standards) National Hospice and Palliative Care Organizations (NHPCO) Standards of Practice for Hospice Programs (2010) is a valuable
LOUISIANA MEDICAID LEVEL OF CARE GUIDELINES
 Optum By United Behavioral Health U.S. Behavioral Health Plan, California Doing Business as OptumHealth Behavioral Solutions of California ( OHBS-CA ) LOUISIANA MEDICAID LEVEL OF CARE GUIDELINES Effective
Optum By United Behavioral Health U.S. Behavioral Health Plan, California Doing Business as OptumHealth Behavioral Solutions of California ( OHBS-CA ) LOUISIANA MEDICAID LEVEL OF CARE GUIDELINES Effective
ELIGIBILITY/REFERRAL, SCREENING, AND ADMISSION FORM COMAR
 6910 Annapolis Road Hyattsville, MD 20784 Telephone: (301) 925-9120 Fax: (301) 851-5199 4607 69 th Avenue Hyattsville, MD 20784 Telephone: (301) 386-0014 Fax: (301) 386-0018 ELIGIBILITY/REFERRAL, SCREENING,
6910 Annapolis Road Hyattsville, MD 20784 Telephone: (301) 925-9120 Fax: (301) 851-5199 4607 69 th Avenue Hyattsville, MD 20784 Telephone: (301) 386-0014 Fax: (301) 386-0018 ELIGIBILITY/REFERRAL, SCREENING,
Rules and Regulations St. Johns Hospital Medical Staff
 Rules and Regulations St. Johns Hospital Medical Staff Approved by MEC: 06/02/2014 Approved by Hospital Board 06/04/2014 MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS A. ADMISSION AND DISCHARGE
Rules and Regulations St. Johns Hospital Medical Staff Approved by MEC: 06/02/2014 Approved by Hospital Board 06/04/2014 MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS A. ADMISSION AND DISCHARGE
Hospice Clinical Record Review
 Purpose: Surveyors may use this worksheet when conducting clinical record reviews during a hospice survey. Directions: Fill in appropriate data. Table 1. Patient Information Patient Information Residence
Purpose: Surveyors may use this worksheet when conducting clinical record reviews during a hospice survey. Directions: Fill in appropriate data. Table 1. Patient Information Patient Information Residence
Procedure. Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013. Title: Universal Protocol / Time Out
 Title: Universal Protocol / Time Out Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013 Procedure Patient Age Group: ( ) N/A (X) All Ages ( ) Newborns ( ) Pediatric
Title: Universal Protocol / Time Out Applies To: UNM Hospitals Responsible Departments: All Revised: 9/2009 updated: 8/2013 Procedure Patient Age Group: ( ) N/A (X) All Ages ( ) Newborns ( ) Pediatric
Organization Review Process Guide Perinatal Care Certification
 Organization Review Process Guide Perinatal Care Certification 2016 Perinatal Care Certification Review Process Guide for Health Care Organizations 2016 What s New? Review process and contents of this
Organization Review Process Guide Perinatal Care Certification 2016 Perinatal Care Certification Review Process Guide for Health Care Organizations 2016 What s New? Review process and contents of this
Simulation Design Template. Location for Reflection:
 Simulation Design Template Date: Discipline: Expected Simulation Run Time: Location: Admission Date: Today s Date: Brief Description of Client Name: Gender: Age: Race: File Name: Student Level: Guided
Simulation Design Template Date: Discipline: Expected Simulation Run Time: Location: Admission Date: Today s Date: Brief Description of Client Name: Gender: Age: Race: File Name: Student Level: Guided
ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN)
 ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN) NAME: EMPLOYMENT/TRANSFER DATE: BLS RENEWAL DATE: ALLIANCE ORIENTATION DATE: HOSPITAL ORIENTATION DATE: NURSING ORIENTATION
ENDOSCOPY ORIENTATION COMPETENCY CLINICAL PLAN PROCEDURE REGISTERED NURSE (RN) NAME: EMPLOYMENT/TRANSFER DATE: BLS RENEWAL DATE: ALLIANCE ORIENTATION DATE: HOSPITAL ORIENTATION DATE: NURSING ORIENTATION
Review for Required Monitors
 Review for Required Monitors The Joint Commission Hospital Accreditation Manual, 2009 Medicare Conditions of Participation, Hospitals Update: February 2009 Indicator / Monitor Restraint, Medical (non-specific
Review for Required Monitors The Joint Commission Hospital Accreditation Manual, 2009 Medicare Conditions of Participation, Hospitals Update: February 2009 Indicator / Monitor Restraint, Medical (non-specific
Psychosocial Rehabilitation (PSR) H2017. Presented by the Clinical and Quality Teams September 2016
 Psychosocial Rehabilitation (PSR) H2017 Presented by the Clinical and Quality Teams After today s training you will be able to: Determine Department of Medical Assistance (DMAS) Medical Necessity Criteria
Psychosocial Rehabilitation (PSR) H2017 Presented by the Clinical and Quality Teams After today s training you will be able to: Determine Department of Medical Assistance (DMAS) Medical Necessity Criteria
This policy applies to any hospital staff, within KKUH/KAUH, who has privileges to enter data into medical records.
 King Khalid K University Hospital King Abdulaziz University Hospital Title: CLINICAL DOCUMENTATION Reviewed by: Date: Department: Unit: Policy Number: HWCPP - 005 Issue Date: DEC 2009 Prepared/Revised
King Khalid K University Hospital King Abdulaziz University Hospital Title: CLINICAL DOCUMENTATION Reviewed by: Date: Department: Unit: Policy Number: HWCPP - 005 Issue Date: DEC 2009 Prepared/Revised
TITLE: Processing Provider Orders: Inpatient and Outpatient
 POLICY and PROCEDURE TITLE: Processing Provider Orders: Inpatient and Outpatient Number: 13211 Version: 13211.10 Type: Patient Care Author: Carol Vanetti; Provider Order Policy Committee Effective Date:
POLICY and PROCEDURE TITLE: Processing Provider Orders: Inpatient and Outpatient Number: 13211 Version: 13211.10 Type: Patient Care Author: Carol Vanetti; Provider Order Policy Committee Effective Date:
NURSE MONITORING PROGRAM HANDBOOK
 Wyoming State Board of Nursing NURSE MONITORING PROGRAM HANDBOOK 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone: 307-777-7616 Fax: 307-777-3519 wsbn.nursemonitoring@wyo.gov I. Introduction Welcome
Wyoming State Board of Nursing NURSE MONITORING PROGRAM HANDBOOK 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone: 307-777-7616 Fax: 307-777-3519 wsbn.nursemonitoring@wyo.gov I. Introduction Welcome
Preparing your Patient for Surgery at The Valley Hospital
 Preparing your Patient for Surgery at The Valley Hospital Ensuring a smooth preoperative course to provide safe and efficient care Cristina Smith, RN, BSN, CPAN HOUSEKEEPING Bathroom location Cell Phone
Preparing your Patient for Surgery at The Valley Hospital Ensuring a smooth preoperative course to provide safe and efficient care Cristina Smith, RN, BSN, CPAN HOUSEKEEPING Bathroom location Cell Phone
Section 6: Referral record headings
 Section 6: Referral record headings Referral record standards: the referral headings are primarily intended for recording the clinical information in referral communication between general practitioners
Section 6: Referral record headings Referral record standards: the referral headings are primarily intended for recording the clinical information in referral communication between general practitioners
