medicaid Case Study: Georgia s Money Follows the Person Demonstration
|
|
|
- Rosemary Diana Dixon
- 5 years ago
- Views:
Transcription
1 I S S U E kaiser commission o n medicaid a n d t h e uninsured December 2011 P A P E R Case Study: Georgia s Money Follows the Person Demonstration Introduction The Georgia Department of Community Health (DCH) implemented the Money Follows the Person (MFP) rebalancing demonstration on September 1, DCH partnered with the Georgia Department of Behavioral Health and Developmental Disabilities (DBHDD) and the Georgia Department of Human Services Division of Aging Services (DHS/DAS) and other state and local agencies and organizations to create the first cross-agency initiative in Georgia s Medicaid program s history. In 2005, before the MFP demonstration began, Georgia s long-term care expenditures were $1.5 billion, with 70 percent of spending devoted to institutional long-term care and 30 percent on home and community-based services (HCBS). One goal of the MFP grant was to increase the percentage of dollars going toward home and community-based services to over 40 percent by the end of December Through MFP, Georgia has achieved a 2 percent growth in annual spending on home and community-based services as of December 31, The Money Follows the Person (MFP) demonstration is a Medicaid initiative designed to reduce reliance on institutional services and develop community-based long-term services and supports options. MFP was first authorized in the DRA of 2005 and then extended under the Affordable Care Act in MFP provides 365 days of enhanced federal funding to states to transition Medicaid individuals living in institutions back to the community. Medicaid beneficiaries must be residing in an institutional setting for at least 90 days to be eligible. Currently, 30 states, including DC, have operational MFP programs, twelve more states have received funding to begin a MFP demonstration program and two states demonstrations are inactive With the extension of MFP under the Affordable Care Act, the state plans to continue the demonstration program through By that time, Georgia is aiming to transition more than 2,000 individuals from institutions back to the community with the help of over $93 million in enhanced federal matching funds to facilitate these transitions. 2 This brief reports on a case study of Georgia s MFP demonstration. It describes key features of the program and highlights recent program experiences. For this case study, we interviewed staff members within the Department of Community Health (DCH) who were knowledgeable about the demonstration. We supplemented interview data with background information obtained from earlier Kaiser Commission on Medicaid and the Uninsured MFP surveys conducted in 2008, 2010 and 2011, as well as from state websites and press reports. Program Features Georgia MFP staff consists of a project director, a policy and planning specialist, data reporting manager, data specialist, housing manager, and an accountant. Georgia MFP operates through two interagency agreements an agreement with DBHDD to transition individuals with developmental disabilities from Intermediate Care Facilities (ICFs), and an agreement with DHS/DAS to transition older adults and people with physical disabilities from nursing facilities G S T R E E T N W, W A S H I N G T O N, D C P 3H 3O 0 N E G : 2S 0T 2R -E 3E 4T 7N- 5W 2, 7 0 W, AFS H A X I N: G2 T0 O2 N - 3, 4D 7C WP HEOB NS IE T: E 2: 0W2 W- 3W 4. 7K -F5F 2. 7O 0 R, G F A X : W E B S I T E : W W W. K F F. O R G
2 The MFP transition process is similar under both agreements both agencies conduct marketing, outreach, and screening of potential MFP participants. Both facilitate person-centered-planning and both facilitate transitions into Georgia HCBS waivers. Under the agreement with DBHDD, case expeditors and planning list administrators working in ICFs facilitate transitions. Under the agreement with DHS/DAS, options counselors and transition coordinators working from the 12 regional Aging and Disability Resource Centers (ADRCs) facilitate transitions. ADRCs are the designated state referral source for MDS Section Q referrals the section that allows individuals living in nursing facilities to express interest in learning more about living outside a nursing facility. Options counselors work with MDSQ referrals and assist individuals with information and referral to MFP. These interagency agreements increase capacity and leverage the resources and expertise of multiple agencies. In Georgia, MFP is a set of transition services designed to assist with relocation to the community using existing Georgia Medicaid home and community-based services waivers. Georgia MFP offers demonstration and transition services to qualified Medicaid eligible seniors, adults and children with physical disabilities, acquired brain injury (ABI), and developmental disabilities. 3 MFP transition coordinators assist participants with enrollment into appropriate waivers and then work with waiver case managers/care coordinators to ensure that waiver services begin on the day of discharge from the institution. For example, older adults can transition into the Elderly and Disabled waiver; adults with physical disabilities and/or ABI may enter the Elderly and Disabled waiver or the Independence Care waiver; and adults and children with developmental disabilities may enter the New Options Waiver (NOW) or the Comprehensive Waiver (COMP). 4 After receiving 365 days of MFP transition services, MFP participants continue to receive services through any or a combination of the following: the Medicaid waiver programs, Medicaid state plan services, state-funded programs, and local community support systems beyond the MFP demonstration period. In addition to HCBS waiver services, participants can receive the following MFP transition services: Peer Support, Trial visits to the community with Personal Support Services, Household furnishings, Household goods and supplies (including one-time purchase of groceries), Moving expenses, Utility deposits, Security deposits, Transition supports (a case-by-case, catch-all category includes assistance with obtaining documents and locating roommates), Transportation (in addition to non-emergency medical transportation), Skilled out-of-home respite, Caregiver training, Ombudsman visits, Equipment and Supplies (DME and Assistive Technology not covered by Medicaid), Vehicle Adaptations, and Environmental Modifications. 2
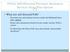
3 Nearly all MFP demonstrations promote self-direction (or consumer direction) of services. Selfdirection refers to various initiatives that give individual beneficiaries control over where, when, and how certain long-term support services are provided. Under Georgia MFP, no cash is exchanged but transition coordinators can set up consumer choice and control of services for the acquisition of household items. For example, working together, participants and transition coordinators determine needs for household items such home furnishings (up to a budget ceiling of $1,500) and goods and supplies ($750 ceiling), and MFP participants select these items. Outreach and Enrollment. Georgia DCH is the lead Medicaid agency and assumes the leadership role in MFP. Georgia MFP outreach and enrollment is accomplished through the interagency agreement/partnership with DBHDD and DHS/DAS. MFP staff produces media and outreach materials including brochures, posters, a MFP Participants Transition Planning Guide, and fact sheets to help participants understand the support and services available through MFP and HCBS waiver programs. 5 Medicaid beneficiaries, currently residing in nursing facilities and interested in enrolling in MFP, complete a referral form 6 that is then sent to the appropriate regional ADRC. ADRC options counselors receive direct referrals from individuals/family members and receive referrals from nursing facilities, including MDS Section Q referrals. Area Agencies on Aging, Centers for Independent Living, and other agencies also make referrals to MFP. Options counselors and MFP transition coordinators screen MFP candidates, assist with applications to appropriate waivers, facilitate person-centered planning for services, assist with housing searches and coordinate environmental modifications. During the first 365 days after transition, the transition coordinator checks in regularly to ensure quality and to inquire if additional services are needed. In addition to being assigned a transition coordinator, MFP participants enrolled in HCBS waivers receive the services of a waiver case manager someone who helps assess need for waiver services, understands the availability of services in the community and helps set up and monitor the individual s waiver service plan. Transition Progress As of June 30, 2011, 651 individuals have been transitioned back to the community and another 212 individuals were in the process of transitioning (Figure 1). Initially, the state set a goal of transitioning over 1,300 people by 2011 but like most states, that target was not achievable for several reasons. State officials faced challenges working across agencies and Distribution of Georgia MFP Transitions, by Target Population % 22% 47% Transitions Completed 3 Figure % 25% 54% Transitions in Progress!"#$%&'()*%$'+%(%,-$).-/%01$) *-2-(034-/5'()*%$'+%(%,-$) NOTE: In Georgia, individuals with mental illness were not part of the current benchmark transitions at the time of the survey. SOURCE: KCMU survey of state MFP demonstrations,
4 across disabilities. MFP was the first cross-agency initiative in the state s Medicaid program history. State officials reported problems related to performance contracting that limited their ability to control implementation and problems hiring competent transition coordinators. Georgia MFP is currently on track and has achieved the revised project benchmarks (618 individuals by December 2011) as directed by the Centers for Medicare and Medicaid Services (CMS). Table 1 shows the total number of MFP transitions by population group, as of June 30, Individuals with developmental disabilities, individuals with physical disabilities and seniors are the target groups most likely to be transitioned. Georgia is developing a mental health rehabilitation option state plan amendment to provide community services to people with severe mental illness, which will allow MFP to add this group as a target population. 7 MFP is developing new transition services for individuals with mental illness that will include life skills coaching/independent living skills training and community ombudsman visits. About 4 percent of MFP participants have been reinstitutionalized either to a hospital, nursing facility, or ICF. The rate of reinstitutionalization was highest among seniors. Georgia attributes its low rate of reinstitutionalization to a thorough transition planning process. TABLE 1. MFP Transitions by Population Group Number of Transitions Completed Number of Transitions in Progress Number of Participants Reinstitutionalized* Seniors NA People with Physical NA Disabilities People with NA Developmental Disabilities People with Mental Illness not part of current benchmark not part of current benchmark not part of current benchmark Total Source: Data reported by Georgia MFP state officials as of June 30, * Number of participants reinstitutionalized not available by type of disability. On average, Georgia MFP participants take less than 90 days to transition home. Affordable, accessible and integrated housing is the biggest barrier to transition. MFP participants complete the waiver assessment process, which takes an average of 60 days. During this time, participants work with transition coordinators to complete housing searches, make connections to community services (healthcare, recreational and employment) and set-up transportation services. MFP participants transition to different living arrangements depending on their disability and age. For example, most individuals with developmental disabilities transitioned to group homes with four or fewer unrelated adults; seniors most often returned to their own homes or a 4
5 relative s home; and individuals with physical disabilities most often moved to their own apartments with the help of housing choice vouchers or other public housing support. Key Partnerships Housing Finance Authority: Georgia MFP has partnered with the State Housing Finance Authority (the Department of Community Affairs-DCA, Rental Assistance Division) by developing a Housing Choice Voucher (HCV) program. DCA has provided 100 HCVs for use by MFP participants during the first four years of the demonstration. The DCA/MFP partnership has now expanded to include six Public Housing Authorities (PHAs) in metro areas in the state. DCA and these six PHAs applied for a total of 615 Category I and 310 Category II HCVs under a new Housing and Urban Development (HUD) Notice of Funding Availability (NOFA) for non-elderly persons with disabilities. The Decatur Housing Authority was awarded 35 Category II HCVs under the NOFA. Georgia MFP has referred MFP participants to Decatur HA to utilize these HCVs. Housing partners are seeking additional technical assistance through MFP from CMS to pursue a number of state-wide strategic initiatives including a state-wide referral network and inventory of available, accessible, affordable and integrated housing. Georgia MFP has also hired a housing manager in an effort to move this agenda forward. Georgia Centers for Independent Living (CILs): Georgia MFP has partnered with CILs throughout the state to provide a variety of support services to MFP participants. CILs are contacted to provide peer support and independent living skills training for MFP participants. CILs provide life skills coaching and independent living skills training. Additional services are being refined including life skills coaching and a community ombudsman role on a fee-for-service basis. Georgia Long-Term Care Ombudsman: Through a partnership with the Georgia longterm care ombudsman, monthly contacts with MFP participants are conducted to review participant health, welfare and safety. These are in addition to the contacts required by MFP and by each waiver case manager. The LTC ombudsman reports complaints and assists MFP participants to address service needs and facilitate on-going communication with transition coordinators and with waiver case managers in an effort to facilitate continuous quality improvement. Georgia Medicaid Infrastructure Grant (MIG): Georgia MFP has formed a new partnership with the University of Georgia Institute on Human Development and Disability, the MIG grantee, to develop an employment initiative for MFP participants. The initiative will focus on improving employment outcomes for MFP participants through person-centered career planning, the development and use of customized employment teams, the vocational discovery process and vocational profile, and links to community services for supported, customized and competitive employment opportunities. 5
6 Data and Evaluation CMS requires states to file quarterly reports each year and has contracted with Mathematica Policy Research (MPR) to perform data analysis on the MFP program. MPR s evaluation of MFP is designed to assess the effects of the transition program moving individuals back to the community as well as states progress in rebalancing their long-term care delivery systems using enhanced matching funds generated by these transitions. 8 In addition to the national level evaluation, Georgia MFP has partnered with the Georgia Health Policy Center (GHPC) at Georgia State University to evaluate the MFP program. GHPC has assisted with the creation of a project logic model so that Georgia can focus on state-specific evaluation metrics as the demonstration progresses. Preliminary findings from data collection and analysis of key evaluation questions on cost utilization, quality of life survey responses and performance measures are now available from the implementation of the demonstration in late CY 2008 through March Georgia Health Policy Center is also conducting first and second-year post transition interviews with MFP participants who have transitioned back to the community as part of the MFP evaluation. With assistance of GHPC, Georgia MFP is undertaking an analysis of per member per month Medicaid paid claims, however initial cost analysis was not complete at the time of this case study. Through March 2011, a total of $1.2 million MFP demonstration funds were spent in Georgia. More than 42% of those funds were spent on environmental modifications. The greatest number of services was provided in ombudsman visits followed by household goods and supplies and equipment and supplies. In January 2010, GHPC began conducting Quality of Life one-year follow-up interviews with individuals formerly enrolled in MFP, after their discharge date. Results were analyzed and reported for 167 follow-up interviews that were completed through June 15, Results from baseline interviews conducted by other project personnel have been compared with results from the follow-up data. The analysis included the entire population of participants and highlights of the findings included: Living situation - Analysis showed overall positive results since baseline, especially on happiness with the living situation and choice of living situation. A larger percentage of respondents could be by themselves, eat when they wanted to, and chose their own foods in the follow-up interviews than in the baseline interviews. Selection of personal care attendants - In follow-up interviews, 91 percent of respondents chose their own personal care attendants as compared to four percent at baseline (in the institution). Satisfaction A higher percentage of respondents were happy with how they lived their lives in the follow-up than in the baseline interviews. Outlook Looking ahead, Georgia MFP is working on adding mental health rehabilitation option services to the Medicaid state plan and MFP is developing new demonstration services with the hopes of transitioning more individuals with mental health needs. Georgia plans to increase outreach to housing authorities to expand the number of housing choice vouchers in metropolitan areas of the state. The MFP housing manager is leading this undertaking. Additionally, Georgia has plans to develop a direct services workforce study so that information about personal support 6
7 services jobs and training is readily available. Georgia is working to create a statewide training program of direct services workers in partnership with the Georgia Department of Labor. The state is expanding person-centered planning, self-direction, and employment opportunities for MFP participants. Finally, with the extension of the MFP demonstration through 2016 and new options to expand Medicaid home and community-based services included in the Affordable Care Act, there will be opportunities for Georgia and other states to expand the number of transitions so that more individuals with long-term services and supports needs can be served in community-based settings. This brief was prepared by Molly O Malley Watts, consultant to the Kaiser Commission on Medicaid and the Uninsured. Special thanks to R.L. Grubbs, Bill Daniels, Iris McIlvaine and other members of the Georgia Department of Community Health who contributed to the content and review of this brief When MFP was initially created in the Deficit Reduction Act of 2005, eligible participants were those individuals who had been residing in institutions for at least six months to two years. With the passage of health reform and the extension of the MFP program through 2016, individuals that reside in an institution for more than 90 consecutive days (not counting days of short-term rehabilitation under Medicare) are now eligible to participate and Noelle Denny-Brown et al., Money Follows the Person Demonstration: Overview of State Grantee Progress, January - June 2010, January 2011,
8 G S T R E E T N W, W A S H I N G T O N, D C P H O N E : ( ) , F A X : ( ) W E B S I T E : W W W. K F F. O R G / K C M U This publication (#8262) is available on the Kaiser Family Foundation s website at A d d i t i o n a l c o p i e s o f t h i s r e p o r t ( # ) a r e a v a i l a b l e o n t h e K a i s e r F a m i l y F o u n d a t i o n s w e b s i t e a t w w w. k f f. o r g. The Kaiser Commission on Medicaid and the Uninsured provides information and analysis on health care coverage and access for the lowincome population, with a special focus on Medicaid s role and coverage of the uninsured. Begun in 1991 and based in the Kaiser Family Foundation's Washington, DC office, the Commission is the largest operating program of the Foundation. The Commission's work is conducted by Foundation staff under the guidance of a bi-partisan group of national leaders and experts in health care and public policy.
MFP enacted into law as part of the DRA. SOURCE: KCMU surveys of state MFP demonstration programs in
 I S S U E P A P E R kaiser commission on medicaid and the uninsured February 2013 Money Follows the Person: A 2012 Survey of Transitions, Services and Costs EXECUTIVE SUMMARY A total of 46 states, including
I S S U E P A P E R kaiser commission on medicaid and the uninsured February 2013 Money Follows the Person: A 2012 Survey of Transitions, Services and Costs EXECUTIVE SUMMARY A total of 46 states, including
Tennessee s Money Follows the Person Demonstration: Supporting Rebalancing in a Managed Long-Term Services and Supports Model
 Tennessee s Money Follows the Person Demonstration: Supporting Rebalancing in a Managed Long-Term Services and Supports Model In 2011, Tennessee was awarded a federal Money Follows the Person (MFP) grant,
Tennessee s Money Follows the Person Demonstration: Supporting Rebalancing in a Managed Long-Term Services and Supports Model In 2011, Tennessee was awarded a federal Money Follows the Person (MFP) grant,
Improving the Continuum of Care: Progress on Selected Provisions of the Affordable Care Act One Year Post-Passage
 Improving the Continuum of Care: Progress on Selected Provisions of the Affordable Care Act One Year Post-Passage March 23, 2011 marks the oneyear anniversary of the signing of the Patient Protection and
Improving the Continuum of Care: Progress on Selected Provisions of the Affordable Care Act One Year Post-Passage March 23, 2011 marks the oneyear anniversary of the signing of the Patient Protection and
MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and s September 22, 2010
 MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and emails September 22, 2010 DATA USE AGREEMENTS (DUA) 1. Do state agencies need a Data Use Agreement to implement
MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and emails September 22, 2010 DATA USE AGREEMENTS (DUA) 1. Do state agencies need a Data Use Agreement to implement
KENTUCKY DECEMBER 7, Cabinet for Health and Family Services HOME AND COMMUNITY BASED SERVICES (HCBS) WAIVER REDESIGN
 KENTUCKY Cabinet for Health and Family HOME AND COMMUNITY BASED SERVICES (HCBS) WAIVER REDESIGN DECEMBER 7, 2016 Session Timeline Time Topic 9:30 9:45 AM Welcome: Introductions & Agenda Review 9:45 10:15
KENTUCKY Cabinet for Health and Family HOME AND COMMUNITY BASED SERVICES (HCBS) WAIVER REDESIGN DECEMBER 7, 2016 Session Timeline Time Topic 9:30 9:45 AM Welcome: Introductions & Agenda Review 9:45 10:15
Long-Term Services and Supports (LTSS): Medicaid s Role and Options for States
 Long-Term Services and Supports (LTSS): Medicaid s Role and Options for States Erica L. Reaves, Policy Analyst State Variation in Long-Term Services and Supports: Location, Location, Location National
Long-Term Services and Supports (LTSS): Medicaid s Role and Options for States Erica L. Reaves, Policy Analyst State Variation in Long-Term Services and Supports: Location, Location, Location National
Money Follows the Person (MFP) Update
 Money Follows the Person (MFP) Update January 2017 General Transition Information 570 Consumers have transitioned out of the ICF/ID or a Nursing facility since September 2008 32 Consumers have transitioned
Money Follows the Person (MFP) Update January 2017 General Transition Information 570 Consumers have transitioned out of the ICF/ID or a Nursing facility since September 2008 32 Consumers have transitioned
A Snapshot of the Connecticut LTSS Rebalancing Agenda
 A Snapshot of the Connecticut LTSS Rebalancing Agenda Agenda Medicaid context and vision State Rebalancing Plan Major elements of rebalancing agenda Money Follows the Person, Nursing Home Rightsizing,
A Snapshot of the Connecticut LTSS Rebalancing Agenda Agenda Medicaid context and vision State Rebalancing Plan Major elements of rebalancing agenda Money Follows the Person, Nursing Home Rightsizing,
The Patient Protection and Affordable Care Act (Public Law )
 Policy Brief No. 2 March 2010 A Summary of the Patient Protection and Affordable Care Act (P.L. 111-148) and Modifications by the On March 23, 2010, President Obama signed into law the Patient Protection
Policy Brief No. 2 March 2010 A Summary of the Patient Protection and Affordable Care Act (P.L. 111-148) and Modifications by the On March 23, 2010, President Obama signed into law the Patient Protection
Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States
 Advancing innovations in health care delivery for low-income Americans Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States March 6, 2018 Michelle Herman Soper and Alexandra
Advancing innovations in health care delivery for low-income Americans Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States March 6, 2018 Michelle Herman Soper and Alexandra
Home and Community-Based Waivers: Opportunities for Community Living for ABI Survivors
 Home and Community-Based Waivers: Opportunities for Community Living for ABI Survivors BIA-MA Brain Injury Conference March 30, 2017 Amy Bernstein Director, Community Based Waivers MassHealth Dorothée
Home and Community-Based Waivers: Opportunities for Community Living for ABI Survivors BIA-MA Brain Injury Conference March 30, 2017 Amy Bernstein Director, Community Based Waivers MassHealth Dorothée
A Self-Advocate s Guide to Medicaid
 Plain Text Edition A Self-Advocate s Guide to Medicaid Part 3: What Does Medicaid Pay For? 1 3. What Does Medicaid Pay For? What services does Medicaid cover? Medicaid coverage refers to what services
Plain Text Edition A Self-Advocate s Guide to Medicaid Part 3: What Does Medicaid Pay For? 1 3. What Does Medicaid Pay For? What services does Medicaid cover? Medicaid coverage refers to what services
Bringing Permanent Supportive Housing to Scale
 Section 811 Project Rental Assistance Bringing Permanent Supportive Housing to Scale Status Report to Congress U.S. Department of Housing and Urban Development Office of Multifamily Housing Programs January
Section 811 Project Rental Assistance Bringing Permanent Supportive Housing to Scale Status Report to Congress U.S. Department of Housing and Urban Development Office of Multifamily Housing Programs January
Living Choice and the Aging and Disability Resource Consortium Nursing Facility Transition. Abstract
 Living Choice and the Aging and Disability Resource Consortium Nursing Facility Transition Abstract The Oklahoma Health Care Authority (OHCA), in partnership with the Oklahoma Department of Human Services
Living Choice and the Aging and Disability Resource Consortium Nursing Facility Transition Abstract The Oklahoma Health Care Authority (OHCA), in partnership with the Oklahoma Department of Human Services
A Self-Advocate s Guide to Medicaid
 Easy Read Edition A Self-Advocate s Guide to Medicaid Part 3: What Does Medicaid Pay For? 1 3. What Does Medicaid Pay For? What services does Medicaid cover? Medicaid coverage refers to what services are
Easy Read Edition A Self-Advocate s Guide to Medicaid Part 3: What Does Medicaid Pay For? 1 3. What Does Medicaid Pay For? What services does Medicaid cover? Medicaid coverage refers to what services are
New Opportunities in Long Term Services and Supports
 Profiles of State Innovation: Long -Term Supports and Services CHCS Webinar November 22, 1010 New Opportunities in Long Term Services and Supports Mary Sowers Director, Division of Community and Institutional
Profiles of State Innovation: Long -Term Supports and Services CHCS Webinar November 22, 1010 New Opportunities in Long Term Services and Supports Mary Sowers Director, Division of Community and Institutional
Real Choice Systems Change Grant Program
 August 2006 Real Choice Systems Change Grant Program FY 2001 Nursing Facility Transition Grantees: Final Report Janet O Keeffe, Dr.P.H., R.N. Christine O Keeffe, B.A. Kristin Siebenaler, M.P.A. David Brown,
August 2006 Real Choice Systems Change Grant Program FY 2001 Nursing Facility Transition Grantees: Final Report Janet O Keeffe, Dr.P.H., R.N. Christine O Keeffe, B.A. Kristin Siebenaler, M.P.A. David Brown,
programs and briefly describes North Carolina Medicaid s preliminary
 State Experiences with Managed Long-term Care in Medicaid* Brian Burwell Vice President, Chronic Care and Disability Medstat Abstract: Across the country, state Medicaid programs are expressing renewed
State Experiences with Managed Long-term Care in Medicaid* Brian Burwell Vice President, Chronic Care and Disability Medstat Abstract: Across the country, state Medicaid programs are expressing renewed
1915(k) Community First Choice Overview
 1915(k) Community First Choice Overview 1 Today s Objectives 1. Brief overview of Community First Choice (CFC) Program & Key Features Other materials available: http://www.medicaid.gov/medicaid-chip-program-information/by-topics/longterm-services-and-supports/home-and-community-based-services/communityfirst-choice-1915-k.html\
1915(k) Community First Choice Overview 1 Today s Objectives 1. Brief overview of Community First Choice (CFC) Program & Key Features Other materials available: http://www.medicaid.gov/medicaid-chip-program-information/by-topics/longterm-services-and-supports/home-and-community-based-services/communityfirst-choice-1915-k.html\
5/30/2012
 The Affordable Care Act Background Coverage Long-term Care Home and Community Based Services Payment Delivery Care Transitions Assuring Quality Supreme Court 5/30/2012 www.nasuad.org BACKGROUND Health
The Affordable Care Act Background Coverage Long-term Care Home and Community Based Services Payment Delivery Care Transitions Assuring Quality Supreme Court 5/30/2012 www.nasuad.org BACKGROUND Health
1915(j) Self-Directed Personal Assistance Services State Plan Option
 1915(j) Self-Directed Personal Assistance Services State Plan Option What are self-directed PAS? 1 Personal care and related services under the Medicaid State plan, and/or Home and community-based services
1915(j) Self-Directed Personal Assistance Services State Plan Option What are self-directed PAS? 1 Personal care and related services under the Medicaid State plan, and/or Home and community-based services
COMMUNITY-BASED LONG TERM CARE PROGRAMS IN WISCONSIN. Attorney Mitchell Hagopian Disability Rights Wisconsin July 2013
 COMMUNITY-BASED LONG TERM CARE PROGRAMS IN WISCONSIN I. INTRODUCTION Attorney Mitchell Hagopian Disability Rights Wisconsin July 2013 In 1981, with the creation of the Community Options Program, the state
COMMUNITY-BASED LONG TERM CARE PROGRAMS IN WISCONSIN I. INTRODUCTION Attorney Mitchell Hagopian Disability Rights Wisconsin July 2013 In 1981, with the creation of the Community Options Program, the state
kaiser medicaid and the uninsured commission on
 I S S U E P A P E R kaiser commission on medicaid and the uninsured A Challenge for States: Assuring Timely Access to Optimal Long-Term Services and Supports in the Community Executive Summary February
I S S U E P A P E R kaiser commission on medicaid and the uninsured A Challenge for States: Assuring Timely Access to Optimal Long-Term Services and Supports in the Community Executive Summary February
Long Term Care Delivery System
 Long Term Care Delivery System October 26-27 th, 2005 Charles Milligan, JD, MPH Medicaid Commission Meeting Preview of Presentation Medicaid long-term care Waivers in long-term care Dual eligibles Challenges
Long Term Care Delivery System October 26-27 th, 2005 Charles Milligan, JD, MPH Medicaid Commission Meeting Preview of Presentation Medicaid long-term care Waivers in long-term care Dual eligibles Challenges
The Money Follows the Person (MFP) Demonstration supports state efforts to help Medicaid
 THE NATIONAL EVALUATION OF THE MONEY FOLLOWS THE PERSON (MFP) DEMONSTRATION GRANT PROGRAM R E P O R T S F R O M T H E F I E L D Post-Institutional Services of MFP Participants: Use and Costs of Community
THE NATIONAL EVALUATION OF THE MONEY FOLLOWS THE PERSON (MFP) DEMONSTRATION GRANT PROGRAM R E P O R T S F R O M T H E F I E L D Post-Institutional Services of MFP Participants: Use and Costs of Community
NH Community Passport Program - CASE STUDY (HCBC-CHOICES FOR INDEPENDENCE WAIVER)
 NH Community Passport Program - CASE STUDY (HCBC-CHOICES FOR INDEPENDENCE WAIVER) For seven years Jeannette Gendron was a resident of the Hillsborough County Home in Goffstown. A native of Manchester,
NH Community Passport Program - CASE STUDY (HCBC-CHOICES FOR INDEPENDENCE WAIVER) For seven years Jeannette Gendron was a resident of the Hillsborough County Home in Goffstown. A native of Manchester,
Housing as Health Care Webinar. Wrapping Tenancy Supports into Your Housing Strategy
 Housing as Health Care Webinar Wrapping Tenancy Supports into Your Housing Strategy National Governors Association Friday, October 28th, 2016 12-1pm EST Dial-in: 888-858-6021; Passcode 2026245354 1 Agenda
Housing as Health Care Webinar Wrapping Tenancy Supports into Your Housing Strategy National Governors Association Friday, October 28th, 2016 12-1pm EST Dial-in: 888-858-6021; Passcode 2026245354 1 Agenda
Section Q. Participation in Assessment and Goal Setting
 Section Q Participation in Assessment and Goal Setting Changes to Section Q MDS 2.0 MDS 3.0 Discharge Potential item asked the assessor if the resident expressed a preference to return to the community
Section Q Participation in Assessment and Goal Setting Changes to Section Q MDS 2.0 MDS 3.0 Discharge Potential item asked the assessor if the resident expressed a preference to return to the community
Long-Term Care Glossary
 Long-Term Care Glossary Adjudicated Claim Activities of Daily Living (ADL) A claim that has reached final disposition such that it is either paid or denied. Basic tasks individuals perform in the course
Long-Term Care Glossary Adjudicated Claim Activities of Daily Living (ADL) A claim that has reached final disposition such that it is either paid or denied. Basic tasks individuals perform in the course
In Tune With Respite. One State s Experience Integrating Respite Into. Health Care Reform
 In Tune With Respite One State s Experience Integrating Respite Into Health Care Reform National Respite Conference Nashville, TN October 8, 2014 Purpose To share South Carolina s experience in building
In Tune With Respite One State s Experience Integrating Respite Into Health Care Reform National Respite Conference Nashville, TN October 8, 2014 Purpose To share South Carolina s experience in building
Long-Term Care Improvements under the Affordable Care Act (ACA)
 Long-Term Care Improvements under the Affordable Care Act (ACA) South Carolina Health Care Implementation Coalition September 17, 2010 JoAnn Lamphere, DrPH Director, State Government Relations Health &
Long-Term Care Improvements under the Affordable Care Act (ACA) South Carolina Health Care Implementation Coalition September 17, 2010 JoAnn Lamphere, DrPH Director, State Government Relations Health &
DEPARTMENT OF ELDER AFFAIRS PROGRAMS AND SERVICES HANDBOOK. Chapter 3. Description of DOEA Coordination With Other State and Federal Programs
 Chapter 3 Description of DOEA Coordination With Other State and Federal Programs TABLE OF CONTENTS Section: Topic Page I. Overview and Specific Legal Authority 3-3 II. 3-5 A. Adult Care Food Program 3-5
Chapter 3 Description of DOEA Coordination With Other State and Federal Programs TABLE OF CONTENTS Section: Topic Page I. Overview and Specific Legal Authority 3-3 II. 3-5 A. Adult Care Food Program 3-5
Alaska Mental Health Trust Authority. Medicaid
 Alaska Mental Health Trust Authority Medicaid November 20, 2014 Background Why focus on Medicaid? Trust result desired in working on Medicaid policy issues and in implementing several of our focus area
Alaska Mental Health Trust Authority Medicaid November 20, 2014 Background Why focus on Medicaid? Trust result desired in working on Medicaid policy issues and in implementing several of our focus area
Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps
 I S S U E P A P E R kaiser commission on medicaid and the uninsured March 2004 Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps In 2000, over 7 million people were dual eligibles, low-income
I S S U E P A P E R kaiser commission on medicaid and the uninsured March 2004 Dual Eligibles: Medicaid s Role in Filling Medicare s Gaps In 2000, over 7 million people were dual eligibles, low-income
Request for an Amendment to a 1915(c) Home and Community-Based Services Waiver
 Page 1 of 11 Request for an Amendment to a 1915(c) Home and Community-Based Services Waiver 1. Request Information A. The State of North Carolina requests approval for an amendment to the following Medicaid
Page 1 of 11 Request for an Amendment to a 1915(c) Home and Community-Based Services Waiver 1. Request Information A. The State of North Carolina requests approval for an amendment to the following Medicaid
Implementing the Affordable Care Act:
 Implementing the Affordable Care Act: Making it Easier For Individuals to Navigate Their Health and Long Term Care 26 th National Home and Community Based Services Conference Tuesday, September 28, 2010
Implementing the Affordable Care Act: Making it Easier For Individuals to Navigate Their Health and Long Term Care 26 th National Home and Community Based Services Conference Tuesday, September 28, 2010
Subtitle E New Options for States to Provide Long-Term Services and Supports
 LONG TERM CARE (SECTION-BY-SECTION ANALYSIS) (Information compiled from the Democratic Policy Committee (DPC) Report on The Patient Protection and Affordable Care Act and the Health Care and Education
LONG TERM CARE (SECTION-BY-SECTION ANALYSIS) (Information compiled from the Democratic Policy Committee (DPC) Report on The Patient Protection and Affordable Care Act and the Health Care and Education
Diamond State Health Plan Plus
 I N T E G R A T E D L O N G T E R M Diamond State Health Plan Plus DSHP-Plus C A R E 1115 Demonstration Waiver Diamond State Health Plan (DSHP) Managed Care Delivery System Operational since January 1996
I N T E G R A T E D L O N G T E R M Diamond State Health Plan Plus DSHP-Plus C A R E 1115 Demonstration Waiver Diamond State Health Plan (DSHP) Managed Care Delivery System Operational since January 1996
Housing HOME Program HUD $2.25 billion To be used for capital investments in Assure HPRP program staff
 List of Funded Programs and Opportunities Housing Community HUD $1 billion Provides communities with funding to Assure HPRP program staff Development Block ensure affordable housing. 70 percent are aware
List of Funded Programs and Opportunities Housing Community HUD $1 billion Provides communities with funding to Assure HPRP program staff Development Block ensure affordable housing. 70 percent are aware
PUBLIC MEETING LONG-TERM CARE WAIVER ENROLLMENT MANAGEMENT SYSTEM (EMS) Presented by: Florida Department of Elder Affairs Staff
 PUBLIC MEETING LONG-TERM CARE WAIVER ENROLLMENT MANAGEMENT SYSTEM (EMS) Rick Scott, Governor Charles T. Corley, Secretary Presented by: Florida Department of Elder Affairs Staff Introductions & Purpose
PUBLIC MEETING LONG-TERM CARE WAIVER ENROLLMENT MANAGEMENT SYSTEM (EMS) Rick Scott, Governor Charles T. Corley, Secretary Presented by: Florida Department of Elder Affairs Staff Introductions & Purpose
Home and Community Based Services Mental Retardation/Developmental Disabilities Providers
 May 2008 Provider Bulletin Number 869 Home and Community Based Services Mental Retardation/Developmental Disabilities Providers Manual Updates and New Manuals Home and Community Based Services Mental Retardation/Developmental
May 2008 Provider Bulletin Number 869 Home and Community Based Services Mental Retardation/Developmental Disabilities Providers Manual Updates and New Manuals Home and Community Based Services Mental Retardation/Developmental
Statewide Medicaid Managed Care Long-term Care Program
 Statewide Medicaid Managed Care Long-term Care Program Justin Senior Deputy Secretary for Medicaid Agency for Health Care Administration July 25, 2013 Presentation Overview Current Medicaid Snapshot and
Statewide Medicaid Managed Care Long-term Care Program Justin Senior Deputy Secretary for Medicaid Agency for Health Care Administration July 25, 2013 Presentation Overview Current Medicaid Snapshot and
Home Care Ombudsman Expansion. Lyle VanDeventer, Deputy State Home Care Ombudsman (v)
 Home Care Ombudsman Expansion Lyle VanDeventer, Deputy State Home Care Ombudsman 217.557.1532 (v) lyle.vandeventer@illinois.gov Service Integration February 22, 2013, the Centers for Medicare and Medicaid
Home Care Ombudsman Expansion Lyle VanDeventer, Deputy State Home Care Ombudsman 217.557.1532 (v) lyle.vandeventer@illinois.gov Service Integration February 22, 2013, the Centers for Medicare and Medicaid
MEDICAID MANAGED LONG-TERM SERVICES AND SUPPORTS OPPORTUNITIES FOR INNOVATIVE PROGRAM DESIGN
 Louisiana Behavioral Health Partnership MEDICAID MANAGED LONG-TERM SERVICES AND SUPPORTS OPPORTUNITIES FOR INNOVATIVE PROGRAM DESIGN Rosanne Mahaney - Delaware Lou Ann Owen - Louisiana Brenda Jackson,
Louisiana Behavioral Health Partnership MEDICAID MANAGED LONG-TERM SERVICES AND SUPPORTS OPPORTUNITIES FOR INNOVATIVE PROGRAM DESIGN Rosanne Mahaney - Delaware Lou Ann Owen - Louisiana Brenda Jackson,
Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10
 Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10 On March 23, 2010, President Obama signed a comprehensive health care reform bill (H.R. 3590) into law. On March
Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10 On March 23, 2010, President Obama signed a comprehensive health care reform bill (H.R. 3590) into law. On March
Supporting MLTSS Consumers through Problem Resolution and Advocacy
 Supporting MLTSS Consumers through Problem Resolution and Advocacy James David Toews, Becky A. Kurtz, Eliza Bangit September 11, 2013 Risks of Managed Long-Term Services and Supports (MLTSS) Many managed
Supporting MLTSS Consumers through Problem Resolution and Advocacy James David Toews, Becky A. Kurtz, Eliza Bangit September 11, 2013 Risks of Managed Long-Term Services and Supports (MLTSS) Many managed
Asset Transfer and Nursing Home Use
 I S S U E kaiser commission on medicaid and the uninsured November 2005 P A P E R Issue Asset Transfer and Nursing Home Use Medicaid paid for nearly half of the $183 billion spent nationally for long-term
I S S U E kaiser commission on medicaid and the uninsured November 2005 P A P E R Issue Asset Transfer and Nursing Home Use Medicaid paid for nearly half of the $183 billion spent nationally for long-term
Expanded Developmental Disability/Delay Acronym Index
 Expanded Developmental Disability/Delay Acronym Index 1 BI Waiver: Brain Injury Waiver Provides home and community based Medicaid benefits as an alternative to hospital or specialized nursing facility
Expanded Developmental Disability/Delay Acronym Index 1 BI Waiver: Brain Injury Waiver Provides home and community based Medicaid benefits as an alternative to hospital or specialized nursing facility
NEW YORK STATE MEDICAID REDESIGN TEAM AND THE AFFORDABLE CARE ACT (MRT & ACA)
 NEW YORK STATE MEDICAID REDESIGN TEAM AND THE AFFORDABLE CARE ACT (MRT & ACA) The Affordable Care Act (ACA) The Affordable Care Act 3 Officially called the Patient Protection and Affordable Care Act (PPACA)
NEW YORK STATE MEDICAID REDESIGN TEAM AND THE AFFORDABLE CARE ACT (MRT & ACA) The Affordable Care Act (ACA) The Affordable Care Act 3 Officially called the Patient Protection and Affordable Care Act (PPACA)
Housing Authority of Travis County. PHA 5 Year Plan. form HUD (1/2007) Page 1 of 7
 Housing Authority of Travis County PHA 5 Year Plan 2015 form HUD-50075 (1/2007) Page 1 of 7 PHA 5-Year and Annual Plan U.S. Department of Housing and Urban Development Office of Public and Indian Housing
Housing Authority of Travis County PHA 5 Year Plan 2015 form HUD-50075 (1/2007) Page 1 of 7 PHA 5-Year and Annual Plan U.S. Department of Housing and Urban Development Office of Public and Indian Housing
Maryland Department of Health and Mental Hygiene FY 2012 Memorandum of Understanding Annual Report of Activities and Accomplishments Highlights
 Maryland Department of Health and Mental Hygiene FY 2012 Memorandum of Understanding Annual Report of Activities and Accomplishments Highlights A Nationally Recognized Partnership Hilltop was founded on
Maryland Department of Health and Mental Hygiene FY 2012 Memorandum of Understanding Annual Report of Activities and Accomplishments Highlights A Nationally Recognized Partnership Hilltop was founded on
kaiser medicaid and the uninsured commission on O L I C Y
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured 1330 G S T R E E T NW, W A S H I N G T O N, DC 20005 P H O N E: (202) 347-5270, F A X: ( 202) 347-5274 W E B S I T E: W W W. K F F.
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured 1330 G S T R E E T NW, W A S H I N G T O N, DC 20005 P H O N E: (202) 347-5270, F A X: ( 202) 347-5274 W E B S I T E: W W W. K F F.
Office of Developmental Programs Service Descriptions
 1 Office of Developmental Programs Descriptions *The service descriptions below do not represent the comprehensive Definition as listed in each of the Waivers. Please refer to the appropriate Waiver Program
1 Office of Developmental Programs Descriptions *The service descriptions below do not represent the comprehensive Definition as listed in each of the Waivers. Please refer to the appropriate Waiver Program
Updated TRANSITION PLAN TO IMPLEMENT THE SETTINGS REQUIREMENT FOR HOME AND COMMUNITY BASED SERVICES CMS FINAL RULE OF JANUARY 2014
 State of Rhode Island & Providence Plantations Updated TRANSITION PLAN TO IMPLEMENT THE SETTINGS REQUIREMENT FOR HOME AND COMMUNITY BASED SERVICES CMS FINAL RULE OF JANUARY 2014 June 7, 2018 Summary...
State of Rhode Island & Providence Plantations Updated TRANSITION PLAN TO IMPLEMENT THE SETTINGS REQUIREMENT FOR HOME AND COMMUNITY BASED SERVICES CMS FINAL RULE OF JANUARY 2014 June 7, 2018 Summary...
NJ Department of Human Services NJ Ombudsman for the Institutionalized Elderly
 NJ Department of Human Services NJ Ombudsman for the Institutionalized Elderly 1 Agenda What is MFP/ I Choose Home NJ? Outreach and Marketing Transition Process CMS Requirements for Quality Management
NJ Department of Human Services NJ Ombudsman for the Institutionalized Elderly 1 Agenda What is MFP/ I Choose Home NJ? Outreach and Marketing Transition Process CMS Requirements for Quality Management
SUPPORTING CONSUMERS WHO TRANSITION OUT OF NURSING HOMES
 SUPPORTING CONSUMERS WHO TRANSITION OUT OF NURSING HOMES What Consumers Say Long-Term Care Ombudsmen: Supporting the Consumer Local LTCO Experience Supporting Consumers Monday, July 14, 2014 WHAT CONSUMERS
SUPPORTING CONSUMERS WHO TRANSITION OUT OF NURSING HOMES What Consumers Say Long-Term Care Ombudsmen: Supporting the Consumer Local LTCO Experience Supporting Consumers Monday, July 14, 2014 WHAT CONSUMERS
MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and s June 7, 2010
 MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and emails June 7, 2010 DATA USE AGREEMENTS (DUA) 1. Do state agencies need a Data Use Agreement to implement
MDS 3.0 Section Q Implementation Questions and Answers from Informing LTC Choice conference and emails June 7, 2010 DATA USE AGREEMENTS (DUA) 1. Do state agencies need a Data Use Agreement to implement
Coverage of Behavioral Health Services for Children, Youth, and Young Adults with Significant Mental Health Conditions
 Coverage of Behavioral Health Services for Children, Youth, and Young Adults with Significant Mental Health Conditions Webinar Website: http://gucchdtacenter.georgetown.edu/resources/tawebinars.html Coverage
Coverage of Behavioral Health Services for Children, Youth, and Young Adults with Significant Mental Health Conditions Webinar Website: http://gucchdtacenter.georgetown.edu/resources/tawebinars.html Coverage
Medicaid 201: Home and Community Based Services
 Medicaid 201: Home and Community Based Services Kathy Poisal Division of Long Term Services and Supports Disabled and Elderly Health Programs Group Center for Medicaid and CHIP Services Centers for Medicare
Medicaid 201: Home and Community Based Services Kathy Poisal Division of Long Term Services and Supports Disabled and Elderly Health Programs Group Center for Medicaid and CHIP Services Centers for Medicare
Medicaid Home- and Community-Based Waiver Programs
 INFORMATION BRIEF Research Department Minnesota House of Representatives 600 State Office Building St. Paul, MN 55155 Danyell Punelli, Legislative Analyst 651-296-5058 Updated: October 2016 Medicaid Home-
INFORMATION BRIEF Research Department Minnesota House of Representatives 600 State Office Building St. Paul, MN 55155 Danyell Punelli, Legislative Analyst 651-296-5058 Updated: October 2016 Medicaid Home-
Rebalancing Long-Term Care Systems in Arkansas: Case Study as of December 2007
 Rebalancing Long-Term Care Systems in : Case Study as of December 2007 Submitted to the Centers for Medicare & Medicaid Services (CMS), Advocacy and Special Initiatives Division CMS Project Officer, Kate
Rebalancing Long-Term Care Systems in : Case Study as of December 2007 Submitted to the Centers for Medicare & Medicaid Services (CMS), Advocacy and Special Initiatives Division CMS Project Officer, Kate
Community Outreach, Engagement, and Volunteerism
 Community Outreach, Engagement, and Volunteerism Overview To address demographic shifts in the Texas population, DADS provides additional supports to state government, local communities, and individuals
Community Outreach, Engagement, and Volunteerism Overview To address demographic shifts in the Texas population, DADS provides additional supports to state government, local communities, and individuals
NEW YORK STATE MEDICAID PROGRAM OFFICE OF MENTAL RETARDATION AND DEVELOPMENTAL DISABILITIES HOME AND COMMUNITY BASED SERVICES WAIVER MANUAL
 NEW YORK STATE MEDICAID PROGRAM OFFICE OF MENTAL RETARDATION AND DEVELOPMENTAL DISABILITIES HOME AND COMMUNITY BASED SERVICES WAIVER MANUAL POLICY GUIDELINES Table of Contents SECTION I - DESCRIPTION OF
NEW YORK STATE MEDICAID PROGRAM OFFICE OF MENTAL RETARDATION AND DEVELOPMENTAL DISABILITIES HOME AND COMMUNITY BASED SERVICES WAIVER MANUAL POLICY GUIDELINES Table of Contents SECTION I - DESCRIPTION OF
City of Tyler Housing Agency s FY FY Year Plan
 City of Tyler Housing Agency s FY 2015- FY 2019 5-Year Plan City of Tyler Housing Agency s FY 2015 - FY 2019 5-Year Plan This section defines the quantifiable accomplishments of the goals and objectives
City of Tyler Housing Agency s FY 2015- FY 2019 5-Year Plan City of Tyler Housing Agency s FY 2015 - FY 2019 5-Year Plan This section defines the quantifiable accomplishments of the goals and objectives
PHA 5-Year and Annual Plan
 PHA 5-Year and Annual Plan U.S. Department of Housing and Urban Development Office of Public and Indian Housing OMB No. 2577-0226 Expires 4/30/2011 1.0 PHA Information PHA Name: HOUSING AUTHORITY OF THE
PHA 5-Year and Annual Plan U.S. Department of Housing and Urban Development Office of Public and Indian Housing OMB No. 2577-0226 Expires 4/30/2011 1.0 PHA Information PHA Name: HOUSING AUTHORITY OF THE
DEPARTMENT OF ELDER AFFAIRS PROGRAMS AND SERVICES HANDBOOK. Chapter 3. Description of DOEA Coordination with Other State and Federal Programs
 Chapter 3 Description of DOEA Coordination with Other State and Federal Programs TABLE OF CONTENTS Section: Topic Page I. Overview and Specific Legal Authority 3-3 II. 3-5 A. Adult Care Food Program 3-5
Chapter 3 Description of DOEA Coordination with Other State and Federal Programs TABLE OF CONTENTS Section: Topic Page I. Overview and Specific Legal Authority 3-3 II. 3-5 A. Adult Care Food Program 3-5
The Commission on Long-Term Care: Background Behind the Mission
 THE BASICS The Commission on Long-Term Care: Background Behind the Mission As part of the American Taxpayer Relief Act of 2012 (ATRA, P.L. 112-240), Congress created a Commission on Long-Term Care 1 that
THE BASICS The Commission on Long-Term Care: Background Behind the Mission As part of the American Taxpayer Relief Act of 2012 (ATRA, P.L. 112-240), Congress created a Commission on Long-Term Care 1 that
Background and Context:
 Session Objectives: Practice Transformation: Preparing for a Value Based Purchasing Environment Susan Brown, MPH, CPHIMS May 2, 2016 Understand the timeline and impact of MACRA/MIPS on health care payment
Session Objectives: Practice Transformation: Preparing for a Value Based Purchasing Environment Susan Brown, MPH, CPHIMS May 2, 2016 Understand the timeline and impact of MACRA/MIPS on health care payment
Medicaid and CHIP Managed Care Final Rule MLTSS
 Medicaid and CHIP Managed Care Final Rule MLTSS John Giles, Technical Director Division of Quality and Health Outcomes Children and Adult Health Programs Group Debbie Anderson, Deputy Director Division
Medicaid and CHIP Managed Care Final Rule MLTSS John Giles, Technical Director Division of Quality and Health Outcomes Children and Adult Health Programs Group Debbie Anderson, Deputy Director Division
STATE MEDICAID HOME CARE POLICIES: INSIDE THE BLACK BOX
 STATE MEDICAID HOME CARE POLICIES: INSIDE THE BLACK BOX Martin Kitchener MBA PhD, Professor (Corresponding author) Department of Social and Behavioral Sciences University of California, San Francisco 3333
STATE MEDICAID HOME CARE POLICIES: INSIDE THE BLACK BOX Martin Kitchener MBA PhD, Professor (Corresponding author) Department of Social and Behavioral Sciences University of California, San Francisco 3333
9/10/2013. The Session s Focus. Status of the NYS FIDA Initiative
 Leading Age NY Financial Manager s Conference, September 10-12, 2013 The Otesaga Resort Hotel, Cooperstown NY Paul Tenan VCC, Inc. FIDA: An Overview and Update The Session s Focus Overview of CMS national
Leading Age NY Financial Manager s Conference, September 10-12, 2013 The Otesaga Resort Hotel, Cooperstown NY Paul Tenan VCC, Inc. FIDA: An Overview and Update The Session s Focus Overview of CMS national
Older Adult Services. Submitted as: Illinois Public Act Status: Enacted into law in Suggested State Legislation
 Older Adult Services This Act is designed to transform the state older adult services system into a primarily home and community-based system, taking into account the continuing need for 24-hour skilled
Older Adult Services This Act is designed to transform the state older adult services system into a primarily home and community-based system, taking into account the continuing need for 24-hour skilled
Open Doors Transition Center Project Peer Outreach and Referral Program
 Open Doors Transition Center Project Peer Outreach and Referral Program Suzanne de Beaumont, Transition Center Project Director Zach Garafalo, Peer Program Director Association on Aging in New York October
Open Doors Transition Center Project Peer Outreach and Referral Program Suzanne de Beaumont, Transition Center Project Director Zach Garafalo, Peer Program Director Association on Aging in New York October
Strengthening Services for Older Adults through Changes to the Older Americans Act
 Strengthening Services for Older Adults through Changes to the Older Americans Act RECOMMENDATIONS FOR THE REAUTHORIZATION OF OAA 2011 A REPORT FOR THE ADMINISTRATION ON AGING (AoA) Prepared by The Social
Strengthening Services for Older Adults through Changes to the Older Americans Act RECOMMENDATIONS FOR THE REAUTHORIZATION OF OAA 2011 A REPORT FOR THE ADMINISTRATION ON AGING (AoA) Prepared by The Social
2013 BOSCOC RFP for Voluntary Reallocation of Funds
 RFP for Voluntary Reallocation of Funds Overview: The Balance of State Continuum of Care will consider Request for Proposals from organizations that wish to voluntarily reallocate their current funds (Transitional
RFP for Voluntary Reallocation of Funds Overview: The Balance of State Continuum of Care will consider Request for Proposals from organizations that wish to voluntarily reallocate their current funds (Transitional
The Money Follows the Person Demonstration in Massachusetts
 The Money Follows the Person Demonstration in Massachusetts Use of Concurrent 1915(b)(c) Waivers to Serve Elders and Adults with Disabilities Transitioning from Long-Stay Facilities HCBS Conference Arlington,
The Money Follows the Person Demonstration in Massachusetts Use of Concurrent 1915(b)(c) Waivers to Serve Elders and Adults with Disabilities Transitioning from Long-Stay Facilities HCBS Conference Arlington,
Estimated Decrease in Expenditure by Service Category
 Public Notice for June 2009 Release PUBLIC NOTICE COLORADO MEDICAID Department of Health Care Policy and Financing Fee-for-Service Provider Payments Effective July 1, 2009, in an effort to reduce expenditures
Public Notice for June 2009 Release PUBLIC NOTICE COLORADO MEDICAID Department of Health Care Policy and Financing Fee-for-Service Provider Payments Effective July 1, 2009, in an effort to reduce expenditures
Maryland Medicaid Program. Aaron Larrimore Medicaid Department of Health and Mental Hygiene May 31, 2012
 Maryland Medicaid Program Aaron Larrimore Medicaid Department of Health and Mental Hygiene May 31, 2012 1 Maryland Medicaid In Maryland, Medicaid is also called Medical Assistance or MA. MA is a joint
Maryland Medicaid Program Aaron Larrimore Medicaid Department of Health and Mental Hygiene May 31, 2012 1 Maryland Medicaid In Maryland, Medicaid is also called Medical Assistance or MA. MA is a joint
Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary
 Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary The Medicaid and CHIP Payment and Access Commission (MACPAC) was established in the Children's Health Insurance Program
Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary The Medicaid and CHIP Payment and Access Commission (MACPAC) was established in the Children's Health Insurance Program
Delaware's Care Transitions Program. Home and Community Based Services Conference September 11, 2013
 Delaware's Care Transitions Program Home and Community Based Services Conference September 11, 2013 Today s Topics Overview the picture in Delaware The need for change Initiatives underway Care Transitions
Delaware's Care Transitions Program Home and Community Based Services Conference September 11, 2013 Today s Topics Overview the picture in Delaware The need for change Initiatives underway Care Transitions
SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS IN SUPPORTED LIVING ARRANGEMENTS
 March 31, 2006 APD OP 17-002 OPERATING PROCEDURE APD OP 17-002 STATE OF FLORIDA AGENCY FOR PERSONS WITH DISABILITIES TALLAHASSEE, March 31, 2006 SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS
March 31, 2006 APD OP 17-002 OPERATING PROCEDURE APD OP 17-002 STATE OF FLORIDA AGENCY FOR PERSONS WITH DISABILITIES TALLAHASSEE, March 31, 2006 SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS
Quadel Consulting & Training, LLC - Enhancements and Best Practices Designed to Expand Resident Choice and Mobility in Minneapolis
 March 21, 2017 MEMORANDUM TO: FROM: SUBJECT: MPHA Board of Commissioners Kyle Hanson, HCV Managing Director Quadel Consulting & Training, LLC - Enhancements and Best Practices Designed to Expand Resident
March 21, 2017 MEMORANDUM TO: FROM: SUBJECT: MPHA Board of Commissioners Kyle Hanson, HCV Managing Director Quadel Consulting & Training, LLC - Enhancements and Best Practices Designed to Expand Resident
NC INNOVATIONS WAIVER HANDBOOK
 A Managed Care Organization of the NC Department of Health & Human Services NC INNOVATIONS WAIVER HANDBOOK Revised April 01, 2013 Sandhills Center provides access to services for mental health, intellectual
A Managed Care Organization of the NC Department of Health & Human Services NC INNOVATIONS WAIVER HANDBOOK Revised April 01, 2013 Sandhills Center provides access to services for mental health, intellectual
Tennessee Department of Health Traumatic Brain Injury Program. Annual Report. July 2010 June Winner, Bicycle Safety Poster Contest
 Tennessee Department of Health Traumatic Brain Injury Program Annual Report July 2010 June 2011 Winner, Bicycle Safety Poster Contest Traumatic Brain Injury Program 2010-2011 ANNUAL REPORT EXECUTIVE SUMMARY
Tennessee Department of Health Traumatic Brain Injury Program Annual Report July 2010 June 2011 Winner, Bicycle Safety Poster Contest Traumatic Brain Injury Program 2010-2011 ANNUAL REPORT EXECUTIVE SUMMARY
Washington State LTSS System, History and Vision
 Washington State LTSS System, History and Vision Bea Rector, Director, Home and Services Aging and Long Term Support Administration Washington State Department of Social and Health Services For Northwest
Washington State LTSS System, History and Vision Bea Rector, Director, Home and Services Aging and Long Term Support Administration Washington State Department of Social and Health Services For Northwest
Long Term Care. Lecture for HS200 Nov 14, 2006
 Long Term Care Lecture for HS200 Nov 14, 2006 Steven P. Wallace, Ph.D. Professor, Dept. Community Health Sciences, SPH and Associate Director, UCLA Center for Health Policy Research What is long-term care
Long Term Care Lecture for HS200 Nov 14, 2006 Steven P. Wallace, Ph.D. Professor, Dept. Community Health Sciences, SPH and Associate Director, UCLA Center for Health Policy Research What is long-term care
SERVICES. The following figures reflect total waiver numbers as of September 12, 2017: Total # Slots Allocated
 Office for Citizens with Developmental Disabilities (OCDD) QUARTERLY DEVELOPMENTAL DISABILITIES (DD) COUNCIL REPORT (Submitted for 3rd Quarter 2017) September 27, 2017 SERVICES Developmental Disability
Office for Citizens with Developmental Disabilities (OCDD) QUARTERLY DEVELOPMENTAL DISABILITIES (DD) COUNCIL REPORT (Submitted for 3rd Quarter 2017) September 27, 2017 SERVICES Developmental Disability
Department of Elder Affairs Programs and Services Handbook Chapter 3: Description of DOEA Coordination with other State/Federal Programs CHAPTER 3
 CHAPTER 3 Description of DOEA Coordination with Other State/Federal Programs 3-1 Table of Contents Section: Topic Page I. Overview and Specific Legal Authority 3-4 II. 3-7 A. Adult Care Food Program 3-7
CHAPTER 3 Description of DOEA Coordination with Other State/Federal Programs 3-1 Table of Contents Section: Topic Page I. Overview and Specific Legal Authority 3-4 II. 3-7 A. Adult Care Food Program 3-7
Letters in the Medicaid Alphabet:
 Letters in the Medicaid Alphabet: OPTIONS FOR FINANCING HOME AND COMMUNITY- BASED SERVICES P R E S E N T E D B Y : R O B I N E. C O O P E R D I R E C T O R O F T E C H N I C A L A S S I S T A N C E N A
Letters in the Medicaid Alphabet: OPTIONS FOR FINANCING HOME AND COMMUNITY- BASED SERVICES P R E S E N T E D B Y : R O B I N E. C O O P E R D I R E C T O R O F T E C H N I C A L A S S I S T A N C E N A
March 31, 2006 APD OP SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS IN SUPPORTED LIVING ARRANGEMENTS
 March 31, 2006 APD OP 17-002 OPERATING PROCEDURE APD OP 17-002 STATE OF FLORIDA AGENCY FOR PERSONS WITH DISABILITIES TALLAHASSEE, March 31, 2006 SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS
March 31, 2006 APD OP 17-002 OPERATING PROCEDURE APD OP 17-002 STATE OF FLORIDA AGENCY FOR PERSONS WITH DISABILITIES TALLAHASSEE, March 31, 2006 SUPPORTED LIVING PROVISION OF IN-HOME SUBSIDIES FOR PERSONS
Managed Long Term Services and Supports (MLTSS) A Forum for Consumers, their Families and Caregivers, Advocates and Community-Based Agencies
 Managed Long Term Services and Supports (MLTSS) A Forum for Consumers, their Families and Caregivers, Advocates and Community-Based Agencies 1 Background To give you an update on the implementation of
Managed Long Term Services and Supports (MLTSS) A Forum for Consumers, their Families and Caregivers, Advocates and Community-Based Agencies 1 Background To give you an update on the implementation of
Application for a 1915(c) Home and Community- Based Services Waiver PROPOSED
 Page 1 of 165 Application for a 1915(c) Home and Community- Based Services Waiver PURPOSE OF THE HCBS WAIVER PROGRAM The Medicaid Home and Community-Based Services (HCBS) waiver program is authorized in
Page 1 of 165 Application for a 1915(c) Home and Community- Based Services Waiver PURPOSE OF THE HCBS WAIVER PROGRAM The Medicaid Home and Community-Based Services (HCBS) waiver program is authorized in
Counting for Dollars: Pinal County, Arizona
 Counting for Dollars: Pinal County, Arizona Federal Assistance Programs that Distributed Funds in Pinal County, Arizona on the Basis of Census-Related Statistics, Fiscal Year 2008 This table lists federal
Counting for Dollars: Pinal County, Arizona Federal Assistance Programs that Distributed Funds in Pinal County, Arizona on the Basis of Census-Related Statistics, Fiscal Year 2008 This table lists federal
FAMILY SELF SUFFICIENCY ACTION PLAN
 FAMILY SELF SUFFICIENCY ACTION PLAN Approved by SNRHA Board of Commissioners June 15, 2017 SOUTHERN NEVADA REGIONAL HOUSING AUTHORITY Supportive Services Department 5390 E. Flamingo Road Las Vegas, NV
FAMILY SELF SUFFICIENCY ACTION PLAN Approved by SNRHA Board of Commissioners June 15, 2017 SOUTHERN NEVADA REGIONAL HOUSING AUTHORITY Supportive Services Department 5390 E. Flamingo Road Las Vegas, NV
LTRAP Voucher, Pre-application & Waiting List FAQs: 2015.
 LTRAP Voucher, Pre-application & Waiting List FAQs: 2015. 1. What is the Housing Choice Voucher program? The Housing Choice Voucher program is HUD s largest rental assistance program; assisting more than
LTRAP Voucher, Pre-application & Waiting List FAQs: 2015. 1. What is the Housing Choice Voucher program? The Housing Choice Voucher program is HUD s largest rental assistance program; assisting more than
Transitions and Long-Term Care: The Minimum Data Set 3.0 Section Q and Money Follows the Person
 Transitions and Long-Term Care: The Minimum Data Set 3.0 Section Q and Money Follows the Person 2 Agenda Housekeeping/Introductions An overview of the Minimum Data Set (MDS) 3.0 Section Q An overview of
Transitions and Long-Term Care: The Minimum Data Set 3.0 Section Q and Money Follows the Person 2 Agenda Housekeeping/Introductions An overview of the Minimum Data Set (MDS) 3.0 Section Q An overview of
Medicaid Coverage of Long-Term Services and Supports
 Medicaid Coverage of Long-Term Services and Supports Kirsten J. Colello Specialist in Health and Aging Policy December 5, 2013 Congressional Research Service 7-5700 www.crs.gov R43328 Summary Long-term
Medicaid Coverage of Long-Term Services and Supports Kirsten J. Colello Specialist in Health and Aging Policy December 5, 2013 Congressional Research Service 7-5700 www.crs.gov R43328 Summary Long-term
H.R. 3962, the Affordable Health Care for America Act: Issues Affecting Long Term Care November 3, Changes to LTC-Related Funding
 H.R. 3962, the Affordable Health Care for America Act: Issues Affecting Long Term Care November 3, 2009 Below is a summary of the provisions of the Affordable Health Care for America Act (H.R. 3962) affecting
H.R. 3962, the Affordable Health Care for America Act: Issues Affecting Long Term Care November 3, 2009 Below is a summary of the provisions of the Affordable Health Care for America Act (H.R. 3962) affecting
Application for a 1915(c) Home and Community-Based Services Waiver
 Page 1 of 76 Application for a 1915(c) Home and Community-Based Services Waiver PURPOSE OF THE HCBS WAIVER PROGRAM The Medicaid Home and Community-Based Services (HCBS) waiver program is authorized in
Page 1 of 76 Application for a 1915(c) Home and Community-Based Services Waiver PURPOSE OF THE HCBS WAIVER PROGRAM The Medicaid Home and Community-Based Services (HCBS) waiver program is authorized in
Promising Practices for Diversion and Transition of Persons with Mental Illness Through the PASRR Processes
 Promising Practices for Diversion and Transition of Persons with Mental Illness Through the PASRR Processes Dee O Connor, PhD Jennifer Ingle, MS, CRC Kimberly Wamback, BA University of Massachusetts Medical
Promising Practices for Diversion and Transition of Persons with Mental Illness Through the PASRR Processes Dee O Connor, PhD Jennifer Ingle, MS, CRC Kimberly Wamback, BA University of Massachusetts Medical
