VHA Safe Patient Handling and Mobility Algorithms (2014 revision) Algorithm 4: Reposition in Chair: Wheelchair, Dependency Chair or Other Chair
|
|
|
- Gregory Henry
- 5 years ago
- Views:
Transcription
1 VHA Safe Patient Handling and Mobility Algorithms (2014 revision) Algorithm 1: Transfer To/From Seated Positions: Bed to Chair, Chair to Chair, Chair to Exam Table Algorithm 2: Lateral Transfer to/from Supine Positions: Bed, Stretcher, Trolley, Procedure Table Algorithm 3: Repositioning in Bed Algorithm 4: Reposition in Chair: Wheelchair, Dependency Chair or Other Chair Algorithm 5: Transport in Bed/Stretcher/Wheelchair Algorithm 6: Toileting Algorithm 7: Showering and Bathing Algorithm 8: Floor/Fall Recovery Algorithm 9: Transfer between Vehicle and Wheelchair, Powered Wheelchair, or Stretcher Algorithm 10: Ambulation Algorithm 11: Patient Handling Task Requiring Lifting of Extremities Algorithm 12: Bariatric Patient Handling Task Requiring Access to Abdominal Area Algorithm 13: Bariatric Patient Handling Task Requiring Access to Perineal Area
2
3 Algorithm 1 Notes SPECIFIC If patient has partial weight-bearing capacity, transfer toward stronger side. Ensure all chairs, beds, stretchers, etc. are locked. To use seated transfer aid, chair arms must recess or be removable. High/low beds, adjustable exam tables and stretchers are ideal for making transfers easier. Always transfer towards stronger side. NEVER use a gait belt to lift, transfer, or catch a patient. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. Verify equipment is locked prior to transfer/movement. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. Working height should be appropriate for staff safety, at about elbow height. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Abdominal binder/pannus sling may be necessary to prevent abdominal area from interfering with patient handling task/transfer. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
4
5 Algorithm 2 Notes SPECIFIC Confirm destination surfaces (bed, stretcher, exam table, etc.) and patient handling equipment MEET WEIGHT, WIDTH, and HEIGHT REQUIREMENTS of patient If patient needs to be pulled up in bed prior to transfer, see Repositioning in Bed (Algorithm 3). High/low beds, adjustable exam tables and stretchers are ideal for making transfers easier. Lock all wheeled equipment before transfer. When using air assisted lateral transfer device, ALWAYS move feet first, followed by upper torso and head, to determine if is safe to continue the move and to prevent patient from falling through the space between sending and receiving surfaces. Destination surface should be ½" lower than sending surface for all lateral patient moves. Ensure that at least one caregiver is on the destination side. For patients with delicate skin or pressure ulcers, care must be taken to avoid shearing force by dragging patient against surfaces. Friction reducing devices vary greatly in design and efficiency. Sometimes a combination of a slide board and another type can reduce forces more than either one alone. The force required to logroll a patient is about 32% of the patient's body weight Caregivers should avoid push or pull forces greater than 20% of their own weight. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient's head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Increase ease in inserting seated slings by using friction reducing device or lateral transfer device. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. Working height should be appropriate for staff safety, at about elbow height. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient's weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
6
7 Algorithm 3 Notes SPECIFIC DO NOT PULL FROM HEAD OF BED. Manual patient repositioning is dangerous. Discourage and remove draw sheets from beds and replace them with full body slings for repositioning. Using draw sheets on beds gives conflicting messages and makes the transition to technology use more difficult. The repositioning sling should be placed before a dependent patient is transferred to the surface. Inflate mattress of low air loss beds to maximum setting to assist in repositioning. Although some specialty beds turn and/or rotate the patient, most specialists confirm that bed rotations are not sufficient to off load pressure off patient and recommend that use of a repositioning sling is the best option for full turns. Confirm with Wound Care that off-loading pressure is accomplished appropriately. When using bed repositioning option, caregiver must assess skin integrity, support the turn, adjust limbs and provide pillow supports. For patients with delicate skin or pressure ulcers, care must be taken to avoid shearing force. Working height should be appropriate for staff safety, at about elbow height. For patients that can assist in moving up in bed, to encourage them to help, ask the patient to hold on the side rails above head, to help pull themselves up in bed, then to flex knees and push on the count of three. Verify equipment is locked prior to transfer/movement. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. The force required to logroll a patient is about 32% of the patient's body weight The force required to pull a dependent patient on a draw sheet is about 72.6% of the patient's body weight Caregivers should avoid push or pull forces greater than 20% of their own weight. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Most bariatric patients have to have the head of the bed elevated at all times to facilitate ease in breathing during repositioning tasks. Encourage patient to move as much as possible independently to minimize caregiver handling tasks and foster patient independence and worsening of functional abilities. Use foam mattresses for patients who have some functional ability if the patient's condition permits. Self-mobilization is easier on a foam mattress than a Low Air Loss Mattress. Use a sealed, high-density foam wedge or similar device to assist in maintaining positioning Some patients have poor tolerance for turns greater than 30 degrees. Keep repositioning sling under patient at all times to minimize high risk handling tasks, if possible. When Low air loss mattress is required the patient is likely to slide down in bed frequently due to slippery mattress cover; use of a repositioning sling under patient facilitates routine movement and will offer patient comfort. Consider use of 2 padded twin turners or bariatric limb slings, one over upper torso/back and one over buttocks area, to turn and reposition patient when there is a need to access the back for wound care. Utilize friction reducing devices to insert twin turner or limb holders. Expanded capacity turning, limb holding, and repositioning slings may help with repositioning patients during bathing. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Abdominal binder/pannus sling may be necessary to prevent abdominal area from interfering with patient handling task/transfer. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
8
9 Algorithm 4 Notes SPECIFIC Take full advantage of chair functions, such as a chair that reclines. May use arm rest to facilitate repositioning. Make sure chair wheels are locked. Friction reducing devices for seated repositioning vary greatly. One way slides, slide sheets, or thin, small slide boards may be appropriate. Do NOT push on knees without friction reduction or manually lift a patient up in a chair. NEVER use a gait belt to lift, transfer, or catch a patient. Caregivers should avoid push or pull forces greater than 20% of their own weight. Avoid shearing forces. Always be aware of and use stronger side, if appropriate. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. Utilize one way slide cushion as much as possible to minimize repositioning needs in chair. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Most bariatric patients are unable to sit upright in seated position due to large abdomen obstructing sitting, so facilitate seating in modified recline for patient comfort and ease in breathing. Verify the bariatric chair meets patient's weight and width at widest part of body, and facilitate ability of patients' feet to reach the floor for safety and comfort. Utilize the seated full body sling that fits the patient's size to position patient during repositioning of patient in chair. Avoid having patient sit on the sling for prolonged periods in a way that would create pressure points. Most bariatric patients require padded slings during positioning in chair. Encourage patient to reposition self as much as possible independently. Often bariatric patients have swelling and poor circulation in the legs, so consider keeping legs elevated on pillows, using limb sling to reposition legs as needed. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Abdominal binder/pannus sling may be necessary to prevent abdominal area from interfering with patient handling task/transfer. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
10
11 Algorithm 5 Notes SPECIFIC Appropriate mode and route of transport requires information gathering prior to transport: What equipment can receiving environment accommodate? Some areas may require stretcher or chair as opposed to bed. What does receiving area require? (i.e., seated patient, patient on air device, specific bed features, etc.) Is width/length/weight capacity of devices adequate for patient? What is the easiest and safest route to transport patient (even surfaces, no inclines, etc.)? If the patient has respiratory distress, the stretcher must be able to maintain a high Fowler's position. If powered devices are not available, use newer transport devices that are meant for transport. Heavy beds (including sand beds) or small wheels will add to difficulty. Plan a path to avoid obstacles, narrow doors, slopes, carpet, tight turns, or sudden stops and to ensure bed/stretcher/wheel chair can be accommodated along the pathway. Verify equipment is locked prior to transferring patient onto or off of transport device. Confirm elevator will accommodate specialty beds and expanded capacity beds/stretchers. Caregivers should avoid push or pull forces greater than 20% of their own weight. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Determine if the stretcher/bed is wide enough for patient to reposition self as needed. Transport devices should be powered if at all possible. Verify that device is fully charged and ready for use at all times. Transport with head in upright or elevated position. Pre-plan the route to transport the patient to facilitate patient respect and dignity as well as ease in maneuvering through wider spaces. Pre-plan transport to morgue upon end of life, using repositioning sling or lateral air transfer device under body bag to minimize transfer risks. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
12
13 Algorithm 6 Notes SPECIFIC Prior to transport, determine if bathroom doorway can accommodate entry of lift and/or wheelchair, staff, and patient. Thresholds may present a problem. Consult with Engineering Service to lower if problematic. If using seated transfer aid, chair arms must recess or be removable. If patient has partial weight-bearing capacity, transfer toward stronger side. Use of powered toilet lift seat facilitates a safer process. Toileting slings (bariatric and non-bariatric) are available for toileting. Verify equipment is locked prior to transfer onto or off of commode. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Check toilet weight capacity. A bariatric patient may need an expanded capacity commode chair, steel toilet, or toilet with enhanced weight support. A standard porcelain toilet typically has a weight limit of 350 pounds. Even a floor-bearing toilet may shear under weight. A standard bathroom toilet often does not provide adequate space for the body of a bariatric patient; use of an expanded capacity commode over a toilet provides safety and privacy for the patient. Place bariatric patient in a room where there is full access to ceiling lift throughout the room, into the shower and over the toilet using one move if available. Use correct size and padded hygiene slings for toileting and showering tasks. Use bariatric standing assist device, if appropriate, to facilitate independence in toileting and preserve as much function as possible. Consider bariatric powered lift toilets if appropriate. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
14
15 Algorithm 7 Notes SPECIFIC Mesh slings (bariatric and non-bariatric) are available for bathing. Turning, limb holding, and repositioning slings may help with repositioning patients during bathing. Verify equipment is locked prior to transfer/movement. Always be aware of and use stronger side, if appropriate. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
16
17 Algorithm 8 Notes SPECIFIC Do not manually lift a patient from the floor. Use SPHM technology. Medical precautions or stabilization do not require manual lifting. A Back Board can be lifted with a repositioning or supine sling or with straps built to connect back board to lift. Some lifts have stretcher attachments to keep a patient flat. Do not allow patient to lean on caregiver for support. Lift connection must go low enough to reach sling connections (loops or clips) without pulling patient up manually to attach. Friction reducing devices aid in transferring a patient onto lifting devices, back boards or slings. If patient falls in a difficult to access area, consider inserting air assisted lifting and/or lateral transfer device or lift sling under patient to facilitate pulling patient out of hard to access area. Sling or air assistive device can then be used to lift the patient. Preserve dignity by facilitating privacy for fall rescue when possible. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. Verify equipment is locked prior to transfer/movement. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. Working height should be appropriate for staff safety, at about elbow height. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Elevate head with pillow prior to moving patient to facilitate patient comfort and ease in breathing. If using air assisted lifting and lateral transfer devices, consider placing seated, supine, or repositioning sling on top of air assisted lateral transfer device prior to placement under patient. Fall rescue will require three or more caregivers to help pick patient up from the floor using lifting devices. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. Suggest applying a sticker to all bariatric equipment with EC (expanded capacity) and the weight capacity of the equipment. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
18
19 Algorithm 9 Notes SPECIFIC Vehicle transfer will be hazardous whenever the patient is combative. Use more staff and minimize contact with the patient. NEVER use a gait belt to lift or transfer a patient. For seated transfer aid, chair must have arms that recess or are removable. Verify equipment is locked prior to transfer/movement. Always transfer towards stronger side, if possible. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. Increase ease in inserting slings by using friction reducing device or lateral transfer device. Verify equipment is locked prior to transfer/movement. If using seated sling, air assisted lateral transfer device or friction reducing device, obtain facility direction for leaving under patient. Working height should be appropriate for staff safety, at about elbow height. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Conditions likely to affect transfer/repositioning techniques. Hip/Knee/Shoulder Replacements Respiratory/Cardiac Compromise Fractures History of Falls Wounds Affecting Transfer/Positioning Splints/Traction Paralysis/Paresis Amputation Severe Osteoporosis Unstable Spine Urinary/Fecal Stoma Severe Pain/Discomfort Severe Edema Contractures/Spasms Postural Hypotension Very Fragile Skin Tubes (IV, Chest, etc.) BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Bariatric size chairs and powered stretchers need to be wide enough to accommodate patient s width and height for patient safety and comfort. Keep patient s head elevated during transfer and transport. If coordinating transport, verify transport vehicle is large enough to accommodate patient, staff, and patient handling equipment. Keep repositioning sling or air transfer device under patient to facilitate lateral transfers if allowed and appropriate. Pre-plan route to minimize transport risks over rough terrain or up or down inclines. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
20
21 Algorithm 10 Notes SPECIFIC Do not bear patient s weight or allow patient to lean on caregiver for support. Assure that lift and sling capacity, size and design can accommodate patient without damage or groin pain. Ambulation slings have a wide range of designs intended to support chest, thighs, and/or pannus. Some designs or patient conditions may require the use of protective undergarments. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
22
23 Algorithm 11 Notes SPECIFIC During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient s weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach,, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. Working height should be appropriate for staff safety, at about elbow height. Increase ease in inserting slings by using friction reducing device or lateral transfer device. Modify use of a bariatric seated sling to elevate limbs for bathing or wound care. To determine safety of lifting an appendage, use the following. A man s leg is approximately 16% of the total body weight. The head is approximately 8%, and an arm is approximately 5%. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers. BARIATRIC For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI over 40 is considered to increase the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, and waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. Consider use of two or more of padded limb holders to support limbs using a four point hanger bar. Consider seated sling straps to support limbs for procedures. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Abdominal binder/pannus sling may be necessary to prevent abdominal area from interfering with patient handling task/transfer. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Inserting sling and/or friction reducing device from head to toe or toe to head rather than log rolling may make sling placement easier. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently.
24
25 Algorithm 12 Notes SPECIFIC During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient's weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. To determine safety of lifting an appendage, use the following. A man's leg is approximately 16% of the total body weight. The head is approximately 8%, and an arm is approximately 5%. Working height should be appropriate for staff safety, at about elbow height. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently. For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI or over 40 is considered a patient that increases the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers.
26
27 Algorithm 13 Notes SPECIFIC During any patient task, under the best of circumstances (no lines, tubes, contractures, etc.), a caregiver may lift no more than 35 pounds of a patient's weight (body, head, appendages). If tubes, lines and other patient items or conditions influencing patient handling are present, or staff must bend, twist or reach, the permissible lifting weight is decreased. If weight limit is exceeded, assistive devices must be used if possible. To determine safety of lifting an appendage, use the following. A man's leg is approximately 16% of the total body weight. The head is approximately 8%, and an arm is approximately 5%. Working height should be appropriate for staff safety, at about elbow height. Prior to starting task, CONFIRM patient handling equipment, slings, and destination locations (bed, commode, wheelchair, etc.) meet WEIGHT, WIDTH, AND HEIGHT requirements of patient. Bariatric patients require more caregivers. Identify a leader when performing tasks with multiple caregivers in order to synchronize efforts and increase safety. Abdominal binder/pannus sling may be necessary to prevent abdominal area from interfering with patient handling task/transfer. A friction reducing device will facilitate insertion and removal of a sling under a bariatric patient. Working height should be appropriate for staff safety, at about elbow height. A multidisciplinary team should problem solve these tasks, communicate to all caregivers, refine as needed and perform consistently. For patient handling purposes, any patient that weighs more than 300 pounds, or 100 pounds over ideal weight, or who has a BMI or over 40 is considered a patient that increases the risk for caregivers while performing patient handling. Waist circumference is also used to identify bariatric patients. Weight, height, waist diameter, waist circumference should be collected on these patients in order to provide safe care and select appropriate equipment, beds, stretchers, wheelchairs, lifts, and other devices. GENERAL NEVER lift patients manually except under emergency situations such as during an active patient code. NEVER catch a falling patient! A caregiver probably cannot stop a patient from falling. Quickly remove obstacles out of the way that may injure the patient s head. Do not allow patient to lean or pull/grab on caregiver for support in movements. Allow and encourage patients to move on their own as much as it is safe to do so. Ask patient what steps can be taken to facilitate ease and comfort in their movement and mobility as they typically understand their strengths and weaknesses. Avoid shearing forces, especially for patients with delicate skin or pressure ulcers.
Chapter 14. Body Mechanics and Safe Resident Handling, Positioning, and Transfers
 Chapter 14 Body Mechanics and Safe Resident Handling, Positioning, and Transfers Body Mechanics Body mechanics means using the body in an efficient and careful way. It involves: Good posture Balance Using
Chapter 14 Body Mechanics and Safe Resident Handling, Positioning, and Transfers Body Mechanics Body mechanics means using the body in an efficient and careful way. It involves: Good posture Balance Using
PURPOSE: POLICY: FACTS:
 Revised Date: 03/13/2018 Page 1 of 14 PURPOSE: It is responsibility of each individual employed at the Black Hills Surgical Hospital to promote employee health and safety. In order to maintain and promote
Revised Date: 03/13/2018 Page 1 of 14 PURPOSE: It is responsibility of each individual employed at the Black Hills Surgical Hospital to promote employee health and safety. In order to maintain and promote
Chapter 17 Part 2. Comfort & Safety. Information you will need
 Chapter 17 Part 2 Body Mechanics Comfort & Safety Protect the person s skin from friction and shearing when moving and lifting (these can cause infection and pressure ulcers. Reduce friction and shearing
Chapter 17 Part 2 Body Mechanics Comfort & Safety Protect the person s skin from friction and shearing when moving and lifting (these can cause infection and pressure ulcers. Reduce friction and shearing
Safe Handling and Mobility. Program Development Guide
 Safe Handling and Mobility Program Development Guide 2 Safe Handling and Mobility Program Development Guide Table of Contents 4 Overview 5 Leadership Commitment and Responsibility 6 Accountability 7 Safe
Safe Handling and Mobility Program Development Guide 2 Safe Handling and Mobility Program Development Guide Table of Contents 4 Overview 5 Leadership Commitment and Responsibility 6 Accountability 7 Safe
SPECIAL HANDLING AND MOVEMENT CHALLENGES RELATED TO BARIATRICS
 SPECIAL HANDLING AND MOVEMENT CHALLENGES RELATED TO BARIATRICS Objectives: 1) To understand what technological solutions are commercially available in the use of patient handling for bariatric patients
SPECIAL HANDLING AND MOVEMENT CHALLENGES RELATED TO BARIATRICS Objectives: 1) To understand what technological solutions are commercially available in the use of patient handling for bariatric patients
Facility and Equipment Assessments and Hands-on Equipment Training
 SPH Training Series Session 2 Facility and Equipment Assessments and Hands-on Equipment Training Western New York Council on Occupational Safety & Health (WNYCOSH) This material was produced under grant
SPH Training Series Session 2 Facility and Equipment Assessments and Hands-on Equipment Training Western New York Council on Occupational Safety & Health (WNYCOSH) This material was produced under grant
Mechanical Ceiling/Floor Transfer (Hoyer)
 Mechanical Ceiling/Floor Transfer (Hoyer) o With 2 or more people determine who is going to be the leader and who is going to assist. o Explain the process to the patient and what is required for them
Mechanical Ceiling/Floor Transfer (Hoyer) o With 2 or more people determine who is going to be the leader and who is going to assist. o Explain the process to the patient and what is required for them
Safe Patient Handling:
 Safe Patient Handling: The Hazards of Immobility Prepared by : Learning Objectives Discuss the opportunity for quality improvement using SPHM practices Discuss expected positive patient outcomes using
Safe Patient Handling: The Hazards of Immobility Prepared by : Learning Objectives Discuss the opportunity for quality improvement using SPHM practices Discuss expected positive patient outcomes using
User Guide (0108) Barton Ceiling Track Lift
 User Guide (0108) Barton Ceiling Track Lift 1 Lift Features 1. Lift capabilities and design features; 2. Lift operation; Ceiling Track Lifts are designed to withstand the rigors of daily institutional
User Guide (0108) Barton Ceiling Track Lift 1 Lift Features 1. Lift capabilities and design features; 2. Lift operation; Ceiling Track Lifts are designed to withstand the rigors of daily institutional
*Before instructing class carefully review Transfer Sheet User Guide*
 Training Guide (0908) Barton Transfer Sheets *Before instructing class carefully review Transfer Sheet User Guide* Introductory Phase Introduction and Statement of Intent 1. Welcome attendees and introduce
Training Guide (0908) Barton Transfer Sheets *Before instructing class carefully review Transfer Sheet User Guide* Introductory Phase Introduction and Statement of Intent 1. Welcome attendees and introduce
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Lift Repositioning and Turning Accessory Operating Instructions
 The EZ Way line of Repositioning and Turning Accessories was designed to aid caregivers in effectively turning patients, repositioning patients, elevating patients over a bed to change bed linen, and weighing
The EZ Way line of Repositioning and Turning Accessories was designed to aid caregivers in effectively turning patients, repositioning patients, elevating patients over a bed to change bed linen, and weighing
Guidelines. Homes. Ergonomics. Musculoskeletal Disorders. for Nursing. for the Prevention of
 Guidelines for Nursing Homes Ergonomics for the Prevention of Musculoskeletal Disorders Table of Contents Executive Summary 2 Section I. Introduction 4 Section II. A Process for Protecting Workers 6 Provide
Guidelines for Nursing Homes Ergonomics for the Prevention of Musculoskeletal Disorders Table of Contents Executive Summary 2 Section I. Introduction 4 Section II. A Process for Protecting Workers 6 Provide
Park Nicollet Health Services
 file://c:\documents and Settings\cruzal\Desktop\Safe Patient Handling\Content_1\01MainMenu_1\01MainMenu_1.html Introduction Main menu 1 of 23 1 / 1 Welcome to the Applying Principles of Safe Patient Handling
file://c:\documents and Settings\cruzal\Desktop\Safe Patient Handling\Content_1\01MainMenu_1\01MainMenu_1.html Introduction Main menu 1 of 23 1 / 1 Welcome to the Applying Principles of Safe Patient Handling
Development of SPH and ISO implemented in the United States
 Development of SPH and ISO implemented in the United States REFERENCES: ISO/TR 12296 Ergonomics: Manual Handling of People in the Healthcare Sector [Reference #: ISO/TR 12296:2012(E)] An edited summary
Development of SPH and ISO implemented in the United States REFERENCES: ISO/TR 12296 Ergonomics: Manual Handling of People in the Healthcare Sector [Reference #: ISO/TR 12296:2012(E)] An edited summary
A safe patient handling continuing education course for allied health professionals
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A safe patient handling continuing education course for allied health professionals Lindsay M. Bartnik
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A safe patient handling continuing education course for allied health professionals Lindsay M. Bartnik
HSC 360b Move and position the individual
 CASE STUDY: Planning a move Shireen is the care worker for Mrs Gold, who is 80. Shireen needs to move Mrs Gold from a bed into a chair. Mrs Gold is only able to assist a little as she has very painful
CASE STUDY: Planning a move Shireen is the care worker for Mrs Gold, who is 80. Shireen needs to move Mrs Gold from a bed into a chair. Mrs Gold is only able to assist a little as she has very painful
The Role of the Emergency Medical Technician Lifting and Moving Patients Safely
 CHAPTER 6 The Role of the Emergency Medical Technician Lifting and Moving Patients Safely Lifts, Drags, Takedowns, and Carries Transporting Patients Safely Transportation Equipment This chapter focuses
CHAPTER 6 The Role of the Emergency Medical Technician Lifting and Moving Patients Safely Lifts, Drags, Takedowns, and Carries Transporting Patients Safely Transportation Equipment This chapter focuses
Handling the Bariatric Patient: Ergonomic Issues HoverTech International All Rights Reserved
 Handling the Bariatric Patient: Ergonomic Issues 2014 Plan Where are you going? 2014 2011 HoverTech International All Rights Reserved Ergonomics Defining Ergonomics Ergonomics is NOT: Buzzword, passing
Handling the Bariatric Patient: Ergonomic Issues 2014 Plan Where are you going? 2014 2011 HoverTech International All Rights Reserved Ergonomics Defining Ergonomics Ergonomics is NOT: Buzzword, passing
Safe handling of bariatric patients and residents September 2015
 RiskTopics Safe handling of bariatric patients and residents September 2015 Introduction As the world population average body weight continues to rise, due primarily to lifestyle choices and high caloric/fat
RiskTopics Safe handling of bariatric patients and residents September 2015 Introduction As the world population average body weight continues to rise, due primarily to lifestyle choices and high caloric/fat
Solutions to Challenges Associated with Bariatric Patients
 Solutions to Challenges Associated with Bariatric Patients Manon Labreche, PT, CEAS 2, CHC Injury Prevention Manager Tampa General Hospital mlabreche@tgh.org Lynda Enos, RN, MS, COHN-S, CPE Ergonomics
Solutions to Challenges Associated with Bariatric Patients Manon Labreche, PT, CEAS 2, CHC Injury Prevention Manager Tampa General Hospital mlabreche@tgh.org Lynda Enos, RN, MS, COHN-S, CPE Ergonomics
2010 Innovative Uses and Tips for Safe Patient Moving Equipment: Safe Patient Moving: the Keys to the Kingdom: Learning Objectives
 2010 Innovative Uses and Tips for Safe Patient Moving Equipment: Better Care, Less Wear Safe Patient Moving: the Keys to the Kingdom: Learning Objectives A. Describe what Consistency Communication Collaboration
2010 Innovative Uses and Tips for Safe Patient Moving Equipment: Better Care, Less Wear Safe Patient Moving: the Keys to the Kingdom: Learning Objectives A. Describe what Consistency Communication Collaboration
Safe Patient Movement and Mobility Improving Outcomes for Patients and Employees. Objectives. Your Presenter. Vision
 Presented by: Janice Homola, ARM Senior Consultant Loss Prevention Services Workers Compensation Services Safe Patient Movement and Mobility Improving Outcomes for Patients and Employees Your Presenter
Presented by: Janice Homola, ARM Senior Consultant Loss Prevention Services Workers Compensation Services Safe Patient Movement and Mobility Improving Outcomes for Patients and Employees Your Presenter
Quality Care is. Partners in. In-Home Aides. Assisting with ambulation and using assistive devices: - March
 In-Home Aides Partners in Quality Care - March 2015 - In-Home Aides Partners in Quality Care is a monthly newsletter published for AHHC of NC and SCHCA member agencies. Copyright AHHC 2015 - May be reproduced
In-Home Aides Partners in Quality Care - March 2015 - In-Home Aides Partners in Quality Care is a monthly newsletter published for AHHC of NC and SCHCA member agencies. Copyright AHHC 2015 - May be reproduced
This report summarizes the ergonomic risk assessment conducted at a Hospital August 2001.
 Naval Facilities Engineering Command Ergonomic Risk Assessment for Naval Hospital, Labor & Delivery - Patient Transport INTRODUCTION This report summarizes the ergonomic risk assessment conducted at a
Naval Facilities Engineering Command Ergonomic Risk Assessment for Naval Hospital, Labor & Delivery - Patient Transport INTRODUCTION This report summarizes the ergonomic risk assessment conducted at a
Patient Transfer Technologies In the Home
 Patient Transfer Technologies In the Home Lori Peculis, PT, ATP Molly Boland, MS, ATP, RET Assistive Technology Unit University of Illinois at Chicago S Transfer Assistance in the Home: Who? Where? Why?
Patient Transfer Technologies In the Home Lori Peculis, PT, ATP Molly Boland, MS, ATP, RET Assistive Technology Unit University of Illinois at Chicago S Transfer Assistance in the Home: Who? Where? Why?
Module 6: Client Moving Techniques * Terms marked by an asterisk are defined in the Glossary
 Module 6: Client Moving Techniques * Terms marked by an asterisk are defined in the Glossary 6.1 Introduction Module 1 introduced the moving task as a consistent set of steps used to move a client. At
Module 6: Client Moving Techniques * Terms marked by an asterisk are defined in the Glossary 6.1 Introduction Module 1 introduced the moving task as a consistent set of steps used to move a client. At
Listed below are additional coding tips: you think the patient can do or what the patient s potential is. your shift, even if it only occurs once.
 1 It is important to always accurately code how much assistance your patients require to perform their activities of daily living and provide assistance in the safest manner possible for you and the patient.
1 It is important to always accurately code how much assistance your patients require to perform their activities of daily living and provide assistance in the safest manner possible for you and the patient.
Opera. With people in mind
 Opera With people in mind Opera... ARJO a prime mover in the handling revolution ARJO patient handling and moving equipment is firmly established as the most acceptable for today's ergonomics-conscious
Opera With people in mind Opera... ARJO a prime mover in the handling revolution ARJO patient handling and moving equipment is firmly established as the most acceptable for today's ergonomics-conscious
NHS Training for Physiotherapy Support Workers. Workbook 15 Transfers
 NHS Training for Physiotherapy Support Workers Workbook 15 Transfers Contents Workbook 15 Transfers 1 15.1 Aim 3 15.2 Learning outcomes 3 15.3 Lying sitting transfer 4 15.4 Teaching a patient to move up
NHS Training for Physiotherapy Support Workers Workbook 15 Transfers Contents Workbook 15 Transfers 1 15.1 Aim 3 15.2 Learning outcomes 3 15.3 Lying sitting transfer 4 15.4 Teaching a patient to move up
How to Safely Transport a Client
 How to Safely Transport a Client INTRODUCTION Medical problems and/or physical limitations can and often do restrict a client s ability to ambulate and move, and transporting clients is a primary responsibility
How to Safely Transport a Client INTRODUCTION Medical problems and/or physical limitations can and often do restrict a client s ability to ambulate and move, and transporting clients is a primary responsibility
Safe moving and handling guidance
 Safe moving and handling guidance An overview of moving and handling in the care industry, from legislation to practical tips, written by Frances Leckie, editor of the Independent Living website Contents:
Safe moving and handling guidance An overview of moving and handling in the care industry, from legislation to practical tips, written by Frances Leckie, editor of the Independent Living website Contents:
Activity 3: TRANSFER TO A WHEELCHAIR Future tense
 Contextualized Grammar I-BEST SUN Path Curriculum Unit for Nursing Assistant with ESL Support - Page 1 of 10 Activity 3: TRANSFER TO A WHEELCHAIR Future tense Learning Goal(s) Demonstrate the indirect
Contextualized Grammar I-BEST SUN Path Curriculum Unit for Nursing Assistant with ESL Support - Page 1 of 10 Activity 3: TRANSFER TO A WHEELCHAIR Future tense Learning Goal(s) Demonstrate the indirect
Ergonomics Issues In Paramedic Duties: A Case Study. Steve Morrissey Ergonomics Consultant Oregon OSHA Consultation
 Ergonomics Issues In Paramedic Duties: A Case Study Steve Morrissey Ergonomics Consultant Oregon OSHA Consultation Introduction Non-binding ergonomic consultation with a large ambulance service in the
Ergonomics Issues In Paramedic Duties: A Case Study Steve Morrissey Ergonomics Consultant Oregon OSHA Consultation Introduction Non-binding ergonomic consultation with a large ambulance service in the
All Departments / Units. System Safe Patient Mobilization Committee
 [X] & PROCEDURE PAGE 1 OF 6 REFERENCE [ ] All Sharp HealthCare AFFECTED DEPARTMENTS: 6 ACCREDITATION: [ ] System Services Outpatient Surgery: [ ] SRS [ ] CV-OPS [ ] SCMG [ ] GPSC [ ] SHP [ ] SMH-OPP Hospitals
[X] & PROCEDURE PAGE 1 OF 6 REFERENCE [ ] All Sharp HealthCare AFFECTED DEPARTMENTS: 6 ACCREDITATION: [ ] System Services Outpatient Surgery: [ ] SRS [ ] CV-OPS [ ] SCMG [ ] GPSC [ ] SHP [ ] SMH-OPP Hospitals
Resuscitation Council (UK) Guidance for safer handling during resuscitation in healthcare settings. Working Group of the Resuscitation Council (UK)
 Guidance for safer handling during resuscitation in healthcare settings Working Group of the Resuscitation Council (UK) November 2009 Guidance for safer handling during resuscitation in healthcare settings
Guidance for safer handling during resuscitation in healthcare settings Working Group of the Resuscitation Council (UK) November 2009 Guidance for safer handling during resuscitation in healthcare settings
Taking Care Of Your Back Manual Handling. Clinical Skills
 Clinical Skills Taking Care of Your Manual Handling Course devised by the Clinical Skills Team Training delivered by Cardiff & Vale UHB (Health, Safety & Environment Unit) Aims & Outcomes Aims & Outcomes
Clinical Skills Taking Care of Your Manual Handling Course devised by the Clinical Skills Team Training delivered by Cardiff & Vale UHB (Health, Safety & Environment Unit) Aims & Outcomes Aims & Outcomes
! "#"!$%&'()*%!+!,-)$(!.%/0%&1! $2345!67!869:59:;!!!! )/%1A""#$%&'()$"%&*"+,(-".'')''/)&-"0)12)'-" 3"
 ! ! "#"!$%&'()*%!+!,-)$(!.%/0%&1! $2345!67!869:59:;!!!! $5
! ! "#"!$%&'()*%!+!,-)$(!.%/0%&1! $2345!67!869:59:;!!!! $5
The Ergonomics of Patient Handling
 The Ergonomics of Patient Handling March 22, 2005 1 Major Healthcare Trends Pressure to Control Costs Emphasis on Reducing Length of Stay Attention to Patient Safety Focus on Nursing Staff Retention/Recruitment
The Ergonomics of Patient Handling March 22, 2005 1 Major Healthcare Trends Pressure to Control Costs Emphasis on Reducing Length of Stay Attention to Patient Safety Focus on Nursing Staff Retention/Recruitment
CNA Training Advisor
 CNA Training Advisor Volume 12 Issue No. 6 JUNE 2014 REDUCING THE RISK OF WORK-RELATED INJURIES Without taking the necessary precautions and adhering to the proper body mechanics, CNAs could be harmed
CNA Training Advisor Volume 12 Issue No. 6 JUNE 2014 REDUCING THE RISK OF WORK-RELATED INJURIES Without taking the necessary precautions and adhering to the proper body mechanics, CNAs could be harmed
Soteria Strains Safe Patient Handling and Mobility Program Guide
 Soteria Strains Safe Patient Handling and Mobility Program Guide Section 2 Identifying Hazards and Assessing Risk V1.0 edited August 21, 2015 A provincial strategy for healthcare workplace musculoskeletal
Soteria Strains Safe Patient Handling and Mobility Program Guide Section 2 Identifying Hazards and Assessing Risk V1.0 edited August 21, 2015 A provincial strategy for healthcare workplace musculoskeletal
2016 School District of Pittsburgh
 2016 School District of Pittsburgh Health Careers Skill Name: Accurately Measures, Records and Reports Client s Oral Temperature ROADMAP: 20 min (vitals, height and weight) EQUIPMENT NEEDED: facility/materials
2016 School District of Pittsburgh Health Careers Skill Name: Accurately Measures, Records and Reports Client s Oral Temperature ROADMAP: 20 min (vitals, height and weight) EQUIPMENT NEEDED: facility/materials
Introduction. Welcome to Human Care.
 Convertible Chairs Introduction We produce and provide lifting solutions for people with special needs. Our products are made to serve as a natural part of life to all our users. Human Care has a proud
Convertible Chairs Introduction We produce and provide lifting solutions for people with special needs. Our products are made to serve as a natural part of life to all our users. Human Care has a proud
Supporting people to move at home. Guide for managers (2015)
 Supporting people to move at home Guide for managers (2015) Supporting people to move at home, Guide for managers (2015) 1. Introduction Acknowledgements 2. Unique features of moving and transferring in
Supporting people to move at home Guide for managers (2015) Supporting people to move at home, Guide for managers (2015) 1. Introduction Acknowledgements 2. Unique features of moving and transferring in
Step by step instructions for each team member when lifting or repositioning patients with suspected or known spinal injury.
 PURPOSE Step by step instructions for each team member when lifting or repositioning patients with suspected or known spinal injury. POLICY STATEMENTS Repositioning or lifting a patient with a suspected
PURPOSE Step by step instructions for each team member when lifting or repositioning patients with suspected or known spinal injury. POLICY STATEMENTS Repositioning or lifting a patient with a suspected
Introduction. Welcome to Human Care.
 Convertible Chairs Introduction We produce and provide lifting solutions for people with special needs. Our products are made to serve as a natural part of life to all our users. Human Care has a proud
Convertible Chairs Introduction We produce and provide lifting solutions for people with special needs. Our products are made to serve as a natural part of life to all our users. Human Care has a proud
Using Body Mechanics
 Promotion of Safety Using Body Mechanics Muscles work best when used correctly Correct use of muscles makes lifting, pulling, and pushing easier Prevents unnecessary fatigue and strain and saves energy
Promotion of Safety Using Body Mechanics Muscles work best when used correctly Correct use of muscles makes lifting, pulling, and pushing easier Prevents unnecessary fatigue and strain and saves energy
CARENDO ERGONOMIC HYGIENE CHAIR WITH UNIQUE CARE RAISER
 CARENDO ERGONOMIC HYGIENE CHAIR WITH UNIQUE CARE RAISER Carendo 3 THE TRUE PROBLEM SOLVER Showering is becoming more common within long term care, but existing methods are uncomfortable for the resident
CARENDO ERGONOMIC HYGIENE CHAIR WITH UNIQUE CARE RAISER Carendo 3 THE TRUE PROBLEM SOLVER Showering is becoming more common within long term care, but existing methods are uncomfortable for the resident
SPINAL PRECAUTIONS: LOG-ROLLING TECHNIQUE PURPOSE POLICY STATEMENTS PRACTICE LEVEL/COMPETENCIES DEFINITIONS
 PURPOSE Step by step instructions for each team member when performing the log-rolling technique to reposition patients with suspected or actual spinal injury. POLICY STATEMENTS Moving a patient with a
PURPOSE Step by step instructions for each team member when performing the log-rolling technique to reposition patients with suspected or actual spinal injury. POLICY STATEMENTS Moving a patient with a
showering solutions Create a safe, efficient and dignified care environment
 showering solutions Create a safe, efficient and dignified care environment with people in mind Real needs and everyday reality Every day, bed-baths compromise the dignity and safety of patients and caregivers,
showering solutions Create a safe, efficient and dignified care environment with people in mind Real needs and everyday reality Every day, bed-baths compromise the dignity and safety of patients and caregivers,
Leicestershire Partnership NHS Trust. Moving and Handling Level 2 Update 2018/19
 Leicestershire Partnership NHS Trust Moving and Handling Level 2 Update 2018/19 Introduction Welcome to your Moving and Handling Level 2 Update for 2018/2019. This session forms part of an on-going programme
Leicestershire Partnership NHS Trust Moving and Handling Level 2 Update 2018/19 Introduction Welcome to your Moving and Handling Level 2 Update for 2018/2019. This session forms part of an on-going programme
Chapter 11. Preventing Falls. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 11 Preventing Falls Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 11.1 Define the key terms and key abbreviations in this chapter. Identify the causes and risk factors for falls.
Chapter 11 Preventing Falls Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 11.1 Define the key terms and key abbreviations in this chapter. Identify the causes and risk factors for falls.
Safe Patient Handling & Early Mobility
 Safe Patient Handling & Early Mobility This workshop is awarded two (2) contact hours through the New York State Nurses Association Accredited Provider Unit. The New York State Nurses Association is accredited
Safe Patient Handling & Early Mobility This workshop is awarded two (2) contact hours through the New York State Nurses Association Accredited Provider Unit. The New York State Nurses Association is accredited
A PRACTICAL GUIDE TO RESIDENT HANDLING
 A PRACTICAL GUIDE TO RESIDENT HANDLING October 2004 Preface Interior Health is a large healthcare organization in British Columbia providing a full range of services to the population within a specified
A PRACTICAL GUIDE TO RESIDENT HANDLING October 2004 Preface Interior Health is a large healthcare organization in British Columbia providing a full range of services to the population within a specified
Ergonomic (MSI) Risk Factor Identification and Assessment Ergonomics Risk Assessment Project. Task List Worksheet
 Ergonomic (MSI) Risk Factor Identification and Assessment Department/Work Area: Maternity Specific Location: Occupation: RN Contact Name: Task List Worksheet Job Summary: Provides nursing care to patients
Ergonomic (MSI) Risk Factor Identification and Assessment Department/Work Area: Maternity Specific Location: Occupation: RN Contact Name: Task List Worksheet Job Summary: Provides nursing care to patients
Home Care Aide Skills Checklist
 Home Care Aide Skills Checklist The following checklists contain the criteria used by the rater to evaluate each candidate s performance for each of the skills included in the Skills Exam. Each checklist
Home Care Aide Skills Checklist The following checklists contain the criteria used by the rater to evaluate each candidate s performance for each of the skills included in the Skills Exam. Each checklist
Wound Care Program for Nursing Assistants- Prevention 101
 Wound Care Program for Nursing Assistants- Prevention 101 Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion of this webinar,
Wound Care Program for Nursing Assistants- Prevention 101 Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion of this webinar,
CARMINA BARIAtRIC shower CoMMode ChAIR
 CARMINA BARIAtRIC shower CoMMode ChAIR with people in mind 2 Carmina A SAfe Showering Solution for bariatric care Carmina is a new solution designed to improve assisted hygiene routines in bariatric environments.
CARMINA BARIAtRIC shower CoMMode ChAIR with people in mind 2 Carmina A SAfe Showering Solution for bariatric care Carmina is a new solution designed to improve assisted hygiene routines in bariatric environments.
ConCerto Shower trolley
 Concerto Shower Trolley Concerto 3 Assisted showering with extra care More and more healthcare facilities are turning to showering for residents personal hygiene routines. Concerto offers a safe, wellproven
Concerto Shower Trolley Concerto 3 Assisted showering with extra care More and more healthcare facilities are turning to showering for residents personal hygiene routines. Concerto offers a safe, wellproven
Safe patient handling for occupational therapy students and practitioners: a course development plan
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Safe patient handling for occupational therapy students and practitioners: a course development plan
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Safe patient handling for occupational therapy students and practitioners: a course development plan
Affinity Four Birthing bed Delivering Safety
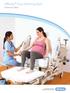 Affinity Four Birthing bed Delivering Safety The perfect combination of safety and ease-of-use In labour and delivery, every second counts. Caregivers must be able to respond quickly and easily, especially
Affinity Four Birthing bed Delivering Safety The perfect combination of safety and ease-of-use In labour and delivery, every second counts. Caregivers must be able to respond quickly and easily, especially
PERSONAL CARE WORKER (PCW) - Job Description
 PERSONAL CARE WORKER (PCW) - Job Description Definition Provides unskilled personal care and household services for stable, maintenance clients in their homes in compliance with a service plan. Level of
PERSONAL CARE WORKER (PCW) - Job Description Definition Provides unskilled personal care and household services for stable, maintenance clients in their homes in compliance with a service plan. Level of
THE INTERVENTIONAL PATIENT HYGIENE COMPANY
 THE INTERVENTIONAL PATIENT HYGIENE COMPANY Born from a core belief in prevention, Interventional Patient Hygiene is a nursing action plan focused on fortifying patients host defenses with evidence-based
THE INTERVENTIONAL PATIENT HYGIENE COMPANY Born from a core belief in prevention, Interventional Patient Hygiene is a nursing action plan focused on fortifying patients host defenses with evidence-based
Ergonomic (MSI) Risk Factor Identification and Assessment. Task List Worksheet
 Department/Work Area: Extended Care Specific Location: Assessed By: Occupation: Care Aide Contact Name: Assessment Date: Task List Worksheet Job Summary: Performs nursing procedures such as taking temperature,
Department/Work Area: Extended Care Specific Location: Assessed By: Occupation: Care Aide Contact Name: Assessment Date: Task List Worksheet Job Summary: Performs nursing procedures such as taking temperature,
Always at Hand for Smooth Transfers
 H A N DY L O W - F R I C T I O N P R O D U C T S Always at Hand for Smooth Transfers Simple aids which are always at hand. This is how one could summarize Liko s new product series Handy. The series consists
H A N DY L O W - F R I C T I O N P R O D U C T S Always at Hand for Smooth Transfers Simple aids which are always at hand. This is how one could summarize Liko s new product series Handy. The series consists
Guidelines for the Prevention of Pressure Ulcers
 Guidelines for the Prevention of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009 1. Introduction Most pressure ulcers are avoidable. Avoidable means that the person receiving care developed a pressure
Guidelines for the Prevention of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009 1. Introduction Most pressure ulcers are avoidable. Avoidable means that the person receiving care developed a pressure
Bariatric. Care Solutions
 Bariatric Care Solutions The Obesity Challenge Obesity is now recognised as a global epidemic. Obesity rates in the UK and Eire are among the highest in Europe and have increased dramatically over the
Bariatric Care Solutions The Obesity Challenge Obesity is now recognised as a global epidemic. Obesity rates in the UK and Eire are among the highest in Europe and have increased dramatically over the
An Update on Safe Patient Handling and Ergonomics
 An Update on Safe Patient Handling and Ergonomics Contact Hours: 1 First Published: April 15, 2014 Course Revised: April 1, 2017 Course Expires: July 30, 2020 Copyright 2017 by RN.com All Rights Reserved.
An Update on Safe Patient Handling and Ergonomics Contact Hours: 1 First Published: April 15, 2014 Course Revised: April 1, 2017 Course Expires: July 30, 2020 Copyright 2017 by RN.com All Rights Reserved.
Adaptation, Equipment and Safety Equipment Assessment. REVISED July 2016
 Adaptation, Equipment and Safety Equipment Assessment REVISED July 2016 Page 1 of 5 Adaptations and Equipment Policy Statement The Wellbeing Residential Group believes that its service users should expect
Adaptation, Equipment and Safety Equipment Assessment REVISED July 2016 Page 1 of 5 Adaptations and Equipment Policy Statement The Wellbeing Residential Group believes that its service users should expect
Redefining Patient Handling. prevention
 Redefining Patient Handling prevention Joerns Healthcare, manufacturer of Hoyer products, is committed to providing a complete line of top quality equipment to the healthcare industry. The name Hoyer is
Redefining Patient Handling prevention Joerns Healthcare, manufacturer of Hoyer products, is committed to providing a complete line of top quality equipment to the healthcare industry. The name Hoyer is
OR Positioning and Pressure Injury Prevention. September 13, Ann N. Tescher, APRN CNS, PhD, CCRN, CWCN Debra L.
 OR Positioning and Pressure Injury Prevention September 13, 2017 Ann N. Tescher, APRN CNS, PhD, CCRN, CWCN Debra L. Fawcett, PhD, RN 2017 National Pressure Ulcer Advisory Panel www.npuap.org NPUAP Mission
OR Positioning and Pressure Injury Prevention September 13, 2017 Ann N. Tescher, APRN CNS, PhD, CCRN, CWCN Debra L. Fawcett, PhD, RN 2017 National Pressure Ulcer Advisory Panel www.npuap.org NPUAP Mission
CARINO. with people in mind
 CARINO Height adjustable hygiene chair with people in mind A BETTER ALTERNATIVE FOR DAILY HYGIENE For many residents and patients assisted hygiene routines consist of being showered on a fixed-height shower
CARINO Height adjustable hygiene chair with people in mind A BETTER ALTERNATIVE FOR DAILY HYGIENE For many residents and patients assisted hygiene routines consist of being showered on a fixed-height shower
R E C L I N E R S E A T I N G
 RECLINER EATING upporting Connections. At Nurture, we believe every interaction between the patient and caregiver matters. To help support these vital connections, we observe what can be better within
RECLINER EATING upporting Connections. At Nurture, we believe every interaction between the patient and caregiver matters. To help support these vital connections, we observe what can be better within
Safe Patient Handling Team Meeting
 Safe Patient Handling Team Meeting Date: Friday, March 30, 2012 Location: Conference Center A Time: 11a-12p MINUTES See last page for Attendance TOPIC DISCUSSION ACTIONS/RECOMMENDATIONS Attendance Progress
Safe Patient Handling Team Meeting Date: Friday, March 30, 2012 Location: Conference Center A Time: 11a-12p MINUTES See last page for Attendance TOPIC DISCUSSION ACTIONS/RECOMMENDATIONS Attendance Progress
Workplace Safety for CNAs
 Workplace Safety for CNAs Contact Hours: 1.0 First Published: December 6, 2005 Revised: December 5, 2008 Revised: December 31, 2012 Revised: August 9, 2017 Course expires: August 31, 2020 Copyright 2017
Workplace Safety for CNAs Contact Hours: 1.0 First Published: December 6, 2005 Revised: December 5, 2008 Revised: December 31, 2012 Revised: August 9, 2017 Course expires: August 31, 2020 Copyright 2017
OUTLINE SPH NEW HIRE TRAINING
 INTRODUCTION OF SPH TEAM CURRENT INJURY GRAPHS OUTLINE SPH NEW HIRE TRAINING BACKGROUND OF SAFE PATIENT HANDLING AB1136 AREAS OF BODY EXPOSURE LIFTING POLICY REFUSAL TO PERFORM PATIENT MOBILITY TRAINING
INTRODUCTION OF SPH TEAM CURRENT INJURY GRAPHS OUTLINE SPH NEW HIRE TRAINING BACKGROUND OF SAFE PATIENT HANDLING AB1136 AREAS OF BODY EXPOSURE LIFTING POLICY REFUSAL TO PERFORM PATIENT MOBILITY TRAINING
CArEnDO ElECtrIC HyGIEnE CHAIr
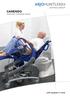 CARENDO electric hygiene chair with people in mind Working methods can put carers health at risk 80 70 60 50 40 30 20 10 Studies have confirmed that carers assisting with washing in bed or ing using a
CARENDO electric hygiene chair with people in mind Working methods can put carers health at risk 80 70 60 50 40 30 20 10 Studies have confirmed that carers assisting with washing in bed or ing using a
Lateral Transfers Boosting Turning Positioning Proning
 Lateral Transfers Boosting Turning Positioning Proning Facilitate all-day patient care with the HoverMatt Single-Patient Use Air Transfer System. Designed to be multifunctional, the HoverMatt Single-Patient
Lateral Transfers Boosting Turning Positioning Proning Facilitate all-day patient care with the HoverMatt Single-Patient Use Air Transfer System. Designed to be multifunctional, the HoverMatt Single-Patient
Spinal Cord Injury T10-L2
 Patient and Family Education Spinal Cord Injury T10-L2 A Guide for Families You are an important member of your child s recovery team. Use this checklist to monitor your child s progress. Our goal is to
Patient and Family Education Spinal Cord Injury T10-L2 A Guide for Families You are an important member of your child s recovery team. Use this checklist to monitor your child s progress. Our goal is to
UNDERSTANDING COEFFICIENT OF FRICTION AND WHY OTHER SLIDE SHEET PROPERTIES ARE ALSO IMPORTANT
 August 2016 UNDERSTANDING COEFFICIENT OF FRICTION AND WHY OTHER SLIDE SHEET PROPERTIES ARE ALSO IMPORTANT by Jamar Health Products, Inc. ABSTRACT BACKGROUND: Discussions about slide sheets, which are meant
August 2016 UNDERSTANDING COEFFICIENT OF FRICTION AND WHY OTHER SLIDE SHEET PROPERTIES ARE ALSO IMPORTANT by Jamar Health Products, Inc. ABSTRACT BACKGROUND: Discussions about slide sheets, which are meant
ICELS Nottingham City and Nottinghamshire County. Policy for the Loan of Equipment into Registered Care Homes for Adults and Older People
 ICELS Nottingham City and Nottinghamshire County Policy for the Loan of Equipment into Registered s for Adults and Older People March 2014 Integrated Community Equipment Loan Service ICELS Policy for the
ICELS Nottingham City and Nottinghamshire County Policy for the Loan of Equipment into Registered s for Adults and Older People March 2014 Integrated Community Equipment Loan Service ICELS Policy for the
MOVE ON: Mobilization Of Vulnerable Elders In Ontario: How to assess and keep our patients moving?
 MOVE ON: Mobilization Of Vulnerable Elders In Ontario: How to assess and keep our patients moving? Objectives Think up and After participating in this educational session, inter professional team members
MOVE ON: Mobilization Of Vulnerable Elders In Ontario: How to assess and keep our patients moving? Objectives Think up and After participating in this educational session, inter professional team members
Occupational Safety for the Nursing Profession
 Occupational Safety for the Nursing Profession Presentation by Risk Management Division Centers for Long Term Care, Inc. Steve Spainhouer, OSHT, ASSE The US Department of Labor states that working in a
Occupational Safety for the Nursing Profession Presentation by Risk Management Division Centers for Long Term Care, Inc. Steve Spainhouer, OSHT, ASSE The US Department of Labor states that working in a
Pressure Ulcer Prevention
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet has been adapted from
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet has been adapted from
Safe Patient Handling and Movement Program May 2008
 Safe Patient Handling and Movement Program May 2008 Winnipeg Regional Health Authority 05-2008 Acknowledgements The information contained in this manual is the result of a collaborative effort between
Safe Patient Handling and Movement Program May 2008 Winnipeg Regional Health Authority 05-2008 Acknowledgements The information contained in this manual is the result of a collaborative effort between
To provide the appropriate way of carrying and/or moving of a patient ensuring the patient's safety
 SUBJECT: PATIENT CARRYING METHODS PURPOSE: To provide the appropriate way of carrying and/or moving of a patient ensuring the patient's safety PROCEDURE: 1. Universal Carry - The Universal Carry is a method
SUBJECT: PATIENT CARRYING METHODS PURPOSE: To provide the appropriate way of carrying and/or moving of a patient ensuring the patient's safety PROCEDURE: 1. Universal Carry - The Universal Carry is a method
Equipment Loan Program
 1 Equipment Loan Program Resource Handbook ALS in the Heartland s Equipment Loan Program The following handbook was developed to provide information about the ALS in the Heartland Equipment Loan Program.
1 Equipment Loan Program Resource Handbook ALS in the Heartland s Equipment Loan Program The following handbook was developed to provide information about the ALS in the Heartland Equipment Loan Program.
Functional Abilities / Core Performance Standards
 Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
CNA Training Advisor
 CNA Training Advisor Volume 13 Issue No. 11 NOVEMBER 2015 Many of us take free, comfortable movement for granted. As people get older, however, muscles gradually lose their strength, endurance, and flexibility.
CNA Training Advisor Volume 13 Issue No. 11 NOVEMBER 2015 Many of us take free, comfortable movement for granted. As people get older, however, muscles gradually lose their strength, endurance, and flexibility.
Manual Handling Policy
 Document Profile Box Document Reference: Version: 0001 Ratified by: Health and Safety Committee Date ratified: Aug 2008 Name of originator/author: Alan Gallagher Name of responsible committee/individual:
Document Profile Box Document Reference: Version: 0001 Ratified by: Health and Safety Committee Date ratified: Aug 2008 Name of originator/author: Alan Gallagher Name of responsible committee/individual:
9/17/2015. Bed Rail Safety A Clinical Process Guideline. Background. Federal Nursing Home Reform Act
 Bed Rail Safety A Clinical Process Guideline Laura Funsch, RN, BSN, MS, Director of Regulatory Strategy Background Safety hazards related to bed rail use have been realized since 1990. Michigan s initial
Bed Rail Safety A Clinical Process Guideline Laura Funsch, RN, BSN, MS, Director of Regulatory Strategy Background Safety hazards related to bed rail use have been realized since 1990. Michigan s initial
Bed Rail Safety A Clinical Process Guideline. Laura Funsch, RN, BSN, MS, Director of Regulatory Strategy
 Bed Rail Safety A Clinical Process Guideline Laura Funsch, RN, BSN, MS, Director of Regulatory Strategy Background Safety hazards related to bed rail use have been realized since 1990. Michigan s initial
Bed Rail Safety A Clinical Process Guideline Laura Funsch, RN, BSN, MS, Director of Regulatory Strategy Background Safety hazards related to bed rail use have been realized since 1990. Michigan s initial
So You re Having a Total Hip Replacement?
 So You re Having a Total Hip Replacement? Your team of nurses, surgeons, therapists and social workers are here to help you every step of the way. This presentation is meant to assist you before, during
So You re Having a Total Hip Replacement? Your team of nurses, surgeons, therapists and social workers are here to help you every step of the way. This presentation is meant to assist you before, during
BED RAIL SAFETY 9/15/2015. A Clinical Process Guideline. Background. Federal Nursing Home Reform Act
 BED RAIL SAFETY A Clinical Process Guideline Laura Funsch, RN, BSN, MS Director of Regulatory Strategy, LeadingAge Michigan Background Safety hazards related to bed rail use have been realized since 1990.
BED RAIL SAFETY A Clinical Process Guideline Laura Funsch, RN, BSN, MS Director of Regulatory Strategy, LeadingAge Michigan Background Safety hazards related to bed rail use have been realized since 1990.
Eleganza 3XC. Designed for ICU
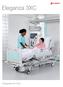 Eleganza 3XC Designed for ICU Benefits of Eleganza 3XC 2 LINET Eleganza 3XC Everything needed to save lives Prevention of pulmonary and cardiac complications Falls protection and pressure ulcer prevention
Eleganza 3XC Designed for ICU Benefits of Eleganza 3XC 2 LINET Eleganza 3XC Everything needed to save lives Prevention of pulmonary and cardiac complications Falls protection and pressure ulcer prevention
SAFE PATIENT HANDLING ACT
 SAFE PATIENT HANDLING ACT WHAT S HAPPENING IN ILLINOIS May 12, 2011 Aida Trinidad Illinois Department of Public Health Division of Health Care Facilities and Programs TITLE 77 IL ADM. CODE 250 HOSPITAL
SAFE PATIENT HANDLING ACT WHAT S HAPPENING IN ILLINOIS May 12, 2011 Aida Trinidad Illinois Department of Public Health Division of Health Care Facilities and Programs TITLE 77 IL ADM. CODE 250 HOSPITAL
PUSH for FACT # 1. Quality Patient Care! What are the Facts about Safe Patient Handling and Movement?
 # 1 : PATIENTS AND THEIR CAREGIVERS ARE INJURED BY MANUAL LIFTING TASKS Safe Patient Handling and Movement: A policy and practice that creates a safe environment for patients and healthcare workers by
# 1 : PATIENTS AND THEIR CAREGIVERS ARE INJURED BY MANUAL LIFTING TASKS Safe Patient Handling and Movement: A policy and practice that creates a safe environment for patients and healthcare workers by
Patient (Animate) Manual Handling Information Theory Booklet For Patient Handling Staff
 Patient (Animate) Manual Handling Information Theory Booklet For Patient Handling Staff Reviewed by: Carol Walpole Specialist Moving and Handling Advisor CONTENTS BARIATRIC HANDLING...3 ASSESSING PATIENT
Patient (Animate) Manual Handling Information Theory Booklet For Patient Handling Staff Reviewed by: Carol Walpole Specialist Moving and Handling Advisor CONTENTS BARIATRIC HANDLING...3 ASSESSING PATIENT
Admission, Transfer, Discharge, and Physical Exams
 62 9 Admission, Transfer, Discharge, and Physical Exams 1. Define important words in this chapter 2. List factors for families in choosing a facility 3. Explain the nursing assistant s role in the emotional
62 9 Admission, Transfer, Discharge, and Physical Exams 1. Define important words in this chapter 2. List factors for families in choosing a facility 3. Explain the nursing assistant s role in the emotional
Manual handling guidance Plus size patient
 Manual handling guidance Plus size patient Policy Title: Executive Summary: These guidelines aim to complement current guidance and provide clear advice to staff on the management of heavy patients who
Manual handling guidance Plus size patient Policy Title: Executive Summary: These guidelines aim to complement current guidance and provide clear advice to staff on the management of heavy patients who
