Interdisciplinary Team Building, Management, and Communication
|
|
|
- Ethan Dean
- 5 years ago
- Views:
Transcription
1 Interdisciplinary Team Building, Management, and Communication Credit Information If you would like to receive continuing education or continuing medical education credit for today s event via the Centers for Medicare & Medicaid Service s Learning Management System, please visit this link for more information: pdf Audio and Platform Information The audio portion of the presentation will automatically stream through your computer speakers. If you experience challenges with the audio, please click the phone icon at the bottom of the screen for dial-in information. If you are experiencing any technical difficulties with this platform, please use the Q&A feature for assistance or click the help button for additional information. 1
2 March 21, 2018 The 2018 Disability-Competent Care Webinar Series: Interdisciplinary Team Building, Management, and Communication
3 Webinar Overview The Lewin Group, under contract with the CMS Medicare-Medicaid Coordination Office, partnered with Christopher Duff and other disability practice experts to develop the 2018 Disability-Competent Care webinar series. This is the fifth webinar in the series. This webinar series builds on the 2017 Disability-Competent Care webinar series, that introduced the model of care and its seven foundational pillars. To view this series, please visit: 017_DCC_Webinar_Series/Series_Overview Each session will be interactive (e.g., polls and interactive chat functions), with 45 minutes of presenter-led discussion, followed by 15 minutes of presenter and participant discussions. Video replay and slide presentation are available after each session at: 3
4 Support Statement This webinar is supported through the Medicare-Medicaid Coordination Office (MMCO) in the Centers for Medicare & Medicaid Services (CMS) to help beneficiaries dually eligible for Medicare and Medicaid have access to seamless, high-quality health care that includes the full range of covered services in both programs. To support providers in their efforts to deliver more integrated, coordinated care to dually eligible beneficiaries, MMCO is developing technical assistance and actionable tools based on successful innovations and care models, such as this webinar. To learn more about current efforts and resources, visit Resources for Integrated Care at: 4
5 Continuing Education Accreditation The Centers for Medicare & Medicaid Services is accredited by the International Association for Continuing Education and Training (IACET) for Continuing Education Units (CEU) and by the Accreditation Council for Continuing Medical Education (ACCME) for Continuing Medical Education (CME, AMA PRA Category 1 credit for physicians and nonphysicians). 5
6 Obtaining Continuing Education Credit Complete the post-test through CMS Learning Management System and score a 80 percent or higher by midnight April 9, CWebinar5_CE_Credit_Guide.pdf 6
7 Introductions Christopher Duff Mary Glover Disability Practice and Policy Consultant Founder, Boston Community Medical Group Cindy Guddal Manager, Allina Health Courage Kenny Rehabilitation Institute 7
8 Webinar Learning Objectives This webinar will emphasize: The structure of the interdisciplinary team (IDT) and how it benefits people with disabilities Approaches to effectively facilitate IDT meetings to ensure they meet the unique needs of people with disabilities The utility of the IDT and how it can be applied in different care settings Strategies to facilitate communication between internal and external IDT members 8
9 Agenda Introduction to the interdisciplinary team (IDT) The IDT at the Boston Community Medical Group Using the IDT in alternative care settings Applying the IDT in alternative models of care and services at Courage Kenny Rehabilitation Institute An IDT within the advanced primary care clinic An IDT within in-home community services Audience questions 9
10 Introduction to the Interdisciplinary Team Mary Glover Founder, Boston Community Medical Group 10
11 Health Disparities Individuals with disabilities are more likely to: 1,2 Experience worse health outcomes Experience difficulties or delays in receiving necessary health care The unique challenges individuals with disabilities face often contribute to health disparities. Several common challenges are: 3 The lack of a strong primary care provider (PCP) relationship. Often PCPs lack the skills or infrastructure required to meet the needs of those with disabilities. The lack of communication and coordination between specialists which may lead to hospitalization for otherwise preventable complications. The use of an IDT may help to address these challenges by creating a team that assumes responsibility for the totality of the participant s care. Sources: 1) Office of the Assistant Secretary for Planning and Evaluation; ) Disability and Health. Healthy People ) Health Affairs Blog;
12 Interdisciplinary Team within DCC Health care is a multi-disciplinary profession in which doctors, nurses, and other providers from different specialties work together, communicate often, and share resources and accountability. Bringing together health care professionals from different disciplines is a central theme woven throughout the disability-competent care (DCC) model and allows for better outcomes. The core members of the DCC interdisciplinary team (IDT) include a primary care practitioner, a nurse, a social worker, and a behavioral health specialist. 12
13 Interdisciplinary Team within DCC The complex needs of the dually eligible population make the use of an IDT a key mechanism for delivering quality health outcomes. In particular, dually eligible beneficiaries often require: Multiple medical specialists (e.g., physicians, occupational therapists, physical therapists, etc.) Complex health and social services (e.g., mental health therapists, housing supports, in-home personal care, eligibility for financial assistance) Immediate responsiveness to prevent the development or escalation of episodes of illness 13
14 Purpose of the Interdisciplinary Team The goal of the IDT is to help participants receive the care they need and achieve their identified goals. The IDT: Facilitates participant goal setting, problem solving, and care in a coordinated, cost-effective manner. Fosters communication among its different members - an essential and a key component to the participant's success. Communication among the different disciplines is often frequent, structured, and documented. Brings together knowledge and specialties from different disciplines. Team members are responsible individually and collectively for the participant s care. Depending on the context of the IDT, participant s input is facilitated by a designated team member. Shared decision making between the participant can add value. 14
15 Responsibilities of the IDT The IDT maintains several responsibilities, including: Addressing urgent and acute episodes of care* Proactively managing emerging needs* Managing care transitions* Assessing and creating the participant s individualized plan of care (IPC) Implementing, managing, and overseeing the IPC Allocating care management and resources Tailoring services and supports *Those with functional limitations are especially vulnerable during these situations and require timely and time intensive intervention. 15
16 Purpose of IDT Meetings Effective IDT meetings are centered around meeting the needs and goals of participants. To accomplish this, regular IDT meetings* can be used as a successful tool. They allow its members to: Build relationships Share information (e.g., participant medical updates, and administrative updates) Work together to identify and solve problems Develop IPCs with input from all disciplines Disseminate learning experiences and foster a continuous learning environment Support other team members *Meeting frequency is dependent on the complexity and unique needs of the participants served by the IDT 16
17 Elements of Effective IDT Meetings Provide all members of the IDT a clear understanding of the team and participant s goals Include appropriate team members Develop an agenda for the meeting Start the meeting on time Take minutes and distribute them promptly after the meeting Build rapport between team members, and include input from the participant Strive for consensus on key decisions Develop action items and assign responsibility Revise the meeting process and structure, as necessary 17
18 IDT at the Boston Community Medical Group Mary Glover Founder, Boston Community Medical Group 18
19 The Boston Community Medical Group The Boston Community Medical Group (BCMG) is an interdisciplinary practice that provides primary care to adults with disabilities and seniors. BCMG was structured as an independent practice group to serve members of Commonwealth Care Alliance (CCA), a health plan serving dually eligible beneficiaries in Massachusetts. All BCMG participants are enrolled in a health plan are dually eligible, except for a small number who have been grandfathered into the plan but who do not qualify for Medicare. BCMG s three primary care center locations provide comprehensive DCC to adults of all ages, including those who may have complex physical, developmental, intellectual, and behavioral health conditions. 19
20 The BCMG Interdisciplinary Teams IDTs at BCMG are comprised of: Nurse practitioners Physicians and physician assistants Social workers Behavioral health specialists Rehabilitation specialists: physical therapy and occupational therapy Durable medical equipment (DME) specialists Administrative support staff Hospitalist External specialists and consultants, as applicable The IDT must be flexible to include additional team members as needed to be responsive to each participant s unique care needs and goals. 20
21 BCMG Team Meetings The IDT at BCMG meets for two hours each week to discuss the panel of participants assigned to the team. On average, 25 percent of the panel will be discussed in one meeting. Weekly meeting attendees include all team members, such as: Nurse practitioners/physician assistants, physicians, and social workers Administrative staff participate in the non-clinical portion of the meeting to discuss operational issues Rehabilitation coordinator: answers questions related to speech, occupational and physical therapy Behavioral health (BH) specialist: offers input regarding BH questions and plans Psychiatrist: provides consultation for complex BH needs (e.g., medication changes) 21
22 BCMG Meeting Agenda A standard agenda at an IDT meeting includes the following items: Announcements Enrollment activity: new cases assigned and presented Clinical coverage and scheduling updates Review of hospitalized participants, including acute, sub-acute, emergency room visits, and recent discharges Clinical presentations and review of guidelines Case discussions with a problem-oriented approach Team members identify cases for discussion Morbidity and mortality rounds 22
23 BCMG IDT Communication A meeting facilitator for the IDT is identified to organize the agenda, take notes, and monitor the time. However, different team members will take turns leading the discussion. Participants and any external specialists are consulted outside of routine IDT meetings due to the large amount of information discussed during settings. A designated team member will be responsible for coordinating consultation. Usually, it is the care coordinator s responsibility to relay information to and from the participant and their specialists. 23
24 IDT Meeting Challenges During weekly meetings, the IDT routinely reviewed the care plans of participants assigned. However, time efficiency became a challenge as the program grew and more participants were being managed by each IDT member. The BCMG team adopted a more problem-oriented approach for the IDT meetings. IDT members were expected to come prepared with participant updates and key questions. IDT managers reviewed the standard agenda to see what could be taken offline, e.g. regular reassessments. Meetings focused on hospitalized participants and those with urgent needs. An increased focus on relaying information rather than in-depth case discussions. 24
25 IDT Meeting Best Practices Value the diversity of opinions among team members. Encourage an environment where providers are comfortable requesting advice from other specialists. Maintain positive group dynamics. Establish reliable, positive working relationships and regular communication exchanges between providers, e.g., between primary care providers (PCPs) and behavioral health specialists. Encourage smooth hand-offs between providers with routine discussions of participant care issues prior to and after same-day visits. PCPs can keep half of their daily schedule available to respond to urgent needs. Encourage the use of new technology and techniques to expand participation and improve efficiency. Offer periodic training and education for staff on specialized topics that are of particular relevance to the participant population, New technologies can include telemedicine and remote monitoring. 25
26 Applying the IDT in Alternative Models of Care and Services at Courage Kenny Rehabilitation Institute Cindy Guddal Manager, Allina Health Courage Kenny Rehabilitation Institute 26
27 Courage Kenny Rehabilitation Institute Courage Kenny Rehabilitation Institute (CKRI), part of Allina Health, provides rehabilitation services for people with shortand long-term chronic conditions, injuries and disabilities. Facilities are located in Minnesota and western Wisconsin. CKRI s unique combination of rehabilitation, support, and lifestyle services address the needs of the whole person. More than 94,000 lives were touched in Two CKRI programs referenced in this webinar are: Advanced primary care clinic In-home community services 27
28 Program Descriptions Advanced Primary Care The Advanced Primary Care (APC) clinic is a state-certified medical home where participants are managed by an IDT. Services include: Primary care services Program goals center on helping the participant manage complex neurological condition(s) in an effort to maximize function and achieve life goals. In-Home Community Services The in-home community services program consists of a several unique LTSS programs. Services include: Independent living skills Community behavioral services Adult rehabilitative mental health services (ARMHS) Program goals center on working with the participants to build a life that is important and meaningful; identify and pursue goals; develop skills, remove barriers, and connect with resources. 28
29 Program Objectives Advanced Primary Care The APC clinic was created to bring coordination between acute care settings and other providers of care; helping to address three immediate challenges. 1. Limited PCP understanding and knowledge of participants with disabilities 2. Limited capacity to meet the populations needs within a traditional primary care clinic context 3. Greater responsiveness / flexibility to meet the needs of participants with disabilities. In-Home Community Services The in-home community services program was designed to work with participants to teach the skills required to work / live within the community and to help address immediate challenges, as they arise. 1. Limited services were available to support participants in achieving goals within: Their home The community 29
30 Program Populations Advanced Primary Care Participants generally have a primary neurologic or other physically disabling injury that limits their ability to obtain primary medical care in a typical clinic setting. 42 percent are dually eligible beneficiaries 34 percent Medicaid-only beneficiaries 11 percent Medicare-only beneficiaries On average, participants have a total of seven co-occurring conditions and 11 active medications. In-Home Community Services Participants have a physical disability such as an acquired brain injury, stroke, spinal cord injury or Cerebral Palsy that limits their ability to be successful in community living. 42 percent are dually eligible beneficiaries 55 percent Medicaid-only beneficiaries Many participants present with cooccurring behavioral health disabilities. 30
31 Program IDTs in Practice IDT Components Advanced Primary Care In-Home Community Services IDT Composition Internal team members External team members IDT Members IDT Leader Care coordinator (registered nurse), primary care provider, PM&R*, occupational and physical therapists, speech therapist, physiatrist, and mental health provider Led by the care coordinator Composition is fluid, includes: case manager (from referral source), provider (from CKRI program), and the participant Led by the external case manager *Physical Medicine and Rehabilitation (PM&R) Physician 31
32 Program IDTs in Practice IDT Components Meeting Structure Meeting Frequency Meeting Duration Communication Methods IDT Goals Advanced Primary Care Formal / standardized Weekly 1 hour Centralized medical record, team meetings, and messaging Coordinating acute and primary care, aligning goals and services, and sharing updates Ad-hoc In-Home Community Services Informal / when problems arise As needed Communication books, phone calls, and planning forms Coordinating care, aligning goals and services to improve functioning within the community, and sharing updates 32
33 Coordinating Communication Methods for managing team communication to reduce silos of care include: Using effective communication methods such as Phone calls Secured messages A communication book carried by participant to prepare for and make notes during the visit A communication book kept in the participant s home that is filled out by home care or service providers when then interact with the participant Written instructions for support persons e.g. a personal care attendant Shared appointments for in-person meetings to include multiple providers in one visit with the participant Keeping an up-to-date list of care team providers and their roles and shared with the participant Routine prioritization of care plan goals and outcomes 33
34 Coordinating Communication Preparing the participant to communicate with their team and providers can improve care coordination. Providers can help build skills that support the participant's effective selfadvocacy: Plan for appointments, e.g. identify questions to be addressed during the appointment Rehearse the appointment to help with assertiveness and encourage active participation Identify recommendations and follow-ups post-appointment and review these with the case manager 34
35 Involving the Participant Provide participants clarity about the various roles of their IDT members and providers: Case manager vs. care coordinator Clinic vs. health plan Which community service provider helps with which health issues Care coordinators from the physician clinic vs. the care coordinator from the health plan Which community service provider provides support for health issues Which provider to contact for support regarding BH issues Respond to the participant and those involved in their care in a timely fashion Understand the barriers people face Address conflicting priorities among the participant, payors, and providers 35
36 Involving the Participant Shared decision making is a process that involves two experts: the provider and the participant. The provider knows the evidence-based medical options The participant knows his or her values, preferences, and particularly, their experience with their disability Together, they choose a treatment, test, or screen after reviewing decision aids/documents that detail options in an unbiased manner. The process of shared decision making helps to ensure that participants are well-informed, and choose a course of care consistent with their values and preferences. Decision aid examples can be found: Conditions-and-Treatments/Health-library/Patient-education/Shareddecision-making-decision-aids/ 36
37 Tools to Support Teamwork, Coordination and Communication Clearly defined and articulated care plans that are shared with the participant and that: Identify goals Describe what is to be done Specify when it is to be done Highlights the responsible party Appointment planning sheets for the participants Summaries of visits, including clear directions for follow-ups Protocols for common medical issues such as: Urinary Tract Infections (UTI s) Skin Breakdowns Upper Respiratory Infections 37
38 Lessons Learned Communication and coordination of care within the IDT is far more effective and efficient when the participant is primarily served within a single care system as compared to providing care across multiple distinct care systems. Regardless of where the IDT resides or functions, there must be an overall coordinator of care and access point for the participant. Routine systems and procedures need to be in place to ensure good communication and that updates are clearly and fluidly disseminated to all involved providers, especially upon the occurrence of an injury or hospitalization. 38
39 First Person Story: Mary Jo Mary Jo is a 60 year old woman with multiple sclerosis and bipolar disorder. She lives alone in a condominium, and her only family members are her elderly parents who live over two hours away. She values her community but has become increasingly isolated. Mary Jo is dually eligible and receives LTSS through a Medicaid waiver. Multiple sclerosis impacts her with cognitive deficits including memory loss, though her mobility is not impaired. Her services from CKRI include primary care at the APC clinic and community-based Independent Living Skills (ILS) services. She also receives in-home nursing and personal care attendant supports and sees medical specialists from providers outside the Allina Health system. ILS services have been instrumental in removing barriers to her receiving proper medical care. 39
40 First Person Story: Mary Jo Coordination strategies included: Working with Mary Jo to keep track of appointments, using memory compensation strategies, cueing her to contact providers as needed, and ensuring that she is providing accurate information to providers. Having the clinic care coordinator follow up with Mary Jo via phone calls and messages, and attending medical appointments when complicated information is shared. A shared medical record that allows each care team member access to the ICP and reinforces follow-up activities. Without this level of coordinated care, Mary Jo is at risk of needing to move to a more supported housing setting, in turn losing her home. She values her independence and the community of people so such a loss would be devastating. 40
41 Coordinating Care Between CKRI Services Care coordination between providers in the clinic and the multiple services offered through in-home community services is critical for achieving care goals. When Mary Jo was served through both programs, successful communication strategies included: A central location to view participant records and notes (e.g., single electronic health record) Frequent communication with care coordinators regarding the participant s needs, preferably through regularly scheduled meetings Having community services staff attend the participant s appointments Defining complementary goals in each service s care plan Care plans are distinct and specific to the service provided, but may have complementary goals (e.g., the clinic may have a goal of improved adherence to special diet; LTSS would have a goal involving meal planning or grocery shopping). 41
42 Audience Questions 42
43 Next Webinar Managing Transitions with Adults with Disabilities Date: March 28 th, 2018 Time: 2:00pm-3:00pm ET 43
44 Thank You for Attending! The video replay, slide presentation, and a summary of the Q&A will be available at: For more information about obtaining CEUs or CMEs via CMS Learning Management System, please visit: inar5_ce_credit_guide.pdf Questions? Please RIC@lewin.com Follow us on Twitter to learn about upcoming webinars and new products! 44
45 Webinar Evaluation Form Your feedback is very important! Please take a moment to complete a brief evaluation on the quality of the webinar. The survey will automatically appear on the screen approximately a minute after the conclusion of the presentation. 45
46 Send Us Your Feedback Help us diversify our series content and address current Disability- Competent Care training needs your input is essential! Please contact us with your suggestions at What We d Like from You: How best to target future Disability-Competent Care webinars to health care providers and plans involved in all levels of the health care delivery process Feedback on these topics as well as ideas for other topics to explore in webinars and additional resources related to Disability- Competent Care 46
47 Sources 1. Office of the Assistant Secretary for Planning and Evaluation. (2016). Report to Congress: Social Risk Factors and Performance under Medicare s Value Based Purchasing Programs 2. Disability and Health. Healthy People Retrieved from: 3. Health Affairs Blog. Realizing the Promise of Integrated Care for the Dual Eligibles. October 22, Retrieved from: 47
48 Resources NPD Solutions: Effective team meetings: Rehabilitation Medicine: Principles and Practice. Joel DeLisa, M.D., Philadelphia, Allina Health: Shared decision making decision aids Treatments/Health-library/Patient-education/Shareddecision-making-decision-aids/ 48
Medicare: 2017 Model of Care Training 4/13/2017
 Medicare: 2017 Model of Care Training Training Objectives This course will describe how MHS Health Wisconsin Medicare Advantage and its contracted providers work together to successfully deliver the Model
Medicare: 2017 Model of Care Training Training Objectives This course will describe how MHS Health Wisconsin Medicare Advantage and its contracted providers work together to successfully deliver the Model
LEADING HEALTHCARE PRACTICES AND TRAINING: DEFINING AND DELIVERING DISABILITY-COMPETENT CARE
 HEALTH CARE AND HUMAN SERVICES POLICY, RESEARCH, AND CONSULTING - WITH REAL-WORLD PERSPECTIVE. LEADING HEALTHCARE PRACTICES AND TRAINING: DEFINING AND DELIVERING DISABILITY-COMPETENT CARE Session VII:
HEALTH CARE AND HUMAN SERVICES POLICY, RESEARCH, AND CONSULTING - WITH REAL-WORLD PERSPECTIVE. LEADING HEALTHCARE PRACTICES AND TRAINING: DEFINING AND DELIVERING DISABILITY-COMPETENT CARE Session VII:
Medicare: 2017 Model of Care Training 12/14/201 7
 Medicare: 2017 Model of Care Training 12/14/201 7 What is the Model of Care? The Model of Care (MOC) is Allwell s plan for delivering our integrated care management program for members with special needs.
Medicare: 2017 Model of Care Training 12/14/201 7 What is the Model of Care? The Model of Care (MOC) is Allwell s plan for delivering our integrated care management program for members with special needs.
Medicare: 2018 Model of Care Training
 Medicare: 2018 Model of Care Training Training Objectives This course will describe how Centene and its contracted providers work together to successfully deliver the duals Model of Care (MOC) program.
Medicare: 2018 Model of Care Training Training Objectives This course will describe how Centene and its contracted providers work together to successfully deliver the duals Model of Care (MOC) program.
INPATIENT ACUTE REHABILITATION HOSPITAL LIMITATIONS, SCOPE AND INTENSITY OF CARE
 INPATIENT ACUTE REHABILITATION HOSPITAL LIMITATIONS, SCOPE AND INTENSITY OF CARE Bacharach Institute for Rehabilitation offers a number of in and outpatient rehabilitation programs and services designed
INPATIENT ACUTE REHABILITATION HOSPITAL LIMITATIONS, SCOPE AND INTENSITY OF CARE Bacharach Institute for Rehabilitation offers a number of in and outpatient rehabilitation programs and services designed
Best Practices. SNP Alliance. October 2013 Commonwealth Care Alliance: Best Practices in Care for Frail and Disabled Medicare Medicaid Enrollees
 SNP Alliance Best Practices October 2013 Commonwealth Care Alliance: Best Practices in Care for Frail and Disabled Medicare Medicaid Enrollees Commonwealth Care Alliance is a Massachusetts-based non-profit,
SNP Alliance Best Practices October 2013 Commonwealth Care Alliance: Best Practices in Care for Frail and Disabled Medicare Medicaid Enrollees Commonwealth Care Alliance is a Massachusetts-based non-profit,
Meaningful Member Engagement Webinar Series
 September 15, 2015 Meaningful Member Engagement Webinar Series Hard-to-Reach Populations: Innovative Strategies to Engage Isolated Individuals with Behavioral Health Needs Hard-to-Reach Populations: Innovative
September 15, 2015 Meaningful Member Engagement Webinar Series Hard-to-Reach Populations: Innovative Strategies to Engage Isolated Individuals with Behavioral Health Needs Hard-to-Reach Populations: Innovative
OneCare Model of Care
 OneCare Model of Care Note: Content of this course was current at the time it was published. As Medicare policy changes frequently, check with your immediate supervisor regarding recent updates. 2018 Learning
OneCare Model of Care Note: Content of this course was current at the time it was published. As Medicare policy changes frequently, check with your immediate supervisor regarding recent updates. 2018 Learning
Model of Care Scoring Guidelines CY October 8, 2015
 Model of Care Guidelines CY 2017 October 8, 2015 Table of Contents Model of Care Guidelines Table of Contents MOC 1: Description of SNP Population (General Population)... 1 MOC 2: Care Coordination...
Model of Care Guidelines CY 2017 October 8, 2015 Table of Contents Model of Care Guidelines Table of Contents MOC 1: Description of SNP Population (General Population)... 1 MOC 2: Care Coordination...
How Managed Long-Term Services and Supports Can Help Family Caregivers
 April 27, 2017 How Managed Long-Term Services and Supports Can Help Family Caregivers Tips for Using this Webinar Platform Phone dial-in information was provided for the first 500 registrants and is available
April 27, 2017 How Managed Long-Term Services and Supports Can Help Family Caregivers Tips for Using this Webinar Platform Phone dial-in information was provided for the first 500 registrants and is available
CAL MEDICONNECT: Understanding the Health Risk Assessment. Physician Webinar Series
 CAL MEDICONNECT: Understanding the Health Risk Assessment Physician Webinar Series Today s Webinar This webinar is part of a series designed specifically for CAPG members. For a general overview of the
CAL MEDICONNECT: Understanding the Health Risk Assessment Physician Webinar Series Today s Webinar This webinar is part of a series designed specifically for CAPG members. For a general overview of the
Special Needs Program Training. Quality Management Department
 10/26/2017 1 Special Needs Program Training Quality Management Department 10/26/2017 2 Special Needs Plan (SNP) Overview 3 SNP Overview Medicare Advantage (MA) plans were created by the Medicare Modernization
10/26/2017 1 Special Needs Program Training Quality Management Department 10/26/2017 2 Special Needs Plan (SNP) Overview 3 SNP Overview Medicare Advantage (MA) plans were created by the Medicare Modernization
Understanding and Leveraging Continuity of Care
 Understanding and Leveraging Continuity of Care Cal MediConnect Providers Summit January 21, 2015 Moderator: Jane Ogle, Consultant, Harbage Consulting www.chcs.org An Overview of Continuity of Care in
Understanding and Leveraging Continuity of Care Cal MediConnect Providers Summit January 21, 2015 Moderator: Jane Ogle, Consultant, Harbage Consulting www.chcs.org An Overview of Continuity of Care in
CME Provider Webinar
 CME Provider Webinar October 19, 2017 2 3 p.m. Welcome & Introductions All phone lines will be muted, please press the raise your hand button or use the typed question feature if you have a question or
CME Provider Webinar October 19, 2017 2 3 p.m. Welcome & Introductions All phone lines will be muted, please press the raise your hand button or use the typed question feature if you have a question or
Building a Culture of Engagement for Medicare- Medicaid Enrollees: Health Plan Approaches
 TECHNICAL ASSISTANCE BRIEF August 2015 Building a Culture of Engagement for Medicare- Medicaid Enrollees: Health Plan Approaches By Sarah Barth and Brianna Ensslin, Center for Health Care Strategies I
TECHNICAL ASSISTANCE BRIEF August 2015 Building a Culture of Engagement for Medicare- Medicaid Enrollees: Health Plan Approaches By Sarah Barth and Brianna Ensslin, Center for Health Care Strategies I
Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees
 TECHNICAL ASSISTANCE BRIEF J UNE 2 0 1 2 Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees I ndividuals eligible for both Medicare and Medicaid (Medicare-Medicaid
TECHNICAL ASSISTANCE BRIEF J UNE 2 0 1 2 Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees I ndividuals eligible for both Medicare and Medicaid (Medicare-Medicaid
Coordinated Care Initiative DRAFT Assessment and Care Coordination Standards November 20, 2012
 Coordinated Care Initiative DRAFT Assessment and Care Coordination Standards November 20, 2012 Table of Contents CARE COORDINATION GENERAL REQUIREMENTS...4 RISK STRATIFICATION AND HEALTH ASSESSMENT PROCESS...6
Coordinated Care Initiative DRAFT Assessment and Care Coordination Standards November 20, 2012 Table of Contents CARE COORDINATION GENERAL REQUIREMENTS...4 RISK STRATIFICATION AND HEALTH ASSESSMENT PROCESS...6
Special Needs Plan Model of Care Chinese Community Health Plan
 Special Needs Plan Model of Care 2017 2017 Chinese Community Health Plan Elements of CCHP SNP Model of Care Special Needs Plan (SNP) Goals CCHP Dual Eligible SNP Enrollment & Eligibility Vulnerable Beneficiaries
Special Needs Plan Model of Care 2017 2017 Chinese Community Health Plan Elements of CCHP SNP Model of Care Special Needs Plan (SNP) Goals CCHP Dual Eligible SNP Enrollment & Eligibility Vulnerable Beneficiaries
Care Transition Toolkit for Persons with Mental Health & Co-Occurring Conditions
 November 30, 2015 Care Transition Toolkit for Persons with Mental Health & Co-Occurring Conditions What It Is and How You Can Use It Care Transition Toolkit for Persons with Mental Health & Co-Occurring
November 30, 2015 Care Transition Toolkit for Persons with Mental Health & Co-Occurring Conditions What It Is and How You Can Use It Care Transition Toolkit for Persons with Mental Health & Co-Occurring
Medicare Shared Savings Program ACO Learning System
 Medicare Shared Savings Program ACO Learning System Coordinating Care for Beneficiaries with Complex Care Needs Wednesday, June 24, 2015 2:30 4:00 PM ET Audio for this session can be streamed through your
Medicare Shared Savings Program ACO Learning System Coordinating Care for Beneficiaries with Complex Care Needs Wednesday, June 24, 2015 2:30 4:00 PM ET Audio for this session can be streamed through your
Patient Navigator Program
 Using Patient Navigators and Education to Improve Post-Acute Transitions Emerging innovators in post-acute care delivery models are finding ways to provide patient-centered, quality care to integrate today
Using Patient Navigators and Education to Improve Post-Acute Transitions Emerging innovators in post-acute care delivery models are finding ways to provide patient-centered, quality care to integrate today
Model Of Care: Care Coordination Interdisciplinary Care Team (ICT)
 Cal MediConnect 2017 Model Of Care: Care Coordination Interdisciplinary Care Team (ICT) 2017 CMC Annual Training Learning Objectives Define the L.A. Care Cal MediConnect (CMC) Model of Care Describe the
Cal MediConnect 2017 Model Of Care: Care Coordination Interdisciplinary Care Team (ICT) 2017 CMC Annual Training Learning Objectives Define the L.A. Care Cal MediConnect (CMC) Model of Care Describe the
WakeMed Rehab Spinal Cord Injury Scope of Service
 WakeMed Rehab Spinal Cord Injury Scope of Service The WakeMed Rehab Continuum provides an integrated, comprehensive delivery of rehabilitation services utilizing evidence-based practice directed toward
WakeMed Rehab Spinal Cord Injury Scope of Service The WakeMed Rehab Continuum provides an integrated, comprehensive delivery of rehabilitation services utilizing evidence-based practice directed toward
SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015
 SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training for our Special Needs Plan at Care Wisconsin.
SPECIAL NEEDS PLAN (SNP) MODEL OF CARE TRAINING 2015 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training for our Special Needs Plan at Care Wisconsin.
Introduction for New Mexico Providers. Corporate Provider Network Management
 Introduction for New Mexico Providers Corporate Provider Network Management Overview New Mexico snapshot. Who we are. Why Medicaid managed care? Why AmeriHealth Caritas? Why partner with us? Medical Management
Introduction for New Mexico Providers Corporate Provider Network Management Overview New Mexico snapshot. Who we are. Why Medicaid managed care? Why AmeriHealth Caritas? Why partner with us? Medical Management
Adapting PACE. PACE Pilots: A New Era for Individuals with Disabilities August 24, 2016
 Adapting PACE PACE Pilots: A New Era for Individuals with Disabilities August 24, 2016 What is PACE? Traditional model for nursing home eligible individuals over age 55 (PACE stands for Program of All-Inclusive
Adapting PACE PACE Pilots: A New Era for Individuals with Disabilities August 24, 2016 What is PACE? Traditional model for nursing home eligible individuals over age 55 (PACE stands for Program of All-Inclusive
Sunflower Health Plan
 Key Components for Successful LTSS Integration: Case Studies of Ten Exemplar Programs Sunflower Health Plan Jennifer Windh September 2016 Long- term services and supports (LTSS) integration is the integration
Key Components for Successful LTSS Integration: Case Studies of Ten Exemplar Programs Sunflower Health Plan Jennifer Windh September 2016 Long- term services and supports (LTSS) integration is the integration
CAL MEDICONNECT: Understanding the Individualized Care Plan & Interdisciplinary Care Team. Physician Group Webinar Series
 CAL MEDICONNECT: Understanding the Individualized Care Plan & Interdisciplinary Care Team Physician Group Webinar Series Today s Webinar This webinar is part of a series designed specifically for physicians.
CAL MEDICONNECT: Understanding the Individualized Care Plan & Interdisciplinary Care Team Physician Group Webinar Series Today s Webinar This webinar is part of a series designed specifically for physicians.
Molina Medicare Model of Care
 Molina Medicare Model of Care Provider Network Molina Healthcare 2018 1 Molina s Mission and Vision Our Vision: We envision a future where everyone receives quality health care Our Mission: To provide
Molina Medicare Model of Care Provider Network Molina Healthcare 2018 1 Molina s Mission and Vision Our Vision: We envision a future where everyone receives quality health care Our Mission: To provide
Strategy for Quality Improvement in Health Care
 Strategy for Quality Improvement in Health Care Neal D. Kohatsu, MD, MPH, DHCS Medical Director Desiree Backman, DrPH, RD, UC Davis Institute for Population Heath Improvement & DHCS Chief Prevention Officer
Strategy for Quality Improvement in Health Care Neal D. Kohatsu, MD, MPH, DHCS Medical Director Desiree Backman, DrPH, RD, UC Davis Institute for Population Heath Improvement & DHCS Chief Prevention Officer
Model of Care Provider Program. This Model of Care Program only applies to those Members enrolled in Freedom plans.
 Model of Care Provider Program This Model of Care Program only applies to those Members enrolled in Freedom plans. Course Rules and Tools Duration: 30 minutes Approximate time this course will require.
Model of Care Provider Program This Model of Care Program only applies to those Members enrolled in Freedom plans. Course Rules and Tools Duration: 30 minutes Approximate time this course will require.
National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network. Monday, September 12, 2011
 National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network Monday, September 12, 2011 Washington, DC Hyatt Regency on Capitol Hill Yellowstone/Everglades 4:00 PM
National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network Monday, September 12, 2011 Washington, DC Hyatt Regency on Capitol Hill Yellowstone/Everglades 4:00 PM
Standardizing LTSS Assessments for State Initiatives
 Standardizing LTSS Assessments for State Initiatives Barbara Gage, Ph.D. Elizabeth Blair G. Lawrence Atkins, Ph.D. April 30, 2014 Supported by a grant from The SCAN Foundation advancing a coordinated and
Standardizing LTSS Assessments for State Initiatives Barbara Gage, Ph.D. Elizabeth Blair G. Lawrence Atkins, Ph.D. April 30, 2014 Supported by a grant from The SCAN Foundation advancing a coordinated and
Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States
 Advancing innovations in health care delivery for low-income Americans Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States March 6, 2018 Michelle Herman Soper and Alexandra
Advancing innovations in health care delivery for low-income Americans Strengthening Long Term Services and Supports (LTSS): Reform Strategies for States March 6, 2018 Michelle Herman Soper and Alexandra
2014 Model of Care. Provider Training. Molina Medicare _rev_8-14_cab
 2014 Model of Care Provider Training Molina Medicare 2014 5-2013_rev_8-14_cab Course Overview The Model of Care (MOC) is Molina Healthcare s documentation of the CMS directed plan for delivering coordinated
2014 Model of Care Provider Training Molina Medicare 2014 5-2013_rev_8-14_cab Course Overview The Model of Care (MOC) is Molina Healthcare s documentation of the CMS directed plan for delivering coordinated
Schwartz Rounds : Librarian Roles and Opportunities. Midwest Chapter, Medical Library Association Annual Meeting, Rochester, MN October 7, 2012
 Schwartz Rounds : Librarian Roles and Opportunities Midwest Chapter, Medical Library Association Annual Meeting, Rochester, MN October 7, 2012 Founded in 1995 at Massachusetts General Hospital, Boston,
Schwartz Rounds : Librarian Roles and Opportunities Midwest Chapter, Medical Library Association Annual Meeting, Rochester, MN October 7, 2012 Founded in 1995 at Massachusetts General Hospital, Boston,
Comment Template for Care Coordination Standards
 GENERAL COMMENTS Thank you for the opportunity to provide input into these very important standards. We offer the following comments in the spirit of improving clarity, consistency, and ease of reading
GENERAL COMMENTS Thank you for the opportunity to provide input into these very important standards. We offer the following comments in the spirit of improving clarity, consistency, and ease of reading
Creating the Collaborative Care Team
 Creating the Collaborative Care Team Social Innovation Fund July 10, 2013 Social Innovation Fund Corporation for National & Community Service Federal Funder The John A. Hartford Foundation Philanthropic
Creating the Collaborative Care Team Social Innovation Fund July 10, 2013 Social Innovation Fund Corporation for National & Community Service Federal Funder The John A. Hartford Foundation Philanthropic
2019 Medicare Advantage and Part D Advance Notice Parts I and II and Draft Call Letter: Ensuring Access to Medical Rehabilitation Services
 DRAFT March 5, 2018 VIA ELECTRONIC MAIL Seema Verma Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 7500 Security Boulevard Baltimore, MD 21244 Re:
DRAFT March 5, 2018 VIA ELECTRONIC MAIL Seema Verma Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 7500 Security Boulevard Baltimore, MD 21244 Re:
Molina Medicare Model of Care. Healthcare Services Molina Healthcare 2016
 Molina Medicare Model of Care Healthcare Services Molina Healthcare 2016 MHTPS_MOCTRN_062016 1 Molina s Mission Our mission is to provide quality health services to financially vulnerable families and
Molina Medicare Model of Care Healthcare Services Molina Healthcare 2016 MHTPS_MOCTRN_062016 1 Molina s Mission Our mission is to provide quality health services to financially vulnerable families and
NetworkCares (PPO SNP) 2017 Model of Care Training. H5215_360r2_ NHIC 01/2017 m-hm-ncprovpres-0117
 NetworkCares (PPO SNP) 2017 Model of Care Training H5215_360r2_092714 NHIC 01/2017 m-hm-ncprovpres-0117 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training
NetworkCares (PPO SNP) 2017 Model of Care Training H5215_360r2_092714 NHIC 01/2017 m-hm-ncprovpres-0117 Introduction This course is offered to meet the CMS regulatory requirements for Model of Care Training
Welcome to the Agency for Health Care Administration (AHCA) Training Presentation for Managed Medical Assistance Specialty Plans
 Welcome to the Agency for Health Care Administration (AHCA) Training Presentation for Managed Medical Assistance Specialty Plans The presentation will begin momentarily. Please dial in to hear audio: 1-888-670-3525
Welcome to the Agency for Health Care Administration (AHCA) Training Presentation for Managed Medical Assistance Specialty Plans The presentation will begin momentarily. Please dial in to hear audio: 1-888-670-3525
Mild-to-Moderate Mental Health Coverage in Medi-Cal: The Challenge and Promise of Coordination between Counties and Health Plans
 Advancing innovations in health care delivery for low-income Americans Mild-to-Moderate Mental Health Coverage in Medi-Cal: The Challenge and Promise of Coordination between Counties and Health Plans December
Advancing innovations in health care delivery for low-income Americans Mild-to-Moderate Mental Health Coverage in Medi-Cal: The Challenge and Promise of Coordination between Counties and Health Plans December
Center for Health Care Strategies, Inc. From the Beneficiary Perspective: Core Elements to Guide Integrated Care for Dual Eligibles IN BRIEF
 CHCS Center for Health Care Strategies, Inc. From the Beneficiary Perspective: Core Elements to Guide Integrated Care for Dual Eligibles Technical Assistance Brief December 2010 By Alice Lind and Suzanne
CHCS Center for Health Care Strategies, Inc. From the Beneficiary Perspective: Core Elements to Guide Integrated Care for Dual Eligibles Technical Assistance Brief December 2010 By Alice Lind and Suzanne
Model of Care Heritage Provider Network & Arizona Priority Care Model of Care 2018
 Model of Care Model of Care 2018 Learning Objectives Program participants will be able to: List two differences between the Complex Care Management (CCM), and Special Needs Program (SNP) programs. Identify
Model of Care Model of Care 2018 Learning Objectives Program participants will be able to: List two differences between the Complex Care Management (CCM), and Special Needs Program (SNP) programs. Identify
ELDER MEDICAL CARE. Elder Medical. Counseling & Support. Hospice. Care. Care
 ELDER MEDICAL CARE Counseling & Support Elder Medical Care Hospice Care Mission To provide counseling, support and care to anyone with a serious illness, so they may live life to the fullest. Vision We
ELDER MEDICAL CARE Counseling & Support Elder Medical Care Hospice Care Mission To provide counseling, support and care to anyone with a serious illness, so they may live life to the fullest. Vision We
Home Health Value-Based Purchasing Series: HHVBP Model 101. Wednesday, February 3, 2016
 Home Health Value-Based Purchasing Series: HHVBP Model 101 Wednesday, February 3, 2016 About the Alliance 501(c)(3) non-profit research foundation Mission: To support research and education on the value
Home Health Value-Based Purchasing Series: HHVBP Model 101 Wednesday, February 3, 2016 About the Alliance 501(c)(3) non-profit research foundation Mission: To support research and education on the value
At EmblemHealth, we believe in helping people stay healthy, get well and live better.
 At EmblemHealth, we believe in helping people stay healthy, get well and live better. Welcome to the 2017 course on Special Needs Plan Model of Care. This year s course is focused on how we can successfully
At EmblemHealth, we believe in helping people stay healthy, get well and live better. Welcome to the 2017 course on Special Needs Plan Model of Care. This year s course is focused on how we can successfully
Section IX Special Needs & Case Management
 Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
PASRR: What You Need to Know Now HHS PASRR Staff
 PASRR: What You Need to Know Now - 2017 HHS PASRR Staff Session Objectives At the conclusion of this session participants will: Be familiar with recent and upcoming PASRR enhancements Know how to respond
PASRR: What You Need to Know Now - 2017 HHS PASRR Staff Session Objectives At the conclusion of this session participants will: Be familiar with recent and upcoming PASRR enhancements Know how to respond
ACCME NEW MENU OF CRITERIA FOR ACCREDITATION WITH COMMENDATION. Ranae Obregon ISMA - Director of Education
 ACCME NEW MENU OF CRITERIA FOR ACCREDITATION WITH COMMENDATION Ranae Obregon ISMA - Director of Education Implementation ACCME-accredited providers receiving accreditation decisions between November 2017
ACCME NEW MENU OF CRITERIA FOR ACCREDITATION WITH COMMENDATION Ranae Obregon ISMA - Director of Education Implementation ACCME-accredited providers receiving accreditation decisions between November 2017
SELKIRK MENTAL HEALTH CENTRE ACQUIRED BRAIN INJURY PROGRAM MODEL OCTOBER Striving for Excellence in Rehabilitation, Recovery, and Reintegration.
 SELKIRK MENTAL HEALTH CENTRE ACQUIRED BRAIN INJURY PROGRAM MODEL OCTOBER 2008 Striving for Excellence in Rehabilitation, Recovery, and Reintegration. SELKIRK MENTAL HEALTH CENTRE ACQUIRED BRAIN INJURY
SELKIRK MENTAL HEALTH CENTRE ACQUIRED BRAIN INJURY PROGRAM MODEL OCTOBER 2008 Striving for Excellence in Rehabilitation, Recovery, and Reintegration. SELKIRK MENTAL HEALTH CENTRE ACQUIRED BRAIN INJURY
Occupational Therapy Assistant (Degree)
 Occupational Therapy Assistant (Degree) (Associate of Applied Science Degree) Objective The program objective is to prepare the student to enter practice as an entry-level occupational therapy assistant
Occupational Therapy Assistant (Degree) (Associate of Applied Science Degree) Objective The program objective is to prepare the student to enter practice as an entry-level occupational therapy assistant
Telemedicine and Health Reform. Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center
 Telemedicine and Health Reform Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center 1 telehealthresourcecenters.org Links to all TRCs National Webinar Series Reimbursement,
Telemedicine and Health Reform Jonathan Neufeld, PhD Clinical Director Upper Midwest Telehealth Resource Center 1 telehealthresourcecenters.org Links to all TRCs National Webinar Series Reimbursement,
The Power and Possibility of PASRR Webinar Series Webinar Assistance
 The Power and Possibility of PASRR Webinar Series Webinar Assistance http://www.pasrrassist.org/resources/webinar-assistance-and-faqs Call-in through one of two ways listed below: Telephone: 1. Locate
The Power and Possibility of PASRR Webinar Series Webinar Assistance http://www.pasrrassist.org/resources/webinar-assistance-and-faqs Call-in through one of two ways listed below: Telephone: 1. Locate
THE PARENT IS YOUR PATIENT TOO!
 THE PARENT IS YOUR PATIENT TOO! MAKING THE CASE FOR INTIMATE PARTNER VIOLENCE ADVOCACY IN THE PEDIATRIC SETTING May 10, 2017 Note: Listen to the webinar using your computer s speakers. There is no phone
THE PARENT IS YOUR PATIENT TOO! MAKING THE CASE FOR INTIMATE PARTNER VIOLENCE ADVOCACY IN THE PEDIATRIC SETTING May 10, 2017 Note: Listen to the webinar using your computer s speakers. There is no phone
Opportunities for Medicaid-Public Health Collaboration to Achieve Mutual Prevention Goals: Lessons from CDC s 6 18 Initiative
 Advancing innovations in health care delivery for low-income Americans Opportunities for Medicaid-Public Health Collaboration to Achieve Mutual Prevention Goals: Lessons from CDC s 6 18 Initiative June
Advancing innovations in health care delivery for low-income Americans Opportunities for Medicaid-Public Health Collaboration to Achieve Mutual Prevention Goals: Lessons from CDC s 6 18 Initiative June
kaiser medicaid and the uninsured commission on O L I C Y
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured 1330 G S T R E E T NW, W A S H I N G T O N, DC 20005 P H O N E: (202) 347-5270, F A X: ( 202) 347-5274 W E B S I T E: W W W. K F F.
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured 1330 G S T R E E T NW, W A S H I N G T O N, DC 20005 P H O N E: (202) 347-5270, F A X: ( 202) 347-5274 W E B S I T E: W W W. K F F.
Beyond Cost and Utilization: Rethinking Evaluation Strategies for Complex Care Programs
 Beyond Cost and Utilization: Rethinking Evaluation Strategies for Complex Care Programs April 9, 2-3:30 pm (ET) Made possible with support from Kaiser Permanente Community Health Housekeeping This event
Beyond Cost and Utilization: Rethinking Evaluation Strategies for Complex Care Programs April 9, 2-3:30 pm (ET) Made possible with support from Kaiser Permanente Community Health Housekeeping This event
MEDICALLY COMPLEX CHILDREN S WAIVER
 MEDICALLY COMPLEX CHILDREN S WAIVER About Us Who is South Carolina Solutions? We are a part of a Family of Companies. Our corporate office, Community Health Solutions, is located in St. Petersburg, FL.
MEDICALLY COMPLEX CHILDREN S WAIVER About Us Who is South Carolina Solutions? We are a part of a Family of Companies. Our corporate office, Community Health Solutions, is located in St. Petersburg, FL.
Program of All-inclusive Care for the Elderly (PACE) Summary and Recommendations
 Program of All-inclusive Care for the Elderly (PACE) PACE Policy Summit Summary and Recommendations PACE Policy Summit On December 6, 2010, the National PACE Association (NPA) convened a policy summit
Program of All-inclusive Care for the Elderly (PACE) PACE Policy Summit Summary and Recommendations PACE Policy Summit On December 6, 2010, the National PACE Association (NPA) convened a policy summit
Going The Distance To Improve The Care Span: The Duel Over The Dual Eligibles And The Implications For Health Reform
 + Going The Distance To Improve The Care Span: The Duel Over The Dual Eligibles And The Implications For Health Reform By Susan Dentzer Editor in Chief, Health Affairs Presentation to the First National
+ Going The Distance To Improve The Care Span: The Duel Over The Dual Eligibles And The Implications For Health Reform By Susan Dentzer Editor in Chief, Health Affairs Presentation to the First National
Options for Integrating Care for Dual Eligible Beneficiaries
 CHCS Center for Health Care Strategies, Inc. Technical Assistance Brief Options for Integrating Care for Dual Eligible Beneficiaries By Melanie Bella and Lindsay Palmer-Barnette, Center for Health Care
CHCS Center for Health Care Strategies, Inc. Technical Assistance Brief Options for Integrating Care for Dual Eligible Beneficiaries By Melanie Bella and Lindsay Palmer-Barnette, Center for Health Care
Karen Stasium, BS, MPT, COS C, HCS D
 Karen Stasium, BS, MPT, COS C, HCS D Objectives Demonstrate how home health therapists are an integral part of minimizing re hospitalizations and safely transitioning the patient from hospital to home
Karen Stasium, BS, MPT, COS C, HCS D Objectives Demonstrate how home health therapists are an integral part of minimizing re hospitalizations and safely transitioning the patient from hospital to home
MedPAC June 2013 Report to Congress: Medicare and the Health Care Delivery System
 MedPAC June 2013 Report to Congress: Medicare and the Health Care Delivery System STEPHANIE KENNAN, SENIOR VICE PRESIDENT 202.857.2922 skennan@mwcllc.com 2001 K Street N.W. Suite 400 Washington, DC 20006-1040
MedPAC June 2013 Report to Congress: Medicare and the Health Care Delivery System STEPHANIE KENNAN, SENIOR VICE PRESIDENT 202.857.2922 skennan@mwcllc.com 2001 K Street N.W. Suite 400 Washington, DC 20006-1040
Advisory Panel on Health System Structure Saskatchewan Ministry of Health 3475 Albert St. Regina, Saskatchewan S4S 6X6
 Saskatchewan Registered Nurses' Association 2066 Retallack Street Regina, Saskatchewan, S4T 7X5 Advisory Panel on Health System Structure Saskatchewan Ministry of Health 3475 Albert St. Regina, Saskatchewan
Saskatchewan Registered Nurses' Association 2066 Retallack Street Regina, Saskatchewan, S4T 7X5 Advisory Panel on Health System Structure Saskatchewan Ministry of Health 3475 Albert St. Regina, Saskatchewan
Special Needs Plan (SNP) Model of Care Training 2018
 Special Needs Plan (SNP) Model of Care Training 2018 Table of Contents Training Overview Pg. 1 Denver Health Medical Plan s (HMO SNP) MOC Annual Training Pg. 2 Special Needs Plans (SNPs) Pg. 2 Special
Special Needs Plan (SNP) Model of Care Training 2018 Table of Contents Training Overview Pg. 1 Denver Health Medical Plan s (HMO SNP) MOC Annual Training Pg. 2 Special Needs Plans (SNPs) Pg. 2 Special
Preventing Sepsis: National Efforts and New Home Care Initiative in New York State A Presentation to the StateWide Senior Action Council
 Preventing Sepsis: National Efforts and New Home Care Initiative in New York State A Presentation to the StateWide Senior Action Council by Amy Bowerman, RN Al Cardillo, LMSW Tom Heymann, MBA Mohawk Valley
Preventing Sepsis: National Efforts and New Home Care Initiative in New York State A Presentation to the StateWide Senior Action Council by Amy Bowerman, RN Al Cardillo, LMSW Tom Heymann, MBA Mohawk Valley
Chapter 2 Provider Responsibilities Unit 6: Behavioral Health Care Specialists
 Chapter 2 Provider Responsibilities Unit 6: Health Care Specialists In This Unit Unit 6: Health Care Specialists General Information 2 Highmark s Health Programs 4 Accessibility Standards For Health Providers
Chapter 2 Provider Responsibilities Unit 6: Health Care Specialists In This Unit Unit 6: Health Care Specialists General Information 2 Highmark s Health Programs 4 Accessibility Standards For Health Providers
Implementing Coordinated Care for Dual Eligibles: Conflicts and Opportunities Prepared by James M. Verdier Mathematica Policy Research
 Implementing Coordinated Care for Dual Eligibles: Conflicts and Opportunities Prepared by James M. Verdier Mathematica Policy Research Workshop on Effectively Integrating Care for Dual Eligibles World
Implementing Coordinated Care for Dual Eligibles: Conflicts and Opportunities Prepared by James M. Verdier Mathematica Policy Research Workshop on Effectively Integrating Care for Dual Eligibles World
Transitions of Care: From Hospital to Home
 Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
Transitions of Care: From Hospital to Home Danielle Hansen, DO, MS (Med Ed) Associate Director, LECOM VP Acute Care Services & Quality/Performance Improvement, Millcreek Community Hospital Objectives Discuss
Model of Care Training
 Medicare Advantage Special Needs Plan Chronic Care Program Model of Care Training 2012-2013 Course Overview This course will describe: PHP s Model of Care Chronic Care Program Health Homes Interdisciplinary
Medicare Advantage Special Needs Plan Chronic Care Program Model of Care Training 2012-2013 Course Overview This course will describe: PHP s Model of Care Chronic Care Program Health Homes Interdisciplinary
EDUCATIONAL RESOURCES. Uniform Data System for Medical Rehabilitation
 EDUCATIONAL RESOURCES Uniform Data System for Medical Rehabilitation Educational Resources Workshops* UDSmr offers subscribers and nonsubscribers a large array of educational services and products: Workshops
EDUCATIONAL RESOURCES Uniform Data System for Medical Rehabilitation Educational Resources Workshops* UDSmr offers subscribers and nonsubscribers a large array of educational services and products: Workshops
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH
 IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
IMPROVING TRANSITIONS OF CARE IN POPULATION HEALTH TABLE OF CONTENTS 1. The Transitions Challenge 2. Impact of Care Transitions 3. Patient Insights from Project Boost 4. Identifying Patients 5. Improving
September 22, 2017 VIA ELECTRONIC SUBMISSION
 September 22, 2017 VIA ELECTRONIC SUBMISSION The Honorable Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services 7500 Security Boulevard Baltimore,
September 22, 2017 VIA ELECTRONIC SUBMISSION The Honorable Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services 7500 Security Boulevard Baltimore,
08/06/2015. Special Needs Plans. SNP Legislative History Highlights
 National Training Program RO V & RO VII St. Louis, August 10-11, 2015 Special Needs Plans Medicare SNPs are a type of Medicare Advantage Plan (like an HMO or PPO). Medicare SNPs limit membership to people
National Training Program RO V & RO VII St. Louis, August 10-11, 2015 Special Needs Plans Medicare SNPs are a type of Medicare Advantage Plan (like an HMO or PPO). Medicare SNPs limit membership to people
4. Responsibilities: Consistent with this MOU, it is AGREED that the Parties shall:
 MEMORANDUM OF UNDERSTANDING BETWEEN DEPARTMENT OF VETERANS AFFAIRS (VA) AND DEPARTMENT OF DEFENSE (DoD) FOR INTERAGENCY COMPLEX CARE COORDINATION REQUIREMENTS FOR SERVICE MEMBERS AND VETERANS 1. PURPOSE:
MEMORANDUM OF UNDERSTANDING BETWEEN DEPARTMENT OF VETERANS AFFAIRS (VA) AND DEPARTMENT OF DEFENSE (DoD) FOR INTERAGENCY COMPLEX CARE COORDINATION REQUIREMENTS FOR SERVICE MEMBERS AND VETERANS 1. PURPOSE:
CareMore Special Needs Plans Model of Care. Annual Evaluation 2015 Performance
 CareMore Special Needs Plans Model of Care Annual Evaluation 2015 Performance The Special Needs Plans (SNPs) Medicare SNPs are a type of Medicare Advantage Plan (like an HMO or PPO). Medicare SNPs limit
CareMore Special Needs Plans Model of Care Annual Evaluation 2015 Performance The Special Needs Plans (SNPs) Medicare SNPs are a type of Medicare Advantage Plan (like an HMO or PPO). Medicare SNPs limit
A Care Coordination Model for Value-Based Performance Programs
 A Care Coordination Model for Value-Based Performance Programs Richard S. Chung, MD Chief Clinical Officer APS Healthcare 8th National Pay for Performance (P4P) Summit February 20, 2013 Hyatt Regency Hotel,
A Care Coordination Model for Value-Based Performance Programs Richard S. Chung, MD Chief Clinical Officer APS Healthcare 8th National Pay for Performance (P4P) Summit February 20, 2013 Hyatt Regency Hotel,
WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service
 WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service WakeMed Rehab Hospital provides an integrated, comprehensive delivery of rehabilitation services utilizing evidenced-based practice directed
WakeMed Rehab Hospital Stroke Rehabilitation Scope of Service WakeMed Rehab Hospital provides an integrated, comprehensive delivery of rehabilitation services utilizing evidenced-based practice directed
CMS-0044-P; Proposed Rule: Medicare and Medicaid Programs; Electronic Health Record Incentive Program Stage 2
 May 7, 2012 Submitted Electronically Ms. Marilyn Tavenner Acting Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Room 445-G, Hubert H. Humphrey Building
May 7, 2012 Submitted Electronically Ms. Marilyn Tavenner Acting Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Room 445-G, Hubert H. Humphrey Building
VNAA BLUEPRINT FOR EXCELLENCE BEST PRACTICES TO REDUCE HOSPITAL ADMISSIONS FROM HOME CARE. Training Slides
 VNAA BLUEPRINT FOR EXCELLENCE BEST PRACTICES TO REDUCE HOSPITAL ADMISSIONS FROM HOME CARE Training Slides 061015 Why Take Action to Prevent Readmissions? Better patient care and patient experience Home
VNAA BLUEPRINT FOR EXCELLENCE BEST PRACTICES TO REDUCE HOSPITAL ADMISSIONS FROM HOME CARE Training Slides 061015 Why Take Action to Prevent Readmissions? Better patient care and patient experience Home
Exhibit A. Part 1 Statement of Work
 Exhibit A Part 1 Statement of Work Contractor shall provide Basic Neurological services as described herein to Medicaid eligible Clients who are authorized to receive services at the Contractor s owned
Exhibit A Part 1 Statement of Work Contractor shall provide Basic Neurological services as described herein to Medicaid eligible Clients who are authorized to receive services at the Contractor s owned
GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 4 ALTERNATE LIVING ARRANGEMENTS
 GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 4 ALTERNATE LIVING ARRANGEMENTS Table of Contents Introduction... 2 Purpose... 2 Serving Senior Medicare-Medicaid Enrollees... 2 How to Use This Tool... 2
GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 4 ALTERNATE LIVING ARRANGEMENTS Table of Contents Introduction... 2 Purpose... 2 Serving Senior Medicare-Medicaid Enrollees... 2 How to Use This Tool... 2
5/26/2015. January 26, 2015 INCENTIVES AND PENALTIES. Medicare Readmission Penalties. CMS Bundled Payment Providers & ACOs in NE
 Agenda ESTABLISHING SHARED EXPECTATIONS New tool of ACOs, Bundled Payments & Readmission Reduction Update on current market pressures driving a focus on care across settings & over time at lowest cost
Agenda ESTABLISHING SHARED EXPECTATIONS New tool of ACOs, Bundled Payments & Readmission Reduction Update on current market pressures driving a focus on care across settings & over time at lowest cost
The Evolving Landscape of Healthcare Payment: Incentive Programs and ACO Model Optimization. Quality Forum August 19, 2015
 The Evolving Landscape of Healthcare Payment: Incentive Programs and ACO Model Optimization Quality Forum August 19, 2015 Ross Manson rmanson@eidebailly.com 701.239.8634 Barb Pritchard bpritchard@eidebailly.com
The Evolving Landscape of Healthcare Payment: Incentive Programs and ACO Model Optimization Quality Forum August 19, 2015 Ross Manson rmanson@eidebailly.com 701.239.8634 Barb Pritchard bpritchard@eidebailly.com
Best Practices in Care Coordination & Transitions of Care Communications
 Best Practices in Care Coordination & Transitions of Care Communications Jessica Carpenter, MS, RD, LDN Director, Disability and Community Services University of Massachusetts Medical School Overview/Agenda
Best Practices in Care Coordination & Transitions of Care Communications Jessica Carpenter, MS, RD, LDN Director, Disability and Community Services University of Massachusetts Medical School Overview/Agenda
Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary
 Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary The Medicaid and CHIP Payment and Access Commission (MACPAC) was established in the Children's Health Insurance Program
Medicaid and CHIP Payment and Access Commission (MACPAC) February 2013 Meeting Summary The Medicaid and CHIP Payment and Access Commission (MACPAC) was established in the Children's Health Insurance Program
Primary Care 101: A Glossary for Prevention Practitioners
 PREVENTION COLLABORATION IN ACTION Engaging the Right Partners Primary Care 101: A Glossary for Prevention Practitioners As the U.S. healthcare landscape continues to change under the Affordable Care Act
PREVENTION COLLABORATION IN ACTION Engaging the Right Partners Primary Care 101: A Glossary for Prevention Practitioners As the U.S. healthcare landscape continues to change under the Affordable Care Act
Welcome to the Webinar!
 Welcome to the Webinar! We will begin the presentation shortly. Thank you for your patience. Attendees can access the presentation slides now at: http://www.mctac.org/page/events A recording of the event
Welcome to the Webinar! We will begin the presentation shortly. Thank you for your patience. Attendees can access the presentation slides now at: http://www.mctac.org/page/events A recording of the event
FIDA. Care Management for ALL
 Care Management for ALL In 2011, Governor Andrew M. Cuomo established a Medicaid Redesign Team (MRT), which initiated significant reforms to the state s Medicaid program. This included a critical initiative
Care Management for ALL In 2011, Governor Andrew M. Cuomo established a Medicaid Redesign Team (MRT), which initiated significant reforms to the state s Medicaid program. This included a critical initiative
Care Model for Tufts Health Plan Senior Care Options
 Care Model for Tufts Health Plan Senior Care Options Tufts Health Plan Core Principles The overarching construct for the Tufts Health Plan Senior Care Options (SCO-SNP) is to improve access to medical,
Care Model for Tufts Health Plan Senior Care Options Tufts Health Plan Core Principles The overarching construct for the Tufts Health Plan Senior Care Options (SCO-SNP) is to improve access to medical,
Professional Development & Training Series: Behavioral Health Quality Assurance (BHQA) Staff
 Professional Development & Training Series: Behavioral Health Quality Assurance (BHQA) Staff Workshop #2: California s Medicaid State Plan: Specialty Mental Health Services & Expanded Definitions San Francisco
Professional Development & Training Series: Behavioral Health Quality Assurance (BHQA) Staff Workshop #2: California s Medicaid State Plan: Specialty Mental Health Services & Expanded Definitions San Francisco
North East Behavioural Supports Ontario Sustainability Plan
 North East Behavioural Supports Ontario Sustainability Plan - 2 - NORTH EAST LHIN BSO SUSTAINABILITY PLAN The development of the North East BSO sustainability plan has provided the North East LHIN with
North East Behavioural Supports Ontario Sustainability Plan - 2 - NORTH EAST LHIN BSO SUSTAINABILITY PLAN The development of the North East BSO sustainability plan has provided the North East LHIN with
Troubleshooting Audio
 Welcome! Audio for this event is available via ReadyTalk Internet Streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome! Audio for this event is available via ReadyTalk Internet Streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
STROKE REHAB PROGRAM
 STROKE REHAB PROGRAM Allied Rehab Hospital is part of Allied Services Integrated Health System, the premier post-acute health-care system in Northeast Pennsylvania, and is the region s leading provider
STROKE REHAB PROGRAM Allied Rehab Hospital is part of Allied Services Integrated Health System, the premier post-acute health-care system in Northeast Pennsylvania, and is the region s leading provider
Improving healthcare for people with special or supportive-care needs
 Kara Carter, Razili Lewis, and Tim Ward Improving healthcare for people with special or supportive-care needs Healthcare Systems & Services September 2016 Certain individuals have especially complex medical
Kara Carter, Razili Lewis, and Tim Ward Improving healthcare for people with special or supportive-care needs Healthcare Systems & Services September 2016 Certain individuals have especially complex medical
Home Health. Improving Patient Outcomes & Reducing Readmissions. Home Health: Improving Outcomes & Reducing Readmissions
 Home Health Improving Patient Outcomes & Reducing Readmissions Home Health: Improving Outcomes & Reducing Readmissions Benefits of Home Health Care Scientific evidence proves people heal more quickly,
Home Health Improving Patient Outcomes & Reducing Readmissions Home Health: Improving Outcomes & Reducing Readmissions Benefits of Home Health Care Scientific evidence proves people heal more quickly,
Why Shepherd? Shepherd Center Patients. Here s How We Measure Up: Shepherd Patient Population
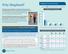 Center Patients Total Patients ABI Patients SCI Patients Other Patients Center specializes in medical treatment, research and rehabilitation for people with spinal cord and brain injury. In CY, had 911
Center Patients Total Patients ABI Patients SCI Patients Other Patients Center specializes in medical treatment, research and rehabilitation for people with spinal cord and brain injury. In CY, had 911
Troubleshooting Audio
 Welcome! Presentation slides can be downloaded from www.qualityreportingcenter.com under Upcoming Events on the right-hand side of the page. Audio for this event is available via ReadyTalk Internet streaming.
Welcome! Presentation slides can be downloaded from www.qualityreportingcenter.com under Upcoming Events on the right-hand side of the page. Audio for this event is available via ReadyTalk Internet streaming.
