4. Services, Surgery, supplies, treatment, or expenses:
|
|
|
- Brianna Hall
- 5 years ago
- Views:
Transcription
1 ARTICLE XVIII. LIMITATIONS AND EXCLUSIONS A. Services, supplies and treatment for services that are not covered under this Contract and complications from services, supplies and treatment for services that are not covered under this Contract are excluded. B. Any of the limitations and exclusions listed in this Contract may be deleted or revised as shown in the Schedule of Benefits. Unless otherwise shown as covered in the Schedule of Benefits, the following are not covered, REGARDLESS OF CLAIM OF MEDICAL NECESSITY: 1. Services, treatments, procedures, equipment, drugs, devices, items or supplies that are not Medically Necessary. 2. Any charges exceeding the Allowable Charge 3. Incremental nursing charges which are in addition to the Hospital s standard charge for Bed, Board and General Nursing Service; charges for luxury accommodations or any accommodations in any Hospital or Allied Health Facility provided primarily for the patient s convenience; or Bed, Board and General Nursing Service in any other room at the same time Benefits are provided for use of a Special Care Unit. 4. Services, Surgery, supplies, treatment, or expenses: a. other than those specifically listed as covered by this Contract or for which a Member has no obligation to pay, or for which no charge or a lesser charge would be made if a Member had no health insurance coverage. Benefits are available when Covered Services are rendered at medical facilities owned and operated by the State of Louisiana or any of its political subdivisions. b. rendered or furnished before the Member s Effective Date or after Member s coverage terminates, except as follows: Medical Benefits in connection with an Admission will be provided for an Admission in progress on the date a Member s coverage under this Contract ends, until the end of that Admission or until a Member has reached any Benefit limitations set in this Contract, whichever occurs first; c. which are performed by or upon the direction of a Provider, Physician or Allied Health Professional acting outside the scope of his license d. to the extent payment has been made or is available under any other contract issued by Louisiana Health Cooperative, Inc. or to the extent provided for under any other contract, except as allowed by law, and except for limited Benefit policies; e. which are Investigational in nature, except as specifically provided in this Contract. Investigational determinations are made in accordance with Our policies and procedures for such determinations which are on file with the Louisiana Department of Insurance; f. rendered as a result of occupational disease or injury compensable under any Workers Compensation Law subject to the provisions of La. R.S. 23:1205(C); g. received from a dental or medical department maintained by or on behalf of an employer, a mutual Benefit association, labor union, trust, or similar person or Group; or h. rendered by a Provider who is the Member s spouse, child, stepchild, parent, stepparent or grandparent. i. Paid or payable under Medicare Part A or Part B when the member has Medicare, except when the Medicare Secondary Payer provisions apply. j. required to treat an Injury or illness are not Covered when a contributing cause was Your commission of or attempt to commit a felony, or to which a contributing cause was the Your being engaged in an illegal occupation.
2 5. Services in the following categories: a. those for diseases contracted or injuries sustained as a result of war, declared or undeclared, or any act of war; b. those for injuries or illnesses found by the Secretary of Veterans' Affairs to have been incurred in or aggravated during the performance of service in the uniformed services; c. those occurring as a result of taking part in a riot or acts of civil disobedience; d. those occurring as a result of a Member s commission or attempted commission of a felony. This exclusion does not apply to the extent inconsistent with the Health Insurance Portability and Accountability Act of 1996 (HIPAA). Benefits are available to the Member for illness or bodily injury due to an act of domestic violence or a medical condition (including both physical and mental health conditions); or in case of emergency care, the initial medical screening examination, treatment and stabilization of an Emergency Medical Condition. e. for treatment of any Member confined in a prison, jail, or other penal institution. 6. Services, surgery, supplies, treatment, or expenses in connection with or related to, or complications from the following REGARDLESS OF CLAIM OF MEDICAL NECESSITY: a. rhinoplasty; b. blepharoplasty services identified by CPT codes 15820, 15821, 15822, 15823; brow ptosis identified by CPT code 67900; or any revised or equivalent codes; c. gynecomastia; d. breast enlargement or reduction, except for breast reconstructive services as specifically provided in this Contract; e. implantation, removal and/or re-implantation of breast implants and services, illnesses, conditions, complications and/or treatment in relation to or as a result of breast implants; f. implantation, removal and/or re-implantation of penile prosthesis and services, illnesses, conditions, complications and/or treatment in relation to or as a result of penile prosthesis; g. diastasis recti; h. biofeedback; i. lifestyle/habit changing clinics and/or programs; j. treatment related to sex transformations, sexual function, sexual dysfunctions or inadequacies. k. industrial testing or self-help programs including, but not limited to stress management programs, work hardening programs and/or functional capacity evaluations; driving evaluations, etc; l. recreational therapy; m. Inpatient pain rehabilitation or pain control programs; and/or n. primarily to enhance athletic abilities. 7. Services, Surgery, supplies, treatment, or expenses related to: a. eyeglasses or contact lenses (except for the initial pair and fitting of eyeglasses or contact lenses required following cataract Surgery), unless shown as covered in the Schedule of Benefits; b. eye exercises, visual training, or orthoptics; c. hearing aids or for examinations for the prescribing or fitting of hearing aids, except as specified in this Contract; d. hair pieces, wigs, hair growth, and/or hair implants; e. the correction of refractive errors of the eye, including, but not limited to, radial keratotomy and laser surgery; or f. visual therapy.
3 8. Services, Surgery, supplies, treatment or expenses related to: a. any costs of donating an organ or tissue for transplant when a Member is a donor except as provided in this Contract; b. transplant procedures for any human organ or tissue transplant not specifically listed as covered. Related services or supplies include administration of high dose chemotherapy to support transplant procedures; c. the transplant of any non-human organ or tissue; or d. bone marrow transplants and stem cell rescue (autologous and allogeneic) are not covered, except as provided in this Contract. 9. Regardless of Medical Necessity, Benefits are not available for any of the following, except as specifically provided for in this Contract: a. weight reduction programs; b. removal of excess fat or skin, regardless of Medical Necessity, or services at a health spa or similar facility; or c. obesity or morbid obesity, regardless of Medical Necessity. 10. Food or food supplements, formulas and medical foods, including those used for gastric tube feedings. This exclusion does not apply to Low Protein Food Products as described in this Contract. 11. Sales tax or interest including sales tax on Prescription Drugs. Any applicable sales tax imposed on Prescription Drugs will be included in the cost of the Prescription Drugs in determining the Member s Coinsurance and Our financial responsibility. We will cover the cost of sales tax imposed on eligible Prescription Drugs, unless the total Prescription Drug Cost is less than the Member s Copayment, in which case, the Member must pay the Prescription Drug cost and sales tax. 12. Personal comfort, personal hygiene and convenience items including, but not limited to, air conditioners, humidifiers, personal fitness equipment, or alterations to a Member s home or vehicle. 13. Charges for the delivery of health care, diagnosis, consultation, or treatment of a Member, unless the Provider is physically present with the Member at the time services are rendered, are not covered unless approved by Us. Covered Services delivered using technology, including but not limited to audio and video transmission, telephone or , may be subject to Authorization as shown in the Schedule of Benefits. 14. Charges for failure to keep a scheduled visit, completion of a Claim form, or obtain medical records or information required to adjudicate a Claim, or for access to or enrollment in or with any Provider. 15. Routine foot care; palliative or cosmetic care or treatment; treatment of flat feet. Except for persons who have been diagnosed with diabetes: cutting or removal of corns and calluses, nail trimming or debriding, or supportive devices of the foot. 16. Any abortion other than to save the life of the mother. 17. Services or supplies related to the diagnosis and treatment of Infertility including, but not limited to, in vitro fertilization, uterine embryo lavage, embryo transfer, artificial insemination, gamete intrafallopian tube transfer, zygote intrafallopian tube transfer, low tubal ovum transfer, and drug
4 or hormonal therapy administered as part of the treatment. Even if fertile, these procedures are not available for Benefits. 18. Services, supplies or treatment related to artificial means of Pregnancy including, but not limited to, in vitro fertilization, uterine embryo lavage, embryo transfer, artificial insemination, gamete intrafallopian tube transfer, zygote intrafallopian tube transfer, low tubal ovum transfer, and drug or hormonal therapy administered as part of the treatment. 19. Services or supplies for pre-implantation genetic diagnosis and pre-genetic determination. 20. Acupuncture, anesthesia by hypnosis, or charges for anesthesia for non-covered services. 21. Services, supplies or treatment for cosmetic purposes, Cosmetic Surgery and any complications of Cosmetic Surgery, unless required for a Congenital Anomaly. 22. Dental Care and Treatment and dental appliances except as specifically provided in this Contract under Oral Surgery Benefits. 23. Except for Cleft lip and Cleft Palate Services, Diagnosis, treatment, or surgery of dentofacial anomalies including, but not limited to, malocclusion, Temporomandibular/Craniomandibular Joint Disorder, hyperplasia or hypoplasia of the mandible and/or maxilla, and any orthognathic condition. 24. Medical exams and/or diagnostic tests for routine or periodic physical examinations, screening examinations and immunizations, including occupational, recreational, camp or school required examinations, except as specifically provided in this Contract. 25. Travel, whether or not recommended by a Physician, and/or Ambulance Services, except as specifically provided in this Contract. 26. Educational services and supplies, training or re-training for a vocation, or the diagnosis, testing, or treatment for remedial reading, dyxlexia and other learning disabilities. This exclusion for educational services and supplies does not apply to training and education for diabetes. 27. Admission to a Hospital primarily for Diagnostic Services, which could have been provided safely and adequately in some other setting, e.g., Outpatient department of a Hospital or Physician s office. 28. Custodial Care, nursing home or custodial home care, regardless of the level of care required or provided. 29. Hospital charges for a well newborn, when not billed as part of the mother s charges. 30. Counseling services such as career counseling, marriage counseling, divorce counseling, parental counseling and job counseling. 31. Any incidental procedure, unbundled procedure, or mutually exclusive procedure, except as described in this Contract. 32. Surgical and medical treatment for snoring in the absence of obstructive sleep apnea, including laser assisted uvulopalatoplasty (LAUP). 33. Paternity tests and tests performed for legal purposes.
5 34. Genetic testing, unless the results are specifically required for a medical treatment decision on the Member, or required by law. 35. Reversal of a voluntary sterilization procedure. 36. Any Durable Medical Equipment, disposable medical equipment, items and supplies over reasonable quantity limits as determined by Us; all defibrillators other than implantable defibrillators Authorized by Us. 37. Sleep studies, unless obtained in a facility that is accredited by the Joint Commission or the American Academy of Sleep Medicine (AASM). If a sleep study is obtained from a facility that is not accredited by one of these bodies, then neither the sleep study nor any professional Claims associated with the sleep study are eligible for coverage. 38. Applied Behavior Analysis. (ABA) that the Company has determined is not Medically Necessary. ABA rendered to Members age seventeen (17) and older. ABA rendered by a Provider that has not been certified as a behavior analyst by the Behavior Analyst Certification Board or rendered by a Provider that has not provided, to the satisfaction of Company, documented evidence of equivalent education, professional training, and supervised experience in ABA. Applied Behavior Analysis is not covered for conditions other than Autism Spectrum Disorders. 39. Additional Exclusions and Limitations may be found in ARTICLE VII: (Prescription Drug Benefits) EXCLUSION TO THE PRESCRIPTION DRUG BENEFIT The following drugs, medicines, and related services and supplies are not covered: 1. Any medical service, prescription drug, medicine, equipment, supply or procedure directly or indirectly related to a condition that is non covered or not Medically Necessary is not Covered. 2. Other than Federal Food and Drug Administration ( FDA ) approved contraception methods, sterilization procedures, and patient education and counseling, abortions, abortion inducing drugs, and sterilization services and brand name contraceptives are Not Covered 3. Drugs and supplies for an Injury are not Covered when a contributing cause was Your voluntary taking of or being under the influence of an intoxicant or narcotic that was not taken or administered on the advice of a Physician, including driving while under the influence of such intoxicant or narcotic. A police officer s or treating Provider s determination that You were functioning under the influence of such intoxicant or narcotic when the Injury was sustained will be sufficient evidence for this Exclusion to apply. 4. Any drug not approved for use by the Federal Food and Drug Administration ( FDA ), unless that drug is recognized for treatment of the covered indication in standard reference compendium or in substantially accepted peer-reviewed medical literature, and is medically necessary. 5. Except for Low Protein Food products, food or nutritional supplements and vitamins are Excluded, including but not limited to, infant formulas and vitamins, herbal supplements and any other nutritional or over-the-counter electrolyte supplements.
6 6. Drugs and supplies required to treat an Injury or illness are not Covered when a contributing cause was Your commission of or attempt to commit a felony, or to which a contributing cause was the Your being engaged in an illegal occupation. 7. Drugs and supplies used to treat a war-related sickness or Injury or a military services-connected disability or condition, are Excluded from Coverage when You are legally entitled to obtain treatment for such condition from the Veteran s Administration ( VA ) and a VA facility is reasonably accessible to You. 8. Treatment, services, and supplies required to treat an Injury or illness that was directly or indirectly caused by an intentional or negligent action by You are not Covered, unless such Injury or illness is the direct result of an act of domestic violence or a medical condition. 9. Studies, treatments, or procedures for sex transformation, sexual identification or sexual dysfunction are not Covered 10. Drugs or supplies for an illness or Injury eligible for, or Covered by, any Federal, 11. State or local Government Workers Compensation Act, Occupational Disease law or other legislation of similar purpose is not Covered, unless the Employer is not required by law to provide such Coverage. 12. Drugs that require prior authorization are not covered without approval from LAHC. 13. Drugs that require step therapy are not covered without approval from LAHC. 14. Drugs in excess of LAHC-established quantity limits are not covered without approval from LAHC. 15. Drugs to replace prescriptions that were lost, misused, destroyed, or stolen are not covered. 16. Drugs that are refilled too soon are not covered without approval from LAHC. 17. Drugs filled at non-participating pharmacies are not covered without approval from LAHC. 18. Drugs that are available over-the-counter (OTC) are not covered unless listed as preventive health by LAHC. 19. Prescriptions for greater than a 30-day supply are not covered. 20. lifestyle-enhancing drugs including but not limited to medications used for cosmetic purposes (e.g., Botox, Renova, Tri-Luma ), hair loss or restoration (e.g., Propecia, Rogaine ), effects of aging on the skin, medications for weight loss (e.g. Xenical ), or medications used to enhance athletic performance; 21. any medication not proven effective in general medical practice; 22. Investigational drugs and drugs used other than for the FDA approved indication, except drugs that are not FDA approved for a particular indication but that are recognized for treatment of the covered indication in a standard reference compendia or as shown in the results of controlled clinical studies published in at least two peer reviewed national professional medical journals and all Medically Necessary services associated with the administration of the drug; 23. fertility drugs; 24. minerals and vitamins, except for vitamins requiring a prescription for dispensation; 25. nutritional or dietary supplements, or herbal supplements and treatments; 26. Prescription vitamins not listed as covered in the Prescription Drug Formulary (including but not limited to Enlyte). 27. drugs that can be lawfully obtained without a Physician s order, including over-the-counter ( OTC ) drugs, or Prescription Drugs for which there is an OTC equivalent available;
7 28. refills in excess of the number specified by the Physician or the dispensing limitation described in this Contract, or a refill prior to seventy-five percent (75%) of day supply used, or any refills dispensed more than one (1) year after the date of the Physician s original prescription; 29. Compounded drugs; 30. Prescription Drugs filled prior to the Member s Effective Date or after a Member s coverage ends; 31. replacement of lost or stolen Prescription Drugs, or those rendered useless by mishandling, damage or breakage; 32. prescription Drugs related to a non-covered service; 33. Prescription Drugs, equipment or substances to treat sexual or erectile dysfunction (e.g., Viagra, Cialis, Levitra ) unless specifically listed as Covered; 34. medication, drugs or substances that are illegal to dispense, possess, consume or use under the laws of the United States or any state, or that are dispensed or used in an illegal manner; 35. growth hormone therapy, except for chronic renal insufficiency, AIDS wasting, and Turners Syndrome, unless an endocrinologist confirms growth hormone deficiency with abnormal provocative stimulation testing; 36. Prescription Drugs for and/or treatment of idiopathic short stature; 37. topically applied prescription drug preparations that are approved by the FDA as medical devices; 38. Drugs used primarily to enhance athletic abilities; 39. lifestyle/habit changing clinics and\or programs; 40. treatment related to sex transformations, sexual function, sexual dysfunctions or inadequacies; 41. Industrial testing of self-help programs including, but not limited to stress management programs, work hardening programs and/or functional capacity evaluations; driving evaluations, etc.; 42. recreational therapy; 43. Inpatient pain rehabilitation or pain control programs. 44. Prescription Drug coverage for Controlled Dangerous Substances may be limited or excluded when Controlled Dangerous Substances have been prescribed by multiple prescribers on a concurrent basis, where a prescriber agrees prescriptions were obtained through Member misrepresentation to that prescriber. Limitation may include, but is not confined to requiring future Controlled Dangerous Substances to be obtained from only one prescriber and one pharmacy. 45. Prescription Drugs subject to the Step Therapy program when the Step Therapy program was not utilized or the drug was not approved by Company or its Pharmacy Benefit Manager.
Regence Engage Plan Highlights For Groups of /1/2016
 Plan Features Provider choice: Members have direct access to their choice of providers. Category 1 are Preferred; Category 2 are Participating; and Category 3 are Non-contracted providers. Simplicity:
Plan Features Provider choice: Members have direct access to their choice of providers. Category 1 are Preferred; Category 2 are Participating; and Category 3 are Non-contracted providers. Simplicity:
PLAN FEATURES PREFERRED CARE
 PLAN DESIGN & BENEFITS - "HMO" PLAN FEATURES Deductible (per calendar year) $200 Individual $400 Family All covered expenses, excluding prescription drugs, accumulate toward the preferred Deductible. Unless
PLAN DESIGN & BENEFITS - "HMO" PLAN FEATURES Deductible (per calendar year) $200 Individual $400 Family All covered expenses, excluding prescription drugs, accumulate toward the preferred Deductible. Unless
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
MEDICAL PLAN EXCLUSIONS. For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered:
 MEDICAL PLAN EXCLUSIONS For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered: (1) Abortion. Services, supplies, care or treatment in connection with an
MEDICAL PLAN EXCLUSIONS For all Medical Benefits shown in the Schedule of Benefits, a charge for the following is not covered: (1) Abortion. Services, supplies, care or treatment in connection with an
PREFERRED CARE. combination of family members; however no single individual within the family will be subject to more than the individual
 PLAN FEATURES Deductible (per plan year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The family Deductible is a cumulative Deductible
PLAN FEATURES Deductible (per plan year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The family Deductible is a cumulative Deductible
CHAPTER 1 SECTION 1.1 EXCLUSIONS TRICARE POLICY MANUAL M, AUGUST 1, 2002 ADMINISTRATIVE. ISSUE DATE: June 1, 1999 AUTHORITY: 32 CFR 199.
 ADMINISTRATIVE CHAPTER 1 SECTION 1.1 ISSUE DATE: June 1, 1999 AUTHORITY: 32 CFR 199.4(g) I. POLICY A. In addition to any definitions, requirements, conditions, or limitations enumerated and described in
ADMINISTRATIVE CHAPTER 1 SECTION 1.1 ISSUE DATE: June 1, 1999 AUTHORITY: 32 CFR 199.4(g) I. POLICY A. In addition to any definitions, requirements, conditions, or limitations enumerated and described in
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived 30% after deductible
 PLAN FEATURES NON- Deductible (per calendar year) $500 Individual $750 Individual $1,500 Family $2,250 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and
PLAN FEATURES NON- Deductible (per calendar year) $500 Individual $750 Individual $1,500 Family $2,250 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred and
Chapter 1 Section 1.2
 Administration Chapter 1 Section 1.2 Issue Date: June 1, 1999 Authority: 32 CFR 199.4(g) 1.0 POLICY 1.1 In addition to any definitions, requirements, conditions, or limitations enumerated and described
Administration Chapter 1 Section 1.2 Issue Date: June 1, 1999 Authority: 32 CFR 199.4(g) 1.0 POLICY 1.1 In addition to any definitions, requirements, conditions, or limitations enumerated and described
Optional PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and
High Deductible Health Plan - H S A PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY
 PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $2,000 Individual $2,600 Family $4,000 Family All covered expenses including prescription drugs accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $2,000 Individual $2,600 Family $4,000 Family All covered expenses including prescription drugs accumulate toward both the preferred
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY - SELF FUNDED
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $250 Individual None Family $750 Family Unless otherwise indicated, the deductible must be met prior to benefits being
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $250 Individual None Family $750 Family Unless otherwise indicated, the deductible must be met prior to benefits being
BlueChoice Opt-Out Open Access
 BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay 1 Out-of-Network You Pay 1 24/7 FIRSTHELP NURSE ADVICE LINE Free advice from a registered nurse BLUE REWARDS Visit www.carefirst.com/bluerewards
BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay 1 Out-of-Network You Pay 1 24/7 FIRSTHELP NURSE ADVICE LINE Free advice from a registered nurse BLUE REWARDS Visit www.carefirst.com/bluerewards
SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS
 SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS 1. General Exclusions. In addition to the Plan's other restrictions, no Plan benefit is payable for any of the following
SCHEDULE A SMITHFIELD FOODS HEALTHCARE PROGRAM SUMMARY PLAN DESCRIPTION EXCLUSIONS 1. General Exclusions. In addition to the Plan's other restrictions, no Plan benefit is payable for any of the following
Your Summary of Benefits ACO Flex
 Your Summary of Benefits ACO Flex Premier ACO Flex 250/15/30 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
Your Summary of Benefits ACO Flex Premier ACO Flex 250/15/30 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
HEALTH SAVINGS ACCOUNT (HSA)
 HSA FEATURES Health Savings Account Amount $600 Employee $1,000 Family Amount contributed to the HSA by the employer. Funded on a quarterly basis. HSA amount reflected is on a per calendar year basis.
HSA FEATURES Health Savings Account Amount $600 Employee $1,000 Family Amount contributed to the HSA by the employer. Funded on a quarterly basis. HSA amount reflected is on a per calendar year basis.
Single/Family $2,500/$5,000 $5,000/$10,000. Single/Family $6,000/$12,000 $10,000/None. Single/Family $5,000/$10,000 $6,250/$12,500
 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Regence EmployeeChoice Plan Highlights Platinum 250, Platinum 500, Gold 500, Gold 1000, Gold 1500, Silver 2500, Bronze Essential /1/2016
 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of-Network provider, the
$10 copay. $10 copay. $10 copay $5 copay $10 copay $5 copay. $10 copay. No charge. No charge. No charge
 PLAN FEATURES * ** Deductible (per calendar ) Member Coinsurance Copay Maximum (per calendar ) Lifetime Maximum Unlimited Primary Care Physician Selection Required Upon enrollment to a Vitalidad Plus plan,
PLAN FEATURES * ** Deductible (per calendar ) Member Coinsurance Copay Maximum (per calendar ) Lifetime Maximum Unlimited Primary Care Physician Selection Required Upon enrollment to a Vitalidad Plus plan,
Blue Cross Premier Bronze
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within BCBSM s unsurpassed statewide PPO network including nationwide coverage.
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within BCBSM s unsurpassed statewide PPO network including nationwide coverage.
CONNECTICUT GENERAL LIFE INSURANCE COMPANY a CIGNA company (called CG) CERTIFICATE RIDER
 Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CONNECTICUT GENERAL LIFE INSURANCE COMPANY a CIGNA company (called CG) CERTIFICATE RIDER No. CR7BIASO3-2 Policyholder:
Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CONNECTICUT GENERAL LIFE INSURANCE COMPANY a CIGNA company (called CG) CERTIFICATE RIDER No. CR7BIASO3-2 Policyholder:
Preferred Providers In-Network You Pay 1. None None None None $1,000 $2,000 $2,000 $2,000. No charge* No charge* No charge* No charge*
 BluePreferred Services ANNUAL DEDUCTIBLE (BENEFIT PERIOD) 3,4 Individual Individual & Child(ren) 5 Individual & Adult Family ANNUAL OUT-OF-POCKET MAXIMUM (BENEFIT PERIOD) 6 Individual Individual & Child(ren)
BluePreferred Services ANNUAL DEDUCTIBLE (BENEFIT PERIOD) 3,4 Individual Individual & Child(ren) 5 Individual & Adult Family ANNUAL OUT-OF-POCKET MAXIMUM (BENEFIT PERIOD) 6 Individual Individual & Child(ren)
The Ins And Outs Of Coverage
 The Ins And Outs Of Coverage Some people under age 65 are eligible for Medicare in addition to any other coverage they may have. The following chart shows how payment is coordinated under various scenarios:
The Ins And Outs Of Coverage Some people under age 65 are eligible for Medicare in addition to any other coverage they may have. The following chart shows how payment is coordinated under various scenarios:
Updated: 10/01/12 Page : 1
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
BlueChoice Opt-Out Open Access
 BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay Out-of-Network You Pay ANNUAL DEDUCTIBLE (Benefit period) 1 Individual Individual & Child(ren) 2 Individual & Adult Family
BlueChoice Opt-Out Open Access Summary of Benefits Services In-Network You Pay Out-of-Network You Pay ANNUAL DEDUCTIBLE (Benefit period) 1 Individual Individual & Child(ren) 2 Individual & Adult Family
Kaiser Permanente (No. and So. California) 2018 Union
 Kaiser Permanente (No. and So. California) General Information Lifetime Maximum Benefit Annual Maximum Benefit Coinsurance Percentage Precertification Requirements Precertification Penalty Health Savings
Kaiser Permanente (No. and So. California) General Information Lifetime Maximum Benefit Annual Maximum Benefit Coinsurance Percentage Precertification Requirements Precertification Penalty Health Savings
SUMMARY OF BENEFITS. It's Your Health. Features that Add Value. You Can Depend on CIGNA HealthCare. Quality Service Is Part of Quality Care
 SUMMARY OF BENEFITS Your CIGNA HealthCare HMO plan Features that Add Value The CIGNA HealthCare 24-Hour Health Information Line SM connects you to registered nurses and a library of hundreds of recorded
SUMMARY OF BENEFITS Your CIGNA HealthCare HMO plan Features that Add Value The CIGNA HealthCare 24-Hour Health Information Line SM connects you to registered nurses and a library of hundreds of recorded
Chapter 12 Benefits and Covered Services
 12 Benefits and Covered Services Health Choice Generations covers the same benefits covered under Original Medicare. Sometimes Medicare adds coverage for a new service during the year. Health Choice Generations
12 Benefits and Covered Services Health Choice Generations covers the same benefits covered under Original Medicare. Sometimes Medicare adds coverage for a new service during the year. Health Choice Generations
Group Hospitalization and Medical Services, Inc.
 Group Hospitalization and Medical Services, Inc. doing business as CareFirst BlueCross BlueShield (CareFirst) 840 First Street, NE Washington, DC 20065 202-479-8000 A not-for-profit health service plan
Group Hospitalization and Medical Services, Inc. doing business as CareFirst BlueCross BlueShield (CareFirst) 840 First Street, NE Washington, DC 20065 202-479-8000 A not-for-profit health service plan
Covered Services List
 CAREPLUS Covered Services List For CeltiCare Health with MassHealth CarePlus Coverage This is a list of all covered services and benefits for MassHealth CarePlus enrolled in CeltiCare Health. The list
CAREPLUS Covered Services List For CeltiCare Health with MassHealth CarePlus Coverage This is a list of all covered services and benefits for MassHealth CarePlus enrolled in CeltiCare Health. The list
WHAT DOES MEDICALLY NECESSARY MEAN?
 WHAT DOES MEDICALLY NECESSARY MEAN? Your Primary Care Provider (PCP) will help you get the services you need that are medically necessary as defined below. Medically Necessary means appropriate and necessary
WHAT DOES MEDICALLY NECESSARY MEAN? Your Primary Care Provider (PCP) will help you get the services you need that are medically necessary as defined below. Medically Necessary means appropriate and necessary
$2,000 Individual. Deductible (per calendar year)
 PLAN FEATURES Deductible (per calendar year) FAMILY PHYSICIANS GROUP $2,000 Individual $4,000 Family Unless otherwise indicated, the deductible must be met prior to benefits being payable. Member cost
PLAN FEATURES Deductible (per calendar year) FAMILY PHYSICIANS GROUP $2,000 Individual $4,000 Family Unless otherwise indicated, the deductible must be met prior to benefits being payable. Member cost
Open Access PLAN DESIGN
 PLAN FEATURES Deductible (per plan year) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family All covered expenses accumulate separately toward preferred or non-preferred Deductible. Unlesss
PLAN FEATURES Deductible (per plan year) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family All covered expenses accumulate separately toward preferred or non-preferred Deductible. Unlesss
BlueChoice HMO Open Access HRA/HSA
 BlueChoice HMO Open Access HRA/HSA Summary of Benefits Services In-Network You Pay 1 BLUE REWARDS Visit www.carefirst.com/bluerewards for more information ANNUAL DEDUCTIBLE (BENEFIT PERIOD) 2 Individual
BlueChoice HMO Open Access HRA/HSA Summary of Benefits Services In-Network You Pay 1 BLUE REWARDS Visit www.carefirst.com/bluerewards for more information ANNUAL DEDUCTIBLE (BENEFIT PERIOD) 2 Individual
Your Summary of Benefits SISC 80-E $20 Anthem Classic PPO
 Your Summary of Benefits SISC 80-E $20 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
Your Summary of Benefits SISC 80-E $20 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
Your Summary of Benefits SISC 80-G $30 Anthem Classic PPO
 Your Summary of Benefits SISC 80-G $30 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
Your Summary of Benefits SISC 80-G $30 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
PLAN DESIGN & BENEFITS PROVIDED BY AETNA HEALTH INC. - FULL RISK
 PLAN FEATURES Deductible (per calendar year) PLAN DESIGN & BENEFITS None Individual None Family The family Deductible is a cumulative Deductible for all family members. The family Deductible can be met
PLAN FEATURES Deductible (per calendar year) PLAN DESIGN & BENEFITS None Individual None Family The family Deductible is a cumulative Deductible for all family members. The family Deductible can be met
PLAN DESIGN AND BENEFITS - PA POS 4.2 with $5/$15/$30 RX PARTICIPATING PROVIDERS
 PLAN FEATURES Deductible (per calendar year) PHYSICIAN SERVICES Primary Care Physician Visits Specialist Office Visits Maternity OB Visits Allergy Treatment Allergy Testing PREVENTIVE CARE Routine Adult
PLAN FEATURES Deductible (per calendar year) PHYSICIAN SERVICES Primary Care Physician Visits Specialist Office Visits Maternity OB Visits Allergy Treatment Allergy Testing PREVENTIVE CARE Routine Adult
AETNA PPO PLAN COVERED DEPENDENTS UNDER 65
 AETNA PPO PLAN COVERED DEPENDENTS UNDER 65 Plan Deductible (per calendar year; applies to all covered services; excludes deductible carryover.) $300 Individual $600 Family $600 Individual $1200 Family
AETNA PPO PLAN COVERED DEPENDENTS UNDER 65 Plan Deductible (per calendar year; applies to all covered services; excludes deductible carryover.) $300 Individual $600 Family $600 Individual $1200 Family
Stanislaus County Medical Benefits EPO Option. In-Network Benefits (Stanislaus County Partners in Out-of-Network Benefits
 Stanislaus County Medical EPO Option The following summary of benefits is a brief outline of the maximum amounts or special limits that may apply to benefits payable under the Plan. For a detailed description
Stanislaus County Medical EPO Option The following summary of benefits is a brief outline of the maximum amounts or special limits that may apply to benefits payable under the Plan. For a detailed description
SUMMARY OF BENEFITS Your CIGNA HealthCare Indemnity plan
 SUMMARY OF BENEFITS Your CIGNA HealthCare Indemnity plan Features that Add Value The CIGNA HealthCare 24-Hour Health Information Line SM connects you to registered nurses and a library of hundreds of recorded
SUMMARY OF BENEFITS Your CIGNA HealthCare Indemnity plan Features that Add Value The CIGNA HealthCare 24-Hour Health Information Line SM connects you to registered nurses and a library of hundreds of recorded
PLAN DESIGN & BENEFITS PROVIDED BY AETNA
 PLAN FEATURES Deductible (per calendar year) PLAN DESIGN & BENEFITS None Individual None Family The family Deductible is a cumulative Deductible for all family members. The family Deductible can be met
PLAN FEATURES Deductible (per calendar year) PLAN DESIGN & BENEFITS None Individual None Family The family Deductible is a cumulative Deductible for all family members. The family Deductible can be met
CA Group Business 2-50 Employees
 PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Member Coinsurance Copay Maximum (per calendar year) Lifetime Maximum Referral Requirement PHYSICIAN SERVICES Primary
COVERED SERVICES LIST FOR HNE BE HEALTHY MEMBERS WITH MASSHEALTH STANDARD OR COMMONHEALTH COVERAGE
 COVERED SERVICES LIST FOR HNE BE HEALTHY MEMBERS WITH MASSHEALTH STANDARD OR COMMONHEALTH COVERAGE This is a list of all covered services and benefits for MassHealth Standard and CommonHealth members enrolled
COVERED SERVICES LIST FOR HNE BE HEALTHY MEMBERS WITH MASSHEALTH STANDARD OR COMMONHEALTH COVERAGE This is a list of all covered services and benefits for MassHealth Standard and CommonHealth members enrolled
Aetna Health of California, Inc.
 Easily locate PrimeCare participating providers at www.aetna.com/docfind/primecare PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral
Easily locate PrimeCare participating providers at www.aetna.com/docfind/primecare PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral
Covered (blood, blood components, human blood products, and their administration) Covered (Some restrictions)
 Washington Apple Health Medical Benefits Allergy Services (Antigen/Allergy Serum/Allergy Shots) Ambulance Services (Air Transportation) by FFS* Ambulance Services (Emergency Transportation) Ambulatory
Washington Apple Health Medical Benefits Allergy Services (Antigen/Allergy Serum/Allergy Shots) Ambulance Services (Air Transportation) by FFS* Ambulance Services (Emergency Transportation) Ambulatory
UNM Medical Plan. summary of benefits. Effective: July 1, 2012
 UNM Medical Plan summary of benefits Effective: July 1, 2012 Offered by The Regents of the University of New Mexico Administered by Lovelace Insurance Company administered by ANNUAL PLAN YEAR DEDUCTIBLE
UNM Medical Plan summary of benefits Effective: July 1, 2012 Offered by The Regents of the University of New Mexico Administered by Lovelace Insurance Company administered by ANNUAL PLAN YEAR DEDUCTIBLE
Annual copay maximum: Individual $500; Family $1,500 The following copay does not apply to the annual copay maximum: for infertility services
 Custom Premier HMO 30/100 (HMO 30 w/o CHIRO) Effective 07.01.2017 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan,
Custom Premier HMO 30/100 (HMO 30 w/o CHIRO) Effective 07.01.2017 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan,
PLAN DESIGN & BENEFITS
 PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum (per calendar year) Poway Unified School District None Individual None Family $1,500 Individual $3,000 Family In-Network expenses include
PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum (per calendar year) Poway Unified School District None Individual None Family $1,500 Individual $3,000 Family In-Network expenses include
Your Summary of Benefits SISC 90-G $20 Anthem Classic PPO
 Your Summary of Benefits SISC 90-G $20 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
Your Summary of Benefits SISC 90-G $20 Anthem Classic PPO This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state members,
CIGNA HMO. Primary Care Physician. Network Benefits. Benefits at a Glance: CIGNA HMO. Insurance Benefits Guide 2010
 , a plan administered by CIGNA HealthCare, is available in all counties in the state except: Abbeville, Aiken, Barnwell, Edgefield, Greenwood, Laurens, McCormick and Saluda. Primary Care Physician With,
, a plan administered by CIGNA HealthCare, is available in all counties in the state except: Abbeville, Aiken, Barnwell, Edgefield, Greenwood, Laurens, McCormick and Saluda. Primary Care Physician With,
Essential Health Benefits Addendum. Office of the Insurance Commissioner Washington State
 Essential Health Benefits Addendum Office of the Insurance Commissioner Washington State 1 Details, details Classification of Services Classification of a service may affect the scope of the available
Essential Health Benefits Addendum Office of the Insurance Commissioner Washington State 1 Details, details Classification of Services Classification of a service may affect the scope of the available
Schedule of Benefits
 3T, 09/09 Schedule of Benefits Services listed below are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and Out-of-Network. Coverage
3T, 09/09 Schedule of Benefits Services listed below are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and Out-of-Network. Coverage
Single/Family $2,500/$5,000 $5,000/$10,000. Single/Family $6,000/$12,000 $10,000/None. Single/Family $5,000/$10,000 $6,250/$12,500
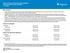 Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of- Network provider, the
Plan Information Provider networks: Members have direct access to their choice of providers. Member cost-sharing is lowest for In-Network providers. If a member chooses an Out-of- Network provider, the
2017 Summary of Benefits
 H5209 004_DSB9 23 16 File & Use 10/14/2016 DHS Approved 10 7 2016 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP) January 1, 2017 to December
H5209 004_DSB9 23 16 File & Use 10/14/2016 DHS Approved 10 7 2016 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP) January 1, 2017 to December
Cigna Health and Life Insurance Company. Plan Benefits. Unlimited. Unlimited. Not applicable. Not applicable. Not applicable
 SUMMARY OF BENEFITS Client Name: Washington County Public Schools Benefit Option Name: Medicare Supplement Effective: July 1, 2018 through June 30, 2019 1 Benefit Description Lifetime Maximum Applies to
SUMMARY OF BENEFITS Client Name: Washington County Public Schools Benefit Option Name: Medicare Supplement Effective: July 1, 2018 through June 30, 2019 1 Benefit Description Lifetime Maximum Applies to
Member Services: Authorizations: Option #2 Authorization Fax:
 Allergy 100% covered Office visit $10 co-pay 100% covered Allergy injections no co-pay Immunotherapy or other therapy -no co-pay Cardiac Rehab 100% covered 100% covered 100% covered Contraceptives Covered
Allergy 100% covered Office visit $10 co-pay 100% covered Allergy injections no co-pay Immunotherapy or other therapy -no co-pay Cardiac Rehab 100% covered 100% covered 100% covered Contraceptives Covered
HUSKY Health Benefits and Prior Authorization Requirements Grid* Inpatient Hospital Effective: January 1, 2012
 100% covered 100% covered 100% covered Prior Authorization Required For all nonmaternity, non-emergent admissions. Maternity Admits: CHNCT requests the hospital to notify us of all deliveries. Emergency
100% covered 100% covered 100% covered Prior Authorization Required For all nonmaternity, non-emergent admissions. Maternity Admits: CHNCT requests the hospital to notify us of all deliveries. Emergency
SUMMARY OF BENEFITS. Your Valley Health System Network and CIGNA HealthCare Open Access Plus In-Network plan
 SUMMARY OF BENEFITS Your Valley Health System Network and CIGNA HealthCare Open Access Plus In-Network plan Features that Add Value Your plan offers the convenience of referral-free access to doctors,
SUMMARY OF BENEFITS Your Valley Health System Network and CIGNA HealthCare Open Access Plus In-Network plan Features that Add Value Your plan offers the convenience of referral-free access to doctors,
Summary of Benefits. Archdiocese of New York. UnitedHealthcare Choice Plan
 Summary of Benefits UnitedHealthcare Choice Plan Archdiocese of New York Active Plan for Non-Bargaining Lay and Religious Effective January 1, 2018, if you have any questions please call United HealthCare
Summary of Benefits UnitedHealthcare Choice Plan Archdiocese of New York Active Plan for Non-Bargaining Lay and Religious Effective January 1, 2018, if you have any questions please call United HealthCare
2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits
 2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits For Oregon counties: Clackamas, Clatsop, Columbia, Jackson, Josephine, Multnomah, Tillamook, Washington and Yamhill H5859_1099_CO_1018 CMS
2018 CareOregon Advantage Plus (HMO-POS SNP) Summary of Benefits For Oregon counties: Clackamas, Clatsop, Columbia, Jackson, Josephine, Multnomah, Tillamook, Washington and Yamhill H5859_1099_CO_1018 CMS
CALIFORNIA Small Group HMO Aetna Health of California, Inc. Plan Effective Date: 04/01/2007. Aetna Value Network* HMO $30/$40
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral Requirement PHYSICIAN SERVICES CALIFORNIA Small Group HMO Primary Care Physician
PLAN FEATURES Deductible (per calendar year) Member Coinsurance Lifetime Maximum Primary Care Physician Selection Referral Requirement PHYSICIAN SERVICES CALIFORNIA Small Group HMO Primary Care Physician
Schedule of Benefits
 SN, 10/09 Schedule of Benefits Services listed are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and. Coverage coverage applies
SN, 10/09 Schedule of Benefits Services listed are covered when Medically Necessary. Please see your Benefit Handbook for details. Your Plan offers two levels of coverage: and. Coverage coverage applies
It s Your Health. Effective July 1, 2012
 SUMMARY OF BENEFITS Your System and CIGNA Choice Fund SM Health Reimbursement Arrangement-Open Access Plus plan Features that Add Value CIGNA Choice Fund combines conventional health coverage with health
SUMMARY OF BENEFITS Your System and CIGNA Choice Fund SM Health Reimbursement Arrangement-Open Access Plus plan Features that Add Value CIGNA Choice Fund combines conventional health coverage with health
Your Out-of-Pocket Type of Service
 Calendar Year Deductible (CYD) 1 $0 single/ 3x family Out-of-Pocket Maximum - Deductibles, coinsurance and copays all accrue toward the outof-pocket maximum. With respect to family plans, an individual
Calendar Year Deductible (CYD) 1 $0 single/ 3x family Out-of-Pocket Maximum - Deductibles, coinsurance and copays all accrue toward the outof-pocket maximum. With respect to family plans, an individual
Summary of Benefits Prominence Preferred Health Insurance Small Group Health Plan
 Calendar Year Deductible (CYD) 2 $1,000 Single / $3,000 Family $3,000 Single / $9,000 Family Coinsurance - Member responsibility 20% coinsurance 50% coinsurance Out-of-Pocket Maximum 3 - Deductibles, coinsurance
Calendar Year Deductible (CYD) 2 $1,000 Single / $3,000 Family $3,000 Single / $9,000 Family Coinsurance - Member responsibility 20% coinsurance 50% coinsurance Out-of-Pocket Maximum 3 - Deductibles, coinsurance
CHIP Perinatal Program Newborn Schedule of Benefits
 Inpatient General Acute and Inpatient Rehabilitation Hospital Services Services include: Hospital-provided Physician or Provider Semi-private room and board (or private if medically necessary as certified
Inpatient General Acute and Inpatient Rehabilitation Hospital Services Services include: Hospital-provided Physician or Provider Semi-private room and board (or private if medically necessary as certified
HEALTH PLAN BENEFITS AND COVERAGE MATRIX
 HEALTH PLAN BENEFITS AND COVERAGE MATRIX THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
HEALTH PLAN BENEFITS AND COVERAGE MATRIX THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
Skilled nursing facility visits
 Modified Premier HMO 20 Non Union This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please refer to your Certificate
Modified Premier HMO 20 Non Union This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please refer to your Certificate
COVERED SERVICES FOR NHP MASSHEALTH MEMBERS
 COVERED SERVICES FOR NHP MASSHEALTH MEMBERS Neighborhood Health Plan Covered Services for MassHealth Standard & CommonHealth, Family Assistance, and CarePlus Issued and effective October 1, 2015 nhp.org/member
COVERED SERVICES FOR NHP MASSHEALTH MEMBERS Neighborhood Health Plan Covered Services for MassHealth Standard & CommonHealth, Family Assistance, and CarePlus Issued and effective October 1, 2015 nhp.org/member
SUMMARY OF BENEFITS. Physician Services Physician Office Visit All services including Lab & X-ray
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. For - Trustees of Dartmouth College Indemnity Plan Direct Access to Obstetricians and Gynecologists - You do not need prior authorization from the
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. For - Trustees of Dartmouth College Indemnity Plan Direct Access to Obstetricians and Gynecologists - You do not need prior authorization from the
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION
 Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
HOME BANK - S2395 NON-GRANDFATHERED CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET
 CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to 26 180 days from incurred Filing Limit date, except when 180 days would
CONSUMER DRIVEN HEALTH PLAN BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to 26 180 days from incurred Filing Limit date, except when 180 days would
SUMMARY OF FAMIS COVERED SERVICES No cost sharing will be charged to American Indians and Alaska Native
 SUMMARY OF COVERED SERVICES No cost sharing will be charged to American Indians and Alaska Native Service Inpatient Hospital Outpatient Hospital $15 per $2 per visit (waived if admitted) $25 per $5 per
SUMMARY OF COVERED SERVICES No cost sharing will be charged to American Indians and Alaska Native Service Inpatient Hospital Outpatient Hospital $15 per $2 per visit (waived if admitted) $25 per $5 per
UNIVERSITY OF MICHIGAN BZK Effective Date: 01/01/2018
 UNIVERSITY OF MICHIGAN 68712000 0070051870000-06BZK Effective Date: 01/01/2018 This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional
UNIVERSITY OF MICHIGAN 68712000 0070051870000-06BZK Effective Date: 01/01/2018 This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional
NY EPO OA 1-09 v Page 1
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance (applies to all expenses unless otherwise stated) Maximum Out-of-Pocket Limit (per calendar year) Lifetime Maximum (per member lifetime)
PLAN FEATURES Deductible (per calendar year) Member Coinsurance (applies to all expenses unless otherwise stated) Maximum Out-of-Pocket Limit (per calendar year) Lifetime Maximum (per member lifetime)
2018 Summary of Benefits
 2018 Summary of Benefits H5209-004_MDASB 9-13-17 Accepted 9/18/2018 DHS Approved 09/13/2017 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP)
2018 Summary of Benefits H5209-004_MDASB 9-13-17 Accepted 9/18/2018 DHS Approved 09/13/2017 This is a summary of drug and health services covered by Care Wisconsin Medicare Dual Advantage Plan (HMO SNP)
2016 Medical Plan Comparison Chart
 2016 Medical Plan Comparison Chart WellStar Health System is committed to helping you control healthcare costs while providing more choices and personal control over your healthcare coverage through the
2016 Medical Plan Comparison Chart WellStar Health System is committed to helping you control healthcare costs while providing more choices and personal control over your healthcare coverage through the
Security Forces SCHEDULE OF BENEFITS Participating Provider Covered Person pays:
 Benefit Local Office Visits/Physician Consultation (per visit/occurrence) Primary Care, Specialist and Walk in Clinics Security Forces Participating Provider Prescription Service rendered at a pharmacy
Benefit Local Office Visits/Physician Consultation (per visit/occurrence) Primary Care, Specialist and Walk in Clinics Security Forces Participating Provider Prescription Service rendered at a pharmacy
Kaiser Permanente Group Plan 301 Benefit and Payment Chart
 301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
Schedule of Benefits - HMO Group - MEDFORD AREA SCHOOL DISTRICT Benefit Year: January 1st through December 31st Effective Date: 01/01/2016
 Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Summary of Benefits. January 1, 2018 December 31, Providence Medicare Dual Plus (HMO SNP)
 Summary of Benefits January 1, 2018 December 31, 2018 Providence Medicare Dual Plus (HMO SNP) This plan is available in Clackamas, Multnomah and Washington counties in Oregon for members who are eligible
Summary of Benefits January 1, 2018 December 31, 2018 Providence Medicare Dual Plus (HMO SNP) This plan is available in Clackamas, Multnomah and Washington counties in Oregon for members who are eligible
RSNA EMPLOYEE BENEFIT TRUST PLAN II S2502 NON GRANDFATHERED PLAN BENEFIT SHEET
 BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to age 26 Filing Limit 1 year from date of service Mailing Address & PPO Company. Remit claims to:
BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Standard COB Dependents Children birth to age 26 Filing Limit 1 year from date of service Mailing Address & PPO Company. Remit claims to:
SUMMARY OF BENEFITS. Features that Add Value. It's Your Health. You Can Depend on CIGNA HealthCare. It's Your Choice
 SUMMARY OF BENEFITS Your CIGNA HealthCare Open Access Plus plan Features that Add Value Your plan offers the convenience of referral-free access to doctors, and the option to select a personal Primary
SUMMARY OF BENEFITS Your CIGNA HealthCare Open Access Plus plan Features that Add Value Your plan offers the convenience of referral-free access to doctors, and the option to select a personal Primary
Aetna Student Health Plan Design and Benefits Summary Columbia University Medical Center
 Aetna Student Health Plan Design and Benefits Summary Columbia University Medical Center Policy Year: 2014-2015 Policy Number: 812835 www.aetnastudenthealth.com (877) 409-7366 This Plan Design and Benefits
Aetna Student Health Plan Design and Benefits Summary Columbia University Medical Center Policy Year: 2014-2015 Policy Number: 812835 www.aetnastudenthealth.com (877) 409-7366 This Plan Design and Benefits
Telemedicine services $0 copay Not applicable Primary care provider (PCP) CYD/Coinsurance CYD/Coinsurance CYD/Coinsurance CYD/Coinsurance
 Calendar Year Deductible (CYD) 2 Plan includes an embedded individual deductible provision. An embedded deductible combines individual and family deductibles in $4,000 Single / $8,000 Family $12,000 Single
Calendar Year Deductible (CYD) 2 Plan includes an embedded individual deductible provision. An embedded deductible combines individual and family deductibles in $4,000 Single / $8,000 Family $12,000 Single
Your Out-of-Pocket Type of Service
 Calendar Year Deductible (CYD) 1 $3,000 single/ 3x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,200 single/ 2x family maximum. With respect to family plans,
Calendar Year Deductible (CYD) 1 $3,000 single/ 3x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,200 single/ 2x family maximum. With respect to family plans,
WILLIS KNIGHTON MEDICAL CENTER S2763 NON GRANDFATHERED PLAN BENEFIT SHEET
 BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Customized COB Dependents Children birth to 26 Filing Limit 12 months For employees that work in a WKHS location within the primary HealthPlus
BENEFIT SHEET GENERAL PLAN INFORMATION Coordination of Benefits Customized COB Dependents Children birth to 26 Filing Limit 12 months For employees that work in a WKHS location within the primary HealthPlus
CLIENT SUMMARY OF BENEFITS
 Connecticut General Life Insurance Co. For - Purdue University Open Access Plus Plan - Copay Plan CLIENT SUMMARY OF BENEFITS Plan Highlights Lifetime Maximum Unlimited Unlimited Inpatient and Outpatient
Connecticut General Life Insurance Co. For - Purdue University Open Access Plus Plan - Copay Plan CLIENT SUMMARY OF BENEFITS Plan Highlights Lifetime Maximum Unlimited Unlimited Inpatient and Outpatient
Schedule of Benefits - Point of Service MOSINEE SCHOOL DISTRICT Benefit Year: January 1st Through December 31st Effective Date: 07/01/2016
 Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Platinum Local Access+ HMO $25 OffEx
 Platinum Local Access+ HMO $25 OffEx Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2015 THIS MATRIX IS INTENDED
Platinum Local Access+ HMO $25 OffEx Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2015 THIS MATRIX IS INTENDED
Benefits. Benefits Covered by UnitedHealthcare Community Plan
 Benefits Covered by UnitedHealthcare Community Plan UnitedHealthcare provides all medically necessary covered services under Medicaid SSI. Some services may require a prior authorization. Specific covered
Benefits Covered by UnitedHealthcare Community Plan UnitedHealthcare provides all medically necessary covered services under Medicaid SSI. Some services may require a prior authorization. Specific covered
BCBSM provides administrative claims services only. Your employer or plan sponsor is financially responsible for claims.
 Michigan Catholic Conference Group Number: 71755 Package Code(s): 010 Section Code(s): 1000, 2000 PPO - PPO1, Hearing, Vision ( Exam only) Effective Date: 01/01/2018 Benefits-at-a-glance This is intended
Michigan Catholic Conference Group Number: 71755 Package Code(s): 010 Section Code(s): 1000, 2000 PPO - PPO1, Hearing, Vision ( Exam only) Effective Date: 01/01/2018 Benefits-at-a-glance This is intended
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Appendix A. Prepared Exclusively for The Dow Chemical Company
 Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Traditional Choice (Over Age 65 Retirees - Comprehensive Medical MAP Plus Option
Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Traditional Choice (Over Age 65 Retirees - Comprehensive Medical MAP Plus Option
RFS-7-62 ATTACHMENT E INDIANA CARE SELECT PROGRAM DESCRIPTION AND COVERED BENEFITS
 The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
HUSKY Health Benefits and Prior Authorization Requirements Grid* Hospital Outpatient Effective: January 1, 2012
 Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co-pays for Emergency Room visits Covered no co-pays for Emergency Room visits.
Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co-pays for Emergency Room visits Covered no co-pays for Emergency Room visits.
Your Plan: Marvell Blue Cross HDHP Your Network: BlueCard PPO
 Your Plan: Marvell Blue Cross HDHP Your Network: BlueCard PPO This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
Your Plan: Marvell Blue Cross HDHP Your Network: BlueCard PPO This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about the benefits in your plan, please
Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses
 Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses Extra benefits when you need them Do you have security in knowing you have help handling your medical expenses? You can with
Aetna Fixed Indemnity Plan Helps pay for the costs of everyday medical expenses Extra benefits when you need them Do you have security in knowing you have help handling your medical expenses? You can with
Sample. Riders, if any, are described after the Exclusions and Limitations sections.
 Kaiser Permanente Added Choice with 80%/0% Out-of-network plan 06 Benefits Summary This is only a summary. It does not fully describe your benefit coverage. For complete details on your benefit coverage,
Kaiser Permanente Added Choice with 80%/0% Out-of-network plan 06 Benefits Summary This is only a summary. It does not fully describe your benefit coverage. For complete details on your benefit coverage,
Schedule of Benefits - Indemnity Group - MEDFORD AREA SCHOOL DISTRICT Benefit Year: January 1st through December 31st Effective Date: 01/01/2016
 Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Member s Responsibility: Deductible, Copays, Coinsurance and Maximums
 Benefits-at-a-Glance for GradCare 2018 This is intended as an easy-to-read summary. It is not a contract. Refer to the Your Benefits chapter in the Certificate for an official description of benefits.
Benefits-at-a-Glance for GradCare 2018 This is intended as an easy-to-read summary. It is not a contract. Refer to the Your Benefits chapter in the Certificate for an official description of benefits.
